How to Enable Participation until the End of Life? A Survey of German Occupational Therapists Working in Palliative Care
Abstract
1. Introduction
- -
- What is the involvement/integration of occupational therapy in palliative care?
- -
- In which areas do occupational therapists work with palliative care patients?
- -
- What specific roles do occupational therapists play in palliative care?
- -
- What is the perceived need for research or continuing education for occupational therapists in palliative care according to these participants?
2. Methods
2.1. Questionnaire Design
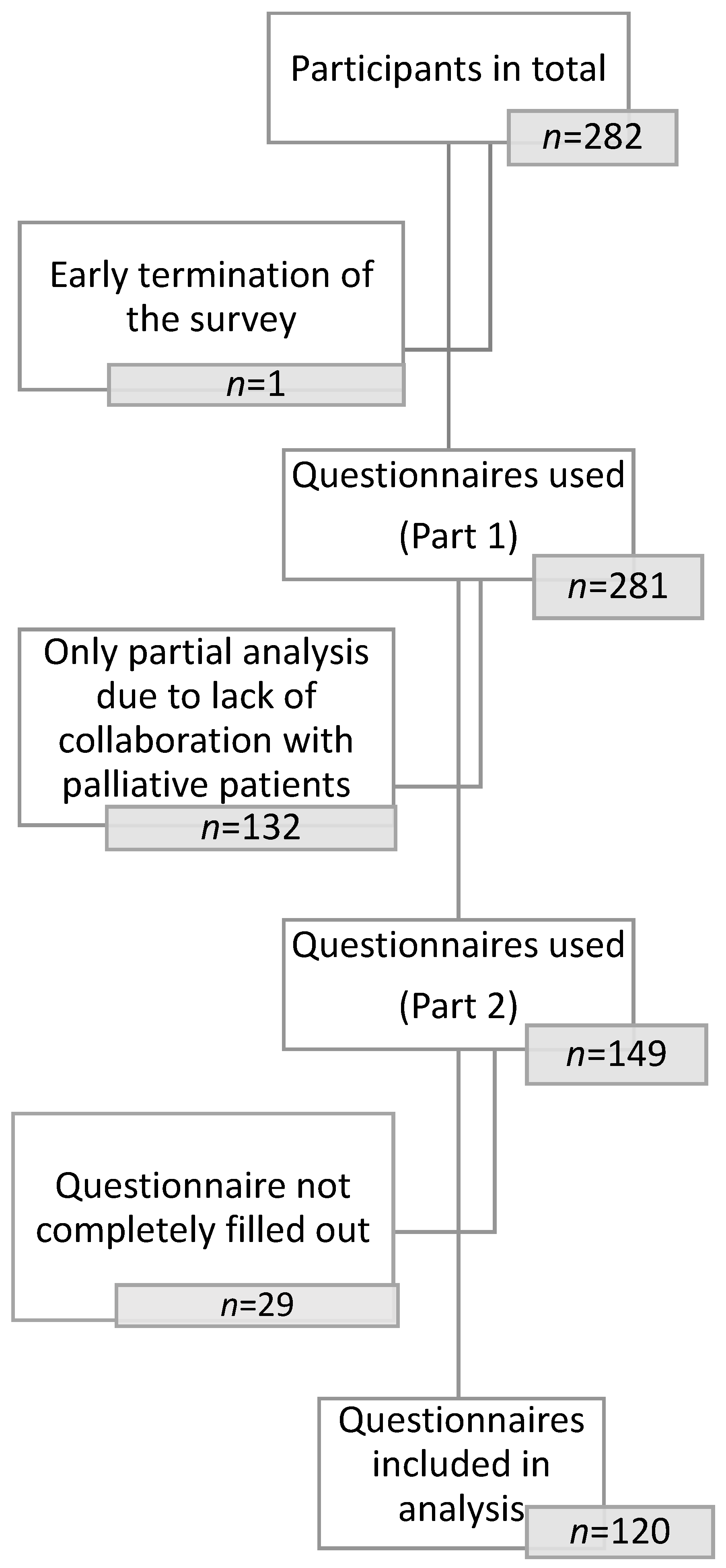
2.2. Sampling and Recruitment
2.3. Data Analysis
3. Results
3.1. Respondent Characteristics
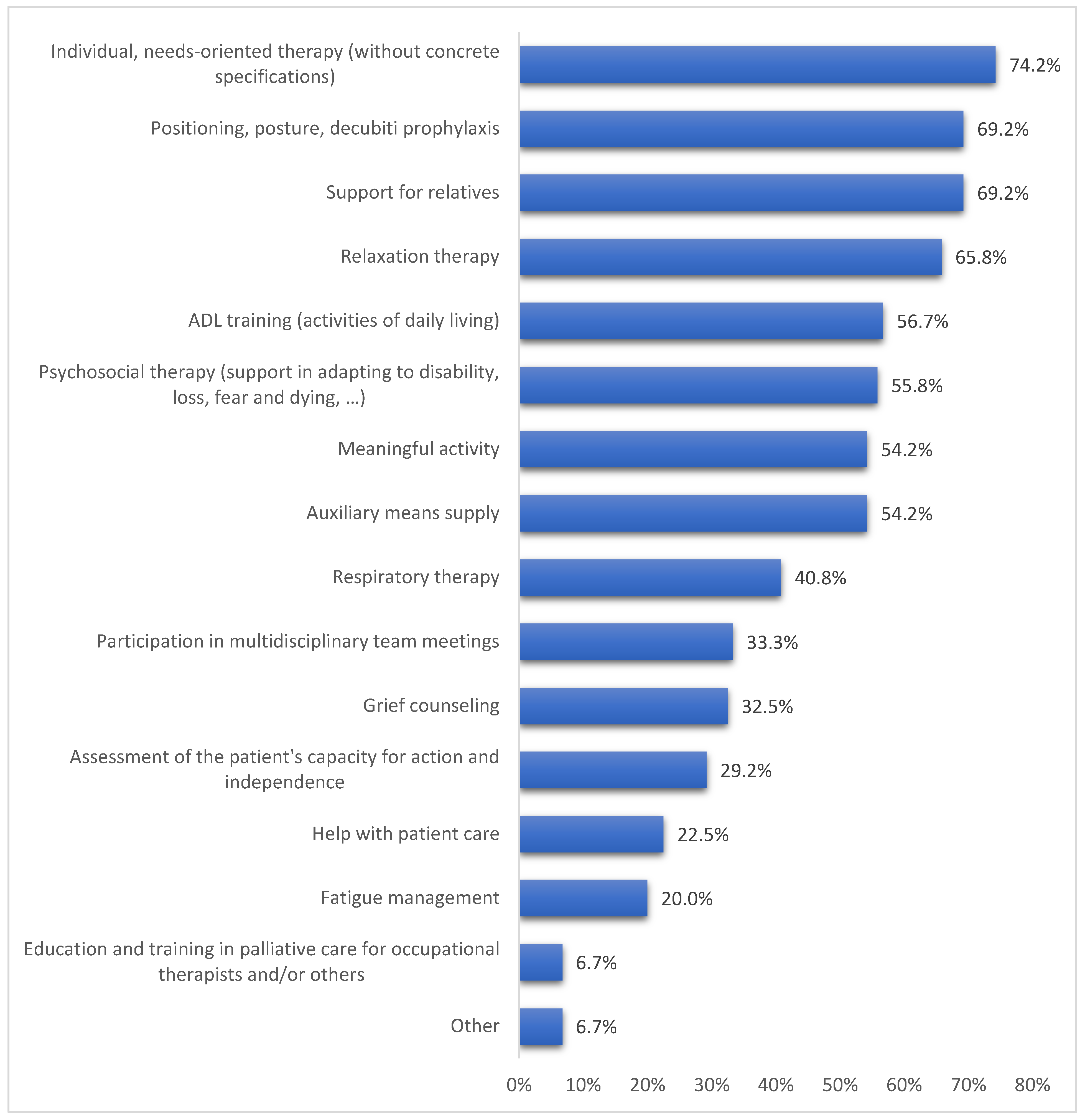
3.2. Fields of Application and Tasks of Palliative Occupational Therapy
3.3. Free-Text Responses
3.4. Topic I: One’s Role in Palliative Care
“I think it’s important to enable quality of life through activity, regardless of the threat of end of life.”(R-130)
“No different than in other areas of occupational therapy. We support everyday life or the management of it. We enable participation in it. Our banner says: ‘everyday life’.”(R-238)
“Occupational therapy care is of great importance to patients. It covers many areas, involves time, can reduce fears and is of great benefit due to the professional competence. Unfortunately, it still lacks recognition by other professions or among physicians...”(R-77)
“It has been my experience that to some primary care physicians and specialists, the expertise of occupational therapists in palliative care is not present nor seems significant, so some clients or their families have to “fight” for prescriptions.”(R-23)
“I try to do everything within my power as a therapist to help the patient do as much as I can. Whether it’s going for walks, cooking, baking, playing games, laughing, reminiscing, massage, relaxation exercises or movement exercises. The tasks are as varied and different as each patient is different.”(R-51)
3.5. Topic II: Stressful Situations
“Related to ignorance among other health care professionals: The constant justification for the work done as well as explanation of the profession. The term “meaningful” is very vague and not certainly tangible to others. This weighs on me. Regarding palliative work with clients, unfortunately we are often only called in at a very late stage, although we could already make a valuable contribution to the participation of the clients at an earlier stage. This is often very frustrating and also stressful when you know that you could have enabled more participation with quite simple redesigns/adaptations of the environment.”(R-281)
3.6. Topic III: Utilization of Occupational Therapy Expertise
“Ignorance regarding the variety of tasks of occupational therapy often hinders its adequate use in palliative care. For example, it is often assumed that occupational therapists can only ‘tinker’ and have no expertise in caring for palliative clientele. Facilitating meaningful activity is a tenet of occupational therapy that is elusive for many. Because of this, we often experience a fundamental problem with our profession, that no one really knows what occupational therapists actually do. Occupational therapy expertise is a very suitable therapy method in palliative care by enabling participation until death—it is just unfortunately considered far too rarely.”(R-281)
“Clearly that would be the responsibility of the medical supply stores, but so far I haven’t found any that would do extensive consultation. I see us as coordinators who would have to build a network or fit into a network so that optimal care for the patient takes place.”(R-254)
“The world doesn’t know about our expertise. Neither doctors nor nurses. Maybe even we ourselves don’t.”(R-238)
“It needs a clearly formulated and delimited task, which corresponds to the occupational therapy and is so also mediatable.”(R-77)
“More intensive attention to this area already in training. Continuing education opportunities.”(R-31)
3.7. Topic IV: Opportunities for Improvement
“Occupational therapy is often not considered in the provision of care. Getting us on board early on, we could accomplish even more....”(R-213)
“As well as basically occupational therapy is not self-explanatory, in palliative care is a lot of knowledge transfer about occupational therapy necessary. Public relations work, participation in the DGP, networking with the regional hospices/palliative care units, updating the existing information material of the DVE”(R-243)
3.8. What Occupational Therapists Who Do Not Work in Palliative Care Think about Palliative Work
4. Discussion
4.1. Significance of the Findings
4.2. Limitations of This Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Peoples, H.; Nissen, N.; Brandt, Å.; la Cour, K. Perceptions of quality of life by people with advanced cancer who live at home. Br. J. Occup. Ther. 2021, 84, 723–730. [Google Scholar] [CrossRef]
- Eriksson, L.; Öster, I.; Lindberg, M. The meaning of occupation for patients in palliative care when in hospital. Palliat Support Care 2016, 14, 541–552. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Deutscher Verband Ergotherapie e.V. Definition-Deutscher Verband Ergotherapie e.V. (DVE). Available online: https://dve.info/ergotherapie/definition (accessed on 30 January 2023).
- Radbruch, L.; SA, P. White paper on standards and norms for hospice and palliative care in Europe: Part 1. Eur. J. Palliat. Care 2010, 17, 22–33. [Google Scholar]
- Pape, A.E.; Gschnell, M.; Maul, J.; Volberg, C. Physio- und Ergotherapie in der deutschen Palliativmedizin–wo stehen wir? Z. Für Evidenz Fortbild. Und Qual. Im Gesundheitswesen 2022, 175, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Eva, G.; Morgan, D. Mapping the scope of occupational therapy practice in palliative care: A European Association for Palliative Care cross-sectional survey. Palliat. Med. 2018, 32, 960–968. [Google Scholar] [CrossRef] [PubMed]
- Statista. Anzahl der Sozialversicherungspflichtig Beschäftigten Ergotherapeuten in Deutschland in den Jahren von 2012 bis 2021. Statista. 2021. Available online: https://de.statista.com/statistik/daten/studie/520504/umfrage/anzahl-beschaeftigter-ergotherapeuten-in-deutschland/ (accessed on 30 January 2023).
- Deutscher Verband Ergotherapie e.V. Ergotherapie in Deutschland Zahlen. Daten. Fakten. 2020, unpublished work. [Google Scholar]
- Halkett, G.; Ciccarelli, M.; Keesing, S.; Aoun, S. Occupational therapy in palliative care: Is it under-utilised in Western Australia? Aust. Occup. Ther. J. 2010, 57, 301–309. [Google Scholar] [CrossRef] [PubMed]
- Hammill, K.; Bye, R.; Cook, C. Workforce profile of Australian occupational therapists working with people who are terminally ill. Aust. Occup. Ther. J. 2017, 64, 58–67. [Google Scholar] [CrossRef] [PubMed]
- Hammill, K.; Bye, R.; Cook, C. Occupational engagement of people living with a life-limiting illness: Occupational therapists’ perceptions. Aust. Occup. Ther. J. 2019, 66, 145–153. [Google Scholar] [CrossRef] [PubMed]
- Pitzen, K.M. Occupational Therapy and Palliative Care: A Survey of Attitudes and Knowledge. 2009. Available online: https://www.semanticscholar.org/paper/Occupational-therapy-and-palliative-care-%3A-a-survey-Pitzen/02d2026c2ff0f7bdf37253bcb8937ac7ee9f2d92 (accessed on 27 February 2023).
- OTAL Occupational Therapy Australia Ltd. Position Statement: Occupational therapy in palliative care. Aust. Occup. Ther. J. 2015, 62, 459–461. [Google Scholar] [CrossRef] [PubMed]
- Dando, N.; d’Avray, L.; Colman, J.; Hoy, A.; Todd, J. Evaluation of an interprofessional practice placement in a UK in-patient palliative care unit. Palliat. Med. 2012, 26, 178–184. [Google Scholar] [CrossRef] [PubMed]
- Palliativversorgung-Deutscher Verband Ergotherapie e.V. (DVE). Available online: https://dve.info/ergotherapie/fachbereiche/palliativversorgung (accessed on 27 February 2023).
- Townsend, E.A. Enabling Occupation: An Occupational Therapy Perspective; Canadian Association of Occupational Therapists: Ottawa, ON, Canada, 1997. [Google Scholar]
- Aitken, A.M. Gemeindenahe Palliative Care: Die Rolle der Pflegeexpertin in der ambulanten Palliative Care; 1. Auflage; Hogrefe AG: Berne, Switzerland, 2012. [Google Scholar]
- Blichfeldt, M.; Gregersen Oestergaard, L.; Sampedro Pilegaard, M.; La Cour, K.; Lindahl-Jacobsen, L. Occupational performance and prioritized problematic everyday occupations among people with advanced cancer living alone versus living with someone. Scand. J. Occup. Ther. 2023, 30, 703–713. [Google Scholar] [CrossRef] [PubMed]
- Vachon, M.L. Staff stress in hospice/palliative care: A review. Palliat. Med. 1995, 9, 91–122. [Google Scholar] [CrossRef] [PubMed]
- Chow, J.K.; Pickens, N.D.; Fletcher, T.; Bowyer, P.; Thompson, M. Missed Opportunities to Ease Suffering: An Explanatory Model of Occupational Therapy Utilization in End-of-Life Care. Am. J. Hosp. Palliat. Care 2022, 104990912211439. [Google Scholar] [CrossRef] [PubMed]
- Rexe, K.; Lammi, B.M.; von Zweck, C. Occupational therapy: Cost-effective solutions for changing health system needs. Healthc. Q. 2013, 16, 69–75. [Google Scholar] [PubMed]
- Chow, J.; Pickens, N. Measuring the Efficacy of Occupational Therapy in End-of-Life Care: A Scoping Review. Am. J. Occup. Ther. 2020, 74, 7401205020p1–7401205020p14. [Google Scholar] [CrossRef] [PubMed]
| n = 281 | Percentage | ||
|---|---|---|---|
| Gender | Female | 258 | 92.1 |
| Male | 19 | 6.7 | |
| Divers | 3 | 1.0 | |
| Age (years) | <25 | 51 | 18.1 |
| 25–35 | 78 | 27.7 | |
| 36–45 | 66 | 23.4 | |
| 46–55 | 53 | 18.5 | |
| >55 | 34 | 12.1 | |
| Qualifications | Currently in training/studying | 67 | 23.9 |
| Completed vocational training | 174 | 62.1 | |
| Bachelor’s degree | 32 | 11.4 | |
| Master’s degree | 9 | 3.2 | |
| Others | 16 | 5.7 | |
| Working with Palliative clients | Yes | 149 | 53.0 |
| No | 132 | 47.0 |
| n = 120 | Percentage | ||
|---|---|---|---|
| Number of years working with palliative clients | <5 | 47 | 39.1 |
| 6–10 | 37 | 30.8 | |
| 11–20 | 31 | 25.8 | |
| 21–30 | 4 | 3.3 | |
| >30 | 1 | 0.8 | |
| Primary collaboration | Children/adolescents | 10 | 8.3 |
| Adults | 62 | 51.6 | |
| Older people (>65 years) | 94 | 78.3 | |
| Employment relationship | Part-time employed | 41 | 34.1 |
| Full-time employed | 34 | 28.3 | |
| Self-employed | 42 | 35.0 | |
| Voluntary work | 6 | 5.0 | |
| Other | 5 | 4.1 | |
| Working area | Clinic (outside a palliative care unit) | 40 | 33.3 |
| Palliative care unit | 24 | 20.0 | |
| Hospice | 5 | 4.1 | |
| Specialized outpatient palliative care team | 5 | 4.1 | |
| Medical practice | 46 | 38.3 | |
| Home visits (outside specialized palliative care) | 60 | 50.0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Volberg, C.; Fleck, P.; Vradelis, P.; Morin, A.; Gschnell, M.; Pape, A.E. How to Enable Participation until the End of Life? A Survey of German Occupational Therapists Working in Palliative Care. J. Clin. Med. 2023, 12, 5257. https://doi.org/10.3390/jcm12165257
Volberg C, Fleck P, Vradelis P, Morin A, Gschnell M, Pape AE. How to Enable Participation until the End of Life? A Survey of German Occupational Therapists Working in Palliative Care. Journal of Clinical Medicine. 2023; 12(16):5257. https://doi.org/10.3390/jcm12165257
Chicago/Turabian StyleVolberg, Christian, Pauline Fleck, Paula Vradelis, Astrid Morin, Martin Gschnell, and Anna Elisabeth Pape. 2023. "How to Enable Participation until the End of Life? A Survey of German Occupational Therapists Working in Palliative Care" Journal of Clinical Medicine 12, no. 16: 5257. https://doi.org/10.3390/jcm12165257
APA StyleVolberg, C., Fleck, P., Vradelis, P., Morin, A., Gschnell, M., & Pape, A. E. (2023). How to Enable Participation until the End of Life? A Survey of German Occupational Therapists Working in Palliative Care. Journal of Clinical Medicine, 12(16), 5257. https://doi.org/10.3390/jcm12165257






