Advancing the Adoption of Continuing Professional Development (CPD) in the United States
Abstract
1. Introduction
2. The Evolution of the Practice of Pharmacy
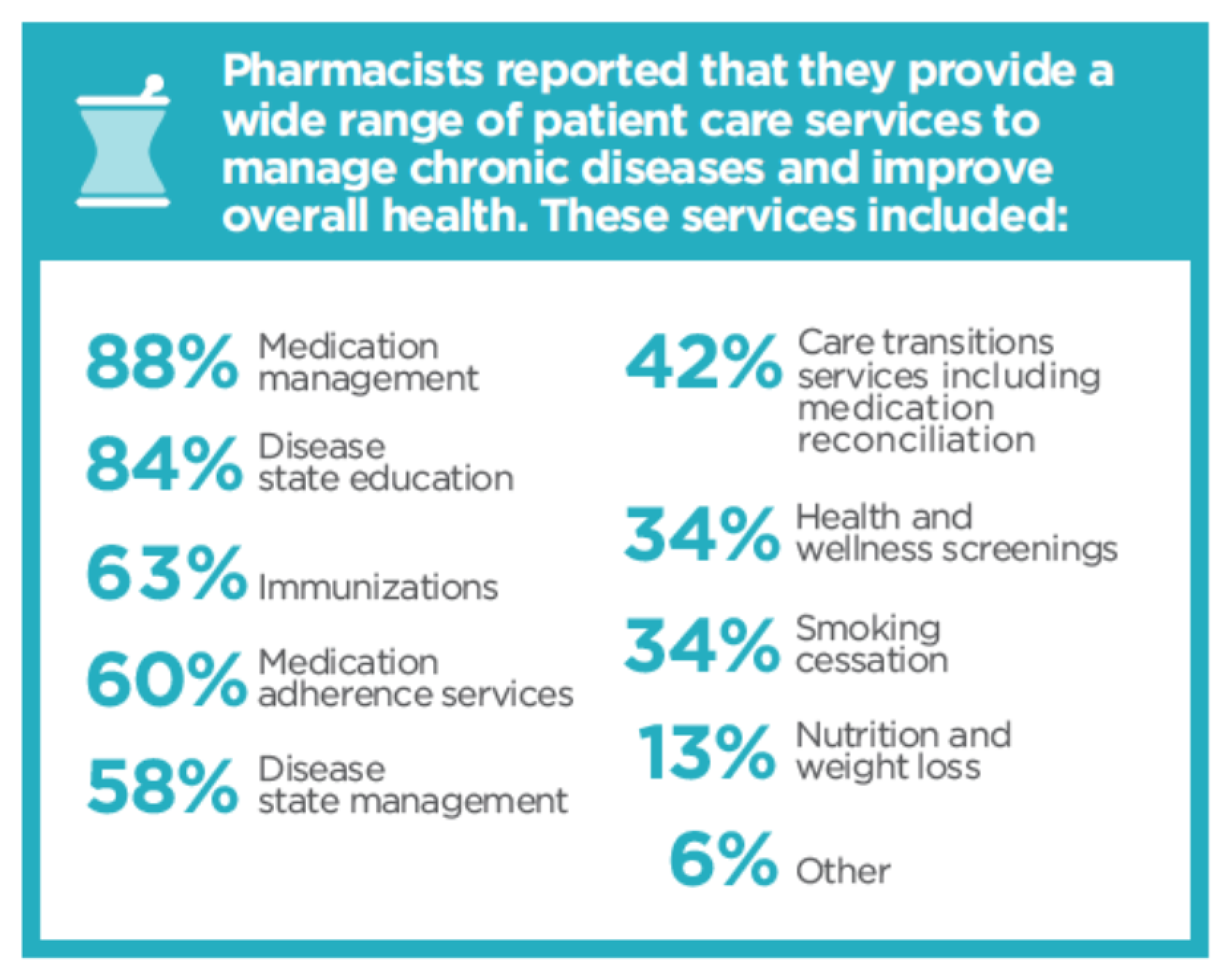
3. Expanded Patient Care Roles for Pharmacists in the United States
4. Expanded Definition of Community-Based Practice in the United States
5. Regulation of Pharmacy Practice in the United States
6. Assuring the Professional Competency of Pharmacists
7. Health Care Practitioner Responsibilities for Ensuring Continuing Professional Competency
Transitioning from a Continuing Education Model to a Continuing Professional Development Model in the United States
- ▪
- A workforce of knowledgeable health professionals is critical to the discovery and application of health care practices to prevent diseases and promote well-being
- ▪
- The absence of a comprehensive and well-integrated system of continuing education in the health professions is an important factor of knowledge and performance deficiencies at the individual and system levels
- ▪
- The new vision for continuing education will be based on an approach called CPD in which learning takes place over a lifetime and stretches beyond the classroom to the point of care
- ▪
- The CPD system is a holistic approach that incorporates a broader variety of learning methods and theories than CE
- ▪
- CPD is learner-driven and tailored to the individual learner’s needs; it includes concepts such as self-directed learning and practice-based learning and teaches how to identify problems and apply solutions
8. Advancing Continuing Professional Development in the Pharmacy Profession
- ▪
- The CPD process is defined as “the responsibility of individual pharmacists for systematic maintenance, development and broadening of knowledge, skills and attitudes, to ensure continuing competence as a professional, throughout their careers”
- ▪
- CE is an important part of a structured CPD program, personalized for each pharmacist
- ▪
- The CPD process should be visible to ensure credibility with the public
- ▪
- CPD must be actively managed and include all the components of the cyclical process
- ▪
- CPD must be an on-going, cyclical process of continuing quality improvement by which pharmacists seek to maintain and enhance their competence in both current duties and anticipated future service developments
- ▪
- Ensure that pharmacists maintain (at an appropriate level) their knowledge, skills, and competence to practice through their careers in their own specific (or current) areas of practice
- ▪
- Improve the pharmacist’s personal performance (i.e., develop knowledge and skills)
- ▪
- Enhance the pharmacist’s career progression
9. The Current U.S. Practice Environment
10. Challenges with the Adoption of CPD
- ▪
- “The CPD approach to learning is embraced more by those with a mentor or colleague demonstrating use or those that incorporated a similar approach during their undergraduate education”
- ▪
- “The flexibility of the CPD approach allows those with specialized practice to engage in learning that is most beneficial to their particular practice (e.g., non-pharmacy conferences, workplace learning, research, etc.)”
- ▪
- “There is value in focusing on an outcome in practice (i.e., applying newly-acquired knowledge to practice)”
- ▪
- “Pharmacists support the CPD process when the impact in practice is recognized”
- ▪
- “The CPD cycle enables a continuous learning process and becomes a valuable platform to reinforce continuing competence within practice”
- ▪
- “Application of the CPD cycle as an approach to lifelong learning in individual practice”
- ▪
- “Changing the focus of CPD to meaningful learning rather than collecting CE points”
- ▪
- “Developing the skills and knowledge to adopt the CPD process under a voluntary system”
- ▪
- “Establishing adequate assessment methods and measures for a portfolio-based system”
- ▪
- “Raising the awareness and recognition from the public on the skills and knowledge that pharmacists continuously develop”
- ▪
- “Ensuring the qualitative assessment of CPD portfolios”
- ▪
- “Lack of technical ‘know-how’ for implementing a robust online system to support the CPD process”
- ▪
- “Ensuring pharmacists engage with the CPD cycle that includes reflection on their practice”
- ▪
- “Minimizing cost constraints for pharmacists to undertake formal CPD programs”
- ▪
- “Making the recording or documentation of learning less onerous”
- ▪
- “Identifying those pharmacists who require additional mentoring or guidance to steer away from the hour or point collecting mentality”
- ▪
- “Ensuring relevant support for pharmacists in non-traditional roles”
11. Technology Solutions to Support the Adoption of CPD
12. My CPD®
- ▪
- Ensure that knowledge, skills, attitudes, and values are kept current
- ▪
- Apply learning to improve practice and/or patient outcomes
- ▪
- Direct career goals or support career advancements or changes
- ▪
- Provide CV or interview templates
- ▪
- Fulfill employment, regulatory and credentialing requirements
13. ADVANCE®
- ▪
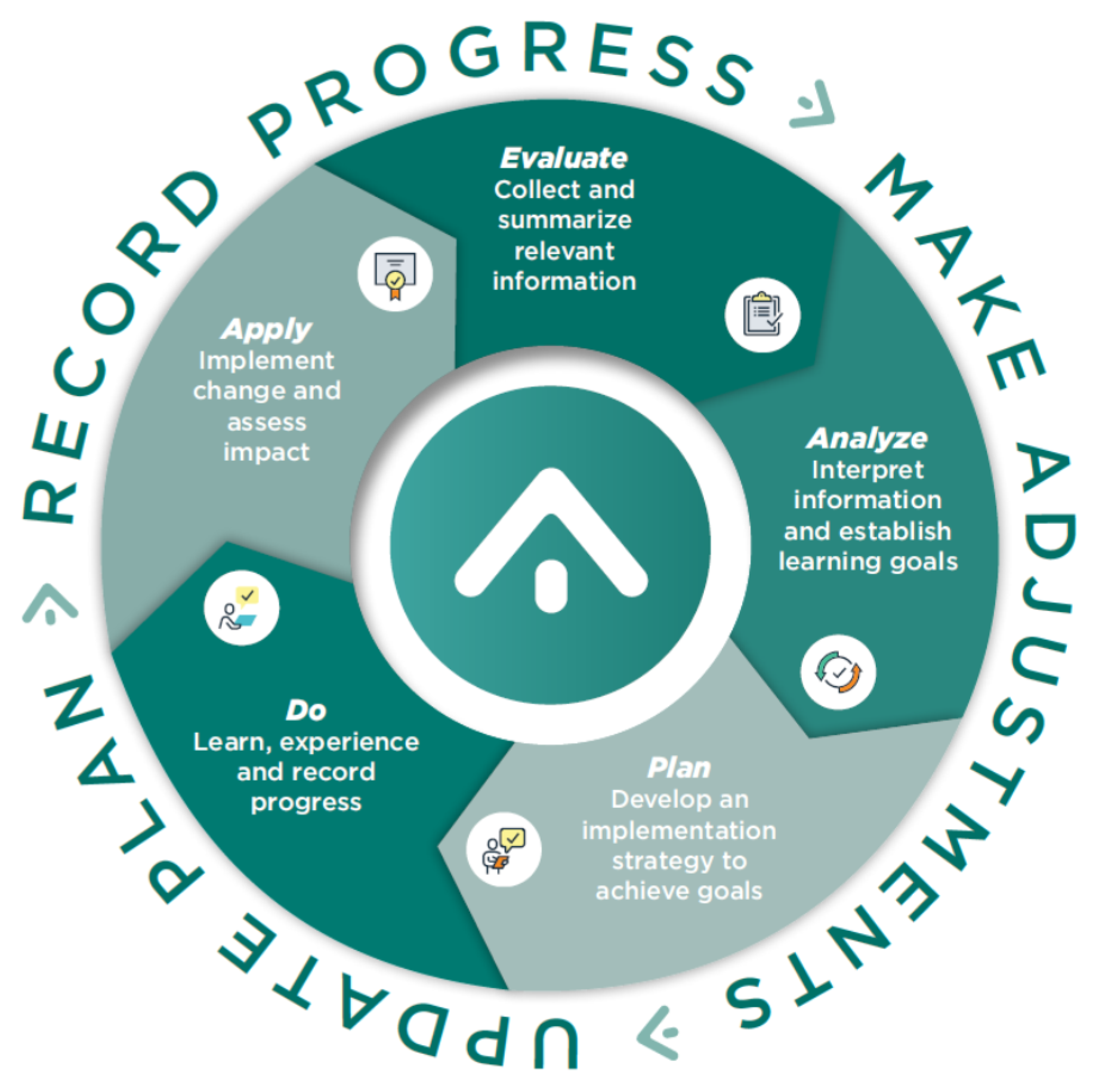
- Evaluate—Guides pharmacists through seven evaluation exercises to determine professional development needs
- ▪
- Analyze—Helps pharmacists determine the meaning of the information provided in the Evaluate step and provides a framework to establish SMART planning goals
- ▪
- Plan—Supports pharmacists by recommending activities and experiences customized to the individual, from which they can create a comprehensive professional development plan
- ▪
- Do—Provides a framework to help pharmacists set priorities and deadlines for all selected activities, track accomplishments, and maintain a professional portfolio
- ▪
- Apply—Prompts pharmacists to reflect on the activities they have completed, consider what they may want to focus on next, and make updates to the professional development plan
- ▪
- Strengths—Leveraging personal strengths can help pharmacists better understand themselves, how they work, and how they contribute to a team.
- ▪
- Professional Skills—Each individual has a unique set of professional skills shaped by past experiences, interests, and goals. Like many aspects of life, professional skills may change or grow over time. This assessment leverages the Entrustable Professional Activities and allows pharmacists to assess both their baseline and progress toward improving their skills.
- ▪
- Personal Attributes—Personal attributes are associated with how an individual’s personality, emotions, and tendencies contribute to their behaviors. These attributes can significantly impact a professional’s ability to interact with others and function effectively.
- ▪
- Interest Areas—Aligning an individual’s career with their interests increases the likelihood that they will achieve professional satisfaction and maximizes the impact of CPD.
- ▪
- Growth and Development—The technology platform evaluates each user’s assessments and provides customized areas for growth and development focused on the improvement of professional skills and personal attributes.
- ▪
- Licensure—Evaluating a summary of your licensure requirements supports pharmacists in designing a professional development plan that simultaneously keeps professional licenses active and individuals moving toward their goals.
- ▪
- Well-Being—Pharmacist well-being is essential to personal and professional productivity, and understanding factors that create stress or support relaxation can positively impact both the personal and professional needs of pharmacists.
14. ADVANCE® Recognition
15. CPD Model Comparison
16. Supporting the Advancement of CPD in the United States
17. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- FIP—International Pharmaceutical Federation. Statement of Professional Standards on Continuing Professional Development. Available online: https://www.fip.org/file/1544 (accessed on 10 June 2020).
- Travlos, D.V.; Baumgartner, J.L.; Rouse, M.; Wadelin, J.W.; Vlasses, P.H. Forty Years of ACPE CPE Accreditation. Am. J. Pharm. Educ. 2017, 81, 5998. [Google Scholar] [CrossRef] [PubMed]
- Hepler, C.D.; Strand, L.M. Opportunities and Responsibilities in Pharmaceutical Care. Am. J. Hosp. Pharm. 1990, 47, 533–543. [Google Scholar] [CrossRef] [PubMed]
- Accreditation Council for Pharmacy Education. Policies and Procedures for ACPE Accreditation of Professional Degree Programs. Available online: https://www.acpe-accredit.org/pdf/CS_PoliciesandProcedures.pdf (accessed on 10 June 2020).
- American Society of Health-System Pharmacists. ASHP’s Pharmacy Residency Match Sees Continued Growth. Available online: https://www.ashp.org/News/2020/04/08/ASHPs-Pharmacy-Residency-Match-Sees-Continued-Growth (accessed on 10 June 2020).
- American Pharmacists Association and American Society of Health-system Pharmacists. Community-based Pharmacy Residency Directors and Preceptors Open Forum. Available online: https://www.youtube.com/watch?v=_TJ3MVM3P6Y&feature=youtu.be (accessed on 4 August 2020).
- Hammond, D.A.; Oyler, D.R.; Devlin, J.W.; Painter, J.T.; Bolesta, S.; Swanson, J.M.; Bailey, B.J.; Branan, T.; Barletta, J.F.; Dunn, B.; et al. Perceived Motivating Factors and Barriers for the Completion of Postgraduate Training Among American Pharmacy Students Prior to Beginning Advanced Pharmacy Practice Experiences. Am. J. Pharm. Educ. 2017, 81, 90. [Google Scholar] [CrossRef] [PubMed]
- Koval, P.V. Growth of Pharmacist Board Certification. Available online: https://www.bpsweb.org/2018/05/03/growth-of-pharmacist-board-certification/ (accessed on 10 June 2020).
- American Pharmacists Association. Pharmacists’ Patient Care Services Digest: Building Momentum. Increasing Access. Available online: https://media.pharmacist.com/documents/APhA_Digest.pdf (accessed on 10 June 2020).
- Centers for Medicaid and Medicare Services. State Flexibility to Facilitate Timely Access to Drug Therapy by Expanding the Scope of Pharmacy Practice Using Collaborative Practice Agreements, Standing Orders or Other Predetermined Protocols. Available online: https://www.medicaid.gov/federal-policy-guidance/downloads/cib011717.pdf (accessed on 10 June 2020).
- National Governor’s Association. The Expanding Role of Pharmacists in a Transformed Health Care System. Available online: https://www.pharmacist.com/article/national-governors-association-states-can-better-integrate-pharmacists-health-care-system?is_sso_called=1 (accessed on 10 June 2020).
- Patients Access to Pharmacists’ Care Coalition. Pharmacist Scope of Services. Available online: https://www.pharmacist.com/sites/default/files/files/PAPCC%20-%20Scope%20of%20Services%20one-pager%20%28final%29.pdf (accessed on 10 June 2020).
- Pharmacy Workforce Center, Inc. 2019 National Pharmacist Workforce Study Final Report. Available online: https://www.aacp.org/sites/default/files/2020-03/2019_NPWS_Final_Report.pdf (accessed on 10 June 2020).
- U.S. Bureau of Labor Statistics. Work Environment. Available online: https://www.bls.gov/ooh/healthcare/pharmacists.htm#tab-3 (accessed on 3 August 2020).
- Bennett, M.; Goode, J.R. Recognition of Community-based Pharmacist Practitioners: Essential Health Care Providers. J. Am. Pharm. Assoc. 2016, 56, 580–583. [Google Scholar] [CrossRef] [PubMed]
- Skelton, J.B.; Owen, J.A. Developing a Vision and Strategic Action Plan for Future Community-based Residency Training. J. Am. Pharm. Assoc. 2016, 56, 584–589. [Google Scholar] [CrossRef] [PubMed]
- National Alliance of State Pharmacy Associations. Pharmacist Administered Vaccines. Available online: https://naspa.us/wp-content/uploads/2019/04/IZ-Authority-012019.pdf (accessed on 10 June 2020).
- National Alliance of State Pharmacy Associations. Prescribing Under a Statewide Protocol, Statewide Standing Order or Unrestricted (Category-Specific) Authority. Available online: https://naspa.us/resource/swp/ (accessed on 17 June 2020).
- Accreditation Council for Pharmacy Education. Continuing Professional Development (CPD). Presentation to the NABP District 3 Meeting. Available online: http://nabpdistrict3.org/uploads/3/2/0/4/3204416/continuing_professional_development_-_mike_rouse_presentation.pdf (accessed on 12 June 2020).
- American Association of Colleges of Pharmacy; American Pharmacists Association. Preliminary Report of the AACP/APhA Task Force on Continuing Competence in Pharmacy-The Continuing Competence of Pharmacists. J. Am. Pharm. Assoc. 1974, 14, 340–345. [Google Scholar]
- National Association of Boards of Pharmacy. CPE Monitor Service Launched. Available online: https://nabp.pharmacy/newsroom/news/cpe-monitor-service-launched/ (accessed on 16 June 2020).
- Wheeler, J.S.; Chisholm-Burns, M. The Benefit of Continuing Professional Development for Continuing Pharmacy Education. Am. J. Pharm. Educ. 2018, 82, 6461. [Google Scholar] [CrossRef] [PubMed]
- Bruno, A. Continuing Professional Development/Continuing Education in Pharmacy: Global Report 2014. The Hague: International Pharmaceutical Federation. Available online: https://www.fip.org/file/1407 (accessed on 14 June 2020).
- American Medical Association. Code of Medical Ethics Overview. Available online: https://www.ama-assn.org/delivering-care/ethics/code-medical-ethics-overview (accessed on 14 June 2020).
- American Pharmacists Association. Code of Ethics for Pharmacists. Available online: https://www.pharmacist.com/code-ethics (accessed on 14 June 2020).
- International Federation of Pharmacists. FIP Statement of Professional Standards: Code of Ethics for Pharmacists. Available online: https://www.fip.org/file/1586 (accessed on 14 June 2020).
- American Nurses Association. Code of Ethics for Nurses. Available online: https://www.nursingworld.org/coe-view-only (accessed on 3 August 2020).
- American Association of Physician Assistants. Guidelines for Ethical Conduct for the PA Profession. Available online: https://www.aapa.org/download/56983/ (accessed on 3 August 2020).
- Institute of Medicine (U.S.) Committee on Planning a Continuing Health Professional Education Institute. Redesigning Continuing Education in the Health Professions; National Academies Press (U.S.): Washington, DC, USA, 2010; ISBN 978-0-309-14078-2. [Google Scholar]
- International Federation of Pharmacists. FIP Statement of Professional Standards Continuing Professional Development. Available online: https://www.fip.org/file/1544 (accessed on 14 June 2020).
- Council on Credentialing in Pharmacy. Resource Document on Continuing Professional Development in Pharmacy. Available online: http://www.pharmacycredentialing.org/Files/cpdprimer.pdf (accessed on 14 June 2020).
- Accreditation Council for Pharmacy Education. Guidance on Continuing Professional Development (CPD) for the Profession of Pharmacy. Available online: https://www.acpe-accredit.org/pdf/CPDGuidance%20ProfessionPharmacyJan2015.pdf (accessed on 14 June 2020).
- Davis, D.; O’Brien, M.A.; Freemantle, N.; Wolf, F.M.; Mazmanian, P.; Taylor-Vaisey, A. Impact of Formal Continuing Medical Education: Do Conferences, Workshops, Rounds, and Other Traditional Continuing Education Activities Change Physician Behavior or Health Care Outcomes? JAMA 1999, 282, 867–874. [Google Scholar] [CrossRef] [PubMed]
- International Federation of Pharmacists. Continuing Professional Development/Continuing Education in Pharmacy: A Global Report. Available online: https://www.fip.org/file/1407 (accessed on 14 June 2020).
- Tofade, T.; Chou, S.; Foushee, L.; Caiola, S.M.; Eckel, S. Continuing Professional Development Training Program Among Pharmacist Preceptors and Non-Preceptors. J. Am. Pharm. Assoc. 2010, 50, 730–735. [Google Scholar] [CrossRef] [PubMed]
- Janke, K.K. Continuing Professional Development: Don’t Miss the Obvious. Am. J. Pharm. Educ. 2010, 74, 31. [Google Scholar] [CrossRef] [PubMed]
- National Association of Boards of Pharmacy. CPE Monitor Plans. Available online: https://nabp.pharmacy/cpe-monitor-service/plans/ (accessed on 14 June 2020).
- American Pharmacists Association. ADVANCE. Available online: https://www.aphaadvance.com/ (accessed on 14 June 2020).
- Bzowyckyj, A.S.; Crabtree, B.; Franson, K.; Klepser, D.; Okere, A.N.; Poirier, T.; Welch, A.; Gandhi, N.; Ragucci, K. Report of the 2019–2020 AACP Academic Affairs Committee Developing the Pharmacist Workforce for Society’s Medication Use Needs in 2030. AJPE 2020, 84. [Google Scholar] [CrossRef]
- Eurostat. Glossary: Lifelong Learning. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php/Glossary:Lifelong_learning#:~:text=Jump%20to%3A%20navigation%20%2C%20search,social%20or%20employment%2Drelated%20perspectives (accessed on 20 June 2020).


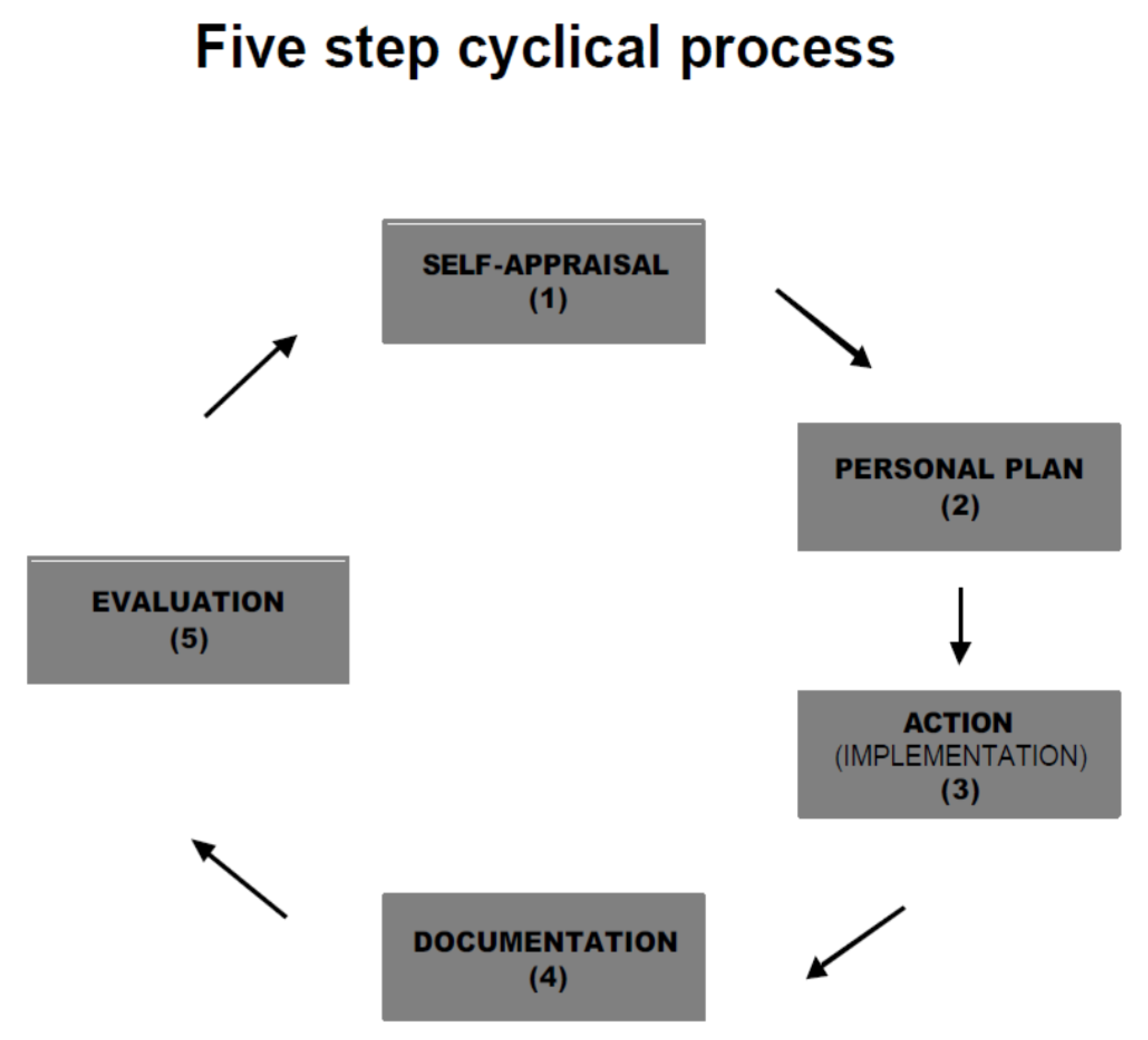
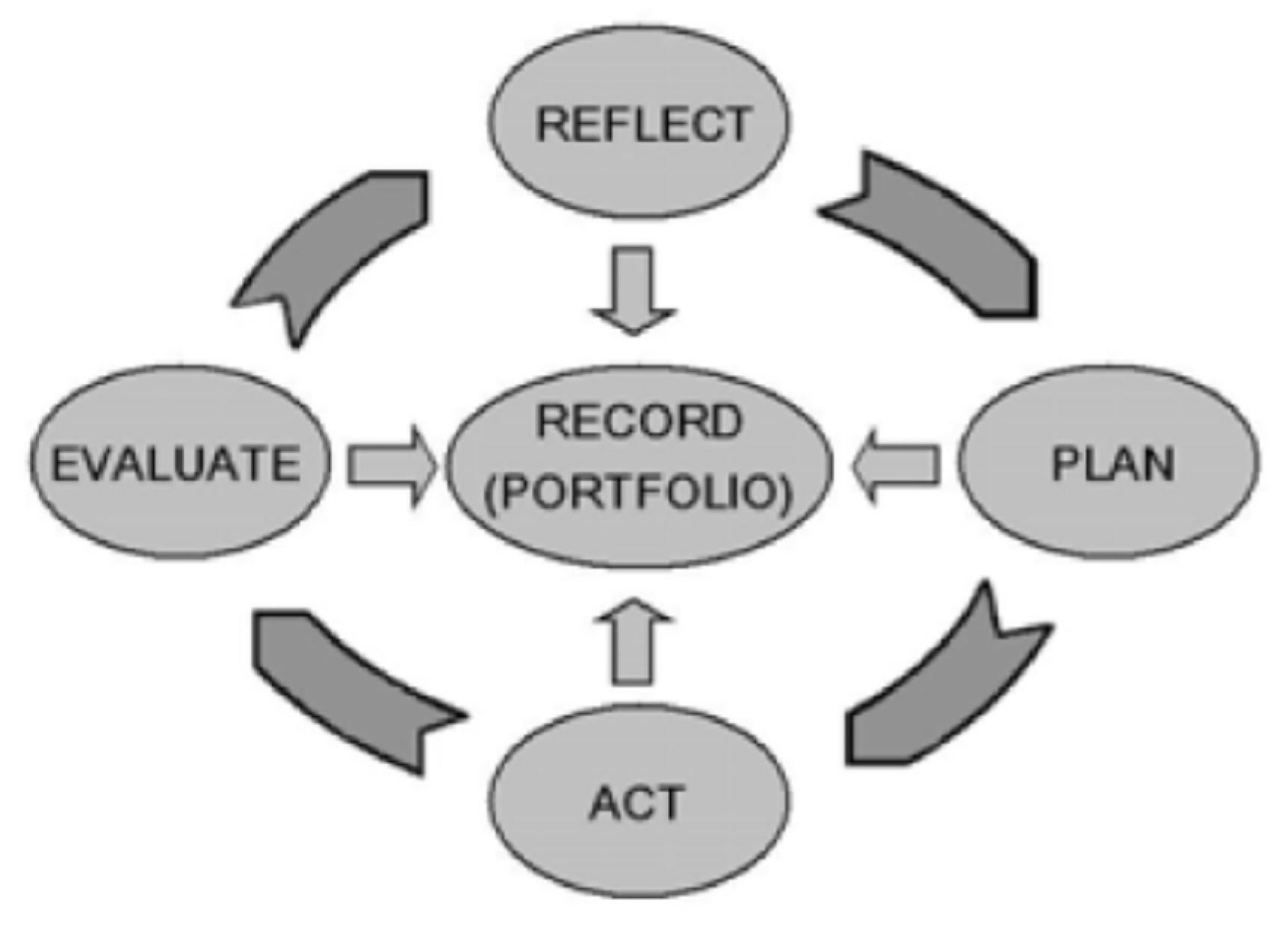
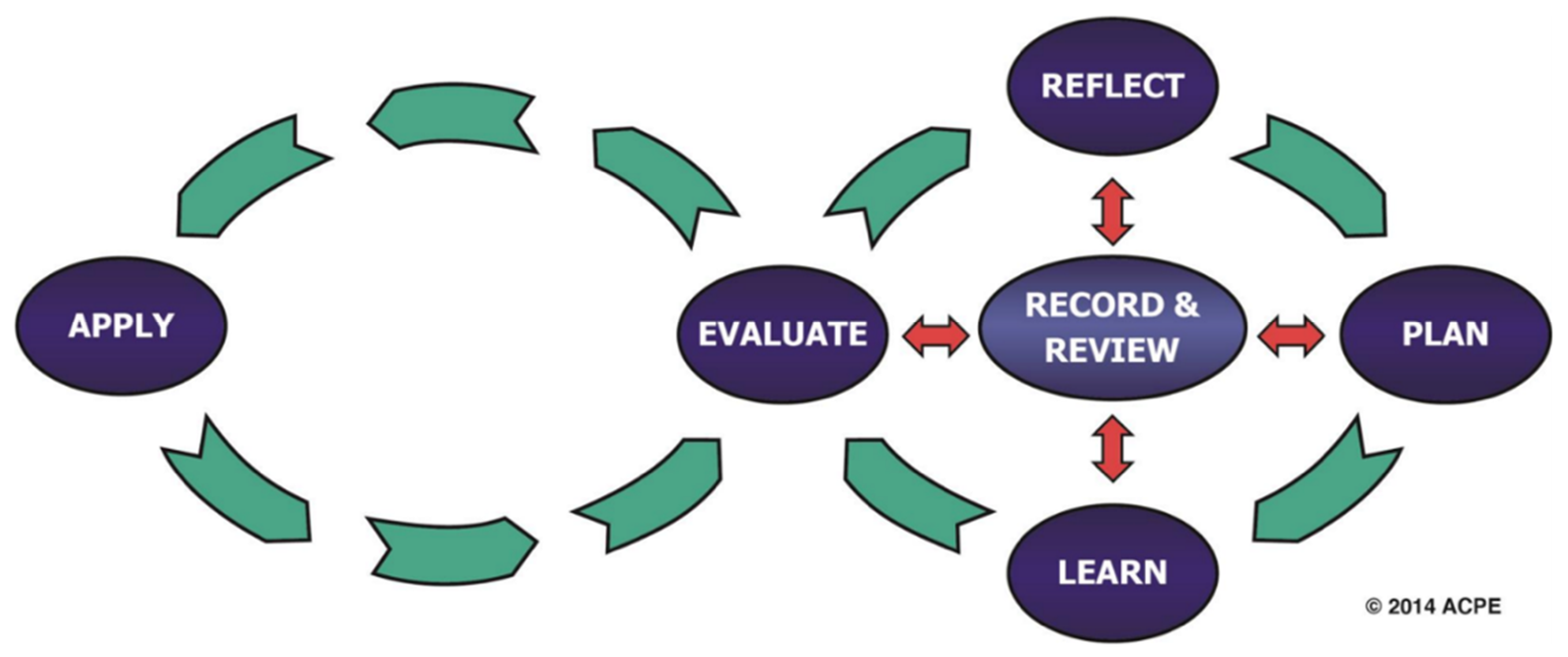
| FIP MODEL | ACPE MODEL | ADVANCE® MODEL | FUNCTION |
|---|---|---|---|
| Self-Appraisal | Reflect | Evaluate Analyze | Completion of an annual self-evaluation—collect and analyze/assess relevant information and determine meaning |
| Personal Plan | Plan | Plan | Creation of a detailed action plan specifying activities and experiences associated with each area of CPD |
| Action Implement | Learn | Do | Engage in activities and experiences and track progress |
| Evaluation | Evaluate Apply | Apply | Implement what was learned and reflect on the impact. Routinely review and update information and make necessary modifications to plan. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Owen, J.A.; Skelton, J.B.; Maine, L.L. Advancing the Adoption of Continuing Professional Development (CPD) in the United States. Pharmacy 2020, 8, 157. https://doi.org/10.3390/pharmacy8030157
Owen JA, Skelton JB, Maine LL. Advancing the Adoption of Continuing Professional Development (CPD) in the United States. Pharmacy. 2020; 8(3):157. https://doi.org/10.3390/pharmacy8030157
Chicago/Turabian StyleOwen, James A., Jann B. Skelton, and Lucinda L. Maine. 2020. "Advancing the Adoption of Continuing Professional Development (CPD) in the United States" Pharmacy 8, no. 3: 157. https://doi.org/10.3390/pharmacy8030157
APA StyleOwen, J. A., Skelton, J. B., & Maine, L. L. (2020). Advancing the Adoption of Continuing Professional Development (CPD) in the United States. Pharmacy, 8(3), 157. https://doi.org/10.3390/pharmacy8030157







