Emergency Pancreatoduodenectomy: A Non-Trauma Center Case Series
Abstract
1. Introduction
2. Materials and Methods
- Demographic data (age, sex, rural or urban area of living)
- Previous medical history (comorbidities)
- Reasons for emergency admission (symptoms and clinical signs)
- Preoperative investigations (blood work and imagistic investigations)
- Initial diagnosis
- Surgical intervention details (type of resection and reconstruction modality, blood loss, operative time)
- Definitive histopathological diagnosis of the resection specimen
- Postoperative investigations
- Patient evolution, including encountered complications
- Reinterventions
- Long term follow-up data
- Overall survival
3. Results
3.1. Case 1
3.2. Case 2
3.3. Case 3
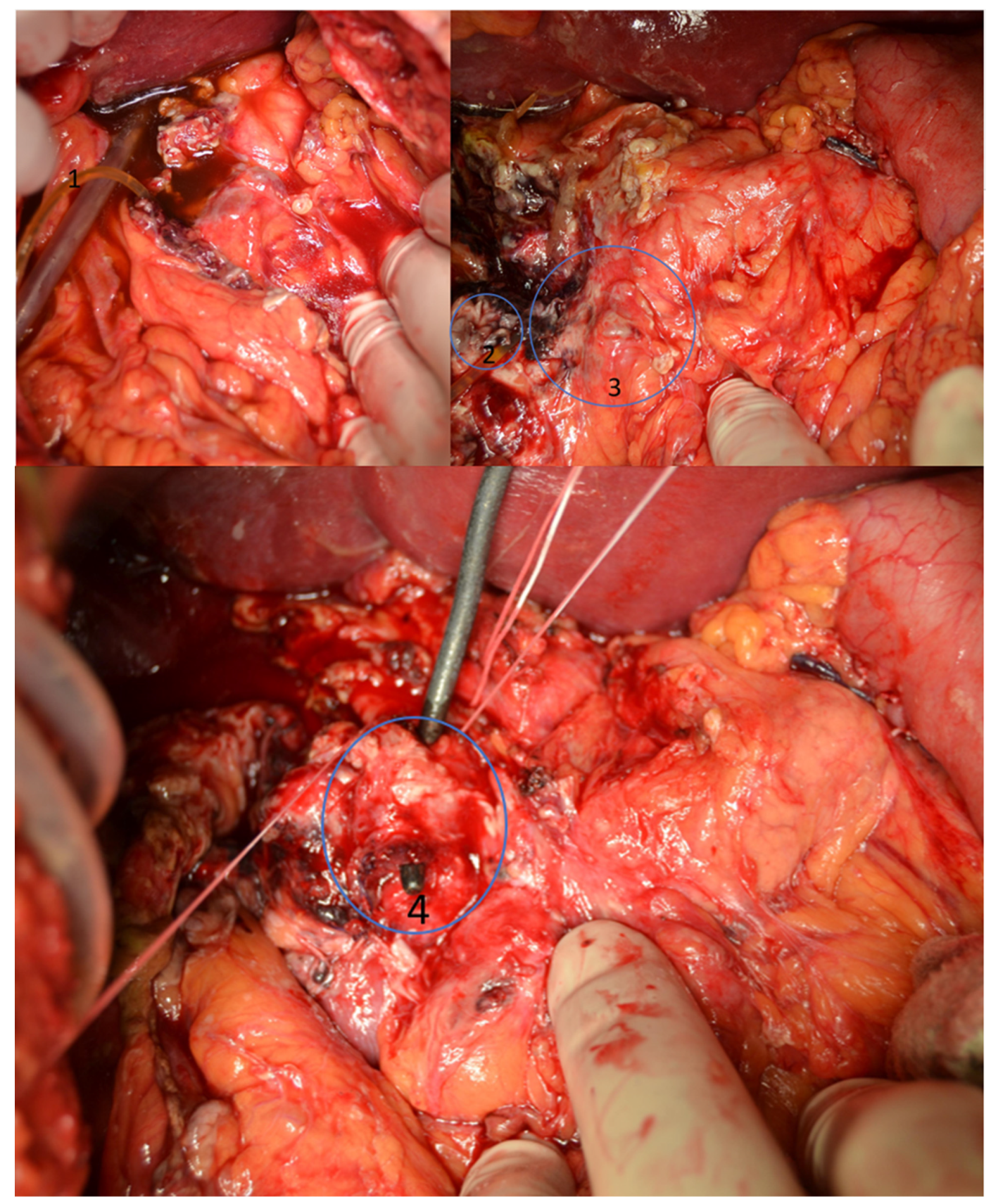
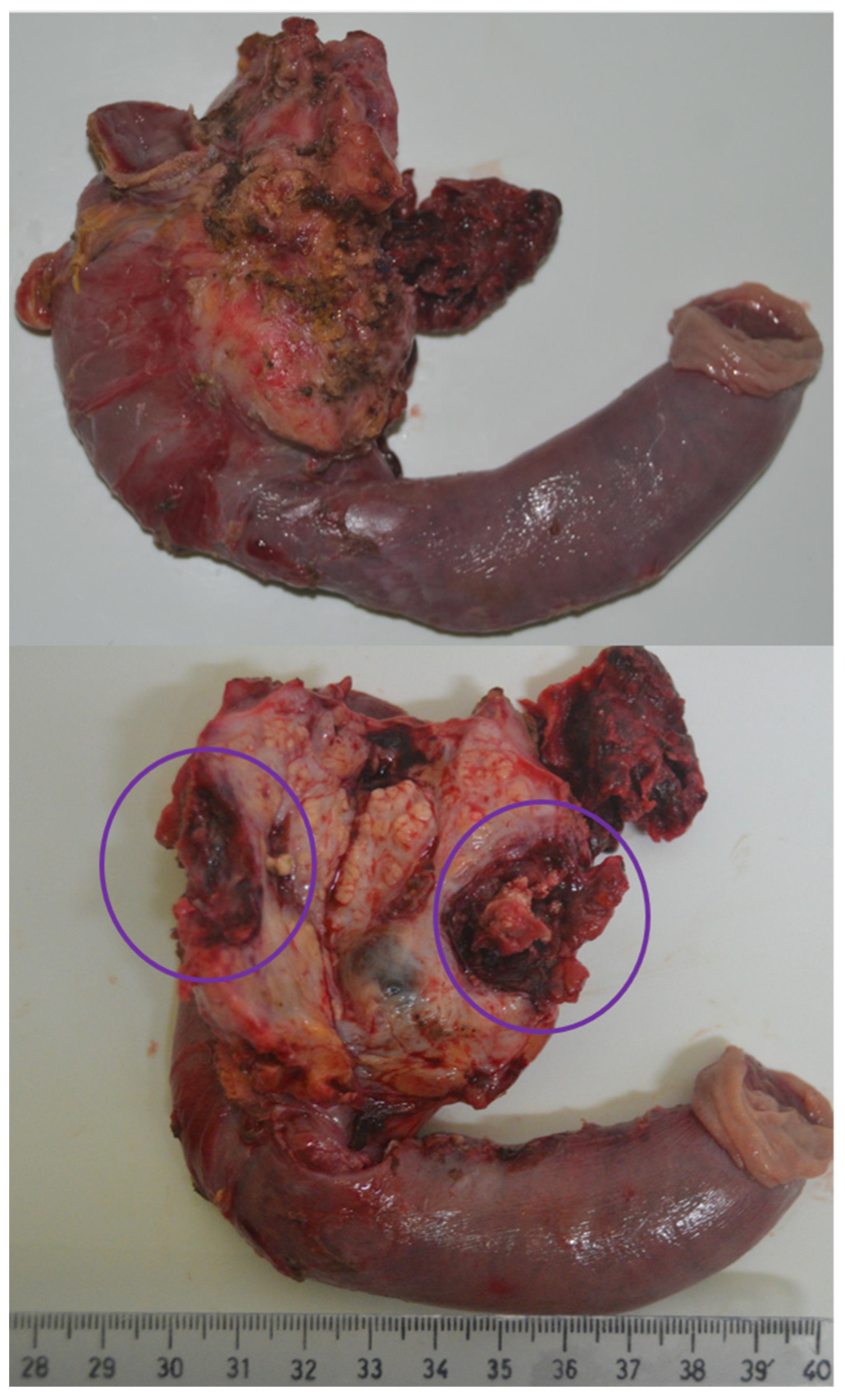
3.4. Case 4
4. Discussion
4.1. Emergency Pancreatoduodenectomy as a Rare Surgical Procedure in Non-Traumatic Cases
4.2. Indication for Surgery
4.3. Surgical Intervention
4.4. Early Postoperative Evolution
4.5. Long-Term Evolution
4.6. Strengths
4.7. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Thal, A.P.; Wilson, R.F. A Pattern of Severe Blunt Trauma to the Region of the Pancreas. Surg. Gynecol. Obstet. 1964, 119, 773–778. [Google Scholar]
- Tsai, C.-Y.; Lai, B.-R.; Wang, S.-Y.; Liao, C.-H.; Liu, Y.-Y.; Kang, S.-C.; Yeh, C.-N.; Jan, Y.-Y.; Yeh, T.-S. The Impact of Preoperative Etiology on Emergent Pancreaticoduodenectomy for Non-Traumatic Patients. World J. Emerg. Surg. 2017, 12, 21. [Google Scholar] [CrossRef]
- Nickel, F.; Haney, C.M.; Kowalewski, K.F.; Probst, P.; Limen, E.F.; Kalkum, E.; Diener, M.K.; Strobel, O.; Müller-Stich, B.P.; Hackert, T. Laparoscopic Versus Open Pancreaticoduodenectomy. Ann. Surg. 2020, 271, 54–66. [Google Scholar] [CrossRef]
- Hüttner, F.J.; Fitzmaurice, C.; Schwarzer, G.; Seiler, C.M.; Antes, G.; Büchler, M.W.; Diener, M.K. Pylorus-Preserving Pancreaticoduodenectomy (Pp Whipple) versus Pancreaticoduodenectomy (Classic Whipple) for Surgical Treatment of Periampullary and Pancreatic Carcinoma. Cochrane Database Syst. Rev. 2016, 2016, CD006053. [Google Scholar] [CrossRef]
- Mezhir, J.J. Management of Complications Following Pancreatic Resection: An Evidence-Based Approach. J. Surg. Oncol. 2013, 107, 58–66. [Google Scholar] [CrossRef]
- Standop, J.; Glowka, T.; Schmitz, V.; Schaefer, N.; Hirner, A.; Kalff, J.C. Emergency Kausch-Whipple Procedure. Pancreas 2010, 39, 156–159. [Google Scholar] [CrossRef]
- Agha, R.A.; Sohrabi, C.; Mathew, G.; Franchi, T.; Kerwan, A.; O’Neill, N.; Thoma, A.; Beamish, A.J.; Noureldin, A.; Rao, A.; et al. The PROCESS 2020 Guideline: Updating Consensus Preferred Reporting Of CasE Series in Surgery (PROCESS) Guidelines. Int. J. Surg. 2020, 84, 231–235. [Google Scholar] [CrossRef]
- Lissidini, G.; Prete, F.P.; Piccinni, G.; Gurrado, A.; Giungato, S.; Prete, F.; Testini, M. Emergency Pancreaticoduodenectomy: When Is It Needed? A Dual Non-Trauma Centre Experience and Literature Review. Int. J. Surg. 2015, 21, S83–S88. [Google Scholar] [CrossRef]
- Strobel, O.; Schneider, L.; Philipp, S.; Fritz, S.; Büchler, M.W.; Hackert, T. Emergency Pancreatic Surgery—Demanding and Dangerous. Langenbeck’s Arch. Surg. 2015, 400, 837–841. [Google Scholar] [CrossRef]
- Nentwich, M.F.; Reeh, M.; Uzunoglu, F.G.; Bachmann, K.; Bockhorn, M.; Izbicki, J.R.; Vashist, Y.K. Non-Trauma Emergency Pancreatoduodenectomies: A Single-Center Retrospective Analysis. World J. Surg. 2016, 40, 2261–2266. [Google Scholar] [CrossRef]
- Z’graggen, K.; Strobel, O.; Schmied, B.M.; Zimmermann, A.; Büchler, M.W. Emergency Pancreatoduodenectomy in Nontrauma Patients. Pancreas 2002, 24, 258–263. [Google Scholar] [CrossRef]
- Gulla, A.; Tan, W.P.; Pucci, M.J.; Dambrauskas, Z.; Rosato, E.L.; Kaulback, K.R.; Pundzius, J.; Barauskas, G.; Yeo, C.J.; Lavu, H. Emergent Pancreaticoduodenectomy: A Dual Institution Experience and Review of the Literature. J. Surg. Res. 2014, 186, 1–6. [Google Scholar] [CrossRef]
- Driedger, M.R.; Puig, C.A.; Thiels, C.A.; Bergquist, J.R.; Ubl, D.S.; Habermann, E.B.; Grotz, T.E.; Smoot, R.L.; Nagorney, D.M.; Cleary, S.P.; et al. Emergent Pancreatectomy for Neoplastic Disease: Outcomes Analysis of 534 ACS-NSQIP Patients. BMC Surg. 2020, 20, 169. [Google Scholar] [CrossRef]
- Oreskovich, M.R.; Carrico, C.J. Pancreaticoduodenectomy for Trauma: A Viable Option? Am. J. Surg. 1984, 147, 618–623. [Google Scholar] [CrossRef]
- Asensio, J.A.; Petrone, P.; Roldán, G.; Kuncir, E.; Demetriades, D. Pancreaticoduodenectomy: A Rare Procedure for the Management of Complex Pancreaticoduodenal Injuries. J. Am. Coll. Surg. 2003, 197, 937–942. [Google Scholar] [CrossRef]
- Wilden, G.M.V.D.; Yeh, D.D.; Hwabejire, J.O.; Klein, E.N.; Fagenholz, P.J.; King, D.R.; de Moya, M.A.; Chang, Y.; Velmahos, G.C. Trauma Whipple: Do or Don’t After Severe Pancreaticoduodenal Injuries? An Analysis of the National Trauma Data Bank (NTDB). World J. Surg. 2014, 38, 335–340. [Google Scholar] [CrossRef]
- Krige, J.E.; Nicol, A.J.; Navsaria, P.H. Emergency Pancreatoduodenectomy for Complex Injuries of the Pancreas and Duodenum. HPB 2014, 16, 1043–1049. [Google Scholar] [CrossRef][Green Version]
- De Carvalho, M.E.A.J.; Cunha, A.G. Pancreaticodudonectomy in Trauma: One or Two Stages? Injury 2020, 51, 592–596. [Google Scholar] [CrossRef]
- Varshney, V.K.; Nayar, R.; Sreesanth, K.S.; Soni, S.; Varshney, B. Emergency Pancreatoduodenectomy for Ampullary Cancer Post-Iatrogenic Duodenal Perforation: No Option but to Strike. Cureus 2020, 12, e11384. [Google Scholar] [CrossRef]
- Yagi, S.; Ida, S.; Ohashi, M.; Kumagai, K.; Hiki, N.; Sano, T.; Nunobe, S. Two Cases of a Perforated Duodenal Diverticulum after Gastrectomy with Roux-En-Y Reconstruction. Surg. Case Rep. 2019, 5, 169. [Google Scholar] [CrossRef]
- Mirea, C.S.; Ciorbagiu, M.C.; Obleaga, C.V.; Moraru, E. Stage IV Duodenal GIST Requiring Emergency Pancreaticoduodenectomy—Diagnosis Difficulties and Therapeutic Options. Rom. J. Morphol. Embryol. 2018, 59, 543–548. [Google Scholar]
- Sakakima, Y.; Inoue, S.; Fujii, T.; Hatsuno, T.; Takeda, S.; Kaneko, T.; Nagasaka, T.; Nakao, A. Emergency Pylorus-Preserving Pancreatoduodenectomy Followed by Second-Stage Pancreatojejunostomy for a Gastrointestinal Stromal Tumor of the Duodenum with an Intratumoral Gas Figure: Report of a Case. Surg. Today 2004, 34, 701–705. [Google Scholar] [CrossRef]
- Hecker, A.; Hecker, B.; Bassaly, B.; Hirschburger, M.; Schwandner, T.; Janßen, H.; Padberg, W. Dramatic Regression and Bleeding of a Duodenal GIST during Preoperative Imatinib Therapy: Case Report and Review. World J. Surg. Oncol. 2010, 8, 47. [Google Scholar] [CrossRef]
- Lupascu, C.; Trofin, A.; Zabara, M.; Vornicu, A.; Cadar, R.; Vlad, N.; Apopei, O.; Grigorean, V.; Lupascu-Ursulescu, C. Emergency Backwards Whipple for Bleeding: Formidable and Definitive Surgery. Gastroenterol. Res. Pract. 2017, 2017, 2036951. [Google Scholar] [CrossRef]
- Lupascu, C.; Ursulescu, C.; Andronic, D. Emergency Pancreaticoduodenectomy for Bleeding Pancreatic Pseudoaneurysm in Patient with Common Mesentery and Replaced Right Hepatic Artery. Chirurgia 2013, 108, 910–914. [Google Scholar]
- Pang, T.C.Y.; Maher, R.; Gananadha, S.; Hugh, T.J.; Samra, J.S. Peripancreatic Pseudoaneurysms: A Management-Based Classification System. Surg. Endosc. 2014, 28, 2027–2038. [Google Scholar] [CrossRef]
- Shell, M.; Reinhart, E.; Smith, S.; DeMarris, D.; Naumann, C. Successful Minimally Invasive Management of a Gastroduodenal Artery Pseudoaneurysm Causing Extrinsic Bile Duct Compression. ACG Case Rep. J. 2021, 8, e00663. [Google Scholar] [CrossRef]
- Koichopolos, J.; Keow, J.; Parfitt, J.; Yoshy, C.; Wiseman, D.; Leslie, K. Complete Duodenal Necrosis Associated with Non-Traumatic Duodenal Hematoma Requiring Emergent Pancreatico-Duodenectomy. Int. J. Surg. Case Rep. 2020, 66, 53–57. [Google Scholar] [CrossRef]
- Tuech, J.-J.; Pessaux, P.; Rege, N.; Bergamaschi, R.; Arnaud, J.-P. Emergency Pancreaticoduodenectomy with Delayed Reconstruction for Bleeding: A Life Saving Procedure. Int. J. Pancreatol. 2001, 29, 59–62. [Google Scholar] [CrossRef]
- Stratigos, P.; Kouskos, E.; Kouroglou, M.; Chrisafis, I.; Fois, L.; Mavrogiorgis, A.; Axiotis, E.; Zamtrakis, S. Emergency Pancreatoduodenectomy (Whipple Procedure) for Massive Upper Gastrointestinal Bleeding Caused by a Diffuse B-Cell Lymphoma of the Duodenum: Report of a Case. Surg. Today 2007, 37, 680–684. [Google Scholar] [CrossRef]
- Eftimie, M.A.; Lungu, V.; Tudoroiu, M.; Vatachki, G.; Batca, S.; David, L. Emergency Pancreatico-Duodenectomy with Superior Mesenteric and Portal Vein Resection and Reconstruction Using a Gore-Tex Vascular Graft. Chirurgia 2017, 112, 50–57. [Google Scholar] [CrossRef]
- Dumitrascu, T.; Ionescu, M.I.; David, L.; Popescu, I. Emergency Pancreaticoduodenectomy in a Patient with an Ampullary Adenocarcinoma Associated with Severe Acute Pancreatitis: A Case Report. Chirurgia 2011, 106, 409–413. [Google Scholar]
- Schorn, S.; Demir, I.E.; Vogel, T.; Schirren, R.; Reim, D.; Wilhelm, D.; Friess, H.; Ceyhan, G.O. Mortality and Postoperative Complications after Different Types of Surgical Reconstruction Following Pancreaticoduodenectomy—A Systematic Review with Meta-Analysis. Langenbeck’s Arch. Surg. 2019, 404, 141–157. [Google Scholar] [CrossRef]
- Maeda, H.; Okabayashi, T.; Kobayashi, M.; Araki, K.; Kohsaki, T.; Nishimori, I.; Onishi, S.; Ito, S.; Ogawa, Y.; Okuda, H.; et al. Emergency Pancreatoduodenectomy for Pancreatic Metastasis from Renal Cell Carcinoma in a Patient with von Hipple-Lindau Disease: A Case Report. Dig. Dis. Sci. 2006, 51, 1383–1387. [Google Scholar] [CrossRef]
- Parray, F.Q.; Lone, I.M.; Chowdri, N.A.; Wani, I.; Wani, M.A.; Gulzar, G.M.; Thakur, N. Emergency Pancreaticoduodenectomy in Duodenal Paraganglioma: Case Report. ISRN Surg. 2011, 2011, 268674. [Google Scholar] [CrossRef][Green Version]
- Kamei, K.; Yasuda, T.; Nakata, Y.; Yamazaki, M.; Ishikawa, H.; Nakai, T.; Takeyama, Y. Gastrointestinal Bleeding as the Initial Manifestation of Pancreatic Adenocarcinoma Successfully Treated by Emergency Pancreaticoduodenectomy: Case Report. Acta Med. Kinki Univ. 2012, 37, 95–97. [Google Scholar]
- Okabayashi, T.; Shima, Y.; Iwata, J.; Sumiyoshi, T.; Kozuki, A.; Tokumaru, T.; Hata, Y.; Noda, Y.; Inagaki, T.; Morishita, S.; et al. Primary Liposarcoma of the Duodenum: A First Case Presentation. Intern. Med. 2013, 52, 2753–2757. [Google Scholar] [CrossRef]
- Emiloju, O.; Candelario, N.; Dourado, C. Metastatic Clear Cell Endometrial Carcinoma: An Unusual Cause of a Common Clinical Presentation. BMJ Case Rep. 2020, 13, e235051. [Google Scholar] [CrossRef]
| No | Year | Age (Years) | Sex | Living Area | Reason for Emergency Presentation | Diagnosis |
|---|---|---|---|---|---|---|
| 1 | 2014 | 65 | M | R | Postoperative complication | Complex iatrogenic lesion of the distal bile duct, duodenum, and head of pancreas |
| 2 | 2016 | 47 | M | U | UGIB-melena | Bleeding duodenal tumor |
| 3 | 2017 | 44 | M | U | UGIB-melena | Fistulized pancreaticoduodenal artery aneurysm in the duodenum |
| 4 | 2021 | 53 | M | R | Upper abdominal pain. Altered general state. | Ruptured gastroduodenal artery aneurysm |
| No | PD Type | Reconstruction of Pancreatic Remnant | Operative Time (min) | Blood Loss (mL) |
|---|---|---|---|---|
| 1 | PD CW | PG | 190 | 300 |
| 2 | PD CW | PG | 300 | 300 |
| 3 | PD PP | PJ | 210 | 700 |
| 4 | PD CW | PJ | 275 | 400 |
| No | In Hospital Stay Days | Intensive Care Unit Stay Days | Complication | Reinterventions | Intra Hospital Death | Postoperative Survival Time (Days) |
|---|---|---|---|---|---|---|
| 1 | 12 | 7 | - | - | 2047 | |
| 2 | 31 | 19 | Intestinal obstruction Wound infection Internal jugular vein thrombosis Clostridium Difficile infection | Yes—Segmental enterectomy | - | 1698 (alive) |
| 3 | 12 | 5 | - | - | 1548 (alive) | |
| 4 | 20 | 20 | HJ anastomotic fistula Thrombosis of IVC and iliac veins Left hepatic lobe ischaemia | Yes—Redo of the HJ | Yes | 20 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schlanger, D.; Popa, C.; Ciocan, A.; Șofron, C.; Al Hajjar, N. Emergency Pancreatoduodenectomy: A Non-Trauma Center Case Series. J. Clin. Med. 2022, 11, 2891. https://doi.org/10.3390/jcm11102891
Schlanger D, Popa C, Ciocan A, Șofron C, Al Hajjar N. Emergency Pancreatoduodenectomy: A Non-Trauma Center Case Series. Journal of Clinical Medicine. 2022; 11(10):2891. https://doi.org/10.3390/jcm11102891
Chicago/Turabian StyleSchlanger, Diana, Călin Popa, Andra Ciocan, Cornelia Șofron, and Nadim Al Hajjar. 2022. "Emergency Pancreatoduodenectomy: A Non-Trauma Center Case Series" Journal of Clinical Medicine 11, no. 10: 2891. https://doi.org/10.3390/jcm11102891
APA StyleSchlanger, D., Popa, C., Ciocan, A., Șofron, C., & Al Hajjar, N. (2022). Emergency Pancreatoduodenectomy: A Non-Trauma Center Case Series. Journal of Clinical Medicine, 11(10), 2891. https://doi.org/10.3390/jcm11102891






