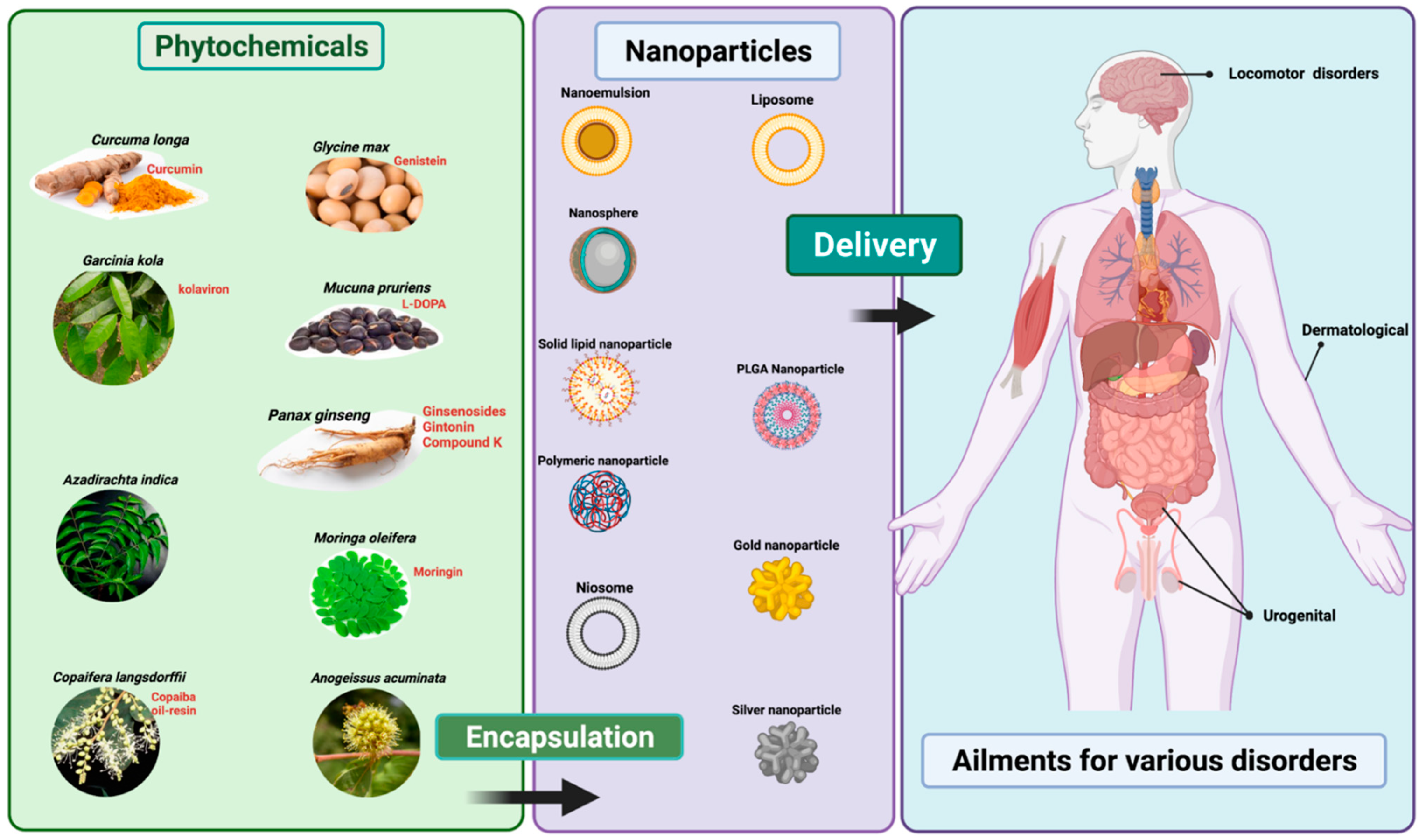
Phytochemicals and Nano-Phytopharmaceuticals Use in Skin, Urogenital and Locomotor Disorders: Are We There?
Abstract
:1. Introduction
2. Materials and Methods
3. Therapeutic Applications of Nano-Phytopharmaceuticals
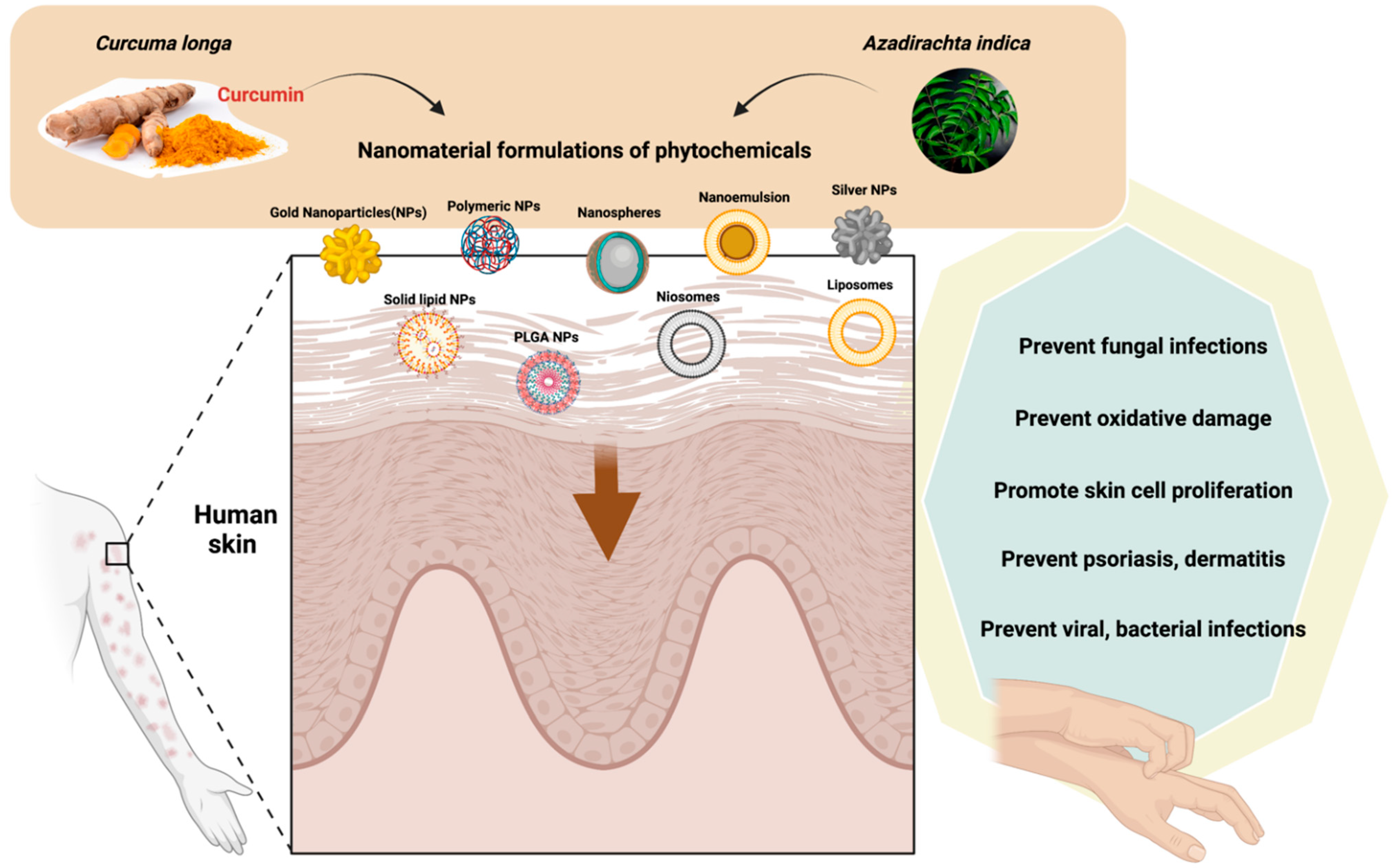
3.1. Nano-Phytopharmaceuticals in Dermal Disorders
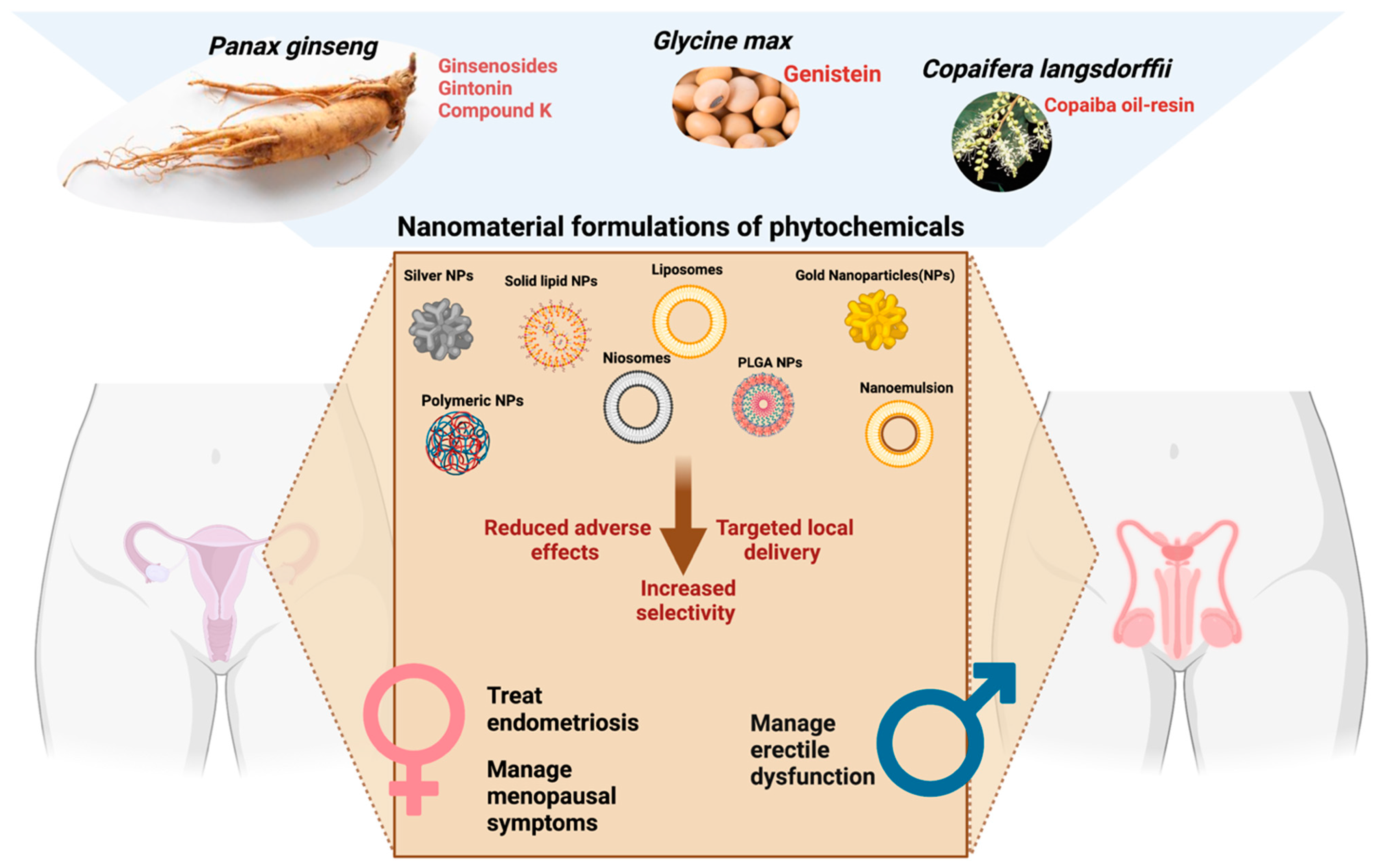
3.2. Nano-Phytopharmaceuticals in Urogenital Disorders
3.3. Nano-Phytopharmaceuticals in Locomotor Disorders
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Kesarwani, K.; Gupta, R.; Mukerjee, A. Bioavailability enhancers of herbal origin: An overview. Asian Pac. J. Trop. Biomed. 2013, 3, 253–266. [Google Scholar] [CrossRef] [Green Version]
- Patridge, E.; Gareiss, P.; Kinch, M.S.; Hoyer, D. An analysis of FDA-approved drugs: Natural products and their derivatives. Drug Discov. Today 2016, 21, 204–207. [Google Scholar] [CrossRef] [PubMed]
- Bonifácio, B.V.; Silva, P.B.; Ramos, M.A.; Negri, K.M.; Bauab, T.M.; Chorilli, M. Nanotechnology-based drug delivery systems and herbal medicines: A review. Int. J. Nanomed. 2014, 9, 1–15. [Google Scholar] [CrossRef] [Green Version]
- Hafez, D.A.; Elkhodairy, K.A.; Teleb, M.; Elzoghby, A.O. Nanomedicine-based approaches for improved delivery of phyto-therapeutics for cancer therapy. Expert Opin. Drug Deliv. 2020, 17, 279–285. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lim, C.L.; Raju, C.S.; Mahboob, T.; Kayesth, S.; Gupta, K.K.; Jain, G.K.; Dhobi, M.; Nawaz, M.; Wilairatana, P.; de Lourdes Pereira, M.; et al. Precision and advanced nano-phytopharmaceuticals for therapeutic applications. Nanomaterials 2022, 12, 238. [Google Scholar] [CrossRef] [PubMed]
- Patra, J.K.; Das, G.; Fraceto, L.F.; Campos, E.V.R.; Rodriguez-Torres, M.D.P.; Acosta-Torres, L.S.; Diaz-Torres, L.A.; Grillo, R.; Swamy, M.K.; Sharma, S.; et al. Nano based drug delivery systems: Recent developments and future prospects. J. Nanobiotechnol. 2018, 16, 71. [Google Scholar] [CrossRef] [Green Version]
- Watkins, R.; Wu, L.; Zhang, C.; Davis, R.M.; Xu, B. Natural product-based nanomedicine: Recent advances and issues. Int. J. Nanomed. 2015, 10, 6055–6074. [Google Scholar] [CrossRef] [Green Version]
- Dowling, A.; Clift, R.; Grobert, N.; Hutton, D.; Oliver, R.; O’neill, O.; Pethica, J.; Pidgeon, N.; Porritt, J.; Ryan, J. Nanoscience and nanotechnologies: Opportunities and uncertainties, lond. R. Soc. R. Acad. Eng. Rep. 2004, 46, 618. [Google Scholar]
- Mishra, V.; Kesharwani, P.; Mohd Amin, M.C.I.; Iyer, A.K. (Eds.) Preface. In Nanotechnology-Based Approaches for Targeting and Delivery of Drugs and Genes; Elsevier: Amsterdam, The Netherlands, 2017; pp. xix–xx. [Google Scholar]
- Sandhiya, V.; Ubaidulla, U. A review on herbal drug loaded into pharmaceutical carrier techniques and its evaluation process. Future J. Pharm. Sci. 2020, 6, 1–16. [Google Scholar] [CrossRef]
- Pelaz, B.; Alexiou, C.; Alvarez-Puebla, R.A.; Alves, F.; Andrews, A.M.; Ashraf, S.; Balogh, L.P.; Ballerini, L.; Bestetti, A.; Brendel, C.; et al. Diverse applications of nanomedicine. ACS Nano 2017, 11, 2313–2381. [Google Scholar] [CrossRef] [Green Version]
- Mitchell, M.J.; Billingsley, M.M.; Haley, R.M.; Wechsler, M.E.; Peppas, N.A.; Langer, R. Engineering precision nanoparticles for drug delivery. Nat. Rev. Drug Discov. 2021, 20, 101–124. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.; Roy, I.; Yang, C.; Prasad, P.N. Nanochemistry and nanomedicine for nanoparticle-based diagnostics and therapy. Chem. Rev. 2016, 116, 2826–2885. [Google Scholar] [CrossRef] [PubMed]
- Sachan, A.K.; Gupta, A. A review on nanotized herbal drugs. Int. J. Pharma. Sci. Res. 2015, 6, 961. [Google Scholar]
- Morigi, V.; Tocchio, A.; Pellegrini, B.C.; Sakamoto, J.H.; Arnone, M.; Tasciotti, E. Nanotechnology in medicine: From inception to market domination. J. Drug Deliv. 2012, 2012, 389485. [Google Scholar] [CrossRef] [PubMed]
- Hay, R.J.; Johns, N.E.; Williams, H.C.; Bolliger, I.W.; Dellavalle, R.P.; Margolis, D.J.; Marks, R.; Naldi, L.; Weinstock, M.A.; Wulf, S.K.; et al. The global burden of skin disease in 2010: An analysis of the prevalence and impact of skin conditions. J. Invest. Dermatol. 2014, 134, 1527–1534. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barankin, B.; DeKoven, J. Psychosocial effect of common skin diseases. Can. Fam. Physician 2002, 48, 712–716. [Google Scholar]
- Hazarika, N.; Archana, M. The psychosocial impact of acne vulgaris. Ind. J. Dermatol. 2016, 61, 515–520. [Google Scholar] [CrossRef]
- Mian, M.; Silfvast-Kaiser, A.; Paek, S.; Kivelevitch, D.; Menter, A. A review of the most common dermatologic conditions and their debilitating psychosocial impacts. Int. Arch. Int. Med. 2019, 3, 018. [Google Scholar] [CrossRef]
- Essendoubi, M.; Gobinet, C.; Reynaud, R.; Angiboust, J.F.; Manfait, M.; Piot, O. Human skin penetration of hyaluronic acid of different molecular weights as probed by raman spectroscopy. Skin Res. Technol. 2016, 22, 55–62. [Google Scholar] [CrossRef]
- Roberts, M.S.; Mohammed, Y.; Pastore, M.N.; Namjoshi, S.; Yousef, S.; Alinaghi, A.; Haridass, I.N.; Abd, E.; Leite-Silva, V.R.; Benson, H.; et al. Topical and cutaneous delivery using nanosystems. J. Control. Release 2017, 247, 86–105. [Google Scholar] [CrossRef] [Green Version]
- Kocbek, P.; Teskač, K.; Kreft, M.E.; Kristl, J. Toxicological aspects of long-term treatment of keratinocytes with ZNO and TiO2 nanoparticles. Small 2010, 6, 1908–1917. [Google Scholar] [CrossRef] [PubMed]
- Schaeffer, H.E.; Krohn, D.L. Liposomes in topical drug delivery. Invest. Ophthalmol. Vis. Sci. 1982, 22, 220–227. [Google Scholar] [PubMed]
- Haider, M.; Abdin, S.M.; Kamal, L.; Orive, G. Nanostructured lipid carriers for delivery of chemotherapeutics: A review. Pharmaceutics 2020, 12, 288. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Xu, Y.; Guo, Y.; Yang, Y.; Meng, Y.; Xia, X.; Liu, Y. Stabilization of deformable nanovesicles based on insulin-phospholipid complex by freeze-drying. Pharmaceutics 2019, 11, 539. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chaiyana, W.; Anuchapreeda, S.; Punyoyai, C.; Neimkhum, W.; Lee, K.-H.; Lin, W.-C.; Lue, S.-C.; Viernstein, H.; Mueller, M. Ocimum sanctum linn. as a natural source of skin anti-ageing compounds. Ind. Crops Prod. 2019, 127, 217–224. [Google Scholar] [CrossRef]
- Chaiyana, W.; Anuchapreeda, S.; Somwongin, S.; Marsup, P.; Lee, K.H.; Lin, W.C.; Lue, S.C. Dermal delivery enhancement of natural anti-ageing compounds from Ocimum sanctum linn. extract by nanostructured lipid carriers. Pharmaceutics 2020, 12, 309. [Google Scholar] [CrossRef] [Green Version]
- Caddeo, C.; Díez-Sales, O.; Pons, R.; Fernàndez-Busquets, X.; Fadda, A.M.; Manconi, M. Topical anti-inflammatory potential of quercetin in lipid-based nanosystems: In vivo and in vitro evaluation. Pharm. Res. 2014, 31, 959–968. [Google Scholar] [CrossRef] [Green Version]
- Kaur, L.; Jain, S.K.; Manhas, R.K.; Sharma, D. Nanoethosomal formulation for skin targeting of amphotericin B: An in vitro and in vivo assessment. J. Liposome Res. 2015, 25, 294–307. [Google Scholar] [CrossRef]
- Ramezanli, T.; Kilfoyle, B.E.; Zhang, Z.; Michniak-Kohn, B.B. Polymeric nanospheres for topical delivery of vitamin D3. Int. J. Pharm. 2017, 516, 196–203. [Google Scholar] [CrossRef] [Green Version]
- Petit, R.G.; Cano, A.; Ortiz, A.; Espina, M.; Prat, J.; Muñoz, M.; Severino, P.; Souto, E.B.; García, M.L.; Pujol, M.; et al. Psoriasis: From pathogenesis to pharmacological and nano-technological-based therapeutics. Int. J. Mol. Sci. 2021, 22, 4983. [Google Scholar] [CrossRef]
- Chen, Y.; Wu, Q.; Zhang, Z.; Yuan, L.; Liu, X.; Zhou, L. Preparation of curcumin-loaded liposomes and evaluation of their skin permeation and pharmacodynamics. Molecules 2012, 17, 5972–5987. [Google Scholar] [CrossRef] [PubMed]
- Waghule, T.; Gorantla, S.; Rapalli, V.K.; Shah, P.; Dubey, S.K.; Saha, R.N.; Singhvi, G. Emerging trends in topical delivery of curcumin through lipid nanocarriers: Effectiveness in skin disorders. AAPS PharmSciTech 2020, 21, 284. [Google Scholar] [CrossRef] [PubMed]
- Paul, A.K.; Jahan, R.; Paul, A.; Mahboob, T.; Bondhon, T.A.; Jannat, K.; Hasan, A.; Nissapatorn, V.; Wilairatana, P.; de Lourdes Pereira, M.; et al. The role of medicinal and aromatic plants against obesity and arthritis: A review. Nutrients 2022, 14, 985. [Google Scholar] [CrossRef] [PubMed]
- Mahmood, A.; Rapalli, V.K.; Waghule, T.; Gorantla, S.; Dubey, S.K.; Saha, R.N.; Singhvi, G. Uv spectrophotometric method for simultaneous estimation of betamethasone valerate and tazarotene with absorption factor method: Application for in-vitro and ex-vivo characterization of lipidic nanocarriers for topical delivery. Spectrochim. Acta Part A Mol. Biomol. Spectrosc. 2020, 235, 118310. [Google Scholar] [CrossRef] [PubMed]
- Battaglia, L.; Gallarate, M. Lipid nanoparticle: State of the art, new preparation methods and challenges in drug delivery. Expert Opin. Drug Deliv. 2012, 9, 497–508. [Google Scholar] [CrossRef]
- Moreno, L.; Puerta, E.; Suárez-Santiago, J.E.; Santos-Magalhães, N.S.; Ramirez, M.J.; Irache, J.M. Effect of the oral administration of nanoencapsulated quercetin on a mouse model of Alzheimer’s disease. Int. J. Pharm. 2017, 517, 50–57. [Google Scholar] [CrossRef]
- Shankar, G.M.; Antony, J.; Anto, R.J. Chapter two-quercetin and tryptanthrin: Two broad spectrum anticancer agents for future chemotherapeutic interventions. In The Enzymes; Bathaie, S.Z., Tamanoi, F., Eds.; Academic Press: Cambridge, MA, USA, 2015; Volume 37, pp. 43–72. [Google Scholar]
- Palle, S.; Neerati, P. Quercetin nanoparticles attenuates scopolamine induced spatial memory deficits and pathological damages in rats. Bull. Fac. Pharm. Cairo Univ. 2017, 55, 101–106. [Google Scholar] [CrossRef] [Green Version]
- de Andrade Teles, R.B.; Diniz, T.C.; Costa Pinto, T.C.; de Oliveira Júnior, R.G.; Gama, E.S.M.; de Lavor, É.M.; Fernandes, A.W.C.; de Oliveira, A.P.; de Almeida Ribeiro, F.P.R.; da Silva, A.A.M.; et al. Flavonoids as therapeutic agents in Alzheimer’s and Parkinson’s diseases: A systematic review of preclinical evidences. Oxidative Med. Cell. Longev. 2018, 2018, 7043213. [Google Scholar] [CrossRef]
- Kim, M.J.; Rehman, S.U.; Amin, F.U.; Kim, M.O. Enhanced neuroprotection of anthocyanin-loaded peg-gold nanoparticles against aβ (1-42)-induced neuroinflammation and neurodegeneration via the NF-(k)b/JNK/GSK3β signaling pathway. Nanomedicine 2017, 13, 2533–2544. [Google Scholar] [CrossRef]
- Khoo, H.E.; Azlan, A.; Tang, S.T.; Lim, S.M. Anthocyanidins and anthocyanins: Colored pigments as food, pharmaceutical ingredients, and the potential health benefits. Food Nutr. Res. 2017, 61, 1361779. [Google Scholar] [CrossRef] [Green Version]
- Cheng, K.K.; Yeung, C.F.; Ho, S.W.; Chow, S.F.; Chow, A.H.; Baum, L. Highly stabilized curcumin nanoparticles tested in an in vitro blood-brain barrier model and in Alzheimer’s disease tg2576 mice. AAPS J. 2013, 15, 324–336. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zubedat, S.; Freed, Y.; Eshed, Y.; Cymerblit-Sabba, A.; Ritter, A.; Nachmani, M.; Harush, R.; Aga-Mizrachi, S.; Avital, A. Plant-derived nanoparticle treatment with cocc 30c ameliorates attention and motor abilities in sleep-deprived rats. Neuroscience 2013, 253, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Chen, J.; Feng, C.; Shao, X.; Liu, Q.; Zhang, Q.; Pang, Z.; Jiang, X. Intranasal nanoparticles of basic fibroblast growth factor for brain delivery to treat Alzheimer’s disease. Int. J. Pharm. 2014, 461, 192–202. [Google Scholar] [CrossRef] [PubMed]
- Manca, M.L.; Manconi, M.; Meloni, M.C.; Marongiu, F.; Allaw, M.; Usach, I.; Peris, J.E.; Escribano-Ferrer, E.; Tuberoso, C.I.G.; Gutierrez, G. Nanotechnology for natural medicine: Formulation of neem oil loaded phospholipid vesicles modified with argan oil as a strategy to protect the skin from oxidative stress and promote wound healing. Antioxidants 2021, 10, 670. [Google Scholar] [CrossRef]
- Maghimaa, M.; Alharbi, S.A. Green synthesis of silver nanoparticles from Curcuma longa l. and coating on the cotton fabrics for antimicrobial applications and wound healing activity. J. Photochem. Photobiol. B Biol. 2020, 204, 111806. [Google Scholar] [CrossRef]
- Zamarioli, C.M.; Martins, R.M.; Carvalho, E.C.; Freitas, L.A. Nanoparticles containing curcuminoids (curcuma longa): Development of topical delivery formulation. Rev. Bras. Farmacogn. 2015, 25, 53–60. [Google Scholar] [CrossRef] [Green Version]
- Masuku, N.P.; Unuofin, J.O.; Lebelo, S.L. Advances in nanoparticle delivery system for erectile dysfunction: An updated review. Sex. Med. 2021, 9, 100420. [Google Scholar] [CrossRef]
- Draganski, A.; Tar, M.T.; Villegas, G.; Friedman, J.M.; Davies, K.P. Topically applied curcumin-loaded nanoparticles treat erectile dysfunction in a rat model of type-2 diabetes. J. Sex. Med. 2018, 15, 645–653. [Google Scholar] [CrossRef]
- Linjawi, S.A. Evaluation of the protective effect of Panax ginseng nanoparticles against nicotine-induced reproductive disorders in male rats. Int. J. Pharma. Sci. Rev. Res. 2015, 32, 38–45. [Google Scholar]
- Das, P.; Kumar, K.; Nambiraj, A.; Awasthi, R.; Dua, K.; Malipeddi, H. Antibacterial and in vitro growth inhibition study of struvite urinary stones using Oxalis corniculata linn. leaf extract and its biofabricated silver nanoparticles. Recent Pat. Drug Deliv. Formul. 2018, 12, 170–178. [Google Scholar] [CrossRef]
- Mishra, M.P.; Padhy, R.N. Antibacterial activity of green silver nanoparticles synthesized from Anogeissus acuminata against multidrug resistant urinary tract infecting bacteria in vitro and host-toxicity testing. J. App. Biomed. 2018, 16, 120–125. [Google Scholar] [CrossRef]
- Santhoshkumar, J.; Kumar, S.V.; Rajeshkumar, S. Synthesis of zinc oxide nanoparticles using plant leaf extract against urinary tract infection pathogen. Resour. Effic. Technol. 2017, 3, 459–465. [Google Scholar] [CrossRef]
- Paralikar, P.; Ingle, A.P.; Tiwari, V.; Golinska, P.; Dahm, H.; Rai, M. Evaluation of antibacterial efficacy of sulfur nanoparticles alone and in combination with antibiotics against multidrug-resistant uropathogenic bacteria. J. Environ. Sci. Health Part A Toxic Hazard Subst. Environ. Eng. 2019, 54, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Yogapiya, R.; Balakrishnaraja, R.; Gowthamraj, G. Comparative analysis and synthesis of silver nano-particles from selected parts of Mimosa pudica to treat urinary tract infection. Res. Sq. 2021; preprint. [Google Scholar] [CrossRef]
- Ranjan, M.P.; Das, M.P.; Kumar, M.S.; Anbarasi, P.; Sindhu, S.; Sagadevan, E.; Arumugam, P. Green synthesis and characteriza-tion of silver nanoparticles from Nigella sativa and its application against UTI causing bacteria. J. Acad. Ind. Res. 2013, 2, 45–49. [Google Scholar]
- Alshahrani, M.Y.; Rafi, Z.; Alabdallah, N.M.; Shoaib, A.; Ahmad, I.; Asiri, M.; Zaman, G.S.; Wahab, S.; Saeed, M.; Khan, S. A comparative antibacterial, antioxidant, and antineoplastic potential of Rauwolfia serpentina (l.) leaf extract with its biologically synthesized gold nanoparticles (r-aunps). Plants 2021, 10, 2278. [Google Scholar] [CrossRef] [PubMed]
- Yüksel, E.; Karakeçili, A.; Demirtaş, T.T.; Gümüşderelioğlu, M. Preparation of bioactive and antimicrobial PLGA membranes by magainin II/EGF functionalization. Int. J. Biol. Macromol. 2016, 86, 162–168. [Google Scholar] [CrossRef]
- Medeiros-Neves, B.; Nemitz, M.C.; Fachel, F.N.S.; Teixeira, H.F. Recent patents concerning the use of nanotechnology-based delivery systems as skin penetration enhancers. Recent Pat. Drug Deliv. Formul. 2019, 13, 192–202. [Google Scholar] [CrossRef]
- Manson, J.E.; Chlebowski, R.T.; Stefanick, M.L.; Aragaki, A.K.; Rossouw, J.E.; Prentice, R.L.; Anderson, G.; Howard, B.V.; Thomson, C.A.; LaCroix, A.Z.; et al. Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the women’s health initiative randomized trials. JAMA 2013, 310, 1353–1368. [Google Scholar] [CrossRef]
- Chen, M.N.; Lin, C.C.; Liu, C.F. Efficacy of phytoestrogens for menopausal symptoms: A meta-analysis and systematic review. Climacteric 2015, 18, 260–269. [Google Scholar] [CrossRef]
- Mathur, M.; Vyas, G. Role of nanoparticles for production of smart herbal drug-An overview. Indian J. Nat. Prod. Resour. 2013, 4, 329–338. [Google Scholar]
- Tang, J.; Xu, N.; Ji, H.; Liu, H.; Wang, Z.; Wu, L. Eudragit nanoparticles containing genistein: Formulation, development, and bioavailability assessment. Int. J. Nanomed. 2011, 6, 2429. [Google Scholar]
- Bilal, I.; Chowdhury, A.; Davidson, J.; Whitehead, S. Phytoestrogens and prevention of breast cancer: The contentious debate. World J. Clin. Oncol. 2014, 5, 705–712. [Google Scholar] [CrossRef] [PubMed]
- Huang, L.; Wang, Z.; Liu, G.; Wu, Y.; Yang, C.; Mei, L.; Zhang, H.; Zeng, X. Fabrication of genistein-loaded biodegradable TPGS-b-PCL nanoparticles for improved therapeutic effects in cervical cancer cells. Int. J. Nanomed. 2015, 10, 2461–2473. [Google Scholar] [CrossRef] [Green Version]
- Johnson, A.; Roberts, R.L.; Elkins, G. Complementary and alternative medicine for menopause. J. Evid. Based Integr. Med. 2019, 24, 2515690X19829380. [Google Scholar] [CrossRef] [Green Version]
- Ruhlen, R.L.; Sun, G.Y.; Sauter, E.R. Black cohosh: Insights into its mechanism(s) of action. Integr. Med. Insights 2008, 3, 21–32. [Google Scholar] [CrossRef] [Green Version]
- Masserini, M. Nanoparticles for brain drug delivery. ISRN Biochem. 2013, 2013, 238428. [Google Scholar] [CrossRef] [Green Version]
- de Almeida Borges, V.R.; da Silva, J.H.; Barbosa, S.S.; Nasciutti, L.E.; Cabral, L.M.; de Sousa, V.P. Development and pharmacological evaluation of in vitro nanocarriers composed of lamellar silicates containing copaiba oil-resin for treatment of endometriosis. Mater. Sci. Eng. C Mater. Biol. Appl. 2016, 64, 310–317. [Google Scholar] [CrossRef]
- Bischoff, E. Potency, selectivity, and consequences of nonselectivity of PDE inhibition. Int. J. Impot Res. 2004, 16 (Suppl. 1), S11–S14. [Google Scholar] [CrossRef] [Green Version]
- Wang, A.Y.; Podlasek, C.A. Role of nanotechnology in erectile dysfunction treatment. J. Sex Med. 2017, 14, 36–43. [Google Scholar] [CrossRef] [Green Version]
- Han, G.; Tar, M.; Kuppam, D.S.; Friedman, A.; Melman, A.; Friedman, J.; Davies, K.P. Nanoparticles as a novel delivery vehicle for therapeutics targeting erectile dysfunction. J. Sex. Med. 2010, 7, 224–233. [Google Scholar] [CrossRef] [PubMed]
- Ratan, Z.A.; Haidere, M.F.; Hong, Y.H.; Park, S.H.; Lee, J.O.; Lee, J.; Cho, J.Y. Pharmacological potential of ginseng and its major component ginsenosides. J. Ginseng Res. 2021, 45, 199–210. [Google Scholar] [CrossRef]
- Choi, Y.D.; Xin, Z.C.; Choi, H.K. Effect of korean red ginseng on the rabbit corpus cavernosal smooth muscle. Int. J. Impot Res. 1998, 10, 37–43. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Stamm, W.E.; Norrby, S.R. Urinary tract infections: Disease panorama and challenges. J. Infect. Dis. 2001, 183, S1–S4. [Google Scholar] [CrossRef] [PubMed]
- Bacheller, C.D.; Bernstein, J.M. Urinary tract infections. Med. Clin. N. Am. 1997, 81, 719–730. [Google Scholar] [CrossRef]
- Wagenlehner, F.M.; Naber, K.G. Uncomplicated urinary tract infections in women. Curr. Opin. Urol. 2001, 11, 49–53. [Google Scholar] [CrossRef] [PubMed]
- Lichtenberger, P.; Hooton, T.M. Complicated urinary tract infections. Curr. Infect. Dis. Rep. 2008, 10, 499–504. [Google Scholar] [CrossRef]
- Nielubowicz, G.R.; Mobley, H.L. Host-pathogen interactions in urinary tract infection. Nat. Rev. Urol. 2010, 7, 430–441. [Google Scholar] [CrossRef]
- Foxman, B. Urinary tract infection syndromes: Occurrence, recurrence, bacteriology, risk factors, and disease burden. Infect. Dis. Clin. N. Am. 2014, 28, 1–13. [Google Scholar] [CrossRef]
- Jacobsen, S.M.; Stickler, D.J.; Mobley, H.L.; Shirtliff, M.E. Complicated catheter-associated urinary tract infections due to Escherichia coli and Proteus mirabilis. Clin. Microbiol. Rev. 2008, 21, 26–59. [Google Scholar] [CrossRef] [Green Version]
- Levison, M.E.; Kaye, D. Treatment of complicated urinary tract infections with an emphasis on drug-resistant gram-negative uropathogens. Curr. Infect. Dis. Rep. 2013, 15, 109–115. [Google Scholar] [CrossRef] [PubMed]
- Ferrer, M.; Méndez-García, C.; Rojo, D.; Barbas, C.; Moya, A. Antibiotic use and microbiome function. Biochem. Pharmacol. 2017, 134, 114–126. [Google Scholar] [CrossRef] [PubMed]
- María, F.C.S. Antibiotic resistance in urinary infection: The never-ending story. Bol. Med. Hosp. Infant. Mex. 2014, 71, 329–331. [Google Scholar] [CrossRef] [Green Version]
- Sharma, I.; Chanda, S.; Yaiphathoi, S. In silico screening of some phytochemicals for treating urinary tract infection (UTI) targeting fimh gene. Afr. J. Biol. Sci. 2021, 3, 157–164. [Google Scholar] [CrossRef]
- Kamaruzzaman, N.F.; Tan, L.P.; Hamdan, R.H.; Choong, S.S.; Wong, W.K.; Gibson, A.J.; Chivu, A.; Pina, M.F. Antimicrobial polymers: The potential replacement of existing antibiotics? Int. J. Mol. Sci. 2019, 20, 2747. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sánchez, S.V.; Navarro, N.; Catalán-Figueroa, J.; Morales, J.O. Nanoparticles as potential novel therapies for urinary tract infections. Front. Cell. Infect. Microbiol. 2021, 11, 656496. [Google Scholar] [CrossRef]
- Kaur, A.; Gupta, S.; Tyagi, A.; Sharma, R.K.; Ali, J.; Gabrani, R.; Dang, S. Development of nanoemulsion based gel loaded with phytoconstituents for the treatment of urinary tract infection and in vivo biodistribution studies. Adv. Pharm. Bull. 2017, 7, 611–619. [Google Scholar] [CrossRef] [Green Version]
- Kaur, A.; Saxena, Y.; Bansal, R.; Gupta, S.; Tyagi, A.; Sharma, R.K.; Ali, J.; Panda, A.K.; Gabrani, R.; Dang, S. Intravaginal delivery of polyphenon 60 and curcumin nanoemulsion gel. AAPS PharmSciTech 2017, 18, 2188–2202. [Google Scholar] [CrossRef]
- Qasim, M.; Singh, B.R.; Naqvi, A.H.; Paik, P.; Das, D. Silver nanoparticles embedded mesoporous SiO2 nanosphere: An effective anticandidal agent against Candida albicans 077. Nanotechnology 2015, 26, 285102. [Google Scholar] [CrossRef]
- Rajivgandhi, G.; Maruthupandy, M.; Muneeswaran, T.; Ramachandran, G.; Manoharan, N.; Quero, F.; Anand, M.; Song, J.M. Biologically synthesized copper oxide nanoparticles enhanced intracellular damage in ciprofloxacin resistant esbl producing bacteria. Microb. Pathog. 2019, 127, 267–276. [Google Scholar] [CrossRef]
- Markovi, T.; Markovi, D.; Peri, T.; Stojkovi, D.; Sokovi, M. Screening of antimicrobial and antioxidant activity of commercial Melaleuca alternifolia (tea tree) essential oils. J. MedPlant Res. 2012, 6, 3852–3858. [Google Scholar]
- Chandra, H.; Patel, D.; Kumari, P.; Jangwan, J.S.; Yadav, S. Phyto-mediated synthesis of zinc oxide nanoparticles of Berberis aristata: Characterization, antioxidant activity and antibacterial activity with special reference to urinary tract pathogens. Mater. Sci. Eng. C Mater. Biol. Appl. 2019, 102, 212–220. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.; Rajeshkumar, S.; Madasamy, M.; Mahendran, V. Green synthesis of copper nanoparticles using Cissus vitiginea and its antioxidant and antibacterial activity against urinary tract infection pathogens. Artif. Cells Nanomed. Biotechnol. 2020, 48, 1153–1158. [Google Scholar] [CrossRef]
- Badiger, A.S.; Maruthi, K.R.; Bajpe, S.N.; Ramu, R.; Jayadev, K. Urinary tract infection - A review on its prevalence and recent advances. J. Pharm. Res. Int. 2021, 33, 582–592. [Google Scholar] [CrossRef]
- Khan, S.; Ibrahim, B.; Akram, M.; Shakil, S.; Ahmad, A.; Ali, S.M.; Siddiqui, M.; Khan, A.U. Antibacterial activity of herbal extracts against multi drug resistant strains of bacteria from clinical origin. Life Sci. Leafl. 2011, 1, 490–498. [Google Scholar]
- Paul, A.K.; Smith, C.M.; Rahmatullah, M.; Nissapatorn, V.; Wilairatana, P.; Spetea, M.; Gueven, N.; Dietis, N. Opioid analgesia and opioid-induced adverse effects: A review. Pharmaceuticals 2021, 14, 1091. [Google Scholar] [CrossRef]
- Warner, T.T. Chapter 8—Movement disorders. In Practical Guide to Neurogenetics; Warner, T.T., Hammans, S.R., Eds.; W.B. Saunders: Philadelphia, PA, USA, 2009; Chapter 8; pp. 102–136. [Google Scholar]
- Di Vico, I.A.; Cirillo, G.; Tessitore, A.; Siciliano, M.; Venturelli, M.; Falup-Pecurariu, C.; Tedeschi, G.; Morgante, F.; Tinazzi, M. Fatigue in hypokinetic, hyperkinetic, and functional movement disorders. Parkinsonism Relat. Disord. 2021, 86, 114–123. [Google Scholar] [CrossRef]
- Paul, A.K.; Gueven, N.; Dietis, N. Profiling the effects of repetitive morphine administration on motor behavior in rats. Molecules 2021, 26, 4355. [Google Scholar] [CrossRef]
- Paul, A.K.; Gueven, N.; Dietis, N. Morphine dosing strategy plays a key role in the generation and duration of the produced antinociceptive tolerance. Neuropharmacology 2017, 121, 158–166. [Google Scholar] [CrossRef]
- Paul, A.K.; Gueven, N.; Dietis, N. Age-dependent antinociception and behavioral inhibition by morphine. Pharmacol. Biochem. Behav. 2018, 168, 8–16. [Google Scholar] [CrossRef]
- Rai, S.N.; Chaturvedi, V.K.; Singh, P.; Singh, B.K.; Singh, M. Mucuna pruriens in parkinson’s and in some other diseases: Recent advancement and future prospective. 3 Biotech 2020, 10, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Mohapatra, S.; Ganguly, P.; Singh, R.; Katiyar, C.K. Estimation of levodopa in the unani drug Mucuna pruriens bak. and its marketed formulation by high-performance thin-layer chromatographic technique. J. AOAC Int. 2020, 103, 678–683. [Google Scholar] [CrossRef] [PubMed]
- Kasture, S.; Mohan, M.; Kasture, V. Mucuna pruriens seeds in treatment of parkinson’s disease: Pharmacological review. Ori. Pharm. Exp. Med. 2013, 13, 165–174. [Google Scholar] [CrossRef]
- Cilia, R.; Laguna, J.; Cassani, E.; Cereda, E.; Pozzi, N.G.; Isaias, I.U.; Contin, M.; Barichella, M.; Pezzoli, G. Mucuna pruriens in parkinson’s disease: A double-blind, randomized, controlled, crossover study. Neurology 2017, 89, 432–438. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cilia, R.; Laguna, J.; Cassani, E.; Cereda, E.; Raspini, B.; Barichella, M.; Pezzoli, G. Daily intake of Mucuna pruriens in advanced parkinson’s disease: A 16-week, noninferiority, randomized, crossover, pilot study. Parkinsonism Relat. Disord. 2018, 49, 60–66. [Google Scholar] [CrossRef]
- Cassani, E.; Cilia, R.; Laguna, J.; Barichella, M.; Contin, M.; Cereda, E.; Isaias, I.U.; Sparvoli, F.; Akpalu, A.; Budu, K.O. Mucuna pruriens for parkinson’s disease: Low-cost preparation method, laboratory measures and pharmacokinetics profile. J. Neurol. Sci. 2016, 365, 175–180. [Google Scholar] [CrossRef] [Green Version]
- Katzenschlager, R.; Evans, A.; Manson, A.; Patsalos, P.; Ratnaraj, N.; Watt, H.; Timmermann, L.; Van der Giessen, R.; Lees, A. Mucuna pruriens in parkinson’s disease: A double blind clinical and pharmacological study. J. Neurol. Neurosurg Psychiatr. 2004, 75, 1672–1677. [Google Scholar] [CrossRef] [Green Version]
- Lieu, C.A.; Venkiteswaran, K.; Gilmour, T.P.; Rao, A.N.; Petticoffer, A.C.; Gilbert, E.V.; Deogaonkar, M.; Manyam, B.V.; Subramanian, T. The antiparkinsonian and antidyskinetic mechanisms of Mucuna pruriens in the MPTP-treated nonhuman primate. Evid. Based Comp. Altern. Med. 2012, 2012, 840247. [Google Scholar] [CrossRef] [Green Version]
- Johnson, S.L.; Park, H.Y.; DaSilva, N.A.; Vattem, D.A.; Ma, H.; Seeram, N.P. Levodopa-reduced Mucuna pruriens seed extract shows neuroprotective effects against parkinson’s disease in murine microglia and human neuroblastoma cells, Caenorhabditis elegans, and Drosophila melanogaster. Nutrients 2018, 10, 1139. [Google Scholar] [CrossRef] [Green Version]
- Arulkumar, S.; Sabesan, M. The behavioral performance tests of Mucuna pruriens gold nanoparticles in the 1-methyl 4-phenyl-1, 2, 3, 6-tetrahydropyridine treated mouse model of parkinsonism. Asia Pac. J. Trop. Dis. 2012, 2, S499–S502. [Google Scholar] [CrossRef]
- Gopalakrishnan, L.; Doriya, K.; Kumar, D.S. Moringa oleifera: A review on nutritive importance and its medicinal application. Food Sci. Hum. Welln. 2016, 5, 49–56. [Google Scholar] [CrossRef] [Green Version]
- Meireles, D.; Gomes, J.; Lopes, L.; Hinzmann, M.; Machado, J. A review of properties, nutritional and pharmaceutical applications of Moringa oleifera: Integrative approach on conventional and traditional asian medicine. Adv. Trad. Med. 2020, 20, 495–515. [Google Scholar] [CrossRef]
- Bakre, A.G.; Aderibigbe, A.O.; Ademowo, O.G. Studies on neuropharmacological profile of ethanol extract of Moringa oleifera leaves in mice. J. Ethnopharmacol. 2013, 149, 783–789. [Google Scholar] [CrossRef] [PubMed]
- Igado, O.O.; Andrioli, A.; Azeez, I.A.; Girolamo, F.; Errede, M.; Aina, O.O.; Glaser, J.; Holzgrabe, U.; Bentivoglio, M.; Olopade, J.O. The ameliorative effects of a phenolic derivative of Moringa oleifera leave against vanadium-induced neurotoxicity in mice. IBRO Rep. 2020, 9, 164–182. [Google Scholar] [CrossRef]
- Kirisattayakul, W.; Wattanathorn, J.; Tong-Un, T.; Muchimapura, S.; Wannanon, P.; Jittiwat, J. Cerebroprotective effect of Moringa oleifera against focal ischemic stroke induced by middle cerebral artery occlusion. Oxidative Med. Cell. Long. 2013, 2013, 951415. [Google Scholar]
- Joy, A.E.; Shyamjith, M.; Bhat, K.S. Acute effect of ethanolic extract of Moringa oleifera on haloperidol induced catalepsy in mice models. Drug Invent. Today 2012, 4, 543–545. [Google Scholar]
- Bhattacharya, A.; Naik, M.R.; Agrawal, D.; Sahu, P.K.; Kumar, S.; Mishra, S.S. Cns depressant and muscle relaxant effect of ethanolic leaf extract of Moringa oleifera on Albino rats. Int. J. PharmTech Res. 2014, 6, 1441–1449. [Google Scholar]
- Prasad, T.N.; Elumalai, E.K. Biofabrication of ag nanoparticles using Moringa oleifera leaf extract and their antimicrobial activity. Asian Pac. J. Trop. Biomed. 2011, 1, 439–442. [Google Scholar] [CrossRef] [Green Version]
- Sathyavathi, R.; Krishna, M.B.; Rao, D.N. Biosynthesis of silver nanoparticles using Moringa oleifera leaf extract and its application to optical limiting. J. Nanosci. Nanotechnol. 2011, 11, 2031–2035. [Google Scholar] [CrossRef]
- Shousha, W.G.; Aboulthana, W.M.; Salama, A.H.; Saleh, M.H.; Essawy, E.A. Evaluation of the biological activity of Moringa oleifera leaves extract after incorporating silver nanoparticles, in vitro study. Bull. Nat. Res. Centr. 2019, 43, 212. [Google Scholar] [CrossRef] [Green Version]
- Adedara, I.A.; Awogbindin, I.O.; Owoeye, O.; Maduako, I.C.; Ajeleti, A.O.; Owumi, S.E.; Patlolla, A.K.; Farombi, E.O. Kolaviron via anti-inflammatory and redox regulatory mechanisms abates multi-walled carbon nanotubes-induced neurobehavioral deficits in rats. Psychopharmacology 2020, 237, 1027–1040. [Google Scholar] [CrossRef] [PubMed]
- Farombi, E.O.; Adedara, I.A.; Ajayi, B.O.; Ayepola, O.R.; Egbeme, E.E. Kolaviron, a natural antioxidant and anti-inflammatory phytochemical prevents dextran sulphate sodium-induced colitis in rats. Basic Clin. Pharmacol. Toxicol. 2013, 113, 49–55. [Google Scholar] [CrossRef] [PubMed]
| Plant Source | Formulation | Study Type | Action | Reference |
|---|---|---|---|---|
| Citrus fruits, onions, apples, parsley, sage, tea, and berries. | Nanoencapsulated quercetin in zein nanoparticles (NPQ) | Preclinical (rats) | NPQ improved memory and cognitive ability in rats (but no effects on locomotor activity test) | [37,38] |
| Citrus fruits, onions, apples, parsley, sage, tea, and berries. | Quercetin nanoparticles | Preclinical (rats) | Quercetin nanoparticles improved memory and pathological damage induced by scopolamine | [39,40] |
| Berries, currants, grapes, red to purplish blue colored leafy vegetables, grains, roots, and tubers. | Anthocyanin-loaded poly (ethylene glycol)-gold nanoparticles (PEG-AuNPs) | Preclinical (mice) | PEG-AuNPs improved amyloid-beta (Aβ1-42) induced neuronal damage and neuroinflammation | [41,42] |
| Curcuma longa L. (Zingiberaceae) | Nano-curcumin particles | Preclinical (mice) | Enhanced memory, motor function, contextual fear | [43] |
| Anamirtacocculus (L.) Wight and Arn. (Menispermaceae) | A.cocculus NPs in cocc 30c, in a homeopathic formulation | Preclinical | Improved attention and motor functions in sleep-deprived rats | [44] |
| Solanum tuberosum L. (Solanaceae) | S.tuberosum Lectin NPs | Preclinical | Helped improved drug delivery enhanced memory and motor function | [45] |
| Azadirachta indica A.Juss. (Meliaceae) | Neem oil incorporated in argan-liposomes and argan-hyalurosomes by sonicating with argan oil, soy lecithin, and water | In vitro | Protected skin cells by reducing oxidative stress | [46]. |
| Curcuma longa L. (Zingiberaceae) | Curcumin formulated with lipid-based nanoparticles such as liposomes, niosomes, solid lipid nanoparticles, and nanostructured lipid carriers | Review | Improved its penetration into skin and thus increased the solubility, stability, and therapeutic efficiencies of curcumin against various dermatological disorders such as psoriasis, dermatitis, bacterial, viral and fungal infections, burns, acne, arthritis, and skin cancer | [33,34] |
| Curcuma longa L. (Zingiberaceae) | C. longa leaves extract Silver nanoparticles (CL-AgNPs) loaded cotton fabric | In vitro | Enhanced wound healing and antimicrobial activity on skin | [47] |
| Curcuma longa L.(Zingiberaceae) | Solid lipid nanoparticles (SLN-curcuminoids) | Ex vivo (Sheep ear skin) | Showed good spreadability and stability on skin | [48] |
| Curcuma longa L. (Zingiberaceae) | Curcumin nanoparticles (curc-NPs) | Preclinical (rats) | Improved erectile response in diabetic male rats | [49,50] |
| Panax ginseng C.A. Mey (Araliaceae) | P.ginseng nanoparticles | Preclinical (rats) | Improved serum testosterone secretion and decrease sperm abnormalities in male rats | [51] |
| Oxaliscorniculata L. (Oxalidaceae) | Aqueous extract of O. corniculata and its biofabricated silver nanoparticles (AgNPs) | In vitro | Effective against urinary tract infection (UTI) causing microorganisms | [52] |
| Anogeissusacuminata Wall.(Combretaceae) | Aqueous leaf extract of A. acuminata and its AgNPs | In vitro | Effective against multidrug resistant UTI causing bacteria | [53] |
| Passiflora caerulea L. (Passifloraceae) | Zinc oxide nanoparticles (ZnO NPs) using P. caerulea extract | In vitro | Effective against multidrug resistant UTI causing bacteria | [54] |
| Catharanthus roseus (L.) G. Don (Apocynaceae) | Sulphur nanoparticles (SNPs) produced from C. roseus leaf extract | In vitro | Effective against multidrug resistant UTI causing bacteria | [55] |
| Mimosa pudica L. (Fabaceae) | Sulphur nanoparticles (SNPs) produced from M. pudica alcoholic extracts | In vitro | Antibacterial effects on uropathogenic E. coli (UPEC) and S. aureus and other UTI pathogens | [56] |
| Nigella sativa L. (Ranunculaceae) | Sulphur nanoparticles (SNPs) produced from seeds of N. sativa L. alcoholic extracts | In vitro | Antibacterial effects on UPEC and S. aureus and other UTI pathogens | [57] |
| Rauwolfia serpentina L. (Apocynaceae) | Biologically synthe-sized gold nanopar-ticles with aqueous leaf extract of R. serpentina L. | In vitro | Antibacterial effects on E. coli and S. aureus | [58] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rajagopal, M.; Paul, A.K.; Lee, M.-T.; Joykin, A.R.; Por, C.-S.; Mahboob, T.; Salibay, C.C.; Torres, M.S.; Guiang, M.M.M.; Rahmatullah, M.; et al. Phytochemicals and Nano-Phytopharmaceuticals Use in Skin, Urogenital and Locomotor Disorders: Are We There? Plants 2022, 11, 1265. https://doi.org/10.3390/plants11091265
Rajagopal M, Paul AK, Lee M-T, Joykin AR, Por C-S, Mahboob T, Salibay CC, Torres MS, Guiang MMM, Rahmatullah M, et al. Phytochemicals and Nano-Phytopharmaceuticals Use in Skin, Urogenital and Locomotor Disorders: Are We There? Plants. 2022; 11(9):1265. https://doi.org/10.3390/plants11091265
Chicago/Turabian StyleRajagopal, Mogana, Alok K. Paul, Ming-Tatt Lee, Anabelle Rose Joykin, Choo-Shiuan Por, Tooba Mahboob, Cristina C. Salibay, Mario S. Torres, Maria Melanie M. Guiang, Mohammed Rahmatullah, and et al. 2022. "Phytochemicals and Nano-Phytopharmaceuticals Use in Skin, Urogenital and Locomotor Disorders: Are We There?" Plants 11, no. 9: 1265. https://doi.org/10.3390/plants11091265
APA StyleRajagopal, M., Paul, A. K., Lee, M.-T., Joykin, A. R., Por, C.-S., Mahboob, T., Salibay, C. C., Torres, M. S., Guiang, M. M. M., Rahmatullah, M., Jahan, R., Jannat, K., Wilairatana, P., de Lourdes Pereira, M., Lim, C. L., & Nissapatorn, V. (2022). Phytochemicals and Nano-Phytopharmaceuticals Use in Skin, Urogenital and Locomotor Disorders: Are We There? Plants, 11(9), 1265. https://doi.org/10.3390/plants11091265









