Effects of Intraoperative Nefopam on Catheter-Related Bladder Discomfort in Patients Undergoing Robotic Nephrectomy: A Randomized Double-Blind Study
Abstract
:1. Introduction
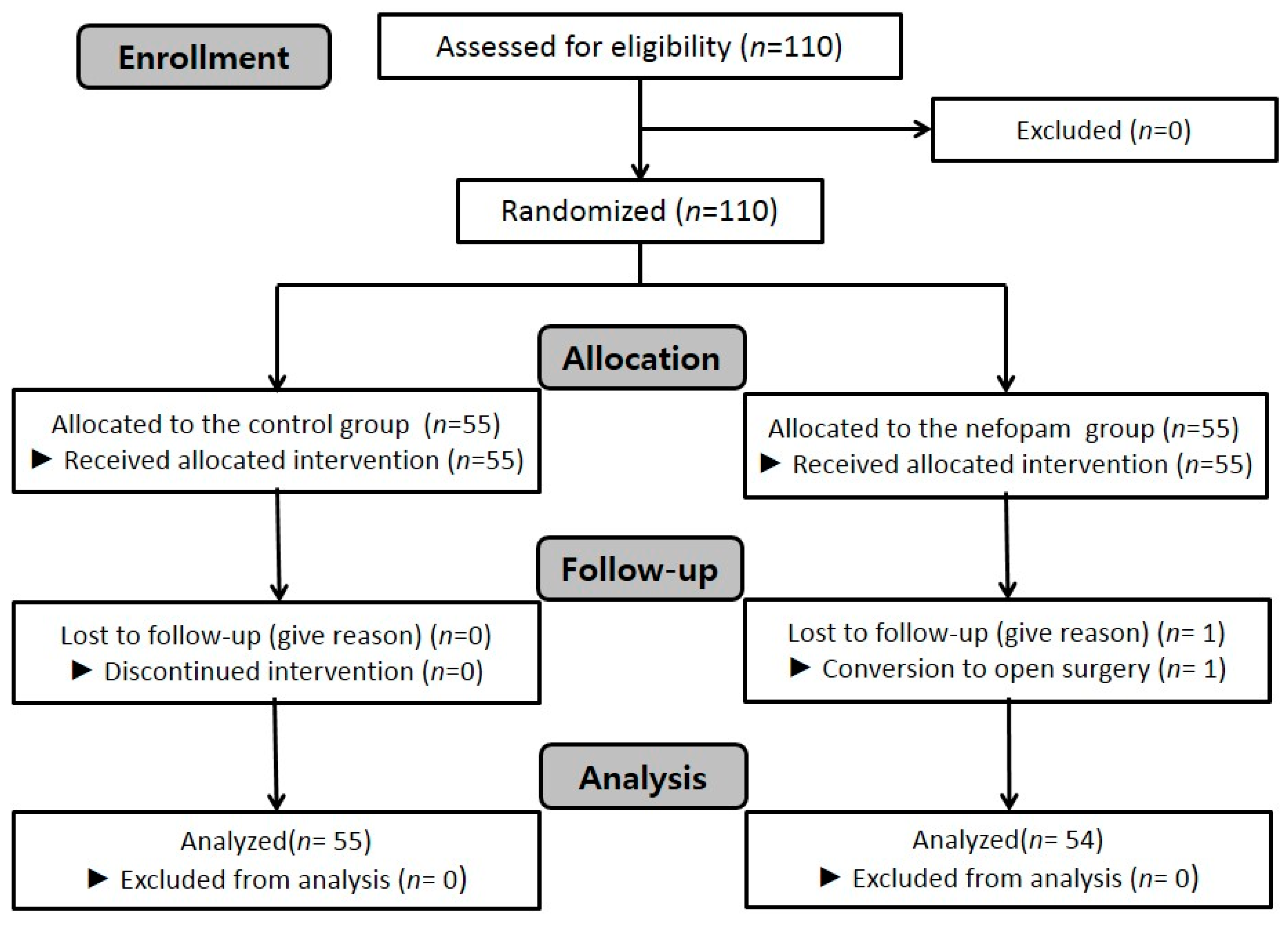
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ryu, J.H.; Hwang, J.W.; Lee, J.W.; Seo, J.S.; Park, H.P.; Oh, A.Y.; Jeon, Y.T. Efficacy of butylscopolamine for the treatment of catheter-related bladder discomfort: A prospective, randomized, placebo-controlled, double-blind study. Br. J. Anaesth. 2013, 111, 932–937. [Google Scholar] [CrossRef]
- Kim, H.C.; Lee, Y.H.; Jeon, Y.T.; Hwang, J.W.; Lim, Y.J.; Park, J.E.; Park, H.P. The effect of intraoperative dexmedetomidine on postoperative catheter-related bladder discomfort in patients undergoing transurethral bladder tumour resection: A double-blind randomised study. Eur. J. Anaesthesiol. 2015, 32, 596–601. [Google Scholar] [CrossRef]
- Wilson, M. Causes and management of indwelling urinary catheter-related pain. Br. J. Nurs. 2008, 17, 232–239. [Google Scholar] [CrossRef]
- Agarwal, A.; Dhiraaj, S.; Pawar, S.; Kapoor, R.; Gupta, D.; Singh, P.K. An evaluation of the efficacy of gabapentin for prevention of catheter-related bladder discomfort: A prospective, randomized, placebo-controlled, double-blind study. Anesth. Analg. 2007, 105, 1454–1457. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Yadav, G.; Gupta, D.; Singh, P.K.; Singh, U. Evaluation of intra-operative tramadol for prevention of catheter-related bladder discomfort: A prospective, randomized, double-blind study. Br. J. Anaesth. 2008, 101, 506–510. [Google Scholar] [CrossRef] [PubMed]
- Binhas, M.; Motamed, C.; Hawajri, N.; Yiou, R.; Marty, J. Predictors of catheter-related bladder discomfort in the post-anaesthesia care unit. Ann. Fr. Anesth. Reanim. 2011, 30, 122–125. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Raza, M.; Singhal, V.; Dhiraaj, S.; Kapoor, R.; Srivastava, A.; Gupta, D.; Singh, P.; Pandey, C.; Singh, U. The efficacy of tolterodine for prevention of catheter-related bladder discomfort: A prospective, randomized, placebo-controlled, double-blind study. Anesth. Analg. 2005, 101, 1065–1067. [Google Scholar] [CrossRef]
- Agarwal, A.; Dhiraaj, S.; Singhal, V.; Kapoor, R.; Tandon, M. Comparison of efficacy of oxybutynin and tolterodine for prevention of catheter related bladder discomfort: A prospective, randomized, placebo-controlled, double-blind study. Br. J. Anaesth. 2006, 96, 377–380. [Google Scholar] [CrossRef] [PubMed]
- Girard, P.; Chauvin, M.; Verleye, M. Nefopam analgesia and its role in multimodal analgesia: A review of preclinical and clinical studies. Clin. Exp. Pharmacol. Physiol. 2016, 43, 3–12. [Google Scholar] [CrossRef] [PubMed]
- Rowbotham, D.J.; Macintyre, P.E.; Walker, S. Clinical Pain Management; Hodder Arnold: London, UK, 2008. [Google Scholar]
- Villier, C.; Mallaret, M.P. Nefopam abuse. Ann. Pharmacother. 2002, 36, 1564–1566. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.C.; Lim, S.M.; Seo, H.; Park, H.P. Effect of glycopyrrolate versus atropine coadministered with neostigmine for reversal of rocuronium on postoperative catheter-related bladder discomfort in patients undergoing transurethral resection of bladder tumor: A prospective randomized study. J. Anesth. 2015, 29, 831–835. [Google Scholar] [CrossRef]
- Cheon, Y.W.; Kim, S.H.; Paek, J.H.; Kim, J.A.; Lee, Y.K.; Min, J.H.; Cho, H.R. Effects of nefopam on catheter-related bladder discomfort in patients undergoing ureteroscopic litholapaxy. Korean J. Anesthesiol. 2018, 71, 201–206. [Google Scholar] [CrossRef]
- Agarwal, A.; Gupta, D.; Kumar, M.; Dhiraaj, S.; Tandon, M.; Singh, P.K. Ketamine for treatment of catheter related bladder discomfort: A prospective, randomized, placebo controlled and double blind study. Br. J. Anaesth. 2006, 96, 587–589. [Google Scholar] [CrossRef]
- Hunskaar, S.; Fasmer, O.B.; Broch, O.J.; Hole, K. Involvement of central serotonergic pathways in nefopam-induced antinociception. Eur. J. Pharmacol. 1987, 138, 77–82. [Google Scholar] [CrossRef]
- Fuller, R.W.; Snoddy, H.D. Evaluation of nefopam as a monoamine uptake inhibitor in vivo in mice. Neuropharmacology 1993, 32, 995–999. [Google Scholar] [CrossRef]
- Fernandez-Sanchez, M.T.; Diaz-Trelles, R.; Groppetti, A.; Manfredi, B.; Brini, A.T.; Biella, G.; Sotgiu, M.L.; Novelli, A. Novel effect of nefopam preventing cGMP increase, oxygen radical formation and neuronal death induced by veratridine. Neuropharmacology 2001, 41, 935–942. [Google Scholar] [CrossRef]
- Verleye, M.; André, N.; Heulard, I.; Gillardin, J.M. Nefopam blocks voltage-sensitive sodium channels and modulates glutamatergic transmission in rodents. Brain Res. 2004, 1013, 249–255. [Google Scholar] [CrossRef]
- Novelli, A.; Díaz-Trelles, R.; Groppetti, A.; Fernández-Sánchez, M.T. Nefopam inhibits calcium influx, cGMP formation, and NMDA receptor-dependent neurotoxicity following activation of voltage sensitive calcium channels. Amino Acids 2005, 28, 183–191. [Google Scholar] [CrossRef]
- Anderson, K.E. Pharmacology of lower urinary tract smooth muscles and penile erectile tissues. Pharmacol. Rev. 1993, 45, 253–308. [Google Scholar]
- McMahon, S.B.; Spillane, K. Brain stem influences on the parasympathetic supply to the urinary bladder of the cat. Brain Res. 1982, 234, 237–249. [Google Scholar] [CrossRef]
- De Groat, W.C. Influence of central serotonergic mechanisms on lower urinary tract function. Urology 2002, 59, 30–36. [Google Scholar] [CrossRef]
- Maggi, C.A.; Borsini, F.; Lecci, A.; Giuliani, S.; Meli, P.; Gragnani, L.; Meli, A. Effect of acute or chronic administration of imipramine on spinal and supraspinal micturition reflexes in rats. J. Pharmacol. Exp. 1989, 248, 278–285. [Google Scholar]
- Sillen, U.; Rubenson, A.; Hjalmas, K. On the localization and mediation of the centrally induced hyperactive urinary bladder response to L-dopa in the rat. Acta Physiol. Scand. 1981, 112, 137–140. [Google Scholar] [CrossRef] [PubMed]
- Bhattu, A.S.; Ganpule, A.; Sabnis, R.B.; Murali, V.; Mishra, S.; Desai, M. Robot-assisted laparoscopic donor nephrectomy vs standard laparoscopic donor nephrectomy: A prospective randomized comparative study. J. Endourol. 2015, 29, 1334–1340. [Google Scholar] [CrossRef] [PubMed]
- Na, H.S.; Oh, A.Y.; Koo, B.W.; Lim, D.J.; Ryu, J.H.; Han, J.W. Preventive Analgesic Efficacy of Nefopam in Acute and Chronic Pain After Breast Cancer Surgery: A Prospective, Double-Blind, and Randomized Trial. Medicine 2016, 95, e3705. [Google Scholar] [CrossRef]
| Control Group (n = 55) | Nefopam Group (n = 54) | |
|---|---|---|
| Age (year) | 51.8 ± 11.7 | 52.6 ± 12.0 |
| Height (cm) | 172.0 ± 7.0 | 171.8 ± 6.0 |
| Weight (kg) | 76.5 ± 11.1 | 74.7 ± 11.5 |
| Body mass index | 25.9 ± 3.0 | 25.3 ± 3.4 |
| Operation time (min) | 141.7 ± 42.0 | 143.9 ± 46.2 |
| Control Group (n = 55) | Nefopam Group (n = 54) | 95% CI of the Difference | p-Value | |
|---|---|---|---|---|
| The severity of CRBD after operation | ||||
| 20 min | 4.8 ± 1.3 | 4.1 ± 0.8 | 4.3 to 4.7 | 0.001 |
| 1 h | 3.5 ± 1.2 | 2.3 ± 1.0 | 2.7 to 3.2 | <0.001 |
| 2 h | 2.7 ± 0.8 | 1.6 ± 0.8 | 2.0 to 2.4 | <0.001 |
| 6 h | 2.5 ± 1.0 | 1.3 ± 0.6 | 1.7 to 2.1 | <0.001 |
| Postoperative pain | ||||
| 20 min | 6.8 ± 0.8 | 6.2 ± 0.9 | 6.4 to 6.7 | 0.001 |
| 1 h | 5.3 ± 1.4 | 4.1 ± 1.5 | 4.4 to 5.0 | <0.001 |
| 2 h | 4.7 ± 1.1 | 3.5 ± 1.0 | 3.9 to 4.4 | <0.001 |
| 6 h | 4.4 ± 1.2 | 3.3 ± 1.3 | 3.6 to 4.1 | <0.001 |
| Control Group (n = 55) | Nefopam Group (n = 54) | p-Value | |
|---|---|---|---|
| The use of rescue analgesics after operation | |||
| 20 min | 55 (100%) | 49 (90.7%) | 0.027 |
| 1 h | 29 (52.7%) | 30 (55.6%) | 0.459 |
| 2 h | 33 (60.0%) | 20 (37.0%) | 0.013 |
| 6 h | 29 (52.7%) | 4 (7.4%) | 0.000 |
| PONV | 2 (3.6%) | 2 (3.7%) | 0.985 |
| Side effects | 0 (0.0%) | 0 (0.0%) | 1.000 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
In, C.-B.; Jeon, Y.-T.; Oh, A.-Y.; Jin, S.-J.; Park, B.-S.; Choi, E.-S. Effects of Intraoperative Nefopam on Catheter-Related Bladder Discomfort in Patients Undergoing Robotic Nephrectomy: A Randomized Double-Blind Study. J. Clin. Med. 2019, 8, 519. https://doi.org/10.3390/jcm8040519
In C-B, Jeon Y-T, Oh A-Y, Jin S-J, Park B-S, Choi E-S. Effects of Intraoperative Nefopam on Catheter-Related Bladder Discomfort in Patients Undergoing Robotic Nephrectomy: A Randomized Double-Blind Study. Journal of Clinical Medicine. 2019; 8(4):519. https://doi.org/10.3390/jcm8040519
Chicago/Turabian StyleIn, Chi-Bum, Young-Tae Jeon, Ah-Young Oh, Se-Jong Jin, Byeong-Seon Park, and Eun-Su Choi. 2019. "Effects of Intraoperative Nefopam on Catheter-Related Bladder Discomfort in Patients Undergoing Robotic Nephrectomy: A Randomized Double-Blind Study" Journal of Clinical Medicine 8, no. 4: 519. https://doi.org/10.3390/jcm8040519
APA StyleIn, C.-B., Jeon, Y.-T., Oh, A.-Y., Jin, S.-J., Park, B.-S., & Choi, E.-S. (2019). Effects of Intraoperative Nefopam on Catheter-Related Bladder Discomfort in Patients Undergoing Robotic Nephrectomy: A Randomized Double-Blind Study. Journal of Clinical Medicine, 8(4), 519. https://doi.org/10.3390/jcm8040519




