Establishing a Pharmacy-Based Patient Registry System: A Pilot Study for Evaluating Pharmacist Intervention for Patients with Long-Term Medication Use
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Disclosure
Appendix A. Data Collection at the Initial and Follow-Up Assessments
- Patient’s ID (automatically assigned at registration)
- Age and sex
- Clinical conditions for long-term medication use
- Date of informed consent
- Contact information if needed
- List of all medications used by the patient (not only dispensed medication at the pharmacy, but also those dispensed at different pharmacies)
- Treatment history
- Other conditions not for long-term medication use
- Lab results (blood pressure, lipid, HbA1c, etc.)
- Treatment conditions (one-pack doses, number of clinics used, etc.)
- Living environments related to treatment (living alone, job, home care, etc.)
- Potential problems reported by patient
- Potential concerns identified by pharmacist
- Preferred methods for follow-up contacts
- Others
- Date of contacts
- Method for monitoring (telephone or visit)
- Changes in medications
- Patient reported adherence or number of medications not used
- Reason for not taking medications as instructed
- Conditional changes (if any)
- Lab results (reported by patients)
- Pharmacist advice given to patients
- Next appointment dates
References
- Abe, S. Japan’s strategy for global health diplomacy: Why it matters. Lancet 2013, 382, 915–916. [Google Scholar] [CrossRef]
- Organisation for Economic Co-operation and Development (OECD). OECD Reviews of Health Care Quality: Japan–Assessment and Recommendations; OECD: Paris, France, 2014. [Google Scholar]
- Nomura, H.; Nakayama, T. The Japanese healthcare system: The issue is to solve the “tragedy of the commons” without making another. BMJ 2005, 331, 648–649. [Google Scholar] [CrossRef] [PubMed]
- Cabinet Office, Government of Japan. General Overview and Examples of the Regulatory Reform Council’s Second Report of Recommendations—Health and Medical Field. Available online: http://www8.cao.go.jp/kisei-kaikaku/english/index-en.html (accessed on 27 October 2017). (In Japanese)
- Ministry of Health, Labour and Welfare. Unused Drugs and Split Dispensing (as a Document Used in Central Social Insurance Medical Council on 22 July 2015). Available online: http://www.mhlw.go.jp/stf/shingi2/0000092094.html (accessed on 27 October 2017). (In Japanese)
- Koyanagi, K.; Kubot, T.; Kobayashi, D.; Kihara, T.; Yoshid, T.; Miisho, T.; Saito, Y.; Uchigoshi, H.; Takaki, J.; Seo, T.; et al. SETSUYAKU-BAG Campaign—Investigation of leftover drugs retained by outpatients and promotion of proper reuse leftover drugs to reduce medical expenses. Yakugak. Zasshi 2013, 133, 1215–1221. [Google Scholar] [CrossRef]
- Nakamura, K.; Urano, K.; Tanaka, M.; Nishiguchi, K.; Sakai, Y.; Katano, T.; Nabekura, T.; Yamamura, K.; Kunimasa, J. The Reduction Impact in Medical Expenses of Pharmaceutical Inquiries on Leftover Medicines at a Community Pharmacy. Jpn. J. Pharm. Health Care Sci. 2014, 40, 522–529. [Google Scholar] [CrossRef]
- Onda, M.; Imai, H.; Kasuga, M.; Yasuda, M.; Shimomura, M.; Okamoto, N.; Takada, Y.; Nanaumi, Y.; Tanaka, Y.; Arakawa, Y. Examining the effect of pharmacists’ visits to housebound patients on the elimination of unused drugs. Jpn. J. Drug. Inform. 2015, 17, 21–33. [Google Scholar]
- Japan Pharmaceutical Association. Study on the Effect of Pharmacist Drug Management for Elderly Patients at Home. Report March 2008. Available online: http://www.nichiyaku.or.jp/action/wp-content/uploads/2008/06/19kourei_hukuyaku1.pdf (accessed on 27 October 2017). (In Japanese).
- Elliott, R.A.; Barber, N.; Clifford, S.; Horne, R.; Hartley, E. The cost effectiveness of a telephone-based pharmacy advisory service to improve adherence to newly prescribed medicines. Pharm. World Sci. 2008, 30, 17–23. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, N.; Nitta, M.; Hara, K.; Watanabe, F.; Akagawa, K.; Kurata, N.; Kamei, M. Community pharmacists provided telephone treatment support for patients who received long-term prescribed medication. Integr. Pharm. Res. Pract. 2016, 5, 27–32. [Google Scholar] [PubMed]
- Ministry of Health, Labour and Welfare 2015: Kanjanotameno Yakkyokubijon (as a Document, “a Vision of Community Pharmacy for Patients” on 23 October 2015). Available online: http://www.mhlw.go.jp/file/04-Houdouhappyou-11121000-Iyakushokuhinkyoku-Soumuka/vision_1.pdf (accessed on 27 October 2017). (In Japanese)
- Donabedian, A. Evaluating the quality of medical care. Milbank Mem. Fund Q. 1966, 44, 166–206. [Google Scholar] [CrossRef]
- Pharmacist Intermediate Intervention Study (PIIS). Available online: http://piis.skr.jp/public.health/home.html (accessed on 25 January 2018). (In Japanese).
- Japanese Society for Applied Therapeutics. Available online: http://www.applied-therapeutics.org (accessed on 25 January 2018). (In Japanese).
- Alliance of Pharmacy Executives. Available online: http://yakukeiren.com (accessed on 25 January 2018). (In Japanese).
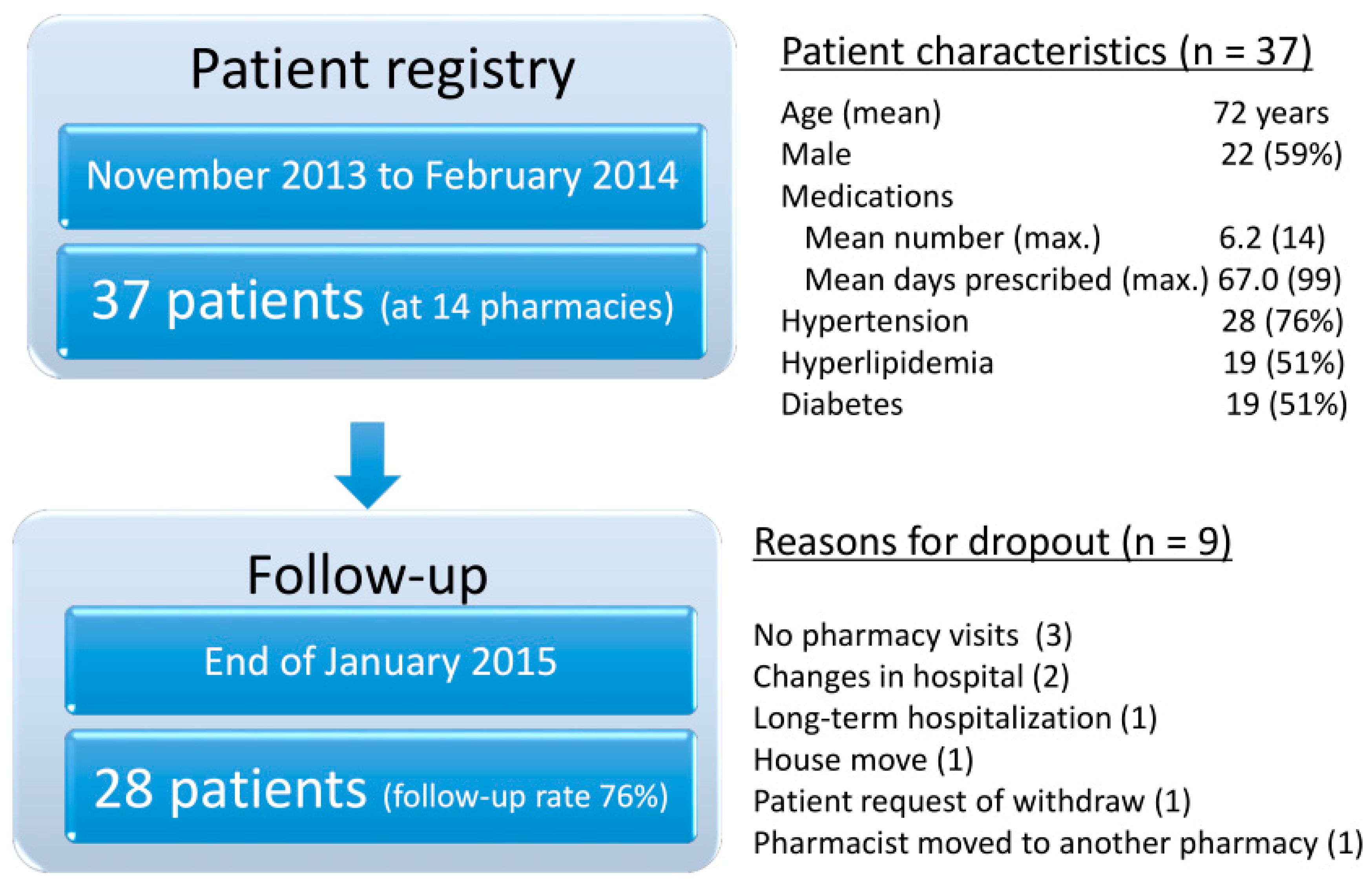
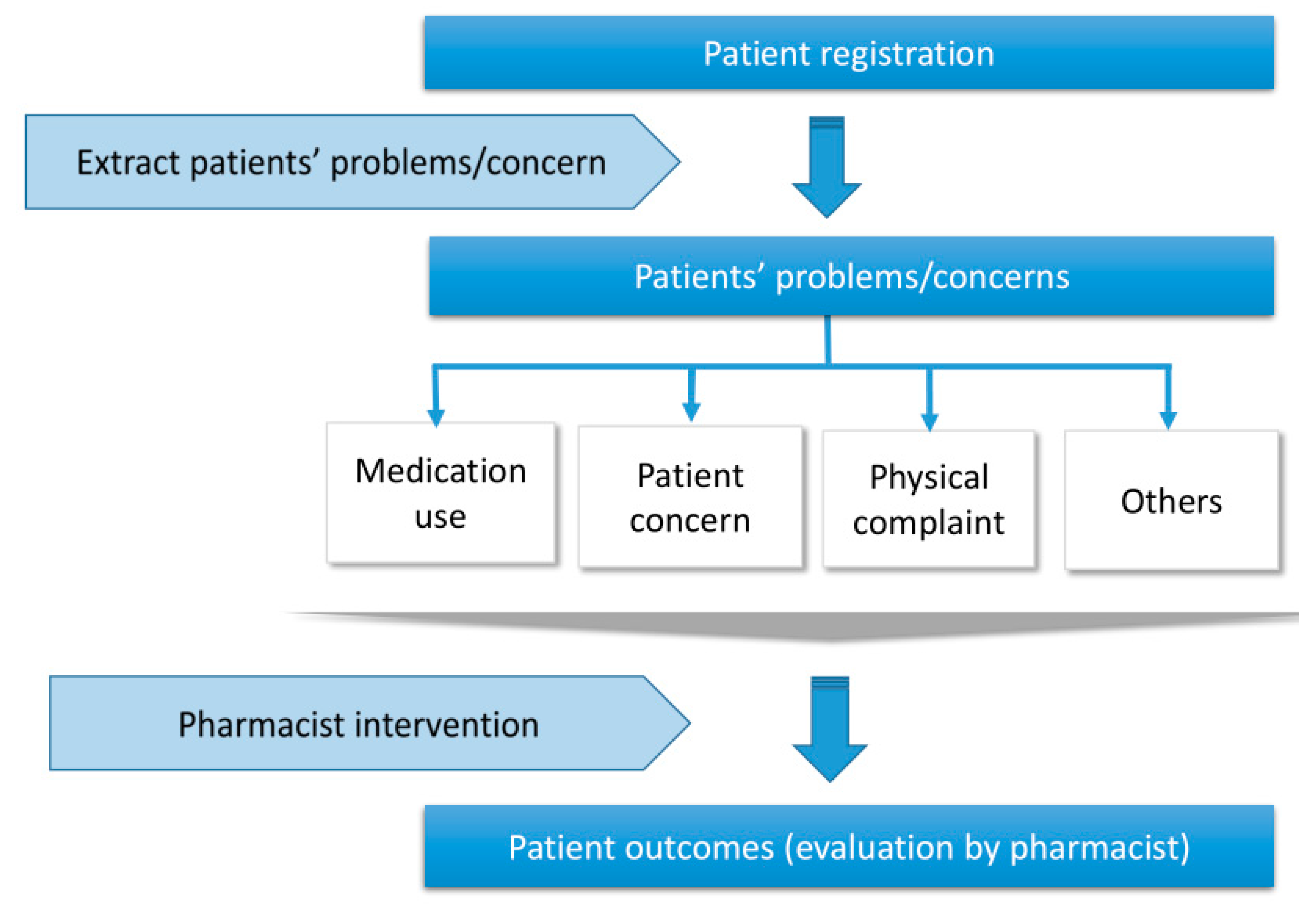
| Category | Potential Problems | Pharmacist Intervention (Suggestion or Recommendation) | Patient Outcomes |
|---|---|---|---|
| 1. Medication Use | |||
| Forget to take medicine when eating out | Keep some tablets in the bag constantly | Adherence was improved. | |
| Forget to take medicine when busy with work | Put the medicine in a conspicuous place Notice that the medicine could be taken also before eating | Adherence was improved. | |
| 2. Concerns | |||
| High blood sugar level despite efforts | Wait for the result of the next health check-up, and consider the possibility of hyperglycemia after a meal, as the current average blood sugar level is still better than before | The blood sugar level fell to the normal range on the next measurement. | |
| Blood pressure variation (low in the morning and high in the night) | Receive counseling from the family doctor | Concern disappeared after hearing that it was not necessary to mind this. | |
| 3. Physical Complaint | |||
| Chest ache after exercise | Get medical consultation for angina pectoris fear | The patient underwent detailed examination and was diagnosed and operated on for angina pectoris. | |
| Dizziness | Drink more water or tea because of possible side effect | Dizziness disappeared after several weeks. | |
| 4. Others | |||
| No interest in the results of the health check | Promote health education | The patient became interested in the value of health check-ups (e.g., purchased books); motivation to receive medical treatment increased. | |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Akazawa, M.; Mikami, A.; Tamura, Y.; Yanagi, N.; Yamamura, S.; Ogata, H. Establishing a Pharmacy-Based Patient Registry System: A Pilot Study for Evaluating Pharmacist Intervention for Patients with Long-Term Medication Use. Pharmacy 2018, 6, 12. https://doi.org/10.3390/pharmacy6010012
Akazawa M, Mikami A, Tamura Y, Yanagi N, Yamamura S, Ogata H. Establishing a Pharmacy-Based Patient Registry System: A Pilot Study for Evaluating Pharmacist Intervention for Patients with Long-Term Medication Use. Pharmacy. 2018; 6(1):12. https://doi.org/10.3390/pharmacy6010012
Chicago/Turabian StyleAkazawa, Manabu, Akiko Mikami, Yuri Tamura, Natsuyo Yanagi, Shinichi Yamamura, and Hiroyasu Ogata. 2018. "Establishing a Pharmacy-Based Patient Registry System: A Pilot Study for Evaluating Pharmacist Intervention for Patients with Long-Term Medication Use" Pharmacy 6, no. 1: 12. https://doi.org/10.3390/pharmacy6010012
APA StyleAkazawa, M., Mikami, A., Tamura, Y., Yanagi, N., Yamamura, S., & Ogata, H. (2018). Establishing a Pharmacy-Based Patient Registry System: A Pilot Study for Evaluating Pharmacist Intervention for Patients with Long-Term Medication Use. Pharmacy, 6(1), 12. https://doi.org/10.3390/pharmacy6010012





