Delay Discounting in Gambling Disorder: Implications in Treatment Outcome
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Procedure
2.3. Baseline Assessment
2.3.1. Delay Discounting Task
2.3.2. Gambling Disorder Diagnosis and Severity
2.3.3. Impulsive Behavior Scale (UPPS-P)
2.3.4. Temperament and Character Inventory-Revised (TCI-R)
2.3.5. Symptom Checklist-Revised (SCL-90-R)
2.3.6. Other Sociodemographic and Clinical Variables
2.4. Statistical Analysis
3. Results
3.1. Characteristics of the Sample
3.2. Association between Delay Discounting and Clinical Profile at Baseline
3.3. Association between Delay Discounting and CBT Outcomes at Baseline
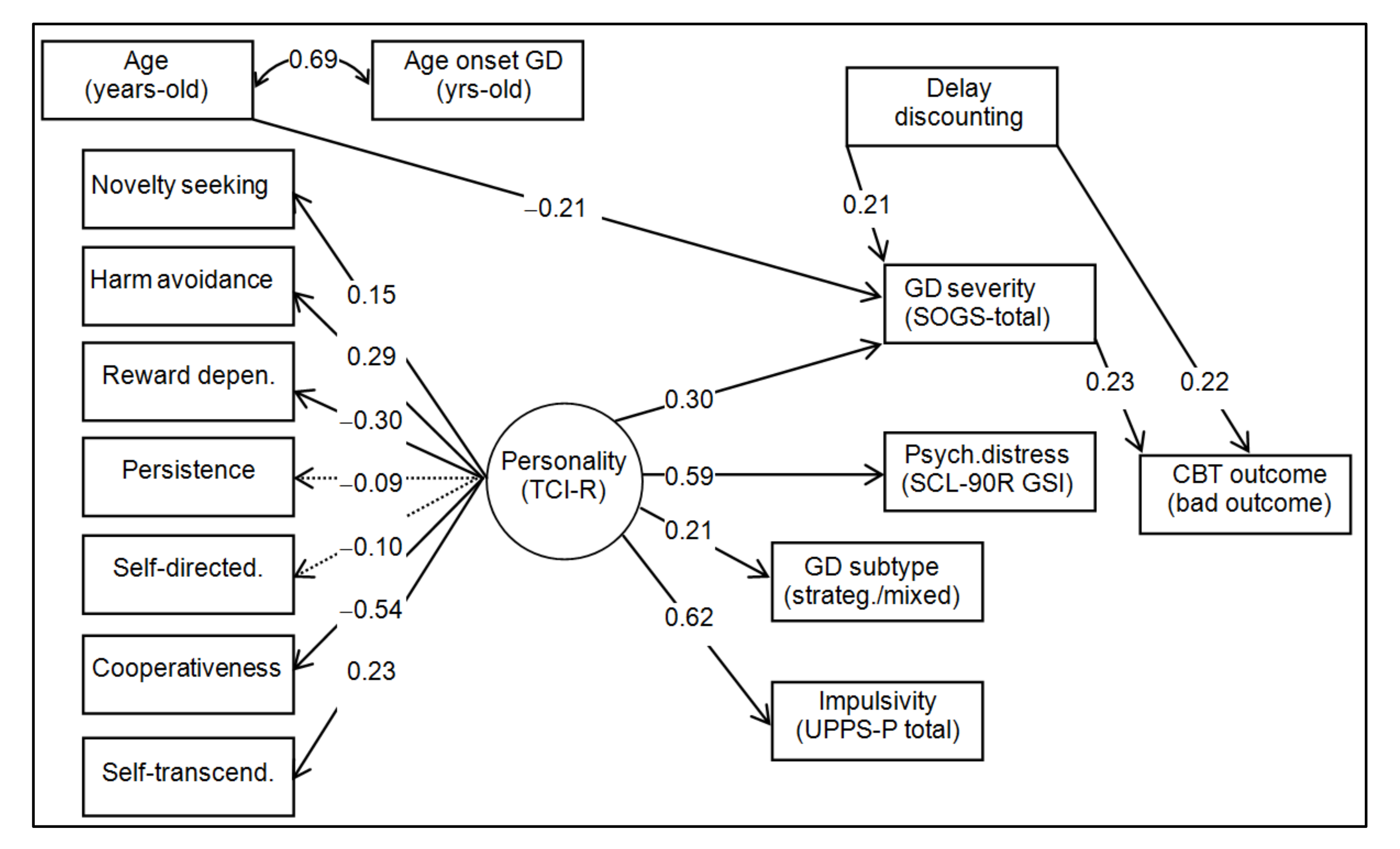
3.4. Path-Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Calado, F.; Griffiths, M.D. Problem gambling worldwide: An update and systematic review of empirical research (2000–2015). J. Behav. Addict. 2016, 5, 592. [Google Scholar] [CrossRef] [PubMed]
- Granero, R.; Penelo, E.; Stinchfield, R.; Fernandez-Aranda, F.; Savvidou, L.G.; Fröberg, F.; Aymamí, N.; Gómez-Peña, M.; Pérez-Serrano, M.; del Pino-Gutiérrez, A.; et al. Is Pathological Gambling Moderated by Age? J. Gambl. Stud. 2013, 30, 475–492. [Google Scholar] [CrossRef] [PubMed]
- Di Nicola, M.; Ferri, V.R.; Moccia, L.; Panaccione, I.; Strangio, A.M.; Tedeschi, D.; Grandinetti, P.; Callea, A.; de-Giorgio, F.; Martinotti, G.; et al. Gender differences and psychopathological features associated with addictive behaviors in adolescents. Front. Psychiatry 2017, 8, 256. [Google Scholar] [CrossRef] [PubMed]
- Subramaniam, M.; Wang, P.; Soh, P.; Vaingankar, J.A.; Chong, S.A.; Browning, C.J.; Thomas, S.A. Prevalence and determinants of gambling disorder among older adults: A systematic review. Addict. Behav. 2015, 41, 199–209. [Google Scholar] [CrossRef] [PubMed]
- Granero, R.; Penelo, E.; Martínez-Giménez, R.; Álvarez-Moya, E.; Gómez-Peña, M.; Aymamí, M.N.; Bueno, B.; Fernández-Aranda, F.; Jiménez-Murcia, S. Sex differences among treatment-seeking adult pathologic gamblers. Compr. Psychiatry 2009, 50, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Lee, R.S.C.; Hoppenbrouwers, S.; Franken, I. A Systematic Meta-Review of Impulsivity and Compulsivity in Addictive Behaviors. Neuropsychol. Rev. 2019, 29, 14–26. [Google Scholar] [CrossRef] [PubMed]
- Rømer Thomsen, K.; Buhl Callesen, M.; Hesse, M.; Lehmann Kvamme, T.; Mulbjerg Pedersen, M.; Uffe Pedersen, M.; Voon, V. Impulsivity traits and addiction-related behaviors in youth. J. Behav. Addict. 2018, 7, 317–330. [Google Scholar] [CrossRef]
- Tiego, J.; Oostermeijer, S.; Prochazkova, L.; Parkes, L.; Dawson, A.; Youssef, G.; Oldenhof, E.; Carter, A.; Segrave, R.A.; Fontenelle, L.F.; et al. Overlapping dimensional phenotypes of impulsivity and compulsivity explain co-occurrence of addictive and related behaviors. CNS Spectr. 2019, 24, 426–440. [Google Scholar] [CrossRef] [PubMed]
- Engel, A.; Cáceda, R. Can Decision Making Research Provide a Better Understanding of Chemical and Behavioral Addictions? Curr. Drug Abuse Rev. 2015, 8, 75–85. [Google Scholar] [CrossRef]
- Del Pino-Gutiérrez, A.; Jiménez-Murcia, S.; Fernández-Aranda, F.; Agüera, Z.; Granero, R.; Hakansson, A.; Fagundo, A.B.; Bolao, F.; Valdepérez, A.; Mestre-Bach, G.; et al. The relevance of personality traits in impulsivity-related disorders: From substance use disorders and gambling disorder to bulimia nervosa. J. Behav. Addict. 2017, 6, 396–405. [Google Scholar] [CrossRef]
- Rochat, L.; Billieux, J.; Gagnon, J.; Van der Linden, M. A multifactorial and integrative approach to impulsivity in neuropsychology: Insights from the UPPS model of impulsivity. J. Clin. Exp. Neuropsychol. 2018, 40, 45–61. [Google Scholar] [CrossRef] [PubMed]
- MacKillop, J.; Weafer, J.; Gray, J.C.; Oshri, A.; Palmer, A.; de Wit, H. The latent structure of impulsivity: Impulsive choice, impulsive action, and impulsive personality traits. Psychopharmacology 2016, 233, 3361–3370. [Google Scholar] [CrossRef] [PubMed]
- Evenden, J. Impulsivity: A discussion of clinical and experimental findings. J. Psychopharmacol. 1999, 13, 180–192. [Google Scholar] [CrossRef] [PubMed]
- Whiteside, S.P.; Lynam, D.R.; Miller, J.D.; Reynolds, S.K. Validation of the UPPS impulsive behaviour scale: A four-factor model of impulsivity. Eur. J. Pers. 2005, 19, 559–574. [Google Scholar] [CrossRef]
- Amlung, M.; Vedelago, L.; Acker, J.; Balodis, I.; MacKillop, J. Steep delay discounting and addictive behavior: A meta-analysis of continuous associations. Addiction 2017, 112, 51–62. [Google Scholar] [CrossRef]
- Kirby, K.N.; Petry, N.M.; Bickel, W.K. Heroin addicts have higher discount rates for delayed rewards than non-drug-using controls. J. Exp. Psychol. Gen. 1999, 128, 78–87. [Google Scholar] [CrossRef]
- Lempert, K.M.; Steinglass, J.E.; Pinto, A.; Kable, J.W.; Simpson, H.B. Can delay discounting deliver on the promise of RDoC? Psychol. Med. 2019, 49, 190–199. [Google Scholar] [CrossRef]
- De Wit, H. Impulsivity as a determinant and consequence of drug use: A review of underlying processes. Addict. Biol. 2009, 14, 22–31. [Google Scholar] [CrossRef]
- Albein-Urios, N.; Martinez-González, J.M.; Lozano, Ó.; Verdejo-Garcia, A. Monetary delay discounting in gambling and cocaine dependence with personality comorbidities. Addict. Behav. 2014, 39, 1658–1662. [Google Scholar] [CrossRef]
- Dixon, M.R.; Marley, J.; Jacobs, E.A. Delay discounting by pathological gamblers. J. Appl. Behav. Anal. 2003, 36, 449. [Google Scholar] [CrossRef]
- Krmpotich, T.; Mikulich-Gilbertson, S.; Sakai, J.; Thompson, L.; Banich, M.T.; Tanabe, J. Impaired decision-making, higher impulsivity, and drug severity in substance dependence and pathological gambling. J. Addict. Med. 2015, 9, 273. [Google Scholar] [CrossRef] [PubMed]
- Petry, N.M. Pathological gamblers, with and without substance use disorders, discount delayed rewards at high rates. J. Abnorm. Psychol. 2001, 110, 482–487. [Google Scholar] [CrossRef] [PubMed]
- Weinsztok, S.; Brassard, S.; Balodis, I.; Martin, L.E.; Amlung, M. Delay Discounting in Established and Proposed Behavioral Addictions: A Systematic Review and Meta-Analysis. Front. Behav. Neurosci. 2021, 15. [Google Scholar] [CrossRef]
- Alessi, S.M.; Petry, N.M. Pathological gambling severity is associated with impulsivity in a delay discounting procedure. Behav. Processes 2003, 64, 345–354. [Google Scholar] [CrossRef]
- Kräplin, A.; Dshemuchadse, M.; Behrendt, S.; Scherbaum, S.; Goschke, T.; Bühringer, G. Dysfunctional decision-making in pathological gambling: Pattern specificity and the role of impulsivity. Psychiatry Res. 2014, 215, 675–682. [Google Scholar] [CrossRef]
- Steward, T.; Mestre-Bach, G.; Fernández-Aranda, F.; Granero, R.; Perales, J.C.; Navas, J.F.; Soriano-Mas, C.; Baño, M.; Fernández-Formoso, J.A.; Martín-Romera, V.; et al. Delay discounting and impulsivity traits in young and older gambling disorder patients. Addict. Behav. 2017, 71, 96–103. [Google Scholar] [CrossRef] [PubMed]
- Michalczuk, R.; Bowden-Jones, H.; Verdejo-Garcia, A.; Clark, L. Impulsivity and cognitive distortions in pathological gamblers attending the UK National Problem Gambling Clinic: A preliminary report. Psychol. Med. 2011, 41, 2625–2635. [Google Scholar] [CrossRef] [PubMed]
- Canale, N.; Vieno, A.; Griffiths, M.D.; Rubaltelli, E.; Santinello, M. Trait urgency and gambling problems in young people by age: The mediating role of decision-making processes. Addict. Behav. 2015, 46, 39–44. [Google Scholar] [CrossRef]
- Álvarez-Moya, E.M.; Jimenez-Murcia, S.; Granero, R.; Vallejo, J.; Krug, I.; Bulik, C.M.; Fernández-Aranda, F. Comparison of personality risk factors in bulimia nervosa and pathological gambling. Compr. Psychiatry 2007, 48, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Janiri, L.; Martinotti, G.; Dario, T.; Schifano, F.; Bria, P. The Gamblers’ Temperament and Character Inventory (TCI) personality profile. Subst. Use Misuse 2007, 42, 975–984. [Google Scholar] [CrossRef]
- Jiménez-Murcia, S.; Granero, R.; Stinchfield, R.; Fernández-Aranda, F.; Penelo, E.; Savvidou, L.G.; Fröberg, F.; Aymamí, N.; Gómez-Peña, M.; Moragas, L.; et al. Typologies of young pathological gamblers based on sociodemographic and clinical characteristics. Compr. Psychiatry 2013, 54, 1153–1160. [Google Scholar] [CrossRef][Green Version]
- Cowlishaw, S.; Merkouris, S.; Dowling, N.; Anderson, C.; Jackson, A.; Thomas, S. Psychological therapies for pathological and problem gambling. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Petry, N.M.; Ginley, M.K.; Rash, C.J. A systematic review of treatments for problem gambling. Psychol. Addict. Behav. 2017, 31, 951–961. [Google Scholar] [CrossRef] [PubMed]
- Di Nicola, M.; De Crescenzo, F.; D’Alò, G.L.; Remondi, C.; Panaccione, I.; Moccia, L.; Molinaro, M.; Dattoli, L.; Lauriola, A.; Martinelli, S.; et al. Pharmacological and Psychosocial Treatment of Adults with Gambling Disorder: A Meta-Review. J. Addict. Med. 2020, 14, e15–e23. [Google Scholar] [CrossRef]
- Mallorquí-Bagué, N.; Vintró-Alcaraz, C.; Verdejo-García, A.; Granero, R.; Fernández-Aranda, F.; Magaña, P.; Mena-Moreno, T.; Aymamí, N.; Gómez-Peña, M.; Del Pino-Gutiérrez, A.; et al. Impulsivity and cognitive distortions in different clinical phenotypes of gambling disorder: Profiles and longitudinal prediction of treatment outcomes. Eur. Psychiatry 2019, 61, 9–16. [Google Scholar] [CrossRef]
- Leblond, J.; Ladouceur, R.; Blaszczynski, A. Which pathological gamblers will complete treatment? Br. J. Clin. Psychol. 2003, 42, 205–209. [Google Scholar] [CrossRef] [PubMed]
- Maccallum, F.; Blaszczynski, A.; Ladouceur, R.; Nower, L. Functional and dysfunctional impulsivity in pathological gambling. Pers. Individ. Dif. 2007, 43, 1829–1838. [Google Scholar] [CrossRef]
- Knezevic-Budisin, B.; Pedden, V.; White, A.; Miller, C.J.; Hoaken, P.N.S. A multifactorial conceptualization of impulsivity: Implications for research and clinical practice. J. Individ. Differ. 2015, 36, 191–198. [Google Scholar] [CrossRef]
- Sharma, L.; Markon, K.E.; Clark, L.A. Toward a theory of distinct types of “impulsive” behaviors: A meta-analysis of self-report and behavioral measures. Psychol. Bull. 2014, 140, 374–408. [Google Scholar] [CrossRef]
- Rizzo, M.F.J.; Navas, J.F.; Steward, T.; López-Gómez, M.; Jiménez-Murcia, S.; Fernández-Aranda, F.; Perales, J.C. Impulsivity and problem awareness predict therapy compliance and dropout from treatment for gambling disorder. Adicciones 2019, 31, 147–159. [Google Scholar] [CrossRef]
- Coughlin, L.N.; Tegge, A.N.; Sheffer, C.E.; Bickel, W.K. A Machine-Learning Approach to Predicting Smoking Cessation Treatment Outcomes. Nicotine Tob. Res. 2020, 22, 415–422. [Google Scholar] [CrossRef]
- Harvanko, A.M.; Strickland, J.C.; Slone, S.A.; Shelton, B.J.; Reynolds, B.A. Dimensions of impulsive behavior: Predicting contingency management treatment outcomes for adolescent smokers. Addict. Behav. 2019, 90, 334–340. [Google Scholar] [CrossRef] [PubMed]
- Loree, A.M.; Lundahl, L.H.; Ledgerwood, D.M. Impulsivity as a predictor of treatment outcome in substance use disorders: Review and synthesis. Drug Alcohol Rev. 2015, 34, 119–134. [Google Scholar] [CrossRef]
- MacKillop, J.; Kahler, C.W. Delayed reward discounting predicts treatment response for heavy drinkers receiving smoking cessation treatment. Drug Alcohol Depend. 2009, 104, 197. [Google Scholar] [CrossRef]
- Sheffer, C.E.; Christensen, D.R.; Landes, R.; Carter, L.P.; Jackson, L.; Bickel, W.K. Delay discounting rates: A strong prognostic indicator of smoking relapse. Addict. Behav. 2014, 39, 1682–1689. [Google Scholar] [CrossRef]
- Petry, N.M. Discounting of probabilistic rewards is associated with gambling abstinence in treatment-seeking pathological gamblers. J. Abnorm. Psychol. 2012, 121, 151–159. [Google Scholar] [CrossRef] [PubMed]
- Jiménez-Murcia, S.; Granero, R.; Fernández-Aranda, F.; Menchón, J.M. Comparison of gambling profiles based on strategic versus non-strategic preferences. Curr. Opin. Behav. Sci. 2020, 31, 13–20. [Google Scholar] [CrossRef]
- Göllner, L.M.; Ballhausen, N.; Kliegel, M.; Forstmeier, S. Delay of gratification, delay discounting and their associations with age, episodic future thinking, and future time perspective. Front. Psychol. 2018, 8, 2304. [Google Scholar] [CrossRef]
- Steinberg, L.; Graham, S.; O’Brien, L.; Woolard, J.; Cauffman, E.; Banich, M. Age differences in future orientation and delay discounting. Child Dev. 2009, 80, 28–44. [Google Scholar] [CrossRef]
- Granero, R.; Fernández-Aranda, F.; Valero-Solís, S.; Del Pinogutiérrez, A.; Mestre-Bach, G.; Baenas, I.; Contaldo, S.F.; Gómez-Peña, M.; Aymamí, N.; Moragas, L.; et al. The influence of chronological age on cognitive biases and impulsivity levels in male patients with gambling disorder. J. Behav. Addict. 2020, 9, 383–400. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Murcia, S.; Aymamí, N.; Gómez-Peña, M.; Álvarez-Moya, E.M.; Vallejo, J. Protocols de Tractament Cognitiu-Conductual pel joc Patològic i D’altres Addiccions no Tòxiques [Cognitive-Behavioral Treatment Protocols for Pathological Gambling and Other Nonsubstance Addictions]; Hospital Universitari de Bellvitge, Departament de Salut, Generalitat de Catalunya: Barcelona, Spain, 2006. [Google Scholar]
- Kirby, K.N.; Maraković, N.N. Delay-discounting probabilistic rewards: Rates decrease as amounts increase. Psychon. Bull. Rev. 1996, 3, 100–104. [Google Scholar] [CrossRef] [PubMed]
- Miranda-Olivos, R.; Steward, T.; Martínez-Zalacaín, I.; Mestre-Bach, G.; Juaneda-Seguí, A.; Jiménez-Murcia, S.; Fernández-Formoso, J.A.; Vilarrasa, N.; Veciana de las Heras, M.; Custal, N.; et al. The neural correlates of delay discounting in obesity and binge eating disorder. J. Behav. Addict. 2021, 10, 498–507. [Google Scholar] [CrossRef] [PubMed]
- Marco-Pallarés, J.; Mohammadi, B.; Samii, A.; Münte, T.F. Brain activations reflect individual discount rates in intertemporal choice. Brain Res. 2010, 1320, 123–129. [Google Scholar] [CrossRef] [PubMed]
- Stinchfield, R. Reliability, validity, and classification accuracy of a measure of DSM-IV diagnostic criteria for pathological gambling. Am. J. Psychiatry 2003, 160, 180–182. [Google Scholar] [CrossRef]
- APA American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders; APA American Psychiatric Association: Washington, DC, USA, 2013. [Google Scholar]
- Pettorruso, M.; Testa, G.; Granero, R.; Martinotti, G.; d’Andrea, G.; di Giannantonio, M.; Fernández-Aranda, F.; Mena-Moreno, T.; Gómez-Peña, M.; Moragas, L.; et al. The transition time to gambling disorder: The roles that age, gambling preference and personality traits play. Addict. Behav. 2021, 116, 106813. [Google Scholar] [CrossRef]
- Jiménez-Murcia, S.; Stinchfield, R.; Álvarez-Moya, E.; Jaurrieta, N.; Bueno, B.; Granero, R.; Aymamí, M.N.; Gómez-Peña, M.; Martínez-Giménez, R.; Fernández-Aranda, F.; et al. Reliability, validity, and classification accuracy of a Spanish translation of a measure of DSM-IV diagnostic criteria for pathological gambling. J. Gambl. Stud. 2009, 25, 93–104. [Google Scholar] [CrossRef]
- Lesieur, H.R.; Blume, S.B. The South Oaks Gambling Screen (SOGS): A new instrument for the identification of Pathological gamblers. Am. J. Psychiatry 1987, 144. [Google Scholar] [CrossRef]
- Echeburúa, E.; Báez, C.; Fernéndez-Montalvo, J.; Páez, D. Cuestionario de juego patológico de South Oaks (SOGS): Validación Española [The South Oaks Gambling Screen (SOGS): Spanish validation]. Análisis y Modif. Conduct. 1994, 20, 769–791. [Google Scholar]
- Verdejo-García, A.; Lozano, Ó.; Moya, M.; Alcázar, M.A.; Pérez-García, M. Psychometric properties of a Spanish version of the UPPS-P impulsive behavior scale: Reliability, validity and association with trait and cognitive impulsivity. J. Pers. Assess. 2010, 92, 70–77. [Google Scholar] [CrossRef]
- Gutiérrez-Zotes, J.A.; Bayón, C.; Montserrat, C.; Valero, J.; Labad, A.; Cloninger, C.R. Temperament and Character Inventory-Revised (TCI-R). Standardization and normative data in a general population sample. Actas Españolas Psiquiatr. 2004, 32, 8–15. [Google Scholar]
- Derogatis, L.R.; Savitz, K.L. The SCL-90-R, Brief Symptom Inventory, and Matching Clinical Rating Scales. In The Use of Psychological Testing for Treatment Planning and Outcomes Assessment, 2nd ed.; Lawrence Erlbaum Associates Publishers: Mahwah, NJ, USA, 1999; pp. 679–724. ISBN 0-8058-2761-7. [Google Scholar]
- Derogatis, L.R. SCL-90-R Cuestionario de 90 Síntomas—Manual.; TEA Editorial: Madrid, Spain, 1994; ISBN 84-7174-714-6. [Google Scholar]
- Stata-Corp. Stata Statistical Software: Release 10; StataCorp LP: College Station, TX, USA, 2007. [Google Scholar]
- Valero-Solís, S.; Granero, R.; Fernández-Aranda, F.; Steward, T.; Mestre-Bach, G.; Mallorquí-Bagué, N.; Martín-Romera, V.; Aymamí, N.; Gómez-Peña, M.; Del Pino-Gutiérrez, A.; et al. The contribution of sex, personality traits, age of onset and disorder duration to behavioral addictions. Front. Psychiatry 2018, 9, 497. [Google Scholar] [CrossRef]
- Petry, N.M. A Comparison of Young, Middle-Aged, and Older Adult Treatment-Seeking Pathological Gamblers. Gerontologist 2002, 42, 92–99. [Google Scholar] [CrossRef] [PubMed]
- Rosnow, R.L.; Rosenthal, R. Computing contrasts, effect sizes, and counternulls on other people’s published data: General procedures for research consumers. Psychol. Methods 1996, 1, 331. [Google Scholar] [CrossRef]
- Mestre-Bach, G.; Steward, T.; Granero, R.; Fernández-Aranda, F.; del Pino-Gutiérrez, A.; Mallorquí-Bagué, N.; Mena-Moreno, T.; Vintró-Alcaraz, C.; Moragas, L.; Aymamí, N.; et al. The predictive capacity of DSM-5 symptom severity and impulsivity on response to cognitive-behavioral therapy for gambling disorder: A 2-year longitudinal study. Eur. Psychiatry 2019, 55, 67–73. [Google Scholar] [CrossRef]
- Stea, J.N.; Hodgins, D.C.; Lambert, M.J. Relations between delay discounting and low to moderate gambling, cannabis, and alcohol problems among university students. Behav. Processes 2011, 88, 202–205. [Google Scholar] [CrossRef] [PubMed]
- Mestre-Bach, G.; Steward, T.; Granero, R.; Fernández-Aranda, F.; Mena-Moreno, T.; Vintró-Alcaraz, C.; Lozano-Madrid, M.; Menchón, J.M.; Potenza, M.N.; Jiménez-Murcia, S. Dimensions of Impulsivity in Gambling Disorder. Sci. Rep. 2020, 10, 397. [Google Scholar] [CrossRef] [PubMed]
- Mestre-Bach, G.; Steward, T.; Granero, R.; Fernández-Aranda, F.; Talón-Navarro, M.T.; Cuquerella, À.; Baño, M.; Moragas, L.; del Pino-Gutiérrez, A.; Aymamí, N.; et al. Gambling and Impulsivity Traits: A Recipe for Criminal Behavior? Front. Psychiatry 2018, 9, 6. [Google Scholar] [CrossRef]
- Jiménez-Murcia, S.; Granero, R.; Fernández-Aranda, F.; Stinchfield, R.; Tremblay, J.; Steward, T.; Mestre-Bach, G.; Lozano-Madrid, M.; Mena-Moreno, T.; Mallorquí-Bagué, N.; et al. Phenotypes in Gambling Disorder Using Sociodemographic and Clinical Clustering Analysis: An Unidentified New Subtype? Front. Psychiatry 2019, 10, 173. [Google Scholar] [CrossRef]
- Cloninger, C.R.; Svrakic, D.M.; Przybeck, T.R. A Psychobiological Model of Temperament and Character. Arch. Gen. Psychiatry 1993, 50. [Google Scholar] [CrossRef]
- Moragas, L.; Granero, R.; Stinchfield, R.; Fernández-Aranda, F.; Fröberg, F.; Aymamí, N.; Gómez-Peña, M.; Fagundo, A.B.; Islam, M.A.; del Pino-Gutiérrez, A.; et al. Comparative analysis of distinct phenotypes in gambling disorder based on gambling preferences. BMC Psychiatry 2015, 15, 86. [Google Scholar] [CrossRef] [PubMed]
- Lévesque, D.; Sévigny, S.; Giroux, I.; Jacques, C. Gambling-Related Cognition Scale (GRCS): Are skills-based games at a disadvantage? Psychol. Addict. Behav. 2017, 31, 647–654. [Google Scholar] [CrossRef]
- Mouneyrac, A.; Lemercier, C.; Le Floch, V.; Challet-Bouju, G.; Moreau, A.; Jacques, C.; Giroux, I. Cognitive Characteristics of Strategic and Non-strategic Gamblers. J. Gambl. Stud. 2018, 34, 199–208. [Google Scholar] [CrossRef] [PubMed]
- Krishnan-Sarin, S.; Reynolds, B.; Duhig, A.M.; Smith, A.; Liss, T.; McFetridge, A.; Cavallo, D.A.; Carroll, K.M.; Potenza, M.N. Behavioral Impulsivity Predicts Treatment Outcome in a Smoking Cessation Program for Adolescent Smokers. Drug Alcohol Depend. 2007, 88, 79. [Google Scholar] [CrossRef]
- Sheffer, C.; MacKillop, J.; McGeary, J.; Landes, R.; Carter, L.; Yi, R.; Jones, B.; Christensen, D.; Stitzer, M.; Jackson, L.; et al. Delay discounting, locus of control, and cognitive impulsiveness independently predict tobacco dependence treatment outcomes in a highly dependent, lower socioeconomic group of smokers. Am. J. Addict. 2012, 21, 221–232. [Google Scholar] [CrossRef] [PubMed]
- Rupp, C.I.; Beck, J.K.; Heinz, A.; Kemmler, G.; Manz, S.; Tempel, K.; Fleischhacker, W.W. Impulsivity and Alcohol Dependence Treatment Completion: Is There a Neurocognitive Risk Factor at Treatment Entry? Alcohol. Clin. Exp. Res. 2016, 40, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Ronzitti, S.; Soldini, E.; Smith, N.; Clerici, M.; Bowden-Jones, H. Gambling Disorder: Exploring Pre-treatment and In-treatment Dropout Predictors. A UK Study. J. Gambl. Stud. 2017, 33, 1277–1292. [Google Scholar] [CrossRef]
- Tárrega, S.; Castro-Carreras, L.; Fernández-Aranda, F.; Granero, R.; Giner-Bartolomé, C.; Aymamí, N.; Gómez-Peña, M.; Santamaría, J.J.; Forcano, L.; Steward, T.; et al. A Serious Videogame as an Additional Therapy Tool for Training Emotional Regulation and Impulsivity Control in Severe Gambling Disorder. Front. Psychol. 2015, 6, 1721. [Google Scholar] [CrossRef]
- Jiménez-Murcia, S.; Granero, R.; Fernández-Aranda, F.; Arcelus, J.; Aymamí, M.N.; Gómez-Peña, M.; Tárrega, S.; Moragas, L.; Del Pino-Gutiérrez, A.; Sauchelli, S.; et al. Predictors of Outcome among Pathological Gamblers Receiving Cognitive Behavioral Group Therapy. Eur. Addict. Res. 2015, 21, 169–178. [Google Scholar] [CrossRef]
- Penelo, E.; Fernández-Aranda, F.; Menchón, J.M.; Granero, R.; Aymamí, N.; Gómezpeña, M.; Moragas, L.; Santamaría, J.J.; Custal, N.; Jiménez-Murcia, S. Comparison between immigrant and Spanish nativeborn pathological gambling patients. Psychol. Rep. 2012, 110, 555–570. [Google Scholar] [CrossRef]
- Potenza, M.N.; Steinberg, M.A.; McLaughlin, S.D.; Wu, R.; Rounsaville, B.J.; O’Malley, S.S. Gender-related differences in the characteristics of problem gamblers using a gambling helpline. Am. J. Psychiatry 2001, 158, 1500–1505. [Google Scholar] [CrossRef] [PubMed]
- Zakiniaeiz, Y.; Cosgrove, K.P.; Mazure, C.M.; Potenza, M.N. Does Telescoping Exist in Male and Female Gamblers? Does It Matter? Front. Psychol. 2017, 8, 1510. [Google Scholar] [CrossRef] [PubMed]
| 1 Group of Age | 2 Gambling Preference | ||||||
|---|---|---|---|---|---|---|---|
| Younger | Middle | Older | Non-Strat | Strategic | Mixed | ||
| 〈 | N = 31 | N = 61 | N = 41 | N = 96 | N = 18 | N = 19 | |
| Age (years-old) | 0.391† | 0.046 | 0.172 | 0.028 | 0.357† | 0.297† | |
| Onset of GD (years-old) | −0.258 † | −0.040 | 0.062 | −0.032 | 0.193 | 0.177 | |
| Duration of GD (years) | 0.527† | 0.039 | −0.078 | 0.051 | 0.056 | 0.152 | |
| Debts due to gambling | 0.113 | −0.009 | 0.066 | 0.038 | −0.007 | −0.213 | |
| DSM-5 criteria for GD | 0.753 | −0.095 | 0.254† | 0.002 | 0.021 | 0.408† | 0.279† |
| SOGS-total | 0.705 | 0.245† | 0.317† | 0.131 | 0.169 | 0.444† | 0.595† |
| SCL-90R GSI | 0.978 | −0.231 | −0.044 | −0.121 | −0.227 | 0.522† | −0.120 |
| SCL-90R PST | 0.978 | −0.151 | 0.039 | −0.057 | −0.138 | 0.533† | 0.060 |
| SCL-90R PSDI | 0.978 | −0.134 | −0.031 | −0.208 | −0.214 | 0.504† | −0.336 † |
| UPPS-P Lack premeditation | 0.802 | −0.132 | 0.112 | 0.133 | 0.032 | 0.251† | 0.459† |
| UPPS-P Lack perseverance | 0.794 | −0.013 | 0.062 | 0.134 | 0.025 | 0.450† | 0.187 |
| UPPS-P Sensation seeking | 0.866 | 0.091 | −0.156 | −0.119 | −0.151 | −0.126 | 0.153 |
| UPPS-P Positive urgency | 0.918 | 0.330† | 0.244† | −0.007 | 0.056 | 0.345† | 0.350† |
| UPPS-P Negative urgency | 0.837 | 0.273† | 0.197 | −0.002 | 0.025 | 0.387† | 0.381† |
| UPPS-P Impulsivity total | 0.918 | 0.224 | 0.141 | 0.013 | −0.009 | 0.344† | 0.526† |
| TCI-R Novelty seeking | 0.707 | 0.048 | −0.068 | 0.092 | 0.039 | 0.105 | −0.092 |
| TCI-R Harm avoidance | 0.708 | −0.173 | 0.240 † | 0.017 | 0.003 | 0.606† | 0.068 |
| TCI-R Reward dependence | 0.704 | 0.148 | −0.122 | −0.040 | 0.001 | −0.223 | −0.078 |
| TCI-R Persistence | 0.877 | −0.087 | −0.221 | −0.187 | −0.161 | −0.431 † | −0.194 |
| TCI-R Self-directedness | 0.819 | −0.176 | −0.133 | −0.023 | 0.009 | −0.557 † | −0.280 † |
| TCI-R Cooperativeness | 0.761 | 0.019 | −0.278 † | −0.232 | −0.181 | −0.450 † | −0.193 |
| TCI-R Self-transcendence | 0.829 | 0.041 | −0.142 | −0.175 | −0.181 | −0.253 † | 0.056 |
| Odds Ratio (OR) | Correlation (R) | |||||
|---|---|---|---|---|---|---|
| Sample Size | Risk Dropout | Risk Relapse | Number Sessions | Number Relapses | Euros Relapses | |
| 1 Groups of age | ||||||
| Younger | 31 | 1.89* | 0.86 | −0.241 † | −0.058 | 0.040 |
| Middle | 61 | 1.37 | 1.59* | −0.160 | 0.133 | 0.101 |
| Older | 41 | 1.41 | 1.26 | −0.153 | 0.074 | −0.010 |
| 2 Gambling preference | ||||||
| Non strategic | 96 | 1.70* | 1.22 | −0.206 | 0.035 | −0.053 |
| Strategic | 18 | 0.62 | 3.01* | 0.207 | 0.425† | 0.255† |
| Mixed | 19 | 4.74* | 1.20 | −0.272 † | −0.082 | 0.220 |
| Dropout | Relapses | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| B | SE | p | OR | 95%CI OR | B | SE | p | OR | 95%CI OR | |||
| Age (years-old) | −0.043 | 0.022 | 0.046* | 0.958 | 0.918 | 0.999 | −0.024 | 0.017 | 0.170 | 0.976 | 0.944 | 1.010 |
| Duration of GD (years) | 0.007 | 0.040 | 0.852 | 1.008 | 0.931 | 1.090 | −0.024 | 0.035 | 0.496 | 0.976 | 0.911 | 1.046 |
| DSM-5 criteria baseline | −0.331 | 0.169 | 0.049* | 0.718 | 0.516 | 0.999 | −0.024 | 0.142 | 0.867 | 0.976 | 0.739 | 1.289 |
| SCL-90R GSI baseline | 0.166 | 0.498 | 0.739 | 1.180 | 0.445 | 3.131 | 0.435 | 0.397 | 0.273 | 1.546 | 0.709 | 3.368 |
| UPPS-P total baseline | 0.007 | 0.013 | 0.621 | 1.007 | 0.980 | 1.034 | −0.014 | 0.011 | 0.214 | 0.986 | 0.965 | 1.008 |
| Gambling preference | −0.219 | 0.551 | 0.691 | 0.803 | 0.273 | 2.368 | −0.081 | 0.445 | 0.855 | 0.922 | 0.386 | 2.205 |
| Delay discounting | 0.441 | 0.186 | 0.018* | 1.554 | 1.080 | 2.235 | 0.302 | 0.144 | 0.036* | 1.352 | 1.020 | 1.792 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mena-Moreno, T.; Testa, G.; Mestre-Bach, G.; Miranda-Olivos, R.; Granero, R.; Fernández-Aranda, F.; Menchón, J.M.; Jiménez-Murcia, S. Delay Discounting in Gambling Disorder: Implications in Treatment Outcome. J. Clin. Med. 2022, 11, 1611. https://doi.org/10.3390/jcm11061611
Mena-Moreno T, Testa G, Mestre-Bach G, Miranda-Olivos R, Granero R, Fernández-Aranda F, Menchón JM, Jiménez-Murcia S. Delay Discounting in Gambling Disorder: Implications in Treatment Outcome. Journal of Clinical Medicine. 2022; 11(6):1611. https://doi.org/10.3390/jcm11061611
Chicago/Turabian StyleMena-Moreno, Teresa, Giulia Testa, Gemma Mestre-Bach, Romina Miranda-Olivos, Rosario Granero, Fernando Fernández-Aranda, José M. Menchón, and Susana Jiménez-Murcia. 2022. "Delay Discounting in Gambling Disorder: Implications in Treatment Outcome" Journal of Clinical Medicine 11, no. 6: 1611. https://doi.org/10.3390/jcm11061611
APA StyleMena-Moreno, T., Testa, G., Mestre-Bach, G., Miranda-Olivos, R., Granero, R., Fernández-Aranda, F., Menchón, J. M., & Jiménez-Murcia, S. (2022). Delay Discounting in Gambling Disorder: Implications in Treatment Outcome. Journal of Clinical Medicine, 11(6), 1611. https://doi.org/10.3390/jcm11061611







