Effect of Aerobic and Anaerobic Exercise on the Complement System of Proteins in Healthy Young Males
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Experimental Protocols
2.3. Blood Testing
2.4. Statistical Analyses
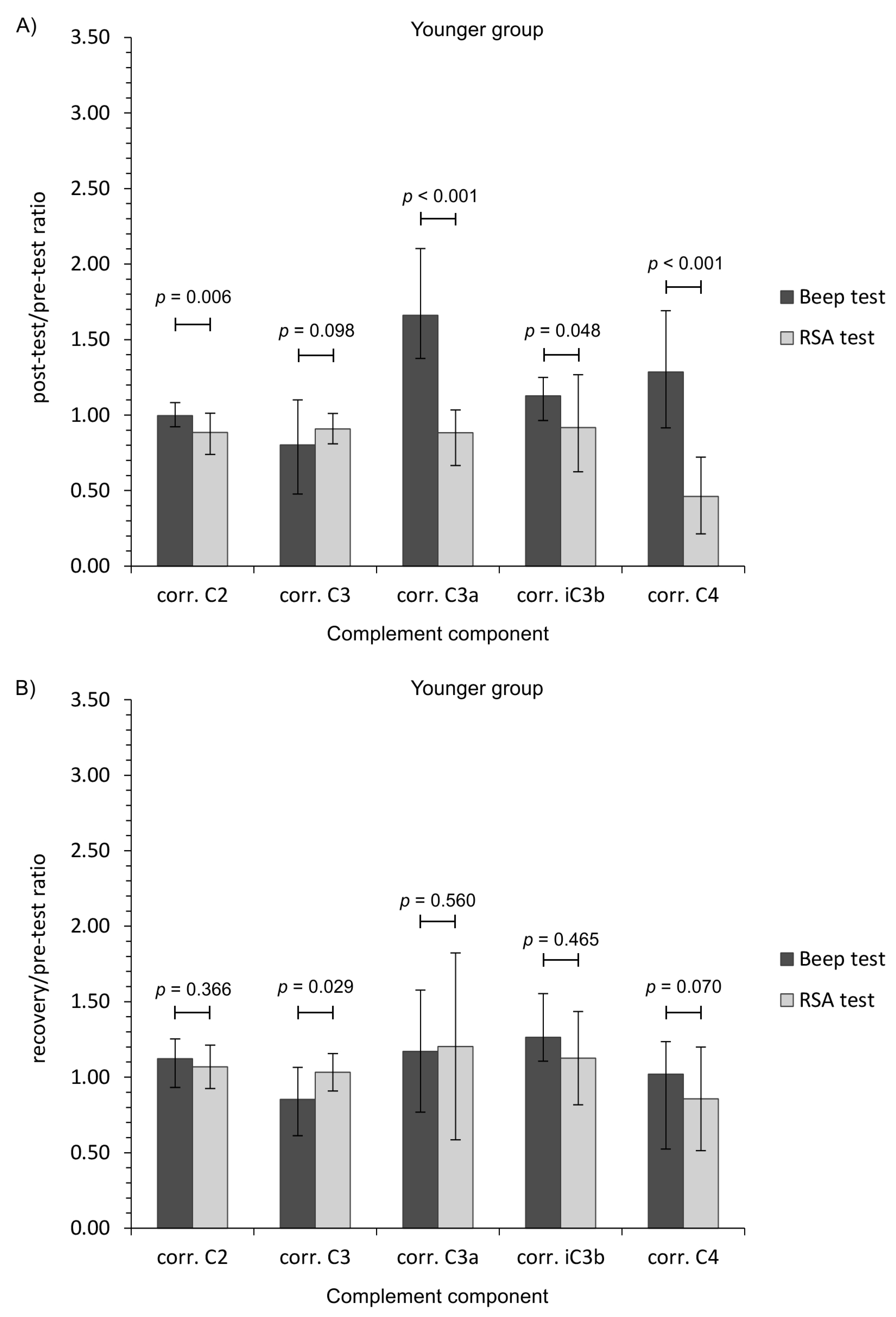
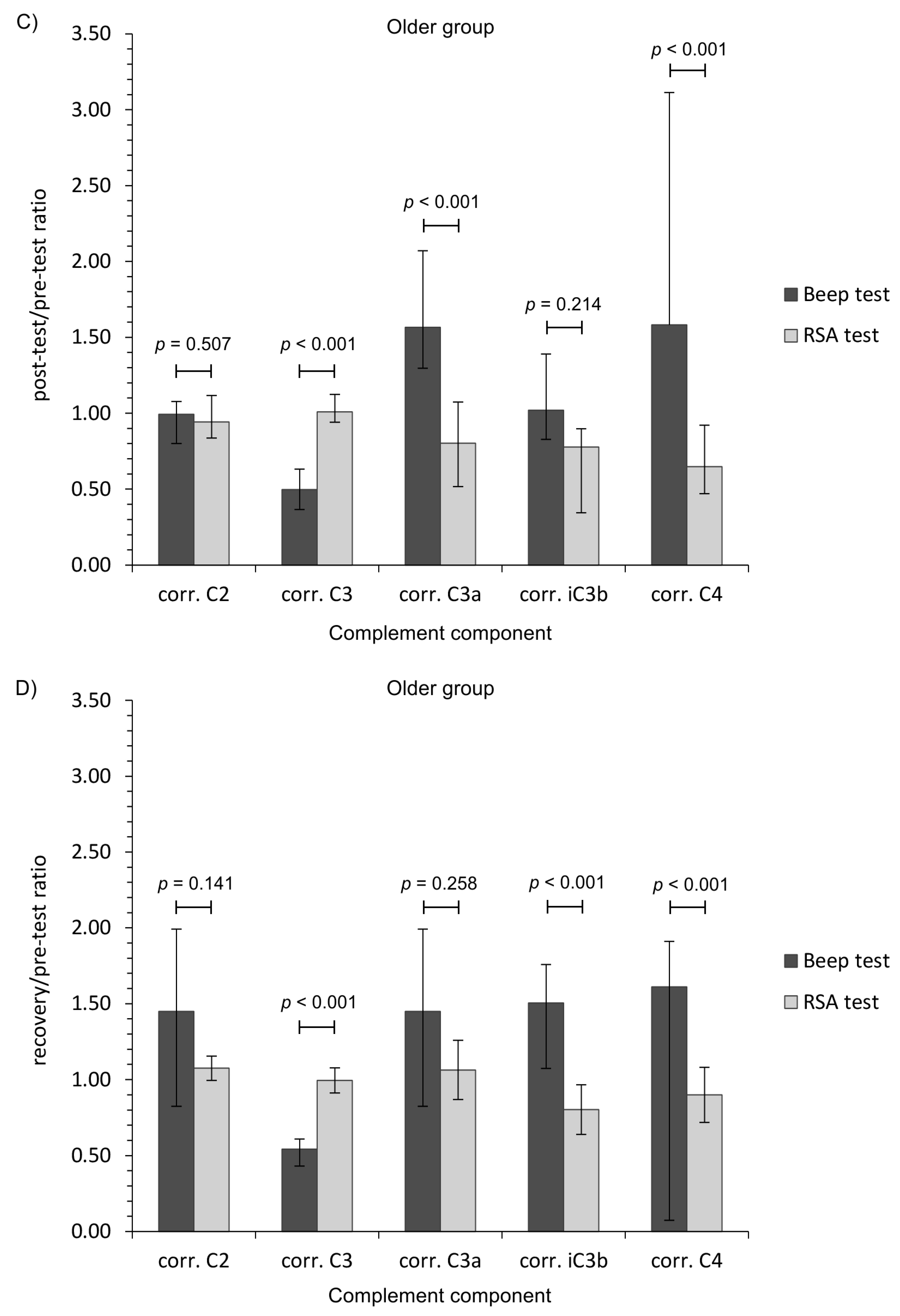
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Medzhitov, R.; Janeway, C.A., Jr. An ancient system of host defense. Curr. Opin. Immunol. 1998, 10, 12–15. [Google Scholar] [CrossRef]
- Carroll, M.C. A protective role for innate immunity in autoimmune disease. Clin. Immunol. 2000, 95, S30–S38. [Google Scholar] [CrossRef]
- Schifferli, J.A.; Ng, Y.C.; Peters, D.K. The role of complement and its receptor in the elimination of immune complexes. N. Engl. J. Med. 1986, 315, 488–495. [Google Scholar] [CrossRef] [PubMed]
- Ricklin, D.; Hajishengallis, G.; Yang, K.; Lambris, J.D. Complement: A key system for immune surveillance and homeostasis. Nat. Immunol. 2010, 11, 785–797. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walport, M.J. Complement. First of two parts. N. Engl. J. Med. 2001, 344, 1058–1066. [Google Scholar] [CrossRef] [PubMed]
- Matsuyama, W.; Nakagawa, M.; Takashima, H.; Muranaga, F.; Sano, Y.; Osame, M. Molecular analysis of hereditary deficiency of the third component of complement (C3) in two sisters. Intern. Med. 2001, 40, 1254–1258. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sarma, J.V.; Ward, P.A. The complement system. Cell Tissue Res. 2011, 343, 227–235. [Google Scholar] [CrossRef]
- Prohászka, Z.; Kirschfink, M.; Frazer-Abel, A. Complement analysis in the era of targeted therapeutics. Mol. Immunol. 2018, 102, 84–88. [Google Scholar] [CrossRef]
- Nieman, D.C. Exercise immunology: Practical applications. Int. J. Sports Med. 1997, 18 (Suppl. 1), S91–S100. [Google Scholar] [CrossRef] [PubMed]
- Peake, J.M.; Neubauer, O.; Della Gatta, P.A.; Nosaka, K. Muscle damage and inflammation during recovery from exercise. J. Appl. Physiol. 2017, 122, 559–570. [Google Scholar] [CrossRef] [PubMed]
- Peake, J.M.; Neubauer, O.; Walsh, N.P.; Simpson, R.J. Recovery of the immune system after exercise. J. Appl. Physiol. 2017, 122, 1077–1087. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Hoffman-Goetz, L. Exercise and the immune system: Regulation, integration, and adaptation. Physiol. Rev. 2000, 80, 1055–1081. [Google Scholar] [CrossRef] [Green Version]
- Liu, X.; Zeng, Z.; Zhao, L.; Xiao, W.; Chen, P. Changes in inflammatory and oxidative stress factors and the protein synthesis pathway in injured skeletal muscle after contusion. Exp. Ther. Med. 2018, 15, 2196–2202. [Google Scholar] [CrossRef]
- Skattum, L.; van Deuren, M.; van der Poll, T.; Truedsson, L. Complement deficiency states and associated infections. Mol. Immunol. 2011, 48, 1643–1655. [Google Scholar] [CrossRef] [PubMed]
- De Cordoba, S.R.; Tortajada, A.; Harris, C.L.; Morgan, B.P. Complement dysregulation and disease: From genes and proteins to diagnostics and drugs. Immunobiology 2012, 217, 1034–1046. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Holers, V.M. Complement and its receptors: New insights into human disease. Annu. Rev. Immunol. 2014, 32, 433–459. [Google Scholar] [CrossRef] [PubMed]
- Dunkelberger, J.R.; Song, W.C. Complement and its role in innate and adaptive immune responses. Cell Res. 2010, 20, 34–50. [Google Scholar] [CrossRef] [Green Version]
- Molina, H.; Holers, V.M.; Li, B.; Fung, Y.; Mariathasan, S.; Goellner, J.; Strauss-Schoenberger, J.; Karr, R.W.; Chaplin, D.D. Markedly impaired humoral immune response in mice deficient in complement receptors 1 and 2. Proc. Natl. Acad. Sci. USA 1996, 93, 3357–3361. [Google Scholar] [CrossRef] [Green Version]
- Qu, H.; Ricklin, D.; Lambris, J.D. Recent developments in low molecular weight complement inhibitors. Mol. Immunol. 2009, 47, 185–195. [Google Scholar] [CrossRef] [Green Version]
- Wagner, E.; Frank, M.M. Therapeutic potential of complement modulation. Nat. Rev. Drug Discov. 2010, 9, 43–56. [Google Scholar] [CrossRef]
- Karacabey, K.; Saygin, O.; Ozmerdivenli, R.; Zorba, E.; Godekmerdan, A.; Bulut, V. The effects of exercise on the immune system and stress hormones in sportswomen. Neuroendocrinol. Lett. 2005, 26, 361–366. [Google Scholar]
- Mashiko, T.; Umeda, T.; Nakaji, S.; Sugawara, K. Position related analysis of the appearance of and relationship between post-match physical and mental fatigue in university rugby football players. Br. J. Sports Med. 2004, 38, 617–621. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Karacabey, K.; Peker, İ.; Saygın, Ö.; Cıloglu, F.; Ozmerdivenli, R.; Bulut, V. Effects of acute aerobic and anaerobic exercise on humoral immune factors in elite athletes. Biotechnol. Biotechnol. Eq. 2005, 19, 175–180. [Google Scholar] [CrossRef]
- Kostrzewa-Nowak, D.; Nowak, R. Analysis of selected T cell subsets in peripheral blood after exhaustive effort among elite soccer players. Biochem. Med. (Zagreb) 2018, 28, 030707. [Google Scholar] [CrossRef] [PubMed]
- Kostrzewa-Nowak, D.; Buryta, R.; Nowak, R. Comparison of selected CD45+ cell subsets’ response and cytokine levels on exhaustive effort among soccer players. J. Med. Biochem. 2019, 38, 256–267. [Google Scholar] [CrossRef] [Green Version]
- Nowak, R.; Kostrzewa-Nowak, D. Assessment of selected exercise-induced CD3+ cell subsets and cell death parameters among soccer players. J. Med. Biochem. 2019, 38, 437–444. [Google Scholar] [CrossRef]
- Kostrzewa-Nowak, D.; Nowak, R. T helper cell-related changes in peripheral blood induced by progressive effort among soccer players. PLoS ONE 2020, 15, e0227993. [Google Scholar] [CrossRef]
- Kostrzewa-Nowak, D.; Ciechanowicz, A.; Clark Jeremy, S.C.; Nowak, R. Damage-associated molecular patterns and Th-cell-related cytokines released after progressive effort. J. Clin. Med. 2020, 9, 876. [Google Scholar] [CrossRef] [Green Version]
- Spielmann, G.; McFarlin, B.K.; O’Connor, D.P.; Smith, P.J.; Pircher, H.; Simpson, R.J. Aerobic fitness is associated with lower proportions of senescent blood T-cells in man. Brain Behav. Immun. 2011, 25, 1521–1529. [Google Scholar] [CrossRef]
- Kakanis, M.W.; Peake, J.; Brenu, E.W.; Simmonds, M.; Gray, B.; Hooper, S.L.; Marshall-Gradisnik, S.M. The open window of susceptibility to infection after acute exercise in healthy young male elite athletes. Exerc. Immunol. Rev. 2010, 16, 119–137. [Google Scholar] [CrossRef] [Green Version]
- Léger, L.A.; Lambert, J. A maximal multistage 20-m shuttle run test to predict VO2 max. Eur. J. Appl. Physiol. Occup. Physiol. 1982, 49, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Metsios, G.S.; Flouris, A.D.; Koutedakis, Y.; Nevill, A. Criterion-related validity and test-retest reliability of the 20 m square shuttle test. J. Sci. Med. Sport 2008, 11, 214–217. [Google Scholar] [CrossRef] [PubMed]
- Chaouachi, A.; Manzi, V.; Wong, D.P.; Chaalali, A.; Laurencelle, L.; Chamari, K.; Castagna, C. Intermittent endurance and repeated sprint ability in soccer players. J. Strength Cond. Res. 2010, 24, 2663–2669. [Google Scholar] [CrossRef] [PubMed]
- Ramos-Campo, D.J.; Martínez-Guardado, I.; Olcina, G.; Marín-Pagán, C.; Martínez-Noguera, F.J.; Carlos-Vivas, J.; Alcaraz, P.E.; Rubio, J.Á. Effect of high-intensity resistance circuit-based training in hypoxia on aerobic performance and repeat sprint ability. Scand. J. Med. Sci. Sports 2018, 28, 2135–2143. [Google Scholar] [CrossRef] [PubMed]
- Flouris, A.D.; Metsios, G.S.; Koutedakis, Y. Enhancing the efficacy of the 20 m multistage shuttle run test. Br. J. Sports Med. 2005, 39, 166–170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Faude, O.; Kindermann, W.; Meyer, T. Lactate threshold concepts: How valid are they? Sports Med. 2009, 39, 469–490. [Google Scholar] [CrossRef]
- Smekal, G.; von Duvillard, S.P.; Pokan, R.; Hofmann, P.; Braun, W.A.; Arciero, P.J.; Tschan, H.; Wonisch, M.; Baron, R.; Bachl, N. Blood lactate concentration at the maximal lactate steady state is not dependent on endurance capacity in healthy recreationally trained individuals. Eur. J. Appl. Physiol. 2012, 112, 3079–3086. [Google Scholar] [CrossRef]
- Beneke, R.; Leithäuser, R.M.; Ochentel, O. Blood lactate diagnostics in exercise testing and training. Int. J. Sports Physiol. Perform. 2011, 6, 8–24. [Google Scholar] [CrossRef] [Green Version]
- Alis, R.; Sanchis-Gomar, F.; Lippi, G.; Roamgnoli, M. Microcentrifuge or automated hematological analyzer to assess hematocrit in exercise? Effect on plasma volume loss calculations. J. Lab. Autom. 2016, 21, 470–477. [Google Scholar] [CrossRef] [Green Version]
- Nieman, D.C.; Tan, S.A.; Lee, J.W.; Berk, L.S. Complement and immunoglobulin levels in athletes and sedentary controls. Int. J. Sports Med. 1989, 10, 124–128. [Google Scholar] [CrossRef]
- Simpson, R.J.; Kunz, H.; Agha, N.; Graff, R. Exercise and the Regulation of Immune Functions. Prog. Mol. Biol. Transl. Sci. 2015, 135, 355–380. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, B.K.; Rohde, T.; Zacho, M. Immunity in athletes. J. Sports Med. Phys. Fit. 1996, 36, 236–245. [Google Scholar]
- Keaney, L.C.; Kilding, A.E.; Merien, F.; Dulson, D.K. The impact of sport related stressors on immunity and illness risk in team-sport athletes. J. Sci. Med. Sport 2018, 21, 1192–1199. [Google Scholar] [CrossRef] [PubMed]
- Walsh, N.P.; Oliver, S.J. Exercise, immune function and respiratory infection: An update on the influence of training and environmental stress. Immunol. Cell Biol. 2016, 94, 132–139. [Google Scholar] [CrossRef]
- Zhao, G.; Zhou, S.; Davie, A.; Su, Q. Effects of moderate and high intensity exercise on T1/T2 balance. Exerc. Immunol. Rev. 2012, 18, 98–114. [Google Scholar]
- Abd El-Kader, S.M.; Al-Shreef, F.M. Inflammatory cytokines and immune system modulation by aerobic versus resisted exercise training for elderly. Afr. Health Sci. 2018, 18, 120–131. [Google Scholar] [CrossRef] [Green Version]
- Gleeson, M.; Walsh, N.P.; British Association of Sport and Exercise Sciences. The BASES expert statement on exercise, immunity, and infection. J. Sports Sci. 2012, 30, 321–324. [Google Scholar] [CrossRef] [Green Version]
- Gleeson, M.; Williams, C. Intense exercise training and immune function. Nestle Nutr. Inst. Workshop Ser. 2013, 76, 39–50. [Google Scholar] [CrossRef]
- Gabriel, H.; Kindermann, W. The acute immune response to exercise: What does it mean? Int. J. Sports Med. 1997, 18 (Suppl. 1), S28–S45. [Google Scholar] [CrossRef]
- Kostrzewa-Nowak, D.; Nowak, R.; Chamera, T.; Buryta, R.; Moska, W.; Cięszczyk, P. Post-effort chances in C-reactive protein level among soccer players at the end of the training season. J. Strength Cond. Res. 2015, 29, 1399–1405. [Google Scholar] [CrossRef]
- Rosety-Rodriguez, M.; Diaz, A.J.; Rosety, I.; Rosety, M.A.; Camacho, A.; Fornieles, G.; Rosety, M.; Ordonez, F.J. Exercise reduced inflammation: But for how long after training? J. Intellect. Disabil. Res. 2014, 58, 874–879. [Google Scholar] [CrossRef] [PubMed]
- Saygin, O.; Karacabey, K.; Ozmerdivenli, R.; Zorba, E.; Ilhan, F.; Bulut, V. Effect of chronic exercise on immunoglobin, complement and leukocyte types in volleyball players and athletes. Neuro Endocrinol. Lett. 2006, 27, 271–276. [Google Scholar] [PubMed]
- Delgado-Alfonso, A.; Pérez-Bey, A.; Conde-Caveda, J.; Izquierdo-Gómez, R.; Esteban-Cornejo, I.; Gómez-Martínez, S.; Marcos, A.; Castro-Piñero, J.; UP&DOWN Study Group. Independent and combined associations of physical fitness components with inflammatory biomarkers in children and adolescents. Pediatr. Res. 2018, 84, 704–712. [Google Scholar] [CrossRef] [PubMed]
- Dufaux, B.; Order, U.; Liesen, H. Effect of a short maximal physical exercise on coagulation, fibrinolysis, and complement system. Int. J. Sports Med. 1991, 12 (Suppl. 1), S38–S42. [Google Scholar] [CrossRef]
- Semple, S.J.; Smith, L.L.; McKune, A.J.; Neveling, N.; Wadee, A. Alterations in acute-phase reactants (CRP, rheumatoid factor, complement, Factor B, and immune complexes) following an ultramarathon. South Afr. J. Sports Med. 2004, 16, 17–21. [Google Scholar] [CrossRef] [Green Version]
- Smith, J.K.; Chi, D.S.; Krish, G.; Reynolds, S.; Cambron, G. Effect of exercise on complement activity. Ann. Allergy 1990, 65, 304–310. [Google Scholar]
- Berk, M.; Wadee, A.A.; Kuschke, R.H.; O’Neill-Kerr, A. Acute phase proteins in major depression. J. Psychosom. Res. 1997, 43, 529–534. [Google Scholar] [CrossRef]
- Navarro Sanz, A.; Barruecos Francioni, J.E.; Sánchez, L.G.; Narvaez de Linares, A.; Galeas-López, J.L.; Robles Rodríguez, A.; Fernández Ortega, J.F. Effect of exhaustive exercise on the immune system, measured through complement activation and C-reactive protein. Arch. Med. Deporte 2013, 30, 348–353. [Google Scholar]
- Semple, S.J.; Smith, L.L.; McKune, A.J.; Hoyos, J.; Mokgethwa, B.; San Juan, A.F.; Lucia, A.; Wadee, A.A. Serum concentrations of C reactive protein, alpha1 antitrypsin, and complement (C3, C4, C1 esterase inhibitor) before and during the Vuelta a España. Br. J. Sports Med. 2006, 40, 124–127. [Google Scholar] [CrossRef] [Green Version]
- Hanson, P.G.; Flaherty, D.K. Immunological responses to training in conditioned runners. Clin. Sci. (Lond.) 1981, 60, 225–228. [Google Scholar] [CrossRef] [Green Version]
- Córdova, A.; Sureda, A.; Tur, J.A.; Pons, A. Immune response to exercise in elite sportsmen during the competitive season. J. Physiol. Biochem. 2010, 66, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Papanastasiou, M.; Koutsogiannaki, S.; Sarigiannis, Y.; Geisbrecht, B.V.; Ricklin, D.; Lambris, J.D. Structural Implications for the Formation and Function of the Complement Effector Protein iC3b. J. Immunol. 2017, 198, 3326–3335. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Manderson, G.A.; Martin, M.; Onnerfjord, P.; Saxne, T.; Schmidtchen, A.; Mollnes, T.E.; Heinegård, D.; Blom, A.M. Interactions of histidine-rich glycoprotein with immunoglobulins and proteins of the complement system. Mol. Immunol. 2009, 46, 3388–3398. [Google Scholar] [CrossRef] [PubMed]
- Shephard, R.J.; Shek, P.N. Acute and chronic over-exertion: Do depressed immune responses provide useful markers? Int. J. Sports Med. 1998, 19, 159–171. [Google Scholar] [CrossRef] [PubMed]
- Artero, E.G.; España-Romero, V.; Jiménez-Pavón, D.; Martinez-Gómez, D.; Warnberg, J.; Gómez-Martínez, S.; González-Gross, M.; Vanhelst, J.; Kafatos, A.; Molnar, D.; et al. Muscular fitness, fatness and inflammatory biomarkers in adolescents. Pediatr. Obes. 2014, 9, 391–400. [Google Scholar] [CrossRef] [Green Version]
- Blankenberg, S.; Barbaux, S.; Tiret, L. Adhesion molecules and atherosclerosis. Atherosclerosis 2003, 170, 191–203. [Google Scholar] [CrossRef]
- Kampert, J.B.; Blair, S.N.; Barlow, C.E.; Kohl, H.W., III. Physical activity, physical fitness, and all-cause and cancer mortality: A prospective study of men and women. Ann. Epidemiol. 1996, 6, 452–457. [Google Scholar] [CrossRef]
- Ruiz, J.R.; Sui, X.; Lobelo, F.; Morrow, J.R., Jr.; Jackson, A.W.; Sjöström, M.; Blair, S.N. Association between muscular strength and mortality in men: Prospective cohort study. BMJ 2008, 337, a439. [Google Scholar] [CrossRef] [Green Version]
- Phillips, C.M.; Dillon, C.B.; Perry, I.J. Does replacing sedentary behaviour with light or moderate to vigorous physical activity modulate inflammatory status in adults? Int. J. Behav. Nutr. Phys. Act. 2017, 14, 138. [Google Scholar] [CrossRef] [Green Version]
| Variable | Younger Group (n = 39) | Older Group (n = 12) | pMW 1 |
|---|---|---|---|
| Age (years) | 16 (15–17) | 19 (18–21) | <0.001 |
| Height (cm) | 180 (177–185) | 182 (180–184) | 0.189 |
| Weight (kg) | 70.2 (64.0–75.3) | 77.3 (72.9–79.2) | 0.010 |
| BMI (kg/m2) | 21.7 (20.0–22.7) | 22.6 (21.9–23.9) | 0.008 |
| BMR (kJ) | 8004 (7636–8933) | 8771 (8219–9016) | 0.229 |
| Fat (%) | 12.5 (9.5–14.6) | 8.6 (6.5–12.7) | 0.060 |
| Fat mass (kg) | 8.6 (6.2–9.9) | 6.5 (4.6–9.4) | 0.296 |
| FFM (kg) | 59.9 (55.6–66.4) | 67.4 (64.4–69.8) | 0.010 |
| TBW (kg) | 43.9 (40.7–48.6) | 49.3 (47.1–51.1) | 0.011 |
| VO2max (mL/kg/min) | 54.62 (51.46–57.78) | 57.78 (53.04–57.78) | 0.256 |
| Test Result | Younger Group (n = 39) | Older Group (n = 12) | pMW 1 |
|---|---|---|---|
| Beep decimal score | 12.7 (10.1–15.3) | 13.7 (10.7–15.0) | 0.257 |
| RSA mean score (s) | 3.28 (3.12–3.55) | 3.22 (3.10–3.37) | 0.271 |
| Variable | Younger Group (n = 39) | Older Group (n = 12) | |||
|---|---|---|---|---|---|
| Beep Test | RSA Test | Beep Test | RSA Test | ||
| Corrected TP (g/L) | pF 1 | 0.009 | <0.001 | 0.338 | 0.002 |
| pre-test | 66.3 (64.2–68.6) | 69.7 aa (67.7–72.1) | 66.6 (64.2–68.2) | 70.8 aa (68.9–72.8) | |
| post-test | 64.4 bb (61.3–70.0) | 67.1 bbb (64.3–69.2) | 66.7 (61.5–68.2) | 65.7 b (63.0–67.6) | |
| recovery | 67.5 (64.7–73.2) | 70.9 (68.1–77.0) | 68.2 (63.3–71.0) | 68.7 (66.1–72.8) | |
| Δ corrected TP | Δp | 3.4 (1.9–5.0) | –2.2 (−4.7–−0.3) | −1.6 (−4.3–1.6) | −4.0 (−6.9–−2.2) |
| Δr | 1.5 (−1.5–4.9) | 0.2 (−2.3–8.3) | 2.1 (−2.8–4.6) | −1.1 (−5.6–3.6) | |
| Corrected albumin (g/L) | pF | <0.001 | <0.001 | 0.338 | 0.009 |
| pre-test | 47.3 (46.2–49.3) | 52.2 aa (49.6–54.4) | 47.5 (46.0–48.1) | 52.9 aa (51.8–55.1) | |
| post-test | 46.0 bbb (42.3–48.4) | 49.7 bbb (47.7–50.7) | 46.1 (44.2–47.2) | 48.2 (46.8–49.0) | |
| recovery | 50.0 c (46.5–52.1) | 52.7 (49.6–55.5) | 48.5 (44.7–50.2) | 49.5 (47.7–52.9) | |
| Δ corrected albumin | Δp | −2.0 (−4.5–0.9) | −2.3 (−4.9–0.4) | −2.0 (−3.0–0.7) | −6.0 (−7.4–−2.8) |
| Δr | 1.6 (−1.1–5.3) | −0.3 (−4.0–7.0) | 1.5 (−1.6–2.3) | −4.8 (−6.1–0.3) | |
| Corrected CRP (mg/L) | pF | <0.001 | 0.003 | 0.039 | 0.779 |
| pre-test | 1.50 aaa (1.00–2.00) | 3.91 aa (3.25–4.50) | 1.15 (0.60–2.00) | 4.89 (4.26–6.16) | |
| post-test | 0.32 (0.00–0.83) | 4.65 (4.08–6.85) | 1.18 b (0.84–1.71) | 5.72 (3.97–6.13) | |
| recovery | 0.20 cc (0.00–1.22) | 4.39 c (2.69–7.37) | 1.94 (1.44–2.30) | 5.00 (4.53–6.25) | |
| Δ corrected CRP | Δp | −1.10 (−1.80–−0.15) | 0.85 (0.04–2.56) | −0.13 (−0.50–0.43) | 0.29 (−048–0.96) |
| Δr | −1.30 (−1.80–0.17) | 0.30 (0.06–2.26) | 0.72 (−0.15–1.26) | 0.09 (−1.34–1.10) | |
| Corrected LA (mmol/L) | pF | <0.001 | <0.001 | <0.001 | <0.001 |
| pre-test | 3.1 aaa (2.8–3.5) | 5.3 aaa (3.0–6.2) | 3.2 aa (2.9–3.5) | 6.1 aaa (5.4–7.3) | |
| post-test | 9.2 bbb (7.5–10.7) | 16.4 bbb (9.8–20.5) | 10.1 bbb (8.9–11.5) | 20.5 bbb (18.3–21.0) | |
| recovery | 3.1 (2.6–3.6) | 4.2 (2.5–5.7) | 2.7 (2.5–3.4) | 5.3 (4.5–6.2) | |
| Δ corrected LA | Δp | 6.1 (4.4–7.6) | 10.4 (6.9–15.7) | 7.2 (5.5–8.0) | 13.8 (11.7–15.3) |
| Δr | −0.1 (−0.6–0.2) | −0.5 (−1.0–0.2) | −0.3 (−0.7–−0.1) | −0.6 (−1.3–−0.2) | |
| Variable | Younger Group (n = 39) | Older Group (n = 12) | |||
|---|---|---|---|---|---|
| Beep Test | RSA Test | Beep Test | RSA Test | ||
| Corrected C2 (ng/mL) | pF 1 | <0.001 | <0.001 | 0.002 | 0.097 |
| pre-test | 8.86 (7.69–9.87) | 7.25 a (6.06–8.36) | 9.57 (7.92–10.31) | 7.57 (6.57–8.12) | |
| post-test | 8.80 bbb (8.08–9.62) | 6.05 bbb (5.22–8.12) | 8.51 bb (7.82–9.52) | 7.00 (6.09–8.08) | |
| recovery | 9.88 cc (8.92–11.21) | 7.95 (6.27–10.0) | 11.33 cc (9.53–13.07) | 8.60 (6.92–9.16) | |
| Δ corrected C2 | Δp | −0.04 (−0.70–0.68) | −0.81 (−1.67–0.16) | −0.23 (−2.01–0.64) | −0.44 (−2.05–0.31) |
| Δr | 1.20 (−0.09–2.39) | 0.40 (−0.53–1.73) | 1.64 (0.43–2.67) | 0.45 (−0.38–1.23) | |
| Corrected C3 (mg/dL) | pF | <0.001 | 0.005 | <0.001 | 0.920 |
| pre-test | 114.2 aaa (80.8–156.3) | 85.0 (74.6–98.6) | 192.7 aaa (189.0–212.9) | 79.6 (66.0–99.4) | |
| post-test | 86.0 b (62.3–111.3) | 74.0 bb (61.6–93.5) | 100.0 (68.7–126.2) | 85.0 (68.4–88.1) | |
| recovery | 92.9 (74.8–118.6) | 91.4 (73.0–103.0) | 110.8 cc (98.2–123.5) | 81.2 (67.9–88.3) | |
| Δ corrected C3 | Δp | −22.8 (−66.5–7.7) | −8.8 (−16.3–0.6) | −102.2 (−118.5–−76.7) | 0.7 (−9.4–6.1) |
| Δr | −15.4 (−46.2–9.1) | 3.2 (−6.6–14.6) | –89.3 (−110.1–−66.1) | −0.3 (−9.1–4.9) | |
| Corrected C3a (ng/mL) | pF | <0.001 | <0.001 | 0.002 | 0.174 |
| pre-test | 0.26 aaa (0.20–0.35) | 0.27 (0.19–0.36) | 0.22 aa (0.19–0.27) | 0.27 (0.22–0.35) | |
| post-test | 0.43 bbb (0.36–0.56) | 0.27 bbb (0.16–0.35) | 0.39 (0.32–0.46) | 0.20 (0.14–0.31) | |
| recovery | 0.31 (0.22–0.40) | 0.35 c (0.27–0.43) | 0.37 (0.25–0.42) | 0.32 (0.26–0.36) | |
| Δ corrected C3a | Δp | 0.19 (0.10–0.27) | −0.04 (−0.09–0.03) | 0.15 (0.08–0.21) | −0.04 (−0.10–0.02) |
| Δr | 0.03 (−0.06–0.13) | 0.05 (0.02–0.18) | 0.10 (−0.03–0.21) | 0.02 (−0.02–0.06) | |
| Corrected iC3b (mg/mL) | pF | 0.001 | 0.855 | 0.006 | 0.174 |
| pre-test | 0.70 (0.66–0.87) | 0.37 (0.30–0.60) | 0.63 (0.54–0.76) | 0.46 (0.28–0.58) | |
| post-test | 0.80 (0.71–0.93) | 0.35 (0.24–0.45) | 0.77 b (0.44–0.90) | 0.36 (0.29–0.47) | |
| recovery | 0.95 ccc (0.76–1.07) | 0.37 (0.30–0.54) | 0.94 c (0.92–1.04) | 0.39 (0.28–0.44) | |
| Δ corrected iC3b | Δp | 0.10 (−0.03–0.18) | −0.05 (−0.23–0.08) | 0.02 (−0.09–0.22) | −0.07 (−0.15–0.06) |
| Δr | 0.21 (−0.02–0.31) | 0.05 (−0.07–0.15) | 0.34 (0.19–0.43) | −0.08 (−0.16–−0.01) | |
| Corrected C4 (mg/dL) | pF | 0.022 | <0.001 | <0.001 | 0.004 |
| pre-test | 9.64 a (5.22–13.80) | 5.31 aaa (2.13–7.84) | 3.33 aa (2.80–8.46) | 8.91 aa (4.75–11.93) | |
| post-test | 10.21 (7.33–15.72) | 2.89 bb (0.45–6.07) | 8.62 (6.20–10.17) | 6.13 (2.45–9.30) | |
| recovery | 10.10 (7.24–15.30) | 4.35 (1.51–6.93) | 9.40 ccc (5.50–13.55) | 9.03 (4.04–12.08) | |
| Δ corrected C4 | Δp | 1.73 (−1.20–4.77) | −1.87 (−2.99–−1.22) | 2.87 (1.81–5.88) | −2.11 (−3.10–−1.56) |
| Δr | 0.14 (−2.79–4.26) | –0.65 (−2.71–0.74) | 4.70 (1.62–6.91) | −0.80 (−1.88–0.77) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kostrzewa-Nowak, D.; Kubaszewska, J.; Nowakowska, A.; Nowak, R. Effect of Aerobic and Anaerobic Exercise on the Complement System of Proteins in Healthy Young Males. J. Clin. Med. 2020, 9, 2357. https://doi.org/10.3390/jcm9082357
Kostrzewa-Nowak D, Kubaszewska J, Nowakowska A, Nowak R. Effect of Aerobic and Anaerobic Exercise on the Complement System of Proteins in Healthy Young Males. Journal of Clinical Medicine. 2020; 9(8):2357. https://doi.org/10.3390/jcm9082357
Chicago/Turabian StyleKostrzewa-Nowak, Dorota, Joanna Kubaszewska, Anna Nowakowska, and Robert Nowak. 2020. "Effect of Aerobic and Anaerobic Exercise on the Complement System of Proteins in Healthy Young Males" Journal of Clinical Medicine 9, no. 8: 2357. https://doi.org/10.3390/jcm9082357
APA StyleKostrzewa-Nowak, D., Kubaszewska, J., Nowakowska, A., & Nowak, R. (2020). Effect of Aerobic and Anaerobic Exercise on the Complement System of Proteins in Healthy Young Males. Journal of Clinical Medicine, 9(8), 2357. https://doi.org/10.3390/jcm9082357





