Abstract
Preeclampsia (PE) is a typical hypertensive disorders of pregnancy (HDP) which can cause substantial morbidity and mortality in both pregnant women and fetuses. The renin-angiotensin system (RAS) genes are the main HDP-causing genes, and Angiotensinogen (AGT) as the initial substrate can directly reflect the activity of the entire RAS. However, the association between AGT SNPs and PE risk has rarely been confirmed. This study was carried out to determine whether AGT SNPs could affect the risk of PE in 228 cases and 358 controls. The genotyping result revealed that the AGT rs7079 TT carrier was related to increased PE risk. Further stratified analysis illustrated that the rs7079 TT genotype significantly increased the PE risk in subgroups of Age < 35, BMI < 25, Albumin (ALB) ≥ 30 and Aspartate aminotransferase (AST) < 30. These findings demonstrated that the rs7079 might be a promising candidate SNP strongly associated with PE susceptibility.
1. Introduction
Hypertensive disorders of pregnancy (HDP) have long been major causes of morbidity and mortality in pregnant women, and the incidence of HDP keeps rising worldwide [1,2]. These pregnancy disorders include gestational hypertension, preeclampsia (PE), and eclampsia, which are characterized by elevated blood pressure and multiple organ disturbances, ranging from mild to severe [3,4]. The PE complicates 3–5% of all pregnancies and is estimated to result in a large number of maternal and fetal deaths globally every year [5,6]. Although the majority of PE usually resolve after delivery or in the early postpartum period, there is increasing evidence that PE confers a noteworthy increase in risks for future long-term health [7,8]. It is irrefutable that a history of PE increases the risk of hypertension, peripheral arterial disease, coronary artery disease and cerebrovascular disease in the future [9,10]. Furthermore, the severity of PE has been shown to accelerate the progression of cardiovascular disease [11]. To date, there is no stable and reliable treatment for PE. Therefore, elucidating the pathogenesis of PE is particularly critical for the diagnosis and treatment of this disease.
With the rapid development of molecular biology technology, the genetic basis of HDP has been initially revealed [12,13]. Previous studies have shown that renalase (RNLS) gene polymorphisms were associated with many diseases, such as essential hypertension, PE [14] and gestational diabetes [15]. A recent study displayed that the interleukin 1 receptor type 1 (IL1R1) rs2071374G variant could lead to an increased risk of PE [16]. The egl-9 family hypoxia inducible factor 1 (EGLN1) rs479200 may have the potential to become a marker to evaluate the genetic predisposition to PE [17]. However, the identified genetic mutation or SNPs can only explain the etiology of PE in a small sample of cases. Therefore, the identification and characterization of more functional mutation sites are critical to fully reveal the pathologic mechanism of PE.
The renin-angiotensin system (RAS) plays a crucial role in maintaining the homeostasis of cardiovascular function, especially the regulation of arterial blood pressure [18,19]. Its dysfunction can lead to a series of cardiovascular diseases [20,21]. Angiotensinogen (AGT), as the initial substrate in the RAS, directly reflects the activity of the entire RAS [22]. So far, the investigation that directly evaluated the effect of AGT SNP on PE is relatively limited. Therefore, the current study aimed to assess the association between AGT gene SNPs and PE risk among Chinese pregnant women.
2. Materials and Methods
All patients and controls in this case-control study were from the Department of Obstetrics and Gynecology, The Third Affiliated Hospital of Guangzhou Medical University, during the period from January 2016 to December 2021. 228 PE patients constituted the case group, and 358 normotensive pregnant women constituted the control group. All PE patients were diagnosed according to the diagnostic criteria of the American College of Obstetrics and Gynecology published in 2013 (systolic and/or diastolic blood pressure ≥ 140/90 mmHg after 20th week of pregnancy, plus proteinuria ≥ 300 mg per 24-h urine collection or ≥ 1+ urine dipstick; in the absence of proteinuria, hypertension in pregnancy with any of the following features: pulmnary edema, platelets count ≤ 10 × 1010/L, impaired liver function, systolic and/or diastolic blood pressure ≥ 160/110 mmHg, renal failure and visual disturbances) [23]. The samples of the control group and the case group were non-probability continuous and random. Normotensive pregnant women without a history of chronic hypertension and complication during pregnancy were defined as the control population. Clinical characteristics and biochemical indicators of all participants were collected for stratified analysis.
The three SNPs to be verified were selected according to the following criteria: The selected SNPs were preferentially located in 3′ and 5′ untranslated regions and exons of AGT gene to maximize the probability that these SNPs were functional; The minor allele frequencies of these selected SNPs should be 5% or greater. Furthermore, any two SNPs should have low linkage disequilibrium (R2 < 0.8). DNA of each subject for genotyping was extracted from a peripheral venous blood sample (200 µL) according to the protocol of the TIANamp Genomic DNA Kit (Tiangen Biotech, Beijing, China). The Genotyping, performed according to the instructions (Applied Biosystems, Waltham, MA, USA), was carried out in a total volume of 10 µL containing the DNA template (1 µL, 2 ng/µL), TaqMan® SNP Genotyping Assay (0.06 µL, 40X), TaqPath ProAm Master Mix (3 µL) and DEPC H2O (add to 10 µL). The Genotyping conditions were as follows: 60 °C for 30 s, 95 °C for 5 min, followed by 40 cycles of 95 °C for 15 s and 60 °C for 1 min. The Genotyping was operated with optical 96 or 384-well plate in an ABI PRISM 7500 PCR instrument (Applied Biosystems). In addition, 5% of the samples were randomly re-tested to make sure that these re-tested samples attain 100% recurrence rate.
The student t-test for continuous variables was employed to evaluate clinical variables differences in the case and control groups. The χ2 test served to know whether these three AGT SNPs in the controls were in Hardy-Weinberg equilibrium (HWE). Crude ratios with respective 95% confidence intervals (CIs) and logistic regression analysis were used to assess the association between HDP risk and AGT SNPs. SPSS software was used to analyze all data in this plot study. The p-value less than 0.05 indicated that the statistical result was defined as significant.
3. Results
3.1. Clinical Characteristics of Cases and Controls
The clinical and demographic characteristics of all participants were shown in Table 1. The statistical results indicated that the body mass index (BMI), maternal age, systolic blood pressure (SBP), diastolic blood pressure (DBP), Aspartate aminotransferase (AST), Alanine aminotransferase (ALT), creatinine (CREA) and uricacid (UA) in the case group were significantly higher than that of the control group (all p < 0.01). On the other hand, gestational age, fetal birth weight, Albumin (ALB) and platelet count (PLT) level were significantly lower in the preeclamptic patients compared to the control subjects (all p < 0.01).

Table 1.
Clinical characteristics overview of the study population.
3.2. Effect of AGT Gene SNPs on PE
The genotype distributions for three selected AGT SNPs showed that there was a significant association between rs7079 TT genotype and PE risk (OR = 3.804, 95% CI = 1.100–13.156, p = 0.035) (Table 2). These results indicated that the rs7079 TT carrier shared a significantly increased risk of PE. Moreover, the AGT rs7079 TT genotype was associated with increased preeclampsia risk in the recessive model (OR = 4.054, 95% CI = 1.178–13.945, p = 0.026) (Table 2). However, we did not detect significant differences in SNP rs4762 and rs5050 in any analysis model. At last, the genotype distribution frequencies of three AGT SNPs of the investigated samples were in accordance with the Hardy-Weinberg equilibrium (HWE) in the control group (Table 3).

Table 2.
Genotype and allelic distribution between PE and healthy controls.

Table 3.
Hardy–Weinberg equilibrium of three AGT SNPs genotype distribution frequency in the control group.
3.3. Stratification Analysis
In order to further clarify the role of the three SNPs in different clinical subgroups, a stratified analysis based on age, BMI and clinical parameters was performed. As presented in Table 4, the rs7079 TT genotype carriers shared significantly increased PE risk in subgroups of Age < 35 (OR = 10.988, 95% CI = 2.342–51.555, p = 0.001), BMI < 25 (OR = 5.153, 95% CI = 1.314–20.212, p = 0.024), ALB ≥ 30 (OR = 5.029, 95% CI = 1.392–18.167, p = 0.019) and AST < 30 (OR = 5.088, 95% CI = 1.573–16.456, p = 0.007).

Table 4.
Stratified analysis for PE susceptibility and AGT rs7079 G > T.
3.4. The Relevance of rs7079 G>T to AGT Expression
To determine whether rs7079 could lead to change of AGT gene expression, the GTEx database was used to verify the correlation between rs7079 G>T and AGT mRNA expression. The results showed that the rs7079 T allele was significantly related to the decrease of AGT expression level in cultured fibroblasts (p = 0.000099) (Figure 1).
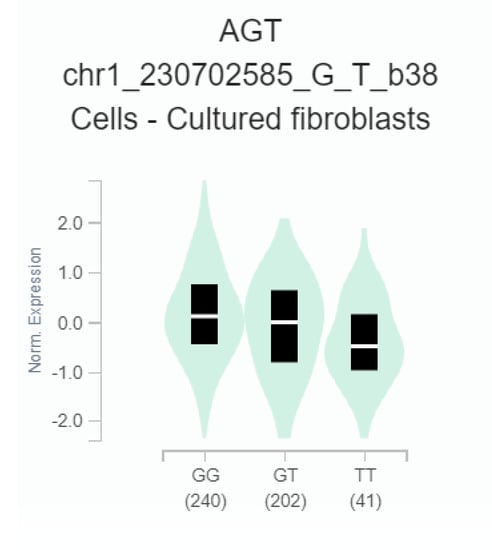
Figure 1.
The effect of rs7079 G>T on Angiotensinogen (AGT) gene expression in cultured fibroblasts (p = 0.000099). The gene expression data was obtained from the public database GTEx portal.
4. Discussion
To date, the AGT gene has been confirmed to be closely related to the occurrence and development of various types of diseases, including cardiovascular disease [24] and colorectal cancer [25]. A recent experimental study pointed out that loss of AGT protein in specific cells can improve high-fat diet-induced insulin tolerance [26]. And Yilmaz et al. reported that urinary AGT levels in 35-week gestational women with PE were significantly elevated compared to normal pregnancies and non-pregnant women [27]. Moreover, consistent evidence found by clinical research showed that plasma-derived oxidized AGT in pregnant women with PE retained a dominant level compared to normotensive controls [28]. These above results indicated the important biological function of AGT in the process of diseases occurrence and development.
Contributions of AGT SNPs to cardiovascular diseases have been widely accepted in recent years [29,30]. In patients with peripheral arterial disease, the association between AGT rs699 CC genotype and high-density lipoprotein (HDL) levels was proved to be significant [31]. The non-alcoholic fatty liver disease (NAFLD) patients with the AGT rs5051 TC + CC genotype had a significantly increased risk of coronary heart disease (CHD) in the northern Chinese Han population [32]. Nonetheless, the association between these three AGT SNPs and PE has not been well established. Through genotyping and stratified analysis of 228 cases and 358 controls, the present study successfully clarified the association between AGT SNPs and PE risk. The rs4762 accompanied by the mutation from threonine to methionine at residence 174 is a typical missense mutation of AGT gene [33]. Previous study confirmed that the rs4762 showed a significant risk for the diabetes mellitus in transplant patients [34]. Another clinical study in Egyptians pointed out the rs4762 variant may increased the risk for end-stage renal failure risk [35]. Compared with rs4762, the AGT rs5050 leads to the transformation from adenine to cytosine in the promoter region of gene. The AGT rs5050 GG carriers with astrocytoma were more likely to have poor prognosis [36]. In children with Kawasaki Disease, rs5050 T>G was associated with the risk of coronary artery aneurysm [37]. However, our findings indicated that there was no statistically significant association between these two SNPs (rs4762 and rs050) and PE susceptibility (Table 2). We speculated that the two functional SNP sites rs4762 and rs050 would not affect the dynamic balance of RAS, so that the susceptibility of PE did not change. The AGT rs7079 located in the 3′UTR is the direct binding site of miR-31 and miR-584 regulating AGT gene expression [38,39]. Moreover, the genotyping results in this study showed that the rs7079 TT genotype was related to increased PE risk (Table 2). The stratified analysis further indicated that the rs7079 TT genotype carriers shared significantly increased PE risk in subgroups of Age < 35, BMI < 25, ALB ≥ 30 and AST < 30 (Table 4). Moreover, we found that the rs7079 T allele resulted in the decrease of AGT expression level in the GTEx portal (Figure 1). Based on the above findings, we speculated that the rs7079 T allele may increase PE risk by disturbing the dynamic equilibrium of the RAS.
There are some deficiencies as follows that could be improved in future research. First, this study only verified the function of three AGT SNPs. More AGT SNPs should be tested to comprehensively evaluate the association between AGT SNPs and PE risk. Second, in consideration of this study’s relatively limited sample size, larger sample sizes are needed to confirm the impact of AGT SNPs on PE risk. Third, the non-genetic risk factors, including environmental factors, life style, and health care, are also considered as the main nosogenesis of PE [40,41]. Therefore, the non-genetic risk factors merit further research in combination with the analysis between the PE risk and SNPs. Finally, the genetic diversity among different ethnic groups also affects the susceptibility to PE. In the subsequent evaluation of the association between AGT gene polymorphisms and susceptibility to PE, it will be a great challenge to exclude functional genetic diversity that may potentially affect the risk of PE.
Author Contributions
Conceptualization, W.W. and Y.C.; Data curation, D.H. and H.X.; Formal analysis, D.H., X.P., H.X. and Y.G.; Funding acquisition, Y.C.; Investigation, D.H., X.P., H.X. and Y.G.; Methodology, H.H. and Y.C.; Project administration, W.W. and Y.C.; Resources, X.P., R.P., Q.L. and H.H.; Software, D.H., X.P. and H.X.; Supervision, W.W. and Y.C.; Validation, W.W. and H.H.; Visualization, D.H.; Writing—original draft, D.H. and Y.C.; Writing—review & editing, D.H. and Y.C. All authors have read and agreed to the published version of the manuscript.
Funding
This work was supported by the National Natural Science Foundation of China [82274130, 82230126, 82171666]; the Major Program of Science and Technology Program of Guangzhou [202103000044]; the Guangzhou Science and Technology Foundation [202102010266]; the Major Basic Research Program of Guangdong [2021ZDZX2041].
Institutional Review Board Statement
This plot study was conducted in accordance with the Declaration of Helsinki and approved by the ethics committee of the third Affiliated Hospital of Guangzhou Medical University (Approval Number: 2014085).
Informed Consent Statement
All participants or their guardians signed written informed consent before the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgments
We thank Jing He for guidance and suggestion to the project.
Conflicts of Interest
The authors declare no conflict of interest.
References
- American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 202: Gestational Hypertension and Preeclampsia. Obstet Gynecol. 2019, 133, 1. [Google Scholar] [CrossRef]
- Garovic, V.D.; Dechend, R.; Easterling, T.; Karumanchi, S.A.; McMurtry Baird, S.; Magee, L.A.; Rana, S.; Vermunt, J.V.; August, P. Hypertension in Pregnancy: Diagnosis, Blood Pressure Goals, and Pharmacotherapy: A Scientific Statement from the American Heart Association. Hypertension 2022, 79, e21–e41. [Google Scholar] [CrossRef] [PubMed]
- Brown, M.A.; Magee, L.A.; Kenny, L.C.; Karumanchi, S.A.; McCarthy, F.P.; Saito, S.; Hall, D.R.; Warren, C.E.; Adoyi, G.; Ishaku, S. The hypertensive disorders of pregnancy: ISSHP classification, diagnosis & management recommendations for international practice. Pregnancy Hypertens. 2018, 13, 291–310. [Google Scholar] [CrossRef] [PubMed]
- Nobles, C.J.; Mendola, P.; Mumford, S.L.; Silver, R.M.; Kim, K.; Andriessen, V.C.; Connell, M.; Sjaarda, L.; Perkins, N.J.; Schisterman, E.F. Preconception Blood Pressure and Its Change into Early Pregnancy: Early Risk Factors for Preeclampsia and Gestational Hypertension. Hypertension 2020, 76, 922–929. [Google Scholar] [CrossRef] [PubMed]
- Chappell, L.C.; Cluver, C.A.; Kingdom, J.; Tong, S. Pre-eclampsia. Lancet 2021, 398, 341–354. [Google Scholar] [CrossRef] [PubMed]
- Abalos, E.; Cuesta, C.; Grosso, A.L.; Chou, D.; Say, L. Global and regional estimates of preeclampsia and eclampsia: A systematic review. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 170, 1–7. [Google Scholar] [CrossRef]
- Ambrožič, J.; Lučovnik, M.; Cvijić, M. Evolution of cardiac geometry and function in women with severe preeclampsia from immediately post-delivery to 1 year postpartum. Int. J. Cardiovasc. Imaging 2021, 37, 2217–2225. [Google Scholar] [CrossRef]
- Khosla, K.; Heimberger, S.; Nieman, K.M.; Tung, A.; Shahul, S.; Staff, A.C.; Rana, S. Long-Term Cardiovascular Disease Risk in Women After Hypertensive Disorders of Pregnancy: Recent Advances in Hypertension. Hypertension 2021, 78, 927–935. [Google Scholar] [CrossRef]
- Brouwers, L.; van der Meiden-van Roest, A.J.; Savelkoul, C.; Vogelvang, T.E.; Lely, A.T.; Franx, A.; van Rijn, B.B. Recurrence of pre-eclampsia and the risk of future hypertension and cardiovascular disease: A systematic review and meta-analysis. Br. J. Obstet. Gynaecol. 2018, 125, 1642–1654. [Google Scholar] [CrossRef]
- Berends, A.L.; de Groot, C.J.; Sijbrands, E.J.; Sie, M.P.; Benneheij, S.H.; Pal, R.; Heydanus, R.; Oostra, B.A.; van Duijn, C.M.; Steegers, E.A. Shared constitutional risks for maternal vascular-related pregnancy complications and future cardiovascular disease. Hypertension 2008, 51, 1034–1041. [Google Scholar] [CrossRef]
- Craici, I.; Wagner, S.; Garovic, V.D. Preeclampsia and future cardiovascular risk: Formal risk factor or failed stress test? Ther. Adv. Cardiovasc. Dis. 2008, 2, 249–259. [Google Scholar] [CrossRef]
- Gray, K.J.; Saxena, R.; Karumanchi, S.A. Genetic predisposition to preeclampsia is conferred by fetal DNA variants near FLT1, a gene involved in the regulation of angiogenesis. Am. J. Obstet. Gynecol. 2018, 218, 211–218. [Google Scholar] [CrossRef]
- Ardissino, M.; Slob, E.A.W.; Millar, O.; Reddy, R.K.; Lazzari, L.; Patel, K.H.K.; Ryan, D.; Johnson, M.R.; Gill, D.; Ng, F.S. Maternal Hypertension Increases Risk of Preeclampsia and Low Fetal Birthweight: Genetic Evidence from a Mendelian Randomization Study. Hypertension 2022, 79, 588–598. [Google Scholar] [CrossRef]
- Bagci, B.; Karakus, S.; Bagci, G.; Sancakdar, E. Renalase gene polymorphism is associated with increased blood pressure in preeclampsia. Pregnancy Hypertens. 2016, 6, 115–120. [Google Scholar] [CrossRef]
- Fatima, S.S.; Jamil, Z.; Alam, F.; Malik, H.Z.; Madhani, S.I.; Ahmad, M.S.; Shabbir, T.; Rehmani, M.N.; Rabbani, A. Polymorphism of the renalase gene in gestational diabetes mellitus. Endocrine 2017, 55, 124–129. [Google Scholar] [CrossRef]
- Sivaraj, N.; Rachel, K.V.; Suvvari, T.K.; Prasad, S.; Boppana, S.H.; Vegi, P.K. Association of IL1R1 gene (SNP rs2071374) with the risk of preeclampsia. J. Reprod. Immunol. 2022, 149, 103463. [Google Scholar] [CrossRef]
- Kumar, K.S.P.; Arcot, M.; Munisamaiah, M.; Balakrishna, S. Novel association of SNP rs479200 in EGLN1 gene with predisposition to preeclampsia. Gene 2019, 705, 1–4. [Google Scholar] [CrossRef]
- Schmieder, R.E.; Hilgers, K.F.; Schlaich, M.P.; Schmidt, B.M. Renin-angiotensin system and cardiovascular risk. Lancet 2007, 369, 1208–1219. [Google Scholar] [CrossRef]
- Paz Ocaranza, M.; Riquelme, J.A.; García, L.; Jalil, J.E.; Chiong, M.; Santos, R.A.S.; Lavandero, S. Counter-regulatory renin-angiotensin system in cardiovascular disease. Nat. Rev. Cardiol. 2020, 17, 116–129. [Google Scholar] [CrossRef]
- Takimoto-Ohnishi, E.; Murakami, K. Renin-angiotensin system research: From molecules to the whole body. J. Physiol. Sci. 2019, 69, 581–587. [Google Scholar] [CrossRef]
- Wu, C.H.; Mohammadmoradi, S.; Chen, J.Z.; Sawada, H.; Daugherty, A.; Lu, H.S. Renin-Angiotensin System and Cardiovascular Functions. Arterioscler. Thromb. Vasc. Biol. 2018, 38, e108–e116. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.; Lu, H.; Cassis, L.A.; Daugherty, A. Molecular and Pathophysiological Features of Angiotensinogen: A Mini Review. N Am. J. Med. Sci. 2011, 4, 183–190. [Google Scholar] [CrossRef]
- American College of Obstetricians and Gynecologists. Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet. Gynecol. 2013, 122, 1122–1131. [Google Scholar] [CrossRef]
- Xu, Y.; Rong, J.; Zhang, Z. The emerging role of angiotensinogen in cardiovascular diseases. J. Cell. Physiol. 2021, 236, 68–78. [Google Scholar] [CrossRef] [PubMed]
- Chen, W.; Chen, Y.; Zhang, K.; Yang, W.; Li, X.; Zhao, J.; Liu, K.; Dong, Z.; Lu, J. AGT serves as a potential biomarker and drives tumor progression in colorectal carcinoma. Int. Immunopharmacol. 2021, 101, 108225. [Google Scholar] [CrossRef]
- Tao, X.R.; Rong, J.B.; Lu, H.S.; Daugherty, A.; Shi, P.; Ke, C.L.; Zhang, Z.C.; Xu, Y.C.; Wang, J.A. Angiotensinogen in hepatocytes contributes to Western diet-induced liver steatosis. J. Lipid. Res. 2019, 60, 1983–1995. [Google Scholar] [CrossRef]
- Yilmaz, Z.; Yildirim, T.; Yilmaz, R.; Aybal-Kutlugun, A.; Altun, B.; Kucukozkan, T.; Erdem, Y. Association between urinary angiotensinogen, hypertension and proteinuria in pregnant women with preeclampsia. J. Renin Angiotensin Aldosterone Syst. 2015, 16, 514–520. [Google Scholar] [CrossRef]
- Dahabiyeh, L.A.; Tooth, D.; Kurlak, L.O.; Mistry, H.D.; Pipkin, F.B.; Barrett, D.A. A pilot study of alterations in oxidized angiotensinogen and antioxidants in pre-eclamptic pregnancy. Sci. Rep. 2020, 10, 1956. [Google Scholar] [CrossRef]
- Watkins, W.S.; Hunt, S.C.; Williams, G.H.; Tolpinrud, W.; Jeunemaitre, X.; Lalouel, J.M.; Jorde, L.B. Genotype-phenotype analysis of angiotensinogen polymorphisms and essential hypertension: The importance of haplotypes. J. Hypertens. 2010, 28, 65–75. [Google Scholar] [CrossRef]
- Mabhida, S.E.; Mashatola, L.; Kaur, M.; Sharma, J.R.; Apalata, T.; Muhamed, B.; Benjeddou, M.; Johnson, R. Hypertension in African Populations: Review and Computational Insights. Genes 2021, 12, 532. [Google Scholar] [CrossRef]
- Junusbekov, Y.; Bayoglu, B.; Cengiz, M.; Dirican, A.; Arslan, C. AGT rs699 and AGTR1 rs5186 gene variants are associated with cardiovascular-related phenotypes in atherosclerotic peripheral arterial obstructive disease. Ir. J. Med. Sci. 2020, 189, 885–894. [Google Scholar] [CrossRef]
- Dong, M.Z.; Lin, Z.H.; Liu, S.S.; Xin, Y.N.; Xuan, S.Y. AGT rs5051 gene polymorphism increases the risk of coronary heart disease in patients with non-alcoholic fatty liver disease in the Han Chinese population. Zhonghua Gan Zang Bing Za Zhi 2021, 29, 1095–1100. [Google Scholar] [CrossRef]
- Lin, R.; Lei, Y.; Yuan, Z.; Ju, H.; Li, D. Angiotensinogen gene M235T and T174M polymorphisms and susceptibility of pre-eclampsia: A meta-analysis. Ann. Hum. Genet 2012, 76, 377–386. [Google Scholar] [CrossRef]
- Lee, S.R.; Moon, J.Y.; Lee, S.H.; Ihm, C.G.; Lee, T.W.; Kim, S.K.; Chung, J.H.; Kang, S.W.; Kim, T.H.; Park, S.J. Angiotensinogen Polymorphisms and Post-Transplantation Diabetes Mellitus in Korean Renal Transplant Subjects. Kidney Blood Press. Res. 2013, 37, 95–102. [Google Scholar] [CrossRef]
- El-Garawani, I.M.; Shaheen, E.M.; El-Seedi, H.R.; Khalifa, S.A.M.; Mersal, G.A.M.; Emara, M.M.; Kasemy, Z.A. Angiotensinogen Gene Missense Polymorphisms (rs699 and rs4762): The Association of End-Stage Renal Failure Risk with Type 2 Diabetes and Hypertension in Egyptians. Genes 2021, 12, 339. [Google Scholar] [CrossRef]
- Perdomo-Pantoja, A.; Mejía-Pérez, S.I.; Reynoso-Noverón, N.; Gómez-Flores-Ramos, L.; Soto-Reyes, E.; Sánchez-Correa, T.E.; Guerra-Calderas, L.; Castro-Hernandez, C.; Vidal-Millán, S.; Sánchez-Corona, J.; et al. Angiotensinogen rs5050 germline genetic variant as potential biomarker of poor prognosis in astrocytoma. PLoS ONE 2018, 13, e0206590. [Google Scholar] [CrossRef]
- Liu, Y.; Fu, L.; Pi, L.; Che, D.; Xu, Y.; Zheng, H.; Long, H.; Zeng, L.; Huang, P.; Zhang, L.; et al. An Angiotensinogen Gene Polymorphism (rs5050) Is Associated with the Risk of Coronary Artery Aneurysm in Southern Chinese Children with Kawasaki Disease. Dis. Markers 2019, 2849695. [Google Scholar] [CrossRef]
- Mopidevi, B.; Ponnala, M.; Kumar, A. Human angiotensinogen +11525 C/A polymorphism modulates its gene expression through microRNA binding. Physiol. Genom. 2013, 45, 901–906. [Google Scholar] [CrossRef]
- Wu, Y.; Wang, M.; Zhang, J.; Sun, N.; Li, C. A new model of the mechanism underlying lead poisoning: SNP in miRNA target region influence the AGT expression level. Hereditas 2019, 156, 6. [Google Scholar] [CrossRef]
- Yang, Y.; Le Ray, I.; Zhu, J.; Zhang, J.; Hua, J.; Reilly, M. Preeclampsia Prevalence, Risk Factors, and Pregnancy Outcomes in Sweden and China. JAMA Netw. Open 2021, 4, e218401. [Google Scholar] [CrossRef]
- Zhang, N.; Tan, J.; Yang, H.; Khalil, R.A. Comparative risks and predictors of preeclamptic pregnancy in the Eastern, Western and developing world. Biochem. Pharmacol. 2020, 182, 114247. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).