New First Line Treatment Options of Clear Cell Renal Cell Cancer Patients with PD-1 or PD-L1 Immune-Checkpoint Inhibitor-Based Combination Therapies
Abstract
1. Introduction
- Significant improvement of overall survival (26 vs. 19.7 months; hazard ratio (HR) 0.73; p = 0.0006)
- Significantly higher objective response rate (26% vs. 5%)
- Better toxicity profile and
- Improved quality of life
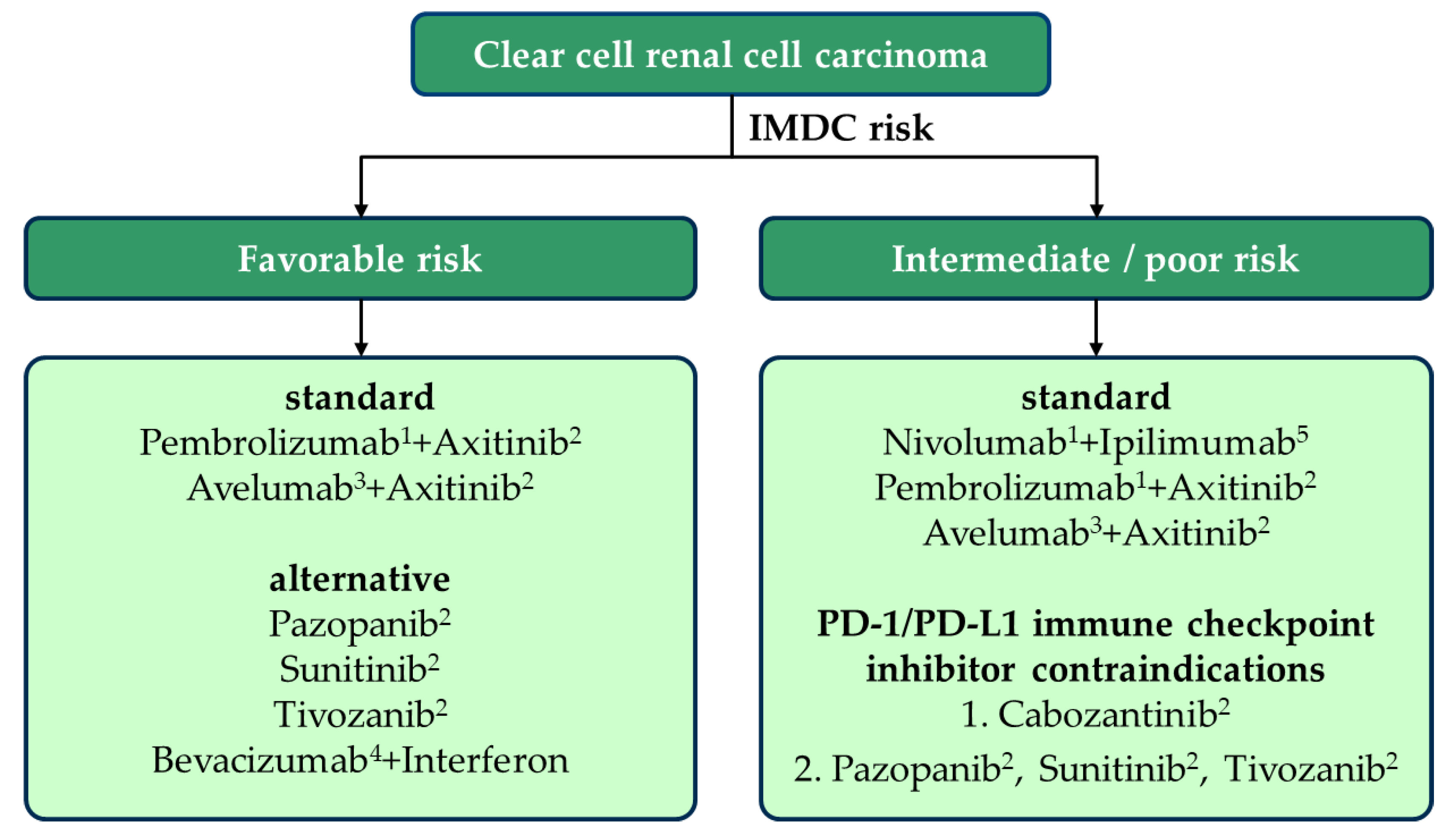
2. Risk Stratification of Metastatic Renal Cell Carcinoma
- Karnofsky performance status <80%
- Time between first diagnosis and start of a systemic therapy <1 year
- Low serum hemoglobin
- High corrected serum calcium (corrected serum calcium [mg/dL] = total calcium [mg/dL] + 0.8 (4.0—serum albumin [g/dL]))
- Neutrophilia
- Thrombophilia
3. Nivolumab Plus Ipilimumab (CheckMate 214)
4. Pembrolizumab Plus Axitinib (Keynote 426)
5. Avelumab Plus Axitinib (JAVELIN 101)
6. Side Effects and Quality of Life
- Grade 1 therapy can be continued,
- Grade 2: Interrupt therapy, start corticosteroid therapy,
- Grade 4: Permanently discontinue therapy, start corticosteroid therapy.
7. Second Line Therapy
8. Non-Clear Cell Renal Cell Carcinoma
9. Conclusions for Clinical Practice
- PD-1/PD-L1 ICIs represent the new backbone of first-line therapy in RCC
- Nivolumab plus Ipilimumab represents a standard first-line therapy for intermediate and high IMDC risk
- Pembrolizumab plus Axitinib or Avelumab plus Axitinib represent standard first-line therapies, regardless of the risk profile
- For patients with a favorable risk profile, a monotherapy with a VEGFR-TKI may be considered as an alternative to the combination therapy
- Patients should be comprehensively advised regarding the advantages and disadvantages of the very different combinations (immune-immune vs. immune-VEGFR-TKI), taking into account the individual situation and therapy objectives.
- Patient information should, among others, include survival benefit, rate of remission, long-term remissions, side effects (chronic side effects of TKIs, risk of immune-mediated adverse events) and quality of life.
Author Contributions
Funding
Conflicts of Interest
References
- Motzer, R.J.; Escudier, B.; McDermott, D.F.; George, S.; Hammers, H.J.; Srinivas, S.; Tykodi, S.S.; Sosman, J.A.; Procopio, G.; Plimack, E.R.; et al. Nivolumab versus everolimus in advanced renal-cell carcinoma. N. Engl. J. Med. 2015, 373, 1803–1813. [Google Scholar] [CrossRef] [PubMed]
- Plimack, E.R.; Motzer, R.J.; Escudier, B. Two-year efficacy and safety update: Phase iii checkmate 025 study of nivolumab vs. everolimus in patients with advanced renal cell carcinoma (arcc). In Proceedings of the ESMO Conference, Copenhagen, Denmark, 7–11 October 2016. [Google Scholar]
- Escudier, B.; Motzer, R.J.; Sharma, P.; Wagstaff, J.; Plimack, E.R.; Hammers, H.J.; Donskov, F.; Gurney, H.; Sosman, J.A.; Zalewski, P.G.; et al. Treatment beyond progression in patients with advanced renal cell carcinoma treated with nivolumab in checkmate 025. Eur. Urol. 2017, 72, 368–376. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Penkov, K.; Haanen, J.; Rini, B.; Albiges, L.; Campbell, M.T.; Venugopal, B.; Kollmannsberger, C.; Negrier, S.; Uemura, M.; et al. Avelumab plus axitinib versus sunitinib for advanced renal-cell carcinoma. N. Engl. J. Med. 2019, 380, 1103–1115. [Google Scholar] [CrossRef] [PubMed]
- Motzer, R.J.; Tannir, N.M.; McDermott, D.F.; Aren Frontera, O.; Melichar, B.; Choueiri, T.K.; Plimack, E.R.; Barthelemy, P.; Porta, C.; George, S.; et al. Nivolumab plus ipilimumab versus sunitinib in advanced renal-cell carcinoma. N. Engl. J. Med. 2018, 378, 1277–1290. [Google Scholar] [CrossRef] [PubMed]
- Rini, B.I.; Plimack, E.R.; Stus, V.; Gafanov, R.; Hawkins, R.; Nosov, D.; Pouliot, F.; Alekseev, B.; Soulieres, D.; Melichar, B.; et al. Pembrolizumab plus axitinib versus sunitinib for advanced renal-cell carcinoma. N. Engl. J. Med. 2019, 380, 1116–1127. [Google Scholar] [CrossRef]
- Albiges, L.; Powles, T.; Staehler, M.; Bensalah, K.; Giles, R.H.; Hora, M.; Kuczyk, M.A.; Lam, T.B.; Ljungberg, B.; Marconi, L.; et al. Updated european association of urology guidelines on renal cell carcinoma: Immune checkpoint inhibition is the new backbone in first-line treatment of metastatic clear-cell renal cell carcinoma. Eur. Urol. 2019, 76, 151–156. [Google Scholar] [CrossRef]
- Motzer, R.J.; Bacik, J.; Murphy, B.A.; Russo, P.; Mazumdar, M. Interferon-alfa as a comparative treatment for clinical trials of new therapies against advanced renal cell carcinoma. J. Clin. Oncol. 2002, 20, 289–296. [Google Scholar] [CrossRef]
- Motzer, R.J.; Mazumdar, M.; Bacik, J.; Berg, W.; Amsterdam, A.; Ferrara, J. Survival and prognostic stratification of 670 patients with advanced renal cell carcinoma. J. Clin. Oncol. 1999, 17, 2530–2540. [Google Scholar] [CrossRef]
- Heng, D.Y.; Xie, W.; Regan, M.M.; Warren, M.A.; Golshayan, A.R.; Sahi, C.; Eigl, B.J.; Ruether, J.D.; Cheng, T.; North, S.; et al. Prognostic factors for overall survival in patients with metastatic renal cell carcinoma treated with vascular endothelial growth factor-targeted agents: Results from a large, multicenter study. J. Clin. Oncol. 2009, 27, 5794–5799. [Google Scholar] [CrossRef]
- Motzer, R.J.; Rini, B.I.; McDermott, D.F.; Aren Frontera, O.; Hammers, H.J.; Carducci, M.A.; Salman, P.; Escudier, B.; Beuselinck, B.; Amin, A.; et al. Nivolumab plus ipilimumab versus sunitinib in first-line treatment for advanced renal cell carcinoma: Extended follow-up of efficacy and safety results from a randomised, controlled, phase 3 trial. Lancet Oncol. 2019, 20, 1370–1385. [Google Scholar] [CrossRef]
- Rini, B.I.; Plimack, E.R.; Stus, V.; Gafanov, R.; Hawkins, R.; Nosov, D.; Pouliot, F.; Soulieres, D.; Melichar, B.; Vynnychenko, I.; et al. Pembrolizumab plus axitinib versus sunitinib as first-line therapy for metastatic renal cell carcinoma: Outcomes by imdc risk and sarcomatoid subgroups of the phase 3 keynote-426 study. In Proceedings of the International Kidney Cancer Symposium (IKCS), Miami, FL, USA, 15–16 November 2019. [Google Scholar]
- Committee for Medicinal Products for Human Use (CHMP). Assessment Report Bavencio; Procedure No. Emea/h/c/004338/ii/0009/g. EMA/CHMP/550625/2019; European Medicines Agency: London, UK, 2019; Available online: https://www.ema.europa.eu/en/documents/variation-report/bavencio-h-c-004338-ii-0009-g-epar-assessment-report-variation_en.pdf (accessed on 15 January 2020).
- Committee for Medicinal Products for Human Use (CHMP). Assessment Report Keytruda; Procedure No. Emea/h/c/003820/ii/0069. EMA/CHMP/455620/2019; European Medicines Agency: London, UK, 2019; Available online: https://www.ema.europa.eu/en/documents/variation-report/keytruda-h-c-3820-ii-0069-epar-assessment-report-variation_en.pdf (accessed on 15 January 2020).
- Larkin, J.; Fishman, M.; Wood, L.; Negrier, S.; Olivier, K.; Pyle, L.; Gorbunova, V.; Jonasch, E.; Andrews, L.; Staehler, M. Axitinib for the treatment of metastatic renal cell carcinoma: Recommendations for therapy management to optimize outcomes. Am. J. Clin. Oncol. 2014, 37, 397–403. [Google Scholar] [CrossRef]
- Rini, B.I.; Escudier, B.; Tomczak, P.; Kaprin, A.; Szczylik, C.; Hutson, T.E.; Michaelson, M.D.; Gorbunova, V.A.; Gore, M.E.; Rusakov, I.G.; et al. Comparative effectiveness of axitinib versus sorafenib in advanced renal cell carcinoma (axis): A randomised phase 3 trial. Lancet 2011, 378, 1931–1939. [Google Scholar] [CrossRef]
- Grimm, M.O.; Bex, A.; De Santis, M.; Ljungberg, B.; Catto, J.W.F.; Roupret, M.; Hussain, S.A.; Bellmunt, J.; Powles, T.; Wirth, M.; et al. Safe use of immune checkpoint inhibitors in the multidisciplinary management of urological cancer: The european association of urology position in 2019. Eur. Urol. 2019, 76, 368–380. [Google Scholar] [CrossRef]
- Grimm, M.O.; Tannir, N.M.; Motzer, R.J.; Plimack, E.R.; McDermott, D.F.; Barthélémy, P.; Porta, C.; George, S.; Powles, T.; Donskov, F.; et al. Checkmate 214 patients who discontinued first-line nivolumab + ipilimumab or sunitinib due to treatment-related adverse events. Urol. A Suppl. 2019, 58, 43. [Google Scholar]
- Cella, D.; Grunwald, V.; Escudier, B.; Hammers, H.J.; George, S.; Nathan, P.; Grimm, M.O.; Rini, B.I.; Doan, J.; Ivanescu, C.; et al. Patient-reported outcomes of patients with advanced renal cell carcinoma treated with nivolumab plus ipilimumab versus sunitinib (checkmate 214): A randomised, phase 3 trial. Lancet Oncol. 2019, 20, 297–310. [Google Scholar] [CrossRef]
- Oppel-Heuchel, H.; Grimm, M.O. Therapy monitoring and management of adverse events in pd-1/pd-l1 immune checkpoint inhibition. Urol. A 2016, 55, 677–690. [Google Scholar] [CrossRef]
- Foller, S.; Oppel-Heuchel, H.; Fetter, I.; Winkler, Y.; Grimm, M.O. Adverse events of immune checkpoint inhibitors. Urol. A 2017, 56, 486–491. [Google Scholar] [CrossRef]
- Auvray, M.; Auclin, E.; Barthelemy, P.; Bono, P.; Kellokumpu-Lehtinen, P.; Gross-Goupil, M.; De Velasco, G.; Powles, T.; Mouillet, G.; Vano, Y.A.; et al. Second-line targeted therapies after nivolumab-ipilimumab failure in metastatic renal cell carcinoma. Eur. J. Cancer 2019, 108, 33–40. [Google Scholar] [CrossRef]
- Escudier, B.; Porta, C.; Schmidinger, M.; Rioux-Leclercq, N.; Bex, A.; Khoo, V.; Grunwald, V.; Gillessen, S.; Horwich, A.; Committee, E.G. Renal cell carcinoma: Esmo clinical practice guidelines for diagnosis, treatment and follow-updagger. Ann. Oncol. 2019, 30, 706–720. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Halabi, S.; Sanford, B.L.; Hahn, O.; Michaelson, M.D.; Walsh, M.K.; Feldman, D.R.; Olencki, T.; Picus, J.; Small, E.J.; et al. Cabozantinib versus sunitinib as initial targeted therapy for patients with metastatic renal cell carcinoma of poor or intermediate risk: The alliance a031203 cabosun trial. J. Clin. Oncol. 2017, 35, 591–597. [Google Scholar] [CrossRef]
- Choueiri, T.K.; Hessel, C.; Halabi, S.; Sanford, B.; Michaelson, M.D.; Hahn, O.; Walsh, M.; Olencki, T.; Picus, J.; Small, E.J.; et al. Cabozantinib versus sunitinib as initial therapy for metastatic renal cell carcinoma of intermediate or poor risk (alliance a031203 cabosun randomised trial): Progression-free survival by independent review and overall survival update. Eur. J. Cancer 2018, 94, 115–125. [Google Scholar] [CrossRef]
- Powles, T.; Motzer, R.J.; Escudier, B.; Pal, S.; Kollmannsberger, C.; Pikiel, J.; Gurney, H.; Rha, S.Y.; Park, S.H.; Geertsen, P.F.; et al. Outcomes based on prior therapy in the phase 3 meteor trial of cabozantinib versus everolimus in advanced renal cell carcinoma. Br. J. Cancer 2018, 119, 663–669. [Google Scholar] [CrossRef]
- Motzer, R.J.; Nosov, D.; Eisen, T.; Bondarenko, I.; Lesovoy, V.; Lipatov, O.; Tomczak, P.; Lyulko, O.; Alyasova, A.; Harza, M.; et al. Tivozanib versus sorafenib as initial targeted therapy for patients with metastatic renal cell carcinoma: Results from a phase iii trial. J. Clin. Oncol. 2013, 31, 3791–3799. [Google Scholar] [CrossRef]
- Rini, B.I.; Pal, S.K.; Escudier, B.J.; Atkins, M.B.; Hutson, T.E.; Porta, C.; Verzoni, E.; Needle, M.N.; McDermott, D.F. Tivozanib versus sorafenib in patients with advanced renal cell carcinoma (tivo-3): A phase 3, multicentre, randomised, controlled, open-label study. Lancet Oncol. 2020, 21, 95–104. [Google Scholar] [CrossRef]
- Suarez, C.; Lee, J.; Ziobro, M.; Gafanov, R.A.; Matveev, V.B.; Donskov, F.; Pouliot, F.; Alekseev, B.Y.; Wiechno, P.J.; Tomczak, P.; et al. First-line pembrolizumab (pembro) monotherapy for advanced non‒clear cell renal cell carcinoma (nccrcc): Updated follow-up for keynote-427 cohort b. Ann. Oncol. 2019, 30, v356–v402. [Google Scholar] [CrossRef]
| Clinical Trial | Median Follow-Up | Number of Patients | IMDC Risk | ORR (%) | PFS (Months) | OS (Months) |
|---|---|---|---|---|---|---|
| CheckMate 214 [11] NCT02231749 | 32.4 months | 249 | favorable | 39 vs. 50 (p < 0.14) | 13.9 vs. 19.9 HR 1.23 (0.90–1.69); p = 0.19 | NA vs. NA HR 1.22 (0.73–2.04); p = 0.44 |
| CheckMate 214 [11] NCT02231749 | 32.4 months | 847 | Inter-mediate and poor | 42 vs. 29 (p < 0.0001) | 8.2 vs. 8.3 HR 0.77 (0.65–0.90); p = 0.0014 | NA vs. 26.6 HR 0.66 (0.54–0.80); p < 0.0001 |
| Keynote 426 [12] NCT02853331 | 16.6 months | 861 | ITT | 60.0 vs. 38.5 (p < 0.0001) | 17.1 vs. 11.1 HR 0.69 (0.57–0.83); p = 0.00005 | NA vs. NA HR 0.59 (0.45–0.78); p = 0.00010 |
| JAVELIN 101 [13] NCT02684006 | Interim analysis 2 | 886 | ITT | 52.5 vs. 27.3 | 13.3 vs. 8.0 HR 0.69 (0.574–0.825) | NA vs. NA HR 0.80 (0.616–1.027); n.s. |
| JAVELIN 101 [13] NCT02684006 | Interim analysis 2 | 560 | PD-L1 positive | 55.9 vs. 27.2 | 13.8 vs. 7.0 HR 0.62 (0.492–0.777) | NA vs. 28.6 HR 0.83 (0.596–1.151); n.s. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Grimm, M.-O.; Leucht, K.; Grünwald, V.; Foller, S. New First Line Treatment Options of Clear Cell Renal Cell Cancer Patients with PD-1 or PD-L1 Immune-Checkpoint Inhibitor-Based Combination Therapies. J. Clin. Med. 2020, 9, 565. https://doi.org/10.3390/jcm9020565
Grimm M-O, Leucht K, Grünwald V, Foller S. New First Line Treatment Options of Clear Cell Renal Cell Cancer Patients with PD-1 or PD-L1 Immune-Checkpoint Inhibitor-Based Combination Therapies. Journal of Clinical Medicine. 2020; 9(2):565. https://doi.org/10.3390/jcm9020565
Chicago/Turabian StyleGrimm, Marc-Oliver, Katharina Leucht, Viktor Grünwald, and Susan Foller. 2020. "New First Line Treatment Options of Clear Cell Renal Cell Cancer Patients with PD-1 or PD-L1 Immune-Checkpoint Inhibitor-Based Combination Therapies" Journal of Clinical Medicine 9, no. 2: 565. https://doi.org/10.3390/jcm9020565
APA StyleGrimm, M.-O., Leucht, K., Grünwald, V., & Foller, S. (2020). New First Line Treatment Options of Clear Cell Renal Cell Cancer Patients with PD-1 or PD-L1 Immune-Checkpoint Inhibitor-Based Combination Therapies. Journal of Clinical Medicine, 9(2), 565. https://doi.org/10.3390/jcm9020565






