1. Introduction
Spiritual retreats have become very popular for individuals seeking to create personal spiritual or psychological growth. Spiritual retreat programs have developed in many religious and secular traditions and typically incorporate a variety of elements including rituals, prayer, meditation, and self-reflection. Thousands of people engage in such retreats each year, with yoga and meditation retreats among the most popular for both their spiritual and therapeutic value (
Edwards 2012;
Hoyez 2007). These retreats are also associated with strong emotional responses, with participants reporting that they experience reductions in stress, anxiety, and depression. In addition, participants commonly report a sense of improved psychological well-being, transformation in the spiritual aspects of their lives, and consequences of the retreat that are life changing (
Kennedy et al. 2002;
Falkenström 2010;
Jacobs et al. 2013). A recent systematic analysis revealed that a variety of retreat programs are associated with both short- and long-term improvements in psychological and spiritual measures (
Naidoo et al. 2018). The improvements may also be observed on novices to those experienced with various spiritual practices (
Montero-Marín et al. 2016). However, no research has been published on the neurological effects of intensive retreat programs such as functional connectivity measured using magnetic resonance imaging (fMRI).
Several studies have focused on the effect of meditation practice over a short and long duration of time from days to years. Both structural and functional changes have been reported that are associated with the long-term practice of meditation (
Newberg et al. 2010;
MacCoon et al. 2014;
Saggar et al. 2015). Studies of functional connectivity have detected changes in default mode network structures such as the prefrontal cortex, anterior and posterior cingulate cortices, inferior parietal cortex, and lateral temporal cortex (
Jang et al. 2011;
Brewer et al. 2011). Other studies have also found changes in functional connectivity between structures in the attention network, salience network, and executive network as a result of meditation programs or retreats (
Hasenkamp and Barsalou 2012;
Kwak et al. 2020).
More broadly, there have been a number of publications concerning the overall relationship between the brain and religious or spiritual phenomena. Studies have explored the relationship between the brain and mystical experiences, near death experiences, religious symbols effects, and religious beliefs in general (
Beauregard and Paquette 2006;
Beauregard et al. 2009;
Harris et al. 2009;
Johnson et al. 2014). This research, sometimes referred to as the field of neurotheology, has provided important information on the intersection between neuroscience and religious studies (
Newberg 2010). At this time, it is unclear how far such research might be able to expand the broader understanding of religious and spiritual phenomena. For example, if studies reveal a significant relationship between religious beliefs and emotional centers in the brain, the finding could have implications on the importance of emotions in understanding those beliefs. On the other hand, if data point to more cognitive processes, this could also influence our understanding of the nature of such beliefs.
Previously, we have reported (
Newberg et al. 2017) on the dopaminergic and serotonergic changes resulting from a one-week spiritual retreat based upon the Spiritual Exercises developed by St. Ignatius Loyola (1491–1556), founder of the Society of Jesus known as the Jesuits. The Ignatian Spiritual Exercises utilize a variety of elements including living in silence, performing prayer and meditation, and personal reflection. Elements also have a specific Christian perspective focusing on topics during contemplative periods including sin, God’s mercy, the life and passion of Jesus, and God’s love. Throughout the duration of the retreat period, individual guidance is provided by a spiritual advisor to facilitate spiritual growth or personal transformation. The transformation can come in the form of a deeper understanding of the person, of the person’s relationship with God, and of the larger understanding of meaning and purpose in the universe (
Sean Salai 2016). Such transformative experiences from the retreat can also be measured using a number of psychological and physiological parameters that reflect long-term effects. We proposed that the Ignatian retreat would be an ideal target for neuroscientific inquiry given its long history, well developed structure, and likelihood of strong spiritual experiences in a relatively short period of time. Thus, in our initial report, we evaluated participants before and after the Ignatian retreat using DaTscan (Ioflupane) single-photon emission computed tomography (SPECT). Interestingly, the results of the study showed a significant reduction in dopamine and serotonin transporter binding after the retreat when compared to the baseline SPECT imaging. Such a change was postulated to be associated with a “priming” of the brain for intense spiritual experiences by enabling the brain to be more affected by the release of serotonin or dopamine. This prior study was the first ever to report such changes in these neurotransmitter systems as a result of participating in a spiritual retreat. Such a finding is also linked to a limited number of other studies that demonstrate the impact during spiritual practices on neurotransmitters such as dopamine and serotonin (
Newberg and Yaden 2018). Further, these findings may have implications for their psychological effects since serotonin and dopamine are well known to be associated with changes in mood and affect, found in various disorders such as depression (
Amsterdam et al. 2012;
Spies et al. 2015).
The present study, on the effects of an Ignatian retreat, takes another step toward a greater understanding of the neurophysiological effects from a structured, prolonged and intense spiritual practice by describing functional connectivity data obtained from the same subjects who were evaluated in our previously published study on serotonin and dopamine transporter imaging. Thus, subjects underwent resting blood oxygen level-dependent (BOLD) magnetic resonance imaging (MRI) before and after they participated in the one-week Ignatian spiritual retreat to observe what longer-standing changes occurred in functional connectivity as a result of undergoing the retreat program. Resting BOLD MRI is a simple technique that acquires imaging over a 5–10 min period in order to assess the MRI signal associated with changes in blood flow and blood oxygenation. When the signal between two brain regions is concordant, they are considered to be functionally connected. Functional connectivity helps show neurophysiological changes associated with different brain states and processes. The changes observed with resting BOLD MRI are distinct from, but can complement, other techniques such as SPECT imaging mentioned above and positron emission tomography (PET) imaging. These latter two techniques involve injecting a radioactive tracer that measures some physiological process in the brain such as cerebral blood flow, metabolism, or neurotransmitter activity.
We hypothesized that given the psychological and spiritual changes anticipated in the retreat, there would be significant changes in functional connectivity in a variety of structures that are associated typically with such practices. Specifically, we hypothesize that areas related to emotional processes that underlie positive feelings such as joy including the limbic system, cerebellum, prefrontal cortex, and basal ganglia, would be significantly different after the retreat. We also expected that areas involved in the default mode network would be different as this area has been shown to be involved with meditation practices. Finally, we hypothesized that there would be significant findings in the dopamine areas of the brain such as the pallidum.
Therefore, the goals of this study were to determine whether the one-week spiritual retreat resulted in changes in functional connectivity and whether any imaging changes related to qualitative changes in psychological or spiritual measures.
2. Methods
2.1. Subjects and Imaging Acquisition
The Thomas Jefferson University Institutional Review Board for human subjects and Radiation Safety reviewed and approved the study protocol and consent form. The subjects were recruited by advertising with local churches and pastoral care departments from the local community. For eligibility, the subjects were permitted to have participated in prior spiritual retreats, but could not have participated previously in an Ignatian-based retreat for one week or longer. All subjects underwent an extensive screening that consisted of their medical and psychiatric history, to ensure that there were no contraindications or risks from the MRI; none of the study subjects had a current disorder, such as stroke, tumor, active cardiac disease, or an Axis I psychiatric disorder that might affect cerebral physiology.
All subjects who participated in this study met the following inclusion criteria: (1) cognitively able to provide informed consent and willingness to complete this study; (2) agreement to attend the one-week spiritual retreat; (3) willing to undergo the full imaging procedures with no metal in their body; and (4) women of childbearing potential with a negative blood or serum pregnancy test.
Subjects were excluded from this study if they had: (1) any neurological or psychiatric disorders, including drug or alcohol abuse, that could interfere with cerebral physiology; (2) any active medical conditions that could interfere with cerebral physiology; (3) currently taking medication(s) (i.e., antidepressants, antipsychotics, anxiolytics, benzodiazepines, sedatives, anti-seizure medications) that could affect cerebral physiology; (4) unable or unwilling to lie still in the scanner; and (5) history of previous brain surgery or intracranial abnormalities that could complicate the interpretation of the brain scans.
Within one month of entering into the one-week spiritual retreat, all subjects completed an initial, evaluation with resting BOLD fMRI along with a completion of a battery of validated psychological and spiritual questionnaires. Afterward, within one week of completing the retreat, the subjects returned for their post retreat evaluation which repeated the resting BOLD fMRI and questionnaires. It should be noted that two subjects received their post retreat scans at 12 and 14 days due to logistical issues with scheduling the scans.
After inclusion and exclusion criteria were met, a total of 14 subjects (8 males and 6 females) were enrolled in this study. The subjects were of ages 24–76 years old with a mean age of 54 ± 13 years with a mean education level of 18.5 ± 1.7 years. All 14 subjects were Christian (7 Catholics, 5 Protestants, 1 Orthodox/Anglican, and 1 Quaker). Eight subjects reported previous experience with different types of religious or spiritual retreats. However, no subject had undergone an Ignatian retreat. Subjects had a low level of depression as a group, with a mean Beck Depression score of 4.4 ± 6.0 (scores below 13 are considered within normal limits) and a moderate amount of anxiety with a mean Spielberger Trait Anxiety score of 29.3 ± 7.2. We did not control for other variables including measures of religiosity at baseline or prior meditation/retreat experience. However, subjects functioned as their own control and thus we planned to evaluate the general change from baseline for the subjects after the retreat program.
2.2. Retreat Description and Components
The intended purpose of the one-week Ignatian retreat is to create a time for greater understanding of an individual’s spiritual life and how to incorporate this new understanding into their everyday life. One goal is to evoke a substantial change and/or deepening of one’s spiritual and religious beliefs. All subjects participated in the one-week Ignatian retreat at the Jesuit Center in Wernersville, Pennsylvania. The retreat site is located in a rural area on 240 acres of natural land with beautiful grounds and art. The retreat is performed primarily in silence. On the first day, each retreatant met with a designated retreat director (usually a priest or nun) who would engage in dialogue and provide daily guidance and insights regarding retreat exercises, plan, and direction each retreatant pursued during the retreat. The retreat is based on the Ignatian exercises (
Mottola 1964) but does not follow them strictly to allow for responsiveness to each person’s retreat experience. The plan for each day consisted of voluntary participation in morning mass with additional time spent extensively in personal reflection, contemplation, and prayer. Each day, a meeting with the spiritual director was planned; meals were eaten in a common dining area with other retreatants that were typically shared in silence.
2.3. Instruments and Measures
Previously, we reported the effect of the retreat on various psychological and spiritual measures, and provided additional background regarding that data so that they might be considered in the context of the functional connectivity results. To summarize briefly, at the time of undergoing the fMRI scans, each participant completed a series of psychological inventories and measures of spirituality. These surveys have been validated originally in large populations and have been used in both clinical and research settings extensively. The battery of psychological and spiritual measures included the following: the Spielberger State Trait Anxiety Inventory (STAI-Y) is a 20 item questionnaire with a four item response to assess symptoms of anxiety (
Spielberger et al. 1983); the Profile of Moods States (POMS) is a 37 item questionnaire with a five item response to assess a variety of symptoms associated with tension, anger, vigor, fatigue, depression, and confusion (
McNair et al. 1971); the Beck Depression Inventory (BDI) is a 21 item questionnaire with four response items to assess symptoms associated with depression (
Beck and Beck 1972); the 12-Item Short Form Health Survey (SF-12) which asks questions associated with general health and well-being (
Ware et al. 1996); the Cloninger Self-Transcendence Scale which has 26 questions rated on a 5-point Likert scale (
Garcia-Romeu 2010); and the Brief Multidimensional Measure of Religiousness/Spirituality which is a 38 item scale evaluating 11 dimensions of religiousness and spirituality (
Fetzer Institute 1999).
The MR imaging was performed on a 3T Philips Achieva scanner using a standard 8 channel head coil. Structural MRI brain images were collected using a T1-weighted Magnetization-Prepared Rapid Gradient Echo (MPRAGE) sequence for anatomical localization. The imaging parameters used were: field of view (FOV) = 25.6 cm, voxel size = 1.0 × 1.0 × 1.0 mm3, matrix size = 256 × 240, the repletion time (TR) = 6.44 s, and echo time (TE) = 3.16 s, slice thickness = 1 mm, number of slices = 170, flip angle = 8° and acquisition time = 280 s. After this structural scan, resting-state functional MRI (rs-fMRI) data were collected using an Echo Planar Imaging (EPI) sequence using the following parameters: FOV = 25.6 cm, voxel size = 2 × 2 × 4 mm3, matrix size = 128 × 128, TR = 2.5 s, TE = 35 ms, slice thickness = 4 mm, number of slices = 34, number of volumes = 120 and acquisition time = 300 s. During the rs-fMRI scan, all subjects were instructed to close their eyes, keep their head still, and relax quietly for approximately 5–6 min.
2.4. Functional Connectivity Image Acquisition and Procedure
In order to process the resting-state BOLD scans, it is important to separate the target low frequency components from physiological noise. The following processing and analysis was performed for the acquired functional volumes in order to uniquely describe the communication between resting-state networks without the effect of noise contaminants. This analysis pipeline is well-established in our institution and widely used in the fMRI community for evaluating rs-fMRI scan data. All resting-state data were spatially preprocessed using SPM12 (Wellcome Department of Cognitive Neurology, University College London, UK) in the Matlab environment (Mathworks, Inc.). Realignment was initially performed to ensure proper voxel to voxel correspondence within the BOLD time series. BOLD is used to differentiates changes in cerebral blood flow (CBF) in fMRI scans and to assess the signal comparison between different structures. The functional volumes from the BOLD fMRI scans were then slice time corrected to account for timing inconsistencies within the EPI data. In order to facilitate the removal (i.e., co-vary out) of confounding temporal factors prior to modeling, scans are segmented into gray matter, white matter, and CSF. Spatial normalization was then performed for each data set and warped to the Montreal Neurological Institute coordinate space through a subject specific deformation field and smoothed with a three dimensional Gaussian kernel with a full width at half maximum (FWHM) of 4 × 4 × 8 mm3. This spatial processing optimizes the data for additional temporal corrections to emphasize the low-frequency resting-state networks of interest for connectivity analysis. The Conn toolbox was integrated into the Matlab environment for component-based noise correction (CompCor) of physiologic and other noise sources such as heart rate or respiratory rate inherent to BOLD imaging.
The preprocessed functional volumes from the prior step were then imported into the Conn toolbox for the resting-state analysis. Structural volumes were separated into white matter, gray matter, and CSF confounds. White matter and CSF confounds were placed in a three-dimensional space and a band-pass filter of 0.008 to 0.09 was applied to restrict analysis to a limited frequency window. For the primary analysis, seed regions of interest (ROI) were used to evaluate specific structures in the frontal, temporal, and parietal lobes, as well as the cerebellum, limbic areas, and cingulate cortex. Changes in functional connectivity between the pre and post retreat scans were analyzed and regions with significant changes reported, corrected using the False Discovery Rate (FDR) method to mitigate against false positives due to multiple comparisons.
4. Discussion
This is the first study that has measured changes in functional connectivity using fMRI with participants in an intensive Ignatian retreat program. The findings, while preliminary, suggest that participation in a spiritual retreat of this type can have a short-term impact on the functional connectivity in brain regions believed to be associated with religious and spiritual practices and experiences. Specifically, structures such as the superior frontal cortex, limbic system, cingulate gyrus, superior temporal lobe and parietal regions have all been found to be involved in meditation- and prayer-based programs both in the short and long term.
It is important to note that the Ignatian has multiple elements including meditation, silence, prayer, self-reflection, and personal spiritual guidance which can all potentially affect brain function (
Newberg and Iversen 2003). In recent years, meditation practices have been studied and have been found to elicit a number of neurophysiological and subjective changes. The literature and our previous research has utilized (fMRI), positron emission tomography (PET), and single-photon emission computed tomography (SPECT) to evaluate changes in cerebral blood flow and brain activation during meditation and prayer states (
Wang et al. 2011;
Garrison et al. 2014;
Kwak et al. 2020). The measurable changes reported in the literature depend in large part on the types of the meditation practice and associated experiences (
Newberg and Iversen 2003). Generally the findings in functional neuroimaging research suggests that there is a network in the brain associated with religious or spiritual practices that include changes in the attentional system including the prefrontal cortex, cingulate gyrus, and superior parietal lobes. Changes in activity appear in the limbic areas such as the amygdala, hippocampus, and thalamus.
It is also important to emphasize that numerous studies have reported that spiritual practices such as the ones involved in the Ignatian retreat improve a number of physical and mental health related measures. For example, various systematic reviews and meta-analyses have demonstrated that religious involvement by itself is associated with lower morbidity and mortality (
McCullough et al. 2000;
Oman et al. 2002). Imaging studies such as the current one might help elucidate the mechanism by which such effects could occur.
Studies focusing on meditation-based practices have demonstrated a significant benefit for patients with disorders such as hypertension, psoriasis, irritable bowel disease, epilepsy, and hormonal related symptoms (
Ooi et al. 2017;
Arias et al. 2006;
Gamret et al. 2018). The benefit might come in the form of helping with coping through such problems or in actually improving various clinical measures.
When it comes to mental health, studies have shown religious beliefs to be associated with improvements in anxiety and depression symptoms (
Captari et al. 2018;
Smith et al. 2003;
Braam et al. 1999). Meditation-based practices have consistently demonstrated improvements in depression and anxiety (
Li and Bressington 2019;
Jain et al. 2007). Even specific prayer-based practices such as performing the Rosary have been found to reduce anxiety symptoms (
Anastasi and Newberg 2008). In the present study, the subjects were found to have significant improvements in measures of tension and fatigue along with the expected increases in religious and spiritual beliefs. The mechanism by which spiritual beliefs and practices likely are associated with psychological and neurophysiological changes are supported by the current research. Brain structures such as the cerebellum and limbic regions are known to be involved in the expression and modulation of emotions. Thus, finding changes in these areas after an intensive spiritual retreat help to clarify how the components of the retreat affect brain processes that lead to psychological changes (
Yaden and Newberg 2018;
Newberg and Yaden 2018).
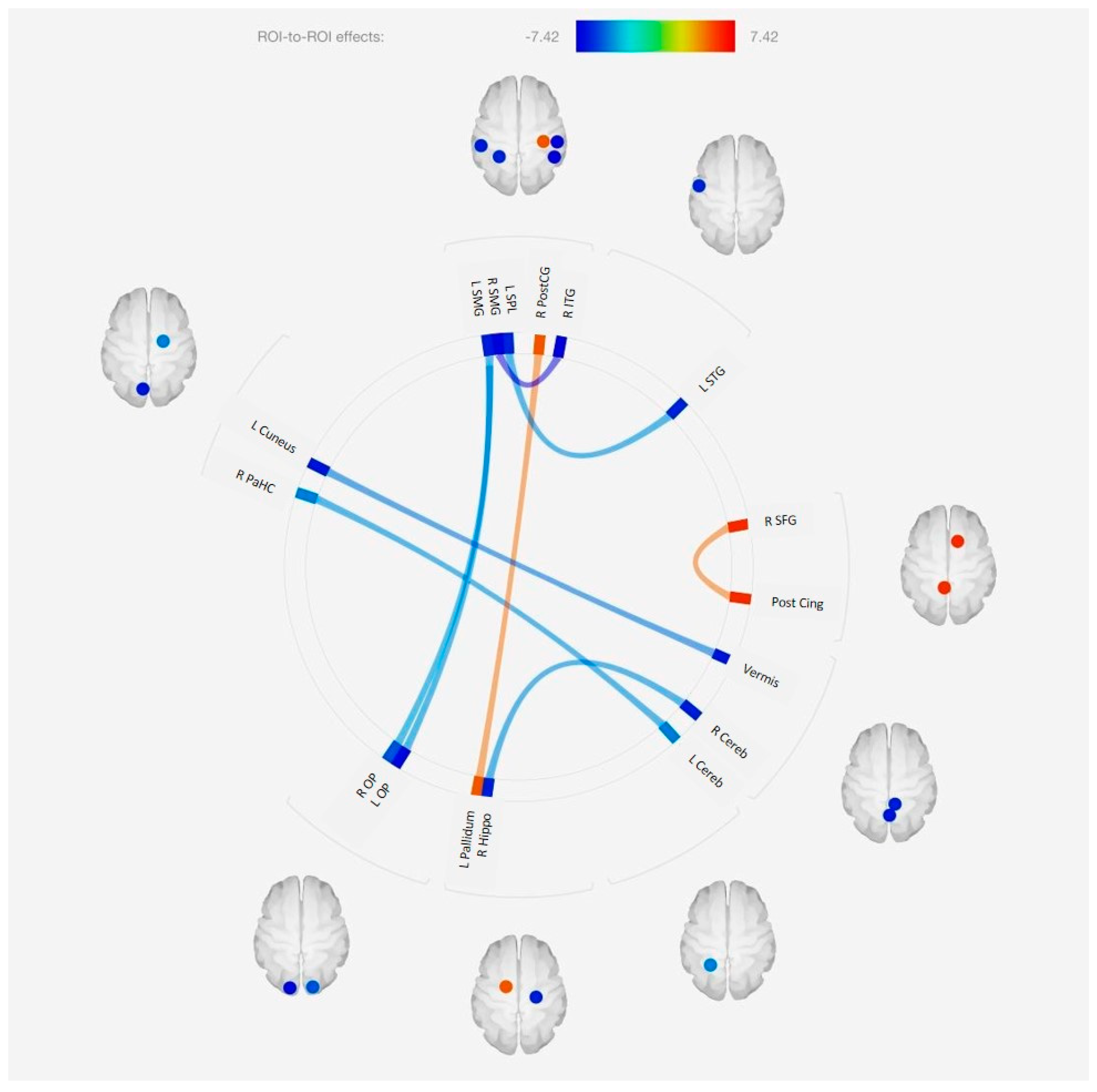
The results from this preliminary study suggest that there are structures with both increased and decreased functional connectivity in the brain. For example, functional connectivity was increased between the posterior cingulate gyrus and the superior frontal gyrus and the left pallidum. Both the superior frontal gyrus and posterior cingulate may be associated with self-awareness since the posterior cingulate is a structure in the self-processing component of the default mode network (
Goldberg et al. 2006). Since a substantial element of the Ignatian retreat is spent in self-reflection and silence, an increased connectivity between these two structures could be consistent with such a subjective response.
The second relationship is particularly relevant with respect to previous findings that showed changes in dopaminergic function when comparing the pre and post retreat results the retreat program. Increased connectivity between the pallidum, the primary dopaminergic region, and the posterior cingulate could reflect how dopamine augments the self-awareness process (
Joensson et al. 2015;
Lou et al. 2017). It is also possible that dopamine supports a more positive outlook on the self. All of the participants reported significant increases in the manner in which they viewed their own self.
Several other structures had reduced connectivity as a result of participation in the retreat. Of note, there was reduced connectivity between the cerebellum and limbic structures such as the hippocampus and parahippocampus. There is increasing evidence that the cerebellum may be particularly involved in the coordination of emotional processes, particularly negative ones (
Utz et al. 2015). The cerebellum connects with the limbic structures both ipsilaterally and contralaterally (
Cacciola et al. 2017). It has also been found that the vermis may be particularly connected to the limbic structures (
Blatt et al. 2013). Diminished connectivity could reflect a more positive emotional response of the individuals, which was reported in terms of reduced depression and anxiety. More importantly, in a spiritual context, the retreat enabled participants to reflect on personal growth positive affective responses which allow for less regulation of negative emotions by the cerebellum. It should be noted that we did not find significant correlations between the qualitative psychological or religious measures and imaging findings, in part due to the small sample size and in part due to the number of comparisons that would have to be made. Furthermore, there was a great deal of uniformity in the subject group with all but two individuals expressing elevated levels of stress or depression. Given the low initial levels of these measures, it was unlikely to be able to assess substantial changes in these measures. However, the results from this study can provide a basis for future, larger studies, that can better assess the relationship between areas of the brain affected by these retreat programs and various subjective, psychological responses.
Decreased connectivity between the superior parietal lobe and superior temporal gyrus could be consistent with our prior hypothesis that these areas are involved in fostering a sense of connectedness and oneness that are characteristic expressions of spiritual experiences. We have proposed that diminished neuronal input into these regions would result in a diminished spatial sense of the self, leading to a sense of oneness (
Newberg and Iversen 2003). This is distinct from the self-reflection associated with the posterior cingulate and pallidum described above.
One important limitation of this pilot study is that there was no comparison group in the sense of having other subjects go through one or more different types of meditation programs. Although we would expect test–retest effects to be minimal in a pure control group (i.e., doing nothing in between evaluations), it is reasonable to conclude that participation in other types of retreats, ranging in duration of time and intensity, could yield similar findings as those that we report here. Or different practices could yield a different set of physiological effects. Meditation programs such as Mindfulness-Based Stress Reduction (MBSR) and Kirtan Kriya meditation research conducted by the authors (
Monti et al. 2012) have resulted in neurophysiological and clinical changes which shared some similarities in terms of affecting the frontal and temporal lobes. However, there are also distinctions between practices both in terms of their respective elements and outcomes. Based upon the feasibility and findings of this preliminary study, we hope that our future research will be able to utilize an active control group and one or more comparison groups to study cohort effects and the many different elements and sources of systematic variance.
One goal of the retreat in the current study is to gain an understanding of how practices incorporated into everyday life can produce substantial change. Such findings are consistent with the activation in brain structures that had altered functional connectivity. The decreased functional connectivity with parietal lobe structures and superior temporal lobe may be associated with differentiation of their self-orienting functions resulting in a feeling of oneness or self-transcendence (
Newberg and Iversen 2003) Functional connectivity changes associated with the dopamine areas of the pallidum might also be associated with alterations in the brain associated with religious and spiritual practices or experience (
Kjaer et al. 2002).
In this study, we did not attempt to differentiate the effects of the various elements of the retreat. It is possible that non-spiritual factors may have been important contributors to the findings such as simply taking time off from work and daily stressors, being in a vacation-like environment, or spending time in nature. Future studies will need to try to delineate which factors are most effective and related to the changes in brain function.
Another issue with our findings is that we might be evaluating the effect of emotional or spiritual experience rather than the effect of the retreat. The practice of prayer could result in changes in the brain. However, the subjective experience associated with that prayer could result in similar brain changes. Given these limitations, it is important to develop future studies to determine the key factors of retreats, both spiritual and secular, to determine whether there are similar effects. The literature has shown longitudinal changes in brain function associated with prolonged exposure to meditation retreats and practices (
Newberg et al. 2010;
MacCoon et al. 2014;
Saggar et al. 2015).
Regarding our study design, the subject selection also raised important methodological challenges for this study and future studies. To begin, since this was a preliminary study, it did not have a sufficient number of subjects to find relationships between other variables such as gender, age, or level of education. However, it was a relatively uniform population in terms of these variables which limits the ability to detect significant effects on the response to the retreat program. We also did not control for baseline measures of religiosity, previous participation in retreats, or level of religious or spiritual practice. In terms of the meditation experience of the subjects, we enrolled subjects with reasonable experience with meditation or spiritual practices. However, it was not clear who would make the best subjects for this retreat study. On one hand, novice individuals might be expected to have a more intense spiritual experience since they have never participated in such a program before. However, people with too little experience with spiritual practices or retreats, might be overwhelmed or confused by the retreat program. They might not be able to engage in the retreat program as fully as someone who was more familiar with the specific elements. Since our goal was to observe the effect of the retreat program rather that assess how different types of individuals might experience it, we decided to not make the level of prior spiritual involvement an inclusion criteria for enrollment. Thus, our only exclusion criterion was that the study subjects were not permitted to have previously participated in this specific Ignatian Spiritual Exercises retreat. However, future studies might be able to explore the effects of age or gender that might contribute to the impact of the retreat. Younger individuals typically have a greater capacity for neuroplasticity, and hence, may derive more change from various training programs such as a spiritual retreat. Women tend to be more likely to engage in meditation practices, but both men and women have found such practices similarly beneficial (
Upchurch and Johnson 2019).
Since the retreat has a Christian perspective, and all participants identified as Christians, there was an inherent bias towards having a positive experience in the retreat. It is important to develop future study designs that can reduce the participants’ personal beliefs and biases and enroll a diverse group of participants to include persons from different traditions in order to be generalizable to the general population.
Overall, these preliminary data represent changes in functional connectivity using fMRI associated with an Ignatian retreat. This preliminary study contributes to the existing literature on the study of meditation, prayer and the associated interconnected networks in the brain that are activated by these practices.