Acupuncture for Depression: A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Methods
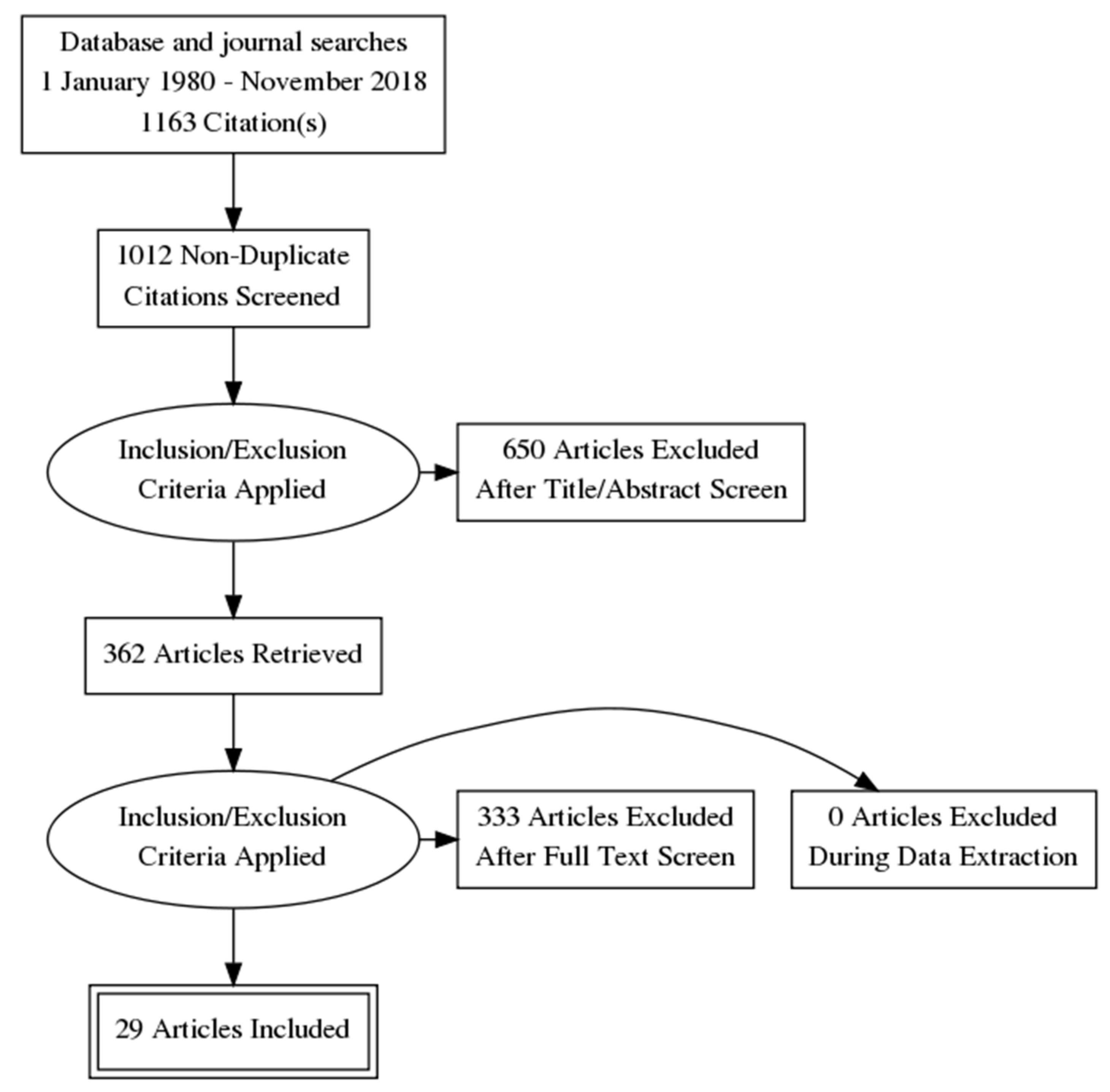
2.1. Search Strategy
- English: Medline, PsychINFO, Google Scholar, and CINAL.
- Chinese: China National Knowledge Infrastructure Database (CNKI) and Wanfang Database.
- Korean: the Korean Studies Information Service System (KISS), DBPIA, Korea Institute of Science and Technology Information, Research Information Service System (RISS), Korea Med, Korean Medical Database (KM base), and Oriental Medicine Advanced Searching Integrated System (OASIS).
2.2. Eligibility Criteria
- Usual care: This varies depending on geographical location and patient preference and for many participants is likely to incorporate SSRI or SNRI classes of anti-depressant medication;
- Sham acupuncture or placebo acupuncture, which could consist of any of the following:
- Invasive acupuncture control: This includes the insertion of acupuncture needles into either ‘non-acupuncture points’, or acupuncture points that are assumed to be unrelated to the treatment of depression. Needles may be inserted superficially or to regular depths;
- Acupuncture plus SSRI/SNRI medication: To reflect clinical practice in western countries, where clinical guidelines are unlikely to recommend acupuncture alone as an alternative to SSRI/SNRI medication or to recommend older tri-cyclic antidepressants (TCAs) [2,3], only trials comparing acupuncture as an adjunct to SSRI or SNRI medication were eligible. For clinical relevance, trials using medication that is no longer in use (such as Flupentixol/melitracen) were not eligible;
- Psychological intervention, such as cognitive behavioural therapy (CBT), psychotherapy, or counseling.
2.3. Data Extraction
- -
- Severity of depression at the end of the intervention;
- -
- Severity of depression at follow-up (short term, medium term, and long term);
- -
- Adverse events.
2.4. Risk of Bias
2.5. Acupuncture Quality
- (1)
- Population Intervention Comparator Outcome measure (PICO) reporting, study design relevance, and paradigm based differential diagnosis (items 1–6);
- (2)
- Acupuncture point selections and locations, in reference to published literature (items 7 and 9);
- (3)
- Description of the needle dimensions, needling technique, and number of treatments (items 8 and 10);
- (4)
- Acupuncturist qualification and training (item 11).
2.6. Meta-Analysis
2.7. Subgroup Analysis
- -
- Comparison between different acupuncture subtypes (manual, electro-acupuncture, and laser acupuncture)*;
- -
- Needle retention time* (<20 min versus >20 min);
- -
- Fixed versus individualised acupuncture.
3. Results
3.1. Design
3.2. Control Groups
3.3. Country
3.4. Sample Sizes
3.5. Participant Criteria
3.6. Interventions
3.6.1. Type of Acupuncture
3.6.2. Frequency of Treatment
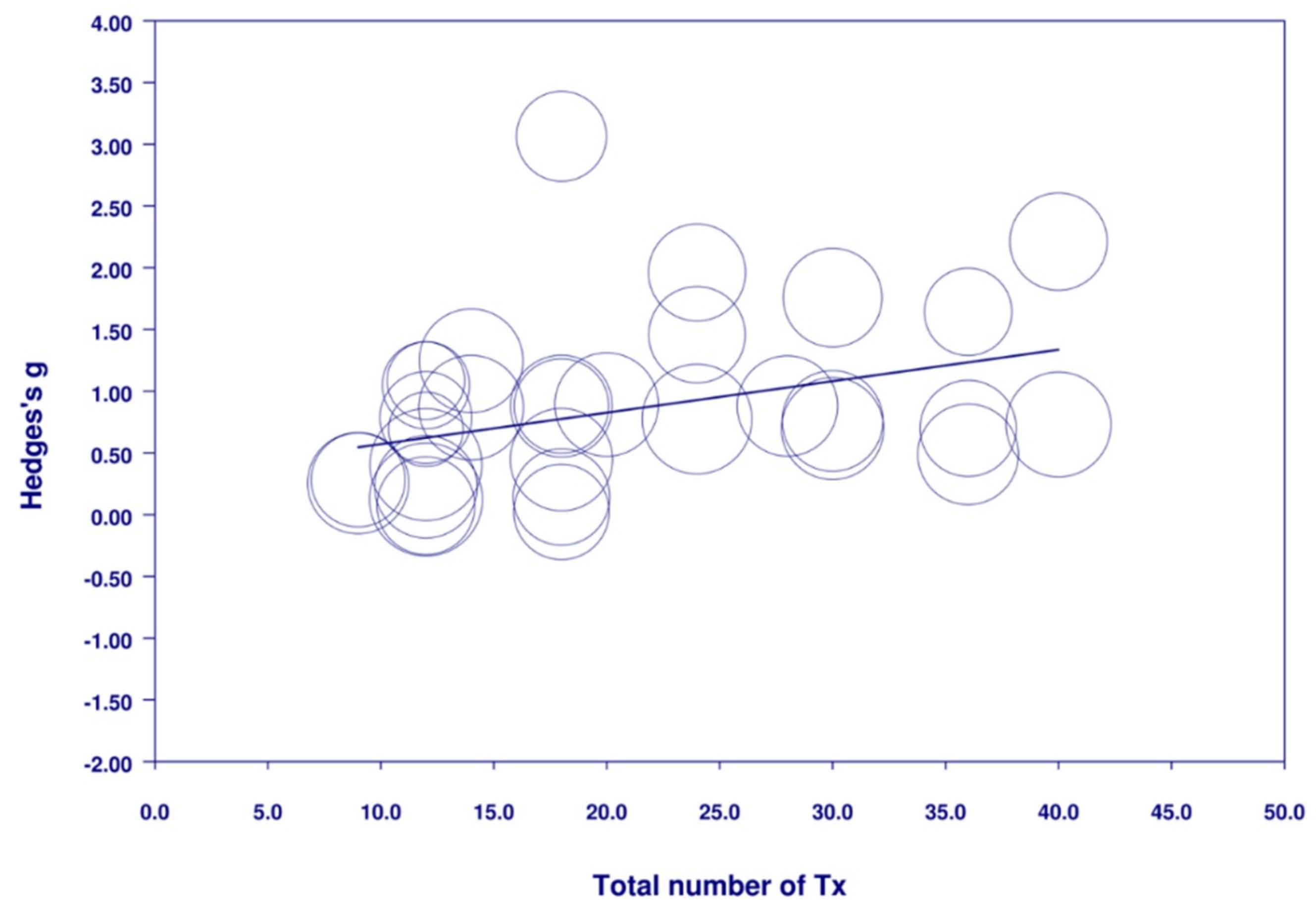
3.6.3. Total Number of Treatments
3.6.4. Duration
3.6.5. Treatment Protocol
3.6.6. Needle Retention Times
3.6.7. NICMAN Scores
3.7. Outcome Measures
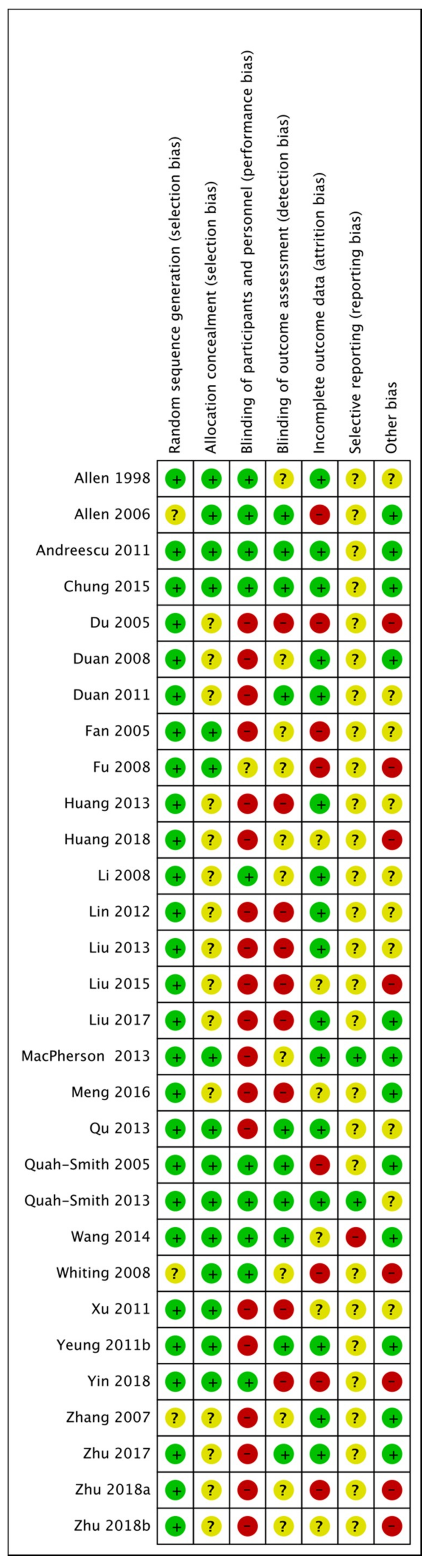
3.8. Risk of Bias in Included Studies
3.8.1. Randomization
3.8.2. Allocation
3.8.3. Blinding
3.8.4. Incomplete Outcome Data
3.8.5. Selective Reporting
3.8.6. Other Potential Sources of Bias
3.9. Acupuncture versus Usual Care
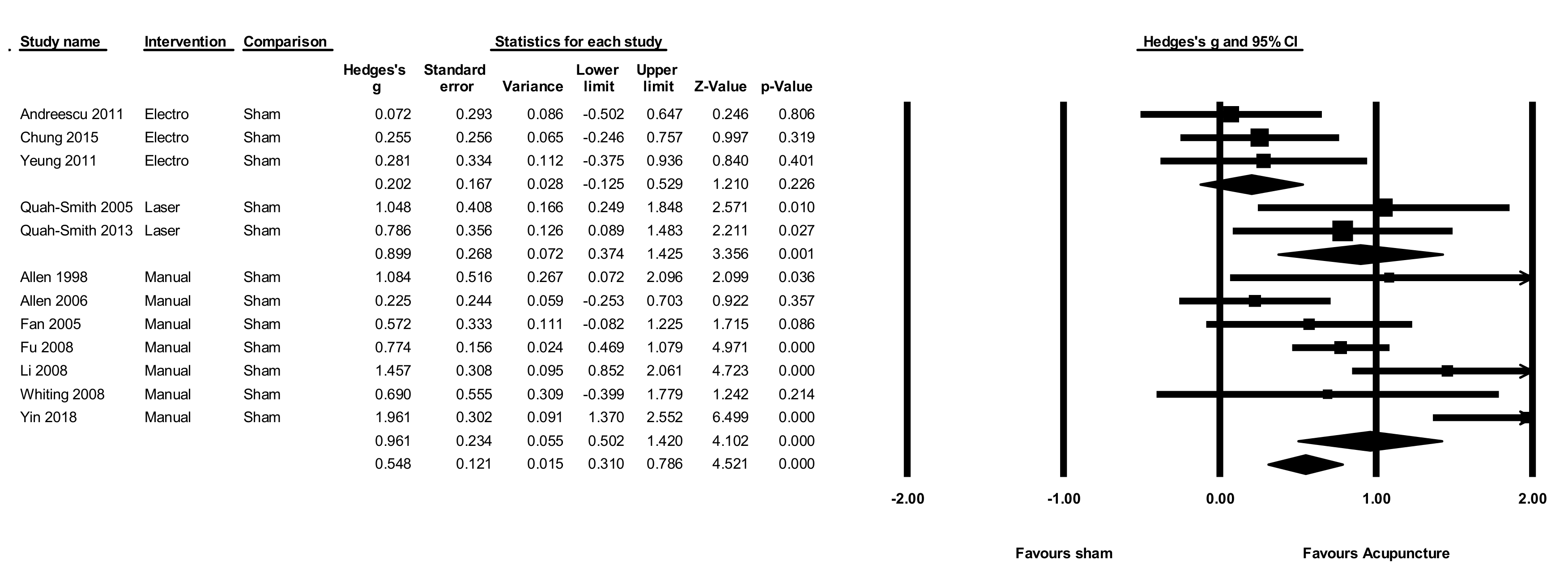
3.10. Acupuncture versus Sham
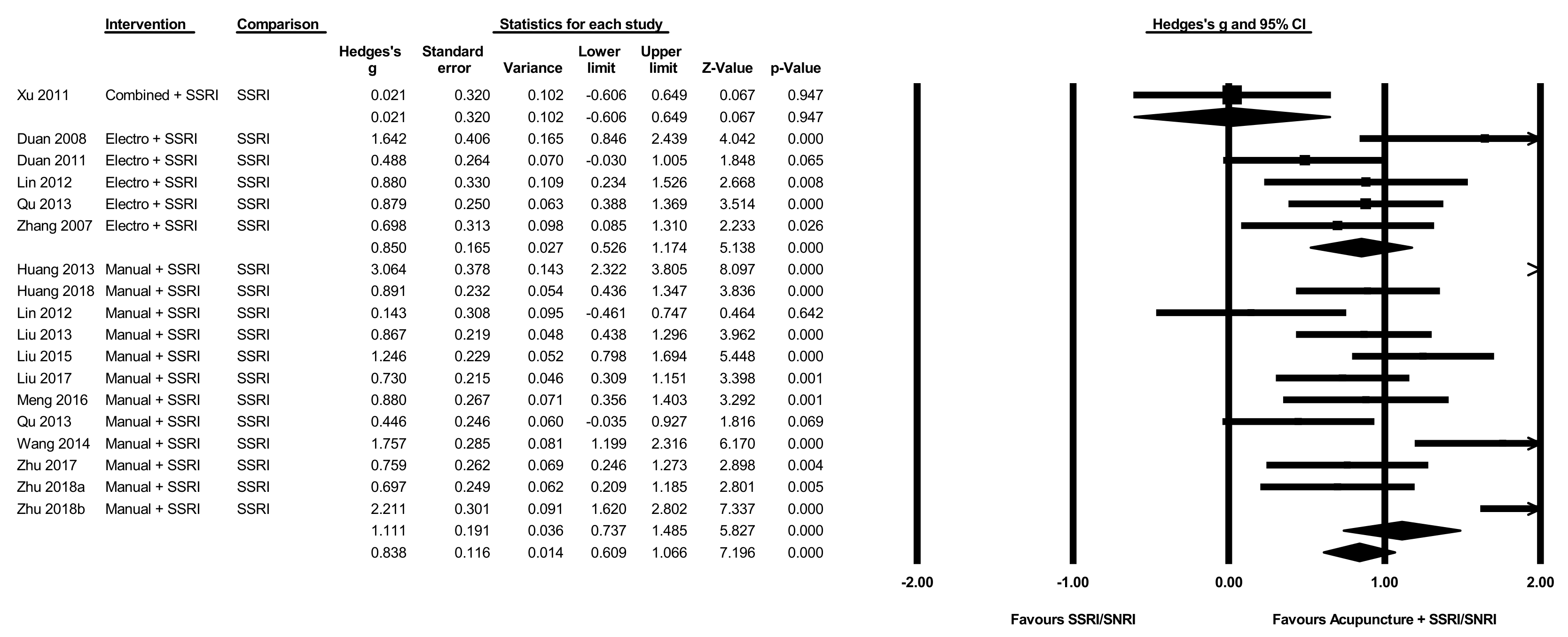
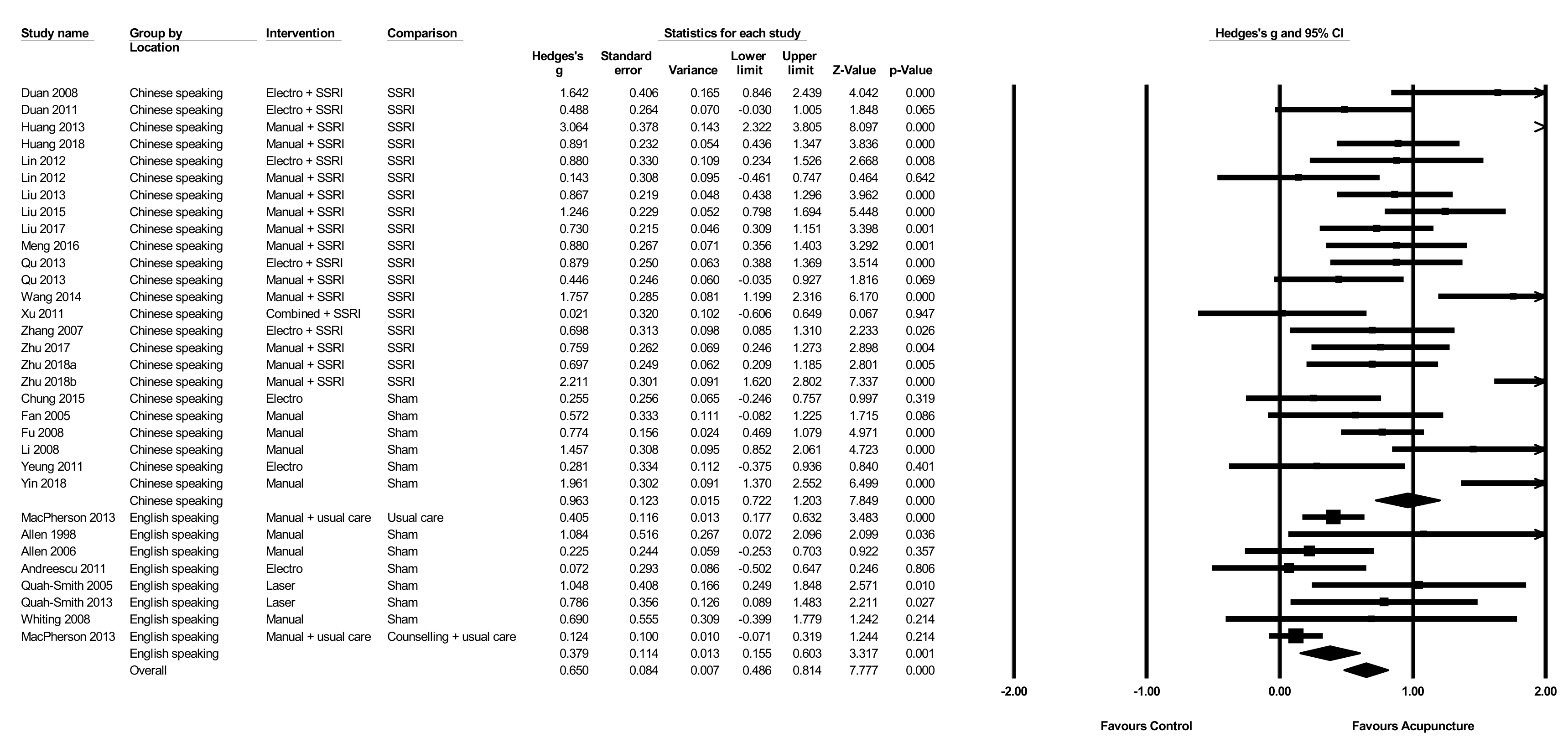
3.11. Acupuncture Plus SSRI/SNRI versus SSRI/SNRI Alone
3.12. Acupuncture versus Psychological Intervention
3.13. Adverse Events
3.14. Subgroup Analysis
3.15. Publication Bias
4. Discussion
4.1. Principal Findings
4.2. Strengths and Limitations
4.3. Implications for Research and Practice
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Hasin, D.S.; Sarvet, A.L.; Meyers, J.L.; Saha, T.D.; Ruan, W.J.; Stohl, M.; Grant, B.F. Epidemiology of adult DSM-5 major depressive disorder and its specifiers in the United States. JAMA Psychiatry 2018, 75, 336–346. [Google Scholar] [CrossRef] [PubMed]
- Malhi, G.S.; Bassett, D.; Boyce, P.; Bryant, R.; Fitzgerald, P.B.; Fritz, K.; Hopwood, M.; Lyndon, B.; Mulder, R.; Murray, G.; et al. Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for mood disorders. Aust. N. Z. J. Psychiatry 2015, 49, 1087–1206. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Health and Care Excellence. Depression in Adults: Recognition and Management (NICE Clinical Guideline 30); NICE: London, UK, 2009. [Google Scholar]
- Kessler, R.C.; Soukup, J.; Davis, R.B.; Foster, D.F.; Wilkey, S.A.; Van Rompay, M.I.; Eisenberg, D.M. The use of complementary and alternative therapies to treat anxiety and depression in the United States. Am. J. Psychiatry 2001, 158, 289–294. [Google Scholar] [CrossRef] [PubMed]
- Hansen, A.H.; Kristoffersen, A.E. The use of CAM providers and psychiatric outpatient services in people with anxiety/depression: A cross-sectional survey. BMC Complement. Altern. Med. 2016, 16, 461. [Google Scholar] [CrossRef] [PubMed]
- Druss, B.G.; Rosenheck, R.A. Use of practitioner-based complementary therapies by persons reporting mental conditions in the United States. Arch. Gen. Psychiatry 2000, 57, 708–714. [Google Scholar] [CrossRef] [PubMed]
- Robinson, N.; Lorenc, A.; Ding, W.; Jia, J.; Bovey, M.; Wang, X.M. Exploring practice characteristics and research priorities of practitioners of traditional acupuncture in China and the EU-A survey. J. Ethnopharmacol. 2012, 140, 604–613. [Google Scholar] [CrossRef] [PubMed]
- Hopton, A.K.; Curnoe, S.; Kanaan, M.; MacPherson, H. Acupuncture in practice: Mapping the providers, the patients and the settings in a national cross-sectional survey. BMJ Open 2012, 2, e000456. [Google Scholar] [CrossRef]
- Hou, Z.; Jiang, W.; Yin, Y.; Zhang, Z.; Yuan, Y. The Current Situation on Major Depressive Disorder in China: Research on Mechanisms and Clinical Practice. Neurosci. Bull. 2016, 32, 389–397. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, Y.; Jiang, H.; Meng, H.; Li, J.; Yang, X.; Zhao, B.; Sun, Y.; Bao, T. Antidepressant Mechanism Research of Acupuncture: Insights from a Genome-Wide Transcriptome Analysis of Frontal Cortex in Rats with Chronic Restraint Stress. Evid.-Based Complementary Altern. Med. 2017, 2017, 1676808. [Google Scholar] [CrossRef]
- Leung, M.C.; Yip, K.K.; Ho, Y.S.; Siu, F.K.; Li, W.C.; Garner, B. Mechanisms underlying the effect of acupuncture on cognitive improvement: A systematic review of animal studies. J. Neuroimmune Pharmacol. 2014, 9, 492–507. [Google Scholar] [CrossRef]
- Armour, M.; Smith, C.A. Treating primary dysmenorrhoea with acupuncture: A narrative review of the relationship between acupuncture ‘dose’ and menstrual pain outcomes. Acupunct. Med. 2016, 34, 416–424. [Google Scholar] [CrossRef] [PubMed]
- White, A.; Cummings, M.; Barlas, P.; Cardini, F.; Filshie, J.; Foster, N.E.; Lundeberg, T.; Stener-Victorin, E.; Witt, C. Defining an adequate dose of acupuncture using a neurophysiological approach—A narrative review of the literature. Acupunct. Med. 2008, 26, 111–120. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.A.; Zaslawski, C.J.; Zheng, Z.; Cobbin, D.; Cochrane, S.; Lenon, G.B.; Loyeung, B.; Meier, P.C.; Walsh, S.; Xue, C.C.; et al. Development of an Instrument to Assess the Quality of Acupuncture: Results from a Delphi Process. J. Altern. Complementary Med. 2011, 17, 441–452. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.A.; Armour, M.; Shewamene, Z.; Tan, H.Y.; Norman, R.J.; Johnson, N.P. Acupuncture performed around the time of embryo transfer: A systematic review and meta-analysis. Reprod. BioMed. Online 2019, 38, 364–379. [Google Scholar] [CrossRef] [PubMed]
- Armour, M.; Dahlen, H.G.; Zhu, X.; Farquhar, C.; Smith, C.A. The role of treatment timing and mode of stimulation in the treatment of primary dysmenorrhea with acupuncture: An exploratory randomised controlled trial. PLoS ONE 2017, 12, e0180177. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.-J.; Kung, Y.-Y.; Kuo, W.-J.; Niddam, D.M.; Chou, C.-C.; Cheng, C.-M.; Yeh, T.-C.; Hsieh, J.-C.; Chiu, J.-H. Effect of acupuncture ‘dose’ on modulation of the default mode network of the brain. Acupunct. Med. 2016, 34, 425–432. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.A.; Armour, M.; Lee, M.S.; Wang, L.Q.; Hay, P.J. Acupuncture for depression. Cochrane Database Syst. Rev. 2018, 3. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-III-R; American Psychiatric Association: Washington, DC, USA, 1987. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-IV; American Psychiatric Association: Washington, DC, USA, 1994. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-5; American Psychiatric Association: Arlington, VA, USA, 2013. [Google Scholar]
- World Health Organization. ICD-10: International Statistical Classification of Diseases and Related Health Problems; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Chinese Society of Psychiatry. The Chinese Classification of Mental Disorders (CCMD-3), 3rd ed.; Shandong Science and Technology Press: Shandong, China, 2001. [Google Scholar]
- Chinese Society of Psychiatry. Classification and Diagnostic Criteria of Mental Disorders in China (CCMD-2); Hunan Medical University: Changsha, China, 1989. [Google Scholar]
- Brugha, T.S.; Bebbington, P.E.; Jenkins, R.; Meltzer, H.; Taub, N.A.; Janas, M.; Vernon, J. Cross validation of a general population survey diagnostic interview: A comparison of CIS-R with SCAN ICD-10 diagnostic categories. Psychol. Med. 1999, 29, 1029–1042. [Google Scholar] [CrossRef]
- Beck, A.T.; Steer, R.A.; Ball, R.; Ranieri, W. Comparison of Beck Depression Inventories -IA and -II in psychiatric outpatients. J. Personal. Assess. 1996, 67, 588–597. [Google Scholar] [CrossRef]
- Park, J.; White, A.; Stevinson, C.; Ernst, E.; James, M. Validating a new non-penetrating sham acupuncture device: Two randomised controlled trials. Acupunct. Med. 2002, 20, 168–174. [Google Scholar] [CrossRef]
- Streitberger, K.; Kleinhenz, J. Introducing a placebo needle into acupuncture research. Lancet 1998, 352, 364–365. [Google Scholar] [CrossRef]
- Cai, R.L.; Shen, G.M.; Wang, H.; Guan, Y.Y. Brain functional connectivity network studies of acupuncture: A systematic review on resting-state fMRI. J. Integr. Med. 2018, 16, 26–33. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.; Altman, D.G.; Gotzsche, P.C.; Juni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.; et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343. [Google Scholar] [CrossRef] [PubMed]
- Armour, M.; Smith, C.A.; Steel, K.A.; Macmillan, F. The effectiveness of self-care and lifestyle interventions in primary dysmenorrhea: A systematic review and meta-analysis. BMC Complement. Altern. Med. 2019, 19, 22. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.A.; Zaslawski, C.J.; Cochrane, S.; Zhu, X.; Zheng, Z.; Loyeung, B.; Meier, P.C.; Walsh, S.; Xue, C.C.; Zhang, A.L.; et al. Reliability of the NICMAN Scale: An Instrument to Assess the Quality of Acupuncture Administered in Clinical Trials. Evid. Based Complement. Alternat. Med. 2017, 2017, 5694083. [Google Scholar] [CrossRef] [PubMed]
- MacPherson, H.; Altman, D.G.; Hammerschlag, R.; Li, Y.; Wu, T.; White, A.; Moher, D.; Group, S.R. Revised STandards for Reporting Interventions in Clinical Trials of Acupuncture (STRICTA): Extending the CONSORT statement. Acupunct. Med. 2010, 28, 83–93. [Google Scholar] [CrossRef] [PubMed]
- Hedges, L.; Olkin, I. Statistical Methods for Meta-Analysis; Academic Press: San Diego, CA, USA, 1985. [Google Scholar]
- Lin, W.R.; Huang, Y.; Chen, J.Q.; Wang, S.X. Global improvement in agitated depression treated with the alliance therapy of acupuncture and seroxat and the observation of the quality of life. Zhongguo Zhen Jiu 2012, 32, 1063–1069. [Google Scholar] [PubMed]
- MacPherson, H.; Richmond, S.; Bland, M.; Brealey, S.; Gabe, R.; Hopton, A.; Keding, A.; Lansdown, H.; Perren, S.; Sculpher, M.; et al. Acupuncture and counselling for depression in primary care: A randomised controlled trial. PLoS Med. 2013, 10, e1001518. [Google Scholar] [CrossRef] [PubMed]
- Qu, S.S.; Huang, Y.; Zhang, Z.J.; Chen, J.Q.; Lin, R.Y.; Wang, C.Q.; Li, G.L.; Wong, H.K.; Zhao, C.H.; Pan, J.Y.; et al. A 6 week randomised controlled trial with 4 week follow up of acupuncture combined with paroxetine in patients with major depressive disorder. J. Psychiatr. Res. 2013, 47, 726–732. [Google Scholar] [CrossRef] [PubMed]
- Duan, D.M.; Tu, Y.; Chen, L.P. Assessment of effectiveness of electroacupuncture and fluoxetine for treatment of depression with physical symptoms. Zhongguo Zhen Jiu 2008, 28, 167–170. [Google Scholar] [PubMed]
- Duan, D.M.; Tu, Y.; Liao, S.; Qin, W. The relevance between symptoms and magnetic resonance imaging analysis of the hippocampus of depressed patients given electro-acupuncture combined with Fluoxetine intervention: A randomized controlled trial. Chin. J. Integr. Med. 2011, 17, 190–199. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Wang, X.J.; Wang, L.L.; Lu, S.F.; Zhu, B.M.; Xu, L. Effect of acupuncture on selective serotonin reuptake inhibitors. Chin. J. Integr. Med. 2013, 33, 1341–1344. [Google Scholar]
- Huang, Z.Y.; Chen, J.D.; Xie, B.; Xia, Y.P.; Wang, W.Q.; Su, Z.B.; Xie, Y.Y.; Tang, F.; Gu, W.J.; Yang, F.L. Clinical curative effect of Shugan Jianpi acupuncture manipulation combined with magnetic stimulation in Yintang acupoint in the treatment of depression with liver-qi stagnation and spleen deficiency type. Chin. J. Behav. Med. Brain Sci. 2018, 27, 333–337. [Google Scholar] [CrossRef]
- Liu, Y.; Feng, H.; Liu, W.J.; Mao, H.J.; Zhang, Y.H.; Hu, L.L.; Yin, Y.; Xu, L.L. Effect of acupuncture of soothing-liver and nourishing-heart method combined with venlafaxine on residual symptoms and serum monoamine neurotransmitter of depressive disorder patients. Chin. J. Gen. Pract. 2017, 15, 1378–1381. [Google Scholar] [CrossRef]
- Liu, Y.; Feng, H.; Mao, H.; Mo, Y.; Yin, Y.; Liu, W.; Song, M.; Wang, S. Impact on serum 5-HT and TH1/TH2 in patients of depressive disorder at acute stage treated with acupuncture and western medication. Chin. Acupunct. Moxibustion 2015, 35, 539–543. [Google Scholar]
- Liu, Y.; Zhang, Y.H.; Jin, M.; Liu, W.J. Study on clinical effect enhancement of acupuncture for depression with chronic pain treated with SSRI antidepressants. Chin. Acupunct. Moxibustion 2013, 13, 689–691. [Google Scholar]
- Meng, X.; Zheng, Z.; Wu, D.; Miao, Y. Observation on the clinical effect of cluster needling method on scalp acupoints of depression. Biotech. World 2016, 2, 86. [Google Scholar]
- Wang, T.; Wang, L.; Tao, W.; Chen, L. Acupuncture combined with an antidepressant for patients with depression in hospital: A pragmatic randomised controlled trial. Acupunct. Med. 2014, 32, 308–312. [Google Scholar] [CrossRef]
- Xu, L.; Wang, L.L. Clinical observation on depression treated by eletroacupuncture combined with western medicine. Chin. Acupunct. Moxibustion 2011, 31, 779–782. [Google Scholar]
- Zhang, G.J.; Shi, Z.Y.; Liu, S.; Gong, S.H.; Liu, J.Q. Clinical observation of treatment of depression by electro-acupuncture combined with paroxetine Clinical observations. Chin. J. Integr. Med. 2007, 13, 228–230. [Google Scholar] [CrossRef]
- Zhu, W.X.; Wang, J.; Wang, Q.S.; Ji, X.D.; Yuan, G.Z. Antidepressant effect of acupuncture and its influence on peripheral inflammatory cytokines. Med. J. Chin. People’s Armed Police Forces 2017, 28, 816–819. [Google Scholar] [CrossRef]
- Zhu, W.X.; Wang, J.; Wang, Q.S.; Ji, X.D.; Yuan, G.Z. Effect of acupuncture on the autonomic nervous system in patients with major depressive disorder. Lishizhen Med. Mater. Med. Res. 2018, 29, 381–383. [Google Scholar] [CrossRef]
- Zhu, Z.M.; Xu, Y.; Zeng, Y.B.; Lu, L.S.; Xu, C.W. Effect of acupuncture combined with sertraline for depression. J. Pract. Tradit. Chin. Med. 2018, 34, 175–176. [Google Scholar]
- Andreescu, C.; Glick, R.M.; Emeremni, C.A.; Houck, P.R.; Mulsant, B.H. Acupuncture for the treatment of major depressive disorder: A randomised controlled trial. J. Clin. Psychiatry 2011, 72, 1129–1135. [Google Scholar] [CrossRef]
- Chung, K.F.; Yeung, W.F.; Yu, Y.M.; Yung, K.P.; Zhang, S.P.; Zhang, Z.J.; Wong, M.-T.; Lee, W.K.; Chan, L.W. Acupuncture for residual insomnia associated with major depressive disorder: A placebo and sham controlled subject and assessor blind randomised trial. J. Clin. Psychiatry 2015, 76, 752–760. [Google Scholar] [CrossRef]
- Fan, L.; Fu, W.B.; Meng, C.R.; Zhu, X.P.; Mi, J.P.; Li, W.X.; Wen, X. Effect of acupuncture at routine acupoint and no-acupoint on depressive neurosis evaluated by Hamilton depression scale. Chin. J. Clin. Rehabil. 2005, 9, 14–16. [Google Scholar]
- Fu, W.B.; Fan, L.; Zhu, X.P.; He, Q.; Wang, L.; Zhuang, L.X.; Liu, Y.S.; Tang, C.Z.; Li, Y.W.; Meng, C.R.; et, al. Acupuncture for treatment of depressive neurosis: A multi-centred randomized controlled trial. Chin. Acupunct. Moxibustion 2008, 28, 3–6. [Google Scholar]
- Li, Y.W.; Fu, W.B.; Zhu, X.P. Clinical observation on acupuncture for depressive of 27 cases. J. Tradit. Chin. Med. 2008, 49, 431–433. [Google Scholar]
- Quah-Smith, I.; Smith, C.; Crawford, J.D.; Russell, J. Laser acupuncture for depression: A randomised double blind controlled trial using low intensity laser intervention. J. Affect. Disord. 2013, 148, 179–187. [Google Scholar] [CrossRef]
- Quah-Smith, J.I.; Tang, W.M.; Russell, J. Laser acupuncture for mild to moderate depression in a primary care setting—A randomised controlled trial. Acupunct. Med. 2005, 23, 103–111. [Google Scholar] [CrossRef]
- Whiting, M.; Leavey, G.; Scammell, A.; Au, S.; King, M. Using acupuncture to treat depression: A feasibility study. Complementary Ther. Med. 2008, 16, 87–91. [Google Scholar] [CrossRef]
- Yeung, M.F.; Chung, K.F.; Tso, K.C.; Zhang, S.P.; Zhang, Z.J.; Ho, L.M. Electroacupuncture for residual insomnia associated with major depressive disorder: A randomised controlled trial. SLEEP 2011, 34, 807–815. [Google Scholar] [CrossRef]
- Yin, P.; Ma, J.; Wu, H.G.; Xu, S.F. Clinical observation of Jie Yu Tong Fu needling for depression coupled with constipation. Shanghai J. Acupunct. Moxibustion 2018, 37, 159–164. [Google Scholar] [CrossRef]
- Allen, J.B.; Schyner, R.N.; Hitt, S.K. The efficacy of acupuncture in the treatment of major depression in women. Psychol. Sci. 1998, 9, 397–401. [Google Scholar] [CrossRef]
- Allen, J.J.; Schyner, R.N.; Chambers, A.S.; Hitt, S.K. Acupuncture for depression: A randomised controlled trial. J. Clin. Psychiatry 2006, 67, 1665–1673. [Google Scholar] [CrossRef]
- Hamilton, M. A rating scale for depression. J. Neurol. Neurosurg. Psychiatry 1960, 23, 56–62. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Cheng, Y.; Tang, Q.S. Abdominal acupuncture in treating liver-qi stagnation and spleen deficiency in the elderly with post-stroke depression: A randomized and controlled observation. Chin. J. Clin. Rehabil. Tissue Eng. Res. 2007, 11, 7791–7794. [Google Scholar]
- Du, Y.H.; Li, G.P.; Yan, H.; Zhang, X.J.; Huang, L.F. Clinical study on needling method for regulating mental activities and soothing liver for treatment of melancholia. Zhongguo Zhen Jiu 2005, 25, 151–154. [Google Scholar]
- Schulz, K.F.; Altman, D.G.; Moher, D. CONSORT 2010 statement: Updated guidelines for reporting parallel group randomized trials. Ann. Intern. Med. 2010, 152, 726–732. [Google Scholar] [CrossRef]
- Mayor, D. An exploratory review of the electroacupuncture literature: Clinical applications and endorphin mechanisms. Acupunct. Med. 2013, 31, 409–415. [Google Scholar] [CrossRef]
- Langevin, H.M.; Schnyer, R.; MacPherson, H.; Davis, R.; Harris, R.E.; Napadow, V.; Wayne, P.M.; Milley, R.J.; Lao, L.; Stener-Victorin, E.; et al. Manual and electrical needle stimulation in acupuncture research: Pitfalls and challenges of heterogeneity. J. Altern. Complement. Med. 2015, 21, 113–128. [Google Scholar] [CrossRef]
- Hopton, A.; Eldred, J.; MacPherson, H. Patients’ experiences of acupuncture and counselling for depression and comorbid pain: A qualitative study nested within a randomised controlled trial. BMJ Open 2014, 4, e005144. [Google Scholar] [CrossRef]
| Study ID | Country | Sample Size | Diagnosis for Inclusion d | Intervention | Control | Number of Treatments | Frequency of Treatment | Variation in Acupuncture Points | Total Number of Acupuncture Points (for Fixed Points Only) | Outcome Measures | NICMAN Score |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Allen 1998 [62] | USA | 17 a | DSM IV | Manual acupuncture | Invasive (Non-specific) | 12 | 2/week then 1/week | Fixed | NR c | HAMD | 21 |
| Allen 2006 [63] | USA | 74 a | DSM-IV | Manual acupuncture | Invasive (Non-specific) | 12 | 2/week then 1/week | Individualised | N/A | HAMD | 23 |
| Andreescu 2011 [52] | USA | 45 | DSM IV | Electro acupuncture | Sham | 12 | 2/week | Fixed | 2 | HAMD | 21 |
| Chung 2015 [53] | Hong Kong | 60 a | DSM IV | Electro acupuncture | Sham | 9 | 3/week | Fixed | 4 | HAMD | 19 |
| Duan 2008 [38] | China | 35 | CCMD | Electro acupuncture + Fluoxetine 20 mg | Fluoxetine 20 mg | 36 | 6/week | Semi-fixed | N/A | HAMD | 16 |
| Duan 2011 [39] | China | 60 | ICD | Electro acupuncture + Fluoxetine 20 mg | Fluoxetine 20 mg | 36 | 6/week | Semi-fixed | N/A | HAMD | 16 |
| Fan 2005 [54] | China | 39 a | CCMD-2 | Manual acupuncture | Sham | NR c | NR c | Fixed | 4 | HAMD | 7 |
| Fu 2008 [55] | China | 176 a | CCMD-2 | Manual acupuncture | Sham | 24 | 2/week | Fixed | 4 | HAMD | 14 |
| Huang 2013 [40] | China | 60 | CCMD | Manual acupuncture + Paroxetine 20–40 mg | Paroxetine 20–40 mg | 18 | 3–4/week | Fixed | 6 | HAMD | 10 |
| Huang 2018 [41] | China | 80 | ICD-10, CCMD-3 | Manual acupuncture + Paroxetine, Sertraline, Citalopram, Fluoxetine (dosage NR c) | Paroxetine, Sertraline, Citalopram, Fluoxetine (dosage NR c) | 20 | 5/week | Fixed | 6 | HAMD, SF-36, TESS | 19 |
| Li 2008 [56] | China | 52 | CCMD-2 | Manual acupuncture | Sham | 24 | 2/week | Fixed | 4 | HAMD | 12 |
| Lin 2012 [35] | China | 92 b | ICD | 1. Electro acupuncture 2. Manual acupuncture + Paroxetine (dosage NR c) | Paroxetine (dosage NR c) | 18 | 3–4/week | 1. Fixed 2. Semi-fixed | 1. 2 2. N/A | HAMD | 11 |
| Liu 2013 [44] | China | 90 | CCMD-3 | Manual Acupuncture + Fluoxetine or Paroxetine (dosage NR c) | Fluoxetine or Paroxetine (dosage NR c) | 14 | 3–4/week | Fixed | 5 | HAMD | 7 |
| Liu 2015 [43] | China | 90 | CCMD-3 | Manual acupuncture + Fluoxetine, paroxetine, citalopram 20–60 mg, sertraline 50–200 mg or fluvoxamine 50–300 mg | Fluoxetine, paroxetine, citalopram 20–60 mg, sertraline 50–200 mg or fluvoxamine 50–300 mg | 14 | 3–4/week | Semi-fixed | N/A | HAMD | 15 |
| Liu 2017 [42] | China | 91 | ICD-10 | Manual acupuncture + Venlafaxine 75–225 mg | Venlafaxine 75–225 mg | 40 | 5/week | Fixed | 8 | HAMD | 15 |
| MacPherson 2013 [36] | UK | 755 | BDI | Manual acupuncture + usual care | 1.Counseling + usual care 2. Usual care | 12 | 1/week | Individualised | N/A | PHQ-9 | 20 |
| Meng 2016 [45] | China | 60 | CCMD-3 | Manual acupuncture + Fluoxetine (2 tablets dosage NR c) | Fluoxetine (2 tablets dosage NR c) | 28 | 7/week | Semi-fixed | N/A | HAMD | 16 |
| Qu 2013 [37] | China | 160 b | ICD | 1. Electro acupuncture 2. Manual acupuncture + Paroxetine 10–40 mg | Paroxetine 10–40 mg | 18 | 3/week | Fixed | 7 | BDI | 19 |
| Quah-Smith 2005 [58] | Australia | 26 | BDI | Laser acupuncture | Sham | 12 | 2/week then 1/week | Individualised | N/A | HAMD | 19 |
| Quah-Smith 2013 [57] | Australia | 37 | DSM IV | Laser acupuncture | Sham | 12 | 2/week then 1/week | Fixed | 5 | HAMD | 21 |
| Wang 2014 [46] | China | 71 | ICD | Manual acupuncture + Fluoxetine 20 mg, paroxetine 20 mg or duloxetine 40 mg | Fluoxetine 20 mg, paroxetine 20 mg or duloxetine 40 mg | 30 | 5/week | Semi-fixed | N/A | HAMD | 19 |
| Whiting 2008 [59] | UK | 17 | CISR | Manual acupuncture | Sham | 12 | NRc | Semi-fixed | N/A | HAMD | 19 |
| Xu 2011 [47] | China | 40 | CCMD | Manual + Electro acupuncture combined + Citalopram, paroxetine or fluoxetine 20 mg | Citalopram, paroxetine or fluoxetine 20 mg | 18 | 3/week | Fixed | 7 | HAMD | 9 |
| Yeung 2011 [60] | Hong Kong | 39 a | DSM-IV | Electro acupuncture | Sham | 9 | 3/week | Fixed | 8 | HAMD | 17 |
| Yin 2018 [61] | China | 64 | CCMD-3, DSM-IV | Manual acupuncture | Sham | 24 | 3/week | Fixed | 10 | HAMD | 18 |
| Zhang 2007 [48] | China | 42 | CCMD | Electro acupuncture + Paroxetine 10–40 mg | Paroxetine 10–40 mg | 36 | 7/week | Semi-fixed | N/A | HAMD | 14 |
| Zhu 2017 [49] | China | 61 | CCMD-3 | Manual acupuncture + Fluoxetine, paroxetine, fluvoxamine, sertraline, citalopram, estalcitalopram (dosage NR c) | Fluoxetine, paroxetine, fluvoxamine, sertraline, citalopram, estalcitalopram (dosage NR c) | 30 | 5/week | Semi-fixed | N/A | HAMD | 19 |
| Zhu 2018 [50] | China | 67 | CCMD-3 | Manual acupuncture + SSRI (Type and dosage NR c) | SSRI (Type and dosage NR c) | 30 | 5/week | Semi-fixed | N/A | HAMD | 20 |
| Zhu 2018 [51] | China | 70 | ICD-10 | Manual acupuncture + Sertraline (dosage NR c) | Sertraline (dosage NR c) | 40 | 5/week | Semi-fixed | N/A | HAMD | 21 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Armour, M.; Smith, C.A.; Wang, L.-Q.; Naidoo, D.; Yang, G.-Y.; MacPherson, H.; Lee, M.S.; Hay, P. Acupuncture for Depression: A Systematic Review and Meta-Analysis. J. Clin. Med. 2019, 8, 1140. https://doi.org/10.3390/jcm8081140
Armour M, Smith CA, Wang L-Q, Naidoo D, Yang G-Y, MacPherson H, Lee MS, Hay P. Acupuncture for Depression: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2019; 8(8):1140. https://doi.org/10.3390/jcm8081140
Chicago/Turabian StyleArmour, Mike, Caroline A. Smith, Li-Qiong Wang, Dhevaksha Naidoo, Guo-Yan Yang, Hugh MacPherson, Myeong Soo Lee, and Phillipa Hay. 2019. "Acupuncture for Depression: A Systematic Review and Meta-Analysis" Journal of Clinical Medicine 8, no. 8: 1140. https://doi.org/10.3390/jcm8081140
APA StyleArmour, M., Smith, C. A., Wang, L.-Q., Naidoo, D., Yang, G.-Y., MacPherson, H., Lee, M. S., & Hay, P. (2019). Acupuncture for Depression: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine, 8(8), 1140. https://doi.org/10.3390/jcm8081140







