Presepsin in the Rapid Response System for Cancer Patients: A Retrospective Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Statistical Analyses
3. Results
3.1. Patient Demographics
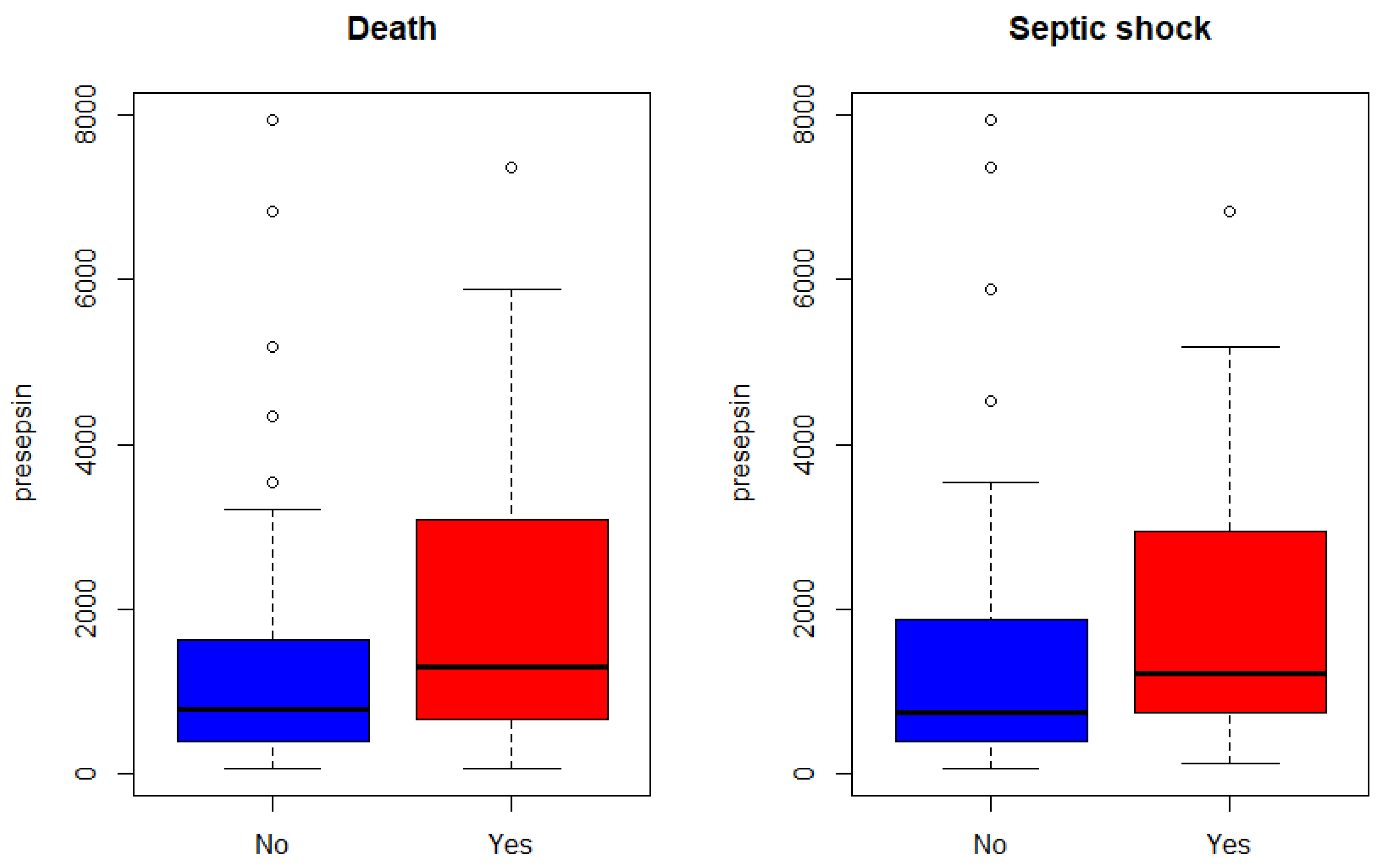
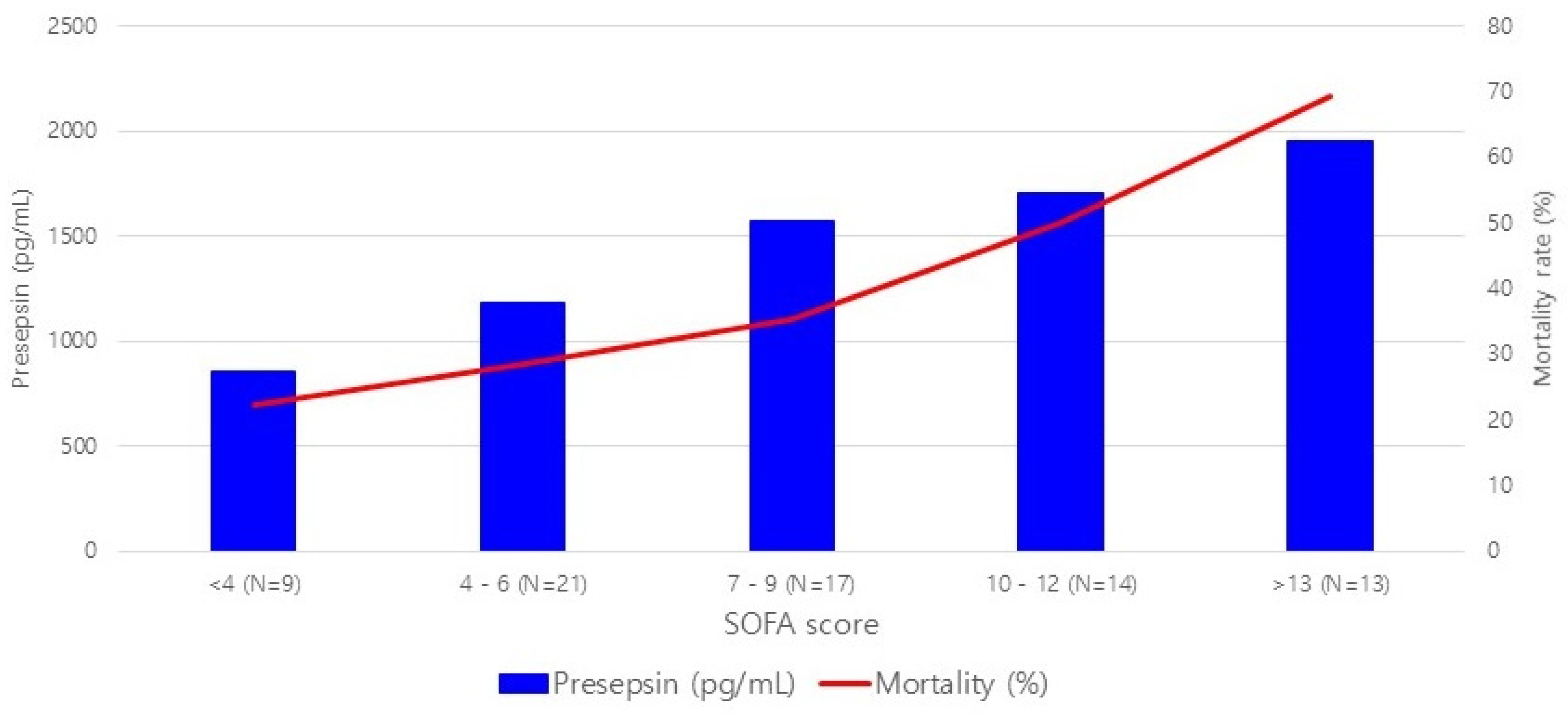
3.2. Markers of Septic Shock and Mortality Risk
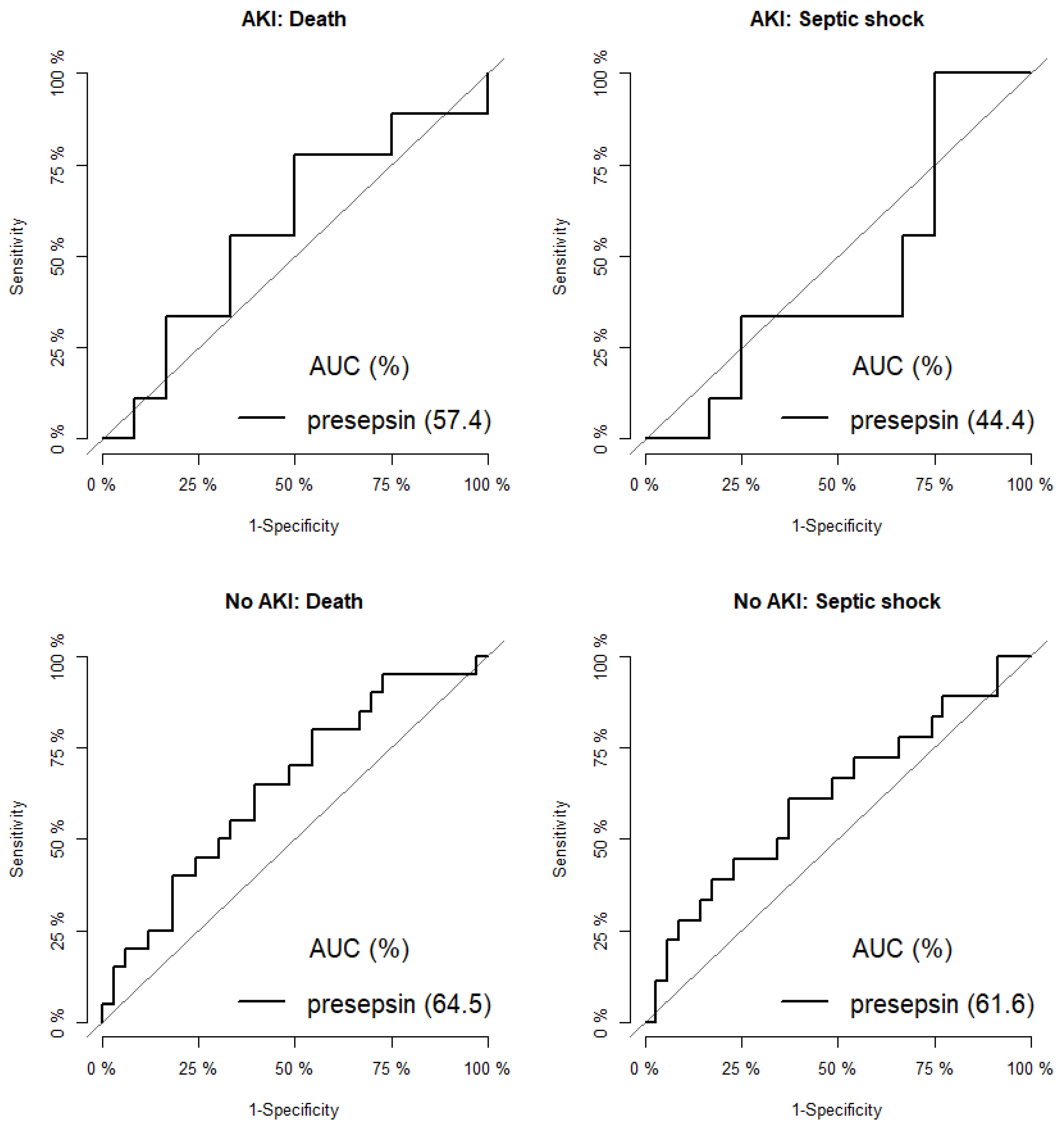
3.3. Markers of Septic Shock in Patients with/without Acute Kidney Injury
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Rhodes, A.A.; Evans, L.E.; Alhazzani, W.; Levy, M.M.; Antonelli, M.; Ferrer, R.; Kumar, A.; Sevransky, J.E.; Sprung, C.L.; Nunnally, M.E.; et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Intensive Care Med. 2017, 43, 304–377. [Google Scholar] [CrossRef]
- Li, J.; Tang, Z.; Xie, M.; Hang, C.; Yu, Y.; Li, C. Association between elevation of plasma biomarkers and monocyte dysfunction and their combination in predicting sepsis: An observational single-centre cohort study. Innate Immun. 2020, 26, 514–527. [Google Scholar] [CrossRef]
- Okamura, Y.; Yokoi, H. Development of a point-of-care assay system for measurement of presepsin (sCD14-ST). Clin. Chim. Acta 2011, 412, 2157–2161. [Google Scholar] [CrossRef]
- Shozushima, T.; Takahashi, G.; Matsumoto, N.; Kojika, M.; Endo, S.; Okamura, Y. Usefulness of presepsin (sCD14-ST) measurements as a marker for the diagnosis and severity of sepsis that satisfied diagnostic criteria of systemic inflammatory response syndrome. J. Infect. Chemother. 2011, 17, 764–769. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.; Chen, Y.-X.; Yin, Q.; Zhao, Y.-Z.; Li, C.-S. Diagnostic value and prognostic evaluation of Presepsin for sepsis in an emergency department. Crit. Care 2013, 17, R244. [Google Scholar] [CrossRef] [PubMed]
- Behnes, M.; Bertsch, T.; Lepiorz, D.; Lang, S.; Trinkmann, F.; Brueckmann, M.; Borggrefe, M.; Hoffmann, U. Diagnostic and prognostic utility of soluble CD 14 subtype (presepsin) for severe sepsis and septic shock during the first week of intensive care treatment. Crit. Care 2014, 18, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, Y.; Ishikura, H.; Nishida, T.; Kawano, Y.; Yuge, R.; Ichiki, R.; Murai, A. Usefulness of presepsin in the diagnosis of sepsis in patients with or without acute kidney injury. BMC Anesthesiol. 2014, 14, 88. [Google Scholar] [CrossRef] [PubMed]
- Singer, M.; Deutschman, C.S.; Seymour, C.W.; Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G.R.; Chiche, J.-D.; Coopersmith, C.M.; et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016, 315, 801–810. [Google Scholar] [CrossRef] [PubMed]
- Khwaja, A. KDIGO Clinical Practice Guidelines for Acute Kidney Injury. Nephron 2012, 120, c179–c184. [Google Scholar] [CrossRef] [PubMed]
- Magrini, L.; Gagliano, G.; Travaglino, F.; Vetrone, F.; Marino, R.; Cardelli, P.; Salerno, G.; Di Somma, S. Comparison between white blood cell count, procalcitonin and C reactive protein as diagnostic and prognostic biomarkers of infection or sepsis in patients presenting to emergency department. Clin. Chem. Lab. Med. 2014, 52, 1465–1472. [Google Scholar] [CrossRef] [PubMed]
- Jekarl, D.W.; Lee, S.; Kim, M.; Kim, Y.; Woo, S.H.; Lee, W.J. Procalcitonin as a prognostic marker for sepsis based on SEPSIS-3. J. Clin. Lab. Anal. 2019, 33, e22996. [Google Scholar] [CrossRef]
- Imai, Y.; Taniguchi, K.; Iida, R.; Nitta, M.; Uchiyma, K.; Takasu, A. Diagnostic accuracy of presepsin in predicting bacteraemia in elderly patients admitted to the emergency department: Prospective study in Japan. BMJ Open 2019, 9, e030421. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, M.; Duzenli, T.; Tanoglu, A.; Cakir Guney, B.; Onal Tastan, Y.; Bicer, H.S. Presepsin:albumin ratio and C-reactive protein:albumin ratio as novel sepsis-based prognostic scores : A retrospective study. Wien. Klin. Wochenschr. 2020, 132, 182–187. [Google Scholar] [CrossRef]
- Fan, F.; Jia, J.; Li, J.; Huo, Y.; Zhang, Y. White blood cell count predicts the odds of kidney function decline in a Chinese community-based population. BMC Nephrol. 2017, 18, 190. [Google Scholar] [CrossRef] [PubMed]
- Sia, P.; Plumb, T.J.; Fillaus, J.A. Type B Lactic Acidosis Associated With Multiple Myeloma. Am. J. Kidney Dis. 2013, 62, 633–637. [Google Scholar] [CrossRef] [PubMed]
- Rice, K.; Schwartz, S.H. Lactic acidosis with small cell carcinoma. Rapid response to chemotherapy. Am. J. Med. 1985, 79, 501–503. [Google Scholar] [CrossRef]
- Nakamura, Y.; Hoshino, K.; Kiyomi, F.; Kawano, Y.; Mizunuma, M.; Tanaka, J.; Nishida, T.; Ishikura, H. Comparison of accuracy of presepsin and procalcitonin concentrations in diagnosing sepsis in patients with and without acute kidney injury. Clin. Chim. Acta 2019, 490, 200–206. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, G.; Shibata, S.; Fukui, Y.; Okamura, Y.; Inoue, Y. Diagnostic accuracy of procalcitonin and presepsin for infectious disease in patients with acute kidney injury. Diagn. Microbiol. Infect. Dis. 2016, 86, 205–210. [Google Scholar] [CrossRef] [PubMed]
- Thursky, K.A.; Worth, L.J. Can mortality of cancer patients with fever and neutropenia be improved? Curr. Opin. Infect. Dis. 2015, 28, 505–513. [Google Scholar] [CrossRef] [PubMed]
- Song, J.-U.; Suh, G.Y.; Park, H.Y.; Lim, S.Y.; Han, S.G.; Kang, Y.R.; Kwon, O.J.; Woo, S.; Jeon, K. Early intervention on the outcomes in critically ill cancer patients admitted to intensive care units. Intensive Care Med. 2012, 38, 1505–1513. [Google Scholar] [CrossRef]
- Yealy, D.M.; Huang, D.T.; Delaney, A.; Knight, M.; Randolph, A.G.; Daniels, R.; Nutbeam, T. Recognizing and managing sepsis: What needs to be done? BMC Med. 2015, 13, 98. [Google Scholar] [CrossRef] [PubMed]


| Variable | Number of Patients (%) (n = 74) |
|---|---|
| Sex | |
| Male | 41 (55.4%) |
| Female | 33 (44.6%) |
| Age | 64.6 (13.6%) |
| Cancer type | |
| Hepatobiliary and pancreatic cancer | 19 (25.6%) |
| Gastrointestinal cancer | 14 (18.9%) |
| Gynecological cancer | 11 (14.8%) |
| Urological cancer | 10 (13.5%) |
| Lung cancer | 10 (13.5%) |
| Hematologic malignancy | 6 (8.1%) |
| Others | 4 (4.9%) |
| Cancer stage | |
| Locally advanced cancer | 53 (71.6%) |
| Metastatic cancer | 21 (28.4%) |
| ICU transfer | 64 (86.5%) |
| Yes | 10 (13.5%) |
| No | |
| Diagnosis at RRS activation | |
| Sepsis | 17 (23.0%) |
| Septic shock | 27 (36.5%) |
| Other shock | 21 (28.4%) |
| Respiratory failure | 7 (9.5%) |
| Others | 2 (2.7%) |
| Pre-existing condition | |
| Chemotherapy within 30 days | 53 (71.6%) |
| Cardiovascular disease | 10 (13.5%) |
| With acute kidney injury | 21 (28.3%) |
| Intervention in place | |
| Continuous vasoactive agent use | 44 (59.5%) |
| Mechanical ventilator use | 21 (28.4%) |
| Continuous renal replacement therapy | 14 (18.9%) |
| Mortality | 29 (39.2%) |
| Variable | Cut off | Sensitivity (95% CI) | Specificity (95% CI) |
|---|---|---|---|
| Septic shock | |||
| WBC | 12,000 | 59.3 | 40.4 |
| CRP | 1.0 | 96.3 | 6.4 |
| Lactic acid | 19.8 | 70.4 | 57.4 |
| Presepsin | 728 | 74.1 | 51.1 |
| Mortality | |||
| WBC | 12,000 | 51.7 | 35.6 |
| CRP | 1.0 | 96.6 | 6.7 |
| Lactic acid | 19.8 | 69.0 | 57.8 |
| Presepsin | 727 | 72.4 | 48.9 |
| Variable | Cut off | Non-Septic Shock (n = 47) | Septic Shock (n = 27) | p-Value * |
|---|---|---|---|---|
| Septic shock | 0.918 | |||
| WBC | <12,000 | 19 | 11 | |
| ≥12,000 | 28 | 16 | ||
| CRP | <1.0 | 3 | 1 | 0.441 |
| ≥1.0 | 44 | 26 | ||
| Lactic acid | <19.8 | 27 | 8 | 0.012 |
| ≥19.8 | 20 | 19 | ||
| Presepsin | <728 | 24 | 7 | 0.079 |
| ≥728 | 23 | 20 | ||
| Mortality | ||||
| WBC | <12,000 | 16 | 14 | 0.397 |
| ≥12,000 | 29 | 15 | ||
| CRP | <1.0 | 3 | 1 | 1.000 |
| ≥1.0 | 42 | 28 | ||
| Lactic acid | <19.8 | 26 | 9 | 0.044 |
| ≥19.8 | 19 | 20 | ||
| Presepsin | <727 | 22 | 8 | 0.114 |
| ≥727 | 23 | 21 |
| Variable | Normal Kidney Function | With AKI | ||
|---|---|---|---|---|
| Sensitivity (95% CI) | Specificity (95% CI) | Sensitivity (95% CI) | Specificity (95% CI) | |
| Septic shock | ||||
| Lactic acid | 55.6 (30.8–78.5) | 60 (42.1–76.1) | 100 (66.4–100) | 50 (21.1–78.9 |
| Presepsin | 61.1 (35.7–82.7) | 62.9 (44.9–78.5) | 100 (66.4–100) | 25 (5.5–57.2) |
| Mortality | ||||
| Lactic acid | 60 (36.1–80.9) | 63.6 (45.1–79.6) | 88.9 (51.8–99.7) | 41.7 (15.2–72.3) |
| Presepsin | 65 (40.8–84.6) | 60.6 (42.1–97.2) | 77.8 (40–97.2) | 50 (21.1–78.9) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, M.-J.; Han, W.-H.; Chun, J.-Y.; Kim, S.-Y.; Kim, J.-H. Presepsin in the Rapid Response System for Cancer Patients: A Retrospective Analysis. J. Clin. Med. 2021, 10, 2153. https://doi.org/10.3390/jcm10102153
Lee M-J, Han W-H, Chun J-Y, Kim S-Y, Kim J-H. Presepsin in the Rapid Response System for Cancer Patients: A Retrospective Analysis. Journal of Clinical Medicine. 2021; 10(10):2153. https://doi.org/10.3390/jcm10102153
Chicago/Turabian StyleLee, Min-Jung, Won-Ho Han, June-Young Chun, Sun-Young Kim, and Jee-Hee Kim. 2021. "Presepsin in the Rapid Response System for Cancer Patients: A Retrospective Analysis" Journal of Clinical Medicine 10, no. 10: 2153. https://doi.org/10.3390/jcm10102153
APA StyleLee, M.-J., Han, W.-H., Chun, J.-Y., Kim, S.-Y., & Kim, J.-H. (2021). Presepsin in the Rapid Response System for Cancer Patients: A Retrospective Analysis. Journal of Clinical Medicine, 10(10), 2153. https://doi.org/10.3390/jcm10102153







