A Cohort of Patients with COVID-19 in a Major Teaching Hospital in Europe
Abstract
1. Introduction
2. Methods
2.1. Study Population
2.2. Data Collection
2.3. Statistical Analysis
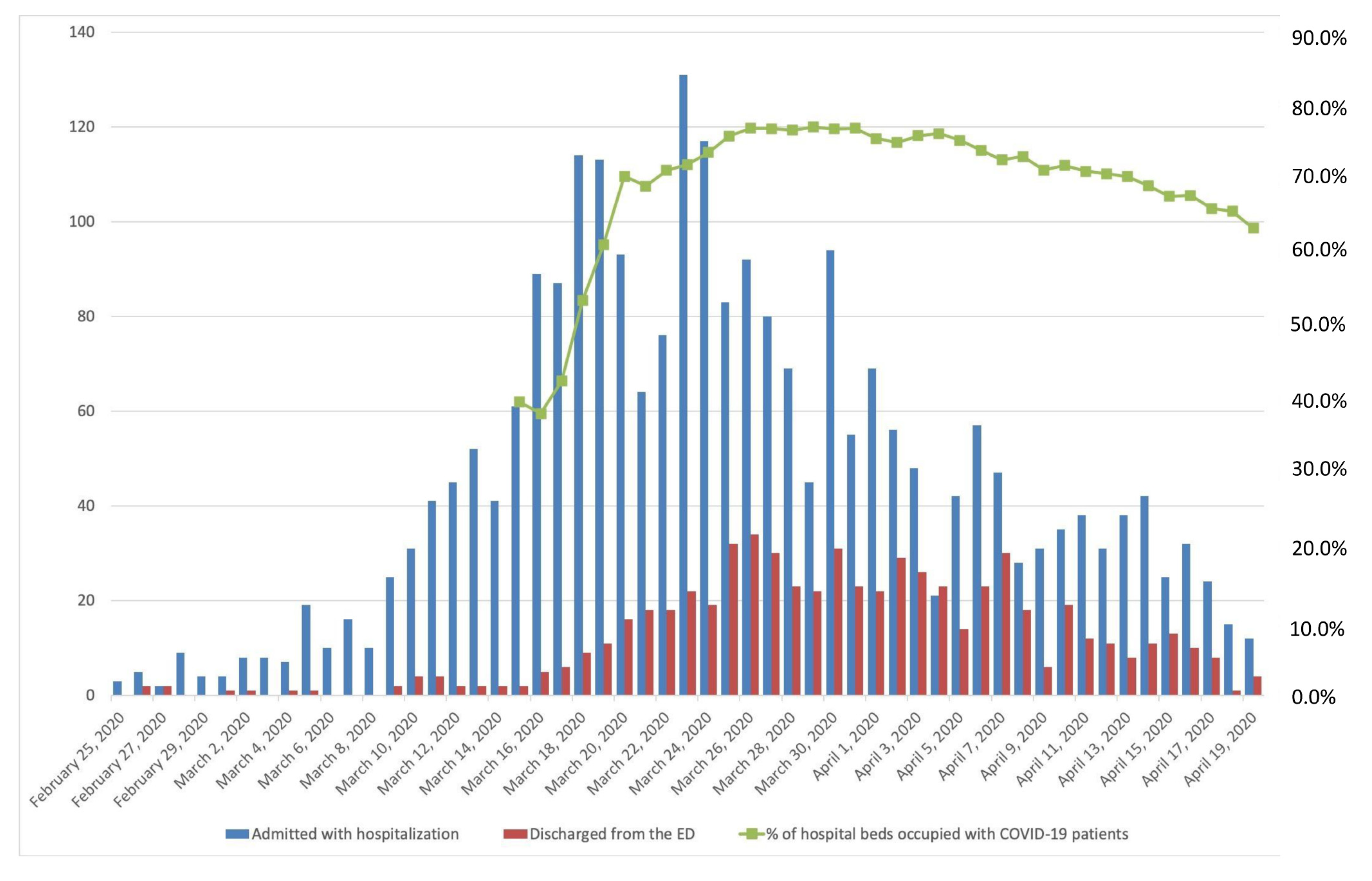
3. Results
4. Discussion
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Spiteri, G.; Fielding, J.; Diercke, M.; Campese, C.; Enouf, V.; Gaymard, A.; Bella, A.; Sognamiglio, P.; Moros, M.J.S.; Riutort, A.N.; et al. First cases of coronavirus disease 2019 (COVID-19) in the WHO European Region, 24 January to 21 February 2020. Eurosurveillance 2020, 25. [Google Scholar] [CrossRef] [PubMed]
- Instituto Nacional de Estadística. Población Residente por Fecha, Sexo y Edad. Madrid, España. Available online: https://www.ine.es/jaxiT3/Tabla.htm?t=9663&L=0 (accessed on 26 April 2020).
- Centro de Coordinación de Alertas y Emergencias Sanitarias. Enfermedad por el Coronavirus (COVID-19). España: Ministerio de Sanidad. Available online: https://www.mscbs.gob.es/profesionales/saludPublica/ccayes/alertasActual/nCov-China/situacionActual.htm (accessed on 26 April 2020).
- COVID-19. Situación Actual en la Comunidad de Madrid. Informe de Situación del 27 de Abril. Available online: https://www.comunidad.madrid/sites/default/files/doc/sanidad/200425_cam_covid19.pdf (accessed on 26 April 2020).
- Ministero della Salute. Covid-19, i casi in Italia il 25 Aprile ore 18. Available online: http://www.salute.gov.it/imgs/C_17_notizie_4605_0_file.pdf (accessed on 26 April 2020).
- New York City Health. COVID-19: Data. Available online: https://www1.nyc.gov/site/doh/covid/covid-19-data.page (accessed on 26 April 2020).
- Novel Coronaviris (nCoV) Acute Respiratory Infection Clinical Characterisation Data Tools. nCoV Case Records Form Version 1.3. 24 Feb 2020. Adapted from Sprint Sari Case Report form by ISARIC. Available online: https://media.tghn.org/medialibrary/2020/03/ISARIC_COVID-19_CRF_V1.3_24Feb2020.pdf (accessed on 16 February 2020).
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria. Available online: https://www.R-project.org. (accessed on 10 April 2020).
- Goyal, P.; Choi, J.J.; Pinheiro, L.C.; Schenck, E.J.; Chen, R.; Jabri, A.; Satlin, M.J.; Campion, T.R., Jr.; Nahid, M.; Ringel, J.B.; et al. Clinical Characteristics of Covid-19 in New York City. New Engl. J. Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Richardson, S.; Hirsch, J.S.; Narasimhan, M.; Crawford, J.M.; McGinn, T.; Davidson, K.W.; Barnaby, D.P.; Becker, L.B.; Chelico, J.D.; Cohen, S.L.; et al. Presenting Characteristics, Comorbidities, and Outcomes Among 5700 Patients Hospitalized With COVID-19 in the New York City Area. JAMA 2020. [Google Scholar] [CrossRef] [PubMed]
- Garg, S.; Kim, L.; Whitaker, M.; O’Halloran, A.; Cummings, C.; Holstein, R.L.; Prill, M.; Chai, S.J.; Kirley, P.D.; Alden, N.B.; et al. Hospitalization rates and characteristics of patients hospitalized with laboratory-confirmed coronavirus disease 2019—COVID-NET, 14 States, 1–30 March 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 458–464. [Google Scholar] [CrossRef] [PubMed]
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef]
- Wang, D.; Hu, B.; Hu, C.; Zhu, F.; Liu, X.; Zhang, J.; Wang, B.; Xiang, H.; Cheng, Z.; Xiong, Y.; et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus-Infected Pneumonia in Wuhan, China. JAMA 2020. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020. [Google Scholar] [CrossRef] [PubMed]
- Centro Internacional sobre el Envejecimiento. Estimaciones de la Población de la Provincia de Madrid. España. Available online: https://cenie.eu/es/observatorio/demografia/madrid (accessed on 26 April 2020).
- Spinato, G.; Fabbris, C.; Polesel, J.; Cazzador, D.; Borsetto, D.; Hopkins, C.; Boscolo-Rizzo, P. Alterations in smell or taste in mildly symptomatic outpatients with SARS-CoV-2 infection. JAMA 2020. [Google Scholar] [CrossRef] [PubMed]
- Shi, S.; Qin, M.; Shen, B.; Cai, Y.; Liu, T.; Yang, F.; Gong, W.; Liu, X.; Liang, J.; Zhao, Q.; et al. Association of cardiac injury with mortality in hospitalized patients with COVID-19 in Wuhan, China. JAMA Cardiol. 2020. [Google Scholar] [CrossRef] [PubMed]
| Variable | Total | Deaths | Live Discharges | p-Value |
|---|---|---|---|---|
| (N = 2226) | (N = 460) | (N = 1766) | ||
| Median age, years (IQR) | 61 (46–78) | 82.5 (76–87) | 56 (42–71) | < 0.001 (w) |
| Sex, n (%) | < 0.001 | |||
| Male | 1074 (48.2) | 286 (62.2) | 788 (44.6) | |
| Female | 1152 (51.8) | 174 (37.8) | 978 (55.4) | |
| Nursing home resident, n (%) | 709 (31.9) | 125 (27.2) | 584 (33.1) | 0.018 |
| Current smokers, n (%) | 157 (7.1) | 44 (9.6) | 113 (6.4) | 0.023 |
| Comorbidities (at least one), n (%) | 1747 (78.5) | 448 (97.4) | 1299 (73.6) | < 0.001 |
| Arterial hypertension | 920 (41.3) | 318 (69.1) | 602 (34.1) | < 0.001 |
| Chronic heart disease | 429 (19.3) | 195 (42.4) | 234 (13.3) | < 0.001 |
| Diabetes mellitus | 381 (17.1) | 157 (34.1) | 224 (12.7) | < 0.001 |
| Rheumatological disease | 268 (12.0) | 80 (17.4) | 188 (10.6) | < 0.001 |
| Solid malignant disease | 252 (11.3) | 93 (20.2) | 159 (9.0) | < 0.001 |
| Obesity | 242 (10.9) | 66 (14.3) | 176 (10.0) | 0.009 |
| Chronic kidney disease | 174 (7.8) | 94 (20.4) | 80 (4.5) | < 0.001 |
| Chronic obstructive pulmonary disease | 153 (6.9) | 65 (14.1) | 88 (5.0) | < 0.001 |
| Other chronic lung diseases | 143 (6.4) | 49 (10.7) | 94 (5.3) | < 0.001 |
| Hematological malignant disease | 133 (6.0) | 46 (10.0) | 87 (4.9) | < 0.001 |
| Asthma | 115 (5.2) | 17 (3.7) | 98 (5.5) | 0.138 |
| Liver disease | 89 (4.0) | 23 (5.0) | 66 (3.7) | 0.272 |
| HIV infection | 13 (0.6) | 4 (0.9) | 9 (0.5) | 0.3218 (f) |
| Symptoms on admission, n (%) | ||||
| Fever | 1585 (71.2) | 325 (70.7) | 1260 (71.3) | 0.814 |
| Cough | 1373 (61.7) | 228 (49.6) | 1145 (64.8) | < 0.001 |
| Dyspnea | 1108 (49.8) | 278 (60.4) | 830 (47.0) | < 0.001 |
| Myalgia | 596 (26.8) | 51 (11.1) | 545 (30.9) | < 0.001 |
| Diarrhea | 484 (21.7) | 62 (13.5) | 422 (23.9) | < 0.001 |
| Headache | 427 (19.2) | 24 (5.2) | 403 (22.8) | < 0.001 |
| Sputum production | 320 (14.4) | 80 (17.4) | 240 (13.6) | 0.046 |
| Nausea or vomiting | 299 (13.4) | 42 (9.1) | 257 (14.6) | 0.003 |
| Anosmia | 284 (12.8) | 5 (1.1) | 279 (15.8) | 0.003 |
| Respiratory status | ||||
| Median SatO2 on admission, % (IQR) | 95 (92–97) | 90 (85–93.3) | 96 (93–97) | < 0.001 (w) |
| SatO2 < 90% on admission, n (%) | 234 (10.5) | 126 (27.4) | 108 (6.1) | < 0.001 |
| Median time from disease onset to hospital admission, days (IQR) | 6 (3–9) | 4 (2–7) | 7 (3–10) | < 0.001 (w) |
| Complications during hospitalization | ||||
| Acute confusional syndrome | 197 (8.8) | 149 (32.4) | 48 (2.7) | < 0.001 |
| Acute kidney failure | 173 (7.8) | 120 (26.1) | 53 (3.0) | < 0.001 |
| Acute respiratory distress syndrome | 109 (4.9) | 94 (20.4) | 15 (0.8) | < 0.001 |
| Bacterial pneumonia | 64 (2.9) | 45 (9.8) | 19 (1.1) | < 0.001 |
| Acute heart failure | 51 (2.3) | 34 (7.4) | 17 (1.0) | < 0.001 |
| Arrhythmia | 46 (2.1) | 33 (7.2) | 12 (0.7) | < 0.001 |
| Treatment regimens, n (%) | ||||
| Hydroxychloroquine + azithromycin | 706 (31.7) | 180 (39.1) | 526 (29.8) | < 0.001 |
| Hydroxychloroquine | 545 (24.5) | 163 (35.4) | 382 (21.6) | < 0.001 |
| Hydroxychloroquine + lopinavir/ritonavir | 116 (5.2) | 23 (5.0) | 93 (5.3) | 0.911 |
| Hydroxychloroquine + azithromycin + lopinavir/ritonavir | 69 (3.1) | 23 (5.0) | 46 (2.6) | 0.012 |
| Lopinavir/ritonavir | 19 (0.8) | 3 (0.6) | 16 (0.9) | 0.216 (f) |
| Variable | Total | Deaths | Live Discharges | p-Value |
|---|---|---|---|---|
| (N = 75) | (N = 55) | (N = 20) | ||
| Median age, years (IQR) | 64 (54–71) | 69 (62–72.5) | 47 (38.5–56) | < 0.001 (w) |
| Sex, n (%) | 0.127 (f) | |||
| Male | 57 (76) | 39 (70.9) | 18 (90) | |
| Female | 18 (24) | 16 (29.1) | 2 (10) | |
| Current smokers, n (%) | 10 (13.3) | 7 (12.7) | 3 (15) | 1.000 (f) |
| Comorbidities (at least one), n (%) | 67 (89.3) | 52 (94.6) | 15 (75) | 0.045 |
| Arterial hypertension | 39 (52.0) | 32 (58.2) | 7 (35) | 0.130 |
| Obesity | 23 (30.7) | 18 (32.7) | 5 (25) | 0.719 |
| Diabetes mellitus | 21 (28.0) | 17 (30.9) | 4 (20) | 0.401 (f) |
| Chronic obstructive pulmonary disease | 13 (17.3) | 12 (21.8) | 1 (5) | 0.165 (f) |
| Chronic heart disease | 11 (14.7) | 10 (18.2) | 1 (5) | 0.269 (f) |
| Solid malignant disease | 9 (12.0) | 6 (10.9) | 3 (15) | 0.693 (f) |
| Rheumatological disease | 7 (9.3) | 5 (9.1) | 2 (10) | 1.000 (f) |
| Chronic kidney disease | 5 (6.7) | 5 (9.1) | 0 (0) | 0.316 (f) |
| Asthma | 4 (5.3) | 3 (5.5) | 1 (5) | 1.000 (f) |
| Other chronic lung diseases | 4 (5.3) | 4 (7.3) | 0 (0) | 0.568 (f) |
| Liver disease | 3 (4.0) | 2 (3.6) | 1 (5) | 1.000 (f) |
| Hematological malignant disease | 3 (4.0) | 3 (5.5) | 0 (0.0) | 0.560 (f) |
| HIV infection | 1 (1.3) | 1 (1.8) | 0 (0) | 1.000 (f) |
| Respiratory status, n (%) | ||||
| SatO2 < 90% on admission | 11 (17) | 9 (16.3) | 2 (10) | 0.717 (f) |
| Age Group | Male | Female | Total | |||
|---|---|---|---|---|---|---|
| N | Mortality, % | N | Mortality, % | N | Mortality, % | |
| 18–29 years | 59 | 0.0 | 100 | 1.0 | 159 | 0.6 |
| 30–39 years | 86 | 0.0 | 133 | 0.0 | 219 | 0 |
| 40–49 years | 120 | 1.7 | 167 | 1.2 | 287 | 1.5 |
| 50–59 years | 166 | 4.8 | 199 | 3.0 | 365 | 3.8 |
| 60–69 years | 120 | 20.0 | 152 | 7.9 | 327 | 11 |
| 70–79 years | 202 | 41.1 | 156 | 25.0 | 358 | 34.1 |
| 80–89 years | 212 | 62.7 | 179 | 41.3 | 391 | 52.9 |
| ≥90 years | 54 | 66.7 | 66 | 60.6 | 120 | 63.3 |
| Variable, Median (IQR) | N with Data | Total | Deaths | Live Discharges | p-Value |
|---|---|---|---|---|---|
| Entire cohort | n = 2226 | n = 460 | n = 1766 | ||
| Lymphocyte count, | 1805 | 0.93 (0.91–0.97) | 0.68 (0.64–0.74) | 1.02 (0.99–1.06) | < 0.001 (w) |
| ×10⁹/L | |||||
| (NR, 1.1–4.5) | |||||
| ALT, U/L | 1526 | 31 (30–33) | 28 (27–31) | 32 (31–34) | < 0.001 (w) |
| (NR, 0–35) | |||||
| Albumin g/dL | 1200 | 4.2 (4.2–4.3) | 3.9 (3.9–4) | 4.3 (4.3–4.4) | < 0.001 (w) |
| (NR, 2.9–5.2) | |||||
| Creatine kinase, U/L | 1241 | 100 (95–105) | 143 (121–164) | 88 (83–95) | < 0.001 (w) |
| (NR, 40–280) | |||||
| Creatinine mg/dL | 1602 | 0.81 (0.8–0.83) | 1.05 (0.99–1.13) | 0.77 (0.75–0.78) | < 0.001 (w) |
| (NR, 0.7–1.3) | |||||
| D-dimer, ng/mL | 982 | 720 (680–758) | 1590 (1309–1952) | 608 (560–648) | < 0.001 (w) |
| (NR, 0–500) | |||||
| Serum ferritin, ng/L | 599 | 346 (312–393) | 588 (490–741) | 313 (261–358) | < 0.001 (w) |
| (NR, 22–322) | |||||
| Platelet count, ×10⁹/L | 1605 | 218 (213–225) | 198 (186–206) | 226 (219–234) | < 0.001 (w) |
| (NR, 150–370) | |||||
| IL-6, pg/mL | 90 | 28.4 (18.8–40.1) | 30.9 (27.2–244) | 26 (17.9–43.9) | < 0.251 (w) |
| (NR, 0–3.4) | |||||
| Lactate dehydrogenase, U/L (NR, 100–190) | 1458 | 321 (315–330) | 380 (364–408) | 308 (301–316) | < 0.001 (w) |
| Procalcitonin, ng/mL | 637 | 0.12 (0.1–0.14) | 0.4 (0.3–0.5) | 0.09 (0.08–0.11) | < 0.001 (w) |
| (NR, 0–0.5) | |||||
| C-reactive protein, mg/L | 1482 | 71.1 (65.6–77.4) | 137.7 (118.1–153.8) | 57.8 (51.8–62) | < 0.001 (w) |
| (NR, 0–5) | |||||
| Prothrombin time, s | 1581 | 11.1 (11.1–11.2) | 11.5 (11.4–11.7) | 10.9 (10.9–11) | < 0.001 (w) |
| High-sensitivity cardiac | 253 | 11.2 (9.1–18.2) | 66.9 (29.7–115.2) | 8.2 (6.4–11) | < 0.001 (w) |
| troponin I, ng/L | |||||
| (NR, 0–53.5) | |||||
| ICU cohort | n=75 | n=55 | n=20 | ||
| Lymphocyte count, × 10⁹/L | 72 | 0.85 (0.77–0.97) | 0.77 (0.66–0.85) | 0.98 (0.87–1.15) | 0.009 (w) |
| (NR, 1.1–4.5) | |||||
| ALT, U/L | 53 | 38 (32–51) | 35 (31–52) | 47 (29–73) | 0.358 (w) |
| (NR, 0–35) | |||||
| Albumin, g/dL | 28 | 4.1 (4.0–4.3) | 4.1 (4–4.4) | 4.3 (4–4.4) | 0.494 (w) |
| (NR, 2.9–5.2) | |||||
| Creatine kinase, U/L | 33 | 122 (102–176 | 122 (99–176) | 135 (107–329) | 0.679 (w) |
| (NR, 40–280) | |||||
| Creatinine, mg/dL | 64 | 0.89 (0.8–1) | 0.92 (0.82–1.16) | 0.85 (0.73–0.97) | 0.094 (w) |
| (NR, 0.7–1.3) | |||||
| D-dimer, ng/mL | 26 | 1075 (752–1256) | 1088 (745–1824) | 758 (752–1647) | 0.527 (w) |
| (NR, 0–500) | |||||
| Serum ferritin, ng/L | 3 | 817 (520–852) | 835 (817–852) | 520 | 1.000 (w) |
| (NR, 22–322) | |||||
| Platelet count, ×10⁹/L | 65 | 185 (170–224) | 185 (165–225) | 205 (175–265) | 0.654 (w) |
| (NR, 150–370) | |||||
| IL-6, pg/mL | 3 | 30.9 (11.5–244.0) | 30.9 (11.5–244) | - | - |
| (NR, 0–3.4) | |||||
| Lactate dehydrogenase, U/L (NR, 100–190) | 33 | 365 (323–451) | 388 (332–520) | 328 (240–401) | 0.190 (w) |
| Procalcitonin, ng/mL | 17 | 0.2 (0.1–0.5) | 0.38 (0.12–0.93) | 0.08 (0.06–0.16) | 0.019 (w) |
| (NR, 0–0.5) | |||||
| C-reactive protein, mg/L | 58 | 139.8 (109.8–188.4) | 151 (118.1–203) | 123.8 (25.1–169.7) | 0.048 (w) |
| (NR, 0–5) | |||||
| Prothrombin time, s | 63 | 11.2 (11.0–11.4) | 11.3 (11–11.5) | 11.1 (10.5–11.4) | 0.177 (w) |
| High-sensitivity cardiac | 7 | 24.6 (11.2–92.7) | 15.4 (11.2–73.4) | 80.2 (67.2–92.7) | 0.190 (w) |
| troponin I, ng/L | |||||
| (NR, 0–53.5) |
| Variable | Multivariate OR (95% CI) | p-Value |
|---|---|---|
| Age, years | 1.105 (1.087–1.124) | < 0.001 |
| Sex, female | 0.547 (0.375–0.794) | 0.002 |
| SatO2 < 90% | 3.805 (2.539–5.723) | < 0.001 |
| Lymphocyte count, ×10⁹/L | 0.573 (0.356–0.879) | 0.017 |
| C-reactive Protein, mg/L | 1.006 (1.003–1.008) | < 0.001 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Borobia, A.M.; Carcas, A.J.; Arnalich, F.; Álvarez-Sala, R.; Monserrat-Villatoro, J.; Quintana, M.; Figueira, J.C.; Torres Santos-Olmo, R.M.; García-Rodríguez, J.; Martín-Vega, A.; et al. A Cohort of Patients with COVID-19 in a Major Teaching Hospital in Europe. J. Clin. Med. 2020, 9, 1733. https://doi.org/10.3390/jcm9061733
Borobia AM, Carcas AJ, Arnalich F, Álvarez-Sala R, Monserrat-Villatoro J, Quintana M, Figueira JC, Torres Santos-Olmo RM, García-Rodríguez J, Martín-Vega A, et al. A Cohort of Patients with COVID-19 in a Major Teaching Hospital in Europe. Journal of Clinical Medicine. 2020; 9(6):1733. https://doi.org/10.3390/jcm9061733
Chicago/Turabian StyleBorobia, Alberto M., Antonio J. Carcas, Francisco Arnalich, Rodolfo Álvarez-Sala, Jaime Monserrat-Villatoro, Manuel Quintana, Juan Carlos Figueira, Rosario M. Torres Santos-Olmo, Julio García-Rodríguez, Alberto Martín-Vega, and et al. 2020. "A Cohort of Patients with COVID-19 in a Major Teaching Hospital in Europe" Journal of Clinical Medicine 9, no. 6: 1733. https://doi.org/10.3390/jcm9061733
APA StyleBorobia, A. M., Carcas, A. J., Arnalich, F., Álvarez-Sala, R., Monserrat-Villatoro, J., Quintana, M., Figueira, J. C., Torres Santos-Olmo, R. M., García-Rodríguez, J., Martín-Vega, A., Buño, A., Ramírez, E., Martínez-Alés, G., García-Arenzana, N., Núñez, M. C., Martí-de-Gracia, M., Moreno Ramos, F., Reinoso-Barbero, F., Martin-Quiros, A., ... on behalf of the COVID@HULP Working Group. (2020). A Cohort of Patients with COVID-19 in a Major Teaching Hospital in Europe. Journal of Clinical Medicine, 9(6), 1733. https://doi.org/10.3390/jcm9061733







