Long-Term Results (up to 20 Years) of 19 mm or Smaller Prostheses in the Aortic Position. Does Size Matter? A Propensity-Matched Survival Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Patient Population
2.3. Definitions
2.4. Propensity Matching
2.5. Objectives
2.6. Statistical Analysis
3. Results
4. Discussion
Study Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Manning, W.J. Asymptomatic Aortic Stenosis in the Elderly: A Clinical Review. JAMA 2013, 310, 1490–1497. [Google Scholar] [CrossRef] [PubMed]
- Eveborn, G.W.; Schirmer, H.; Heggelund, G.; Lunde, P.; Rasmussen, K. The Evolving Epidemiology of Valvular Aortic Stenosis. the Tromsø Study. HEART 2013, 99, 396–400. [Google Scholar] [CrossRef] [Green Version]
- Falk, V.; Baumgartner, H.; Bax, J.J.; De Bonis, M.; Hamm, C.; Holm, P.J.; Iung, B.; Lancellotti, P.; Lansac, E.; Muñoz, D.R.; et al. 2017 ESC/EACTS Guidelines for the Management of Valvular Heart Disease. Eur. Heart J. 2017, 38, 2739–2791. [Google Scholar] [CrossRef]
- Writing Committee Members; Otto, C.M.; Nishimura, R.A.; Bonow, R.O.; Carabello, B.A.; Erwin, J.P.; Gentile, F.; Jneid, H.; Krieger, E.V.; Mack, M.; et al. 2020 ACC/AHA Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2021, 77, 450–500. [Google Scholar] [CrossRef]
- Wilbring, M.; Alexiou, K.; Schumann, E.; Matschke, K.; Tugtekin, S.M. Isolated Aortic Valve Replacement in Patients with Small Aortic Annulus-a High-Risk Group on Long-Term Follow-Up. Thorac. Cardiovasc. Surg. 2013, 61, 379–385. [Google Scholar] [CrossRef] [PubMed]
- Freitas-Ferraz, A.B.; Tirado-Conte, G.; Dagenais, F.; Ruel, M.; Al-Atassi, T.; Dumont, E.; Mohammadi, S.; Bernier, M.; Pibarot, P.; Rodés-Cabau, J. Aortic Stenosis and Small Aortic Annulus. Circulation 2019, 139, 2685–2702. [Google Scholar] [CrossRef] [PubMed]
- Pibarot, P.; Dumesnil, J.G. Hemodynamic and Clinical Impact of Prosthesis-Patient Mismatch in the Aortic Valve Position and Its Prevention. J. Am. Coll. Cardiol. 2000, 36, 1131–1141. [Google Scholar] [CrossRef] [Green Version]
- Rao, V.; Jamieson, W.R.; Ivanov, J.; Armstrong, S.; David, T.E. Prosthesis-Patient Mismatch Affects Survival after Aortic Valve Replacement. Circulation 2000, 102, III5-9. [Google Scholar] [CrossRef]
- Cribier, A.; Eltchaninoff, H.; Bash, A.; Borenstein, N.; Tron, C.; Bauer, F.; Derumeaux, G.; Anselme, F.; Laborde, F.; Leon, M.B. Percutaneous Transcatheter Implantation of an Aortic Valve Prosthesis for Calcific Aortic Stenosis: First Human Case Description. Circulation 2002, 106, 3006–3008. [Google Scholar] [CrossRef]
- Makkar, R.R.; Thourani, V.H.; Mack, M.J.; Kodali, S.K.; Kapadia, S.; Webb, J.G.; Yoon, S.-H.; Trento, A.; Svensson, L.G.; Herrmann, H.C.; et al. Five-Year Outcomes of Transcatheter or Surgical Aortic-Valve Replacement. N. Engl. J. Med. 2020, 382, 799–809. [Google Scholar] [CrossRef]
- Pibarot, P.; Salaun, E.; Dahou, A.; Avenatti, E.; Guzzetti, E.; Annabi, M.-S.; Toubal, O.; Bernier, M.; Beaudoin, J.; Ong, G.; et al. Echocardiographic Results of Transcatheter Versus Surgical Aortic Valve Replacement in Low-Risk Patients: The PARTNER 3 Trial. Circulation 2020, 141, 1527–1537. [Google Scholar] [CrossRef] [PubMed]
- Borger, M.A.; Carson, S.M.; Ivanov, J.; Rao, V.; Scully, H.E.; Feindel, C.M.; David, T.E. Stentless Aortic Valves Are Hemodynamically Superior to Stented Valves during Mid-Term Follow-up: A Large Retrospective Study. Ann. Thorac. Surg. 2005, 80, 2180–2185. [Google Scholar] [CrossRef]
- Kulik, A.; Al-Saigh, M.; Chan, V.; Masters, R.G.; Bédard, P.; Lam, B.-K.; Rubens, F.D.; Hendry, P.J.; Mesana, T.G.; Ruel, M. Enlargement of the Small Aortic Root during Aortic Valve Replacement: Is There a Benefit? Ann. Thorac. Surg. 2008, 85, 94–100. [Google Scholar] [CrossRef] [PubMed]
- Coutinho, G.F.; Correia, P.M.; Paupério, G.; de Oliveira, F.; Antunes, M.J. Aortic Root Enlargement Does Not Increase the Surgical Risk and Short-Term Patient Outcome? Eur. J. Cardiothorac. Surg. 2011, 40, 441–447. [Google Scholar] [CrossRef] [Green Version]
- Tam, D.Y.; Dharma, C.; Rocha, R.V.; Ouzounian, M.; Wijeysundera, H.C.; Austin, P.C.; Fremes, S.E. Early and Late Outcomes Following Aortic Root Enlargement: A Multicenter Propensity Score-Matched Cohort Analysis. J. Thorac. Cardiovasc. Surg. 2020, 160, 908–919.e15. [Google Scholar] [CrossRef]
- David, T.E.; Uden, D.E. Aortic Valve Replacement in Adult Patients with Small Aortic Annuli. Ann. Thorac. Surg. 1983, 36, 577–583. [Google Scholar] [CrossRef]
- Massias, S.A.; Pittams, A.; Mohamed, M.; Ahmed, S.; Younas, H.; Harky, A. Aortic Root Enlargement: When and How. J. Card. Surg. 2021, 36, 229–235. [Google Scholar] [CrossRef]
- Peterson, M.D.; Borger, M.A.; Feindel, C.M.; David, T.E. Aortic Annular Enlargement during Aortic Valve Replacement: Improving Results with Time. Ann. Thorac. Surg. 2007, 83, 2044–2049. [Google Scholar] [CrossRef]
- Beckmann, E.; Martens, A.; Alhadi, F.; Hoeffler, K.; Umminger, J.; Kaufeld, T.; Sarikouch, S.; Koigeldiev, N.; Cebotari, S.; Schmitto, J.D.; et al. Aortic Valve Replacement with Sutureless Prosthesis: Better than Root Enlargement to Avoid Patient-Prosthesis Mismatch? Interact. Cardiovasc. Thorac. Surg. 2016, 22, 744–749. [Google Scholar] [CrossRef] [Green Version]
- Coti, I.; Haberl, T.; Scherzer, S.; Shabanian, S.; Binder, T.; Kocher, A.; Laufer, G.; Andreas, M. Rapid-Deployment Aortic Valves for Patients With a Small Aortic Root: A Single-Center Experience. Ann. Thorac. Surg. 2020, 110, 1549–1556. [Google Scholar] [CrossRef]
- Rahimtoola, S.H. The Problem of Valve Prosthesis-Patient Mismatch. Circulation 1978, 58, 20–24. [Google Scholar] [CrossRef] [Green Version]
- Walther, T.; Rastan, A.; Falk, V.; Lehmann, S.; Garbade, J.; Funkat, A.K.; Mohr, F.W.; Gummert, J.F. Patient Prosthesis Mismatch Affects Short- and Long-Term Outcomes after Aortic Valve Replacement. Eur. J. Cardiothorac. Surg. 2006, 30, 15–19. [Google Scholar] [CrossRef] [PubMed]
- Head, S.J.; Mokhles, M.M.; Osnabrugge, R.L.J.; Pibarot, P.; Mack, M.J.; Takkenberg, J.J.M.; Bogers, A.J.J.C.; Kappetein, A.P. The Impact of Prosthesis-Patient Mismatch on Long-Term Survival after Aortic Valve Replacement: A Systematic Review and Meta-Analysis of 34 Observational Studies Comprising 27 186 Patients with 133 141 Patient-Years. Eur. Heart. J. 2012, 33, 1518–1529. [Google Scholar] [CrossRef] [Green Version]
- Fallon, J.M.; DeSimone, J.P.; Brennan, J.M.; O’Brien, S.; Thibault, D.P.; DiScipio, A.W.; Pibarot, P.; Jacobs, J.P.; Malenka, D.J. The Incidence and Consequence of Prosthesis-Patient Mismatch After Surgical Aortic Valve Replacement. Ann. Thorac. Surg. 2018, 106, 14–22. [Google Scholar] [CrossRef] [Green Version]
- Alvarez, J.R.; Quiroga, J.S.; Fernandez, M.V.; Nazar, B.A.; Sampedro, F.G.; Martinez Comendador, J.M.; Martinez Cereijo, J.M.; Alves Perez, M.T. Up to Twenty-Five-Year Survival after Aortic Valve Replacement with Size 19 Mm Valves. Interact. Cardiovasc. Thorac. Surg. 2010, 10, 32–35. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Koene, B.M.; Soliman Hamad, M.A.; Bouma, W.; Mariani, M.A.; Peels, K.C.; van Dantzig, J.-M.; van Straten, A.H. Impact of Prosthesis-Patient Mismatch on Early and Late Mortality after Aortic Valve Replacement. J. Cardiothorac. Surg. 2013, 8, 96. [Google Scholar] [CrossRef] [Green Version]
- Koch, C.G.; Khandwala, F.; Estafanous, F.G.; Loop, F.D.; Blackstone, E.H. Impact of Prosthesis-Patient Size on Functional Recovery after Aortic Valve Replacement. Circulation 2005, 111, 3221–3229. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carrier, M.; Pellerin, M.; Perrault, L.P.; Hébert, Y.; Pagé, P.; Cartier, R.; Dyrda, I.; Pelletier, L.C. Experience with the 19-Mm Carpentier-Edwards Pericardial Bioprosthesis in the Elderly. Ann. Thorac. Surg. 2001, 71, S249–S252. [Google Scholar] [CrossRef]
- Kato, Y.; Hattori, K.; Motoki, M.; Takahashi, Y.; Kotani, S.; Nishimura, S.; Shibata, T. Optimal Results of Aortic Valve Replacement with Small Mechanical Valves (<19 Mm). J. Heart Valve Dis. 2013, 22, 468–475. [Google Scholar]
- Domoto, S.; Niinami, H.; Uwabe, K.; Koike, H.; Tabata, M.; Morita, K.; Kambe, M.; Iguchi, A. Comparison of Early Haemodynamics of 19-Mm Aortic Valve Bioprostheses in Patients with a Small Aortic Annulus. Interact. Cardiovasc. Thorac. Surg. 2016, 22, 19–25. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- You, J.H.; Jeong, D.S.; Sung, K.; Kim, W.S.; Carriere, K.C.; Lee, Y.T.; Park, P.W. Aortic Valve Replacement With Carpentier-Edwards: Hemodynamic Outcomes for the 19-Mm Valve. Ann. Thorac. Surg. 2016, 101, 2209–2216. [Google Scholar] [CrossRef] [Green Version]
- He, G.W.; Grunkemeier, G.L.; Gately, H.L.; Furnary, A.P.; Starr, A. Up to Thirty-Year Survival after Aortic Valve Replacement in the Small Aortic Root. Ann. Thorac. Surg. 1995, 59, 1056–1062. [Google Scholar] [CrossRef]
- Medalion, B.; Lytle, B.W.; McCarthy, P.M.; Stewart, R.W.; Arheart, K.L.; Arnold, J.H.; Loop, F.D.; Cosgrove, D.M. Aortic Valve Replacement for Octogenarians: Are Small Valves Bad? Ann. Thorac. Surg. 1998, 66, 699–705; discussion 705–706. [Google Scholar] [CrossRef]
- Izzat, M.B.; Kadir, I.; Reeves, B.; Wilde, P.; Bryan, A.J.; Angelini, G.D. Patient-Prosthesis Mismatch Is Negligible with Modern Small-Size Aortic Valve Prostheses. Ann. Thorac. Surg. 1999, 68, 1657–1660. [Google Scholar] [CrossRef]
- Hanayama, N.; Christakis, G.T.; Mallidi, H.R.; Joyner, C.D.; Fremes, S.E.; Morgan, C.D.; Mitoff, P.R.R.; Goldman, B.S. Patient Prosthesis Mismatch Is Rare after Aortic Valve Replacement: Valve Size May Be Irrelevant. Ann. Thorac. Surg. 2002, 73, 1822–1829; discussion 1829. [Google Scholar] [CrossRef]
- Christakis, G.T.; Joyner, C.D.; Morgan, C.D.; Fremes, S.E.; Buth, K.J.; Sever, J.Y.; Rao, V.; Panagiotopoulos, K.P.; Murphy, P.M.; Goldman, B.S. Left Ventricular Mass Regression Early after Aortic Valve Replacement. Ann. Thorac. Surg. 1996, 62, 1084–1089. [Google Scholar] [CrossRef]
- Colli, A.; Marchetto, G.; Salizzoni, S.; Rinaldi, M.; Di Marco, L.; Pacini, D.; Di Bartolomeo, R.; Nicolini, F.; Gherli, T.; Agrifoglio, M.; et al. The TRIBECA Study: (TRI)Fecta (B)Ioprosthesis (E)Valuation versus (C)Arpentier Magna-Ease in (A)Ortic Position. Eur. J. Cardiothorac. Surg. 2016, 49, 478–485. [Google Scholar] [CrossRef] [Green Version]
- Allen, K.B.; Chhatriwalla, A.K.; Cohen, D.J.; Saxon, J.T.; Aggarwal, S.; Hart, A.; Baron, S.; Davis, J.R.; Pak, A.F.; Dvir, D.; et al. Bioprosthetic Valve Fracture to Facilitate Transcatheter Valve-in-Valve Implantation. Ann. Thorac. Surg. 2017, 104, 1501–1508. [Google Scholar] [CrossRef] [Green Version]
- Sathananthan, J.; Sellers, S.; Barlow, A.M.; Stanová, V.; Fraser, R.; Toggweiler, S.; Allen, K.B.; Chhatriwalla, A.; Murdoch, D.J.; Hensey, M.; et al. Valve-in-Valve Transcatheter Aortic Valve Replacement and Bioprosthetic Valve Fracture Comparing Different Transcatheter Heart Valve Designs: An Ex Vivo Bench Study. JACC Cardiovasc. Interv. 2019, 12, 65–75. [Google Scholar] [CrossRef]
- Lopez, S.; Meyer, P.; Teboul, J.; Deharo, P.; Mihoubi, A.; Elbeze, J.P.; Lena, D.; Camarasa, P.; Laborde, J.C.; Drogoul, L. Transcatheter Valve-in-Valve Implantation in a Degenerated Very Small Mitroflow Prosthesis. Interact. Cardiovasc. Thorac. Surg. 2018, 27, 850–855. [Google Scholar] [CrossRef]
- Patel, J.S.; Krishnaswamy, A.; White, J.; Mick, S.; Navia, J.; Mehta, A.; Bakaeen, F.; Popovic, Z.; Svensson, L.; Kapadia, S.R. Optimizing Hemodynamics of Transcatheter Aortic Valve-in-Valve Implantation in 19-Mm Surgical Aortic Prostheses. Catheter. Cardiovasc. Interv. 2018, 92, 550–554. [Google Scholar] [CrossRef] [PubMed]
- Garcia, D.; Pibarot, P.; Dumesnil, J.G.; Sakr, F.; Durand, L.G. Assessment of Aortic Valve Stenosis Severity: A New Index Based on the Energy Loss Concept. Circulation 2000, 101, 765–771. [Google Scholar] [CrossRef] [PubMed]
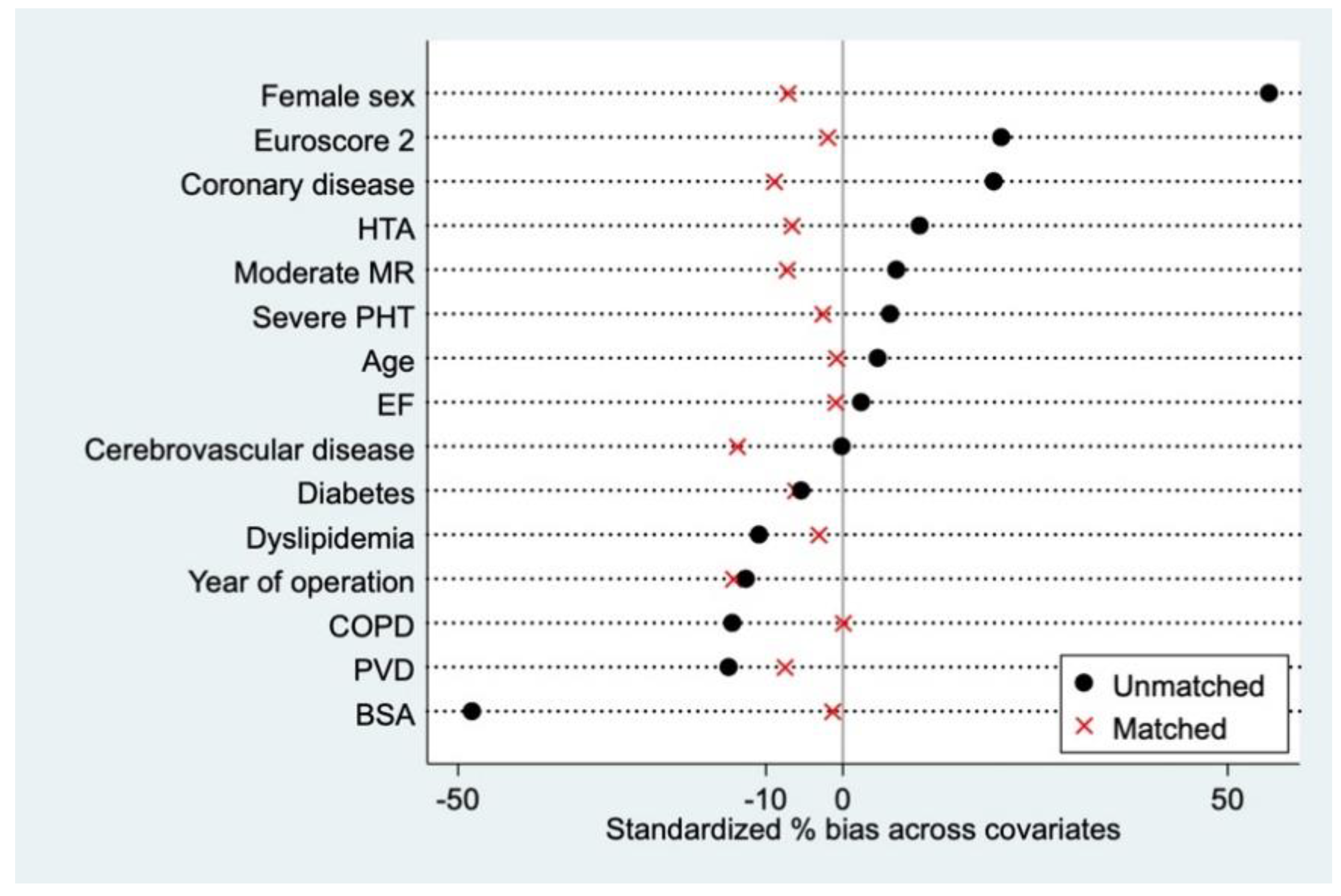

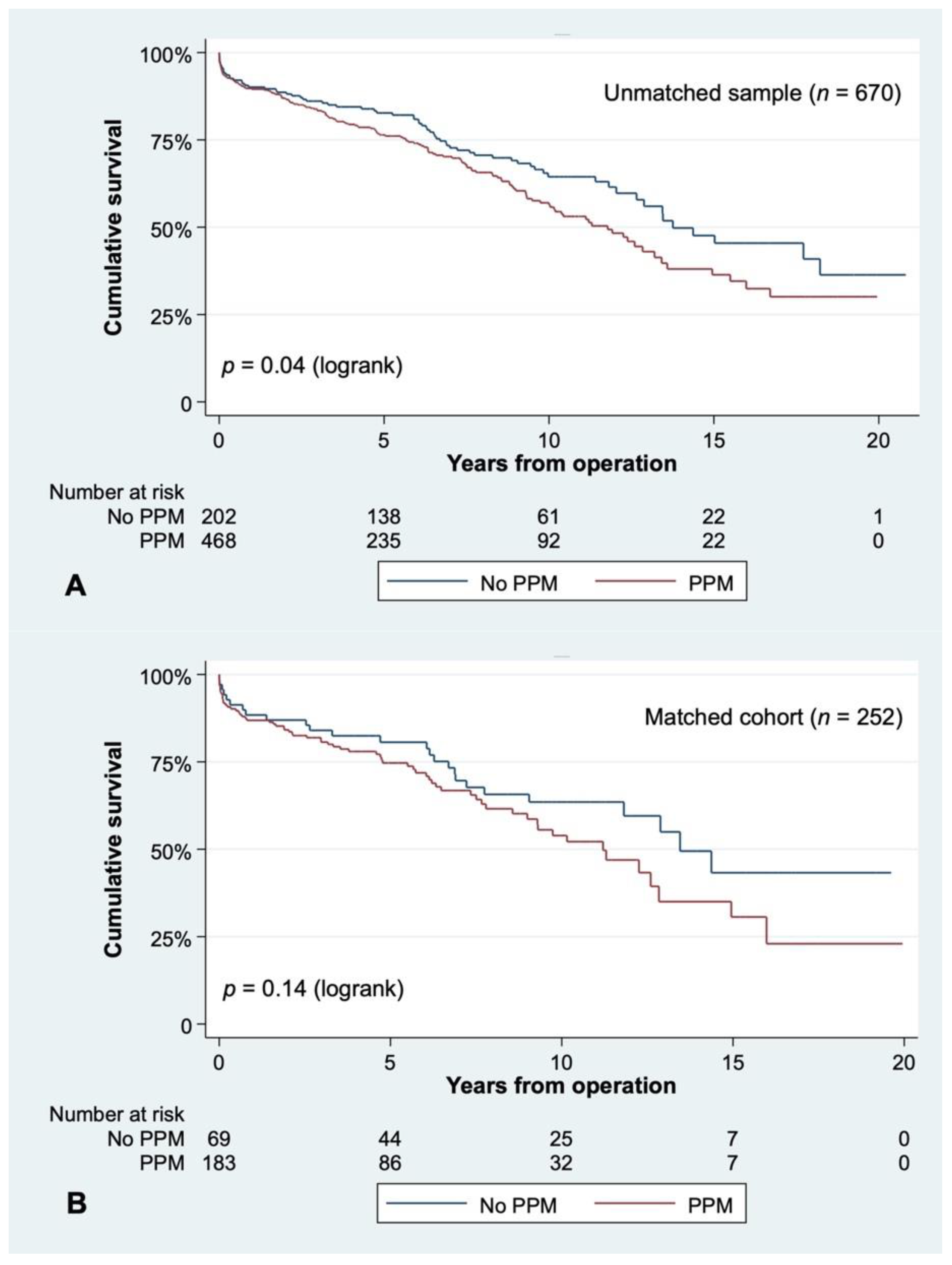

| Variable | All Patients | Matched Cohort | ||||
|---|---|---|---|---|---|---|
| Valve ≤ 19 (n = 132) | Valve ≥ 21 (n = 538) | p Value | Valve ≤ 19 (n = 126) | Valve ≥ 21 (n = 126) | p Value | |
| n (%) | n (%) | n (%) | n (%) | |||
| Age | 64.55 ± 11.08 | 64.82 ± 12.45 | 0.54 | 64.39 ± 11.20 | 64.5 ± 13.95 | 0.94 |
| Female sex | 109 (82.59) | 311 (57.81) | <0.01 | 103 (81.75) | 107 (84.92) | 0.49 |
| EuroSCORE II | 2.67 ± 3.16 | 2.11 ± 1.80 | <0.01 | 2.54 ± 3.07 | 2.59 ± 2.10 | 0.87 |
| Aortic stenosis | 121 (91.67) | 510 (94.80) | 0.16 | 115 (91.27) | 116 (92.06) | 0.82 |
| Arterial hypertension | 89 (67.42) | 340 (63.20) | 0.36 | 84 (66.67) | 88 (69.84) | 0.58 |
| Severe pulmonary hypertension | 14 (10.61) | 46 (8.55) | 0.45 | 14 (11.11) | 15 (11.90) | 0.84 |
| Diabetes | 22 (16.67) | 102 (18.96) | 0.54 | 20 (15.87) | 23 (18.25) | 0.61 |
| CAD 1 | 24 (18.18) | 61 (11.34) | 0.03 | 20 (15.87) | 24 (19.05) | 0.5 |
| COPD 2 | 2 (1.52) | 22 (4.09) | 0.15 | 2 (1.59) | 2 (1.59) | 1.00 |
| Dyslipidemia | 61 (46.21) | 282 (52.42) | 0.20 | 60 (47.62) | 62 (49.21) | 0.80 |
| PVD 3 | 4 (3.03) | 33 (6.13) | 0.16 | 4 (3.17) | 6 (4.76) | 0.51 |
| Cerebrovascular disease | 4 (3.03) | 18 (3.35) | 0.85 | 3 (2.38) | 6 (4.76) | 0.30 |
| LV-EF 4 | 52.41 ± 9.19 | 52 ± 9.60 | 0.66 | 52.82 ± 8.62 | 52.92 ± 10.30 | 0.93 |
| Moderate mitral regurgitation | 35 (26.32) | 65 (21.74) | 0.29 | 33 (26.19) | 37 (29.37) | 0.57 |
| Moderate tricuspid regurgitation | 9 (6.82) | 21 (3.90) | 0.14 | 9 (7.14) | 7 (5.56) | 0.60 |
| BSA 5 | 1.71 ± 0.19 | 1.80 ± 0.19 | <0.01 | 1.71 ± 0.19 | 1.71 ± 0.20 | 0.91 |
| Mean aortic gradient | 55.78 ± 21.06 | 54.14 ± 19.01 | 0.39 | 55.61 ± 21.46 | 52.72 ± 18.91 | 0.26 |
| BMI 6 | 26.05 ± 4.62 | 26.97 ± 4.89 | 0.04 | 26.06 ± 4.51 | 26.15 ± 5.33 | 0.88 |
| Valve Type | All Patients | Matched Cohort | ||
|---|---|---|---|---|
| n | % | n | % | |
| Mechanic | ||||
| Sorin Carbomedics TopHat | 121 | 18.05 | 43 | 17.06 |
| St Jude Masters | 113 | 16.86 | 45 | 17.86 |
| Carbomedics Orbis Model 100 | 43 | 6.41 | 19 | 7.54 |
| Medtronic Open Pivot | 37 | 5.52 | 15 | 5.95 |
| Sorin Bicarbon | 34 | 5.07 | 16 | 6.35 |
| St Jude Regent | 30 | 4.48 | 9 | 3.57 |
| Carbomedics Standard | 15 | 2.24 | 9 | 3.57 |
| Medtronic Hall | 11 | 1.64 | 2 | 0.79 |
| Sorin Allcarbon | 5 | 0.75 | 3 | 1.19 |
| Medtronic Advantage | 4 | 0.6 | 0 | 0 |
| ON-X | 2 | 0.3 | 0 | 0 |
| St Jude HP | 1 | 0.15 | 1 | 0.4 |
| Biologic | ||||
| Edwards Perimount 2900 | 113 | 16.87 | 41 | 16.27 |
| Medtronic Hancock II | 74 | 11.05 | 22 | 8.73 |
| St Jude Epic | 29 | 4.33 | 13 | 5.16 |
| Braile FABP | 17 | 2.54 | 7 | 2.78 |
| Sorin Mitroflow | 7 | 1.04 | 1 | 0.4 |
| Medtronic Freestyle | 6 | 0.9 | 4 | 1.59 |
| Sulzer Carbomedics Labcor | 5 | 0.75 | 1 | 0.4 |
| St Jude Trifecta | 2 | 0.3 | 1 | 0.4 |
| Sorin Pericarbon | 1 | 0.15 | 0 | 0 |
| Total | 670 | 100 | 252 | 100 |
| Variable | Valve ≤ 19 n (%) | Valve ≥ 21 n (%) | p |
|---|---|---|---|
| Concomitant procedures | 15.08% | 11.9% | 0.46 |
| CABG | 9 (7.14) | 8 (6.35) | 0.80 |
| Mitral valve replacement | 7 (5.56) | 2 (1.59) | 0.09 |
| Mitral valve repair | 1 (0.79) | 3 (2.59) | 0.27 |
| Aortic annulus enlargement | 2 (1.58) | 1 (0.79) | 0.56 |
| Ascending aortic replacement | 0 (0) | 1 (0.79) | 0.31 |
| Carotid endarterectomy | 1 (0.85) | 0 (0) | 0.33 |
| Operative data | |||
| Bypass time (mean ± SD) | 120.23 ± 88.17 | 102.73 ± 38.35 | 0.04 |
| Cross-clamp time (mean ± SD) | 77.73 ± 43.43 | 66.72 ± 16.71 | <0.01 |
| Postoperative length of stay (mean ± SD) | 12.08 ± 25.20 | 9.22 ± 4.79 | 0.21 |
| Early mortality (<30 days) | 5 (3.97) | 7 (5.56) | 0.55 |
| EOAi (cm2/m2) | 0.67 ± 0.13 | 0.84 ± 0.20 | <0.01 |
| PPM | 110 (87.30) | 73 (57.94) | <0.01 |
| Severe PPM | 68 (53.97) | 18 (14.29) | <0.01 |
| EuroSCORE II risk score | 2.54 ± 3.07 | 2.59 ± 2.10 | 0.87 |
| Follow-up (years) (mean ± SD) | 6.54 ± 4.60 | 5.98 ± 4.47 | 0.32 |
| Variable | All Patients (n = 670) | Matched Cohort (n = 252) | ||
|---|---|---|---|---|
| HR (95% CI) | p Value | HR (95% CI) | p Value | |
| Valve size | 0.92 (0.62–1.35) | 0.68 | 0.76 (0.49–1.17) | 0.22 |
| PPM | 1.06 (0.76–1.48) | 0.72 | 1.56 (0.95–2.54) | 0.07 |
| Male sex | 0.84 (0.62–1.16) | 0.30 | ||
| Age (per year) | 1.04 (1.03–1.06) | <0.01 | ||
| Arterial hypertension | 0.92 (0.67–1.28) | 0.65 | ||
| Bypass time (per min) | 1.005 (1.003–1.008) | <0.01 | ||
| Dyslipidemia | 0.77 (0.56–1.06) | 0.11 | ||
| Creatinine (per mg%) | 1.30 (1.13–1.50) | <0.01 | ||
| CAD 1 | 1.25 (0.83–1.88) | 0.27 | ||
| Ejection fraction | 0.98 (0.97–0.99) | 0.04 | ||
| COPD 2 | 0.73 (0.31–1.70) | 0.47 | ||
| Diabetes | 1.63 (1.14–2.52) | <0.01 | ||
| BMI | 0.97 (0.99–1.01) | 0.17 | ||
| PVD 3 | 1.94 (1.16–3.25) | 0.01 | ||
| Cerebrovascular disease | 1.70 (0.82–3.53) | 0.14 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Feier, H.; Grigorescu, A.; Falnita, L.; Rachita, O.; Gaspar, M.; Luca, C.T. Long-Term Results (up to 20 Years) of 19 mm or Smaller Prostheses in the Aortic Position. Does Size Matter? A Propensity-Matched Survival Analysis. J. Clin. Med. 2021, 10, 2055. https://doi.org/10.3390/jcm10102055
Feier H, Grigorescu A, Falnita L, Rachita O, Gaspar M, Luca CT. Long-Term Results (up to 20 Years) of 19 mm or Smaller Prostheses in the Aortic Position. Does Size Matter? A Propensity-Matched Survival Analysis. Journal of Clinical Medicine. 2021; 10(10):2055. https://doi.org/10.3390/jcm10102055
Chicago/Turabian StyleFeier, Horea, Andrei Grigorescu, Lucian Falnita, Oana Rachita, Marian Gaspar, and Constantin T. Luca. 2021. "Long-Term Results (up to 20 Years) of 19 mm or Smaller Prostheses in the Aortic Position. Does Size Matter? A Propensity-Matched Survival Analysis" Journal of Clinical Medicine 10, no. 10: 2055. https://doi.org/10.3390/jcm10102055
APA StyleFeier, H., Grigorescu, A., Falnita, L., Rachita, O., Gaspar, M., & Luca, C. T. (2021). Long-Term Results (up to 20 Years) of 19 mm or Smaller Prostheses in the Aortic Position. Does Size Matter? A Propensity-Matched Survival Analysis. Journal of Clinical Medicine, 10(10), 2055. https://doi.org/10.3390/jcm10102055






