Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study
Abstract
1. Introduction
2. Experimental Section
2.1. Materials and Methods
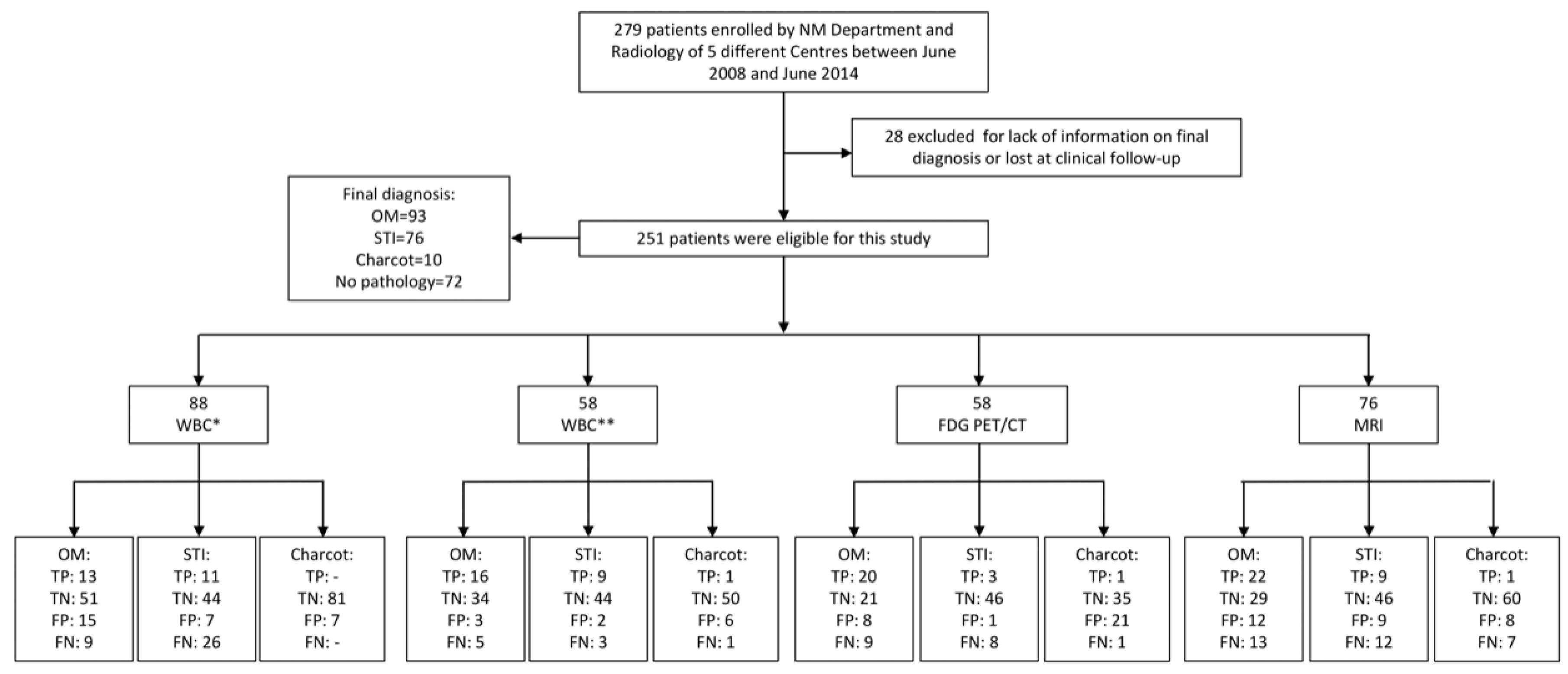
2.1.1. Patients
- Type 1 or type 2 diabetes treated with oral medications or insulin;
- Suspected DFI based on clinical presentation of foot wounds according to Perfusion, Extent, Depth, Infection, Sensation of Infectious Diseases Society of America (PEDIS/IDSA) classification [1];
- At least one out of the three imaging modalities performed for suspected DFI;
- Final diagnosis provided by gold standard;
- Bony abnormalities detected by plain radiographs;
- Palpable bone at “probe-to-bone test” (in presence of open wounds);
- Raised inflammatory markers.
- Lack of information on final diagnosis;
- Patients lost at clinical follow-up.
2.1.2. Imaging Modalities and Analysis
2.1.3. Interpretation Criteria for WBC Scintigraphy
- Acquired according to EANM recommendations: Interpretation criteria were used as recommended by the guidelines [20] and obtained by both visual and, in equivocal cases, semi-quantitative analysis by drawing region of interests (ROIs) on target (T) and contralateral side as background (B) in order to calculate the T/B ratio. OM was defined when WBC focal accumulation at 20–24 h was higher in intensity than at 3–4 h. STI was defined when WBC focal or diffuse accumulation at 20–24 h was lower than at 3–4 h. Charcot was defined when diffuse WBC accumulation at 20–24 h was similar or decreased compared to the uptake at 3–4 h.
- Acquired not according to EANM recommendation: In the case scans were performed with only one time point acquisition, they were classified as follows: OM was defined when the WBC focal accumulation was higher than surrounding tissues. STI was defined when WBC accumulation (both focal or diffuse) was observed in the superficial regions of the foot. Charcot was defined when diffuse WBC accumulation at the mid/hindfoot was observed.
2.1.4. Interpretation Criteria for FDG PET/CT
2.1.5. Interpretation Criteria for MRI
- (a)
- Ulcer (skin interruption with raised margins and associated soft tissue defect);
- (b)
- Sinus tract (“tram track” pattern post-Gd enhancement);
- (c)
- Cellulitis (skin thickening and soft tissue edema with low T1 and T2 signal and post-Gd enhancement);
- (d)
- Abscesses (signal intensity of fluid with post-Gd peripheral rim-like enhancement);
- (e)
- Gangrene (post-Gd non-enhancing area of devitalized tissue that is sharply demarcated from surrounding viable tissue, without (dry gangrene) or with air bubbles in the soft tissue (wet gangrene));
- (f)
- Tenosynovitis (area of post-Gd peri-tendinous enhancement coursing through an area of cellulitis and adjacent to an infected ulcer).
2.1.6. Therapeutic Management
- No treatment (including offloading);
- Conventional wound care and topic antibiotic treatment;
- Systemic antibiotic treatment;
- Surgery (debridement or amputation).
2.1.7. Gold Standard
2.1.8. Statistical Analysis
3. Results
3.1. WBC Scintigraphy
3.2. FDG PET/CT.
3.3. MRI
3.4. Comparison between WBC Scintigraphy, FDG PET/CT, and MRI in Suspected DFI
3.5. Comparison between WBC Scintigraphy Performed according and not according to EANM Guidelines
3.6. Comparison between WBC Scintigraphy, FDG PET/CT, and MRI according to the Location of Disease
3.7. Correlation between the Findings of Diagnostic Tests and Therapeutic Management
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Lipsky, B.A.; Berendt, A.R.; Cornia, P.B.; Pile, J.C.; Peters, E.J.; Armstrong, D.G.; Deery, H.G.; Embil, J.M.; Joseph, W.S.; Karchmer, A.W.; et al. 2012 Infectious Diseases Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot infections. Clin. Infect. Dis. 2012, 54, 132–173. [Google Scholar] [CrossRef]
- Lipsky, B.A.; Aragón-Sánchez, J.; Diggle, M.; Embil, J.; Kono, S.; Lavery, L.; Senneville, É.; Urbančič-Rovan, V.; Van Asten, S. IWGDF guidance on the diagnosis and management of foot infections in persons with diabetes. Diabetes Metab. Res. Rev. 2016, 32, 45–74. [Google Scholar] [CrossRef]
- Treglia, G.; Sadeghi, R.; Annunziata, S.; Zakavi, S.R.; Caldarella, C.; Muoio, B.; Bertagna, F.; Ceriani, L.; Giovannella, L. Diagnostic performance of Fluorine-18-Fluorodeoxyglucose positron emission tomography for the diagnosis of osteomyelitis related to diabetic foot: A systematic review and a meta-analysis. Foot 2013, 23, 140–148. [Google Scholar] [CrossRef]
- Markakis, K.; Bowling, F.L.; Boulton, A.J. The diabetic foot in 2015: An overview. Diabetes Metab. Res. Rev. 2016, 32, 169–178. [Google Scholar] [CrossRef]
- Zhang, P.; Lu, J.; Jing, Y.; Tang, S.; Zhu, D.; Bi, Y. Global epidemiology of diabetic foot ulceration: A systematic review and meta-analysis. Ann. Med. 2017, 49, 106–116. [Google Scholar] [CrossRef]
- Brennan, M.B.; Hess, T.M.; Bartle, B.; Cooper, J.M.; Kang, J.; Huang, E.S.; Smith, M.; Sohn, M.W.; Crnich, C. Diabetic foot ulcer severity predicts mortality among veterans with type 2 diabetes. J. Diabetes Complicat. 2017, 31, 556–561. [Google Scholar] [CrossRef]
- Capriotti, G.; Chianelli, M.; Signore, A. Nuclear medicine imaging of diabetic foot infection: Results of meta-analysis. Nucl. Med. Commun. 2006, 27, 757–764. [Google Scholar] [CrossRef]
- Prompers, L.; Huijberts, M.; Apelqvist, J.; Jude, E.; Piaggesi, A.; Bakker, K.; Edmonds, M.; Holstein, P.; Jirkovska, A.; Mauricio, D.; et al. High prevalence of ischaemia, infection and serious comorbidity in patients with diabetic foot disease in Europe. Baseline results from the Eurodiale study. Diabetologia 2007, 50, 18–25. [Google Scholar] [CrossRef]
- Lipsky, B.A. Osteomyelitis of the foot in diabetic patients. Clin. Infect. Dis. 1997, 25, 1318–1326. [Google Scholar] [CrossRef]
- Lavery, L.A.; Armstrong, D.G.; Wunderlich, R.P.; Mohler, M.J.; Wendel, C.S.; Lipsky, B.A. Risk factors for foot infections in individuals with diabetes. Diabetes Care 2006, 29, 1288–1293. [Google Scholar] [CrossRef]
- Gierbolini, R. Charcot’s foot: Often overlooked complication of diabetes. J. Am. Acad. Phys. Assist. 1994, 12, 62–68. [Google Scholar]
- Dinh, M.T.; Abad, C.L.; Safdar, N. Diagnostic accuracy of the physical examination and imaging tests for osteomyelitis underlying diabetic foot ulcers: Meta-analysis. Clin. Infect. Dis. 2008, 47, 519–527. [Google Scholar] [CrossRef]
- Grayson, M.L.; Gibbons, G.W.; Balogh, K.; Levin, E.; Karchmer, A.W. Probing to bone in infected pedal ulcers: A clinical sign of underlying osteomyelitis in diabetic patients. JAMA 1995, 273, 721–723. [Google Scholar] [CrossRef]
- Glaudemans, A.W.J.M.; Jutte, P.C.; Cataldo, M.A.; Cassar-Pullicino, V.; Gheysens, O.; Borens, O.; Trampuz, A.; Wörtler, K.; Petrosillo, N.; Winkler, H.; et al. Consensus document for the diagnosis of peripheral bone infection in adults: A joint paper by the EANM, EBJIS, and ESR (with ESCMID endorsement). Eur. J. Nucl. Med. Mol. Imaging 2019, 46, 957–970. [Google Scholar] [CrossRef]
- Familiari, D.; Glaudemans, A.W.; Vitale, V.; Prosperi, D.; Bagni, O.; Lenza, A.; Cavallini, M.; Scopinaro, F.; Signore, A. Can sequential 18F-FDG PET/CT replace WBC imaging in the diabetic foot? J. Nucl. Med. 2011, 52, 1012–1019. [Google Scholar] [CrossRef]
- Glaudemans, A.W.; Uçkay, I.; Lipsky, B.A. Challenges in diagnosing infection in the diabetic foot. Diabet Med. 2015, 32, 748–759. [Google Scholar] [CrossRef]
- Tan, P.L.; The, J. MRI of the diabetic foot: Differentiation of infection from neuropathic change. Br. J. Radiol. 2007, 80, 939–948. [Google Scholar] [CrossRef]
- De Vries, E.F.; Roca, M.; Jamar, F.; Israel, O.; Signore, A. Guidelines for the labelling of leucocytes with 99mTc-HMPAO. Inflammation/Infection Taskgroup of the European Association of Nuclear Medicine. Eur J. Nucl. Med. Mol. Imaging 2010, 37, 842–848. [Google Scholar] [CrossRef]
- Roca, M.; de Vries, E.F.; Jamar, F.; Israel, O.; Signore, A. Guidelines for the labelling of leucocytes with 111In-oxine. Inflammation/Infection Taskgroup of the European Association of Nuclear Medicine. Eur. J. Nucl. Med. Mol. Imaging 2010, 37, 835–841. [Google Scholar] [CrossRef]
- Signore, A.; Jamar, F.; Israel, O.; Buscombe, J.; Martin-Comin, J.; Lazzeri, E. Clinical indications, image acquisition and data interpretation for white blood cells and anti-granulocyte monoclonal antibody scintigraphy: An EANM procedural guideline. Eur. J. Nucl. Med. Mol. Imaging 2018, 45, 1816–1831. [Google Scholar] [CrossRef]
- Jamar, F.; Buscombe, J.; Chiti, A.; Christian, P.E.; Delbeke, D.; Donohoe, K.J.; Israel, O.; Martin-Comin, J.; Signore, A. EANM/SNMMI guideline for 18F-FDG use in inflammation and infection. J. Nucl. Med. 2013, 54, 647–658. [Google Scholar] [CrossRef] [PubMed]
- Signore, A.; Sconfienza, L.M.; Borens, O.; Glaudemans, A.W.J.M.; Cassar-Pullicino, V.; Trampuz, A.; Winkler, H.; Gheysens, O.; Vanhoenacker, F.M.H.M.; Petrosillo, N.; et al. Consensus document for the diagnosis of prosthetic joint infections: A joint paper by the EANM, EBJIS, and ESR (with ESCMID endorsement). Eur. J. Nucl. Med. Mol. Imaging 2019, 46, 971–988. [Google Scholar] [CrossRef] [PubMed]
- Lauri, C.; Tamminga, M.; Glaudemans, A.W.J.M.; Juárez Orozco, L.E.; Erba, P.A.; Jutte, P.C.; Lipsky, B.A.; IJzerman, M.J.; Signore, A.; Slart, R.H.J.A. Detection of Osteomyelitis in the Diabetic Foot by Imaging Techniques: A Systematic Review and Meta-analysis Comparing MRI, White Blood Cell Scintigraphy, and FDG-PET. Diabetes Care 2017, 40, 1111–1120. [Google Scholar] [CrossRef] [PubMed]
- Donovan, A.; Schweitzer, M.E. Use of MR imaging in diagnosing diabetes-related pedal osteomyelitis. Radiographics 2010, 30, 723–736. [Google Scholar] [CrossRef]
- Ledermann, H.P.; Morrison, W.B.; Schweitzer, M.E. MR image analysis of pedal osteomyelitis: Distribution, patterns of spread, and frequency of associated ulceration and septic arthritis. Radiology 2002, 223, 747–755. [Google Scholar] [CrossRef]
- Ahmadi, M.E.; Morrison, W.B.; Carrino, J.A.; Schweitzer, M.E.; Raikin, S.M.; Ledermann, H.P. Neuropathic arthropathy of the foot with and without superimposed osteomyelitis: MR imaging characteristics. Radiology 2006, 238, 622–631. [Google Scholar] [CrossRef]
- Glaudemans, A.W.; de Vries, E.F.; Vermeulen, L.E.; Slart, R.H.; Dierckx, R.A.; Signore, A. A large retrospective single-centre study to define the best image acquisition protocols and interpretation criteria for white blood cell scintigraphy with (99)mTc-HMPAO-labelled leucocytes in musculoskeletal infections. Eur. J. Nucl. Med. Mol. Imaging 2013, 40, 1760–1769. [Google Scholar] [CrossRef]
- Erba, P.A.; Glaudemans, A.W.; Veltman, N.C.; Sollini, M.; Pacilio, M.; Galli, F.; Dierckx, R.A.; Signore, A. Image acquisition and interpretation criteria for 99mTc-HMPAO-labelled white blood cell scintigraphy: Results of a multicenter study. Eur. J. Nucl Med. Mol. Imaging 2014, 41, 615–623. [Google Scholar] [CrossRef]
- Lauri, C.; Glaudemans, A.W.J.M.; Signore, A. Leukocyte Imaging of the Diabetic Foot. Curr. Pharm. Des. 2018, 24, 1270–1276. [Google Scholar] [CrossRef]
- Keidar, Z.; Militianu, D.; Melamed, E.; Bar-Shalom, R.; Israel, O. The diabetic foot: Initial experience with 18F-FDG PET/CT. J. Nucl. Med. 2005, 46, 444–449. [Google Scholar]
- Basu, S.; Chryssikos, T.; Houseni, M.; Scot Malay, D.; Shah, J.; Zhuang, H.; Alavi, A. Potential role of FDG PET in the setting of diabetic neuro-osteoarthropathy: Can it differentiate uncomplicated Charcot’s neuroarthropathy from osteomyelitis and soft-tissue infection? Nucl. Med. Commun. 2007, 28, 465–472. [Google Scholar] [CrossRef] [PubMed]
- Kagna, O.; Srour, S.; Melamed, E.; Militianu, D.; Keidar, Z. FDG PET/CT imaging in the diagnosis of osteomyelitis in the diabetic foot. Eur. J. Nucl. Med. Mol Imaging 2012, 39, 1545–1550. [Google Scholar] [CrossRef] [PubMed]
- Shagos, G.S.; Shanmugasundaram, P.; Varma, A.K.; Padma, S.; Sarma, M. 18-F flourodeoxy glucose positron emission tomography-computed tomography imaging: A viable alternative to three phase bone scan in evaluating diabetic foot complications? Indian J. Nucl. Med. 2015, 30, 97–103. [Google Scholar] [CrossRef] [PubMed]
- Nawaz, A.; Torigian, D.A.; Siegelman, E.S.; Basu, S.; Chryssikos, T.; Alavi, A. Diagnostic performance of FDG-PET, MRI, and plain film radiography (PFR) for the diagnosis of osteomyelitis in the diabetic foot. Mol. Imaging Biol. 2010, 12, 335–342. [Google Scholar] [CrossRef]
- Newman, L.G.; Waller, J.; Palestro, C.J.; Hermann, G.; Klein, M.J.; Schwartz, M.; Harrington, E.; Harrington, M.; Roman, S.H.; Stagnaro-Green, A. Leukocyte scanning with 111In is superior to magnetic resonance imaging in diagnosis of clinically unsuspected osteomyelitis in diabetic foot ulcers. Diabetes Care. 1992, 15, 1527–1530. [Google Scholar] [CrossRef]
- Craig, J.G.; Amin, M.B.; Wu, K.; Eyler, W.R.; van Holsbeeck, M.T.; Bouffard, J.A.; Shirazi, K. Osteomyelitis of the diabetic foot: MR imaging-pathologic correlation. Radiology 1997, 203, 849–855. [Google Scholar] [CrossRef]
- Erdman, W.A.; Tamburro, F.; Jayson, H.T.; Weatherall, P.T.; Ferry, K.B.; Peshock, R.M. Osteomyelitis: Characteristics and pitfalls of diagnosis with MR imaging. Radiology 1991, 180, 533–539. [Google Scholar] [CrossRef]
- Lipman, B.T.; Collier, B.D.; Carrera, G.F.; Timins, M.E.; Erickson, S.J.; Johnson, J.E.; Mitchell, J.R.; Hoffmann, R.G.; Finger, W.A.; Krasnow, A.Z.; et al. Detection of osteomyelitis in the neuropathic foot: Nuclear medicine, MRI and conventional radiography. Clin. Nucl. Med. 1998, 23, 77–82. [Google Scholar] [CrossRef]
- Fujii, M.; Armstrong, D.G.; Terashi, H. Efficacy of magnetic resonance imaging in diagnosing diabetic foot osteomyelitis in the presence of ischemia. J. Foot Ankle Surg. 2013, 52, 717–723. [Google Scholar] [CrossRef]
- Morrison, W.B.; Schweitzer, M.E.; Wapner, K.L.; Hecht, P.J.; Gannon, F.H.; Behm, W.R. Osteomyelitis in feet of diabetics: Clinical accuracy, surgical utility, and cost-effectiveness of MR imaging. Radiology 1995, 196, 557–564. [Google Scholar] [CrossRef]
- Ledermann, H.P.; Schweitzer, M.E.; Morrison, W.B. Non-enhancing tissue on MR imaging of pedal infection: Characterization of necrotic tissue and associated limitations for diagnosis of osteomyelitis and abscess. Am. J. Roentgenol. 2002, 178, 215–222. [Google Scholar] [CrossRef] [PubMed]
- Leone, A.; Cassar-Pullicino, V.N.; Semprini, A.; Tonetti, L.; Magarelli, N.; Colosimo, C. Neuropathic osteoarthropathy with and without superimposed osteomyelitis in patients with a diabetic foot. Skeletal Radiol. 2016, 45, 735–754. [Google Scholar] [CrossRef] [PubMed]
- Glaudemans, A.W.; Prandini, N.; Di Girolamo, M.; Argento, G.; Lauri, C.; Lazzeri, E.; Muto, M.; Sconfienza, L.M.; Signore, A. Hybrid imaging of musculoskeletal infections. Q. J. Nucl. Med. Mol. Imaging 2018, 62, 3–13. [Google Scholar] [CrossRef] [PubMed]
- Catalano, O.; Maccioni, F.; Lauri, C.; Auletta, S.; Dierckx, R.; Signore, A. Hybrid imaging in Crohn’s disease: From SPECT/CT to PET/MR and new image interpretation criteria. Q. J. Nucl. Med. Mol. Imaging 2018, 62, 40–55. [Google Scholar] [CrossRef]
- Heiba, S.; Knešaurek, K. Evaluation of diabetic foot infection in nuclear medicine. Q. J. Nucl. Med. Mol. Imaging 2017, 61, 283–291. [Google Scholar] [CrossRef]
| Age (Years) (Mean ± SD) | Gender (F/M) (%) | DM1/DM2 (%) | Glycaemia (mmol/L) (Mean ± SD) | Hb1Ac (%) (Mean ± SD) | ESR (mm/h) (Mean ± SD) | CRP (mg/L) (Mean ± SD) | |
|---|---|---|---|---|---|---|---|
| All patients (251) | 60.7 ± 10.8 | 34.3/65.7 | 17.1/82.9 | 9.1 ± 3.4 | 8.0 ± 1.9 | 47.3 ± 28.5 | 43.0 ± 73.1 |
| WBC * (88) | 64.2 ± 10.9 | 44.3/55.7 | 15.9/84.1 | 8.5 ± 2.8 | 7.7 ± 1.6 | 45.6 ± 28.0 | 14.3 ± 32.8 |
| WBC ** (58) | 57.2 ± 10.3 | 32.7/67.3 | 15.5/84.5 | 9.7 ± 4.2 | 9.2 ± 2.6 | 56.6 ± 35.9 | 73.4 ± 58.6 |
| MRI (76) | 59.2 ± 10.6 | 25.0/75.0 | 22.4/77.6 | 10.5 ± 4.0 | 8.2 ± 2. 2 | 48.2 ± 27.5 | 87.4 ± 100 |
| FDG (58) | 58.0 ± 9.0 | 29.3/70.7 | 10.3/89.7 | 7.8 ± 2.6 | 8.3 ± 1.9 | n.r. | n.r. |
| OM (93) | 59.6 ± 11.1 | 26.9/73.1 | 20.4/79.6 | 9.5 ± 3.3 | 8.4 ± 1.9 | 55.9 ± 32.1 | 68.3 ± 93.7 |
| STI (76) | 62.3 ± 10.01 | 38.1/61.9 | 19.7/80.3 | 9.0 ± 3.6 | 7.8 ± 1.7 | 46.7 ± 26.9 | 27.9 ± 53.4 |
| Charcot (10) | 56.5 ± 10.1 | 20.0/80.0 | 20.0/80.0 | n.r. | 7.4 ± 1.7 | n.r. | 42.8 ± 71.5 |
| No pathology (72) | 60.7 ± 10.9 | 43.0/57.0 | 9.7/90.3 | 8.5 ± 3.2 | 7.7 ± 1.9 | 37.6 ± 23.1 | 27.7 ± 53.7 |
| Cultures from Aspirates (in 67 Patients) | Cultures from Bone Biopsies (in 14 Patients) |
|---|---|
| Negative: 13.4% | Negative: 28.6% Polymicrobial: 28.6% Staph. aureus: 28.6% Pseud. aeruginosa: 14.2% |
| Staph. aureus: 26.9% | |
| Polymicrobial: 23.8% | |
| Strept. epidermidis: 10.4% | |
| P. aeruginosa: 7.5% | |
| Acinetobacter: 4.5% | |
| Staph. haemolyticus: 4.5% | |
| E. faecalis: 3.0% | |
| Proteus mirabilis: 1.5% | |
| E. coli: 1.5% | |
| Strept. agalactiae: 1.5% | |
| Citrobacter freundii: 1.5% |
| Sensitivity (%) (95% CI) | Specificity (%) (95% CI) | Accuracy (%) (95% CI) | |
|---|---|---|---|
| OM (WBC *) | 59.1 (38.5–79.6) | 77.3 (67.2–87.4) | 72.7 (63.4–82.0) |
| STI (WBC *) | 29.7 (15.0–44.5) | 86.3 (76.8–95.7) | 62.5 (52.4–72.6) |
| Charcot (WBC *) | n.c. | 92.0 (86.4–97.7) | n.c. |
| OM (WBC-EANM **) | 76.2 (58.0–94.4) | 91.9 (83.1–100) | 86.2 (77.3–95.1) |
| STI (WBC-EANM **) | 75.0 (50.5–99.5) | 95.7 (88.9–100) | 91.4 (84.2–98.6) |
| Charcot (WBC-EANM **) | n.c. | 89.3 (81.2–97.4) | 87.9 (79.5–96.3) |
| OM (FDG PET/CT) | 69.0 (52.1–85.8) | 72.4 (56.1–88.7) | 70.7 (59.0–82.4) |
| STI (FDG PET/CT) | 27.3 (1.0–54.0) | 97.9 (93.7–100) | 84.5 (75.2–93.8) |
| Charcot (FDG PET/CT) | n.c. | 62.5 (49.8–75.2) | 62.1 (49.6–74.6) |
| OM (MRI) | 62.9 (46.8–78.9) | 70.7 (56.8–84.7) | 67.1 (56.5–77.7) |
| STI (MRI) | 42.9 (21.7–64.0) | 83.6 (73.9–93.4) | 72.4(62.3–82.4) |
| Charcot (MRI) | n.c. | 88.2 (80.6–95.9) | 80.3 (71.3–89.2) |
| Final Diagnosis | Intensity | SUVmax (Mean ± SD 1) | SUVmax Ratio (Mean ± SD 1) | |
|---|---|---|---|---|
| Focal Uptake (%) | Diffuse Uptake (%) | |||
| OM | 62.1 | 37.9 | 5.3 ± 2.1 | 3.9 ± 2.4 |
| STI | 54.5 | 45.5 | 5.4 ± 1.8 | 4.2 ± 2.1 |
| Charcot | 0 | 100 | 4.9 ± 1.9 | 4.9 ± 1.6 |
| Sensitivity (%) (95% CI) | Specificity (%) (95% CI) | Accuracy (%) (95% CI) | ||||
|---|---|---|---|---|---|---|
| Forefoot | Mid-Hindfoot | Forefoot | Mid-Hindfoot | Forefoot | Mid-Hindfoot | |
| OM (WBC-EANM **) | 78.6 (57.1–100) | 71.4 (38.0–100) | 88.9 (68.4–100) | 85.7 (59.8–100) | 82.6 (67.1–98.1) | 78.6 (57.1–100) |
| STI (WBC-EANM **) | 85.7 (59.8–100) | 60.0 (17.1–100) | 87.5 (71.3–100) | 100 (100–100) | 87.0 (73.2–100) | 85.7 (67.4–100) |
| OM (FDG PET/CT) | 91.7 (76.0–100) | 52.9 (29.2–76.7) | 60.0 (17.1–100) | 72.7 (46.4–99.0) | 82.4 (64.2–100) | 60.7 (42.6–78.8) |
| STI (FDG PET/CT) | 50.0 (1.0–99.0) | 14.3 (0.0–40.2) | 100 (100–100) | 100 (100–100) | 88.2 (75.9–100) | 78.6 (63.4–93.8) |
| OM (MRI) | 72.0 (54.0–89.6) | 40.0 (9.6–70.4) | 61.9 (41.1–82.7) | 76.9 (54.0–99.8) | 67.4 (53.8–80.9) | 60.9 (40.9–80.8) |
| STI (MRI) | 42.9 (16.9–68.8) | 42.9 (6.2–79.5) | 93.8 (85.4–100) | 75.0 (53.8–96.2) | 78.3 (66.3–90.2) | 65.2 (45.7–84.7) |
| Therapeutic Strategy in OM | Diagnosis according to Imaging Modalities (%) | |||
|---|---|---|---|---|
| Conventional wound care and topic antibiotic treatment 2.8% | WBC | |||
| Negative 0% | OM 100% | STI 0% | Charcot 0% | |
| FDG (no patients) | ||||
| MRI | ||||
| Negative 0% | OM 0% | STI 0% | Charcot 100% | |
| Systemic antibiotic treatment 32.8% | WBC | |||
| Negative 0% | OM 83% | STI 0% | Charcot 17% | |
| FDG | ||||
| Negative 0% | OM 50% | STI 0% | Charcot 50% | |
| MRI | ||||
| Negative 9% | OM 73% | STI 9% | Charcot 9% | |
| Surgery (debridement or amputation) 64.4% | WBC | |||
| Negative 3% | OM 77% | STI 10% | Charcot 10% | |
| FDG | ||||
| Negative 0% | OM 83% | STI 0% | Charcot 17% | |
| MRI | ||||
| Negative 20% | OM 65% | STI 5% | Charcot 10% | |
| Therapeutic Strategy in STI | Diagnosis according to Imaging Modalities (%) | |||
|---|---|---|---|---|
| No treatment 1.7% | WBC | |||
| Negative 0% | OM 100% | STI 0% | Charcot 0% | |
| FDG (no patients) | ||||
| MRI (no patients) | ||||
| Conventional wound care and topic antibiotic treatment 15% | WBC | |||
| Negative 78% | OM 0% | STI 22% | Charcot 0% | |
| FDG (no patients) | ||||
| MRI (no patients) | ||||
| Systemic antibiotic treatment 68.3% | WBC | |||
| Negative 19% | OM 23% | STI 39% | Charcot 19% | |
| FDG (no patients) | ||||
| MRI | ||||
| Negative 15% | OM 15% | STI 47% | Charcot 23% | |
| Surgery (debridement or amputation) 15% | WBC | |||
| Negative 14% | OM 0% | STI 72% | Charcot 14% | |
| FDG (no patients) | ||||
| MRI | ||||
| Negative 0% | OM 33% | STI 66% | Charcot 0% | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lauri, C.; Glaudemans, A.W.J.M.; Campagna, G.; Keidar, Z.; Muchnik Kurash, M.; Georga, S.; Arsos, G.; Noriega-Álvarez, E.; Argento, G.; Kwee, T.C.; et al. Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study. J. Clin. Med. 2020, 9, 1645. https://doi.org/10.3390/jcm9061645
Lauri C, Glaudemans AWJM, Campagna G, Keidar Z, Muchnik Kurash M, Georga S, Arsos G, Noriega-Álvarez E, Argento G, Kwee TC, et al. Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study. Journal of Clinical Medicine. 2020; 9(6):1645. https://doi.org/10.3390/jcm9061645
Chicago/Turabian StyleLauri, Chiara, Andor W.J.M. Glaudemans, Giuseppe Campagna, Zohar Keidar, Marina Muchnik Kurash, Stamata Georga, Georgios Arsos, Edel Noriega-Álvarez, Giuseppe Argento, Thomas C. Kwee, and et al. 2020. "Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study" Journal of Clinical Medicine 9, no. 6: 1645. https://doi.org/10.3390/jcm9061645
APA StyleLauri, C., Glaudemans, A. W. J. M., Campagna, G., Keidar, Z., Muchnik Kurash, M., Georga, S., Arsos, G., Noriega-Álvarez, E., Argento, G., Kwee, T. C., Slart, R. H. J. A., & Signore, A. (2020). Comparison of White Blood Cell Scintigraphy, FDG PET/CT and MRI in Suspected Diabetic Foot Infection: Results of a Large Retrospective Multicenter Study. Journal of Clinical Medicine, 9(6), 1645. https://doi.org/10.3390/jcm9061645










