Green Prescriptions and Their Co-Benefits: Integrative Strategies for Public and Environmental Health
Abstract
1. Introduction, Issues and Philosophical Perspective
1.1. Issue 1: A Need for Public Health Innovation
- Improve public health and wellbeing;
- Close the health inequality gap; and,
- Alleviate the financial burden currently facing health services and the wider economy
1.2. Issue 2: Biodiversity Conservation and Ecosystem Resilience
1.3. Planetary Health, Biophilosophy and the Symbiocene
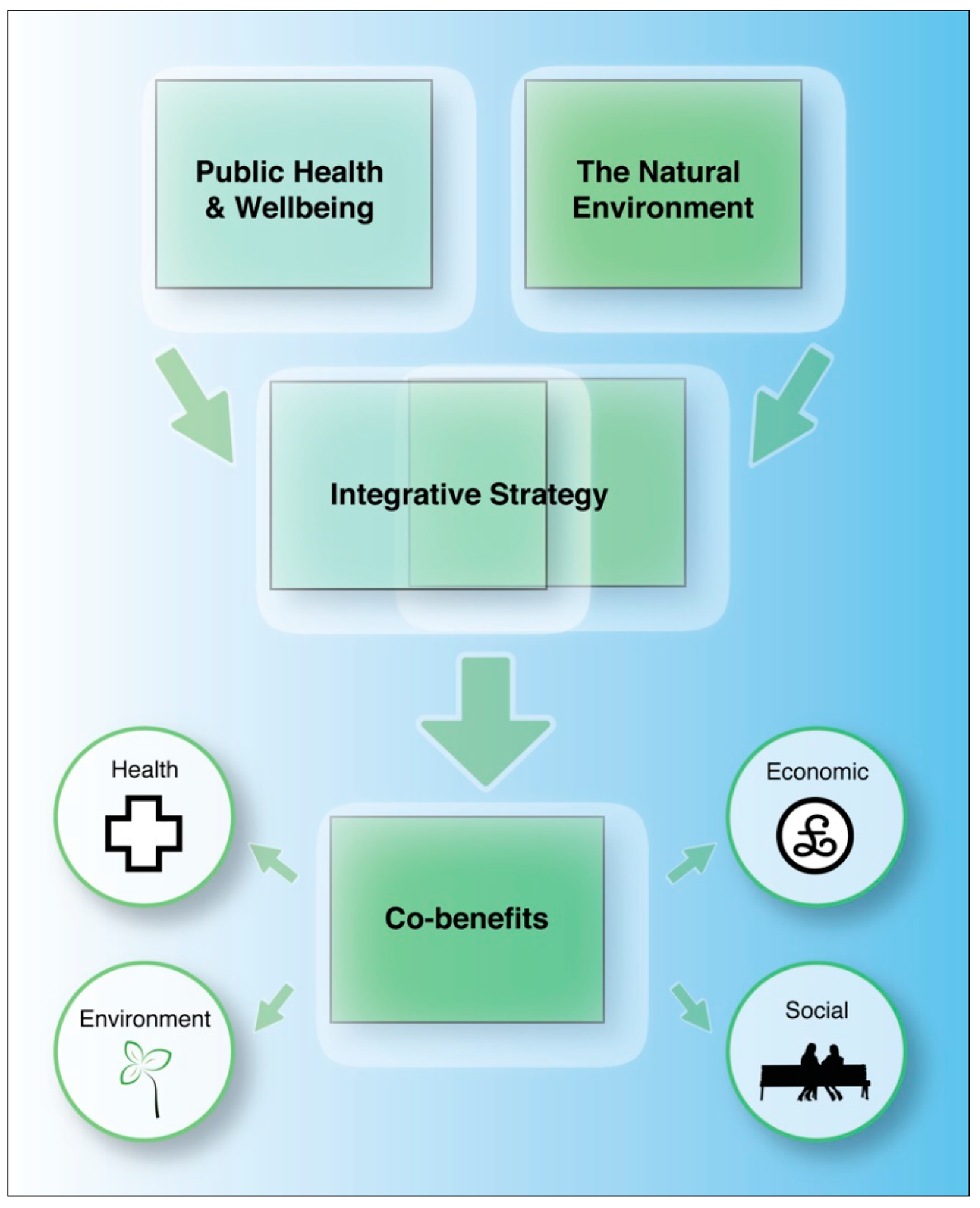
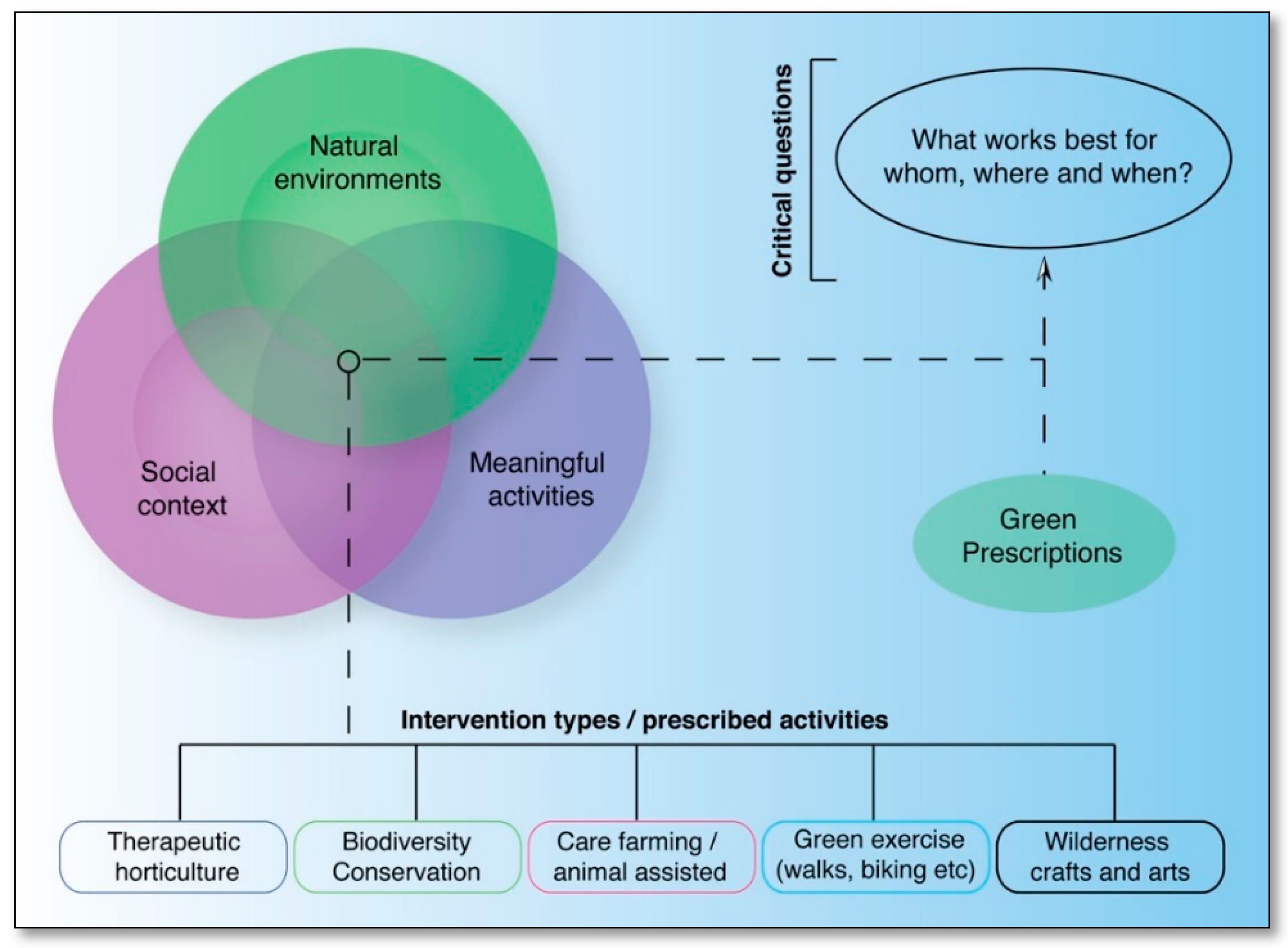
2. Green Prescriptions: An Integrative Approach
- therapeutic horticulture;
- biodiversity conservation;
- care farming (the use of farming practices for health, socialising and education);
- green exercise (e.g. nature walks, biking, climbing);
- wilderness arts and crafts
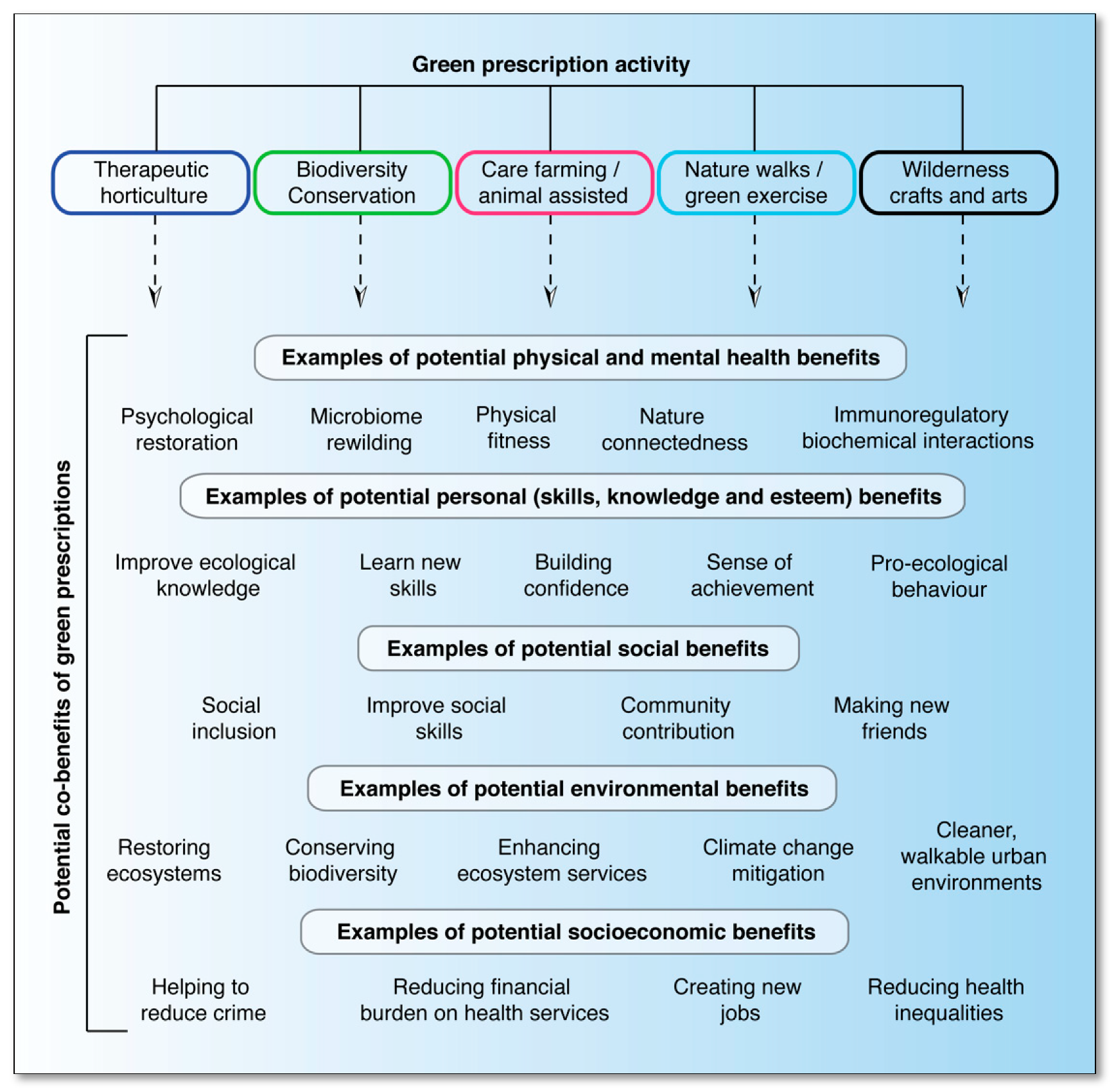
3. Green Prescriptions: Potential Co-Benefits
4. Challenges and Remaining Fundamental Questions
5. Future Studies
- Can green prescriptions save medical practices money and other resources?
- If so, which type of intervention is most effective?
- Does this vary between geographic regions or between areas with different socioeconomic statuses?
- Which patients will benefit the most from green prescriptions?
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Peltola, H.; Heinonen, O.P.; Valle, M.; Paunio, M.; Virtanen, M.; Karanko, V.; Cantell, K. The elimination of indigenous measles, mumps, and rubella from Finland by a 12-year, two-dose vaccination program. New Engl. J. Med. 1994, 331, 1397–1402. [Google Scholar] [CrossRef] [PubMed]
- Vyse, A.J.; Gay, N.J.; White, J.M.; Ramsay, M.E.; Brown, D.W.; Cohen, B.J.; Hesketh, L.M.; Morgan-Capner, P.; Miller, E. Evolution of surveillance of measles, mumps, and rubella in England and Wales: Providing the platform for evidence-based vaccination policy. Epidemiol. Rev. 2002, 24, 125–136. [Google Scholar] [CrossRef] [PubMed]
- Tabar, L.; Yen, M.F.; Vitak, B.; Chen, H.H.; Smith, R.A.; Duffy, S.W. Mammography service screening and mortality in breast cancer patients: 20-year follow-up before and after introduction of screening. Lancet 2003, 361, 1405–1410. [Google Scholar] [CrossRef]
- Park, J.H.; Anderson, W.F.; Gail, M.H. Improvements in US breast cancer survival and proportion explained by tumor size and estrogen-receptor status. J. Clin. Oncol. 2015, 33, 2870–2876. [Google Scholar] [CrossRef] [PubMed]
- Haahtela, T.; Holgate, S.; Pawankar, R.; Akdis, C.A.; Benjaponpitak, S.; Caraballo, L.; Demain, J.; Portnoy, J.; von Hertzen, L. The biodiversity hypothesis and allergic disease: World allergy organization position statement. World Allergy Organ. J. 2013, 6, 3. [Google Scholar] [CrossRef]
- Von Hertzen, L.; Beutler, B.; Bienenstock, J.; Blaser, M.; Cani, P.D.; Eriksson, J.; Färkkilä, M.; Haahtela, T.; Hanski, I.; Jenmalm, M.C.; et al. Helsinki alert of biodiversity and health. Ann. Med. 2015, 47, 218–225. [Google Scholar] [CrossRef]
- Raymond, C.M.; Frantzeskaki, N.; Kabisch, N.; Berry, P.; Breil, M.; Nita, M.R.; Geneletti, D.; Calfapietra, C. A framework for assessing and implementing the co-benefits of nature-based solutions in urban areas. Environ. Sci. Policy 2017, 77, 15–24. [Google Scholar] [CrossRef]
- Ostfeld, R.S. Biodiversity loss and the ecology of infectious disease. Lancet Planet. Health 2017, 1, e2–e3. [Google Scholar] [CrossRef]
- Bragg, R.; Leck, C. Good Practice in Social Prescribing for Mental Health: The Role of Nature-Based Interventions; Natural England Commissioned Reports; 2017. Available online: http://publications.naturalengland.org.uk/publication/5134438692814848 (accessed on 15 January 2019).
- Bloomfield, D. What makes nature-based interventions for mental health successful? BJPsych Int. 2017, 14, 82–85. [Google Scholar] [CrossRef]
- O’Brien, L.; Townsend, M.; Ebden, M. ‘Doing something positive’: Volunteers’ experiences of the well-being benefits derived from practical conservation activities in nature. VOLUNTAS Int. J. Volunt. Nonprofit Organ. 2010, 21, 525–545. [Google Scholar] [CrossRef]
- World Health Organisation. Commission on Social Determinants of Health. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health: Final Report of the Commission on Social Determinants of Health. 2008. Available online: http://apps.who.int/iris/bitstream/handle/10665/43943/9789241563703_eng.pdf;jsessionid=8AD4D28DF8105162B09759F36FC24E72?sequence=1 (accessed on 30 November 2018).
- Walsh, D.; Bendel, N.; Jones, R.; Hanlon, P. It’s not ‘just deprivation’: Why do equally deprived UK cities experience different health outcomes? Public Health 2010, 124, 487–495. [Google Scholar] [CrossRef] [PubMed]
- Marmot, M.; Bell, R. Fair society, healthy lives. Public Health 2012, 126, S4–S10. [Google Scholar] [CrossRef] [PubMed]
- Scarborough, P.; Bhatnagar, P.; Wickramasinghe, K.K.; Allender, S.; Foster, C.; Rayner, M. The economic burden of ill health due to diet, physical inactivity, smoking, alcohol and obesity in the UK: An update to 2006–07 NHS costs. J. Public Health 2011, 33, 527–535. [Google Scholar] [CrossRef] [PubMed]
- Naylor, C.; Parsonage, M.; McDaid, D.; Knapp, M.; Fossey, M.; Galea, A. Long-Term Conditions and Mental Health: The Cost of Co-Morbidities; The Kings Fund and Centre for Mental Health Report; The Kings Fund: London, UK, 2011. [Google Scholar]
- NHS. Health Survey for England: Weight. In NHS Digital; 2016. Available online: http://healthsurvey.hscic.gov.uk/data-visualisation/data-visualisation/explore-the-trends/weight.aspx (accessed on 30 November 2018).
- Al-Goblan, A.S.; Al-Alfi, M.A.; Khan, M.Z. Mechanism linking diabetes mellitus and obesity. Diabetes Metab. Syndr. Obes. Targets Ther. 2014, 7, 587–591. [Google Scholar] [CrossRef] [PubMed]
- Riley, L.; Guthold, R.; Cowan, M.; Savin, S.; Bhatti, L.; Armstrong, T.; Bonita, R. The World Health Organization STEPwise approach to noncommunicable disease risk-factor surveillance: Methods, challenges, and opportunities. Am. J. Public Ealth 2016, 106, 74–78. [Google Scholar] [CrossRef] [PubMed]
- Bridges, A.J.; Andrews, A.R., III; Villalobos, B.T.; Pastrana, F.A.; Cavell, T.A.; Gomez, D. Does integrated behavioral health care reduce mental health disparities for Latinos? Initial findings. J. Lat. Psychol. 2014, 2, 37–53. [Google Scholar] [CrossRef] [PubMed]
- McManus, S.; Bebbington, P.; Jenkins, R.; Brugha, T. Mental Health and Wellbeing in England: Adult Psychiatric Morbidity Survey 2014: A Survey Carried Out for NHS Digital by NatCen Social Research and the Department of Health Sciences, University of Leicester. NHS Digital, 29 September 2016. [Google Scholar]
- Patel, V.; Chatterji, S. Integrating mental health in care for noncommunicable diseases: An imperative for person-centered care. Health Aff. 2015, 34, 1498–1505. [Google Scholar] [CrossRef]
- Varghese, C. Reducing premature mortality from non-communicable diseases, including for people with severe mental disorders. World Psychiatry 2017, 16, 45–47. [Google Scholar] [CrossRef]
- Allen, L.N.; Feigl, A.B. What’s in a name? A call to reframe non-communicable diseases. Lancet Glob. Health 2017, 5, e129–e130. [Google Scholar] [CrossRef]
- Nethan, S.; Sinha, D.; Mehrotra, R. Non Communicable Disease Risk Factors and their Trends in India. Asian Pac. J. Cancer Prev. 2017, 18, 2005–2010. [Google Scholar]
- Soliveres, S.; Van Der Plas, F.; Manning, P.; Prati, D.; Gossner, M.M.; Renner, S.C.; Alt, F.; Arndt, H.; Baumgartner, V.; Binkenstein, J.; et al. Biodiversity at multiple trophic levels is needed for ecosystem multifunctionality. Nature 2016, 536, 456–459. [Google Scholar] [CrossRef] [PubMed]
- Pienkowski, T.; Dickens, B.L.; Sun, H.; Carrasco, L.R. Empirical evidence of the public health benefits of tropical forest conservation in Cambodia: A generalised linear mixed-effects model analysis. Lancet Planet. Health 2017, 1, e180–e187. [Google Scholar] [CrossRef]
- Oliveira Hagen, E.; Hagen, O.; Ibáñez-Álamo, J.D.; Petchey, O.L.; Evans, K.L. Impacts of urban areas and their characteristics on avian functional diversity. Front. Ecol. Evolut. 2017, 5, 84. [Google Scholar] [CrossRef]
- Allentoft, M.E.; O’Brien, J. Global amphibian declines, loss of genetic diversity and fitness: A review. Diversity 2010, 2, 47–71. [Google Scholar] [CrossRef]
- Pinsky, M.L.; Palumbi, S.R. Meta-analysis reveals lower genetic diversity in overfished populations. Mol. Ecol. 2014, 23, 29–39. [Google Scholar] [CrossRef]
- Ceulemans, T.; Stevens, C.J.; Duchateau, L.; Jacquemyn, H.; Gowing, D.J.; Merckx, R.; Wallace, H.; Van Rooijen, N.; Goethem, T.; Bobbink, R.; et al. Soil phosphorus constrains biodiversity across European grasslands. Glob. Chang. Biol. 2014, 20, 3814–3822. [Google Scholar] [CrossRef]
- Prescott, S.L.; Logan, A.C. Larger than life: Injecting hope into the planetary health paradigm. Challenges 2018, 9, 13. [Google Scholar] [CrossRef]
- Myers, S.S. Planetary health: Protecting human health on a rapidly changing planet. Lancet 2017, 390, 2860–2868. [Google Scholar] [CrossRef]
- Canavan, C.R.; Noor, R.A.; Golden, C.D.; Juma, C.; Fawzi, W. Sustainable food systems for optimal planetary health. Trans. R. Soc. Trop. Med. Hyg. 2017, 111, 238–240. [Google Scholar] [CrossRef]
- Schwartz, R.M.; Liu, B.; Lieberman-Cribbin, W.; Taioli, E. Displacement and mental health after natural disasters. Lancet Planet. Health 2017, 1, e314. [Google Scholar] [CrossRef]
- Borrell-Carrió, F.; Suchman, A.L.; Epstein, R.M. The biopsychosocial model 25 years later: Principles, practice, and scientific inquiry. Ann. Fam. Med. 2004, 2, 576–582. [Google Scholar] [CrossRef]
- Prescott, S.L.; Logan, A.C. Down to earth: Planetary health and biophilosophy in the symbiocene epoch. Challenges 2017, 8, 19. [Google Scholar] [CrossRef]
- Albrecht, G. Ecopsychology in the Symbiocene. Ecopsychology 2014, 6, 58–59. [Google Scholar] [CrossRef]
- Huff, C. The growth of holistic health. Philadelphia Inquirer, 3 November 1977; 52. [Google Scholar]
- Salk, J.E. Biology in the future. Perspect. Biol. Med. 1962, 5, 423–431. [Google Scholar] [CrossRef] [PubMed]
- Gehlert, S.; Murray, A.; Sohmer, D.; McClintock, M.; Conzen, S.; Olopade, O. The importance of transdisciplinary collaborations for understanding and resolving health disparities. Soc. Work Public Health 2010, 25, 408–422. [Google Scholar] [CrossRef] [PubMed]
- Nyatanyi, T.; Wilkes, M.; McDermott, H.; Nzietchueng, S.; Gafarasi, I.; Mudakikwa, A.; Kinani, J.F.; Rukelibuga, J.; Omolo, J.; Mupfasoni, D.; et al. Implementing One Health as an integrated approach to health in Rwanda. BMJ Glob. Health 2017, 2, e000121. [Google Scholar] [CrossRef]
- Kesebir, S.; Kesebir, P. A growing disconnection from nature is evident in cultural products. Perspect. Psychol. Sci. 2017, 12, 258–269. [Google Scholar] [CrossRef] [PubMed]
- Lederbogen, F.; Kirsch, P.; Haddad, L.; Streit, F.; Tost, H.; Schuch, P.; Wüst, S.; Pruessner, J.C.; Rietschel, M.; Deuschle, M.; et al. City living and urban upbringing affect neural social stress processing in humans. Nature 2011, 474, 498–501. [Google Scholar] [CrossRef] [PubMed]
- Cox, D.T.; Shanahan, D.F.; Hudson, H.L.; Plummer, K.E.; Siriwardena, G.M.; Fuller, R.A.; Anderson, K.; Hancock, S.; Gaston, K.J. Doses of neighborhood nature: The benefits for mental health of living with nature. BioScience 2017, 67, 147–155. [Google Scholar] [CrossRef]
- Bertram, C.; Rehdanz, K. The role of urban green space for human well-being. Ecol. Econ. 2015, 120, 139–152. [Google Scholar] [CrossRef]
- Soga, M.; Gaston, K.J. Extinction of experience: The loss of human–nature interactions. Front. Ecol. Environ. 2016, 14, 94–101. [Google Scholar] [CrossRef]
- Kuenzig, M.E.; Barnabe, C.; Seow, C.H.; Eksteen, B.; Negron, M.E.; Rezaie, A.; Panaccione, R.; Benchimol, E.I.; Sadatsafavi, M.; Aviña-Zubieta, J.A.; et al. Asthma is associated with subsequent development of inflammatory bowel disease: A population-based case–control study. Clin. Gastroenterol. Hepatol. 2017, 15, 1405–1412. [Google Scholar] [CrossRef] [PubMed]
- Earl, C.S.; An, S.Q.; Ryan, R.P. The changing face of asthma and its relation with microbes. Trends Microbiol. 2015, 23, 408–418. [Google Scholar] [CrossRef] [PubMed]
- Robinson, J.; Mills, J.; Breed, M. Walking Ecosystems in Microbiome-Inspired Green Infrastructure: An Ecological Perspective on Enhancing Personal and Planetary Health. Challenges 2018, 9, 40. [Google Scholar] [CrossRef]
- Robinson, J.M.; Jorgensen, A. Rekindling Old Friendships in New Landscapes: The Environment-Microbiome-Health Axis in the Realms of Landscape Research. People Nat. 2018. under review. [Google Scholar]
- Rook, G.A. Regulation of the immune system by biodiversity from the natural environment: An ecosystem service essential to health. Proc. Natl. Acad. Sci. USA 2013, 110, 18360–18367. [Google Scholar] [CrossRef] [PubMed]
- Wen, L.M.; Kite, J.; Merom, D.; Rissel, C. Time spent playing outdoors after school and its relationship with independent mobility: A cross-sectional survey of children aged 10–12 years in Sydney, Australia. Int. J. Behav. Nutr. Phys. Act. 2009, 6, 15. [Google Scholar] [CrossRef] [PubMed]
- Rosiek, A.; Maciejewska, N.F.; Leksowski, K.; Rosiek-Kryszewska, A.; Leksowski, Ł. Effect of television on obesity and excess of weight and consequences of health. Int. J. Environ. Res. Public Health 2015, 12, 9408–9426. [Google Scholar] [CrossRef]
- Bekoff, M.; Bexell, S.M. Ignoring nature: Why we do it, the dire consequences, and the need for a paradigm shift to save animals, habitats, and ourselves. Hum. Ecol. Rev. 2010, 17, 70–74. [Google Scholar]
- Pérez, C.G.; Soutelo, S.G.; Mosqueira, M.M.; Soto, J.L. Spa techniques and technologies: From the past to the present. Sustain. Water Resour. Manag. 2017. [Google Scholar] [CrossRef]
- van Tubergen, A.; van der Linden, S. A brief history of spa therapy. Ann. Rheum. Dis. 2002, 61, 273–275. [Google Scholar] [CrossRef] [PubMed]
- Maretzki, T.W. The Kur in West Germany as an interface between naturopathic and allopathic ideologies. Soc. Sci. Med. 1987, 24, 1061–1068. [Google Scholar] [CrossRef]
- Antonelli, M.; Donelli, D. Effects of balneotherapy and spa therapy on levels of cortisol as a stress biomarker: A systematic review. Int. J. Biometeorol. 2018, 62, 913–924. [Google Scholar] [CrossRef] [PubMed]
- Jepson, R.; Robertson, R.; Cameron, H. Green Prescription Schemes: Mapping and Current Practice; NHS Health Scotland: Edinburgh, UK, 2010. [Google Scholar]
- Patel, A.; Schofield, G.M.; Kolt, G.S.; Keogh, J.W. General practitioners’ views and experiences of counselling for physical activity through the New Zealand Green Prescription program. BMC Fam. Pract. 2011, 12, 119. [Google Scholar] [CrossRef] [PubMed]
- Kolt, G.S.; Schofield, G.M.; Kerse, N.; Garrett, N.; Schluter, P.J.; Ashton, T.; Patel, A. The Healthy Steps Study: A randomized controlled trial of a pedometer-based Green Prescription for older adults. Trial protocol. BMC Public Health 2009, 9, 404. [Google Scholar] [CrossRef]
- Victoria State Government. Gardening—People with Disabilities. 2018. Available online: https://www.betterhealth.vic.gov.au/health/healthyliving/gardening-people-with-disabilities (accessed on 30 November 2018).
- Poulsen, D.; Stigsdotter, U.; Davidsen, A. “That Guy, Is He Really Sick at All?” An Analysis of How Veterans with PTSD Experience Nature-Based Therapy. InHealthcare 2018, 6, 64. [Google Scholar] [CrossRef] [PubMed]
- Millar, S.L.; Donnelly, M. Promoting mental wellbeing: Developing a theoretically and empirically sound complex intervention. J. Public Health 2013, 36, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Seymour, V.; King, M.; Antonaci, R. Understanding the impact of volunteering on pro-environmental behavioural change. Volunt. Sect. Rev. 2018, 9, 73–88. [Google Scholar] [CrossRef]
- Annis, G.M.; Pearsall, D.R.; Kahl, K.J.; Washburn, E.L.; May, C.A.; Taylor, R.F.; Cole, J.B.; Ewert, D.N.; Game, E.T.; Doran, P.J. Designing coastal conservation to deliver ecosystem and human well-being benefits. PLoS ONE 2017, 12, e0172458. [Google Scholar] [CrossRef] [PubMed]
- Flies, E.J.; Skelly, C.; Lovell, R.; Breed, M.F.; Phillips, D.; Weinstein, P. Cities, biodiversity and health: We need healthy urban microbiome initiatives. Cities Health 2018. [Google Scholar] [CrossRef]
- Mills, J.G.; Weinstein, P.; Gellie, N.J.; Weyrich, L.S.; Lowe, A.J.; Breed, M.F. Urban habitat restoration provides a human health benefit through microbiome rewilding: The Microbiome Rewilding Hypothesis. Restor. Ecol. 2017, 25, 866–872. [Google Scholar] [CrossRef]
- Vardakoulias, O. The Economic Benefits of Ecominds: A Case Study Approach. MIND. July 2013. Available online: https://www.mind.org.uk/media/338566/The-Economic-Benefits-of-Ecominds-report.pdf (accessed on 15 January 2019).
- Kimberlee, R. Gloucestershire clinical commissioning group’s social prescribing service: Evaluation report. 2016. Available online: http://eprints.uwe.ac.uk/30293/ (accessed on 15 January 2019).
- Dayson, C.; Bashir, N.; Bennett, E. The Rotherham Social Prescribing Service for People with Long-term Health Conditions. Annual Report; Sheffield Hallam University: Sheffield, UK, 2016; Available online: http://shura.shu.ac.uk/17296/1/rotherham-social-prescribing-service-annual-report.pdf (accessed on 1 December 2018).
- Seltenrich, N. Just what the doctor ordered: Using parks to improve children’s health. Environ. Health Perspect. 2015, 123, A254–A529. [Google Scholar] [CrossRef] [PubMed]
- Maier, J.; Jette, S. Promoting nature-based activity for people with mental illness through the US “Exercise Is Medicine” initiative. Am. J. Public Health 2016, 106, 796–799. [Google Scholar] [CrossRef] [PubMed]
- Swinburn, B.A.; Walter, L.G.; Arroll, B.; Tilyard, M.W.; Russell, D.G. Green prescriptions: Attitudes and perceptions of general practitioners towards prescribing exercise. Br. J. Gen Pr. 1997, 47, 567–569. [Google Scholar]
- Gribben, B.; Goodyear-Smith, F.; Grobbelaar, M.; O’Neill, D.; Walker, S. The early experience of general practitioners using Green Prescription. N. Z. Med. J. 2000, 113, 372–373. [Google Scholar] [PubMed]
- Lovell, R.; Depledge, M.; Maxwell, S. Health and the Natural Environment: A Review of Evidence, Policy, Practice and Opportunities for the Future. 2018. Available online: https://beyondgreenspace.net/2018/09/07/defra_health_review/ (accessed on 30 November 2018).
- Bell, S.L.; Leyshon, C.; Foley, R.; Kearns, R.A. The “healthy dose” of nature: A cautionary tale. Geogr. Compass. 2018, e12415. [Google Scholar] [CrossRef]
- Husk, K.; Lovell, R.; Garside, R. Prescribing gardening and conservation activities for health and wellbeing in older people. Maturitas 2018, 110, A1–A2. [Google Scholar] [CrossRef]
- Allen, R.W.; Barn, P.K.; Lanphear, B.P. Randomized controlled trials in environmental health research: Unethical or underutilized? PLoS Med. 2015, 12, e1001775. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Robinson, J.M.; Breed, M.F. Green Prescriptions and Their Co-Benefits: Integrative Strategies for Public and Environmental Health. Challenges 2019, 10, 9. https://doi.org/10.3390/challe10010009
Robinson JM, Breed MF. Green Prescriptions and Their Co-Benefits: Integrative Strategies for Public and Environmental Health. Challenges. 2019; 10(1):9. https://doi.org/10.3390/challe10010009
Chicago/Turabian StyleRobinson, Jake M., and Martin F. Breed. 2019. "Green Prescriptions and Their Co-Benefits: Integrative Strategies for Public and Environmental Health" Challenges 10, no. 1: 9. https://doi.org/10.3390/challe10010009
APA StyleRobinson, J. M., & Breed, M. F. (2019). Green Prescriptions and Their Co-Benefits: Integrative Strategies for Public and Environmental Health. Challenges, 10(1), 9. https://doi.org/10.3390/challe10010009




