1. Introduction
Steroids are organic compounds, derivatives of the cyclic hydrocarbon sterane, composed of four conjugated homocyclic rings. It is comprised of three cyclohexanes and one cyclopentane ring. Individual rings are marked with consecutive letters of the alphabet, and individual carbon atoms are numbered [
1]. Depending on the type of steroid, this skeleton can be extended in various ways with additional carbon atoms, creating various systems, such as the systems of estran, androstane, pregnane, cholate and cholestane. Various functional groups, such as OH, CHO, COOH or CO, can be attached to these systems, changing their biological activity to a large extent. Depending on the function and use, steroids can be divided into five main groups, which include sterols, corticosteroids, anabolic steroids, sex hormones and prohormones. In medical therapy, steroids are used in a wide variety of diseases, including topical conditions, inflammation, autoimmune diseases, allergies or cancer treatment [
2,
3,
4,
5]. Steroids, due to their immunosuppressive properties, are also commonly used after organ transplantation to reduce the risk of rejecting an organ [
6,
7,
8]. Apart from its beneficial properties, steroids taken without proper supervision may also cause serious health conditions, such as hypertension, glaucoma, osteoporosis or headaches [
9,
10,
11].
Hormones are organic substances that play a regulatory role in organisms. They are most often produced by the endocrine glands (less often by endocrine tissues) and then transported through the blood to the target cells. Hormone binding by a receptor located on the surface or inside the cell triggers a series of reactions that stimulate or inhibit specific metabolic processes in order to maintain homeostasis of the entire body [
12]. There are several different criteria for classifying hormones: due to their place of formation, the chemical structure, mechanism of action, or exerted final effect. Due to the chemical structure, four main groups of hormones can be distinguished, such as peptide and protein hormones, amino acid derivative hormones, steroid hormones and fatty acid analogs [
13]. It is known that hormones also affect the functioning of the immune system and even behavior. Therefore, diseases resulting from hormonal disorders have serious consequences on health and can cause multi-organ symptoms. Not only are hormones produced in our body glands, but they are also an important part of the common medicines used in the treatment of hypothyroidism, polycystic ovaries syndrome, breast and prostate cancer, adult acne conditions and during hormone replacement therapy [
14,
15,
16].
By considering the importance of the steroid and hormone families, numerous attempts have been made through the years in order to detect them with high sensitivity using different analytical techniques. Most of the biological samples containing steroids and hormones are analyzed using gas or liquid chromatography coupled with the mass spectrometer [
17,
18,
19,
20,
21,
22]. Determination of the analyte by using these techniques is very accurate; however, the whole analytical procedure is expensive, time-consuming and often requires long and complicated sample pretreatment and specialized skills of the analyst. Considering these disadvantages, electrochemical methods and the development of new electrochemical sensors are gaining much attention lately due to their simplicity, high sensitivity, easiness and low financial outlay. Electroanalysis is one of the analytical methods that help to detect and quantify the analyte in an aqueous solution. Electroanalytical methods, such as voltammetry and polarography, are based on registering the current vs. voltage relation on a voltammogram or polarogram. Voltammetric and polarographic measurements are characterized by potential, which is related to the qualitative properties of the analyte, and the current, which is related to the qualitative amount of the analyte in the measurement cell. The selectivity of the electrochemical methods depends on the accessible potential range for the chosen electrode, the number of compounds in the sample and the half-width of each signal. The choice of optimal techniques depends on several factors, such as the nature of the analyte, the type and material of the electrode and the choice of supporting electrolyte. Specifically, the size and morphology of the working electrode can be very crucial to the analytical response of the system.
This review aims to describe the possibilities of the electrochemical hormones and steroid determination assays that can be successfully applied for their highly sensitive measurements. It is impossible to quote all the papers concerning this topic; thus, only selected manuscripts containing voltammetric, polarographic and amperometric methods are cited. The authors focused on the most recent positions published since 2000.
2. Electrochemical Techniques used for Hormones and Steroids Determination
Electrochemistry is a well-established analytical branch and is widely used for the determination of pharmaceutical compounds. The most popular electrochemical techniques used in hormone and steroid analyses are voltammetry and polarography. Notably, voltammetry, which is considered a fast, accurate and high sensitive method, is a willingly chosen technique for the routine quality assurance analysis of electroactive analytes. In voltammetry, a few specific techniques used for qualitative and quantitative measurements can be distinguished, such as cyclic voltammetry (CV), linear sweep voltammetry (LSV), differential pulse voltammetry (DPV) or square-wave voltammetry (SWV). What the above have in common is the basis of signal registration, which is based on the application of a specific potential to the working electrode and registration of the current change in the applied potential range. CV studies are usually used to determine the type of transport of the analyte to the surface of the working electrode, which may be limited by adsorption or diffusion. Additionally, the use of the CV technique allows us to distinguish if the electrode process is reversible or irreversible and thus could be a useful tool for explaining the electrode reaction in detail by giving the possibility to calculate the number of electrons exchanged. CV is very rarely used for the quantitative analysis of compounds because of its lower sensitivity in comparison with other voltammetric techniques. For this type of analysis, the DPV and SWV techniques are widely used. Among the voltammetric techniques, DPV and SWV offer much better sensitivity with a more beneficial signal-to-noise factor, which results in the possibility of performing measurements of electroactive compounds at trace levels. Therefore, these two techniques are used for the studies of active substances present in the pharmaceutical products, such as tablets, creams, ointments, injections, etc., and also often provide opportunities to perform measurements in biological samples, such as urine, blood, serum, etc.
A typical electrochemical sensor used during voltammetric measurements comprises a working electrode, an auxiliary electrode (e.g., platinum rod) and a reference electrode (usually a saturated calomel electrode or Ag/AgCl electrode). The most known working electrodes belong to the family of mercury electrodes, with the dropping mercury electrode (DME) and hanging drop mercury electrode (HMDE) as representatives. Mercury is characterized as the most desired, nearly perfectly polarizable electrode material due to its properties, which include its easy renewal and smooth drop surface, which result in high sensitivity and broad potential windows in the cathodic range. Due to the mentioned properties, the use of mercury in working electrode construction enables the measurement of a wide variety of electroactive compounds. The main disadvantage of the mercury electrodes is the high toxicity of this element, which requires careful work and the utilization of toxic mercury waste after the measurements. Therefore, solid electrodes as an alternative to mercury electrodes are nowadays preferable due to their non-toxic construction. Solid electrodes, made of materials, such as glassy carbon, graphite, noble metals or diamond-related materials, etc., may be characterized by a wide range of working potentials in the anodic region in comparison to the mercury electrodes. The main disadvantage of such electrodes is the necessity for surface preparation before measurement, based on the use of the polishing powder or chemical pretreatment. Solid electrodes also provide a great opportunity to investigate the influence of the surface modifiers’ application on their working surface, which usually results in the improvement of the parameters such as sensitivity and selectivity and allows us to obtain lower detection limits in comparison with the bare electrode. The most popular modifiers include conducting polymers, metallic and non-metallic nanoparticles, carbon nanomaterials, biological compounds or silica-based materials.
A wide variety of working electrodes based on mercury, glassy carbon, noble metals, carbon paste, pyrolytic graphite, molecularly imprinted polymers, carbon nanotubes, nanocomposites, etc., have been developed for the highly sensitive determination of hormones and steroids since 2000. Most of the methods reported so far required immunosensors, which lower the limits of detection in comparison to the classic constructions, which is the impact of the specific bond between the antibody and the analyte, which is strengthened by the catalytic properties of the nanoparticles used in the sensing component of immunosensors.
3. Electrochemical Measurements of Hormones and Steroids
3.1. Pituitary Gland Hormones
The pituitary gland is a small, endocrine gland placed at the base of the mammal brain. It is responsible for the secretion of hormones that affects bone growth, blood pressure, energy management and functions of the sex organs. The pituitary gland also controls the thyroid gland’s work and metabolism and affects the reproduction process, levels of electrolytes and temperature regulation [
23,
24].
Human growth hormone (hGH) is a peptide hormone stored and secreted by the somatotropic cells and is based in the anterior pituitary gland. HGH is one of the crucial factors responsible for human development. It also stimulates the production of insulin-like growth factor 1 (IGF-1) and increases the concentration of glucose and free fatty acids. Its recombinant form—somatotropin—is available by prescription and used in the treatment of growth hormone deficiency [
25,
26,
27]. When considering the electrochemical possibilities of hGH determination, there are not many papers with such assays. The lowest obtained detection limit was expressed in the picogram units, which allows for performing analyses on blood or serum samples. The working electrodes used for the high sensitive determination of hGH comprised either specific hGH antibodies or the receptor membrane was constructed via direct electro-polymerization of aniline on the surface of electrodes in the presence of hGH as a template (
Table 1). Additionally, it was proven that, based on the voltammetric measurements, it is possible to determine hGH in spiked human serum and plasma and in saliva samples.
Adrenocorticotropic hormone (ACTH) is a peptide hormone of the pituitary gland, classified as a tropic hormone. It stimulates the adrenal cortex to secrete corticosteroids, mineralocorticoids and androgens. Increasing the concentration of ACTH in the blood is one of the body’s first responses to stress. This hormone indirectly influences the body’s protein, carbohydrate and mineral metabolism and also inhibits cell proliferation. Moreover, it has anti-inflammatory and antiallergic properties. Its synthetic form is used to diagnose or exclude primary and secondary adrenal insufficiency, Addison’s disease, and related conditions [
28,
29]. In the current literature, only two voltammetric assays of ACTH determination are reported. In both cases, the screen-printed carbon electrode was modified with immobilized anti-ACTH antibodies. The lowest limit of detection obtained using such prepared working electrodes was equal to 18 ng/L (
Table 1), and the assays were applied for sensitive ACTH determination in human serum samples.
Prolactin (PRL) is a protein hormone best known as a stimulant of breast milk production in mammals. It is secreted in response to physical activity, eating, nursing or mating. Its secretion is also inhibited in some cells in the course of certain cancers and in the endometrium. Excess prolactin (hyperprolactinaemia), often caused by pituitary adenomas, may be responsible for infertility and amenorrhea-galactorrhea syndrome [
30,
31,
32]. For the voltammetric detection of prolactin, mainly the differential pulse technique has been involved for a highly sensitive prolactin determination. Considering the type of sensors being used as working electrodes, the biggest group comprises immunosensors with specific anti-PRL antibodies placed in the receptor layer. The detection limit obtained with this type of sensor is about 4 pg/mL. Apart from the immunosensors, the hanging mercury drop electrode and electrodes decorated with gold nanoparticles, conducting polymers or carbon nanomaterials were used for a PRL determination as well, with good sensitivity and detection limits occurring as low as 38.9 pg/ms (
Table 1). Prolactin was determined using voltammetric assays in the samples, such as human urine, saliva, serum and different pharmaceutical formulations.
Thyroid-stimulating hormone (TSH) is a glycoprotein hormone produced by the pituitary gland and comprises alpha and beta subunits. In humans, it causes an increase in the mass of the thyroid gland, an increase in blood flow through this organ and an increase in the production and secretion of thyroid hormones: thyroxine and triiodothyronine. The regulation of thyrotropin secretion is based on the principle of negative feedback with thyroid hormones; secretion is also inhibited by somatostatin and dopamine and stimulated by thyreoliberin and stress or cold [
33,
34,
35]. Only a few voltammetric assays of TSH determination have been reported sincse 2000. Most of them use specific anti-TSH antibodies immobilized on the surface of the working glassy carbon or gold electrode. Such a modification allows for achieving a detection limit as low as 0.005 µIU mL
−1, and the proposed biosensors were successfully applied for a highly sensitive TSH determination in serum samples, which confirms the usefulness of the developed method (
Table 1). TSH was measured electrochemically in human serum samples and in pharmaceutical formulations (tablets).
Follicle-stimulating hormone (FSH) is a glycoprotein hormone comprising 207 amino acids arranged into two subunits. It is secreted by the anterior pituitary gland in both women and men. Acting together with the luteinizing hormone in women, it stimulates the maturation of ovarian follicles and the production of estrogens, and in men, it controls the function of the testicles. In women, FSH stimulates follicular maturation and the secretion of oestrogens from the follicular cells of the ovaries. It also increases the activity of the aromatase enzyme. In men, it causes enlargement of the seminal tubes, stimulates spermatogenesis and increases the production of the androgen-binding protein necessary for the proper functioning of testosterone. During menopause, due to the extinction of the hormonal activity of the gonads, both women and men have elevated levels of FSH in the blood and, and thus, in the urine. Recent research indicates that follicle-stimulating hormone receptors are found in the cells of many types of cancer. This may be important in the diagnosis of neoplasms and allow the creation of drugs targeting cells with FSH receptors [
36,
37,
38,
39,
40]. Considering the current electrochemical methods of FSH determination, only a few assays have been reported since 2000. Two of them are based on the use of the FSH-specific antibodies entrapped in the modifier layer with reduced graphene oxide, thionine, gold nanoparticles and multi-walled carbon nanotubes. The lowest obtained detection limit obtained with the use of such immunosensors was about 0.05 mIU/mL. In another reported voltammetric assay, the molecularly imprinted polymer, designed in the presence of the FSH particle, was used as a receptor layer along with nickel–cobalt oxide and reduced graphene oxide. The FSH detection limit, in this case, was equal to 0.1 pM (
Table 1). The FSH hormone was also measured in samples such as whole human blood and human serum using voltammetric assays.
In
Table 1, the electrochemical methods of hGH, ACTH, prolactin, TSH and FSH determination are compared.
Table 1.
Electrochemical methods of pituitary gland hormones determination.
Table 1.
Electrochemical methods of pituitary gland hormones determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit | Linear Range | Source |
|---|
| Human Growth Hormone | DPV | SPCE | AuNP/PEDOT/CNT/anti-hGH | 0.1 M PBS pH 7.4 | n/i | 4.4 pg mL−1 | 0.005–1000 ng mL−1 | [41] |
| SWV | GCE | MIP/Fe3O4 | 0.2 M PBS pH 6.92 | n/i | 0.6 × 10−10 g cm−3 | 1.0 × 10−10–1.0 × 10−7 g cm−3 | [42] |
| SWV | SPAuE | TsMBs–mAbhGH–hGH–pAbhGH– anti-IgG–AP | 0.1 M Trizma + 1 mM MgCl2 buffer pH 9.0 | 120 | 0.005 ng mL−1 | 0.01–100 ng mL−1 | [43] |
| Adrenocorticotropic hormone (ACTH) | DPV | SPCE | Strept-AP/Biotin-ACTH/anti-ACTH/APBA | n/i | n/i | 40 pg L−1 | 5.0 × 10−3 –0.1 ng mL−1 | [44] |
| DPV | SPCE | Strept-AP/Biotin-ACTH/anti-ACTH/APBA | n/i | n/i | 18 pg L−1 | 0.025–1.0 pg mL−1 | [45] |
| Prolactin | DPV | SPCE | Anti-PRL–streptavidin-MBs (magnetic beads) | n/i | n/i | 3.7 ng mL−1 | 10–2000 ng mL−1 | [46] |
| DPV | GCE | GPPD-labeled HRP-anti-PRL | ABS pH 5.0 | n/i | 0.1 ng mL−1 | 0.5–180 ng mL−1 | [47] |
| DPV | CPE | HRP-Ab/PRL/Ab/TGA/nano-Au/CILE | 0.1 M PBS pH 7.0 | 400 | 12.5 mIU L−1 | 25.0–2000.0 mIU L−1 | [48] |
| DPV | GCE | AP-anti-PRL–PRL-pPPA/MWCNTs | 0.1 M PBS pH 7.2 | n/i | 3 pg mL−1 | 10−2–104 ng mL−1 | [49] |
| DPV | GCE | Graphene/AuNPs | 0.01 M PBS pH 7.4 | n/i | 38.9 pg mL−1 | 100 pg mL−1–50 ng mL−1 | [50] |
| DPV | GCE | Anti-PRL/pPPA/MWCNTs | PBS pH 7.4 | n/i | 4 pg mL−1 | 10−2–104 ng mL−1 | [51] |
| DPV | CNT/SPCEs | AuNPs/PEDOT | 0.1 M PBS pH 7.4 | n/i | 0.22 pg mL−1 | 0.1–150 ng mL−1 | [41] |
| SWV | HMDE | - | phosphate buffer pH 6.5 | 90 | n/i | 0.089–16.36 ng mL−1 | [52] |
| DPV | GCE | Graphene/SWCNT/AuNPs/CT | 5.0 mL DEA + 0.75 mg mL−1 α-NP | n/i | 47 pg mL−1 | 50–3200 pg mL−1 | [53] |
| TSH | SWV | GCE | azo compound film | 0.1 M phosphate buffer pH 8.0 | n/i | 0.04 μIU mL−1 | 0.2–20.0 μIU mL−1 | [54] |
| DPV | Au | anti-TSH/AuNP-GO | 0.1 M ABS + 6 mM H2O2 pH 6.0 | n/i | 0.005 µIU mL−1 | 0.01–20 µIU mL−1 | [55] |
| DPV | Au | GPG-labeled HRP-Ab2 | 0.1 M ABS + 6 mM H2O2 pH 5.0 | n/i | 0.005 µIU mL−1 | 0.01–20 µIU mL−1 | [56] |
| DPV | CPE | AuNPs/anti-TSH | 0.1 M PBS pH 7.0 + 5.0 mM OAP + 1 mM H2O2 | n/i | 0.1 ng mL−1 | 0.2–90.0 ng mL−1 | [57] |
| FSH | DPV | SPE | r-GO/thionine Thi/Au NPs/anti- FSH | 0.1 M PBS | n/i | 1 mIU mL−1 | 1–100 mIU mL−1 | [58] |
| DPV | SPE | r-GO/MWCNTs/ Thi/Au NPs/anti- FSH | 0.1 M PBS pH 7.4 | 1500 | 0.05 mIU mL−1 | 1–250 mIU mL−1 | [59] |
| LSV | indium tin oxide (ITO) | FSH-MIP/NiCo2O4/rGO/ | 0.1 M PBS pH 8.5 | n/i | 0.1 × 10−12 M | 0.1 × 10−12–1 × 10−6 M | [60] |
3.2. Adrenal Gland Hormones
The adrenal gland is a paired, small endocrine gland located retroperitoneally at the upper pole of the kidney. The adrenal gland comprises cortical and spinal parts, which differ in structure and function. The cortex is the main mass of the gland (80% to 90% of the entire adrenal gland). The cortex produces steroids, which can be divided into three subgroups: mineralocorticosteroids, of which aldosterone has the strongest effect; glucocorticosteroids, the most important of which is cortisol and sex hormones (androgens). The adrenal medulla produces catecholamines. It constantly secretes small amounts of adrenaline into the blood, while all emotional states suddenly release large amounts of it into the blood. Small amounts of norepinephrine are also produced in the adrenal medulla. Hormones secreted by the adrenal cortex maintain the body’s water and mineral balance (aldosterone), help in situations of long-term stress and increase blood glucose levels [
12,
13,
61].
Adrenaline (epinephrine) is an animal hormone and a catecholamine neurotransmitter produced by the endocrine glands of the nerve crest and is secreted at the end of sympathetic nervous system fibers. The term adrenaline is used interchangeably with epinephrine, as both terms refer to exactly the same substance. Adrenaline is also known as the 3xF hormone—the hormone of fear, fight and flight. Adrenaline plays a decisive role in the stress mechanism, the rapid response of the human body and vertebrate animals to a threat, and is manifested by an accelerated heartbeat, increase in blood pressure, bronchial and laryngeal expansion, dilatation of the pupils, etc. In addition, adrenaline regulates the level of glucose in the blood by increasing the breakdown of glycogen into glucose in the liver (glycogenolysis). Adrenaline is also found in plants. Its pharmacological significance is limited due to the low durability of the hormone. Adrenaline is used in cases of cardiac arrest regardless of the mechanism. It has the effect of stimulating the contractility of the heart muscle, improving the conduction of stimuli in the heart, as well as improving the effectiveness of electrical defibrillation. Adrenaline, given in the case of anaphylaxis, quickly relieves the symptoms of an acute allergic reaction. It causes the blood vessels to contract rapidly, which raises blood pressure. The smooth muscles of the bronchi, larynx and throat also relax, which makes breathing easier. Epinephrine also reduces swelling around the mouth and face. Adrenaline is the first-line drug of choice for the treatment of anaphylaxis and the second-line drug for the treatment of cardiogenic shock. It is also used in cases of bronchial asthma attacks and acute allergic reactions when the administration of other drugs does not help and the disease becomes life-threatening. Adrenaline is also used in laryngology and dentistry. It is sometimes used, for example, to reduce bleeding, as it strongly narrows blood vessels [
62,
63,
64,
65].
Noradrenaline (norepinephrine) is an organic chemical compound from the group of catecholamines, classified both as a neurotransmitter and hormone, and is secreted in the adrenal medulla and locus coeruleus, usually together with adrenaline. Norepinephrine mobilizes the brain and body to act. Its secretion is lowest during sleep and increases by 180% when awake. It achieves much higher levels in stressful and dangerous situations (fight-or-flight response). In the brain, norepinephrine increases agitation and alertness, supports wakefulness, enhances remembering and recalling and enables concentration, as well as increases anxiety and fear, the excess of which leads to anxiety disorders. In the rest of the body, norepinephrine speeds up the heart rate and increases blood pressure, releases stored glucose, increases blood flow to the skeletal muscles, reduces blood flow to the digestive system, and inhibits bladder emptying and motor activity in the gastrointestinal tract. Norepinephrine, as medicine, is injected in cases of critically low blood pressure [
12,
13,
66,
67].
In the current literature, there are numerous reports of adrenaline and noradrenaline determination by using popular voltammetric techniques—cyclic voltammetry, differential pulse voltammetry and square-wave voltammetry. Glassy carbon electrodes, along with the carbon paste electrode, were the most popular working electrodes used in the measurements. Almost in each case, they were modified with different materials in order to achieve higher sensitivity and lower limits of detection. The lowest obtained LOD values were equal to 8.7 × 10
−10 M and 8.7 × 10
−10 M for adrenaline and norepinephrine, respectively (
Table 2). The voltammetric assays for adrenaline determination were tested on real sample analyses, such as body fluids (serum and urine) and pharmaceutical products in the form of injections.
Cortisol (hydrocortisone) is a natural steroid hormone produced by the band layer of the adrenal cortex. It is the main representative of glucocorticosteroids. It has a wide impact on metabolism and is sometimes called the stress hormone, along with adrenaline. It has an anti-inflammatory effect and retains salt in the body. Cortisol increases blood glucose levels, which is indicated in response to stress. Cortisol also releases amino acids from peripheral tissues and inhibits the rate of their absorption by skeletal muscles, accelerates gluconeogenesis, and finally accelerates the breakdown of fatty acids into ketone bodies. Chronic excess of cortisol in the blood leads to the characteristic displacement of adipose tissue deposits (buffalo neck, full moon face, abdominal obesity, lean limbs), thinning of the skin, the formation of characteristic pink stretch marks, acne and insulin resistance, which is a picture of Cushing’s syndrome [
68,
69,
70,
71]. The cortisol electrochemical detection assays, since 2000, were mostly performed on solid electrodes, and glassy carbon and gold electrode in particular. In some reported works, immunosensors with anti-cortisol antibodies were used, which allows for obtaining the lowest detection limit, which was equal to 0.64 pM. In such immunosensors, besides the antibody component of the modifier layer, other components, such as conducting polymers or metal nanoparticles, are used to provide the sensor’s stability and even enhance the electrochemical reaction of the analyte. Cortisol could also be measured using a refreshable mercury film electrode with a low detection limit of 4.8 nM (
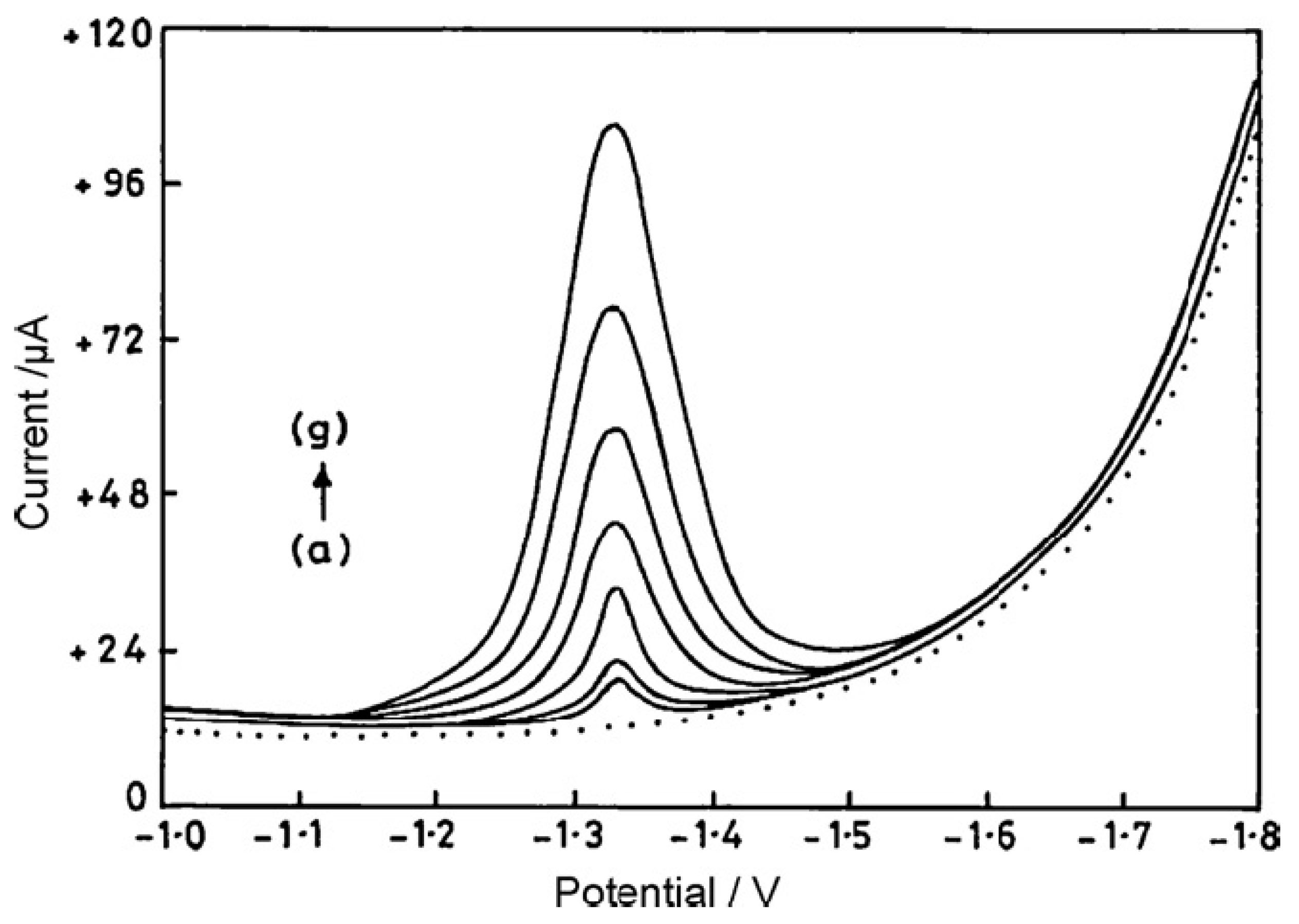
Table 2). Cortisol determination was also performed in the complex matrices, such as human serum and plasma, whole blood and saliva. Additionally, pharmaceutical formulations, such as tablets, creams and ointments, were tested for the possibility of hydrocortisone measurements with success. Samples of the hydrocortisone calibration graphs are presented in
Figure 1 [
72].
In
Table 2, the electrochemical methods of adrenaline, norepinephrine and cortisol determination are compared.
Figure 1.
Osteryoung square-wave voltammograms recorded for (a) PBS (background) at the bare EPPGE (· · ·) and (b) increasing concentration of HC at the bare EPPGE electrode (—). Curves were recorded at (a) 100 nM, (b) 250 nM, (c) 500 nM, (d) 750 nM, (e) 1000 nM, (f) 1500 nM and (g) 2000 nM concentration in PBS of pH 7.2. Reprinted from
A comparison of edge- and basal-plane pyrolytic graphite electrodes towards the sensitive determination of hydrocortisone, Talanta, Vol 83, Rajendra N. Goyal, Sanghamitra Chatterjee, Anoop Raj Singh Rana, Pages 149–155, 2011, with permission from Elsevier [
72].
Figure 1.
Osteryoung square-wave voltammograms recorded for (a) PBS (background) at the bare EPPGE (· · ·) and (b) increasing concentration of HC at the bare EPPGE electrode (—). Curves were recorded at (a) 100 nM, (b) 250 nM, (c) 500 nM, (d) 750 nM, (e) 1000 nM, (f) 1500 nM and (g) 2000 nM concentration in PBS of pH 7.2. Reprinted from
A comparison of edge- and basal-plane pyrolytic graphite electrodes towards the sensitive determination of hydrocortisone, Talanta, Vol 83, Rajendra N. Goyal, Sanghamitra Chatterjee, Anoop Raj Singh Rana, Pages 149–155, 2011, with permission from Elsevier [
72].
Table 2.
Electrochemical methods of adrenal gland hormones determination.
Table 2.
Electrochemical methods of adrenal gland hormones determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit, M | Linear Range, M | Source |
|---|
| Adrenaline | SWV | GC | poly(1-methylpyrrole) | 0.1 M PBS pH 4.5 | 0.1 | 8.7 × 10−10 | 3.0 × 10−9–2.0 × 10−8 | [73] |
| DPV | PIGE | PR | 0.1 M PBS pH 7.0 | n/i | 8.0 × 10−7 | 3.0 × 10−6–90.0 × 10−6 | [74] |
| SWV | CPE | CuFe2O4/ILs | 0.1 M PBS pH 7.4 | n/i | 0.07 × 10−6 | 0.1 × 10−6–400 × 10−6 | [75] |
| SWV | CPE | PtNP/IL/LAC | 0.1 M PBS pH 6.5 | n/i | 2.9 × 10−7 | 10.0 × 10−7–2.1 × 10−4 | [76] |
| DPV | CPE | 2,2’-[1,2-Ethanediylbis(nitriloethylidyne)]-bishydroquinone | 0.1 M PBS pH 7.0 | n/i | 2.2 × 10−7 | 7.0 × 10−7–1.2 × 10−3 | [77] |
| Amperometry | CPE | GP/mineral oil/polyphenol oxidase | 0.1 M acetate buffer pH 4.4 | 0 | 1.5 × 10−5 | 5.0 × 10−5–3.5 × 10−4 | [78] |
| SWV | CPE | GP–Nujol–peroxidase—CHIT | 0.1 M PBS pH 7.0 | n/i | 4.0 × 10−7 | 2.0 × 10−6–1.1 × 10−4 | [79] |
| SWV | CPE | GP–Nujol–BMIPF6–peroxidase—CHIT | 0.1 M PBS pH 7.0 | n/i | 2.3 × 10−7 | 9.9 × 10−7–1.2 × 10−4 | [79] |
| CV | CPE | GP–binder–poly(isonicotinic acid) | 0.1 M PBS pH 5.3 | n/i | 1.0 × 10−6 | 5.0 × 10−6–1.0 × 10−4 | [80] |
| DPV | GC | Poly (eriochrome Black T) | 0.05 M PBS pH 3.5 | n/i | 3.0 × 10−7 | 2.5 × 10−6–5.1 × 10−5 | [81] |
| DPV | GC | 5,5-ditetradecyl-2-(2-trimethyl-ammonioethyl)-1,3-dioxane bromide | 0.1 M PBS pH 6.0 | n/i | 1.0 × 10−8 | 1.0 × 10−8 –1.0 × 10−4 | [82] |
| DPV | Au | Meso-2,3-dimercaptosuccinic | 0.1 M PBS pH 7.7 | n/i | 5.3 × 10−8 | 4.0 × 10−4–4.0 × 10−3 | [83] |
| CV | SPE | - | 0.1 M H2SO4 + 0.01 M KCl pH 1 | 600 | 1.3 × 10−7 | 2.9 × 10−7–1.0 × 10−4 | [84] |
| CV | GC | Caffeic acid | 0.1 M PBS pH 7.7 | n/i | 2.0 × 10−7 | 2.0 × 10−6–8.0 × 10−5 | [85] |
| CV | AuE | AuNP/DTT | 0.1 M PBS pH 7.0 | n/i | 6.0× 10−8 | 1.0 × 10−7–8.0 × 10−4 | [86] |
| SWV | AuE | Triazole | 0.1 M B-R buffer pH 4.4 | 180 | 1.0 × 10−8 | 1.0 × 10−7–1.0 × 10−5 | [87] |
| DPV | CPE | Laccase-peroxidase | 0.1 M PBS pH 6.0 | 60 | 2.5 × 10−8 | 6.1 × 10−6-1.0 × 10−4 | [88] |
| DPV | GCE | HT/MWCNT | 0.1 M PBS pH 7.0 | n/i | 0.024 × 10−6 | 0.2 × 10−6–319.7 × 10−6 | [89] |
| SWV | BDDFE | - | 0.5 M HClO4 | n/i | 0.21 × 10−6 | 0.7 × 10−6–60 × 10−6 | [90] |
| DPV | CPE | FePC/MWCNT | PBS pH 7.4 | n/i | 2.1 × 10−7 | - | [91] |
| DPV | CPE | IL/CNT | PBS pH 7.0 | n/i | 0.09 × 10−6 | 0.3 × 10−6–450 × 10−6 | [92] |
| DPV | GCE | SWCNT/CT/IL | PBS pH 7.0 | 60 | 0.09 × 10−6 | 1 × 10−6–580 × 10−6 | [93] |
| DPV | GCE | PP/MWCNT | PBS pH 6.0 | 60 | 0.04 × 10−6 | 0.1×10−6–8 × 10−6 | [94] |
| DPV | AuE | PMP | PBS pH 7.2 | n/i | 0.1 × 10−6 | - | [95] |
| DPV | GCE | Au/PP | 0.1 M PBS pH 7.0 | 240 | 0.03 × 10−6 | 0.3 × 10−6–21 × 10−6 | [96] |
| DPV | GCE | PT | PBS pH 7.4 | n/i | 0.3 × 10−6 | 2 × 10−6–600 × 10−6 | [97] |
| DPV | GCE | PMP | PBS pH 4.0 | n/i | 0.17 × 10−6 | 0.75 × 10−6–200 × 10−6 | [98] |
| DPV | GCE | Pt-AuNP | PBS pH 7.0 | n/i | 57 × 10−6 | 63–400 × 10−6 | [99] |
| DPV | CPE | acetylene black | 0.5 M H2SO4 + SDS | 70 | 1.0 × 10−8 | 5.0 × 10−8–7.0 × 10−6 | [100] |
| DPV | GCE | IMWCNT | 0.15 M PBS pH 7.0 | n/i | 0.96 × 10−6 | 1.3 × 10−6–833.3 × 10−6 | [101] |
| DPV | MIP | - | 0.1 M K4Fe(CN)6 + 0.1 M KNO3 | n/i | 2 × 10−9 | 1 × 10−9 –100 × 10−9 | [102] |
| DPV | GCE | RuON | 0.1 M PBS pH 7.0 | n/i | 0.45 × 10−6 | 2.0–65.5 × 10−6 | [103] |
| DPV | GCE | pEDOT-CH2OH-MIP/MXene/CNHs | 0.1 M phosphate buffer 7.4 | 420 | 0.3 × 10−9 | 1 × 10−9–60 × 10−6 | [104] |
| DPV | CNTPE | poly(phenylmethanoic acid) PPMAM | 0.2 M PBS pH 7.0 | 60 | 4.5 × 10−8 | 10–110 × 10−6 | [105] |
| DPV | GCE | Pd/BiVO4 | PBS | n/i | 0.154 × 10−6 | 0.9–27.5 × 10−6 | [106] |
| SWV | GCE | phosphorus-doped microporous carbon spheroidal structures (P-MCSs) | 0.1 M PB pH 7.0 | n/i | 2 × 10−9 | 0.01–2 × 10−6 | [107] |
| DPV | CPE | sodium alpha-olefin sulfonate (SAOS) | 0.2 M PBS pH 7.4 | n/i | 0.14 × 10−6 | 10–70 × 10−6 | [108] |
| DPV | CPE | triiodide ions immobilized in an anion-exchange resin | PBS pH 6.0 | n/i | 3.9 × 10−6 | 2.0 × 10−5–3.1 × 10−4 | [109] |
| DPV | Au | ME/Au SAMs | 0.04 M B-R buffer pH 4.0 | 250 | 3.3 × 10−8 | 1.0 × 10−7–1.0 × 10−4 | [110] |
| Norepinephrine | SWV | GCE | TAPP | PBS pH 7.4 | n/i | - | 1.0 × 10−6–5.0 × 10−5 | [111] |
| SWV | Pd | graphene | PBS pH 7.2 | n/i | 67.4 × 10−9 | 0.0005–0.5 × 10−3 | [112] |
| CV | GCE | graphene | PBS pH 7.0 | 120 | 400 × 10−9 | 6.00 × 10−7–1.20 × 10−4 | [113] |
| CV | GCE | graphene | PBS pH 4.0 | n/i | 100 × 10−9 | 0.6–1000 × 10−6 | [114] |
| DPV | GCE | PEDOPA-NFs | 0.1 M PBS pH 7.4 | n/i | 50 × 10−9 | 0.3–10 × 10−6 | [115] |
| DPV | GCE | Polyisonicotinic acid | PBS pH 5.6 | n/i | 6.0 × 10−9 | 4.0 × 10−7–2.0 × 10−4 | [116] |
| CV | GCE | SWCNT | B–R buffer pH 5.72 | n/i | 6000 × 10−9 | 1.0 × 10−5–1.1 × 10−3 | [117] |
| DPV | GCE | C-Ni | PBS pH 7.0 | 120 | 60 × 10−9 | 2.0 × 10−7–8.0 × 10−5 | [118] |
| CV | Graphite | β-CD/CNT | 0.1 M PBS pH 6.0 | n/i | 5.0 × 10−7 | 1.0 × 10−6–3.0 × 10−4 | [119] |
| CV | Au | TLA | PBS pH 5.91 | 2 | 2.0 × 10−6 | 4.0 × 10−5–2.0 × 10−3 | [120] |
| SWV | EPPGE | MWNT | PBS pH 7.2 | n/i | 0.90 × 10−10 | 0.5–100 × 10−9 | [121] |
| DPV | CPE | ZrO2NPs | 0.1 M PBS pH 7.0 | n/i | 8.9 × 10−8 | 1.0 × 10−7–2.0 × 10−3 | [122] |
| CV | GCE | Calix[4]arene crown-4 | 0.1 M PB pH 6.0 | n/i | 2.8 × 10−7 | 5.5 × 10−7–2.3 × 10−4 | [123] |
| CV | Au | C60-[dimethyl-(β-cyclode×trin)]2/Nafion | 0.1 M PB pH 6.0 | n/i | 8.0 × 10−6 | 5.0 × 10−5–5.8 × 10−4 | [124] |
| SWV | GCE | Poly2,4,6-trimethylpyridine | PBS pH 7.4 | n/i | 8.0 × 10−6 | 5.0 × 10−3–1.0 × 10−1 | [125] |
| CV | GCE | Poly(cresol red) | 0.1 M PBS pH 3.0 | n/i | 2.0 × 10−7 | 3.0 × 10−6–3.0 × 10−5 | [126] |
| CV | GCE | Nickel(II) complex | 0.1 M PBS pH 7.4 | n/i | 7.7 × 10−9 | 1.0 × 10−7–1.0 × 10−5 | [127] |
| DPV | GCE | Au NPs | PBS pH 7.0 | n/i | 2.0 × 10−8 | 5.0 × 10−7–8.0 × 10−5 | [128] |
| DPV | TiO2 NPs—CPE | 2,2’-[1,2-butanediylbis(nitriloethylidyne)]-bishydroquinone | pH 8.0 | n/i | 5.0 × 10−7 | 4.0 × 10−6–1.1 × 10−3 | [129] |
| CPV | SPE | PAA-MWCNTs | 0.1 M PBS pH 7.5 | 1500 | 1.3 × 10−7 | 0–1.0 × 10−5 | [130] |
| SWV | ITO | AuNPs | PBS pH 7.2 | n/i | 87 × 10−9 | 100 × 10−9–25 × 10−6 | [131] |
| DPV | CPE | MCM-41 | PBS pH 7.0 | n/i | 4.0 × 10−8 | 7.0 × 10−8–2.0 × 10−3 | [132] |
| DPV | CPE | Molybdenum (VI) complex | PBS pH 7.0 | n/i | 4.3 × 10−8 | 8.0 × 10−8–7.0 × 10−4 | [133] |
| DPV | GCE | Hematoxylin | 0.15 M PBS pH 7.0 | n/i | 1.4 × 10−7 | 5.0 × 10−7–2.7 × 10−4 | [134] |
| DPV | CPE | 3,4-dihydroxybenzaldehyde-2,4-dinitrophenylhydrazone | 0.1 M PBS pH 7.0 | n/i | 7.7 × 10−8 | 1.0 × 10−7–8.0 × 10−4 | [135] |
| DPV | CPE | Ferrocenemonocarboxylic acid (FMC) | 0.1 M phosphate buffer pH 7.0 | n/i | 1.6 × 10−7 | 5.2 × 10−7–5.3 × 10−4 | [136] |
| DPV | CPE | Chloranile | 0.1 M PBS pH 7.0 | n/i | 1.12 × 10−8 | 3.0 × 10−8 –5.0 × 10−4 | [137] |
| DPV | GCE | Polycalconcarboxylic acid | PBS pH 6.0 | n/i | 0.1 × 10−6 | 0.63–62.5 × 10−6 | [138] |
| DPV | GCE | Au-NPs/poly(2-amino-2-hydroxymethyl-propane-1,3-diol) | PBS pH 3.0 | n/i | 0.07 × 10−6 | 1.3–230.1 × 10−6 | [139] |
| CV | GCE | MWCNT/FCo98 (cobalt ferrite nanoparticles) | 0.1 M PBS pH 7.0 | n/i | 0.76 × 10−6 | 0.16–1.91 × 10−3 | [140] |
| CV | CPE | poly (rhodamine B) | 0.2 M PBS pH 7.4 | n/i | 1.8 × 10−6 | 20–90 × 10−6 | [141] |
| SWV | GCE | GQDs/AuNPs (quantum dots) | PBS pH 7.0 | 30 | 0.15 × 10−6 | 0.5–7.5 × 10−6 | [142] |
| DPV | Au | Cys/CDs/Tyr | 0.1 M PBS pH 7.0 | n/i | 196 × 10−9 | 1–200 × 10−6 | [143] |
| SWV | GCE | P(L-Arg)/ERGO | PBS pH 7.0 | n/i | 4.22 × 10−8 | 2 × 10−5–8 × 10−7 | [144] |
| DPV | CPE | GQDs/IL | 0.1 M PBS pH 7.0 | n/i | 0.06 × 10−6 | 0.2–400 × 10−6 | [145] |
| SWV | PGE | - | 0.1 M PBS pH 7.4 | n/i | 9.92 × 107 | 2.5 × 10−4–2.5 × 10−6 | [146] |
| CV | CPE | MnCr2O4 | 0.2 M PBS pH 7.4 | n/i | 0.034 × 10−6 | 0.3 × 10−6–4.5 × 10−6 | [147] |
| DPV | CPE | MWCNTs/CILE | 0.1 M PBS pH 7.0 | n/i | 0.09 × 10−6 | 0.3–450 × 10−6 | [148] |
| SWV | CPE | 5-mino-3′,4′-dimethyl-biphenyl-2-ol | 0.1 M PBS pH 7.0 | n/i | 5.9 × 10−7 | 1.2 × 10−6–9.0 × 10−4 | [149] |
| DPV | CPE | poly(glutamic acid) | 0.2 M PBS pH 7.4 | n/i | 0.43 × 10−6 | n/i | [150] |
| DPV | CPE | CNT + ferrocene (FC) | 0.1 M PBS pH 7.0 | n/i | 0.21 × 10−6 | 0.47–500.0 × 10−6 | [151] |
| CV | CPE | Tx-100 | 0.1 M PBS pH 7.0 | n/i | 5.0 × 10−6 | 0.5 × 10−4–2.0 × 10−4 | [152] |
| SWV | CPE | MWNTs/MBIDZCl | 0.1 M PBS pH 7.0 | n/i | 0.08 × 10−6 | 0.2–500 × 10−6 | [153] |
| Cortisol (hydrocortisone) | DPV | Hg(Ag)FE | - | Acetate buffer pH 4.2 | 30 | 4.8 × 10−9 | 0.02 × 10−6–1.2 × 10−6 | [154] |
| SWV | EPPG | - | PBS pH 7.2 | - | 88 × 10−9 | 100–2000 × 10−9 | [72] |
| SWV | SPE | mAbC | PBS pH 7.4 | - | 1.7 × 10−9 | 1.7 × 10−9–1.2 × 10−7 | [155] |
| CV | Au | BSA/C-Mab/PPAuNP | PBS pH 7.0 | - | 1 × 10−12 | 1 × 10−12–100 × 10−9 | [156] |
| CV | Au | EA/anti-AbC/DTSP | 0.05 M PBS pH 7.4 | n/i | 2.8 × 10−11 | 10 × 10−12–100 × 10−9 | [157] |
| DPV | ITo | AbC/NiO | PBS pH 7.0 | n/i | 0.89 × 10−12 | 2.8 × 10−12–27.5 × 10−3 | [158] |
| amperometry | Au | AbC | 0.01 M PBS pH 7.5 + glucose | n/i | 2.8 × 10−9 | 3.4 × 10−9–5.5 × 10−7 | [159] |
| amperometry | SPE | RGO/ AbC | PBS pH 7.4 | n/i | 2.8 × 10−10 | 2.8 × 10−10–5.5 × 10−7 | [160] |
| CV | Au | ZnO/AbC | 0.01 M PBS pH 7.4 | n/i | 1 × 10−12 | 1 × 10−12–100 × 10−9 | [161] |
| DPV | GCE | HRP-Strept-Biotin-AbC/AuNPs/MrGO/Nafion | 0.1 M pH 7.0 PBS + 2 mM o-PD + 4 mM H2O2 | n/i | 1.4 × 10−10 | 2.8 × 10−10–2.8 × 10−6 | [162] |
| DPV | CPE | β-cyclodextrin | 0.04 M B-R pH 3.0 | 150 | 3.7 × 10−7 | 4.2 × 10−7–2.5 × 10−5 | [163] |
| DPV | SPE | AbC/ protein A-magnetic beads | 0.1 M Trizma + 1 mM MgCl2 pH 9.0 | n/i | 9.7 × 10−12 | 1.4 × 10−11–4.1 × 10−7 | [164] |
| SWV | Au | AuNPs/AbC | 0.02 mM PBS pH 7.4 | n/i | 4.4 × 10−11 | 0.14 × 10−9–7 × 10−9 | [165] |
| CV | IDE/Cr/Si | AbC /DTSP-SAM | PBS pH 7.4 | n/i | 2.8 × 10−11 | 2.8 × 10−11–2.8 × 10−8 | [166] |
| CV | SPE | MIP-PPy | 0.01 M PBS pH 7.4 | n/i | 1 × 10−12 | 1 × 10−12–10 × 10−6 | [167] |
| SWV | CPE | AuNPs/MWCNT/IL | 0.1 M Trizma buffer pH 9.0 | n/i | 2.5 × 10−7 | 2.8 × 10−7–3.3 × 10−4 | [53] |
| DPV | GCE | CoO NPs/Naf | 0.1 M NaOH pH 12.0 | n/i | 0.49 × 10−9 | 0.001–9.0 × 10−6 | [168] |
| DPV | SPCE | cortisol-AP/anti-cortisol/APBA | n/i | n/i | 1.0 × 10−10 | 2.8 × 10−10–1.4 × 10−6 | [44] |
| DPV | GCE | PDA-ERGO polydopamine/rGO | 0.1 M acetate buffer pH 5.2 | n/i | 0.006 × 10−9 | 0.001–50 × 10−6 | [169] |
| CV | SPCE | MIP | K3[Fe(CN)6]/K4[Fe(CN)6] + 0.1 M KCl | n/i | 1.2 × 10−9 | 1.3–20 × 10−9 | [170] |
| DPV | Nano-porous GCE | - | 0.1 M PBS pH 2 | n/i | 30 × 10−9 | 0.1–42 × 10−6 | [171] |
| CV | Au | BSA/Anti-Cab/Ag@AgO–PANI | PBS pH 7.0 + 0.9% NaCl | n/i | 0.64 × 10−12 | 1 × 10−12–1 × 10−6 | [172] |
| CV | Pt | Anti-Cab | PBS | n/i | 2.8 × 10−9 | 2.8 × 10−9–2.8 × 10−8 | [173] |
| CV | Si | rGO/Au IDA | 0.05 M bicarbonate–carbonate buffer pH 9.6 | n/i | 2.8 × 10−9 | 0–500 × 10−6 | [174] |
3.3. Pancreatic Hormones
The pancreas is a glandular organ of vertebrates, while the islet pancreas also occurs in other chordates. It takes various forms in different taxa. It can be a compact organ, or it can be scattered among other tissues. It arises from three buds in the intestinal epithelium, one of which disappears in mammals. It consists of two types of tissue: follicular and insular. Pancreatic follicles are exocrine glands that produce many digestive enzymes and break down different types of food. They combine with the secretions of the walls of the exit ducts leading into the intestine to form pancreatic juice. Pancreatic islets diffuse or form a separate organ. There are five types of cells. They function as endocrine glands, secreting, e.g., hormones, such as insulin, somatostatin, and also glucagon in gnathostomatas [
175,
176,
177,
178].
Insulin is an anabolic peptide hormone with a systemic effect that plays an essential role in the metabolism of carbohydrates, as well as proteins and fats, secreted by the endocrine part of the pancreas, more specifically by the beta cells of Langerhans islands. The primary task of insulin is to lower blood glucose levels. This happens in four different ways: by increasing glucose transport to insulin-responsive tissues, increasing the use and storage of glucose by tissues, increasing the use of amino acids and increasing fat synthesis. A synthetic form of insulin is commonly used in the treatment of type 1 diabetes, where the pancreatic beta islet cells stop producing this hormone, which in turn causes chronic hyperglycemia [
179,
180,
181,
182]. When considering the still-growing amount of diabetes causes and the importance of the accurate systems of direct insulin measurements in the human body, new electrochemical sensors for insulin determination are still demanded. Since 2000, numerous works of voltammetric and amperometric insulin determination methods have been reported. Most of them used glassy carbon electrodes as working electrodes, modified by different types of nanomaterials, such as carbon nanotubes, nickel nanoparticles or reduced graphene oxide. Among the various materials, transition metal oxides and hydroxides have attracted great interest in electrochemical studies because of their excellent electrocatalytic activity toward different compounds. The use of such modifiers allows for obtaining picomolar insulin limits of detection (
Table 3). The great interest in insulin determination, therefore, results in the preparation of voltammetric assays for its sensitive measurement in human serum and plasma samples and in injections commonly used by people with diabetes.
In
Table 3, the electrochemical methods of insulin determination are compared.
Table 3.
Electrochemical methods of pancreatic hormones determination.
Table 3.
Electrochemical methods of pancreatic hormones determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Detection Limit | Linear Range | Source |
|---|
| Insulin | amperometry | CNT-NiCoO2 /Nafion | - | 0.1 M PBS pH 7.5 | 0.22 µg mL−1 | 0.1–31.5 µg mL−1 | [183] |
| FIA | CCE | CHN | 0.3 M PBS pH 10 | 0.11 × 10−9 M | 0.5–15 × 10−9 M | [184] |
| Amperometry | GCE | IrOx | 0.1 mM Na3IrCl6 + 0.2 M HCl pH 7.4 | 20 × 10−9 M | 50–500 × 10−9 M | [185] |
| Amperometry | CCE | [Ru(bpy) (tpy)CI]PF6 | 0.1 M PBS pH 7.0 | 0.4 × 10−9 M | 0.5–850 × 10−9 M | [186] |
| FIA | CPE | RuOx | 0.1 M NaCl + 0.05 M phosphate buffer pH 7.4 | 50 × 10−9 M | 100–1000 × 10−9 M | [187] |
| FIA | GCE | RuOx-CNT | 0.05 M PBS pH 7.4 | 1 × 10−9 M | 10–80 × 10−9 M | [188] |
| Amperometry | SPE | MWCNT/NiONPs | 0.1 M NaOH pH 13 | 6.1 × 10−9 M | 20–260 × 10−9 M | [189] |
| FIA | GCE | SiC | PBS pH 7.4 | 0.0033 × 10−9 M | 0.1–0.6 × 10−9 M | [190] |
| Amperometry | CPE | Si | PBS pH 2.0 | 36 × 10−12 M | 90–1400 × 10−12 M | [191] |
| FIA | C | RuRDMs | 0.2 M PBS pH 7.0 | 2 × 10−9 M | 6–400 × 10−9 M | [192] |
| Amperometry | GCE | CT/CNT | PBS pH 7.4 | 30 × 10−9 M | 100–3000 × 10−9 M | [193] |
| CV | ITO | NiNPs | 0.1 M NaOH | 10 × 10−9 M | 1 × 10−9–125 × 10−9 M | [194] |
| CV | CFME | NiNPs/CNTs | 0.1 M NaOH | 270 × 10−9 M | 2–20 × 10−6 M | [195] |
| DPV | GCE | SiO2 NPs/Nafion | 0.1 M PBS pH 7.35 | 3.1 × 10−9 M | 10–50 × 10−9 M | [196] |
| FIA | GC | CNT | 0.05 M PBS pH 7.4 | 14 × 10−9 M | 100–1000 × 10−9 M | [197] |
| FIA | CCE | NiNPs | 0.1 M PBS pH 13 | 2.6 × 10−12 M | 15–100 × 10−12 M | [198] |
| CV | GC | rGO | 0.1 M PBS pH 7.4 | 350 × 10−12 M | 4–640 × 10−9 M | [199] |
| amperometry | GC | NiO/guanine | PBS pH 7.4 | 22 × 10−12 M | 100 × 10−12 M–4 × 10−6 M | [200] |
| amperometry | GCE | Ni(OH)2NPs/Nafion-MWCNT | 0.1 M NaOH | 85 × 10−9 M | 0–40 × 10−6 M | [201] |
| SWV | PGE | NiNPs/MB | B-R buffer pH 7.0 | 33.17 × 10−9 M | 25–450 × 10−9 M | [202] |
| CV | TFT microelectrodes | MWCNT | 0.05 M PBS pH 7.4 | 250 × 10−9 M | 250 × 10−9–1.6 × 10−6 M | [203] |
| FIA | GCE | CoOx | PBS pH 9.0 | 25 × 10−12 M | 100 × 10−12 M–15 × 10−9 M | [204] |
3.4. Pineal Gland Hormones
The pineal gland is one of the endocrine glands, which lies between the upper mounds of the lamina. The pineal gland cells—pinealocytes—produce the so-called sleep hormone – melatonin, a derivative of tryptophan [
205,
206,
207]. Melatonin and its derivative metabolites are secreted into the cerebrospinal fluid and into the blood. Its secretion is closely related to light stimulation; its presence inhibits the production of this hormone. In mammals, it also has an inhibitory effect on the secretion of gonadotropic hormones, preventing premature sexual maturation. The secretory activity of the pineal gland follows the daily rhythm of changes in lighting and probably affects the rhythmicity of various physiological functions. In mammals, the secretion of the pineal gland is controlled by impulses sent by the eye’s retina. Disturbances in the work of this gland cause disturbance of the circadian rhythm and, in the long term, disturbances in the development of gonads. Melatonin is sold in the form of over-the-counter tablets as a drug to help people fall asleep, who have disturbed circadian rhythms, or for blind patients and those with sleep disorders related to changing time zones (sudden change in time zone syndrome) [
208,
209,
210,
211,
212].
A large variety of sensors based on polymers, nanoparticles, carbon-based materials, hybrid arrangements and biomolecules were used for the highly sensitive determination of melatonin. According to the literature, melatonin determination on an unmodified solid electrode has been performed on a boron-doped diamond electrode, carbon paste electrode and glassy carbon electrode thus far. In order to obtain a high sensitivity of the performed measurements, different types of electrode modifications have been developed since then. The most popular include multi-walled carbon nanotubes, palladium nanoparticles, nanorods of ZnO
2, graphene or carbon black. The lowest detection limit obtained for melatonin was measured using the alternating current voltammetry with a carbon paste electrode as a working electrode, and it was equal to 9 × 10
−11 M (
Table 4). Samples of the melatonin calibration graphs are presented in
Figure 2 [
213]. Melatonin measurements were performed using voltammetric techniques in the samples, such as human serum and plasma, urine, and in pharmaceutical formulations in the form of tablets.
In
Table 4, the electrochemical methods of melatonin determination are compared.
Figure 2.
Melatonin calibration graphs (
A) with corresponding voltammograms (
B) measured on a glassy carbon electrode modified with carbon black [
213]. The following curves in picture A stand for preconcentration times: a: 0 s, b: 3 s, c: 6 s, d: 10 s and e: 20 s, measurements carried out in the 0.1 mol L
−1 phosphate buffer pH 6.2. Reprinted from
Carbon black as a glassy carbon electrode modifier for high sensitive melatonin determination, Journal of Electroanalytical Chemistry, Vol 799, Joanna Smajdor, Robert Piech, Magdalena Pięk, Beata Paczosa-Bator, Pages 278–284, 2017, with permission from Elsevier.
Figure 2.
Melatonin calibration graphs (
A) with corresponding voltammograms (
B) measured on a glassy carbon electrode modified with carbon black [
213]. The following curves in picture A stand for preconcentration times: a: 0 s, b: 3 s, c: 6 s, d: 10 s and e: 20 s, measurements carried out in the 0.1 mol L
−1 phosphate buffer pH 6.2. Reprinted from
Carbon black as a glassy carbon electrode modifier for high sensitive melatonin determination, Journal of Electroanalytical Chemistry, Vol 799, Joanna Smajdor, Robert Piech, Magdalena Pięk, Beata Paczosa-Bator, Pages 278–284, 2017, with permission from Elsevier.
Table 4.
Electrochemical methods of pineal gland hormones determination.
Table 4.
Electrochemical methods of pineal gland hormones determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit, M | Linear Range, M | Source |
|---|
| Melatonin | DPV | GCE | CB/DMF | 0.1 M phosphate buffer pH 6.2 | 45 | 1.9 × 10−8 | 0.05 × 10−6–12 × 10−6 | [213] |
| CV | BDD | - | 1 M KCl | n/i | 1.03 × 10−5 | 3.4 × 10−4–6.8 × 10−4 | [214] |
| SWV | GCE | AHNSA/PdNPs/ErGO | 1 M phosphate buffer pH 7.2 | n/i | 0.09 × 10−6 | 5 × 10−6–100 × 10−6 | [215] |
| SWV | BDD | - | 0.1 M B-R buffer pH 3.0 | 60 | 1.1 × 10−7 | 0.5 × 10−6–4.0 × 10−6 | [216] |
| DPV | GCE | - | 0.5 M H2SO4 + 20% methanol pH 2.15 | n/i | 5.86 × 10−6 | 20 × 10−6–80 × 10−6 | [217] |
| amperometry | GCE | MnHCF/PEDOT | 0.1 M KCl buffer pH 1.5 | 3 | 100 × 10−6 | 100–4600 × 10−6 | [218] |
| DPV | GCE | RGO/RuO2 | PBS pH 7.0 | n/i | 0.18 × 10−6 | 2–20 × 10−6 | [219] |
| LSV | GCE | - | 0.05 M phosphate buffer pH 3.0 | n/i | 1.1 × 10−5 | 2.7 × 10−5–2.2 × 10−4 | [220] |
| DPV | GCE | 3DG/AuNPs | 0.04 M PBS pH 7.4 | n/i | 0.0082 × 10−6 | 0.05-50 × 10−6 | [221] |
| amperometry | CPE | - | 0.1 M HClO4 | 0 | 8 × 10−9 | 10−8–10−5 | [222] |
| DPV | CILE | MWCNTs–CoHNPs | 0.01 M PBS pH 7.5 | 90 | 0.004 × 10−6 | 0.01–50 × 10−6 | [223] |
| SWV | GPT/WPE | - | 0.1 M phosphate buffer pH 7.4 | n/i | 32.5 × 10−9 | 0.8–100 × 10−6 | [224] |
| SWV | SPE | - | 0.1 M phosphate buffer pH 5.0 | n/i | 25.8 × 10−9 | 0.25–75 × 10−6 | [225] |
| LSV | GCE | MWNTs-DHP | 0.01 M PBS pH 7.5 | 180 | 0.02 × 10−6 | 0.08–10 × 10−6 | [226] |
| OSWSV | AGCE | - | 0.04 M B-R buffer pH 6.7 | 120 | 0.05 × 10−6 | 0.8–10 × 10−6 | [227] |
| SWV | CPE | Graphene/Fe2O3 | B–R buffer pH 5.0 | n/i | 8.4 × 10−9 | 0.02–5.8 × 10−6 | [228] |
| ACV | CPE | - | 0.1 M HClO4 | 600 | 9.0 × 10−11 | 1.0 × 10−10–1.0 × 10−9 | [229] |
| SWV | HMDE | - | acetate buffer pH 5.0 | 30 | 3.1 × 10−10 | 1 × 10−9–1 × 10−7 | [230] |
| SWV | GCE | GR/AHNSA/MM | PBS pH 7.2 | 240 | 60 × 10−10 | 0.05–100 × 10−6 | [231] |
| SWV | Gr-AV | - | 0.5 M McIlvaine buffer solution pH 7.0 | n/i | 0.49 × 10−6 | 10–100 × 10−6 | [232] |
| DPV | CPE | PdNP@Al2O3 | 0.1 M PB pH 7.0 | n/i | 21.6 × 10−9 | 6 × 10−9–1.4 × 10−3 | [233] |
| DPV | GCE | - | B–R buffer pH 4.3 | n/i | 1.48 × 10−6 | 10–500 × 10−6 | [234] |
| SWV | Au | acetylene black NPs-chitosan (AB-C) | 0.1 M PBS pH 7.0 | 0 | 1.9 × 10−6 | 2 × 10−5–4.5 × 10−4 | [235] |
| DPV | SPE | MWCNTs | 50 mM phosphate buffer pH 7.6 | n/i | 1.1 × 10−6 | 0.005–3 × 10−3 | [236] |
| CV | SPE | graphene | 0.1 M PBS pH 7.0 | n/i | 0.87 × 10−6 | 1–300 × 10−6 | [237] |
3.5. Ovarian Hormones
The ovarium is a gonad found in the females of most animals (except for sponges). Usually, a paired organ is found in females, which is the developmental equivalent of the testicles. The ovaries lie inside the peritoneal cavity at the side walls of the pelvis on the posterior surface of the broad ligaments of the uterus, to which they are attached by the short mesentery. The ovaries serve a dual purpose: the production of eggs and the secretion of female sex hormones (estrogens, progesterone, relaxin and androgens). From the moment a woman reaches sexual maturity until the end of her reproductive function (menopause), the so-called Graaf’s follicle contains an egg. A follicle that is ripe to rupture is 1–1.5 cm in diameter, and the egg cell is about 0.2 mm. Follicle maturation occurs under the influence of the follicle-stimulating hormone, and under the influence of the luteinizing hormone, the amount of fluid in the follicle increases, and finally, it ruptures. When the follicle ruptures, the egg enters the fallopian tube, and the rest of the follicle produces a red body—and a corpus luteum from it—which releases the progesterone necessary to implant a fertilized egg into the uterine mucosa [
238,
239,
240].
Estrogens are a group of sex hormones that include the three main forms of estrogen naturally occurring in women: estrone (E1), estradiol (E2) and estriol (E3), as well as the estrogen produced only during pregnancy, estetrol (E4). Estrogens are called female hormones, and they play the most important role in the female body, but they are also essential for men, where a deficiency in the testes can cause infertility. Estrogens are steroidal hormones; they differ in the number and arrangement of the hydroxyl groups. They affect many features and functions of the body, especially the female body. They are mainly responsible for the development of second or third-order sexual characteristics of a woman’s body, regulation of the menstrual cycle, lipid and calcium metabolism or increasing blood clotting. During the menstrual cycle, the estradiol levels fluctuate, which produces specific physiological effects that prepare the uterus to receive and facilitate a fertilized egg, mainly by causing endometrial growth [
241,
242,
243,
244].
In the current literature, the topic of estrogen-compound determination is still gaining popularity due to being considered as a group of one of the biggest environmental pollutants, which has the ability to interfere with the endocrine system. In particular, the electrochemical methods have received extensive attention from researchers because of its sensitivity and short time of analysis. Square wave voltammetry and differential pulse voltammetry are especially useful for the detection of small amounts of estrogen. The lowest detection limits for E1, E2 and E3 were equal to 0.23 pM, 0.54 pM and 0.5 nM, respectively (
Table 5). In order to check the utility of the proposed methods for routine quality control analyses, the measurements were performed in samples, such as water (tap water, wastewater and surface water) human urine, blood, serum, plasma, animal tissues and milk. Samples of the estradiol calibration graphs are presented in
Figure 3 [
245].
Progesterone (lutein) is a female sex hormone with a steroid structure, produced mainly by the luteal cells in the luteal phase. It is one of the most important hormones secreted by the ovaries. This hormone enables the embryo to implant in the uterine mucosa and maintains the pregnancy. If pregnancy does not occur, progesterone secretion is reduced, and corpus luteum luteolysis occurs. The rapid reduction in blood progesterone levels results in a controlled shedding of the lining of the womb (menstruation). After fertilization, progesterone is initially secreted by the corpus luteum, and in the 14–18 weeks of pregnancy (in humans), it is also produced by the placenta. In the female body, progesterone works through the appropriate receptors located, among others, in the uterus, mammary glands, CNS (central nervous system) and pituitary gland. Progesterone acts synergistically with estrogens on the mammary gland, stimulating the growth of the glandular cells and ductal epithelium and participating in the expression of the receptors necessary for lactation. Other metabolic effects of progesterone include an increasing body temperature, stimulating breathing, lowering the concentration of amino acids in the blood serum, normalization of blood glucose levels, and antiandrogenic activity consisting in the activity’s inhibition of 5-alpha reductase, which transforms testosterone into dihydrotestosterone. The fall in progesterone levels after childbirth causes mood swings, known as postnatal depression [
246,
247,
248,
249]. Many electrochemical techniques of progesterone determination are based on the modification of solid electrodes with a layer comprising progesterone-specific antibodies or aptamers. The use of such immunosensors allows for obtaining a progesterone limit of detection as low as 1.86 pM. Additionally, modifiers, such as metal oxides, multi-walled carbon nanotubes, conducting polymers or other carbon nanomaterials, are commonly used in progesterone determination assays. The limits of detection, obtained in the literature since 2000, allow for the measurement of progesterone in samples, such as human serum, plasma, milk, and in pharmaceutical formulations in the form of injections.
In
Table 5, the electrochemical methods of estradiol, estriol, estrone and progesterone determination are compared.
Figure 3.
Estradiol calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 60 s (
B) measured on a glassy carbon electrode modified with carbon black [
245]. The following curves in picture A stand for preconcentration times: a: 60 s, b: 20 s and c: 5 s, measurements carried out in the 0.1 mol L
−1 phosphate buffer pH 6.2. Reprinted from
Glassy carbon electrode modified with carbon black for sensitive estradiol determination by means of voltammetry and flow injection analysis with amperometric detection, Analytical Biochemistry, Vol 544, Joanna Smajdor, Robert Piech, Martyna Ławrywianiec, Beata Paczosa-Bator, Pages 7–12, 2018, with permission from Elsevier.
Figure 3.
Estradiol calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 60 s (
B) measured on a glassy carbon electrode modified with carbon black [
245]. The following curves in picture A stand for preconcentration times: a: 60 s, b: 20 s and c: 5 s, measurements carried out in the 0.1 mol L
−1 phosphate buffer pH 6.2. Reprinted from
Glassy carbon electrode modified with carbon black for sensitive estradiol determination by means of voltammetry and flow injection analysis with amperometric detection, Analytical Biochemistry, Vol 544, Joanna Smajdor, Robert Piech, Martyna Ławrywianiec, Beata Paczosa-Bator, Pages 7–12, 2018, with permission from Elsevier.
Table 5.
Electrochemical methods of ovarian hormone determination.
Table 5.
Electrochemical methods of ovarian hormone determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit | Linear Range | Source |
|---|
| Estradiol | DPV | GCE | CB/DMF | 0.1 M phosphate buffer pH 6.2 | 60 | 9.2 × 10−8 M | 0.15 × 10−6–3.5 × 10−6 M | [245] |
| DPV | GCE | RGO/CuTthP | 0.1 M PBS pH 7.0 | n/i | 5.3 × 10−9 M | 0.1–1.0 × 10−6 M | [250] |
| LSV | GCE | Nafion | phosphate buffer pH 8.0 + CTAB | 360 | 1 × 10−9 M | 2.5 × 10−8–1.5 × 10−6 M | [251] |
| SWV | GCE | CNT–Ni (cyclam) | 0.1 M PBS pH 7.2 | n/i | 60 × 10−9 M | 0.5–40 × 10−6 M | [252] |
| amperometry | SPC | anti-estradiol-Biotin-Strept-ABAg | 0.05 M PBS pH 6.0 | 0 | 2.8 × 10–12 M | 3.7 × 10–12 –9.2 × 10–10 M | [253] |
| SWV | WGE | CCh | 0.1 M PBS pH 7.0 | 60 | 4 × 10−7 M | 4 × 10−6–4 × 10−5 M | [254] |
| SWV | Au | AuNPs/Protein G | 0.02 M PBS pH 7.4 | n/i | 6.6 × 10–12 M | 6.6 × 10–12 –4.4 × 10−9 M | [255] |
| FFTSWV | CPE | (Tb2(CO3)3) NPs | PBS pH 5.0 | n/i | 3.7 × 10–11 M | 3.7 × 10–10–3.7 × 10–5 M | [256] |
| DPV | GCE | - | 0.05 M H2SO4 methanol/water 9:1 | n/i | 1.21 × 10−5 M | 4 × 10−5–1 × 10−3 M | [257] |
| DPV | GCE | BPIDS | PBS pH 10.0 | 180 | 5.0 × 10−8 M | 1.0 × 10−7–1.0 × 10−5 M | [258] |
| DPV | CPE | GNR-FS-Au-CA | 0.1 M PBS pH 5.0 | 180 | 0.0074 × 10−6 M | 0.1–5.0 × 10−6 M | [259] |
| LSV | GCE | RGO-DHP | 0.05 M PBS pH 7.0 | 240 | 0.077 × 10−6 M | 0.4–10 × 10−6 M | [260] |
| SWV | HMDE | - | 0.03 M B-R buffer pH 10.0 | 30 | 0.3 µg L−1 | Up to 21.8 µg L−1 | [261] |
| DPV | CPE | Cu-BTC | phosphate buffer pH 7.0 | 120 | 0.001 × 10−6 M | 0.003–0.75 × 10−6 M | [262] |
| SWV | GCE | NiFe2O4-MC | 0.1 M TBATFB | n/i | 6.88 × 10−9 M | 20–566 × 10−9 M | [263] |
| SWV | GCE | Pt/MWNTs | PBS pH 7.0 | 180 | 1.8 × 10−7 M | 5.0 × 10−7–1.5 × 10−5 M | [264] |
| amperometry | CPE | FeTPyPz | 0.1 M PBS pH 6.0 | 0 | 1.3 × 10−5 M | 4.5 × 10−5–4.5 × 10−4 M | [265] |
| SWV | CPE | CuO | 0.1 M B-R buffer pH 9.0 | n/i | 21 × 10−9 M | 60-800 × 10−9 M | [266] |
| LSV | GCE | poly(L-serine) | 0.1 M phosphate buffer pH 6.5 | 120 | 2.0 × 10−8 M | 1.0 × 10−7–3.0 × 10−5 M | [267] |
| CV | GCE | MWNT-[bmim]PF6 | 0.1 M PBS 7.0 | 270 | 5.0 × 10−9 M | 1.0 × 10−8–1.0 × 10−6 M | [268] |
| LSV | GCE | Al2O3 | 0.1 M phosphate buffer pH 8.0 | 120 | 8 × 10−8 M | 4 × 10−7–4 × 10−5 M | [269] |
| DPV | GCE | CdSe-BSA-antiE2 | 0.1 M acetate buffer pH 4.5 | 150 | 1.8 × 10–10 M | 1.8 × 10–10–3.7 × 10–10 M | [270] |
| DPV | GCE | Lac/rGO-RhNP | 0.1 M PBS 7.0 | n/i | 0.54 × 10−12 M | 0.9–11 × 10−12 M | [271] |
| SWV | GCE | MWNT-Nafion | 0.1 M phosphate buffer pH 7.0 | 300 | 1 × 10–8 M | 2.5 × 10–7–10 × 10–6 M | [272] |
| DPV | GC | nanosized biochar particles BCNPs | 0.05 M phosphate buffer pH 4.0 | 1200 | 11.3 × 10−9 M | - | [273] |
| DPV | SPE | CuP/ P6LC/Nafion film | 0.1 M phosphate buffer pH 5.0 | n/i | 5 × 10−9 M | 8 × 10−8–7.3 × 10−6 M | [274] |
| SWV | BDD | CB | 0.1 M phosphate buffer pH 12.0 | 120 | 2.2 × 10−9 M | 5–100 × 10−9 M | [275] |
| SWV | Au | PEDOT/AuNP | PBS pH 7.5 | n/i | 0.02 × 10−9 M | 0.1–100 × 10−9 M | [276] |
| Estriol | SWV | CPE | Fe3O4NPs | 0.1 M B-R buffer pH 6.0 | - | 2.7 × 10−6 M | 3.0 × 10−6 –1.1 × 10−4 M | [277] |
| DPV | GC | rGO–SbNPs | 0.1 M PBS pH 9.0 | 30 | 5.0 × 10−10 M | 2.0 × 10−7–1.4 × 10−6 M | [278] |
| DPV | GC | rGO/AgNPs | 0.2 M PBS pH 9.0 | 30 | 21.0 × 10−9 M | 0.1–3.0 × 10−6 M | [279] |
| SWV | BDD | - | 0.005 M NaOH pH 12.0 | n/i | 1.7 × 10−7 M | 2.0 × 10−7–2.0 × 10−5 M | [280] |
| CV | CPE | PGM | 0.2 M PBS pH 6.0 | n/i | 8.7 × 10−7 M | 2 × 10−6–1 × 10−4 M | [281] |
| DPV | GCE | CNB/AgNPs | 0.1 M PBS pH 7.0 | n/i | 0.16 × 10−6 M | 0.2 -3.0 × 10−6 M | [282] |
| SWV | GCE | Pt/MWNTs | PBS pH 7.0 | 180 | 620 × 10−9 M | 1.0 × 10−6–7.5 × 10−5 M | [264] |
| CV | GCE | Ni | 0.1 M NaOH pH 12.0 | n/i | 1.0 × 10−7 M | 5.0 × 10−6–1.0 × 10−4 M | [283] |
| LSV | GCE | RGO/GNPs/PS | 0.2 M PBS pH 5.7 | n/i | 0.48 × 10−6 M | 1.5–22 × 10−6 M | [284] |
| DPV | CPE | SDS- PXAMCNTG | 0.1 M PBS pH 7.0 | 80 | 1.9 × 10−7 M | 10–70 × 10−6 M | [285] |
| DPV | CPE | L-proline | 0.1 M PBS pH 6.5 | n/i | 2.2 × 10−7 M | 6 × 10−6-6 × 10−5 M | [286] |
| DPV | GCE | Co-poly(Met) | 0.1 M PBS pH 7.0 | n/i | 0.034 × 10−6 M | 0.596-4.76 × 10−6 M | [287] |
| CV | GCE | Ni/Co | 0.1 M PBS pH 7.0 | n/i | 0.42 × 10−9 M | 1 × 10−9–14 × 10−9 M | [288] |
| amperometry | GCE | Lac/rGO/Sb2O5 | 0.1 M PBS pH 7.0 | - | 1.1 × 10−8 M | 2.5 × 10−8–1.03 × 10−6 M | [289] |
| Estron | SWV | GCE | AuNPs-pNap | CBS pH 5.0 | n/i | 2.3 × 10−13 pg mL−1 | 3.0 × 10−13–2 × 10−4 pg mL−1 | [290] |
| SWV | WGE | CCh | 0.1 M PBS pH 7.0 | 60 | 1 × 10−7 M | 3 × 10−7–3 × 10−5 M | [254] |
| SWV | BDD | - | 0.25 M H2SO4 | n/i | 0.10 × 10−6 M | 0.1–2.0 × 10−6 M | [291] |
| SWV | GCE | Pt/MWNTs | PBS pH 7.0 | 180 | 840 × 10−9 M | 2.0 × 10−6–5.0 × 10−5 M | [264] |
| SWV | CPE | Fe3O4 NP-BMI.PF6 | 0.2 M B–R buffer pH 12.0 | 5 | 0.47 × 10−6 M | 4–100 × 10−6 M | [292] |
| SWV | CPE | - | 0.1 M PBS pH 8.0 | 180 | 4.0 × 10−8 M | 9.0 × 10−8–8.0 × 10−6 M | [293] |
| LSV | GCE | MWNT/CR | 0.1 M PBS pH 8.0 | 400 | 5.0 × 10−9 M | 5.0 × 10−8–2.0 × 10−5 M | [294] |
| SWV | GCE | MWCNT-COOH | B-R buffer pH 7.0 | n/i | 0.117 × 10−6 M | 1.0–9.0 × 10−6 M | [295] |
| DPV | GCE | MoSI NWs | PBS pH 7.2 | n/i | 5.2 × 10−12 g mL−1 | 2 × 10−12–2 × 10−11 g mL−1 | [296] |
| Progesterone | SWV | BiFE | - | 0.1 M B–R buffer pH 12.0 | 60 | 0.18 × 10−6 M | 0.40–7.90 × 10−6 M | [297] |
| amperometry | GCE | Mn(III)-SB | 0.1 M NaOH pH 13.0 | n/i | 11.4 × 10−9 M | 0.022–0.25 × 10−6 M | [298] |
| SWV | GCE | - | 0.1 M N(C4H9)4PF6 + acetonitrile | n/i | 500 × 10−9 M | 4.0–1000 × 10−6 M | [299] |
| SWV | GCE | GO-IMZ | 0.1 M NaOH pH 13.0 | n/i | 68 × 10−9 M | 0.22–14.0 × 10−6 M | [300] |
| SWV | Au | mAbP4-AuNPs | 0.001 M CBS pH 5.0 | n/i | 0.25 × 10−9 M | 0.0016–0.038 × 10−6 M | [301] |
| DPV | GCE | Fe3O4@GQD/f–MWCNTs | 0.1 M PBS pH 7.0 | 140 | 2.2 × 10−9 M | 0.01–3.0 × 10−6 M | [302] |
| DPV | GCE | Sn nanorods | 0.2 M NaOH pH 13.0 | - | 0.12 × 10−6 M | 40–600 × 10−6 M | [303] |
| amperometry | SPE | mAbP4 | 0.1 M Diethanolamine–HCl buffer pH 9.85 | - | - | 0.0–0.079 × 10−6 M | [304] |
| DPV | SPE | (prog)–BSA conjugate | milk | n/i | 9.5 × 10−9 M | 0.05–0.81 × 10−6 M | [305] |
| DPV | CFP carbon fiber paper | CNS Carbon nanospheres | PBS pH 7.0 | n/i | 0.012 × 10−9 M | 37.4 × 10−12–0.25 × 10−9 M | [306] |
| SWV | nsBiFE | - | 0.1 M Na-PBS | 60 | - | 0.1– 0.7 × 10−6 M | [307] |
| amperometry | gold-graphite-Teflon | mAbP4 | 0.1 M diethanolamine-HCl buffer pH 10.0 | - | 2.7 × 10−9 M | 0.0–0.095 × 10−6 M | [308] |
| amperometry | GCE | mAbP4/HRP/pyrocatechol | 0.01 M PBS pH 7.0 | - | 0.63 × 10−9 M | 0.0016–0.04 × 10−6 M | [309] |
| amperometry | gold–graphite–Teflon | mAbP4 | 0.1 M TRIS pH 7.0 + 20 µM phenyl phosphate | - | 1.4 × 10−9 M | 0.0–0.13 × 10−6 M | [310] |
| SWV | CPE | Gd2(WO4)3NPs | 0.1 M B–R buffer pH 11.5 | n/i | 50 × 10−9 M | 0.1–1 × 10−6 M | [311] |
| SWV | SPE | AuNPs/AMBI/rGO | 0.1 M sodium hydroxide | n/i | 0.28 × 10−9 M | 0.9 × 10−9–27 × 10−6 M | [312] |
| DPV | GCE | PEDOT/ZrO2-NPs | CBS 0.1 M, pH 4 | n/i | 0.32 × 10−9 M | 1 × 10−9–6 × 10−3 M | [313] |
| DPV | SPE | BSA/aptamer/GQDs–NiO-AuNFs/f-MWCNTs | 0.1 M KCl + 5.0 mM K3[Fe(CN)6] | n/i | 1.86 × 10−12 M | 0.01–1000 × 10−9 M | [314] |
| DPV | GCE | GQD-PSSA/GO | 0.1 M CBS pH 6.0 | 180 | 0.31 × 10−9 M | 0.1–6.0 × 10−6 M | [315] |
| DPV | GCE | PEDOT/ZrO2-NPs | n/i | n/i | 0.32 × 10−9 M | 1–100 × 10−9 M | [313] |
3.6. Testicular Hormones
The testes are gonads found in most males of animals (except sponges). Male mammals have two testicles that are most often found in the scrotum—the fascia-dermal sac originating from the abdominal wall. In most mammals, the testes are located outside the body, suspended by a spermatic cord in the scrotum. This is because spermatogenesis is more efficient at temperatures lower than about 37 degrees Celsius inside the body. Similar to the ovaries (whose counterparts are), the testes are a component of two systems: the reproductive system (as gonads) and the endocrine system (as endocrine glands). The functions of the testicles are sperm production and the production of male sex hormones (including testosterone). Both sperm-forming and endocrine functions are under the control of the hormones produced by the anterior pituitary gland, which are lutropin (LH) and follicle-stimulating hormone (FSH) [
316,
317,
318].
Testosterone is an organic chemical compound from the group of androgens, the basic male sex steroid hormone. It is produced by Leydig interstitial cells in the testes under the influence of the luteinizing hormone and also in small amounts by the adrenal cortex, ovaries and placenta. In the blood, only a small part of testosterone is in the free form and bound to albumin, with the rest being bound (inactive) with the SHBG transport protein (sex hormone binding globulin). In target tissues, testosterone is converted into a 2.5 times stronger form of 5-α-dihydrotestosterone. In order to exert its biological effects, testosterone binds with the receptors for steroid hormones located in the cytoplasm and nucleus of the effector cells. The treatment uses testosterone derivatives—esters for oral use or injection with a slow release from the muscle tissue. Testosterone is responsible for shaping sex and sexual characteristics in utero, spermatogenesis, development of secondary sexual characteristics, stimulating protein synthesis, increasing blood cholesterol and stimulating the development of the prostate gland, which stimulates the development of prostate cancer. Testosterone, when used in women, has an anabolic effect; however, it is very rarely practiced medicinally due to undesirable effects, such as masculinization and hirsutism. It is most often used in the case of advanced, hormonally active tumors [
319,
320,
321].
A variety of electrochemical techniques among the different types of working electrodes were implemented for highly sensitive testosterone determination. Aside from the classic construction of the hanging mercury drop electrode, on which the testosterone limit of detection was equal, mostly solid electrodes modified with different layers and carbon paste electrodes were used. The lowest testosterone detection limit reported in the papers since 2000 was obtained using the gold electrode modified by a layer of molecularly imprinted polysiloxane thin film formed in the presence of testosterone, and it was equal to 10 fM. In the construction of other modifier layers, testosterone antibodies, carbon nanotubes, metal nanoparticles and oxides were commonly used (
Table 6). In order to check the utility of the proposed methods for routine quality control analysis, the measurements of testosterone were performed in samples such as human urine, blood, plasma, serum and saliva.
In
Table 6, the electrochemical methods of testosterone determination are compared.
Table 6.
Electrochemical methods of testicular hormones determination.
Table 6.
Electrochemical methods of testicular hormones determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit | Linear Range | Source |
|---|
| Testosterone | OSWV | EPPGE | SWCNT | PBS pH 7.2 | n/i | 2.8 × 10−9 M | 5–1000 × 10−9 M | [322] |
| SWV | GCE | - | 0.1 M B-R buffer pH 5.0 + 3 mM CTAB | 120 | 1.2 × 10−9 M | 10–70 × 10−9 M | [323] |
| CV | GCE | CoOx | 0.10 M NaOH pH 12.5 | n/i | 0.16 × 10−6 M | 0.33–2.00 × 10−6 M | [324] |
| DPV | GCE | rGO | borate buffer pH 5.4 + CTAB | n/i | 0.1 × 10−9 M | 2.0–210.0 × 10−9 M | [325] |
| SWV | BiFE | - | 0.1 M B-R buffer pH 5.0 + 3 mM CTAB | 120 | 0.3 × 10−9 M | 1–45 × 10−9 M | [326] |
| DPV | CPE | MWCNT/MD | n/i | n/i | 1.33 × 10−11 M | 10 × 10−10–10 × 10−8 M | [327] |
| amperometry | Teflon | antitestosterone/MWCNT/AuNPs | 0.5 mM catechol+ PBS of pH 7.4 + H2O2 | - | 2.9 × 10−10 M | 3.5 × 10−9–3.5 × 10−8 M | [328] |
| SWV | GCE | Pb | 0.05 M acetate buffer pH 5.2 + Pb(NO3)2 | 120 | 9 × 10−9 M | 2 × 10−8–3 × 10−7 M | [329] |
| SWV | Au | DMIP | 0.01 M PBS pH 7.2 | - | 10 × 10−15 M | 10–100 × 10−15 M | [330] |
| amperometry | Si | α-testosterone mAb | PBS pH 7.0 + 1 mM H2O2 + 1 mM HQ | n/i | 43 × 10−12 M | 34 × 10−12 – 34 × 10−9 M | [331] |
| DPV | HMDE | - | B-R buffer pH 6.5 | 300 | 5 × 10−9 M | 1 × 10−8 – 7.3 × 10−6 M | [332] |
| amperometry | SPCE | pBDBT/AbTES | 5.0 mM [Fe(CN)6]3−/4− in 0.1 M KCl | n/i | 17 ng mL−1 | 10–500 ng mL−1 | [333] |
3.7. Other Hormones and Steroids
Aside from the previously described, the human body produces many other hormones, not only by the glands (e.g., human chorionic gonadotropin, thyroxine) but also by the adipose cells (leptin) or intestinal tract (serotonin). Thanks to modern medicine, we are able to compensate for the deficiency of the natural hormone by replacing it with an artificial one (e.g., sodium levothyroxine). Additionally, the still-growing industry of contraceptive drugs causes the development of new synthetic hormones that are similar to the natural ones (e.g., ethinylestradiol, drospirenon) [
334,
335,
336,
337,
338]. Samples of the sodium levothyroxine and human chorionic gonadotropin sodium calibration graphs are presented in
Figure 4 [
339] and
Figure 5 [
340].
Figure 4.
Spironolactone calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 20 s (
B) measured on refreshable silver-based amalgam film electrode [
339]. The following curves in picture A stand for preconcentration times: a: 0 s, b: 3 s, c: 5 s, d: 10 s, e: 20 s, f: 30 s and g: 45 s, measurements carried out in the 0.031 mol L
−1 acetate buffer, pH 4.6. Reprinted from
Spironolactone voltammetric determination on renewable amalgam film electrode, Steroids, Vol 130, Joanna Smajdor, Robert Piech, Beata Paczosa-Bator, Pages 1–6, 2018, with permission from Elsevier.
Figure 4.
Spironolactone calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 20 s (
B) measured on refreshable silver-based amalgam film electrode [
339]. The following curves in picture A stand for preconcentration times: a: 0 s, b: 3 s, c: 5 s, d: 10 s, e: 20 s, f: 30 s and g: 45 s, measurements carried out in the 0.031 mol L
−1 acetate buffer, pH 4.6. Reprinted from
Spironolactone voltammetric determination on renewable amalgam film electrode, Steroids, Vol 130, Joanna Smajdor, Robert Piech, Beata Paczosa-Bator, Pages 1–6, 2018, with permission from Elsevier.
Figure 5.
Calibration curves of the electrochemical immunosensor toward hCG standards in pH 7.0 PBS containing 2 mmol L
−1 H
2O
2. Reprinted from
Ultrasensitive electrochemical immunosensor based on Au nanoparticles dotted carbon nanotube–graphene composite and functionalized mesoporous materials, Biosensors and Bioelectronics, Vol 33, Juanjuan Lu, Shiquan Liu, Shenguang Ge, Mei Yan, Jinghua Yu, Xiutao Hu, Pages 29–35, 2012, with permission from Elsevier [
340].
Figure 5.
Calibration curves of the electrochemical immunosensor toward hCG standards in pH 7.0 PBS containing 2 mmol L
−1 H
2O
2. Reprinted from
Ultrasensitive electrochemical immunosensor based on Au nanoparticles dotted carbon nanotube–graphene composite and functionalized mesoporous materials, Biosensors and Bioelectronics, Vol 33, Juanjuan Lu, Shiquan Liu, Shenguang Ge, Mei Yan, Jinghua Yu, Xiutao Hu, Pages 29–35, 2012, with permission from Elsevier [
340].
Another important class of biologically active compounds present in the WHO list of essential medicines is the steroid group. Steroids can be naturally produced by the organism and synthesized through chemical reactions. What they have in common is a tetracyclic carbon skeleton with 21 carbon atoms. In the human body, two classes of steroids can be distinguished: glucocorticoids and mineralocorticoids. Glucocorticoids are natural hormones that are produced by the adrenal cortex. They are of great importance in terms of metabolism, the immunological system, as well as the secretion of other hormones. The main representatives of this class of steroids are prednisone, dexamethasone or betamethasone. Mineralocorticosteroids are hormones produced in the human body by the glomerular layer of the adrenal cortex. They affect the inorganic metabolism. The main representative of mineralocorticosteroids is aldosterone. Its most important activity is the retention of sodium ions (Na+) in the body and the intracellular influx of potassium ions (K+) and the secondary retention of water in the body.
The construction of the working electrodes in the assays of steroid determination usually comprises the solid electrode covered by the modifier layer. Additionally, classical mercury electrodes can be found in the literature, as well as carbon paste electrodes comprising carbon nanomaterials, often with the addition of nanoparticles (
Table 7). Samples of the dexamethasone calibration graphs are presented in
Figure 6 [
341] and
Figure 7 [
342]. Steroids and synthetic hormones were measured in different matrices, such as human urine, serum and plasma, using voltammetric methods.
Figure 6.
Dexamethasone calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 30 s (
B) measured on refreshable silver-based amalgam film electrode [
341]. The following curves in picture A stand for preconcentration times: a: 3 s, b: 5 s, c: 10 s, d: 20 s, e: 30 s, and f: 45 s, measurements carried out in the 0.04 mol L
−1 acetate buffer pH 4.4. Reprinted from
Highly sensitive voltammetric determination of dexamethasone on amalgam film electrode, Journal of Electroanalytical Chemistry, Vol 809, Joanna Smajdor, Robert Piech, Beata Paczosa-Bator, Pages 147–152, 2018, with permission from Elsevier.
Figure 6.
Dexamethasone calibration graphs (
A) with corresponding voltammograms for the preconcentration time of 30 s (
B) measured on refreshable silver-based amalgam film electrode [
341]. The following curves in picture A stand for preconcentration times: a: 3 s, b: 5 s, c: 10 s, d: 20 s, e: 30 s, and f: 45 s, measurements carried out in the 0.04 mol L
−1 acetate buffer pH 4.4. Reprinted from
Highly sensitive voltammetric determination of dexamethasone on amalgam film electrode, Journal of Electroanalytical Chemistry, Vol 809, Joanna Smajdor, Robert Piech, Beata Paczosa-Bator, Pages 147–152, 2018, with permission from Elsevier.
Figure 7.
Square-wave voltammograms for DMZ in BR buffer (pH 2.0) on the HMDE with f = 100 s
−1, a = 15 mV, dEs = 2 mV, E
acc = −0.60 V, t
acc = 15 s, and concentrations in the interval from 4.98 × 10
−8 to 6.10 × 10
−7 mol L
−1 DMZ. Inset: Analytical curves obtained from voltammograms presented in the main panel. Reprinted from
Square-wave adsorptive voltammetry of dexamethasone: Redox mechanism, kinetic properties, and electroanalytical determinations in multicomponent formulations, Analytical Biochemistry, Vol 413, Thiago Mielle B.F. Oliveira, Francisco Wirley P. Ribeiro, Janete E.S. Soares, Pedro de Lima-Neto, Adriana N. Correia, Pages 148–156, 2011, with permission from Elsevier [
342].
Figure 7.
Square-wave voltammograms for DMZ in BR buffer (pH 2.0) on the HMDE with f = 100 s
−1, a = 15 mV, dEs = 2 mV, E
acc = −0.60 V, t
acc = 15 s, and concentrations in the interval from 4.98 × 10
−8 to 6.10 × 10
−7 mol L
−1 DMZ. Inset: Analytical curves obtained from voltammograms presented in the main panel. Reprinted from
Square-wave adsorptive voltammetry of dexamethasone: Redox mechanism, kinetic properties, and electroanalytical determinations in multicomponent formulations, Analytical Biochemistry, Vol 413, Thiago Mielle B.F. Oliveira, Francisco Wirley P. Ribeiro, Janete E.S. Soares, Pedro de Lima-Neto, Adriana N. Correia, Pages 148–156, 2011, with permission from Elsevier [
342].
Table 7.
Electrochemical methods of other hormones and steroid determination.
Table 7.
Electrochemical methods of other hormones and steroid determination.
| Analyte | Technique | Working Electrode | Modifier | Medium | Preconcentration Time, s | Detection Limit | Linear Range | Source |
|---|
| Cyproterone | SWV | GCP | AuNPs/f-MWCNT | PBS pH 5.0 | 30 | 1.7 × 10−8 M | 9.9 × 10−8–1.2 × 10−5 M | [343] |
| DDP | DME | - | B-R buffer pH 10 | - | 3.1 × 10−7 M | 1.2 × 10−6–7.7 × 10−5 M | [344] |
| Danazol | SW-AdSV | HMDE | - | 0.04 M B–R buffer pH 2 | 60 | 5.7 × 10−9 M | 7.5 × 10−8–3.8 × 10−7 M | [345] |
| DPP | DME | - | B–R buffer pH 1.0 | - | 1.0 × 10−6 M | 5 × 10−6–1 × 10−4 M | [346] |
| Human chorionic gonadotropin | CV | GCE | GNPs/pPA/MWNTs | 0.1 M PBS pH 7.0 | n/i | 0.3 mIU mL−1 | 1.0–160.0 mIU mL−1 | [347] |
| DPV | GCE | HRP/Ab2/GNPs/PB/CNTs | 0.1 M PBS pH 6.0 | n/i | 0.023 mIU mL−1 | 0.05–150 mIU mL−1 | [348] |
| amperometry | GCE | Anti-hCG/NPG-Gs | 0.067 M PBS pH 7.4 | n/i | 0.034 ng mL−1 | 0.5–40.00 ng mL−1 | [349] |
| amperometry | GCE | anti-hCG/Pt–Au alloy nanotube array | 0.1 M PBS pH 7.5 | n/i | 12 mIU mL−1 | 25–400 mIU mL−1 | [350] |
| CV | GCE | anti-hCG/nano-Au/MB | 0.1 M PBS pH 6.5 | n/i | 0.3 mIU mL−1 | 1.0–100.0 mIU mL−1 | [351] |
| Amperometry/CV | SiC | anti-HCG /Multi-layer epitaxial graphene (MEG) | PBS pH 7.4 | n/i | 5.62 ng mL−1 | 0.62–5.6 ng mL−1 | [352] |
| DPV | Gr–IL–Ct | PtNPs | 0.1 M PBS pH 7.4 + 5 mM RU + 0.1 M KCl | n/i | 0.00035 mIU mL−1 | 0.001–350 mIU mL−1 | [353] |
| amperometry | GCE | Anti-hCG/nano-gold and CS hybrid film | 0.1 M PBS pH 6.5 + 0.99 mM H2O2 | n/i | 0.1 mIU mL−1 | 0.2–100 mIU mL−1 | [354] |
| CV | GCE | Pd–Al alloy/HRP-Ab2/hCG/Ab1/GNps/PB/GNPs | 0.1 M PBS pH 7.2 + 0.8 mM H2O2 | n/i | 9.3 pg mL−1 | 0.5–200 pg mL−1 | [355] |
| amperometry | GCE | Anti-hCG/AuNPs | 0.1 M PBS pH 6.5 + 0.99 mM H2O2 | n/i | 0.08 × 10−9 M | 0.1–100 × 10−9 M | [356] |
| DPV | GCE | Anti-hCG/Au/MWCNTs/GS | 0.1 M PBS pH 7.0 + 2 mM H2O2 | n/i | 0.0026 × 10−9 M | 0.005–500 × 10−9 M | [340] |
| DPV | Au | Anti-hCG/AuNPs/Cys/AuNps | 0.1 M phosphate buffer pH 7.5 | n/i | 0.3 pg mL−1 | 0.001–60.7 ng mL−1 | [357] |
| CV | GCE | Anti-hCG/NP-Pd/MWCNTs-BMIMPF6 | PBS pH 7.2 + 0.2 M KCl | n/i | 3.2 pg mL−1 | 0.05–50 ng mL−1 | [358] |
| amperometry | GCE | Anti-hCG/Pd@SBA-15/TH/HSO3-GS | PBS pH 7.4 | n/i | 8.6 pg mL−1 | 0.01–16.00 ng mL−1 | [359] |
| amperometry | GCE | Pt@MSNi/HRP/Ab2/hCG Antigene/Ab1/TH/Graphene | 0.1 M PBS pH 7.4 | n/i | 7.5 pg mL−1 | 0.01–12 ng mL−1 | [360] |
| DPV | GE Graphite electrode | HRP-anti-hCG | 0.1 M PBS pH 7.0 | n/i | 0.3 × 10−9 M | 0.5–50 × 10−9 M | [361] |
| DPV | GCE | BSA/anti-hCG/Au@SiC–CS | PBS pH 7.4 + 0.1 M KCl | n/i | 0.042 IU L−1 | 0.1–100 IU L−1 | [362] |
| DPV | SPE | ALP-IgG labeled GNPs/Ab2 | PBS pH 7.4 | n/i | 0.36 × 10−9 M | 1.0 × 10−9–100.0 × 10−6 M | [363] |
| DPV | GC | Co-poly(Met) | 0.1 M PBS pH 7.0 | n/i | 0.113 × 10−6 M | 0.596–4.76 × 10−6 M | [364] |
| SWV | CPE | β-hCG-mAb/protein A | 0.05 M PBS pH 7.4 | n/i | 15 × 10−9 M | 30–200 × 10−9 M | [365] |
| DPV | GCE | GS/IL/HNP-AuAg | PBS pH 7.2 + 0.2 M KCl | n/i | 0.01 ng mL−1 | 0.05–35 ng mL−1 | [366] |
| DPV | GCE | HRP-anti-hCG/hCG/AuNPs-SG | 0.1 M PBS pH 7.0 | n/i | 1.4 × 10−9 M | 5.0–30.0 × 10−9 M | [367] |
| DPV | CE | Au/Mab/hCGs | 0.05 M PBS pH 7.4 | n/i | 612 × 10−15 M | 0–2 ng mL−1 | [368] |
| amperometry | GCE | AuNPs/TB/Hb/MWNT–CS | PBS pH 6.5 + 2.1 mM H2O2 | n/i | 0.3 × 10−9 M | 0.8 - 500 × 10−9 M | [369] |
| DPV | GCE | AgNPNPs/Gr-IL-Ct | 0.1 M phosphate buffer pH 7.0 + 5 mM riboflavin | n/i | 0.0066 × 10−9 M | 0.0212–530 × 10−9 M | [370] |
| SWV | GCE | BSA/anti-hCG/CNOs/AuNPs/PEG | [Fe(CN)6]3−/4− | n/i | 0.1 fg mL−1 | 0.1 fg mL−1– 1 ng mL−1 | [371] |
| DPV | GCE | Anti-hCG/AuNPs/Gr-IL-Chit | n/i | n/i | 0.0016 mIU mL−1 | 0.005-411.28 mIU mL−1 | [372] |
| amperometry | Au | Hb/anti-HCG/AuNPs/{NPB/l-cys}2 | 0.025 M PBS pH 6.5 | n/i | 0.2 × 10−9 M | 0.5–200 × 10−9 M | [373] |
| Leptin | DPV | GCE | SWCNTs-CT | DEA buffer solution + 0.75 mg mL−1 α-NP | n/i | 5 pg mL−1 | 0–1000 ng mL−1 | [374] |
| SWV | GCE | PG-BP | 0.1 M PBS pH 7.4 | n/i | 0.036 pg mL−1 | 0.150–2500 pg mL−1 | [375] |
| DPV | GCE | SWNTs/CT | DEA buffer solution + 1 mg mL−1 α-NP pH 9.5 | n/i | 30 pg mL−1 | 0.05–500 ng mL−1 | [376] |
| CV | GCE | Protein G/PPy/PPa/Au | 0.01 M PBS + 1% serum pH 7.4 | n/i | 10 ng mL−1 | 10–100000 ng mL−1 | [377] |
| DPV | SPE | BSA/anti-LEP/EDC/NHS/MPA/Au/ Ce3NbO7/CeO2 | 0.1 M PBS pH 7.4 | n/i | 0.138 pg mL−1 | 0.5–12000 pg mL−1 | [378] |
| CV | ITO-PET sheets | cyanogen bromide (CNBr) anti-leptin antibody | n/i | n/i | 0.0086 pg mL−1 | 0.05–100 pg mL−1 | [379] |
| DPV | SPCEs | Magnetic beads SPCE | Tris buffer+ 5% BSA pH 7.2 | n/i | 0.5 pg mL−1 | 5–100 pg mL−1 | [380] |
| Levonorgestrel | SWV | HMDE | - | B–R buffer pH 3 | 150 | 4.8 × 10−10 M | 1 × 10−9–1 × 10−7 M | [381] |
| SWV | solid amalgam electrode | AgNPs | 0.04 M B-R buffer pH 6.0. | 70 | 9.09 × 10−8 M | 5.0 × 10−7–1.0 × 10−5 M | [382] |
| Methylprednisolone | DPV | GCE | fullerene-C60 | 0.5 M PBS pH 7.2 | n/i | 5.6 × 10−9 M | 5.0 × 10−9–1.0 × 10−6 M | [383] |
| SWV | EPPGE | SWNTs | 1.0 M PBS pH 7.2 | n/i | 4.5 × 10−9 M | 5–500 × 10−9 M | [384] |
| DPV | ITO | AuNPs | 0.5 M PBS pH 7.2 | n/i | 2.7 × 10−7 M | 0.01–1.0 × 10−6 M | [385] |
| Nandrolone | SWV | GCE | fullerene-C60 | 0.05 M PBS pH 7.2 | n/i | 0.42 × 10−9 M | 50 × 10−6–0.1 × 10−9 M | [386] |
| OSWV | EPPGE | - | 0.05 M PBS pH 7.2 | n/i | 1.5 × 10−11 M | 0.01–50 × 10−9 M | [387] |
| DPV | ITO | AuNPs | PBS pH 7.2 | n/i | 1.4 × 10−7 M | 50 × 10−9–1.5 × 10−6 M | [388] |
| Oxytocin | amperometry | BDD | - | Tris buffer pH 7.4 | n/i | 50 × 10−9 M | 0.1–10 × 10−6 M | [389] |
| Serotonin | DPV | GCE | MWCNT | phosphate buffer pH 7.0 | 120 | 5 × 10−9 M | 2 × 10−8–5 × 10−6 M | [390] |
| DPV | GCE | choline | 0.1 M PBS pH 4.0 | n/i | 5 × 10−7 M | 1 × 10−6–3 × 10−5 M | [391] |
| OSW | CPE | iron(II) phthalocyanine complexes [FeTSPc]4− | pH 7.4 | n/i | 1 × 10−6 M | 1 × 10−6 –1.51 × 10−5 M | [392] |
| SWV | GCE | C-undecylcalix [4]resorcinarene (CUCR) | 0.2 M phosphate buffer pH 7.0 | 120 | 3.0 × 10−8 M | 1.0 × 10−7–1.0 × 10−5 M | [393] |
| DPV | graphite | MWCNT | 50 mM phosphate buffer pH 7.4 | n/i | 0.2 × 10−6 M | 1.0–15 × 10−6 M | [394] |
| SWV | ITO | AuNPs | 0.1 M PBS pH 7.2 | n/i | 3.0 × 10−9 M | 1.0 × 10−8–2.5 × 10−4 M | [395] |
| SWV | EPPG | polymelamine | PBS pH 7.2 | n/i | 30 × 10−9 M | 0.1–100 × 10−6 M | [396] |
| DPV | GCE | nano-Au/PPyox | 0.1 M PBS pH 7.0 | 240 | 1.0 × 10−9 M | 7.0 × 10−9–2.2 × 10−6 M | [397] |
| DPV | GCE | reduced graphene oxide (RGO) | 0.1 M PBS pH 7.4 | n/i | 3.2 × 10−8 M | 1.0 × 10−6–1.0 × 10−4 M | [398] |
| CV | pencil graphite electrode (PGE) | poly(pyrrole-3-carboxylicacid) (p(P3CA) | 0.1 M PBS pH 5.0 | 90 | 2.5 × 10−9 M | 0.01–1.0 × 10−6 M | [399] |
| DPV | Pt | MWCNT/PPy/AgNPs | 0.2 M PBS pH 8.0 | n/i | 0.15 × 10−6 M | 0.50–5.0 × 10−6 M | [400] |
| DPV | GCE | poly(phenosafranine) | 0.1 M PBS pH 7.1 | n/i | 20 × 10−9 M | - | [401] |
| amperometry | BDD | - | 0.1 M phosphate buffer pH 7.0 | - | 10 × 10−9 M | 10 × 10−9 –50 × 10−6 M | [402] |
| SWV | Au | acetylene black nanoparticles-chitosan (AB-C) | 0.1 M PBS pH 7.0 | 0 | 1.6 × 10−7 M | 5 × 10−7–1.0 × 10−4 M | [235] |
| SWV | GCE | AuNPs | 0.2 M PBS pH 7.0 | n/i | 2.0 × 10−8 M | 6.0 × 10−8–6.0 × 10−6 M | [403] |
| DPV | GCE | 5-hydroxytryptophan (5-HTP) | 0.1 M PBS pH 6.0 | n/i | 1.7 × 10−6 M | 5.0 × 10−6–3.5 × 10−5 M | [404] |
| DPV | GCE | MWNTs-MO-Gel | 0.1 M phosphate buffer pH 7.0 | 240 | 8.0 × 10−8 M | 20 × 10−9–7 × 10−6 M | [405] |
| Triamcinolone | SWV | GCE | - | 0.1 M KOH pH 13.0 | 60 | 2.5 × 10−8 M | 3.8 × 10−8–1.2 × 10−4 M | [406] |
| OSWV | EPPG | SWNTs/fullerene-C60 | phosphate buffer pH 7.2 | | 8.9 × 10−10 M | 0.1-25 × 10−9 M | [407] |
| Thyroxine | DPV | Ag | 1, 3 diacryl urea, (DAU) | PBS pH 6.0 | 150 | 7.7 × 10−12 M | 1.3 × 10−11–2.2 × 10−8 M | [408] |
| CV | CPE | PVP | 0.1 M NaOH + CTAB pH 13.0 | 300 | 8 × 10−8 M | 2 × 10−7–9 × 10−6 M | [409] |
| LSV | GCE | SWNT | 0.1 M NaOH + CTAB pH 13.0 | 120 | 2 × 10−8 M | 1 × 10−7–7 × 10−6 M | [410] |
| CV | CPE | - | 0.1 M HCl + CTAB | 300 | 6.5 × 10−9 M | 2 × 10−7–9 × 10−6 M | [411] |
| DPV | GCE | MWCNT | 0.1 M HCl | 120 | 6.4 × 10−9 M | 1.9 × 10−8–5.1 × 10−7 M | [412] |
| CV | CPE | AuNPs/rGO | 0.1 M HCl | n/i | 1.0 × 10−9 M | 1.0–14.0 × 10−9 M | [413] |
| Mometasone | SWV | GE | SWCNT | 0.1 M phosphate buffer pH 7.2 + CTAB | - | 1.23 × 10−6 M | 10–1000 × 10−6 M | [414] |
| Dienogest | DPP | DME | - | phosphate buffer pH 10.8 | - | 0.58 × 10−6 M | 2.0 × 10−6 –1.0 × 10−4 M | [415] |
| SWV | GCE | ERGO/f-MWCNT/AuNPs | 0.1 M PB solution pH 3.0 | 60 | 1.88 × 10−8 M | 2.0 × 10−7–6.0 × 10−6 M | [416] |
| Drospirenone | DPV | Hg(Ag)FE | - | Acetate buffer pH 6.0 + Marlinat | 60 | 1.7 × 10−9 M | 2.5 × 10−9–1.0 × 10−8 M | [417] |
| SWV | HMDE | - | 0.04 M B-R buffer pH 8.0 | 30 | 0.027 µg mL−1 | 1.36 × 10−6–1.91 × 10−7 M | [418] |
| Finasteride | DPP | CGME | - | Ethanol + 0.0625 M H2SO4 pH<2 | n/i | 7.59 × 10−6 M | 5 × 10−5–5 × 10−4 M | [419] |
| Spironolactone | DPV | Hg(Ag)FE | - | 0.03 M acetate buffer pH 4.6 | 45 | 4.7·10−9 M | 15·10−9–3.0·10−6 M | [339] |
| DPV | HMDE | - | B-R buffer pH 9.0 | 60 | 1.1 × 10−11 M | 1.2 × 10−10–9.6 × 10−7 M | [420] |
| SWV | CPE | AuNPs@FCBN-PE | PBS pH 4.0 | 60 | 3.34 × 10−9 M | 12–1200 × 10−9 M | [421] |
| DPV | HMDE | - | B-R buffer pH 2.5 | 90 | 1.72 × 10−10 M | 1 × 10−8–2.5 × 10−7 M | [422] |
| Ethinylestradiol | DPV | GCE | CB/DMF | 0.01 M borate buffer pH 10.0 | 20 | 0.13 × 10−6 M | 0.25 × 10−6–3.0 × 10−6 M | [423] |
| SWV | GCE | MWCNTs | 10 mM H2SO4 pH 2 | 60 | 3.4 × 10–14 M | 1.2 × 10–13–2.4 × 10–10 M | [424] |
| amperometry | GCE | AgNPs/SiO2/GO/anti-EE2 | 0.1 M PBS pH 7.2 + 45 µL1 mM HQ + 5 µL 50 mM H2O2 | 0 | 2.2 × 10–11 M | 3.4 × 10–11-1.7 × 10–7 M | [425] |
| SWV | HMDE | - | B–R buffer pH 7.0 | 60 | 5.9 × 10−10 M | 2.9 × 10−9–5 × 10−7 M | [426] |
| LSV | CPE | - | 0.07 M phosphate buffer pH 8.04 + CPB | 150 | 3.0 × 10−8 M | 5.0 × 10−8–2.0 × 10−5 M | [427] |
| SWV | FTO | Chi/CNTs | 0.01 M PBS pH 7.0 | 150 | 0.09 × 10−6 M | 0.05–20 × 10−6 M | [428] |
| DPV | HMDE | - | 0.03 M B-R buffer pH 10.0 | 30 | 9.7 µg L−1 | Up to 400.5 µg L−1 | [261] |
| DPV | HMDE | - | 0.04 M B-R buffer pH 8.0 | 30 | 3.58 ng mL−1 | 6.75 × 10−8–6.07 × 10−7 M | [418] |
| SWV | GCE | MWCNTs-CoPc | 0.1 M phosphate buffer pH 7.0 | n/i | 2.2 × 10−6 M | 2.5–90 × 10−6 M | [429] |
| DPV | HMDE | - | B–R buffer pH 7.0 | 150 | 1.7 × 10–9 M | 1.3 × 10–8–2.0 × 10–7 M | [430] |
| SWV | BDD | - | 0.1 M B-R buffer pH 8.0 | n/i | 2.4 × 10−7 M | 9.9 × 10−7–5.2 × 10−6 M | [431] |
| DPV | GCE | rGO/RuO2 | 0.1 M PBS pH 7.0 | n/i | 2.0 × 10−9 M | 5.5 × 10−8 –1.2 × 10−6 M | [432] |
| Prednisolone | DPV | Hg(Ag)FE | - | 0.075 M acetate buffer pH 3.8 | 20 | 0.01 × 10−6 M | 0.05 × 10−6–2.25 × 10−6 M | [433] |
| amperometry | FTO | α-NiCe | 1.0 M KOH | 0 | 8.4 × 10−9 M | 0.5–76.9 × 10−6 M | [434] |
| OSWV | EPPG | SWNT | Phosphate buffer pH 7.2 | n/i | 0.45 × 10−8 M | 0.01–100 × 10−6 M | [435] |
| DPV | Au | Fullerene C60 | 0.1 M PBS pH 7.2 | n/i | 26 × 10−9 M | 1 × 10−6–0.1 × 10−3 M | [436] |
| DPV | HMDE | - | 0.04 M B-R buffer pH 3.5 | 40 | 1.1 × 10–7 M | 2.0 × 10–7–4.0 × 10–7 M | [437] |
| DPV | CPE | β-cyclode × trin | B-R buffer pH 3.0 | 150 | 4.8 × 10−7 M | 5.6 × 10−7–2 × 10−5 M | [438] |
| OSWV | EPPG | Fullerene C60 | PBS pH 7.2 | n/i | 4.8 × 10−8 M | 0.05–50 × 10−6 M | [439] |
| SWV | GC | OMC | 0.05 M PBS pH 7.2 | n/i | 0.057 × 10−6 M | 0.06–40 × 10−6 M | [440] |
| DPV | MIP | MWCNT | Phosphate buffer pH 4.0 | 60 | 0.05 × 10−6 M | 0.08–160 × 10−6 M | [441] |
| DPV | HMDE | - | B-R buffer pH 3.78 | n/i | 1.6 × 10–8 M | 5.6 × 10–8 –1.1 × 10–6 M | [442] |
| SWV | GCE | carbon nano sphere (CNSs) modified | 0.1 M PBS pH 7.2 | n/i | 73 × 10−9 M | 3-50 × 10−6 M | [163] |
| Betamethasone | DPV | Hg(Ag)FE | - | 0.1 M acetate buffer pH 3.0 | 45 | 1.6 × 10−9 M | 5.0 × 10−9 –0.8 × 10−6 M | [443] |
| SWV | EPPG | SWNT | 1 M PBS pH 7.2 | n/i | 0.25 × 10−9 M | 0.5–100 × 10−9 M | [444] |
| OSWV | EPPG | SWNT | 1 M PBS pH 7.2 | n/i | 0.5 × 10−9 M | 1–25 × 10−9 M | [445] |
| DPP | HMDE | - | 0.04 M B-R buffer pH 1.7 | n/i | 2.7 × 10−6 M | 3.9 × 10–6–1.1 × 10–4 M | [446] |
| Sodium levothyroxine | DPV | Hg(Ag)FE | - | 0.1 M sodium tetraborate solution + 300 µl HCl (1:10) pH 2.3 | 30 | 1.8 × 10−8 M | 0.025 × 10−6–4.0 × 10−6 M | [447] |
| DPV | SPE | CNT | 0.1 M acetate buffer pH 4.0 | 300 | 30 × 10−9 M | 0.1–0.9 × 10−9 M | [448] |
| CV | CPE | - | 0.1 M HCl + 0.1 mM phenyl hydrazine | n/i | 2.5 × 10−6 M | 0.025–0.1 × 10−3 M | [449] |
| CV | CPE | - | 0.1 M HCl | n/i | n/i | 2 × 10−4–2.2 × 10−3 M | [450] |
| DPV | GCE | MWCNTs/CC-SH/Au | PBS pH 7.2 | n/i | 2.84 × 10−9 M | 10–120 × 10−9 M | [451] |
| Dexamethasone | DPV | Hg(Ag)FE | - | 0.04 M acetate buffer pH 4.4 | 45 | 1.6 × 10−9 M | 2.5 × 10−9 –2.3 × 10−7 M | [341] |
| SWV | HMDE | - | 0.04 M B-R buffer pH 2.0 | 15 | 2.54 × 10−9 M | 5.0 × 10−8 –6.1 × 10−7 M | [342] |
| SWV | PGE | Fullerene C60 | PBS pH 7.2 | n/i | 5.5 × 10−8 M | 0.05–100 × 10−6 M | [452] |
| SWV | HMDE | - | 0.04 M B-R buffer pH 2.0 | 15 | 2.54 × 10–9 M | 7.5 × 10–9–1.8 × 10–8 M | [453] |
| DPV | CPE | Β-cyclodextrin | B-R buffer pH 3.0 | 150 | 3.6 × 10–7 M | 4.1 × 10–7–2 × 10–5 M | [163] |
| DPV | CFMS | - | 0.1 M PBS pH 7.3 | n/i | 4 × 10−9 M | 10 × 10−9–40 × 10−6 M | [454] |
| DPV | CILE | Fe3O4/PANI–Cu | 0.1 M KH2PO4 pH 2.0 | n/i | 3.0 × 10–9 M | 0.05–30 × 10−6 M | [455] |
| DPP | HMDE | - | Acetate buffer pH 5.0 | 0 | 7.6 × 10−6 M | 25.5–122.3 × 10−6 M | [456] |
| LSV | CPE | polyglycine-MWCNTs | B-R buffer pH 3.0 | 60 | 2.2 × 10–7 M | 4.8 × 10–7–4.9 × 10–5 M | [457] |
| SWV | Au | DNA aptamer | 0.01 M PBS buffer pH 7.4 | n/i | 2.12 × 10−9 M | 2.5–100 × 10−9 M | [458] |
| DPV | Nano-porous GCE | - | 0.1 M PBS pH 2 | n/i | 5 × 10−9 M | 0.02–22 × 10−6 M | [171] |
| DPV | GCE | Graphene nanoplate GNP | 0.1 M PBS pH 7.3 | n/i | 15 × 10–9 M | 0.1-5000 × 10–6 M | [459] |
| SWV | EPPGE | SWNT | phosphate buffer pH 7.2 | n/i | 9.1 × 10−10 M | 8.2 × 10−8–9.1 × 10−10 M | [460] |
| SWV | PE | MWCNTs | Acetate buffer pH 4.0 | 30 | 0.09 × 10−6 M | 0.15–100 × 10−6 M | [461] |
4. Future Trends
There is still a growing interest in designing a new construction of the working electrodes to prepare new measurement assays and obtain lower limits of detection. There is still a wide variety of possible modifier combinations that may result in discovering new analytical assays of hormones in steroids. Specifically, the field of immunosensors is very promising for this case, considering the possibilities of obtaining low detection limits by using specific antibodies for the selected analyte. Additionally, increased interest in the construction of the new hybrid composites of modifier layers is promising, considering the new possibilities of developing voltammetric assays for highly sensitive hormone and steroid determinations. The choice of electrode modifier is always connected with the possibility of improving the sensitivity of the measurements. One way of making such an improvement is by increasing the working surface of the working electrode, which is a natural consequence of nanomaterials usage in the modifier layer. Another way of improving the sensitivity of the measurements is the impact of the electrocatalytic properties of the modifiers. Hybrid materials are nowadays gaining more interest as electrode modifiers due to the possibility of mixing the properties of different components. Modifiers, such as metal nanoparticles or metal oxides, positively affect the easiness of electron transference during the electrode process, which influences the current response of the analyte. Modifiers’ compositions of the nanoparticles mixed with carbon nanomaterials can be described as the increased density of active sites and large surface area, which ensures multiple absorption active sites and better electrical conductivity in comparison with the unmodified electrode. However, the use of electrochemical techniques for the highly sensitive hormone and steroid determination may also be limited in the case of analyses of non-electroactive compounds. Additionally, an analysis of the real samples, such as human body fluids, may be troublesome due to its complex organic matrix, which may interfere with the measurements and influence the lower sensitivity of the detection. However, considering all the above, it can be said that the voltammetric techniques can be useful in the context of pharmaceutical formulation quality control.
5. Conclusions
Numerous cases of voltammetric measurements of electroactive samples with biological significance, such as hormones and steroids, have been reported since 2000. The voltammetric and polarographic techniques, due to their sensitivity and easiness, could be used alternatively to other, more complicated analytical assays. The process of sample preparation for electrochemical measurements is usually quick and does not require expensive procedures. Moreover, the mechanisms of analyte reactions on the surface of a working electrode and its redox properties, which can be investigated using the cyclic voltammetry technique, could provide additional knowledge about the interaction of the compound with cells and tissues. It has also been proven that electrochemical techniques are useful for hormone and steroid determination, not only in a simple supporting electrolyte but also in more complex matrices, such as tablets, ointments, creams and different biological fluids.