Factors Enhancing Serum Syndecan-1 Concentrations: A Large-Scale Comprehensive Medical Examination
Abstract
1. Introduction
2. Experimental Section
2.1. Study Population
2.2. Ethics Approval and Consent to Participate
2.3. Consent for Publication
2.4. Clinical Assessments
2.5. Laboratory Data
2.6. Statistical Analyses
3. Results
3.1. Characteristics of the Patients
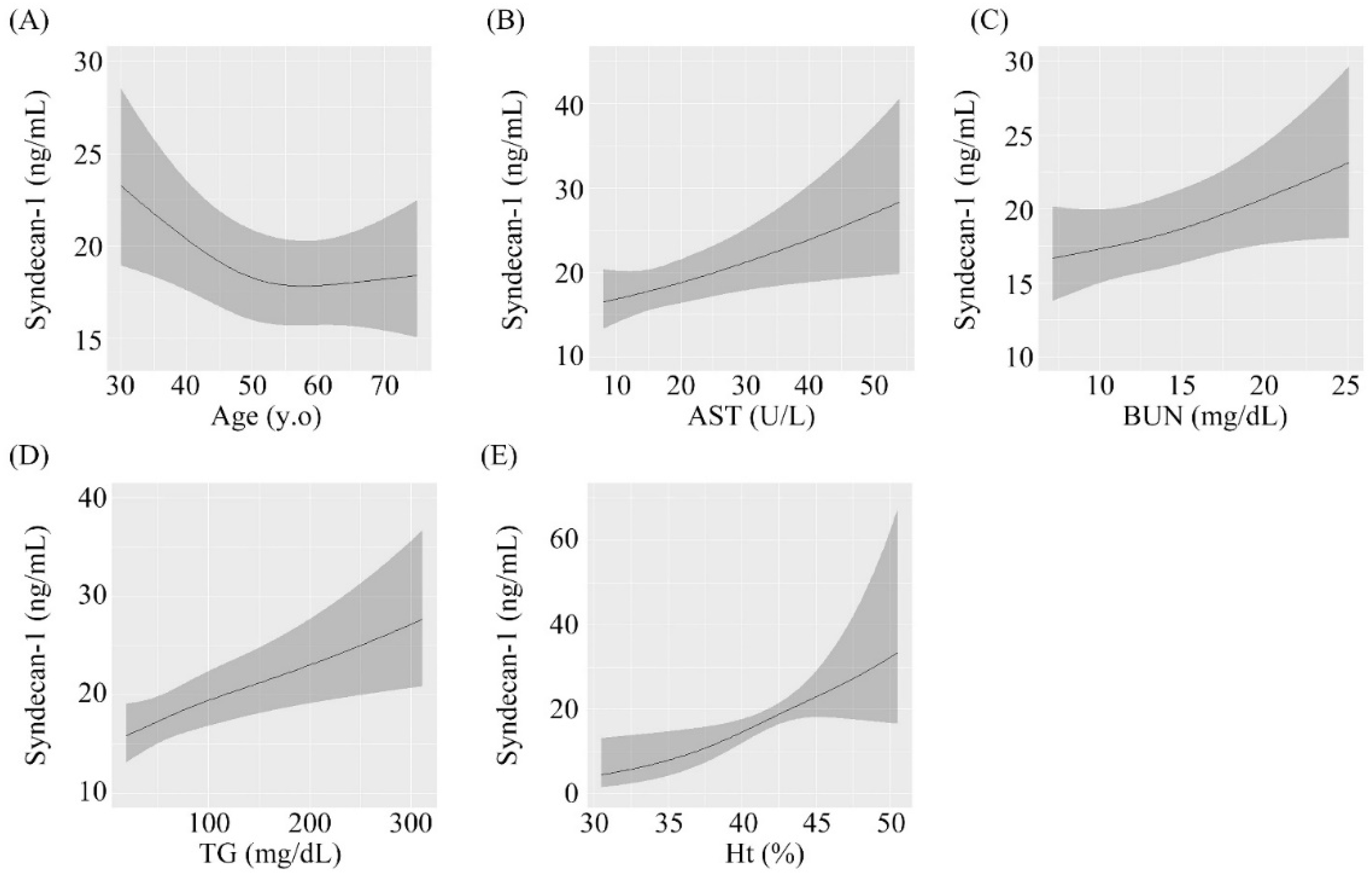
3.2. Associations of Serum Syndecan-1 with Various Parameters
3.3. Subgroup Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Tabit, C.E.; Chung, W.B.; Hamburg, N.M.; Vita, J.A. Endothelial dysfunction in diabetes mellitus: Molecular mechanisms and clinical implications. Rev. Endocr. Metab. Disord. 2010, 11, 61–74. [Google Scholar] [CrossRef] [PubMed]
- Vaisman, B.L.; Andrews, K.L.; Khong, S.M.; Wood, K.C.; Moore, X.L.; Fu, Y.; Kepka-Lenhart, D.M.; Morris Jr, S.M.; Remaley, A.T.; Chin-Dusting, J.P. Selective endothelial overexpression of arginase II induces endothelial dysfunction and hypertension and enhances atherosclerosis in mice. PLoS ONE 2012, 7, e39487. [Google Scholar] [CrossRef] [PubMed]
- Sharma, S.; Singh, M.; Sharma, P.L. Mechanism of attenuation of diabetes mellitus and hypercholesterolemia induced vascular endothelial dysfunction by protein tyrosine phosphatase inhibition. Vascul. Pharmacol. 2011, 54, 80–87. [Google Scholar] [CrossRef]
- Goon, P.K.Y.; Lip, G.Y.H.; Boos, C.J.; Stonelake, P.S.; Blann, A.D. Circulating endothelial cells, endothelial progenitor cells, and endothelial microparticles in cancer. Neoplasia 2006, 8, 79–88. [Google Scholar] [CrossRef]
- Lefer, A.M. Endothelial dysfunction as a trigger for ischemia-reperfusion injury. J. Thromb. 1997, 4, 63–65. [Google Scholar] [CrossRef]
- Maniatis, N.A.; Orfanos, S.E. The endothelium in acute lung injury/acute respiratory distress syndrome. Curr. Opin. Crit. Care 2008, 14, 22–30. [Google Scholar] [CrossRef]
- Annuk, M.; Zilmer, M.; Fellstrom, B. Endothelium-dependent vasodilation and oxidative stress in chronic renal failure: Impact on cardiovascular disease. Kidney Int. Suppl. 2003, 84, S50–S53. [Google Scholar] [CrossRef] [PubMed]
- Murdaca, G.; Colombo, B.M.; Cagnati, P.; Gulli, R.; Spano, F.; Puppo, F. Endothelial dysfunction in rheumatic autoimmune diseases. Atherosclerosis 2012, 224, 309–317. [Google Scholar] [CrossRef]
- Bijl, M. Endothelial activation, endothelial dysfunction and premature atherosclerosis in systemic autoimmune diseases. Neth. J. Med. 2003, 61, 273–277. [Google Scholar] [PubMed]
- Thijssen, D.H.; Black, M.A.; Pyke, K.E.; Padilla, J.; Atkinson, G.; Harris, R.A.; Parker, B.; Widlansky, M.E.; Tschakovsky, M.E.; Green, D.J. Assessment of flow-mediated dilation in humans: A methodological and physiological guideline. Am. J. Physiol. Heart Circ. Physiol. 2011, 300, H2–H12. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, J.C.; Pyke, K.E. Flow-mediated dilation stimulated by sustained increases in shear stress: A useful tool for assessing endothelial function in humans? Am. J. Physiol. Heart Circ. Physiol. 2018, 314, H508–H520. [Google Scholar] [CrossRef]
- Becker, B.F.; Chappell, D.; Jacob, M. Endothelial glycocalyx and coronary vascular permeability: The fringe benefit. Basic Res. Cardiol. 2010, 105, 687–701. [Google Scholar] [CrossRef]
- Luft, J.H. Fine structures of capillary and endocapillary layer as revealed by ruthenium red. Fed. Proc. 1966, 25, 1773–1783. [Google Scholar]
- Rehm, M.; Zahler, S.; Lötsch, M.; Welsch, U.; Conzen, P.; Jacob, M.; Becker, B.F. Endothelial glycocalyx as an additional barrier determining extravasation of 6% hydroxyethyl starch or 5% albumin solutions in the coronary vascular bed. Anesthesiology 2004, 100, 1211–1223. [Google Scholar] [CrossRef]
- Okada, H.; Takemura, G.; Suzuki, K.; Oda, K.; Takada, C.; Hotta, Y.; Miyazaki, N.; Tsujimoto, A.; Muraki, I.; Ando, Y.; et al. Three-dimensional ultrastructure of capillary endothelial glycocalyx under normal and experimental endotoxemic conditions. Crit. Care 2017, 21, 261. [Google Scholar] [CrossRef]
- Ando, Y.; Okada, H.; Takemura, G.; Suzuki, K.; Takada, C.; Tomita, H.; Zaikokuji, R.; Hotta, Y.; Miyazaki, N.; Yano, H.; et al. Brain-specific ultrastructure of capillary endothelial glycocalyx and its possible contribution for blood brain barrier. Sci. Rep. 2018, 8, 17523. [Google Scholar] [CrossRef]
- Inagawa, R.; Okada, H.; Takemura, G.; Suzuki, K.; Takada, C.; Yano, H.; Ando, Y.; Usui, T.; Hotta, Y.; Miyazaki, N.; et al. Ultrastructural alteration of pulmonary capillary endothelial glycocalyx during endotoxemia. Chest 2018, 154, 317–325. [Google Scholar] [CrossRef]
- Lee, W.L.; Slutsky, A.S. Sepsis and endothelial permeability. N. Engl. J. Med. 2010, 363, 689–691. [Google Scholar] [CrossRef]
- Woodcock, T.E.; Woodcock, T.M. Revised Starling equation and the glycocalyx model of transvascular fluid exchange: An improved paradigm for prescribing intravenous fluid therapy. Br. J. Anaesth. 2012, 108, 384–394. [Google Scholar] [CrossRef]
- Chelazzi, C.; Villa, G.; Mancinelli, P.; De Gaudio, A.R.; Adembri, C. Glycocalyx and sepsis-induced alterations in vascular permeability. Crit. Care 2015, 19, 26. [Google Scholar] [CrossRef]
- Paulus, P.; Jennewein, C.; Zacharowski, K. Biomarkers of endothelial dysfunction: Can they help us deciphering systemic inflammation and sepsis? Biomarkers 2011, 16, S11–S21. [Google Scholar] [CrossRef]
- Salmon, A.H.; Satchell, S.C. Endothelial glycocalyx dysfunction in disease: Albuminuria and increased microvascular permeability. J. Pathol. 2012, 226, 562–574. [Google Scholar] [CrossRef]
- Li, L.; Ly, M.; Linhardt, R.J. Proteoglycan sequence. Mol. Biosyst. 2012, 8, 1613–1625. [Google Scholar] [CrossRef]
- Rehm, M.; Bruegger, D.; Christ, F.; Conzen, P.; Thiel, M.; Jacob, M.; Chappell, D.; Stoeckelhubar, M.; Welsch, U.; Reichart, B.; et al. Shedding of the endothelial glycocalyx in patients undergoing major vascular surgery with global and regional ischemia. Circulation 2007, 116, 1896–1906. [Google Scholar] [CrossRef]
- Puskarich, M.A.; Cornelius, D.C.; Tharp, J.; Nandi, U.; Jones, A.E. Plasma syndecan-1 levels identify a cohort of patients with severe sepsis at high risk for intubation after large-volume intravenous fluid resuscitation. J. Crit. Care 2016, 36, 125–129. [Google Scholar] [CrossRef]
- Ostrowski, S.R.; Haase, N.; Müller, R.B.; Møller, M.H.; Pott, F.C.; Perner, A.; Johansson, P.I. Association between biomarkers of endothelial injury and hypocoagulability in patients with severe sepsis: A prospective study. Crit. Care 2015, 19, 191. [Google Scholar] [CrossRef]
- Arthur, A.; McCall, P.J.; Jolly, L.; Kinsella, J.; Kirk, A.; Shelley, B.G. Endothelial glycocalyx layer shedding following lung resection. Biomark. Med. 2016, 10, 1033–1038. [Google Scholar] [CrossRef]
- Murphy, L.S.; Wickersham, N.; McNeil, J.B.; Shaver, C.M.; May, A.K.; Bastarache, J.A.; Ware, L.B. Endothelial glycocalyx degradation is more severe in patients with non-pulmonary sepsis compared to pulmonary sepsis and associates with risk of ARDS and other organ dysfunction. Ann. Intensiv. Care 2017, 7, 102. [Google Scholar] [CrossRef]
- Henrich, M.; Gruss, M.; Weigand, M.A. Sepsis-induced degradation of endothelial glycocalix. Sci. World J. 2010, 10, 917–923. [Google Scholar] [CrossRef]
- Kim, Y.H.; Nijst, P.; Kiefer, K.; Tang, W.H. Endothelial glycocalyx as biomarker for cardiovascular diseases: Mechanistic and clinical implications. Curr. Heart Fail. Rep. 2017, 14, 117–126. [Google Scholar] [CrossRef]
- Libório, A.B.; Braz, M.B.M.; Seguro, A.C.; Meneses, G.C.; de Oliveira Neves, F.M.; Pedrosa, D.C.; de Góes Cavalcanti, L.P.; Martins, A.M.C.; de Francesco Daher, E. Endothelial glycocalyx damage is associated with leptospirosis acute kidney injury. Am. J. Trop. Med. Hyg. 2015, 92, 611–616. [Google Scholar] [CrossRef]
- De Oliveira Neves, F.M.; Meneses, G.C.; Sousa, N.E.A.; Parahyba, M.C.; Martins, A.M.C.; Libório, A.B. Syndecan-1 in acute decompensated heart failure—Association with renal function and mortality. Circ. J. 2015, 79, 1511–1519. [Google Scholar] [CrossRef]
- Padberg, J.S.; Wiesinger, A.; di Marco, G.S.; Reuter, S.; Grabner, A.; Kentrup, D.; Lukasz, A.; Oberleithner, H.; Pavenstädt, H.; Brand, M.; et al. Damage of the endothelial glycocalyx in chronic kidney disease. Atherosclerosis 2014, 234, 335–343. [Google Scholar] [CrossRef]
- Grundmann, S.; Fink, K.; Rabadzhieva, L.; Bourgeois, N.; Schwab, T.; Moser, M.; Bode, C.; Busch, H.J. Perturbation of the endothelial glycocalyx in post cardiac arrest syndrome. Resuscitation 2012, 83, 715–720. [Google Scholar] [CrossRef]
- Muller, R.B.; Ostrowski, S.R.; Haase, N.; Wetterslev, J.; Perner, A.; Johansson, P.I. Markers of endothelial damage and coagulation impairment in patients with severe sepsis resuscitated with hydroxyethyl starch 130/0.42 vs Ringer acetate. J. Crit. Care. 2016, 32, 16–20. [Google Scholar] [CrossRef]
- Ostrowski, S.R.; Gaini, S.; Pedersen, C.; Johansson, P.I. Sympathoadrenal activation and endothelial damage in patients with varying degrees of acute infectious disease: An observational study. J. Crit. Care 2015, 30, 90–96. [Google Scholar] [CrossRef]
- Sloop, G.D.; Weidman, J.J.; St Cyr, J.A. Perspective: Interesterified triglycerides, the recent increase in deaths from heart disease, and elevated blood viscosity. Ther. Adv. Cardiovasc. Dis. 2018, 12, 23–28. [Google Scholar] [CrossRef]
- Florian, J.A.; Kosky, J.R.; Ainslie, K.; Pang, Z.; Dull, R.O.; Tarbell, J.M. Heparan sulfate proteoglycan is a mechanosensor on endothelial cells. Circ. Res. 2003, 93, e136–e142. [Google Scholar] [CrossRef]
- Mochizuki, S.; Vink, H.; Hiramatsu, O.; Kajita, T.; Shigeto, F.; Spaan, J.A.; Kajiya, F. Role of hyaluronic acid glycosaminoglycans in shear-induced endothelium-derived nitric oxide release. Am. J. Physiol. Heart Circ. Physiol. 2003, 285, H722–H726. [Google Scholar] [CrossRef]
- Thi, M.M.; Tarbell, J.M.; Weinbaum, S.; Spray, D.C. The role of the glycocalyx in reorganization of the actin cytoskeleton under fluid shear stress: A “bumper-car” model. Proc. Natl. Acad. Sci. USA 2004, 101, 16483–16488. [Google Scholar] [CrossRef]
- Arisaka, T.; Mitsumata, M.; Kawasumi, M.; Tohjima, T.; Hirose, S.; Yoshida, Y. Effects of shear stress on glycosaminoglycan synthesis in vascular endothelial cells. Ann. N. Y. Acad. Sci. 1995, 748, 543–554. [Google Scholar] [CrossRef]
- Gouverneur, M.; Spaan, J.A.; Pannekoek, H.; Fontijn, R.D.; Vink, H. Fluid shear stress stimulates incorporation of hyaluronan into endothelial cell glycocalyx. Am. J. Physiol. Heart Circ. Physiol. 2006, 290, H458–H452. [Google Scholar] [CrossRef]
- Zeng, Y.; Tarbell, J M. The adaptive remodeling of endothelial glycocalyx in response to fluid shear stress. PLoS ONE 2014, 9, e86249. [Google Scholar]
- Huo, Y.; Kassab, G.S. Effect of compliance and hematocrit on wall shear stress in a model of the entire coronary arterial tree. J. Appl. Physiol. 2009, 107, 500–505. [Google Scholar] [CrossRef]
- Chang, E.; Harley, C.B. Telomere length and replicative aging in human vascular tissues. Proc. Natl. Acad. Sci. USA. 1995, 92, 11190–11194. [Google Scholar] [CrossRef]
- Stanford, K.I.; Bishop, J.R.; Foley, E.M.; Gonzales, J.C.; Niesman, I.R.; Witztum, J.L.; Esko, J.D. Syndecan-1 is the primary heparan sulfate proteoglycan mediating hepatic clearance of triglyceride-rich lipoproteins in mice. J. Clin. Invest. 2009, 119, 3236–3245. [Google Scholar] [CrossRef]
- Fuki, I.V.; Kuhn, K.M.; Lomazov, I.R.; Rothman, V.L.; Tuszynski, G.P.; Iozzo, R.V.; Swenson, T.L.; Fisher, E.A.; Williams, K.J. The syndecan family of proteoglycans. Novel receptors mediating internalization of atherogenic lipoproteins in vitro. J. Clin. Invest. 1997, 100, 1611–1622. [Google Scholar] [CrossRef]
- Zeng, B.J.; Mortimer, B.C.; Martins, I.J.; Seydel, U.; Redgrave, T.G. Chylomicron remnant uptake is regulated by the expression and function of heparan sulfate proteoglycan in hepatocytes. J. Lipid Res. 1998, 39, 845–860. [Google Scholar]
- Yu, K.C.; Chen, W.; Cooper, A.D. LDL receptor-related protein mediates cell-surface clustering and hepatic sequestration of chylomicron remnants in LDLR-deficient mice. J. Clin. Invest. 2001, 107, 1387–1394. [Google Scholar] [CrossRef]
- Meyer, M.E.; Williams, K.J. Transmembrane and cytoplasmic domains of syndecan mediate a multi-step endocytic pathway involving detergent-insoluble membrane rafts. Biochem. J. 2000, 351, 607–612. [Google Scholar]
- Cortés, V.; Amigo, L.; Donoso, K.; Valencia, I.; Quiñones, V.; Zanlungo, S.; Brandan, E.; Rigotti, A. Adenovirus-mediated hepatic syndecan-1 overexpression induces hepatocyte proliferation and hyperlipidaemia in mice. Liver Int. 2007, 27, 569–581. [Google Scholar] [CrossRef]
- Sherr, C.J.; DePinho, R.A. Cellular senescence: Mitotic clock or culture shock? Cell 2000, 102, 407–410. [Google Scholar] [CrossRef]
- Constantinescu, A.A.; Vink, H.; Spaan, J.A. Elevated capillary tube hematocrit reflects degradation of endothelial cell glycocalyx by oxidized LDL. Am. J. Physiol. Heart Circ. Physiol. 2001, 280, H1051–H1057. [Google Scholar] [CrossRef]
- Nieuwdorp, M.; Mooij, H.L.; Kroon, J.; Atasever, B.; Spaan, J.A.; Ince, C.; Holleman, F.; Diamant, M.; Heine, R.J.; Hoekstra, J.B.; et al. Endothelial glycocalyx damage coincides with microalbuminuria in type 1 diabetes. Diabetes 2006, 55, 1127–1132. [Google Scholar] [CrossRef]
- Nieuwdorp, M.; van Haeften, T.W.; Gouverneur, M.C.; Mooij, H.L.; van Lieshout, M.H.; Levi, M.; Meijers, J.C.; Holleman, F.; Hoekstra, J.B.; Vink, H.; et al. Loss of endothelial glycocalyx during acute hyperglycemia coincides with endothelial dysfunction and coagulation activation in vivo. Diabetes 2006, 55, 480–486. [Google Scholar] [CrossRef] [PubMed]
- Broekhuizen, L.N.; Lemkes, B.A.; Mooij, H.L.; Meuwese, M.C.; Verberne, H.; Holleman, F.; Schlingemann, R.O.; Nieuwdorp, M.; Stroes, E.S.; Vink, H. Effect of sulodexide on endothelial glycocalyx and vascular permeability in patients with type 2 diabetes mellitus. Diabetologia 2010, 53, 2646–2655. [Google Scholar] [CrossRef] [PubMed]
| Median or Number | (25–75 Percentile) | |
|---|---|---|
| Number of Cases | 1312 | |
| Age | 51 | (43–59) |
| Sex (M/F) | 819/493 | |
| BMI (kg/m2) | 22.6 | (20.6–24.8) |
| SBP (mmHg) | 122 | (111–132) |
| TP (g/dL) | 7.3 | (7.1–7.6) |
| Alb (g/dL) | 4.3 | (4.2–4.5) |
| T-Bil (mg/dL) | 0.7 | (0.5–0.9) |
| AST (U/L) | 17 | (14–22) |
| ALT (U/L) | 16 | (12–23) |
| LDH (U/L) | 242 | (219–268) |
| BUN (mg/dL) | 13.4 | (11.4–15.8) |
| Cre (mg/dL) | 0.77 | (0.64–0.88) |
| CRP (mg/dL) | 0.04 | (0.02–0.09) |
| FBS (mg/dL) | 97 | (92–104) |
| HbA1c (%) | 5.4 | (5.3–5.6) |
| TG (mg/dL) | 68 | (47–99) |
| HDL –cho (mg/dL) | 63 | (51–78) |
| LDL-cho (mg/dL) | 115 | (97–134) |
| UA (mg/dL) | 5.0 | (4.0–6.0) |
| Hb (g/dL) | 14.6 | (13.4–15.5) |
| Ht (%) | 42.1 | (39.0–44.6) |
| WBC (×103/µl) | 5000 | (4200–5900) |
| Plt (×104/µl) | 22.4 | (19.3–25.7) |
| History of Present Illness | Number | (Percentage) |
| Hypertension | 234 | (17.8%) |
| Diabetes Mellitus | 80 | (6.1%) |
| Hyperlipidemia | 173 | (13.2%) |
| Hyper Uric Acid | 70 | (5.3%) |
| Malignant Neoplasm | 65 | (5.0%) |
| 25 Percentile | 75 Percentile | Fold-Change [IQR] | 95%LCI | 95%UCI | p-Value | |
|---|---|---|---|---|---|---|
| Age | 43 | 59 | 0.903 | 0.831 | 0.982 | 0.016 |
| Sex—Female: Male | - | - | 0.883 | 0.759 | 1.026 | 0.105 |
| Medication—Yes: No | - | - | 1.030 | 0.944 | 1.124 | 0.505 |
| BMI (kg/m2) | 20.6 | 24.8 | 0.995 | 0.939 | 1.054 | 0.863 |
| SBP (mmHg) | 111 | 132 | 0.972 | 0.908 | 1.039 | 0.471 |
| TP (g/dL) | 7.1 | 7.6 | 0.979 | 0.918 | 1.044 | 0.755 |
| Alb (g/dL) | 4.2 | 4.5 | 0.980 | 0.913 | 1.051 | 0.784 |
| T-Bil (mg/dL) | 0.5 | 0.9 | 0.940 | 0.865 | 1.021 | 0.168 |
| AST (U/L) | 14 | 22 | 1.093 | 0.996 | 1.200 | 0.020 |
| ALT (U/L) | 12 | 23 | 1.046 | 0.945 | 1.158 | 0.484 |
| LDH (U/L) | 219 | 268 | 0.979 | 0.916 | 1.045 | 0.680 |
| BUN (mg/dL) | 11.4 | 15.8 | 1.083 | 1.018 | 1.152 | 0.013 |
| Cre (mg/dL) | 0.64 | 0.88 | 1.048 | 0.952 | 1.154 | 0.591 |
| CRP (mg/dL) | 0.02 | 0.09 | 1.023 | 0.935 | 1.119 | 0.725 |
| FBS (mg/dL) | 92 | 104 | 0.993 | 0.929 | 1.061 | 0.603 |
| HbA1c (%) | 5.3 | 5.6 | 0.954 | 0.907 | 1.004 | 0.077 |
| TG (mg/dL) | 47 | 99 | 1.131 | 1.030 | 1.242 | <0.001 |
| HDL-cho (mg/dL) | 51 | 78 | 1.078 | 0.989 | 1.174 | 0.118 |
| LDL-cho (mg/dL) | 97 | 134 | 0.970 | 0.913 | 1.031 | 0.515 |
| UA (mg/dL) | 4.0 | 6.0 | 0.998 | 0.917 | 1.087 | 0.341 |
| Hb (g/dL) | 13.4 | 15.5 | 0.663 | 0.470 | 0.934 | 0.050 |
| Ht (%) | 39.0 | 44.6 | 1.726 | 1.233 | 2.417 | 0.006 |
| WBC (×103/µl) | 4200 | 5900 | 0.976 | 0.909 | 1.047 | 0.666 |
| Plt (×104/µl) | 19.3 | 25.7 | 1.02 | 0.960 | 1.084 | 0.674 |
| Median or Number | (25–75 Percentile) | |
|---|---|---|
| Number of Cases | 78 | |
| Age | 46 | (42–52) |
| Sex (M/F) | 41/37 | |
| BMI (kg/m2) | 21.9 | (20.2–22.8) |
| SBP (mmHg) | 110 | (102–119) |
| TP (g/dL) | 7.2 | (7.0–7.4) |
| Alb (g/dL) | 4.3 | (4.1–4.5) |
| T-Bil (mg/dL) | 0.7 | (0.5–0.8) |
| AST (U/L) | 16 | (13–19) |
| ALT (U/L) | 14 | (10–18) |
| LDH (U/L) | 235 | (210–255) |
| BUN (mg/dL) | 12.9 | (11.0–14.4) |
| Cre (mg/dL) | 0.72 | (0.62–0.86) |
| CRP (mg/dL) | 0.03 | (0.01–0.05) |
| FBS (mg/dL) | 94 | (88–98) |
| HbA1c (%) | 5.3 | (5.2–5.5) |
| TG (mg/dL) | 63 | (49–84) |
| HDL-cho (mg/dL) | 67 | (57–81) |
| LDL-cho (mg/dL) | 105 | (90–117) |
| UA (mg/dL) | 4.7 | (4.0–5.6) |
| Hb (g/dL) | 14.2 | (13.5–15.0) |
| Ht (%) | 41.1 | (39.2–43.7) |
| WBC (×103/µl) | 5150 | (4525–5875) |
| Plt (×104/µl) | 22.2 | (19.0–24.2) |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oda, K.; Okada, H.; Suzuki, A.; Tomita, H.; Kobayashi, R.; Sumi, K.; Suzuki, K.; Takada, C.; Ishihara, T.; Suzuki, K.; et al. Factors Enhancing Serum Syndecan-1 Concentrations: A Large-Scale Comprehensive Medical Examination. J. Clin. Med. 2019, 8, 1320. https://doi.org/10.3390/jcm8091320
Oda K, Okada H, Suzuki A, Tomita H, Kobayashi R, Sumi K, Suzuki K, Takada C, Ishihara T, Suzuki K, et al. Factors Enhancing Serum Syndecan-1 Concentrations: A Large-Scale Comprehensive Medical Examination. Journal of Clinical Medicine. 2019; 8(9):1320. https://doi.org/10.3390/jcm8091320
Chicago/Turabian StyleOda, Kazumasa, Hideshi Okada, Akio Suzuki, Hiroyuki Tomita, Ryo Kobayashi, Kazuyuki Sumi, Kodai Suzuki, Chihiro Takada, Takuma Ishihara, Keiko Suzuki, and et al. 2019. "Factors Enhancing Serum Syndecan-1 Concentrations: A Large-Scale Comprehensive Medical Examination" Journal of Clinical Medicine 8, no. 9: 1320. https://doi.org/10.3390/jcm8091320
APA StyleOda, K., Okada, H., Suzuki, A., Tomita, H., Kobayashi, R., Sumi, K., Suzuki, K., Takada, C., Ishihara, T., Suzuki, K., Kano, S., Kondo, K., Iwashita, Y., Yano, H., Zaikokuji, R., Sampei, S., Fukuta, T., Kitagawa, Y., Okamoto, H., ... Ogura, S. (2019). Factors Enhancing Serum Syndecan-1 Concentrations: A Large-Scale Comprehensive Medical Examination. Journal of Clinical Medicine, 8(9), 1320. https://doi.org/10.3390/jcm8091320





