Oral Complications of ICU Patients with COVID-19: Case-Series and Review of Two Hundred Ten Cases
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Case-Series of ICU Patients in Banska Bystrica
3.1.1. Case Report No. 1
3.1.2. Case Report No. 2
3.1.3. Case Report No. 3
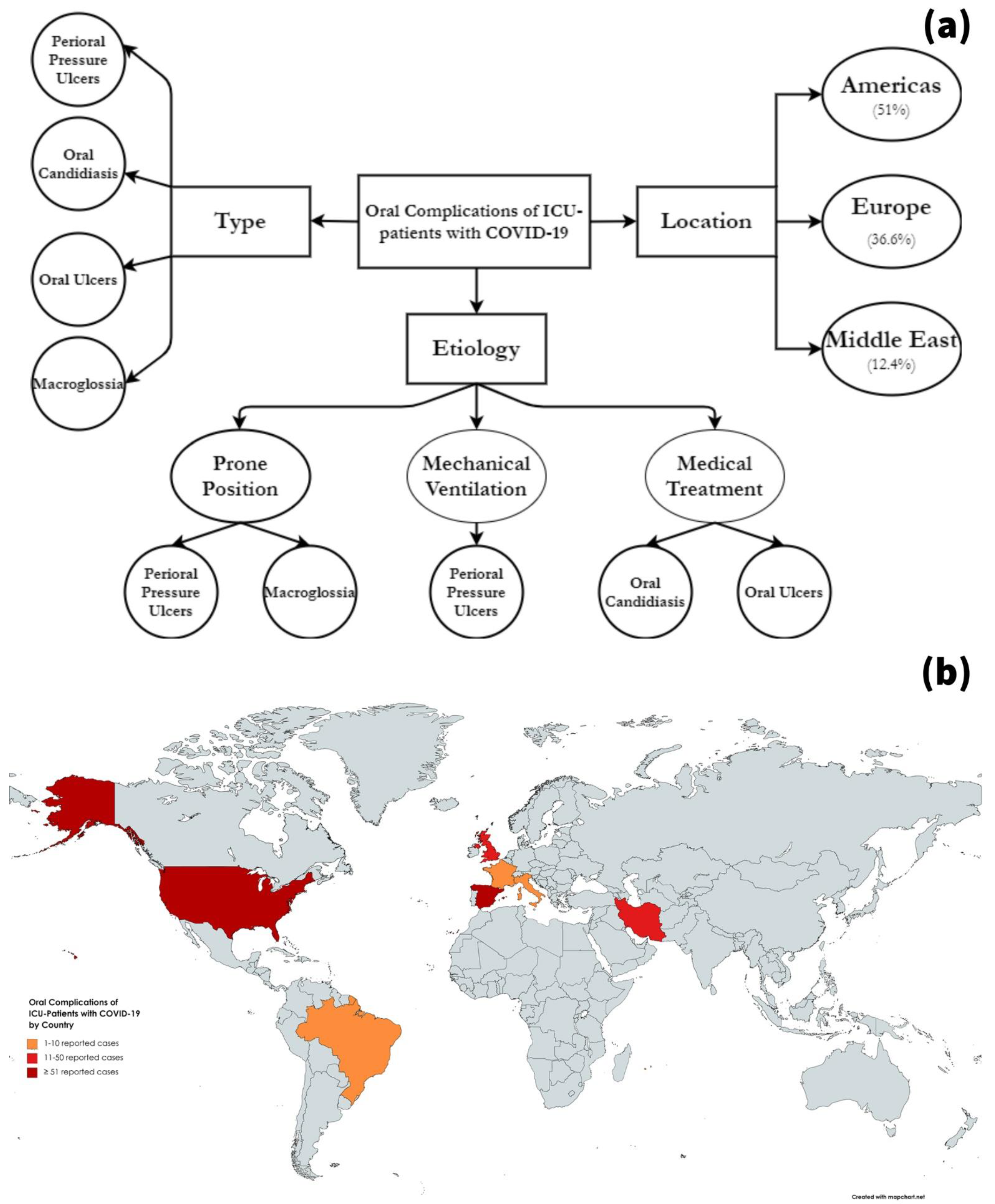
3.2. Literature Review
3.2.1. Perioral Pressure Ulcers (ICD-11: EH90)
3.2.2. Oral Candidiasis (ICD-11: 1F23.0)
3.2.3. Oral Ulcers (ICD-11: DA01)
3.2.4. Macroglossia (ICD-11: DA03.5)
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Iranmanesh, B.; Khalili, M.; Amiri, R.; Zartab, H.; Aflatoonian, M. Oral manifestations of COVID -19 disease: A review article. Dermatol. Ther. 2020, 14578. [Google Scholar] [CrossRef]
- Riad, A.; Klugar, M.; Krsek, M. COVID-19-Related Oral Manifestations: Early Disease Features? Oral Dis. 2020, 13516. [Google Scholar] [CrossRef] [PubMed]
- Riad, A.; Kassem, I.; Badrah, M.; Klugar, A.M. The manifestation of oral mucositis in COVID-19 patients: A case-series. Dermatol. Ther. 2020, 33, e14479. [Google Scholar] [CrossRef]
- Riad, A.; Kassem, I.; Issa, J.; Badrah, M.; Klugar, M. Angular cheilitis of COVID-19 patients: A case-series and literature review. Oral Dis. 2020, 13675. [Google Scholar] [CrossRef]
- Riad, A.; Kassem, I.; Stanek, J.; Badrah, M.; Klugarova, J.; Klugar, M. Aphthous Stomatitis in COVID -19 Patients: Case-series and Literature Review. Dermatol. Ther. 2021, e14735. [Google Scholar] [CrossRef]
- Riad, A.; Kassem, I.; Badrah, M.; Klugar, M. Acute parotitis as a presentation of COVID-19? Oral Dis. 2020, 13571. [Google Scholar] [CrossRef]
- Riad, A.; Kassem, I.; Hockova, B.; Badrah, M.; Klugar, M. Tongue Ulcers Associated with SARS-COV-2 Infection: A case-series. Oral Dis. 2020, 13635. [Google Scholar] [CrossRef]
- Xu, H.; Zhong, L.; Deng, J.; Peng, J.; Dan, H.; Zeng, X.; Li, T.; Chen, Q. High expression of ACE2 receptor of 2019-nCoV on the epithelial cells of oral mucosa. Int. J. Oral Sci. 2020, 12, 1–5. [Google Scholar] [CrossRef]
- Dziedzic, A.; Wojtyczka, R.D. The impact of coronavirus infectious disease 19 (COVID-19) on oral health. Oral Dis. 2020, 13359. [Google Scholar] [CrossRef]
- UpToDate Coronavirus Disease 2019 (COVID-19): Critical Care and Airway Management Issues. Available online: https://www.uptodate.com/contents/coronavirus-disease-2019-covid-19-critical-care-and-airway-management-issues (accessed on 7 January 2021).
- Wollina, U.; Nowak, A. Dermatology in the Intensive Care Unit. Our Dermatol. Online 2012, 3, 298–303. [Google Scholar] [CrossRef]
- Zhao, T.; Wu, X.; Zhang, Q.; Li, C.; Worthington, H.V.; Hua, F. Oral hygiene care for critically ill patients to prevent ventilator-associated pneumonia. Cochrane Database Syst. Rev. 2020, 12, CD008367. [Google Scholar] [CrossRef]
- Pokorná, A.; Benešová, K.; Jarkovský, J.; Mužík, J.; Beeckman, D. Pressure Injuries in Inpatient Care Facilities in the Czech Republic. J. Wound, Ostomy Cont. Nurs. 2017, 44, 331–335. [Google Scholar] [CrossRef]
- Badia, M.; Trujillano, J.; Gascó, E.; Casanova, J.M.; Alvarez, M.; León, M. Skin lesions in the ICU. Intensiv. Care Med. 1999, 25, 1271–1276. [Google Scholar] [CrossRef]
- Gagnier, J.J.; Kienle, G.; Altman, D.G.; Moher, D.; Sox, H.; Riley, D.; Allaire, A.; The CARE Group. The CARE guidelines: Consensus-based clinical case reporting guideline development. BMJ Case Rep. 2013, 53, 1541–1547. [Google Scholar] [CrossRef]
- World Medical Association. World medical association declaration of Helsinki: Ethical principles for medical research involving human subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef]
- Holt, E. COVID-19 testing in Slovakia. Lancet Infect. Dis. 2021, 21, 32. [Google Scholar] [CrossRef]
- Committee on Publication Ethics (COPE). Core Practices. Available online: https://publicationethics.org/core-practices (accessed on 7 January 2021).
- Seirafianpour, F.; Sodagar, S.; Pour Mohammad, A.; Panahi, P.; Mozafarpoor, S.; Almasi, S.; Goodarzi, A. Cutaneous manifestations and considerations in COVID-19 pandemic: A systematic review. Dermatol. Ther. 2020, 33, e13986. [Google Scholar] [CrossRef]
- Rekhtman, S.; Tannenbaum, R.; Strunk, A.; Birabaharan, M.; Wright, S.; Grbic, N.; Joseph, A.; Lin, S.K.; Zhang, A.C.; Lee, E.C.; et al. Eruptions and Related Clinical Course Among 296 Hospitalized Adults with Confirmed COVID-19. J. Am. Acad. Dermatol. 2020. [Google Scholar] [CrossRef]
- Martel, T.; Orgill, D.P. Medical Device–Related Pressure Injuries during the COVID-19 Pandemic. J. Wound Ostomy Cont. Nurs. 2020, 47, 430–434. [Google Scholar] [CrossRef]
- Ibarra, G.; Rivera, A.; Fernandez-Ibarburu, B.; Lorca-García, C.; Garcia-Ruano, A. Prone position pressure sores in the COVID-19 pandemic: The Madrid experience. J. Plast. Reconstr. Aesthetic Surg. 2020. [Google Scholar] [CrossRef]
- Shearer, S.C.; Parsa, K.M.; Bs, A.N.; Bs, T.P.; Walsh, A.R.; Fernandez, S.; Gao, W.Z.; Pierce, M.L. Facial Pressure Injuries from Prone Positioning in the COVID-19 Era. Laryngoscope 2021, 29374. [Google Scholar] [CrossRef]
- Salehi, M.; Ahmadikia, K.; Mahmoudi, S.; Kalantari, S.; Siahkali, S.J.; Izadi, A.; Kord, M.; Manshadi, S.A.D.; Seifi, A.; Ghiasvand, F.; et al. Oropharyngeal candidiasis in hospitalised COVID-19 patients from Iran: Species identification and antifungal susceptibility pattern. Mycoses 2020, 63, 771–778. [Google Scholar] [CrossRef]
- Sleiwah, A.; Nair, G.; Mughal, M.; Lancaster, K.; Ahmad, I. Perioral pressure ulcers in patients with COVID-19 requiring invasive mechanical ventilation. Eur. J. Plast. Surg. 2020, 43, 727–732. [Google Scholar] [CrossRef]
- Dos Santos, J.A.; Normando, A.G.C.; Da Silva, R.L.C.; De Paula, R.M.; Cembranel, A.C.; Santos-Silva, A.R.; Guerra, E.N.S. Oral mucosal lesions in a COVID-19 patient: New signs or secondary manifestations? Int. J. Infect. Dis. 2020, 97, 326–328. [Google Scholar] [CrossRef]
- Andrews, E.; Lezotte, J.; Ackerman, A.M. Lingual compression for acute macroglossia in a COVID-19 positive patient. BMJ Case Rep. 2020, 13, e237108. [Google Scholar] [CrossRef] [PubMed]
- Brandão, T.B.; Gueiros, L.A.; Melo, T.S.; Prado-Ribeiro, A.C.; Nesrallah, A.C.F.A.; Prado, G.V.B.; Santos-Silva, A.R.; Migliorati, C.A. Oral lesions in patients with SARS-CoV-2 infection: Could the oral cavity be a target organ? Oral Surgery Oral Med. Oral Pathol. Oral Radiol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Perrillat, A.; Foletti, J.-M.; Lacagne, A.-S.; Guyot, L.; Graillon, N. Facial pressure ulcers in COVID-19 patients undergoing prone positioning: How to prevent an underestimated epidemic? J. Stomatol. Oral Maxillofac. Surg. 2020, 121, 442–444. [Google Scholar] [CrossRef]
- Ramondetta, A.; Ribero, S.; Costi, S.; Dapavo, P. Pression-induced facial ulcers by prone position for COVID -19 mechanical ventilation. Dermatol. Ther. 2020, 33, e13748. [Google Scholar] [CrossRef]
- Singh, C.; Tay, J.; Shoqirat, N. Skin and Mucosal Damage in Patients Diagnosed With COVID-19. J. Wound Ostomy Cont. Nurs. 2020, 47, 435–438. [Google Scholar] [CrossRef] [PubMed]
- Siotos, C.; Bonett, A.M.; Hansdorfer, M.A.; Siotou, K.; Kambeyanda, R.H.; Dorafshar, A. Medical Device Related Pressure Ulcer of the Lip in a Patient with COVID-19: Case Report and Review of the Literature. J. Stomatol. Oral Maxillofac. Surg. 2020. [Google Scholar] [CrossRef]
- Zingarelli, E.M.; Ghiglione, M.; Pesce, M.; Orejuela, I.; Scarrone, S.; Panizza, R. Facial Pressure Ulcers in a COVID-19 50-year-old Female Intubated Patient. Indian J. Plast. Surg. 2020, 53, 144–146. [Google Scholar] [CrossRef]
- Australian Government National Health and Medical Research Council (NHMRC). Australian Guidelines for the Clinical Care of People with COVID-19. Australian Clinical Practice Guidelines. Available online: https://www.clinicalguidelines.gov.au/register/australian-guidelines-clinical-care-people-covid-19 (accessed on 17 September 2020).
- Moore, Z.; Patton, D.; Avsar, P.; McEvoy, N.L.; Curley, G.; Budri, A.; Nugent, L.; Walsh, S.; O’Connor, T. Prevention of pressure ulcers among individuals cared for in the prone position: Lessons for the COVID-19 emergency. J. Wound Care 2020, 29, 312–320. [Google Scholar] [CrossRef]
- Pokorná, A.; Saibertová, S.; Velichová, R.; Vasmanská, S. Sorrorigenní rány, jejich identifikace a pruběh péce. In Proceedings of the Ceska a Slovenska Neurologie a Neurochirurgie; Purkyne, J.E., Ed.; Czech Medical Association: Prague, Czechia, 2016; Volume 78, pp. S31–S36. [Google Scholar]
- Kambová, V.; Pokorná, A.; Saibertová, S. The knowledge and practises of nurses in the prevention of medical devices related injuries in intensive care—Questionnaire survey. Česká Slov. Neurol. Neurochir. 2019, 82, S19–S22. [Google Scholar] [CrossRef]
- Baraboutis, I.G.; Gargalianos, P.; Aggelonidou, E.; Adraktas, A. Initial Real-Life Experience from a Designated COVID-19 Centre in Athens, Greece: A Proposed Therapeutic Algorithm. SN Compr. Clin. Med. 2020, 2, 689–693. [Google Scholar] [CrossRef]
- Cantini, F.; Niccoli, L.; Matarrese, D.; Nicastri, E.; Stobbione, P.; Goletti, D. Baricitinib therapy in COVID-19: A pilot study on safety and clinical impact. J. Infect. 2020, 81, 318–356. [Google Scholar] [CrossRef] [PubMed]
- Corchuelo, J.; Ulloa, F.C. Oral manifestations in a patient with a history of asymptomatic COVID-19: Case report. Int. J. Infect. Dis. 2020, 100, 154–157. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, M.D.; Romera, A.J.; Villarroel, M. Oral manifestations associated with COVID-19. Oral Dis. 2020, 13555. [Google Scholar] [CrossRef] [PubMed]
- Dima, M.; Enatescu, I.; Craina, M.; Petre, I.; Iacob, E.R.; Iacob, D. First neonates with severe acute respiratory syndrome coronavirus 2 infection in Romania. Medicine 2020, 99, e21284. [Google Scholar] [CrossRef] [PubMed]
- Riad, A.; Gad, A.; Hockova, B.; Klugar, M. Oral candidiasis in non-severe COVID-19 patients: Call for antibiotic stewardship. Oral Surg. 2020, 12561. [Google Scholar] [CrossRef] [PubMed]
- DePasse, J.M.; Palumbo, M.A.; Haque, M.; Eberson, C.P.; Daniels, A.H. Complications associated with prone positioning in elective spinal surgery. World J. Orthop. 2015, 6, 351–359. [Google Scholar] [CrossRef]
- Zeidler, A.; Karpiński, T.M. SARS-CoV, MERS-CoV, SARS-CoV-2 Comparison of Three Emerging Coronaviruses. Jundishapur J. Microbiol. 2020, 13, 1–8. [Google Scholar] [CrossRef]
- Ma, X.; Vervoort, D. Critical care capacity during the COVID-19 pandemic: Global availability of intensive care beds. J. Crit. Care 2020, 58, 96–97. [Google Scholar] [CrossRef] [PubMed]
- Wollina, U. Challenges of COVID-19 pandemic for dermatology. Dermatol. Ther. 2020, 33, e13430. [Google Scholar] [CrossRef] [PubMed]
- Attia, S.; Howaldt, H.-P. Impact of COVID-19 on the Dental Community: Part I before Vaccine (BV). J. Clin. Med. 2021, 10, 288. [Google Scholar] [CrossRef] [PubMed]
- Maspero, C.; Maspero, C.; Cavagnetto, D.; El Morsi, M.; Fama, A.; Farronato, M. Available Technologies, Applications and Benefits of Teleorthodontics. A Literature Review and Possible Applications during the COVID-19 Pandemic. J. Clin. Med. 2020, 9, 1891. [Google Scholar] [CrossRef]
- Ministry of Investments Regional Development and Informatization of the Slovak Republic (MIRRI) Coronavirus (COVID-19) in the Slovak Republic in numbers. Koronavírus a Slovensko. Available online: https://korona.gov.sk/en/coronavirus-covid-19-in-the-slovak-republic-in-numbers/ (accessed on 10 January 2021).
- Bezerra, T.M.M.; Feitosa, S.G.; Carneiro, D.T.O.; Costa, F.-W.-G.; Pires, F.R.; Pereira, K.M.A. Oral lesions in COVID-19 infection: Is long-term follow-up important in the affected patients? Oral Dis. 2020, 13705. [Google Scholar] [CrossRef]
- Rawson, T.M.; Moore, L.S.P.; Zhu, N.; Ranganathan, N.; Skolimowska, K.; Gilchrist, M.; Satta, G.; Cooke, G.; Holmes, A. Bacterial and Fungal Coinfection in Individuals With Coronavirus: A Rapid Review To Support COVID-19 Antimicrobial Prescribing. Clin. Infect. Dis. 2020, 71. [Google Scholar] [CrossRef]
- Bhimraj, A.; Morgan, R.L.; Shumaker, A.H.; Lavergne, V.; Baden, L.; Cheng, V.C.-C.; Edwards, K.M.; Gandhi, R.; Muller, W.J.; O’Horo, J.C.; et al. Infectious Diseases Society of America Guidelines on the Treatment and Management of Patients With Coronavirus Disease 2019 (COVID-19). Clin. Infect. Dis. 2020. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Clinical Management of COVID-19—Interim Guidance. COVID-19: Clinical Care. Available online: https://www.who.int/publications/i/item/clinical-management-of-covid-19 (accessed on 13 January 2021).
- CIHR COVID19 Recommendations. Evidenceprime. Available online: https://covid19.qa.evidenceprime.com/ (accessed on 13 January 2021).
- Stevens, A.; Lotfi, T.; Akl, E.A.; Falavigna, M.; Kredo, T.; Mathew, J.L.; Avey, M.T.; Brignardello-Petersen, R.; Chu, D.K.; Dewidar, O.; et al. The eCOVID-19 living recommendations map and gateway to contextualisation. Introduction and background. Cochrane Database Syst. Rev. 2020. [Google Scholar] [CrossRef]
| Patient No. 1 | Patient No. 2 | Patient No. 3 | |
|---|---|---|---|
| Age, gender | 68-year-old, Male | 61-year-old, Male | 64-year-old, Male |
| Medical anamnesis | Arterial hypertension, chronic hepatopathy, hypercholesterolemia, and gastroesophageal reflux disease. | Obesity, arterial hypertension, and a history of myocardial infarction and septic shock. Chronic medications: Egiramlon (Ramipril), Ebrantil (Urapidil), Tenaxum (Rilmenidine), and Metoprolol. | Chronic medications: Coaxil (Tianeptine), Trittico (Trazodone), and Cefixime. |
| COVID-19-related treatment before ICU admission | Ceftriaxone, Klacid (Clarithromycin), Remdesivir, Paracetamol, Solumedrol (Methylprednisolone), Vitamin C, Vitamin B1, and Fraxiparine (Nadroparin calcium). Nasogastric tube: Isoprinosine (Inosine pranobex), Atorvastatin, Lagosa, Vigantol (Cholecalciferol), Zinc, and Quamatel (Famotidine). | Ceftriaxone, Remdesivir, Dexamethasone, Polyoxidonium, Vitamin C, Vitamin B1, and Fraxiparine (Nadroparin calcium). Nasogastric tube: Isoprinosine (Inosine pranobex), Atorvastatin, Lagosa, Vigantol (Cholecalciferol), Zinc, and Quamatel (Famotidine). | Cefixime, Remdesivir, Solumedrol (Methylprednisolone). |
| Date of ICU admission | 8 November 2020 | 12 November 2020 | 14 November 2020 |
| Dermatologic complications (extraoral) | No | Yes | Yes |
| Oral examination | Haemorrhagic ulcers in the middle third of the dorsal surface of the tongue. | Haemorrhagic ulcers along the lips and focal necrosis affecting the anterior third of the dorsal surface of the tongue accompanied by white patches. | Painful haemorrhagic ulcers along the upper and lower lips. Viral exanthem on the skin in the form of painless macules. |
| Reverse transcription-polymerase chain reaction (RT-PCR) 1 | LRTS: positive Nasopharyngeal: positive Lingual: positive | LRTS: positive Nasopharyngeal: negative Lingual: negative | LRTS: positive Nasopharyngeal: positive Lingual: positive |
| Microbiological assessment | Pseudomonas aeruginosa | Gram-positive cocci, Enterococcus faecalis, and Pseudomonas aeruginosa | Klebsiella pneumoniae |
| Post-ICU outcomes | Deceased on 11 December 2020 due to septic shock and multiple organ dysfunction syndrome. | Released from ICU on 21 December 2020 in good condition and without intubation. | Released from ICU on 17 December 2020 after two consecutive negative RT-PCR results on December 14th and 16th, 2020. |
| Study, Location | N | Gender | Age | MED-COVID-19 | Complication | Onset | Duration | MED-Oral | Aetiology |
|---|---|---|---|---|---|---|---|---|---|
| Amorim dos Santos et al. [26] 2020; Brasilia (Brazil) | 1 | Male | 67 | Initially: hydroxychloroquine sulphate, ceftriaxone sodium, and azithromycin. Later: meropenem, sulfamethoxazole, trimethoprim, immunosuppressants, and anticoagulants. | Oral Candidiasis | After 24 days of ICU admission. | 2 weeks. | Systemic fluconazole and oral nystatin. | Opportunistic fungal infection due to COVID-19 treatments (antibiotics) which lead to immune dysregulation. |
| Andrews et al. [27] 2020; (Michigan, USA) | 1 | Female | 40 | Initially: hydroxychloroquine sulphate, methylprednisolone, and tocilizumab. Later: 16 h. prone/8 h. supine (11 days). | Acute Macroglossia | After 11 days of prone position. | 11 days. | Lingual compression. | Prolonged course of prone positioning for treatment of COVID-19. |
| Brandao et al. [28] 2020; (Sao Paolo, Brazil) | 3 | 1 Female 2 Male | 81, 71, and 72 | Azithromycin, piperacillin/tazobactam, and ceftriaxone. | Herpetic Ulcers and Haemorrhagic Ulcers | After 5, 4, and 5 days of respiratory symptoms. | 11, >15, and 7 days. | Acyclovir and PBMT. | The ICU admission leads to immune dysfunction. |
| Ibarra et al. [22] 2020; (Madrid, Spain) | 57 | 16 Female 41 Male | μ = 61 years old (56–69) | 16 h. prone/8 h. supine (μ = 6 days). | Perioral Pressure Ulcers | N/A | N/A | All the cases were managed with dressings. | Prone position pressure ulcers are dependent on the clinical manoeuvre. |
| Martel et al. [21] 2020; (Massachusetts, USA) | 18 | N/A | N/A | N/A | Perioral Pressure Ulcers | N/A | N/A | All the cases were managed with dressings. | Prolonged placement in a prone position and use of respiratory support equipment. |
| Perrillat et al. [29] 2020; (Marseille, France) | 2 | 2 Male | 27, 50 | 6 prone sessions (12 h. each) 9 prone sessions (12 h. each) | Perioral Pressure Ulcers | N/A | N/A | Debridement of necrotic tissue and paraffin gauze dressing. | Prone positioning monitored by less experienced staff. |
| Ramondetta et al. [30] 2020; (Turin, Italy) | 1 | Male | 48 | Initially: hydroxychloroquine and antiviral treatment. Later: prone positioning cycles (5 days). | Perioral Pressure Ulcers | After 15 days of ICU admission. | N/A | Advanced dressings. | The pressure exercised during the prone positioning phases. |
| Rekhtman et al. [20] 2020 (New York, USA) | 13 | N/A | N/A | Mechanical ventilation. | Perioral Pressure Ulcers | N/A | N/A | N/A | Increased pressure from endotracheal tubes or medical equipment used to hold tubes in place. |
| Salehi et al. [24] 2020; (Tehran, Iran) | 26 | N/A | N/A | Antiviral, antibacterial, and corticosteroids. | Oropharyngeal Candidiasis | N/A | N/A | Fluconazole, nystatin and caspofungin. | Immune dysregulation due to ICU admission and broad-spectrum antibiotic. |
| Shearer et al. [23] 2020; (Washington DC, USA) | 68 | N/A | N/A | Mechanical ventilation. μ of prone positioning = 5.14 days (1–26). | Perioral Pressure Ulcers | N/A | N/A | Antimicrobial dressings. | Longer duration of prone position appears to confer greater risk for developing these pressure injuries. |
| Singh et al. [31] 2020; (California, USA) | 2 | 1 Female 1 Male | 44, 71 | Directly admitted to the ICU, a course of azithromycin and prednisone at home. Mechanical ventilation. | Perioral Pressure Ulcers | 4 days after prone positioning; 5 days after prone positioning. | N/A | Pressure-relieving turns and position system, bordered foam dressings, fluidised positioners. | Prone positioning. |
| Siotos et al. [32] 2020; (Illinois, USA) | 1 | Female | 82 | Mechanical ventilation. | Perioral Pressure Ulcers | 10 days after prone positioning. | N/A | Surgical removal by full-thickness excision. | Prone positioning. |
| Sleiwah et al. [25] 2020; (London, UK) | 16 | 2 Female 14 Male | μ = 58.6 years old (40–77) | Mechanical ventilation, and vasopressors. μ of prone positioning = 5.2 days (2–7). | Perioral Pressure Ulcers | N/A | N/A | N/A | Prone positioning. |
| Zingarelli et al. [33] 2020; (Alessandria, Italy) | 1 | Female | 50 | Initially: acetaminophen and antibiotics. Later: ICU admission, mechanical ventilation. | Perioral Pressure Ulcers | After 15 days of ICU admission. | 1 week | Advanced dressings. | Prone positioning. |
| Total | 210 | 23 Female 62 Male | μ = 60.2 years old (27–81) | Antibiotics, hydroxychloroquine, corticosteroids, mechanical ventilation, and prone positioning. | Perioral pressure ulcers, candidiasis, stomatitis, and macroglossia. | Range 4–24 days after ICU admission. | Range 1–2 weeks. | Dressings, position change, antifungals, and antivirals. | Prone positioning, mechanical ventilation, antibiotic therapy, HAIs. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hocková, B.; Riad, A.; Valky, J.; Šulajová, Z.; Stebel, A.; Slávik, R.; Bečková, Z.; Pokorná, A.; Klugarová, J.; Klugar, M. Oral Complications of ICU Patients with COVID-19: Case-Series and Review of Two Hundred Ten Cases. J. Clin. Med. 2021, 10, 581. https://doi.org/10.3390/jcm10040581
Hocková B, Riad A, Valky J, Šulajová Z, Stebel A, Slávik R, Bečková Z, Pokorná A, Klugarová J, Klugar M. Oral Complications of ICU Patients with COVID-19: Case-Series and Review of Two Hundred Ten Cases. Journal of Clinical Medicine. 2021; 10(4):581. https://doi.org/10.3390/jcm10040581
Chicago/Turabian StyleHocková, Barbora, Abanoub Riad, Jozef Valky, Zuzana Šulajová, Adam Stebel, Rastislav Slávik, Zuzana Bečková, Andrea Pokorná, Jitka Klugarová, and Miloslav Klugar. 2021. "Oral Complications of ICU Patients with COVID-19: Case-Series and Review of Two Hundred Ten Cases" Journal of Clinical Medicine 10, no. 4: 581. https://doi.org/10.3390/jcm10040581
APA StyleHocková, B., Riad, A., Valky, J., Šulajová, Z., Stebel, A., Slávik, R., Bečková, Z., Pokorná, A., Klugarová, J., & Klugar, M. (2021). Oral Complications of ICU Patients with COVID-19: Case-Series and Review of Two Hundred Ten Cases. Journal of Clinical Medicine, 10(4), 581. https://doi.org/10.3390/jcm10040581








