Adherence to the Mediterranean Diet Is Associated with a More Favorable Left Ventricular Geometry in Patients with End-Stage Kidney Disease
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Clinical Data
2.3. Mediterranean Diet Score
2.4. Echocardiography
2.5. Malnutrition-Inflammation Score
2.6. Laboratory Measurements
2.7. Statistical Analysis
3. Results
3.1. Study Population
3.2. Patients with and without Left Ventricular Hypertrophy (LVH)
3.3. Predictors of Left Ventricular Hypertrophy (LVH)
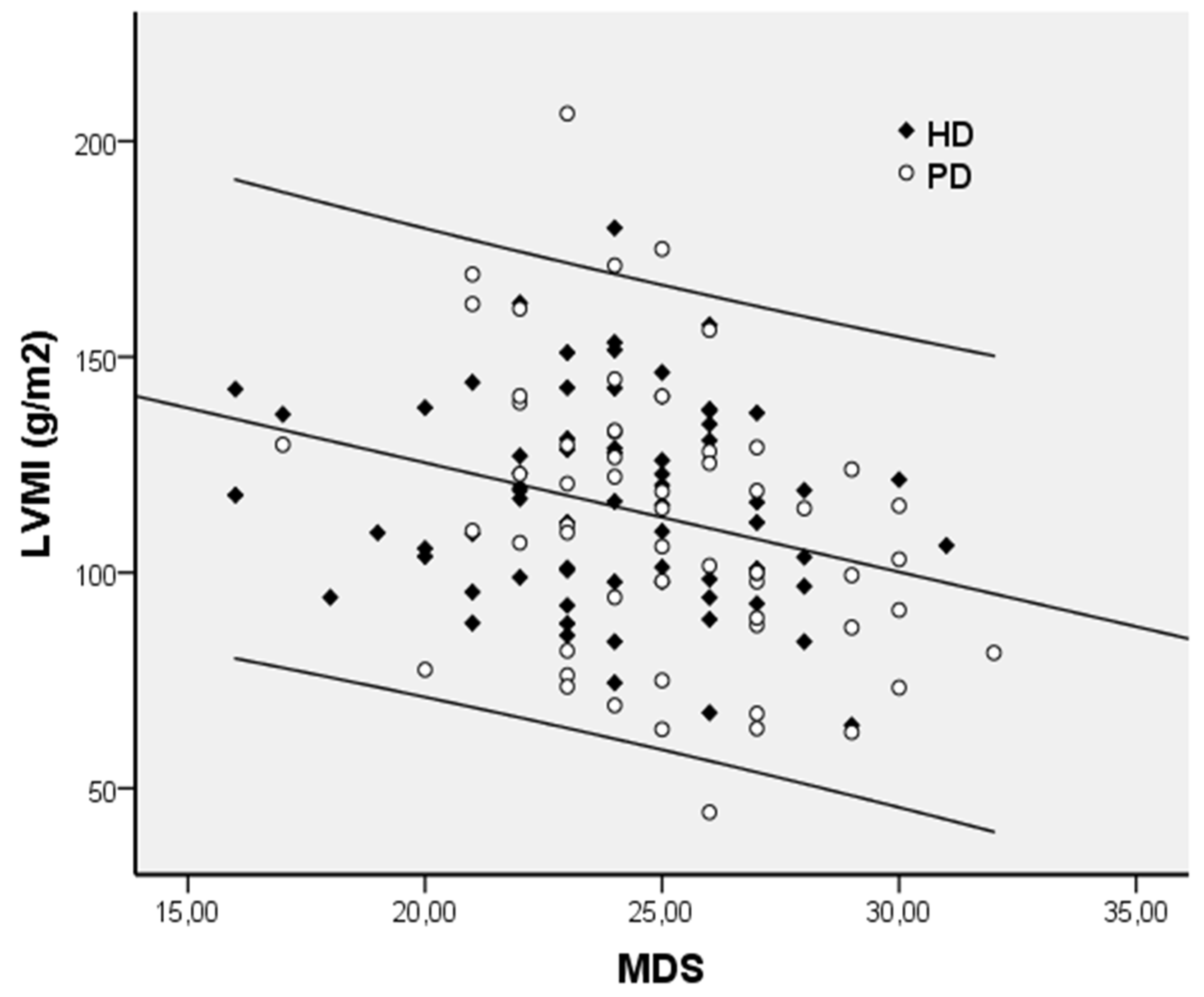
3.4. Determinants of Left Ventricular Mass Index (LVMI)
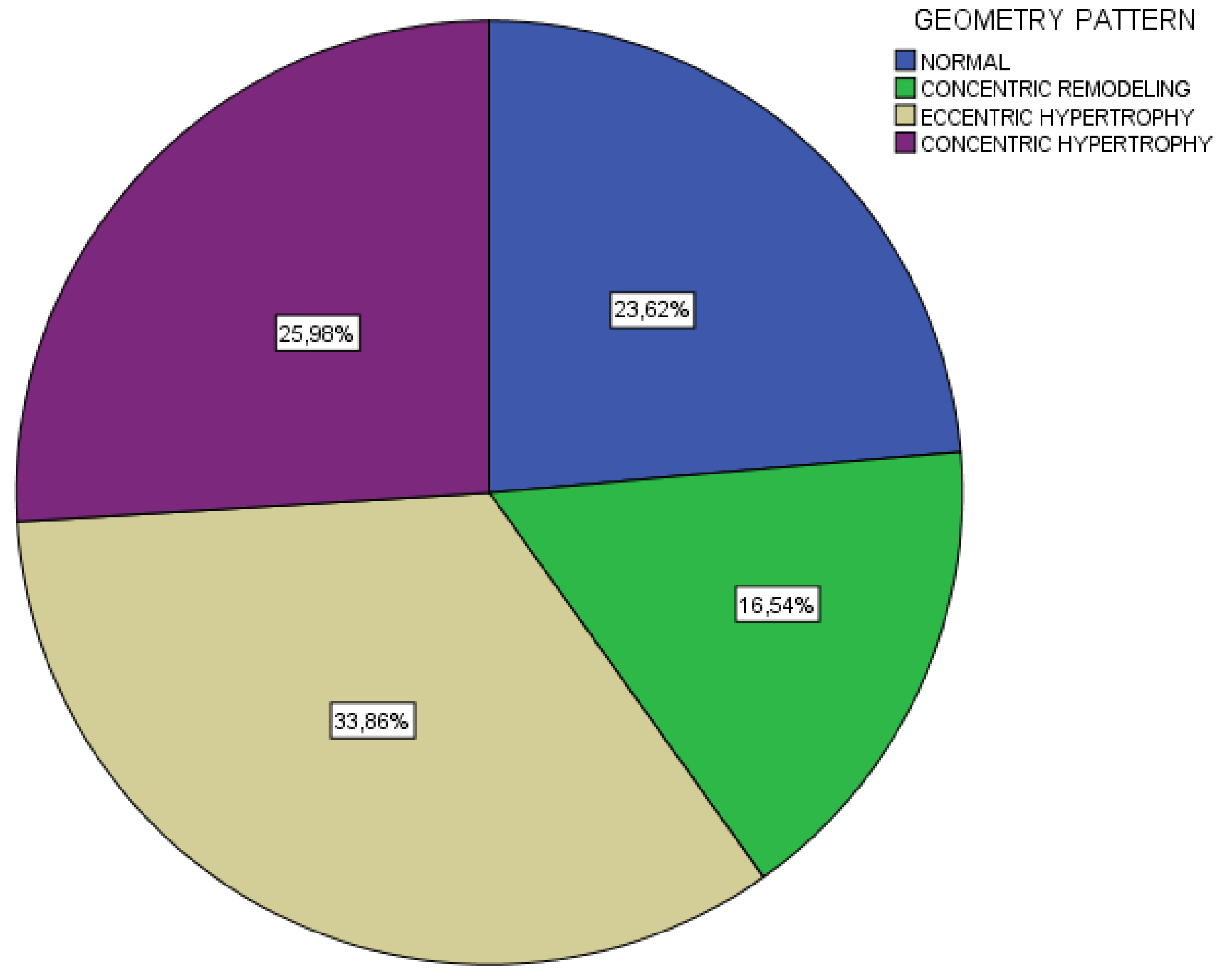
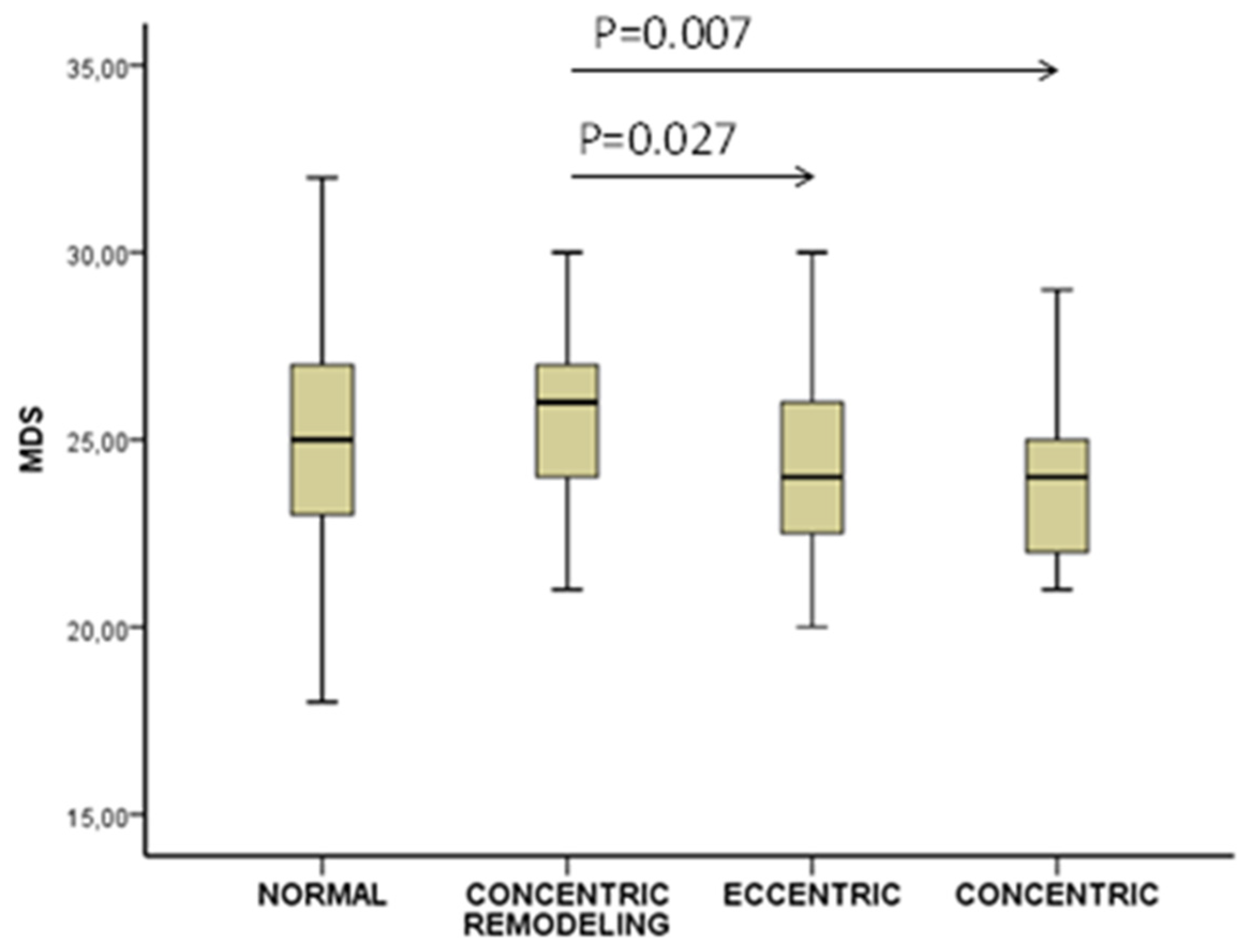
3.5. ΜDS as Major Determinant of Left Ventricular Geometry Patterns
3.6. Determinants of MDS
3.7. MDS as a Risk Indicator for CVD
3.8. Associations of Risk Factors for CVD with Med Diet Food Categories
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mafham, M.; Emberson, J.; Landray, M.J.; Wen, C.-P.; Baigent, C. Estimated Glomerular Filtration Rate and the Risk of Major Vascular Events and All-Cause Mortality: A Meta-Analysis. PLoS ONE 2011, 6, e25920. [Google Scholar] [CrossRef] [PubMed]
- Lindner, A.; Charra, B.; Sherrard, D.J.; Scribner, B.H. Accelerated Atherosclerosis in Prolonged Maintenance Hemodialysis. N. Engl. J. Med. 1974, 290, 697–701. [Google Scholar] [CrossRef] [PubMed]
- Krediet, R.T.; Balafa, O. Cardiovascular risk in the peritoneal dialysis patient. Nat. Rev. Nephrol. 2010, 6, 451–460. [Google Scholar] [CrossRef]
- Staplin, N.; Haynes, R.; Herrington, W.G.; Reith, C.; Cass, A.; Fellström, B.; Jiang, L.; Kasiske, B.L.; Krane, V.; Levin, A.; et al. Smoking and Adverse Outcomes in Patients With CKD: The Study of Heart and Renal Protection (SHARP). Am. J. Kidney Dis. 2016, 68, 371–380. [Google Scholar] [CrossRef]
- Prospective Studies Collaboration; Whitlock, G.; Lewington, S.; Sherliker, P.; Clarke, R.; Emberson, J.; Halsey, J.; Qizilbash, N.; Collins, R.; Peto, R. Body-mass index and cause-specific mortality in 900,000 adults: Collaborative analyses of 57 prospective studies. Lancet 2009, 373, 1083–1096. [Google Scholar] [CrossRef]
- Brenner, B.M.; Cooper, M.E.; De Zeeuw, D.; Keane, W.F.; Mitch, W.E.; Parving, H.-H.; Remuzzi, G.; Snapinn, S.M.; Zhang, Z.; Shahinfar, S. Effects of Losartan on Renal and Cardiovascular Outcomes in Patients with Type 2 Diabetes and Nephropathy. N. Engl. J. Med. 2001, 345, 861–869. [Google Scholar] [CrossRef] [PubMed]
- Wanner, C.; Krane, V.; März, W.; Olschewski, M.; Mann, J.F.; Ruf, G.; Ritz, E.; Diabetes, G.; Dialysis Study Investigators. Atorvastatin in patients with type 2 diabetes mellitus undergoing hemodialysis. N. Engl. J. Med. 2005, 353, 238–248. [Google Scholar] [CrossRef]
- Fellström, B.C.; Jardine, A.G.; Schmieder, R.E.; Holdaas, H.; Bannister, K.; Beutler, J.; Chae, D.-W.; Chevaile, A.; Cobbe, S.M.; Grönhagen-Riska, C.; et al. Rosuvastatin and Cardiovascular Events in Patients Undergoing Hemodialysis. N. Engl. J. Med. 2009, 360, 1395–1407. [Google Scholar] [CrossRef]
- Palmer, S.C.; Navaneethan, S.D.; Craig, J.; Johnson, D.W.; Tonelli, M.; Garg, A.X.; Pellegrini, F.; Ravani, P.; Jardine, M.; Perkovic, V.; et al. Meta-analysis: Erythropoiesis-Stimulating Agents in Patients with Chronic Kidney Disease. Ann. Intern. Med. 2010, 153, 23–33. [Google Scholar] [CrossRef]
- Jamal, S.A.; Fitchett, D.; Lok, C.E.; Mendelssohn, D.C.; Tsuyuki, R.T. The effects of calcium-based versus non-calcium-based phosphate binders on mortality among patients with chronic kidney disease: A meta-analysis. Nephrol. Dial. Transpl. 2009, 24, 3168–3174. [Google Scholar] [CrossRef]
- Thadhani, R.; Appelbaum, E.; Pritchett, Y.; Chang, Y.; Wenger, J.; Tamez, H.; Bhan, I.; Agarwal, R.; Zoccali, C.; Wanner, C.; et al. Vitamin D Therapy and Cardiac Structure and Function in Patients with Chronic Kidney Disease: The PRIMO randomized controlled trial. JAMA 2012, 307, 674–684. [Google Scholar] [CrossRef] [PubMed]
- Wang, A.Y.-M.; Fang, F.; Chan, J.; Wen, Y.-Y.; Qing, S.; Chan, I.H.-S.; Lo, G.; Lai, K.-N.; Lo, W.-K.; Lam, C.W.-K.; et al. Effect of Paricalcitol on Left Ventricular Mass and Function in CKD—The OPERA Trial. J. Am. Soc. Nephrol. 2014, 25, 175–186. [Google Scholar] [CrossRef] [PubMed]
- Parfrey, P.S.; Drüeke, T.B.; Block, G.A.; Correa-Rotter, R.; Floege, J.; Herzog, C.A.; London, G.M.; Mahaffey, K.W.; Moe, S.M.; Wheeler, D.C.; et al. The Effects of Cinacalcet in Older and Younger Patients on Hemodialysis: The Evaluation of Cinacalcet HCl Therapy to Lower Cardiovascular Events (EVOLVE) Trial. Clin. J. Am. Soc. Nephrol. 2015, 10, 791–799. [Google Scholar] [CrossRef] [PubMed]
- Wheeler, D.C.; London, G.M.; Parfrey, P.S.; Block, G.A.; Correa-Rotter, R.; Dehmel, B.; Drüeke, T.B.; Floege, J.; Kubo, Y.; Mahaffey, K.W.; et al. Effects of Cinacalcet on Atherosclerotic and Nonatherosclerotic Cardiovascular Events in Patients Receiving Hemodialysis: The EValuation of Cinacalcet HCl Therapy to Lower CardioVascular Events (EVOLVE) Trial. J. Am. Heart Assoc. 2014, 3, e001363. [Google Scholar] [CrossRef] [PubMed]
- Ganau, A.; Devereux, R.B.; Roman, M.J.; de Simone, G.; Pickering, T.G.; Saba, P.S.; Vargiu, P.; Simongini, I.; Laragh, J.H. Patterns of left ventricular hypertrophy and geometric remodeling in essential hypertension. J. Am. Coll. Cardiol. 1992, 19, 1550–1558. [Google Scholar] [CrossRef]
- Suh, S.H.; Oh, T.R.; Choi, H.S.; Kim, C.S.; Bae, E.H.; Oh, K.-H.; Lee, J.; Jung, J.Y.; Lee, K.-B.; Ma, S.K.; et al. Association between Left Ventricular Geometry and Renal Outcomes in Patients with Chronic Kidney Disease: Findings from Korean Cohort Study for Outcomes in Patients With Chronic Kidney Disease Study. Front. Cardiovasc. Med. 2022, 9, 848692. [Google Scholar] [CrossRef]
- Lee, Y.-T.; Chiu, H.-C.; Su, H.-M.; Voon, W.-C.; Lin, T.-H.; Lai, W.-T.; Sheu, S.-H.; Lee, H.-C.C.Y.-T. Presence of Chronic Kidney Disease and Subsequent Changes of Left Ventricular Geometry over 4 Years in an Apparently Healthy Population Aged 60 and Older. Hypertens. Res. 2008, 31, 913–920. [Google Scholar] [CrossRef][Green Version]
- Shi, H.; Wang, X.; Li, J.; Song, G.; Huang, Z.; Guo, X.; Guo, J.; Lv, Z.; Li, H.; Ge, J.; et al. Association of Left Ventricular Hypertrophy with a Faster Rate of Renal Function Decline in Elderly Patients with Non-End-Stage Renal Disease. J. Am. Heart Assoc. 2015, 4, e002213. [Google Scholar] [CrossRef]
- Amann, K.; Rychlík, I.; Miltenberger-Milteny, G.; Ritz, E. Left ventricular hypertrophy in renal failure. Kidney Int. 1998, 54, S78–S85. [Google Scholar] [CrossRef]
- Nubé, M.J.; Hoekstra, T.; Doganer, V.; Bots, M.L.; Blankestijn, P.J.; Dorpel, M.V.D.; Kamp, O.; Ter Wee, P.M.; Zuijdewijn, C.L.M.D.R.V.; Grooteman, M.P.C. Left ventricular geometric patterns in end-stage kidney disease: Determinants and course over time. Hemodial. Int. 2018, 22, 359–368. [Google Scholar] [CrossRef]
- Agodi, A.; Maugeri, A.; Kunzova, S.; Sochor, O.; Bauerova, H.; Kiacova, N.; Barchitta, M.; Vinciguerra, M. Association of Dietary Patterns with Metabolic Syndrome: Results from the Kardiovize Brno 2030 Study. Nutrients 2018, 10, 898. [Google Scholar] [CrossRef] [PubMed]
- Levitan, E.B.; Ahmed, A.; Arnett, D.K.; Polak, J.F.; Hundley, W.G.; Bluemke, D.; Heckbert, S.R.; Jacobs, D.R.; Nettleton, J.A. Mediterranean diet score and left ventricular structure and function: The Multi-Ethnic Study of Atherosclerosis. Am. J. Clin. Nutr. 2016, 104, 595–602. [Google Scholar] [CrossRef] [PubMed]
- Gardener, H.; Rundek, T.; Wright, C.B.; Gu, Y.; Scarmeas, N.; Homma, S.; Russo, C.; Elkind, M.S.; Sacco, R.L.; Di Tullio, M.R. A Mediterranean-Style Diet and Left Ventricular Mass (from the Northern Manhattan Study). Am. J. Cardiol. 2015, 115, 510–514. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, H.T.; Bertoni, A.G.; Nettleton, J.A.; Bluemke, D.A.; Levitan, E.B.; Burke, G.L. DASH Eating Pattern Is Associated with Favorable Left Ventricular Function in the Multi-Ethnic Study of Atherosclerosis. J. Am. Coll. Nutr. 2012, 31, 401–407. [Google Scholar] [CrossRef] [PubMed]
- Chauveau, P.; Aparicio, M.; Bellizzi, V.; Campbell, K.; Hong, X.; Johansson, L.; Kolko, A.; Molina, P.; Sezer, S.; Wanner, C.; et al. Mediterranean diet as the diet of choice for patients with chronic kidney disease. Nephrol. Dial. Transpl. 2018, 33, 725–735. [Google Scholar] [CrossRef]
- Cases, A.; Cigarrán-Guldrís, S.; Mas, S.; Gonzalez-Parra, E. Vegetable-Based Diets for Chronic Kidney Disease? It Is Time to Reconsider. Nutrients 2019, 11, 1263. [Google Scholar] [CrossRef] [PubMed]
- Daugirdas, J.T.; Depner, T.A.; Inrig, J.; Mehrotra, R.; Rocco, M.V.; Suri, R.S.; Weiner, D.E.; Greer, N.; Ishani, A.; MacDonald, R.; et al. KDOQI Clinical Practice Guideline for Hemodialysis Adequacy: 2015 Update. Am. J. Kidney Dis. 2015, 66, 884–930. [Google Scholar] [CrossRef]
- Brown, E.A.; Blake, P.G.; Boudville, N.; Davies, S.; De Arteaga, J.; Dong, J.; Finkelstein, F.; Foo, M.; Hurst, H.; Johnson, D.W.; et al. International Society for Peritoneal Dialysis practice recommendations: Prescribing high-quality goal-directed peritoneal dialysis. Perit. Dial. Int. J. Int. Soc. Perit. Dial. 2020, 40, 244–253. [Google Scholar] [CrossRef]
- Gunsolus, I.; Sandoval, Y.; Smith, S.W.; Sexter, A.; Schulz, K.; Herzog, C.A.; Apple, F.S. Renal Dysfunction Influences the Diagnostic and Prognostic Performance of High-Sensitivity Cardiac Troponin I. J. Am. Soc. Nephrol. 2018, 29, 636–643. [Google Scholar] [CrossRef]
- Collet, J.-P.; Thiele, H.; Barbato, E.; Barthélémy, O.; Bauersachs, J.; Bhatt, D.L.; Dendale, P.; Dorobantu, M.; Edvardsen, T.; Folliguet, T.; et al. 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur. Heart J. 2021, 42, 1289–1367. [Google Scholar] [CrossRef]
- Panagiotakos, D.B.; Pitsavos, C.; Arvaniti, F.; Stefanadis, C. Adherence to the Mediterranean food pattern predicts the prevalence of hypertension, hypercholesterolemia, diabetes and obesity, among healthy adults; the accuracy of the MedDietScore. Prev. Med. 2007, 44, 335–340. [Google Scholar] [CrossRef] [PubMed]
- Lang, R.M.; Bierig, M.; Devereux, R.B.; Flachskampf, F.A.; Foster, E.; Pellikka, P.A.; Picard, M.; Roman, M.J.; Seward, J.; Shanewise, J.S.; et al. Recommendations for Chamber Quantification: A Report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, Developed in Conjunction with the European Association of Echocardiography, a Branch of the European Society of Cardiology. J. Am. Soc. Echocardiogr. 2005, 18, 1440–1463. [Google Scholar] [CrossRef]
- Lang, R.M.; Bierig, M.; Devereux, R.B.; Flachskampf, F.A.; Foster, E.; Pellikka, P.A.; Picard, M.; Roman, M.J.; Seward, J.B.; Shanewise, J.S. Recommendations for chamber quantification. Eur. J. Echocardiogr. 2006, 7, 79–108. [Google Scholar] [CrossRef] [PubMed]
- Koren, M.J.; Devereux, R.B.; Casale, P.N.; Savage, D.D.; Laragh, J.H. Relation of Left Ventricular Mass and Geometry to Morbidity and Mortality in Uncomplicated Essential Hypertension. Ann. Intern. Med. 1991, 114, 345–352. [Google Scholar] [CrossRef] [PubMed]
- Kalantar-Zadeh, K.; Kopple, J.D.; Block, G.; Humphreys, M.H. A Malnutrition-Inflammation Score is correlated with morbidity and mortality in maintenance hemodialysis patients. Am. J. Kidney Dis. 2001, 38, 1251–1263. [Google Scholar] [CrossRef]
- Rees, K.; Takeda, A.; Martin, N.; Ellis, L.; Wijesekara, D.; Vepa, A.; Das, A.; Hartley, L.; Stranges, S. Mediterranean-style diet for the primary and secondary prevention of cardiovascular disease. Cochrane Database Syst. Rev. 2019, 3, CD009825. [Google Scholar] [CrossRef]
- Maugeri, A.; Hruskova, J.; Jakubik, J.; Hlinomaz, O.; Medina-Inojosa, J.R.; Barchitta, M.; Agodi, A.; Vinciguerra, M. How dietary patterns affect left ventricular structure, function and remodelling: Evidence from the Kardiovize Brno 2030 study. Sci. Rep. 2019, 9, 19154. [Google Scholar] [CrossRef]
- Ozkahya, M.; Ok, E.; Cirit, M.; Aydin, S.; Akçiçek, F.; Başçi, A.; Mees, E.J.D. Regression of left ventricular hypertrophy in haemodialysis patients by ultrafiltration and reduced salt intake without antihypertensive drugs. Nephrol. Dial. Transpl. 1998, 13, 1489–1493. [Google Scholar] [CrossRef]
- Gallieni, M.; Pedone, M. Left ventricular hypertrophy and serum phosphate in peritoneal dialysis patients. Kidney Int. 2013, 84, 850. [Google Scholar] [CrossRef]
- Agarwal, R. Blood Pressure and Mortality among Hemodialysis Patients. Hypertension 2010, 55, 762–768. [Google Scholar] [CrossRef]
- Martins, V.S.; Adragão, T.; Aguiar, L.; Pinto, I.; Dias, C.; Figueiredo, R.; Lourenço, P.; Pascoal, T.; Pereira, J.; Pinheiro, T.; et al. Prognostic Value of the Malnutrition-inflammation Score in Hospitalization and Mortality on Long-term Hemodialysis. J. Ren. Nutr. 2021, 32, 569–577. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.R.; Lee, Y.-K.; Cho, A.J.; Park, H.C.; Han, C.H.; Choi, M.-J.; Koo, J.-R.; Yoon, J.-W.; Noh, J.W. Malnutrition, inflammation, progression of vascular calcification and survival: Inter-relationships in hemodialysis patients. PLoS ONE 2019, 14, e0216415. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.; Cai, K.; Luo, Q.; Wang, L.; Hong, Y. Baseline Serum Magnesium Level and Its Variability in Maintenance Hemodialysis Patients: Associations with Mortality. Kidney Blood Press. Res. 2019, 44, 222–232. [Google Scholar] [CrossRef] [PubMed]
- Shimohata, H.; Yamashita, M.; Ohgi, K.; Tsujimoto, R.; Maruyama, H.; Takayasu, M.; Hirayama, K.; Kobayashi, M. The relationship between serum magnesium levels and mortality in non-diabetic hemodialysis patients: A 10-year follow-up study. Hemodial. Int. 2019, 23, 369–374. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.; Li, Q.; Fan, L.; Zeng, D.; Chi, X.; Guan, B.; Hu, B.; Lu, Y.; Yun, C.; Krämer, B.; et al. Prognostic Value of Serum Magnesium in Mortality Risk among Patients on Hemodialysis: A Meta-Analysis of Observational Studies. Kidney Dis. 2021, 7, 24–33. [Google Scholar] [CrossRef]
- Hu, E.A.; Coresh, J.; Anderson, C.A.; Appel, L.J.; Grams, M.E.; Crews, D.C.; Mills, K.T.; He, J.; Scialla, J.; Rahman, M.; et al. Adherence to Healthy Dietary Patterns and Risk of CKD Progression and All-Cause Mortality: Findings from the CRIC (Chronic Renal Insufficiency Cohort) Study. Am. J. Kidney Dis. 2021, 77, 235–244. [Google Scholar] [CrossRef]
- Lang, R.M.; Badano, L.P.; Mor-Avi, V.; Afilalo, J.; Armstrong, A.; Ernande, L.; Flachskampf, F.A.; Foster, E.; Goldstein, S.A.; Kuznetsova, T.; et al. Recommendations for Cardiac Chamber Quantification by Echocardiography in Adults: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J. Am. Soc. Echocardiogr. 2015, 28, 1–39.e14. [Google Scholar] [CrossRef]
| How Often Do You Consume (Servings/Week or Otherwise Stated) | Frequency of Consumption | |||||
|---|---|---|---|---|---|---|
| Non-Refined Cereals (Whole Grain Bread, Pasta, Rice, etc.) | Never | 1–6 | 7–12 | 13–18 | 19–31 | >32 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Potatoes | Never | 1–4 | 5–8 | 9–12 | 13–18 | >18 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Fruits | Never | 1–4 | 5–8 | 9–15 | 16–21 | >22 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Vegetables | Never | 1–6 | 7–12 | 13–20 | 21–32 | >33 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Legumes | Never | <1 | 1–2 | 3–4 | 5–6 | >6 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Fish | Never | <1 | 1–2 | 3–4 | 5–6 | >6 |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Red meat and products | ≤1 | 2–3 | 4–5 | 6–7 | 8–10 | >10 |
| 5 | 4 | 3 | 2 | 1 | 0 | |
| Poultry | ≤3 | 4–5 | 5–6 | 7–8 | 9–10 | >10 |
| 5 | 4 | 3 | 2 | 1 | 0 | |
| Full fat dairy products (cheese, yogurt, milk) | ≤10 | 11–15 | 16–20 | 21–28 | 29–30 | >30 |
| 5 | 4 | 3 | 2 | 1 | 0 | |
| Use of olive oil in cooking (times/week) | Never | Rare | <1 | 1–3 | 3–5 | Daily |
| 0 | 1 | 2 | 3 | 4 | 5 | |
| Alcoholic beverages (mL/day, 100 mL = 12 g ethanol) | <300 | 300 | 400 | 500 | 600 | >700 or 0 |
| 5 | 4 | 3 | 2 | 1 | 0 | |
| Characteristic | All Patients (n = 127) | LVH (n = 81) | NO LVH (n = 46) | p-Value | r | p-Value |
|---|---|---|---|---|---|---|
| Age (year) | 62 ± 15 | 66 ± 13 | 55 ± 16 | 0.000 | 0.270 | 0.002 |
| Sex (male/females) | 77/50 | 31/15 | 46/35 | 0.240 | −0.187 | 0.035 |
| Dialysis mode [(HD = 1/PD = 2) (n)] | 69/58 | 22/24 | 47/34 | 0.267 | −0.082 | 0.358 |
| Dialysis vintage (months) | 36 (15–60) | 36 (17–58) | 35 (12–68) | 0.425 | −0.129 | 0.151 |
| Diabetes mellitus (%) | 26.8 | 33.3 | 15.2 | 0.027 | 0.093 | 0.278 |
| Peripheral vascular disease (%) | 37 | 44.4 | 23.9 | 0.021 | 0.191 | 0.031 |
| Coronary artery disease (%) | 28.3 | 34.6 | 17.4 | 0.039 | 0.158 | 0.076 |
| Hypertension (%) | 75.6 | 79 | 69.6 | 0.234 | 0.178 | 0.046 |
| Stroke (%) | 15 | 17.3 | 10.9 | 0.330 | 0.011 | 0.905 |
| Smoking (%) | 22.1 | 26.4 | 14.6 | 0.148 | 0.255 | 0.006 |
| Body mass index (Kg/m2) | 26.2 ± 4.7 | 27.5 ± 4.9 | 24.1 ± 3.5 | 0.000 | 0.230 | 0.009 |
| SBP (mmHg) | 133 ± 19 | 135 ± 19 | 129 ± 28 | 0.086 | 0.259 | 0.03 |
| DBP (mmHg) | 76 ± 14 | 76 ± 13 | 776 ± 15 | 0.891 | 0.019 | 0.833 |
| Pulse pressure (mmHg) | 57 ± 15 | 59 ± 14 | 53 ± 15 | 0.009 | 0.321 | 0.000 |
| LVMI index (g/m2) | 114.2 ± 28.1 | 129.5 ± 21.2 | 87.2 ± 15.4 | 0.000 | − | − |
| ACEi/ARBs (%) | 42.5 | 45.7 | 37 | 0.339 | 0.162 | 0.069 |
| B-BLOCKERS (%) | 67.5 | 71.6 | 60 | 0.183 | 0.182 | 0.042 |
| CCB (%) | 40.5 | 46.9 | 28.9 | 0.048 | 0.238 | 0.007 |
| DIURETICS (%) | 28.3 | 28.4 | 28.3 | 0.987 | 0.003 | 0.978 |
| CALCIMIMETICS (%) | 32.3 | 27.2 | 41.3 | 0.075 | −0.156 | 0.080 |
| Nutritional and biochemical | ||||||
| Albumin (g/dL) | 3.6 ± 0.5 | 3.6 ± 0.5 | 3.8 ± 0.4 | 0.011 | −0.119 | 0.183 |
| Creatinine (mg/dL) | 8.7 ± 3.0 | 8.3 ± 2.8 | 9.4 ± 2.3 | 0.054 | −0.051 | 0.569 |
| Hemoglobin (g/dL) | 11.7 (11.1–12.4) | 11.7 (11.2–12.2) | 11.7 (11.0–12.6) | 0.887 | −0.103 | 0.250 |
| Total Cholesterol (mg/dL) | 159 ± 35 | 159 ± 35 | 159 ± 36 | 0.969 | −0.069 | 0.441 |
| HDL (mg/dL) | 43 ± 11 | 42 ± 11 | 46 ± 11 | 0.093 | −0.158 | 0.077 |
| LDL (mg/dL) | 85 ± 28 | 85 ± 29 | 86 ± 28 | 0.832 | −0.058 | 0.519 |
| Triglycerides (mg/dL) | 140 (103–184) | 133 (105–191) | 140 (100–178) | 0.477 | 0.002 | 0.914 |
| Calcium (mg/dL) | 9.2 ± 0.6 | 9.3 ± 0.6 | 9.1 ± 0.6 | 0.034 | 0.173 | 0.052 |
| Magnesium (mg/dL) | 2.2 ± 0.4 | 2.1 ± 0.3 | 2.4 ± 0.4 | 0.000 | −0.219 | 0.014 |
| Potassium (mmol/L) | 4.72 ± 0.68 | 4.83 ± 0.67 | 4.67 ± 0.70 | 0.208 | −0.011 | 0.902 |
| Phosphorus (mg/dL) | 5.0 ± 1.3 | 5.0 ± 0.1.3 | 5.0 ± 1.3 | 0.958 | 0.010 | 0.914 |
| Parathormone (pg/mL) | 262 (144–404) | 256 (148–408) | 275 (143–398) | 0.857 | 0.081 | 0.365 |
| MIS | 4,56 ± 2.47 | 5.0 ± 2.7 | 3.9 ± 1.9 | 0.017 | 0.237 | 0.007 |
| MDS | 24.4 ± 3 | 24 ± 2.7 | 25 ± 3.4 | 0.016 | −0.273 | 0.002 |
| Parameter | Univariate | Multivariable | ||
|---|---|---|---|---|
| OR (95%CI) | p | OR (95%CI) | p | |
| Age (↑ 1 year) | 1.05 (1.02–1.08) | 0.000 | - | - |
| PVD (presence) | 2.55 (2.14–5.70) | 0.023 | - | - |
| CAD (presence) | 2.51 (1.03–6.11 | 0.043 | 8.81(2.25–34.49) | 0.002 |
| Diabetes (presence) | 2.79 (1.10–7.04 | 0.030 | - | - |
| ΒΜΙ (↑ 1 Kg/m2) | 1.21 (1.09–1.35) | 0.000 | 1.33 (1.14–1.55) | 0.000 |
| PP (↑ 1 mmHg) | 1.04 (1.01–1.06) | 0.011 | 1.05 (1.01–1.09) | 0.013 |
| sAlb (↑ 1 g/dL) | 0.38 (0.18–0.82) | 0.013 | - | - |
| MIS (↑ 1 point) | 1.28 (1.03–1.47) | 0.020 | 1.28 (1.01–1.61) | 0.039 |
| sMg (↑ mg/dL) | 0.13 (0.04–0.41) | 0.000 | 0.08 (0.02–0.38) | 0.002 |
| MDS (↑ 1 point) | 0.85 (0.75–0.97) | 0.018 | 0.82 (0.68–0.99) | 0.037 |
| Sex (male = 1/female = 2) | 1.57 (0.74–3.35) | 0.247 | 7.29 (2.11–25.16) | 0.002. |
| Parameter | B | Standard Error | Standard B | p | Partial r | Adjusted R2 Change (Cumulative Variability) |
|---|---|---|---|---|---|---|
| (Constant) | 114,449 | 23,85 | 0 | |||
| MDS | −2.217 | 0.778 | −0.243 | 0.005 | −0.265 | 0.089 (0.089) |
| AGE | 0.432 | 0.156 | 0.235 | 0.007 | 0.258 | 0.06 (0.149) |
| SMOKING | 16.023 | 5.772 | 0.234 | 0.006 | 0.258 | 0.046 (0.195) |
| PP | 0.413 | 0.166 | 0.214 | 0.014 | 0.233 | 0.036 (0.231) |
| Factor | Low MDS ≤ 24 (n = 63) | High MDS > 24 (n = 64) | p | r | p |
|---|---|---|---|---|---|
| PVD (%) | 46 | 28.1 | 0.037 | −0.201 | 0.024 |
| SBP (mmHg) | 137 ± 17 | 129 ± 20 | 0.013 | −0.283 | 0.001 |
| DBP (mmHg) | 78 ± 14 | 73 ± 13 | 0.044 | −0.233 | 0.008 |
| HDL (mg/dL) | 41 ± 10 | 45 ± 11 | 0.032 | 0.207 | 0.020 |
| LDL (mg/dL) | 90 ± 32 | 81 ± 23 | 0.046 | −0.190 | 0.033 |
| sMg (mg/dL) | 2.2 ± 0.3 | 2.3 ± 0.4 | 0.048 | 0.240 | 0.007 |
| sCa (mg/dL) | 9.3 ± 0.5 | 9.1 ± 0.6 | 0.046 | −0.189 | 0.034 |
| sAlb (g/dL) | 3.5 ± 0.5 | 3.7 ± 0.5 | 0.023 | 0.228 | 0.010 |
| MIS (points) | 4.7 ± 2.7 | 4.4 ± 2.3 | 0.398 | −0.179 | 0.044 |
| K (mmol/L) | 4.75 ± 0.68 | 4.70 ± 0.69 | 0.696 | −0.040 | 0.696 |
| Variables | Q1 (≤22) n = 28 | Q2 (23–24) n = 37 | Q3 (25–26) n = 30 | Q4 (≥27) n = 32 | p for Trend |
|---|---|---|---|---|---|
| Cardiac measures | |||||
| A. LVH | 0.005 | ||||
| absent | 27.6 (8) | 27.8 (10) | 26.7 (8) | 62.5 (20) | |
| present | 71.4 (20) | 73.0 (27) | 73.3 (22) | 37.5 (12) | |
| B. Geometry pattern | 0.041 | ||||
| normal | 24.1 (7) | 19.4 (7) | 16.7 (5) | 34.4 (11) | |
| cLVR | 6.9 (2) | 11.1 (4) | 13.3 (4) | 34.4 (11) | |
| eLVH | 35.7 (10) | 37.8 (14) | 43.3 (13) | 18.8 (6) | |
| cLVH | 32.1 (9) | 33.3 (12) | 26.7 (8) | 12.5 (4) | |
| Co-morbidities | |||||
| PVD | 39.3 (11) | 51.4 (19) | 36.7 (11) | 18.8 (6) | 0.048 |
| CAD | 14.3 (4) | 32.4 (12) | 36.7 (11) | 28.1 (9) | 0.256 |
| STROKE | 14.3 (4) | 27 (10) | 13.3 (4) | 3.1 (1) | 0.050 |
| Anti-HTN drugs | |||||
| ACEI/ARB | 57.1 (16) | 37.8 (14) | 26.7 (8) | 50 (16) | 0.086 |
| B-BLOCKERS | 78.6 (22) | 64.9 (24) | 80 (24) | 48.4 (15) | 0.030 |
| CCB | 46.4 (13) | 37.8 (14) | 43.3 (13) | 35.5 (11) | 0.816 |
| BMI (mean ± SD) | 26 ± 5.0 | 26.9 ± 5.1 | 26.6 ± 5.0 | 25.2 ± 3.6 | 0.502 |
| GROUP A ‘Avoid Foods’ | GROUP B ‘Recommended Foods’ | GROUP C ‘FVL’ | ||||
|---|---|---|---|---|---|---|
| Factor | r | p | r | p | r | p |
| LVMI | −0.210 | 0.210 | −0.213 | 0.016 | −0.235 | 0.008 |
| * Cardiac geometry | 0.079 | 0.375 | −0.254 | 0.004 | −.0329 | 0.000 |
| LVH | −0.019 | 0.832 | −0.235 | 0.008 | −0.236 | 0.008 |
| PVD | −0.075 | 0.405 | −0.203 | 0.022 | −0.115 | 0.198 |
| Stroke | −0.077 | 0.389 | −0.130 | 0.145 | −0.175 | 0.049 |
| SBP | −0.191 | 0.032 | −0.143 | 0.110 | −0.137 | 0.125 |
| LDL | −0.101 | 0.260 | −0.209 | 0.019 | 0.155 | 0.083 |
| sMg | −0.193 | 0.030 | 0.396 | 0.000 | 0.395 | 0.000 |
| MIS | 0.001 | 0.988 | −0.128 | 0.152 | −0.176 | 0.047 |
| Albumin | 0.001 | 0.988 | 0.259 | 0.003 | 0.188 | 0.035 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bacharaki, D.; Petrakis, I.; Kyriazis, P.; Markaki, A.; Pleros, C.; Tsirpanlis, G.; Theodoridis, M.; Balafa, O.; Georgoulidou, A.; Drosataki, E.; et al. Adherence to the Mediterranean Diet Is Associated with a More Favorable Left Ventricular Geometry in Patients with End-Stage Kidney Disease. J. Clin. Med. 2022, 11, 5746. https://doi.org/10.3390/jcm11195746
Bacharaki D, Petrakis I, Kyriazis P, Markaki A, Pleros C, Tsirpanlis G, Theodoridis M, Balafa O, Georgoulidou A, Drosataki E, et al. Adherence to the Mediterranean Diet Is Associated with a More Favorable Left Ventricular Geometry in Patients with End-Stage Kidney Disease. Journal of Clinical Medicine. 2022; 11(19):5746. https://doi.org/10.3390/jcm11195746
Chicago/Turabian StyleBacharaki, Dimitra, Ioannis Petrakis, Periklis Kyriazis, Anastasia Markaki, Christos Pleros, Georgios Tsirpanlis, Marios Theodoridis, Olga Balafa, Anastasia Georgoulidou, Eleni Drosataki, and et al. 2022. "Adherence to the Mediterranean Diet Is Associated with a More Favorable Left Ventricular Geometry in Patients with End-Stage Kidney Disease" Journal of Clinical Medicine 11, no. 19: 5746. https://doi.org/10.3390/jcm11195746
APA StyleBacharaki, D., Petrakis, I., Kyriazis, P., Markaki, A., Pleros, C., Tsirpanlis, G., Theodoridis, M., Balafa, O., Georgoulidou, A., Drosataki, E., & Stylianou, K. (2022). Adherence to the Mediterranean Diet Is Associated with a More Favorable Left Ventricular Geometry in Patients with End-Stage Kidney Disease. Journal of Clinical Medicine, 11(19), 5746. https://doi.org/10.3390/jcm11195746





