Overview of Availability, Cost, and Affordability of Antibiotics for Adults in Jordan: An AWaRe Classification Perspective
Abstract
:1. Introduction
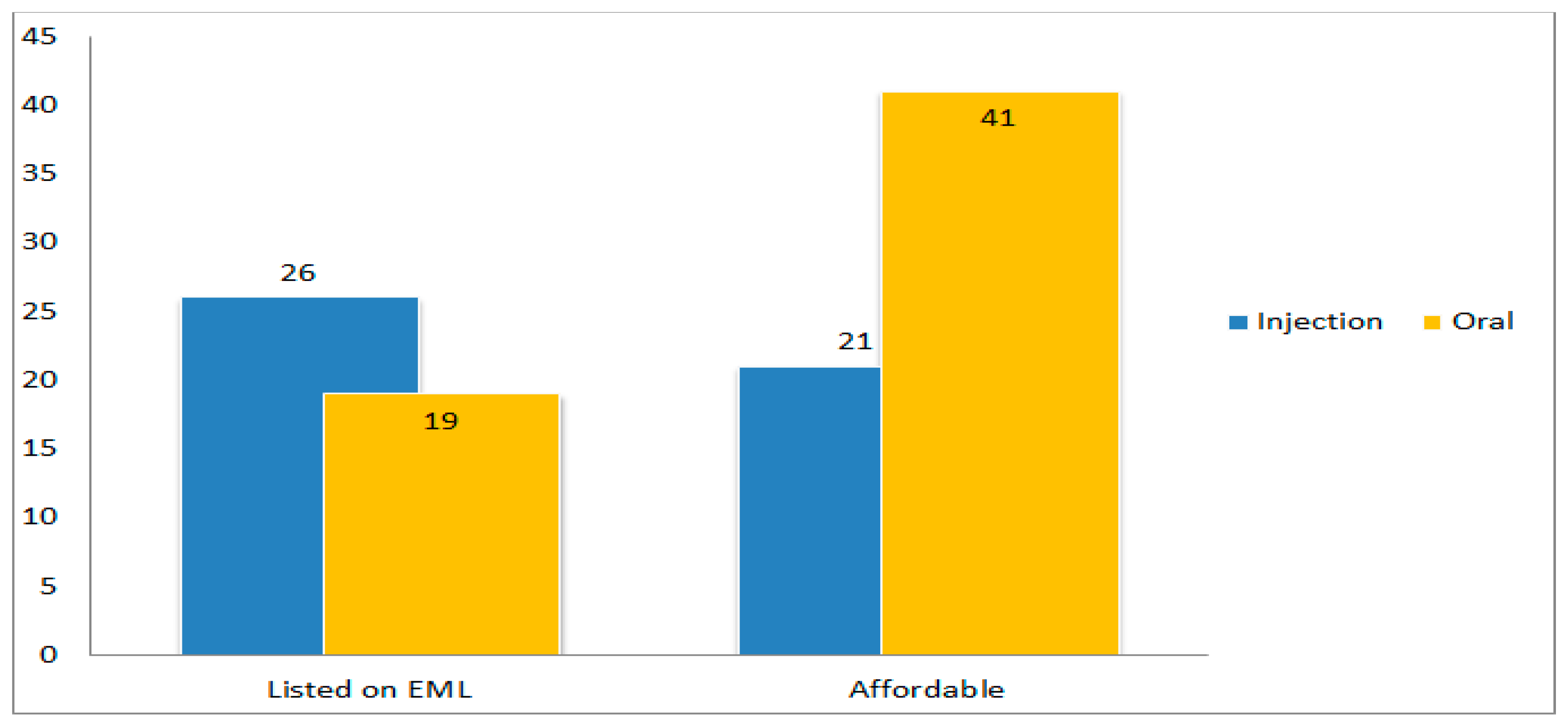
2. Results
Affordability of the Antibiotics
3. Discussion
4. Methods
4.1. Sources of Data
- 1-
- The WHO AWaRe classification of antibiotics for the evaluation and monitoring of use, 2023. This was downloaded from the 2023 AWaRe classification webpage of the WHO [4]. Information such as the 2023 AWaRe classification of antibiotics, pharmacological class, and the Anatomical Therapeutic Chemical (ATC) code of the antibiotics were extracted from this source.
- 2-
- The 23rd EML that was issued in 2023 [22] was utilized to determine the status of listing of each antibiotic (according to its dosage form and route of administration).
- 3-
- An index that uses ATC codes was used to find each antibiotic’s DDD. The ATC/DDD index is a searchable version of the complete ATC index with DDDs provided online by the WHO Collaborating Centre for Drug Statistics Methodology and the Norwegian Institute of Public Health [23].
- 4-
- Drug information, prices, and leaflets webpage by JFDA [24]. Prices of registered antibiotic items in all available packs for all marketing authorization holders in Jordan could be found through this official webpage.
4.2. Cost of DDD
4.3. Affordability
4.4. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Minarini, L.A.D.R.; de Andrade, L.N.; De Gregorio, E.; Grosso, F.; Naas, T.; Zarrilli, R.; Camargo, I.L.B.C. Editorial: Antimicrobial Resistance as a Global Public Health Problem: How Can We Address It? Front. Public Health 2020, 8, 612844. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Report on Surveillance of Antibiotic Consumption: 2016–2018 Early Implementation. Geneva. 2018. Available online: https://www.who.int/publications/i/item/who-report-on-surveillance-of-antibiotic-consumption (accessed on 28 August 2023).
- Cox, J.A.; Vlieghe, E.; Mendelson, M.; Wertheim, H.; Ndegwa, L.; Villegas, M.V.; Gould, I.; Hara, G.L. Antibiotic stewardship in low- and middle-income countries: The same but different? Clin. Microbiol. Infect. 2017, 23, 812–818. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO AWaRe (access, watch, reserve) classification of antibiotics for evaluation and monitoring of use, 2023. In Proceedings of the Selection and Use of Essential Medicines 2023: Executive Summary of the Report of the 24th WHO Expert Committee on the Selection and Use of Essential Medicines, Geneva, Switzerland, 24–28 April 2023; Available online: https://www.who.int/publications/i/item/WHO-MHP-HPS-EML-2023.04 (accessed on 28 August 2023).
- The WHO AWaRe (Access, Watch, Reserve) Antibiotic Book; World Health Organization: Geneva, Switzerland, 2022; Available online: https://iris.who.int/bitstream/handle/10665/365135/WHO-MHP-HPS-EML-2022.02-eng.pdf (accessed on 28 August 2023).
- European Centre for Disease Prevention and Control. Antimicrobial Consumption in the EU/EEA (ESAC-Net)—Annual Ep-idemiological Report 2021; UCDC: Stockholm, Sweden, 2022; Available online: https://www.ecdc.europa.eu/sites/default/files/documents/ESAC-Net_AER_2021_final-rev.pdf (accessed on 28 August 2023).
- Talaat, M.; Tolba, S.; Abdou, E.; Sarhan, M.; Gomaa, M.; Hutin, Y.J.-F. Over-Prescription and Overuse of Antimicrobials in the Eastern Mediterranean Region: The Urgent Need for Antimicrobial Stewardship Programs with Access, Watch, and Reserve Adoption. Antibiotics 2022, 11, 1773. [Google Scholar] [CrossRef] [PubMed]
- Biro, A.; Elek, P. The effect of primary care availability on antibiotic consumption in Hungary: A population based panel study using unfilled general practices. BMJ Open 2019, 9, e028233. [Google Scholar] [CrossRef] [PubMed]
- García, P.R.; Villar, F.A. Effects of economic and health policies on the consumption of antibiotics in a Spanish region. Expert Rev. Pharmacoeconomics Outcomes Res. 2019, 20, 379–386. [Google Scholar] [CrossRef]
- Rojas, P.; Antoñanzas, F. Policies to Reduce Antibiotic Consumption: The Impact in the Basque Country. Antibiotics 2020, 9, 423. [Google Scholar] [CrossRef] [PubMed]
- Nga, D.T.T.; Chuc, N.T.K.; Hoa, N.P.; Nguyen, N.T.T.; Loan, H.T.; Toan, T.K.; Phuc, H.D.; Horby, P.; Van Yen, N.; Van Kinh, N.; et al. Antibiotic sales in rural and urban pharmacies in northern Vietnam: An observational study. BMC Pharmacol. Toxicol. 2014, 15, 6. [Google Scholar] [CrossRef] [PubMed]
- Costantini, S.; Walensky, R.P. The Costs of Drugs in Infectious Diseases: Branded, Generics, and Why We Should Care. J. Infect. Dis. 2019, 221, 690–696. [Google Scholar] [CrossRef] [PubMed]
- Pulcini, C.; Beovic, B.; Béraud, G.; Carlet, J.; Cars, O.; Howard, P.; Levy-Hara, G.; Li, G.; Nathwani, D.; Roblot, F.; et al. Ensuring universal access to old antibiotics: A critical but neglected priority. Clin. Microbiol. Infect. 2017, 23, 590–592. [Google Scholar] [CrossRef] [PubMed]
- Making Medicines Affordable: A National Imperative. In National Academies of Sciences, Engineering, and Medicine, Health and Medicine Division, Board on Health Care Services, Committee on Ensuring Patient Access to Affordable Drug Therapies; Chapter 1: The Affordability Conundrum; Nass, S.J.; Madhavan, G.; Augustine, N.R. (Eds.) National Academies Press: Washington, DC, USA, 2017. [Google Scholar]
- Measuring Medicine Prices, Availability, Affordability and Price Components, 2nd ed.; World Health Organization and Health Action International: Geneva, Switzerland, 2008; Available online: https://iris.who.int/bitstream/handle/10665/70013/WHO_PSM_PAR_2008.3_eng.pdf?sequence=1 (accessed on 28 August 2023).
- Klein, E.Y.; Milkowska-Shibata, M.; Tseng, K.K.; Sharland, M.; Gandra, S.; Pulcini, C.; Laxminarayan, R. Assessment of WHO antibiotic consumption and access targets in 76 countries, 2000–15: An analysis of pharmaceutical sales data. Lancet Infect. Dis. 2020, 21, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Versporten, A.; Zarb, P.; Caniaux, I.; Gros, M.-F.; Drapier, N.; Miller, M.; Jarlier, V.; Nathwani, D.; Goossens, H.; Koraqi, A.; et al. Antimicrobial consumption and resistance in adult hospital inpatients in 53 countries: Results of an internet-based global point prevalence survey. Lancet Glob. 2018, 6, e619–e629. [Google Scholar] [CrossRef] [PubMed]
- Abu-Ajaleh, S.; Elhajji, F.D.; Al-Bsoul, S.; Abu Farha, R.; Al-Hammouri, F.; Amer, A.; Al Rusasi, A.; Al-Azzam, S.; Araydah, M.; Aldeyab, M.A. An Evaluation of the Impact of Increasing the Awareness of the WHO Access, Watch, and Reserve (AWaRe) Antibiotics Classification on Knowledge, Attitudes, and Hospital Antibiotic Prescribing Practices. Antibiotics 2023, 12, 951. [Google Scholar] [CrossRef] [PubMed]
- Al-Azzam, S.; Mhaidat, N.M.; Banat, H.A.; Alfaour, M.; Ahmad, D.S.; Muller, A.; Al-Nuseirat, A.; Lattyak, E.A.; Conway, B.R.; Aldeyab, M.A. An Assessment of the Impact of Coronavirus Disease (COVID-19) Pandemic on National Antimicrobial Consumption in Jordan. Antibiotics 2021, 10, 690. [Google Scholar] [CrossRef] [PubMed]
- Elhajji, F.D.; Al-Taani, G.M.; Anani, L.; Al-Masri, S.; Abdalaziz, H.; Qabba’h, S.H.; Al Bawab, A.Q.; Scott, M.; Farren, D.; Gilmore, F.; et al. Comparative point prevalence survey of antimicrobial consumption between a hospital in Northern Ireland and a hospital in Jordan. BMC Heal. Serv. Res. 2018, 18, 849. [Google Scholar] [CrossRef] [PubMed]
- Abu Hammour, K.; Al-Heyari, E.; Allan, A.; Versporten, A.; Goossens, H.; Abu Hammour, G.; Manaseer, Q. Antimicrobial Consumption and Resistance in a Tertiary Care Hospital in Jordan: Results of an Internet-Based Global Point Prevalence Survey. Antibiotics 2020, 9, 598. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. World Health Organization Model List of Essential Medicines—23rd List, 2023. In Proceedings of the Selection and Use of Essential Medicines 2023: Executive Summary of the Report of the 24th WHO Expert Committee on the Selection and Use of Essential Medicines, Geneva, Switzerland, 24–28 April 2023; Available online: https://www.who.int/publications/i/item/WHO-MHP-HPS-EML-2023.02 (accessed on 29 August 2023).
- WHO Collaborating Centre for Drug Statistics Methodology and Norwegian Institute of Public Health. ATC/DDD Index 2023. Oslo. 2023. Available online: https://www.whocc.no/atc_ddd_index/ (accessed on 22 March 2022).
- Jordan Food and Drug Administration. Drug information, Prices, and Leaflets. Available online: http://www.jfda.jo/Pages/viewpage.aspx?pageID=184 (accessed on 27 August 2023).
- WHO Collaborating Centre for Drug Statistics Methodology and Norwegian Institute of Public Health. DDD Definition and General Considerations. Oslo. 2023. Available online: https://www.whocc.no/ddd/definition_and_general_considera/ (accessed on 8 May 2020).
- Gauthaman, J.; Jayanthi, M. Wide Cost Variations Observed in Antibiotics and Analgesics Prescribed for Dental Care in India: A Price and Affordability Analysis. Cureus 2022, 14, e21755. [Google Scholar] [CrossRef] [PubMed]
- Jordanian Ministry of Labor. The Tertiary Labor Committee Keeps the Minimum Wage Limit. February 2023. Available online: https://mol.gov.jo/ar/NewsDetails/%d8%a7%d9%84%d9%84%d8%ac%d9%86%d8%a9_%d8%a7%d9%84%d8%ab%d9%84%d8%a7%d8%ab%d9%8a%d8%a9_%d9%84%d8%b4%d8%a4%d9%88%d9%86_%d8%a7%d9%84%d8%b9%d9%85%d9%84_%d8%aa%d8%a8%d9%82%d9%8a_%d8%b9%d9%84%d9%89_%d8%a7%d9%84%d8%ad%d8%af_%d8%a7%d9%84%d8%a3%d8%af%d9%86%d9%89_%d9%84%d9%84%d8%a3%d8%ac%d9%88%d8%b1 (accessed on 30 August 2023).
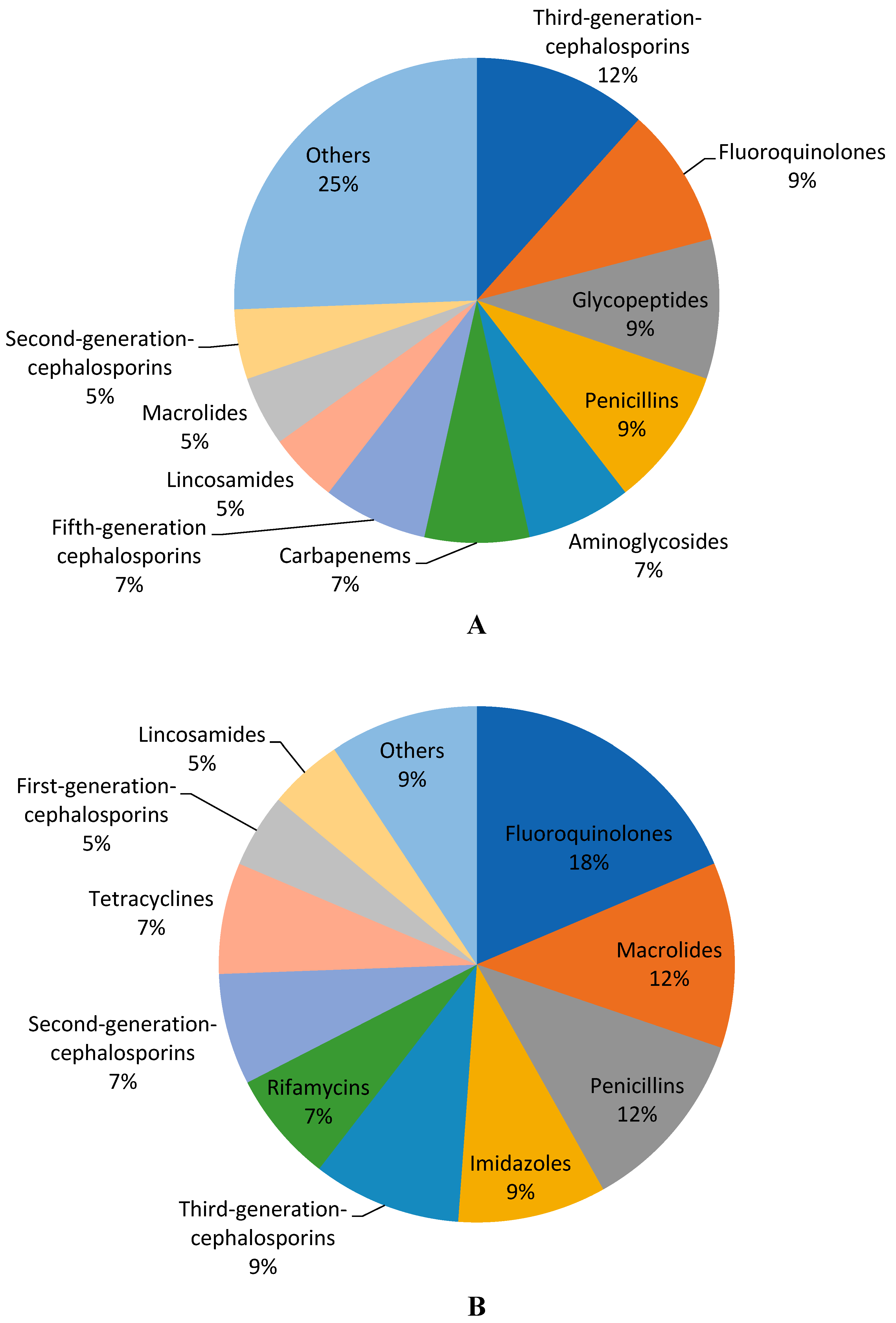
| WHO AWaRe Category | Antibiotic | ATC Code | Listed on EML | DDD (g) | Mean Cost (JOD/DDD) | Number of MAH |
|---|---|---|---|---|---|---|
| Access | Amikacin | J01GB06 | Yes | 1 | 7.66 | 4 |
| Amoxicillin/clavulanic acid | J01CR02 | Yes | 3 | 4.45 | 3 | |
| Ampicillin | J01CA01 | Yes | 6 | 3.9 | 2 | |
| Benzathine-benzylpenicillin | J01CE08 | Yes | 3.6 | 4.67 | 1 | |
| Cefazolin | J01DB04 | Yes | 3 | 5.76 | 2 | |
| Clindamycin | J01FF01 | Yes | 1.8 | 14.89 | 3 | |
| Cloxacillin | J01CF02 | Yes | 2 | 4.65 | 1 | |
| Gentamicin | J01GB03 | Yes | 0.24 | 2.2 | 3 | |
| Metronidazole | J01XD01 | Yes | 1.5 | 4.75 | 8 | |
| Procaine-benzylpenicillin | J01CE09 | Yes | 0.6 | 2.54 | 1 | |
| Spectinomycin | J01XX04 | Yes | 3 | 5.93 | 1 | |
| Sulfamethoxazole/trimethoprim | J01EE01 | Yes | 2 | 7.24 | 1 | |
| Watch | Azithromycin | J01FA10 | No | 0.5 | 8.03 | 3 |
| Cefepime | J01DE01 | No | 4 | 20.74 | 3 | |
| Cefotaxime | J01DD01 | Yes | 4 | 21.15 | 3 | |
| Cefoxitin | J01DC01 | No | 6 | 35.76 | 1 | |
| Ceftazidime | J01DD02 | Yes | 4 | 11.59 | 6 | |
| Ceftizoxime | J01DD07 | No | 4 | 33.58 | 2 | |
| Ceftriaxone | J01DD04 | Yes | 2 | 11.31 | 11 | |
| Cefuroxime | J01DC02 | Yes | 3 | 5.92 | 7 | |
| Ciprofloxacin | J01MA02 | Yes | 0.8 | 30.61 | 7 | |
| Clarithromycin | J01FA09 | Yes | 1 | 27.1 | 1 | |
| Delafloxacin | J01MA23 | No | 0.6 | 111.28 | 1 | |
| Ertapenem | J01DH03 | No | 1 | 24.18 | 2 | |
| Imipenem/cilastatin | J01DH51 | Yes | 2 | 31.91 | 5 | |
| Levofloxacin | J01MA12 | No | 0.5 | 13.94 | 6 | |
| Lincomycin | J01FF02 | No | 1.8 | 5.34 | 5 | |
| Meropenem | J01DH02 | Yes | 3 | 31.33 | 5 | |
| Moxifloxacin | J01MA14 | No | 0.4 | 16.15 | 3 | |
| Piperacillin/tazobactam | J01CR05 | Yes | 14 | 30.75 | 4 | |
| Teicoplanin | J01XA02 | No | 0.4 | 7.73 | 5 | |
| Tobramycin | J01GB01 | No | 0.24 | 12.69 | 1 | |
| Vancomycin | J01XA01 | Yes | 2 | 18.74 | 9 | |
| Reserve | Ceftaroline-fosamil | J01DI02 | No | 1.2 | 72.47 | 1 |
| Ceftazidime/avibactam | J01DD52 | Yes | 6 | 268.38 | 1 | |
| Ceftobiprole-medocaril | J01DI01 | No | 1.5 | 133.9 | 1 | |
| Ceftolozane/tazobactam | J01DI54 | Yes | 3 | 221.96 | 1 | |
| Colistin | J01XB01 | Yes | 9 | 63.03 | 1 | |
| Daptomycin | J01XX09 | No | 0.28 | 49.06 | 1 | |
| Linezolid | J01XX08 | Yes | 1.2 | 64.45 | 1 | |
| Oritavancin | J01XA05 | No | 1.2 | 609.93 | 1 | |
| Telavancin | J01XA03 | No | 0.75 | 93.6 | 1 | |
| Tigecycline | J01AA12 | No | 0.1 | 60.58 | 2 |
| WHO AWaRe Category | Antibiotic | ATC Code | Listed on EML 2023 | DDD (g) | Mean Cost (JOD/DDD) | Number of MAH |
|---|---|---|---|---|---|---|
| Access | Amoxicillin | J01CA04 | Yes | 1.5 | 0.46 | 12 |
| Amoxicillin/clavulanic acid | J01CR02 | Yes | 1.5 | 0.83 | 10 | |
| Ampicillin | J01CA01 | No | 2 | 0.46 | 4 | |
| Cefadroxil | J01DB05 | No | 2 | 1.37 | 6 | |
| Cefalexin | J01DB01 | Yes | 2 | 0.78 | 9 | |
| Clindamycin | J01FF01 | Yes | 1.2 | 1.66 | 5 | |
| Cloxacillin | J01CF02 | Yes | 2 | 0.78 | 2 | |
| Doxycycline | J01AA02 | Yes | 0.1 | 0.24 | 8 | |
| Flucloxacillin | J01CF05 | Yes | 2 | 0.83 | 1 | |
| Metronidazole | P01AB01 | Yes | 2 | 0.34 | 7 | |
| Ornidazole | P01AB03 | No | 1.5 | 1.76 | 2 | |
| Phenoxymethylpenicillin | J01CE02 | Yes | 2 | 0.39 | 1 | |
| Secnidazole | P01AB07 | No | 2 | 3.38 | 1 | |
| Sulfamethoxazole/trimethoprim | J01EE01 | Yes | 2 | 0.37 | 3 | |
| Tetracycline | J01AA07 | No | 1 | 0.24 | 1 | |
| Tinidazole | P01AB02 | No | 2 | 2.28 | 3 | |
| Watch | Azithromycin | J01FA10 | Yes | 0.3 | 0.72 | 16 |
| Cefaclor | J01DC04 | No | 1 | 1.19 | 8 | |
| Cefdinir | J01DD15 | No | 0.6 | 3.72 | 4 | |
| Cefditoren-pivoxil | J01DD16 | No | 0.4 | 1.97 | 1 | |
| Cefixime | J01DD08 | Yes | 0.4 | 2.41 | 10 | |
| Cefpodoxime-proxetil | J01DD13 | No | 0.4 | 2.9 | 5 | |
| Cefprozil | J01DC10 | No | 1 | 3.25 | 2 | |
| Cefuroxime | J01DC02 | No | 0.5 | 0.59 | 10 | |
| Ciprofloxacin | J01MA02 | Yes | 1 | 1.15 | 17 | |
| Clarithromycin | J01FA09 | Yes | 0.5 | 0.87 | 11 | |
| Delafloxacin | J01MA23 | No | 0.9 | 66.66 | 1 | |
| Erythromycin | J01FA01 | No | 2 | 0.58 | 2 | |
| Levofloxacin | J01MA12 | Yes | 0.5 | 1.46 | 14 | |
| Lincomycin | J01FF02 | No | 1.8 | 0.85 | 1 | |
| Lomefloxacin | J01MA07 | No | 0.4 | 1.29 | 1 | |
| Moxifloxacin | J01MA14 | Yes | 0.4 | 1.77 | 8 | |
| Norfloxacin | J01MA06 | No | 0.8 | 0.58 | 4 | |
| Ofloxacin | J01MA01 | No | 0.4 | 1.54 | 1 | |
| Pefloxacin | J01MA03 | No | 0.8 | 1.09 | 2 | |
| Rifabutin | J04AB04 | Yes | 0.15 | 2.91 | 1 | |
| Rifampicin | J04AB02 | Yes | 0.6 | 0.43 | 2 | |
| Rifaximin | A07AA11 | No | 0.6 | 1.57 | 1 | |
| Roxithromycin | J01FA06 | No | 0.3 | 0.76 | 5 | |
| Spiramycin | J01FA02 | No | 3 | 0.66 | 3 | |
| Fosfomycin | J01XX01 | No | 3 | 4.48 | 2 | |
| Minocycline | J01AA08 | No | 0.2 | 0.85 | 1 | |
| Reserve | Linezolid | J01XX08 | Yes | 1.2 | 45.98 | 4 |
| WHO AWaRe Category | Antibiotic | Cost Range (JOD/DDD) | Cost Ratio | % Cost Variation | Affordable |
|---|---|---|---|---|---|
| Access | Amikacin | 6.15–8.83 | 1.44 | 43.6 | Yes |
| Amoxicillin/clavulanic acid | 3.27–5.58 | 1.71 | 70.6 | Yes | |
| Ampicillin | 2.99–4.91 | 1.64 | 64.2 | Yes | |
| Benzathine-benzylpenicillin | 4.67 | 1.00 | 0.0 | Yes | |
| Cefazolin | 4.70–6.48 | 1.38 | 37.9 | Yes | |
| Clindamycin | 6.09–19.20 | 3.15 | 215.3 | Yes | |
| Cloxacillin | 4.03–5.27 | 1.31 | 30.8 | Yes | |
| Gentamicin | 1.11–3.78 | 3.41 | 240.5 | Yes | |
| Metronidazole | 3.26–9.14 | 2.80 | 180.4 | Yes | |
| Procaine-benzylpenicillin | 2.54 | 1.00 | 0.0 | Yes | |
| Spectinomycin | 5.93 | 1.00 | 0.0 | Yes | |
| Sulfamethoxazole/trimethoprim | 7.24 | 1.00 | 0.0 | Yes | |
| Watch | Azithromycin | 5.24–10.62 | 2.03 | 102.7 | Yes |
| Cefepime | 14.64–25.40 | 1.73 | 73.5 | No | |
| Cefotaxime | 11.92–24.24 | 2.03 | 103.4 | No | |
| Cefoxitin | 35.76 | 1.00 | 0.0 | No | |
| Ceftazidime | 6.88–18.56 | 2.70 | 169.8 | Yes | |
| Ceftizoxime | 22.90–37.44 | 1.63 | 63.5 | No | |
| Ceftriaxone | 2.98–20.20 | 6.78 | 577.9 | Yes | |
| Cefuroxime | 3.39–10.12 | 2.99 | 198.5 | Yes | |
| Ciprofloxacin | 11.96–56.34 | 4.71 | 371.1 | No | |
| Clarithromycin | 27.10 | 1.00 | 0.0 | No | |
| Delafloxacin | 111.28 | 1.00 | 0.0 | No | |
| Ertapenem | 18.69–29.66 | 1.59 | 58.7 | No | |
| Imipenem/cilastatin | 25.00–39.68 | 1.59 | 58.7 | No | |
| Levofloxacin | 7.30–22.94 | 3.14 | 214.2 | Yes | |
| Lincomycin | 4.68–6.66 | 1.42 | 42.3 | Yes | |
| Meropenem | 16.69–57.11 | 3.42 | 242.2 | No | |
| Moxifloxacin | 7.20–22.19 | 3.08 | 208.2 | Yes | |
| Piperacillin/tazobactam | 25.13–36.69 | 1.46 | 46.0 | No | |
| Teicoplanin | 3.69–12.40 | 3.36 | 236.0 | Yes | |
| Tobramycin | 12.69 | 1.00 | 0.0 | No | |
| Vancomycin | 8.01–29.28 | 3.66 | 265.5 | Yes | |
| Reserve | Ceftaroline-fosamil | 72.47 | 1.00 | 0.0 | No |
| Ceftazidime/avibactam | 268.38 | 1.00 | 0.0 | No | |
| Ceftobiprole-medocaril | 133.90 | 1.00 | 0.0 | No | |
| Ceftolozane/tazobactam | 221.96 | 1.00 | 0.0 | No | |
| Colistin | 59.72–66.33 | 1.11 | 11.1 | No | |
| Daptomycin | 49.06 | 1.00 | 0.0 | No | |
| Linezolid | 61.06–67.84 | 1.11 | 11.1 | No | |
| Oritavancin | 609.93 | 1.00 | 0.0 | No | |
| Telavancin | 93.60 | 1.00 | 0.0 | No | |
| Tigecycline | 51.66–69.50 | 1.35 | 34.5 | No |
| WHO AWaRe Category | Antibiotic | Cost Range (JOD/DDD) | Cost Ratio | % Cost Variation | Affordable |
|---|---|---|---|---|---|
| Access | Amoxicillin | 0.13–0.77 | 5.92 | 492.3 | Yes |
| Amoxicillin/clavulanic acid | 0.61–1.29 | 2.11 | 111.5 | Yes | |
| Ampicillin | 0.30–0.79 | 2.63 | 163.3 | Yes | |
| Cefadroxil | 0.85–2.48 | 2.92 | 191.8 | Yes | |
| Cefalexin | 0.29–1.22 | 4.21 | 320.7 | Yes | |
| Clindamycin | 1.38–2.00 | 1.45 | 44.9 | Yes | |
| Cloxacillin | 0.67–0.83 | 1.24 | 23.9 | Yes | |
| Doxycycline | 0.17–0.35 | 2.06 | 105.9 | Yes | |
| Flucloxacillin | 0.83 | 1.00 | 0.0 | Yes | |
| Metronidazole | 0.19–0.69 | 3.63 | 263.2 | Yes | |
| Ornidazole | 1.56–1.95 | 1.25 | 25.0 | Yes | |
| Phenoxymethylpenicillin | 0.39 | 1.00 | 0.0 | Yes | |
| Secnidazole | 3.01–3.75 | 1.25 | 24.6 | Yes | |
| Sulfamethoxazole/trimethoprim | 0.21–0.63 | 3.00 | 200.0 | Yes | |
| Tetracycline | 0.21–0.26 | 1.24 | 23.8 | Yes | |
| Tinidazole | 2.09–2.78 | 1.33 | 33.0 | Yes | |
| Watch | Azithromycin | 0.47–0.90 | 1.91 | 91.5 | Yes |
| Cefaclor | 0.78–1.43 | 1.83 | 83.3 | Yes | |
| Cefdinir | 3.40–4.47 | 1.31 | 31.5 | Yes | |
| Cefditoren-pivoxil | 1.97 | 1.00 | 0.0 | Yes | |
| Cefixime | 1.19–3.12 | 2.62 | 162.2 | Yes | |
| Cefpodoxime-proxetil | 2.30–3.83 | 1.67 | 66.5 | Yes | |
| Cefprozil | 3.00–3.66 | 1.22 | 22.0 | Yes | |
| Cefuroxime | 0.38–0.78 | 2.05 | 105.3 | Yes | |
| Ciprofloxacin | 0.45–2.38 | 5.29 | 428.9 | Yes | |
| Clarithromycin | 0.55–1.32 | 2.40 | 140.0 | Yes | |
| Delafloxacin | 66.66 | 1.00 | 0.0 | No | |
| Erythromycin | 0.31–0.80 | 2.58 | 158.1 | Yes | |
| Levofloxacin | 0.62–1.81 | 2.92 | 191.9 | Yes | |
| Lincomycin | 0.75–0.94 | 1.25 | 25.3 | Yes | |
| Lomefloxacin | 1.14 | 1.26 | 26.3 | Yes | |
| Moxifloxacin | 1.01–2.17 | 2.15 | 114.9 | Yes | |
| Norfloxacin | 0.50–0.73 | 1.46 | 46.0 | Yes | |
| Ofloxacin | 1.41–1.66 | 1.18 | 17.7 | Yes | |
| Pefloxacin | 1.03–1.13 | 1.10 | 9.7 | Yes | |
| Rifabutin | 2.91 | 1.00 | 0.0 | Yes | |
| Rifampicin | 0.41–0.47 | 1.15 | 14.6 | Yes | |
| Rifaximin | 1.57 | 1.00 | 0.0 | Yes | |
| Roxithromycin | 0.67–0.83 | 1.24 | 23.9 | Yes | |
| Spiramycin | 0.380.96 | 2.53 | 152.6 | Yes | |
| Fosfomycin | 3.78–5.17 | 1.37 | 36.8 | Yes | |
| Minocycline | 0.73–0.96 | 1.32 | 31.5 | Yes | |
| Reserve | Linezolid | 29.70–82.50 | 2.78 | 177.8 | No |
| Access | Watch | Reserve | Sig. (ρ) | |
|---|---|---|---|---|
| N | 28 | 47 | 11 | |
| Mean JOD/DDD (S.E.) | 3.03 (0.61) | 13.11 (2.94) | 153.03 (50.81) | <0.001 * |
| Mean MAHs (S.E.) | 3.75 (0.60) | 4.74 (0.60) | 1.36 (0.28) | 0.003 * |
| Affordable (%) | 28 (100.0%) | 34 (72.3%) | 0 (0.0%) | <0.001 ** |
| Affordable | Non-Affordable | Sig. (ρ) | |
|---|---|---|---|
| N | 62 | 24 | |
| Mean MAH (S.E.) | 4.69 (0.50) | 1.95 (0.30) | 0.001 * |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Darwish Elhajji, F.; Abuhasheesh, S.; Al Rusasi, A.; Aldeyab, M.A. Overview of Availability, Cost, and Affordability of Antibiotics for Adults in Jordan: An AWaRe Classification Perspective. Antibiotics 2023, 12, 1576. https://doi.org/10.3390/antibiotics12111576
Darwish Elhajji F, Abuhasheesh S, Al Rusasi A, Aldeyab MA. Overview of Availability, Cost, and Affordability of Antibiotics for Adults in Jordan: An AWaRe Classification Perspective. Antibiotics. 2023; 12(11):1576. https://doi.org/10.3390/antibiotics12111576
Chicago/Turabian StyleDarwish Elhajji, Feras, Sahar Abuhasheesh, Ahmed Al Rusasi, and Mamoon A. Aldeyab. 2023. "Overview of Availability, Cost, and Affordability of Antibiotics for Adults in Jordan: An AWaRe Classification Perspective" Antibiotics 12, no. 11: 1576. https://doi.org/10.3390/antibiotics12111576
APA StyleDarwish Elhajji, F., Abuhasheesh, S., Al Rusasi, A., & Aldeyab, M. A. (2023). Overview of Availability, Cost, and Affordability of Antibiotics for Adults in Jordan: An AWaRe Classification Perspective. Antibiotics, 12(11), 1576. https://doi.org/10.3390/antibiotics12111576






