Development of a Derivatization Method for Investigating Testosterone and Dehydroepiandrosterone Using Tandem Mass Spectrometry in Saliva Samples from Young Professional Soccer Players Pre- and Post-Training
Abstract
:1. Introduction
2. Materials and Methods
2.1. Chemicals and Materials
2.2. Preparation of 2-Hydrazino-1-Methylpyridine Derivative (HMP)
2.3. Instrumentation
2.3.1. Liquid Chromatographic Conditions
2.3.2. Mass Spectrometric Conditions
2.4. Experimental Design
2.5. Pre-Treatment and Extraction of Samples
2.6. Derivatization of Androgens with 2-Hydrazino-1-Methylpyridine Derivative HMP
2.7. Method Validation
2.7.1. Extraction Recovery
2.7.2. Matrix Effect
2.7.3. Specificity
2.7.4. Linearity and Calibration Standards of the Saliva
2.7.5. Sensitivity: Limit of Detection (LOD) and Limit of Quantification (LOQ)
LOQ = 10* Sy /Am
2.7.6. Accuracy and Precision
2.7.7. Stability
3. Results and Discussion
3.1. Optimization of Reaction Conditions in Derivatization Steroids with HMP
3.2. Optimization of LC Conditions
3.3. Optimization of MS Conditions
3.4. Collection of Saliva and Pre-Treatment
3.5. Solid Phase Extraction Cartridge Selection
3.6. Method Validation
3.6.1. Extraction Recovery from Spiked Human Saliva
3.6.2. Matrix Effects
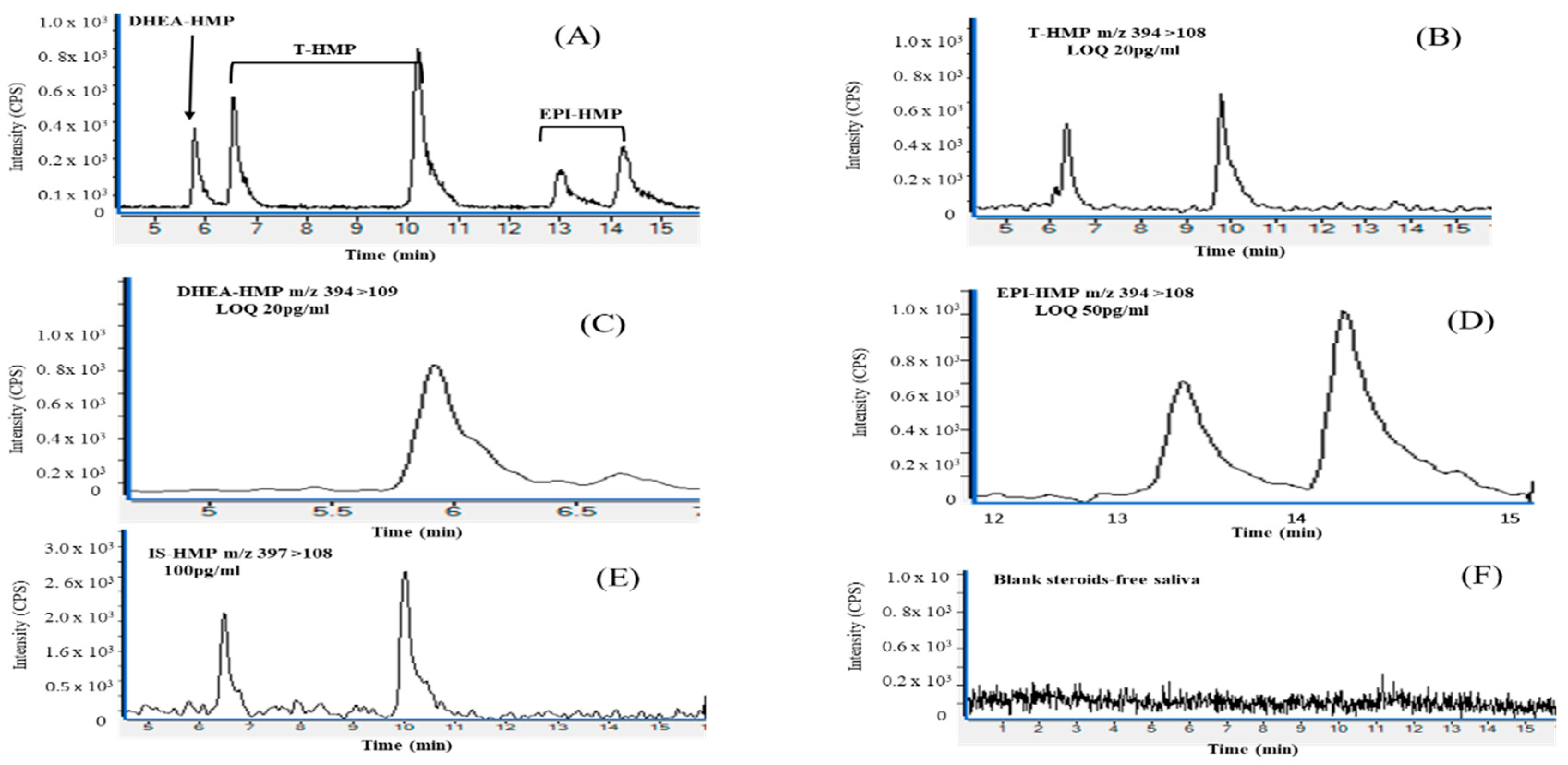
3.6.3. Specificity
3.6.4. Linearity and Calibration of Standards Spiked into Saliva
3.6.5. Sensitivity: Limit of Detection (LOD) and Limit of Quantification (LOQ)
3.6.6. Accuracy and Precision
3.6.7. Stability
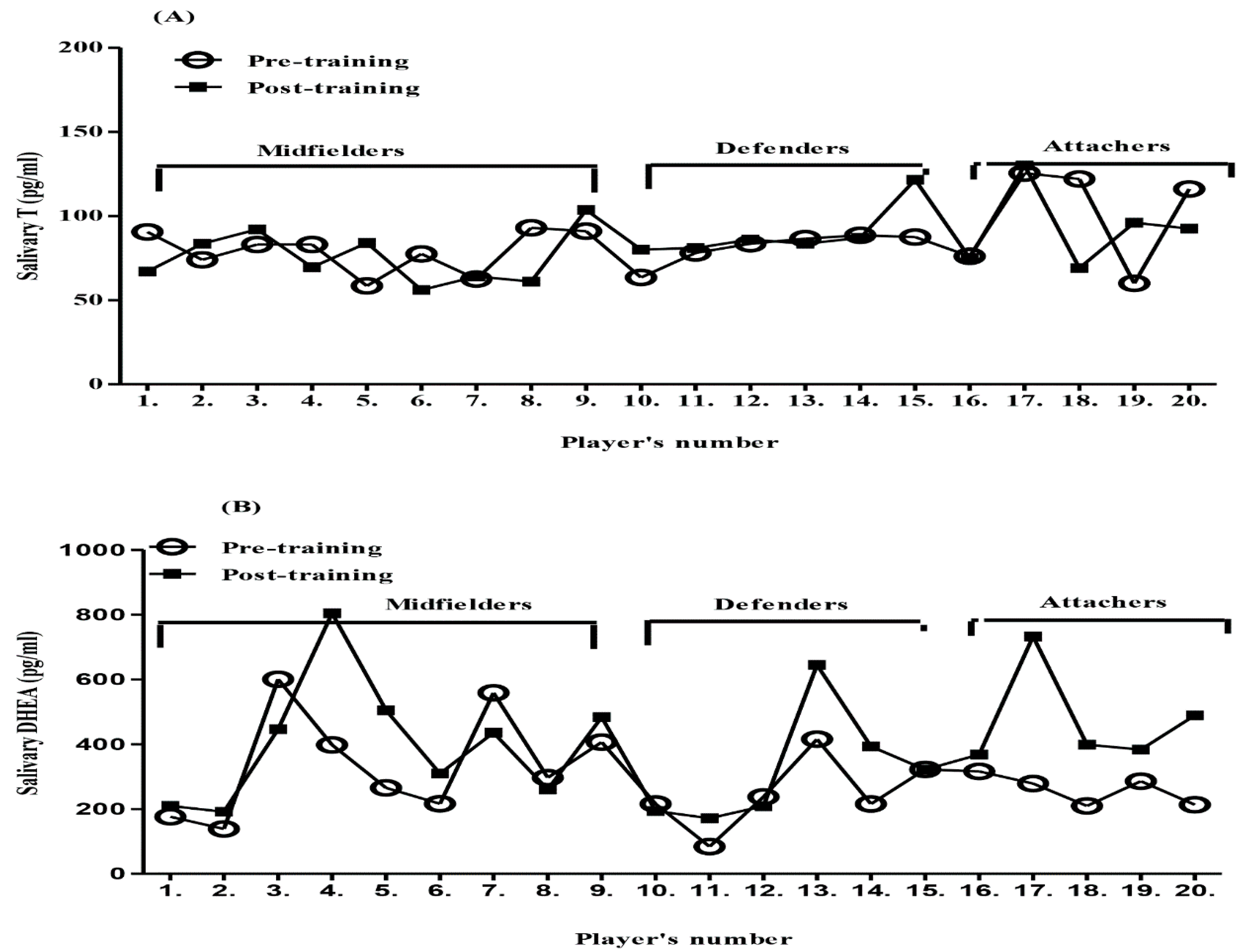
4. Method Application
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Mooradian, A.D.; Morley, J.E.; Korenman, S.G. Biological actions of androgens. Endocr. Rev. 1987, 8, 1–28. [Google Scholar] [CrossRef] [PubMed]
- Granger, D.A.; Schwartz, E.B.; Booth, A.; Curran, M.; Zakaria, D. Assessing dehydroepiandrosterone in saliva: A simple radioimmunoassay for use in studies of children, adolescents and adults. Psychoneuroendocrinology 1999, 24, 567–579. [Google Scholar] [CrossRef]
- Clark, L.C., Jr.; Kochakian, C.D.; Lobotsky, J. The in vitro metabolism of ∆4 -androstenedione-3,17 to testosterone, cis-testosterone, and several unidentified steroids. J. Biol. Chem. 1947, 171, 493–500. [Google Scholar] [PubMed]
- Arlt, W. Dehydroepiandrosterone and ageing. Best Pract. Res. Clin. Endocrinol. Metab. 2004, 18, 363–380. [Google Scholar] [CrossRef]
- Higashi, T.; Shibayama, Y.; Shimada, K. Determination of salivary dehydroepiandrosterone using liquid chromatography-tandem mass spectrometry combined with charged derivatization. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2007, 846, 195–201. [Google Scholar] [CrossRef]
- Ahu, R.S.; Lee, Y.J.; Choi, J.Y.; Kwon, H.B.; Chun, S.I. Salivary cortisol and DHEA levels in the Korean population: Age-related differences, diurnal rhythm, and correlations with serum levels. Yonsei Med. J. 2007, 48, 379–388. [Google Scholar]
- Keevil, B.G.; MacDonald, P.; Macdowall, W.; Lee, D.M.; Wu, F.C.W.; NATSAL Team. Salivary testosterone measurement by liquid chromatography tandem mass spectrometry in adult males and females. Ann. Clin. Biochem. 2014, 51, 368–378. [Google Scholar] [CrossRef]
- Dunn, J.F.; Nisula, B.C.; Rodbard, D. Transport of Steroid Hormones: Binding of 21 Endogenous Steroids to Both Testosterone-Binding Globulin and Corticosteroid-Binding Globulin in Human Plasma. J. Clin. Endocrinol. Metab. 1981, 53, 58–68. [Google Scholar] [CrossRef] [PubMed]
- Shibayama, Y.; Higashi, T.; Shimada, K.; Odani, A.; Mizokami, A.; Konaka, H.; Koh, E.; Namiki, M. Simultaneous determination of salivary testosterone and dehydroepiandrosterone using LC-MS/MS: Method development and evaluation of applicability for diagnosis and medication for late-onset hypogonadism. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2009, 877, 2615–2623. [Google Scholar] [CrossRef] [PubMed]
- Keevil, B.G.; Clifton, S.; Tanton, C.; Macdowall, W.; Copas, A.J.; Lee, D.; Field, N.; Mitchell, K.R.; Sonnenberg, P.; Bancroft, J.; et al. Distribution of Salivary Testosterone in Men and Women in a British General Population-Based Sample: The Third National Survey of Sexual Attitudes and Lifestyles (Natsal-3). J. Endocr. Soc. 2017, 1, 14–25. [Google Scholar]
- Di Luigi, L.; Baldari, C.; Gallotta, M.C.; Perroni, F.; Romanelli, F.; Lenzi, A.; Guidetti, L. Salivary Steroids at Rest and After a Training Load in Young Male Athletes: Relationship with Chronological Age and Pubertal Development. Int. J. Sports Med. 2006, 27, 709–717. [Google Scholar] [CrossRef]
- Beaven, C. Salivary testosterone and cortisol responses following four resistance training protocols in professional rugby players. J. Strength Cond. Res. 2008, 22, 426–432. [Google Scholar] [CrossRef] [PubMed]
- Rowell, A.E.; Aughey, R.J.; Hopkins, W.G.; Esmaeili, A.; Lazarus, B.H.; Cormack, S.J. Effects of training and competition load on neuromuscular recovery, testosterone, cortisol, and match performance during a season of professional football. Front. Physiol. 2018, 9, 668. [Google Scholar] [CrossRef] [PubMed]
- Lipsett, M.B.; Sarfaty, G.A.; Wilson, H.; Wayne Bardin, C.; Fishman, L.M. Metabolism of Testosterone and Related Steroids in Metastatic Interstitial Cell Carcinoma of the. J. Clin. Investig. 1966, 45, 1700–1709. [Google Scholar] [CrossRef]
- WADA. Prohibited List; World Anti-Doping Agency: Montreal, QC, Canada, 2017. [Google Scholar]
- Deshmukh, N.I.K.; Barker, J.; Petroczi, A.; Naughton, D.P. Detection of testosterone and epitestosterone in human hair using liquid chromatography-tandem mass spectrometry. J. Pharm. Biomed. Anal. 2012, 67–68, 154–158. [Google Scholar] [CrossRef] [PubMed]
- Jenkinson, C.; Deshmukh, N.I.; Shah, I.; Zachar, G.; Szekely, A.D.; Petroczi, A.; Naughton, D.P. LC-MS/MS-Based Assay for Free and Deconjugated Testosterone and Epitestosterone in Rat Urine and Serum. J. Anal. Bioanal. Tech. 2014, s5. [Google Scholar] [CrossRef]
- Draper, A.J.; Madan, A.; Smith, K.; Parkinson, A. Development of a non-high pressure liquid chromatography assay to determine testosterone hydroxylase (CYP3A) activity in human liver microsomes. Drug Metab. Dispos. Biol. Fate Chem. 1998, 26, 299–304. [Google Scholar]
- Shimada, K.; Mitamura, K.; Higashi, T. Gas chromatography and high-performance liquid chromatography of natural steroids. J. Chromatogr. A 2001, 935, 141–172. [Google Scholar] [CrossRef]
- Gonzalo-Lumbreras, R.; Pimentel-Trapero, D.; Izquierdo-Hornillos, R. Development and method validation for testosterone and epitestosterone in human urine samples by liquid chromatography applications. J. Chromatogr. Sci. 2003, 41, 261–265. [Google Scholar] [CrossRef]
- Rauh, M. Steroid measurement with LC-MS/MS in pediatric endocrinology. Mol. Cell. Endocrinol. 2009, 301, 272–281. [Google Scholar] [CrossRef]
- Higashi, T.; Yamauchi, A.; Shimada, K. 2-Hydrazino-1-methylpyridine: A highly sensitive derivatization reagent for oxosteroids in liquid chromatography–electrospray ionization-mass spectrometry. J. Chromatogr. B 2005, 825, 214–222. [Google Scholar] [CrossRef]
- Büttler, R.M.; Peper, J.S.; Crone, E.A.; Lentjes, E.G.; Blankenstein, M.A.; Heijboer, A.C. Reference values for salivary testosterone in adolescent boys and girls determined using Isotope-Dilution Liquid-Chromatography Tandem Mass Spectrometry (ID-LC-MS/MS). Clin. Chim. Acta 2016, 456, 15–18. [Google Scholar] [CrossRef]
- Santa, T.; Al-Dirbashi, O.Y.; Fukushima, T. Derivatization reagents in liquid chromatography/electrospray ionization tandem mass spectrometry for biomedical analysis. Drug Discov. Ther. 2007, 1, 108–118. [Google Scholar]
- Lai, C.-C.; Tsai, C.-H.; Tsai, F.-J.; Lee, C.-C.; Lin, W.-D. Rapid monitoring assay of congenital adrenal hyperplasia with microbore high-performance liquid chromatography/electrospray ionization tandem mass spectrometry from dried blood spots. Rapid Commun. Mass Spectrom. 2001, 15, 2145–2151. [Google Scholar] [CrossRef]
- Quirke, J.M.E.; Adams, C.L.; Van Berkel, G.J. Chemical Derivatization for Electrospray Ionization Mass Spectrometry. 1. Alkyl Halides, Alcohols, Phenols, Thiols, and Amines. Anal. Chem. 1994, 66, 1302–1315. [Google Scholar] [CrossRef]
- Ostatníková, D.; Pastor, K.; Putz, Z.; Dohnányiová, M.; Mat’ašeje, A.; Hampl, R. Salivary testosterone levels in preadolescent children. BMC Pediatr. 2002, 2, 5. [Google Scholar]
- Morley, J.E.; Perry, H.M.; Patrick, P.; Dollbaum, C.M.; Kells, J.M. Validation of salivary testosterone as a screening test for male hypogonadism. Aging Male 2006, 9, 165–169. [Google Scholar] [CrossRef]
- Yasuda, M.; Honma, S.; Furuya, K.; Yoshii, T.; Kamiyama, Y.; Ide, H.; Muto, S.; Horie, S. Diagnostic significance of salivary testosterone measurement revisited: Using liquid chromatography/mass spectrometry and enzyme-linked immunosorbent assay. J. Men’s Health 2008, 5, 56–63. [Google Scholar] [CrossRef]
- Cardoso, E.M.; Contreras, L.N.; Tumilasci, E.G.; Elbert, A.; Aguirre, E.C.; Aquilano, D.R.; Arregger, A.L. Salivary testosterone for the diagnosis of androgen deficiency in end-stage renal disease. Nephrol. Dial. Transplant. 2010, 26, 677–683. [Google Scholar] [CrossRef]
- Macdonald, P.R.; Owen, L.J.; Wu, F.C.; Macdowall, W.; Keevil, B.G. A liquid chromatography-tandem mass spectrometry method for salivary testosterone with adult male reference interval determination. Clin. Chem. 2011, 57, 774–775. [Google Scholar] [CrossRef]
- Maya, J.; Marquez, P.; Peñailillo, L.; Contreras-Ferrat, A.; Deldicque, L.; Zbinden-Foncea, H. Salivary Biomarker Responses to Two Final Matches in Women’s Professional Football. J. Sports Sci. Med. 2016, 15, 365–371. [Google Scholar]
- Clifton, S.; Macdowall, W.; Copas, A.J.; Tanton, C.; Keevil, B.G.; Lee, D.M.; Mitchell, K.R.; Field, N.; Sonnenberg, P.; Bancroft, J.; et al. Salivary testosterone levels and health status in men and women in the British general population: Findings from the third National Survey of Sexual Attitudes and Lifestyles (Natsal-3). J. Clin. Endocrinol. Metab. 2016, 101, jc20161669. [Google Scholar] [CrossRef]
- Food and Drug Administration. Available online: https://www.fda.gov/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/default.htm (accessed on 9 April 2019).
- Hall, T.G.; Smukste, I.; Bresciano, K.R.; Wang, Y.; McKearn, D.; Savage, R.E. Identifying and Overcoming Matrix Effects in Drug Discovery and Development. Intech Eur. 2012, 18, 389–420. [Google Scholar]
- Shou, W.; Naidong, W. Simple means to alleviate sensitivity loss by trifluoroacetic acid (TFA) mobile phases in the hydrophilic interaction chromatography–electrospray tandem mass spectrometric (HILIC–ESI/MS/MS) bioanalysis of basic compounds. J. Chromatogr. B 2005, 825, 186–192. [Google Scholar] [CrossRef]
- Choo, R.E.; Huestis, M.A. Oral fluid as a diagnostic tool. Clin. Chem. Lab. Med. 2004, 42, 1273–1287. [Google Scholar] [CrossRef]
- Gröschl, M.; Köhler, H.; Topf, H.G.; Rupprecht, T.; Rauh, M. Evaluation of saliva collection devices for the analysis of steroids, peptides and therapeutic drugs. J. Pharm. Biomed. Anal. 2008, 47, 478–486. [Google Scholar] [CrossRef]
- Gröschl, M.; Rauh, M. Influence of commercial collection devices for saliva on the reliability of salivary steroids analysis. Steroids 2006, 71, 1097–1100. [Google Scholar] [CrossRef]
- Sample Prep—SPE Method Development Tool—CHROMacademy. Available online: https://www.chromacademy.com/chromatography-SPE-Meth-Dev.html (accessed on 9 April 2019).
- Cormack, S.J.; Newton, R.U.; McGuigan, M.R.; Cormie, P. Neuromuscular and endocrine responses of elite players during an Australian rules football season. Int. J. Sports Physiol. Perform. 2008, 3, 439–453. [Google Scholar] [CrossRef]
- Howe, C.; Alshehri, A.; Muggeridge, D.; Mullen, A.; Boyd, M.; Spendiff, O.; Moir, H.; Watson, D. Untargeted Metabolomics Profiling of an 80.5 km Simulated Treadmill Ultramarathon. Metabolites 2018, 8, 14. [Google Scholar] [CrossRef]
| Author, Year (Ref.) | Analyte | Instrument | Collection Method | Extraction | Derivative | Chromatography | LOQ | Case Samples |
|---|---|---|---|---|---|---|---|---|
| Granger et al.,1999 [2] | DHEA | radioimmunoassay | directly | 64 (8–11 y) 96 (12–17 y) 48 (30–45 y) | ||||
| Ostatníková et al., 2002 [27] | T | radioimmunoassay | directly | 77 girls & 126 boys (6–9 y) | ||||
| Morley et al., 2006 [28] | T | radioimmunoassay | directly | 1454 (20–89 y) male | ||||
| Ahu et al. 2007 [6] | Cortisol and DHEA | radioimmunoassay | directly | 359 (21–96 y) male &female | ||||
| Higashi et al., 2007 [5] | DHEA | LC–ESI-MS–MS | directly | SPE Strata-X (ethyl acetate) * | (HMP) incubation (60 °C for 1 h) | ODS-H-80 column (10 µL injected) | 25 pg/mL | 3 (33–23 y) male 3 (22–24 y) female |
| Beaven et al., 2008 [12] | Cortisol and T | immunoassay | Directly | 23 men rugby players | ||||
| Yasuda., 2008 [29] | T | LC-MS and ELISA | directly | LLE (ethyl acetate) | CD-C18 column | 51 (30–85 y) 29 (55–78 y) | ||
| Shibayamaet al.,2009 [9] | DHEA and T | LC–ESI-MS–MS | directly | SPE Strata-X (ethyl acetate) * | (HMP) incubation (60 °C for 1 h) | AYMC-Pack Pro C18 RS column (10 µL injected) | 10 pg/mL | 114 (21–89 y) |
| Cardoso et al.,2010 [30] | T | radioimmunoassay | directly | 60 (20–60 y) male | ||||
| Macdonald et al., 2011 [31] | T | LC-MS/MS | directly | LLE (methyl-tert-butyl ether) | C18 column | 7 pg/mL | 103 (16–74 y) male | |
| Keevil et al., 2014 [7] | T | LC-MS/MS | directly | LLE (methyl-tert-butyl ether) * | C8 column (35 µL injected) | 1.5 pg/mL | 104 males 91 females | |
| Maya et al., 2016 [32] | Cortisol and T | ELISA | directly | 16 (22.5 ± 2.1 y) female players | ||||
| Clifton et al., 2016 [33] | T | LC-MS/MS | directly | LLE (methyl-tert-butyl ether) * | C8 column (35 µL injected) | 1.8 pg/mL | 1599 male 2123 female (18–74 y) | |
| Büttler et al., 2016 [23] | T | LC-MS/MS | directly | (SPE) Symbiosis online solid phase extraction | methoxylamine hydrochloride | LOD 1.3 pg/mL | 131 girls and 123 boys (8–26 y) | |
| Keevil et al., 2017 [10] | T | LC-MS/MS | directly | LLE (methyl-tert-butyl ether) * | C8 column (35 µL injected) | 1.5 pg/mL | 1675 male 2453 female | |
| Rowell et al., 2018 [13] | Cortisol and T | ELISA | directly | 23 (23 ± 4.1 y) Football player | ||||
| This study | DHEA and T | LC-MS/MS | Salivette Polyester | (SPE) Strata-XL polymeric reverse phase (ACN) * | (HMP) incubation (50 °C for 30 min) | Ultracore 2.5 Superphenylhexyl column (10 µL injected) | 20 pg/mL | 20 (20.6± 1.4 y) male football players |
| Analyte | MRM Transition (m/z) | Fragmentation Voltage | CE (V) |
|---|---|---|---|
| T-HMP | 394 > 108 | 130 | 40 |
| T-d3-HMP | 397 > 108 | 200 | 50 |
| EPI-HMP | 394 > 108 | 210 | 40 |
| DHEA-HMP | 394 > 109 | 120 | 35 |
| Parameter | Ranges | The Optimum Conditions |
|---|---|---|
| Delta | 400–600–800 | 800 |
| Gas temperature | 300–325–350 °C | 350 °C |
| Gas flow | 8–9–10–11 L/min | 9 L/min |
| Nebulization pressure | 15–20–25–30 psi | 20 psi |
| Compounds | Concentration (pg/mL) | Level | Average Ratio | Extraction Recovery | |
|---|---|---|---|---|---|
| Extracted | Non-Extracted | ||||
| n = 3 | Mean ± S.D. * | Mean± S.D. * | (%) | ||
| T | 100 | Low | 7037 ± 416 | 6650 ± 197 | 105.8 |
| 400 | Medium | 21,797 ± 766 | 21,590 ± 1569 | 101.0 | |
| 800 | High | 56,725 ± 2196 | 63,539 ± 5556 | 89.3 | |
| DHEA | 100 | Low | 5072 ± 207 | 4880 ± 532 | 103.9 |
| 400 | Medium | 21,760 ± 1214 | 23,187 ± 1181 | 93.8 | |
| 800 | High | 48,749 ± 1297 | 52,424 ± 4102 | 93.0 | |
| EPI | 100 | Low | 3853 ± 233 | 3828 ± 261 | 100.7 |
| 400 | Medium | 12,629 ± 745 | 12,420 ± 119 | 101.7 | |
| 800 | High | 23,231 ± 1872 | 23,424 ± 2244 | 99.2 | |
| T-d3 | 200 | IS | 7727 ± 882 | 8720 ± 883 | 112.8 |
| Analyte | LOD pg/mL | LLOQ pg/mL | Slope | Intercept | r | |||
|---|---|---|---|---|---|---|---|---|
| Mean | S.D. | RSD | Mean | S.D. | Mean | |||
| T | 4 | 20 | 0.0337 | 0.000954 | 2.83068 | 0.280067 | 0.016757 | 0.9978 |
| DHEA | 6 | 20 | 0.034333 | 0.000551 | 1.60414 | 0.224933 | 0.023755 | 0.9996 |
| EPI | 14 | 50 | 0.0186 | 0.000173 | 0.93121 | 0.326333 | 0.041834 | 0.995 |
| Analyte | Concentration | Level | Intra-Day | Inter-Day | ||||
|---|---|---|---|---|---|---|---|---|
| (pg/mL) | RSD a (%) | Mean (pg/mL) | Accuracy b | RSD a (%) | Mean (pg/mL) | Accuracy b | ||
| T | 50 | Low | 6.8 | 46.8 | 93.5 | 9.9 | 47.0 | 93.9 |
| 400 | Medium | 5.9 | 401 | 100.5 | 4.1 | 409.8 | 102.4 | |
| 800 | High | 3.0 | 816 | 102.0 | 5.5 | 760.4 | 95.1 | |
| DHEA | 50 | Low | 4.1 | 51.2 | 102.4 | 8.6 | 57.2 | 114.5 |
| 400 | Medium | 1.8 | 405.0 | 102.5 | 10.8 | 398.4 | 99.6 | |
| 800 | High | 2.3 | 795.8 | 99.5 | 7.4 | 784.8 | 98.1 | |
| EPI | 50 | Low | 8.9 | 49.8 | 99.6 | 9.9 | 47.0 | 93.9 |
| 400 | Medium | 3.4 | 427.8 | 106.9 | 4.1 | 409.8 | 102.4 | |
| 800 | High | 4.7 | 731.4 | 91.4 | 5.5 | 760.4 | 95.0 | |
| Treatment | T a | DHEA a | EPI a | ||||
|---|---|---|---|---|---|---|---|
| 100 | 800 | 100 | 800 | 100 | 800 | ||
| Freezing/thawing, 1 cycle | −20 °C | 100.1 ± 9.1 | 98.0 ± 1.7 | 100.1 ± 0.1 | 97.1 ± 1.8 | 98.0 ± 0.5 | 97.2 ± 5.7 |
| 4 °C | 98.1 ± 3.9 | 97.2 ± 0.6 | 96.4 ± 0.6 | 96.7 ± 1.6 | 94.8 ± 2.3 | 95.2 ± 5.1 | |
| Auto-sampler | 97.0 ± 2.2 | 96.9 ± 3.2 | 95.1 ± 1.0 | 95.7 ± 1.4 | 95.7 ± 0.8 | 92.5 ± 3.3 | |
| Freezing/thawing, 2 cycles | −20 °C | 97.2 ± 4.0 | 98.7 ± 0.0 | 99.8 ± 2.3 | 96.9 ± 2.3 | 94.4 ± 3.1 | 95.7 ± 2.2 |
| 4 °C | 98.1 ± 2.6 | 95.7 ± 3.3 | 96.7 ± 5.7 | 97.3 ± 4.9 | 92.8 ± 2.7 | 93.5 ± 0.1 | |
| Auto-sampler | 93.8 ± 1.6 | 94.6 ± 6.4 | 95.5 ± 1.8 | 92.3 ± 1.0 | 94.8 ± 5.5 | 91.4 ± 6.5 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alzahrani, M.A.; O. Alshuwaier, G.; S. Aljaloud, K.; Gibson, C.; Khalaf, A.; S. Alhawiti, A.; G. Watson, D. Development of a Derivatization Method for Investigating Testosterone and Dehydroepiandrosterone Using Tandem Mass Spectrometry in Saliva Samples from Young Professional Soccer Players Pre- and Post-Training. Sci. Pharm. 2019, 87, 11. https://doi.org/10.3390/scipharm87020011
Alzahrani MA, O. Alshuwaier G, S. Aljaloud K, Gibson C, Khalaf A, S. Alhawiti A, G. Watson D. Development of a Derivatization Method for Investigating Testosterone and Dehydroepiandrosterone Using Tandem Mass Spectrometry in Saliva Samples from Young Professional Soccer Players Pre- and Post-Training. Scientia Pharmaceutica. 2019; 87(2):11. https://doi.org/10.3390/scipharm87020011
Chicago/Turabian StyleAlzahrani, Mansour A., Ghareeb O. Alshuwaier, Khalid S. Aljaloud, Colin Gibson, Abedawn Khalaf, Aliyah S. Alhawiti, and David G. Watson. 2019. "Development of a Derivatization Method for Investigating Testosterone and Dehydroepiandrosterone Using Tandem Mass Spectrometry in Saliva Samples from Young Professional Soccer Players Pre- and Post-Training" Scientia Pharmaceutica 87, no. 2: 11. https://doi.org/10.3390/scipharm87020011
APA StyleAlzahrani, M. A., O. Alshuwaier, G., S. Aljaloud, K., Gibson, C., Khalaf, A., S. Alhawiti, A., & G. Watson, D. (2019). Development of a Derivatization Method for Investigating Testosterone and Dehydroepiandrosterone Using Tandem Mass Spectrometry in Saliva Samples from Young Professional Soccer Players Pre- and Post-Training. Scientia Pharmaceutica, 87(2), 11. https://doi.org/10.3390/scipharm87020011






