Evaluation of Medication Prescribing Applications Available in Australia
Abstract
:1. Introduction
2. Materials and Methods
2.1. Identifying and Characterising Apps
2.1.1. Eligibility Criteria
2.1.2. Search Strategy
2.1.3. Databases Searched
2.1.4. App Feature Data Extraction
2.2. Assessment of Safe Prescribing
2.2.1. Mock Consumer Case Construction
2.2.2. Assessment of Adherence to NPS Competency Guidelines
2.3. Data Analysis and Synthesis
3. Results
3.1. Application Characteristics
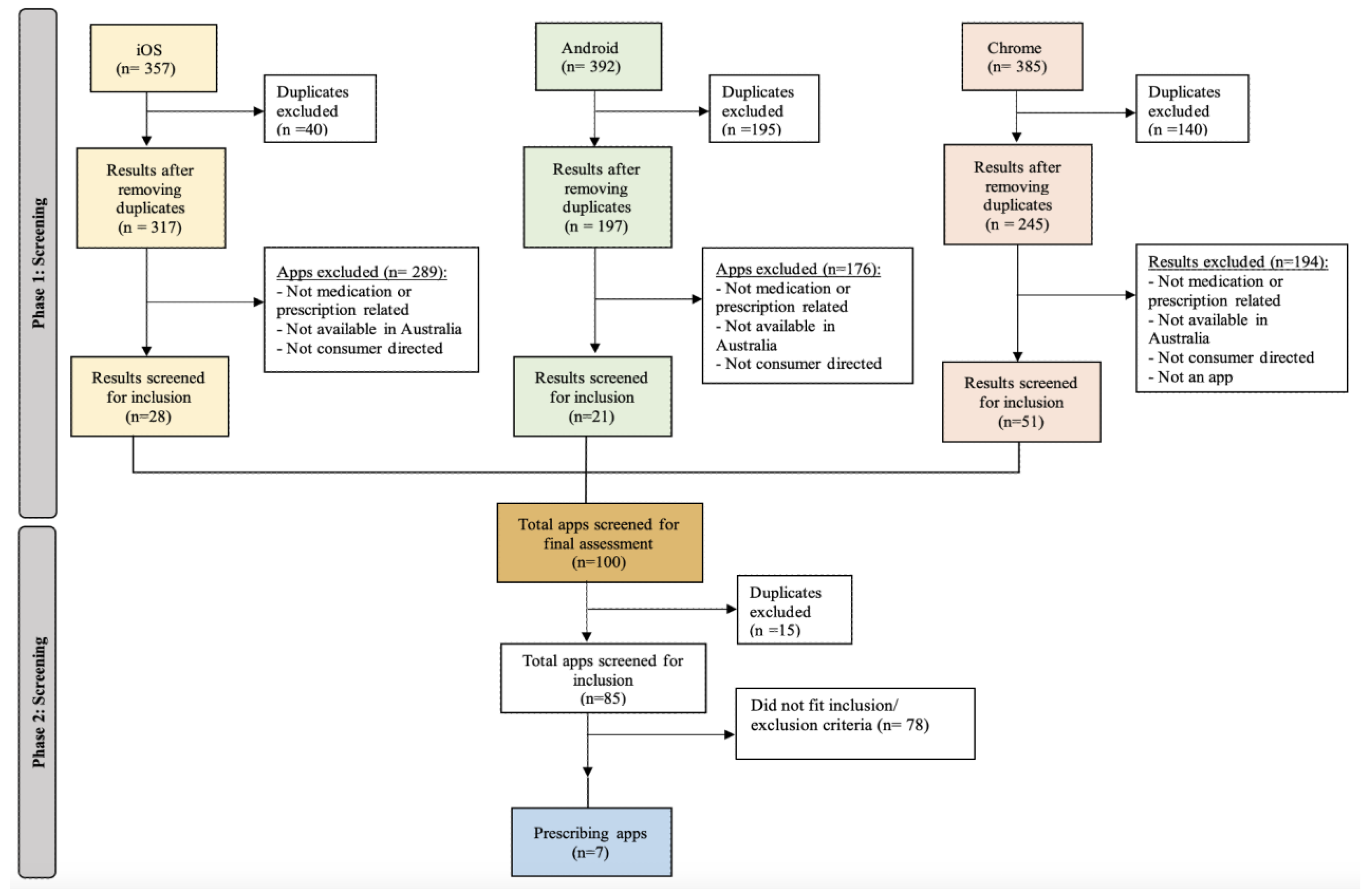
3.1.1. Search and Categorisation
3.1.2. Prescribing App Features
3.2. Analysis of Prescription Request Apps
Adherence to NPS Competency Framework for Safe Prescribing
Prescribing Stage 1: Information Gathering
Stage 2: Decision Making
Stage 3: Communicate Decision
Stage 4: Monitor and Review
4. Discussion
4.1. Strengths & Limitations
4.2. Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Aitken, M.; Nass, D. Digital Health Trends 2021: Innovation, Evidence, Regulation, and Adoption; IQVIA: Durham, NC, USA, 2021. [Google Scholar]
- Adapa, S. Adoption of internet shopping: Cultural considerations in India and Australia. J. Internet Bank. Commer. 2008, 13, 1–17. [Google Scholar]
- Australian Government Department of Health and Ageing. Standard for the Uniform Scheduling of Medicines and Poisons (SUSMP); Australian Government Department of Health and Ageing: Canberra, Australia, 2022; p. 6. [Google Scholar]
- Medical Board of Australia. Guidelines for Technology-Based Patient Consultations. Available online: https://www.medicalboard.gov.au/documents/default.aspx?record=WD12%2f7052&dbid=AP&chksum=BWu6uoWlwW2PcJUUZUwcRw%3d%3d (accessed on 9 January 2023).
- Choice of Contraceptive Method. Available online: https://tgldcdp-tg-org-au.eu1.proxy.openathens.net/viewTopic?etgAccess=true&guidelinePage=Sexual%20and%20Reproductive%20Health&topicfile=contraceptive-choice (accessed on 10 August 2022).
- Chrystyn, H.; van der Palen, J.; Sharma, R.; Barnes, N.; Delafont, B.; Mahajan, A.; Thomas, M. Device errors in asthma and COPD: Systematic literature review and meta-analysis. NPJ Prim. Care Respir Med. 2017, 27, 22. [Google Scholar] [CrossRef] [PubMed]
- Rodler, S.; von Büren, J.; Buchner, A.; Stief, C.; Elkhanova, K.; Wülfing, C.; Jungmann, S. Epidemiology and treatment barriers of patients with erectile dysfunction using an online prescription platform: A cross-sectional study. Sex. Med. 2020, 8, 370–377. [Google Scholar] [CrossRef] [PubMed]
- Australian Medicines Handbook: AMH 2022. Available online: https://amhonline-amh-net-au.eu1.proxy.openathens.net/chapters/genitourinary-drugs/drugs-sexual-dysfunction/erectile-dysfunction (accessed on 12 August 2022).
- Australian Government Department of Health and Ageing. PBS Expenditure and Prescriptions Report 1 July 2020 to 30 June 2021. Available online: https://www.pbs.gov.au/info/statistics/expenditure-prescriptions/pbs-expenditure-and-prescriptions-report-30-june-2021 (accessed on 12 August 2022).
- Torales, J.; Ríos-González, C.; Barrios, I.; O’Higgins, M.; González, I.; García, O.; Castaldelli-Maia, J.M.; Ventriglio, A. Self-perceived stress during the quarantine of COVID-19 pandemic in Paraguay: An exploratory survey. Front. Psychiatry 2020, 11, 558691. [Google Scholar] [CrossRef] [PubMed]
- Chopra, D.; Bhandari, B.; Sidhu, J.K.; Jakhar, K.; Jamil, F.; Gupta, R. Prevalence of self-reported anxiety and self-medication among upper and middle socioeconomic strata amidst COVID-19 pandemic. J. Educ. Health Promot. 2021, 10, 73. [Google Scholar] [CrossRef] [PubMed]
- Finkelstein, Y.; Aks, S.E.; Hutson, J.R.; Juurlink, D.N.; Nguyen, P.; Dubnov-Raz, G.; Pollak, U.; Koren, G.; Bentur, Y. Colchicine poisoning: The dark side of an ancient drug. Clin. Toxicol. 2010, 48, 407–414. [Google Scholar] [CrossRef] [PubMed]
- Lum, E.; Mitchell, C.; Coombes, I. The competent prescriber: 12 core competencies for safe prescribing. Aust. Prescr. 2013, 36, 13–16. [Google Scholar] [CrossRef]
- The Royal Australian College of General Practitioners. Standards for General Practices, 5th edition. Available online: https://www.racgp.org.au/getattachment/ece472a7-9a15-4441-b8e5-be892d4ffd77/Standards-for-general-practices-5th-edition.aspx (accessed on 10 August 2022).
- National Safety and Quality Health Service (NSQHS) Standards Medication Safety Standard—Medication Management Processes. Available online: https://www.safetyandquality.gov.au/standards/nsqhs-standards/medication-safety-standard (accessed on 12 August 2022).
- AusDI. Available online: https://ausdi-hcn-com-au.eu1.proxy.openathens.net/quickSearch.hcn (accessed on 10 August 2022).
- Monthly Index of Medical Specialities Australia. Available online: https://www.mims.com.au/index.php/products/emims (accessed on 10 August 2022).
- Preston, C.L. Stockley’s Drug Interactions Pocket Companion 2016; Pharmaceutical Press: London, UK, 2016. [Google Scholar]
- Therapeutic Guidelines. Available online: https://tgldcdp.tg.org.au/index (accessed on 10 August 2022).
- Palchik, N.S.; Wolf, F.M.; Cassidy, J.T.; Ike, R.W.; Davis, W.K. Comparing information-gathering strategies of medical students and physicians in diagnosing simulated medical cases. Acad. Med. 1990, 65, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Stowasser, D.A.; Allinson, Y.M.; O’Leary, M. Understanding the Medicines Management Pathway. J. Pharm. Pract. Res. 2004, 34, 293–296. [Google Scholar] [CrossRef]

| Item | Response |
|---|---|
| App Names | Free text |
| Process of obtaining a script | Free text |
| Method for receiving prescription | Free text |
| Medicine Catalogue | Free text |
| Dispensed by a local pharmacy | Free text |
| Who can you obtain a script for? | Anyone/Yourself. Elaborate if necessary |
| Prescription type | New and/or Repeat prescriptions Private and/or subsidised by the Australian Pharmaceutical Benefits Scheme |
| Are brands available for purchase? | Yes/No |
| Bulk Billing | Yes/No |
| Personal Information Collected | Free text |
| Popularity of app/number of downloads | Free text |
| Consult style (e.g., online, telehealth) | Free text |
| Cost for online consult | Free text |
| Other comments | Free text |
| Medication | Rationale for Selection |
|---|---|
| Combined oral contraceptive pill (Levlen®, containing ethinylestradiol 30 mcg and levonorgestrel 150 mcg) | Appropriate contraceptive choice requires careful consideration of drug interactions, contraindications, adverse effects, and an individual’s circumstances [5]. |
| Fluticasone/salmeterol MDI | Misused inhaler devices can impact disease management; asthma requires frequent monitoring [6]. |
| Sildenafil | Potential for serious drug interactions; commonly self-selected, which may lead to misdiagnosis of other serious conditions such as cardiovascular disease [7,8]. |
| Sertraline | A commonly prescribed antidepressant in Australia [9]. The prevalence of poor mental health conditions may lead to inappropriate self-medicating [10,11]. |
| Colchicine | Has a narrow therapeutic window, the potential for serious drug interactions and can have complex dosing regimens [12]. |
| Four Stages of Prescribing | 12 Core Competencies |
|---|---|
| (1) Information gathering (skill of gathering relevant information to inform selection of treatment) | 1. Take and/or review medical history |
| 2. Take and/or review medication history and reconcile this with medical history | |
| 3. Undertake further physical examination/investigations where appropriate | |
| 4. Assess adherence to current and past medication and risk factors for non-adherence | |
| (2) Decision-making (collaborative decision-making with the patient/carer; selection of treatment) | 5. Identify key health and/or medication-related issues with the patient, including making or reviewing the diagnosis |
| 6. Determine how well disease and symptoms are managed/controlled | |
| 7. Determine whether current symptoms are modifiable by symptomatic treatment or disease modifying treatment | |
| 8. Consider ideal therapy (drug and non-drug), taking into account actual and potential contraindications/concerns: drug–patient, drug–disease, drug–drug interactions | |
| 9. Select drug, form, route, dose, frequency, duration of treatment | |
| (3) Communicate decision (safely and effectively communicate treatment decisions to other health professionals and the patient/carer in both the ambulatory and the inpatient setting) | 10. Communicate prescribing decision in an ambulatory care setting |
| 11. Communicate prescribing decision in an inpatient setting | |
| (4) Monitor and review (review the therapeutic and adverse impact of treatment) | 12. Review control of symptoms and signs, adherence, and patient’s outcomes |
| App A | App B | App C | App D | App E | App F | App G | |
|---|---|---|---|---|---|---|---|
| Platforms | Web, iOS, Android | Web, iOS, Android | Web, iOS, Android | Web | Web, iOS, Android | Web | Web |
| Telehealth Option | ✓ | ✓ | ✓ | ✓ | |||
| Who Can You Obtain a Prescription For? | |||||||
| Self | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Others | ✓ | ✓ | ✓ | ✓ | |||
| Prescription Available | |||||||
| New (without telehealth) | ✓ | ✓ | ✓ | ✓ | ✓ | ||
| Repeat (without telehealth) | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| PBS | ✓ | ✓ | ✓ | ||||
| Private | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ |
| Method of Obtaining Prescription | |||||||
| E-script | ✓ | ✓ | ✓ | ||||
| Postal | ✓ | * | ✓ | * | * | ||
| Sent to local pharmacy | ✓ | ✓ | |||||
| Number of Medications Available | 184 | 190 | - | 76 | - | - | 11 |
| Available Medicine Catalogue | Heartburn, anaphylaxis, blood pressure, blood thinners, cholesterol, diabetes, eye condition, gout, headache & migraines, men’s health, mental health, neurological diseases, opioid safety, pain management, respiratory conditions, sexual health, skin care, sleep, thyroid medications, travel, urinary incontinence, vitamins, weight loss, women’s health | Heartburn, allergies, blood pressure, cholesterol, cold & flu, diabetes, gout, headache & migraines, men’s health, mental health, respiratory conditions, skin care, women’s health | Heartburn, allergies, blood pressure, bone health, cholesterol, diabetes, gout, headache & migraines, men’s health, mental health, pain management, respiratory conditions, skin care, urinary incontinence, women’s health | Heartburn, cold & flu, gout, headache & migraines, mental health, respiratory conditions, sexual health, skin care, sleep, smoking cessation thyroid medications, travel, weight loss, women’s health | Heartburn, allergies, blood pressure, cholesterol, cold & flu, diabetes, gout, headache & migraines, men’s health, mental health, respiratory conditions, skin care, women’s health | Heartburn, cold and flu, respiratory conditions, skin care, sleep, women’s health | Women’s health (contraception only) |
| Methods to Obtain Prescription | Search medication by name or medication catalogue followed by selecting a medication, complete an online questionnaire*, select method for receiving prescription doctor reviews information (*Some medication requires telehealth) | Select medical condition, type in medication of desire with dose, complete an online questionnaire, select collection method, doctor reviews information | Select ‘new prescription’ or ‘repeat prescription’ tab. Telehealth consult is required for all new prescriptions. For repeat prescription - search medication by name, select collection method, complete an online questionnaire, reviewed by doctor | Search for medication by name or search for medication catalogue followed by selecting a medication, complete an online questionnaire, reviewed by doctor, medication will be sent to the patient | Select medical condition, type in medication of desire with dose, complete an online questionnaire, select collection method, doctor reviews information | Select medical conditions, fill in personal details, complete an online questionnaire, reviewed by doctor (receive text or email when script is ready) | Select ‘contraception’ tab, complete a questionnaire, select pill brand, reviewed by doctor, medication sent to the patient |
| Four Prescribing Stages | Core Competencies | App A | App B | App C | App D | App E | App F | App G | |||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Information gathering | 1 | Medical history | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||
| 2 | Medication history | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||||||||
| 3 | Further information | ||||||||||||||||||||||||||||||||||||
| 4 | Adherence | ✓ | |||||||||||||||||||||||||||||||||||
| Decision-making | 5 | Shared decision-making | |||||||||||||||||||||||||||||||||||
| 6 | Disease management | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||||||||
| 7 | Indication | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||||
| 8a | Other treatment | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||||||||
| 8b | Contraindications | ✓ | * | ✓ | ✓ | ✓ | * | ✓ | ✓ | ✓ | * | ✓ | ✓ | ✓ | ✓ | ✓ | * | ✓ | ✓ | ✓ | ✓ | * | ✓ | ||||||||||||||
| 9 | Dose regimen | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||||||||||||||
| Communicate decision | 10 | In an outpatient setting | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | |||||||||||||||||||||||||||||
| Monitor and review | 12 | Treatment monitoring | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ✓ | ||||||||||||||
| Total number of questions | 13 | 7 | 9 | 18 | 7 | 24 | 21 | 22 | 17 | 19 | 17 | 8 | 12 | 9 | 12 | 20 | 10 | 15 | 7 | 12 | 14 | 8 | 21 | 14 | 29 | ||||||||||||
| Ethinylestradiol/levonorgestrel | Fluticasone/Salmeterol | Sildenafil | Colchicine | Sertraline | Not available in-app | ||||||||||||||||||||||||||||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Amin, R.; Cato, M.; Rahavi, S.; Tran, K.; Lee, K.; Lobo, E.; Mill, D.; Page, A.; Salter, S. Evaluation of Medication Prescribing Applications Available in Australia. Pharmacy 2023, 11, 49. https://doi.org/10.3390/pharmacy11020049
Amin R, Cato M, Rahavi S, Tran K, Lee K, Lobo E, Mill D, Page A, Salter S. Evaluation of Medication Prescribing Applications Available in Australia. Pharmacy. 2023; 11(2):49. https://doi.org/10.3390/pharmacy11020049
Chicago/Turabian StyleAmin, Riya, Melissa Cato, Sasha Rahavi, Kristin Tran, Kenneth Lee, Elton Lobo, Deanna Mill, Amy Page, and Sandra Salter. 2023. "Evaluation of Medication Prescribing Applications Available in Australia" Pharmacy 11, no. 2: 49. https://doi.org/10.3390/pharmacy11020049
APA StyleAmin, R., Cato, M., Rahavi, S., Tran, K., Lee, K., Lobo, E., Mill, D., Page, A., & Salter, S. (2023). Evaluation of Medication Prescribing Applications Available in Australia. Pharmacy, 11(2), 49. https://doi.org/10.3390/pharmacy11020049








