Dissatisfaction with Married Life in Men Is Related to Increased Stroke and All-Cause Mortality
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Data Assessment
2.3. Stroke and All-Cause Mortality Assessment
2.4. Marital Satisfaction Assessment
2.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cherlin, A.J. Marriage, Divorce, Remarriage (Rev. and enl. ed.); Harvard University Press: Cambridge, MA, USA, 1992. [Google Scholar]
- Robles, T.F. Marital Quality and Health: Implications for Marriage in the 21st Century. Curr. Dir. Psychol. Sci. 2014, 23, 427–432. [Google Scholar] [CrossRef] [PubMed]
- Bennett-Britton, I.; Teyhan, A.; Macleod, J.; Sattar, N.; Smith, G.D.; Ben-Shlomo, Y. Changes in marital quality over 6 years and its association with cardiovascular disease risk factorsm in men: Findings from the ALSPAC prospectiven cohort study. J. Epidemiol. Community Health 2017, 71, 1094–1100. [Google Scholar] [CrossRef] [PubMed]
- Fincham, F.D.; Bradbury, T.N. The Impact of Attributions in Marriage: A Longitudinal Analysis. J. Pers. Soc. Psychol. 1987, 53, 510–517. [Google Scholar] [CrossRef] [PubMed]
- Robles, T.F.; Slatcher, R.B.; Trombello, J.M.; McGinn, M.M. Marital quality and health: A meta-analytic review. Psychol. Bull. 2014, 140, 140–187. [Google Scholar] [CrossRef] [PubMed]
- Coyne, J.C.; Rohrbaugh, M.J.; Shoham, V.; Sonnega, J.S.; Nicklas, J.M.; Cranford, J.A. Prognostic importance of marital quality for survival of congestive heart failure. Am. J. Cardiol. 2001, 88, 526–529. [Google Scholar] [CrossRef]
- King, K.B.; Reis, H.T. Marriage and long-term survival after coronary artery bypass grafting. Health Psychol. 2012, 31, 55–62. [Google Scholar] [CrossRef]
- Whisman, M.A.; Gilmour, A.L.; Salinger, J.M. Marital satisfaction and mortality in the United States adult population. Health Psychol. 2018, 37, 1041–1044. [Google Scholar] [CrossRef]
- Goldbourt, U.; Yaari, S.; Medalie, J.H. Factors Predictive of Long-Term Coronary Heart Disease Mortality among 10,059 Male Israeli Civil Servants and Municipal Employees. Cardiology 1993, 82, 100–121. [Google Scholar] [CrossRef]
- Tanne, D.; Yaari, S.; Goldbourt, U. Risk Profile and Prediction of Long-Term Ischemic Stroke Mortality. Circulation 1998, 98, 1365–1371. [Google Scholar] [CrossRef]
- Kahn, H.A.; Medalie, J.H.; Neufeld., H.N.; Riss, E.; Balogh, M.; Groen, J.S.I. Serum cholesterol: Its distribution and association with dietary and other variables in a survey of 10,000 men-PubMed. Israel J. Med. Sci. 1969, 5, 1117–1127. [Google Scholar]
- Roach, A.J.; Frazier, L.P.; Bowden, S.R. The Marital Satisfaction Scale: Development of a Measure for Intervention Research. J. Marriage Fam. 1981, 43, 537. [Google Scholar] [CrossRef]
- Fowers, B.J.; Olson, D.H. ENRICH Marital Satisfaction Scale: A Brief. Research and Clinical Tool. J. Fam. Psychol. 1993, 7, 176–185. [Google Scholar] [CrossRef]
- Kim, E.S.; Kubzansky, L.D.; Soo, J.; Boehm, J.K. Maintaining Healthy Behavior: A Prospective Study of Psychological Well-Being and Physical Activity. Ann. Behav. Med. 2017, 51, 337–347. [Google Scholar] [CrossRef]
- Koivumaa-Honkanen, H.; Honkanen, R.; Viinamäki, H.; Heikkilä, K.; Kaprio, J.; Koskenvuo, M. Self-reported Life Satisfaction and 20-Year Mortality in Healthy Finnish Adults. Am. J. Epidemiol. 2000, 152, 983–991. [Google Scholar] [CrossRef] [PubMed]
- Pillay-van Wyk, V.; Bradshaw, D. Mortality and socioeconomic status: The vicious cycle between poverty and ill health. Lancet Glob. Health 2017, 5, e851–e852. [Google Scholar] [CrossRef]
- Lotan, K.; Goldbourt, U.; Gerber, Y. Smoking Status and Incidence of Cancer After Myocardial Infarction: A Follow-Up Study of over 20 Years. Am. J. Med. 2017, 130, 1084–1091. [Google Scholar] [CrossRef] [PubMed]
- Doll, R.; Peto, R.; Boreham, J.; Sutherland, I. Mortality in relation to smoking: 50 Years’ observations on male British doctors. Br. Med. J. 2004, 328, 1519–1528. [Google Scholar] [CrossRef] [PubMed]
- Spring, B.; King, A.C.; Pagoto, S.L.; Van Horn, L.; Fisher, J.D. Fostering multiple healthy lifestyle behaviors for primary prevention of cancer. Am. Psychol. 2015, 70, 75–90. [Google Scholar] [CrossRef]
- Gerber, Y.; Myers, V.; Goldbourt, U.; Benyamini, Y.; Scheinowitz, M.; Drory, Y. Long-term trajectory of leisure time physical activity and survival after first myocardial infarction: A population-based cohort study. Eur. J. Epidemiol. 2011, 26, 109–116. [Google Scholar] [CrossRef]
- Paffenbarger, R.S.; Blair, S.N.; Lee, I.M. A history of physical activity, cardiovascular health and longevity: The scientific contributions of Jeremy N Morris, DSc, DPH, FRCP. Int. J. Epidemiol. 2001, 30, 1184–1192. [Google Scholar] [CrossRef]
- Booth, F.W.; Roberts, C.K.; Thyfault, J.P.; Ruegsegger, G.N.; Toedebusch, R.G. Role of inactivity in chronic diseases: Evolutionary insight and pathophysiological mechanisms. Physiol. Rev. 2017, 97, 1351–1402. [Google Scholar] [CrossRef]
- Brubaker, T.; Challenges, J.K.-F. Relations: Undefined Challenges to the American Family; Sage: Newbury Park, CA, USA, 1993. [Google Scholar]
- Gottman, J.M. What Predicts Divorce? The Relationship between Marital Processes and Marital Outcomes; Lawrence Erlbaum Associates, Inc.: Mahwah, NJ, USA, 1994. [Google Scholar]
- Allred, C. Age Variation in the Divorce Rate, 1990 & 2017. Fam. Profiles 1990, 13. [Google Scholar] [CrossRef]
- Bulanda, J.R.; Brown, J.S.; Yamashita, T. Marital quality, marital dissolution, and mortality risk during the later life course. Soc. Sci. Med. 2016, 165, 119–127. [Google Scholar] [CrossRef]
- Sbarra, D.A.; Law, R.W.; Portley, R.M. Divorce and Death: A Meta-Analysis and Research Agenda for Clinical, Social, and Health Psychology. Perspect. Psychol. Sci. 2011, 6, 454–474. [Google Scholar] [CrossRef]
- Sbarra, D.A. Divorce and health: Current trends and future directions. Psychosom. Med. 2015, 77, 227–236. [Google Scholar] [CrossRef]
- Carstensen, L.L.; Gottman, J.M.; Levenson, R.W. Emotional behavior in long-term marriage. Psychol Aging. 1995, 10, 140–149. [Google Scholar] [CrossRef]
- Birditt, K.S.; Brown, E.; Orbuch, T.L.; McIlvane, J.M. Marital Conflict Behaviors and Implications for Divorce Over 16 Years. J. Marriage Fam. 2010, 72, 1188–1204. [Google Scholar] [CrossRef] [PubMed]
- Parenting Support | Adler Centre: Adlerian Psychology Association of BC. Available online: https://adlercentre.ca/parenting-workshops/ (accessed on 28 August 2020).
- Walsh, F. A family resilience framework: Innovative practice applications. Fam. Relat. 2002, 51, 130–137. [Google Scholar] [CrossRef]
- Halford, W.K. Treatment Manuals for Practitioners. Brief Therapy for Couples: Helping Partners Help Themselves; The Guilford Press: New York, NY, USA, 2001. [Google Scholar]
- Shapiro, A.F.; Gottman, J.M. Effects on Marriage of a Psycho-Communicative-Educational Intervention With Couples Undergoing the Transition to Parenthood, Evaluation at 1-Year Post Intervention. J. Fam. Commun. 2005, 5, 1–24. [Google Scholar] [CrossRef]
- Tanne, D.; Goldbourt, U.; Medalie, J.H. Perceived Family Difficulties and Prediction of 23-Year Stroke Mortality among Middle-Aged Men. Cereb. Dis. 2004, 18, 277–282. [Google Scholar] [CrossRef] [PubMed]
- Johnson, D.R.; Amoloza, T.O.; Booth, A. Stability and Developmental Change in Marital Quality: A Three-Wave Panel Analysis. J. Marriage Fam. 1992, 54, 582. [Google Scholar] [CrossRef]
- Johnson, D.R.; Booth, A. Marital Quality: A Product of the Dyadic Environment or Individual Factors? Soc. Forces 1998, 76, 883–904. [Google Scholar] [CrossRef]
- Stavrova, O. Having a Happy Spouse Is Associated With Lowered Risk of Mortality. Psychol. Sci. 2019, 30, 798–803. [Google Scholar] [CrossRef] [PubMed]
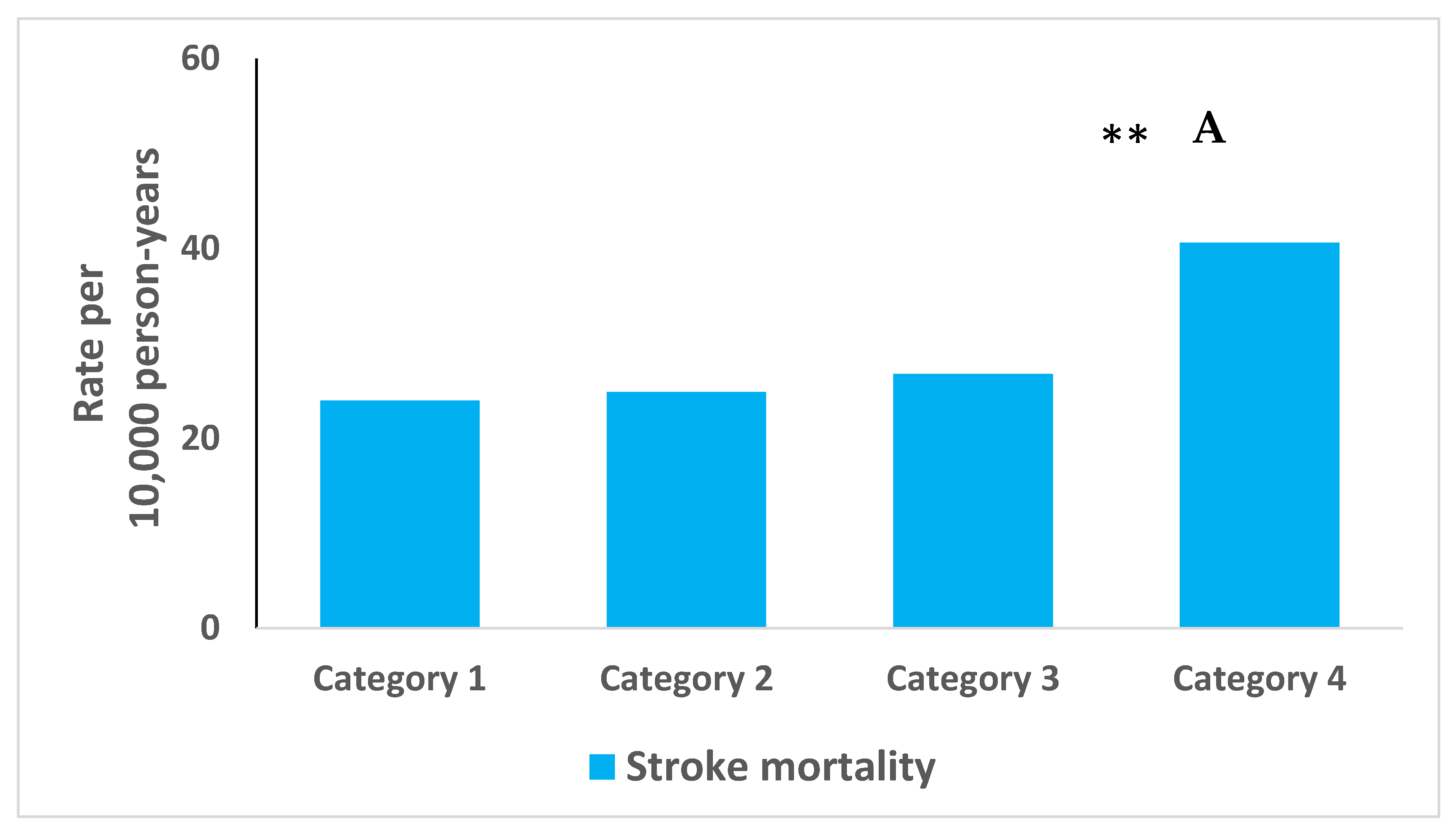
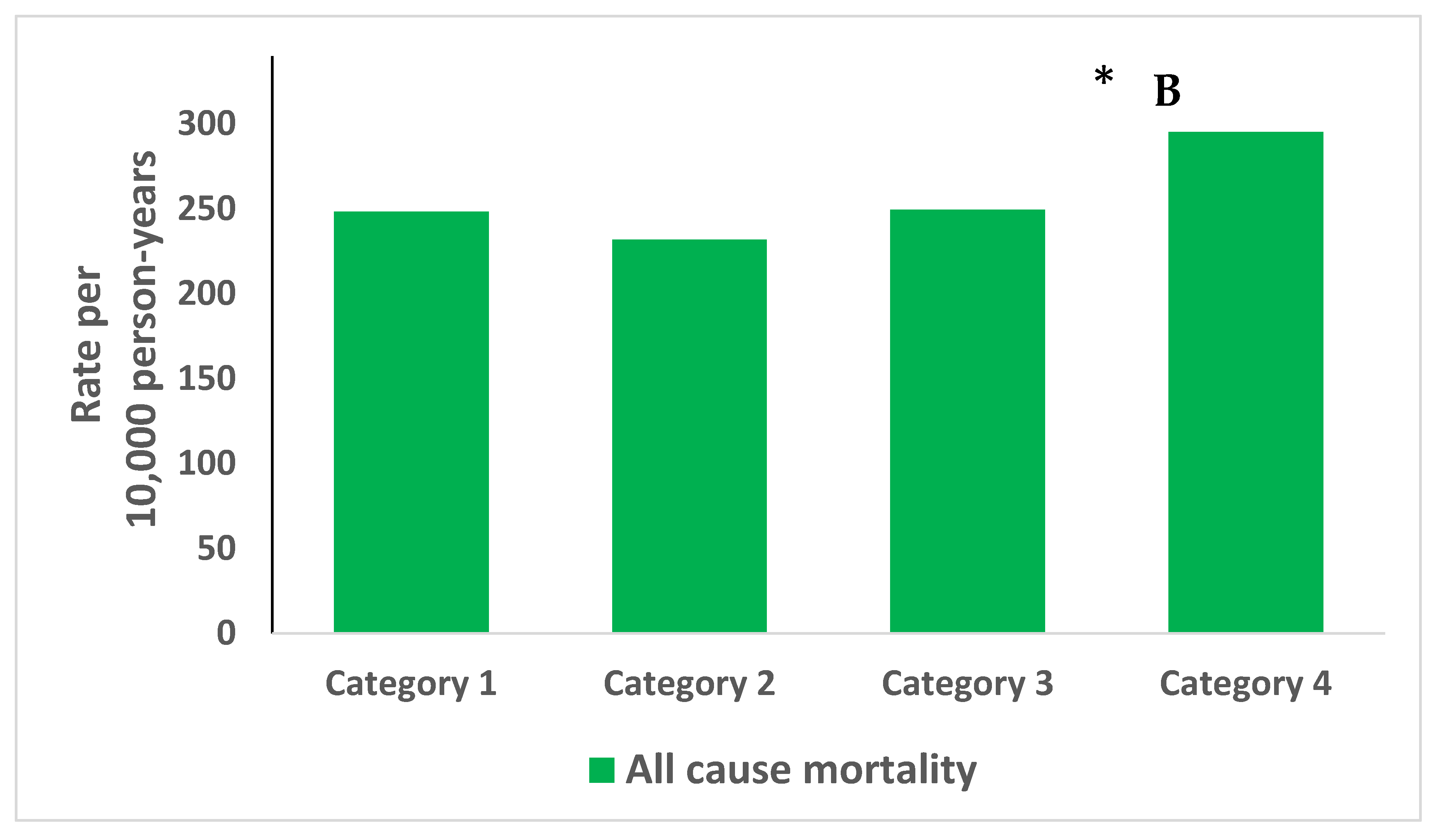
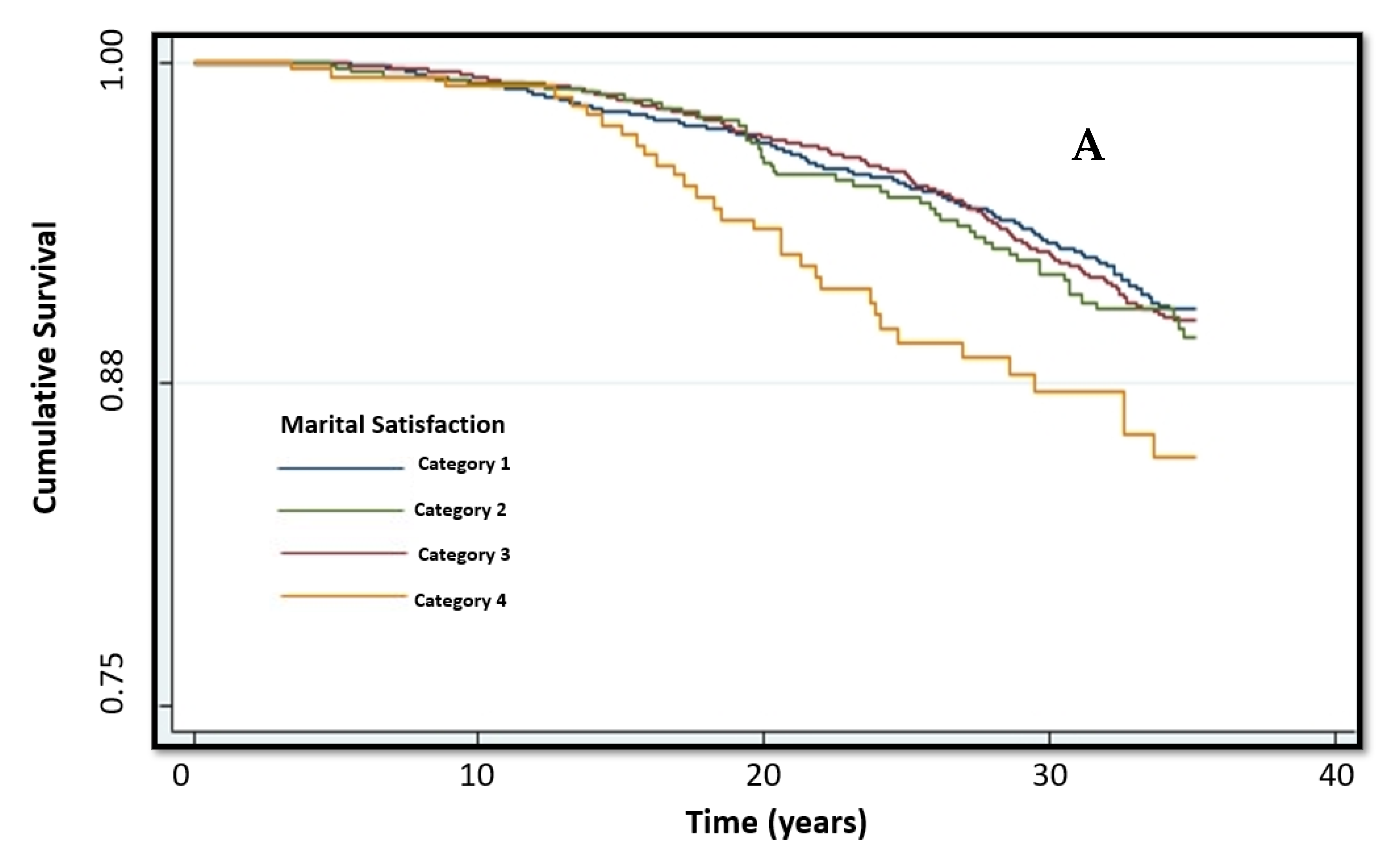
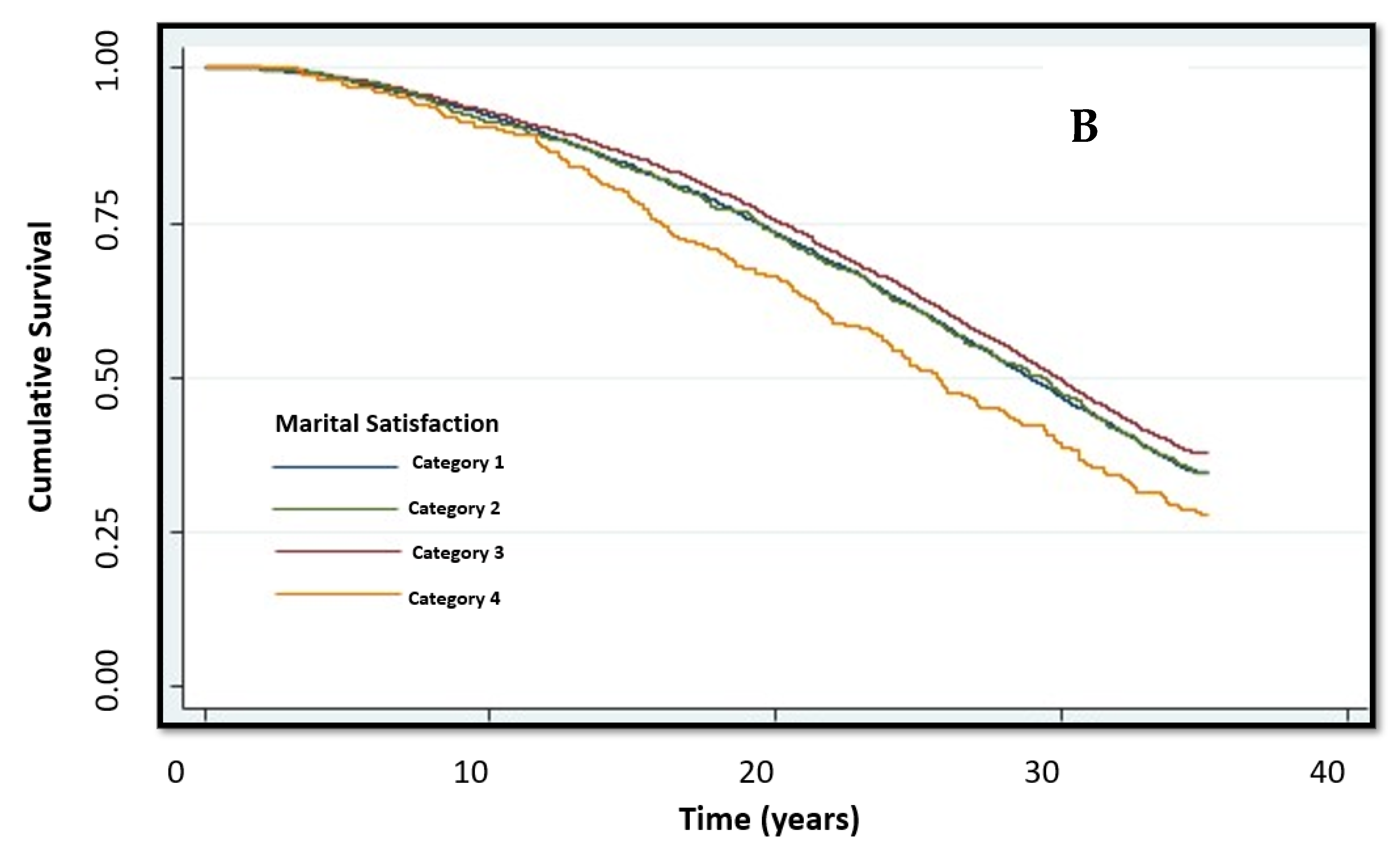
| Characteristic | Total Study Population | Category 1 (n = 3829) | Category 2 (n = 4052) | Category 3 (n = 741) | Category 4 (n = 323) | P of Trend |
|---|---|---|---|---|---|---|
| Age (y) | 49.1 ± 6.7 | 49.5 ± 6.7 | 48.8 ± 6.6 | 49.1 ± 6.7 | 49.4 ± 6.8 | p < 0.01 |
| Systolic pressure (mmHg) | 138 ± 22 | 139 ± 22 | 137 ± 21 | 136 ± 21 | 136 ± 20 | 0.01 |
| Diastolic pressure (mmHg) | 84 ± 11 | 87 ± 12 | 86 ± 12 | 85 ± 12 | 86 ± 11 | p < 0.01 |
| Total cholesterol (mg/dl) | 208 ± 39 | 208 ± 39 | 207 ± 38 | 206 ± 38 | 208 ± 40 | 0.36 |
| HDL-c (mg/dl) | 40.8 ± 9.6 | 40.9 ± 9.5 | 40.7 ± 9.7 | 40.8 ± 9.5 | 40.0 ± 9.9 | 0.22 |
| Diabetes (%) | 4.6 | 4.9 | 4.2 | 4.0 | 6.2 | 0.19 |
| Smoking (% at any time) | 67.7 | p < 0.01 | ||||
| Never smoking | 32.3 | 32.1 | 33.3 | 31.1 | 24.3 | |
| Quit smoking | 16.8 | 17.4 | 16.9 | 14.3 | 15.1 | |
| 1–10 cigarettes p/day | 15.2 | 14.5 | 15.3 | 16.5 | 18.0 | |
| 11–20 cigarettes p/day | 16.3 | 17.1 | 15.6 | 15.8 | 16.7 | |
| 20+ cigarettes p/day | 19.4 | 18.9 | 18.9 | 22.3 | 25.9 | |
| BMI | 25.9 ± 3.2 | 25.9 ± 3.3 | 25.9 ± 3.2 | 25.9 ± 3.2 | 25.8 ± 3.5 | 0.99 |
| Leisure-time physical activity (%) | 0.15 | |||||
| None | 60.4 | 57.6 | 57.4 | 59.0 | ||
| Sporadic | 13.7 | 15.7 | 15.8 | 14.7 | ||
| Light | 18.1 | 18.7 | 18.1 | 18.3 | ||
| Intensive | 7.8 | 8.0 | 8.7 | 8.0 | ||
| SES | 2.6 ± 1.2 | 2.6 ± 1.3 | 2.6 ± 1.2 | 2.4 ± 1.1 | 1 ± 1.2 | p < 0.01 |
| Family problems | 3.5 ± 2.4 | 2.7 ± 2.1 | 3.0 ± 2.2 | 4.3 ± 2.3 | 4.5 ± 2.3 | p < 0.01 |
| Analysis | Stroke Mortality | All-Cause Mortality | |||
|---|---|---|---|---|---|
| HR | 95% CI | HR | 95% CI | ||
| Model 1 | |||||
| Category 2 | 1.11 | 0.93–1.32 | 0.99 | 0.94–1.14 | |
| Category 3 | 1.16 | 0.86–1.57 | 1.04 | 0.94–1.15 | |
| Category 4 | 1.75 | 1.21–2.53 | 1.23 | 1.07–1.40 | |
| Model 2 | |||||
| Category 2 | 1.18 | 0.99–1.41 | 1.02 | 0.97–1.08 | |
| Category 3 | 1.3 | 0.96–1.76 | 1.08 | 0.98–1.20 | |
| Category 4 | 1.95 | 1.34–2.82 | 1.26 | 1.10–1.44 | |
| Model 3 | |||||
| Category 2 | 1.15 | 0.95–1.38 | 1.02 | 0.96–1.08 | |
| Category 3 | 1.11 | 0.80–1.55 | 1.06 | 0.95–1.18 | |
| Category 4 | 1.94 | 1.41–2.90 | 1.21 | 1.04–1.41 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lev-ari, S.; Gepner, Y.; Goldbourt, U. Dissatisfaction with Married Life in Men Is Related to Increased Stroke and All-Cause Mortality. J. Clin. Med. 2021, 10, 1729. https://doi.org/10.3390/jcm10081729
Lev-ari S, Gepner Y, Goldbourt U. Dissatisfaction with Married Life in Men Is Related to Increased Stroke and All-Cause Mortality. Journal of Clinical Medicine. 2021; 10(8):1729. https://doi.org/10.3390/jcm10081729
Chicago/Turabian StyleLev-ari, Shahar, Yftach Gepner, and Uri Goldbourt. 2021. "Dissatisfaction with Married Life in Men Is Related to Increased Stroke and All-Cause Mortality" Journal of Clinical Medicine 10, no. 8: 1729. https://doi.org/10.3390/jcm10081729
APA StyleLev-ari, S., Gepner, Y., & Goldbourt, U. (2021). Dissatisfaction with Married Life in Men Is Related to Increased Stroke and All-Cause Mortality. Journal of Clinical Medicine, 10(8), 1729. https://doi.org/10.3390/jcm10081729







