What Is Next in Computer-Assisted Spine Surgery? Advances in Image-Guided Robotics and Extended Reality
Abstract
1. Introduction
2. Materials and Methods
3. Results
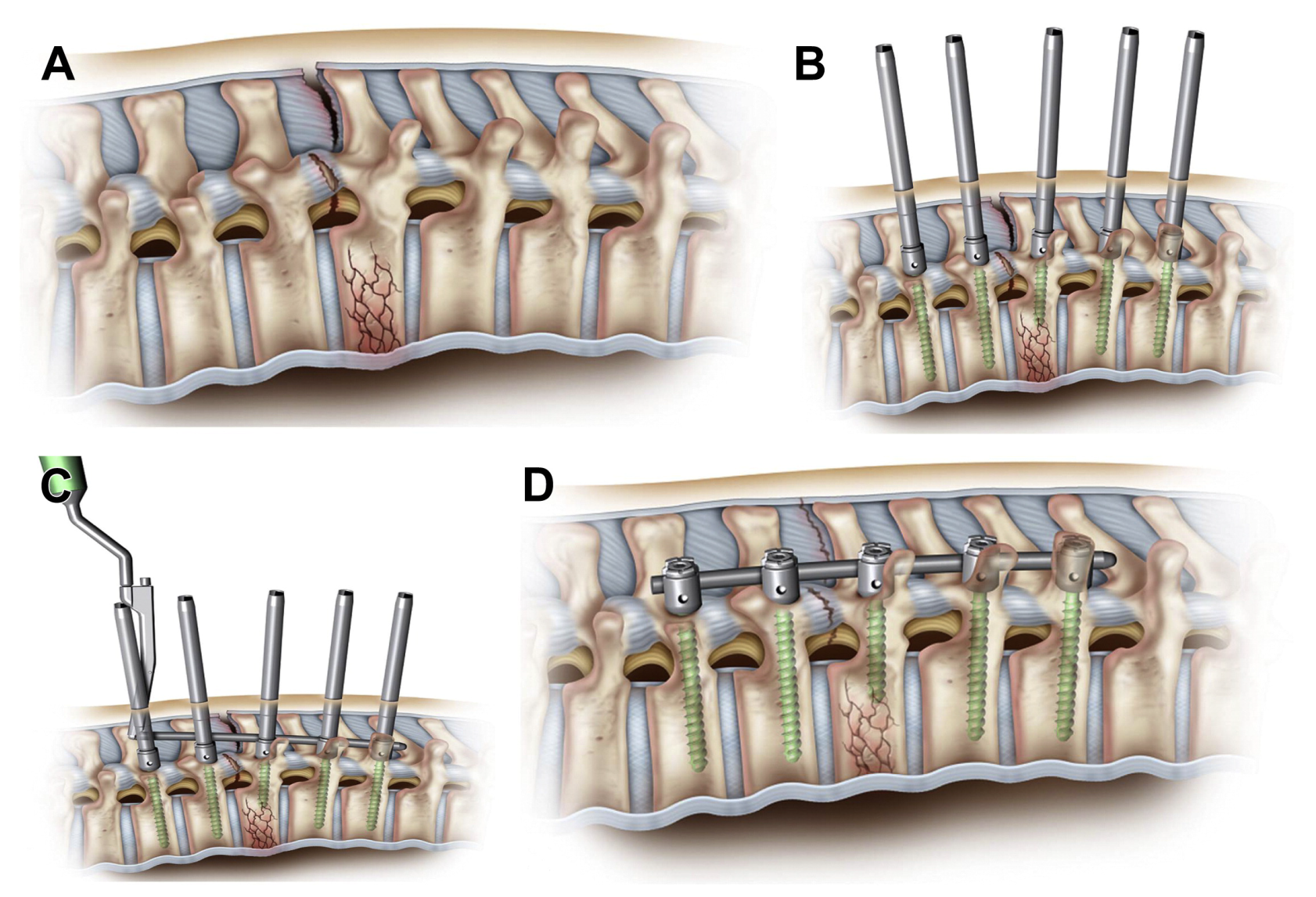
3.1. Accuracy
- A
- in the pedicle of vertebra screw position without breach detected;
- B
- screw exceeding the pedicle cortex is maximum 2 mm;
- C
- screw exceeding the pedicle cortex is 2–4 mm;
- D
- screw exceeding the pedicle cortex is 4–6 mm;
- E
- screw exceeding is more than 6 mm or outside of the pedicle.
- LTE: 2.78 mm .
- ATE: 4.85° .
- LTE: 3.96 mm .
- ATE: 5.02° .
- LTE: 1.52 mm .
- ATE: 4.92° .
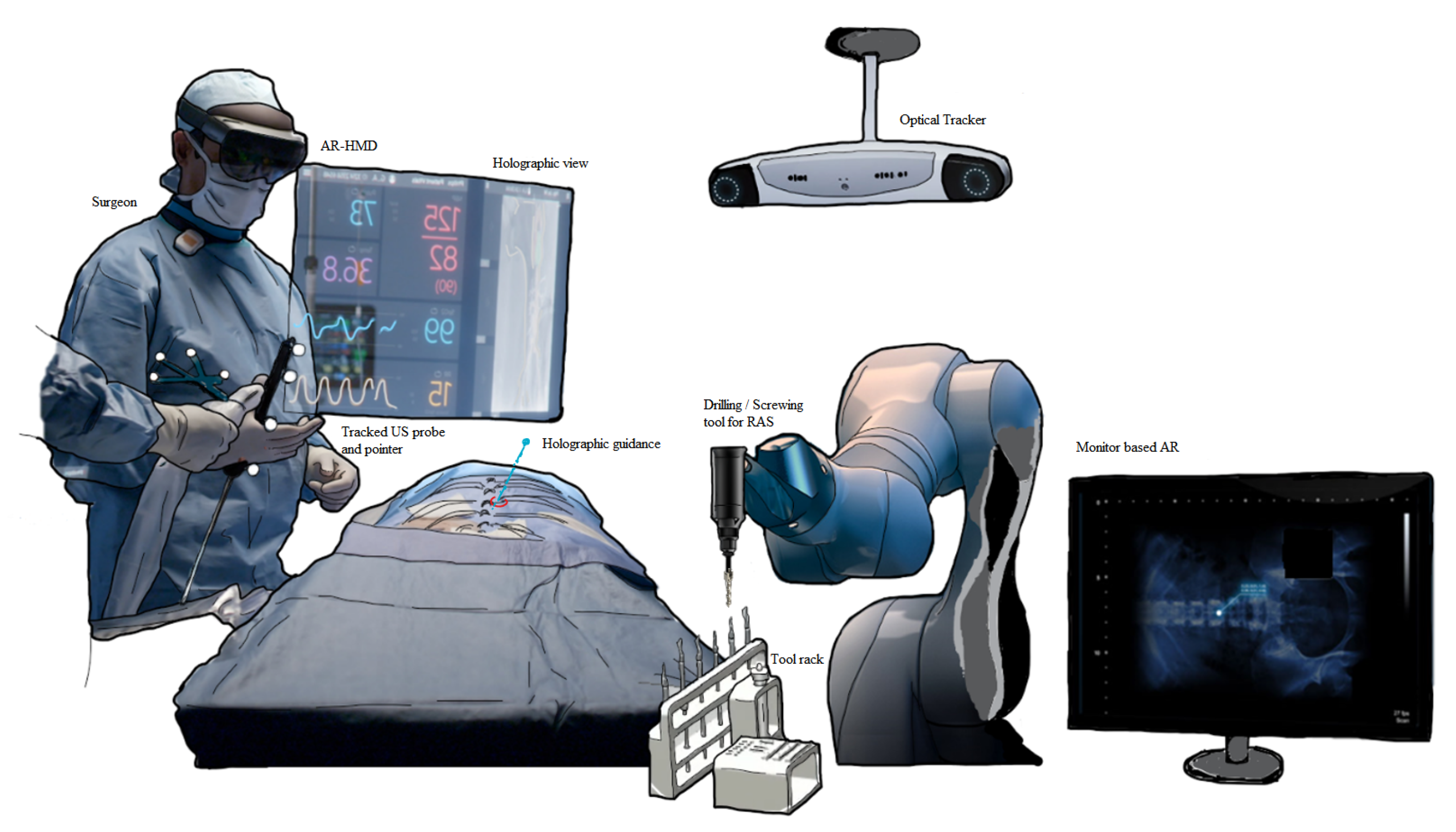
3.2. HMDs and Registration
3.3. User Experience of Surgeons
4. Discussion
4.1. Accuracy and Clinical Outcomes
4.2. Patient–Image Registration and Surgical Workflow
4.3. Ergonomics and Further Perspectives
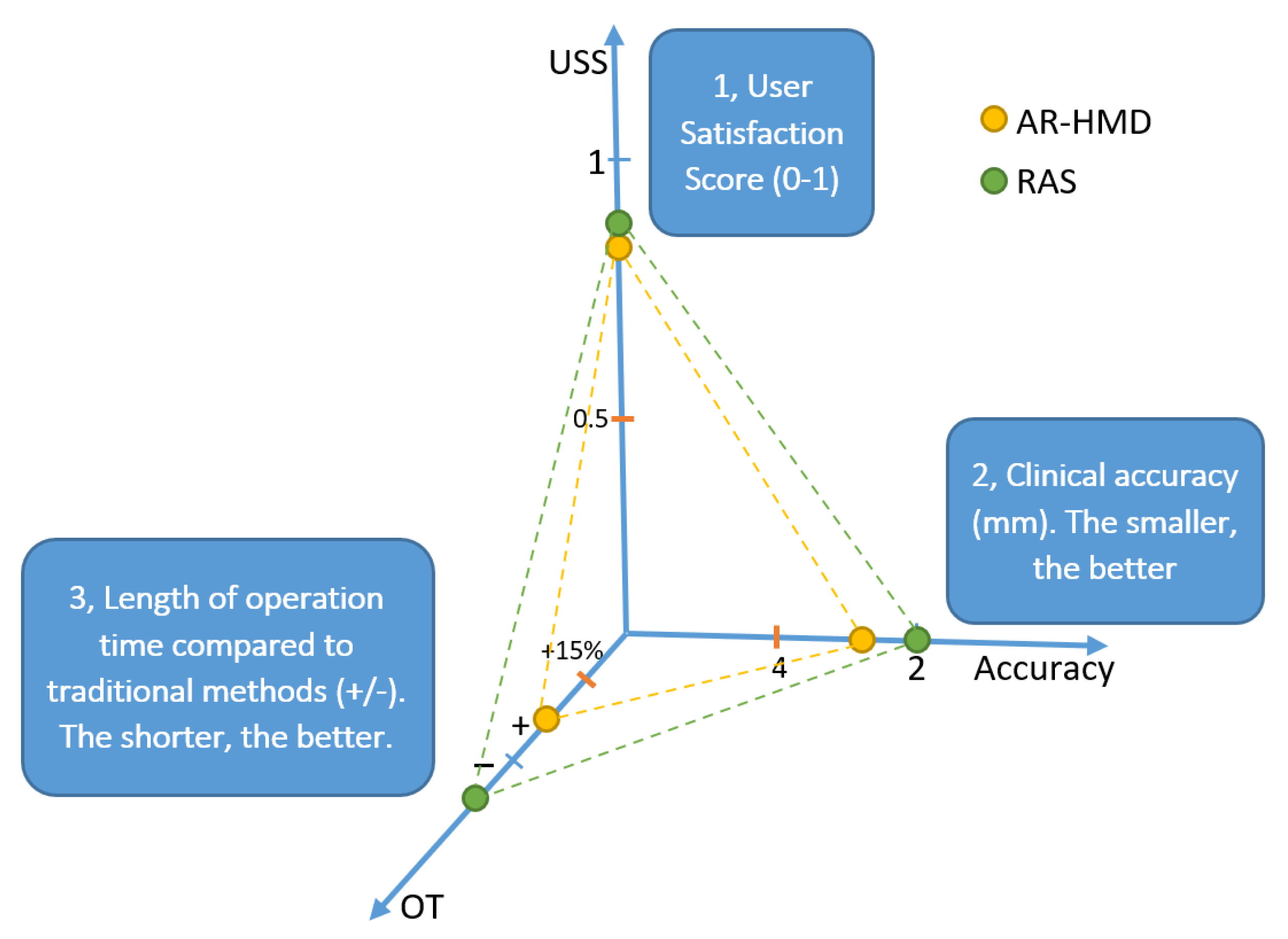
4.3.1. User Satisfaction Score
- Ergonomics: Weight and comfort in wearing the device for short- (<60 min) and long-term (>60 min) use. Overheating the device, sweating or humidity could present as distracting factors.
- Field of View (FoV): Both the size and the angular position of the FoV need to be matched to the surgical procedure.
- Image Quality, Accuracy and Immersion: Clear, accurate and contrasted visibility of AR elements on the transparent display, without disturbing the surgical field.
- Control: Precision and accuracy of the gaze/motion/voice commands of the device.
- Usability and Setup: Experience in understanding and using the HMD interface through starting up, image–patient registration and navigation.
- A future-proof application and overall satisfaction levels.
4.3.2. Technical Requirements and Benchmarking
- Essential Requirements:
- –
- Wide Field of View, humidity-free see-through display with dust, water and droplet resistance (IP65).
- –
- Built-in-one computer with a high-computing capacity.
- –
- Wireless connection.
- –
- Long battery life.
- –
- Easy, understandable user interface.
- –
- Support for setup, registration and calibration.
- –
- Ergonomics and balanced weight under 400 g.
- –
- Touchless and controller-free navigation with gaze/motion/voice commands.
- Additional Requirements:
- –
- Automatic focus adjusting to pupils;
- –
- Image, video and audio capturing, streaming.
- –
- Haptic/vibration feedback.
- –
- Environmental and/or situational awareness monitoring.
4.3.3. Situation Awareness
4.3.4. Standardized Scoring and Visualization Method for Surgical Navigation and Guidance Devices
5. Conclusions
Funding
Data Availability Statement
Conflicts of Interest
Abbreviations
| AR | Augmented Reality |
| ATE | Angular Trajectory Error |
| CAS/CIS | Computer-Assisted/Integrated Surgery |
| FDA | U.S. Food and Drug Administration |
| FH | Free-Handed (vertebral procedure) |
| GRS | Gertzbein–Robbins Scale |
| HMD | Head-Mounted Display |
| IGS | Image-Guided Surgery |
| LTE | Linear Tip Error |
| MR | Mixed Reality |
| OT | Operating Time |
| PSP | Pedicle Screw Placement |
| RAS | Robot-Assisted Surgery |
| XR | Extended Reality |
References
- Taylor, R.H.; Simaan, N.; Menciassi, A.; Yang, G.Z. Surgical robotics and computer-integrated interventional medicine. Proc. IEEE 2022, 110, 823–834. [Google Scholar] [CrossRef]
- Georgiou, K.E.; Georgiou, E.; Satava, R.M. 5G Use in Healthcare: The Future is Present. JSLS J. Soc. Laparosc. Robot. Surg. 2021, 25, e2021.00064. [Google Scholar] [CrossRef] [PubMed]
- Fichtinger, G.; Troccaz, J.; Haidegger, T. Image-guided interventional robotics: Lost in translation? Proc. IEEE 2022, 110, 932–950. [Google Scholar] [CrossRef]
- Ravindra, V.M.; Senglaub, S.S.; Rattani, A.; Dewan, M.C.; Härtl, R.; Bisson, E.; Park, K.B.; Shrime, M.G. Degenerative lumbar spine disease: Estimating global incidence and worldwide volume. Glob. Spine J. 2018, 8, 784–794. [Google Scholar] [CrossRef]
- Deepak Awasthi, M.; Najeeb Thomas, M. Pedicle Screw Placement. Available online: https://www.medschool.lsuhsc.edu/neurosurgery/nervecenter/tlscrew.html (accessed on 2 November 2022).
- Dahdaleh, N.S.; Smith, Z.A.; Hitchon, P.W. Percutaneous pedicle screw fixation for thoracolumbar fractures. Neurosurg. Clin. 2014, 25, 337–346. [Google Scholar] [CrossRef]
- Staartjes, V.E.; Klukowska, A.M.; Schröder, M.L. Pedicle screw revision in robot-guided, navigated, and freehand thoracolumbar instrumentation: A systematic review and meta-analysis. World Neurosurg. 2018, 116, 433–443. [Google Scholar] [CrossRef]
- Adogwa, O.; Parker, S.L.; Shau, D.; Mendelhall, S.K.; Aaronson, O.; Cheng, J.; Devin, C.J.; McGirt, M.J. Cost per quality-adjusted life year gained of revision fusion for lumbar pseudoarthrosis: Defining the value of surgery. Clin. Spine Surg. 2015, 28, 101–105. [Google Scholar] [CrossRef]
- Amato, V.; Giannachi, L.; Irace, C.; Corona, C. Accuracy of pedicle screw placement in the lumbosacral spine using conventional technique: Computed tomography postoperative assessment in 102 consecutive patients. J. Neurosurg. Spine 2010, 12, 306–313. [Google Scholar] [CrossRef]
- Du, J.P.; Fan, Y.; Wu, Q.N.; Zhang, J.; Hao, D.J. Accuracy of pedicle screw insertion among 3 image-guided navigation systems: Systematic review and meta-analysis. World Neurosurg. 2018, 109, 24–30. [Google Scholar] [CrossRef]
- Siller, S.; Raith, C.; Zausinger, S.; Tonn, J.C.; Szelenyi, A. Indication and technical implementation of the intraoperative neurophysiological monitoring during spine surgeries—A transnational survey in the German-speaking countries. Acta Neurochir. 2019, 161, 1865–1875. [Google Scholar] [CrossRef]
- Khamis, A.; Meng, J.; Wang, J.; Azar, A.T.; Prestes, E.; Takács, Á.; Rudas, I.J.; Haidegger, T. Robotics and intelligent systems against a pandemic. Acta Polytech. Hung. 2021, 18, 13–35. [Google Scholar] [CrossRef]
- Smith, A.D.; Chapin, J.; Birinyi, P.V.; Bhagvath, P.V.; Hall, A.F. Automated polyaxial screw placement using a commercial-robot-based, image-guided spine surgery system. IEEE Trans. Med. Robot. Bionics 2020, 3, 74–84. [Google Scholar] [CrossRef]
- Overley, S.C.; Cho, S.K.; Mehta, A.I.; Arnold, P.M. Navigation and robotics in spinal surgery: Where are we now? Neurosurgery 2017, 80, S86–S99. [Google Scholar] [CrossRef] [PubMed]
- Haidegger, T. Autonomy for surgical robots: Concepts and paradigms. IEEE Trans. Med. Robot. Bionics 2019, 1, 65–76. [Google Scholar] [CrossRef]
- Haidegger, T. Probabilistic Method to Improve the Accuracy of Computer-Integrated Surgical Systems. Acta Polytech. Hung. 2019, 16, 119–140. [Google Scholar] [CrossRef]
- Menger, R.P.; Savardekar, A.R.; Farokhi, F.; Sin, A. A cost-effectiveness analysis of the integration of robotic spine technology in spine surgery. Neurospine 2018, 15, 216. [Google Scholar] [CrossRef]
- 3D Slicer Image Computing Platform. Available online: https://https://www.slicer.org/ (accessed on 9 September 2022).
- Móga, K.; Boesl, D.B.; Haidegger, T. Augmented/Mixed Reality Technologies Supporting Digital Surgery. In Proceedings of the IEEE 19th International Symposium on Intelligent Systems and Informatics (SISY), Subotica, Serbia, 16–18 September 2021; IEEE: Piscataway, NJ, USA, 2021; pp. 183–189. [Google Scholar]
- Microsoft HoloLens 2. Available online: https://www.microsoft.com/en-us/hololens/industry-healthcare (accessed on 22 August 2022).
- Philips Showcases Unique Augmented Reality Concept for Image-Guided Minimally Invasive Therapies Developed with Microsoft. Available online: https://www.philips.com/a-w/about/news/archive/standard/news/press/2019/20190224-philips-showcases-unique-augmented-reality-concept-for-image-guided-minimally-invasive-therapies-developed-with-microsoft.html (accessed on 22 September 2022).
- NDI Navigate New Possibilities. Available online: https://www.ndigital.com/ (accessed on 22 September 2022).
- Burström, G.; Persson, O.; Edström, E.; Elmi-Terander, A. Augmented reality navigation in spine surgery: A systematic review. Acta Neurochir. 2021, 163, 843–852. [Google Scholar] [CrossRef]
- PRISMA. PRISMA Statement. Available online: http://www.prisma-statement.org/PRISMAStatement/ (accessed on 22 June 2022).
- Motahari-Nezhad, H.; Fgaier, M.; Péntek, M.; Gulácsi, L.; Zrubka, Z. Populations, Interventions, and Outcomes in Digital Biomarker-Based Interventions’ Systematic Reviews: A Scoping Review. Value Health 2022, 25, S534. [Google Scholar] [CrossRef]
- Molina, C.A.; Sciubba, D.M.; Greenberg, J.K.; Khan, M.; Witham, T. Clinical accuracy, technical precision, and workflow of the first in human use of an augmented-reality head-mounted display stereotactic navigation system for spine surgery. Oper. Neurosurg. 2021, 20, 300–309. [Google Scholar] [CrossRef]
- Li, J.; Zhang, H.; Li, Q.; Yu, S.; Chen, W.; Wan, S.; Chen, D.; Liu, R.; Ding, F. Treating lumbar fracture using the mixed reality technique. BioMed Res. Int. 2021, 2021, 6620746. [Google Scholar] [CrossRef]
- Liu, A.; Jin, Y.; Cottrill, E.; Khan, M.; Westbroek, E.; Ehresman, J.; Pennington, Z.; Lo, L.S.-f.; Sciubba, D.M.; Molina, C.A.; et al. Clinical accuracy and initial experience with augmented reality–assisted pedicle screw placement: The first 205 screws. J. Neurosurg. Spine 2021, 36, 351–357. [Google Scholar] [CrossRef] [PubMed]
- Dennler, C.; Bauer, D.E.; Scheibler, A.G.; Spirig, J.; Götschi, T.; Fürnstahl, P.; Farshad, M. Augmented reality in the operating room: A clinical feasibility study. BMC Musculoskelet. Disord. 2021, 22, 451. [Google Scholar] [CrossRef] [PubMed]
- Yahanda, A.T.; Moore, E.; Ray, W.Z.; Pennicooke, B.; Jennings, J.W.; Molina, C.A. First in-human report of the clinical accuracy of thoracolumbar percutaneous pedicle screw placement using augmented reality guidance. Neurosurg. Focus 2021, 51, E10. [Google Scholar] [CrossRef] [PubMed]
- Farshad, M.; Fürnstahl, P.; Spirig, J.M. First in man in situ augmented reality pedicle screw navigation. N. Am. Spine Soc. J. (NASSJ) 2021, 6, 100065. [Google Scholar] [CrossRef] [PubMed]
- Bhatt, F.R.; Orosz, L.D.; Tewari, A.; Boyd, D.; Roy, R.; Good, C.R.; Schuler, T.C.; Haines, C.M.; Jazini, E. Augmented Reality-Assisted Spine Surgery: An Early Experience Demonstrating Safety and Accuracy with 218 Screws. Glob. Spine J. 2022, 21925682211069321. [Google Scholar] [CrossRef]
- Felix, B.; Kalatar, S.B.; Moatz, B.; Hofstetter, C.; Karsy, M.; Parr, R.; Gibby, W. Augmented Reality Spine Surgery Navigation: Increasing Pedicle Screw Insertion Accuracy for Both Open and Minimally Invasive Spine Surgeries. Spine 2022, 47, 865–872. [Google Scholar] [CrossRef]
- Spirig, J.M.; Roner, S.; Liebmann, F.; Fürnstahl, P.; Farshad, M. Augmented reality-navigated pedicle screw placement: A cadaveric pilot study. Eur. Spine J. 2021, 30, 3731–3737. [Google Scholar] [CrossRef]
- Farshad, M.; Spirig, J.M.; Suter, D.; Hoch, A.; Burkhard, M.D.; Liebmann, F.; Farshad-Amacker, N.A.; Fürnstahl, P. Operator independent reliability of direct augmented reality navigated pedicle screw placement and rod bending. N. Am. Spine Soc. J. (NASSJ) 2021, 8, 100084. [Google Scholar] [CrossRef]
- Dennler, C.; Safa, N.A.; Bauer, D.E.; Wanivenhaus, F.; Liebmann, F.; Götschi, T.; Farshad, M. Augmented Reality Navigated Sacral-Alar-Iliac Screw Insertion. Int. J. Spine Surg. 2021, 15, 161–168. [Google Scholar] [CrossRef]
- Frisk, H.; Lindqvist, E.; Persson, O.; Weinzierl, J.; Bruetzel, L.K.; Cewe, P.; Burström, G.; Edström, E.; Elmi-Terander, A. Feasibility and accuracy of thoracolumbar pedicle screw placement using an augmented reality head mounted device. Sensors 2022, 22, 522. [Google Scholar] [CrossRef]
- Yanni, D.S.; Ozgur, B.M.; Louis, R.G.; Shekhtman, Y.; Iyer, R.R.; Boddapati, V.; Iyer, A.; Patel, P.D.; Jani, R.; Cummock, M.; et al. Real-time navigation guidance with intraoperative CT imaging for pedicle screw placement using an augmented reality head-mounted display: A proof-of-concept study. Neurosurg. Focus 2021, 51, E11. [Google Scholar] [CrossRef] [PubMed]
- Urakov, T.M. Augmented reality-assisted pedicle instrumentation: Versatility across major instrumentation sets. Spine 2020, 45, E1622–E1626. [Google Scholar] [CrossRef] [PubMed]
- Gertzbein, S.D.; Robbins, S.E. Accuracy of pedicular screw placement in vivo. Spine 1990, 15, 11–14. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.N.; Fan, Y.; Hao, D.J. Risk factors for robot-assisted spinal pedicle screw malposition. Sci. Rep. 2019, 9, 3025. [Google Scholar] [CrossRef] [PubMed]
- Microsoft. Hololens. Available online: https://www.microsoft.com/en-us/hololens (accessed on 13 July 2022).
- Augmedics. xVision. Available online: https://augmedics.com/ (accessed on 13 July 2022).
- Elmi-Terander, A.; Burström, G.; Nachabé, R.; Fagerlund, M.; Ståhl, F.; Charalampidis, A.; Edström, E.; Gerdhem, P. Augmented reality navigation with intraoperative 3D imaging vs fluoroscopy-assisted free-hand surgery for spine fixation surgery: A matched-control study comparing accuracy. Sci. Rep. 2020, 10, 707. [Google Scholar] [CrossRef]
- Hoeckelmann, M.; Rudas, I.J.; Fiorini, P.; Kirchner, F.; Haidegger, T. Current capabilities and development potential in surgical robotics. Int. J. Adv. Robot. Syst. 2015, 12, 61. [Google Scholar] [CrossRef]
- Van Dijk, J.D.; van den Ende, R.P.; Stramigioli, S.; Köchling, M.; Höss, N. Clinical pedicle screw accuracy and deviation from planning in robot-guided spine surgery: Robot-guided pedicle screw accuracy. Spine 2015, 40, E986–E991. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.; Meyers, J.E.; Siasios, I.; Pollina, J. Next-generation robotic spine surgery: First report on feasibility, safety, and learning curve. Oper. Neurosurg. 2019, 17, 61–69. [Google Scholar] [CrossRef]
- Jiang, B.; Pennington, Z.; Zhu, A.; Matsoukas, S.; Ahmed, A.K.; Ehresman, J.; Mahapatra, S.; Cottrill, E.; Sheppell, H.; Manbachi, A.; et al. Three-dimensional assessment of robot-assisted pedicle screw placement accuracy and instrumentation reliability based on a preplanned trajectory. J. Neurosurg. Spine 2020, 33, 519–528. [Google Scholar] [CrossRef]
- Lopez, I.; Benzakour, A.; Mavrogenis, A.; Benzakour, T.; Ahmad, A.; Lemée, J. Robotics in spine surgery: Systematic review of literature. Int. Orthop. 2022, 1–10. [Google Scholar] [CrossRef]
- Zhang, J.N.; Fan, Y.; He, X.; Liu, T.J.; Hao, D.J. Comparison of robot-assisted and freehand pedicle screw placement for lumbar revision surgery. Int. Orthop. 2021, 45, 1531–1538. [Google Scholar] [CrossRef]
- Yson, S.C.; Sembrano, J.N.; Sanders, P.C.; Santos, E.R.G.; Ledonio, C.G.T.; Polly, D.W., Jr. Comparison of cranial facet joint violation rates between open and percutaneous pedicle screw placement using intraoperative 3-D CT (O-arm) computer navigation. Spine 2013, 38, E251–E258. [Google Scholar] [CrossRef]
- Tovar, M.A.; Dowlati, E.; Zhao, D.Y.; Khan, Z.; Pasko, K.B.; Sandhu, F.A.; Voyadzis, J.M. Robot-assisted and augmented reality–assisted spinal instrumentation: A systematic review and meta-analysis of screw accuracy and outcomes over the last decade. J. Neurosurg. Spine 2022, 37, 299–314. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.J.; Zhou, L.P.; Zhang, H.Q.; Ge, P.; Jia, C.Y.; Shen, C.L. Rates and risk factors of intrapedicular accuracy and cranial facet joint violation among robot-assisted, fluoroscopy-guided percutaneous, and freehand techniques in pedicle screw fixation of thoracolumbar fractures: A comparative cohort study. BMC Surg. 2022, 22, 52. [Google Scholar] [CrossRef] [PubMed]
- Garcia, D.; Akinduro, O.O.; De Biase, G.; Sousa-Pinto, B.; Jerreld, D.J.; Dholakia, R.; Borah, B.; Nottmeier, E.; Deen, H.G.; Fox, W.C.; et al. Robotic-assisted vs. nonrobotic-assisted minimally invasive transforaminal lumbar interbody fusion: A cost-utility analysis. Neurosurgery 2022, 90, 192–198. [Google Scholar] [CrossRef] [PubMed]
- Takács, B.; Haidegger, T. Fasttracking Technology Transfer in Medical Robotics. In Proceedings of the 2021 IEEE 21st International Symposium on Computational Intelligence and Informatics (CINTI), Budapest, Hungary, 18–20 November 2021; pp. 61–66. [Google Scholar]
- Malham, G.M.; Munday, N.R. Comparison of novel machine vision spinal image guidance system with existing 3D fluoroscopy-based navigation system: A randomized prospective study. Spine J. 2022, 22, 561–569. [Google Scholar] [CrossRef]
- Ahmad, H.S.; Yoon, J.W. Intra-operative wearable visualization in spine surgery: Past, present, and future. J. Spine Surg. 2022, 8, 132. [Google Scholar] [CrossRef] [PubMed]
- Tu, P.; Qin, C.; Guo, Y.; Li, D.; Lungu, A.J.; Wang, H.; Chen, X. Ultrasound image guided and mixed reality-based surgical system with real-time soft tissue deformation computing for robotic cervical pedicle screw placement. IEEE Trans. Biomed. Eng. 2022, 69, 2593–2603. [Google Scholar] [CrossRef]
- Xu, D.-r.; Luan, L.-r.; Ma, X.-x.; Cong, Z.-c.; Zhou, C.-l. Comparison of electromagnetic and optical navigation assisted Endo-TLIF in the treatment of lumbar spondylolisthesis. BMC Musculoskelet. Disord. 2022, 23, 522. [Google Scholar] [CrossRef]
- Franz, A.M.; Haidegger, T.; Birkfellner, W.; Cleary, K.; Peters, T.M.; Maier-Hein, L. Electromagnetic tracking in medicine—A review of technology, validation, and applications. IEEE Trans. Med Imaging 2014, 33, 1702–1725. [Google Scholar] [CrossRef]
- Sirokai, B.; Kiss, M.; Kovács, L.; Benyó, B.I.; Benyó, Z.; Haidegger, T. Best Practices in Electromagnetic Tracking System Assessment. 2012. Available online: https://repozitorium.omikk.bme.hu/bitstream/handle/10890/4783/137019.pdf?sequence=1 (accessed on 22 August 2022).
- Vasan, N.; Scherman, D.B.; Kam, A. A tale of two robots: Operating times and learning curves in robot-assisted lumbar fusion. J. Clin. Neurosci. 2022, 97, 42–48. [Google Scholar] [CrossRef] [PubMed]
- Luengo-Matos, S.; Sánchez-Gómez, L.M.; Hijas-Gómez, A.I.; García-Carpintero, E.E.; Ballesteros-Massó, R.; Polo-deSantos, M. Efficacy and safety of robotic spine surgery: Systematic review and meta-analysis. J. Orthop. Traumatol. 2022, 23, 49. [Google Scholar] [CrossRef] [PubMed]
- Cofano, F.; Di Perna, G.; Bozzaro, M.; Longo, A.; Marengo, N.; Zenga, F.; Zullo, N.; Cavalieri, M.; Damiani, L.; Boges, D.J.; et al. Augmented reality in medical practice: From spine surgery to remote assistance. Front. Surg. 2021, 8, 657901. [Google Scholar] [CrossRef] [PubMed]
- Bitkina, O.V.; Kim, H.K.; Park, J. Usability and user experience of medical devices: An overview of the current state, analysis methodologies, and future challenges. Int. J. Ind. Ergon. 2020, 76, 102932. [Google Scholar] [CrossRef]
- Questionnaire for User Interaction Satisfaction (QUIS). Available online: https://www.umventures.org/technologies/quis%E2%84%A2-questionnaire-user-interaction-satisfaction-0 (accessed on 22 August 2022).
- Olsson, T. Concepts and subjective measures for evaluating user experience of mobile augmented reality services. In Human Factors in Augmented Reality Environments; Springer: Berlin/Heidelberg, Germany, 2013; pp. 203–232. [Google Scholar]
- Haidegger, T.; Kazanzides, P.; Rudas, I.; Benyó, B.; Benyó, Z. The importance of accuracy measurement standards for computer-integrated interventional systems. In Proceedings of the EURON GEM Sig Workshop on the Role of Experiments in Robotics Research at IEEE ICRA, Anchorage, AK, USA, 3 May 2010; pp. 1–6. [Google Scholar]
- Nagy, T.D.; Ukhrenkov, N.; Drexler, D.A.; Takács, Á.; Haidegger, T. Enabling quantitative analysis of situation awareness: System architecture for autonomous vehicle handover studies. In Proceedings of the 2019 IEEE International Conference on Systems, Man and Cybernetics (SMC), Bari, Italy, 6–9 October 2019; IEEE: Piscataway, NJ, USA, 2019; pp. 904–908. [Google Scholar]
- Woodward, J.; Ruiz, J. Analytic review of using augmented reality for situational awareness. IEEE Trans. Vis. Comput. Graph. 2022. Online ahead of print. [Google Scholar] [CrossRef]
- Gnjatović, M.; Maček, N.; Adamović, S. Putting Humans Back in the Loop: A Study in Human–Machine Cooperative Learning. Acta Polytech. Hung. 2020, 17, 191–210. [Google Scholar] [CrossRef]
- Nagy, T.D.; Haidegger, T. Performance and Capability Assessment in Surgical Subtask Automation. Sensors 2022, 22, 2501. [Google Scholar] [CrossRef]


| Author | Year | Use Case | # Cases | # Screws | Linear Tip Error (mm) | Angular Traj. Error (°) | Gertzbein–Robbins Scale | Device |
|---|---|---|---|---|---|---|---|---|
| Molina, C.A. et al. [26] | 2021/3 | in vivo | 1 | 6 | 2.07 (1.62–2.52) | 2.41 (1.57–3.25) | 100% A | xvision, Augmedics |
| Li, J. et al. [27] | 2021/3 | in vivo | 7 | 57 | N/A | N/A | 100% A | MITINS system (HoloLens) |
| Liu, A. et al. [28] | 2021/10 | in vivo | 28 | 205 | N/A | N/A | 98% A and B | xvision, Augmedics |
| Dennler, C. et al. [29] | 2021/5 | in vivo | 25 | N/A | N/A | N/A | “increased intraop. accuracy (78 ± 23 points)” | HoloLens |
| Yahanda, A.T. et al. [30] | 2021/8 | in vivo | 9 | 63 | N/A | N/A | 96.8% A, 3.2% B | xvision, Augmedics |
| Farshad, M. et al. [31] | 2021/5 | in vivo | 1 | 4 | 3.5 ± 1.9 | 7.3 ± 3.6 | N/A | HoloLens 2 |
| Bhatt, F.R. et al. [32] | 2022/1 | in vivo | 32 | 222 | N/A | N/A | 97.1% A and B | xvision, Augmedics |
| Felix, B. et al. [33] | 2022/2 | cadaver | 7 | 124 | 1.9 | 2.4 | 96% A and B | HoloLens 2 |
| Spirig, J.M. et al. [34] | 2021/12 | cadaver | 2 | 8 | 5.99 ± 3.60 | 5.88 ± 3.69 | N/A | HoloLens |
| Farshad, M. et al. [35] | 2021/1 | cadaver | 8 | 160 | 4 ± 2.7 | 6.8 ± 3.9 | 97.5% A and B | HoloLens 2 |
| Dennler, C. et al. [36] | 2021/2 | phantom | 1 | 40 | N/A | −10.8 ± 11.77 | 97.5% A | HoloLens |
| Frisk, H. et al. [37] | 2022/1 | phantom | 4 | 48 | 1.4 ± 0.8 | 3.0 ± 1.4 | 94% A and B | MagicLeap |
| Yanni, D.S. et al. [38] | 2021/8 | phantom | 24 | 192 | N/A | 5 | 98.4% A and B | SpineAR (prototype) |
| Urakov, T.M. [39] | 2020/12 | phantom | 5 | 60 | N/A | N/A | 97% | Caduceus AR |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Móga, K.; Ferencz, A.; Haidegger, T. What Is Next in Computer-Assisted Spine Surgery? Advances in Image-Guided Robotics and Extended Reality. Robotics 2023, 12, 1. https://doi.org/10.3390/robotics12010001
Móga K, Ferencz A, Haidegger T. What Is Next in Computer-Assisted Spine Surgery? Advances in Image-Guided Robotics and Extended Reality. Robotics. 2023; 12(1):1. https://doi.org/10.3390/robotics12010001
Chicago/Turabian StyleMóga, Kristóf, Andrea Ferencz, and Tamás Haidegger. 2023. "What Is Next in Computer-Assisted Spine Surgery? Advances in Image-Guided Robotics and Extended Reality" Robotics 12, no. 1: 1. https://doi.org/10.3390/robotics12010001
APA StyleMóga, K., Ferencz, A., & Haidegger, T. (2023). What Is Next in Computer-Assisted Spine Surgery? Advances in Image-Guided Robotics and Extended Reality. Robotics, 12(1), 1. https://doi.org/10.3390/robotics12010001








