Capabilities of Double-Resonance LPG and SPR Methods for Hypersensitive Detection of SARS-CoV-2 Structural Proteins: A Comparative Study
Abstract
1. Introduction
1.1. Comparison of SARS-CoV-2 Clinical Detection Techniques
1.2. Biosensors for Rapid Detection of SARS-CoV-2
2. Reagents and Materials
2.1. Structural Proteins
2.1.1. SARS-CoV-2 Spike S1 Subunit Protein
2.1.2. SARS-CoV-2 Nucleocapsid Protein
2.2. Antibodies
2.2.1. Anti-SARS-CoV-1/2 NP Antibody
2.2.2. SARS-CoV-2 Nucleocapsid Polyclonal Antibody
2.3. Reagents for ELISA
2.3.1. SARS-CoV-2 Antigen ELISA Kit: N Proteins
2.3.2. SARS-CoV-2 Antigen ELISA Kit: S Proteins
2.3.3. COVID-19 Antigen Rapid Test
3. Optical Platforms and Functionalization for Virus-Sensing Applications
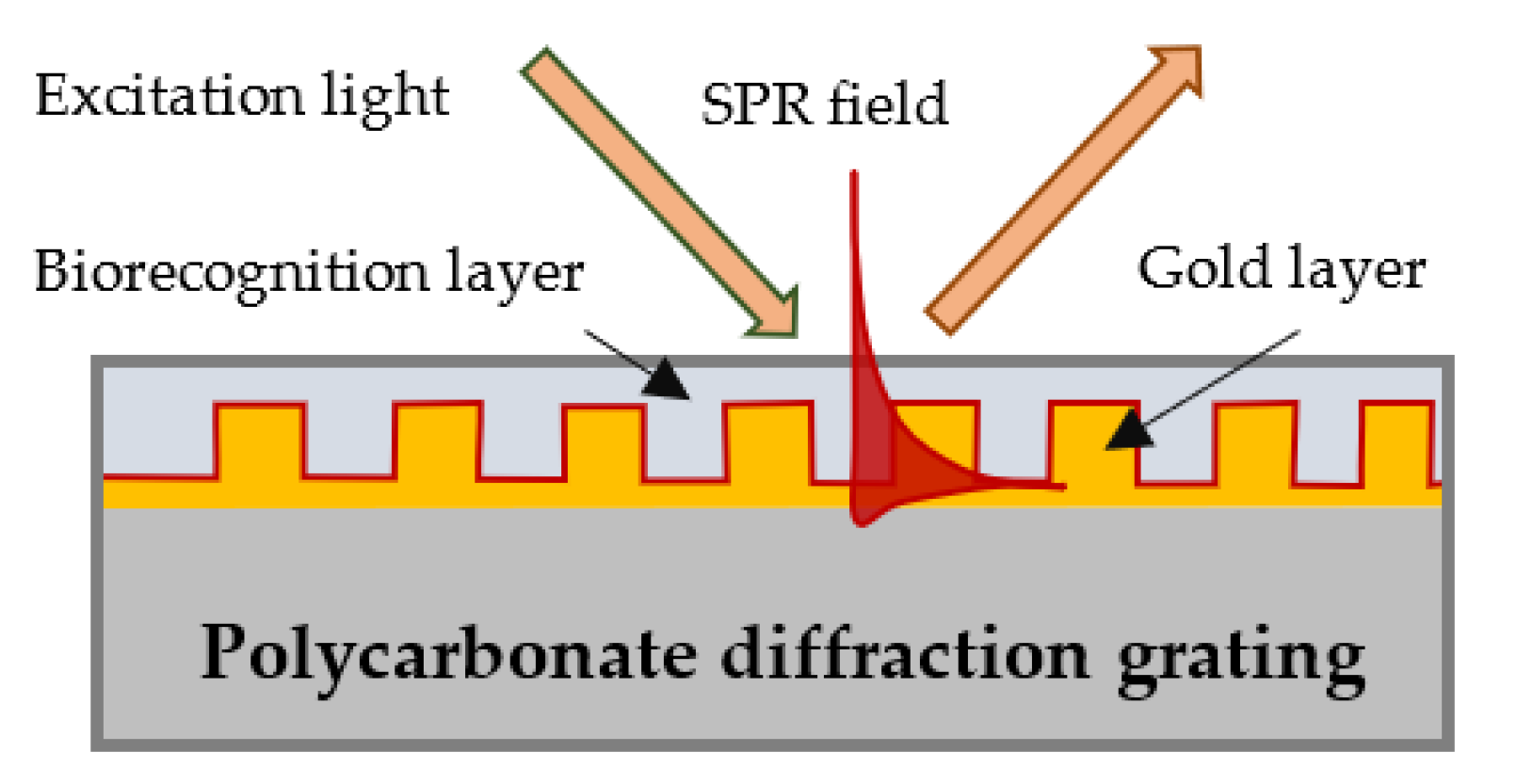
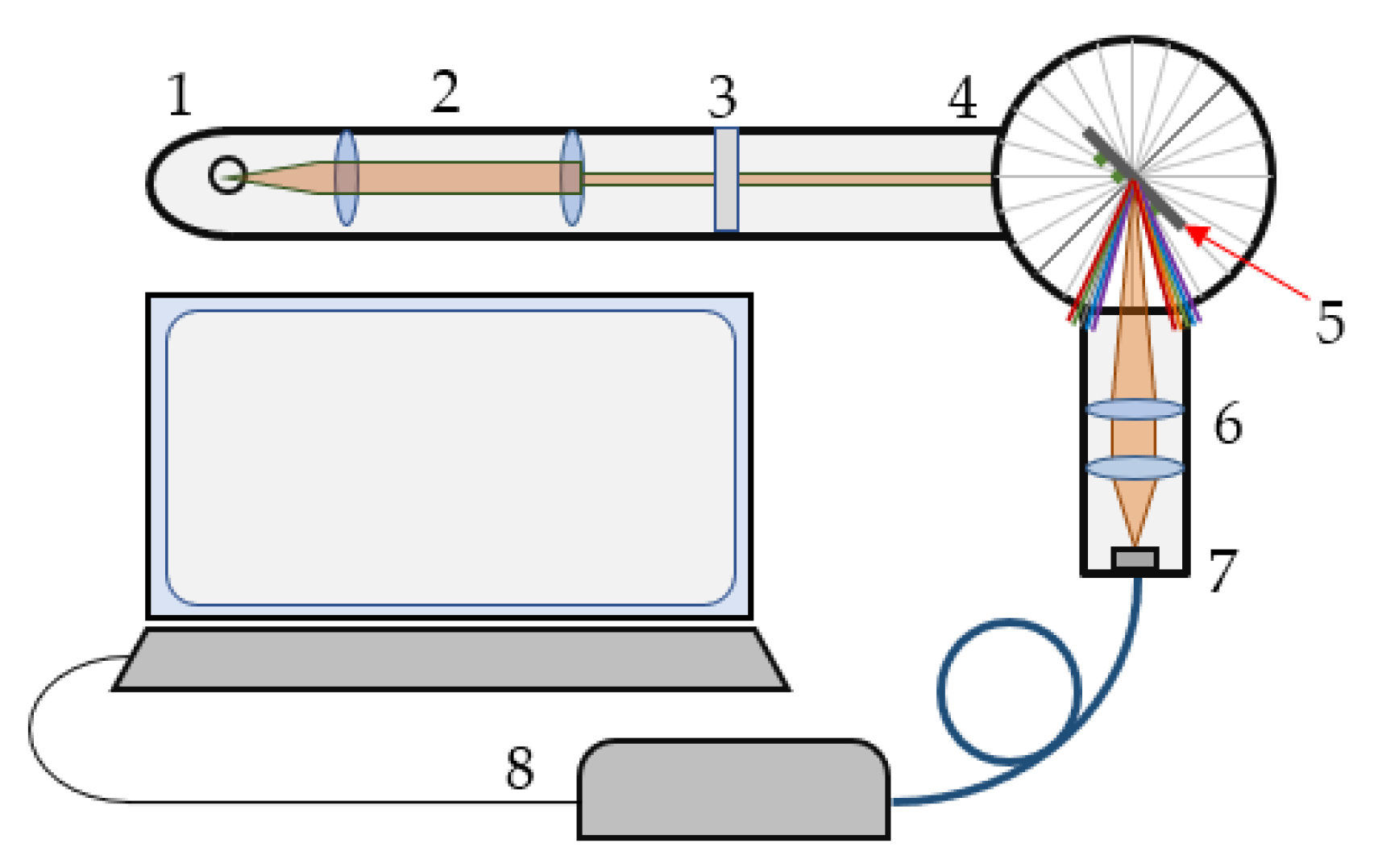
3.1. SPR Platforms
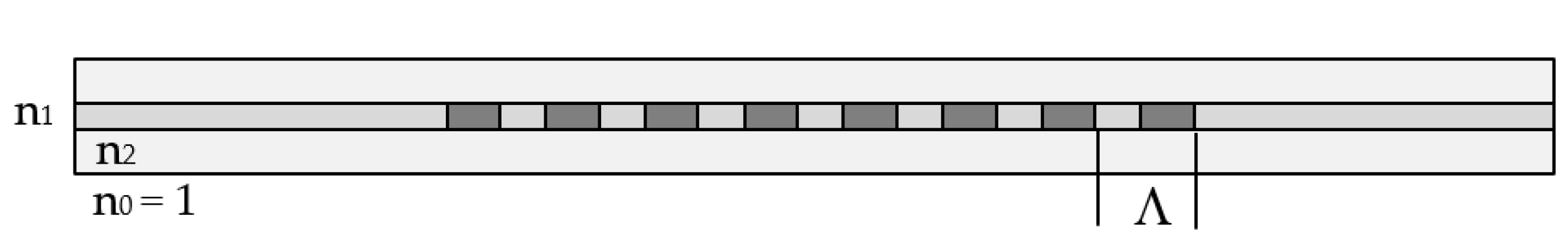
3.2. Double-Resonance Long-Period Gratings (DR LPG)
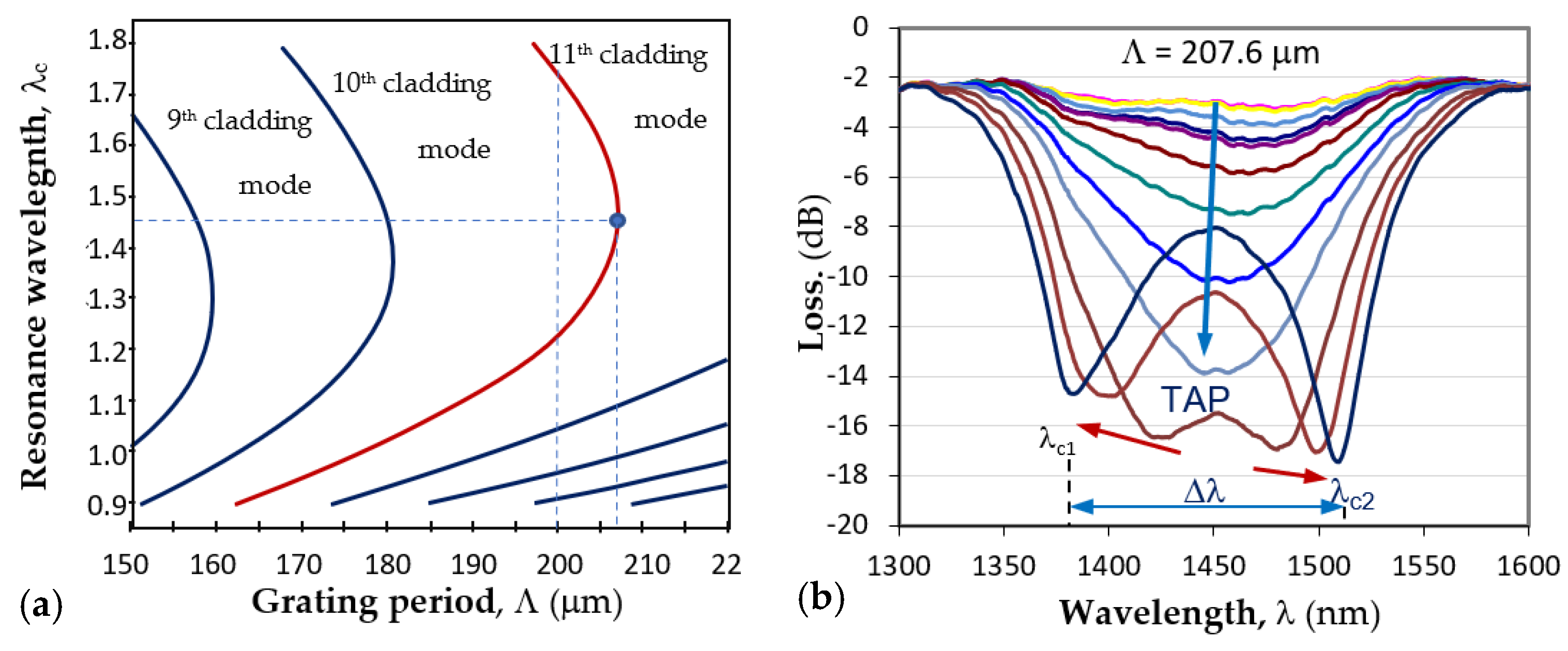
3.2.1. Turn-Around Point (TAP) and Double Resonance (DR) LPGs
3.2.2. DR LPG Fabrication and Calibration Procedure
3.3. Functionalization of the Platforms
4. Experiment, Results, and Analysis
4.1. Measurement Procedures
4.1.1. DR LPG Measurement Procedure
- The functionalized grating was placed in the measurement set-up using the same weight and at the same temperature as during the calibration measurement.
- The spectral separation was measured in air and in water immediately after immersion in water and 5 min later, which is referred to as Δλ0. The purpose of the 5 min waiting period was to allow for the grating to reach thermodynamic equilibrium in the liquid.
- The spectra for each concentration, starting from the lowest to the highest, were consecutively measured. Measurements were recorded immediately after the insertion into a particular concentration, after 2.5 min, and at 5 min.
- After the measurement at the highest concentration was performed, the spectra in water and in air were remeasured.
- The spectral separation Δλ = λc2 − λc1 for each measurement was determined.
- Next, the change in the spectral separation at a given concentration Δλi with respect to that in water Δλ0 was defined as
- Because the accumulation of the detected protein increased the refractive index upon the surface of the grating, the spectral changes, δλi, were converted into refractive index changes, δni, for the corresponding concentration by taking into account the sensitivity, Sn, of the particular grating. From (3) and (4), it follows that
- Ultimately, the dependence δni(Ci) was plotted for each protein and functionalization (mAb and pAb).
4.1.2. SPR Measurement Procedure
- After the gold layer was deposited on the polycarbonate substrate, the plasmon resonance was measured at six different points of the diffraction grating surface to eliminate the influence of the grooves’ curvature on the resonance spectral shift.
- After gilded diffraction gratings were functionalized, the measurement was performed at the same points to evaluate the quality of the ligand layer. The spectral position of the resonances at each point was taken as a reference, against which the shift due to the antibody–antigen interaction was considered.
- The SPR chips were incubated for 20 min in N- and S-protein solutions of different concentrations at room temperature. Special attention was paid to ensure the uniform coverage of the entire surface of the biochip. Then biochips were washed with deionized water (<2 µS/cm), after which the liquid phase was removed by centrifugation.
- Plasmon resonances were measured at the same six points on the biochip surface, and resonance wavelength shift was estimated as the difference from the reference resonance. Then, corresponding displacement average values and the absolute measurement errors were determined.
4.2. Results
4.2.1. DR LPG Results


| DR LPG | P102 | P111 | P099 | P112 |
|---|---|---|---|---|
| Functionalization | mAb | mAb | pAb | pAb |
| δn∞ | 0.0069 | 0.0069 | 0.01 | 0.01 |
| a | 1.58 | 2.0145 | 1.1 | 2.250 |
| α | 0.166 | 0.329 | 0.071 | 0.245 |
| R2 | 0.9762 | 0.9773 | 0.9576 | 0.9986 |
| DR LPG | P102 | P111 | P099 | P112 |
|---|---|---|---|---|
| Functionalization | mAb | mAb | pAb | pAb |
| A | 0.0012 | 0.0009 | 0.0006 | 0.0015 |
| C0 | 0.18888 | 0.07765 | 0.36788 | 0.05322 |
| R2 | 0.921 | 0.9576 | 0.9981 | 0.9825 |
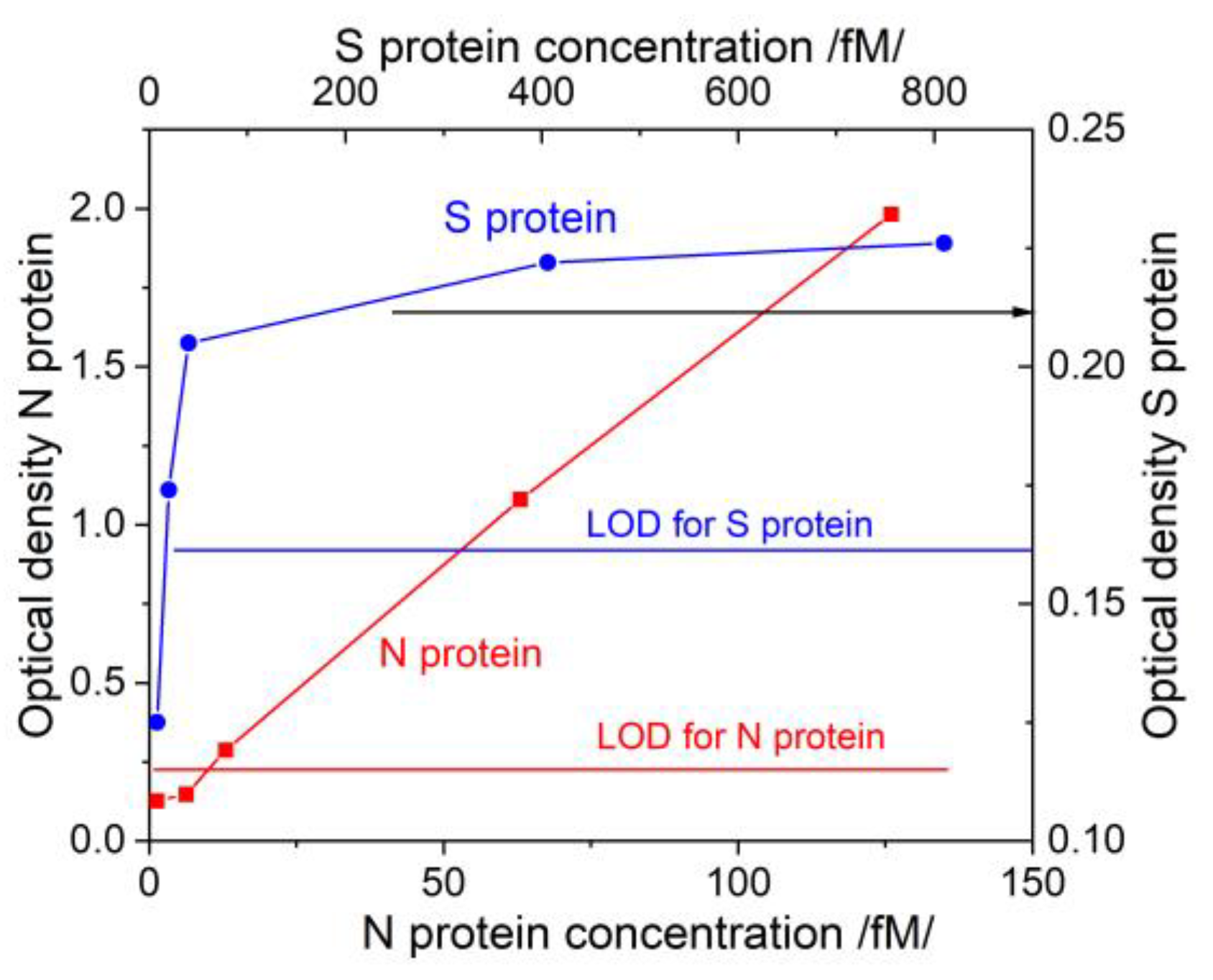
4.2.2. SPR Measurement Results
4.3. Comparative Analysis: DR LPG vs. SPR
4.4. Comparative Analysis: DR LPG/SPR vs. ELISA/Rapid Antigen Test

| Ligand | N-mAb | N-pAb | |
|---|---|---|---|
| Detected Proteins | N-Protein | N Protein | |
| Biosensor | DR LPG | 13 fmol | 20 fmol |
| SPR | 126 fmol | 126 fmol | |
| Clinical test | ELISA | 10 fmol | -- |
| Rapid antigen test | 126 fmol | -- | |
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hamed, M.A. An overview on COVID-19: Reality and expectation. Bull. Natl. Res. Cent. 2020, 44, 86. [Google Scholar] [CrossRef] [PubMed]
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A novel coronavirus from patients with pneumonia in China 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef]
- García-Basteiro, A.L.; Chaccour, C.; Guinovart, C.; Llupià, A.; Brew, J.; Trilla, A.; Plasencia, A. Monitoring the COVID-19 epidemic in the context of widespread local transmission. Lancet Respir. Med. 2020, 8, 440–442. [Google Scholar] [CrossRef] [PubMed]
- LeBlanc, J.J.; Gubbay, J.B.; Li, Y.; Needle, R.; Arneson, S.R.; Marcino, D.; Charest, H.; Desnoyers, G.; Dust, K.; Fattouh, R.; et al. Real-time PCR-based SARS-CoV-2 detection in Canadian laboratories. J. Clin. Virol. 2020, 128, 104433. [Google Scholar] [CrossRef] [PubMed]
- Lamb, L.E.; Bartolone, S.N.; Ward, E.; Chancellor, M.B. Rapid. Detection of Novel Coronavirus/Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) by Reverse Transcription-Loop-Mediated Isothermal Amplification. PLoS ONE 2020, 15, e0234682. [Google Scholar] [CrossRef] [PubMed]
- Nazario-Toole, A.; Nguyen, H.M.; Xia, H.; Frankel, D.N.; Kieffer, J.W.; Gibbons, T.F. Sequencing SARS-CoV-2 from antigen tests. PLoS ONE 2022, 17, e0263794. [Google Scholar] [CrossRef] [PubMed]
- Drain, P.K. Rapid diagnostic testing for SARS-CoV-2. N. Engl. J. Med. 2022, 386, 264–272. [Google Scholar] [CrossRef] [PubMed]
- Amanat, F.; Nguyen, T.; Chromikova, V.; Strohmeier, S.; Stadlbauer, D.; Javier, A.; Jiang, K.; Asthagiri-Arunkumar, G.; Polanco, J.; Bermudez-Gonzalez, M.; et al. A serological assay to detect SARS-CoV-2 seroconversion in humans. Nat. Med. 2020, 26, 1033–1036. [Google Scholar] [CrossRef]
- Yongchen, Z.; Shen, H.; Wang, X.; Shi, X.; Li, Y.; Yan, J.; Chen, Y.; Gu, B. Different longitudinal patterns of nucleic acid and serology testing results based on disease severity of COVID-19 patients. Emerg. Microbes Infect. 2020, 9, 833–836. [Google Scholar] [CrossRef]
- Wang, W.; Xu, Y.; Gao, R.; Lu, R.; Han, K.; Wu, G.; Tan, W. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA 2020, 323, 1843–1844. [Google Scholar] [CrossRef]
- Sandri, T.L.; Inoue, J.; Geiger, J.; Griesbaum, J.-M.; Heinzel, C.; Burnet, M.; Fendel, R.; Kremsner, P.; Held, J.; Kreidenweiss, A. Complementary methods for SARS-CoV-2 diagnosis in times of material shortage. Sci. Rep. 2021, 11, 11899. [Google Scholar] [CrossRef]
- Liu, R.; Yi, S.; Zhang, J.; Lv, Z.; Zhu, C.; Zhang, Y. Viral load dynamics in sputum and nasopharyngeal swab in patients with COVID-19. J. Dent. Res. 2020, 99, 1239–1244. [Google Scholar] [CrossRef] [PubMed]
- Tastanova, A.; Stoffel, C.I.; Dzung, A.; Cheng, P.F.; Bellini, E.; Johansen, P.; Duda, A.; Nobbe, S.; Lienhard, R.; Bosshard, P.P.; et al. A Comparative Study of Real-Time RT-PCR-Based SARS-CoV-2 Detection Methods and Its Application to Human-Derived and Surface Swabbed Material. J. Mol. Diagn. 2021, 23, 796–804. [Google Scholar] [CrossRef] [PubMed]
- Carmagnola, D.; Toma, M.; Henin, D.; Perrotta, M.; Pellegrini, G.; Dellavia, C. Personal Protection Equipment and Infection Control Procedures among Health Workers during the COVID-19 Pandemic. Healthcare 2022, 10, 944. [Google Scholar] [CrossRef]
- Weissleder, R.; Lee, H.; Ko, J.; Pittet, M.J. COVID-19 Diagnostics in Context. Sci. Transl. Med. 2020, 12, 1931. [Google Scholar] [CrossRef] [PubMed]
- Afzal, A. Molecular Diagnostic Technologies for COVID-19: Limitations and Challenges. J. Adv. Res. 2020, 26, 149–159. [Google Scholar] [CrossRef] [PubMed]
- Aguilar-Shea, A.L.; Vera-García, M.; Güerri-Fernández, R. Rapid antigen tests for the detection of SARS-CoV-2: A narrative review. Aten. Prim. 2021, 53, 102127. [Google Scholar] [CrossRef] [PubMed]
- Ang, G.Y.; Chan, K.G.; Yean, C.Y.; Yu, C.Y. Lateral Flow Immunoassays for SARS-CoV-2. Diagnostics 2022, 12, 2854. [Google Scholar] [CrossRef]
- Iglòi, Z.; Velzing, J.; van Beek, J.; van de Vijver, D.; Aron, G.; Ensing, R.; Benschop, K.; Han, W.; Boelsums, T.; Koopmans, M.; et al. Clinical evaluation of Roche Sd Biosensor rapid antigen test for SARS-CoV-2 in municipal health service testing site, the Netherlands. Emerg. Infect. Dis. 2021, 27, 1323–1329. [Google Scholar] [CrossRef]
- Jin, Y.; Wang, M.; Zuo, Z.; Fan, C.; Ye, F.; Cai, Z.; Wang, Y.; Cui, H.; Pan, K.; Xu, A. Diagnostic value and dynamic variance of serum antibody in coronavirus disease 2019. Int. J. Infect Dis. 2020, 94, 49–52. [Google Scholar] [CrossRef]
- Lino, A.; Cardoso, M.A.; Gonçalves, H.M.R.; Martins-Lopes, P. SARS-CoV-2 Detection Methods. Chemosensors 2022, 10, 221. [Google Scholar] [CrossRef]
- Zeng, W.; Liu, G.; Ma, H.; Zhao, D.; Yang, Y.; Liu, M.; Mohammed, A.; Zhao, C.; Yang, Y.; Xie, J.; et al. Biochemical characterization of SARS-CoV-2 nucleocapsid protein. Biochem. Biophys. Res. Commun. 2020, 527, 618–623. [Google Scholar] [CrossRef]
- Tan, Y.-J.; Goh, P.-Y.; Fielding, B.C.; Shen, S.; Chou, C.-F.; Fu, J.-L.; Leong, H.N.; Leo, Y.S.; Ooi, E.E.; Ling, A.E. Profiles of antibody responses against severe acute respiratory syndrome coronavirus recombinant proteins and their potential use as diagnostic markers. Clin. Diagn. Lab. Immunol. 2004, 11, 362–371. [Google Scholar]
- Leung, D.; Hang, T.C.; Hung, M.C.; Chan, P.S.; Cheung, J.; Niu, H.; Tam, J.; Lim, P. Antibody response of patients with severe acute respiratory syndrome (SARS) targets the viral nucleocapsid. JID 2004, 190, 379–386. [Google Scholar] [CrossRef] [PubMed]
- Ravi, A.; Prabath Singh, V.; Chandran, R.; Venugopal, K.; Haridas, K.; Kavitha, R. COVID-19 Antibody Tests: An Overview. J. Pharm. Bioallied Sci. 2021, 13, 48. [Google Scholar] [CrossRef]
- Ge, C.; Feng, J.; Zhang, J.; Hu, K.; Wang, D.; Zha, L.; Hu, X.; Li, R. Aptamer/antibody sandwich method for digital detection of SARS-CoV2 nucleocapsid protein. Talanta 2022, 236, 122847. [Google Scholar] [CrossRef]
- Zamzami, M.A.; Rabbani, G.; Ahmad, A.; Basalah, A.; Al-Sabban, W.; Ahn, S.N.; Choudhry, H. Carbon nanotube field-effect transistor (CNT-FET)-based biosensor for rapid detection of SARS-CoV-2 (COVID-19) surface spike protein S1. Bioelectrochemistry 2022, 143, 107982. [Google Scholar] [CrossRef] [PubMed]
- Seo, G.; Lee, G.; Kim, M.J.; Baek, S.H.; Choi, M.; Ku, K.B.; Lee, C.S.; Jun, S.; Park, D.; Kim, H.G.; et al. Rapid Detection of COVID-19 Causative Virus (SARS-CoV-2) in Human Nasopharyngeal Swab Specimens Using Field-Effect Transistor-Based Biosensor. ACS Nano 2020, 14, 5135–5142. [Google Scholar] [CrossRef] [PubMed]
- Eftimov, T.; Janik, M.; Koba, M.; Śmietana, M.; Mikulic, P.; Bock, W. Long-Period Gratings and Microcavity In-Line Mach Zehnder Interferometers as Highly Sensitive Optical Fiber Platforms for Bacteria Sensing. Sensors 2020, 20, 3772. [Google Scholar] [CrossRef]
- Janczuk-Richter, M.; Gromadzka, B.; Richter, Ł.; Panasiuk, M.; Zimmer, K.; Mikulic, P.; Bock, W.J.; Maćkowski, S.; Śmietana, M.; Niedziółka Jönsson, J. Immunosensor Based on Long-Period Fiber Gratings for Detection of Viruses Causing Gastroenteritis. Sensors 2020, 20, 813. [Google Scholar] [CrossRef]
- Quero, G.; Zuppolini, S.; Consales, M.; Diodato, L.; Vaiano, P.; Venturelli, A.; Santucci, M.; Spyrakis, F.; Costi, M.P.; Giordano, M.; et al. Long period fiber grating working in reflection mode as valuable biosensing platform for the detection of drug resistant bacteria. Sens. Actuators B Chem. 2016, 230, 510–520. [Google Scholar] [CrossRef]
- Dey, T.K.; Biswas, P.; Basumallick, N.; Bandyopadhyay, S. Realization of Long Period Fiber Grating in Reflection Mode Operating Near Turn Around Point. IEEE Sens. J. 2017, 17, 4100–4106. [Google Scholar] [CrossRef]
- Śmietana, M.; Mikulic, P.; Bock, W.J. Nano-coated long-period gratings for detection of sub-nanometric changes in thin-film thickness. Sens. Actuators A Phys. 2018, 270, 79–83. [Google Scholar] [CrossRef]
- Debowska, A.K.; Smietana, M.; Mikulic, P.; Bock, W.J. High temperature nano-coated electric-arc-induced long-period gratings working at the dispersion turning point for refractive index sensing. Jpn. J. Appl. Phys. 2014, 53, 08ME01. [Google Scholar] [CrossRef]
- Piestrzyńska, M.; Dominik, M.; Kosiel, K.; Janczuk-Richter, M.; Szot-Karpińska, K.; Brzozowska, E.; Shao, L.; Niedziółka-Jonsson, J.; Bock, W.J.; Śmietana, M. Ultrasensitive tantalum oxide nano-coated long-period gratings for detection of various biological targets. Biosens. Bioelectron. 2019, 133, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.-L.; Kim, J.; Choi, S.; Han, J.; Seo, G.; Lee, W.Y. Fiber-optic label-free biosensor for SARS-CoV-2 spike protein detection using biofunctionalized long-period fiber grating. Talanta 2021, 235, 122801. [Google Scholar] [CrossRef]
- Janik, M.; Gabler, T.; Koba, M.; Panasiuk, M.; Dashkevich, Y.; Łęga, T.; Dąbrowska, A.; Naskalska, A.; Żołędowska, S.; Nidzworski, D.; et al. Low-volume label-free SARS-CoV-2 detection with the microcavity-based optical fiber sensor. Sci. Rep. 2023, 13, 1512. [Google Scholar] [CrossRef]
- Lim, W.Y.; Lan, B.L.; Ramakrishnan, N. Emerging Biosensors to Detect Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2): A Review. Biosensors 2021, 11, 434. [Google Scholar] [CrossRef]
- Mauriz, E. Recent progress in plasmonic biosensing schemes for virus detection. Sensors 2020, 20, 47452. [Google Scholar] [CrossRef] [PubMed]
- Arano-Martinez, J.A.; Martínez-González, C.L.; Salazar, M.I.; Torres-Torres, C. A Framework for Biosensors Assisted by Multiphoton Effects and Machine Learning. Biosensors 2022, 12, 710. [Google Scholar] [CrossRef]
- Pandey, P.S.; Raghuwanshi, S.K.; Ansari, M.T.I.; Kumar, S. SPR Based Biosensing Chip for COVID-19 Diagnosis—A Review. IEEE Sens. J. 2022, 22, 13800–13810. [Google Scholar] [CrossRef] [PubMed]
- Kisov, H.; Dyankov, G.; Belina, E.; Petrov, M.; Naradikian, H.; Dimitrova, T.; Malinowski, N. Surface plasmon excitation on a grating assisted by a cholesteric liquid crystal layer. Appl. Opt. 2022, 61, 2019–2024. [Google Scholar] [CrossRef]
- Dyankov, G.; Borisova, E.; Belina, E.; Kisov, H.; Angelov, I.; Gisbrecht, A.; Strijkova, V.; Malinowski, N. A Surface Plasmon Resonance Biosensor Based on Directly Immobilized Hemoglobin and Myoglobin. Sensors 2020, 20, 5572. [Google Scholar] [CrossRef] [PubMed]
- Dyankov, G.; Eftimov, T.; Malinovski, N.; Belina, E.; Kisov, H.; Mikulic, P.; Bock, W. Highly Efficient Biosensor based on MAPLE Deposited Hemoglobin on LPGs Around Phase Matching Turning Point. Opt. Laser Technol. 2019, 123, 105907. [Google Scholar] [CrossRef]
- Qiu, G.; Gai, Z.; Tao, Y.; Schmitt, J.; Kullak-Ublick, G.A.; Wang, J. Dual-Functional Plasmonic Photothermal Biosensors for Highly Accurate Severe Acute Respiratory Syndrome Coronavirus 2 Detection. ACS Nano 2020, 14, 5268–5277. [Google Scholar] [CrossRef]
- Yano, T.; Kajisa, T.; Ono, M.; Miyasaka, Y.; Hasegawa, Y.; Saito, A.; Otsuka, K.; Sakane, A.; Sasaki, T.; Yasutomo, K.; et al. Ultrasensitive detection of SARS-CoV-2 nucleocapsid protein using large gold nanoparticle-enhanced surface plasmon resonance. Sci. Rep. 2022, 12, 1060. [Google Scholar] [CrossRef]
- Wu, Q.; Wu, W.; Chen, F.; Ren, P. Highly Sensitive and Selective Surface Plasmon Resonance Biosensor for the Detection of SARS-CoV-2 Spike S1 Protein. Analyst 2022, 147, 2809–2818. [Google Scholar] [CrossRef] [PubMed]


| DR LPG | P102 | P111 | P099 | P112 |
|---|---|---|---|---|
| Number of periods, N | 235 | 235 | 240 | 235 |
| SRI sensitivity Sn (nm/r.i.u) | 1732.8 | 2327.2 | 2081.4 | 2440.9 |
| Functionalization | mAb | mAb | pAb | pAb |
| Maximum concentration (fmol) | 450 | 800 | 450 | 800 |
| Maximum shift (nm) | 8.5 | 7.5 | 6 | 14.5 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Eftimov, T.; Genova-Kalou, P.; Dyankov, G.; Bock, W.J.; Mankov, V.; Shoar Ghaffari, S.; Veselinov, P.; Arapova, A.; Makouei, S. Capabilities of Double-Resonance LPG and SPR Methods for Hypersensitive Detection of SARS-CoV-2 Structural Proteins: A Comparative Study. Biosensors 2023, 13, 318. https://doi.org/10.3390/bios13030318
Eftimov T, Genova-Kalou P, Dyankov G, Bock WJ, Mankov V, Shoar Ghaffari S, Veselinov P, Arapova A, Makouei S. Capabilities of Double-Resonance LPG and SPR Methods for Hypersensitive Detection of SARS-CoV-2 Structural Proteins: A Comparative Study. Biosensors. 2023; 13(3):318. https://doi.org/10.3390/bios13030318
Chicago/Turabian StyleEftimov, Tinko, Petia Genova-Kalou, Georgi Dyankov, Wojtek J. Bock, Vihar Mankov, Sanaz Shoar Ghaffari, Petar Veselinov, Alla Arapova, and Somayeh Makouei. 2023. "Capabilities of Double-Resonance LPG and SPR Methods for Hypersensitive Detection of SARS-CoV-2 Structural Proteins: A Comparative Study" Biosensors 13, no. 3: 318. https://doi.org/10.3390/bios13030318
APA StyleEftimov, T., Genova-Kalou, P., Dyankov, G., Bock, W. J., Mankov, V., Shoar Ghaffari, S., Veselinov, P., Arapova, A., & Makouei, S. (2023). Capabilities of Double-Resonance LPG and SPR Methods for Hypersensitive Detection of SARS-CoV-2 Structural Proteins: A Comparative Study. Biosensors, 13(3), 318. https://doi.org/10.3390/bios13030318






