The Efficacy of Strength Exercises for Reducing the Symptoms of Menopause: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol and Registry
2.2. Study Design
2.3. Source Data and Search Strategy
2.4. Study Screening: Inclusion and Exclusion Criteria
2.5. Data Extraction
2.6. Risk-of-Bias Tool
3. Results
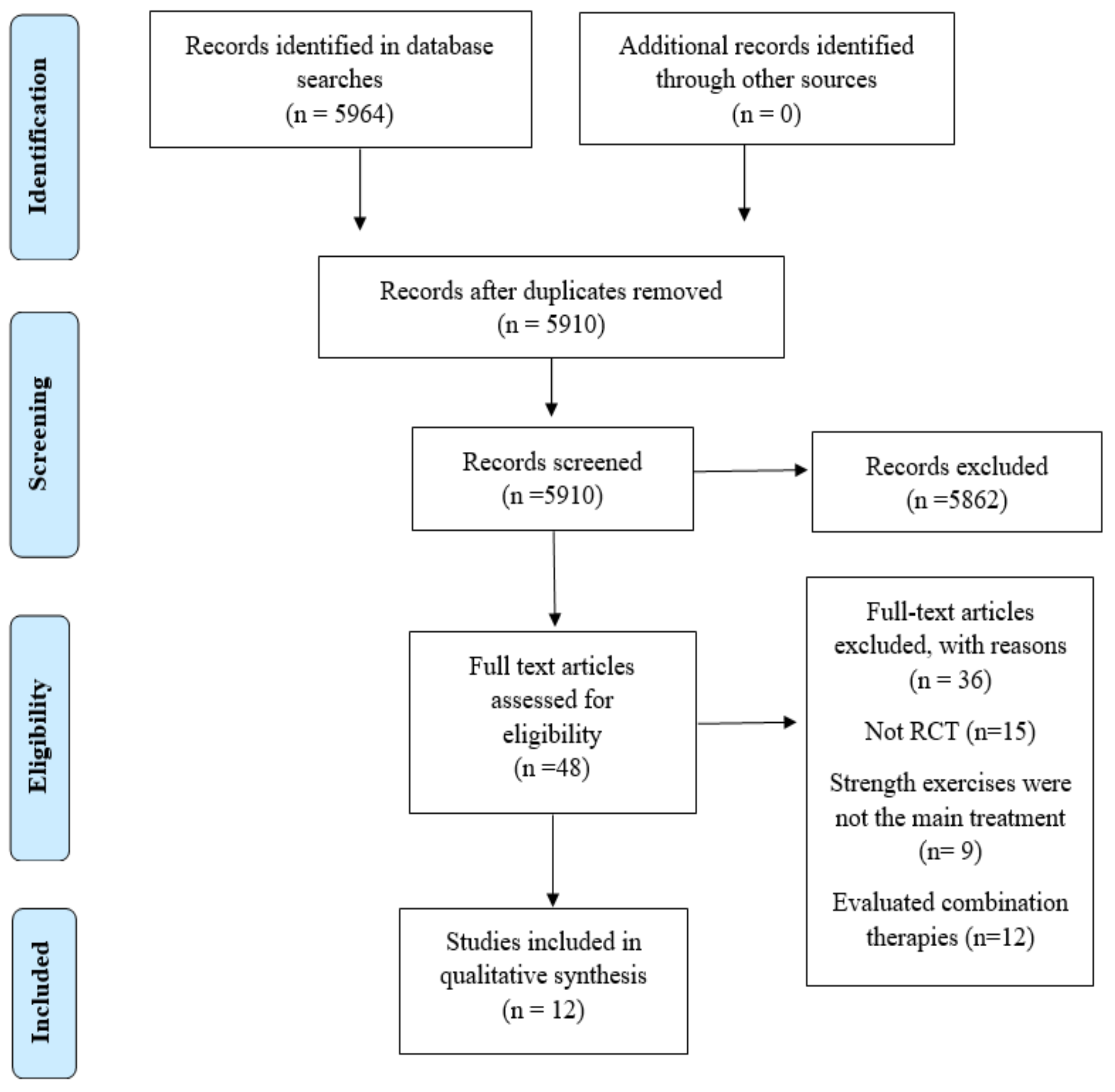
3.1. Search Results
3.2. Characteristics of the Included Studies
3.3. Characteristics of the Strength Exercises in the Included Studies
3.4. Methodological Quality of the Included Studies
3.5. Results of the Included Studies
3.5.1. Strength
3.5.2. Physical Activity
3.5.3. Bone Density
3.5.4. Hormonal and Metabolic Changes
3.5.5. Other Variables Analyzed
4. Discussion
4.1. Summary of Evidence
4.2. Agreements or Disagreements with Other Studies or Reviews
4.3. Limitations and Strengths of the Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Harlow, S.D.; Gass, M.; Hall, J.E.; Lobo, R.; Maki, P.; Rebar, R.W.; Sherman, S.; Sluss, P.M.; de Villiers, T.J. Executive summary of the stages of reproductive aging workshop + 10: Addressing the unfinished agenda of staging reproductive aging. J. Clin. Endocrinol. Metab. 2012, 97, 1159–1168. [Google Scholar] [CrossRef] [PubMed]
- Torres-Jiménex, A.P.; Torres-Rincón, J.M. Climaterio y menopausia. Rev. Fac. Med. UNAM 2018, 61, 51–58. [Google Scholar]
- Blümel, J.E.; Hernández, J.A.; Motta, E. Age at menopause in Latin America. Menopause 2006, 13, 706–712. [Google Scholar] [CrossRef] [PubMed]
- Guyton, A.C.; Hall, J.E. Fisiología Médica, 12th ed.; Elsevier: Barcelona, Spain, 2011; pp. 987–1002. [Google Scholar]
- Lumsden, M.A.; Davies, M.; Sarri, G. Diagnosis and management of menopause: The national institute of health and care excellence (NICE) guideline. JAMA Intern. Med. 2016, 176, 1205–1206. [Google Scholar] [CrossRef] [PubMed]
- Freeman, E.W.; Sammel, M.D.; Lin, H.; Gracia, C.R.; Pien, G.W.; Nelson, D.B.; Sheng, L. Symptoms associated with menopausal transition and reproductive hormones in midlife women. Obstet. Gynecol. 2007, 110, 230–240. [Google Scholar] [CrossRef]
- Berin, E.; Hammar, M.; Lindblom, H.; Lindh-Åstrand, L.; Rubér, M.; Spetz Holm, A.-C. Resistance training for hot flushes in postmenopausal women: A randomised controlled trial. Maturitas 2019, 126, 55–60. [Google Scholar] [CrossRef]
- Hunter, M.S.; Gentry-Maharaj, A.; Ryan, A.; Burnell, M.; Lanceley, A.; Fraser, L.; Jacobs, I.; Menon, U. Prevalence, frequency and problem rating of hot flushes persist in older postmenopausal women: Impact of age, body mass index, hysterectomy, hormone therapy use, lifestyle and mood in a cross-sectional cohort study of 10 418 British women aged 54–65. BJOG 2011, 119, 40–50. [Google Scholar] [CrossRef]
- Daly, R.M.; Via, J.D.; Duckham, R.L.; Fraser, S.F.; Helge, E.W. Exercise for the prevention of osteoporosis in postmenopausal women: An evidence-based guide to the optimal prescription. Braz. J. Phys. Ther. 2019, 23, 170–180. [Google Scholar] [CrossRef]
- Rang, H.; Dale, M. Farmacología, 6th ed.; Elsevier: Barcelona, Spain, 2008; pp. 445–461. [Google Scholar]
- Pinkerton, J.V.; Sánchez-Aguirre, F.; Blake, J.; Cosman, F.; Nodis, H.N.; Hoffstetter, S.; Kaunitz, A.M.; Kingsberg, S.A.; Maki, P.M.; Manson, J.E.; et al. The NAMS 2017 hormone therapy position statement of the North American menopause society. Menopause 2017, 24, 728–753. [Google Scholar]
- Berin, E.; Hammar, M.; Lindblom, H.; Lindh-Åstrand, L.; Rubér, M.; Spetz Holm, A.-C. Resistance training for hot flushes in postmenopausal women: Randomized controlled trial protocol. Maturitas 2016, 85, 96–103. [Google Scholar] [CrossRef]
- MacLennan, A.H.; Broadbent, J.L.; Lester, S.; Moore, V. Oral oestrogen and combined oestrogen/progestogen therapy versus placebo for hot fluses (Review). Cochrane Database Syst. Rev. 2004, 2004, 2978. [Google Scholar]
- Li, W.-C.; Chen, Y.-C.; Yang, R.-S.; Tsauo, J.-Y. Effects of exercise programmes on quality of life in osteoporotic and osteopenic postmenopausal women: A systematic review and meta-analysis. Clin. Rehabil. 2009, 23, 888–896. [Google Scholar] [CrossRef] [PubMed]
- Hakestad, K.A.; Torstveit, M.K.; Nordsletten, L.; Risberg, M.A. Effect of exercises with weight vests and a patient education programme for women with osteopenia and a healed wrist fracture: A randomized, controlled trial of the OsteoACTIVE programme. BMC Musculoskelet. Disord. 2015, 16, 352–361. [Google Scholar] [CrossRef] [PubMed]
- Kahn, K.; McKay, H.; Kannus, R.; Bailey, D.; Wark, J.; Bennel, K. Physical Activity and Bone Health, 1st ed.; Human Kinetics: Champaign, IL, USA, 2001; pp. 1–288. [Google Scholar]
- Wardlaw, S.L.; Wehrenberg, W.B.; Ferin, M.; Antunes, J.L.; Frantz, A.G. Effect of sex steroids on beta-endorphin in hypophyseal portal blood. J. Clin. Endocrinol. Metab. 1982, 55, 877–881. [Google Scholar] [CrossRef] [PubMed]
- Urrútia, G.; Bonfill, X. Declaración prisma: Una propuesta para mejorar la publicación de revisiones sistemáticas y metaanálisis. Med. Clin. 2010, 135, 507–511. [Google Scholar] [CrossRef] [PubMed]
- Almeida, M.O.; Yamato, T.P.; Parreira, P.D.C.S.; Costa, L.O.P.; Kamper, S.; Saragiotto, B.T. Overall confidence in the results of systematic reviews on exercise therapy for chronic low back pain: A cross-sectional analysis using the assessing the methodological quality of systematic reviews (AMSTAR) 2 tool. Braz. J. Phys. Ther. 2020, 24, 103–117. [Google Scholar] [CrossRef]
- Da Costa-Santos, M.; Andrucioli de Mattos-Pimenta, C.; Cuce-Nobre, M.R. The PICO strategy for the research question construction and evidence search. Rev. Lat. Am. Enfermagen. 2007, 15, 3. [Google Scholar]
- Higgins, J.P.T.; Altman, D.G.; Gøtzche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savović, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.C. The Cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, 5928. [Google Scholar] [CrossRef]
- Hartley, C.; Folland, J.P.; Kerslake, R.; Brooke-Wavell, K. High-impact exercise increased femoral neck bone density with no adverse effects on imaging markers of knee osteoarthritis in postmenopausal women. J. Bone Miner. Res. 2020, 35, 53–63. [Google Scholar] [CrossRef]
- Son, W.-M.; Pekas, E.J.; Park, S.-Y. Twelve weeks of resistance band exercise training improves age-associated hormonal decline, blood pressure, and body composition in postmenopausal women with stage 1 hypertension: A randomized clinical trial. Menopause 2020, 27, 199–207. [Google Scholar] [CrossRef]
- Bittar, S.T.; Maeda, S.S.; Marone, M.M.S.; Santili, C. Physical exercises with free weights and elastic bands can improve body composition parameters in postmenopausal women: WEB protocol with a randomized controlled trial. Menopause 2016, 23, 383–389. [Google Scholar] [CrossRef]
- Prado-Nunes, P.R.; Corrêa-Barcelos, L.; Alves-Oliveira, A.; Furlanetto-Júnior, R.; Martins, F.M.; Lera-Orsatti, C.; Resende, E.A.M.R.; Lera-Orsatti, F. Effect of resistance training on muscular strength and indicators of abdominal adiposity, metabolic risk, and inflammation in postmenopausal women: Controlled and randomized clinical trial of efficacy of training volume. AGE 2016, 38, 40. [Google Scholar] [CrossRef]
- Martinho, N.M.; Silva, V.R.; Marques, J.; Carvalho, L.C.; Iunes, D.H.; Botelho, S. The effects of training by virtual reality or gym ball on pelvic floor muscle strength in postmenopausal women: A randomized controlled trial. Braz. J. Phys. Ther. 2016, 20, 248–257. [Google Scholar] [CrossRef]
- Multanen, J.; Rantalainen, T.; Kautiainen, H.; Ahola, R.; Jämsa, T.; Nieminen, M.T.; Lammentausta, E.; Häkkinen, A.; Kiviranta, I.; Heinonen, A. Effect of progressive high-impact exercise on femoral neck structural strength in postmenopausal women with mild knee osteoarthritis: A 12-month RCT. Osteoporos. Int. 2017, 28, 1323–1333. [Google Scholar] [CrossRef]
- Ganderton, C.; Semciw, A.; Cook, J.; Moreira, E.; Pizzari, T. Gluteal loading versus sham exercises to improve pain and dysfunction in postmenopausal women with greater trochanteric pain syndrome: A randomized controlled trial. J. Women Health 2018, 27, 6. [Google Scholar] [CrossRef]
- Watson, S.L.; Weeks, B.K.; Weis, L.J.; Harding, A.T.; Horan, S.A.; Beck, B.R. High-intensity resistance and impact training improves bone mineral density and physical function in postmenopausal women with osteopenia and osteoporosis: The LIFTMOR randomized controlled trial. J. Bone Miner. Res. 2018, 33, 211–220. [Google Scholar] [CrossRef]
- Nunes, R.P.P.; Barcelos, L.C.; Oliveira, A.A.; Furnaletto, R.; Martins, F.M.; Resende, E.A.M.R.; Lera-Orsatti, F. Muscular strength adaptations and hormonal responses after two different multiple-set protocols of resistance training in postmenopausal women. J. Strength Cond. Res. 2017, 33, 1276–1285. [Google Scholar] [CrossRef]
- Watson, S.L.; Weeks, B.K.; Weis, L.J.; Harding, A.T.; Horan, S.A.; Beck, B.R. High-intensity exercise did not cause vertebral fractures and improves thoracic kyphosis in postmenopausal women with low to very low bone mass: The LIFTMOR trial. Osteoporos. Int. 2019, 30, 957–964. [Google Scholar] [CrossRef]
- Fernandes, M.L.D.; de Oliveira, M.L.; Lirani-Galvão, A.P.; Marin-Mio, R.V.; dos Santos, R.N.; Lazaretti-Castro, M. Physical exercise and osteoporosis: Effects of different types of exercises on bone and physical function of postmenopausal women. Arq. Bras. Endocrinol. Metabol. 2014, 58, 514–522. [Google Scholar]
- Shojaa, M.; von-Stengel, S.; Kohl, M.; Schoene, D.; Kemmler, W. Effects of dynamic resistance exercise on bone mineral density in postmenopausal women: A systematic review and meta-analysis with special emphasis on exercise parameters. Osteoporos. Int. 2020, 31, 1427–1444. [Google Scholar] [CrossRef]
- Howe, T.E.; Shea, B.; Dawson, L.J.; Downie, F.; Murray, A.; Ross, C.; Harbour, R.; Caldwell, L.; Creed, G. Exercise for preventing and treating osteoporosis in postmenopausal women. Cochrane Database Syst. Rev. 2011, 7, CD000333. [Google Scholar] [CrossRef] [PubMed]
- Martyn-St. James, M.; Caroll, S. High intensity resistance training and postmenopausal bone loss: A meta-analysis. Osteoporos. Int. 2006, 17, 1225–1240. [Google Scholar] [CrossRef] [PubMed]
- Elley, G.A.; Kelley, K.S.; Tran, Z.V. Resistance training and bone mineral density in women: A meta-analysis of controlled trials. Am. J. Phys. Med. Rehabil. 2001, 80, 65–77. [Google Scholar]
- Zhao, R.; Zhang, M.; Zhang, Q. The effectiveness of combined exercise interventions for preventing postmenopausal bone loss: A systematic review and meta-analysis. J. Orthop. Sports Phys. Ther. 2017, 47, 241–251. [Google Scholar] [CrossRef] [PubMed]
- Atapattu, P.M.; Fernando, D.; Wasalathanthri, S.; de Silva, A. Menopause and exercise: Linking pathophysiology to effects. Arch. Med. 2015, 28, 1–8. [Google Scholar]
- Sternfeld, B.; Dugan, S. Physical activity and health during the menopausal transition. Obstet. Gynecol. Clin. N. Am. 2011, 38, 537–566. [Google Scholar] [CrossRef] [PubMed]
- Cramer, H.; Peng, W.; Lauche, R. Yoga for menopausal symptoms: A systematic review and meta-analysis. Maturias 2018, 109, 13–25. [Google Scholar] [CrossRef] [PubMed]
- Daley, A.; Stokes-Lampard, H.; Thomas, A.; MacArthur, C. Exercise for vasomotor menopausal symptoms. Cochrane Database Syst. Rev. 2014, 11, CD006108. [Google Scholar] [CrossRef]
- Hoga, L.; Rodolpho, J.; Goncalves, B.; Quirino, B. Women’s experience of menopause: A systematic review of qualitative evidence. JBI Database Syst. Rev. Implement. Rep. 2015, 13, 250–337. [Google Scholar] [CrossRef]
- Nguyen, T.M.; Do, T.T.T.; Tran, T.N.; Kim, J.H. Exercise and quality of life in women with menopausal symptoms: A systematic review and meta-analysis of randomized controlled trials. Int. J. Environ. Res. Public Health 2020, 17, 7049. [Google Scholar] [CrossRef]
| Study | Country | Funding | Sample Size | Mean Age | Attrition | Diagnosis | Duration | Intervention | Outcome Measures | Results |
|---|---|---|---|---|---|---|---|---|---|---|
| Berin, E. et al., 2019 [7] | Sweden | Yes | N = 58 EG = 29 CG = 29 | 55.3 | NR | Postmenopausal women ≥12 months amenorrhea | 15 weeks | EG = R (three times/week, with 225 min as the maximum exercise per week). CG = no intervention | Moderate to severe change in heart rate. HF change. Change between HF and minutes of physical activity. Physical activity tolerance (IPAQ) | The moderate to severe heart failure decreased more in EG than in CG (difference of means: −2.7, 95% CI −4.2–−1.3). The mean percentage reduction was −43.6% (−56.0–−31.3) in EG versus no change in CG. |
| Hakestad, K.A. et al., 2015 [15] | Norway | Yes | N = 194 EG = 42 CG = 38 | 64.7 | NR | Postmenopausal women with low BMD + fracture of healed wrist > 2 years | 6 months | EG = ST + EQ CG = no intervention. Two group sessions and one at home (each 1 h) a week. | Quadricep strength (dynamometer). Body anthropometry (BMI). Absolute mass, % fat and BMD (DXA). Dynamic balance (FSST). Ability to walk (6 min walk test). Physical activity level (PASE). Quality of life (SF-36). | The means calculated for the EG improved or were stable during the follow-up, except for the reduction in right quadricep strength and the BMD in the lumbar spine and femoral trochanter. For CG, the mean values decreased during the follow-up, except for some of the variables for quadricep strength. There were no significant differences between the two groups during the 1-year follow-up for any of the outcome measures. |
| Hartley, C. et al., 2020 [22] | United Kingdom | Yes | N = 42 EG = 21 CG = 21 | 61.7 | NR | Postmenopausal women ≥12 months amenorrhea | 6 months | EG: EL CG: CL Both <15 min/day. One session/day. | BMD, BMC and femoral neck Z (DXA) Biochemical composition of the cartilage joint and associated disease with OA (magnetic resonance imaging—T2 relaxometry). | The BMD of the femoral neck, BMC and Z increased in EG (+0.81%, +0.69% and +3.18%, respectively) compared with CG (−0.57%, −0.71% and −0.75%: all interaction effects p < 0.05). There was no overall effect given that the mean T2 relaxation time (principal effect of time p = 0.011) did not differ between EL and CL. |
| Son, W.M. et al., 2020 [23] | South Korea | No | N = 20 EG = 10 CG = 10 | 67.7 | NR | Postmenopausal women ≥12 months amenorrhea and stage 1 hypertension | 12 weeks | EG = ERB CG = no intervention. Both three times/week for 60 min/session. | Values for estradiol, GH, IGF-1, DHEA-S (blood sample), BP (automatic sphygmomanometer), body mass, % body fat and lean body mass (anthropometry and bioelectrical impedance). | Significant group changes by time (p < 0.05) for estradiol, GH, IGF-1, DHEA-S and lean body mass, which increased significantly (p < 0.05), and systolic blood pressure, total body mass, body mass index and % body fat, which decreased significantly (p < 0.05) in EG, compared with no change in CG. There were no significant differences (p > 0.05) in diastolic blood pressure after 12 weeks. |
| Bittar, S.T. et al., 2015 [24] | Brazil | No | N = 60 EG = 30 CG = 30 | 67.3 | G1 = 14 G2 = 12 | Postmenopausal women >12 months | 12 months | EG = SE (1 h, two times/week). CG = HE (two times/week). | BMD (DXA). Body composition, fat and lean mass (absorptiometry). | EG exhibited increased lean mass in the arms (p = 0.003) and legs (p = 0.011), total lean tissue (p = 0.015) and appendicular lean mass index (p = 0.001) compared with the baseline. CG showed no differences in lean mass. |
| Prado-Nunes, P.R. et al., 2016 [25] | Brazil | Yes | N = 32 CG= 13 EG1 = 13 EG2 = 12 | 61.3 | 6 | Postmenopausal women >12 months. FSH >40 mUl/mL | 16 weeks | CG = S (two times/week). EG1 = LV (three times/week). EG2 = HV (three times/week). | Leg extension strength (dynamometer). Body anthropometry (measuring tape, adipometer). Metabolic and inflammatory indicators (blood test). | EG2 experienced a reduction in total cholesterol and a smaller change in IL-6 compared with G1 (11.2% (P25–75, −7.6–28.4%) vs. 99.55% (P25–75 = 18.5–377.0%) for G3 and G1, respectively; p = 0.049) EG1 experienced a reduction in the percentage of HbA1c. There were positive correlations between WHR and IL-6 and between IL-6 and total cholesterol. |
| Martinho, N.M. et al., 2016 [26] | Brazil | Yes | N = 47 EG = 27 CG = 20 | 61.4 | NR | Postmenopausal women >12 months | 5 weeks | EG = RV. CG = M, S, ST and RE Both 30 min, two times/week. | SP strength (vaginal palpation and dynamometer) | There were no significant differences between the groups in most of the analyzed parameters. The muscle resistance was increased in EG (p = 0.003; effect size, 0.89; difference of means, 1.37; 95% CI 0.46–2.28). |
| Multanem, J. et al., 2017 [27] | Finland | No | N = 80 EG = 40 CG = 40 | 58.3 | 4 | Postmenopausal women with knee pain in recent days | 12 weeks | EG = leaps (three times/week, lasting 55 min). CG = no intervention. | Bone strength (femoral neck scanner). Knee cartilage (scanner). Physical activity (body movement monitors). Aerobic exercise load (number and intensity of leaps). Quality of life (SF-36). | Significant difference between the groups in the strength of the femoral neck flexion in favor of EG at 12 months (p < 0.01). The change in resistance to the femoral neck flexion remained significant after adjusting the baseline value, age, height and body mass (p = 0.020). In all participants, the change in resistance to flexion was associated with the total physical activity load (p = 0.012). EG had no effect on knee cartilage composition. |
| Ganderton, C. et al., 2018 [28] | Australia | Yes | N = 94 EG = 46 CG = 48 | 61. 8 | NR | Postmenopausal women >52 weeks of amenorrhea with trochanteric pain | 52 weeks | EG = strengthening exercise program. GLoBE + HE CG = e.g., simulated + HE Both 12 weeks | Gluteal tendon pain (VISA-G questionnaire). Perceived improvement in hip dysfunction (OHS and global rating of change). Quality of life (AQoL). Hip dysfunction and osteoarthritis (HOOS and lateral hip questionnaire). | EG achieved a significantly higher score in VISA-G, HOOS, OHS and lateral hip pain compared with CG. However, the intent-to-treat analysis showed no differences between the groups. There were no differences between the groups in the global rating of change at 12 (p = 0.340) and 52 weeks (p = 0.746). There was a significant improvement in the VISA-G score for both groups at 12 and 52 weeks (p < 0.001). |
| Watson, S.L. et al., 2018 [29] | Australia | No | N = 101 EG = 49 CG = 52 | 65 | NR | Postmenopausal women with low bone mass | 8 months | EG = W+ R CG = HE Both twice a week for 30 min. | Physical activity level (IPAQ). Daily calcium intake (AusCal). FN and LS BMD (DXA). Dominant or nondominant heels (QUS). Leg extension strength (dynamometer). Leg neuromuscular performance (maximum vertical leap test in a force plate). | Largest effects in EG for LS-BMD (2.9% and 2.8% vs. −1.2% and 2.8%, p < 0.001), FN-BMD (0.3% and 2.6% vs. −1.9% and 2.6%, p = 0.004), FN cortical thickness (13.6 16.6% vs. 6.3% and 16.6%, p = 0.014), height (0.2 and 0.5 cm versus −0.2, 0.2 and 0.5 cm p = 0.004) and all the performance measurements (p < 0.001). |
| Nunes, R.P.P. et al., 2019 [30] | Brazil | Yes | N = 38 CG = 13 EG1 = 13 EG2 = 12 | 60.9 | NR | Postmenopausal women ≥12 month amenorrhea + FSH >40 mIU·mL−1 + E2 ≤54.7 pg·mL−1 | 16 weeks | CG = control. No RT, only S two times/week. EG1 = W+ LV + E; 45 min x three times/week. EG2 = W+ HV + E; 90 min x three times/week. | Strength performance (maximum strength test). Dietary intake E, CHO, LIP, PTN (food record). DHEA- S, TT, CO, TT:CO, IGF- 1 (blood sample). | EG1 and EG2 increased the performance of 1RM in all exercises compared with CG. There were no differences in strength performance between EG1 and EG2, except with the bar curl, which only increased in EG1. EG1 and EG2 increased the lean mass compared with CG (CG = 0.8 (95% CI 20.1–1.8) kg; EG1 = 2.2 (95% CI 1.7–2.7) kg; EG2 = 2.4 (95% CI 1.2–3.6) kg; p ANOVA = 0.037). There were no differences for the food intake and hormonal responses. |
| Watson, S.L. et al., 2019 [31] | Australia | NR | N = 51 EG = 25 CG = 26 | 64 | NR | Postmenopausal women with low bone mass | 8 months | EG = W+ R. CG = HE. Both twice a week for 30 min. | Magnitude of kyphosis (DXA, inclinometer and flexicurve) | EG obtained a high reduction in thoracic kyphosis in standing compared with G2 (−6.7 ± 8.2° vs. −1.6 ± 8.1°, p = 0.031). The two groups achieved an improvement within the group in kyphosis in the relaxed position, measured by the inclinometer and flexicurve (p < 0.05). There were no changes in the classification of vertebral fractures in EG after the intervention. |
| Study | Type | Material | Time/Session | Series | Repetitions | Repetition Time | Supervised |
|---|---|---|---|---|---|---|---|
| Berin, E. et al., 2019 [7] | C+ chest press, leg press, rowing, F leg, pulldown, E leg, abdominals and E of back + dynamic and static stretching | Physical fitness machines | 225 min/week as the maximum (7–10 min of C+ stretching) | 2 | 8–12 | NR | Yes |
| Hakestad, K.A. et al., 2015 [15] | F, E and W exercises. | Weighted vest | 60 min | NR | NR | NR | NR |
| Hartley, C. et al., 2020 [22] | W+ Leap with a single unilateral leg. | NR | 8–9 min (C- 5 min + 3 or 4 min leap) | 5 (15 s rest between series) | 10 | NR | Yes |
| Son, W.M. et al., 2020 [23] | W+ R (rowing, biceps curl, F shoulder, flexing, FE hip, heel raising, squats) + Cool down | Elastic band | 60 min (40 min R) | 1–4 weeks: 2–3 series (40–50% of 1RM). 5–8 weeks: 2–3 series (50–60% of 1RM). 9–12 weeks: 3–4 series (60–70% of 1RM). | 1–4 weeks: 11–12 reps 5–8 weeks: 13–14 reps 9–12 weeks: 15–16 reps | NR | Yes |
| Bittar, S.T. et al., 2015 [24] | W+ impact exercises with fast walking with active movement of the arms and/or step exercises on a treadmill + R for arms, legs and abdomen + e.g., recreational exercises with a ball and a massage. | Elastic bands + improvised weights | 60 min (10 min W, 20–25 min impact exercises with walking, 20–25 min R and 5 min, e.g., recreational exercises with a ball and a massage). | R—3 | W (2 reps) R (10 reps) | W (20 s) | Yes |
| Prado- Nunes, P.R. et al., 2016 [25] | W+ Squats, F legs, E arms, bench press, rowing, pull down, triceps pulley and flexing with bar. | Physical fitness machines | NR | In W, 1 series exercise; in G1, 3 series (with 1.5 min between series) or in G3, 6 series. | W (15 reps) Exercise (8–12 reps) | W (40% of 1RM) Exercise (70% of 1RM) | Yes |
| Martinho, N.M. et al., 2016 [26] | Pelvic movements, maintaining control and trunk stabilization, with abdominal activation. | Virtual reality | 30 min | 4 (games) | 1 | 5 min | Yes |
| Multanem, J. et al., 2017 [27] | Leap exercises with change in direction with music. | NR | 55 min | NR | NR | NR | Yes |
| Ganderton, C. et al., 2018 [28] | Isometric load gluteus medius and minimus + strengthening of quadriceps and calves. | Chair as a safety measure | NR | 2–4 | 5–15 | 40 s | Yes |
| Watson, S.L. et al., 2018 [29] | W (dead weight) + R (dead weight, air pressure and squats) | Physical fitness machines | 30 min | W—2 R—5 | W—5 (50–70% of 1RM) W—5 (> 80–85% of 1RM) | NR | Yes |
| Nunes, R.P.P. et al., 2019 [30] | W+ squats, leg curl, leg extension, bench press, rowing, pull down, bar curl, triceps pulley + S | Physical fitness machines | EG1 = 45 min EG2 = 90 min. | W = 1 series (40% of 1RM). EG1 = 3 series (70% of 1RM). EG2 = 6 series (70% of 1RM). | W = 15 reps. EG1 = 8–12 reps. EG2 = 8–12 reps. | NR | Yes |
| Watson, S.L. et al., 2019 [31] | R progressive (low load, dead weight, bench press and back squats) + CI (dominated with leaps) | Physical fitness machines | 30 min | 5 | 5 (80–85% of 1RM) | NR | Yes |
| Study | Criteria | |||||||
|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | |
| Berin, E. et al., 2019 [7] | Low | Low | High | Low | Low | Low | Low | Low |
| Hakestad, K.A. et al., 2015 [15] | Low | Low | Low | Low | Low | Low | Low | Low |
| Hartley, C. et al., 2020 [22] | High | Low | Low | Low | Low | Low | Low | Low |
| Son, W.M. et al., 2020 [23] | Low | Low | Low | High | Low | Low | Low | Low |
| Bittar, S.T. et al., 2015 [24] | Low | High | High | High | Low | Low | Low | Unclear |
| Prado- Nunes, P.R. et al., 2016 [25] | High | High | High | High | Low | Low | Low | High |
| Martinho, N.M. et al., 2016 [26] | Low | Low | Low | High | Low | Low | Low | Low |
| Multanem, J. et al., 2017 [27] | Low | High | Low | High | Low | Low | Low | Low |
| Ganderton, C. et al., 2018 [28] | Low | High | Low | Low | Low | Low | Low | Low |
| Watson, S.L. et al., 2018 [29] | Low | Low | High | High | Low | Low | Low | Unclear |
| Nunes, R.P.P. et al., 2019 [30] | High | High | High | High | Low | Low | Low | High |
| Watson, S.L. et al., 2019 [31] | Low | Low | High | High | High | Low | Low | Unclear |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Capel-Alcaraz, A.M.; García-López, H.; Castro-Sánchez, A.M.; Fernández-Sánchez, M.; Lara-Palomo, I.C. The Efficacy of Strength Exercises for Reducing the Symptoms of Menopause: A Systematic Review. J. Clin. Med. 2023, 12, 548. https://doi.org/10.3390/jcm12020548
Capel-Alcaraz AM, García-López H, Castro-Sánchez AM, Fernández-Sánchez M, Lara-Palomo IC. The Efficacy of Strength Exercises for Reducing the Symptoms of Menopause: A Systematic Review. Journal of Clinical Medicine. 2023; 12(2):548. https://doi.org/10.3390/jcm12020548
Chicago/Turabian StyleCapel-Alcaraz, Ana María, Héctor García-López, Adelaida María Castro-Sánchez, Manuel Fernández-Sánchez, and Inmaculada Carmen Lara-Palomo. 2023. "The Efficacy of Strength Exercises for Reducing the Symptoms of Menopause: A Systematic Review" Journal of Clinical Medicine 12, no. 2: 548. https://doi.org/10.3390/jcm12020548
APA StyleCapel-Alcaraz, A. M., García-López, H., Castro-Sánchez, A. M., Fernández-Sánchez, M., & Lara-Palomo, I. C. (2023). The Efficacy of Strength Exercises for Reducing the Symptoms of Menopause: A Systematic Review. Journal of Clinical Medicine, 12(2), 548. https://doi.org/10.3390/jcm12020548





