Pet Owners and Antibiotics: Knowledge, Opinions, Expectations, and Communication Preferences
Abstract
:1. Introduction
2. Results
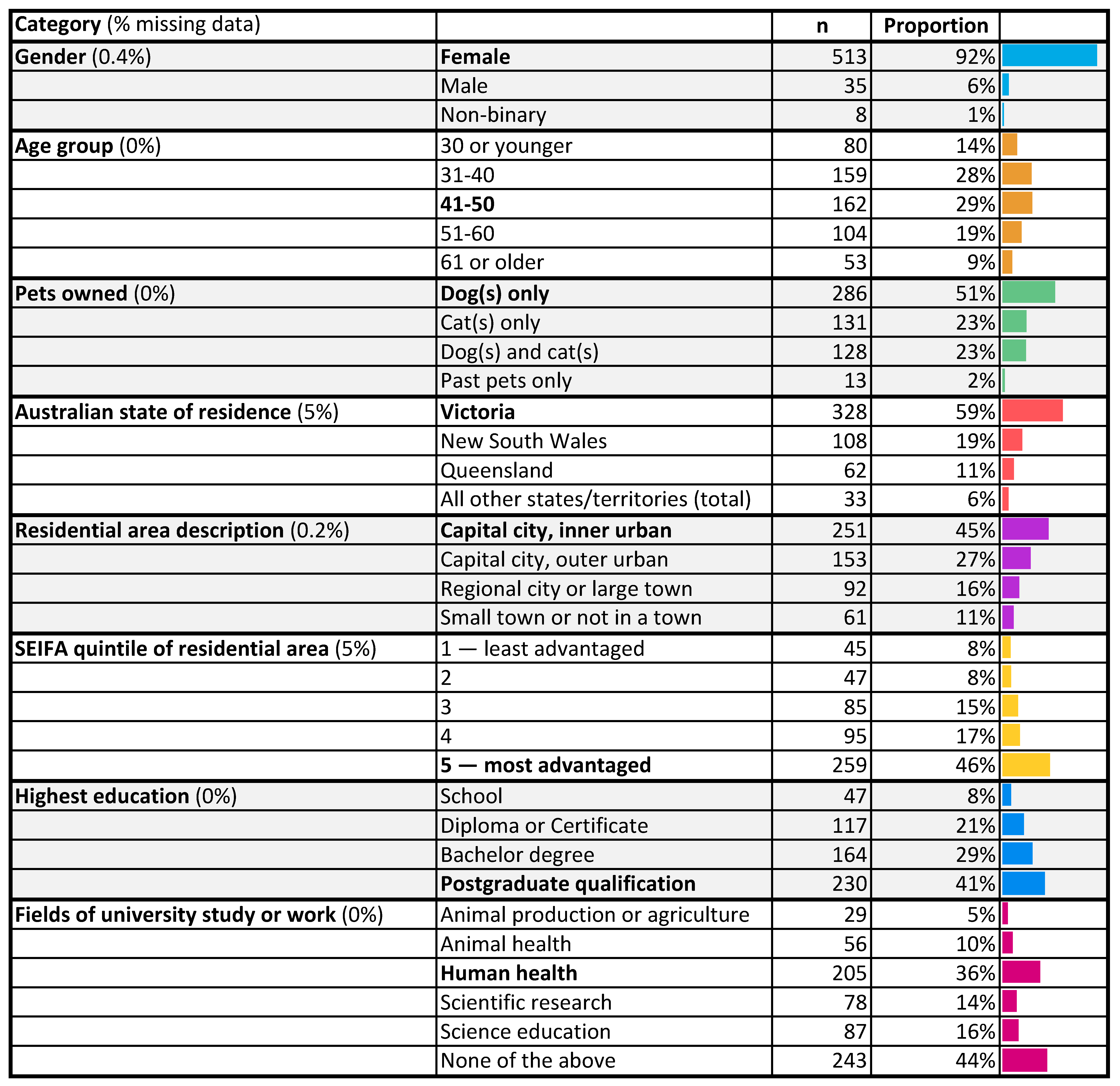
2.1. Respondents
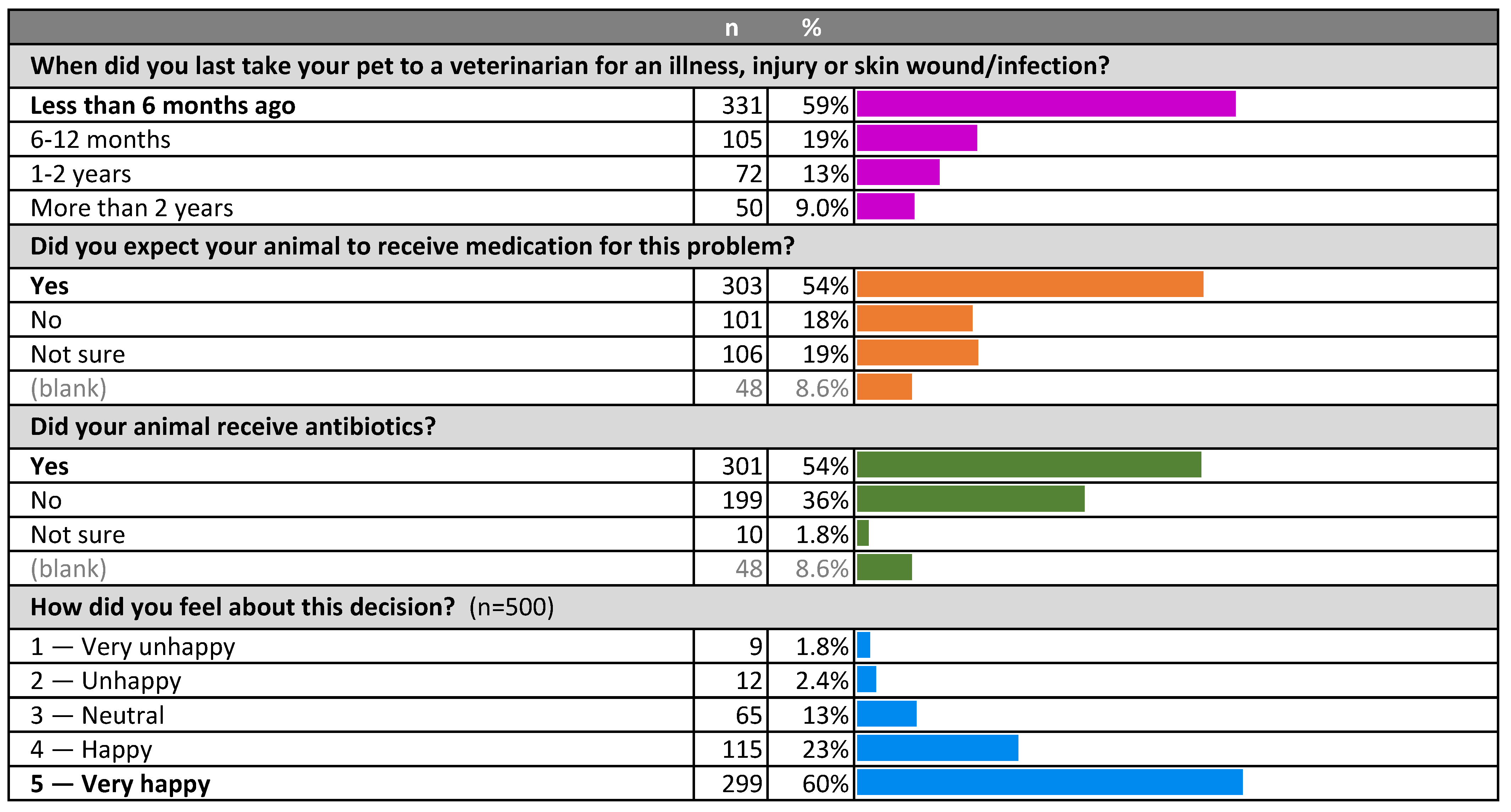
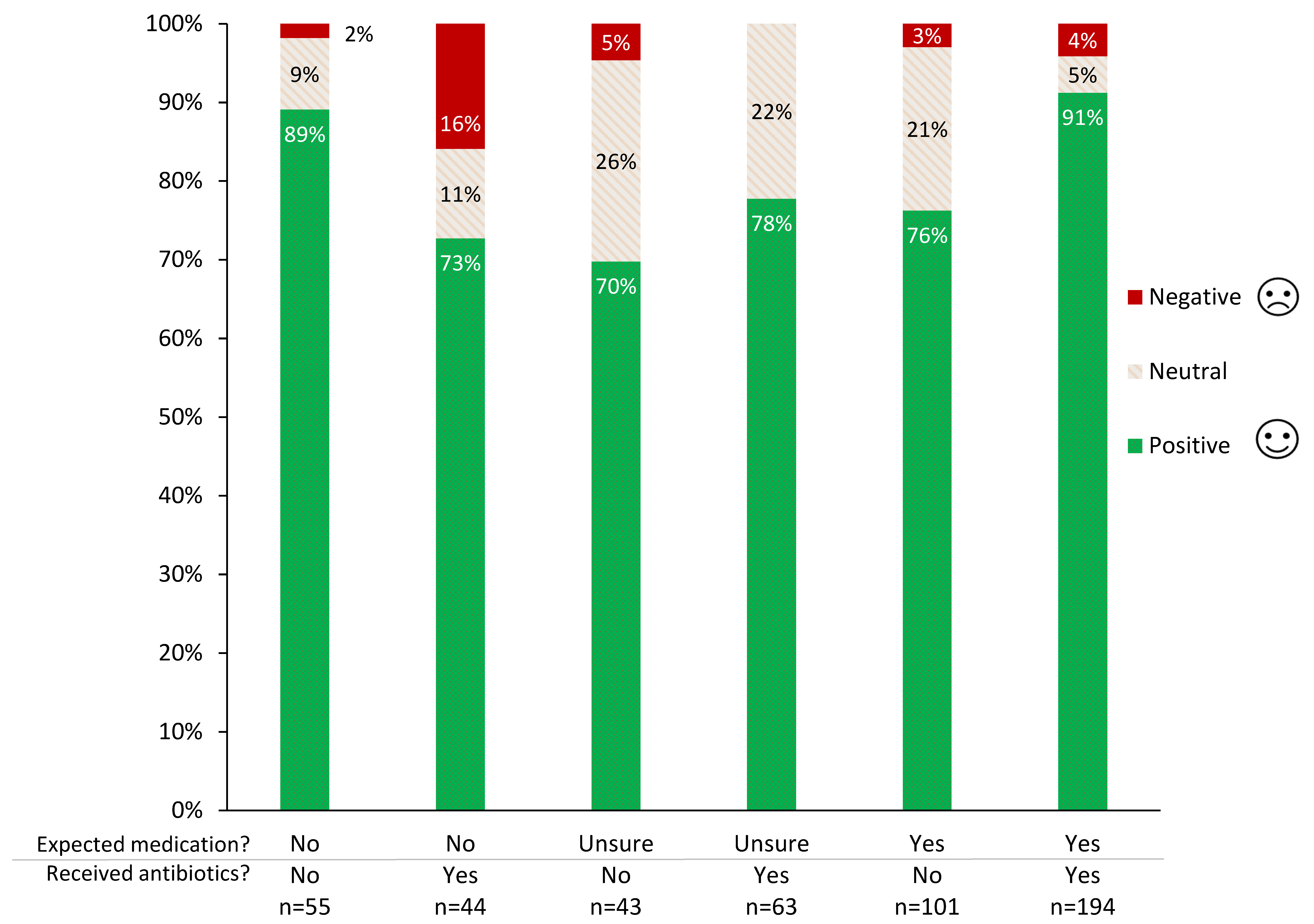
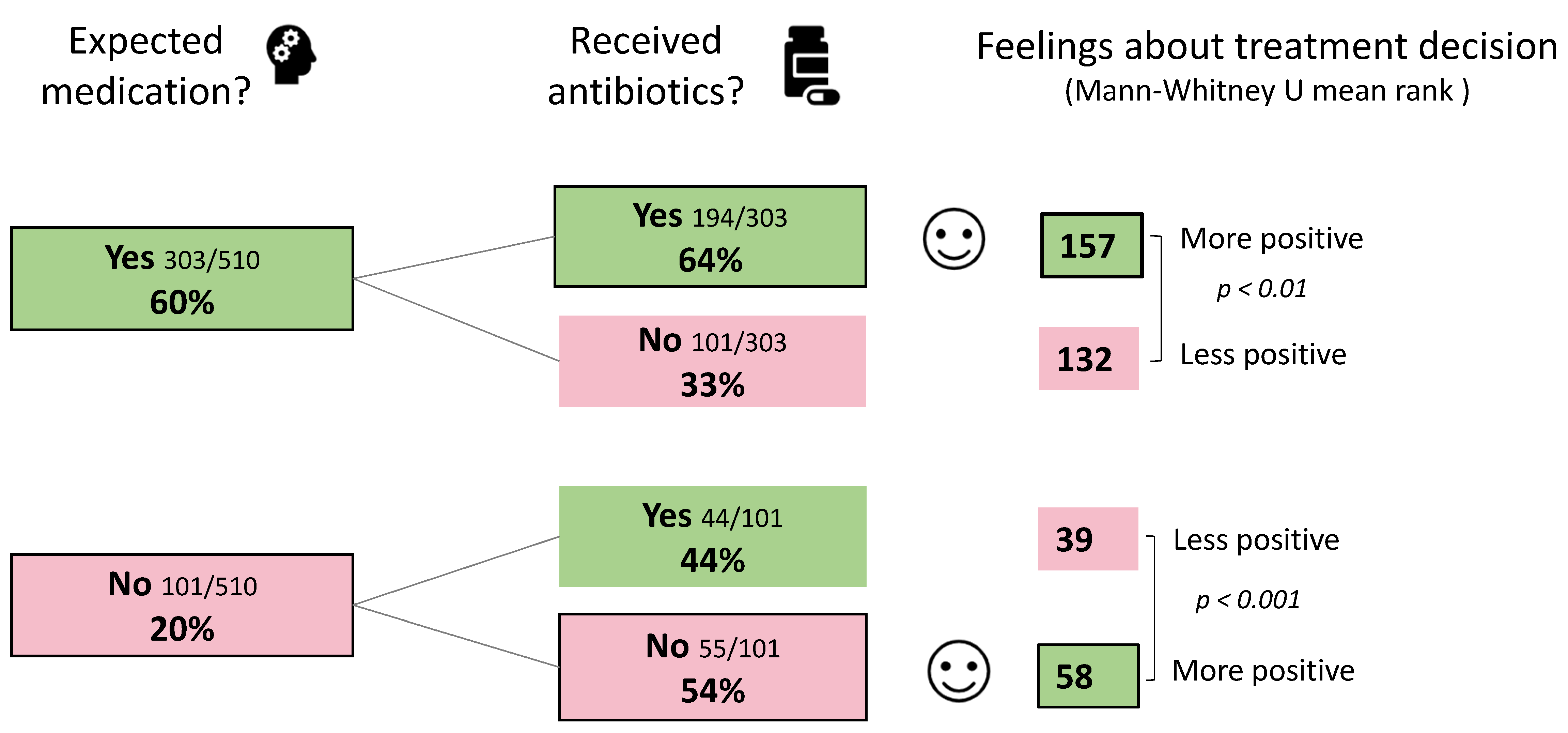
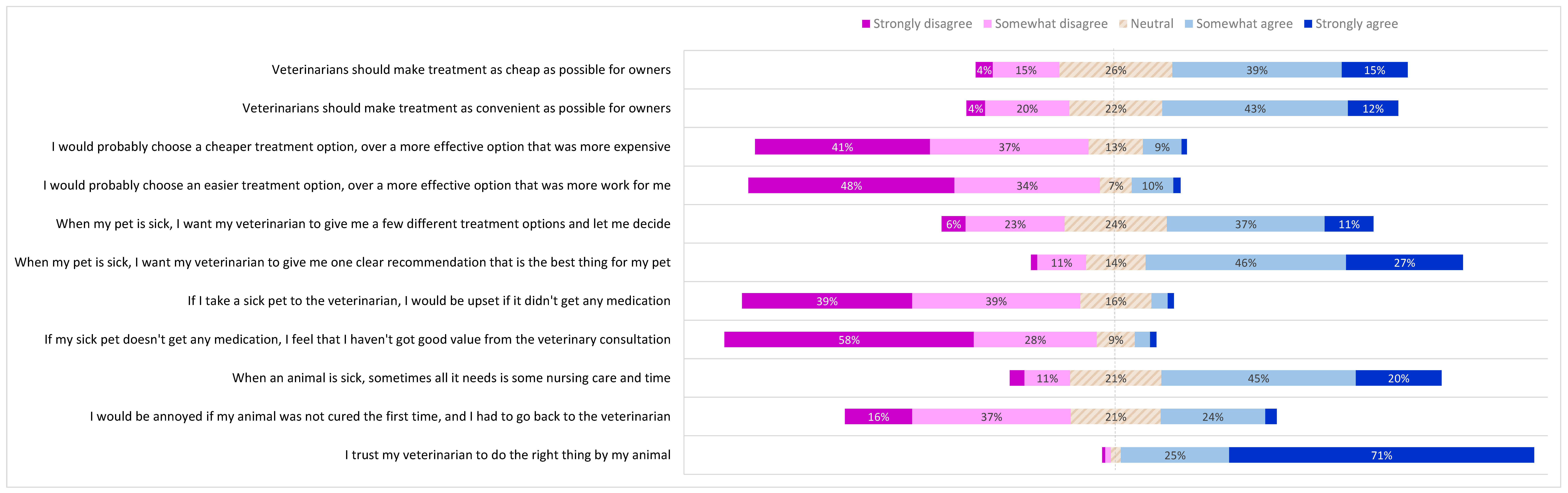
2.2. Pet Owner Expectations of the Veterinary Consultation, Treatment Preferences and Trust
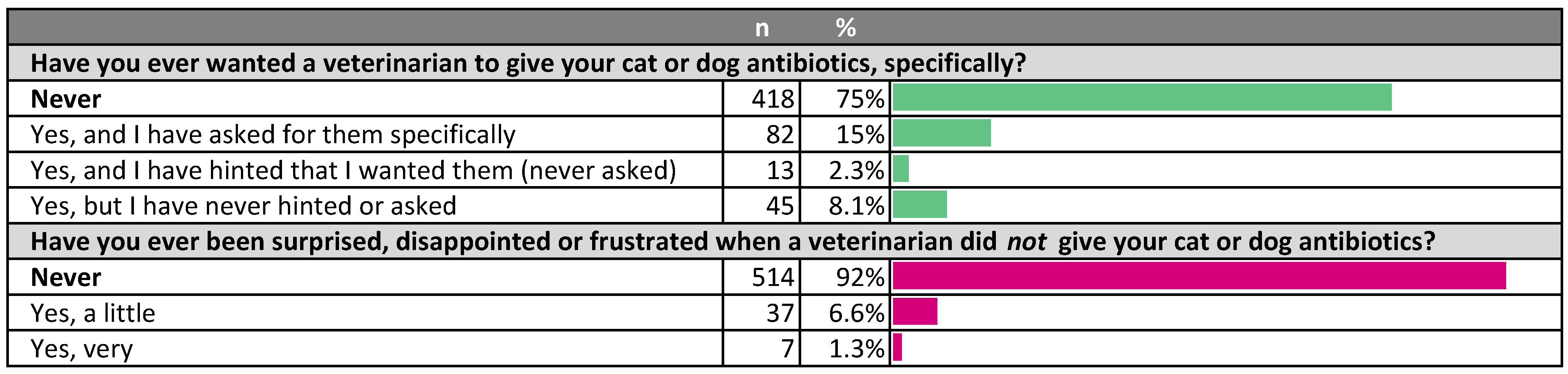
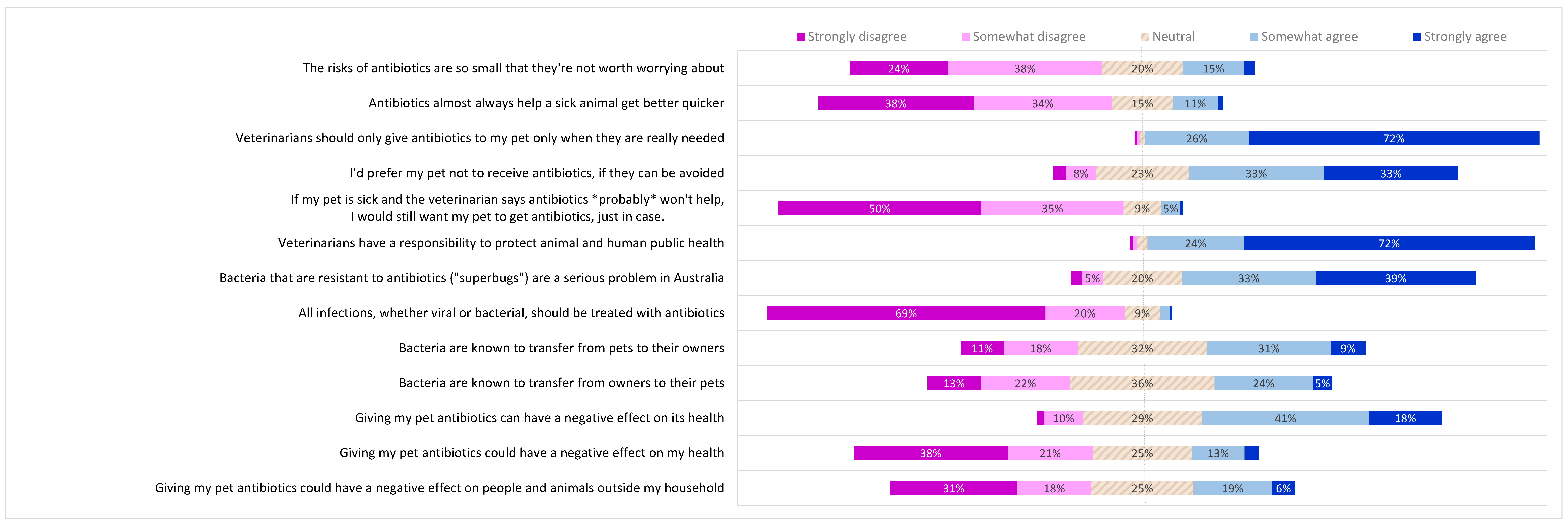
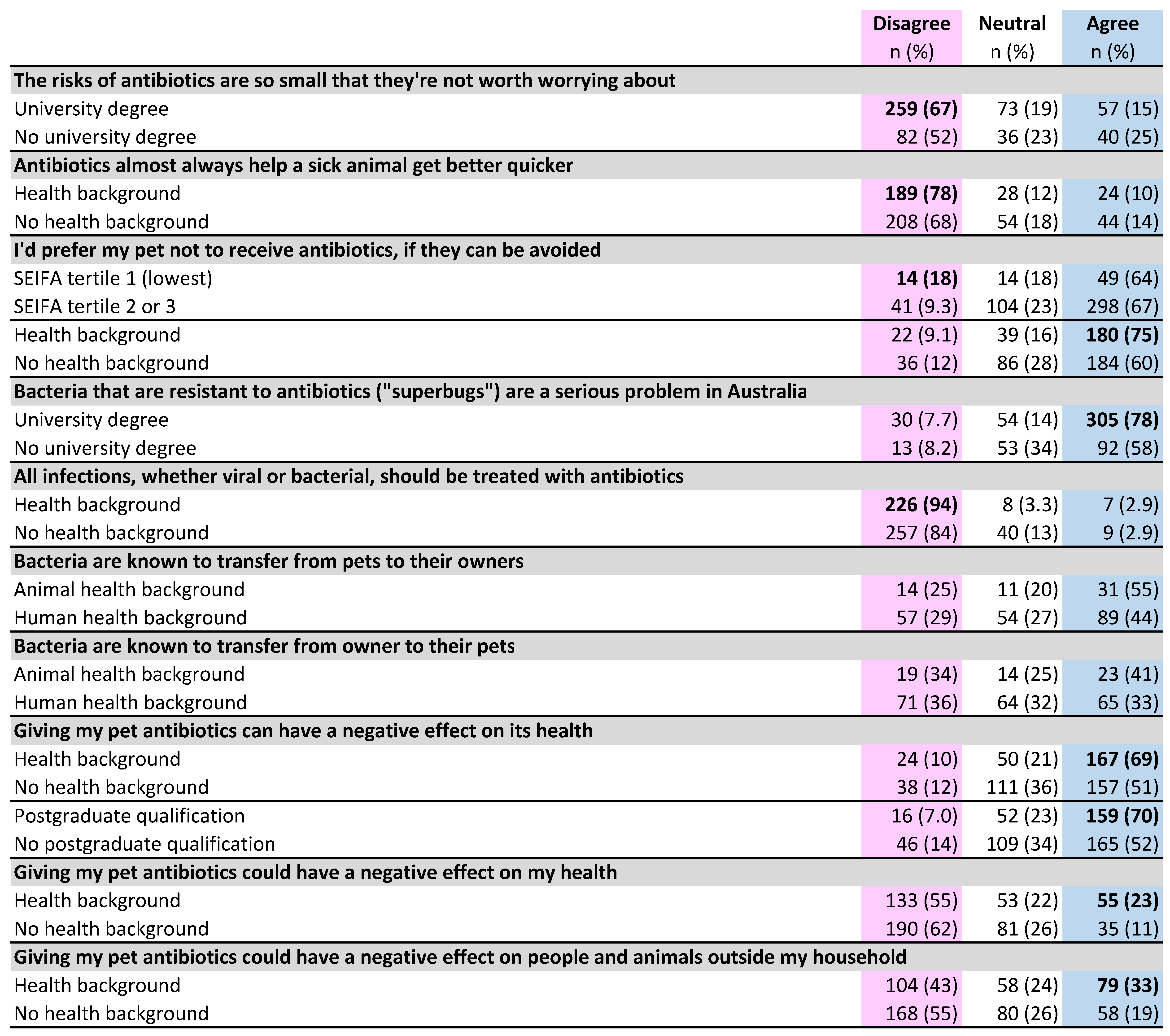
2.3. Pet Owner Opinions on Antibiotic Use; Knowledge of Microbiology and Antibiotic Resistance
2.4. Communication Preferences
2.4.1. Communication Preferences When Not Prescribing Antibiotics, and Delayed Prescribing Preferences
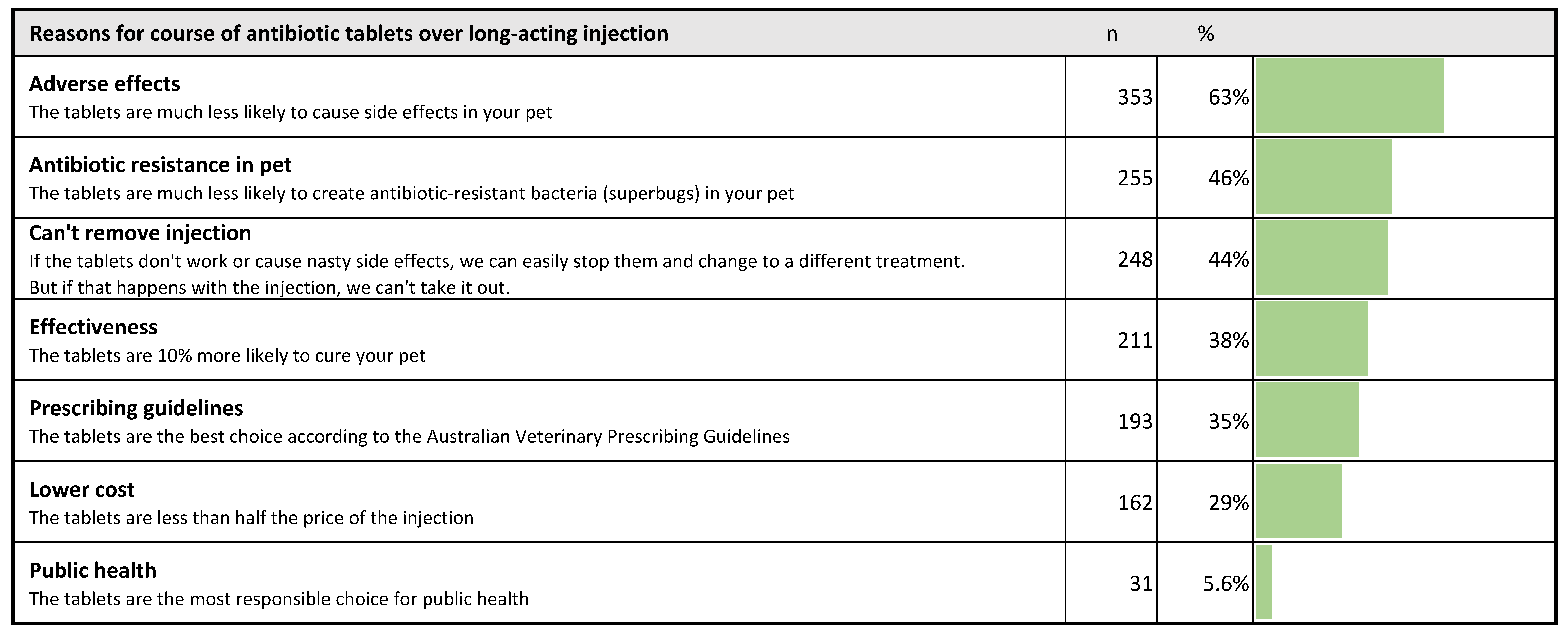
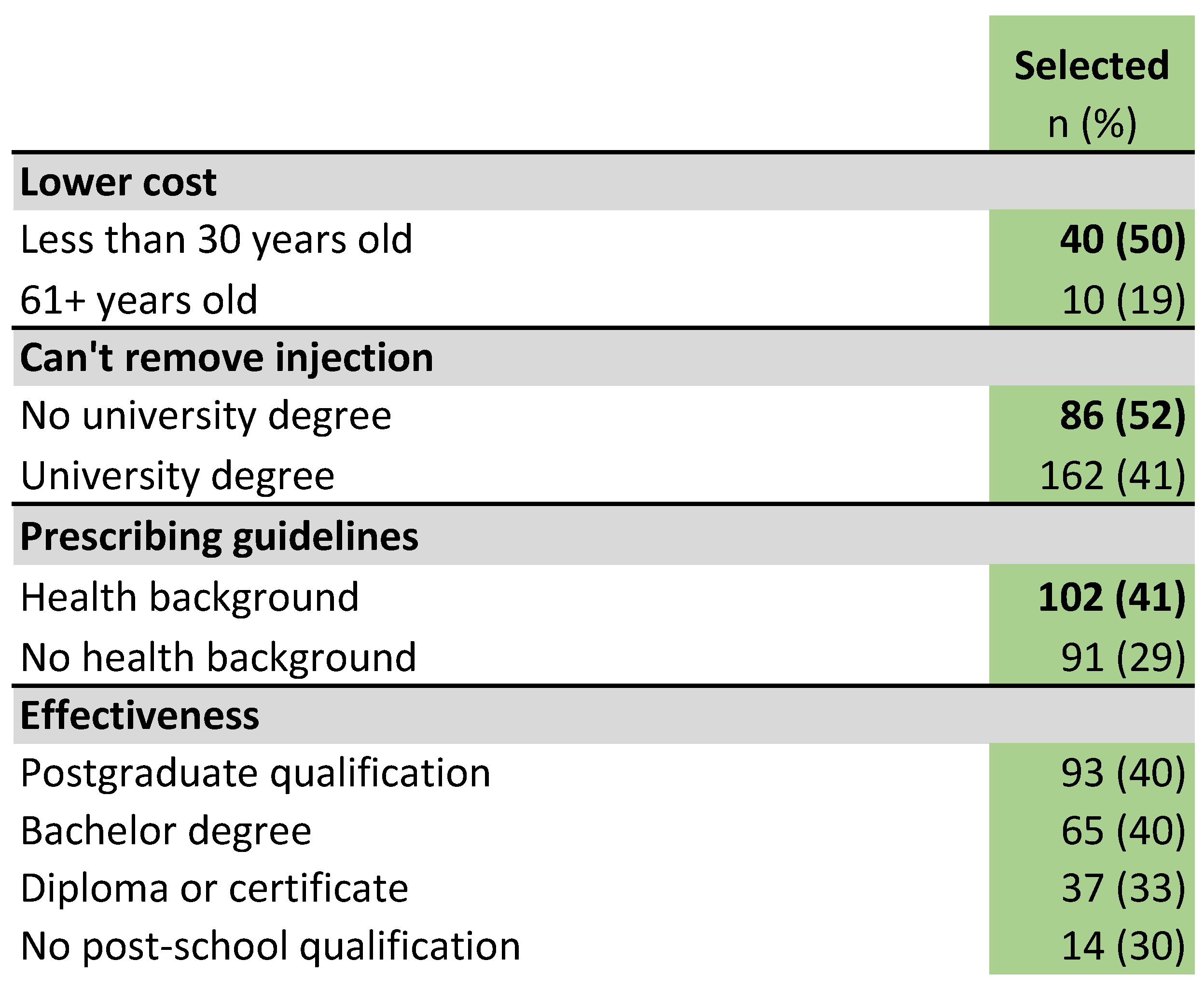
2.4.2. Reasons to Give a Course of Antibiotic Tablets, Rather Than a Single, Long-Acting Injection
3. Discussion
3.1. Pet Owner Expectations of the Veterinary Consultation, Treatment Preferences and Trust
3.2. Pet Owner Opinions on Antibiotic Use; Knowledge of Microbiology and Antibiotic Resistance
3.3. Communication Preferences
3.4. Strengths and Limitations
4. Materials and Methods
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Animal Medicines Australia. Pets in Australia: A National Survey of Pets and People. 2019. Available online: https://animalmedicinesaustralia.org.au/report/pets-in-australia-a-national-survey-of-pets-and-people/ (accessed on 28 August 2021).
- Hardefeldt, L.Y.; Selinger, J.; Stevenson, M.A.; Gilkerson, J.R.; Crabb, H.; Billman-Jacobe, H.; Thursky, K.; Bailey, K.E.; Awad, M.; Browning, G.F. Population wide assessment of antimicrobial use in dogs and cats using a novel data source—A cohort study using pet insurance data. Vet. Microbiol. 2018, 225, 34–39. [Google Scholar] [CrossRef]
- Buckland, E.L.; O’Neill, D.; Summers, J.; Mateus, A.; Church, D.; Redmond, L.; Brodbelt, D. Characterisation of antimicrobial usage in cats and dogs attending UK primary care companion animal veterinary practices. Vet. Rec. 2016, 179, 489. [Google Scholar] [CrossRef] [Green Version]
- Singleton, D.A.; Sánchez-Vizcaíno, F.; Dawson, S.; Jones, P.H.; Noble, P.J.M.; Pinchbeck, G.L.; Williams, N.J.; Radford, A.D. Patterns of antimicrobial agent prescription in a sentinel population of canine and feline veterinary practices in the United Kingdom. Vet. J. 2017, 224, 18–24. [Google Scholar] [CrossRef] [Green Version]
- Schmitt, K.; Lehner, C.; Schuller, S.; Schüpbach-Regula, G.; Mevissen, M.; Peter, R.; Müntener, C.R.; Naegeli, H.; Willi, B. Antimicrobial use for selected diseases in cats in Switzerland. BMC Vet. Res. 2019, 15, 94. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Joosten, P.; Ceccarelli, D.; Odent, E.; Sarrazin, S.; Graveland, H.; van Gompel, L.; Battisti, A.; Caprioli, A.; Franco, A.; Wagenaar, J.A.; et al. Antimicrobial Usage and Resistance in Companion Animals: A Cross-Sectional Study in Three European Countries. Antibiotics 2020, 9, 87. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Galarce, N.; Arriagada, G.; Sánchez, F.; Venegas, V.; Cornejo, J.; Lapierre, L. Antimicrobial Use in Companion Animals: Assessing Veterinarians’ Prescription Patterns through the First National Survey in Chile. Animals 2021, 11, 348. [Google Scholar] [CrossRef]
- Goggs, R.; Menard, J.M.; Altier, C.; Cummings, K.J.; Jacob, M.E.; Lalonde-Paul, D.F.; Papich, M.G.; Norman, K.N.; Fajt, V.R.; Scott, H.M.; et al. Patterns of antimicrobial drug use in veterinary primary care and specialty practice: A 6-year multi-institution study. J. Vet. Intern. Med. 2021, 35, 1496–1508. [Google Scholar] [CrossRef] [PubMed]
- Hur, B.A.; Hardefeldt, L.Y.; Verspoor, K.M.; Baldwin, T.; Gilkerson, J.R. Describing the antimicrobial usage patterns of companion animal veterinary practices; free text analysis of more than 4.4 million consultation records. PLoS ONE 2020, 15, e0230049. [Google Scholar] [CrossRef] [Green Version]
- De Briyne, N.; Atkinson, J.; Pokludov, L.; Borriello, S.P.; Price, S. Factors influencing antibiotic prescribing habits and use of sensitivity testing amongst veterinarians in Europe. Vet. Rec. 2013, 173, 475. [Google Scholar] [CrossRef] [Green Version]
- Currie, K.; King, C.; Nuttall, T.; Smith, M.; Flowers, P. Expert consensus regarding drivers of antimicrobial stewardship in companion animal veterinary practice: A Delphi study. Vet. Rec. 2018, 182, 691. [Google Scholar] [CrossRef] [Green Version]
- Hopman, N.E.M.; Hulscher, M.E.J.L.; Graveland, H.; Speksnijder, D.C.; Wagenaar, J.A.; Broens, E.M. Factors influencing antimicrobial prescribing by Dutch companion animal veterinarians: A qualitative study. Prev. Vet. Med. 2018, 158, 106–113. [Google Scholar] [CrossRef]
- King, C.; Smith, M.; Currie, K.; Dickson, A.; Smith, F.; Davis, M.; Flowers, P. Exploring the behavioural drivers of veterinary surgeon antibiotic prescribing: A qualitative study of companion animal veterinary surgeons in the UK. BMC Vet. Res. 2018, 14, 332. [Google Scholar] [CrossRef]
- Smith, M.; King, C.; Davis, M.; Dickson, A.; Park, J.; Smith, F.; Currie, K.; Flowers, P. Pet owner and vet interactions: Exploring the drivers of AMR. Antimicrob. Resist. Infect. Control 2018, 7, 46. [Google Scholar] [CrossRef] [PubMed]
- Dickson, A.; Smith, M.; Smith, F.; Park, J.; King, C.; Currie, K.; Langdridge, D.; Davis, M.; Flowers, P. Understanding the relationship between pet owners and their companion animals as a key context for antimicrobial resistance-related behaviours: An interpretative phenomenological analysis. Health Psychol. Behav. Med. 2019, 7, 45–61. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zoetis Australia Pty Ltd. Convenia (Cefovecin Sodium), Product Information. Available online: https://websvr.infopest.com.au/LabelRouter?LabelType=L&Mode=1&ProductCode=60461 (accessed on 30 September 2021).
- Burke, S.; Black, V.; Sánchez-Vizcaíno, F.; Radford, A.; Hibbert, A.; Tasker, S. Use of cefovecin in a UK population of cats attending first-opinion practices as recorded in electronic health records. J. Feline Med. Surg. 2017, 19, 687–692. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hardefeldt, L.; Hur, B.; Verspoor, K.; Baldwin, T.; Bailey, K.E.; Scarborough, R.; Richards, S.; Billman-Jacobe, H.; Browning, G.F.; Gilkerson, J. Use of cefovecin in dogs and cats attending first-opinion veterinary practices in Australia. Vet. Rec. 2020, 187, 2020–2105. [Google Scholar] [CrossRef] [PubMed]
- Tompson, A.C.; Chandler, C.I.R.; Mateus, A.L.P.; O’Neill, D.G.; Chang, Y.-M.; Brodbelt, D.C. What drives antimicrobial prescribing for companion animals? A mixed-methods study of UK veterinary clinics. Prev. Vet. Med. 2020, 183, 105117. [Google Scholar] [CrossRef]
- Stein, M.R.; Evason, M.D.; Stull, J.W.; McClure, J.T.; Weese, J.S. Knowledge, attitudes and influencers of North American dog-owners surrounding antimicrobials and antimicrobial stewardship. J. Small Anim. Pract. 2021, 62, 442–449. [Google Scholar] [CrossRef]
- Stallwood, J.; Shirlow, A.; Hibbert, A. A UK-based survey of cat owners’ perceptions and experiences of antibiotic usage. J. Feline Med. Surg. 2020, 22, 69–76. [Google Scholar] [CrossRef]
- Rhys-Davies, L.; Ogden, J. Vets’ and Pet Owners’ Views About Antibiotics for Companion Animals and the Use of Phages as an Alternative. Front. Vet. Sci. 2020, 7, 513770. [Google Scholar] [CrossRef]
- Redding, L.E.; Cole, S.D. Pet owners’ knowledge of and attitudes toward the judicious use of antimicrobials for companion animals. J. Am. Vet. Med. Assoc. 2019, 254, 626–635. [Google Scholar] [CrossRef]
- Mangione-Smith, R.; McGlynn, E.A.; Elliott, M.N.; McDonald, L.; Franz, C.E.; Kravitz, R.L. Parent Expectations for Antibiotics, Physician-Parent Communication, and Satisfaction. Arch. Pediatr. Adolesc. Med. 2001, 155, 800. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mateus, A.L.P.; Brodbelt, D.C.; Barber, N.; Stärk, K.D.C. Qualitative study of factors associated with antimicrobial usage in seven small animal veterinary practices in the UK. Prev. Vet. Med. 2014, 117, 68–78. [Google Scholar] [CrossRef]
- Mangione-Smith, R.; McGlynn, E.A.; Elliott, M.N.; Krogstad, P.; Brook, R.H. The Relationship Between Perceived Parental Expectations and Pediatrician Antimicrobial Prescribing Behavior. Pediatrics 1999, 103, 711–718. [Google Scholar] [CrossRef] [PubMed]
- Mangione-Smith, R.; Elliott, M.N.; Stivers, T.; McDonald, L.L.; Heritage, J. Ruling Out the Need for Antibiotics. Arch. Pediatr. Adolesc. Med. 2006, 160, 945–952. [Google Scholar] [CrossRef]
- Ong, S.; Nakase, J.; Moran, G.J.; Karras, D.J.; Kuehnert, M.J.; Talan, D.A. Antibiotic Use for Emergency Department Patients With Upper Respiratory Infections: Prescribing Practices, Patient Expectations, and Patient Satisfaction. Ann. Emerg. Med. 2007, 50, 213–220. [Google Scholar] [CrossRef] [PubMed]
- Agriculture Victoria. Not All Bugs Need Drugs. Available online: https://agriculture.vic.gov.au/livestock-and-animals/livestock-health-and-welfare/antibiotic-resistant-infections/information-for-vets (accessed on 5 October 2021).
- Galli, I.; Fasanelli, R. Public understanding of science and common sense: Social representations of the human microbiome among the expert and non-expert public. Health Psychol. 2020, 7, 205510292091323. [Google Scholar] [CrossRef] [PubMed]
- Vallin, M.; Polyzoi, M.; Marrone, G.; Rosales-Klintz, S.; Wisell, K.T.; Lundborg, C.S. Knowledge and Attitudes towards Antibiotic Use and Resistance—A Latent Class Analysis of a Swedish Population-Based Sample. PLoS ONE 2016, 11, e0152160. [Google Scholar] [CrossRef] [Green Version]
- Stivers, T. Non-antibiotic treatment recommendations: Delivery formats and implications for parent resistance. Soc. Sci. Med. 2005, 60, 949–964. [Google Scholar] [CrossRef] [Green Version]
- Feenberg, D.; Ganguli, I.; Gaulé, P.; Gruber, J. It’s Good to Be First: Order Bias in Reading and Citing NBER Working Papers. Rev. Econ. Stat. 2017, 99, 32–39. [Google Scholar] [CrossRef]
- University of Melbourne. Australian Veterinary Prescribing Guidelines, Dogs and Cats. 2019. Available online: https://vetantibiotics.fvas.unimelb.edu.au/about/resources/ (accessed on 1 September 2021).
- Jessen, L.R.; Damborg, P.P.; Spohr, A.; Sørensen, M.; Langhorn, R.; Goericke-Pesch, S.K.; Houser, G.; Willesen, J.; Schjærff, M.; Eriksen, T.; et al. Antibiotic Use Guidelines for Companion Animal Practice, 2nd ed.; Companion Animal Group, Danish Veterinary Association: Frederiksberg, Denmark, 2019; Available online: www.ddd.dk/sektioner/familiedyr/antibiotikavejledning/Documents/Assembled_FINAL.pdf (accessed on 28 August 2021).
- Australian Bureau of Statistics. Historical Population Data, 2016. 2019. Available online: https://www.abs.gov.au/statistics/people/population/historical-population/latest-release#data-download (accessed on 10 June 2021).
- Australian Bureau of Statistics. Qualifications and Work 2018-19. 2020. Available online: https://www.abs.gov.au/statistics/people/education/qualifications-and-work/2018-19#data-download (accessed on 10 June 2021).
- Poon, C.; Koehler, D.; Buehler, R. On the psychology of self-prediction: Consideration of situational barriers to intended actions. Judgm. Decis. 2014, 9, 207–225. [Google Scholar]
- Søgaard, A.J.; Selmer, R.; Bjertness, E.; Thelle, D. The Oslo Health Study: The impact of self-selection in a large, population-based survey. Int. J. Equity Health 2004, 3, 3. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Strandhagen, E.; Berg, C.; Lissner, L.; Nunez, L.; Rosengren, A.; Torén, K.; Thelle, D.S. Selection bias in a population survey with registry linkage: Potential effect on socioeconomic gradient in cardiovascular risk. Eur. J. Epidemiol. 2010, 25, 163–172. [Google Scholar] [CrossRef] [PubMed]
- Regber, S.; Novak, M.; Eiben, G.; Lissner, L.; Hense, S.; Sandström, T.Z.; Ahrens, W.; Mårild, S. Assessment of selection bias in a health survey of children and families—The IDEFICS Sweden-study. BMC Public Health 2013, 13, 418. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Australian Bureau of Statistics. Census of Population and Housing: Socio-Economic Indexes for Areas (SEIFA), Australia, 2016. 2018. Available online: https://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2033.0.55.0012016?OpenDocument (accessed on 10 June 2021).




Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scarborough, R.; Hardefeldt, L.; Browning, G.; Bailey, K. Pet Owners and Antibiotics: Knowledge, Opinions, Expectations, and Communication Preferences. Antibiotics 2021, 10, 1326. https://doi.org/10.3390/antibiotics10111326
Scarborough R, Hardefeldt L, Browning G, Bailey K. Pet Owners and Antibiotics: Knowledge, Opinions, Expectations, and Communication Preferences. Antibiotics. 2021; 10(11):1326. https://doi.org/10.3390/antibiotics10111326
Chicago/Turabian StyleScarborough, Ri, Laura Hardefeldt, Glenn Browning, and Kirsten Bailey. 2021. "Pet Owners and Antibiotics: Knowledge, Opinions, Expectations, and Communication Preferences" Antibiotics 10, no. 11: 1326. https://doi.org/10.3390/antibiotics10111326
APA StyleScarborough, R., Hardefeldt, L., Browning, G., & Bailey, K. (2021). Pet Owners and Antibiotics: Knowledge, Opinions, Expectations, and Communication Preferences. Antibiotics, 10(11), 1326. https://doi.org/10.3390/antibiotics10111326







