Applications of Nanosheets in Frontier Cellular Research
Abstract
1. Introduction
2. Nanosheets as a Substrate
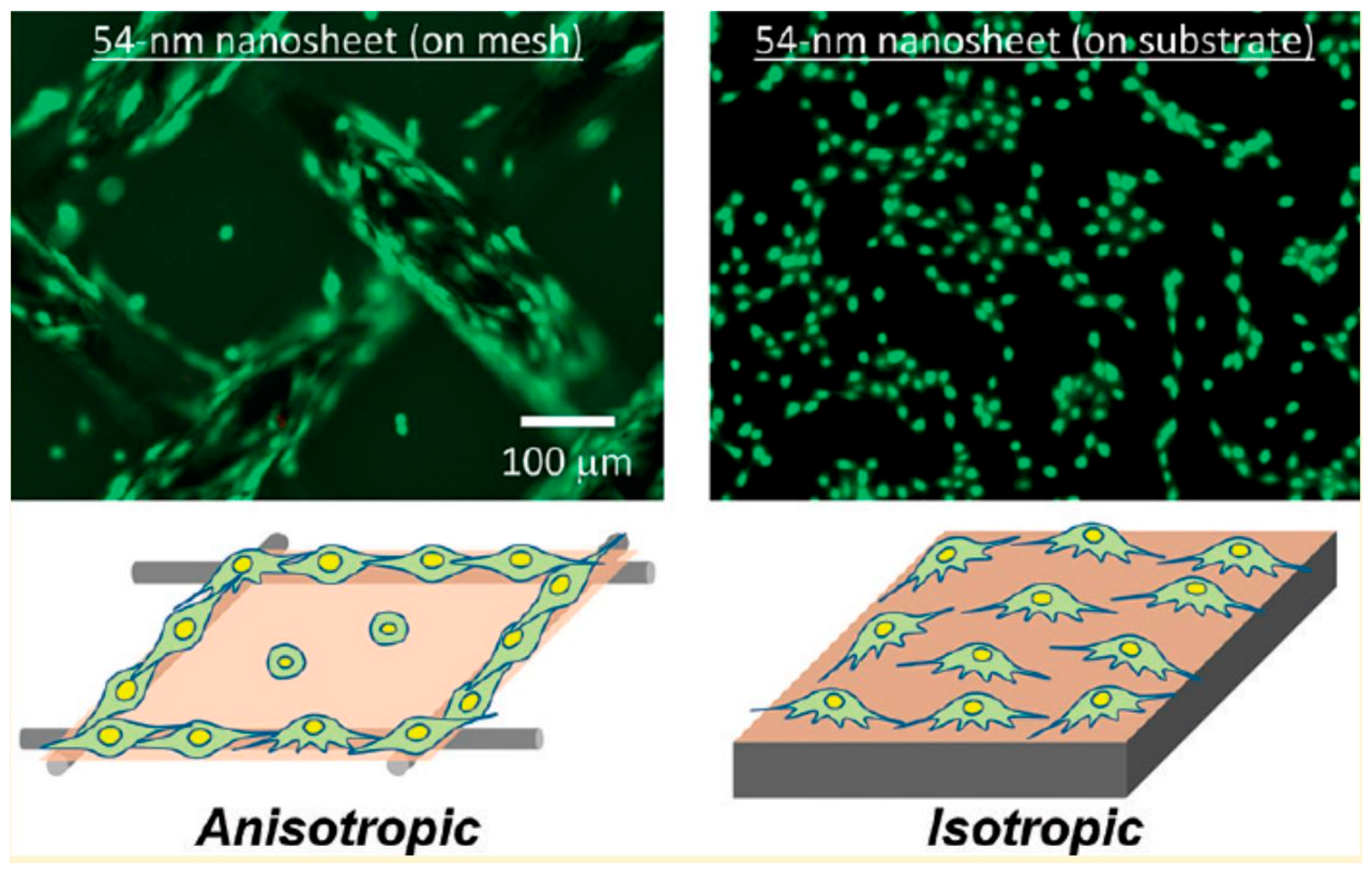
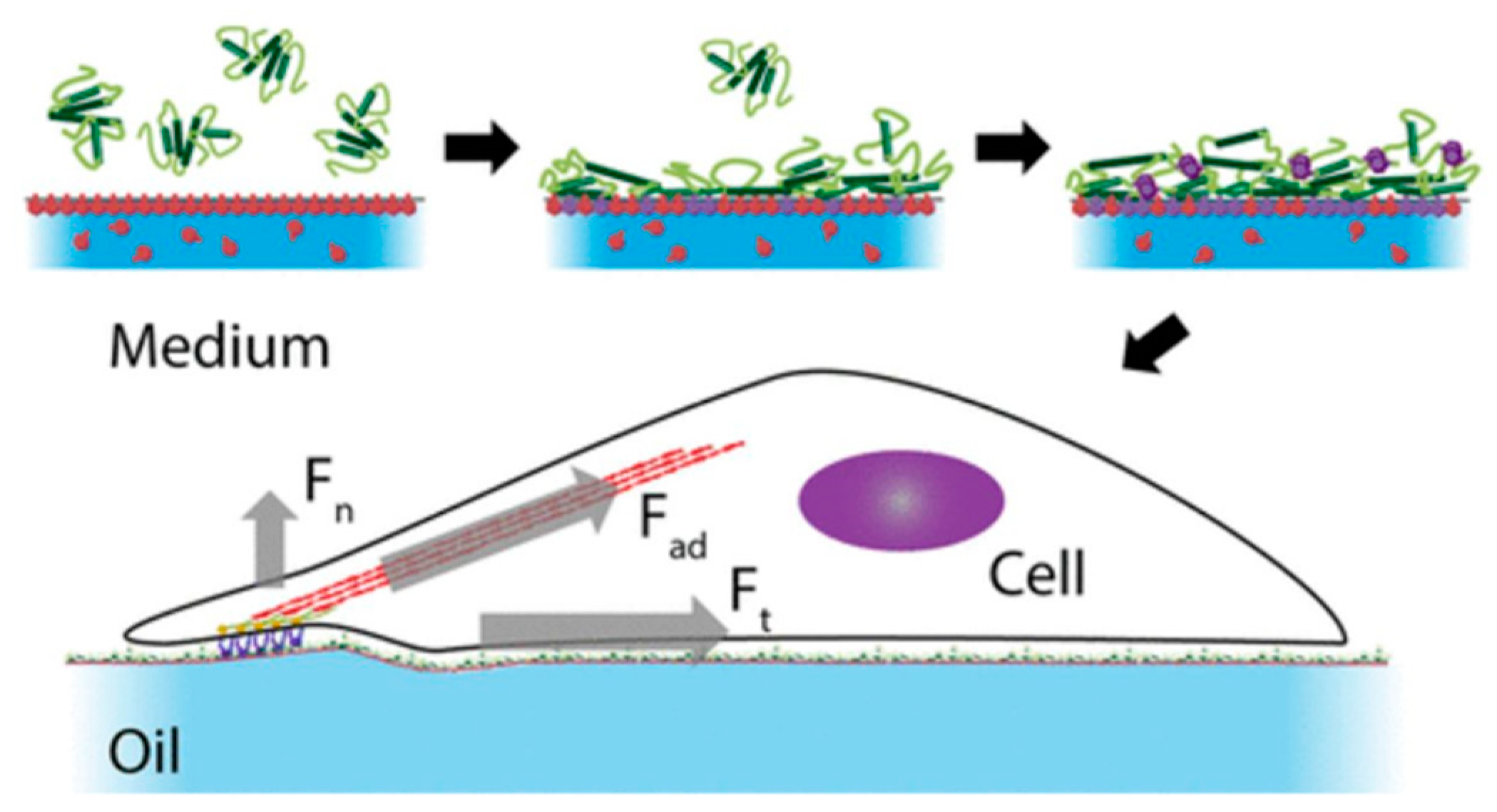
2.1. Effects of Nanosheets on Cell Adhesion and Function
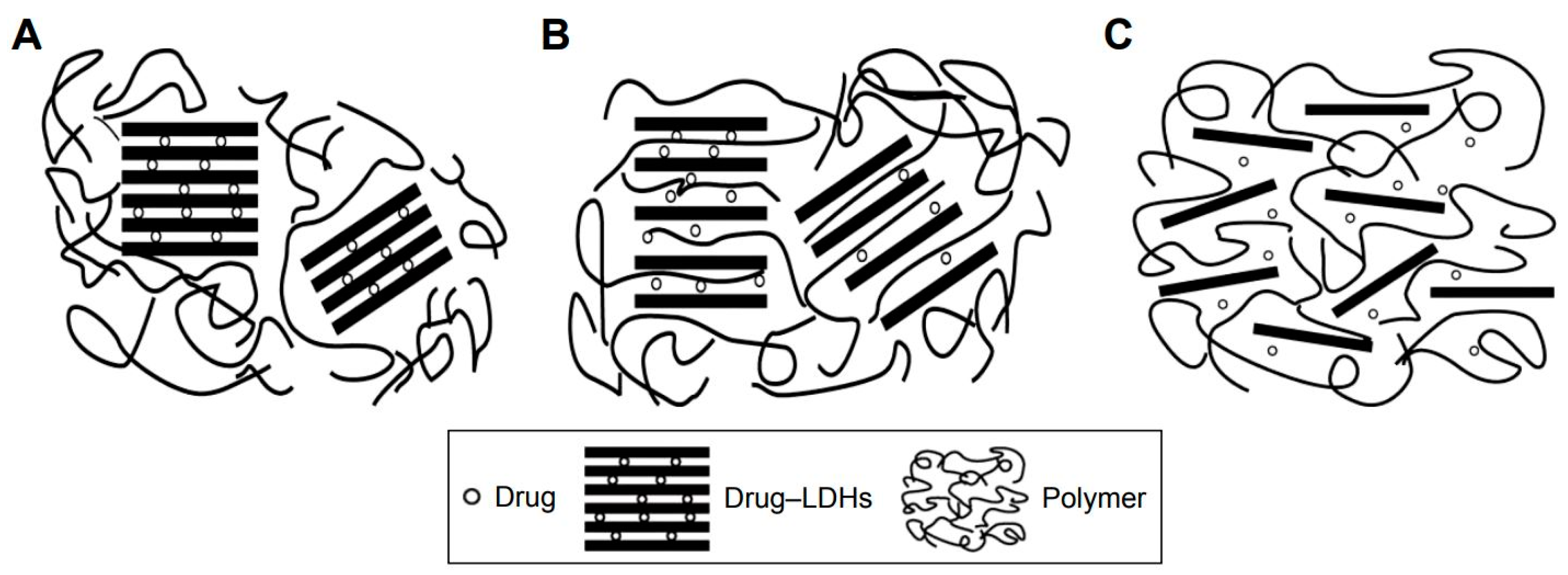
2.2. Delivery Functions Acted on by Nanosheets
3. Nanosheets as a Sensitive Surface
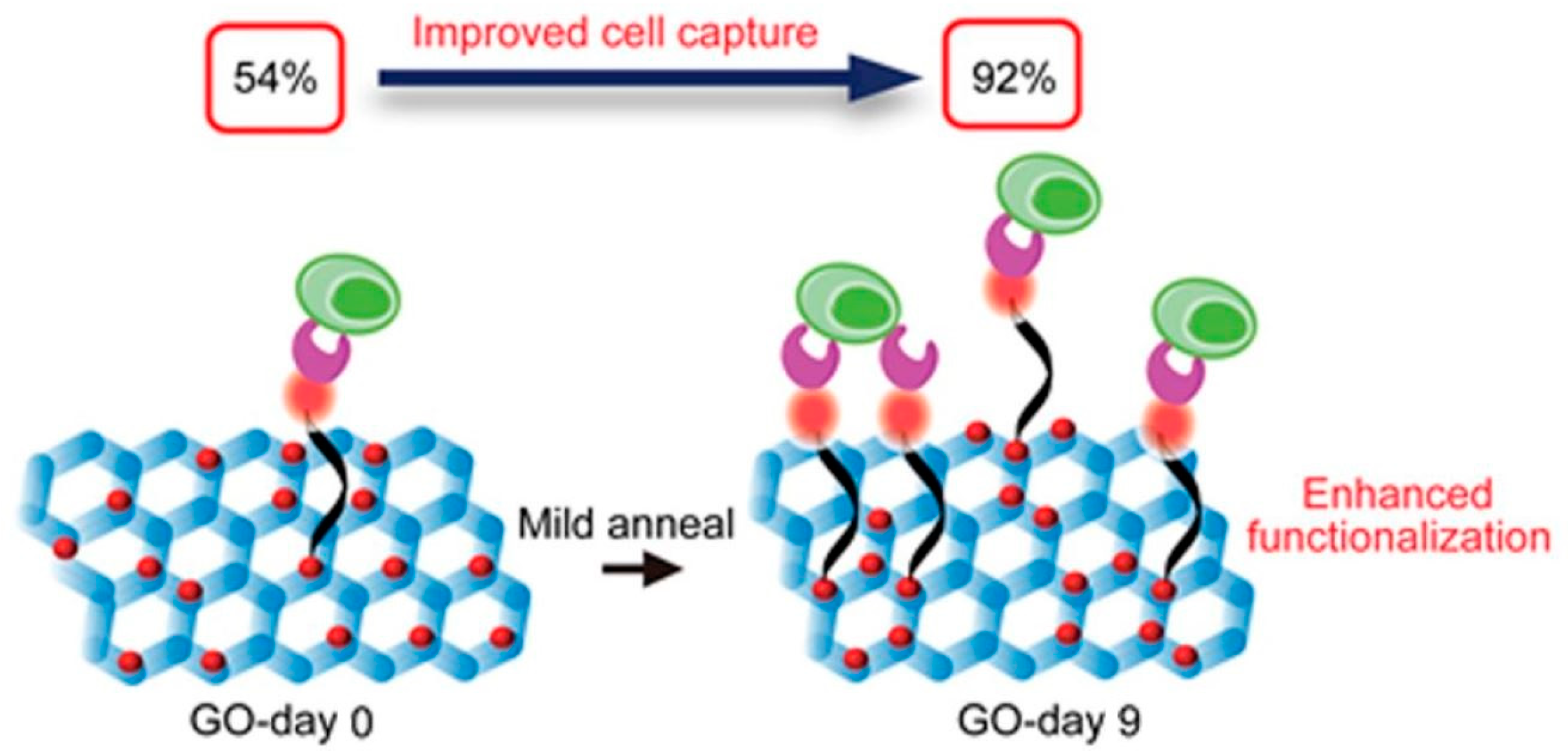
3.1. Cell Capturing Using Surface-Modified Nanosheets
3.2. Cell Sensing and Imaging
4. Nanosheets in Regenerative Medicine
4.1. Nanosheets as a Scaffold Element
4.2. Nanosheets for Stem Cell Differentiation and Tissue Regeneration
5. Important Issues: Internalization, Distribution, and Cellular Responses
6. Cost, Fabrication, and Limitation
7. Conclusions and Perspectives
Author Contributions
Funding
Conflicts of Interest
References
- Li, X.; Zhang, G.; Bai, X.; Sun, X.; Wang, X.; Wang, E.; Dai, H. Highly conducting graphene sheets and Langmuir-Blodgett films. Nat. Nanotechnol. 2008, 3, 538–542. [Google Scholar] [CrossRef] [PubMed]
- Coleman, J.N.; Lotya, M.; O’Neill, A.; Bergin, S.D.; King, P.J.; Khan, U.; Young, K.; Gaucher, A.; De, S.; Smith, R.J.; et al. Two-Dimensional Nanosheets Produced by Liquid Exfoliation of Layered Materials. Science 2011, 331, 568–571. [Google Scholar] [CrossRef] [PubMed]
- Fujie, T.; Okamura, Y.; Takeoka, S. Ubiquitous Transference of a Free—Standing Polysaccharide Nanosheet with the Development of a Nano-Adhesive Plaster. Adv. Mater. 2007, 19, 3549–3553. [Google Scholar] [CrossRef]
- Zhang, S.; Sunami, Y.; Hashimoto, H. Mini Review: Nanosheet Technology towards Biomedical Application. Nanomaterials 2017, 7, 246. [Google Scholar] [CrossRef] [PubMed]
- Novoselov, K.S.; Geim, A.K.; Morozov, S.V.; Jiang, D.; Zhang, Y.; Dubonos, S.V.; Grigorieva, I.V.; Firsov, A.A. Electric Field Effect in Atomically Thin Carbon Films. Science 2004, 306, 666–669. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Robinson, J.T.; Sun, X.; Dai, H. PEGylated Nano-Graphene Oxide for Delivery of Water Insoluble Cancer Drugs. J. Am. Chem. Soc. 2008, 130, 10876–10877. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Zeng, Z.; Li, H.; Li, F.; Fan, C.; Zhang, H. Single-Layer MoS2-Based Nanoprobes for Homogeneous Detection of Biomolecules. J. Am. Chem. Soc. 2013, 135, 5998–6001. [Google Scholar] [CrossRef] [PubMed]
- Fujie, T.; Ricotti, L.; Desii, A.; Menciassi, A.; Dario, P.; Mattoli, V. Evaluation of Substrata Effect on Cell Adhesion Properties Using Freestanding Poly(l-lactic acid) Nanosheets. Langmuir 2011, 27, 13173–13182. [Google Scholar] [CrossRef] [PubMed]
- Oudeng, G.; Au, M.; Shi, J.; Wen, C.; Yang, M. One-Step in Situ Detection of miRNA-21 Expression in Single Cancer Cells Based on Biofunctionalized MoS2 Nanosheets. ACS Appl. Mater. Interfaces 2018, 10, 350–360. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Bao, W.; Umar, A.; Wang, Q.; O’Hare, D.; Wan, Y. Delaminated Layered Double Hydroxide Nanosheets as an Efficient Vector for DNA Delivery. J. Biomed. Nanotechnol. 2016, 12, 922–933. [Google Scholar] [CrossRef] [PubMed]
- Berlin, J.M.; Leonard, A.D.; Pham, T.T.; Sano, D.; Marcano, D.C.; Yan, S.; Fiorentino, S.; Milas, Z.L.; Kosynkin, D.V.; Katherine Price, B.; et al. Effective Drug Delivery, in vitro and in vivo, By Carbon-Based Nanovectors Non-Covalently Loaded With Unmodified Paclitaxel. ACS Nano 2010, 4, 4621–4636. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Yuan, H.; von dem Bussche, A.; Creighton, M.; Hurt, R.H.; Kane, A.B.; Gao, H. Graphene microsheets enter cells through spontaneous membrane penetration at edge asperities and corner sites. Proc. Natl. Acad. Sci. USA 2013, 110, 12295–12300. [Google Scholar] [CrossRef] [PubMed]
- Komasa, S.; Kusumoto, T.; Taguchi, Y.; Nishizaki, H.; Sekino, T.; Umeda, M.; Okazaki, J.; Kawazoe, T. Effect of Nanosheet Surface Structure of Titanium Alloys on Cell Differentiation. J. Nanomater. 2014, 2014, 170. [Google Scholar] [CrossRef]
- Li, H.; Fierens, K.; Zhang, Z.; Vanparijs, N.; Schuijs, M.J.; Van Steendam, K.; Feiner Gracia, N.; De Rycke, R.; De Beer, T.; De Beuckelaer, A.; et al. Spontaneous Protein Adsorption on Graphene Oxide Nanosheets Allowing Efficient Intracellular Vaccine Protein Delivery. ACS Appl. Mater. Interfaces 2016, 8, 1147–1155. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, J.; Nagai, N.; Nishizawa, M.; Abe, T.; Kaji, H. Electrochemical manipulation of cell populations supported by biodegradable polymeric nanosheets for cell transplantation therapy. Biomater. Sci. 2017, 5, 216–222. [Google Scholar] [CrossRef] [PubMed]
- Kou, Z.; Wang, X.; Yuan, R.; Chen, H.; Zhi, Q.; Gao, L.; Wang, B.; Guo, Z.; Xue, X.; Cao, W.; et al. A promising gene delivery system developed from PEGylated MoS2 nanosheets for gene therapy. Nanoscale Res. Lett. 2014, 9, 587. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Z.; Fan, H.; Zhou, G.; Bai, H.; Liang, H.; Wang, R.; Zhang, X.; Tan, W. Activatable Fluorescence/MRI Bimodal Platform for Tumor Cell Imaging via MnO2 Nanosheet-Aptamer Nanoprobe. J. Am. Chem. Soc. 2014, 136, 11220–11223. [Google Scholar] [CrossRef] [PubMed]
- Dong, J.; Zhang, K.; Li, X.; Qian, Y.; Zhu, H.; Yuan, D.; Xu, Q.-H.; Jiang, J.; Zhao, D. Ultrathin two-dimensional porous organic nanosheets with molecular rotors for chemical sensing. Nat. Commun. 2017, 8, 1142. [Google Scholar] [CrossRef] [PubMed]
- Liang, Q.; Li, Z.; Bai, Y.; Huang, Z.-H.; Kang, F.; Yang, Q.-H. Reduced-sized monolayer carbon nitride nanosheets for highly improved photoresponse for cell imaging and photocatalysis. Sci. China Mater. 2017, 60, 109–118. [Google Scholar] [CrossRef]
- Brent, J.R.; Savjani, N.; O’Brien, P. Synthetic approaches to two-dimensional transition metal dichalcogenide nanosheets. Prog. Mater. Sci. 2017, 89, 411–478. [Google Scholar] [CrossRef]
- Sang, X.; Li, X.; Zhao, W.; Dong, J.; Rouleau, C.M.; Geohegan, D.B.; Ding, F.; Xiao, K.; Unocic, R.R. In situ edge engineering in two-dimensional transition metal dichalcogenides. Nat. Commun. 2018, 9, 2051. [Google Scholar] [CrossRef] [PubMed]
- Nurunnabi, M.; Nafiujjaman, M.; Lee, S.-J.; Park, I.-K.; Huh, K.M.; Lee, Y.-K. Preparation of ultra-thin hexagonal boron nitride nanoplates for cancer cell imaging and neurotransmitter sensing. Chem. Commun. 2016, 52, 6146–6149. [Google Scholar] [CrossRef] [PubMed]
- Xu, K.; Shen, X.; Chen, W.; Mu, C.; Jiang, C.; Zhao, Y.; Cai, K. Nanosheet-pore topographical titanium substrates: A biophysical regulator of the fate of mesenchymal stem cells. J. Mater. Chem. B 2016, 4, 1797–1810. [Google Scholar] [CrossRef]
- Komasa, S.; Yingmin, S.; Taguchi, Y.; Yamawaki, I.; Tsutsumi, Y.; Kusumoto, T.; Nishizaki, H.; Miyake, T.; Umeda, M.; Tanaka, M.; et al. Bioactivity of Titanium Surface Nanostructures Following Chemical Processing and Heat Treatment. J. Hard Tissue Biol. 2015, 24, 257–266. [Google Scholar] [CrossRef]
- Fujie, T.; Mori, Y.; Ito, S.; Nishizawa, M.; Bae, H.; Nagai, N.; Onami, H.; Abe, T.; Khademhosseini, A.; Kaji, H. Micropatterned Polymeric Nanosheets for Local Delivery of an Engineered Epithelial Monolayer. Adv. Mater. 2014, 26, 1699–1705. [Google Scholar] [CrossRef] [PubMed]
- Sharafeldin, M.; Bishop, G.W.; Bhakta, S.; El-Sawy, A.; Suib, S.L.; Rusling, J.F. Fe3O4 nanoparticles on graphene oxide sheets for isolation and ultrasensitive amperometric detection of cancer biomarker proteins. Biosens. Bioelectron. 2017, 91, 359–366. [Google Scholar] [CrossRef] [PubMed]
- Sabbaghi-Nadooshan, R.; Siasar Karbasaki, M. Diagnosis GLY120 Antigen for the Blood and Breast Cancers Using Graphene Nanosheet. Int. J. Nanosci. Nanotechnol. 2017, 13, 327–333. [Google Scholar]
- Suzuki, S.; Nishiwaki, K.; Takeoka, S.; Fujie, T. Large-Scale Fabrication of Porous Polymer Nanosheets for Engineering Hierarchical Cellular Organization. Adv. Mater. Technol. 2016, 1, 1600064. [Google Scholar] [CrossRef]
- Lee, W.C.; Loh, K.P.; Lim, C.T. When stem cells meet graphene: Opportunities and challenges in regenerative medicine. Biomaterials 2018, 155, 236–250. [Google Scholar]
- Okada, S.; Ito, H.; Nagai, A.; Komotori, J.; Imai, H. Adhesion of osteoblast-like cells on nanostructured hydroxyapatite. Acta Biomater. 2010, 6, 591–597. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, E.R.; Walter, M.N.M.; Reza, M.; Castelletto, V.; Ruokolainen, J.; Connon, C.J.; Alves, W.A.; Hamley, I.W. Self-Assembled Arginine-Capped Peptide Bolaamphiphile Nanosheets for Cell Culture and Controlled Wettability Surfaces. Biomacromolecules 2015, 16, 3180–3190. [Google Scholar] [CrossRef] [PubMed]
- Niwa, D.; Fujie, T.; Lang, T.; Goda, N.; Takeoka, S. Heterofunctional nanosheet controlling cell adhesion properties by collagen coating. J. Biomater. Appl. 2011, 27, 131–141. [Google Scholar] [CrossRef] [PubMed]
- Laurenti, M.; Al Subaie, A.; Abdallah, M.-N.; Cortes, A.R.G.; Ackerman, J.L.; Vali, H.; Basu, K.; Zhang, Y.L.; Murshed, M.; Strandman, S.; et al. Two-Dimensional Magnesium Phosphate Nanosheets Form Highly Thixotropic Gels That Up-Regulate Bone Formation. Nano Lett. 2016, 16, 4779–4787. [Google Scholar] [CrossRef] [PubMed]
- Shao, S.-Y.; Ming, P.-P.; Qiu, J.; Yu, Y.-J.; Yang, J.; Chen, J.-X.; Tang, C.-B. Modification of a SLA titanium surface with calcium-containing nanosheets and its effects on osteoblast behavior. RSC Adv. 2017, 7, 6753–6761. [Google Scholar] [CrossRef]
- Ma, Q.; Liao, J.; Tian, T.; Zhang, Q.; Cai, X. A potential flower-like coating consisting of calcium-phosphate nanosheets on titanium surface. Chin. Chem. Lett. 2017, 28, 1893–1896. [Google Scholar] [CrossRef]
- Kong, D.; Megone, W.; Nguyen, K.D.Q.; Di Cio, S.; Ramstedt, M.; Gautrot, J.E. Protein Nanosheet Mechanics Controls Cell Adhesion and Expansion on Low-Viscosity Liquids. Nano Lett. 2018, 18, 1946–1951. [Google Scholar] [CrossRef] [PubMed]
- Sun, C.; Wakefield, D.L.; Han, Y.; Muller, D.A.; Holowka, D.A.; Baird, B.A.; Dichtel, W.R. Graphene Oxide Nanosheets Stimulate Ruffling and Shedding of Mammalian Cell Plasma Membranes. Chem 2016, 1, 273–286. [Google Scholar] [CrossRef] [PubMed]
- Tian, X.; Yang, Z.; Duan, G.; Wu, A.; Gu, Z.; Zhang, L.; Chen, C.; Chai, Z.; Ge, C.; Zhou, R. Graphene Oxide Nanosheets Retard Cellular Migration via Disruption of Actin Cytoskeleton. Small 2016, 13, 1602133. [Google Scholar] [CrossRef] [PubMed]
- Pan, Y.-T.; Smith, C.E.; Kwok, K.S.; Chen, J.; Kong, H.; Yang, H. Functionalized ultrathin palladium nanosheets as patches for HepG2 cancer cells. Chem. Commun. 2015, 51, 14171–14174. [Google Scholar] [CrossRef] [PubMed]
- Gu, Z.; Li, W.; Hong, L.; Zhou, R. Exploring biological effects of MoS2 nanosheets on native structures of α-helical peptides. J. Chem. Phys. 2016, 144, 175103. [Google Scholar] [CrossRef] [PubMed]
- Sasidharan, A.; Panchakarla, L.S.; Chandran, P.; Menon, D.; Nair, S.; Rao, C.N.R.; Koyakutty, M. Differential nano-bio interactions and toxicity effects of pristine versus functionalized graphene. Nanoscale 2011, 3, 2461–2464. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; Zhu, S.; Wang, M.; Li, Y.; Shi, P.; Huang, X. Delivery of Paclitaxel Using PEGylated Graphene Oxide as a Nanocarrier. ACS Appl. Mater. Interfaces 2015, 7, 1355–1363. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Davis, C.; Cai, W.; He, L.; Chen, X.; Dai, H. Circulation and long-term fate of functionalized, biocompatible single-walled carbon nanotubes in mice probed by Raman spectroscopy. Proc. Natl. Acad. Sci. USA 2008, 105, 1410–1415. [Google Scholar] [CrossRef] [PubMed]
- Sacchetti, C.; Motamedchaboki, K.; Magrini, A.; Palmieri, G.; Mattei, M.; Bernardini, S.; Rosato, N.; Bottini, N.; Bottini, M. Surface Polyethylene Glycol Conformation Influences the Protein Corona of Polyethylene Glycol-Modified Single-Walled Carbon Nanotubes: Potential Implications on Biological Performance. ACS Nano 2013, 7, 1974–1989. [Google Scholar] [CrossRef] [PubMed]
- Luo, N.; Weber, J.K.; Wang, S.; Luan, B.; Yue, H.; Xi, X.; Du, J.; Yang, Z.; Wei, W.; Zhou, R.; et al. PEGylated graphene oxide elicits strong immunological responses despite surface passivation. Nat. Commun. 2017, 8, 14537. [Google Scholar] [CrossRef] [PubMed]
- Xu, M.; Zhu, J.; Wang, F.; Xiong, Y.; Wu, Y.; Wang, Q.; Weng, J.; Zhang, Z.; Chen, W.; Liu, S. Improved In Vitro and In Vivo Biocompatibility of Graphene Oxide through Surface Modification: Poly(Acrylic Acid)-Functionalization is Superior to PEGylation. ACS Nano 2016, 10, 3267–3281. [Google Scholar] [CrossRef] [PubMed]
- Thumann, G.; Viethen, A.; Gaebler, A.; Walter, P.; Kaempf, S.; Johnen, S.; Salz, A.K. The in vitro and in vivo behaviour of retinal pigment epithelial cells cultured on ultrathin collagen membranes. Biomaterials 2009, 30, 287–294. [Google Scholar] [CrossRef] [PubMed]
- Stanzel, B.V.; Liu, Z.; Brinken, R.; Braun, N.; Holz, F.G.; Eter, N. Subretinal Delivery of Ultrathin Rigid-Elastic Cell Carriers Using a Metallic Shooter Instrument and Biodegradable Hydrogel Encapsulation. Investig. Ophthalmol. Vis. Sci. 2012, 53, 490–500. [Google Scholar] [CrossRef] [PubMed]
- Tao, S.; Young, C.; Redenti, S.; Zhang, Y.; Klassen, H.; Desai, T.; Young, M.J. Survival, migration and differentiation of retinal progenitor cells transplanted on micro-machined poly(methyl methacrylate) scaffolds to the subretinal space. Lab Chip 2007, 7, 695–701. [Google Scholar] [CrossRef] [PubMed]
- Chi, H.; Gu, Y.; Xu, T.; Cao, F. Multifunctional organic-inorganic hybrid nanoparticles and nanosheets based on chitosan derivative and layered double hydroxide: Cellular uptake mechanism and application for topical ocular drug delivery. Int. J. Nanomed. 2017, 12, 1607–1620. [Google Scholar] [CrossRef] [PubMed]
- Xie, M.; Zhang, F.; Liu, L.; Zhang, Y.; Li, Y.; Li, H.; Xie, J. Surface modification of graphene oxide nanosheets by protamine sulfate/sodium alginate for anti-cancer drug delivery application. Appl. Surf. Sci. 2018, 440, 853–860. [Google Scholar] [CrossRef]
- Tao, W.; Zhu, X.; Yu, X.; Zeng, X.; Xiao, Q.; Zhang, X.; Ji, X.; Wang, X.; Shi, J.; Zhang, H.; et al. Black Phosphorus Nanosheets as a Robust Delivery Platform for Cancer Theranostics. Adv. Mater. 2016, 29, 1603276. [Google Scholar] [CrossRef] [PubMed]
- Li, B.L.; Setyawati, M.I.; Chen, L.; Xie, J.; Ariga, K.; Lim, C.-T.; Garaj, S.; Leong, D.T. Directing Assembly and Disassembly of 2D MoS2 Nanosheets with DNA for Drug Delivery. ACS Appl. Mater. Interfaces 2017, 9, 15286–15296. [Google Scholar] [CrossRef] [PubMed]
- Dowaidar, M.; Abdelhamid, H.N.; Hällbrink, M.; Zou, X.; Langel, Ü. Graphene oxide nanosheets in complex with cell penetrating peptides for oligonucleotides delivery. Biochim. Biophys. Acta (BBA) Gen. Subj. 2017, 1861, 2334–2341. [Google Scholar] [CrossRef] [PubMed]
- Ji, Q.; Yamazaki, T.; Hanagata, N.; Lee, M.V.; Hill, J.P.; Ariga, K. Silica-based gene reverse transfection: An upright nanosheet network for promoted DNA delivery to cells. Chem. Commun. 2012, 48, 8496–8498. [Google Scholar] [CrossRef] [PubMed]
- Huang, N.-C.; Ji, Q.; Ariga, K.; Hsu, S.-H. Nanosheet transfection: Effective transfer of naked DNA on silica glass. NPG Asia Mater. 2015, 7, e184. [Google Scholar] [CrossRef]
- Nagrath, S.; Sequist, L.V.; Maheswaran, S.; Bell, D.W.; Irimia, D.; Ulkus, L.; Smith, M.R.; Kwak, E.L.; Digumarthy, S.; Muzikansky, A.; et al. Isolation of rare circulating tumour cells in cancer patients by microchip technology. Nature 2007, 450, 1235–1239. [Google Scholar] [CrossRef] [PubMed]
- Saucedo-Zeni, N.; Mewes, S.; Niestroj, R.; Gasiorowski, L.; Murawa, D.; Nowaczyk, P.; Tomasi, T.; Weber, E.; Dworacki, G.; Morgenthaler, N.G.; et al. A novel method for the in vivo isolation of circulating tumor cells from peripheral blood of cancer patients using a functionalized and structured medical wire. Int. J. Oncol. 2012, 41, 1241–1250. [Google Scholar] [PubMed]
- Asadian-Birjand, M.; Biglione, C.; Bergueiro, J.; Cappelletti, A.; Rahane, C.; Chate, G.; Khandare, J.; Klemke, B.; Strumia Miriam, C.; Calderón, M. Transferrin Decorated Thermoresponsive Nanogels as Magnetic Trap Devices for Circulating Tumor Cells. Macromol. Rapid Commun. 2015, 37, 439–445. [Google Scholar] [CrossRef] [PubMed]
- Zheng, X.; Cheung, L.S.-L.; Schroeder, J.A.; Jiang, L.; Zohar, Y. A high-performance microsystem for isolating circulating tumor cells. Lab Chip 2011, 11, 3269–3276. [Google Scholar] [CrossRef] [PubMed]
- Ozkumur, E.; Shah, A.M.; Ciciliano, J.C.; Emmink, B.L.; Miyamoto, D.T.; Brachtel, E.; Yu, M.; Chen, P.-I.; Morgan, B.; Trautwein, J.; et al. Inertial Focusing for Tumor Antigen–Dependent and –Independent Sorting of Rare Circulating Tumor Cells. Sci. Transl. Med. 2013, 5, 179ra47. [Google Scholar] [CrossRef] [PubMed]
- Yoon, H.J.; Kozminsky, M.; Nagrath, S. Emerging Role of Nanomaterials in Circulating Tumor Cell Isolation and Analysis. ACS Nano 2014, 8, 1995–2017. [Google Scholar] [CrossRef] [PubMed]
- Bardhan, N.M.; Kumar, P.V.; Li, Z.; Ploegh, H.L.; Grossman, J.C.; Belcher, A.M.; Chen, G.-Y. Enhanced Cell Capture on Functionalized Graphene Oxide Nanosheets through Oxygen Clustering. ACS Nano 2017, 11, 1548–1558. [Google Scholar] [CrossRef] [PubMed]
- Yoon, H.J.; Kim, T.H.; Zhang, Z.; Azizi, E.; Pham, T.M.; Paoletti, C.; Lin, J.; Ramnath, N.; Wicha, M.S.; Hayes, D.F.; et al. Sensitive capture of circulating tumour cells by functionalized graphene oxide nanosheets. Nat. Nanotechnol. 2013, 8, 735–741. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.-Y.; Li, Z.; Theile, C.S.; Bardhan, N.M.; Kumar, P.V.; Duarte, J.N.; Maruyama, T.; Rashidfarrokh, A.; Belcher, A.M.; Ploegh, H.L. Graphene Oxide Nanosheets Modified with Single Domain Antibodies for Rapid and Efficient Capture of Cells. Chemistry 2015, 21, 17178–17183. [Google Scholar] [CrossRef] [PubMed]
- Ou, M.; Huang, J.; Yang, X.; Quan, K.; Yang, Y.; Xie, N.; Wang, K. MnO2 nanosheet mediated “DD–A” FRET binary probes for sensitive detection of intracellular mRNA. Chem. Sci. 2017, 8, 668–673. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.; Kong, X.J.; Yu, R.Q.; Chen, T.T.; Chu, X. MnO2Nanosheet-based Fluorescence Sensing Platform for Sensitive Detection of Endonuclease. Anal. Sci. 2017, 33, 783–788. [Google Scholar] [CrossRef] [PubMed]
- Tanveer, A.T.; Md Zahidul, I.P.; Hasan, H.; Alma, A.M.R.; Trefa, M.A.; Jacqueline, L.W.; Shaowei, Z. In vitro toxic effects of reduced graphene oxide nanosheets on lung cancer cells. Nanotechnology 2017, 28, 504001. [Google Scholar]
- Thirumalraj, B.; Dhenadhayalan, N.; Chen, S.-M.; Liu, Y.-J.; Chen, T.-W.; Liang, P.-H.; Lin, K.-C. Highly sensitive fluorogenic sensing of L-Cysteine in live cells using gelatin-stabilized gold nanoparticles decorated graphene nanosheets. Sens. Actuators B Chem. 2018, 259, 339–346. [Google Scholar] [CrossRef]
- Thangasamy, P.; Santhanam, M.; Sathish, M. Supercritical Fluid Facilitated Disintegration of Hexagonal Boron Nitride Nanosheets to Quantum Dots and Its Application in Cells Imaging. ACS Appl. Mater. Interfaces 2016, 8, 18647–18651. [Google Scholar] [CrossRef] [PubMed]
- Olivier, G.K.; Cho, A.; Sanii, B.; Connolly, M.D.; Tran, H.; Zuckermann, R.N. Antibody-Mimetic Peptoid Nanosheets for Molecular Recognition. ACS Nano 2013, 7, 9276–9286. [Google Scholar] [CrossRef] [PubMed]
- Ohshima, H.; Tatemichi, M.; Sawa, T. Chemical basis of inflammation-induced carcinogenesis. Arch. Biochem. Biophys. 2003, 417, 3–11. [Google Scholar] [CrossRef]
- Maruyama, W.; Dostert, P.; Matsubara, K.; Naoi, M. N-methyl(r)salsolinol produces hydroxyl radicals: Involvement to neurotoxicity. Free Radic. Biol. Med. 1995, 19, 67–75. [Google Scholar] [CrossRef]
- Amatore, C.; Arbault, S.; Bruce, D.; de Oliveira, P.; Erard, M.; Vuillaume, M. Characterization of the Electrochemical Oxidation of Peroxynitrite: Relevance to Oxidative Stress Bursts Measured at the Single Cell Level. Chem. Eur. J. 2001, 7, 4171–4179. [Google Scholar] [CrossRef]
- Miller, E.W.; Albers, A.E.; Pralle, A.; Isacoff, E.Y.; Chang, C.J. Boronate-Based Fluorescent Probes for Imaging Cellular Hydrogen Peroxide. J. Am. Chem. Soc. 2005, 127, 16652–16659. [Google Scholar] [CrossRef] [PubMed]
- Bai, J.; Jiang, X. A Facile One-Pot Synthesis of Copper Sulfide-Decorated Reduced Graphene Oxide Composites for Enhanced Detecting of H2O2 in Biological Environments. Anal. Chem. 2013, 85, 8095–8101. [Google Scholar] [CrossRef] [PubMed]
- Tang, J.; Quan, Y.; Zhang, Y.; Jiang, M.; Al-Enizi, A.M.; Kong, B.; An, T.; Wang, W.; Xia, L.; Gong, X.; et al. Three-dimensional WS2 nanosheet networks for H2O2 produced for cell signaling. Nanoscale 2016, 8, 5786–5792. [Google Scholar] [CrossRef] [PubMed]
- Qi, M.; Zhang, Y.; Cao, C.; Zhang, M.; Liu, S.; Liu, G. Decoration of Reduced Graphene Oxide Nanosheets with Aryldiazonium Salts and Gold Nanoparticles toward a Label-Free Amperometric Immunosensor for Detecting Cytokine Tumor Necrosis Factor-α in Live Cells. Anal. Chem. 2016, 88, 9614–9621. [Google Scholar] [CrossRef] [PubMed]
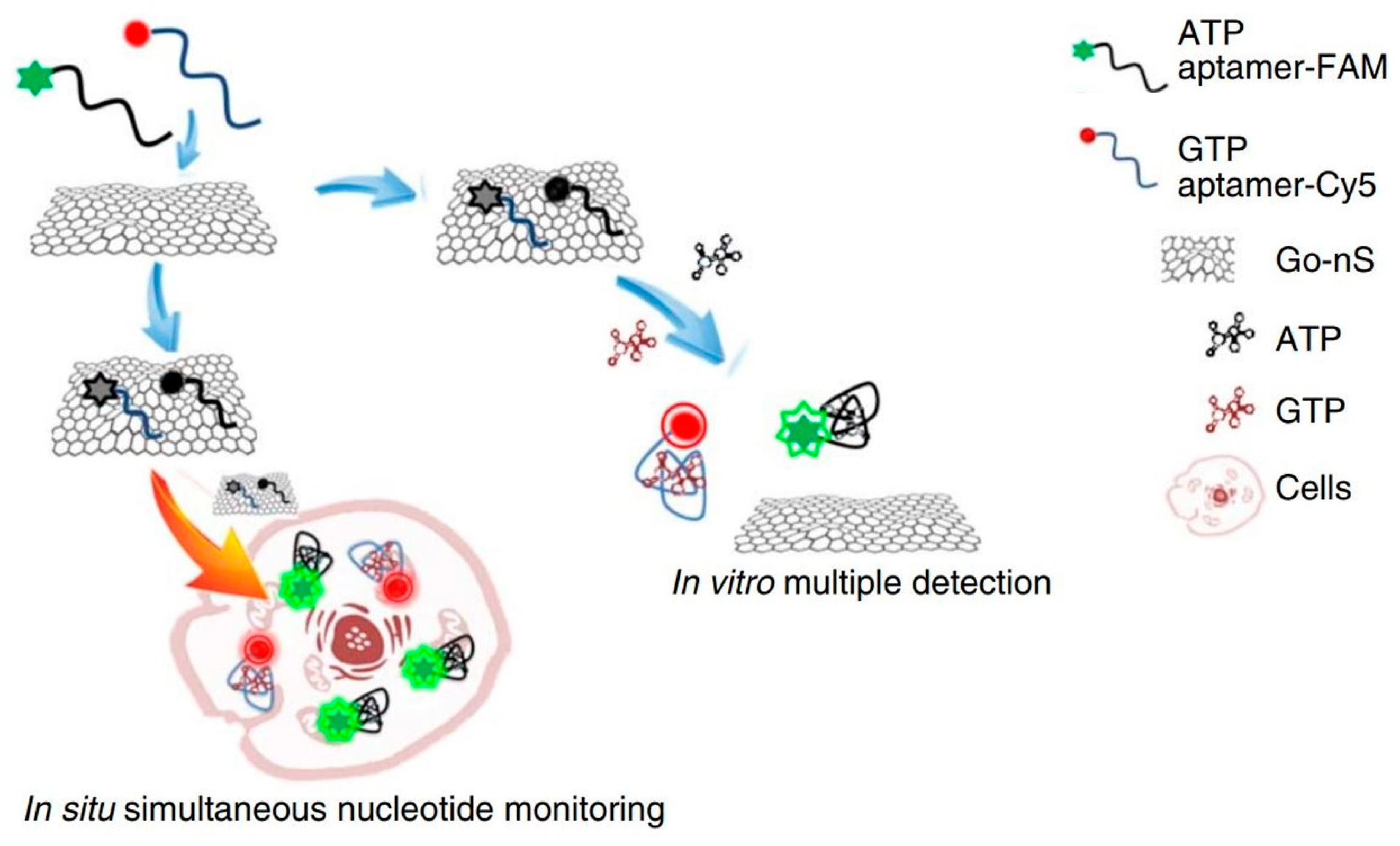
- Wang, Y.; Tang, L.; Li, Z.; Lin, Y.; Li, J. In situ simultaneous monitoring of ATP and GTP using a graphene oxide nanosheet–based sensing platform in living cells. Nat. Protoc. 2014, 9, 1944–1955. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Ishida, Y.; Ebina, Y.; Sasaki, T.; Hikima, T.; Takata, M.; Aida, T. An anisotropic hydrogel with electrostatic repulsion between cofacially aligned nanosheets. Nature 2014, 517, 68–72. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Yu, J.; Chang, H. Two dimensional nanosheets as conductive, flexible elements in biomaterials. J. Mater. Chem. B 2015, 3, 4959–4964. [Google Scholar] [CrossRef]
- Shuai, C.; Han, Z.; Feng, P.; Gao, C.; Xiao, T.; Peng, S. Akermanite scaffolds reinforced with boron nitride nanosheets in bone tissue engineering. J. Mater. Sci. Mater. Med. 2015, 26, 188. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Li, T.; Ma, H.; Zhai, D.; Jiang, C.; Chang, J.; Wang, J.; Wu, C. A 3D-printed scaffold with MoS2 nanosheets for tumor therapy and tissue regeneration. NPG Asia Mater. 2017, 9, e376. [Google Scholar] [CrossRef]
- Chueng, S.-T.D.; Yang, L.; Zhang, Y.; Lee, K.-B. Multidimensional nanomaterials for the control of stem cell fate. Nano Converg. 2016, 3, 23. [Google Scholar] [CrossRef] [PubMed]
- Jing, G.; Wang, Z.; Zhuang, X.; He, X.; Wu, H.; Wang, Q.; Cheng, L.; Liu, Z.; Wang, S.; Zhu, R. Suspended graphene oxide nanosheets maintain the self-renewal of mouse embryonic stem cells via down-regulating the expression of Vinculin. Biomaterials 2018, 171, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Bressan, E.; Ferroni, L.; Gardin, C.; Sbricoli, L.; Gobbato, L.; Ludovichetti, F.S.; Tocco, I.; Carraro, A.; Piattelli, A.; Zavan, B. Graphene based scaffolds effects on stem cells commitment. J. Transl. Med. 2014, 12, 296. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.C.; Lim, C.H.Y.X.; Shi, H.; Tang, L.A.L.; Wang, Y.; Lim, C.T.; Loh, K.P. Origin of Enhanced Stem Cell Growth and Differentiation on Graphene and Graphene Oxide. ACS Nano 2011, 5, 7334–7341. [Google Scholar] [CrossRef] [PubMed]
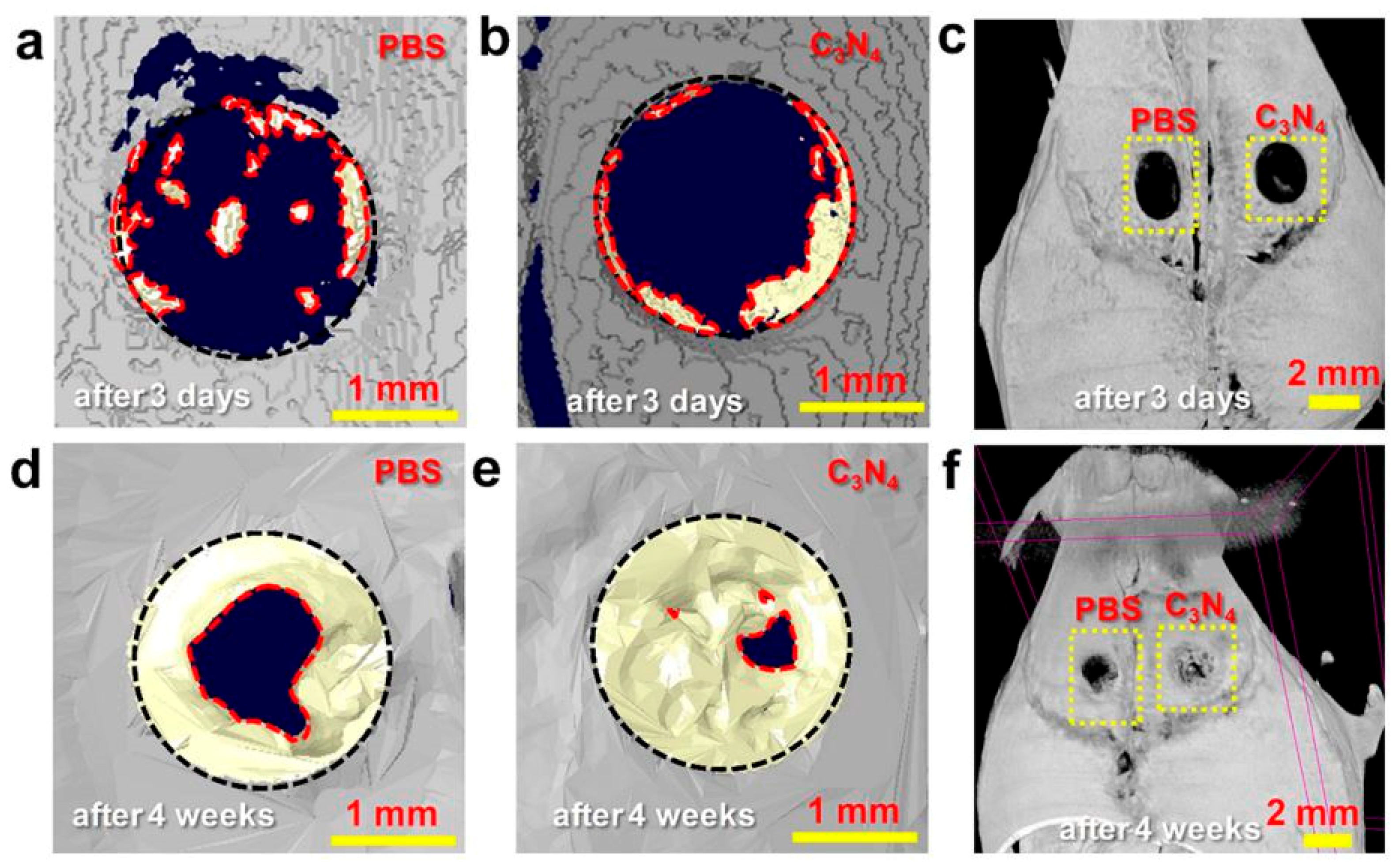
- Tiwari, J.N.; Seo, Y.-K.; Yoon, T.; Lee, W.G.; Cho, W.J.; Yousuf, M.; Harzandi, A.M.; Kang, D.-S.; Kim, K.-Y.; Suh, P.-G.; et al. Accelerated Bone Regeneration by Two-Photon Photoactivated Carbon Nitride Nanosheets. ACS Nano 2017, 11, 742–751. [Google Scholar] [CrossRef] [PubMed]
- Mayor, S.; Pagano, R.E. Pathways of clathrin-independent endocytosis. Nat. Rev. Mol. Cell Biol. 2007, 8, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Matesanz, M.-C.; Vila, M.; Feito, M.-J.; Linares, J.; Gonçalves, G.; Vallet-Regi, M.; Marques, P.-A.A.; Portolés, M.-T. The effects of graphene oxide nanosheets localized on F-actin filaments on cell-cycle alterations. Biomaterials 2013, 34, 1562–1569. [Google Scholar] [CrossRef] [PubMed]
- Linares, J.; Matesanz, M.C.; Vila, M.; Feito, M.J.; Gonçalves, G.; Vallet-Regí, M.; Marques, P.-A.A.; Portolés, M.T. Endocytic Mechanisms of Graphene Oxide Nanosheets in Osteoblasts, Hepatocytes and Macrophages. ACS Appl. Mater. Interfaces 2014, 6, 13697–13706. [Google Scholar] [CrossRef] [PubMed]
- Mu, Q.; Su, G.; Li, L.; Gilbertson, B.O.; Yu, L.H.; Zhang, Q.; Sun, Y.-P.; Yan, B. Size-Dependent Cell Uptake of Protein-Coated Graphene Oxide Nanosheets. ACS Appl. Mater. Interfaces 2012, 4, 2259–2266. [Google Scholar] [CrossRef] [PubMed]
- Bramini, M.; Sacchetti, S.; Armirotti, A.; Rocchi, A.; Vázquez, E.; León Castellanos, V.; Bandiera, T.; Cesca, F.; Benfenati, F. Graphene Oxide Nanosheets Disrupt Lipid Composition, Ca2+ Homeostasis, and Synaptic Transmission in Primary Cortical Neurons. ACS Nano 2016, 10, 7154–7171. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Shen, S.; Liu, Z.; Ji, M. Label-Free, Quantitative Imaging of MoS2-Nanosheets in Live Cells with Simultaneous Stimulated Raman Scattering and Transient Absorption Microscopy. Adv. Biosyst. 2017, 1, 1700013. [Google Scholar] [CrossRef]
- Li, Y.; Lu, Z.; Li, Z.; Nie, G.; Fang, Y. Cellular uptake and distribution of graphene oxide coated with layer-by-layer assembled polyelectrolytes. J. Nanopart. Res. 2014, 16, 2384. [Google Scholar] [CrossRef]
- Jin, C.; Wang, F.; Tang, Y.; Zhang, X.; Wang, J.; Yang, Y. Distribution of Graphene Oxide and TiO2-Graphene Oxide Composite in A549 Cells. Biol. Trace Elem. Res. 2014, 159, 393–398. [Google Scholar] [CrossRef] [PubMed]
- Zhang, B.; Wei, P.; Zhou, Z.; Wei, T. Interactions of graphene with mammalian cells: Molecular mechanisms and biomedical insights. Adv. Drug Deliv. Rev. 2016, 105, 145–162. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Wu, Q.; Zhao, Y.; Bai, Y.; Chen, P.; Xia, T.; Wang, D. Response of MicroRNAs to In Vitro Treatment with Graphene Oxide. ACS Nano 2014, 8, 2100–2110. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Liu, Y.; Fu, Y.; Wei, T.; Le Guyader, L.; Gao, G.; Liu, R.-S.; Chang, Y.-Z.; Chen, C. The triggering of apoptosis in macrophages by pristine graphene through the MAPK and TGF-beta signaling pathways. Biomaterials 2012, 33, 402–411. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.-D.; Chen, J.; Min, Y.; Park Gyeong, B.; Shen, X.; Song, S.-S.; Sun, Y.-M.; Wang, H.; Long, W.; Xie, J.; et al. Metabolizable Bi2Se3 Nanoplates: Biodistribution, Toxicity, and Uses for Cancer Radiation Therapy and Imaging. Adv. Funct. Mater. 2013, 24, 1718–1729. [Google Scholar] [CrossRef]
- Yin, F.; Hu, K.; Chen, Y.; Yu, M.; Wang, D.; Wang, Q.; Yong, K.-T.; Lu, F.; Liang, Y.; Li, Z. SiRNA Delivery with PEGylated Graphene Oxide Nanosheets for Combined Photothermal and Genetherapy for Pancreatic Cancer. Theranostics 2017, 7, 1133–1148. [Google Scholar] [CrossRef] [PubMed]
- Zhou, T.; Zhang, B.; Wei, P.; Du, Y.; Zhou, H.; Yu, M.; Yan, L.; Zhang, W.; Nie, G.; Chen, C.; et al. Energy metabolism analysis reveals the mechanism of inhibition of breast cancer cell metastasis by PEG-modified graphene oxide nanosheets. Biomaterials 2014, 35, 9833–9843. [Google Scholar] [CrossRef] [PubMed]
- Gerweck, L.E.; Seetharaman, K. Cellular pH Gradient in Tumor versus Normal Tissue: Potential Exploitation for the Treatment of Cancer. Cancer Res. 1996, 56, 1194–1198. [Google Scholar] [PubMed]
- Hao, Y.; Wang, L.; Zhang, B.; Li, D.; Meng, D.; Shi, J.; Zhang, H.; Zhang, Z.; Zhang, Y. Manganese dioxide nanosheets-based redox/pH-responsive drug delivery system for cancer theranostic application. Int. J. Nanomed. 2016, 11, 1759–1778. [Google Scholar]
- Miao, W.; Shim, G.; Lee, S.; Lee, S.; Choe, Y.S.; Oh, Y.-K. Safety and tumor tissue accumulation of pegylated graphene oxide nanosheets for co-delivery of anticancer drug and photosensitizer. Biomaterials 2013, 34, 3402–3410. [Google Scholar] [CrossRef] [PubMed]
- Desgrosellier, J.S.; Cheresh, D.A. Integrins in cancer: Biological implications and therapeutic opportunities. Nat. Rev. Cancer 2010, 10, 9–22. [Google Scholar] [CrossRef] [PubMed]
- Song, Z.; Chang, Y.; Xie, H.; Yu, X.-F.; Chu, P.K.; Chen, T. Decorated ultrathin bismuth selenide nanosheets as targeted theranostic agents for in vivo imaging guided cancer radiation therapy. NPG Asia Mater. 2017, 9, e439. [Google Scholar] [CrossRef]
- Li, Z.; Shao, J.; Luo, Q.; Yu, X.-F.; Xie, H.; Fu, H.; Tang, S.; Wang, H.; Han, G.; Chu, P.K. Cell-borne 2D nanomaterials for efficient cancer targeting and photothermal therapy. Biomaterials 2017, 133, 37–48. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wei, Y.; Shi, X.; Gao, H. Cellular entry of graphene nanosheets: The role of thickness, oxidation and surface adsorption. RSC Adv. 2013, 3, 15776–15782. [Google Scholar] [CrossRef]
- Mao, J.; Guo, R.T.; Yan, L. Simulation and analysis of cellular internalization pathways and membrane perturbation for graphene nanosheets. Biomaterials 2014, 35, 6069–6077. [Google Scholar] [CrossRef] [PubMed]
- Yang, W.; Zhang, X.; Xie, Y. Advances and challenges in chemistry of two-dimensional nanosheets. Nano Today 2016, 11, 793–816. [Google Scholar] [CrossRef]
- Shen, J.; Zhu, Y.; Jiang, H.; Li, C. 2D nanosheets-based novel architectures: Synthesis, assembly, and applications. Nano Today 2016, 11, 483–520. [Google Scholar] [CrossRef]
- Xie, W.; Zhu, X.; Xu, S.; Yi, S.; Guo, Z.; Kuang, J.; Deng, Y. Cost-effective fabrication of graphene-like nanosheets from natural microcrystalline graphite minerals by liquid oxidation-reduction method. RSC Adv. 2017, 7, 32008–32019. [Google Scholar] [CrossRef]
- Kim, K.S.; Zhao, Y.; Jang, H.; Lee, S.Y.; Kim, J.M.; Kim, K.S.; Ahn, J.-H.; Kim, P.; Choi, J.-Y.; Hong, B.H. Large-scale pattern growth of graphene films for stretchable transparent electrodes. Nature 2009, 457, 706–710. [Google Scholar] [CrossRef] [PubMed]
- Tetlow, H.; Posthuma de Boer, J.; Ford, I.J.; Vvedensky, D.D.; Coraux, J.; Kantorovich, L. Growth of epitaxial graphene: Theory and experiment. Phys. Rep. 2014, 542, 195–295. [Google Scholar] [CrossRef]
- McAllister, M.J.; Li, J.-L.; Adamson, D.H.; Schniepp, H.C.; Abdala, A.A.; Liu, J.; Herrera-Alonso, M.; Milius, D.L.; Car, R.; Prud’homme, R.K.; et al. Single Sheet Functionalized Graphene by Oxidation and Thermal Expansion of Graphite. Chem. Mater. 2007, 19, 4396–4404. [Google Scholar] [CrossRef]
- Faggio, G.; Capasso, A.; Messina, G.; Santangelo, S.; Dikonimos, T.; Gagliardi, S.; Giorgi, R.; Morandi, V.; Ortolani, L.; Lisi, N. High-Temperature Growth of Graphene Films on Copper Foils by Ethanol Chemical Vapor Deposition. J. Phys. Chem. C 2013, 117, 21569–21576. [Google Scholar] [CrossRef]
- Ping, G.; Zhang, J.; Cheng, J.; Shi, L. Graphene nanosheets prepared by low-temperature exfoliation and reduction technique toward fabrication of high-performance poly(1-butene)/graphene films. Iran. Polym. J. 2017, 26, 55–69. [Google Scholar] [CrossRef]
- Kuilla, T.; Bhadra, S.; Yao, D.; Kim, N.H.; Bose, S.; Lee, J.H. Recent advances in graphene based polymer composites. Prog. Polym. Sci. 2010, 35, 1350–1375. [Google Scholar] [CrossRef]
- Guo, X.; Mei, N. Assessment of the toxic potential of graphene family nanomaterials. J. Food Drug Anal. 2014, 22, 105–115. [Google Scholar] [CrossRef] [PubMed]
- Yue, H.; Wei, W.; Yue, Z.; Wang, B.; Luo, N.; Gao, Y.; Ma, D.; Ma, G.; Su, Z. The role of the lateral dimension of graphene oxide in the regulation of cellular responses. Biomaterials 2012, 33, 4013–4021. [Google Scholar] [CrossRef] [PubMed]
- Kurapati, R.; Kostarelos, K.; Prato, M.; Bianco, A. Biomedical Uses for 2D Materials Beyond Graphene: Current Advances and Challenges Ahead. Adv. Mater. 2016, 28, 6052–6074. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.; Peng, R. Growth and Follow-Up of Primary Cortical Neuron Cells on Nonfunctionalized Graphene Nanosheet Film. J. Appl. Biomater. Funct. Mater. 2016, 14, 26–34. [Google Scholar] [CrossRef] [PubMed]
- Antoni, D.; Burckel, H.; Josset, E.; Noel, G. Three-Dimensional Cell Culture: A Breakthrough in Vivo. Int. J. Mol. Sci. 2015, 16, 5517–5527. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Hu, J.; Athanasiou, K.A. The Role of Tissue Engineering in Articular Cartilage Repair and Regeneration. Crit. Rev. Biomed. Eng. 2009, 37, 1–57. [Google Scholar] [CrossRef] [PubMed]
- Nel, A.E.; Madler, L.; Velegol, D.; Xia, T.; Hoek, E.M.; Somasundaran, P.; Klaessig, F.; Castranova, V.; Thompson, M. Understanding biophysicochemical interactions at the nano-bio interface. Nat. Mater. 2009, 8, 543–557. [Google Scholar] [CrossRef] [PubMed]
| Materials | Modification/ Functionalization/FABrication | Applications | Effectiveness | Ref. | |
|---|---|---|---|---|---|
| Cell adhesion | RFL4FR | ̶ | Improved adhesion/growth of hCSF cells | Wettability enhancement | [31] |
| PLLA | Collagen coating | Adhesion of NIH3T3 cell line | [32] | ||
| Calcium-phosphate nanosheet + titanium | ̶ | Improved adhesion of osteoblast cell | Wettability enhancement | [35] | |
| Delivery substrate | PLGA | Engineered cell monolayer on surface | Injection into subretinal space together with cells | Small size; high flexibility and biodegradability | [25] |
| BP | Modification with polyethylene glycol-amine | Drug and dye carrier | Targeted cancer therapy | [52] | |
| GO | Cell-penetrating peptides | Plasmid transfection into Hela cells | Cytotoxicity reduction and biocompatibility improvement | [54] | |
| Cell capturing | GO | NeutrAvidin (cancer-related biomarker) coating | Capturing of cancer cells: MCF-7, Hs-578T, and PC-3 | Sensitive, microfluidic-free, and planar | [64] |
| GO | A phase transformation through oxygen clustering | Capturing of Class-II MHC-positive cells | Sensitive, microfluidic-free, and planar | [63] | |
| GO | Coating with VHH7 and VHH DC 13 | Capturing of Class II MHC-eGFP+ and CD11b+ cells | Effective, rapid, and microfluidic-free | [65] | |
| Cell sensing /imaging | WS2 | Three-dimensional reconstruction | Sensing of H2O2 in living RAW 264.7 macrophage cells | Effective in a three-dimensional structure | [77] |
| Reduced GO | Decoration with gold nanoparticles and aryldiazonium salts | Sensing of TNF-α secreted by live BV-2 cells | High sensitivity and stability | [78] | |
| MnO2 | In combination with fluorescent probe | Tumor cell imaging after cell uptake | Fluorescence off/on switch | [17] | |
| Scaffold elements | Akermanite + boron nitride nanosheets (BNNSs) | Fabrication technique: selective laser sintering system | In vivo-like microenvironment for MG63 osteoblast-like cells | Increased compressive strength and fracture toughness | [82] |
| Polymer ethyl acetate solution (poly(d,l-lactic acid) and polystyrene) | Fabrication technique: gravure coating and polymer-based phase separation | Application as a basement membrane for the cell–cell (C2C12 myoblasts) communication | Porous nanosheets | [28] | |
| PLGA | Self-assemble monolayer of L-cysteine | Transplantation of cells on PLGA | PLGA detachment from substrate in response to a negative electrical potential | [15] | |
| Stem cell differentiation and tissue regeneration | GO | ̶ | Sustaining the self-renewal of mouse embryonic stem cells | A signaling pathway involving integrin | [85] |
| GO | ̶ | Differentiation of MSCs to adipogenesis | High affinity of insulin resulting from H-bonding and electrostatic interactions | [87] | |
| C3N4 nanosheets | ̶ | Accelerated bone regeneration | Increase of cytosolic Ca2+ by photoinduced charge transfer | [88] | |
| Internalization and redistribution of nanosheets and cellular organelles | GO | PEGylation + FITC | Investigation of cellular distribution | Co-localization with F-actin filaments | [90] |
| GO or TiO2–GO composite | ̶ | Investigation of cytotoxicity on A549 cells | Internalization and entry into the cytoplasm and nucleus | [96] | |
| Pristine graphene | ̶ | Investigation of the biological effects on murine RAW 264.7 macrophages | Redistribution of pro-apoptotic mitochondrial factors | [99] | |
| GO | PEGylation | A potential anti-metastatic agent | Impairment of mitochondrial oxidative phosphorylation | [102] |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, W.; Sunami, Y.; Kimura, H.; Zhang, S. Applications of Nanosheets in Frontier Cellular Research. Nanomaterials 2018, 8, 519. https://doi.org/10.3390/nano8070519
Huang W, Sunami Y, Kimura H, Zhang S. Applications of Nanosheets in Frontier Cellular Research. Nanomaterials. 2018; 8(7):519. https://doi.org/10.3390/nano8070519
Chicago/Turabian StyleHuang, Wenjing, Yuta Sunami, Hiroshi Kimura, and Sheng Zhang. 2018. "Applications of Nanosheets in Frontier Cellular Research" Nanomaterials 8, no. 7: 519. https://doi.org/10.3390/nano8070519
APA StyleHuang, W., Sunami, Y., Kimura, H., & Zhang, S. (2018). Applications of Nanosheets in Frontier Cellular Research. Nanomaterials, 8(7), 519. https://doi.org/10.3390/nano8070519






