A Comprehensive Study on Tear Meniscus Height Inter-Eye Differences in Aqueous Deficient Dry Eye Diagnosis
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample
2.2. Study Design and Protocol
2.3. Procedure, Diagnostic and Classification Criteria
- Tear film osmolarity was measured using a TearLab osmometer (TearLab, Escondido, CA, USA) [48]. The diagnostic cut-off values for DED diagnosis were tear osmolarity ≥ 308 mOsm/L and/or an osmolarity difference between eyes < 8 mOsm/L.
- FBUT and corneal staining were recorded using a Topcon® (Topcon Corporation, Tokio, Japan) SL-D4 slit lamp equipped with a DC4 video camera (Topcon Corporation, Japan) and non-preserved fluorescein [11,16,17]. The diagnostic cut-off values for DED diagnosis were an FBUT ≤ 10 s and/or corneal staining (Oxford grade) ≥ 2.
2.4. Statistical Analysis
3. Results
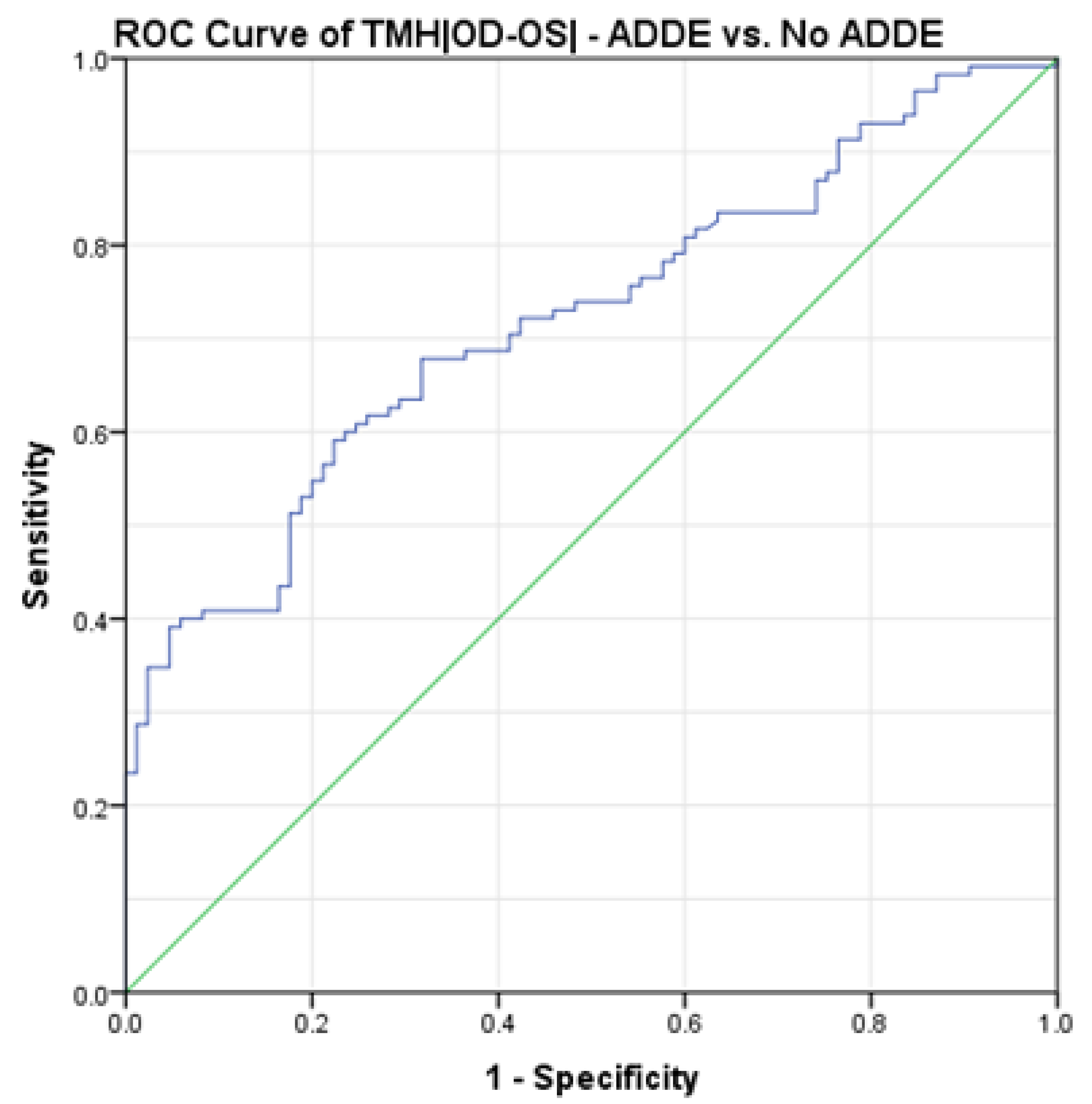
3.1. Assessment of TMH|OD-OS| Cut-Off Value to Differentiate between ADDE and No ADDE Participants
3.2. Cross-Validation of TMH|OD-OS| Cut-Off Value to Differentiate between ADDE and No ADDE Participants
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Craig, J.P.; Nichols, K.K.; Akpek, E.K.; Caffery, B.; Dua, H.S.; Joo, C.K.; Liu, Z.; Nelson, J.D.; Nichols, J.J.; Tsubota, K.; et al. TFOS DEWS II Definition and Classification Report. Ocul. Surf. 2017, 15, 276–283. [Google Scholar] [CrossRef] [PubMed]
- Lemp, M.A.; Foulks, G.N. The definition and classification of dry eye disease: Report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop. Ocul. Surf. 2007, 5, 75–92. [Google Scholar] [CrossRef]
- Wolffsohn, J.S.; Arita, R.; Chalmers, R.; Djalilian, A.; Dogru, M.; Dumbleton, K.; Gupta, P.K.; Karpecki, P.; Lazreg, S.; Pult, H.; et al. TFOS DEWS II Diagnostic Methodology report. Ocul. Surf. 2017, 15, 539–574. [Google Scholar] [CrossRef] [PubMed]
- Bron, A.J.; de Paiva, C.S.; Chauhan, S.K.; Bonini, S.; Gabison, E.E.; Jain, S.; Knop, E.; Markoulli, M.; Ogawa, Y.; Perez, V.; et al. TFOS DEWS II pathophysiology report. Ocul. Surf. 2017, 15, 438–510. [Google Scholar] [CrossRef]
- Baudouin, C.; Messmer, E.M.; Aragona, P.; Geerling, G.; Akova, Y.A.; Benítez-del-Castillo, J.; Boboridis, K.G.; Merayo-Lloves, J.; Rolando, M.; Labetoulle, M. Revisiting the vicious circle of dry eye disease: A focus on the pathophysiology of meibomian gland dysfunction. Br. J. Ophthalmol. 2016, 100, 300–306. [Google Scholar] [CrossRef] [PubMed]
- King-Smith, P.E.; Ramamoorthy, P.; Braun, R.J.; Nichols, J.J. Tear film images and breakup analyzed using fluorescent quenching. Investig. Ophthalmol. Vis. Sci. 2013, 54, 6003–6011. [Google Scholar] [CrossRef] [PubMed]
- Braun, R.J.; King-Smith, P.E.; Begley, C.G.; Li, L.; Gewecke, N.R. Dynamics and function of the tear film in relation to the blink cycle. Prog. Retin. Eye Res. 2015, 45, 132–164. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, B.D.; Crews, L.A.; Messmer, E.M.; Foulks, G.N.; Nichols, K.K.; Baenninger, P.; Geerling, G.; Figueiredo, F.; Lemp, M.A. Correlations between commonly used objective signs and symptoms for the diagnosis of dry eye disease: Clinical implications. Acta Ophthalmol. 2014, 92, 161–166. [Google Scholar] [CrossRef]
- Li, M.; Du, C.; Zhu, D.; Shen, M.; Cui, L.; Wang, J. Daytime variations of tear osmolarity and tear meniscus volume. Eye Contact Lens. 2012, 38, 282–287. [Google Scholar] [CrossRef]
- Bron, A.J.; Tomlinson, A.; Foulks, G.N.; Pepose, J.S.; Baudouin, C.; Geerling, G.; Nichols, K.K.; Lemp, M.A. Rethinking dry eye disease: A perspective on clinical implications. Ocul. Surf. 2014, 12, S1–S31. [Google Scholar] [CrossRef]
- Sabucedo-Villamarin, B.; Pena-Verdeal, H.; Garcia-Queiruga, J.; Giraldez, M.J.; Garcia-Resua, C.; Yebra-Pimentel, E. Categorization of the Aqueous Deficient Dry Eye by a Cut-Off Criterion of TMH Measured with Tearscope. Life 2022, 12, 2007. [Google Scholar] [CrossRef]
- Arita, R.; Minoura, I.; Morishige, N.; Shirakawa, R.; Fukuoka, S.; Asai, K.; Goto, T.; Imanaka, T.; Nakamura, M. Development of Definitive and Reliable Grading Scales for Meibomian Gland Dysfunction. Am. J. Ophthalmol. 2016, 169, 125–137. [Google Scholar] [CrossRef] [PubMed]
- Moreno, I.; Verma, S.; Gesteira, T.F.; Coulson-Thomas, V.J. Recent advances in age-related meibomian gland dysfunction (ARMGD). Ocul. Surf. 2023, 30, 298–306. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.T.M.; Muntz, A.; Lim, J.; Kim, J.S.; Lacerda, L.; Arora, A.; Craig, J.P. Ageing and the natural history of dry eye disease: A prospective registry-based cross-sectional study. Ocul. Surf. 2020, 18, 736–741. [Google Scholar] [CrossRef]
- Stapleton, F.; Abad, J.C.; Barabino, S.; Burnett, A.; Iyer, G.; Lekhanont, K.; Li, T.; Liu, Y.; Navas, A.; Obinwanne, C.J.; et al. TFOS lifestyle: Impact of societal challenges on the ocular surface. Ocul. Surf. 2023, 28, 165–199. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Cheng, W.; Liu, C.; Jin, X.; Ming, S.; Zhao, D.; Feng, X. Evaluation of effects of 3% diquafosol ophthalmic solution on preocular tear film stability after trabeculectomy. Int. Ophthalmol. 2022, 43, 1903–1910. [Google Scholar] [CrossRef]
- Johnson, M.E.; Murphy, P.J. The Effect of instilled fluorescein solution volume on the values and repeatability of TBUT measurements. Cornea 2005, 24, 811–817. [Google Scholar] [CrossRef]
- Kim, Y.H.; Graham, A.D.; Li, W.; Radke, C.J.; Lin, M.C. Human Lacrimal Production Rate and Wetted Length of Modified Schirmer’s Tear Test Strips. Transl. Vis. Sci. Technol. 2019, 8, 40. [Google Scholar] [CrossRef] [PubMed]
- Hao, Y.; Jin, T.; Zhu, L.; Zhao, M.; Wang, S.; Li, Z.; Tian, L.; Jie, Y. Validation of the phenol red thread test in a Chinese population. BMC Ophthalmol. 2023, 23, 498. [Google Scholar] [CrossRef]
- Niedernolte, B.; Trunk, L.; Wolffsohn, J.S.; Pult, H.; Bandlitz, S. Evaluation of tear meniscus height using different clinical methods. Clin. Exp. Optom. 2021, 104, 583–588. [Google Scholar] [CrossRef]
- Singh, S.; Srivastav, S.; Modiwala, Z.; Ali, M.H.; Basu, S. Repeatability, reproducibility and agreement between three different diagnostic imaging platforms for tear film evaluation of normal and dry eye disease. Eye 2023, 37, 2042–2047. [Google Scholar] [CrossRef] [PubMed]
- Karampatakis, V.; Karamitsos, A.; Skriapa, A.; Pastiadis, G. Comparison between normal values of 2- and 5-minute Schirmer test without anesthesia. Cornea 2010, 29, 497–501. [Google Scholar] [CrossRef] [PubMed]
- Ekici, E.; Caglar, C.; Akgumus, E.U. The Repeatability, Reproducibility, and Correlation of the Schirmer Test: A Comparison of Open versus Closed Eye. Korean J. Ophthalmol. 2022, 36, 306–312. [Google Scholar] [CrossRef]
- Clinch, T.E.; Benedetto, D.A.; Felberg, N.T.; Laibson, P.R. Schirmer’s test. A closer look. Arch. Ophthalmol. 1983, 101, 1383–1386. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Xu, Z.; Gong, Q.; Ren, W.; Chen, L.; Lu, F.; Hu, L. The Role of Different Tear Volume Detection Methods in the Evaluation and Diagnosis of Mild Dry Eye Disease. Transl. Vis. Sci. Technol. 2022, 11, 15. [Google Scholar] [CrossRef] [PubMed]
- Lemp, M.A.; Bron, A.J.; Baudouin, C.; Benitez Del Castillo, J.M.; Geffen, D.; Tauber, J.; Foulks, G.N.; Pepose, J.S.; Sullivan, B.D. Tear osmolarity in the diagnosis and management of dry eye disease. Am. J. Ophthalmol. 2011, 151, 792–798 e791. [Google Scholar] [CrossRef]
- Jacobi, C.; Jacobi, A.; Kruse, F.E.; Cursiefen, C. Tear film osmolarity measurements in dry eye disease using electrical impedance technology. Cornea 2011, 30, 1289–1292. [Google Scholar] [CrossRef]
- Tsubota, K.; Yokoi, N.; Watanabe, H.; Dogru, M.; Kojima, T.; Yamada, M.; Kinoshita, S.; Kim, H.M.; Tchah, H.W.; Hyon, J.Y.; et al. A New Perspective on Dry Eye Classification: Proposal by the Asia Dry Eye Society. Eye Contact Lens. 2020, 46 (Suppl. S1), S2–S13. [Google Scholar] [CrossRef]
- Tsubota, K.; Yokoi, N.; Shimazaki, J.; Watanabe, H.; Dogru, M.; Yamada, M.; Kinoshita, S.; Kim, H.M.; Tchah, H.W.; Hyon, J.Y.; et al. New Perspectives on Dry Eye Definition and Diagnosis: A Consensus Report by the Asia Dry Eye Society. Ocul. Surf. 2017, 15, 65–76. [Google Scholar] [CrossRef]
- Tomlinson, A.; Bron, A.J.; Korb, D.R.; Amano, S.; Paugh, J.R.; Pearce, E.I.; Yee, R.; Yokoi, N.; Arita, R.; Dogru, M. The international workshop on meibomian gland dysfunction: Report of the diagnosis subcommittee. Investig. Ophthalmol. Vis. Sci. 2011, 52, 2006–2049. [Google Scholar] [CrossRef]
- Keech, A.; Senchyna, M.; Jones, L. Impact of time between collection and collection method on human tear fluid osmolarity. Curr. Eye Res. 2013, 38, 428–436. [Google Scholar] [CrossRef] [PubMed]
- Nolfi, J.; Caffery, B. Randomized comparison of in vivo performance of two point-of-care tear film osmometers. Clin. Ophthalmol. 2017, 11, 945–950. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Gokhale, M.; Stahl, U.; Jalbert, I. In situ osmometry: Validation and effect of sample collection technique. Optom. Vis. Sci. Off. Publ. Am. Acad. Optom. 2013, 90, 359–365. [Google Scholar] [CrossRef] [PubMed]
- Pena-Verdeal, H.; Garcia-Queiruga, J.; Sabucedo-Villamarin, B.; Giraldez, M.J.; Garcia-Resua, C.; Yebra-Pimentel, E. Capability of the Inter-Eye Differences in Osmolarity, Break-Up Time and Corneal Staining on the Diagnostic of Dry Eye. Ocul. Immunol. Inflamm. 2023, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Nilsen, C.; Graae Jensen, P.; Gundersen, M.; Utheim, O.A.; Gjerdrum, B.; Gundersen, K.G.; Jahanlu, D.; Potvin, R. The Significance of Inter-Eye Osmolarity Difference in Dry Eye Diagnostics. Clin. Ophthalmol. 2023, 17, 829–835. [Google Scholar] [CrossRef] [PubMed]
- Pena-Verdeal, H.; Garcia-Resua, C.; Vazquez-Sanchez, C.; Garcia-Queiruga, J.; Giraldez, M.J.; Yebra-Pimentel, E. Inter-eye osmolarity differences in patients with symptomatic and non-symptomatic dry eyes. Arq. Bras. Oftalmol. 2020, 83, 103–108. [Google Scholar] [CrossRef] [PubMed]
- Tong, L.; Teng, L.S. Review of Literature on Measurements of Non-invasive Break Up Times, Lipid Morphology and Tear Meniscal Height Using Commercially Available Hand-held Instruments. Curr. Eye Res. 2018, 43, 567–575. [Google Scholar] [CrossRef]
- Garcia-Queiruga, J.; Pena-Verdeal, H.; Sabucedo-Villamarin, B.; Giraldez, M.J.; Garcia-Resua, C.; Yebra-Pimentel, E. A cross-sectional study of non-modifiable and modifiable risk factors of dry eye disease states. Contact Lens Anterior Eye J. Br. Contact Lens Assoc. 2023, 46, 101800. [Google Scholar] [CrossRef]
- Pena-Verdeal, H.; Noya-Padin, V.; Losada-Oubina, M.; Saborido-Rey, M.; Vilas-Alonso, M.; Giraldez, M.J. Changes of symptomatology, tear film and ocular surface integrity one week during Somofilcon-A and Omafilcon-A lens wear. Eur. J. Ophthalmol. 2022, 33, 890–899. [Google Scholar] [CrossRef]
- Pucker, A.D. A Review of the Compatibility of Topical Artificial Tears and Rewetting Drops with Contact Lenses. Contact Lens Anterior Eye J. Br. Contact Lens Assoc. 2020, 43, 426–432. [Google Scholar] [CrossRef]
- Nichols, K.K.; Mitchell, G.L.; Zadnik, K. The repeatability of clinical measurements of dry eye. Cornea 2004, 23, 272–285. [Google Scholar] [CrossRef] [PubMed]
- Wong, H. Minimum important difference is minimally important in sample size calculations. Trials 2023, 24, 34. [Google Scholar] [CrossRef] [PubMed]
- Obuchowski, N.A.; Bullen, J.A. Receiver operating characteristic (ROC) curves: Review of methods with applications in diagnostic medicine. Phys. Med. Biol. 2018, 63, 07TR01. [Google Scholar] [CrossRef] [PubMed]
- Nahm, F.S. Receiver operating characteristic curve: Overview and practical use for clinicians. Korean J. Anesthesiol. 2022, 75, 25–36. [Google Scholar] [CrossRef] [PubMed]
- Wolffsohn, J.S.; Wang, M.T.M.; Vidal-Rohr, M.; Menduni, F.; Dhallu, S.; Ipek, T.; Acar, D.; Recchioni, A.; France, A.; Kingsnorth, A.; et al. Demographic and lifestyle risk factors of dry eye disease subtypes: A cross-sectional study. Ocul. Surf. 2021, 21, 58–63. [Google Scholar] [CrossRef]
- Armstrong, R.A. Statistical guidelines for the analysis of data obtained from one or both eyes. Ophthalmic. Physiol. Opt. 2013, 33, 7–14. [Google Scholar] [CrossRef] [PubMed]
- Akowuah, P.K.; Adjei-Anang, J.; Nkansah, E.K.; Fummey, J.; Osei-Poku, K.; Boadi, P.; Frimpong, A.A. Comparison of the performance of the dry eye questionnaire (DEQ-5) to the ocular surface disease index in a non-clinical population. Contact Lens Anterior Eye J. Br. Contact Lens Assoc. 2022, 45, 101441. [Google Scholar] [CrossRef] [PubMed]
- Tavakoli, A.; Markoulli, M.; Flanagan, J.; Papas, E. The validity of point of care tear film osmometers in the diagnosis of dry eye. Ophthalmic. Physiol. Opt. 2022, 42, 140–148. [Google Scholar] [CrossRef]
- Lam, A.K.; Tai, S.K.; Chan, J.K.; Ng, R.W. Lower Tear Meniscus Height Measurements Using Keratography and Swept-Source Optical Coherence Tomography and Effect of Fluorescein Instillation Methods. Curr. Eye Res. 2019, 44, 1203–1208. [Google Scholar] [CrossRef]
- Pena-Verdeal, H.; Garcia-Resua, C.; Barreira, N.; Giraldez, M.J.; Yebra-Pimentel, E. Interobserver variability of an open-source software for tear meniscus height measurement. Contact Lens Anterior Eye J. Br. Contact Lens Assoc. 2016, 39, 249–256. [Google Scholar] [CrossRef]
- Fodor, E.; Hagyo, K.; Resch, M.; Somodi, D.; Nemeth, J. Comparison of Tearscope-plus versus slit lamp measurements of inferior tear meniscus height in normal individuals. Eur. J. Ophthalmol. 2010, 20, 819–824. [Google Scholar] [CrossRef]
- Armstrong, R.A.; Davies, L.N.; Dunne, M.C.; Gilmartin, B. Statistical guidelines for clinical studies of human vision. Ophthalmic. Physiol. Opt. 2011, 31, 123–136. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.; Vanathi, M.; Kishore, A.; Gupta, N.; Tandon, R. Evaluation of strip meniscometry, tear meniscus height and depth in the diagnosis of dry eye disease in asian Indian eyes. Ocul. Surf. 2019, 17, 747–752. [Google Scholar] [CrossRef] [PubMed]
- Qiu, X.; Gong, L.; Lu, Y.; Jin, H.; Robitaille, M. The diagnostic significance of Fourier-domain optical coherence tomography in Sjogren syndrome, aqueous tear deficiency and lipid tear deficiency patients. Acta Ophthalmol. 2012, 90, e359–e366. [Google Scholar] [CrossRef] [PubMed]
- Messmer, E.M.; von Lindenfels, V.; Garbe, A.; Kampik, A. Matrix Metalloproteinase 9 Testing in Dry Eye Disease Using a Commercially Available Point-of-Care Immunoassay. Ophthalmology 2016, 123, 2300–2308. [Google Scholar] [CrossRef] [PubMed]
- Pult, H.; Purslow, C.; Murphy, P.J. The relationship between clinical signs and dry eye symptoms. Eye 2011, 25, 502–510. [Google Scholar] [CrossRef] [PubMed]
- Versura, P.; Frigato, M.; Cellini, M.; Mule, R.; Malavolta, N.; Campos, E.C. Diagnostic performance of tear function tests in Sjogren’s syndrome patients. Eye 2007, 21, 229–237. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, O.M.; Dogru, M.; Ward, S.K.; Matsumoto, Y.; Wakamatsu, T.H.; Ishida, K.; Tsuyama, A.; Kojima, T.; Shimazaki, J.; Tsubota, K. The efficacy, sensitivity, and specificity of strip meniscometry in conjunction with tear function tests in the assessment of tear meniscus. Investig. Ophthalmol. Vis. Sci. 2011, 52, 2194–2198. [Google Scholar] [CrossRef]
- Akpek, E.K.; Bunya, V.Y.; Saldanha, I.J. Sjogren’s Syndrome: More Than Just Dry Eye. Cornea 2019, 38, 658–661. [Google Scholar] [CrossRef]
- Sabucedo-Villamarin, B.; Pena-Verdeal, H.; Garcia-Queiruga, J.; Giraldez, M.J.; Garcia-Resua, C.; Yebra-Pimentel, E. Longitudinal analysis of variation in status and diagnostic stability of untreated dry eye disease. Ocul. Surf. 2023, 29, 298–300. [Google Scholar] [CrossRef]
- Lienert, J.P.; Tarko, L.; Uchino, M.; Christen, W.G.; Schaumberg, D.A. Long-term Natural History of Dry Eye Disease from the Patient’s Perspective. Ophthalmology 2016, 123, 425–433. [Google Scholar] [CrossRef]
- Lo, C.; Yang, M.; Rootman, D. Natural history of inflammatory and non-inflammatory dry eye in thyroid eye disease. Orbit 2021, 40, 389–393. [Google Scholar] [CrossRef]
| Mean | SD | Minimum | Maximum | |
|---|---|---|---|---|
| Age (years) | 49.8 | 14.29 | 18.0 | 81.0 |
| OSDI (Score | 31.85 | 15.99 | 12.50 | 83.33 |
| Osmolarity (mOsm/L) | 321.9 | 19.31 | 275.0 | 400.0 |
| Osmolarity |OD-OS| (mOsm/L) | 11.8 | 12.47 | 0.0 | 71.0 |
| Corneal Staining | 0 * | 1 ** | 0 | 4 |
| FBUT (s) | 7.19 | 6.46 | 0.79 | 65.13 |
| TMH (mm) | 0.199 | 0.099 | 0.06 | 0.64 |
| TMH |OD-OS| (mm) | 0.040 | 0.039 | 0.00 | 0.22 |
| TMH|OD-OS| = 0.033 mm | Total | |||
|---|---|---|---|---|
| ADDE | No ADDE | |||
| TFOS DEWS II | ADDE | 48 | 15 | 63 |
| No ADDE | 38 | 59 | 97 | |
| Total | 86 | 74 | 160 | |
| Mean | SD | Minimum | Maximum | |
|---|---|---|---|---|
| Age (years) | 51.1 | 12.97 | 21.0 | 76.0 |
| OSDI (Score | 30.47 | 14.45 | 12.50 | 77.27 |
| Osmolarity (mOsm/L) | 323.8 | 18.08 | 293.0 | 400.0 |
| Osmolarity |OD-OS| (mOsm/L) | 12.7 | 10.46 | 1.0 | 62.0 |
| Corneal Staining | 0.5 * | 1 ** | 0 | 4 |
| FBUT (s) | 7.59 | 5.42 | 1.46 | 26.46 |
| TMH (mm) | 0.212 | 0.066 | 0.09 | 0.46 |
| TMH |OD-OS| (mm) | 0.034 | 0.035 | 0.00 | 0.19 |
| TMH|OD-OS| = 0.033 mm | Total | |||
|---|---|---|---|---|
| ADDE | No ADDE | |||
| TFOS DEWS II | ADDE | 13 | 1 | 14 |
| No ADDE | 22 | 24 | 46 | |
| Total | 35 | 25 | 60 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pena-Verdeal, H.; Garcia-Queiruga, J.; Sabucedo-Villamarin, B.; Garcia-Resua, C.; Giraldez, M.J.; Yebra-Pimentel, E. A Comprehensive Study on Tear Meniscus Height Inter-Eye Differences in Aqueous Deficient Dry Eye Diagnosis. J. Clin. Med. 2024, 13, 659. https://doi.org/10.3390/jcm13030659
Pena-Verdeal H, Garcia-Queiruga J, Sabucedo-Villamarin B, Garcia-Resua C, Giraldez MJ, Yebra-Pimentel E. A Comprehensive Study on Tear Meniscus Height Inter-Eye Differences in Aqueous Deficient Dry Eye Diagnosis. Journal of Clinical Medicine. 2024; 13(3):659. https://doi.org/10.3390/jcm13030659
Chicago/Turabian StylePena-Verdeal, Hugo, Jacobo Garcia-Queiruga, Belen Sabucedo-Villamarin, Carlos Garcia-Resua, Maria J. Giraldez, and Eva Yebra-Pimentel. 2024. "A Comprehensive Study on Tear Meniscus Height Inter-Eye Differences in Aqueous Deficient Dry Eye Diagnosis" Journal of Clinical Medicine 13, no. 3: 659. https://doi.org/10.3390/jcm13030659
APA StylePena-Verdeal, H., Garcia-Queiruga, J., Sabucedo-Villamarin, B., Garcia-Resua, C., Giraldez, M. J., & Yebra-Pimentel, E. (2024). A Comprehensive Study on Tear Meniscus Height Inter-Eye Differences in Aqueous Deficient Dry Eye Diagnosis. Journal of Clinical Medicine, 13(3), 659. https://doi.org/10.3390/jcm13030659











