Elevated Plasma Bioactive Adrenomedullin and Mortality in Cardiogenic Shock: Results from the OptimaCC Trial
Abstract
1. Introduction
2. Methods
2.1. Study Design
2.2. Participants and Inclusion, Non-Inclusion Criteria in the Princeps Study
2.3. Study Endpoints
2.4. Bio-ADM Measurement
2.5. Statistical Analyses
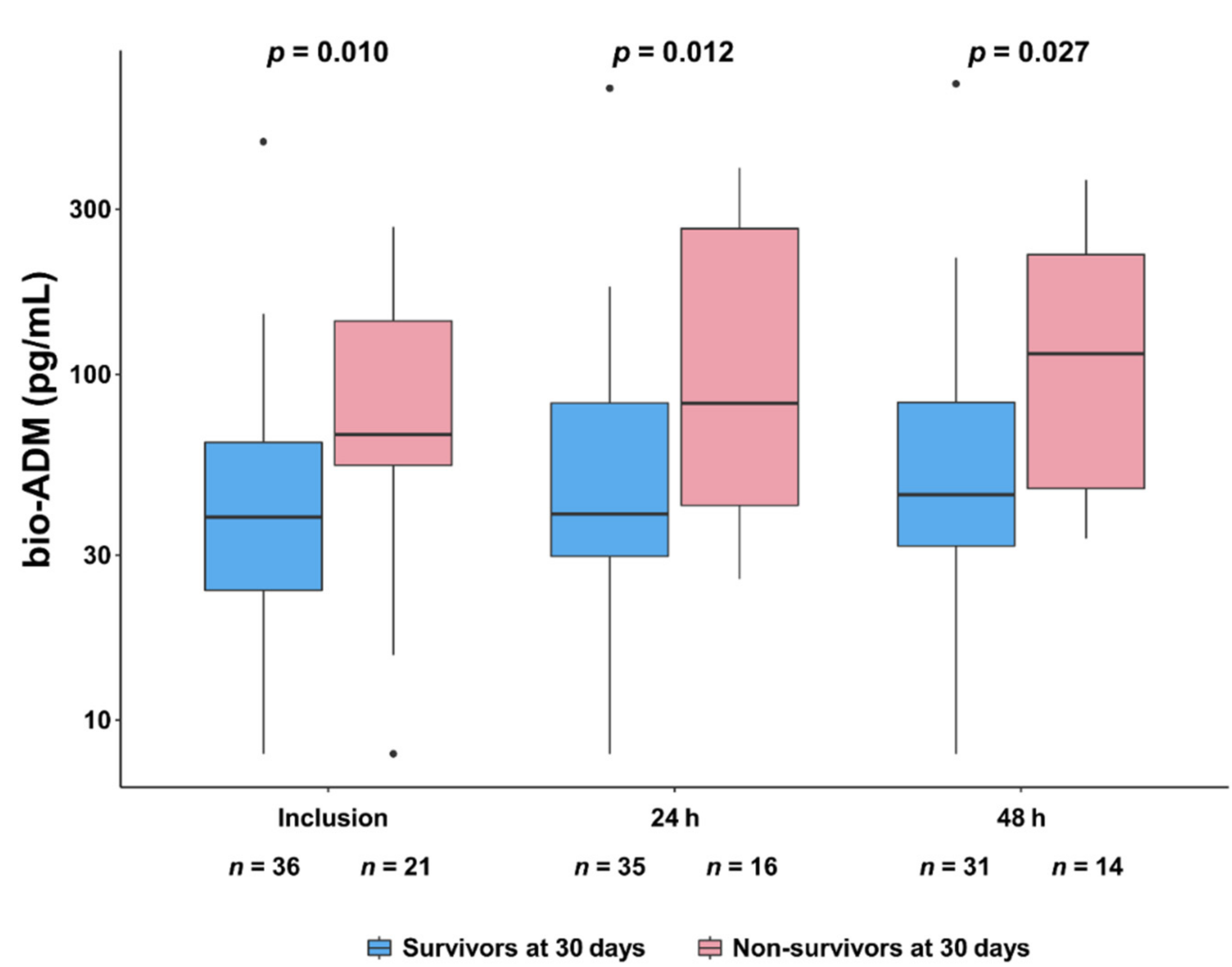
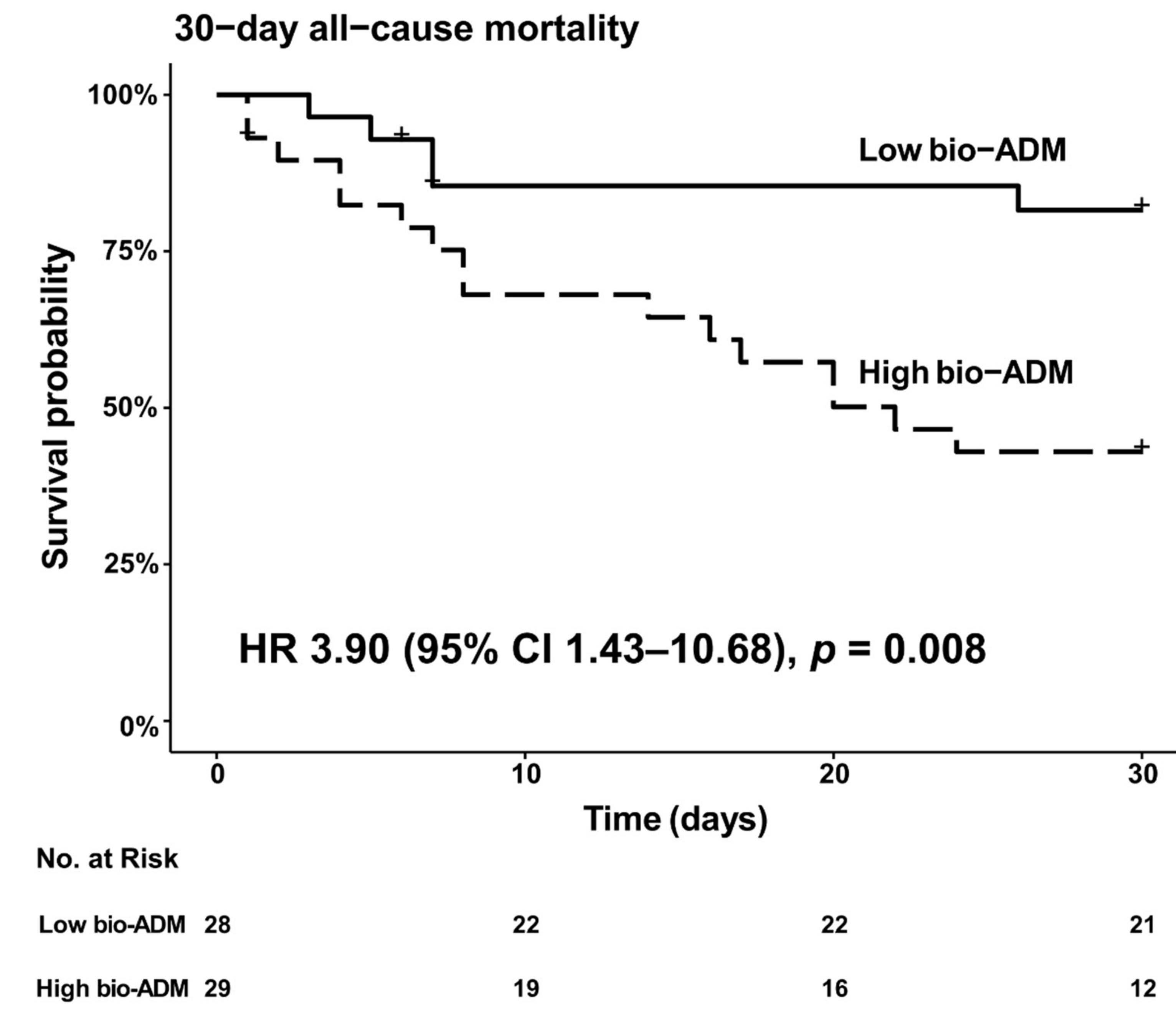
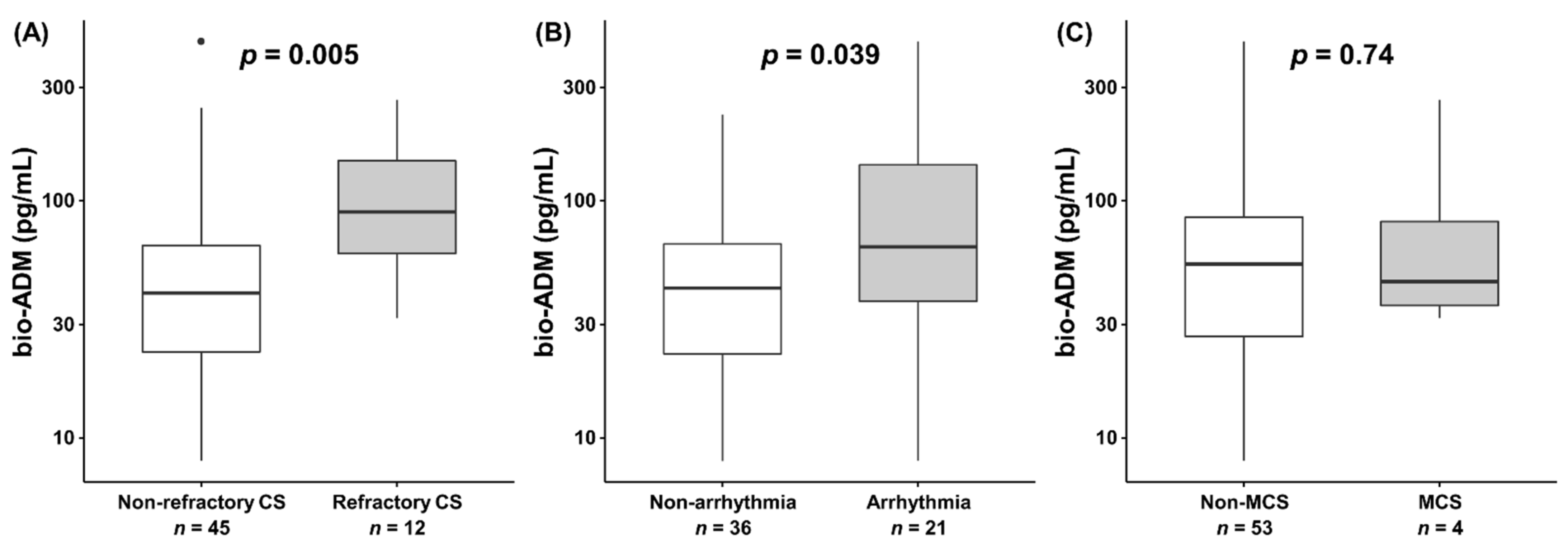
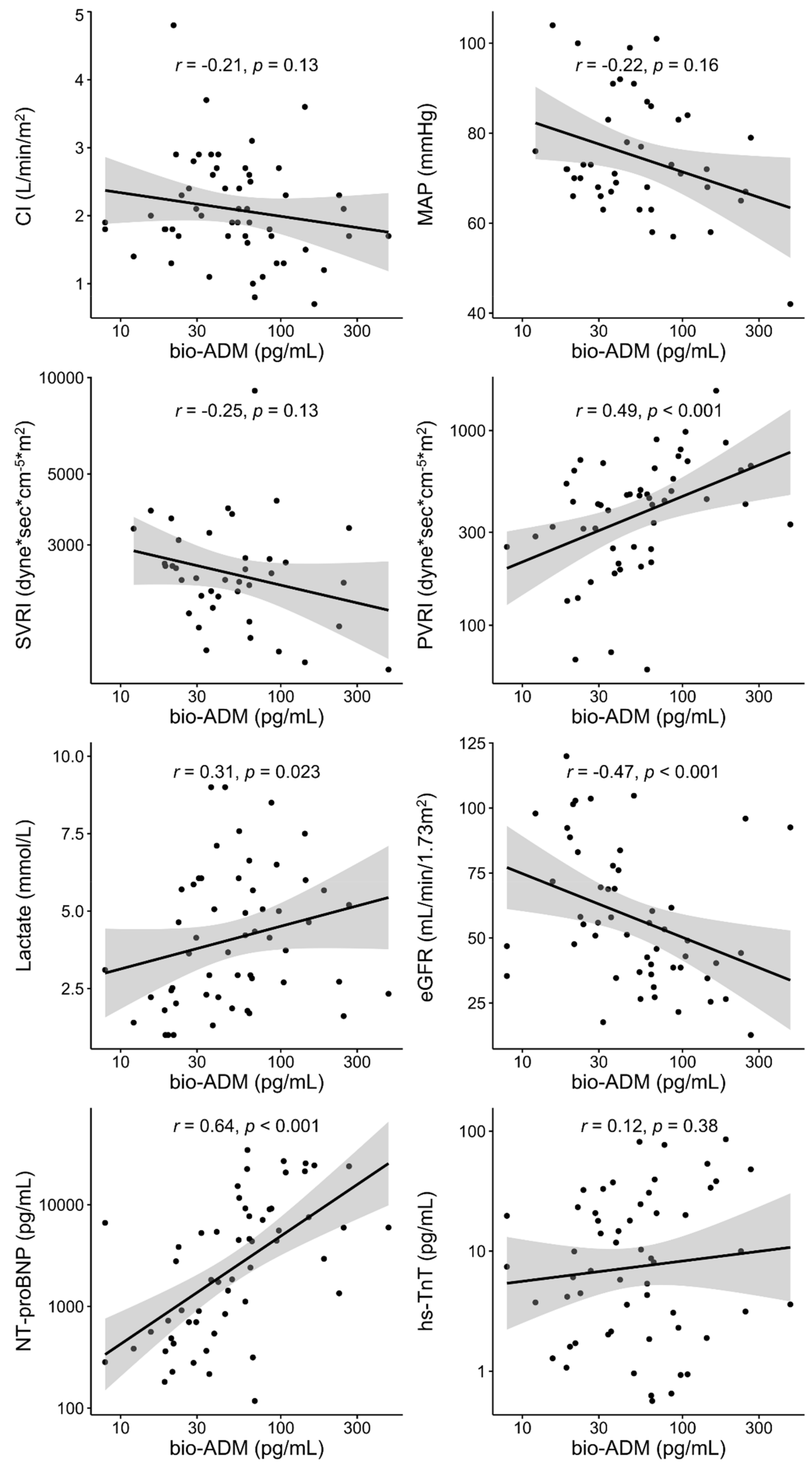
3. Results
4. Discussion
5. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
References
- Ibanez, B.; James, S.; Agewall, S.; Antunes, M.J.; Bucciarelli-Ducci, C.; Bueno, H.; Caforio, A.L.P.; Crea, F.; Goudevenos, J.A.; Halvorsen, S.; et al. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur. Heart J. 2018, 39, 119–177. [Google Scholar] [CrossRef]
- Van Diepen, S.; Katz, J.N.; Albert, N.M.; Henry, T.D.; Jacobs, A.K.; Kapur, N.K.; Kilic, A.; Menon, V.; Ohman, E.M.; Sweitzer, N.K.; et al. Contemporary Management of Cardiogenic Shock: A Scientific Statement from the American Heart Association. Circulation 2017, 136, e232–e268. [Google Scholar] [CrossRef] [PubMed]
- Ponikowski, P.; Voors, A.A.; Anker, S.D.; Bueno, H.; Cleland, J.G.F.; Coats, A.J.S.; Falk, V.; González-Juanatey, J.R.; Harjola, V.P.; Jankowska, E.A.; et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution. Eur. J. Heart Fail. 2016, 18, 891–975. [Google Scholar] [CrossRef] [PubMed]
- Aissaoui, N.; Puymirat, E.; Tabone, X.; Charbonnier, B.; Schiele, F.; Lefèvre, T.; Durand, E.; Blanchard, D.; Simon, T.; Cambou, J.P.; et al. Improved outcome of cardiogenic shock at the acute stage of myocardial infarction: A report from the USIK 1995, USIC 2000, and FAST-MI French Nationwide Registries. Eur. Heart J. 2012, 33, 2535–2543. [Google Scholar] [CrossRef] [PubMed]
- Levy, B.; Bastien, O.; Benjelid, K.; Cariou, A.; Chouihed, T.; Combes, A.; Mebazaa, A.; Megarbane, B.; Plaisance, P.; Ouattara, A.; et al. Experts’ recommendations for the management of adult patients with cardiogenic shock. Ann. Intensive Care 2015, 5, 17. [Google Scholar] [CrossRef] [PubMed]
- Hochman, J.S.; Sleeper, L.A.; Webb, J.G.; Sanborn, T.A.; White, H.D.; Talley, J.D.; Buller, C.E.; Jacobs, A.K.; Slater, J.N.; Col, J.; et al. Early Revascularization in Acute Myocardial Infarction Complicated by Cardiogenic Shock. N. Engl. J. Med. 1999, 341, 625–634. [Google Scholar] [CrossRef]
- Baran, D.A.; Grines, C.L.; Bailey, S.; Burkhoff, D.; Hall, S.A.; Henry, T.D.; Hollenberg, S.M.; Kapur, N.K.; O’Neill, W.; Ornato, J.P.; et al. SCAI clinical expert consensus statement on the classification of cardiogenic shock: This document was endorsed by the American College of Cardiology (ACC), the American Heart Association (AHA), the Society of Critical Care Medicine (SCCM), and the Societ. Catheter. Cardiovasc. Interv. 2019, 94, 29–37. [Google Scholar] [CrossRef]
- Shah, M.; Patnaik, S.; Patel, B.; Ram, P.; Garg, L.; Agarwal, M.; Agrawal, S.; Arora, S.; Patel, N.; Wald, J.; et al. Trends in mechanical circulatory support use and hospital mortality among patients with acute myocardial infarction and non-infarction related cardiogenic shock in the United States. Clin. Res. Cardiol. 2018, 107, 287–303. [Google Scholar] [CrossRef]
- Kitamura, K.; Kangawa, K.; Kawamoto, M.; Ichiki, Y.; Nakamura, S.; Matsuo, H.; Eto, T. Adrenomedullin: A novel hypotensive peptide isolated from human pheochromocytoma. Biochem. Biophys. Res. Commun. 1993, 192, 553–560. [Google Scholar] [CrossRef]
- Kato, J.; Kitamura, K.; Matsui, E.; Tanaka, M.; Ishizaka, Y.; Kita, T.; Kangawa, K.; Eto, T. Plasma adrenomedullin and natriuretic peptides in patients with essential or malignant hypertension. Hypertens. Res. Clin. Exp. 1999, 22, 61–65. [Google Scholar] [CrossRef]
- Yuyun, M.F.; Narayan, H.K.; Ng, L.L. Prognostic Significance of Adrenomedullin in Patients with Heart Failure and With Myocardial Infarction. Am. J. Cardiol. 2015, 115, 986–991. [Google Scholar] [CrossRef] [PubMed]
- Voors, A.A.; Kremer, D.; Geven, C.; ter Maaten, J.M.; Struck, J.; Bergmann, A.; Pickkers, P.; Metra, M.; Mebazaa, A.; Düngen, H.D.; et al. Adrenomedullin in heart failure: Pathophysiology and therapeutic application. Eur. J. Heart Fail. 2019, 21, 163–171. [Google Scholar] [CrossRef]
- Miyao, Y.; Nishikimi, T.; Goto, Y.; Miyazaki, S.; Daikoku, S.; Morii, I.; Matsumoto, T.; Takishita, S.; Miyata, A.; Matsuo, H.; et al. Increased plasma adrenomedullin levels in patients with acute myocardial infarction in proportion to the clinical severity. Heart 1998, 79, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Yoshibayashi, M.; Kamiya, T.; Kitamura, K.; Saito, Y.; Kangawa, K.; Nishikimi, T.; Matsuoka, H.; Eto, T.; Matsuo, H. Plasma levels of adrenomedullin in primary and secondary pulmonary hypertension in patients <20 years of age. Am. J. Cardiol. 1997, 79, 1556–1558. [Google Scholar] [CrossRef]
- Nishikimi, T.; Nagata, S.; Sasaki, T.; Tomimoto, S.; Matsuoka, H.; Takishita, S.; Kitamura, K.; Miyata, A.; Matsuo, H.; Kangawa, K. Plasma concentrations of adrenomedullin correlate with the extent of pulmonary hypertension in patients with mitral stenosis. Heart 1997, 78, 390–395. [Google Scholar] [CrossRef]
- Mebazaa, A.; Geven, C.; Hollinger, A.; Wittebole, X.; Chousterman, B.G.; Blet, A.; Gayat, E.; Hartmann, O.; Scigalla, P.; Struck, J.; et al. Circulating adrenomedullin estimates survival and reversibility of organ failure in sepsis: The prospective observational multinational Adrenomedullin and Outcome in Sepsis and Septic Shock-1 (AdrenOSS-1) study. Crit. Care 2018, 22, 354. [Google Scholar] [CrossRef]
- Lemasle, L.; Blet, A.; Geven, C.; Cherifa, M.; Deniau, B.; Hollinger, A.; Fournier, M.C.; Monnet, X.; Rennuit, I.; Darmon, M.; et al. Bioactive Adrenomedullin, Organ Support Therapies, and Survival in the Critically Ill: Results from the French and European Outcome Registry in ICU Study. Crit. Care Med. 2020, 48, 49–55. [Google Scholar] [CrossRef]
- Marino, R.; Struck, J.; Maisel, A.S.; Magrini, L.; Bergmann, A.; Somma, S.D. Plasma adrenomedullin is associated with short-term mortality and vasopressor requirement in patients admitted with sepsis. Crit. Care 2014, 18. [Google Scholar] [CrossRef]
- Kim, H.; Hur, M.; Struck, J.; Bergmann, A.; Di Somma, S. Circulating biologically active adrenomedullin predicts organ failure and mortality in sepsis. Ann. Lab. Med. 2019, 39, 454–463. [Google Scholar] [CrossRef] [PubMed]
- Koyama, T.; Sakurai, T.; Kamiyoshi, A.; Ichikawa-Shindo, Y.; Kawate, H.; Shindo, T. Adrenomedullin-RAMP2 system in vascular endothelial cells. J. Atheroscler. Thromb. 2015, 22, 647–653. [Google Scholar] [CrossRef] [PubMed]
- Weber, J.; Sachse, J.; Bergmann, S.; Sparwaßer, A.; Struck, J.; Bergmann, A. Sandwich Immunoassay for Bioactive Plasma Adrenomedullin. J. Appl. Lab. Med. 2017, 2, 222–233. [Google Scholar] [CrossRef]
- Tolppanen, H.; Rivas-Lasarte, M.; Lassus, J.; Sans-Roselló, J.; Hartmann, O.; Lindholm, M.; Arrigo, M.; Tarvasmäki, T.; Köber, L.; Thiele, H.; et al. Adrenomedullin: A marker of impaired hemodynamics, organ dysfunction, and poor prognosis in cardiogenic shock. Ann. Intensive Care 2017, 7, 6. [Google Scholar] [CrossRef]
- Levy, B.; Clere-Jehl, R.; Legras, A.; Morichau-Beauchant, T.; Leone, M.; Frederique, G.; Quenot, J.-P.; Kimmoun, A.; Cariou, A.; Lassus, J.; et al. Epinephrine Versus Norepinephrine for Cardiogenic Shock After Acute Myocardial Infarction. J. Am. Coll. Cardiol. 2018, 72, 173–182. [Google Scholar] [CrossRef]
- Vincent, J.L.; Moreno, R.; Takala, J.; Willatts, S.; De Mendonça, A.; Bruining, H.; Reinhart, C.K.; Suter, P.M.; Thijs, L.G. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. Intensive Care Med. 1996, 22, 707–710. [Google Scholar] [CrossRef]
- Harjola, V.P.; Lassus, J.; Sionis, A.; Køber, L.; Tarvasmäki, T.; Spinar, J.; Parissis, J.; Banaszewski, M.; Silva-Cardoso, J.; Carubelli, V.; et al. Clinical picture and risk prediction of short-term mortality in cardiogenic shock. Eur. J. Heart Fail. 2015, 17, 501–509. [Google Scholar] [CrossRef]
- Pöss, J.; Köster, J.; Fuernau, G.; Eitel, I.; de Waha, S.; Ouarrak, T.; Lassus, J.; Harjola, V.P.; Zeymer, U.; Thiele, H.; et al. Risk Stratification for Patients in Cardiogenic Shock After Acute Myocardial Infarction. J. Am. Coll. Cardiol. 2017, 69, 1913–1920. [Google Scholar] [CrossRef]
- Kuroki, N.; Abe, D.; Iwama, T.; Sugiyama, K.; Akashi, A.; Hamabe, Y.; Aonuma, K.; Sato, A. Prognostic effect of estimated glomerular filtration rate in patients with cardiogenic shock or cardiac arrest undergoing percutaneous veno-arterial extracorporeal membrane oxygenation. J. Cardiol. 2016, 68, 439–446. [Google Scholar] [CrossRef] [PubMed]
- Fuernau, G.; Desch, S.; de Waha-Thiele, S.; Eitel, I.; Neumann, F.J.; Hennersdorf, M.; Felix, S.B.; Fach, A.; Böhm, M.; Pöss, J.; et al. Arterial Lactate in Cardiogenic Shock: Prognostic Value of Clearance Versus Single Values. JACC Cardiovasc. Interv. 2020, 13, 2208–2216. [Google Scholar] [CrossRef] [PubMed]
- Lemm, H.; Prondzinsky, R.; Geppert, A.; Russ, M.; Huber, K.; Werdan, K.; Buerke, M. BNP and NT-proBNP in patients with acute myocardial infarction complicated by cardiogenic shock: Results from the IABP Shock trial. Crit. Care 2010, 14, P146. [Google Scholar] [CrossRef][Green Version]
- Supeł, K.; Kacprzak, M.; Zielińska, M. The prognostic value of MR-proadrenomedullin in patients with acute coronary syndrome complicated by cardiogenic shock. Biomarkers 2017, 22, 296–303. [Google Scholar] [CrossRef]
- Frydland, M.; Møller, J.E.; Lindholm, M.G.; Hansen, R.; Wiberg, S.; Lerche Helgestad, O.K.; Thomsen, J.H.; Goetze, J.P.; Engstrøm, T.; Frikke-Schmidt, R.; et al. Biomarkers predictive of late cardiogenic shock development in patients with suspected ST-elevation myocardial infarction. Eur. Heart J. Acute Cardiovasc. Care 2020, 9, 557–566. [Google Scholar] [CrossRef]
- Katayama, T.; Nakashima, H.; Takagi, C.; Honda, Y.; Suzuki, S.; Yano, K. Predictors of mortality in patients with acute myocardial infarction and cardiogenic shock. Circ. J. 2005, 69, 83–88. [Google Scholar] [CrossRef]
- Nishikimi, T.; Kitamura, K.; Saito, Y.; Shimada, K.E.; Ishimitsu, T.; Takamiya, M.; Kangawa, K.; Matsuo, H.; Eto, T.; Omae, T.; et al. Clinical studies on the sites of production and clearance of circulating adrenomedullin in human subjects. Hypertension 1994, 24, 600–604. [Google Scholar] [CrossRef]
- Nishikimi, T.; Nagata, S.; Sasaki, T.; Yoshihara, F.; Nagaya, N.; Horio, T.; Matsuo, H.; Matsuoka, H.; Kangawa, K. The active molecular form of plasma adrenomedullin is extracted in the pulmonary circulation in patients with mitral stenosis: Possible role of adrenomedullin in pulmonary hypertension. Clin. Sci. 2001, 100, 61–66. [Google Scholar] [CrossRef]
- Watanabe, K.; Nishikimi, T.; Takamuro, M.; Yasuda, K.; Ishikawa, Y.; Tanabe, S.; Yamada, O.; Nagaya, N.; Matsuoka, H.; Kangawa, K.; et al. Two Molecular Forms of Adrenomedullin in Congenital Heart Disease. Pediatric Cardiol. 2003, 24, 559–565. [Google Scholar] [CrossRef]
- Kettner, J. Cardiogenic shock. Intervenční a Akutní Kardiologie 2018, 17, 71–74. [Google Scholar] [CrossRef]
- Squara, P.; Hollenberg, S.; Payen, D. Reconsidering Vasopressors for Cardiogenic Shock: Everything Should Be Made as Simple as Possible, but Not Simpler. Chest 2019, 156, 392–401. [Google Scholar] [CrossRef] [PubMed]
- Charles, C.J.; Lainchbury, J.G.; Nicholls, M.G.; Rademaker, M.T.; Richards, A.M.; Troughton, R.W. Adrenomedullin and the renin-angiotensin-aldosterone system. Regul. Pept. 2003, 112, 41–49. [Google Scholar] [CrossRef]
- Geven, C.; Kox, M.; Pickkers, P. Adrenomedullin and adrenomedullin-targeted therapy as treatment strategies relevant for sepsis. Front. Immunol. 2018, 9, 292. [Google Scholar] [CrossRef]
- Nishikimi, T.; Karasawa, T.; Inaba, C.; Ishimura, K.; Tadokoro, K.; Koshikawa, S.; Yoshihara, F.; Nagaya, N.; Sakio, H.; Kangawa, K.; et al. Effects of long-term intravenous administration of adrenomedullin (AM) plus hANP therapy in acute decompensated heart failure-A pilot study. Circ. J. 2009, 73, 892–898. [Google Scholar] [CrossRef] [PubMed]
- Nagaya, N.; Miyatake, K.; Kangawa, K.; Nishikimi, T.; Uematsu, M.; Satoh, T.; Oya, H.; Kyotani, S.; Sakamaki, F.; Ueno, K.; et al. Haemodynamic and hormonal effects of adrenomedullin in patients with pulmonary hypertension. Heart 2000, 84, 653–658. [Google Scholar] [CrossRef] [PubMed]
- Deniau, B.; Takagi, K.; Asakage, A.; Mebazaa, A. Adrecizumab: An investigational agent for the biomarker-guided treatment of sepsis. Expert Opin. Investig. Drugs 2021, 30, 95–102. [Google Scholar] [CrossRef] [PubMed]
- Geven, C.; Blet, A.; Kox, M.; Hartmann, O.; Scigalla, P.; Zimmermann, J.; Marx, G.; Laterre, P.F.; Mebazaa, A.; Pickkers, P. A double-blind, placebo-controlled, randomised, multicentre, proof-of-concept and dose-finding phase II clinical trial to investigate the safety, tolerability and efficacy of adrecizumab in patients with septic shock and elevated adrenomedullin concentrat. BMJ Open 2019, 9, e024475. [Google Scholar] [CrossRef] [PubMed]
- Laterre, P.-F.; Pickkers, P.; Marx, G.; Wittebole, X.; Meziani, F.; Dugernier, T.; Huberlant, V.; Schuerholz, T.; François, B.; Lascarrou, J.-B.; et al. Safety and tolerability of non-neutralizing adrenomedullin antibody adrecizumab (HAM8101) in septic shock patients: The AdrenOSS-2 phase 2a biomarker-guided trial. Intensive Care Med. 2021, in press. [Google Scholar]
| Variables | Total n = 57 | 30-Day Survivors n = 36 | 30-Day Non-Survivors n = 21 | p-Value |
|---|---|---|---|---|
| Demographics | ||||
| Age (years) | 67 (55–77) | 65 (53–73) | 76 (66–81) | 0.008 |
| Female gender | 19 (33%) | 8 (22%) | 11 (52%) | 0.040 |
| Medical history | ||||
| Hypertension | 14 (25%) | 5 (14%) | 9 (43%) | 0.024 |
| Diabetes | 6 (11%) | 5 (14%) | 1 (5%) | 0.40 |
| Stroke | 4 (7%) | 2 (6%) | 2 (10%) | 0.62 |
| Myocardial infarction | 4 (7%) | 2 (6%) | 2 (10%) | 0.62 |
| Severity scores | ||||
| SOFA score | 9 (8–12) | 9 (8–13) | 10 (9–12) | 0.61 |
| CardShock risk score | 4 (3–5) | 4 (3–5) | 5 (4–7) | 0.044 |
| IABP-SHOCK risk score | 2 (1–3) | 2 (1–3) | 2 (1–4) | 0.54 |
| Clinical presentation at inclusion | ||||
| Body mass index (kg/m2) | 25.4 (22.3–27.4) | 25.4 (22.2–27.5) | 25.7 (22.3–27.3) | 0.93 |
| Heart rate (bpm) | 96 (81–111) | 92 (77–111) | 100 (88–107) | 0.61 |
| Systolic arterial pressure (mmHg) | 101 (95–118) | 100 (95–118) | 102 (95–114) | 1.00 |
| Diastolic arterial pressure (mmHg) | 58 (53–64) | 58 (52–65) | 56 (53–61) | 0.70 |
| Mean arterial pressure (mmHg) | 72 (67–83) | 72 (68–85) | 68 (67–78) | 0.47 |
| SvO2 (%) | 71 (60–79) | 74 (68–81) | 60 (50–70) | <0.001 |
| Mechanical ventilation | 46 (90%) | 32 (89%) | 14 (93%) | 1.00 |
| LVEF (%) | 35 (25–40) | 37 (30–44) | 30 (24–38) | 0.080 |
| Laboratory findings at inclusion | ||||
| eGFR (mL/min/1.73 m2) | 52.3 (38.2–76.5) | 55.9 (38.6 – 83.7) | 46.9 (34.6–59.2) | 0.14 |
| AST (UI/L) | 471 (208–790) | 430 (170–719) | 558 (329–1175) | 0.17 |
| ALT (UI/L) | 149 (74–224) | 110 (56–198) | 155 (99–298) | 0.14 |
| NT-proBNP (pg/mL) | 2860 (666–7584) | 1739 (566–5344) | 6635 (1346–22,458) | 0.017 |
| hs-TnT (pg/mL) | 7.7 (2.3–21.4) | 5.8 (2.7–17.9) | 11.8 (2.1–38.2) | 0.24 |
| Lactate (mmol/L) | 3.9 (2.3–5.7) | 3.9 (2.2–5.9) | 3.9 (2.7–5.6) | 0.81 |
| Adverse events in ICU | ||||
| Refractory cardiogenic shock | 12 (21%) | 1 (3%) | 11 (52%) | <0.001 |
| Arrhythmias | 21 (37%) | 12 (33%) | 9 (43%) | 0.57 |
| MCS implantation | 4 (7%) | 2 (6%) | 2 (10%) | 0.62 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Takagi, K.; Levy, B.; Kimmoun, A.; Miró, Ò.; Duarte, K.; Asakage, A.; Blet, A.; Deniau, B.; Schulte, J.; Hartmann, O.; et al. Elevated Plasma Bioactive Adrenomedullin and Mortality in Cardiogenic Shock: Results from the OptimaCC Trial. J. Clin. Med. 2021, 10, 4512. https://doi.org/10.3390/jcm10194512
Takagi K, Levy B, Kimmoun A, Miró Ò, Duarte K, Asakage A, Blet A, Deniau B, Schulte J, Hartmann O, et al. Elevated Plasma Bioactive Adrenomedullin and Mortality in Cardiogenic Shock: Results from the OptimaCC Trial. Journal of Clinical Medicine. 2021; 10(19):4512. https://doi.org/10.3390/jcm10194512
Chicago/Turabian StyleTakagi, Koji, Bruno Levy, Antoine Kimmoun, Òscar Miró, Kévin Duarte, Ayu Asakage, Alice Blet, Benjamin Deniau, Janin Schulte, Oliver Hartmann, and et al. 2021. "Elevated Plasma Bioactive Adrenomedullin and Mortality in Cardiogenic Shock: Results from the OptimaCC Trial" Journal of Clinical Medicine 10, no. 19: 4512. https://doi.org/10.3390/jcm10194512
APA StyleTakagi, K., Levy, B., Kimmoun, A., Miró, Ò., Duarte, K., Asakage, A., Blet, A., Deniau, B., Schulte, J., Hartmann, O., Cotter, G., Davison, B. A., Gayat, E., & Mebazaa, A. (2021). Elevated Plasma Bioactive Adrenomedullin and Mortality in Cardiogenic Shock: Results from the OptimaCC Trial. Journal of Clinical Medicine, 10(19), 4512. https://doi.org/10.3390/jcm10194512







