Association between Circulation Indole-3-Acetic Acid Levels and Stem Cell Factor in Maintenance Hemodialysis Patients: A Cross-Sectional Study
Abstract
1. Introduction
2. Experimental Section
2.1. Subjects
2.2. Comorbidity and Biochemical Measurements
2.3. Mass Spectrometry for Indole-3-Acetic Acid Measurement
2.4. Proteomic Profiling
2.5. Statistical Analysis
2.6. Pathway Analysis
3. Results
3.1. Demographic and Clinical Characteristics
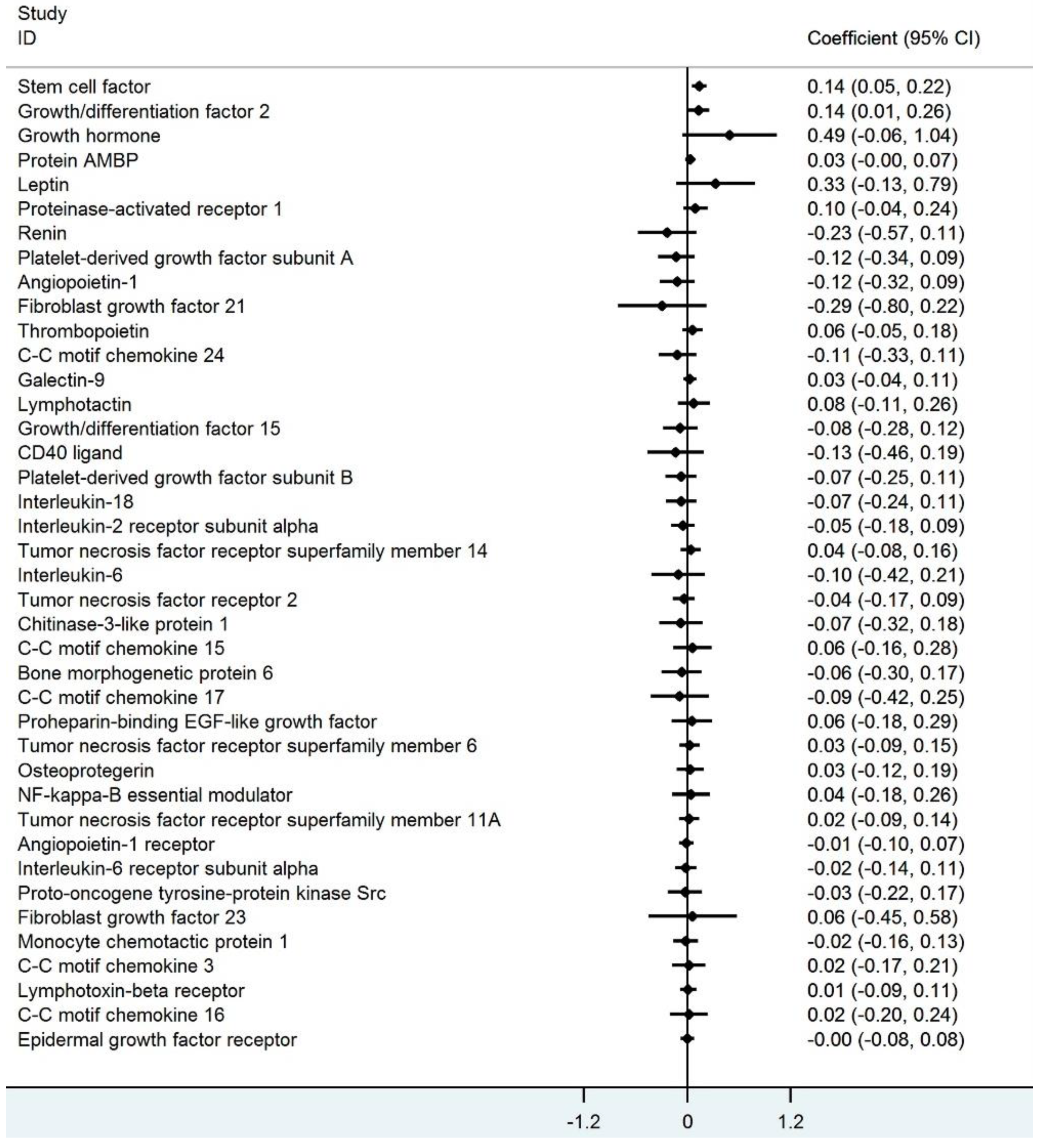
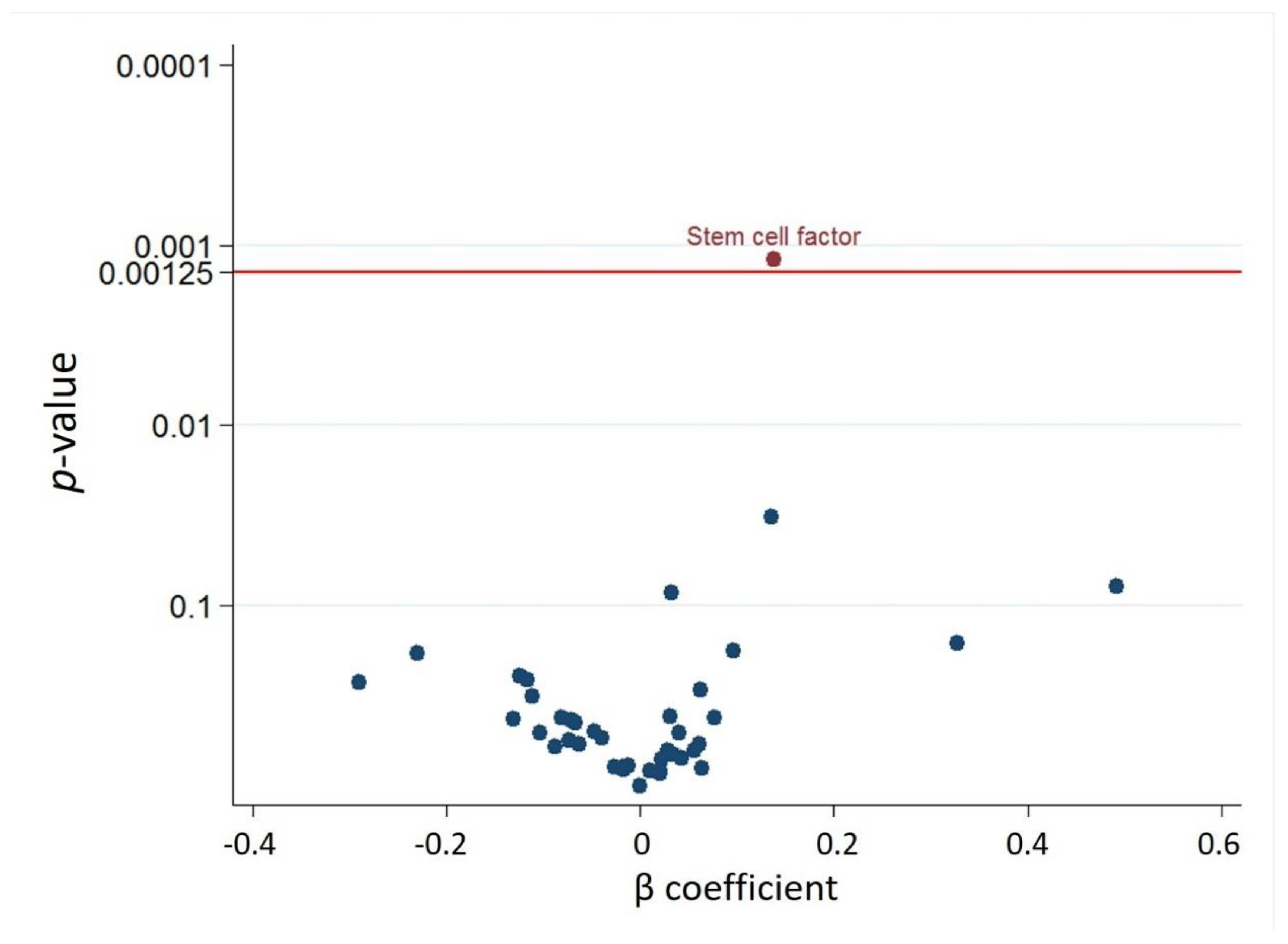
3.2. Discovery Phase
3.3. Best Estimates Phase
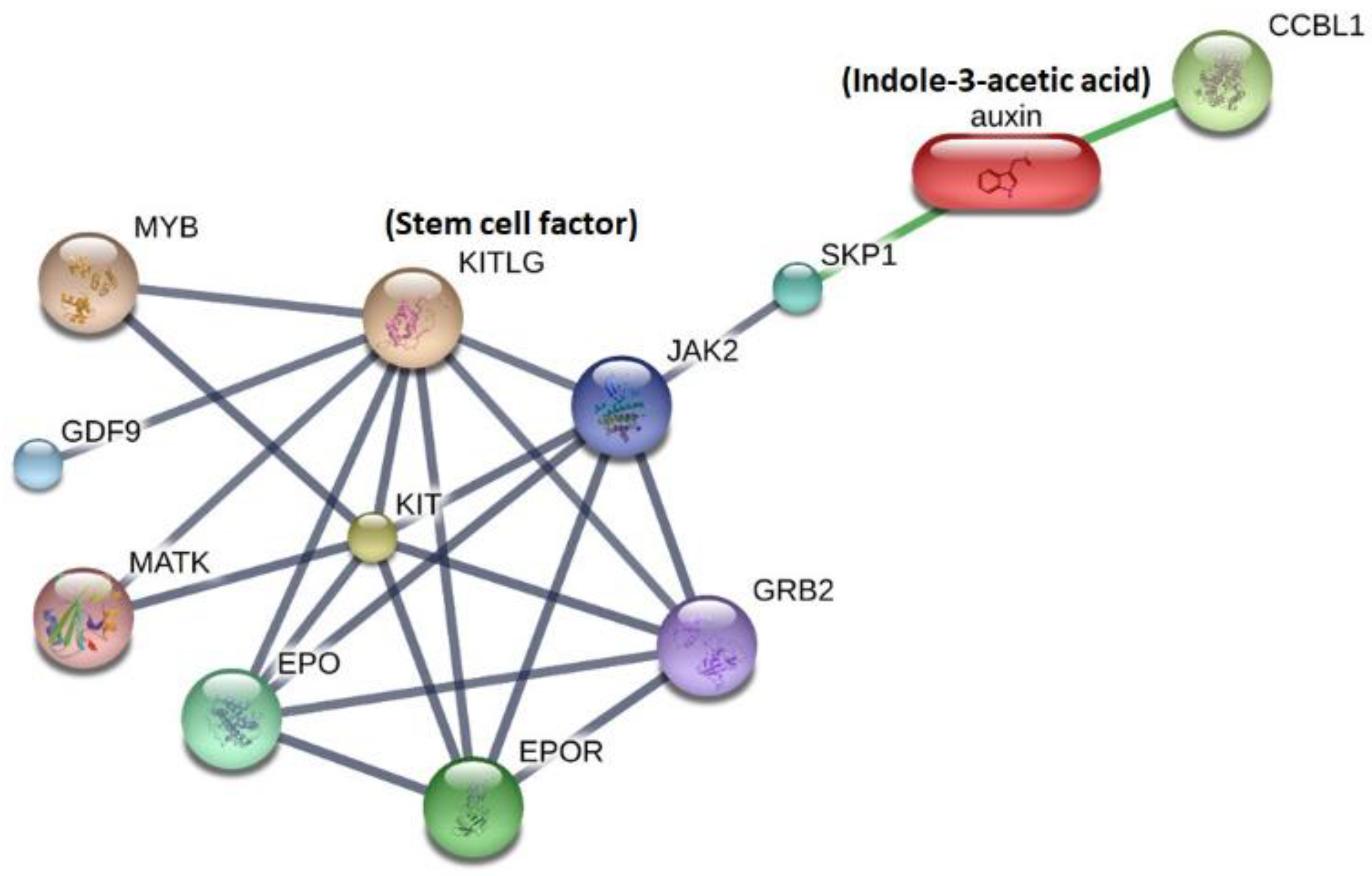
3.4. A Bioinformatics Approach to Link IAA with SCF
4. Discussion
4.1. Principal Observations
4.2. The Cardiovascular Damage of IAA
4.3. The Potential Mechanism to Link IAA and SCF
4.4. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Gansevoort, R.T.; Correa-Rotter, R.; Hemmelgarn, B.R.; Jafar, T.H.; Heerspink, H.J.; Mann, J.F.; Matsushita, K.; Wen, C.P. Chronic kidney disease and cardiovascular risk: Epidemiology, mechanisms, and prevention. Lancet 2013, 382, 339–352. [Google Scholar] [CrossRef]
- Go, A.S.; Chertow, G.M.; Fan, D.; McCulloch, C.E.; Hsu, C.Y. Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N. Engl. J. Med. 2004, 351, 1296–1305. [Google Scholar] [CrossRef] [PubMed]
- Chronic Kidney Disease Prognosis, C.; Matsushita, K.; van der Velde, M.; Astor, B.C.; Woodward, M.; Levey, A.S.; de Jong, P.E.; Coresh, J.; Gansevoort, R.T. Association of estimated glomerular filtration rate and albuminuria with all-cause and cardiovascular mortality in general population cohorts: A collaborative meta-analysis. Lancet 2010, 375, 2073–2081. [Google Scholar]
- Hemmelgarn, B.R.; Manns, B.J.; Lloyd, A.; James, M.T.; Klarenbach, S.; Quinn, R.R.; Wiebe, N.; Tonelli, M.; Alberta Kidney Disease, N. Relation between kidney function, proteinuria, and adverse outcomes. JAMA 2010, 303, 423–429. [Google Scholar] [CrossRef]
- Cozzolino, M.; Mangano, M.; Stucchi, A.; Ciceri, P.; Conte, F.; Galassi, A. Cardiovascular disease in dialysis patients. Nephrol. Dial. Transplant. 2018, 33 (Suppl. S3), iii28–iii34. [Google Scholar] [CrossRef]
- Meijers, B.K.; Van Kerckhoven, S.; Verbeke, K.; Dehaen, W.; Vanrenterghem, Y.; Hoylaerts, M.F.; Evenepoel, P. The uremic retention solute p-cresyl sulfate and markers of endothelial damage. Am. J. Kidney Dis. 2009, 54, 891–901. [Google Scholar] [CrossRef]
- Meijers, B.K.; Claes, K.; Bammens, B.; de Loor, H.; Viaene, L.; Verbeke, K.; Kuypers, D.; Vanrenterghem, Y.; Evenepoel, P. P-cresol and cardiovascular risk in mild-to-moderate kidney disease. Clin. J. Am. Soc. Nephrol. 2010, 5, 1182–1189. [Google Scholar] [CrossRef]
- Yamamoto, H.; Tsuruoka, S.; Ioka, T.; Ando, H.; Ito, C.; Akimoto, T.; Fujimura, A.; Asano, Y.; Kusano, E. Indoxyl sulfate stimulates proliferation of rat vascular smooth muscle cells. Kidney Int. 2006, 69, 1780–1785. [Google Scholar] [CrossRef]
- Dou, L.; Jourde-Chiche, N.; Faure, V.; Cerini, C.; Berland, Y.; Dignat-George, F.; Brunet, P. The uremic solute indoxyl sulfate induces oxidative stress in endothelial cells. J. Thromb. Haemost. 2007, 5, 1302–1308. [Google Scholar] [CrossRef]
- Yu, M.; Kim, Y.J.; Kang, D.H. Indoxyl sulfate-induced endothelial dysfunction in patients with chronic kidney disease via an induction of oxidative stress. Clin. J. Am. Soc. Nephrol. 2011, 6, 30–39. [Google Scholar] [CrossRef]
- Jourde-Chiche, N.; Dou, L.; Cerini, C.; Dignat-George, F.; Vanholder, R.; Brunet, P. Protein-bound toxins--update 2009. Semin. Dial. 2009, 22, 334–339. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Prado, R.; Esteras, R.; Perez-Gomez, M.V.; Gracia-Iguacel, C.; Gonzalez-Parra, E.; Sanz, A.B.; Ortiz, A.; Sanchez-Nino, M.D. Nutrients turned into toxins: Microbiota modulation of nutrient properties in chronic kidney disease. Nutrients 2017, 9, 489. [Google Scholar] [CrossRef] [PubMed]
- Dou, L.; Sallee, M.; Cerini, C.; Poitevin, S.; Gondouin, B.; Jourde-Chiche, N.; Fallague, K.; Brunet, P.; Calaf, R.; Dussol, B.; et al. The cardiovascular effect of the uremic solute indole-3 acetic acid. J. Am. Soc. Nephrol. 2015, 26, 876–887. [Google Scholar] [CrossRef] [PubMed]
- Gondouin, B.; Cerini, C.; Dou, L.; Sallee, M.; Duval-Sabatier, A.; Pletinck, A.; Calaf, R.; Lacroix, R.; Jourde-Chiche, N.; Poitevin, S.; et al. Indolic uremic solutes increase tissue factor production in endothelial cells by the aryl hydrocarbon receptor pathway. Kidney Int. 2013, 84, 733–744. [Google Scholar] [CrossRef]
- Chitalia, V.C.; Shivanna, S.; Martorell, J.; Balcells, M.; Bosch, I.; Kolandaivelu, K.; Edelman, E.R. Uremic serum and solutes increase post-vascular interventional thrombotic risk through altered stability of smooth muscle cell tissue factor. Circulation 2013, 127, 365–376. [Google Scholar] [CrossRef]
- Addi, T.; Poitevin, S.; McKay, N.; El Mecherfi, K.E.; Kheroua, O.; Jourde-Chiche, N.; de Macedo, A.; Gondouin, B.; Cerini, C.; Brunet, P.; et al. Mechanisms of tissue factor induction by the uremic toxin indole-3 acetic acid through aryl hydrocarbon receptor/nuclear factor-kappa b signaling pathway in human endothelial cells. Arch. Toxicol. 2019, 93, 121–136. [Google Scholar] [CrossRef]
- Borges, N.A.; Barros, A.F.; Nakao, L.S.; Dolenga, C.J.; Fouque, D.; Mafra, D. Protein-bound uremic toxins from gut microbiota and inflammatory markers in chronic kidney disease. J. Ren. Nutr. 2016, 26, 396–400. [Google Scholar] [CrossRef]
- Claro, L.M.; Moreno-Amaral, A.N.; Gadotti, A.C.; Dolenga, C.J.; Nakao, L.S.; Azevedo, M.L.V.; de Noronha, L.; Olandoski, M.; de Moraes, T.P.; Stinghen, A.E.M.; et al. The impact of uremic toxicity induced inflammatory response on the cardiovascular burden in chronic kidney disease. Toxins 2018, 10, 384. [Google Scholar] [CrossRef]
- Jeong, Y.M.; Oh, M.H.; Kim, S.Y.; Li, H.; Yun, H.Y.; Baek, K.J.; Kwon, N.S.; Kim, W.Y.; Kim, D.S. Indole-3-acetic acid/horseradish peroxidase induces apoptosis in tccsup human urinary bladder carcinoma cells. Pharmazie 2010, 65, 122–126. [Google Scholar]
- Kim, D.S.; Jeon, S.E.; Park, K.C. Oxidation of indole-3-acetic acid by horseradish peroxidase induces apoptosis in g361 human melanoma cells. Cell. Signal. 2004, 16, 81–88. [Google Scholar] [CrossRef]
- Muslin, A.J. Mapk signalling in cardiovascular health and disease: Molecular mechanisms and therapeutic targets. Clin. Sci. 2008, 115, 203–218. [Google Scholar] [CrossRef] [PubMed]
- Denise Martin, E.; De Nicola, G.F.; Marber, M.S. New therapeutic targets in cardiology: P38 alpha mitogen-activated protein kinase for ischemic heart disease. Circulation 2012, 126, 357–368. [Google Scholar] [CrossRef] [PubMed]
- Kalantar-Zadeh, K.; Tortorici, A.R.; Chen, J.L.; Kamgar, M.; Lau, W.L.; Moradi, H.; Rhee, C.M.; Streja, E.; Kovesdy, C.P. Dietary restrictions in dialysis patients: Is there anything left to eat? Semin. Dial. 2015, 28, 159–168. [Google Scholar] [CrossRef] [PubMed]
- Wright, M.; Southcott, E.; MacLaughlin, H.; Wineberg, S. Clinical practice guideline on undernutrition in chronic kidney disease. BMC Nephrol. 2019, 20, 370. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.T.; Wu, P.H.; Lee, H.H.; Mubanga, M.; Chen, C.S.; Kuo, M.C.; Chiu, Y.W.; Kuo, P.L.; Hwang, S.J. Indole-3 acetic acid increased risk of impaired cognitive function in patients receiving hemodialysis. Neurotoxicology 2019, 73, 85–91. [Google Scholar] [CrossRef] [PubMed]
- Lind, L.; Arnlov, J.; Lindahl, B.; Siegbahn, A.; Sundstrom, J.; Ingelsson, E. Use of a proximity extension assay proteomics chip to discover new biomarkers for human atherosclerosis. Atherosclerosis 2015, 242, 205–210. [Google Scholar] [CrossRef]
- Benjamini Yoav, H.Y. Controlling the false discovery rate: A practical and powerful approach to multiple testing. J. R. Stat. Soc. Ser. B (Methodol.) 1995, 57, 12. [Google Scholar] [CrossRef]
- Szklarczyk, D.; Santos, A.; von Mering, C.; Jensen, L.J.; Bork, P.; Kuhn, M. Stitch 5: Augmenting protein-chemical interaction networks with tissue and affinity data. Nucleic Acids Res. 2016, 44, D380–D384. [Google Scholar] [CrossRef]
- Evenepoel, P.; Meijers, B.K.; Bammens, B.R.; Verbeke, K. Uremic toxins originating from colonic microbial metabolism. Kidney Int. Suppl. 2009, S12–S19. [Google Scholar] [CrossRef]
- Brito, J.S.; Borges, N.A.; Esgalhado, M.; Magliano, D.C.; Soulage, C.O.; Mafra, D. Aryl hydrocarbon receptor activation in chronic kidney disease: Role of uremic toxins. Nephron 2017, 137, 1–7. [Google Scholar] [CrossRef]
- Gouroju, S.; Rao, P.; Bitla, A.R.; Vinapamula, K.S.; Manohar, S.M.; Vishnubhotla, S. Role of gut-derived uremic toxins on oxidative stress and inflammation in patients with chronic kidney disease. Indian J. Nephrol. 2017, 27, 359–364. [Google Scholar]
- Jourde-Chiche, N.; Dou, L.; Sabatier, F.; Calaf, R.; Cerini, C.; Robert, S.; Camoin-Jau, L.; Charpiot, P.; Argiles, A.; Dignat-George, F.; et al. Levels of circulating endothelial progenitor cells are related to uremic toxins and vascular injury in hemodialysis patients. J. Thromb. Haemost. 2009, 7, 1576–1584. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, Y.; Itoh, H.; Fujioka, T.; Sato, F.; Kawasaki, K.; Sato, Y.; Sato, Y.; Ohno, K.; Mimata, H.; Kishino, S. Association of plasma concentration of 4beta-hydroxycholesterol with cyp3a5 polymorphism and plasma concentration of indoxyl sulfate in stable kidney transplant recipients. Drug Metab. Dispos. 2014, 42, 105–110. [Google Scholar] [CrossRef]
- Karu, N.; McKercher, C.; Nichols, D.S.; Davies, N.; Shellie, R.A.; Hilder, E.F.; Jose, M.D. Tryptophan metabolism, its relation to inflammation and stress markers and association with psychological and cognitive functioning: Tasmanian chronic kidney disease pilot study. BMC Nephrol. 2016, 17, 171. [Google Scholar] [CrossRef] [PubMed]
- Mutsaers, H.A.; Wilmer, M.J.; Reijnders, D.; Jansen, J.; van den Broek, P.H.; Forkink, M.; Schepers, E.; Glorieux, G.; Vanholder, R.; van den Heuvel, L.P.; et al. Uremic toxins inhibit renal metabolic capacity through interference with glucuronidation and mitochondrial respiration. Biochim. Biophys. Acta 2013, 1832, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Gao, C.; Ji, S.; Dong, W.; Qi, Y.; Song, W.; Cui, D.; Shi, J. Indolic uremic solutes enhance procoagulant activity of red blood cells through phosphatidylserine exposure and microparticle release. Toxins 2015, 7, 4390–4403. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Nishimura, N.; Kuo, V.; Fiehn, O.; Shahbaz, S.; Van Winkle, L.; Matsumura, F.; Vogel, C.F. Activation of aryl hydrocarbon receptor induces vascular inflammation and promotes atherosclerosis in apolipoprotein e-/- mice. Arterioscler. Thromb. Vasc. Biol. 2011, 31, 1260–1267. [Google Scholar] [CrossRef]
- Boitano, A.E.; Wang, J.; Romeo, R.; Bouchez, L.C.; Parker, A.E.; Sutton, S.E.; Walker, J.R.; Flaveny, C.A.; Perdew, G.H.; Denison, M.S.; et al. Aryl hydrocarbon receptor antagonists promote the expansion of human hematopoietic stem cells. Science 2010, 329, 1345–1348. [Google Scholar] [CrossRef]
- Cardoso, H.J.; Figueira, M.I.; Socorro, S. The stem cell factor (scf)/c-kit signalling in testis and prostate cancer. J. Cell Commun. Signal. 2017, 11, 297–307. [Google Scholar] [CrossRef]
- Kitoh, T.; Ishikawa, H.; Ishii, T.; Nakagawa, S. Elevated scf levels in the serum of patients with chronic renal failure. Br. J. Haematol. 1998, 102, 1151–1156. [Google Scholar] [CrossRef]
- Lennartsson, J.; Ronnstrand, L. Stem cell factor receptor/c-kit: From basic science to clinical implications. Physiol. Rev. 2012, 92, 1619–1649. [Google Scholar] [CrossRef] [PubMed]
- Ashman, L.K. The biology of stem cell factor and its receptor c-kit. Int. J. Biochem. Cell Biol. 1999, 31, 1037–1051. [Google Scholar] [CrossRef]
- Ali, S.R.; Hippenmeyer, S.; Saadat, L.V.; Luo, L.; Weissman, I.L.; Ardehali, R. Existing cardiomyocytes generate cardiomyocytes at a low rate after birth in mice. Proc. Natl. Acad. Sci. USA 2014, 111, 8850–8855. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.L.; Meng, Y.; Kim, J.Y.; Baek, E.J.; Suh, W. Direct and differential effects of stem cell factor on the neovascularization activity of endothelial progenitor cells. Cardiovasc. Res. 2011, 92, 132–140. [Google Scholar] [CrossRef] [PubMed]
- Torsney, E.; Xu, Q. Resident vascular progenitor cells. J. Mol. Cell. Cardiol. 2011, 50, 304–311. [Google Scholar] [CrossRef]
- Matsui, J.; Wakabayashi, T.; Asada, M.; Yoshimatsu, K.; Okada, M. Stem cell factor/c-kit signaling promotes the survival, migration, and capillary tube formation of human umbilical vein endothelial cells. J. Biol. Chem. 2004, 279, 18600–18607. [Google Scholar] [CrossRef]
- Wang, C.H.; Verma, S.; Hsieh, I.C.; Hung, A.; Cheng, T.T.; Wang, S.Y.; Liu, Y.C.; Stanford, W.L.; Weisel, R.D.; Li, R.K.; et al. Stem cell factor attenuates vascular smooth muscle apoptosis and increases intimal hyperplasia after vascular injury. Arterioscler. Thromb. Vasc. Biol. 2007, 27, 540–547. [Google Scholar] [CrossRef]
- Singla, D.K.; Singla, R.D.; Lamm, S.; Glass, C. Tgf-beta2 treatment enhances cytoprotective factors released from embryonic stem cells and inhibits apoptosis in infarcted myocardium. Am. J. Physiol. Heart Circ. Physiol. 2011, 300, H1442–H1450. [Google Scholar] [CrossRef]
- Sato, E.; Saigusa, D.; Mishima, E.; Uchida, T.; Miura, D.; Morikawa-Ichinose, T.; Kisu, K.; Sekimoto, A.; Saito, R.; Oe, Y.; et al. Impact of the oral adsorbent ast-120 on organ-specific accumulation of uremic toxins: Lc-ms/ms and ms imaging techniques. Toxins 2017, 10, 19. [Google Scholar] [CrossRef]
- Santana Machado, T.; Poitevin, S.; Paul, P.; McKay, N.; Jourde-Chiche, N.; Legris, T.; Mouly-Bandini, A.; Dignat-George, F.; Brunet, P.; Masereeuw, R.; et al. Indoxyl sulfate upregulates liver p-glycoprotein expression and activity through aryl hydrocarbon receptor signaling. J. Am. Soc. Nephrol. 2018, 29, 906–918. [Google Scholar]
- Liabeuf, S.; Drueke, T.B.; Massy, Z.A. Protein-bound uremic toxins: New insight from clinical studies. Toxins 2011, 3, 911–919. [Google Scholar] [CrossRef] [PubMed]
- Stockler-Pinto, M.B.; Soulage, C.O.; Borges, N.A.; Cardozo, L.; Dolenga, C.J.; Nakao, L.S.; Pecoits-Filho, R.; Fouque, D.; Mafra, D. From bench to the hemodialysis clinic: Protein-bound uremic toxins modulate nf-kappab/nrf2 expression. Int. Urol. Nephrol. 2018, 50, 347–354. [Google Scholar] [CrossRef] [PubMed]
- Bataille, S.; Pelletier, M.; Sallee, M.; Berland, Y.; McKay, N.; Duval, A.; Gentile, S.; Mouelhi, Y.; Brunet, P.; Burtey, S. Indole 3-acetic acid, indoxyl sulfate and paracresyl-sulfate do not influence anemia parameters in hemodialysis patients. BMC Nephrol. 2017, 18, 251. [Google Scholar] [CrossRef] [PubMed]
- Brito, J.S.; Borges, N.A.; Anjos, J.S.D.; Nakao, L.S.; Stockler-Pinto, M.B.; Paiva, B.R.; Cardoso-Weide, L.C.; Cardozo, L.; Mafra, D. Aryl hydrocarbon receptor and uremic toxins from the gut microbiota in chronic kidney disease patients: Is there a relationship between them? Biochemistry 2019, 58, 2054–2060. [Google Scholar] [CrossRef]
- Watanabe, H.; Miyamoto, Y.; Otagiri, M.; Maruyama, T. Update on the pharmacokinetics and redox properties of protein-bound uremic toxins. J. Pharm. Sci. 2011, 100, 3682–3695. [Google Scholar] [CrossRef]
- De Smet, R.; Dhondt, A.; Eloot, S.; Galli, F.; Waterloos, M.A.; Vanholder, R. Effect of the super-flux cellulose triacetate dialyser membrane on the removal of non-protein-bound and protein-bound uraemic solutes. Nephrol. Dial. Transplant. 2007, 22, 2006–2012. [Google Scholar] [CrossRef]
- Deltombe, O.; Van Biesen, W.; Glorieux, G.; Massy, Z.; Dhondt, A.; Eloot, S. Exploring protein binding of uremic toxins in patients with different stages of chronic kidney disease and during hemodialysis. Toxins 2015, 7, 3933–3946. [Google Scholar] [CrossRef]
- Eloot, S.; Van Biesen, W.; Glorieux, G.; Neirynck, N.; Dhondt, A.; Vanholder, R. Does the adequacy parameter kt/v(urea) reflect uremic toxin concentrations in hemodialysis patients? PLoS ONE 2013, 8, e76838. [Google Scholar] [CrossRef]

| N = 331 | |
|---|---|
| Age (years) | 59.3 ± 11.6 |
| Male | 177 (53.5%) |
| Smoking | 36 (10.9%) |
| Hemodialysis duration, years | 5 (10) |
| Body mass index, kg/m2 | 23.6 (4.8) |
| Cause of ESRD | |
| Hypertension | 36 (10.9%) |
| Diabetes Mellitus | 117 (35.3%) |
| Glomerulonephritis | 117 (35.3%) |
| Others * | 61 (18.4%) |
| Arteriovenous shunt | |
| Arteriovenous fistula | 290 (87.6%) |
| Arteriovenous graft | 41 (12.4%) |
| Comorbidities | |
| Diabetes mellitus | 144 (43.5%) |
| Hypertension | 256 (77.3%) |
| Dyslipidemia | 126 (38.1%) |
| Medications | |
| Antiplatelets/Warfarin | 95 (28.7%) |
| Anti-hypertensive drugs | 156 (47.1%) |
| Diabetic treatment drugs | 111 (33.5%) |
| Laboratory data | |
| Albumin, g/dL | 3.87 ± 0.29 |
| Ionized Calcium, mg/dL | 4.6 (0.64) |
| Phosphate, mg/dL | 4.6 (1.4) |
| High sensitivity C-reactive protein, mg/L | 0.83 (2.68) |
| Total Kt/V | 1.56 (0.32) |
| Uremic toxin (total form) | |
| Indole-3-acetic acid, µg/mL | 0.92 (1) |
| β Coefficient (95% CI) | P-Value | |
|---|---|---|
| Indole-3-acetic acid (µg/mL) | 0.13 (0.04–0.21) | 0.004 |
| Age | −0.0006 (−0.0003–0.002) | 0.66 |
| Sex | −0.06 (−0.12–0.003) | 0.063 |
| Smoking | 0.01 (−0.08–0.10) | 0.80 |
| Hemodialysis duration (years) | −0.002 (−0.008–0.003) | 0.51 |
| Body mass index (kg/m2) | −0.001 (−0.005–0.002) | 0.50 |
| Cause of ESRD: Hypertension | −0.02 (−0.13–0.09) | 0.76 |
| Cause of ESRD: Diabetes Mellitus | 0.12 (−0.008–0.25) | 0.07 |
| Cause of ESRD: Glomerulonephritis | 0.007 (−0.08–0.09) | 0.86 |
| Diabetes Mellitus comorbidity | −0.15 (−0.26–-0.03) | 0.01 |
| Hypertension comorbidity | −0.03 (−0.11–0.05) | 0.48 |
| Hyperlipidemia comorbidity | 0.03 (−0.04–0.09) | 0.42 |
| Antiplatelet/warfarin | −0.02 (−0.08–0.05) | 0.60 |
| Anti-hypertensive drugs | −0.05 (−0.11–0.02) | 0.18 |
| Diabetic treatment drugs | −0.02 (−0.12–0.09) | 0.74 |
| Albumin (g/dL) | 0.16 (0.06–0.26) | 0.002 |
| Ionized Calcium (mg/dL) | −0.04 (−0.1–0.03) | 0.24 |
| Phosphate (mg/dL) | −0.01 (−0.04–0.02) | 0.44 |
| High sensitivity C-reactive protein (mg/L) | 0.00009 (−0.007–0.008) | 0.82 |
| Total Kt/V | 0.02 (−0.11–0.15) | 0.74 |
| Functional Enrichments in Your Network | |||
|---|---|---|---|
| Pathway ID | Pathway Description | Count in the Gene Set | Bonferroni Corrected p-Value |
| Biological Process (GO) | |||
| GO:0031399 | Regulation of protein modification process | 8 | 0.000877 |
| GO:0031401 | Positive regulation of protein modification process | 7 | 0.000877 |
| GO:0038162 | Erythropoietin-mediated signaling pathway | 2 | 0.000877 |
| GO:0042523 | Positive regulation of tyrosine phosphorylation of Stat5 protein | 3 | 0.000877 |
| GO:0008284 | Positive regulation of cell proliferation | 6 | 0.00237 |
| GO:0036018 | Cellular response to erythropoietin | 2 | 0.00237 |
| GO:0050731 | Positive regulation of peptidyl-tyrosine phosphorylation | 4 | 0.00237 |
| GO:0050776 | Regulation of immune response | 6 | 0.00237 |
| GO:0048872 | Homeostasis of number of cells | 4 | 0.00276 |
| GO:0045087 | Innate immune response | 6 | 0.00355 |
| GO:0030218 | Erythrocyte differentiation | 3 | 0.00497 |
| GO:0035234 | Ectopic germ cell programmed cell death | 2 | 0.00553 |
| GO:0034101 | Erythrocyte homeostasis | 3 | 0.00608 |
| GO:0043408 | Regulation of MAPK cascade | 5 | 0.00608 |
| GO:0001932 | Regulation of protein phosphorylation | 6 | 0.0084 |
| GO:0031325 | Positive regulation of cellular metabolic process | 8 | 0.00915 |
| GO:0002376 | Immune system process | 7 | 0.0104 |
| GO:0033033 | Negative regulation of myeloid cell apoptotic process | 2 | 0.0109 |
| GO:0001934 | Positive regulation of protein phosphorylation | 5 | 0.0151 |
| GO:0002768 | Immune response-regulating cell Surface receptor signaling pathway | 4 | 0.0151 |
| GO:0043067 | Regulation of programmed cell death | 6 | 0.0151 |
| GO:0045597 | Positive regulation of cell differentiation | 5 | 0.0151 |
| GO:0048070 | Regulation of developmental pigmentation | 2 | 0.0151 |
| GO:1902531 | Regulation of intracellular signal transduction | 6 | 0.0151 |
| GO:0043069 | Negative regulation of programmed cell death | 5 | 0.0173 |
| GO:0048015 | Phosphatidylinositol-mediated signaling | 3 | 0.0187 |
| GO:0009888 | Tissue development | 6 | 0.0205 |
| GO:0048568 | Embryonic organ development | 4 | 0.0208 |
| GO:0008543 | Fibroblast growth factor receptor signaling pathway | 3 | 0.025 |
| GO:0035162 | Embryonic hemopoiesis | 2 | 0.025 |
| GO:0038095 | Fc-epsilon receptor signaling pathway | 3 | 0.0261 |
| GO:0030097 | hemopoiesis | 4 | 0.0305 |
| GO:0042517 | Positive regulation of tyrosine phosphorylation of Stat3 protein | 2 | 0.0323 |
| GO:0044344 | Cellular response to fibroblast growth factor stimulus | 3 | 0.0323 |
| GO:0046777 | Protein autophosphorylation | 3 | 0.033 |
| GO:0046579 | Positive regulation of Ras protein signal transduction | 2 | 0.0346 |
| GO:0007173 | Epidermal growth factor receptor signaling pathway | 3 | 0.0374 |
| GO:0051347 | Positive regulation of transferase activity | 4 | 0.0374 |
| GO:0002520 | Immune system development | 4 | 0.0403 |
| GO:0048584 | Positive regulation of response to stimulus | 6 | 0.0403 |
| GO:0038083 | Peptidyl-tyrosine autophosphorylation | 2 | 0.0419 |
| GO:0048678 | Response to axon injury | 2 | 0.0468 |
| GO:0061515 | Myeloid cell development | 2 | 0.0468 |
| GO:0034097 | Response to cytokine | 4 | 0.048 |
| GO:0071363 | Cellular response to growth factor stimulus | 4 | 0.0496 |
| Molecular Function (GO) | |||
| GO:0005126 | Cytokine receptor binding | 4 | 0.0187 |
| Kyoto Encyclopedia of Genes and Genomes (KEGG) Pathways | |||
| 4151 | PI3K-Akt signaling pathway | 7 | 6.42 × 10−8 |
| 4640 | Hematopoietic cell lineage | 4 | 1.92 × 10−5 |
| 4630 | Jak-STAT signaling pathway | 4 | 0.00014 |
| 4060 | Cytokine-cytokine receptor interaction | 4 | 0.000836 |
| 4014 | Ras signaling pathway | 3 | 0.0142 |
| 5221 | Acute myeloid leukemia | 2 | 0.022 |
| 4917 | Prolactin signaling pathway | 2 | 0.027 |
| 5200 | Pathways in cancer | 3 | 0.027 |
| 4916 | Melanogenesis | 2 | 0.0445 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wu, P.-H.; Lin, Y.-T.; Wu, P.-Y.; Lee, H.-H.; Lee, S.-C.; Hung, S.-C.; Chen, S.-C.; Kuo, M.-C.; Chiu, Y.-W. Association between Circulation Indole-3-Acetic Acid Levels and Stem Cell Factor in Maintenance Hemodialysis Patients: A Cross-Sectional Study. J. Clin. Med. 2020, 9, 124. https://doi.org/10.3390/jcm9010124
Wu P-H, Lin Y-T, Wu P-Y, Lee H-H, Lee S-C, Hung S-C, Chen S-C, Kuo M-C, Chiu Y-W. Association between Circulation Indole-3-Acetic Acid Levels and Stem Cell Factor in Maintenance Hemodialysis Patients: A Cross-Sectional Study. Journal of Clinical Medicine. 2020; 9(1):124. https://doi.org/10.3390/jcm9010124
Chicago/Turabian StyleWu, Ping-Hsun, Yi-Ting Lin, Pei-Yu Wu, Hei-Hwa Lee, Su-Chu Lee, Szu-Chun Hung, Szu-Chia Chen, Mei-Chuan Kuo, and Yi-Wen Chiu. 2020. "Association between Circulation Indole-3-Acetic Acid Levels and Stem Cell Factor in Maintenance Hemodialysis Patients: A Cross-Sectional Study" Journal of Clinical Medicine 9, no. 1: 124. https://doi.org/10.3390/jcm9010124
APA StyleWu, P.-H., Lin, Y.-T., Wu, P.-Y., Lee, H.-H., Lee, S.-C., Hung, S.-C., Chen, S.-C., Kuo, M.-C., & Chiu, Y.-W. (2020). Association between Circulation Indole-3-Acetic Acid Levels and Stem Cell Factor in Maintenance Hemodialysis Patients: A Cross-Sectional Study. Journal of Clinical Medicine, 9(1), 124. https://doi.org/10.3390/jcm9010124







