Radial Artery Access for Percutaneous Cardiovascular Interventions: Contemporary Insights and Novel Approaches
Abstract
1. Introduction
2. Evidence Supporting Transradial Artery Access
3. Technical Factors and Access-Site Complications
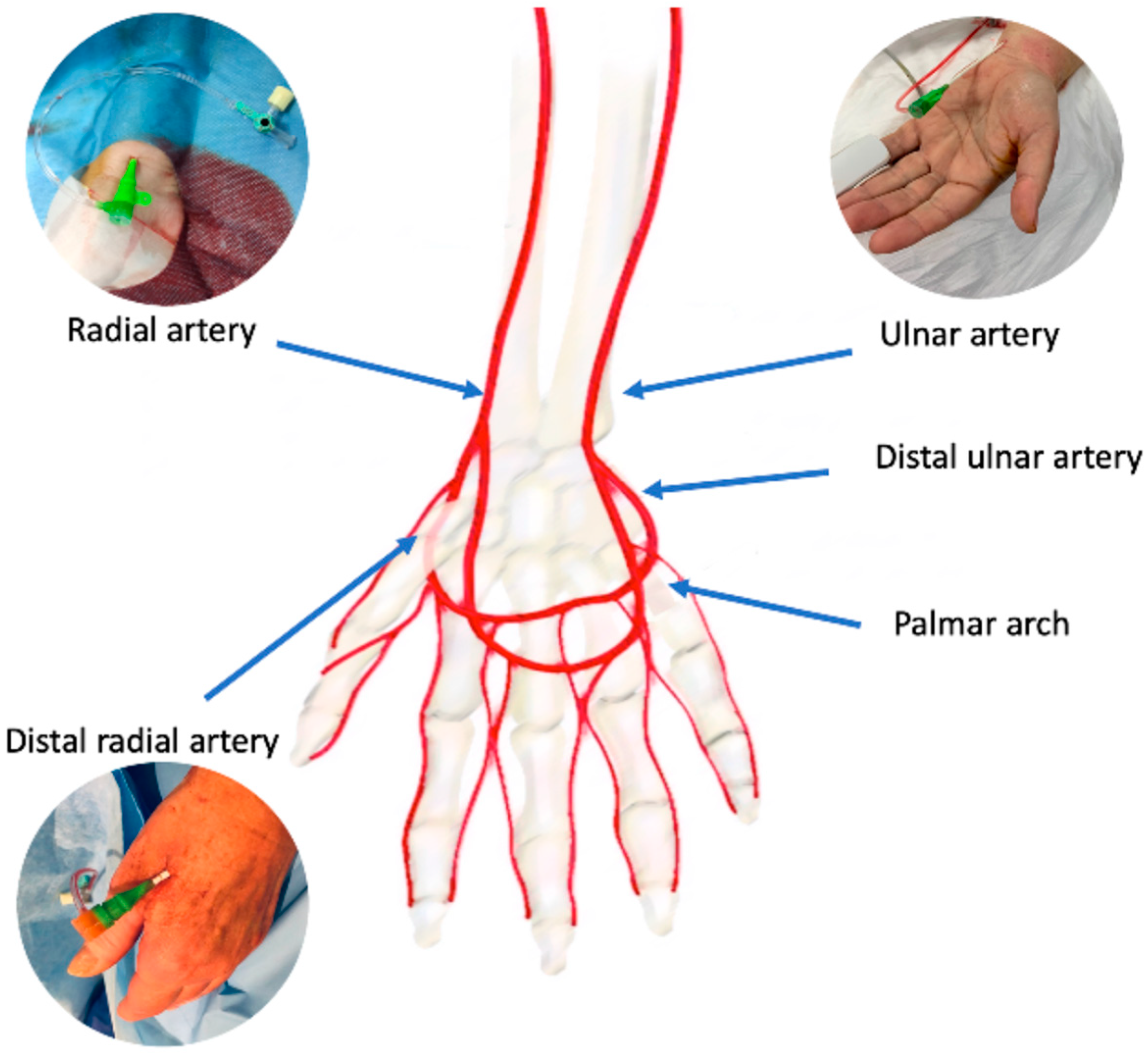
4. The Distal Radial Approach
5. Radial Artery Approach Limitations
6. The Ulnar Artery Approach
7. Radial Access for Non-Coronary Cardiovascular Interventions
8. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Radner, S. Thoracal Aortography by Catheterization from the Radial Artery: Preliminary Report of a New Technique. Acta Radiol. 1948, 29, 178–180. [Google Scholar] [CrossRef] [PubMed]
- Campeau, L. Percutaneous radial artery approach for coronary angiography. Catheter. Cardiovasc. Diagn. 1989, 16, 3–7. [Google Scholar] [CrossRef]
- Kiemeneij, F.; Jan Laarman, G. Percutaneous transradial artery approach for coronary stent implantation. Catheter. Cardiovasc. Diagn. 1993, 30, 173–178. [Google Scholar] [CrossRef]
- Chase, A.J.; Fretz, E.B.; Warburton, W.P.; Klinke, W.P.; Carere, R.G.; Pi, D.; Berry, B.; Hilton, J.D. Association of the arterial access site at angioplasty with transfusion and mortality: The M.O.R.T.A.L study (Mortality benefit Of Reduced Transfusion after percutaneous coronary intervention via the Arm or Leg). Heart 2008, 94, 1019–1025. [Google Scholar] [CrossRef] [PubMed]
- Cantor, W.J.; Mehta, S.R.; Yuan, F.; Džavík, V.; Worthley, M.; Niemelä, K.; Valentin, V.; Fung, A.; Cheema, A.N.; Widimsky, P.; et al. Radial versus femoral access for elderly patients with acute coronary syndrome undergoing coronary angiography and intervention: Insights from the RIVAL trial. Am. Heart J. 2015, 170, 880–886. [Google Scholar] [CrossRef] [PubMed]
- Romagnoli, E.; Biondi-Zoccai, G.; Sciahbasi, A.; Politi, L.; Rigattieri, S.; Pendenza, G.; Summaria, F.; Patrizi, R.; Borghi, A.; Di Russo, C.; et al. Radial Versus Femoral Randomized Investigation in ST-Segment Elevation Acute Coronary Syndrome. J. Am. Coll. Cardiol. 2012, 60, 2481–2489. [Google Scholar] [CrossRef] [PubMed]
- Bernat, I.; Horak, D.; Stasek, J.; Mates, M.; Pesek, J.; Ostadal, P.; Hrabos, V.; Dusek, J.; Koza, J.; Sembera, Z.; et al. ST-Segment Elevation Myocardial Infarction Treated by Radial or Femoral Approach in a Multicenter Randomized Clinical Trial. J. Am. Coll. Cardiol. 2014, 63, 964–972. [Google Scholar] [CrossRef]
- Valgimigli, M. Design and rationale for the Minimizing Adverse haemorrhagic events by TRansradial access site and systemic Implementation of angioX program. Am. Heart J. 2014, 168, 838–845.e6. [Google Scholar] [CrossRef]
- On Behalf of the Matrix Investigators; Valgimigli, M.; Calabrò, P.; Cortese, B.; Frigoli, E.; Garducci, S.; Rubartelli, P.; Andò, G.; Santarelli, A.; Galli, M.; et al. Scientific Foundation and Possible Implications for Practice of the Minimizing Adverse Haemorrhagic Events by Transradial Access Site and Systemic Implementation of AngioX (MATRIX) Trial. J. Cardiovasc. Trans. Res. 2014, 7, 101–111. [Google Scholar] [CrossRef]
- Valgimigli, M.; Gagnor, A.; Calabró, P.; Frigoli, E.; Leonardi, S.; Zaro, T.; Rubartelli, P.; Briguori, C.; Andò, G.; Repetto, A.; et al. Radial versus femoral access in patients with acute coronary syndromes undergoing invasive management: A randomised multicentre trial. Lancet 2015, 385, 2465–2476. [Google Scholar] [CrossRef]
- Valgimigli, M.; Frigoli, E.; Leonardi, S.; Vranckx, P.; Rothenbühler, M.; Tebaldi, M.; Varbella, F.; Calabrò, P.; Garducci, S.; Rubartelli, P.; et al. Radial versus femoral access and bivalirudin versus unfractionated heparin in invasively managed patients with acute coronary syndrome (MATRIX): Final 1-year results of a multicentre, randomised controlled trial. Lancet 2018, 392, 835–848. [Google Scholar] [CrossRef]
- Andò, G.; Capodanno, D. Radial Versus Femoral Access in Invasively Managed Patients with Acute Coronary Syndrome: A Systematic Review and Meta-analysis. Ann. Intern. Med. 2015, 163, 932. [Google Scholar] [CrossRef] [PubMed]
- Andò, G.; Capodanno, D. Radial Access Reduces Mortality in Patients with Acute Coronary Syndromes. JACC Cardiovasc. Interv. 2016, 9, 660–670. [Google Scholar] [CrossRef] [PubMed]
- Le May, M.R.; Wells, G.; So, D.Y. The safety and efficacy of femoral access vs. radial access in STEMI. In Proceedings of the ACC 2019, New Orleans, LA, USA, 18 March 2019. [Google Scholar]
- Brzezinski, M.; Luisetti, T.; London, M.J. Radial Artery Cannulation: A Comprehensive Review of Recent Anatomic and Physiologic Investigations. Anesth. Analg. 2009, 109, 1763–1781. [Google Scholar] [CrossRef]
- Barbeau, G.R.; Arsenault, F.; Dugas, L.; Simard, S.; Larivière, M.M. Evaluation of the ulnopalmar arterial arches with pulse oximetry and plethysmography: Comparison with the Allen’s test in 1010 patients. Am. Heart J. 2004, 147, 489–493. [Google Scholar] [CrossRef]
- De Rosa, S.; Passafaro, F.; Polimeni, A.; Sorrentino, S.; Indolfi, C. A novel quick and easy test for radial artery occlusion with the laser Doppler scan. JACC Cardiovasc. Interv. 2014, 7, e89–e90. [Google Scholar] [CrossRef]
- Indolfi, C.; Passafaro, F.; Sorrentino, S.; Spaccarotella, C.; Mongiardo, A.; Torella, D.; Polimeni, A.; Sabatino, J.; Curcio, A.; De Rosa, S. Hand Laser Perfusion Imaging to Assess Radial Artery Patency: A Pilot Study. J. Clin. Med. 2018, 7, 319. [Google Scholar] [CrossRef]
- Valgimigli, M.; Campo, G.; Penzo, C.; Tebaldi, M.; Biscaglia, S.; Ferrari, R. Transradial Coronary Catheterization and Intervention Across the Whole Spectrum of Allen Test Results. J. Am. Coll. Cardiol. 2014, 63, 1833–1841. [Google Scholar] [CrossRef]
- Van Leeuwen, M.A.H.; Hollander, M.R.; van der Heijden, D.J.; van de Ven, P.M.; Opmeer, K.H.M.; Taverne, Y.J.H.J.; Ritt, M.J.P.F.; Kiemeneij, F.; van Mieghem, N.M.; van Royen, N. The ACRA Anatomy Study (Assessment of Disability After Coronary Procedures Using Radial Access): A Comprehensive Anatomic and Functional Assessment of the Vasculature of the Hand and Relation to Outcome After Transradial Catheterization. Circ. Cardiovasc. Interv. 2017, 10. [Google Scholar] [CrossRef]
- van Leeuwen, M.A.H.; van der Heijden, D.J.; Hollander, M.R.; Mulder, M.J.; van de Ven, P.M.; Ritt, M.J.P.F.; Kiemeneij, F.; van Mieghem, N.M.; van Royen, N. ACRA Perfusion Study: The Impact of Transradial Intervention on Digital Hand Perfusion. Circ. Cardiovasc. Interv. 2019, 12. [Google Scholar] [CrossRef]
- Rao, S.V.; Stone, G.W. Arterial access and arteriotomy site closure devices. Nat. Rev. Cardiol. 2016, 13, 641–650. [Google Scholar] [CrossRef] [PubMed]
- Pancholy, S.B.; Sanghvi, K.A.; Patel, T.M. Radial artery access technique evaluation trial: Randomized comparison of seldinger versus modified seldinger technique for arterial access for transradial catheterization. Catheter. Cardiovasc. Interv. 2012, 80, 288–291. [Google Scholar] [CrossRef]
- Polimeni, A.; Passafaro, F.; De Rosa, S.; Sorrentino, S.; Torella, D.; Spaccarotella, C.; Mongiardo, A.; Indolfi, C. Clinical and Procedural Outcomes of 5-French versus 6-French Sheaths in Transradial Coronary Interventions. Medicine 2015, 94, e2170. [Google Scholar] [CrossRef] [PubMed]
- Rathore, S.; Stables, R.H.; Pauriah, M.; Hakeem, A.; Mills, J.D.; Palmer, N.D.; Perry, R.A.; Morris, J.L. Impact of Length and Hydrophilic Coating of the Introducer Sheath on Radial Artery Spasm During Transradial Coronary Intervention. JACC Cardiovasc. Interv. 2010, 3, 475–483. [Google Scholar] [CrossRef]
- Costa, F.; van Leeuwen, M.A.H.; Daemen, J.; Diletti, R.; Kauer, F.; van Geuns, R.-J.; Ligthart, J.; Witberg, K.; Zijlstra, F.; Valgimigli, M.; et al. The Rotterdam Radial Access Research: Ultrasound-Based Radial Artery Evaluation for Diagnostic and Therapeutic Coronary Procedures. Circ. Cardiovasc. Interv. 2016, 9. [Google Scholar] [CrossRef] [PubMed]
- Seto, A.H.; Roberts, J.S.; Abu-Fadel, M.S.; Czak, S.J.; Latif, F.; Jain, S.P.; Raza, J.A.; Mangla, A.; Panagopoulos, G.; Patel, P.M.; et al. Real-Time Ultrasound Guidance Facilitates Transradial Access. JACC Cardiovasc. Interv. 2015, 8, 283–291. [Google Scholar] [CrossRef] [PubMed]
- Bertrand, O.F.; Rao, S.V.; Pancholy, S.; Jolly, S.S.; Rodés-Cabau, J.; Larose, É.; Costerousse, O.; Hamon, M.; Mann, T. Transradial Approach for Coronary Angiography and Interventions. JACC Cardiovasc. Interv. 2010, 3, 1022–1031. [Google Scholar] [CrossRef]
- Sciahbasi, A.; Romagnoli, E.; Burzotta, F.; Trani, C.; Sarandrea, A.; Summaria, F.; Pendenza, G.; Tommasino, A.; Patrizi, R.; Mazzari, M.; et al. Transradial approach (left vs. right) and procedural times during percutaneous coronary procedures: TALENT study. Am. Heart J. 2011, 161, 172–179. [Google Scholar] [CrossRef]
- Pancholy, S.B.; Joshi, P.; Shah, S.; Rao, S.V.; Bertrand, O.F.; Patel, T.M. Effect of Vascular Access Site Choice on Radiation Exposure During Coronary Angiography. JACC Cardiovasc. Interv. 2015, 8, 1189–1196. [Google Scholar] [CrossRef]
- Sciahbasi, A.; Frigoli, E.; Sarandrea, A.; Rothenbühler, M.; Calabrò, P.; Lupi, A.; Tomassini, F.; Cortese, B.; Rigattieri, S.; Cerrato, E.; et al. Radiation Exposure and Vascular Access in Acute Coronary Syndromes. J. Am. Coll. Cardiol. 2017, 69, 2530–2537. [Google Scholar] [CrossRef]
- Sciahbasi, A.; Frigoli, E.; Sarandrea, A.; Calabrò, P.; Rubartelli, P.; Cortese, B.; Tomassini, F.; Zavalloni, D.; Tebaldi, M.; Calabria, P.; et al. Determinants of radiation dose during right transradial access: Insights from the RAD-MATRIX study. Am. Heart J. 2018, 196, 113–118. [Google Scholar] [CrossRef] [PubMed]
- Andò, G.; Costa, F.; Boretti, I.; Trio, O.; Valgimigli, M. Benefit of radial approach in reducing the incidence of acute kidney injury after percutaneous coronary intervention: A meta-analysis of 22,108 patients. Int. J. Cardiol. 2015, 179, 309–311. [Google Scholar] [CrossRef] [PubMed]
- Andò, G.; Costa, F.; Trio, O.; Oreto, G.; Valgimigli, M. Impact of vascular access on acute kidney injury after percutaneous coronary intervention. Cardiovasc. Revasc. Med. 2016, 17, 333–338. [Google Scholar] [CrossRef] [PubMed]
- Andò, G.; Cortese, B.; Russo, F.; Rothenbühler, M.; Frigoli, E.; Gargiulo, G.; Briguori, C.; Vranckx, P.; Leonardi, S.; Guiducci, V.; et al. Acute Kidney Injury After Radial or Femoral Access for Invasive Acute Coronary Syndrome Management. J. Am. Coll. Cardiol. 2017, 69, 2592–2603. [Google Scholar] [CrossRef]
- Rothenbühler, M.; Valgimigli, M.; Odutayo, A.; Frigoli, E.; Leonardi, S.; Vranckx, P.; Turturo, M.; Moretti, L.; Amico, F.; Uguccioni, L.; et al. Association of acute kidney injury and bleeding events with mortality after radial or femoral access in patients with acute coronary syndrome undergoing invasive management: Secondary analysis of a randomized clinical trial. Eur. Heart J. 2019, 40, 1226–1232. [Google Scholar] [CrossRef]
- Amato, J.J.; Solod, E.; Cleveland, R.J. A “second” radial artery for monitoring the perioperative pediatric cardiac patient. J. Pediatr. Surg. 1977, 12, 715–717. [Google Scholar] [CrossRef]
- Kiemeneij, F. Left distal transradial access in the anatomical snuffbox for coronary angiography (ldTRA) and interventions (ldTRI). EuroIntervention 2017, 13, 851–857. [Google Scholar] [CrossRef]
- Davies, R.E.; Gilchrist, I.C. Back hand approach to radial access: The snuff box approach. Cardiovasc. Revasc. Med. 2018, 19, 324–326. [Google Scholar] [CrossRef]
- Babunashvili, A.; Dundua, D. Recanalization and reuse of early occluded radial artery within 6 days after previous transradial diagnostic procedure. Catheter. Cardiovasc. Interv. 2011, 77, 530–536. [Google Scholar] [CrossRef]
- Indolfi, C.; Passafaro, F.; Mongiardo, A.; Spaccarotella, C.; Torella, D.; Sorrentino, S.; Polimeni, A.; Emanuele, V.; Curcio, A.; De Rosa, S. Delayed sudden radial artery rupture after left transradial coronary catheterization: A case report. Medicine 2015, 94, e634. [Google Scholar] [CrossRef]
- Lee, S.H. Wonju Severance Christian Hospital, Wonju, Gangwon-do, Korea, Comparison of Success Rate Between Distal Radial Approach and Radial Approach in STEMI. Available online: https://clinicaltrials.gov/ct2/show/NCT03611725 (accessed on 20 September 2019).
- Pancholy, S.; Coppola, J.; Patel, T.; Roke-Thomas, M. Prevention of radial artery occlusion-Patent hemostasis evaluation trial (PROPHET study): A randomized comparison of traditional versus patency documented hemostasis after transradial catheterization: Prevention of Radial Artery Occlusion. Catheter. Cardiovasc. Interv. 2008, 72, 335–340. [Google Scholar] [CrossRef] [PubMed]
- Pancholy, S.B.; Bernat, I.; Bertrand, O.F.; Patel, T.M. Prevention of Radial Artery Occlusion After Transradial Catheterization: The PROPHET-II Randomized Trial. JACC Cardiovasc. Interv. 2016, 9, 1992–1999. [Google Scholar] [CrossRef] [PubMed]
- Pancholy, S.B.; Patel, T.M. Effect of duration of hemostatic compression on radial artery occlusion after transradial access. Catheter. Cardiovasc. Interv. 2012, 79, 78–81. [Google Scholar] [CrossRef] [PubMed]
- Rao, S.V.; Bernat, I.; Bertrand, O.F. Remaining challenges and opportunities for improvement in percutaneous transradial coronary procedures. Eur. Heart J. 2012, 33, 2521–2526. [Google Scholar] [CrossRef]
- Wagener, J.F.; Rao, S.V. Radial artery occlusion after transradial approach to cardiac catheterization. Curr. Atheroscler. Rep. 2015, 17, 489. [Google Scholar] [CrossRef]
- Pancholy, S.B. Strategies to prevent radial artery occlusion after transradial PCI. Curr. Cardiol. Rep. 2014, 16, 505. [Google Scholar] [CrossRef]
- Spaulding, C.; Lefèvre, T.; Funck, F.; Thébault, B.; Chauveau, M.; Ben Hamda, K.; Chalet, Y.; Monségu, H.; Tsocanakis, O.; Py, A.; et al. Left radial approach for coronary angiography: Results of a prospective study. Catheter. Cardiovasc. Diagn. 1996, 39, 365–370. [Google Scholar] [CrossRef]
- Dharma, S.; Kedev, S.; Patel, T.; Kiemeneij, F.; Gilchrist, I.C. A novel approach to reduce radial artery occlusion after transradial catheterization: Postprocedural/prehemostasis intra-arterial nitroglycerin. Catheter. Cardiovasc. Interv. 2015, 85, 818–825. [Google Scholar] [CrossRef]
- Kwok, C.S.; Rashid, M.; Fraser, D.; Nolan, J.; Mamas, M. Intra-arterial vasodilators to prevent radial artery spasm: A systematic review and pooled analysis of clinical studies. Cardiovasc. Revasc. Med. 2015, 16, 484–490. [Google Scholar] [CrossRef]
- Webb, J.G.; Wood, D.A. Current status of transcatheter aortic valve replacement. J. Am. Coll. Cardiol. 2012, 60, 483–492. [Google Scholar] [CrossRef]
- Werdan, K.; Gielen, S.; Ebelt, H.; Hochman, J.S. Mechanical circulatory support in cardiogenic shock. Eur. Heart J. 2014, 35, 156–167. [Google Scholar] [CrossRef] [PubMed]
- Alaswad, K.; Menon, R.V.; Christopoulos, G.; Lombardi, W.L.; Karmpaliotis, D.; Grantham, J.A.; Marso, S.P.; Wyman, M.R.; Pokala, N.R.; Patel, S.M.; et al. Transradial approach for coronary chronic total occlusion interventions: Insights from a contemporary multicenter registry. Catheter. Cardiovasc. Interv. 2015, 85, 1123–1129. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, Y.; Moriyama, N.; Ochiai, T.; Takada, T.; Tobita, K.; Shishido, K.; Sugitatsu, K.; Yamanaka, F.; Mizuno, S.; Murakami, M.; et al. Transradial Coronary Interventions for Complex Chronic Total Occlusions. JACC Cardiovasc. Interv. 2017, 10, 235–243. [Google Scholar] [CrossRef] [PubMed]
- Gokhroo, R.; Kishor, K.; Ranwa, B.; Bisht, D.; Gupta, S.; Padmanabhan, D.; Avinash, A. Ulnar Artery Interventions Non-Inferior to Radial Approach: AJmer Ulnar ARtery (AJULAR) Intervention Working Group Study Results. J Invasive Cardiol. 2016, 28, 1–8. [Google Scholar] [PubMed]
- Liu, J.; Fu, X.-H.; Xue, L.; Wu, W.-L.; Gu, X.-S.; Li, S.-Q. A comparative study of transulnar and transradial artery access for percutaneous coronary intervention in patients with acute coronary syndrome. J. Interv. Cardiol. 2014, 27, 525–530. [Google Scholar] [CrossRef]
- Kedev, S.; Zafirovska, B.; Dharma, S.; Petkoska, D. Safety and feasibility of transulnar catheterization when ipsilateral radial access is not available. Catheter. Cardiovasc. Interv. 2014, 83, E51–E60. [Google Scholar] [CrossRef]
- Geng, W.; Fu, X.; Gu, X.; Jiang, Y.; Fan, W.; Wang, Y.; Li, W.; Xing, K.; Liu, C. Safety and feasibility of transulnar versus transradial artery approach for coronary catheterization in non-selective patients. Chin. Med. J. 2014, 127, 1222–1228. [Google Scholar]
- Deshmukh, A.R.; Kaushik, M.; Aboeata, A.; Abuzetun, J.; Burns, T.L.; Nubel, C.A.; White, M.D.; Lanspa, T.J.; Hunter, C.B.; Mooss, A.N.; et al. Efficacy and safety of transulnar coronary angiography and interventions—A single center experience. Catheter. Cardiovasc. Interv. 2014, 83, E26–E31. [Google Scholar] [CrossRef]
- Kwan, T.W.; Ratcliffe, J.A.; Chaudhry, M.; Huang, Y.; Wong, S.; Zhou, X.; Pancholy, S.; Patel, T. Transulnar catheterization in patients with ipsilateral radial artery occlusion. Catheter. Cardiovasc. Interv. 2013, 82, E849–E855. [Google Scholar] [CrossRef]
- Hahalis, G.; Tsigkas, G.; Xanthopoulou, I.; Deftereos, S.; Ziakas, A.; Raisakis, K.; Pappas, C.; Sourgounis, A.; Grapsas, N.; Davlouros, P.; et al. Transulnar compared with transradial artery approach as a default strategy for coronary procedures: A randomized trial. The Transulnar or Transradial Instead of Coronary Transfemoral Angiographies Study (the AURA of ARTEMIS Study). Circ. Cardiovasc. Interv. 2013, 6, 252–261. [Google Scholar] [CrossRef]
- Aptecar, E.; Pernes, J.-M.; Chabane-Chaouch, M.; Bussy, N.; Catarino, G.; Shahmir, A.; Bougrini, K.; Dupouy, P. Transulnar versus transradial artery approach for coronary angioplasty: The PCVI-CUBA study. Catheter. Cardiovasc. Interv. 2006, 67, 711–720. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.-Z.; Zhou, Y.-J.; Zhao, Y.-X.; Guo, Y.-H.; Liu, Y.-Y.; Shi, D.-M.; Wang, Z.-J.; Jia, D.-A.; Yang, S.-W.; Nie, B.; et al. Safety and efficacy of transulnar approach for coronary angiography and intervention. Chin. Med. J. 2010, 123, 1774–1779. [Google Scholar] [PubMed]
- Bi, X.; Wang, Q.; Liu, D.; Gan, Q.; Liu, L. Is the Complication Rate of Ulnar and Radial Approaches for Coronary Artery Intervention the Same? Angiology 2017, 68, 919–925. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, R.; Zaky, F.; Ekmejian, A.; Curtis, E.; Lee, A. Safety and efficacy of ulnar artery approach for percutaneous cardiac catheterization: Systematic review and meta-analysis. Catheter. Cardiovasc. Interv. 2018, 91, 1273–1280. [Google Scholar] [CrossRef] [PubMed]
- Sanghvi, K.; Kurian, D.; Coppola, J. Transradial intervention of iliac and superficial femoral artery disease is feasible. J. Interv. Cardiol. 2008, 21, 385–387. [Google Scholar] [CrossRef] [PubMed]
- Allende, R.; Ribeiro, H.B.; Puri, R.; Urena, M.; Abdul-Jawad, O.; del Trigo, M.; Veiga, G.; del Rosario Ortas, M.; Paradis, J.-M.; De Larochellière, R.; et al. The transradial approach during transcatheter structural heart disease interventions: A review. Eur. J. Clin. Investig. 2015, 45, 215–225. [Google Scholar] [CrossRef]
- Sawaya, F.J.; Louvard, Y.; Spaziano, M.; Morice, M.-C.; Hage, F.; El-Khoury, C.; Roy, A.; Garot, P.; Hovasse, T.; Benamer, H.; et al. Short and long-term outcomes of alcohol septal ablation with the trans-radial versus the trans-femoral approach: A single center-experience. Int. J. Cardiol. 2016, 220, 7–13. [Google Scholar] [CrossRef]
- Osken, A.; Aydin, E.; Akdemir, R.; Gunduz, H. Percutaneous Closure of an Aortic Prosthetic Paravalvular Leak with Device in a Patient Presenting with Heart Failure. Heart Views 2015, 16, 56–58. [Google Scholar] [CrossRef]
- Sanghvi, K.; Selvaraj, N.; Luft, U. Percutaneous closure of a perimembranous ventricular septal defect through arm approach (radial artery and basilic vein). J. Interv. Cardiol. 2014, 27, 199–203. [Google Scholar] [CrossRef]
- Saia, F.; Marrozzini, C.; Moretti, C.; Ciuca, C.; Taglieri, N.; Bordoni, B.; Dall’ara, G.; Alessi, L.; Lanzillotti, V.; Bacchi-Reggiani, M.L.; et al. The role of percutaneous balloon aortic valvuloplasty as a bridge for transcatheter aortic valve implantation. EuroIntervention 2011, 7, 723–729. [Google Scholar] [CrossRef]
- Kumar, A.; Paniagua, D.; Hira, R.S.; Alam, M.; Denktas, A.E.; Jneid, H. Balloon Aortic Valvuloplasty in the Transcatheter Aortic Valve Replacement Era. J. Invasive Cardiol. 2016, 28, 341–348. [Google Scholar] [PubMed]
- Tumscitz, C.; Campo, G.; Tebaldi, M.; Gallo, F.; Pirani, L.; Biscaglia, S. Safety and Feasibility of Transradial Mini-Invasive Balloon Aortic Valvuloplasty: A Pilot Study. JACC Cardiovasc. Interv. 2017, 10, 1375–1377. [Google Scholar] [CrossRef] [PubMed]
- Kadakia, M.B.; Herrmann, H.C.; Desai, N.D.; Fox, Z.; Ogbara, J.; Anwaruddin, S.; Jagasia, D.; Bavaria, J.E.; Szeto, W.Y.; Vallabhajosyula, P.; et al. Factors associated with vascular complications in patients undergoing balloon-expandable transfemoral transcatheter aortic valve replacement via open versus percutaneous approaches. Circ. Cardiovasc. Interv. 2014, 7, 570–576. [Google Scholar] [CrossRef] [PubMed]
- van Son, J.A.; Smedts, F.; Vincent, J.G.; van Lier, H.J.; Kubat, K. Comparative anatomic studies of various arterial conduits for myocardial revascularization. J. Thorac. Cardiovasc. Surg. 1990, 99, 703–707. [Google Scholar]
- Gkaliagkousi, E.; Douma, S. The pathogenesis of arterial stiffness and its prognostic value in essential hypertension and cardiovascular diseases. Hippokratia 2009, 13, 70–75. [Google Scholar]
- Faurie, B.; Abdellaoui, M.; Wautot, F.; Staat, P.; Champagnac, D.; Wintzer-Wehekind, J.; Vanzetto, G.; Bertrand, B.; Monségu, J. Rapid pacing using the left ventricular guidewire: Reviving an old technique to simplify BAV and TAVI procedures. Catheter. Cardiovasc. Interv. 2016, 88, 988–993. [Google Scholar] [CrossRef]
| Trial, Year | N. of Patients | STEMI% | NSTE-ACS% | All-Cause Mortality% | MACE% | Access-Site Bleeding% | Major Bleeding% |
|---|---|---|---|---|---|---|---|
| RIVAL, 2011 | |||||||
| Radial | 3507 | 27 | 73 | 1.3 | 3.2 | 1.4 | 0.7 |
| Femoral | 3514 | 29 | 71 | 1.5 | 3.2 | 3.7 | 0.9 |
| RIFLE-STEACS, 2012 | |||||||
| Radial | 500 | 100 | - | 5.2 | 7.2 | 2.6 | 1.8 |
| Femoral | 501 | 100 | 9.2 | 11.4 | 6.8 | 2.8 | |
| STEMI-RADIAL, 2014 | |||||||
| Radial | 348 | 100 | - | 2.3 | 3.4 | 0.6 | 1.4 |
| Femoral | 359 | 100 | 3.1 | 4.2 | 5.3 | 7.2 | |
| MATRIX, 2015 | |||||||
| Radial | 4197 | 48 | 52 | 1.6 | 8.8 | 0.4 | 1.5 |
| Femoral | 207 | 48 | 52 | 2.2 | 10.2 | 1 | 2.3 |
| SAFARI-STEMI, 2019 | |||||||
| Radial | 1136 | 100 | - | 1.5 | 4 | - | 1.1 |
| Femoral | 1156 | 100 | 1.3 | 3.4 | 1.3 |
| First Author, Year | N. of Patients (TUA/TRA) | STEMI% (TUA/TRA) | NSTEMI% (TUA/TRA) | Successful Vascular Access% (TUA/TRA) | Crossover to Other Approach% (TUA/TRA) | Arterial Access Time (min) (TUA/TRA) | PCI% (TUA/TRA) | Bleeding or Hematoma% (TUA/TRA) | Occlusion% (TUA/TRA) | MACE% (TUA/TRA) |
|---|---|---|---|---|---|---|---|---|---|---|
| Aptecar, 2006 | 216/215 | 17.5/16.7 | 22.5/27.6 | 93.1/95.5 | 6.9/4.2 | NR | 43.5/44.2 | 6.8/8.1 | 5.7/4.7 | 2.1/4.2 |
| Li, 2010 | 118/122 | 4.2/4.9 | 77.1/73 | 98.3/100 | 1.7/0 | NR | 65/69.2 | 5.9/5.7 | 1.7/4.9 | 0/0 |
| Hahalis, 2013 | 462/440 | 14.1/13.2 | 37.4/38.4 | 67.7/99.1 | 32.3/5.9 | NR | 36.4/32.7 | 3.2/0.5 | 10.4/4.3 | 2.8/3.4 |
| Geng, 2014 | 271/264 | 14.4/13.6 | 72.7/70.4 | 91.5/95.1 | 8.5/4.2 | NR | 62.4/52.3 | 13.2/7.9 | 1.9/5.8 | 9.4/8.7 |
| Liu, 2014 | 317/319 | 19.6/20.4 | 75.9/77.4 | 92.7/95.9 | 1.6/1.9 | 6.3 ± 1.3/5.9 ± 1.2 | 100/100 | 4.1/9.4 | 6.3/4.7 | 1.9/2.5 |
| Gokhroo, 2016 | 1270/1262 | 48.3/45.2 | 27.6/30.6 | 95.6/96.2 | 4.4/3.8 | 5.6 ± 2.1/5.9 ± 1.7 | NR | 6.2/6.7 | 6.1/6.6 | 2.9/3.2 |
| Bi, 2017 | 220/225 | NR | NR | 90.9/92.9 | 9.1/7.1 | NR | 66.8/62.2 | 28.6/11.5 | 2.7/9.3 | NR |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scalise, R.F.M.; Salito, A.M.; Polimeni, A.; Garcia-Ruiz, V.; Virga, V.; Frigione, P.; Andò, G.; Tumscitz, C.; Costa, F. Radial Artery Access for Percutaneous Cardiovascular Interventions: Contemporary Insights and Novel Approaches. J. Clin. Med. 2019, 8, 1727. https://doi.org/10.3390/jcm8101727
Scalise RFM, Salito AM, Polimeni A, Garcia-Ruiz V, Virga V, Frigione P, Andò G, Tumscitz C, Costa F. Radial Artery Access for Percutaneous Cardiovascular Interventions: Contemporary Insights and Novel Approaches. Journal of Clinical Medicine. 2019; 8(10):1727. https://doi.org/10.3390/jcm8101727
Chicago/Turabian StyleScalise, Renato Francesco Maria, Armando Mariano Salito, Alberto Polimeni, Victoria Garcia-Ruiz, Vittorio Virga, Pierpaolo Frigione, Giuseppe Andò, Carlo Tumscitz, and Francesco Costa. 2019. "Radial Artery Access for Percutaneous Cardiovascular Interventions: Contemporary Insights and Novel Approaches" Journal of Clinical Medicine 8, no. 10: 1727. https://doi.org/10.3390/jcm8101727
APA StyleScalise, R. F. M., Salito, A. M., Polimeni, A., Garcia-Ruiz, V., Virga, V., Frigione, P., Andò, G., Tumscitz, C., & Costa, F. (2019). Radial Artery Access for Percutaneous Cardiovascular Interventions: Contemporary Insights and Novel Approaches. Journal of Clinical Medicine, 8(10), 1727. https://doi.org/10.3390/jcm8101727







