Does Statin Therapy Reduce the Risks of Mortality and Major Adverse Cardiac and Cerebrovascular Events in Young Adults with End-Stage Renal Disease? Population-Based Cohort Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Source
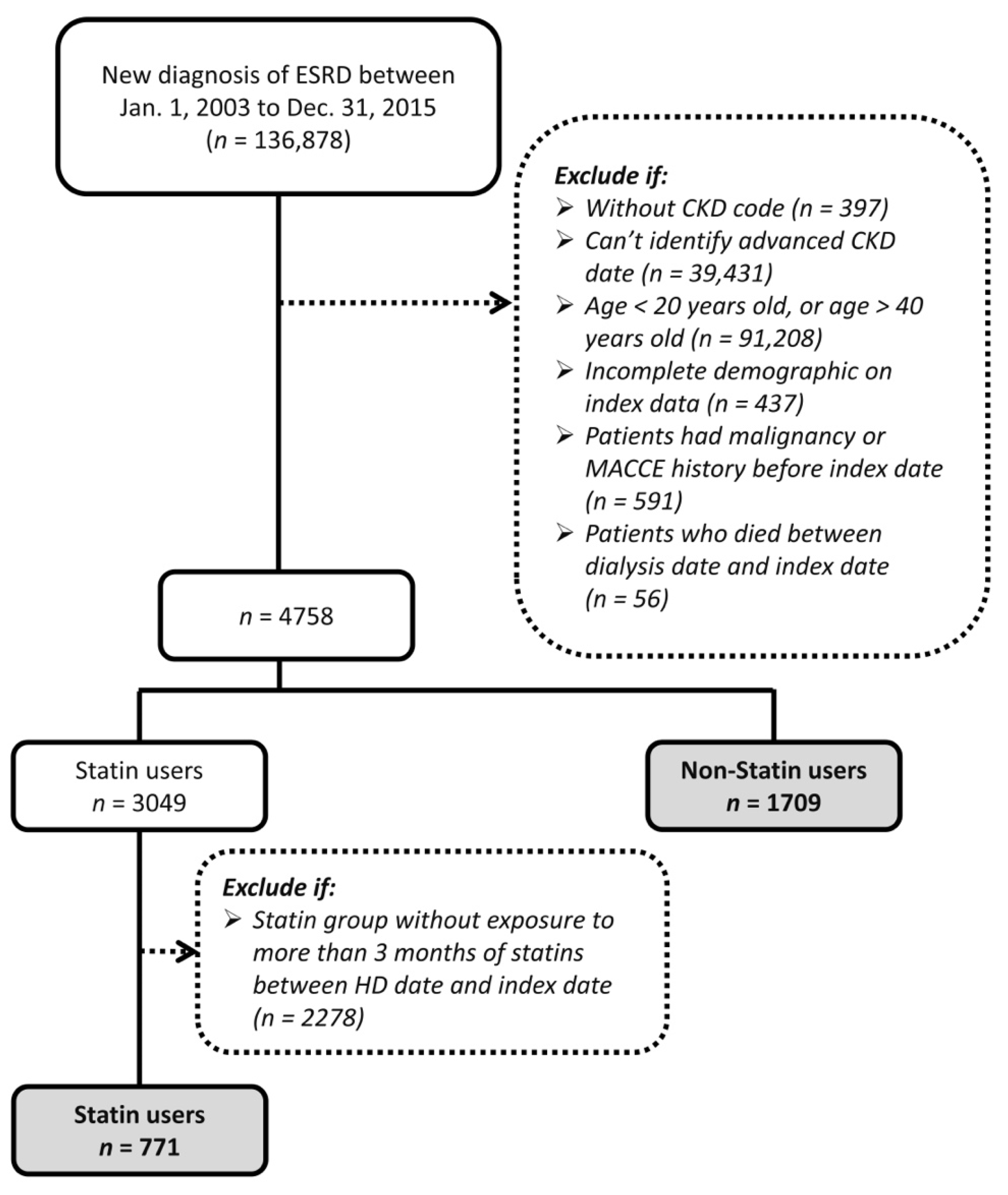
2.2. Study Design
2.3. Covariates and Outcomes
2.4. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Outcomes
3.3. Subgroup Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- The 4S Group. Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: The Scandinavian Simvastatin Survival Study (4S). Lancet 1994, 344. [Google Scholar] [CrossRef]
- Hebert, P.R. Cholesterol Lowering with Statin Drugs, Risk of Stroke, and Total Mortality. JAMA 1997, 278. [Google Scholar] [CrossRef]
- Holdaas, H.; Fellström, B.; Jardine, A.G.; Holme, I.; Nyberg, G.; Fauchald, P.; Grönhagen-Riska, C.; Madsen, S.; Neumayer, H.H.; Cole, E.; et al. Effect of fluvastatin on cardiac outcomes in renal transplant recipients: A multicentre, randomised, placebo-controlled trial. Lancet 2003, 361, 2024–2031. [Google Scholar] [CrossRef]
- Armitage, J.; Bowman, L. Cardiovascular outcomes among participants with diabetes in the recent large statin trials. Curr. Opin. Lipidol. 2004, 15, 439–446. [Google Scholar] [CrossRef] [PubMed]
- Baigent, C.; Keech, A.; Kearney, P.M.; Blackwell, L.; Buck, G.; Pollicino, C.; Kirby, A.; Sourjina, T.; Peto, R.; Collins, R.; et al. Efficacy and safety of cholesterol-lowering treatment: Prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 2005, 366, 1267–1278. [Google Scholar] [CrossRef] [PubMed]
- Wanner, C.; Krane, V.; Marz, W.; Olschewski, M.; Mann, J.F.; Ruf, G.; Ritz, E.; German, D. Dialysis Study I. Atorvastatin in patients with type 2 diabetes mellitus undergoing hemodialysis. N. Engl. J. Med. 2005, 353, 238–248. [Google Scholar] [CrossRef]
- Fellstrom, B.C.; Jardine, A.G.; Schmieder, R.E.; Holdaas, H.; Bannister, K.; Beutler, J.; Chae, D.W.; Chevaile, A.; Cobbe, S.M.; Gronhagen-Riska, C.; et al. Aurora Study Group. Rosuvastatin and cardiovascular events in patients undergoing hemodialysis. N. Engl. J. Med. 2009, 360, 1395–1407. [Google Scholar] [CrossRef] [Green Version]
- Baigent, C.; Landray, M.J.; Reith, C.; Emberson, J.; Wheeler, D.C.; Tomson, C.; Wanner, C.; Krane, V.; Cass, A.; Craig, J.; et al. The effects of lowering LDL cholesterol with simvastatin plus ezetimibe in patients with chronic kidney disease (Study of Heart and Renal Protection): A randomised placebo-controlled trial. Lancet 2011, 377, 2181–2192. [Google Scholar] [CrossRef] [Green Version]
- Herrington, W.G.; Emberson, J.; Mihaylova, B.; Blackwell, L.; Reith, C.; Solbu, M.D.; Mark, P.B.; Fellström, B.; Jardine, A.G.; Wanner, C.; et al. Impact of renal function on the effects of LDL cholesterol lowering with statin-based regimens: A meta-analysis of individual participant data from 28 randomised trials. Lancet Diabetes Endocrinol. 2016, 4, 829–839. [Google Scholar] [CrossRef] [Green Version]
- Querfeld, U. The clinical significance of vascular calcification in young patients with end-stage renal disease. Pediatr. Nephrol. 2004, 19, 478–484. [Google Scholar] [CrossRef]
- Wanner, C.; Amann, K.; Shoji, T. The heart and vascular system in dialysis. Lancet 2016, 388, 276–284. [Google Scholar] [CrossRef]
- Foley, R.N.; Parfrey, P.S.; Harnett, J.D.; Kent, G.M.; Murray, D.C.; Pe, B. The Prognostic Importance of Left Ventricular Geometry in Uremic Cardiomyopathy1. J. Am. Soc. Nephrol. 1995, 5, 2024–2031. [Google Scholar] [CrossRef]
- Chavers, B.M.; Li, S.; Collins, A.J.; Ca, H. Cardiovascular disease in pediatric chronic dialysis patients. Kidney Int. 2002, 62, 648–653. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ferris, M.E.; Mahan, J.D. Pediatric chronic kidney disease and the process of health care transition. Semin. Nephrol. 2009, 29, 435–444. [Google Scholar] [CrossRef]
- Ku, E.; Mitsnefes, M.M. Cardiovascular disease in young adults with incident ESRD. Nat. Rev. Nephrol. 2019, 15, 390–391. [Google Scholar] [CrossRef] [PubMed]
- Diaz-Gonzalez de Ferris, M.E. Adolescents and emerging adults with chronic kidney disease: Their unique morbidities and adherence issues. Blood Purif. 2011, 31, 203–208. [Google Scholar] [CrossRef]
- Wong, C.J.; Moxey-Mims, M.; Jerry-Fluker, J.; Warady, B.A.; Furth, S.L. CKiD (CKD in children) prospective cohort study: A review of current findings. Am. J. Kidney Dis. 2012, 60, 1002–1011. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tsai, T.C.; Chen, Y.C.; Lo, C.W.; Wang, W.S.; Lo, S.S.; Tang, G.J.; Thien, P.F. Incidence and renal survival of ESRD in the young Taiwanese population. Clin. J. Am. Soc. Nephrol. 2014, 9, 302–309. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ferris, M.E.; Miles, J.A.; Seamon, M.L. Adolescents and Young Adults with Chronic or End-Stage Kidney Disease. Blood Purif. 2016, 41, 205–210. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Modi, Z.J.; Lu, Y.; Ji, N.; Kapke, A.; Selewski, D.T.; Dietrich, X.; Abbott, K.; Nallamothu, B.K.; Schaubel, D.E.; Saran, R.; et al. Risk of Cardiovascular Disease and Mortality in Young Adults with End-stage Renal Disease: An Analysis of the US Renal Data System. JAMA Cardiol. 2019, 4, 353–362. [Google Scholar] [CrossRef] [Green Version]
- Kochanek, K.D.; Murphy, S.L.; Xu, J.; Tejada-Vera, B. Deaths: Final data for 2014, national vital statistics reports: From the Centers for Disease Control and Prevention, National Center for Health Statistics. Natl. Vital Stat. Syst. 2016, 65, 1–122. [Google Scholar]
- Hsing, A.W.; Ioannidis, J.P. Nationwide Population Science: Lessons from the Taiwan National Health Insurance Research Database. JAMA Intern. Med. 2015, 175, 1527–1529. [Google Scholar] [CrossRef] [PubMed]
- Lin, L.Y.; Warren-Gash, C.; Smeeth, L.; Chen, P.C. Data resource profile: The National Health Insurance Research Database (NHIRD). Epidemiol. Health 2018, 40, e2018062. [Google Scholar] [CrossRef]
- Roffman, C.E.; Buchanan, J.; Allison, G.T. Charlson Comorbidities Index. J. Physiother. 2016, 62, 171. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cheng, C.L.; Lee, C.H.; Chen, P.S.; Li, Y.H.; Lin, S.J.; Yang, Y.H. Validation of acute myocardial infarction cases in the national health insurance research database in Taiwan. J. Epidemiol. 2014, 24, 500–507. [Google Scholar] [CrossRef] [Green Version]
- Hsieh, C.Y.; Chen, C.H.; Li, C.Y.; Lai, M.L. Validating the diagnosis of acute ischemic stroke in a National Health Insurance claims database. J. Formos. Med. Assoc. 2015, 114, 254–259. [Google Scholar] [CrossRef]
- Xu, S.; Ross, C.; Raebel, M.A.; Shetterly, S.; Blanchette, C.; Smith, D. Use of stabilized inverse propensity scores as weights to directly estimate relative risk and its confidence intervals. Value Health 2010, 13, 273–277. [Google Scholar] [CrossRef] [Green Version]
- McCaffrey, D.F.; Griffin, B.A.; Almirall, D.; Slaughter, M.E.; Ramchand, R.; Burgette, L.F. A tutorial on propensity score estimation for multiple treatments using generalized boosted models. Stat. Med. 2013, 32, 3388–3414. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Austin, P.C. Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat. Med. 2009, 28, 3083–3107. [Google Scholar] [CrossRef] [Green Version]
- Goodman, W.G.; Goldin, J.; Kuizon, B.D.; Yoon, C.; Gales, B.; Sider, D.; Wang, Y.; Chung, J.; Emerick, A.; Greaser, L.; et al. Coronary-artery calcification in young adults with end-stage renal disease who are undergoing dialysis. N. Engl. J. Med. 2000, 342, 1478–1483. [Google Scholar] [CrossRef]
- Atkinson, M.A.; Lestz, R.M.; Fivush, B.A.; Silverstein, D.M. Comparative clinical outcomes between pediatric and young adult dialysis patients. Pediatr. Nephrol. 2011, 26, 2219–2226. [Google Scholar] [CrossRef]
- Efe, D.; Kocaoz, S. Adherence to diet and fluid restriction of individuals on hemodialysis treatment and affecting factors in Turkey. Jpn. J. Nurs. Sci. 2015, 12, 113–123. [Google Scholar] [CrossRef]
- Beerendrakumar, N.; Ramamoorthy, L.; Haridasan, S. Dietary and Fluid Regime Adherence in Chronic Kidney Disease Patients. J. Caring Sci. 2018, 7, 17–20. [Google Scholar] [CrossRef]
- Prichard, S.S. Comorbidities and their impact on outcome in patients with end-stage renal disease. Kidney Int. 2000, 57, S100–S104. [Google Scholar] [CrossRef] [Green Version]
- Chen, Z.; Qureshi, A.R.; Parini, P.; Hurt-Camejo, E.; Ripsweden, J.; Brismar, T.B.; Barany, P.; Jaminon, A.M.; Schurgers, L.J.; Heimburger, O.; et al. Does statins promote vascular calcification in chronic kidney disease? Eur. J. Clin. Investig. 2017, 47, 137–148. [Google Scholar] [CrossRef]
- Henein, M.; Granasen, G.; Wiklund, U.; Schmermund, A.; Guerci, A.; Erbel, R.; Raggi, P. High dose and long-term statin therapy accelerate coronary artery calcification. Int. J. Cardiol. 2015, 184, 581–586. [Google Scholar] [CrossRef]
- Puri, R.; Nicholls, S.J.; Shao, M.; Kataoka, Y.; Uno, K.; Kapadia, S.R.; Tuzcu, E.M.; Nissen, S.E. Impact of statins on serial coronary calcification during atheroma progression and regression. J. Am. Coll. Cardiol. 2015, 65, 1273–1282. [Google Scholar] [CrossRef]
- Ferencik, M.; Chatzizisis, Y.S. Statins and the coronary plaque calcium “paradox”: Insights from non-invasive and invasive imaging. Atherosclerosis 2015, 241, 783–785. [Google Scholar] [CrossRef]
- De Vriese, A.S. Should Statins Be Banned from Dialysis? J. Am. Soc. Nephrol. 2017, 28, 1675–1676. [Google Scholar] [CrossRef] [PubMed]
- Hirota, Y.; Nakagawa, K.; Sawada, N.; Okuda, N.; Suhara, Y.; Uchino, Y.; Kimoto, T.; Funahashi, N.; Kamao, M.; Tsugawa, N.; et al. Functional characterization of the vitamin K2 biosynthetic enzyme UBIAD1. PLoS ONE 2015, 10, e0125737. [Google Scholar] [CrossRef] [Green Version]
- Cranenburg, E.C.; Schurgers, L.J.; Uiterwijk, H.H.; Beulens, J.W.; Dalmeijer, G.W.; Westerhuis, R.; Magdeleyns, E.J.; Herfs, M.; Vermeer, C.; Laverman, G.D. Vitamin K intake and status are low in hemodialysis patients. Kidney Int. 2012, 82, 605–610. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Caluwe, R.; Pyfferoen, L.; De Boeck, K.; De Vriese, A.S. The effects of vitamin K supplementation and vitamin K antagonists on progression of vascular calcification: Ongoing randomized controlled trials. Clin. Kidney J. 2016, 9, 273–279. [Google Scholar] [CrossRef]
- Krueger, T.; Schlieper, G.; Schurgers, L.; Cornelis, T.; Cozzolino, M.; Jacobi, J.; Jadoul, M.; Ketteler, M.; Rump, L.C.; Stenvinkel, P.; et al. Vitamin K1 to slow vascular calcification in haemodialysis patients (VitaVasK trial): A rationale and study protocol. Nephrol. Dial. Transplant. 2014, 29, 1633–1638. [Google Scholar] [CrossRef] [PubMed]



| Before PSW | After PSW | |||||
|---|---|---|---|---|---|---|
| Statin Users (n = 771) | Nonstatin Users (n = 1709) | ASMD | Statin Users (n = 635) | Nonstatin Users (n = 1601) | ASMD | |
| Age (years) | 33.81 ± 5.03 | 32.89 ± 5.67 | 0.1713 | 33.42 ± 4.72 | 33.1 ± 5.33 | 0.0645 |
| Male, n (%) | 300 (38.91) | 990 (57.93) | 0.3876 | 289 (45.56) | 850 (53.08) | 0.1509 |
| Urb, n (%) | 0.1439 | 0.0493 | ||||
| Urban | 221 (28.66) | 431 (25.22) | 180 (28.36) | 416 (25.96) | ||
| Suburban | 257 (33.33) | 519 (30.37) | 196 (30.98) | 495 (30.94) | ||
| Rural | 293 (38.00) | 759 (44.41) | 258 (27.19) | 690 (43.10) | ||
| Occupation, n (%) | 0.1245 | 0.0958 | ||||
| Dependent | 80 (10.38) | 230 (13.46) | 72 (11.32) | 202 (12.62) | ||
| Civil servants | 20 (2.59) | 47 (2.75) | 15 (2.37) | 43 (2.68) | ||
| Nonmanual worker | 230 (29.83) | 444 (25.98) | 181 (28.37) | 436 (27.26) | ||
| Manual worker | 256 (33.20) | 549 (32.12) | 202 (31.85) | 514 (32.10) | ||
| Other | 185 (23.99) | 439 (25.69) | 163 (25.83) | 406 (25.34) | ||
| Income (NTD), n (%) | 0.2232 | 0.0777 | ||||
| Dependent | 80 (10.38) | 230 (13.46) | 72 (11.32) | 202 (12.62) | ||
| <17,280 | 219 (28.40) | 556 (32.53) | 195 (30.70) | 513 (32.08) | ||
| 17,280–21,008 | 156 (20.23) | 374 (21.88) | 136 (21.52) | 338 (21.13) | ||
| 21,009–33,229 | 187 (24.25) | 336 (19.66) | 136 (21.52) | 328 (20.48) | ||
| >33,300 | 129 (16.73) | 213 (12.46) | 95 (14.94) | 219 (13.69) | ||
| Comorbidities, n (%) | ||||||
| Atrial fibrillation | 0 (0.00) | 3 (0.18) | 0.0593 | 0 (0.00) | 4 (0.23) | 0.0674 |
| Chronic pulmonary disease | 20 (2.59) | 35 (2.05) | 0.0363 | 15 (2.30) | 32 (1.97) | 0.0228 |
| Connective tissue disease | 94 (12.19) | 140 (8.19) | 0.1325 | 66 (10.42) | 148 (9.27) | 0.0386 |
| Diabetes mellitus | 299 (38.78) | 185 (10.83) | 0.6841 | 135 (21.34) | 259 (16.15) | 0.1332 |
| Heart failure | 39 (5.06) | 96 (5.62) | 0.0249 | 28 (4.43) | 84 (5.23) | 0.0370 |
| Hypertension | 582 (75.49) | 1019 (59.63) | 0.3438 | 435 (68.62) | 1013 (63.29) | 0.1125 |
| Liver cirrhosis | 3 (0.39) | 29 (1.70) | 0.1290 | <3 (<0.45) | 22 (1.36) | 0.1290 |
| Peripheral arterial disease | 7 (0.91) | 26 (1.52) | 0.0560 | 4 (0.65) | 21 (1.31) | 0.0674 |
| Polycystic kidney disease | 5 (0.65) | 22 (1.29) | 0.0653 | 9 (1.39) | 18 (1.13) | 0.0234 |
| Charlson comorbidity index, | 2.25 ± 1.1 | 1.88 ± 0.98 | 0.3592 | 1.99 ± 0.91 | 1.94 ± 0.96 | 0.0580 |
| Medications, n (%) | ||||||
| ACEi/ARB | 438 (56.81) | 592 (34.64) | 0.4565 | 287 (45.21) | 634 (39.58) | 0.1141 |
| Other anti-HTN | 598 (77.56) | 845 (49.44) | 0.6107 | 398 (62.76) | 900 (56.24) | 0.1331 |
| Aspirin/Plavix | 64 (8.30) | 58 (3.39) | 0.2103 | 30 (4.81) | 58 (3.63) | 0.0586 |
| Insulin | 151 (19.58) | 73 (4.27) | 0.4862 | 64 (10.12) | 111 (6.96) | 0.1131 |
| OHA | 123 (15.95) | 49 (2.87) | 0.4599 | 50 (7.81) | 73 (4.59) | 0.1339 |
| No. of outpatient visits in the previous year | 33.68 ± 14.70 | 29.51 ± 12.40 | 0.3061 | 31.00 ± 11.69 | 30.32 ± 12.38 | 0.0562 |
| Hospitalizations in the previous year, n (%) | 339 (43.90) | 639 (37.97) | 0.1342 | 257 (40.60) | 620 (38.72) | 0.0384 |
| Statin Users | Nonstatin Users | Statin Users vs. Nonstatin Users | |||||
|---|---|---|---|---|---|---|---|
| No. of Event | Person-Years | Incidence Rate | No. of Event | Person-Years | Incidence Rate | SHR/HR (95%CI); p Value | |
| MACCE a | 87 | 3263.61 | 2.65 (2.09–3.21) | 138 | 9608.12 | 1.44 (1.20–1.68) | 1.87 (1.43–2.45); <0.0001 |
| AMI | 51 | 3376.31 | 1.51 (1.09–1.92) | 30 | 9940.81 | 0.30 (0.19–0.41) | 5.34 (3.40–8.39); <0.0001 |
| Stroke | 16 | 3475.96 | 0.46 (0.24–0.69) | 68 | 9815.81 | 0.70 (0.53–0.86) | 0.66 (0.39–1.14); 0.1368 |
| CV death | 8 | 3524.99 | 0.23 (0.10–0.44) | 17 | 10,025.6 | 0.17 (0.09–0.25) | 1.33 (0.57–3.08); 0.5132 |
| All-cause mortality | 69 | 3524.99 | 1.96 (1.50–2.42) | 229 | 10,025.6 | 2.28 (1.99–2.58) | 0.87 (0.66–1.14); 0.3058 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cheng, Y.-L.; Yang, H.-Y.; Wu, C.-Y.; Tsai, C.-Y.; Chen, C.-Y.; Hsiao, C.-C.; Hsu, H.-H.; Tian, Y.-C.; Yen, C.-L. Does Statin Therapy Reduce the Risks of Mortality and Major Adverse Cardiac and Cerebrovascular Events in Young Adults with End-Stage Renal Disease? Population-Based Cohort Study. J. Clin. Med. 2021, 10, 2097. https://doi.org/10.3390/jcm10102097
Cheng Y-L, Yang H-Y, Wu C-Y, Tsai C-Y, Chen C-Y, Hsiao C-C, Hsu H-H, Tian Y-C, Yen C-L. Does Statin Therapy Reduce the Risks of Mortality and Major Adverse Cardiac and Cerebrovascular Events in Young Adults with End-Stage Renal Disease? Population-Based Cohort Study. Journal of Clinical Medicine. 2021; 10(10):2097. https://doi.org/10.3390/jcm10102097
Chicago/Turabian StyleCheng, Ya-Lien, Huang-Yu Yang, Chao-Yi Wu, Chung-Ying Tsai, Chao-Yu Chen, Ching-Chung Hsiao, Hsiang-Hao Hsu, Ya-Chung Tian, and Chieh-Li Yen. 2021. "Does Statin Therapy Reduce the Risks of Mortality and Major Adverse Cardiac and Cerebrovascular Events in Young Adults with End-Stage Renal Disease? Population-Based Cohort Study" Journal of Clinical Medicine 10, no. 10: 2097. https://doi.org/10.3390/jcm10102097
APA StyleCheng, Y.-L., Yang, H.-Y., Wu, C.-Y., Tsai, C.-Y., Chen, C.-Y., Hsiao, C.-C., Hsu, H.-H., Tian, Y.-C., & Yen, C.-L. (2021). Does Statin Therapy Reduce the Risks of Mortality and Major Adverse Cardiac and Cerebrovascular Events in Young Adults with End-Stage Renal Disease? Population-Based Cohort Study. Journal of Clinical Medicine, 10(10), 2097. https://doi.org/10.3390/jcm10102097






