Mexican Plants and Derivates Compounds as Alternative for Inflammatory and Neuropathic Pain Treatment—A Review
Abstract
1. Introduction
2. Preclinical Studies of Mexican Medicinal Plants Used in Inflammatory and Neuropathic Pain Treatment
2.1. Salvia divinorum Epling and Játiva
2.2. Heliopsis longipes (A. Gray) S.F.Blake
2.3. Artemisia ludoviciana Nutt
2.4. Caulerpa mexicana Sonder ex Kützing
2.5. Agastache mexicana (Kunth) Lint and Epling
2.6. Ligusticum porteri J.M.Coult. and Rose
2.7. Clinopodium mexicanum Benth Govaerts
2.8. Tilia americana var Mexicana (Schltdl.) Hardin
2.9. Acourtia thurberi (A. Gray) Reveal and R. M. King
2.10. Cyrtopodium macrobulbon (Lex.) G.A. Romero and Carnevali
2.11. Ternstroemia sylvatica Schltdl. and Cham
2.12. Conyza filaginoides (D.C.) Hieron
2.13. Choisya ternata Kunth
2.14. Mimosa albida Humb. and Bonpl. ex Willd
2.15. Heterotheca inuloides Cass
2.16. Calea Zacatechichi Schltdl
2.17. Geranium bellum Rose
2.18. Piper auritum Kunth
2.19. Sphaeralcea angustifolia (Cav.) G. Don
2.20. Acacia farnesiana (Willd.) Kuntze
2.21. Rubus coriifolius Liebm
2.22. Oenothera rosea L’Hér. ex Aiton
2.23. Chamaedora tepejilote Oerst
2.24. Astianthus viminalis (Kunth) Baill
2.25. Brickellia veronicaefolia Kunth DC
2.26. Brickellia paniculata (Mill.) B.L.Rob
2.27. Justicia spicigera Schltdl
2.28. Lantana hispida Kunth
2.29. Pittocaulon bombycophole (Bullock), velatum (Greenm), praecox (Cav.) and hintonii H.Rob. and Brettell
2.30. Amphipterygium adstringens Standl
2.31. Gnaphalium sp.
2.32. Swietenia humilis Zucc
2.33. Ageratina pichinchensis (Kunth) R. King and H. Rob.
2.34. Tithonia tubaeformis (Jacq.) Cass
3. Future Directions in Preclinical Assays for Mexican Medicinal Plants
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Woolf, C.J. Central sensitization: Implications for the diagnosis and treatment of pain. Pain 2011, 152, S2–S15. [Google Scholar] [CrossRef]
- Jensen, T.S.; Baron, R.; Haanpää, M.; Kalso, E.; Loeser, J.D.; Rice, A.S.C.; Treede, R.D. A new definition of neuropathic pain. Pain 2011, 152, 2204–2205. [Google Scholar] [CrossRef]
- IASP. IASP Terminology. Available online: https://www.iasp-pain.org/Education/Content.aspx?ItemNumber=1698#Neuropathicpain (accessed on 9 September 2019).
- Treede, R.D.; Rief, W.; Barke, A.; Aziz, Q.; Bennett, M.I.; Benoliel, R.; Cohen, M.; Evers, S.; Finnerup, N.B.; First, M.B.; et al. A classification of chronic pain for ICD-11. Pain 2015, 156, 1003–1007. [Google Scholar] [CrossRef]
- Treede, R.-D.; Rief, W.; Barke, A.; Aziz, Q.; Bennett, M.I.; Benoliel, R.; Cohen, M.; Evers, S.; Finnerup, N.B.; First, M.B.; et al. Chronic pain as a symptom or a disease: The IASP Classification of Chronic Pain for the International Classification of Diseases (ICD-11). Pain 2019, 160, 19–27. [Google Scholar] [CrossRef]
- Fayaz, A.; Croft, P.; Langford, R.M.; Donaldson, L.J.; Jones, G.T. Prevalence of chronic pain in the UK: A systematic review and meta- analysis of population studies. BMJ Open 2016, 6, e010364. [Google Scholar] [CrossRef]
- Hylands-White, N.; Duarte, R.V.; Raphael, J.H. An overview of treatment approaches for chronic pain management. Rheumatol. Int. 2017, 37, 29–42. [Google Scholar] [CrossRef]
- Attal, N.; Cruccu, G.; Baron, R.; Haanpää, M.; Hansson, P.; Jensen, T.S.; Nurmikko, T. EFNS guidelines on the pharmacological treatment of neuropathic pain: 2010 revision. Eur. J. Neurol. 2010, 17, 1113–1123. [Google Scholar] [CrossRef] [PubMed]
- Carter, G.T.; Duong, V.; Ho, S.; Ngo, K.C.; Greer, C.L.; Weeks, D.L. Side effects of commonly prescribed analgesic medications. Phys. Med. Rehabil. Clin. N. Am 2014, 25, 457–470. [Google Scholar] [CrossRef]
- Garland, E.L. Treating chronic pain: The need for non-opioid options. Expert Rev. Clin. Pharmacol. 2014, 7, 545–550. [Google Scholar] [CrossRef]
- Finnerup, N.B.; Attal, N.; Haroutounian, S.; McNicol, E.; Baron, R.; Dworkin, R.H.; Gilron, I.; Haanpää, M.; Hansson, P.; Jensen, T.S.; et al. Pharmacotherapy for neuropathic pain in adults: A systematic review and meta-analysis. Lancet Neurol. 2015, 14, 162–173. [Google Scholar] [CrossRef]
- Finnerup, N.B.; Sindrup, S.H.; Jensen, T.S. The evidence for pharmacological treatment of neuropathic pain. Pain 2010, 150, 573–581. [Google Scholar] [CrossRef]
- Alonso-Castro, A.J.; Dominguez, F.; Maldonado-Miranda, J.J.; Castillo-Perez, L.J.; Carranza-Alvarez, C.; Solano, E.; Isiordia-Espinoza, M.A.; Del Carmen Juarez-Vazquez, M.; Zapata-Morales, J.R.; Argueta-Fuertes, M.A.; et al. Use of medicinal plants by health professionals in Mexico. J. Ethnopharmacol. 2017, 198, 81–86. [Google Scholar] [CrossRef]
- Estrada-Soto, S.; Sanchez-Recillas, A.; Navarrete-Vazquez, G.; Castillo-Espana, P.; Villalobos-Molina, R.; Ibarra-Barajas, M. Relaxant effects of Artemisia ludoviciana on isolated rat smooth muscle tissues. J. Ethnopharmacol. 2012, 139, 513–518. [Google Scholar] [CrossRef]
- Frei, B.; Baltisberger, M.; Sticher, O.; Heinrich, M. Medical ethnobotany of the Zapotecs of the Isthmus-Sierra (Oaxaca, Mexico). Documentation and assessment of indigenous uses. J. Ethnopharmacol. 1998, 62, 149–165. [Google Scholar] [CrossRef]
- Juárez-Vázquez, M.C.; Carranza-Alvarez, C.; Alonso-Castro, A.J.; Gonzalez-Alcaraz, V.F.; Bravo-Acevedo, E.; Chamarro-Tinajero, F.J.; Solano, E. Ethnobotany of medicinal plants used in Xalpatlahuac, Guerrero, Mexico. J. Ethnopharmacol. 2013, 148, 521–527. [Google Scholar] [CrossRef]
- Moreno-Salazar, S.F.; Robles-Zepeda, R.E.; Johnson, D.E. Plant folk medicines for gastrointestinal disorders among the main tribes of Sonora, Mexico. Fitoterapia 2008, 79, 132–141. [Google Scholar] [CrossRef]
- Robles-Zepeda, R.E.; Valenzuela-Antelo, O.; Garibay-Escobar, A.; Velázquez-Contreras, C.; Navarro-Navarro, M.; Contreras, L.R.; Corral, O.L.; Lozano-Taylor, J. Use of complementary and alternative medicine in a region of Northwest Mexico. J. Altern. Complement. Med. 2011, 17, 787–788. [Google Scholar] [CrossRef]
- Sanadgol, N.; Zahedani, S.S.; Sharifzadeh, M.; Khalseh, R.; Barbari, G.R.; Abdollahi, M. Recent Updates in Imperative Natural Compounds for Healthy Brain and Nerve Function: A Systematic Review of Implications for Multiple Sclerosis. Curr. Drug Targets 2017, 18, 1499–1517. [Google Scholar] [CrossRef]
- Valdivia-Correa, B.; Gómez-Gutiérrez, C.; Uribe, M.; Méndez-Sánchez, N. Herbal medicine in Mexico: A cause of hepatotoxicity. A critical review. Int. J. Mol. Sci. 2016, 17, 235. [Google Scholar] [CrossRef]
- Sharma, A.; Flores-Vallejo, R.D.C.; Cardoso-Taketa, A.; Villarreal, M.L. Antibacterial activities of medicinal plants used in Mexican traditional medicine. J. Ethnopharmacol. 2017, 208, 264–329. [Google Scholar] [CrossRef]
- Delgado-Altamirano, R.; Monzote, L.; Pinon-Tapanes, A.; Vibrans, H.; Rivero-Cruz, J.F.; Ibarra-Alvarado, C.; Rojas-Molina, A. In vitro antileishmanial activity of Mexican medicinal plants. Heliyon 2017, 3, e00394. [Google Scholar] [CrossRef] [PubMed]
- Andrade-Cetto, A.; Heinrich, M. Mexican plants with hypoglycaemic effect used in the treatment of diabetes. J. Ethnopharmacol. 2005, 99, 325–348. [Google Scholar] [CrossRef]
- Lopez-Rubalcava, C.; Estrada-Camarena, E. Mexican medicinal plants with anxiolytic or antidepressant activity: Focus on preclinical research. J. Ethnopharmacol. 2016, 186, 377–391. [Google Scholar] [CrossRef]
- Alvarez, L.; Nunez, M.; Del Carmen Perez, M.; Villarreal, M.L.; Delgado, G. Chemical and Biological Study of Astianthus viminalis. Planta Med. 1994, 60, 98. [Google Scholar] [CrossRef]
- Alonso-Castro, A.J.; Villarreal, M.L.; Salazar-Olivo, L.A.; Gomez-Sanchez, M.; Dominguez, F.; Garcia-Carranca, A. Mexican medicinal plants used for cancer treatment: Pharmacological, phytochemical and ethnobotanical studies. J. Ethnopharmacol. 2011, 133, 945–972. [Google Scholar] [CrossRef]
- Jacobo-Herrera, N.J.; Jacobo-Herrera, F.E.; Zentella-Dehesa, A.; Andrade-Cetto, A.; Heinrich, M.; Perez-Plasencia, C. Medicinal plants used in Mexican traditional medicine for the treatment of colorectal cancer. J. Ethnopharmacol. 2016, 179, 391–402. [Google Scholar] [CrossRef]
- Ibarra-Alvarado, C.; Rojas, A.; Mendoza, S.; Bah, M.; Gutierrez, D.M.; Hernandez-Sandoval, L.; Martinez, M. Vasoactive and antioxidant activities of plants used in Mexican traditional medicine for the treatment of cardiovascular diseases. Pharm. Biol. 2010, 48, 732–739. [Google Scholar] [CrossRef]
- Argueta, A.; Gallardo, V.M.C. Instituto Nacional Indigenista. In Atlas of Plants from Mexican Traditional Medicine, 1st ed.; National Indigenous Institute: Mexico City, Mexico, 1994; pp. 1355–1356. [Google Scholar]
- Gonzalez-Ramirez, A.; Gonzalez-Trujano, M.E.; Pellicer, F.; Lopez-Munoz Francisco, J. Anti-nociceptive and anti-inflammatory activities of the Agastache mexicana extracts by using several experimental models in rodents. J. Ethnopharmacol. 2012, 142, 700–705. [Google Scholar] [PubMed]
- Linares, E.; Bye, R.A.J. A study of four medicinal plant complexes of Mexico and adjacent United States. J. Ethnopharmacol. 1987, 19, 153–183. [Google Scholar] [CrossRef]
- John, T.F.; French, L.G.; Erlichman, J.S. The antinociceptive effect of salvinorin A in mice. Eur. J. Pharmacol. 2006, 545, 129–133. [Google Scholar] [CrossRef]
- McCurdy, C.R.; Sufka, K.J.; Smith, G.H.; Warnick, J.E.; Nieto, M.J. Antinociceptive profile of salvinorin A, a structurally unique kappa opioid receptor agonist. Pharmacol. Biochem. Behav. 2006, 83, 109–113. [Google Scholar] [CrossRef]
- Simon-Arceo, K.; Gonzalez-Trujano, M.E.; Coffeen, U.; Fernandez-Mas, R.; Mercado, F.; Almanza, A.; Contreras, B.; Jaimes, O.; Pellicer, F. Neuropathic and inflammatory antinociceptive effects and electrocortical changes produced by Salvia divinorum in rats. J. Ethnopharmacol. 2017, 206, 115–124. [Google Scholar] [CrossRef]
- Tlacomulco-Flores, L.L.; Deciga-Campos, M.; Gonzalez-Trujano, M.E.; Carballo-Villalobos, A.I.; Pellicer, F. Antinociceptive effects of Salvia divinorum and bioactive salvinorins in experimental pain models in mice. J. Ethnopharmacol. 2019, 248, 112276. [Google Scholar] [CrossRef]
- Molina-Torres, J.; Garcia-Chavez, A.; Ramirez-Chavez, E. Antimicrobial properties of alkamides present in flavouring plants traditionally used in Mesoamerica: Affinin and capsaicin. J. Ethnopharmacol. 1999, 64, 241–248. [Google Scholar] [CrossRef]
- Ogura, M.; Cordell, G.A.; Quinn, M.L.; Leon, C.; Benoit, P.S.; Soejarto, D.D.; Farnsworth, N.R. Ethnopharmacologic studies. I. Rapid solution to a problem—Oral use of Heliopsis longipes—By means of a multidisciplinary approach. J. Ethnopharmacol. 1982, 5, 215–219. [Google Scholar] [CrossRef]
- Little, E.L.J. Heliopsis longipes, a Mexican insecticidal plant species. J. Wash. Acad. Sci. 1948, 38, 269–274. [Google Scholar]
- Ortiz, M.I.; Carino-Cortes, R.; Perez-Hernandez, N.; Ponce-Monter, H.; Fernandez-Martinez, E.; Castaneda-Hernandez, G.; Acosta-Madrid, I.I.; Cilia-Lopez, V.G. Antihyperalgesia induced by Heliopsis longipes extract. Proc. West. Pharmacol Soc. 2009, 52, 75–77. [Google Scholar] [PubMed]
- Acosta-Madrid, I.I.; Castaneda-Hernandez, G.; Cilia-Lopez, V.G.; Carino-Cortes, R.; Perez-Hernandez, N.; Fernandez-Martinez, E.; Ortiz, M.I. Interaction between Heliopsis longipes extract and diclofenac on the thermal hyperalgesia test. Phytomedicine 2009, 16, 336–341. [Google Scholar] [CrossRef] [PubMed]
- Carino-Cortes, R.; Gayosso-De-Lucio, J.A.; Ortiz, M.I.; Sanchez-Gutierrez, M.; Garcia-Reyna, P.B.; Cilia-Lopez, V.G.; Perez-Hernandez, N.; Moreno, E.; Ponce-Monter, H. Antinociceptive, genotoxic and histopathological study of Heliopsis longipes S.F. Blake in mice. J. Ethnopharmacol. 2010, 130, 216–221. [Google Scholar] [CrossRef] [PubMed]
- Rios, M.Y.; Aguilar-Guadarrama, A.B.; Gutierrez, M.D.C. Analgesic activity of affinin, an alkamide from Heliopsis longipes (Compositae). J. Ethnopharmacol. 2007, 110, 364–367. [Google Scholar] [CrossRef]
- Deciga-Campos, M.; Rios, M.Y.; Aguilar-Guadarrama, A.B. Antinociceptive effect of Heliopsis longipes extract and affinin in mice. Planta Med. 2010, 76, 665–670. [Google Scholar] [CrossRef]
- de la Rosa-Lugo, V.; Acevedo-Quiroz, M.; Deciga-Campos, M.; Rios, M.Y. Antinociceptive effect of natural and synthetic alkamides involves TRPV1 receptors. J. Pharm. Pharmacol. 2017, 69, 884–895. [Google Scholar] [CrossRef] [PubMed]
- Cilia-Lopez, V.G.; Juarez-Flores, B.I.; Aguirre-Rivera, J.R.; Reyes-Aguero, J.A. Analgesic activity of Heliopsis longipes and its effect on the nervous system. Pharm. Biol. 2010, 48, 195–200. [Google Scholar] [CrossRef] [PubMed]
- Rodeiro, I.; Donato, M.T.; Jimenez, N.; Garrido, G.; Molina-Torres, J.; Menendez, R.; Castell, J.V.; Gomez-Lechon, M.J. Inhibition of human P450 enzymes by natural extracts used in traditional medicine. Phytother. Res. 2009, 23, 279–282. [Google Scholar] [CrossRef]
- Naturalista. Available online: https://www.naturalista.mx/observations (accessed on 12 November 2019).
- Monroy-Ortiz, C.; Castillo-España, P. Plantas Medicinales Utilizadas en el Estado de Morelos, 2nd ed.; Centro de Investigaciones Biológicas, Universidad Autonoma del Estado de Morelos: Cuernavaca, Mexico, 2007; pp. 58–62. [Google Scholar]
- Anaya-Eugenio, G.D.; Rivero-Cruz, I.; Rivera-Chavez, J.; Mata, R. Hypoglycemic properties of some preparations and compounds from Artemisia ludoviciana Nutt. J. Ethnopharmacol. 2014, 155, 416–425. [Google Scholar] [CrossRef]
- Estrada-Castillon, E.; Soto-Mata, B.E.; Garza-Lopez, M.; Villarreal-Quintanilla, J.A.; Jimenez-Perez, J.; Pando-Moreno, M.; Sanchez-Salas, J.; Scott-Morales, L.; Cotera-Correa, M. Medicinal plants in the southern region of the State of Nuevo Leon, Mexico. J. Ethnobiol. Ethnomed. 2012, 8, 45. [Google Scholar] [CrossRef]
- Castillo-Juarez, I.; Gonzalez, V.; Jaime-Aguilar, H.; Martinez, G.; Linares, E.; Bye, R.; Romero, I. Anti-Helicobacter pylori activity of plants used in Mexican traditional medicine for gastrointestinal disorders. J. Ethnopharmacol. 2009, 122, 402–405. [Google Scholar] [CrossRef]
- Castillo, S.L.; Heredia, N.; Contreras, J.F.; Garcia, S. Extracts of edible and medicinal plants in inhibition of growth, adherence, and cytotoxin production of Campylobacter jejuni and Campylobacter coli. J. Food Sci. 2011, 76, M421–M426. [Google Scholar] [CrossRef]
- Lopes-Lutz, D.; Alviano, D.S.; Alviano, C.S.; Kolodziejczyk, P.P. Screening of chemical composition, antimicrobial and antioxidant activities of Artemisia essential oils. Phytochemistry 2008, 69, 1732–1738. [Google Scholar] [CrossRef]
- Said Fernandez, S.; Ramos Guerra, M.C.; Mata Cardenas, B.D.; Vargas Villarreal, J.; Villarreal Trevino, L. In vitro antiprotozoal activity of the leaves of Artemisia ludoviciana. Fitoterapia 2005, 76, 466–468. [Google Scholar] [CrossRef]
- Anaya-Eugenio, G.D.; Rivero-Cruz, I.; Bye, R.; Linares, E.; Mata, R. Antinociceptive activity of the essential oil from Artemisia ludoviciana. J. Ethnopharmacol. 2016, 179, 403–411. [Google Scholar] [CrossRef] [PubMed]
- Carneiro, J.G.; Rodrigues, J.A.G.; de Sousa Oliveira Vanderlei, E.; Souza, R.B.; Quindere, A.L.G.; Coura, C.O.; de Araujo, I.W.F.; Chaves, H.V.; Bezerra, M.M.; Benevides, N.M.B. Peripheral antinociception and anti-inflammatory effects of sulphated polysaccharides from the alga Caulerpa mexicana. Basic Clin. Pharmacol. Toxicol. 2014, 115, 335–342. [Google Scholar] [CrossRef] [PubMed]
- Carneiro, J.G.; Holanda, T.B.L.; Quinderé, A.L.G.; Frota, A.F.; Soares, V.V.M.; Sousa, R.S.; Carneiro, M.A.; Martins, D.S.; Gomes-Duarte, A.S.; Benevides, N.M.B. Gastroprotective Effects of Sulphated Polysaccharides from the Alga Caulerpa mexicana Reducing Ethanol-Induced Gastric Damage. Pharmaceuticals 2018, 11, 6. [Google Scholar] [CrossRef]
- Da Matta, C.B.B.; de Souza, E.T.; de Queiroz, A.C.; de Lira, D.P.; de Araujo, M.V.; Cavalcante-Silva, L.H.A.; de Miranda, G.E.C.; de Araujo-Junior, J.X.; Barbosa-Filho, J.M.; de Oliveira Santos, B.V.; et al. Antinociceptive and anti-inflammatory activity from algae of the genus Caulerpa. Mar. Drugs 2011, 9, 307–318. [Google Scholar] [CrossRef]
- Sanders, R.W. Taxonomy of Agastache Section Brittonastrum (Lamiaceae-Nepeteae). Syst Bot Monogr. 1987, 15, 1–92. [Google Scholar] [CrossRef]
- Santillán-Ramírez, M.A.; López-Villafranco, M.E.; Aguilar-Rodríguez, S.; Aguilar-Contreras, A. Estudio etnobotánico, arquitectura foliar y anatomía vegetativa de Agastache mexicana ssp. mexicana y A. mexicana ssp. xolocotziana. Rev. Mex. Biodivers. 2008, 79, 513–524. [Google Scholar]
- Ventura-Martinez, R.; Rodriguez, R.; Gonzalez-Trujano, M.E.; Angeles-Lopez, G.E.; Deciga-Campos, M.; Gomez, C. Spasmogenic and spasmolytic activities of Agastache mexicana ssp. mexicana and A. mexicana ssp. xolocotziana methanolic extracts on the guinea pig ileum. J. Ethnopharmacol. 2017, 196, 58–65. [Google Scholar] [CrossRef]
- Navarrete, A.; Avila-Rosas, N.; Majin-Leon, M.; Balderas-Lopez, J.L.; Alfaro-Romero, A.; Tavares-Carvalho, J.C. Mechanism of action of relaxant effect of Agastache mexicana ssp.mexicana essential oil in guinea-pig trachea smooth muscle. Pharm. Biol. 2017, 55, 96–100. [Google Scholar] [CrossRef]
- Flores-Flores, A.; Hernandez-Abreu, O.; Rios, M.Y.; Leon-Rivera, I.; Aguilar-Guadarrama, B.; Castillo-Espana, P.; Perea-Arango, I.; Estrada-Soto, S. Vasorelaxant mode of action of dichloromethane-soluble extract from Agastache mexicana and its main bioactive compounds. Pharm. Biol. 2016, 54, 2807–2813. [Google Scholar] [CrossRef]
- Estrada-Reyes, R.; Lopez-Rubalcava, C.; Ferreyra-Cruz, O.A.; Dorantes-Barron, A.M.; Heinze, G.; Moreno Aguilar, J.; Martinez-Vazquez, M. Central nervous system effects and chemical composition of two subspecies of Agastache mexicana; an ethnomedicine of Mexico. J. Ethnopharmacol. 2014, 153, 98–110. [Google Scholar] [CrossRef] [PubMed]
- Carmona-Castro, G.; Estrada-Soto, S.; Arellano-Garcia, J.; Arias-Duran, L.; Valencia-Diaz, S.; Perea-Arango, I. High accumulation of tilianin in in-vitro cultures of Agastache mexicana and its potential vasorelaxant action. Mol. Biol. Rep. 2019, 46, 1107–1115. [Google Scholar] [CrossRef]
- Gonzalez-Trujano, M.E.; Ponce-Munoz, H.; Hidalgo-Figueroa, S.; Navarrete-Vazquez, G.; Estrada-Soto, S. Depressant effects of Agastache mexicana methanol extract and one of major metabolites tilianin. Asian Pac. J. Trop. Med. 2015, 8, 185–190. [Google Scholar] [CrossRef]
- Hernandez-Abreu, O.; Torres-Piedra, M.; Garcia-Jimenez, S.; Ibarra-Barajas, M.; Villalobos-Molina, R.; Montes, S.; Rembao, D.; Estrada-Soto, S. Dose-dependent antihypertensive determination and toxicological studies of tilianin isolated from Agastache mexicana. J. Ethnopharmacol. 2013, 146, 187–191. [Google Scholar] [CrossRef]
- Verano, J.; Gonzalez-Trujano, M.E.; Deciga-Campos, M.; Ventura-Martinez, R.; Pellicer, F. Ursolic acid from Agastache mexicana aerial parts produces antinociceptive activity involving TRPV1 receptors, cGMP and a serotonergic synergism. Pharmacol. Biochem. Behav. 2013, 110, 255–264. [Google Scholar] [CrossRef]
- Gonzalez-Trujano, M.E.; Ventura-Martinez, R.; Chavez, M.; Diaz-Reval, I.; Pellicer, F. Spasmolytic and antinociceptive activities of ursolic acid and acacetin identified in Agastache mexicana. Planta Med. 2012, 78, 793–796. [Google Scholar] [CrossRef]
- Bhat, R.A.; Lingaraju, M.C.; Pathak, N.N.; Kalra, J.; Kumar, D.; Kumar, D.; Tandan, S.K. Effect of ursolic acid in attenuating chronic constriction injury-induced neuropathic pain in rats. Fundam. Clin. Pharmacol. 2016, 30, 517–528. [Google Scholar] [CrossRef]
- Appelt, G.D. Pharmacological aspects of selected herbs employed in Hispanic folk medicine in the San Luis Valley of Colorado, USA: I. Ligusticum porteri (osha) and Matricaria chamomilla (manzanilla). J. Ethnopharmacol. 1985, 13, 51–55. [Google Scholar] [CrossRef]
- Bye, R.A. Medicinal plants of the sierra madre: Comparative study of tarahumara and Mexican market plants. Econ. Bot. 1986, 40, 103–124. [Google Scholar] [CrossRef]
- Velazquez-Moyado, J.A.; Martinez-Gonzalez, A.; Linares, E.; Bye, R.; Mata, R.; Navarrete, A. Gastroprotective effect of diligustilide isolated from roots of Ligusticum porteri coulter & rose (Apiaceae) on ethanol-induced lesions in rats. J. Ethnopharmacol. 2015, 174, 403–409. [Google Scholar] [PubMed]
- Velazquez-Moyado, J.A.; Balderas-Lopez, J.L.; Pineda-Pena, E.A.; Sanchez-Ortiz, B.L.; Tavares-Carvalho, J.C.; Navarrete, A. Diligustilide releases H2S and stabilizes S-nitrosothiols in ethanol- induced lesions on rat gastric mucosa. Inflammopharmacology 2018, 26, 611–619. [Google Scholar] [CrossRef]
- Pineda-Pena, E.A.; Meza-Perez, D.G.; Chavez-Pina, A.E.; Velazquez-Moyado, J.A.; Tavares-Carvalho, J.C.; Navarrete Castro, A. Pharmacodynamic interaction of 3alpha-hydroxymasticadienonic acid and diligustilide against indomethacin-induced gastric damage in rats. Drug Dev. Res. 2019, 80, 585–594. [Google Scholar]
- Leon, A.; Toscano, R.A.; Tortoriello, J.; Delgado, G. Phthalides and other constituents from Ligusticum porteri; sedative and spasmolytic activities of some natural products and derivatives. Nat. Prod. Res. 2011, 25, 1234–1242. [Google Scholar] [CrossRef]
- Del-Angel, M.; Nieto, A.; Ramirez-Apan, T.; Delgado, G. Anti-inflammatory effect of natural and semi-synthetic phthalides. Eur. J. Pharmacol. 2015, 752, 40–48. [Google Scholar] [CrossRef]
- Juarez-Reyes, K.; Angeles-Lopez, G.E.; Rivero-Cruz, I.; Bye, R.; Mata, R. Antinociceptive activity of Ligusticum porteri preparations and compounds. Pharm. Biol. 2014, 52, 14–20. [Google Scholar] [CrossRef]
- Deciga-Campos, M.; Gonzalez-Trujano, E.; Navarrete, A.; Mata, R. Antinociceptive effect of selected Mexican traditional medicinal species. Proc. West. Pharmacol Soc. 2005, 48, 70–72. [Google Scholar]
- Castaneda Sortibran, A.; Tellez, M.G.O.; Ocotero, V.M.; Carballo-Ontiveros, M.A.; Garcia, A.M.; Valdes, R.J.J.; Gutierrez, E.R.; Rodriguez-Arnaiz, R. Chronic toxicity, genotoxic assay, and phytochemical analysis of four traditional medicinal plants. J. Med. Food 2011, 14, 1018–1022. [Google Scholar] [CrossRef] [PubMed]
- Deciga-Campos, M.; Rivero-Cruz, I.; Arriaga-Alba, M.; Castaneda-Corral, G.; Angeles-Lopez, G.E.; Navarrete, A.; Mata, R. Acute toxicity and mutagenic activity of Mexican plants used in traditional medicine. J. Ethnopharmacol. 2007, 110, 334–342. [Google Scholar] [CrossRef]
- León, A.; Delgado, G. Diligustilide: Enantiomeric Derivatives, Absolute Configuration and Cytotoxic Properties. J. Mex. Chem. Soc. 2012, 52, 222–226. [Google Scholar] [CrossRef]
- Estrada-Reyes, R.; Martinez-Vazquez, M.; Gallegos-Solis, A.; Heinze, G.; Moreno, J. Depressant effects of Clinopodium mexicanum Benth. Govaerts (Lamiaceae) on the central nervous system. J. Ethnopharmacol. 2010, 130, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Cassani, J.; Araujo, A.G.E.; Martinez-Vazquez, M.; Manjarrez, N.; Moreno, J.; Estrada-Reyes, R. Anxiolytic-like and antinociceptive effects of 2(S)-neoponcirin in mice. Molecules 2013, 18, 7584–7599. [Google Scholar] [CrossRef]
- The Plant List. Available online: http://www.theplantlist.org/ (accessed on 5 October 2019).
- Perez-Ortega, G.; Guevara-Fefer, P.; Chavez, M.; Herrera, J.; Martinez, A.; Martinez, A.L.; Gonzalez-Trujano, M.E. Sedative and anxiolytic efficacy of Tilia americana var. mexicana inflorescences used traditionally by communities of State of Michoacan, Mexico. J. Ethnopharmacol. 2008, 116, 461–468. [Google Scholar] [CrossRef] [PubMed]
- Aguirre-Hernandez, E.; Gonzalez-Trujano, M.E.; Martinez, A.L.; Moreno, J.; Kite, G.; Terrazas, T.; Soto-Hernandez, M. HPLC/MS analysis and anxiolytic-like effect of quercetin and kaempferol flavonoids from Tilia americana var. mexicana. J. Ethnopharmacol. 2010, 127, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Herrera-Ruiz, M.; Roman-Ramos, R.; Zamilpa, A.; Tortoriello, J.; Jimenez-Ferrer, J.E. Flavonoids from Tilia americana with anxiolytic activity in plus-maze test. J. Ethnopharmacol. 2008, 118, 312–317. [Google Scholar] [CrossRef]
- Aguirre-Hernandez, E.; Martinez, A.L.; Gonzalez-Trujano, M.E.; Moreno, J.; Vibrans, H.; Soto-Hernandez, M. Pharmacological evaluation of the anxiolytic and sedative effects of Tilia americana L. var. mexicana in mice. J. Ethnopharmacol. 2007, 109, 140–145. [Google Scholar] [CrossRef]
- Cardenas-Rodriguez, N.; Gonzalez-Trujano, M.E.; Aguirre-Hernandez, E.; Ruiz-Garcia, M.; Sampieri, A., 3rd; Coballase-Urrutia, E.; Carmona-Aparicio, L. Anticonvulsant and antioxidant effects of Tilia americana var. mexicana and flavonoids constituents in the pentylenetetrazole-induced seizures. Oxid Med. Cell Longev. 2014, 329172. [Google Scholar]
- Angeles-Lopez, G.E.; Gonzalez-Trujano, M.E.; Gomez, C.; Chanez-Cardenas, M.E.; Ventura-Martinez, R. Neuroprotective effects of Tilia americana var. mexicana on damage induced by cerebral ischaemia in mice. Nat. Prod. Res. 2016, 30, 2115–2119. [Google Scholar] [CrossRef]
- Martinez, A.L.; Gonzalez-Trujano, M.E.; Aguirre-Hernandez, E.; Moreno, J.; Soto-Hernandez, M.; Lopez-Munoz, F.J. Antinociceptive activity of Tilia americana var. mexicana inflorescences and quercetin in the formalin test and in an arthritic pain model in rats. Neuropharmacology 2009, 56, 564–571. [Google Scholar] [CrossRef]
- Rzedowski, J. Some aditions to the genus Acourtia (Compositae, Mutisieae). Bot. Sci. 1983, 97–109. [Google Scholar]
- Alarcon-Aguilar, F.J.; Roman-Ramos, R.; Jimenez-Estrada, M.; Reyes-Chilpa, R.; Gonzalez-Paredes, B.; Flores-Saenz, J.L. Effects of three Mexican medicinal plants (Asteraceae) on blood glucose levels in healthy mice and rabbits. J. Ethnopharmacol. 1997, 55, 171–177. [Google Scholar] [CrossRef]
- Martinez, A.L.; Madariaga-Mazon, A.; Rivero-Cruz, I.; Bye, R.; Mata, R. Antidiabetic and Antihyperalgesic Effects of a Decoction and Compounds from Acourtia thurberi. Planta Med. 2017, 83, 534–544. [Google Scholar] [CrossRef] [PubMed]
- Morales-Sanchez, V.; Rivero-Cruz, I.; Laguna-Hernandez, G.; Salazar-Chavez, G.; Mata, R. Chemical composition, potential toxicity, and quality control procedures of the crude drug of Cyrtopodium macrobulbon. J. Ethnopharmacol. 2014, 154, 790–797. [Google Scholar] [CrossRef] [PubMed]
- Tortoriello, J.; Romero, O. Plants used by Mexican traditional medicine with presumable sedative properties: An ethnobotanical approach. Arch. Med. Res. 1992, 23, 111–116. [Google Scholar]
- Gutiérrez, S.L.G.; Chilpa, R.R.; Jaime, H.B.; Guzmán Gutiérrez, S.L.; Reyes Chilpa, R.; Bonilla Jaime, H. Medicinal plants for the treatment of “nervios”, anxiety, and depression in Mexican Traditional Medicine. Rev. Bras. Farmacogn. 2014, 24, 591–608. [Google Scholar] [CrossRef]
- Moreno-Quiros, C.V.; Sanchez-Medina, A.; Vazquez-Hernandez, M.; Hernandez Reyes, A.G.; Garcia-Rodriguez, R.V. Antioxidant, anti-inflammatory and antinociceptive potential of Ternstroemia sylvatica Schltdl. & Cham. Asian Pac. J. Trop. Med. 2017, 10, 1047–1053. [Google Scholar]
- Balderas-Lopez, J.L.; Alfaro-Romero, A.; Monroy, A.; Lopez-Villafranco, M.E.; Rivero-Cruz, J.F.; Navarrete, A. Toxic rather than neuropharmacological effect of Ternstroemia sylvatica fruits and identification of 28-O-[beta-l-6-rhamnopyranosyl]-R1-barrigenol as a new compound with toxic effects in mice. Pharm. Biol. 2013, 51, 1451–1458. [Google Scholar] [CrossRef]
- Molina, M.; Contreras, C.M.; Tellez-Alcantara, P.; Rodriguez, F. Sedative actions of Ternstroemia sylvatica in the male rat. Phytomedicine 1999, 6, 115–118. [Google Scholar] [CrossRef]
- Rojas, A.; Cruz, S.; Rauch, V.; Bye, R.; Linares, E.; Mata, R. Spasmolytic potential of some plants used in Mexican traditional medicine for the treatment of gastrointestinal disorders. Phytomedicine 1995, 2, 51–55. [Google Scholar] [CrossRef]
- Ovalle-Magallanes, B.; Deciga-Campos, M.; Mata, R. Antinociceptive and hypoglycaemic evaluation of Conyza filaginoides (D.C.) Hieron Asteraceae. J. Pharm. Pharmacol. 2015, 67, 1733–1743. [Google Scholar] [CrossRef]
- Calzada, F.; Cedillo-Rivera, R.; Mata, R. Antiprotozoal activity of the constituents of Conyza filaginoides. J. Nat. Prod. 2001, 64, 671–673. [Google Scholar] [CrossRef]
- Mata, R.; Rojas, A.; Acevedo, L.; Estrada, S.; Calzada, F.; Rojas, I.; Bye, R.; Linares, E. Smooth muscle relaxing flavonoids and terpenoids from Conyza filaginoides. Planta Med. 1997, 63, 31–35. [Google Scholar] [CrossRef]
- Wahab, I.R.A.; Wong, N.S.H.; Boylan, F. Choisyaternatine, a new alkaloid isolated from Choisya ternata. Planta Med. 2012, 78, 1597–1600. [Google Scholar] [CrossRef] [PubMed]
- Radulovic, N.S.; Miltojevic, A.B.; McDermott, M.; Waldren, S.; Parnell, J.A.; Pinheiro, M.M.G.; Fernandes, P.D.; de Sousa Menezes, F. Identification of a new antinociceptive alkaloid isopropyl N-methylanthranilate from the essential oil of Choisya ternata Kunth. J. Ethnopharmacol. 2011, 135, 610–619. [Google Scholar] [CrossRef]
- Radulovic, N.S.; Miltojevic, A.B.; Randjelovic, P.J.; Stojanovic, N.M.; Boylan, F. Effects of methyl and isopropyl N-methylanthranilates from Choisya ternata Kunth (Rutaceae) on experimental anxiety and depression in mice. Phytother. Res. 2013, 27, 1334–1338. [Google Scholar] [CrossRef]
- Pinheiro, M.M.G.; Radulovic, N.S.; Miltojevic, A.B.; Boylan, F.; Dias Fernandes, P. Antinociceptive esters of N-methylanthranilic acid: Mechanism of action in heat-mediated pain. Eur. J. Pharmacol. 2014, 727, 106–114. [Google Scholar] [CrossRef]
- Pinheiro, M.M.G.; Miltojevic, A.B.; Radulovic, N.S.; Abdul-Wahab, I.R.; Boylan, F.; Fernandes, P.D. Anti-inflammatory activity of Choisya ternata Kunth essential oil, ternanthranin, and its two synthetic analogs (methyl and propyl N-methylanthranilates). PLoS ONE 2015, 10, e0121063. [Google Scholar] [CrossRef]
- Rejon-Orantes, J.C.; Suarez, D.P.P.; Rejon-Rodriguez, A.; Hernandez, S.H.; Lievano, O.E.G.; Rodriguez, D.L.; de la Mora, M.P. Aqueous root extracts from Mimosa albida Humb. & Bonpl. ex Willd display antinociceptive activity in mice. J. Ethnopharmacol. 2013, 149, 522–526. [Google Scholar]
- Rodriguez-Chavez, J.L.; Egas, V.; Linares, E.; Bye, R.; Hernandez, T.; Espinosa-Garcia, F.J.; Delgado, G. Mexican Arnica (Heterotheca inuloides Cass. Asteraceae: Astereae): Ethnomedical uses, chemical constituents and biological properties. J. Ethnopharmacol. 2017, 195, 39–63. [Google Scholar] [CrossRef]
- Gene, R.M.; Segura, L.; Adzet, T.; Marin, E.; Iglesias, J. Heterotheca inuloides: Anti-inflammatory and analgesic effect. J. Ethnopharmacol. 1998, 60, 157–162. [Google Scholar] [CrossRef]
- Segura, L.; Freixa, B.; Ringbom, T.; Vila, R.; Perera, P.; Adzet, T.; Bohlin, L.; Canigueral, S. Anti-inflammatory activity of dichloromethane extract of Heterotheca inuloides in vivo and in vitro. Planta Med. 2000, 66, 553–555. [Google Scholar] [CrossRef]
- Rocha-Gonzalez, H.I.; Blaisdell-Lopez, E.; Granados-Soto, V.; Navarrete, A. Antinociceptive effect of 7-hydroxy-3,4-dihydrocadalin isolated from Heterotheca inuloides: Role of peripheral 5-HT(1) serotonergic receptors. Eur. J. Pharmacol. 2010, 649, 154–160. [Google Scholar] [CrossRef]
- Rocha-Gonzalez, H.I.; Ramirez-Aguilar, M.; Granados-Soto, V.; Reyes-Garcia, J.G.; Torres-Lopez, J.E.; Huerta-Cruz, J.C.; Navarrete, A. Antineuropathic effect of 7-hydroxy-3,4-dihydrocadalin in streptozotocin- induced diabetic rodents. BMC Complement. Altern. Med. 2014, 14, 129. [Google Scholar] [CrossRef]
- Kubo, I.; Muroi, H.; Kubo, A.; Chaudhuri, S.K.; Sanchez, Y.; Ogura, T. Antimicrobial agents from Heterotheca inuloides. Planta Med. 1994, 60, 218–221. [Google Scholar] [CrossRef]
- Kubo, I.; Chaudhuri, S.K.; Kubo, Y.; Sanchez, Y.; Ogura, T.; Saito, T.; Ishikawa, H.; Haraguchi, H. Cytotoxic and antioxidative sesquiterpenoids from Heterotheca inuloides. Planta Med. 1996, 62, 427–430. [Google Scholar] [CrossRef]
- Rodriguez-Chavez, J.L.; Rufino-Gonzalez, Y.; Ponce-Macotela, M.; Delgado, G. In vitro activity of “Mexican Arnica” Heterotheca inuloides Cass natural products and some derivatives against Giardia intestinalis. Parasitology 2015, 142, 576–584. [Google Scholar] [CrossRef]
- Delgado, G.; del Socorro Olivares, M.; Chavez, M.I.; Ramirez-Apan, T.; Linares, E.; Bye, R.; Espinosa-Garcia, F.J. Antiinflammatory constituents from Heterotheca inuloides. J. Nat. Prod. 2001, 64, 861–864. [Google Scholar] [CrossRef]
- Mayagoitia, L.; Diaz, J.L.; Contreras, C.M. Psychopharmacologic analysis of an alleged oneirogenic plant: Calea zacatechichi. J. Ethnopharmacol. 1986, 18, 229–243. [Google Scholar] [CrossRef]
- Venegas-Flores, H.; Segura-Cobos, D.; Vazquez-Cruz, B. Antiinflammatory activity of the aqueous extract of Calea zacatechichi. Proc. West. Pharmacol. Soc. 2002, 45, 110–111. [Google Scholar]
- Roman Ramos, R.; Alarcon-Aguilar, F.; Lara-Lemus, A.; Flores-Saenz, J.L. Hypoglycemic effect of plants used in Mexico as antidiabetics. Arch. Med. Res. 1992, 23, 59–64. [Google Scholar]
- Wu, H.; Fronczek, F.R.; Burandt, C.L.J.; Zjawiony, J.K. Antileishmanial Germacranolides from Calea zacatechichi. Planta Med. 2011, 77, 749–753. [Google Scholar] [CrossRef]
- Salaga, M.; Kowalczuk, A.; Zielinska, M.; Blazewicz, A.; Fichna, J. Calea zacatechichi dichloromethane extract exhibits antidiarrheal and antinociceptive effects in mouse models mimicking irritable bowel syndrome. Naunyn Schmiedebergs Arch. Pharmacol. 2015, 388, 1069–1077. [Google Scholar] [CrossRef]
- Salaga, M.; Fichna, J.; Socala, K.; Nieoczym, D.; Pierog, M.; Zielinska, M.; Kowalczuk, A.; Wlaz, P. Neuropharmacological characterization of the oneirogenic Mexican plant Calea zacatechichi aqueous extract in mice. Metab. Brain Dis. 2016, 31, 631–641. [Google Scholar] [CrossRef]
- Velazquez-Gonzalez, C.; Carino-Cortes, R.; Gayosso de Lucio, J.A.; Ortiz, M.I.; De la OArciniega, M.; Altamirano-Baez, D.A.; Angeles, L.J.-; Bautista-Avila, M. Antinociceptive and anti-inflammatory activities of Geranium bellum and its isolated compounds. BMC Complement. Altern. Med. 2014, 14, 506. [Google Scholar] [CrossRef]
- Gayosso-De-Lucio, J.A.; Torres-Valencia, J.M.; Cerda-Garcia-Rojas, C.M.; Joseph-Nathan, P. Ellagitannins from Geranium potentillaefolium and G. bellum. Nat. Prod. Commun. 2010, 5, 531–534. [Google Scholar] [CrossRef] [PubMed]
- Gayosso-De-Lucio, J.; Torres-Valencia, M.; Rojo-Dominguez, A.; Najera-Pena, H.; Aguirre-Lopez, B.; Salas-Pacheco, J.; Avitia-Dominguez, C.; Tellez-Valencia, A. Selective inactivation of triosephosphate isomerase from Trypanosoma cruzi by brevifolin carboxylate derivatives isolated from Geranium bellum Rose. Bioorg. Med. Chem. Lett. 2009, 19, 5936–5939. [Google Scholar] [CrossRef] [PubMed]
- Langhammer, L. Piper auritum H. B. K.—An anatomical-histochemical study. Piperaceae used in folk medicine—A comparative anatomical-histochemical study. 1. Planta Med. 1970, 19, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Salehi, B.; Zakaria, Z.A.; Gyawali, R.; Ibrahim, S.A.; Rajkovic, J.; Shinwari, Z.K.; Khan, T.; Sharifi-Rad, J.; Ozleyen, A.; Turkdonmez, E.; et al. Piper Species: A Comprehensive Review on Their Phytochemistry, Biological Activities and Applications. Molecules 2019, 24, 1364. [Google Scholar] [CrossRef]
- Macias-Peacok, B.; Perez-Jackson, L.; Suarez-Crespo, M.F.; Fong-Dominguez, C.O.; Pupo-Perera, E. Use of medicinal plants during pregnancy. Rev. Med. Inst. Mex. Seguro Soc. 2009, 47, 331–334. [Google Scholar] [PubMed]
- Monzote, L.; Garcia, M.; Montalvo, A.M.; Scull, R.; Miranda, M. Chemistry, cytotoxicity and antileishmanial activity of the essential oil from Piper auritum. Mem. Inst. Oswaldo Cruz. 2010, 105, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, A.M.N.; Gutierrez, R.M.P.; Cotera, L.B.F. Antidiabetic activity of Piper auritum leaves in streptozotocin-induced diabetic rat, beneficial effect on advanced glycation endproduct. Chin. J. Integr. Med. 2014. [Google Scholar] [CrossRef]
- Gutierrez, R.M.P. Effect of the hexane extract of Piper auritum on insulin release from beta-cell and oxidative stress in streptozotocin-induced diabetic rat. Pharmacogn. Mag. 2012, 8, 308–313. [Google Scholar] [CrossRef]
- Meckes, M.; David-Rivera, A.D.; Nava-Aguilar, V.; Jimenez, A. Activity of some Mexican medicinal plant extracts on carrageenan-induced rat paw edema. Phytomedicine 2004, 11, 446–451. [Google Scholar] [CrossRef]
- Perez-Hernandez, J.; Gonzalez-Cortazar, M.; Marquina, S.; Herrera-Ruiz, M.; Meckes-Fischer, M.; Tortoriello, J.; Cruz-Sosa, F.; Nicasio-Torres, M.P. Sphaeralcic acid and tomentin, anti-inflammatory compounds produced in cell suspension cultures of Sphaeralcea angustifolia. Planta Med. 2014, 80, 209–214. [Google Scholar] [CrossRef]
- Romero-Cerecero, O.; Meckes-Fischer, M.; Zamilpa, A.; Enrique Jimenez-Ferrer, J.; Nicasio-Torres, P.; Perez-Garcia, D.; Tortoriello, J. Clinical trial for evaluating the effectiveness and tolerability of topical Sphaeralcea angustifolia treatment in hand osteoarthritis. J. Ethnopharmacol. 2013, 147, 467–473. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Winder, L.R.; Goni-Cedeno, S.; Olguin-Lara, P.A.; Diaz-Salgado, G.; Arriaga-Jordan, C.M. Huizache (Acacia farnesiana) whole pods (flesh and seeds) as an alternative feed for sheep in Mexico. Trop. Anim. Health Prod. 2009, 41, 1615–1621. [Google Scholar] [CrossRef] [PubMed]
- Hernandez-Garcia, E.; Garcia, A.; Avalos-Alanis, F.G.; Rivas-Galindo, V.M.; Delgadillo-Puga, C.; Camacho-Corona, M.D.R. Nuclear magnetic resonance spectroscopy data of isolated compounds from Acacia farnesiana (L) Willd fruits and two esterified derivatives. Data Br. 2019, 22, 255–268. [Google Scholar] [CrossRef]
- Lin, A.-S.; Lin, C.-R.; Du, Y.-C.; Lubken, T.; Chiang, M.Y.; Chen, I.-H.; Wu, C.-C.; Hwang, T.-L.; Chen, S.-L.; Yen, M.-H.; et al. Acasiane A and B and farnesirane A and B, diterpene derivatives from the roots of Acacia farnesiana. Planta Med. 2009, 75, 256–261. [Google Scholar] [CrossRef] [PubMed]
- Trivedi, C.P.; Modi, N.T.; Sarin, R.K.; Rao, S.S. Bronchodilator and anti-inflammatory effect of glycosidal fraction of Acacia farnesiana. Indian J. Physiol. Pharmacol. 1986, 30, 267–268. [Google Scholar]
- Claudia, D.P.; Mario, C.-H.; Arturo, N.O.; Omar Noel, M.-C.; Antonio, N.C.; Teresa, R.A.; Zenon Gerardo, L.-T.; Margarita, D.M.; Marsela Alejandra, A.-I.; Yessica Rosalina, C.M.; et al. Phenolic Compounds in Organic and Aqueous Extracts from Acacia farnesiana Pods Analyzed by ULPS-ESI-Q-oa/TOF-MS. In Vitro Antioxidant Activity and Anti-Inflammatory Response in CD-1 Mice. Molecules 2018, 23, 2386. [Google Scholar] [CrossRef]
- Berlin, E.A.; Berlin, B. Medical Ethnobiology of the Highland Maya of Chiapas, Mexico: The Gastrointestinal Diseases, 1st ed.; Princeton University Press: Princeton, NJ, USA, 1996; pp. 126–451. [Google Scholar]
- Alanís, A.D.; Calzada, F.; Cedillo-Rivera, R.; Meckes, M. Antiprotozoal activity of the constituents of Rubus coriifolius. Phytother. Res. 2003, 17, 681–682. [Google Scholar] [CrossRef]
- Soto, J.; Gomez, C.; Calzada, F.; Ramirez, M.E. Ultrastructural changes on Entamoeba histolytica HM1-IMSS caused by the flavan-3-ol, (-)-epicatechin. Planta Med. 2010, 76, 611–612. [Google Scholar] [CrossRef]
- Gonzalez-Hernandez, S.; Gonzalez-Ramirez, D.; Davila-Rodriguez, M.I.; Jimenez-Arellanez, A.; Meckes-Fischer, M.; Said-Fernandez, S.; Cortes-Gutierrez, E.I. Absence of toxicity and genotoxicity in an extract of Rubus coriifolius. Genet. Mol. Res. 2016, 15, 1–12. [Google Scholar] [CrossRef]
- Quinonez-Bastidas, G.N.; Pineda-Farias, J.B.; Flores-Murrieta, F.J.; Rodriguez-Silverio, J.; Reyes-Garcia, J.G.; Godinez-Chaparro, B.; Granados-Soto, V.; Rocha-Gonzalez, H.I. Antinociceptive effect of (-)-epicatechin in inflammatory and neuropathic pain in rats. Behav. Pharmacol. 2018, 29, 270–279. [Google Scholar] [CrossRef]
- Calva-Candelaria, N.; Melendez-Camargo, M.E.; Montellano-Rosales, H.; Estrada-Perez, A.R.; Rosales-Hernandez, M.C.; Fragoso-Vazquez, M.J.; Martinez-Archundia, M.; Correa-Basurto, J.; Marquez-Flores, Y.K. Oenothera rosea L Her. ex Ait attenuates acute colonic inflammation in TNBS-induced colitis model in rats: In vivo and in silico myeloperoxidase role. Biomed. Pharmacother. 2018, 108, 852–864. [Google Scholar] [CrossRef] [PubMed]
- Almora-Pinedo, Y.; Arroyo-Acevedo, J.; Herrera-Calderon, O.; Chumpitaz-Cerrate, V.; Hanari-Quispe, R.; Tinco-Jayo, A.; Franco-Quino, C.; Figueroa-Salvador, L. Preventive effect of Oenothera rosea on N-methyl-N-nitrosourea-(NMU) induced gastric cancer in rats. Clin. Exp. Gastroenterol. 2017, 10, 327–332. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Márquez-Flores, Y.K.; Meléndez-Camargo, M.E.; García-Mateos, N.J.; Huerta-Anaya, M.C.; Pablo-Pérez, S.S.; Silva-Torres, R. Phytochemical composition and pharmacological evaluation of different extracts of Oenothera rosea L’Hér. ex Ait (Onagraceae) aerial part. South Afr. J. Bot. 2018, 116, 245–250. [Google Scholar] [CrossRef]
- Jimenez, A.; Meckes, M.; Alvarez, V.; Torres, J.; Parra, R. Secondary metabolites from Chamaedora tepejilote (Palmae) are active against Mycobacterium tuberculosis. Phytother. Res. 2005, 19, 320–322. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Arellanes, A.; Meckes, M.; Ramirez, R.; Torres, J.; Luna-Herrera, J. Activity against multidrug-resistant Mycobacterium tuberculosis in Mexican plants used to treat respiratory diseases. Phytother. Res. 2003, 17, 903–908. [Google Scholar] [CrossRef]
- Jimenez-Arellanes, A.; Luna-Herrera, J.; Cornejo-Garrido, J.; Lopez-Garcia, S.; Castro-Mussot, M.E.; Meckes-Fischer, M.; Mata-Espinosa, D.; Marquina, B.; Torres, J.; Hernandez-Pando, R. Ursolic and oleanolic acids as antimicrobial and immunomodulatory compounds for tuberculosis treatment. BMC Complement. Altern. Med. 2013, 13, 258. [Google Scholar] [CrossRef]
- Perez Gutierrez, R.M.; Vargas Solis, R.; Garcia Baez, E.; Gallardo Navarro, Y. Hypoglycemic activity of constituents from Astianthus viminalis in normal and streptozotocin-induced diabetic mice. J. Nat. Med. 2009, 63, 393–401. [Google Scholar] [CrossRef]
- Perez, R.M.; Cervantes, H.; Zavala, M.A.; Sanchez, J.; Perez, S.; Perez, C. Isolation and hypoglycemic activity of 5, 7,3′-trihydroxy-3,6,4′-trimethoxyflavone from Brickellia veronicaefolia. Phytomedicine 2000, 7, 25–29. [Google Scholar] [CrossRef]
- Perez-Gutierrez, R.M.; Perez-Gonzalez, C.; Zavala-Sanchez, M.A.; Perez-Gutierrez, S. Hypoglycemic activity of Bouvardia terniflora, Brickellia veronicaefolia, and Parmentiera edulis. Salud Publica Mex. 1998, 40, 354–358. [Google Scholar] [CrossRef]
- Perez, G.R.M.; Vargas, S.R.; Martinez, M.F.J.; Cordova, R.I. Antioxidant and free radical scavenging activities of 5,7,3′-trihydroxy-3,6,4′-trimethoxyflavone from Brickellia veronicaefolia. Phytother. Res. 2004, 18, 428–430. [Google Scholar] [CrossRef] [PubMed]
- Rivero-Cruz, B.; Rivero-Cruz, I.; Rodriguez, J.M.; Cerda-Garcia-Rojas, C.M.; Mata, R. Qualitative and quantitative analysis of the active components of the essential oil from Brickellia veronicaefolia by nuclear magnetic resonance spectroscopy. J. Nat. Prod. 2006, 69, 1172–1176. [Google Scholar] [CrossRef] [PubMed]
- Rivero-Cruz, B.; Rojas, M.A.; Rodriguez-Sotres, R.; Cerda-Garcia-Rojas, C.M.; Mata, R. Smooth muscle relaxant action of benzyl benzoates and salicylic acid derivatives from Brickellia veronicaefolia on isolated guinea-pig ileum. Planta Med. 2005, 71, 320–325. [Google Scholar] [CrossRef] [PubMed]
- Meckes, M.; Calzada, F.; Paz, D.; Rodriguez, J.; Ponce-Monter, H. Inhibitory effect of xanthomicrol and 3 alpha-angeloyloxy-2 alpha- hydroxy-13,14Z-dehydrocativic acid from Brickellia paniculata on the contractility of guinea-pig ileum. Planta Med. 2002, 68, 467–469. [Google Scholar] [CrossRef] [PubMed]
- Meckes, M.; Roman-Ramos, R.; Perez, S.; Calzada, F.; Ponce-Monter, H. Effects of a labdane diterpene isolated from Brickellia paniculata on intracellular Ca2+ deposit of guinea-pig ileal longitudinal muscle. Planta Med. 2002, 68, 601–604. [Google Scholar] [CrossRef] [PubMed]
- Ponce-Monter, H.; Perez, S.; Zavala, M.A.; Perez, C.; Meckes, M.; Macias, A.; Campos, M. Relaxant effect of xanthomicrol and 3alpha-angeloyloxy-2alpha- hydroxy-13,14z-dehydrocativic acid from Brickellia paniculata on rat uterus. Biol. Pharm. Bull. 2006, 29, 1501–1503. [Google Scholar] [CrossRef][Green Version]
- Baqueiro-Pena, I.; Guerrero-Beltran, J.A. Physicochemical and antioxidant characterization of Justicia spicigera. Food Chem. 2017, 218, 305–312. [Google Scholar] [CrossRef]
- Gonzalez-Trujano, M.E.; Dominguez, F.; Perez-Ortega, G.; Aguillon, M.; Martinez-Vargas, D.; Almazan-Alvarado, S.; Martinez, A. Justicia spicigera Schltdl. and kaempferitrin as potential anticonvulsant natural products. Biomed. Pharmacother. 2017, 92, 240–248. [Google Scholar] [CrossRef]
- Cassani, J.; Dorantes-Barron, A.M.; Novales, L.M.; Real, G.A.; Estrada-Reyes, R. Anti-depressant-like effect of kaempferitrin isolated from Justicia spicigera Schltdl (Acanthaceae) in two behavior models in mice: Evidence for the involvement of the serotonergic system. Molecules 2014, 19, 21442–21461. [Google Scholar] [CrossRef]
- Garcia-Rios, R.I.; Mora-Perez, A.; Gonzalez-Torres, D.; Carpio-Reyes, R.J.; Soria-Fregozo, C. Anxiolytic-like effect of the aqueous extract of Justicia spicigera leaves on female rats: A comparison to diazepam. Phytomedicine 2019, 55, 9–13. [Google Scholar] [CrossRef]
- Ortiz-Andrade, R.; Cabanas-Wuan, A.; Arana-Argaez, V.E.; Alonso-Castro, A.J.; Zapata-Bustos, R.; Salazar-Olivo, L.A.; Dominguez, F.; Chavez, M.; Carranza-Alvarez, C.; Garcia-Carranca, A. Antidiabetic effects of Justicia spicigera Schltdl (Acanthaceae). J. Ethnopharmacol. 2012, 143, 455–462. [Google Scholar] [CrossRef]
- Alonso-Castro, J.A.; Maldonado-Miranda, J.A.J.; Zarate-Martinez, A.; Jacobo-Salcedo, M.D.R.; Fernandez-Galicia, C.; Alejandro Figueroa-Zuniga, L.; Abel Rios-Reyes, N.; Angel de Leon-Rubio, M.; Medellin-Castillo, N.A.; Reyes-Munguia, A.; et al. Medicinal plants used in the Huasteca Potosina, Mexico. J. Ethnopharmacol. 2012, 143, 292–298. [Google Scholar] [CrossRef]
- Ponce-Macotela, M.; Rufino-Gonzalez, Y.; de la Mora-de la Mora, J.I.; Gonzalez-Maciel, A.; Reynoso-Robles, R.; Martinez-Gordillo, M.N. Mortality and morphological changes in Giardia duodenalis induced by exposure to ethanolic extracts of Justicia spicigera. Proc. West. Pharmacol. Soc. 2001, 44, 151–152. [Google Scholar] [PubMed]
- Zapata-Morales, J.R.; Alonso-Castro, A.J.; Dominguez, F.; Carranza-Alvarez, C.; Castellanos, L.M.O.; Martinez-Medina, R.M.; Perez-Urizar, J. Antinociceptive Activity of an Ethanol Extract of Justicia spicigera. Drug Dev. Res. 2016, 77, 180–186. [Google Scholar] [CrossRef] [PubMed]
- De Melo, G.O.; Malvar, D.C.; Vanderlinde, F.A.; Rocha, F.F.; Pires, P.A.; Costa, E.A.; de Matos, L.G.; Kaiser, C.R.; Costa, S.S. Antinociceptive and anti-inflammatory kaempferol glycosides from Sedum dendroideum. J. Ethnopharmacol. 2009, 124, 228–232. [Google Scholar] [CrossRef]
- Angeles-Lopez, G.E.; Gonzalez-Trujano, M.E.; Rodriguez, R.; Deciga-Campos, M.; Brindis, F.; Ventura-Martinez, R. Gastrointestinal activity of Justicia spicigera Schltdl. in experimental models. Nat. Prod. Res. 2019, 1–5. [Google Scholar] [CrossRef]
- Martinez Alfaro, M.A. Medicinal plants used in a Totonac community of the Sierra Norte de Puebla: Tuzamapan de Galeana, Puebla, Mexico. J. Ethnopharmacol. 1984, 11, 203–221. [Google Scholar] [CrossRef]
- Jimenez-Arellanes, A.; Meckes, M.; Torres, J.; Luna-Herrera, J. Antimycobacterial triterpenoids from Lantana hispida (Verbenaceae). J. Ethnopharmacol. 2007, 111, 202–205. [Google Scholar] [CrossRef]
- Silva, G.N.; Martins, F.R.; Matheus, M.E.; Leitao, S.G.; Fernandes, P.D. Investigation of anti-inflammatory and antinociceptive activities of Lantana trifolia. J. Ethnopharmacol. 2005, 100, 254–259. [Google Scholar] [CrossRef]
- Uzcategui, B.; Avila, D.; Suarez-Roca, H.; Quintero, L.; Ortega, J.; Gonzalez, B. Anti-inflammatory, antinociceptive, and antipyretic effects of Lantana trifolia Linnaeus in experimental animals. Investig. Clin. 2004, 45, 317–322. [Google Scholar]
- Arciniegas, A.; Gonzalez, K.; Perez-Castorena, A.-L.; Nieto-Camacho, A.; Villasenor, J.-L.; Romo de Vivar, A. Sesquiterpenoids from Pittocaulon filare. J. Nat. Prod. 2014, 77, 1304–1310. [Google Scholar] [CrossRef] [PubMed]
- Rosell, J.A.; Olson, M.E. Testing implicit assumptions regarding the age vs. size dependence of stem biomechanics using Pittocaulon (Senecio) praecox (Asteraceae). Am. J. Bot. 2007, 94, 161–172. [Google Scholar] [CrossRef]
- Ortiz palacios, L.; Cervantes Gutiérrez, V.; Chimal Hernandez, A. Plantas Medicinales de San Francisco Tlatenco, 1st ed.; UAM-Xochimilco: Ciudad de Mexico, Mexico, 2017; p. 98. [Google Scholar]
- Marin-Loaiza, J.C.; Nieto-Camacho, A.; Cespedes, C.L. Antioxidant and anti-inflammatory activities of Pittocaulon species from Mexico. Pharm. Biol. 2013, 51, 260–266. [Google Scholar] [CrossRef]
- Marin Loaiza, J.C.; Ernst, L.; Beuerle, T.; Theuring, C.; Cespedes, C.L.; Hartmann, T. Pyrrolizidine alkaloids of the endemic Mexican genus Pittocaulon and assignment of stereoisomeric 1,2-saturated necine bases. Phytochemistry 2008, 69, 154–167. [Google Scholar] [CrossRef] [PubMed]
- Robles-Zepeda, R.E.; Velazquez-Contreras, C.A.; Garibay-Escobar, A.; Galvez-Ruiz, J.C.; Ruiz-Bustos, E. Antimicrobial activity of Northwestern Mexican plants against Helicobacter pylori. J. Med. Food 2011, 14, 1280–1283. [Google Scholar] [CrossRef]
- Rodriguez-Canales, M.; Jimenez-Rivas, R.; Canales-Martinez, M.M.; Garcia-Lopez, A.J.; Rivera-Yanez, N.; Nieto-Yanez, O.; Ledesma-Soto, Y.; Sanchez-Torres, L.E.; Rodriguez-Sosa, M.; Terrazas, L.I.; et al. Protective Effect of Amphipterygium adstringens Extract on Dextran Sulphate Sodium-Induced Ulcerative Colitis in Mice. Mediat. Inflamm. 2016, 2016, 8543561. [Google Scholar] [CrossRef]
- Navarrete, A.; Oliva, I.; Sanchez-Mendoza, M.E.; Arrieta, J.; Cruz-Antonio, L.; Castaneda-Hernandez, G. Gastroprotection and effect of the simultaneous administration of Cuachalalate (Amphipterygium adstringens) on the pharmacokinetics and anti-inflammatory activity of diclofenac in rats. J. Pharm. Pharmacol. 2005, 57, 1629–1636. [Google Scholar] [CrossRef]
- Oviedo-Chavez, I.; Ramirez-Apan, T.; Soto-Hernandez, M.; Martinez-Vazquez, M. Principles of the bark of Amphipterygium adstringens (Julianaceae) with anti-inflammatory activity. Phytomedicine 2004, 11, 436–445. [Google Scholar] [CrossRef]
- Arrieta, J.; Benitez, J.; Flores, E.; Castillo, C.; Navarrete, A. Purification of gastroprotective triterpenoids from the stem bark of Amphipterygium adstringens; role of prostaglandins, sulfhydryls, nitric oxide and capsaicin-sensitive neurons. Planta Med. 2003, 69, 905–909. [Google Scholar]
- Zheng, X.; Wang, W.; Piao, H.; Xu, W.; Shi, H.; Zhao, C. The genus Gnaphalium, L. (Compositae): Phytochemical and pharmacological characteristics. Molecules 2013, 18, 8298–8318. [Google Scholar] [CrossRef]
- Rojas, G.; Levaro, J.; Tortoriello, J.; Navarro, V. Antimicrobial evaluation of certain plants used in Mexican traditional medicine for the treatment of respiratory diseases. J. Ethnopharmacol. 2001, 74, 97–101. [Google Scholar] [CrossRef]
- Villagomez-Ibarra, J.R.; Sanchez, M.; Espejo, O.; Zuniga-Estrada, A.; Torres-Valencia, J.M.; Joseph-Nathan, P. Antimicrobial activity of three Mexican Gnaphalium species. Fitoterapia 2001, 72, 692–694. [Google Scholar] [CrossRef]
- Huang, D.; Chen, Y.; Chen, W.; Liu, Y.; Yao, F.; Xue, D.; Sun, L. Anti-inflammatory effects of the extract of Gnaphalium affine D. Don in vivo and in vitro. J. Ethnopharmacol. 2015, 176, 356–364. [Google Scholar] [CrossRef]
- Ovalle-Magallanes, B.; Medina-Campos, O.N.; Pedraza-Chaverri, J.; Mata, R. Hypoglycemic and antihyperglycemic effects of phytopreparations and limonoids from Swietenia humilis. Phytochemistry 2015, 110, 111–119. [Google Scholar] [CrossRef] [PubMed]
- Ovalle-Magallanes, B.; Navarrete, A.; Haddad, P.S.; Tovar, A.R.; Noriega, L.G.; Tovar-Palacio, C.; Mata, R. Multi-target antidiabetic mechanisms of mexicanolides from Swietenia humilis. Phytomedicine 2019, 58, 152891. [Google Scholar] [CrossRef]
- Jimenez, A.; Villarreal, C.; Toscano, R.A.; Cook, M.; Arnason, J.T.; Bye, R.; Mata, R. Limonoids from Swietenia humilis and Guarea grandiflora (Meliaceae)Taken in part from the PhD and MS theses of C. Villarreal and M. A. Jiménez, respectively. Phytochemistry 1998, 49, 1981–1988. [Google Scholar] [CrossRef]
- Ovalle-Magallanes, B.; Deciga-Campos, M.; Mata, R. Antihyperalgesic activity of a mexicanolide isolated from Swietenia humilis extract in nicotinamide-streptozotocin hyperglycemic mice. Biomed. Pharmacother. 2017, 92, 324–330. [Google Scholar] [CrossRef] [PubMed]
- Rzedowski, J.; Rzedowski, G.C. Flora Fanerogámica del Valle de México, 1st ed.; Insittuto de Ecología: Mexico City, Mexico, 1985; p. 454. [Google Scholar]
- Romero-Cerecero, O.; Zamilpa, A.; Diaz-Garcia, E.R.; Tortoriello, J. Pharmacological effect of Ageratina pichinchensis on wound healing in diabetic rats and genotoxicity evaluation. J. Ethnopharmacol. 2014, 156, 222–227. [Google Scholar] [CrossRef]
- Sanchez-Mendoza, M.E.; Rodriguez-Silverio, J.; Rivero-Cruz, J.F.; Rocha-Gonzalez, H.I.; Pineda-Farias, J.B.; Arrieta, J. Antinociceptive effect and gastroprotective mechanisms of 3,5-diprenyl-4-hydroxyacetophenone from Ageratina pichinchensis. Fitoterapia 2013, 87, 11–19. [Google Scholar] [CrossRef]
- Romero-Cerecero, O.; Zamilpa, A.; Tortoriello, J. Pilot study that evaluated the clinical effectiveness and safety of a phytopharmaceutical elaborated with an extract of Ageratina pichinchensis in patients with minor recurrent aphthous stomatitis. J. Ethnopharmacol. 2015, 173, 225–230. [Google Scholar] [CrossRef] [PubMed]
- Romero-Cerecero, O.; Islas-Garduno, A.L.; Zamilpa, A.; Tortoriello, J. Effectiveness of Ageratina pichinchensis Extract in Patients with Vulvovaginal Candidiasis. A Randomized, Double-Blind, and Controlled Pilot Study. Phytother. Res. 2017, 31, 885–890. [Google Scholar] [CrossRef] [PubMed]
- Romero-Cerecero, O.; Zamilpa, A.; Tortoriello, J. Effectiveness and tolerability of a standardized extract from Ageratina pichinchensis in patients with diabetic foot ulcer: A randomized, controlled pilot study. Planta Med. 2015, 81, 272–278. [Google Scholar] [CrossRef]
- Romero-Cerecero, O.; Zamilpa, A.; Jimenez-Ferrer, E.; Tortoriello, J. Therapeutic effectiveness of Ageratina pichinchensis on the treatment of chronic interdigital tinea pedis: A randomized, double-blind clinical trial. J. Altern. Complement. Med. 2012, 18, 607–611. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Caamal, A.; Ferrufino-Acosta, L.F.; Diaz-Maradiaga, R.F.; Rodriguez-Delcid, D.; Mussali-Galante, P.; Tovar-Sanchez, E. Species distribution modelling and cpSSR reveal population history of the Neotropical annual herb Tithonia rotundifolia (Asteraceae). Plant. Biol. 2019, 21, 248–258. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Martínez, K.; García-Valencia, S.; Soto-Simental, S.; Zepeda-Bastida, A.; Ayala-Martínez, M.; Pérez-Martínez, K.; García-Valencia, S.; Soto-Simental, S.; Zepeda-Bastida, A.; Ayala-Martínez, M. Productive parameters rabbits fed with different parts of the Tithonia tubaeformis plant. Abanico Vet. 2018, 8, 108–114. [Google Scholar]
- Dávalos, J.; Gutiérrez-Lomelí, M.; Siller, F.; Rodriguez-Sahagun, A.; Del Rio, J.A.; Guerrero, P.; Del Toro, L. Screening fitoquímico y capacidad antiinflamatoria de hojas de Tithonia tubaeformis. Biotecnia 2013, 15, 53. [Google Scholar] [CrossRef]
- Nawaz, N.U.A.; Saeed, M.; Rauf, K.; Usman, M.; Arif, M.; Ullah, Z.; Raziq, N. Antinociceptive effectiveness of Tithonia tubaeformis in a vincristine model of chemotherapy-induced painful neuropathy in mice. Biomed. Pharmacother. 2018, 103, 1043–1051. [Google Scholar] [CrossRef] [PubMed]
- Yezierski, R.P.; Hansson, P. Inflammatory and Neuropathic Pain From Bench to Bedside: What Went Wrong? J. Pain 2018, 19, 571–588. [Google Scholar] [CrossRef]
- Clark, J.D. Preclinical Pain Research: Can We Do Better? Anesthesiology 2016, 125, 846–849. [Google Scholar] [CrossRef]
- Friedl, K.E. Analysis: Overcoming the “valley of death”: Mouse models to accelerate translational research. Diabetes Technol. Ther. 2006, 8, 413–414. [Google Scholar] [CrossRef] [PubMed]
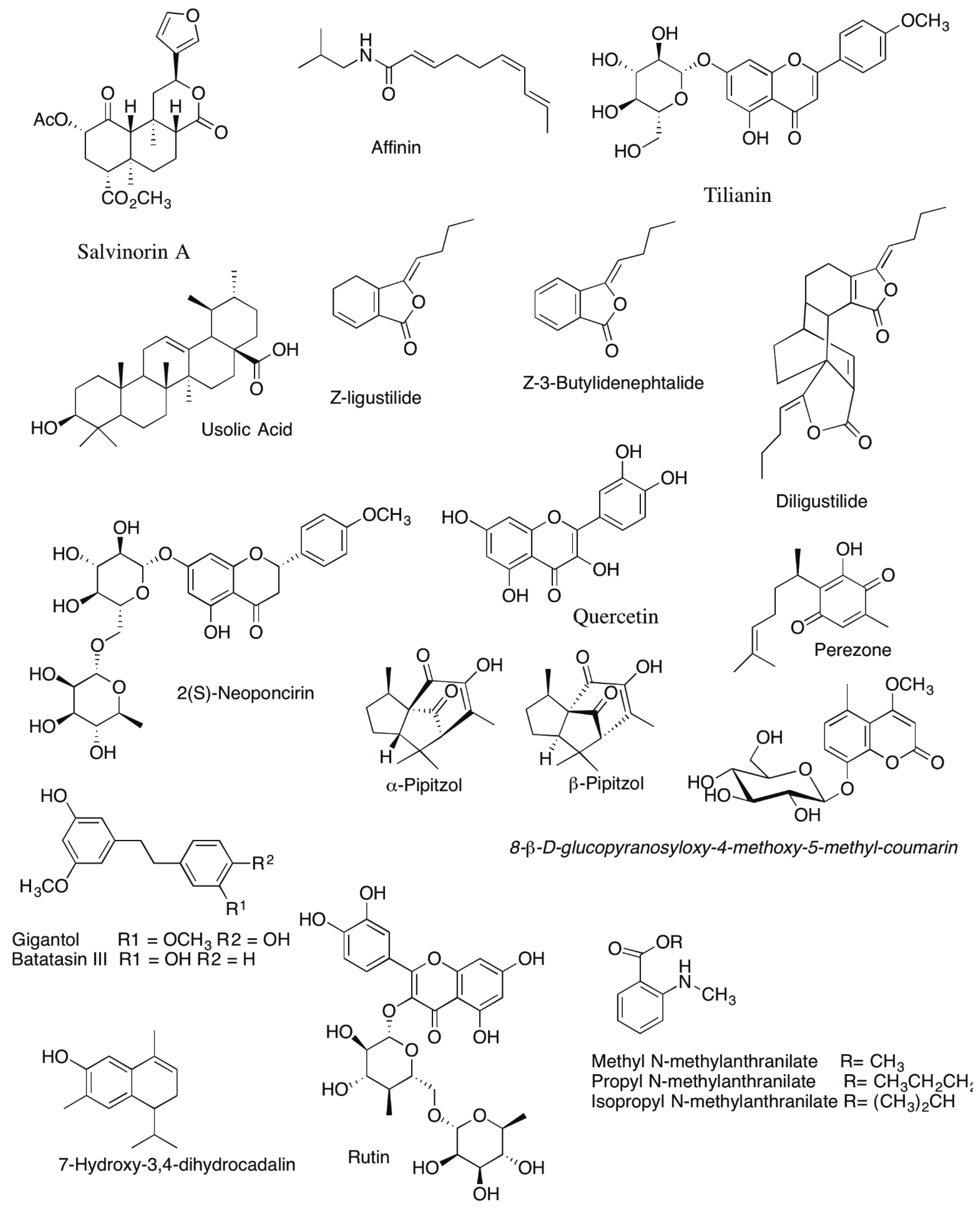
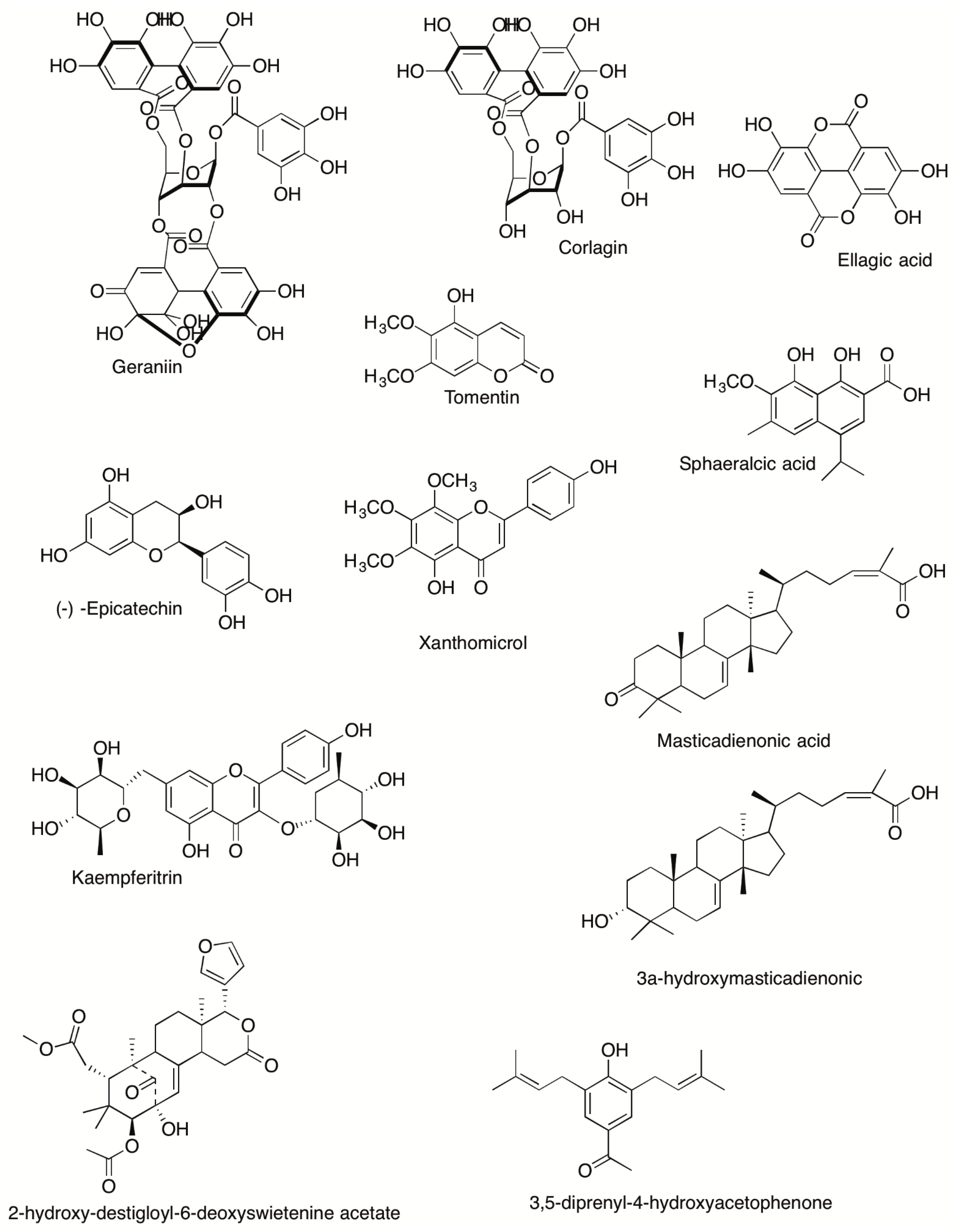
| Plant | Type of Extract | Experimental Model | Species | Possible Mechanism of Action | Reference |
|---|---|---|---|---|---|
| Salvia divinorum | Salvinorin A (11.6, 13.9, 18.5, 20.8 and 23.1 nmol, i.t.) | Tail flick test | Mice | Activation of kappa-opioid receptors | [32] |
| Salvia divinorum | Salvinorin A (0.5, 1.0, 2.0 and 4.0 mg/kg, i.p.) | Tail flick test Hot plate test Acetic acid-induced writhing | Male Swiss mice | Activation of kappa-opioid receptors | [33] |
| Salvia divinorum | Acetonic extract (30, 100 and 200 mg/kg, i.p.) | Sciatic loose nerve ligature-induced mechanical and thermal hyperalgesia Carrageenan-induced edema | Male Wistar rats | Activation of kappa-opioid receptors | [34] |
| Salvia divinorum | Ethyl acetate extract (31.6, 100 and 316 mg/kg, i.p.) and Mixure salvinorins (30 mg/kg, i.p) | Acetic acid-induced writhing Formalin test | Male and female Swiss albino mice | Opioids and 5-HT1A | [35] |
| Heliopsis longipes | Ethanolic extract (10, 30, 100 and 300 mg/kg. i.p.) | Thermal hyperalgesia | Balb/c mice | Not studied | [39] |
| Heliopsis longipes | Ethanolic extract (10, 30, 100 and 300 mg/kg, p.o.) | Carrageenan-induced hyperalgesia (hot box test) | Male Balb/c mice | Synergistic actions with diclofenac | [40] |
| Heliopsis longipes | Ethanolic extract (3, 10, 30 and 100 mg/kg, p.o.) | Acetic acid-induced writhing Hot plate | Male CD1+ mice | Not studied | [41] |
| Heliopsis longipes | Affinin (1, 3, 10, 100, 300 and 600 µg/region), Longipinamide A andLlongipenamide B compounds (0.1, 1, 10, 30 and 100 µg/region) | Formalin-induced orofacial pain | Female Swiss Webster mice | TRPV1 | [44] |
| Heliopsis longipes | Ethanolic extract (10 mg/kg, i.p.) Afinin (1 mg/kg, i.p.) | Acetic acid-induced writhing Hot plate test | Male albino mice | Not studied | [45] |
| Heliopsis longipes | Acetonic extract (1, 10, 17.78, 31.6, 56.23 mg/kg, i.p.) Affinin (10, 17.78, 31.62, 56.23, 74.98 mg/kg, i.p.) | Capsaicin-induced hyperalgesia Acetic acid-induced writhing | Male ICR mice | Activation of nitric oxide, K+ channels, opioid, GABAergic and serotonergic system | [43] |
| Artemisia ludoviciana | Essential oil (1, 10, 31.6, 100 and 316 mg/kg, i.p.) | Hot plate test Formalin-induced hyperalgesia | Male ICR mice | Activation of Opioid system | [55] |
| Caulerpa mexicana | Sulphated polysaccharides (5, 10 and 20 mg/kg i.v.) (5, 10 and 20 mg/kg, s.c.) * | Acetic acid-induced writhing (no effect) Formalin-induced hyperalgesia (no effect) Carrageenan, dextran, histamine and serotonin -induced paw edema* | Male and female Swiss mice Male Wistar rats | Histamine is the main target of paw edema inflammation | [56] |
| Caulerpa mexicana | Methanolic extract Ethyl acetate extract Hexanic Chloroform extract (100 mg/kg, p.o.) | Formalin-induced hyperalgesia Acetic acid-induced writhing Hot plate test Carrageenan-induced peritonitis | Female Swiss mice | Not studied | [58] |
| Agastache mexicana | Hexane extract Ethyl acetate extract methanolic extract (100 mg/kg, i.p.) Ursolic acid compound (1, 3, 10, 30 and 100 mg/kg, i.p) | Acid acetic-induced writhing Formalin-induced hyperalgesia Intracolonic stimulation with capsaicin | Male and female Swiss albino mice and Wistar rats | Possible participation of cGMP and 5-HT1A receptors. | [68] |
| Agastache mexicana | Ursolic compound (1–100 mg/kg) Acacetin compound (1–100 mg/kg, i.p.) (1–300 mg/kg p.o.) | Acetic acid-induced writhing | Male and female Swiss albino mice | Not studied | [69] |
| Agastache mexicana | Hexane extract Ethyl acetate extract Methanolic extract (10, 30, 100, 300 and/or 562.3 mg/kg or 1000 mg/kg, i.p) | Acetic acid-induced writhing Formalin-induced hyperalgesia Hot box test PIFIR model | Female Swiss albino mice | Not studied | [30] |
| Ligusticum porteri | Organic extract Aqueous extract Essential oil (31.6, 100 and 316 mg/kg, p.o.) Z-ligustilide compound Z-3-butylidenephthalide compound Diligustilide compound (10, 31.6, 56.2 mg/kg, p.o.) | Acetic acid- induced writhing Hot plate test | Male ICR mice | Not studied | [78] |
| Ligusticum porteri | Methanolic-chloroform extract (150, 275 and 300 mg/kg, i.p.) | Writhing test | Male ICR mice | Not studied | [79] |
| Clinopodium mexicanum | Aqueous extract (1, 5, 10 and 100 mg/kg, i.p.) | Hot plate test | Male Swiss Webster mice | Not studied | [83] |
| Clinopodium mexicanum | 2 (S)-neopincirin (1, 10, 20 and 40 mg/kg, i.p.) | Hot plate test | Male Swiss Webster mice | GABAergic system was involved in the anxiolytic effect exerted by 2(S)-neopincirin | [84] |
| Tilia americana var mexicana | Aqueous extract Quercentin (30 and 100 mg/kg, i.p.) | Formalin-induced hyperalgesia PIFIR model | Male Wistar rats | Activation of 5-HT1A receptors | [92] |
| Acourtia thurberi | Decoction (31.6, 100, 316.2 µg/paw and 31.6, 100 and 316.2 mg/kg, p.o.) Perezone (3.2, 10 and 31.6 µg/paw, s.c.) Mixure of α-pipitzol, β-pipitzul (3.2, 10 and 31.6 µg/paw, s.c.) 8-β-D-glucopyranosyloxy-4-methoxy-5-methyl-coumarin (3.2, 10 and 31.6 µg/paw, s.c.) | Formalin-induced hyperalgesia in normal and diabetic mice | Male ICR mice | Not studied | [95] |
| Cyrtopodium macrobulbon | Organic extract Aqueous extract (31.6, 100 and 316 mg/kg, p.o.) | Hot plate test Writhing test | Male ICR mice | Not studied | [96] |
| Ternstroemia sylvatica | Chloroform and Ethanolic extract (250 and 500 mg/kg i.p.) | Croton oil- and TAP-induced ear edema Carrageenan-induced paw edema Acid acetic-induced writhing test Formalin-induced hyperalgesia | Male ICR mice | Not studied | [99] |
| Conyza filaginoides | Organic extract (31, 100 and 316 mg/kg, p.o.) (1, 10, 30, 56, 100 µg/paw, s.c.) | Acetic acid-induced writhing Hot plate test Formalin-induced hyperalgesia in normal and diabetic mice | Male ICR mice | GABAergic and opioid pathways | [103] |
| Choisya ternata | Essential oil Ethanolic extract (10, 30 and 100 mg/kg, p.o.) Methyl N- methylanthranilate compound Isopropyl N-methylanthranilatePropyl N-methylanthranilate compound (0.3, 1 and 3 mg/kg, p.o.) | Acetic acid-induced writhing test Hot plate test | Male Swiss mice | Not studied | [107] |
| Choisya ternata | Isopropyl (ISOAN) compound Methyl (MAN) compound Propyl N-methylanthranilate (PAN) compound (0.3, 1 and 3 mg/kg, p.o.) | Formalin-induced hyperalgesia Capsaicin and Glutamate-induced nociception test Tail flick test Hot plate test | Male and female Swiss mice | K+ATP channels (ISOAN) Adrenergic, nitrergic and serotoninergic pathways (ISOAN and MAN) | [109] |
| Choisya ternata | Essential oil ternanthranin (3, 10 and 30 mg/kg, p.o.) | Formalin-induced hyperalgesia Carrageenan-induced paw edema | Male Webster mice | Reduction of nitric oxide, TNF-α and IL-1β | [110] |
| Mimosa albida | Aqueous extract (2.5, 25 and 50 mg/kg, i.p.) | Hot plate test Acetic acid-induced writhing | Male ICR mice | Not involved opioid receptors | [111] |
| Heterotheca inuloides | HI-2 fraction (butanol fraction) from the aqueous extract | Acetic acid-induced writhing test Carrageenan-induced paw edema Dextran-induced paw edema | Female Wistar rats and male Swiss CD-1 mice | Not studied | [113] |
| Heterothecainuloides | 7-hydroxy-3,4-dihydrocadalin compound (10, 100 and 1000 µg/paw, s.c.) | Formalin-induced hyperalgesia Mechanical hyperalgesia (Randall–Selitto) Carrageenan-induced paw edema | Female Wistar rats | Activation the 5-HT1A, 5-HT1B, 5-HT1D, but not opioid receptors | [115] |
| Heterothecainuloides | 7-hydroxy-3,4-dihydrocadalin (0.03, 0.3, 3 and 30 mg/kg, p.o.) | Formalin induced hyperalgesia in diabetic neuropathy * | Female Wistar rats | Activation of serotonin, but not opioid receptors. Antioxidant effect (malondialdehyde) | [116] |
| Calea zacatechichi | Dichloromethane extract (200 mg/kg, p.o.) | Intracolonic instillation of mustard oil test Acetic acid-induced writhing | Male C57BL/6N mice | Not studied | [125] |
| Calea zacatechichi | Aqueous extract (200 mg/kg, p.o.) | Hot plate test Acetic acid-induced writhing | Male albino Swiss mice | Not studied | [126] |
| Geranium bellum | Acetone-aqueous extract (200, 400 and 800 µg/paw, s.c.) (75, 150 and 300 mg/kg, p.o.) Geraniin Corilagin Quercetin Ellagic acid (5–25 mg/kg, p.o.) Geraniin Quercentin Ellagic acid and Corilagin derivates from AC-AE Geranium bellum | Formalin-induced hyperalgesia Acetic acid-induced Hot plate test | Male Wistar rats Female CD1 albino mice | Not studied | [127] |
| Sphaeralceaangustifolia | Chloroform extract (400 mg/kg, i.p.) | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Acacia farnesiana | Ethanol extract (400 mg/kg, i.p.) | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Rubuscoriifolius | Chloroform:methanolic extract (1:1) (400 mg/kg, i.p.) | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Oenotherarosea | Methanolic extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Oenothera rosea | Ethanolic and Ethyl acetate extract (50, 100 and 200 mg/kg, p.o.) | Acetic acid-induced writhing Hot plate test | Female NIH Swiss mice | Not studied | [151] |
| Chamaedora tepejilote | Aqueous extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Astianthus viminalis | Methanolic extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Brickellia veronicaefolia | Methanolic-chloroform extract (150, 300 and 600 mg/kg, p.o.) | Writhing test | Male ICR mice | Not studied | [79] |
| Brickelliapaniculata | Methanolic extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Justiciaspicigera, | Methanolic extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Justicia spicigera | Ethanolic extract (50, 100 and 200 mg/kg, p.o.) | Formalin-induced hyperalgesia test Hot plate test Tail flick test Acetic acid-induced writhing t | Male Balb/C mice | Not studied | [171] |
| Lantanahispida | Methanolic extract | Carrageenan-induced paw edema | Male Sprague-Dawley rats | Not studied | [136] |
| Pittocaulon bombycophole P. velatum P. praecox P. hintonii | Dichloromethane extract (100 mg/kg, i.p.) | Carrageenan-induced paw edema (no effect) | Male Wistar rats | Not studied | [181] |
| Swietenia humilis | Aqueous extract (10, 31.6, 56.2, 100 and 177 μ/paw, s.c.) Mexicanolide compound (0.5, 1, 2, 3 and 3.5 μg/paw, s.c.) | Formalin-induced hyperalgesia in diabetic mice | Male ICR mice | GABAA, 5-HT2A/C and opiod receptors, as well as the nitrergic system. | [195] |
| Ageratina pichinchensis | 3,5-diprenyl-4-hydroxyacetophenone compound (10, 32, 56 and 100 mg/kg, p.o.) (100, 128, 320 and 562 mg/kg, p.o.) | Carrageenan-induced thermal hyperalgesia Allodynia induced by spinal nerve ligation (L5/L6) | Male Wistar rats | Not studied | [198] |
| Tithonia tubaeformis | Hydromethanolic extract (100 and 200 mg/kg, p.o.) | Tail immersion test Acid acetic-induced writhing Vincristine-induced neuropathy | Balb/c mice | Not studied | [206] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Quiñonez-Bastidas, G.N.; Navarrete, A. Mexican Plants and Derivates Compounds as Alternative for Inflammatory and Neuropathic Pain Treatment—A Review. Plants 2021, 10, 865. https://doi.org/10.3390/plants10050865
Quiñonez-Bastidas GN, Navarrete A. Mexican Plants and Derivates Compounds as Alternative for Inflammatory and Neuropathic Pain Treatment—A Review. Plants. 2021; 10(5):865. https://doi.org/10.3390/plants10050865
Chicago/Turabian StyleQuiñonez-Bastidas, Geovanna N., and Andrés Navarrete. 2021. "Mexican Plants and Derivates Compounds as Alternative for Inflammatory and Neuropathic Pain Treatment—A Review" Plants 10, no. 5: 865. https://doi.org/10.3390/plants10050865
APA StyleQuiñonez-Bastidas, G. N., & Navarrete, A. (2021). Mexican Plants and Derivates Compounds as Alternative for Inflammatory and Neuropathic Pain Treatment—A Review. Plants, 10(5), 865. https://doi.org/10.3390/plants10050865







