A Review of Emergency and Disaster Management in the Process of Healthcare Operation Management for Improving Hospital Surgical Intake Capacity
Abstract
1. Introduction
Terminology
2. A Mathematical Framework for Current OM Approaches
2.1. Number of ORs and Flexibility
2.2. Staffing Decisions
2.3. Optimal Block Sizes
2.4. OR Scheduling
2.5. Improving Schedules
2.6. Major Incident Situation Happened; How Do CCUS and Specialist Staff Act?
- (a)
- Capacity of a conventional response at least 20 percent greater than the baseline incentive care unit maximum;
- (b)
- Crisis response is able to expand via at least 200% above baseline incentive care unit max capacity via regional, local, national, and international agencies;
- (c)
- Ability to expand quickly in the event of an emergency by at least 100% above baseline incentive care unit maximum capacity by utilizing local and regional resources.
- -
- Vasopressor administration
- -
- Mechanical ventilation
- -
- Sedation and analgesia
- -
- If recommended by the hospital or a region, the best therapeutics and interventions, such as renal replacement therapy and nutrition for patients who cannot eat by mouth
- -
- IV fluid resuscitation
- -
- Antidote or antimicrobial administration for special disease processes, if applicable
- -
- Algorithms to decrease adverse consequences of critical care and critical illness.
- -
- Training and education of specialists and staff
- -
- A degree of equipment stockpiling or recognition of substitute resources (e.g., use of anesthetic ventilators to supply ventilatory support and NIV machines)
- -
- Recognition of specialists and staff via transferable skills like recovery nurses, respiratory nurses, and previous critical care nurses;
3. A Mathematical Framework for Emergency Departments (EDs)
- What factors can most effectively sculpt (even out) the demand for ED services?
- How can the ED service processes be improved? Improvement is measured with respect to certain performance metrics that we discuss in (Section 3.1).
- How can hospital managers ensure that there is an adequate supply of downstream beds for ED patients who may need additional hospital services?
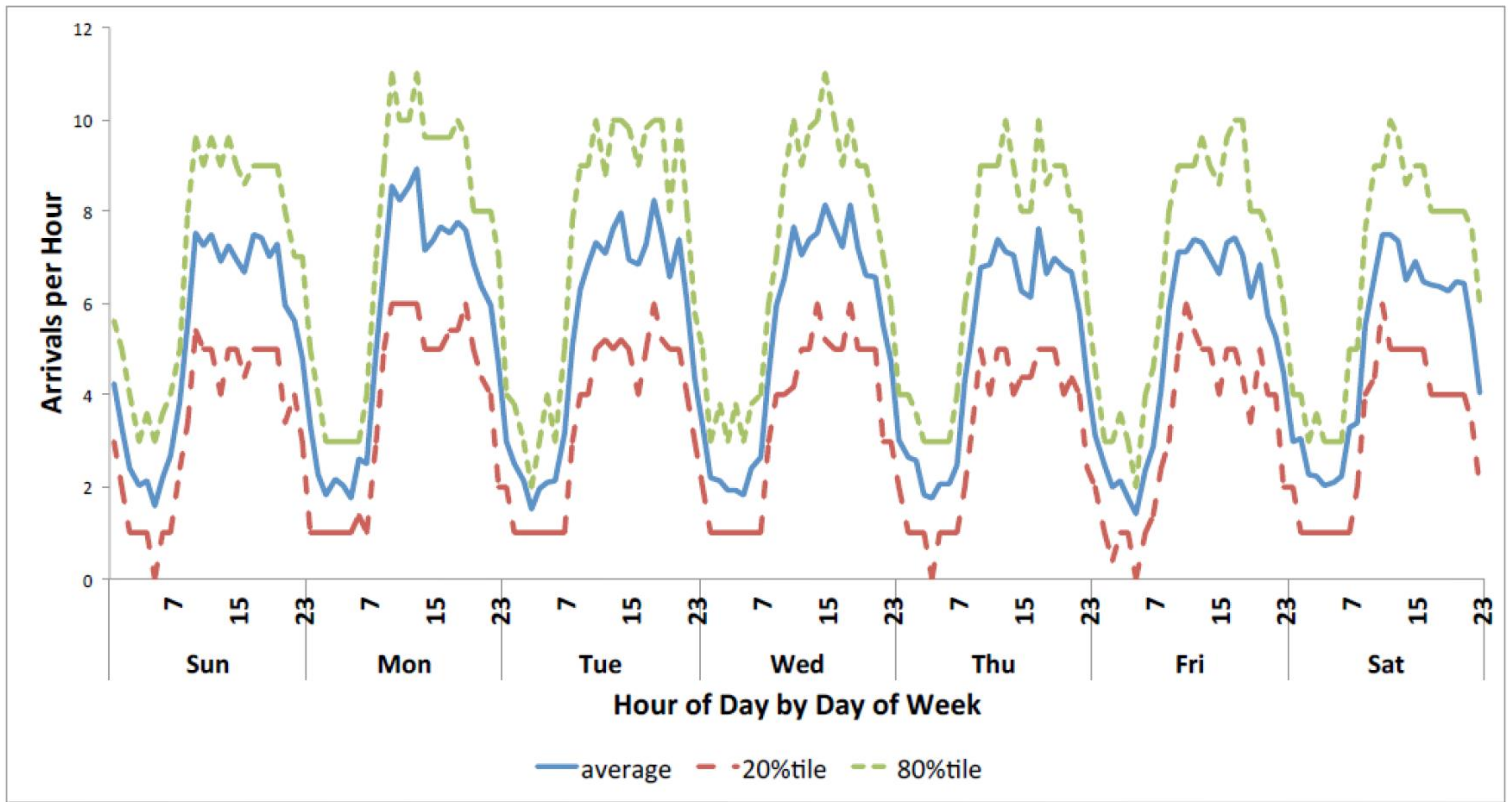
3.1. ED Demand
- Balking-related metrics: include patients leaving without being seen (LWBS) and ambulance diversions [63].
- Capacity-related metrics: frequency of ED census approaching or exceeding the available ED beds or personnel capacity, the daily number of ED visits exceeding a targeted number, and ED nurses or physicians reporting being rushed [66].
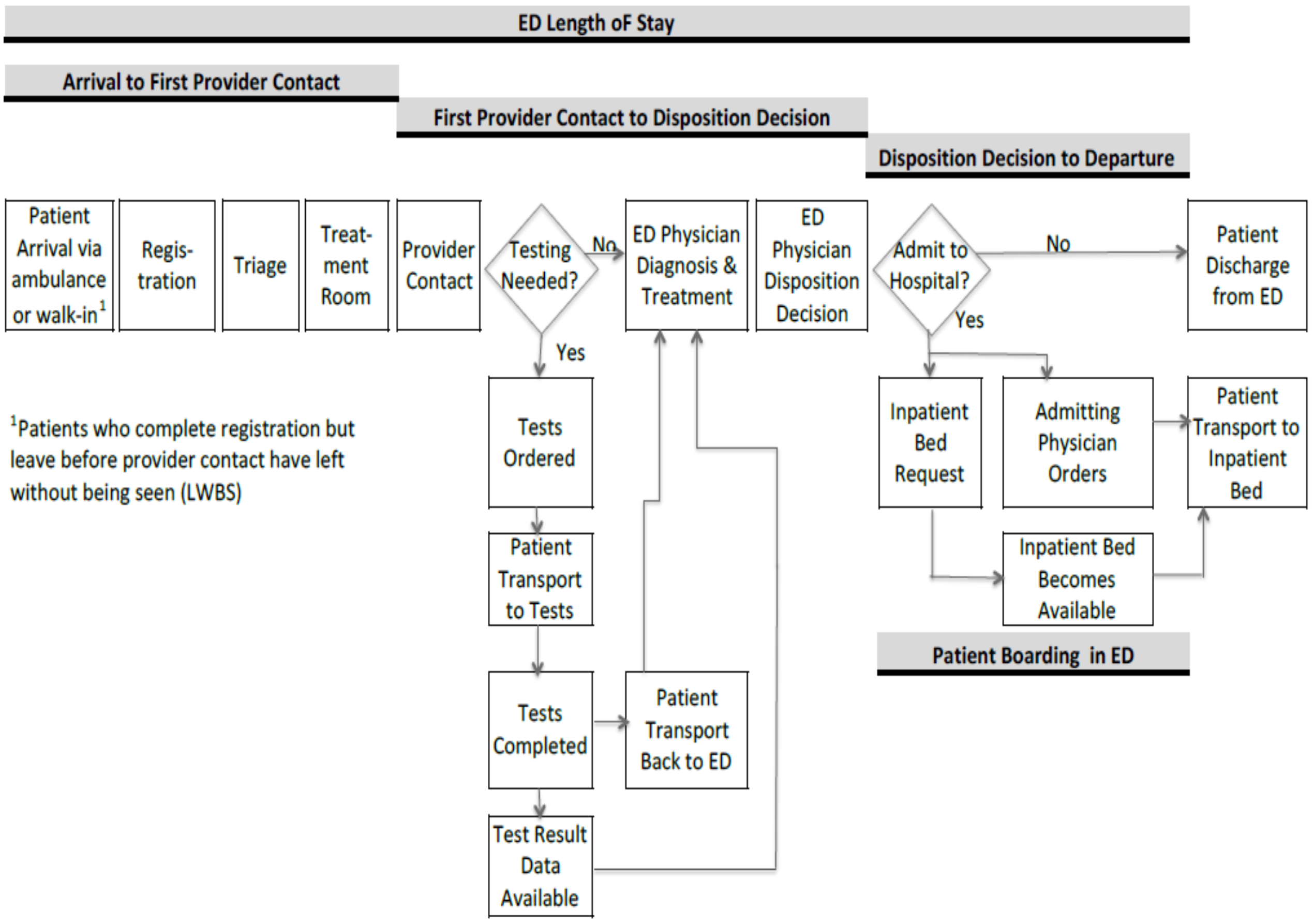
3.2. ED Treatment Process
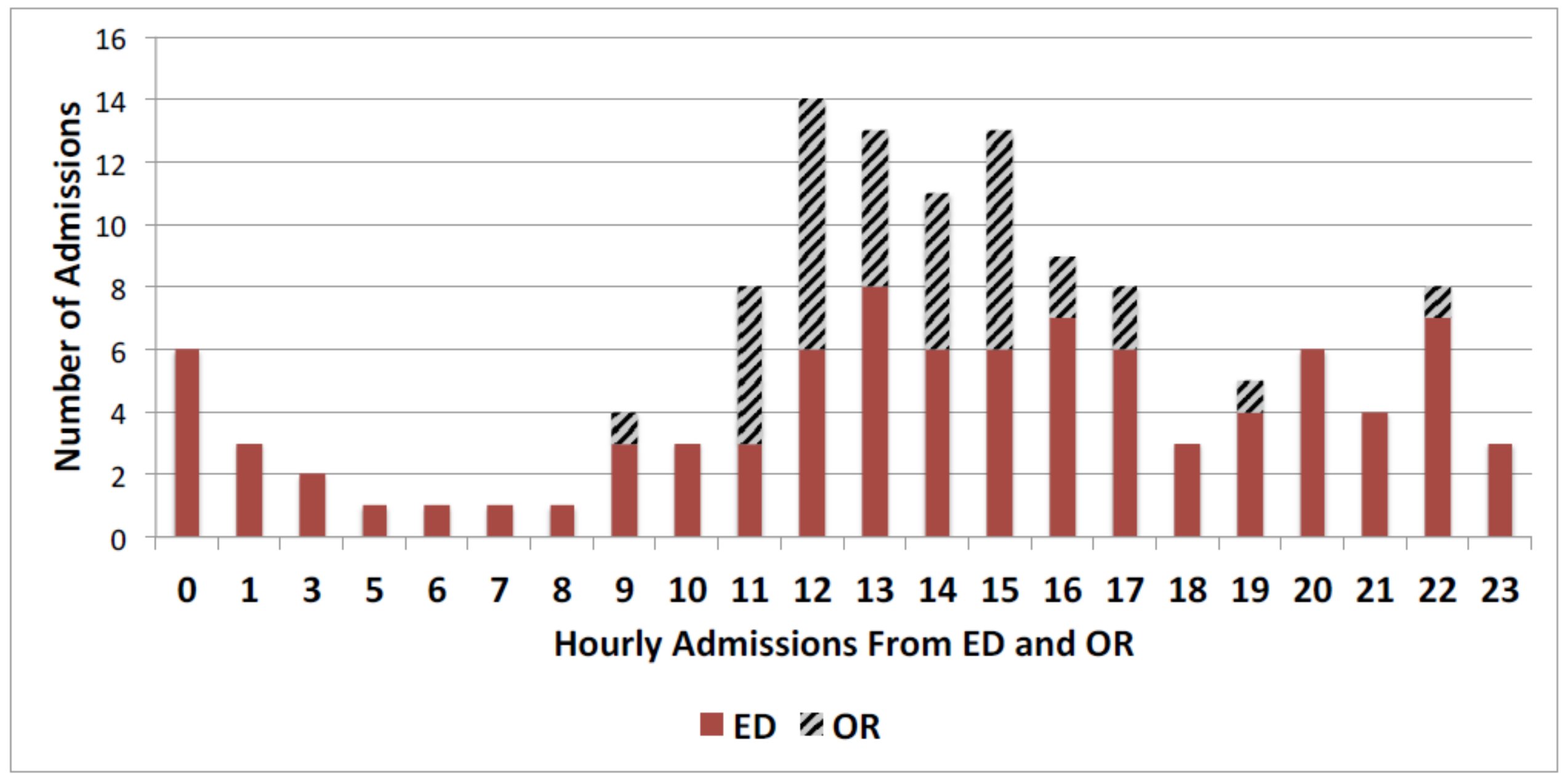
3.3. Downstream Bed Availability
4. OM Opportunities
5. Impact of Unit Size & Scope
5.1. The Impact of the Choice of Performance Metrics
5.2. The Impact of Patient Movement Policies
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Nomenclatures
| A&E | Accident and Emergency |
| ABM | Total Surgery Minutes |
| ADT | Admission, discharge, and transfer system |
| ANA | American Nurses Association |
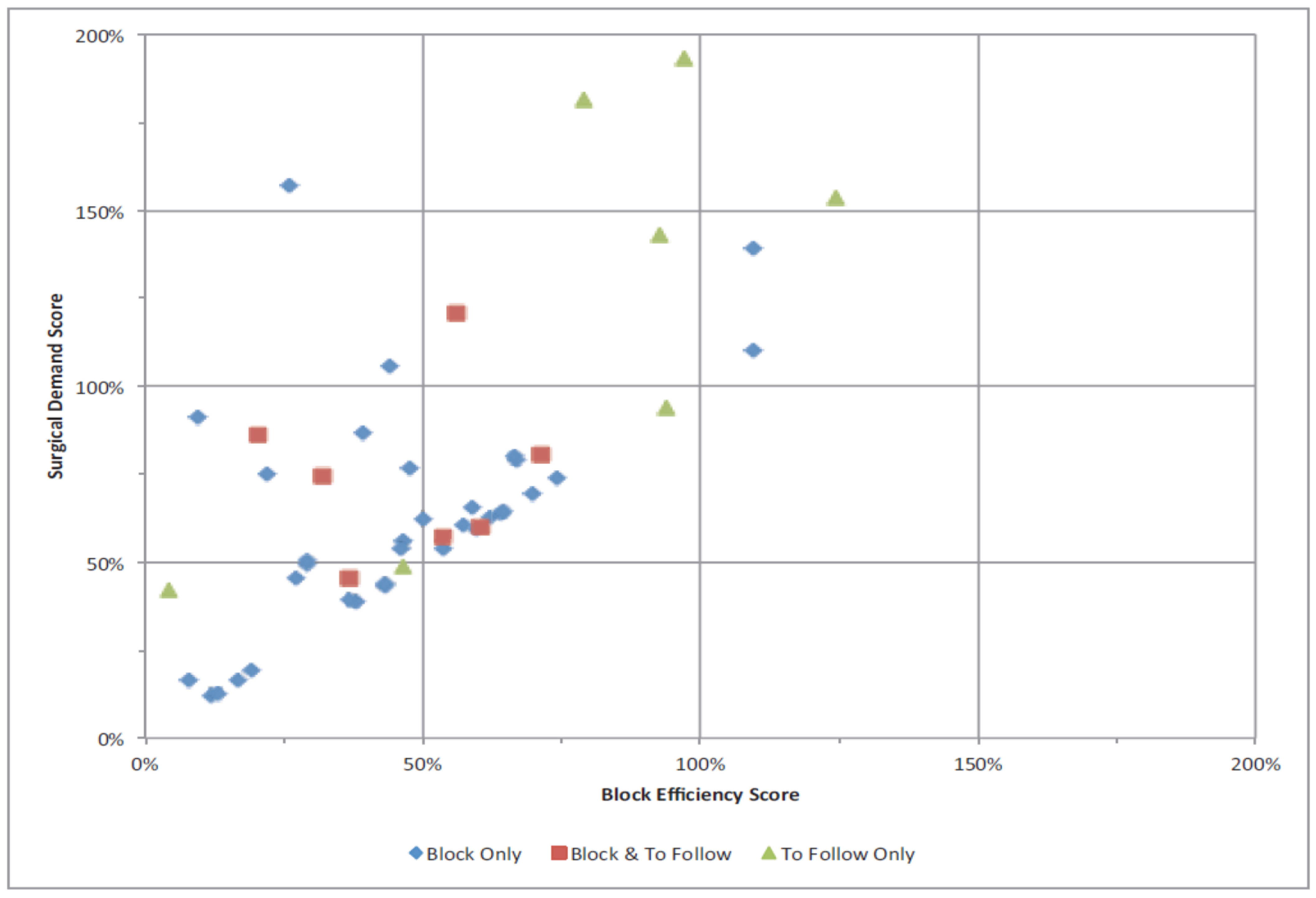
| BES | Block Efficiency Score |
| CCDF | Complementary Cumulative Distribution Function |
| CCU | Critical Care Unit |
| CDF | Cumulative Distribution Function |
| CMS | Centres for Medicare and Medicaid Services |
| CQI | Clinical Quality Indicators |
| EDs | Emergency Department |
| EMTALA | Emergency Medical Treatment & Labor Act |
| ESI | Emergency Severity Index |
| FTE | Full-time equivalent |
| GBD | The Global Burden of Disease Study |
| ICU | Incentive Care Unit |
| LOS | Length of Stay |
| NDNQI | National Database of Nursing Quality Indicators |
| NHPPD | Nursing Hours per Patient Day |
| OM | Operations Management |
| ORs | Operating Room |
| OT | Overtime |
| QED | Quality-in-Emergency-care-Dashboard |
| SDS | Supply Demand Score |
| TDABC | Time-driven activity-based costing |
| TBM | Total in _ Block Minutes |
| TSM | Total Surgery Minutes |
References
- President’s Council of Advisors on Science and Technology (U.S.). Report to the President, Better Health Care and Lower Costs: Accelerating Improvement through Systems Engineering; Technical Report; Executive Office of the President, President’s Council of Advisors on Science and Technology: Washington, DC, USA, 2014.
- Olivares, M.; Terwiesch, C.; Cassorla, L. Structural Estimation of The Newsvendor Model: An Application To Reserving Operating Room Time. Manag. Sci. 2008, 54, 41–55. [Google Scholar] [CrossRef]
- Magerlein, J.M.; Martin, J.B. Surgical Demand Scheduling: A Review. Health Serv. Res. 1978, 13, 418–433. [Google Scholar] [PubMed]
- Blake, J.; Carter, M. Surgical Process Scheduling: A Structured Review. J. Soc. Health Syst. 1997, 5, 17–30. [Google Scholar] [PubMed]
- Gupta, D. Surgical Suites’ Operations Management. Prod. Oper. Manag. 2007, 16, 689–700. [Google Scholar] [CrossRef]
- Gupta, D.; Denton, B. Appointment Scheduling in Health Care: Challenges and Opportunities. IIE Trans. 2008, 40, 800–819. [Google Scholar] [CrossRef]
- Cardoen, B.; Demeulemeester, E.; Beliën, J. Operating Room Planning and Scheduling: A Literature Review. Eur. J. Oper. Res. 2010, 201, 921–932. [Google Scholar] [CrossRef]
- Guerriero, F.; Guido, R. Operational Research in The Management Of The Operating Theatre: A Survey. Health Care Manag. Sci. 2011, 14, 89–114. [Google Scholar] [CrossRef]
- May, J.H.; Spangler, W.E.; Strum, D.P.; Vargas, L.G. The Surgical Scheduling Problem: Current Research and Future Opportunities. Prod. Oper. Manag. 2011, 20, 392–405. [Google Scholar] [CrossRef]
- Dexter, F. Bibliography of Operating Room Management Articles. 2015. Available online: http://www.franklindexter.net/bibliography_TOC.htm (accessed on 13 December 2015).
- Seiden, S.S. On The Online Bin Packing Problem. J. ACM 2002, 49, 640–671. [Google Scholar] [CrossRef]
- Coffman, E.J.; Garey, M.; Johnson, D. Approximation Algorithms for Bin Packing: A Survey. In Approximation Algorithms for NPHard Problems; Hochbaum, D., Ed.; PWS Publishing: Boston, MA, USA, 1999; Chapter 2; p. 02116. [Google Scholar]
- Jackson, R.L. The business of surgery. Health Manag. Technol. 2002, 23, 20–22. [Google Scholar]
- Goldman, J.; Knappenberger, H. How To Determine The Optimum Number Of Operating Rooms. Mod. Hosp. 1968, 111, 114–116. [Google Scholar] [PubMed]
- Lovejoy, W.S.; Li, Y. Hospital Operating Room Capacity Expansion. Manag. Sci. 2002, 48, 1369–1387. [Google Scholar] [CrossRef]
- Buzacott, J.A.; Mandelbaum, M. Flexibility In Manufacturing And Services: Achievements, Insights And Challenges. Flex. Serv. Manuf. J. 2008, 20, 13–58. [Google Scholar] [CrossRef]
- Bassamboo, A.; Randhawa, R.S.; Van Mieghem, J.A. Optimal Flexibility Configurations In Newsvendor Networks: Going Beyond Chaining And Pairing. Manag. Sci. 2010, 56, 1285–1303. [Google Scholar] [CrossRef]
- Johns Hopkins University, Armstrong Institute for Patient Safety and Quality. Improving the Emergency Department Discharge Process: Environmental Scan Report; Technical report; Johns Hopkins University: Baltimore, MD, USA, 2014. Available online: http://www.ahrq.gov/professionals/systems/hospital/edenvironmentalscan/edenvironmentalscan.pdf (accessed on 25 December 2015).
- Iravani, S.M.; Van Oyen, M.; Sims, K.T. Structural Flexibility: A New Perspective on the Design of Manufacturing and Service Operations. Manag. Sci. 2005, 51, 151–166. [Google Scholar] [CrossRef]
- Chen, X.; Zhang, J.; Zhou, Y. Optimal Sparse Designs for Process Flexibility via Probabilistic Expanders. 2014. Available online: http://ssrn.com/abstract=2400768 (accessed on 18 August 2014).
- Kesavan, S.; Staats, B.R.; Gilland, W. Volume Flexibility in Services: The Costs and Benefits of Flexible Labor Resources. Manag. Sci. 2014, 60, 1884–1906. [Google Scholar] [CrossRef]
- Bandi, C.; Bertsimas, D. Tractable stochastic analysis in high dimensions via robust optimization. Math. Program. 2012, 134, 23–70. [Google Scholar] [CrossRef]
- Miller, H.E.; Pierskalla, W.P.; Rath, G.J. Nurse Scheduling Using Mathematical Programming. Oper. Res. 1976, 24, 857–870. [Google Scholar] [CrossRef]
- Yankovic, N.; Green, L.V. Identifying Good Nursing Levels: A Queuing Approach. Oper. Res. 2011, 59, 942–955. [Google Scholar] [CrossRef]
- Véricourt, F.D.; Jennings, O.B. Nurse Staffing in Medical Units: A Queueing Perspective. Oper. Res. 2011, 59, 1320–1331. [Google Scholar] [CrossRef]
- Lim, G.J.; Mobasher, A.; Kardar, L.; Côté, M.J. Nurse Scheduling. In Handbook of Healthcare System Scheduling: Delivering Care When and Where It Is Needed; Hall, R.W., Ed.; Springer: New York, NY, USA, 2011; Chapter 3; pp. 31–64. [Google Scholar]
- Bard, J.F.; Purnomo, H.W. Preference Scheduling for Nurses Using Column Generation. Eur. J. Oper. Res. 2005, 164, 510–534. [Google Scholar] [CrossRef]
- Bard, J.F.; Purnomo, H.W. Hospital-Wide Reactive Scheduling of Nurses with Preference Considerations. IIE Trans. 2005, 37, 589–608b. [Google Scholar] [CrossRef]
- McManus, M.; Long, M.; Cooper, A.; Mandell, J.; Berwick, D.; Pagano, M.; Litvak, E. Variability in Surgical Caseload and Access to Intensive Care Services. Anesthesiology 2003, 98, 1491–1496. [Google Scholar] [CrossRef] [PubMed]
- Heydari, M.; Lai, K.K. A study on risk and expense evaluation of agility supply management of machinery. Discret. Dyn. Nat. Soc. 2020, 2020, 7030642. [Google Scholar] [CrossRef]
- Heydari, M.; Lai, K.K.; Xiaohu, Z. How to Manage Red Alert in Emergency and Disaster Unit in the Hospital? Evidence From London. Front. Public Health 2021, 9, 634417. [Google Scholar] [CrossRef] [PubMed]
- Heydari, M.; Lai, K.K.; Zhou, X. Creating sustainable order fulfillment processes through managing the risk: Evidence from the disposable products industry. Sustainability 2020, 12, 2871. [Google Scholar] [CrossRef]
- Heydari, M.; Xiaohu, Z.; Lai, K.K.; Yuxi, Z. Evaluation of Organizational Performance Strategies. Proc. Natl. Aviat. Univ. 2020, 82, 77–93. [Google Scholar] [CrossRef]
- Denton, B.; Gupta, D. A Sequential Bounding Approach for Optimal Appointment Scheduling. IIE Trans. 2003, 35, 1003–1016. [Google Scholar] [CrossRef]
- Hans, E.; Wullink, G.; van Houdenhoven, M.; Kazemier, G. Robust Surgery Loading. Eur. J. Oper. Res. 2008, 185, 1038–1050. [Google Scholar] [CrossRef]
- Begen, M.; Queyranne, M. Appointment Scheduling with Discrete Random Durations. Math. Oper. Res. 2009, 41, 845–854. [Google Scholar]
- Begen, M.; Levi, R.; Queyranne, M. Technical Note: A Sampling-Based Approach to Appointment Scheduling. Oper. Res. 2012, 60, 675–681. [Google Scholar] [CrossRef]
- Kong, Q.; Lee, C.; Teo, C.; Zheng, Z. Scheduling Arrivals to A Stochastic Service Delivery System Using Copositive Cones. Oper. Res. 2013, 61, 711–726. [Google Scholar] [CrossRef]
- Gerchak, Y.; Gupta, D.; Henig, M. Reservation Planning for Elective Surgery Under Uncertain Demand for Emergency Surgery. Manag. Sci. 1996, 42, 321–334. [Google Scholar] [CrossRef]
- Li, F.; Gupta, D.; Potthoff, S. Improving Operating Room Schedules. Health Care Manag. Sci. 2015, 19, 261–278. [Google Scholar] [CrossRef] [PubMed]
- National Center for Health Statistics. Health, United States 2012: With Special Feature on Emergency Care; Technical report; National Center for Health Statistics: Hyattsville, MD, USA, 2013.
- Hsia, R.; Kellermann, A.; Yu-Chu, S. Factors Associated with Closures of Emergency Departments in the United States. JAMA 2011, 305, 1978–1985. [Google Scholar] [CrossRef]
- Roberge, D.; Pineault, R.; Larouche, D.; Poirier, L.R. The Continuing Saga of Emergency Room Overcrowding: Are We Aiming at the Right Target? Healthc. Policy 2010, 5, 27–39. [Google Scholar] [CrossRef][Green Version]
- Mason, S. Keynote Address: United Kingdom Experiences of Evaluating Performance and Quality in Emergency Medicine. Acad. Emerg. Med. 2011, 18, 1234–1238. [Google Scholar] [CrossRef]
- Hassan, H.; McMillan, P.; Walsh, C.; Higginson, I. The Drive for Quality: How to Achieve Safe, Sustainable Care in Our Emergency Departments? System Benchmarks and Recommendations; Technical Report; The College of Emergency Medicine, 2013; Available online: http://www.collemergencymed.ac.uk/Shop-Floor/ProfessionalAffairs/QualityintheEmergencyDepartment (accessed on 2 March 2012).
- Heyworth, J. Emergency Medicine-Quality Indicators: The United Kingdom Perspective. Acad. Emerg. Med. 2011, 18, 1239–1241. [Google Scholar] [CrossRef]
- Jayaprakash, N.; O’Sullivan, R.; Bey, T.; Ahmed, S.S.; Lotfipour, S. Crowding and Delivery of Healthcare in Emergency Departments: The European Perspective. West. J. Emerg. Med. 2009, 10, 233–239. [Google Scholar]
- Moineddin, R.; Meaney, C.; Agha, M.; Zagorski, B.; Glazier, R.H. Modeling Factors Influencing the Demand for Emergency Department Services in Ontario: A Comparison of Methods. BMC Emerg. Med. 2011, 11, 13. [Google Scholar] [CrossRef]
- Ovens, H. Ed Overcrowding: The Ontario Approach. Acad. Emerg. Med. 2011, 18, 1242–1245. [Google Scholar] [CrossRef]
- Pines, J.M.; Hilton, J.A.; Weber, E.J.; Alkemade, A.J.; Al Shabanah, H.; Anderson, P.D.; Bernhard, M.; Bertini, A.; Gries, A.; Ferrandiz, S.; et al. International Perspectives on Emergency Department Crowding. Acad. Emerg. Med. 2011, 18, 1358–1370. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, T.; Nishida, M.; Suzuki, Y.; Kobayashi, K. The Imminent Healthcare and Emergency Care Crisis in Japan. West. J. Emerg. Med. 2008, 9, 91–96. [Google Scholar] [PubMed]
- Allon, G.; Deo, S.; Lin, W. The Impact of Size and Occupancy of Hospital on the Extent of Ambulance Diversion: Theory and Evidence. Oper. Res. 2013, 61, 544–562. [Google Scholar] [CrossRef]
- Flores-Mateo, G.; Violan-Fors, C.; Carrillo-Santisteve, P.; Peiró, S.; Argimon, J.-M. Effectiveness of Organizational Interventions to Reduce Emergency Department Utilization: A Systematic Review. PLoS ONE 2012, 7, e35903. [Google Scholar] [CrossRef] [PubMed]
- Morganti, K.G.; Bauhoff, S.; Blanchard, J.C.; Abir, M. The Evolving Role of Emergency Departments in the United States; Technical Report; RAND Corporation: Santa Monica, CA, USA, 2013. [Google Scholar]
- O’Malley, A.S. After-Hours Access to Primary Care Practices Linked with Lower Emergency Department Use and Less Unmet Medical Need. Health Aff. 2013, 32, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Yaremchuk, K.; Schwartz, J.; Nelson, M. Copayment Levels and Their Influence on Patient Behavior in Emergency Room Utilization In An HMP Population. J. Manag. Care Med. 2010, 13, 27–31. [Google Scholar]
- Pitts, S.R.; Carrier, E.R.; Rich, E.C.; Kellermann, A.L. Where Americans Get Acute Care: Increasingly, It’s Not at Their Doctor’s Office. Health Aff. 2010, 29, 1620–1629. [Google Scholar] [CrossRef]
- DeLia, D.; Cantor, J. Emergency Department Utilization and Capacity; Research Synthesis Report, No. 17; Technical Report 17; 2009. Available online: http://www.rwjf.org/content/dam/farm/reports/reports/2009/rwjf43565 (accessed on 25 December 2015).
- Zibulewsky, J. The Emergency Medical Treatment and Active Labor Act (EMTALA): What It Is and What It Means for Physicians. Proc. Bayl. Univ. Med. Cent. 2001, 14, 339–346. [Google Scholar] [CrossRef]
- Robertson-Steel, I. Evolution of triage systems. Emerg. Med. J. EMJ 2006, 23, 154–155. [Google Scholar] [CrossRef]
- Gilboy, N.; Paula, T.; Travers, D.; Rosenau, A.M. Emergency Severity Index (ESI): A Triage Tool for Emergency Department Care, Version 4; AHRQ Publication No. 12-0014; Agency for Healthcare Research and Quality: Rockville, MD, USA, 2011. Available online: http://www.ahrq.gov/professionals/systems/hospital/esi/index.html (accessed on 11 November 2015).
- Rosen, M.; Dietz, A.; Yang, T.; Priebe, C.; Pronovost, P. An Integrative Framework for Sensor-Based Measurement of Teamwork in Healthcare. J. Am. Med Inform. Assoc. 2014, 22, 11–18. [Google Scholar] [CrossRef] [PubMed]
- Eitel, D.R.; Rudkin, S.E.; Malvehy, M.A.; Killeen, J.P.; Pines, J.M. Improving Service Quality by Understanding Emergency Department Flow: A White Paper and Position Statement Prepared for The American Academy of Emergency Medicine. J. Emerg. Med. 2010, 38, 70–79. [Google Scholar] [CrossRef] [PubMed]
- Handel, D.; Epstein, S.; Khare, R.; Abernethy, D.; Klauer, K.; Pilgrim, R.; Soremekun, O.; Sayan, O. Interventions to Improve the Timeliness of Emergency Care. Acad. Emerg. Med. 2011, 18, 1295–1302. [Google Scholar] [CrossRef]
- Welch, S. Using Data to Drive Emergency Department Design: A Metasynthesis. Health Environ. Res. Des. J. 2012, 5, 26–45. [Google Scholar] [CrossRef] [PubMed]
- Hwang, U.; Concato, J. Care in The Emergency Department: How Crowded Is Overcrowded? Acad. Emerg. Med. 2004, 11, 1097–1101. [Google Scholar] [CrossRef] [PubMed]
- McHugh, M.; Dyke, K.V.; McClelland, M.; Moss, D. Improving Patient Flow and Reducing Emergency Department Crowding: A Guide for Hospitals; Technical Report, Agency for Healthcare Research and Quality Publication No. 11(12)-0094; AHRQ: Rockville, MD, USA, 2011.
- Pricewaterhouse Coopers. The Price of Excess: Identifying Waste in Healthcare Spending; Technical Report; Pricewaterhouse Coopers, 2011; Available online: https://www.pwc.com/us/en/healthcare/publications/the-price-ofexcess.html (accessed on 25 April 2011).
- Wiler, J.; Beck, D.; Asplin, B.; Granovsky, M.; Moorhead, J.; Pilgrim, R.; Schuur, J. Episodes of Care: Is Emergency Medicine Ready? Ann. Emerg. Med. 2012, 59, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Chronic Diseases: The Power to Prevent, The Call to Control, At-A-Glance 2009; Technical Report; U.S. Department of Health and Human Services, 2009. Available online: https://www.cdc.gov/nccdphp/publications/AAG/pdf/chronic.pdf (accessed on 10 June 2009).
- Carrus, B.; Corbett, S.; Khandelwal, D. A Hospital-Wide Strategy for Fixing Emergency-Department Overcrowding; Technical Report; McKinsey & Company, 2010; Available online: http://www.mckinsey.com/insights/health_systems_and_services/a_hospital-wide_strategy_for_fixing_emergency-department_overcrowding (accessed on 25 December 2015).
- Hoot, N.R.; Aronsky, D. Systematic Review of Emergency Department Crowding: Causes, Effects, And Solutions. Ann. Emerg. Med. 2008, 52, 126–136. [Google Scholar] [CrossRef]
- Pham, J.C.; Patel, R.; Millin, M.G.; Kirsch, T.D.; Chanmugam, A. The Effects of Ambulance Diversion: A Comprehensive Review. Acad. Emerg. Med. 2006, 13, 1220–1227. [Google Scholar] [CrossRef]
- Peck, J.S.; Benneyan, J.C.; Nightingale, D.J.; Gaehde, S.A. Predicting Emergency Department Inpatient Admissions To Improve Same-Day Patient Flow. Acad. Emerg. Med. 2012, 19, E1045–E1054. [Google Scholar] [CrossRef]
- Peck, J.S.; Gaehde, S.A.; Nightingale, D.J.; Gelman, D.Y.; Huckins, D.S.; Lemons, M.F.; Dickson, E.W.; Benneyan, J.C. Generalizability of A Simple Approach for Predicting Hospital Admission from An Emergency Department. Acad. Emerg. Med. 2013, 20, 1156–1163. [Google Scholar] [CrossRef]
- Saghafian, S.; Hopp, W.J.; Oyen, M.P.V.; Desmond, J.S.; Steven, L.; Complexity-augmented, S.L.K.; Kronick, S.L. Complexity-Augmented Triage: A Tool for Improving Patient Safety and Operational Efficiency. Manuf. Serv. Oper. Manag. 2014, 16, 329–345. [Google Scholar] [CrossRef]
- Betcheva, L.; Erhun, F.; Jiang, H. OM Forum—Supply chain thinking in healthcare: Lessons and outlooks. Manuf. Serv. Oper. Manag. 2021, 23, 1333–1353. [Google Scholar] [CrossRef]
- Stickels, C.P.; Nadarajah, R.; Gale, C.P.; Jiang, H.; Sharkey, K.J.; Gibbison, B.; Holliman, N.; Lombardo, S.; Schewe, L.; Sommacal, M.; et al. Aortic stenosis post-COVID-19: A mathematical model on waiting lists and mortality. BMJ Open 2022, 12, e059309. [Google Scholar] [CrossRef] [PubMed]
- Ali, I.; Kannan, D. Mapping research on healthcare operations and supply chain management: A topic modelling-based literature review. Ann. Oper. Res. 2022, 315, 29–55. [Google Scholar] [CrossRef] [PubMed]
- Yao, W.; Chu, C.; Li, Z. The Adoption and Implementation of RFID Technologies In Healthcare: A Literature Review. J. Med. Syst. 2012, 36, 3507–3525. [Google Scholar] [CrossRef]
- Plambeck, E.; Mohsen, B.; Erjie, A.; Sara, K.; Mike, A. Forecasting Emergency Department Wait Times. No. 3187. 2014. Available online: https://www.gsb.stanford.edu/faculty-research/publications/accurate-ed-wait-time-prediction (accessed on 17 July 2015).
- American Hospital Association. The State of America’s Hospitals—Taking the Pulse. In Results of AHA Survey of Hospital Leaders, March/April 2010; Technical Report; American Hospital Association, 2010; Available online: http://www.aha.org/research/rc/stat-studies/Studies.shtml (accessed on 15 November 2015).
- Lang, T.A.; Hodge, M.; Olson, V.; Romano, P.S.; Kravitz, R.L. Nurse—Patient Ratios: A Systematic Review on the Effects of Nurse Staffing on Patient, Nurse Employee, and Hospital Outcomes. J. Nurs. Adm. 2004, 34, 326–337. [Google Scholar] [CrossRef]
- Rae, P.J.; Pearce, S.; Greaves, P.J.; Dall’Ora, C.; Griffiths, P.; Endacott, R. Outcomes sensitive to critical care nurse staffing levels: A systematic review. Intensive Crit. Care Nurs. 2021, 67, 103110. [Google Scholar] [CrossRef]
- Finkler, S.A. Essentials of Cost Accounting for Health Care Organizations; Aspen Publishers, Inc.: Boston, MA, USA, 1994. [Google Scholar]
- The Truth about Nursing org. Why Are Those Nurses Hogging So Much of The Hospital Budget?! 25 March 2011. Available online: http://www.truthaboutnursing.org/news/2011/mar/25_hogging.html (accessed on 23 August 2014).
- Unruh, L. Nurse Staffing and Patient, Nurse, And Financial Outcomes. Am. J. Nurs. 2008, 108, 62–71. [Google Scholar] [CrossRef]
- Adynski, G.I.; Sherwood, G.; Ikharo, E.; Tran, A.; Jones, C.B. Outpatient Nurse Staffing Relationship with Organizational, Nurse and Patient Outcomes: A Scoping Review. Int. J. Nurs. Stud. Adv. 2022, 4, 100064. [Google Scholar] [CrossRef]
- Needleman, J.; Buerhaus, P.; Mattke, S.; Stewart, M.; Zelevinsky, K. Nurse-Staffing Levels and the Quality of Care in Hospitals. N. Engl. J. Med. 2002, 346, 1715–1722. [Google Scholar] [CrossRef]
- Dall’Ora, C.; Saville, C.; Rubbo, B.; Turner, L.; Jones, J.; Griffiths, P. Nurse staffing levels and patient outcomes: A systematic review of longitudinal studies. Int. J. Nurs. Stud. 2022, 134, 104311. [Google Scholar] [CrossRef] [PubMed]
- OECD. Health at a Glance 2013: OECD Indicators; Technical Report; OECD Publishing: Paris, France, 2013. [Google Scholar]
- GBD 2013 Mortality and Causes of Death Collaborators. Global, Regional, And National Age-Sex-Specific All-Cause and Cause-Specific Mortality For 240 Causes of Death, 1990–2013: A Systematic Analysis for The Global Burden of Disease Study 2013. Lancet 2015, 385, 117–171. [Google Scholar] [CrossRef]
- The Henry J Kaiser Family Foundation. Distribution Of National Health Expenditures, By Type of Service (In Billions). 2014. Available online: http://kff.org/health-costs/slide/distribution-of-national-healthexpenditures-by-type-of-service-in-billions-2012/ (accessed on 21 October 2015).
- Kroneman, M.; Siegers, J. The Effect of Hospital Bed Reduction on the Use of Beds: A Comparative Study of 10 European Countries. Soc. Sci. Med. 2004, 59, 1731–1740. [Google Scholar] [CrossRef] [PubMed]
- Morgan, D.; Astolfi, R. Health Spending Growth at Zero: Which Countries, Which Sectors Are Most Affected. In OECD Health Working Papers; Technical Report No. 60; OECD Publishing: Paris, France, 2013. [Google Scholar]
- Medicare Payment Advisory Committee. Report to the Congress: Medicare Payment Policy; Technical Report; MEDPAC: Washington, DC, USA, 2014.
- Weaver, C.; Mathews, A.; McGinty, T. Medicare Rules Reshape Hospital Admissions; Return-Visit Rate Drops, But Change in Billing Tactics Skews Numbers. Wall Str. J. 2015. Available online: http://search.proquest.com.ezp3.lib.umn.edu/docview/1738104542/74F154E37D6D4459PQ/2?accountid=14586 (accessed on 2 December 2015).
- Heydari, M.D.; Lai, K.K. The Effect Employee Commitment on Service Performance through a Mediating Function of Organizational Citizenship Behaviour Using Servqual and Collaborative Filtering Modeling: Evidence From China’s Hospitality Industry. J. Tour. Hosp. 2019, 8, 2167-0269. [Google Scholar] [CrossRef]
- Heydari, M.; Xiaohu, Z.; Saeidi, M.; Lai, K.K.; Shang, Y.; Yuxi, Z. Analysis of the role of social support-cognitive psychology and emotional process approach. Eur. J. Transl. Myol. 2020, 30, 8975. [Google Scholar] [CrossRef]
- Adam, S.K.; Osborne, S. Critical Care Nursing: Science and Practice; Oxford University Press: Oxford, UK, 2005. [Google Scholar]
- Avidan, V.; Hersch, M.; Spira, R.M.; Einav, S.; Goldberg, S.; Schecter, W. Civilian hospital response to a mass casualty event: The role of the intensive care unit. J. Trauma Acute Care Surg. 2007, 62, 1234–1239. [Google Scholar] [CrossRef]
- Rubinson, L.; Hick, J.L.; Hanfling, D.G.; Devereaux, A.V.; Dichter, J.R.; Christian, M.D.; Talmor, D.; Medina, J.; Curtis, J.R.; Geiling, J.A. Definitive care for the critically ill during a disaster: A framework for optimizing critical care surge capacity: From a Task Force for Mass Critical Care summit meeting, January 26–27, 2007, Chicago, IL. Chest 2008, 133, 18S–31S. [Google Scholar]
- DeBoisblanc, B.P. Black Hawk, please come down: Reflections on a hospital’s struggle to survive in the wake of Hurricane Katrina. Am. J. Respir. Crit. Care Med. 2005, 172, 1239–1240. [Google Scholar] [CrossRef]
- Christian, M.D.; Sprung, C.L.; King, M.A.; Dichter, J.R.; Kissoon, N.; Devereaux, A.V.; Gomersall, C.D. Triage: Care of the critically ill and injured during pandemics and disasters: CHEST consensus statement. Chest 2014, 146, e61S–e74S. [Google Scholar] [CrossRef]
- Awad, A.; Trenfield, S.J.; Pollard, T.D.; Ong, J.J.; Elbadawi, M.; McCoubrey, L.E.; Goyanes, A.; Gaisford, S.; Basit, A.W. Connected healthcare: Improving patient care using digital health technologies. Adv. Drug Deliv. Rev. 2021, 178, 113958. [Google Scholar] [CrossRef]
- Heydari, M.; Fan, Y.; Saeidi, M.; Lai, K.K.; Li, X.; Chen, Y.; Yang, J.; Cai, X.; Zhang, X. Emergency and Disaster Logistics Processes for Managing ORs Capacity in Hospitals: Evidence from United States. Int. J. Bus. Manag. 2022, 1, 63–85. [Google Scholar]
- Childers, C.P.; Maggard-Gibbons, M. Understanding costs of care in the operating room. JAMA Surg. 2018, 153, e176233. [Google Scholar] [CrossRef] [PubMed]
- Guzman, M.J.; Gitelis, M.E.; Linn, J.G.; Ujiki, M.B.; Waskerwitz, M.; Umanskiy, K.; Muldoon, J.P. A model of cost reduction and standardization: Improved cost savings while maintaining the quality of care. Dis. Colon Rectum 2015, 58, 1104–1107. [Google Scholar] [CrossRef] [PubMed]
- Yangyang, R.Y.; Abbas, P.I.; Smith, C.M.; Carberry, K.E.; Ren, H.; Patel, B.; Lopez, M.E. Time-driven activity-based costing to identify opportunities for cost reduction in pediatric appendectomy. J. Pediatr. Surg. 2016, 51, 1962–1966. [Google Scholar]

| Selected Day of Week | Shift Types | Shift Start Times | ||||||
|---|---|---|---|---|---|---|---|---|
| 7:30 | 7:45 | 8:00 | 8:15 | 8:30 | 8: 45 | 9:00 | ||
| Current | 8 h | 10 | n.a. | n.a. | n.a. | n.a. | n.a. | n.a. |
| 10 h | n.a. | n.a. | n.a. | n.a. | n.a. | n.a. | n.a. | |
| 12 h | 6 | n.a. | n.a. | n.a. | n.a. | n.a. | n.a. | |
| Proposed | 8 h | 3 | n.a. | 3 | n.a. | n.a. | n.a. | 2 |
| 10 h | n.a. | n.a. | 1 | n.a. | 1 | n.a. | n.a. | |
| 12 h | n.a. | 1 | n.a. | n.a. | n.a. | n.a. | n.a. | |
| Service | DoW | n | B (min) | Initial Config | Revised Config | W (min) | A/W | Initial Unit | Revised Unit | |
|---|---|---|---|---|---|---|---|---|---|---|
| A | M | 49 | 2 | 900 | 7:30–15:00 7:30–15:00 | 7:30–12:00 7:30–18:00 | 46,588 | 0.95 | 55 | 66 |
| A | T | 50 | 2 | 900 | 7:30–15:00 7:30–15:00 | 7:30–14:00 7:30–16:00 | 50,438 | 0.89 | 62 | 69 |
| A | W | 51 | 2 | 900 | 7:30–15:00 7:30–15:00 | 7:30–13:45 7:30–16:15 | 46,115 | 1.00 | 53 | 65 |
| A | TR | 50 | 2 | 1020 | 7:30–15:00 7:30–17:00 | 7:30–13:30 7:30–18:30 | 48,119 | 1.06 | 59 | 61 |
| A | F | 49 | 2 | 900 | 7:30–15:00 7:30–15:00 | 7:30–13:30 7:30–16:30 | 47,134 | 0.94 | 53 | 61 |
| B | F | 45 | 2 | 1020 | 7:30–16:00 8:30–17:00 | 7:30–15:00 7:30–17:00 | 28,620 | 1.60 | 49 | 51 |
| C | M | 27 | 2 | 720 | 9:30–13:30 9:00–17:00 | 9:00–13:30 10:00–17:30 | 11,876 | 1.64 | 40 | 45 |
| C | T | 34 | 2 | 720 | 9:00–17:00 11:00–15:00 | 9:00–17:00 10:30–14:30 | 14,946 | 1.64 | 40 | 50 |
| ESI Level | Description |
|---|---|
| ESI Level 1 | The patient requires immediate life-saving intervention (1–3% of all ED patients) |
| ESI Level 2 | The patient should not wait to be seen if they are in a high-risk situation, are confused, lethargic, or disoriented, or are in excruciating pain or distress (20–30% of all ED patients) |
| ESI Level 3 | The patient is not Level 1 or Level 2, has vital signs within the accepted range for the patient’s age, and is predicted to require two or more resources, such as labs; diagnostic testing; intravenous fluids; intravenous, intramuscular or nebulized medications; specialty consultation; and/or a simple procedure or complex procedure (30–40% of all ED patients) |
| ESI Level 4 | The patient has vital signs within the accepted range for the patient’s age and is predicted to use one resource. Levels 4 and 5 combined comprise 20–35% of all ED patients. Level 4 is an appropriate level to stream through the fast track. |
| ESI Level 5 | The patient has vital signs within the accepted range for the patient’s age and is predicted to require no resources. Levels 4 and 5 combined comprise 20–35% of all ED patients. Level 5 is an appropriate level to stream through fast-track. |
| QED Indicators ([63], p. 31), (CQI; United Kingdom) | CMS Indicators McHugh et al. ([67], p. 5), (United States) |
| Time in the ED—% less than 4 h | The median patient time from ED arrival to ED departure for patients who were discharged |
| % of patients with ED stay exceeding 6 h | Median time from ED arrival to ED departure for admitted patients |
| Time for arrival to treatment by a decision-maker—% within 60 min or less | Door-to-diagnostic time, i.e., time to evaluation by a qualified medical professional |
| % Left Without Being Seen | The patient left before being seen |
| % Unplanned re-attendance to the ED within 7 days | No equivalent metric |
| No equivalent metric | The average amount of time admitted patients spend between being accepted and leaving |
| Time to initial assessment for patients arriving by ambulance—% less than 15 min | No equivalent metric |
| Absentee Rate | Metric | Poisson LOS | Geometric LOS | ||
|---|---|---|---|---|---|
| Targeting | Static Priority | Targeting | Static Priority | ||
| 0% | Min OT/Shift | 0.83 | 0.95 | 0.54 | 0.61 |
| # Unserved/Shift | 0.74 | 0.65 | 0.49 | 0.43 | |
| Movement | 0.43 | 0.4 | 0.34 | 0.25 | |
| 10% | Min OT/Shift | 2.37 | 2.38 | 1.75 | 1.74 |
| # Unserved/Shift | 1.17 | 1.21 | 0.86 | 0.92 | |
| Movement | 0.75 | 0.49 | 0.87 | 0.57 | |
| 20% | Min OT/Shift | 4.22 | 4.18 | 3.53 | 3.48 |
| # Unserved/Shift | 1.45 | 1.58 | 1.21 | 1.34 | |
| Movement | 0.61 | 0.39 | 0.76 | 0.45 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Heydari, M.; Lai, K.K.; Fan, Y.; Li, X. A Review of Emergency and Disaster Management in the Process of Healthcare Operation Management for Improving Hospital Surgical Intake Capacity. Mathematics 2022, 10, 2784. https://doi.org/10.3390/math10152784
Heydari M, Lai KK, Fan Y, Li X. A Review of Emergency and Disaster Management in the Process of Healthcare Operation Management for Improving Hospital Surgical Intake Capacity. Mathematics. 2022; 10(15):2784. https://doi.org/10.3390/math10152784
Chicago/Turabian StyleHeydari, Mohammad, Kin Keung Lai, Yanan Fan, and Xiaoyang Li. 2022. "A Review of Emergency and Disaster Management in the Process of Healthcare Operation Management for Improving Hospital Surgical Intake Capacity" Mathematics 10, no. 15: 2784. https://doi.org/10.3390/math10152784
APA StyleHeydari, M., Lai, K. K., Fan, Y., & Li, X. (2022). A Review of Emergency and Disaster Management in the Process of Healthcare Operation Management for Improving Hospital Surgical Intake Capacity. Mathematics, 10(15), 2784. https://doi.org/10.3390/math10152784








