Repetitive Transcranial Magnetic Stimulation Therapy (rTMS) for Endometriosis Patients with Refractory Pelvic Chronic Pain: A Pilot Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethics Approval
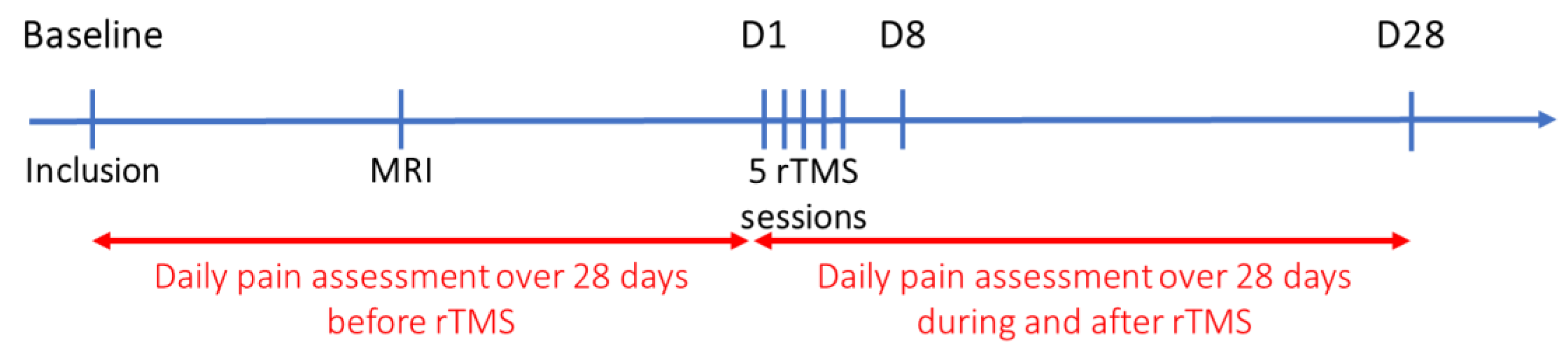
2.2. Design of The Study
2.3. Patient Selection
2.4. Evaluation Criteria
2.5. Experimental Procedure
2.6. Statistical Analyses
2.7. Ethical and Legal Considerations
3. Results
3.1. Feasability
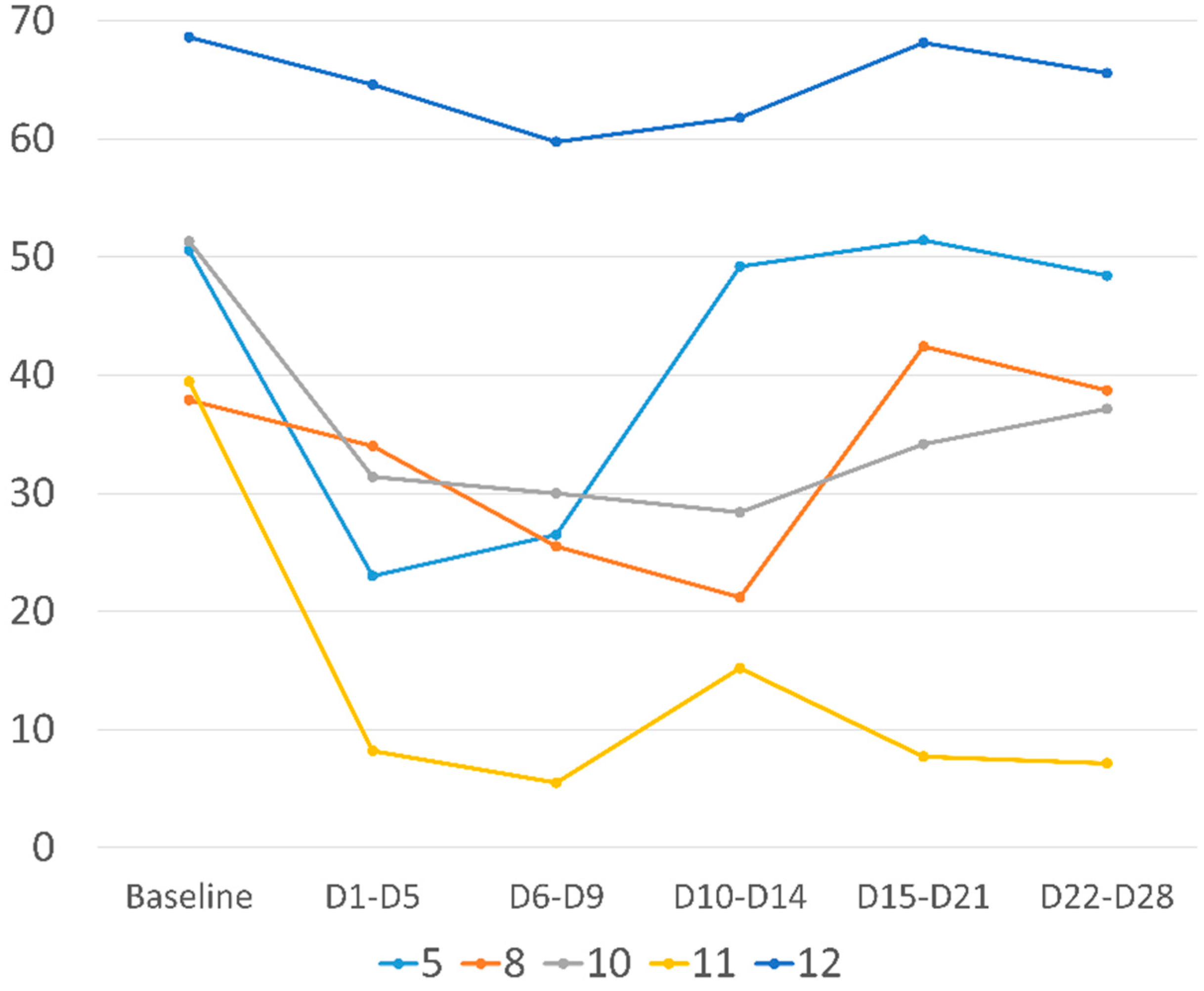
3.2. Impact on Pain
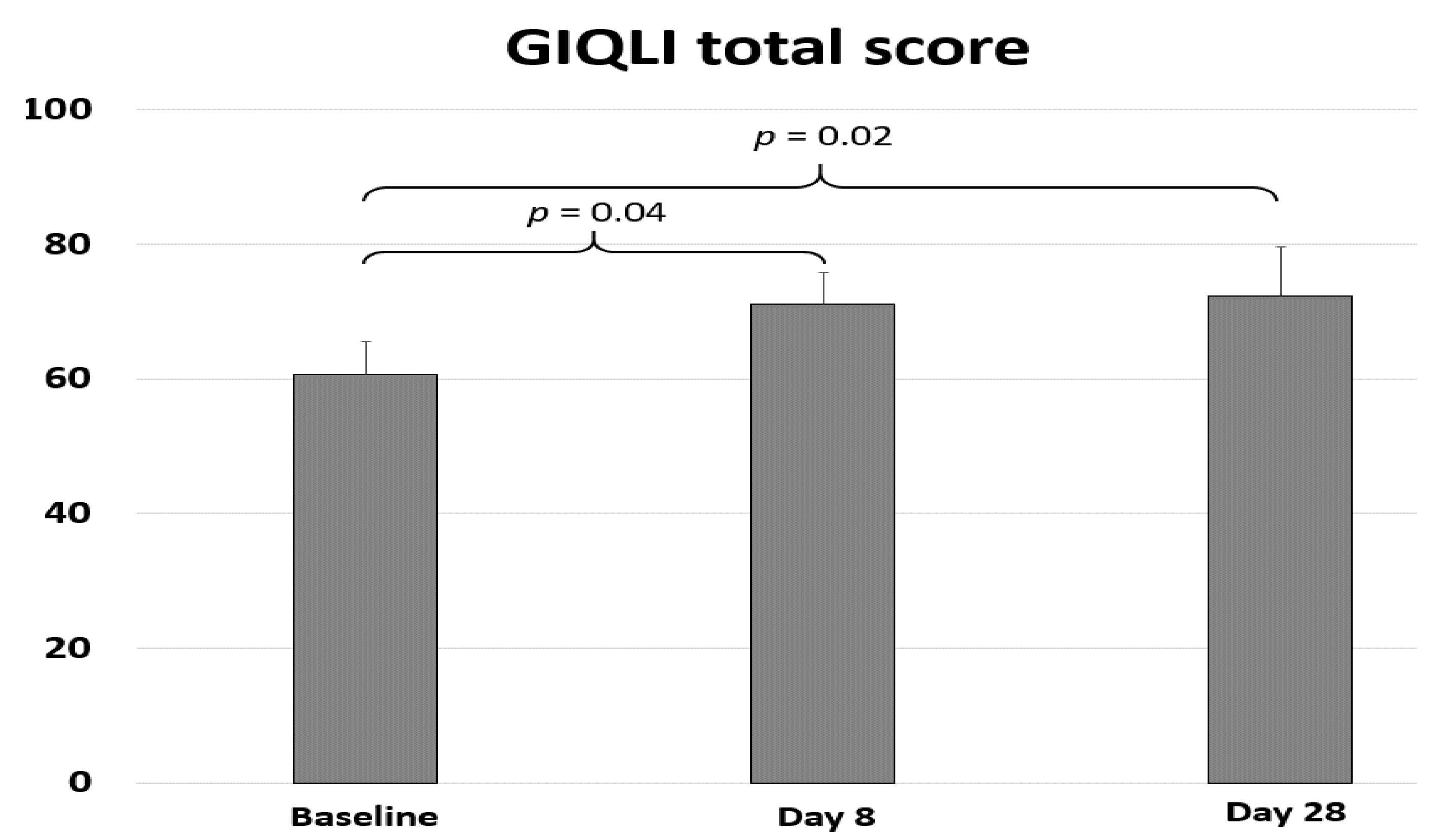
3.3. Patient Global Impression of Change and Quality of Life
4. Discussion
5. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Crosignani, P.; Olive, D.; Bergqvist, A.; Luciano, A. Advances in the management of endometriosis: An update for clinicians. Hum. Reprod. Update 2006, 12, 179–189. [Google Scholar] [CrossRef] [PubMed]
- Mowers, E.L.; Lim, C.S.; Skinner, B.; Mahnert, N.; Kamdar, N.; Morgan, D.M.; As-Sanie, S. Prevalence of Endometriosis During Abdominal or Laparoscopic Hysterectomy for Chronic Pelvic Pain. Obstet. Gynecol. 2016, 127, 1045–1053. [Google Scholar] [CrossRef] [PubMed]
- Stratton, P.; Berkley, K.J. Chronic pelvic pain and endometriosis: Translational evidence of the relationship and implications. Hum. Reprod. Update 2011, 17, 327–346. [Google Scholar] [CrossRef] [PubMed]
- Brown, J.; Farquhar, C. Endometriosis: An Overview of Cochrane Reviews. Available online: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD009590.pub2/full (accessed on 15 March 2019).
- Mira, T.A.A.; Buen, M.M.; Borges, M.G.; Yela, D.A.; Benetti-Pinto, C.L. Systematic review and meta-analysis of complementary treatments for women with symptomatic endometriosis. Int. J. Gynaecol. Obstet. 2018, 143, 2–9. [Google Scholar] [CrossRef]
- Laganà, A.S.; Condemi, I.; Retto, G.; Muscatello, M.R.A.; Bruno, A.; Zoccali, R.A.; Triolo, O.; Cedro, C. Analysis of psychopathological comorbidity behind the common symptoms and signs of endometriosis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2015, 194, 30–33. [Google Scholar] [CrossRef] [PubMed]
- Passard, A.; Attal, N.; Benadhira, R.; Brasseur, L.; Saba, G.; Sichere, P.; Perrot, S.; Januel, D.; Bouhassira, D. Effects of unilateral repetitive transcranial magnetic stimulation of the motor cortex on chronic widespread pain in fibromyalgia. Brain J. Neurol. 2007, 130, 2661–2670. [Google Scholar] [CrossRef] [PubMed]
- Boyer, L.; Dousset, A.; Roussel, P.; Dossetto, N.; Cammilleri, S.; Piano, V.; Khalfa, S.; Mundler, O.; Donnet, A.; Guedj, E. rTMS in fibromyalgia: A randomized trial evaluating QoL and its brain metabolic substrate. Neurology 2014, 82, 1231–1238. [Google Scholar] [CrossRef] [PubMed]
- Lefaucheur, J.-P.; André-Obadia, N.; Antal, A.; Ayache, S.S.; Baeken, C.; Benninger, D.H.; Cantello, R.M.; Cincotta, M.; de Carvalho, M.; De Ridder, D.; et al. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS). Clin. Neurophysiol. 2014, 125, 2150–2206. [Google Scholar] [CrossRef] [PubMed]
- Cruccu, G.; Garcia-Larrea, L.; Hansson, P.; Keindl, M.; Lefaucheur, J.-P.; Paulus, W.; Taylor, R.; Tronnier, V.; Truini, A.; Attal, N. EAN guidelines on central neurostimulation therapy in chronic pain conditions. Eur. J. Neurol. 2016, 23, 1489–1499. [Google Scholar] [CrossRef]
- Hou, W.-H.; Wang, T.-Y.; Kang, J.-H. The effects of add-on non-invasive brain stimulation in fibromyalgia: A meta-analysis and meta-regression of randomized controlled trials. Rheumatology 2016, 55, 1507–1517. [Google Scholar] [CrossRef] [PubMed]
- Fregni, F.; Potvin, K.; Dasilva, D.; Wang, X.; Lenkinski, R.E.; Freedman, S.D.; Pascual-Leone, A. Clinical effects and brain metabolic correlates in non-invasive cortical neuromodulation for visceral pain. Eur. J. Pain 2011, 15, 53–60. [Google Scholar] [CrossRef]
- Melchior, C.; Gourcerol, G.; Chastan, N.; Verin, E.; Menard, J.F.; Ducrotte, P.; Leroi, A.M. Effect of transcranial magnetic stimulation on rectal sensitivity in irritable bowel syndrome: A randomized, placebo-controlled pilot study. Colorectal Dis. 2014, 16, O104–O111. [Google Scholar] [CrossRef]
- Bourdel, N.; Alves, J.; Pickering, G.; Ramilo, I.; Roman, H.; Canis, M. Systematic review of endometriosis pain assessment: How to choose a scale? Hum. Reprod. Update 2015, 21, 136–152. [Google Scholar] [CrossRef] [PubMed]
- Chauvet, P.; Auclair, C.; Mourgues, C.; Canis, M.; Gerbaud, L.; Bourdel, N. Psychometric properties of the French version of the Endometriosis Health Profile-30, a health-related quality of life instrument. J. Gynecol. Obstet. Hum. Reprod. 2017, 46, 235–242. [Google Scholar] [CrossRef] [PubMed]
- Cleeland, C.S.; Ryan, K.M. Pain assessment: Global use of the Brief Pain Inventory. Ann. Acad. Med. Singapore 1994, 23, 129–138. [Google Scholar] [PubMed]
- Spielberger, C.; Gorsuch, R.; Lushene, R.; Vagg, P.; Jacobs, G. Manual for the State-Trait Anxiety Inventory; Consulting Psychologists Press: Palo Alto, CA, USA, 1983. [Google Scholar]
- Ware, J.E.; Sherbourne, C.D. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef]
- Slim, K.; Bousquet, J.; Kwiatkowski, F.; Lescure, G.; Pezet, D.; Chipponi, J. [First validation of the French version of the Gastrointestinal Quality of Life Index (GIQLI)]. Gastroenterol. Clin. Biol. 1999, 23, 25–31. [Google Scholar]
- Beck, A.T.; Steer, R.; Brown, G. Manual for the Beck Depression Inventory-II; Psychological Corporation: San Antonio, TX, USA, 1996. [Google Scholar]
- Sullivan, M.J.L.; Bishop, S.; Pivik, J. The Pain Catastrophizing Scale: Development and validation. Psychol. Assess. 1995, 7, 524–532. [Google Scholar] [CrossRef]
- Loas, G.; Otmani, O.; Verrier, A.; Fremaux, D.; Marchand, M.P. Factor analysis of the French version of the 20-Item Toronto Alexithymia Scale (TAS-20). Psychopathology 1996, 29, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Mhalla, A.; Baudic, S.; Ciampi de Andrade, D.; Gautron, M.; Perrot, S.; Teixeira, M.J.; Attal, N.; Bouhassira, D. Long-term maintenance of the analgesic effects of transcranial magnetic stimulation in fibromyalgia. Pain 2011, 152, 1478–1485. [Google Scholar] [CrossRef]
- Lefaucheur, J.P.; Hatem, S.; Nineb, A.; Ménard-Lefaucheur, I.; Wendling, S.; Keravel, Y.; Nguyen, J.P. Somatotopic organization of the analgesic effects of motor cortex rTMS in neuropathic pain. Neurology 2006, 67, 1998–2004. [Google Scholar] [CrossRef] [PubMed]
- Andre-Obadia, N.; Magnin, M.; Simon, E.; Garcia-Larrea, L. Somatotopic effects of rTMS in neuropathic pain? A comparison between stimulation over hand and face motor areas. Eur. J. Pain 2018, 22, 707–715. [Google Scholar] [CrossRef] [PubMed]
- Nahmias, F.; Debes, C.; de Andrade, D.C.; Mhalla, A.; Bouhassira, D. Diffuse analgesic effects of unilateral repetitive transcranial magnetic stimulation (rTMS) in healthy volunteers. Pain 2009, 147, 224–232. [Google Scholar] [CrossRef]
- Moisset, X.; Goudeau, S.; Poindessous-Jazat, F.; Baudic, S.; Clavelou, P.; Bouhassira, D. Prolonged Continuous Theta-burst Stimulation is More Analgesic than “Classical” High Frequency Repetitive Transcranial Magnetic Stimulation. Brain Stimul. 2015, 8, 135–141. [Google Scholar] [CrossRef] [PubMed]
- De Andrade, D.C.; Mhalla, A.; Adam, F.; Texeira, M.J.; Bouhassira, D. Neuropharmacological basis of rTMS-induced analgesia: The role of endogenous opioids. Pain 2011, 152, 320–326. [Google Scholar] [CrossRef]
- Morris, S.B.; DeShon, R.P. Combining effect size estimates in meta-analysis with repeated measures and independent-groups designs. Psychol. Methods 2002, 7, 105–125. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; L. Erlbaum Associates: Mahwah, NJ, USA, 1988. [Google Scholar]
- Hodaj, H.; Payen, J.-F.; Lefaucheur, J.-P. Therapeutic impact of motor cortex rTMS in patients with chronic neuropathic pain even in the absence of an analgesic response. A case report. Neurophysiol. Clin. 2018, 48, 303–308. [Google Scholar] [CrossRef] [PubMed]
- Mease, P.J.; Spaeth, M.; Clauw, D.J.; Arnold, L.M.; Bradley, L.A.; Russell, I.J.; Kajdasz, D.K.; Walker, D.J.; Chappell, A.S. Estimation of minimum clinically important difference for pain in fibromyalgia. Arthritis Care Res. 2011, 63, 821–826. [Google Scholar] [CrossRef]
- Wong, K.; Zeng, L.; Zhang, L.; Bedard, G.; Wong, E.; Tsao, M.; Barnes, E.; Danjoux, C.; Sahgal, A.; Holden, L.; et al. Minimal clinically important differences in the brief pain inventory in patients with bone metastases. Support. Care Cancer 2013, 21, 1893–1899. [Google Scholar] [CrossRef] [PubMed]
- Raman, S.; Ding, K.; Chow, E.; Meyer, R.M.; van der Linden, Y.M.; Roos, D.; Hartsell, W.F.; Hoskin, P.; Wu, J.S.Y.; Nabid, A.; et al. Minimal clinically important differences in the EORTC QLQ-C30 and brief pain inventory in patients undergoing re-irradiation for painful bone metastases. Qual. Life Res. 2018, 27, 1089–1098. [Google Scholar] [CrossRef]
- Quesada, C.; Pommier, B.; Fauchon, C.; Bradley, C.; Créac’h, C.; Vassal, F.; Peyron, R. Robot-Guided Neuronavigated Repetitive Transcranial Magnetic Stimulation (rTMS) in Central Neuropathic Pain. Arch. Phys. Med. Rehabil. 2018, 99, 2203.e1–2215.e1. [Google Scholar] [CrossRef]
- Bourdel, N.; Chauvet, P.; Billone, V.; Douridas, G.; Fauconnier, A.; Gerbaud, L.; Canis, M. Systematic review of quality of life measures in patients with endometriosis. PLoS ONE 2019, 14, e0208464. [Google Scholar] [CrossRef] [PubMed]
- Shi, H.-Y.; Lee, K.-T.; Lee, H.-H.; Uen, Y.-H.; Na, H.-L.; Chao, F.-T.; Chiu, C.-C. The minimal clinically important difference in the Gastrointestinal Quality-of-Life Index after cholecystectomy. Surg. Endosc. 2009, 23, 2708–2712. [Google Scholar] [CrossRef] [PubMed]
- Ahdab, R.; Ayache, S.S.; Brugières, P.; Goujon, C.; Lefaucheur, J.-P. Comparison of “standard” and “navigated” procedures of TMS coil positioning over motor, premotor and prefrontal targets in patients with chronic pain and depression. Neurophysiol. Clin. 2010, 40, 27–36. [Google Scholar] [CrossRef] [PubMed]
- Baptista, A.F.; Fernandes, A.M.B.L.; Sá, K.N.; Okano, A.H.; Brunoni, A.R.; Lara-Solares, A.; Jreige Iskandar, A.; Guerrero, C.; Amescua-García, C.; Kraychete, D.C.; et al. Latin American and Caribbean consensus on noninvasive central nervous system neuromodulation for chronic pain management (LAC2-NIN-CP). Pain Rep. 2019, 4, e692. [Google Scholar] [CrossRef]
- Moisset, X.; Lefaucheur, J.-P. Non pharmacological treatment for neuropathic pain: Invasive and non-invasive cortical stimulation. Rev. Neurol. 2019, 175, 51–58. [Google Scholar] [CrossRef]
- Moisset, X.; de Andrade, D.C.; Bouhassira, D. From pulses to pain relief: An update on the mechanisms of rTMS-induced analgesic effects. Eur. J. Pain 2016, 20, 689–700. [Google Scholar] [CrossRef]
- McClintock, S.M.; Reti, I.M.; Carpenter, L.L.; McDonald, W.M.; Dubin, M.; Taylor, S.F.; Cook, I.A.; O’Reardon, J.; Husain, M.M.; Wall, C.; et al. Consensus Recommendations for the Clinical Application of Repetitive Transcranial Magnetic Stimulation (rTMS) in the Treatment of Depression. J. Clin. Psychiatry 2018, 79, 16cs10905. [Google Scholar] [CrossRef]
- André-Obadia, N.; Magnin, M.; Garcia-Larrea, L. On the importance of placebo timing in rTMS studies for pain relief. Pain 2011, 152, 1233–1237. [Google Scholar] [CrossRef]
- Pommier, B.; Créac’h, C.; Beauvieux, V.; Nuti, C.; Vassal, F.; Peyron, R. Robot-guided neuronavigated rTMS as an alternative therapy for central (neuropathic) pain: Clinical experience and long-term follow-up. Eur. J. Pain 2016, 20, 907–916. [Google Scholar] [CrossRef] [PubMed]
| Age | Pain Treatment | Mean Baseline Pain | Pain at D8 | Pain Variation | PGIC at D8 | Pain at D28 | |
|---|---|---|---|---|---|---|---|
| 1 | 49 | Tramadol | 53 | 57 | +8% | Minimally improved | 27 |
| 2 | 32 | No | 54 | 50 | −7% | No change | 60 |
| 3 | 41 | NSAID, tramadol | 40 | 40 | +1% | No change | 53 |
| 4 | 34 | No | 70 | 75 | +7% | No change | 74 |
| 5 | 26 | Morphine | 51 | 4 | −92% | Much improved | 69 |
| 6 | 48 | Acetaminophene | 54 | 53 | −3% | Minimally improved | 53 |
| 7 | 32 | Mephenesine | 50 | 50 | 0% | Minimally improved | 35 |
| 8 | 39 | No | 38 | 21 | −45% | Minimally improved | 27 |
| 9 | 52 | NSAID | 55 | 50 | −10% | Minimally improved | 50 |
| 10 | 29 | NSAID | 51 | 25 | −51% | Minimally improved | 40 |
| 11 | 40 | No | 39 | 3 | −92% | Minimally improved | 5 |
| 12 | 40 | NSAID, Acetaminophene | 69 | 58 | −15% | Minimally improved | 63 |
| Mean | 38 ± 8 | 50 ± 13 | 41 ± 22 | −18% | 9/12 improved | 46 ± 16 |
| Intensity D1 | Intensity D8 | Intensity D28 | Interference D1 | Interference D8 | Interference D28 | |
|---|---|---|---|---|---|---|
| 1 | 5.3 | 4.8 | 3.8 | 8.0 | 2.3 | 2.6 |
| 2 | 5.0 | 3.8 | 6.5 | 8.6 | 3.6 | 8.9 |
| 3 | 7.0 | 6.3 | 5.8 | 7.9 | 7.1 | 6.3 |
| 4 | 7.0 | 4.5 | 2.5 | 6.7 | 4.4 | 3.1 |
| 5 | 4.8 | 1.8 | 3.8 | 8.3 | 4.0 | 7.1 |
| 6 | 3.3 | 3.5 | 1.0 | 5.6 | 4.1 | 0.7 |
| 7 | 5.3 | 5.3 | 5.5 | 8.3 | 5.1 | 8.1 |
| 8 | 4.0 | 2.8 | 4.0 | 6.3 | 4.6 | 4.0 |
| 9 | 4.5 | 4.8 | 4.8 | 4.0 | 6.0 | 7.9 |
| 10 | 4.5 | 3.5 | 5.0 | 4.6 | 3.0 | 0.1 |
| 11 | 3.3 | 1.5 | 2.0 | 2.0 | 1.9 | 1.7 |
| 12 | 7.3 | 7.3 | 7.3 | 4.4 | 4.4 | 4.4 |
| Mean | 5.1 ± 1.4 | 4.1 ± 1.6 | 4.3 ± 1.9 | 6.2 ± 2.1 | 4.2 ± 1.5 | 4.6 ± 3.0 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pinot-Monange, A.; Moisset, X.; Chauvet, P.; Gremeau, A.-S.; Comptour, A.; Canis, M.; Pereira, B.; Bourdel, N. Repetitive Transcranial Magnetic Stimulation Therapy (rTMS) for Endometriosis Patients with Refractory Pelvic Chronic Pain: A Pilot Study. J. Clin. Med. 2019, 8, 508. https://doi.org/10.3390/jcm8040508
Pinot-Monange A, Moisset X, Chauvet P, Gremeau A-S, Comptour A, Canis M, Pereira B, Bourdel N. Repetitive Transcranial Magnetic Stimulation Therapy (rTMS) for Endometriosis Patients with Refractory Pelvic Chronic Pain: A Pilot Study. Journal of Clinical Medicine. 2019; 8(4):508. https://doi.org/10.3390/jcm8040508
Chicago/Turabian StylePinot-Monange, Anne, Xavier Moisset, Pauline Chauvet, Anne-Sophie Gremeau, Aurélie Comptour, Michel Canis, Bruno Pereira, and Nicolas Bourdel. 2019. "Repetitive Transcranial Magnetic Stimulation Therapy (rTMS) for Endometriosis Patients with Refractory Pelvic Chronic Pain: A Pilot Study" Journal of Clinical Medicine 8, no. 4: 508. https://doi.org/10.3390/jcm8040508
APA StylePinot-Monange, A., Moisset, X., Chauvet, P., Gremeau, A.-S., Comptour, A., Canis, M., Pereira, B., & Bourdel, N. (2019). Repetitive Transcranial Magnetic Stimulation Therapy (rTMS) for Endometriosis Patients with Refractory Pelvic Chronic Pain: A Pilot Study. Journal of Clinical Medicine, 8(4), 508. https://doi.org/10.3390/jcm8040508






