Heart Team for Optimal Management of Patients with Severe Aortic Stenosis—Long-Term Outcomes and Quality of Life from Tertiary Cardiovascular Care Center
Abstract
1. Introduction
2. Methods and Study Design
Statistical Analysis
3. Results
3.1. Study Population
3.2. Echocardiographic Parameters
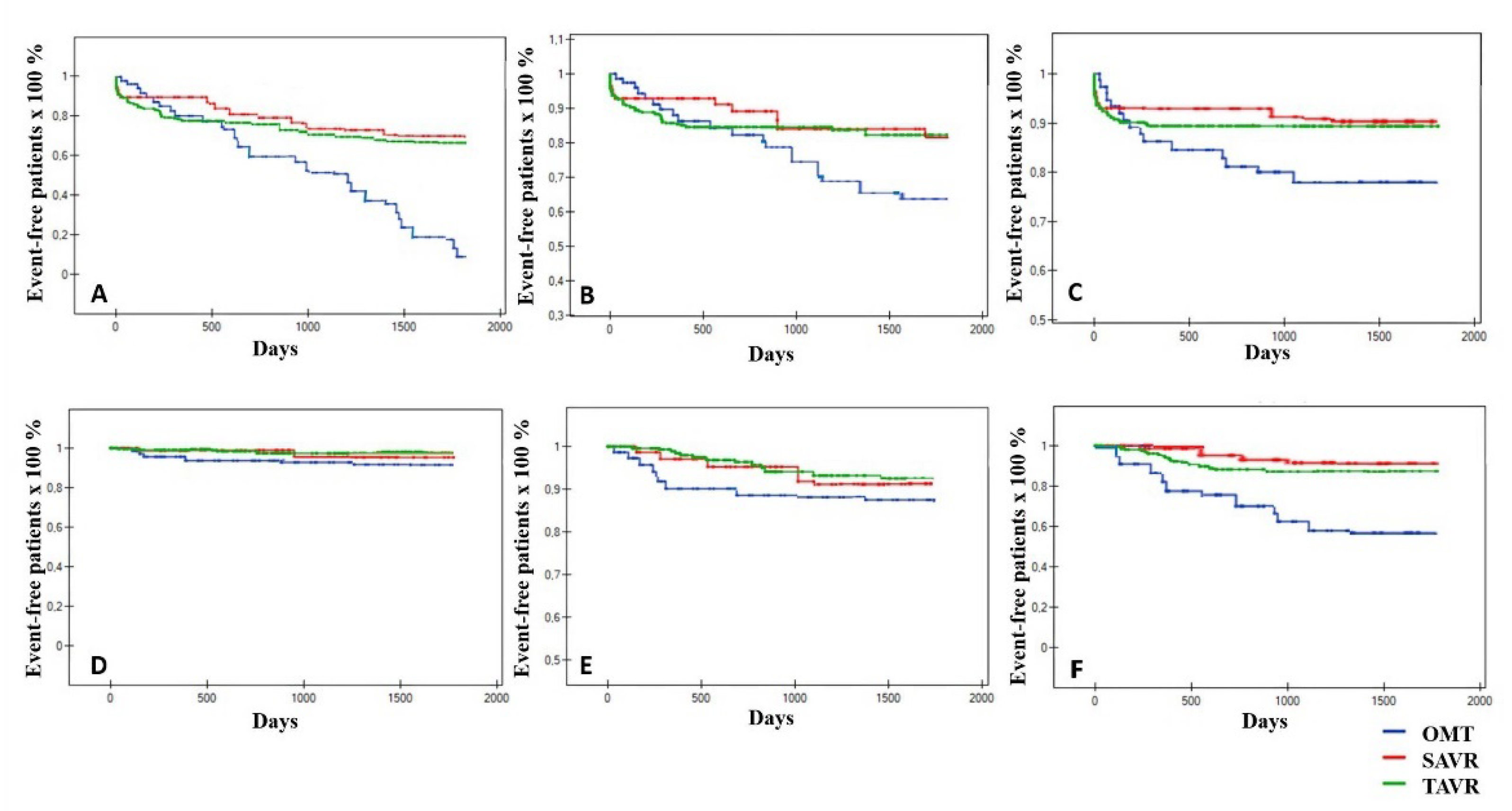
3.3. Endpoints
3.4. Quality of Life
4. Discussion
5. Conclusions
6. Limitations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Vahanian, A.; Beyersdorf, F.; Praz, F.; Milojevic, M.; Baldus, S.; Bauersachs, J.; Capodanno, D.; Conradi, L.; De Bonis, M.; De Paulis, R.; et al. For the ESC/EACTS Scientific Document Group 2021. ESC/EACTS Guidelines for the management of valvular heart disease. Eur. Heart J. 2021, 60, 727–800. [Google Scholar] [CrossRef]
- Otto, C.M.; Nishimura, R.A.; Bonow, R.O.; Carabello, B.A.; Erwin, J.P., III; Gentile, F.; Jneid, H.; Krieger, E.V.; Mack, M.; McLeod, C.; et al. 2020 ACC/AHA Guideline for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J. Am. Coll Cardiol. 2021, 77, 25–197. [Google Scholar] [CrossRef] [PubMed]
- Osnabrugge, R.L.; Mylotte, D.; Head, S.J.; Van Mieghem, N.M.; Nkomo, V.T.; LeReun, C.M.; Bogers, A.J.; Piazza, N.; Kappetein, A.P. Aortic stenosis in the elderly: Disease prevalence and number of candidates for transcatheter aortic valve replacement: A meta-analysis and modeling study. J. Am. Coll Cardiol. 2013, 62, 1002–1012. [Google Scholar] [CrossRef]
- Antonides, C.H.F.J.; Mack, M.J.; Kappetein, A.P. Approaches to the Role of The Heart Team in Therapeutic Decision Making for Heart Valve Disease. Struct. Heart 2017, 1, 249–255. [Google Scholar] [CrossRef]
- Coylewright, M.; O’Neill, E.; Sherman, A.; Gerling, M.; Adam, K.; Xu, K.; Grande, S.W.; Dauerman, H.L.; Dodge, S.E.; Sobti, N.K.; et al. The Learning Curve for Shared Decision-making in Symptomatic Aortic Stenosis. JAMA Cardiol. 2020, 5, 442–448. [Google Scholar] [CrossRef]
- De Jaegere, P.P.T.; de Weger, A.; den Heijer, P.; Verkroost, M.; Baan, J.; de Kroon, T.; America, Y.; Bruinsma, G.B.B. Treatment decision for transcatheter aortic valve implantation: The role of the heart team. Neth. Heart J. 2020, 28, 229–239. [Google Scholar] [CrossRef]
- Subban, V.; Murdoch, D.; Savage, M.L.; Crowhurst, J.; Saireddy, R.; Poon, K.K.; Incani, A.; Bett, N.; Burstow, D.J.; Scalia, G.M.; et al. Outcomes of transcatheter aortic valve implantation in high surgical risk and inoperable patients with aortic stenosis: A single Australian Centre experience. Intern. Med. J. 2016, 46, 42–51. [Google Scholar] [CrossRef] [PubMed]
- Thyregod, H.G.H.; Holmberg, F.; Gerds, T.A.; Ihlemann, N.; Søndergaard, L.; Steinbrüchel, D.A.; Olsen, P.S. Heart Team therapeutic decision-making and treatment in severe aortic valve stenosis. Scand. Cardiovasc. J. 2016, 50, 146–153. [Google Scholar] [CrossRef]
- Rea, C.W.; Wang, T.K.M.; Ruygrok, P.N.; Sidhu, K.; Ramanathan, T.; Nand, P.; Stewart, J.T.; Webster, M.W.I. Characteristics and Outcomes of Patients with Severe Aortic Stenosis Discussed by the Multidisciplinary “Heart Team” According to Treatment Allocation. Heart Lung. Circ. 2020, 29, 368–373. [Google Scholar] [CrossRef]
- Bakelants, E.; Belmans, A.; Verbrugghe, P.; Adriaenssens, T.; Jacobs, S.; Bennett, J.; Meuris, B.; Desmet, W.; Rega, F.; Herijgers, P.; et al. Clinical outcomes of heart-team-guided treatment decisions in high-risk patients with aortic valve stenosis in a health-economic context with limited resources for transcatheter valve therapies. Acta Cardiol. 2019, 74, 489–498. [Google Scholar] [CrossRef] [PubMed]
- Kaier, K.; Gutmann, A.; Vach, W.; Sorg, S.; Siepe, M.; von zur Mühlen, C.; Moser, M.; Blanke, P.; Beyersdorf, F.; Zehender, M.; et al. “Heart Team” decision making in elderly patients with symptomatic aortic valve stenosis who underwent AVR or TAVI—A look behind the curtain. Results of the prospective TAVI Calculation of Costs Trial (TCCT). EuroIntervention 2015, 11, 793–798. [Google Scholar] [CrossRef]
- Coylewright, M.; Mack, M.J.; Holmes, D.R., Jr.; O’Gara, P.T. A call for an evidence-based approach to the Heart Team for patients with severe aortic stenosis. J. Am. Coll Cardiol. 2015, 65, 1472–1480. [Google Scholar] [CrossRef]
- Martínez, G.J.; Seco, M.; Jaijee, S.K.; Adams, M.R.; Cartwright, B.L.; Forrest, P.; Celermajer, D.S.; Vallely, M.P.; Wilson, M.K.; Ng, M.K.C. Introduction of an interdisciplinary heart team-based transcatheter aortic valve implantation programme: Short and mid-term outcomes. Intern. Med. J. 2014, 44, 876–883. [Google Scholar] [CrossRef] [PubMed]
- Dubois, C.; Coosemans, M.; Rega, F.; Poortmans, G.; Belmans, A.; Adriaenssens, T.; Herregods, M.C.; Goetschalckx, K.; Desmet, W.; Janssens, S.; et al. Prospective evaluation of clinical outcomes in all-comer high-risk patients with aortic valve stenosis undergoing medical treatment, transcatheter or surgical aortic valve implantation following heart team assessment. Interact. Cardiovasc. Thorac. Surg. 2013, 17, 492–500. [Google Scholar] [CrossRef]
- Tirado-Conte, G.; Espejo-Paeres, C.; Nombela-Franco, L.; Jimenez-Quevedo, P.; Cobiella, J.; Vivas, D.; de Agustín, J.A.; McInerney, A.; Pozo, E.; Salinas, P.; et al. Performance of the heart team approach in daily clinical practice in high-risk patients with aortic stenosis. J. Card. Surg. 2021, 36, 31–39. [Google Scholar] [CrossRef] [PubMed]
- Ak, A.; Porokhovnikov, I.; Kuethe, F.; Schulze, P.C.; Noutsias, M.; Schlattmann, P. Transcatheter vs. surgical aortic valve replacement and medical treatment: Systematic review and meta-analysis of randomized and non-randomized trials. Herz 2018, 43, 325–337. [Google Scholar] [CrossRef] [PubMed]
- Holmes, D.R., Jr.; Rich, J.B.; Zoghbi, W.A.; Mack, M.J. The heart team of cardiovascular care. J. Am. Coll Cardiol. 2013, 61, 903–907. [Google Scholar] [CrossRef]
- Nallamothu, B.K.; Cohen, D.J. No “I” in Heart Team: Incentivizing multidisciplinary care in cardiovascular medicine. Circ. Cardiovasc. Qual. Outcomes 2012, 5, 410–413. [Google Scholar] [CrossRef]
- Head, S.J.; Kaul, S.; Mack, M.J.; Serruys, P.W.; Taggart, D.P.; Holmes, D.R., Jr.; Leon, M.B.; Marco, J.; Bogers, A.J.J.C.; Kappetein, A.P. The rationale for Heart Team decision-making for patients with stable, complex coronary artery disease. Eur. Heart J. 2013, 34, 2510–2518. [Google Scholar] [CrossRef]
- Eggebrecht, H.; Schmermund, A.; Mehta, R.H. Reducing severe intraprocedural complications during transcatheter aortic valve implantation with an interdisciplinary heart team approach. Eur. J. Cardiothorac. Surg. 2014, 45, 203–204. [Google Scholar] [CrossRef][Green Version]
- Mack, M.J.; Leon, M.B.; Smith, C.R.; Miller, D.C.; Moses, J.W.; Tuzcu, E.M.; Webb, J.G.; Douglas, P.S.; Anderson, W.N.; Blackstone, E.H.; et al. For the PARTNER 1 trial Investigators. 5-Year outcomes of transcatheter aortic valve replacement or surgical aortic valve replacement for high surgical risk patients with aortic stenosis (PARTNER 1): A randomised controlled trial. Lancet 2015, 385, 2477–2484. [Google Scholar] [CrossRef]
- Kapadia, S.R.; Leon, M.B.; Makkar, R.R.; Tuzcu, E.M.; Svensson, L.G.; Kodali, S.K.; Webb, J.G.; Mack, M.J.; Douglas, P.S.; Thourani, V.H.; et al. For the PARTNER trial investigators. 5-Year outcomes of transcatheter aortic valve replacement compared with standard treatment for patients with inoperable aortic stenosis (PARTNER 1): A randomised controlled trial. Lancet 2015, 385, 2485–2491. [Google Scholar] [CrossRef]
- Gleason, T.G.; Reardon, M.J.; Popma, J.J.; Deeb, G.M.; Yakubov, S.J.; Lee, J.S.; Kleiman, N.S.; Chetcuti, S.; Hermiller, J.B., Jr.; Heiser, J.; et al. For the CoreValve, U.S. Pivotal High Risk Trial Clinical Investigators. 5-Year outcomes of self-expanding transcatheter versus surgical aortic valve replacement in high-risk patients. J. Am. Coll Cardiol. 2018, 72, 2687–2696. [Google Scholar] [CrossRef] [PubMed]
- Serruys, P.W.; Morice, M.C.; Kappetein, A.P.; Colombo, A.; Holmes, D.R.; Mack, M.J.; Ståhle, E.; Feldman, T.E.; van der Brand, M.; Bass, E.J.; et al. For the SYNTAX Investigators. Percutaneous coronary intervention versus coronary-artery bypass grafting for severe coronary artery disease. N. Engl. J. Med. 2009, 360, 961–972. [Google Scholar] [CrossRef] [PubMed]
- Leon, M.B.; Smith, C.R.; Mack, M.; Miller, C.; Moses, J.W.; Svensson, L.G.; Tuzcu, E.M.; Webb, J.G.; Fontana, G.P.; Makkar, R.R.; et al. For the PARTNER Trial Investigators. Transcatheter aortic valve implantation for aortic stenosis in patients who cannot undergo surgery. N. Engl. J. Med. 2010, 363, 1597–1607. [Google Scholar] [CrossRef]
- Smith, C.R.; Leon, M.B.; Mack, M.J.; Miller, D.C.; Moses, J.W.; Svensson, L.G.; Tuzcu, E.M.; Webb, J.G.; Fontana, G.P.; Makkar, R.R.; et al. For the PARTNER Trial Investigators. Transcatheter versus surgical aortic-valve replacement in high-risk patients. N. Engl. J. Med. 2011, 364, 2187–2198. [Google Scholar] [CrossRef]
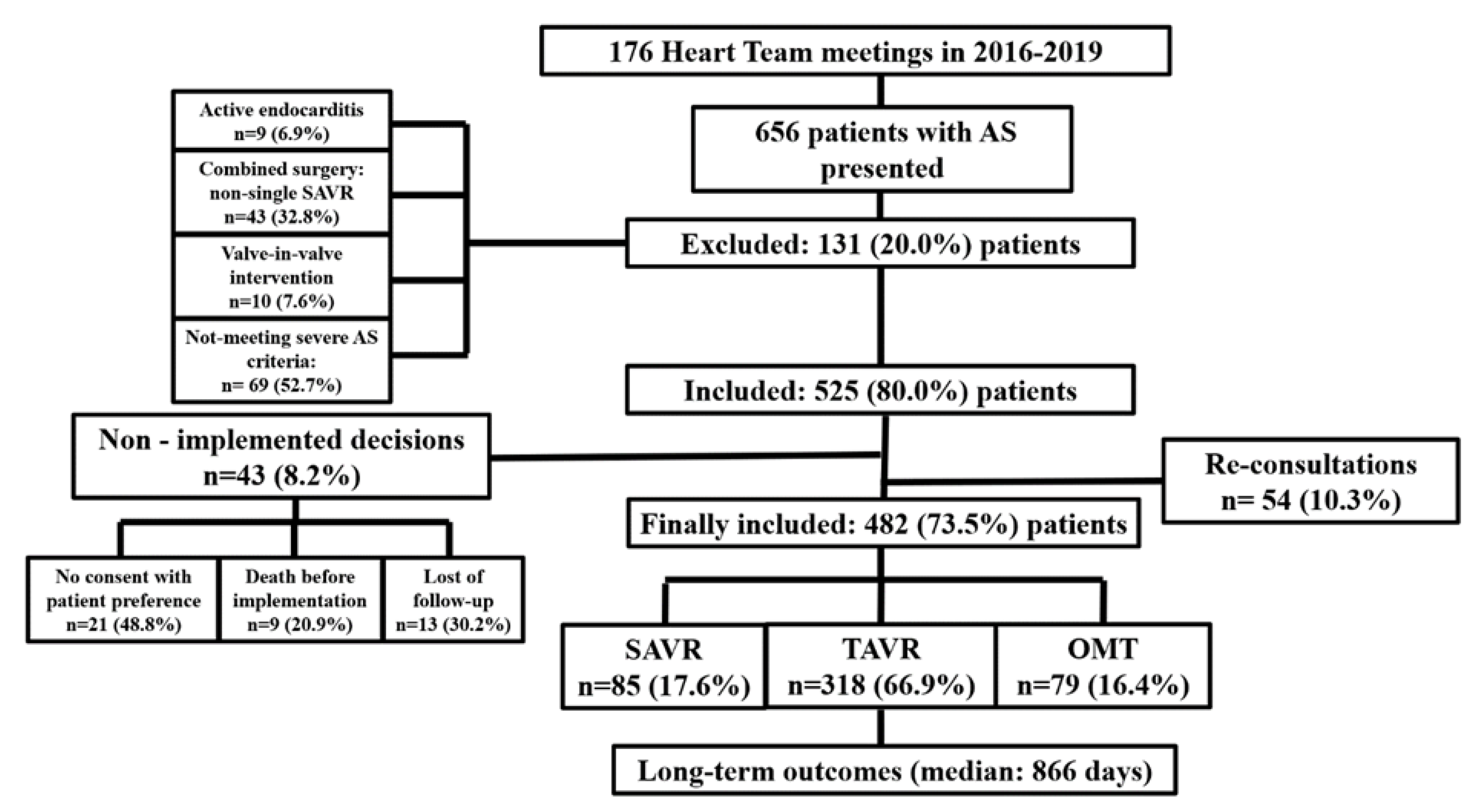
| Baseline Characteristic | Overall (482) | TAVR (318) | SAVR (85) | OMT (79) | p Value |
|---|---|---|---|---|---|
| Age, years; mean (SD) | 78.1 (7.9) | 79.0 (7.2) | 71.0 (6.2) | 81.7 (8.0) | <0.01 |
| Gender, male (%) | 225 (46.7) | 149 (46.9) | 44 (51.8) | 32 (40.5) | 0.35 |
| BMI, kg/m2; mean (SD) | 27.8 (4.9) | 28.2 (4.8) | 27.9 (3.9) | 26.4 (5.9) | 0.01 |
| Heart Failure, n (%) | 400 (83.0) | 279 (87.7) | 50 (58.8) | 71 (89.9) | <0.01 |
| NYHA, mean (SD) | 2.35 (0.79) | 2.28 (0.71) | 2.17 (0.77) | 2.84 (0.93) | <0.01 |
| CAD, n (%) | 284 (58.9) | 188 (51.9) | 39 (45.9) | 57 (72.2) | <0.01 |
| Diabetes, n (%) | 176 (36.5) | 120 (37.7) | 23 (27.1) | 33 (41.8) | 0.11 |
| Hypertension, n (%) | 417 (86.5) | 276 (86.8) | 72 (84.7) | 69 (87.3) | 0.86 |
| Previous stroke/TIA, n (%) | 47 (9.8) | 30 (9.4) | 4 (4.7) | 13 (16.5) | 0.04 |
| Atrial fibrillation, n (%) | 171 (35.5) | 122 (38.4) | 19 (22.4) | 30 (38.0) | 0.02 |
| Previous MI, n (%) | 99 (20.5) | 49 (15.4) | 13 (15.3) | 37 (46.8) | <0.01 |
| Previous PCI, n (%) | 246 (51.0) | 167 (52.5) | 30 (35.3) | 49 (62.0) | <0.01 |
| Previous CABG, n (%) | 53 (11.0) | 29 (9.1) | 10 (11.8) | 14 (17.7) | 0.09 |
| Previous non-aortic VS, n (%) | 25 (5.2) | 14 (4.4) | 3 (3.5) | 8 (10.1) | 0.09 |
| History of pacemaker, n (%) | 71 (14.7) | 57 (17.9) | 1 (1.2) | 13 (16.5) | <0.01 |
| ≥Moderate MR, n (%) | 26 (5.4) | 11 (3.5) | 3 (3.5) | 12 (15.2) | <0.01 |
| ≥Moderate TR, n (%) | 26 (5.4) | 14 (4.4) | 1 (1.2) | 11 (13.9) | <0.01 |
| PAD, n (%) | 86 (17.8) | 48 (15.1) | 9 (10.6) | 29 (36.7) | <0.01 |
| CKD, n (%) | 303 (62.9) | 223 (70.1) | 31 (36.5) | 49 (62.0) | <0.01 |
| Anemia, n (%) | 289 (60.0) | 206 (64.8) | 25 (29.4) | 58 (73.4) | <0.01 |
| Dyslipidemia, n (%) | 371 (77.0) | 248 (78.0) | 64 (75.2) | 59 (74.7) | 0.76 |
| COPD, n (%) | 72 (14.9) | 42 (13.2) | 6 (7.1) | 24 (30.4) | <0.01 |
| Severe PH, n (%) | 46 (9.5) | 21 (6.6) | 3 (3.5) | 22 (27.8) | <0.01 |
| Cancer, n (%) | 69 (14.3) | 39 (12.3) | 9 (10.6) | 21 (26.6) | <0.01 |
| Smoking, n (%) | 323 (67.0) | 216 (67.9) | 53 (62.4) | 54 (68.4) | 0.6 |
| Frailty, n (%) | 221 (45.9) | 151 (47.5) | 11 (12.9) | 59 (74.7) | <0.01 |
| EuroSCORE II, %; mean (SD) | 9.3 (9.7) | 9.7 (11.0) | 5.7 (4.0) | 11.4 (7.3) | <0.01 |
| STS score, %; mean (SD) | 5.9 (2.0) | 6.0 (2.1) | 3.6 (1.7) | 7.1 (2.6) | <0.01 |
| Baseline | At Discharge | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Echocardiographic Parameter | Overall (483) | TAVR (318) | SAVR (85) | OMT | p Value | Overall (377) | TAVR (298) | SAVR (79) | OMT (79) | p Value |
| LVEF, %; mean (SD) | 52.5 (13.4) | 54.2 (12.5) | 56.5 (12.1) | 41.6 (12.5) | <0.01 | 55.9 (10.6) | 55.4 (10.9) | 57.3 (9.9) | - | 0.2 |
| LVEDD, cm; mean (SD) | 5.3 (0.78) | 5.2 (0.76) | 5.3 (0.82) | 5.4 (0.79) | 0.16 | 5.2 (0.80) | 5.2 (0.78) | 5.0 (0.85) | - | 0.03 |
| LVESD, cm; mean (SD) | 3.2 (0.79) | 3.2 (0.77) | 3.2 (0.81) | 3.3 (0.82) | 0.63 | 3.2 (0.76) | 3.2 (0.76) | 3.2 (0.78) | - | 0.76 |
| IVSD, cm; mean (SD) | 1.36 (0.18) | 1.35 (0.18) | 1.39 (0.16) | 1.33 (0.19) | 0.11 | 1.33 (0.17) | 1.33 (0.18) | 1.34 (0.16) | - | 0.76 |
| AVA, cm2; mean (SD) | 0.78 (0.15) | 0.79 (0.16) | 0.76 (0.14) | 0.77 (0.13) | 0.25 | 1.78 (0.40) | 1.77 (0.41) | 1.82 (0.37) | - | 0.44 |
| AVA I, cm2/m2; mean (SD) | 0.47 (0.18) | 0.45 (0.16) | 0.49 (0.18) | 0.53 (0.20) | <0.01 | 0.97 (0.24) | 0.96 (0.25) | 0.99 (0.18) | - | 0.51 |
| PAV, m/s; mean (SD) | 4.38 (0.94) | 4.34 (0.94) | 4.59 (0.97) | 4.32 (0.91) | 0.07 | 2.23 (0.79) | 2.27 (0.74) | 2.16 (0.89) | - | 0.19 |
| DVI; mean (SD) | 0.20 (0.05) | 0.20 (0.05) | 0.21 (0.04) | 0.20 (0.06) | 0.39 | 0.41 (0.09) | 0.40 (0.09) | 0.45 (0.08) | - | <0.01 |
| Peak AVG, mmHg; mean (SD) | 68.6 (24.5) | 69.2 (26.4) | 70.3 (20.7) | 64.2 (19.6) | 0.21 | 20.3 (7.6) | 21.2 (7.4) | 17.3 (7.5) | - | <0.01 |
| Mean AVG, mmHg; mean (SD) | 42.6 (16.3) | 42.3 (16.4) | 45.4 (12.6) | 41.0 (19.2) | 0.18 | 12.4 (6.0) | 12.7 (6.0) | 11.3 (5.7) | - | 0.07 |
| Bicuspid valve, n (%) | 40 (8.3) | 20 (6.3) | 13 (15.3) | 7 (8.9) | 0.03 | - | - | - | - | - |
| ≥Moderate PVAR, n/all (%) | - | - | - | - | - | 5 (1.3) | 5 (1.7) | 0 (0.0) | - | 0.25 |
| ≥Moderate total AR, n/all (%) | - | - | - | - | - | 9 (2.4) | 8 (2.7) | 1 (1.3) | - | 0.46 |
| Endpoints | TAVR (318) | SAVR (85) | OMT (79) | p Value Overall | TAVR vs. SAVR HR [95% CI]; p | SAVR vs. OMT HR [95% CI]; p | TAVR vs. OMT HR [95% CI]; p |
|---|---|---|---|---|---|---|---|
| Primary Endpoint, n (%) | 110 (34.6) | 28 (32.9) | 75 (94.9) | <0.01 | 1.05 [0.73–1.51]; 0.78 | 0.35 [0.22–0.55]; < 0.01 | 0.36 [0.25–0.53]; <0.01 |
| Secondary Endpoints, n (%) | |||||||
| All-cause mortality | 50 (15.7) | 14 (16.5) | 29 (36.7) | <0.01 | 0.95 [0.55–1.65]; 0.88 | 0.45 [0.22–0.90]; <0.01 | 0.43 [0.24–0.75]; <0.01 |
| Non-fatal strokes | 18 (5.7) | 7 (8.2) | 11 (13.9) | 0.04 | 0.69 [0.29–1.65]; 0.38 | 0.59 [0.19–1.81]; 0.25 | 0.41 [0.17–1.00]; 0.01 |
| Non-fatal disabling strokes | 9 (2.8) | 4 (4.7) | 8 (10.1) | 0.02 | 0.60 [0.19–1.89]; 0.39 | 0.46 [0.11–2.02]; 0.19 | 0.28 [0.09–0.91]; <0.01 |
| CV death | 36 (11.3) | 9 (10.6) | 19 (24.1) | <0.01 | 1.07 [0.55–2.06]; 0.85 | 0.44 [0.19–1.02]; 0.02 | 0.47 [0.24–0.93]; <0.01 |
| Non-fatal MI | 9 (2.8) | 3 (3.5) | 8 (10.1) | 0.01 | 0.80 [0.25–2.60]; 0.74 | 0.35 [0.08–1.57]; 0.09 | 0.28 [0.08–0.94]; <0.01 |
| AKI (30 days) | 9 (2.8) | 12 (14.1) | - | - | 0.20 [0.07–0.57]; <0.01 | - | - |
| New onset AF (30 days) | 24 (7.5) | 13 (15.3) | 2 (2.5) | <0.01 | 0.49 [0.21–1.14]; 0.03 | 6.04 [2.06–17.73]; <0.01 | 2.98 [1.25–7.09]; 0.11 |
| New onset AF (EOF) | 38 (11.9) | 19 (22.4) | 10 (12.7) | 0.05 | 0.53 [0.28–1.02]; 0.01 | 1.77 [0.78–4.02]; 0.11 | 0.94 [0.49–1.83]; 0.86 |
| Major bleeding (30 days) | 19 (6.0) | 11 (12.9) | - | - | 0.46 [0.19–1.11]; 0.02 | - | - |
| Major bleeding (EOF) | 36 (11.3) | 17 (20.0) | 1 (1.3) | <0.01 | 0.57 [0.28–1.16]; 0.04 | 15.80 [6.33–39.45]; <0.01 | 8.94 [4.28–18.67]; <0.01 |
| Major vascular complications (30 days) | 32 (10.06) | 2 (2.35) | - | - | 4.28 [2.21–8.29]; 0.02 | - | - |
| Infective valve endocarditis (30 days) | 5 (1.6) | 1 (1.2) | - | - | 1.33 [0.19–9.50]; 0.79 | - | - |
| Infective valve endocarditis (EOF) | 8 (2.5) | 3 (3.5) | 3 (3.8) | 0.78 | 0.71 [0.18–2.90]; 0.61 | 0.93 [0.15–5.61]; 0.93 | 0.66 [0.16–2.81]; 0.54 |
| Permanent pacemaker implantation (30 days) | 53 (16.7) | 6 (7.1) | - | - | 2.36 [1.26–4.41]; 0.03 | - | - |
| Permanent pacemaker implantation (EOF) | 72 (22.6) | 9 (10.6) | 6 (7.6) | 0.01 | 2.14 [1.22–3.76]; 0.01 | 1.39 [0.68–2.87]; 0.51 | 2.98 [1.67–5.32]; <0.01 |
| Aortic valve re-interventions (EOF) | 6 (1.9) | 2 (2.4) | - | - | 0.80 [0.15–4.38]; 0.78 | - | - |
| Non-fatal rehospitalizations for AS (EOF) | 51 (16.0) | 10 (11.8) | 38 (48.1) | <0.01 | 1.36 [0.80–2.31]; 0.33 | 0.24 [0.12–0.48]; <0.01 | 0.33 [0.19–0.57]; <0.01 |
| In-hospital mortality | 20 (6.3) | 6 (7.1) | - | - | 0.89 [0.35–2.29]; 0.8 | - | - |
| ICU stay, days (SD) | 1.8 (3.8) | 4.2 (3.7) | - | - | <0.01 | - | - |
| TAVR (318/268) | SAVR (85/71) | OMT (79/50) | p-Value | |
|---|---|---|---|---|
| Physical Component Summary (PCS) | ||||
| Before SAVR, TAVR, HT disscusion; mean (SD) | 81.5 (14.4) | 79.2 (16.5) | 83.1 (13.0) | 0.22 |
| After SAVR, TAVR, HT disscusion—at the end of follow up; mean (SD) | 69.5 (13.9) | 65.7 (16.1) | 84.1 (12.5) | <0.01 |
| Mental Component Summary (MCS) | ||||
| Before SAVR, TAVR, HT disscusion; mean (SD) | 52.9 (8.6) | 52.1 (9.8) | 53.8 (7.8) | 0.46 |
| After SAVR, TAVR, HT disscusion—at the end of follow up; mean (SD) | 41.4 (8.3) | 39.1 (9.2) | 56.5 (8.0) | <0.01 |
| Total | ||||
| Before SAVR, TAVR, HT disscusion; mean (SD) | 134.5 (17.5) | 131.3 (20.2) | 136.9 (13.8) | 0.12 |
| After SAVR, TAVR, HT disscusion—at the end of follow up; mean (SD) | 111.0 (16.9) | 104.8 (21.0) | 140.6 (13.5) | <0.01 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jonik, S.; Marchel, M.; Pędzich-Placha, E.; Huczek, Z.; Kochman, J.; Ścisło, P.; Czub, P.; Wilimski, R.; Hendzel, P.; Opolski, G.; et al. Heart Team for Optimal Management of Patients with Severe Aortic Stenosis—Long-Term Outcomes and Quality of Life from Tertiary Cardiovascular Care Center. J. Clin. Med. 2021, 10, 5408. https://doi.org/10.3390/jcm10225408
Jonik S, Marchel M, Pędzich-Placha E, Huczek Z, Kochman J, Ścisło P, Czub P, Wilimski R, Hendzel P, Opolski G, et al. Heart Team for Optimal Management of Patients with Severe Aortic Stenosis—Long-Term Outcomes and Quality of Life from Tertiary Cardiovascular Care Center. Journal of Clinical Medicine. 2021; 10(22):5408. https://doi.org/10.3390/jcm10225408
Chicago/Turabian StyleJonik, Szymon, Michał Marchel, Ewa Pędzich-Placha, Zenon Huczek, Janusz Kochman, Piotr Ścisło, Paweł Czub, Radosław Wilimski, Piotr Hendzel, Grzegorz Opolski, and et al. 2021. "Heart Team for Optimal Management of Patients with Severe Aortic Stenosis—Long-Term Outcomes and Quality of Life from Tertiary Cardiovascular Care Center" Journal of Clinical Medicine 10, no. 22: 5408. https://doi.org/10.3390/jcm10225408
APA StyleJonik, S., Marchel, M., Pędzich-Placha, E., Huczek, Z., Kochman, J., Ścisło, P., Czub, P., Wilimski, R., Hendzel, P., Opolski, G., Grabowski, M., & Mazurek, T. (2021). Heart Team for Optimal Management of Patients with Severe Aortic Stenosis—Long-Term Outcomes and Quality of Life from Tertiary Cardiovascular Care Center. Journal of Clinical Medicine, 10(22), 5408. https://doi.org/10.3390/jcm10225408






