COVID-19 Vaccine Hesitancy—A Scoping Review of Literature in High-Income Countries
Abstract
:1. Introduction
2. Methodology
2.1. Protocol and Registration
2.2. Eligibility Criteria and Information Sources
2.3. Search Strategy
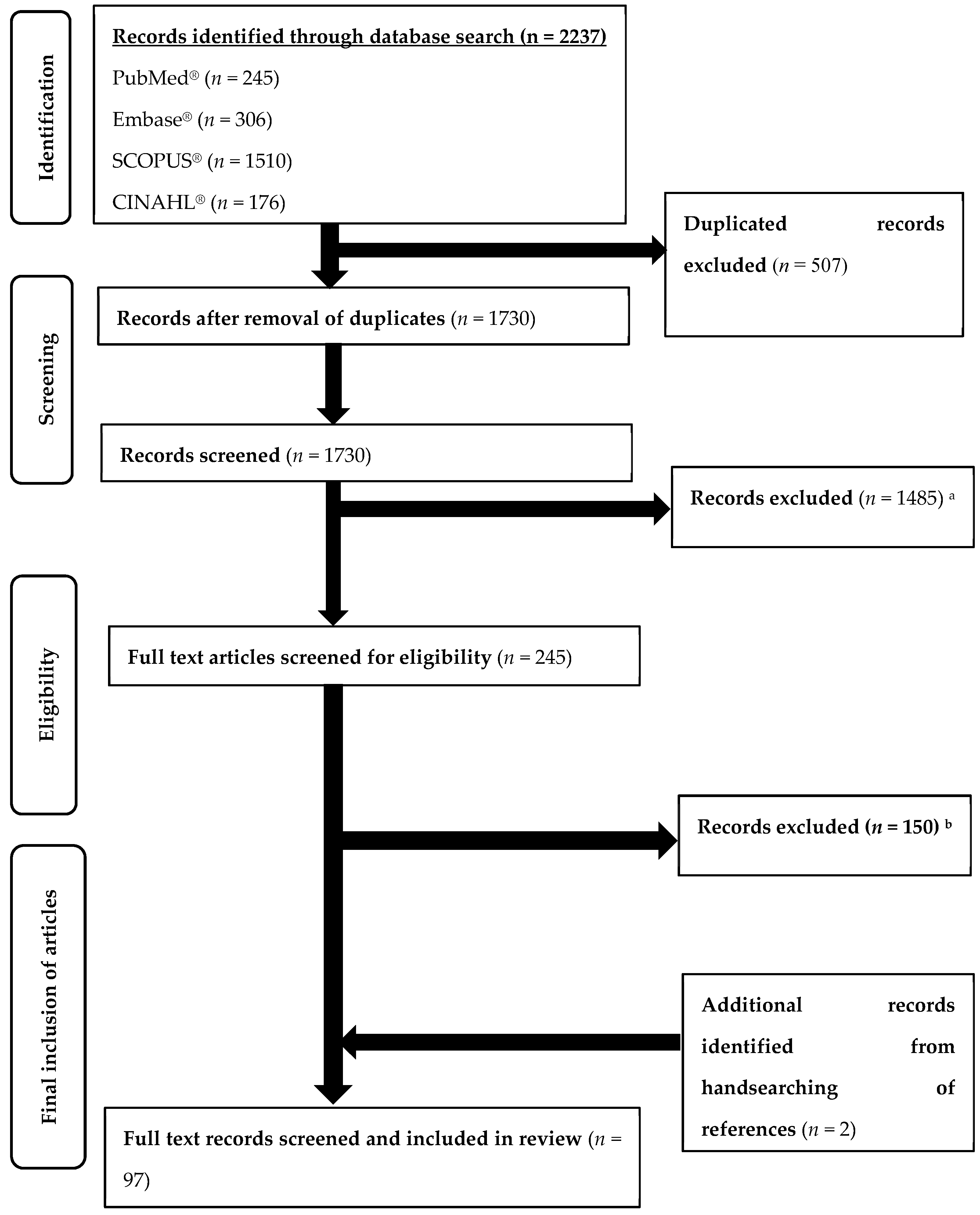
2.4. Selection of Sources of Evidence, Data Charting Process, and Data Items
2.5. Critical Appraisal of Individual Sources of Evidence
2.6. Summary and Synthesis of Results
2.7. Data Availability Statement
3. Results
3.1. Characteristics of Included Studies
3.2. Study Population
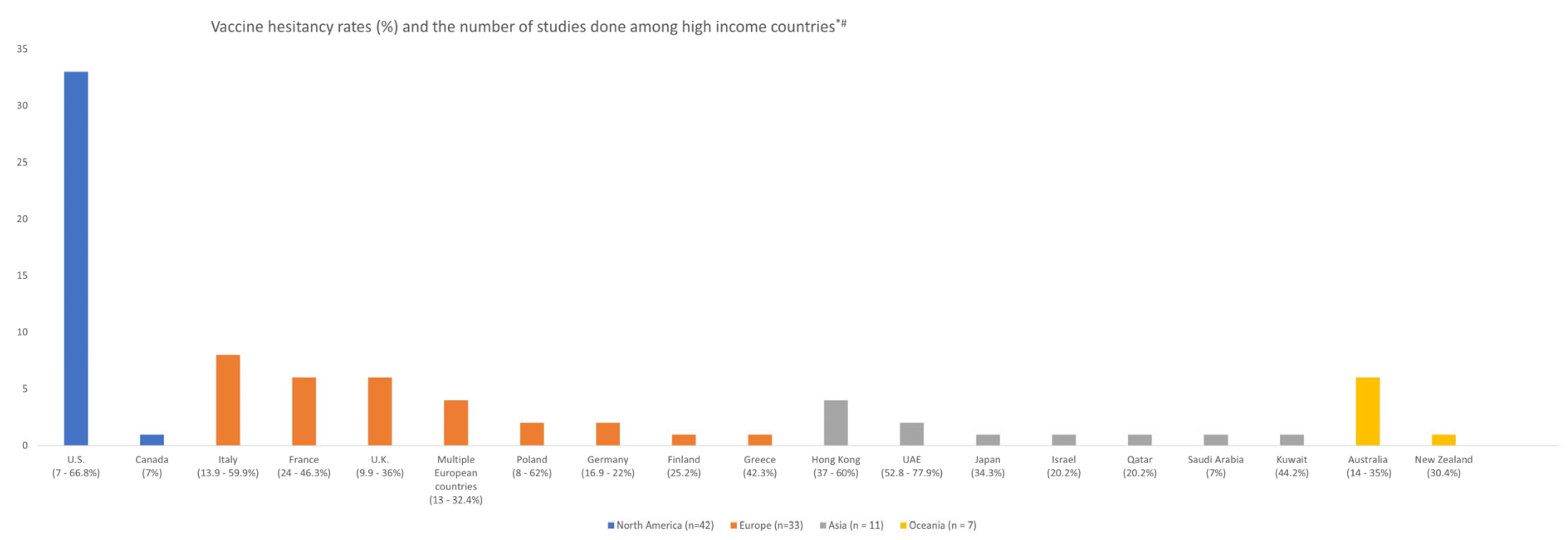
3.3. Vaccine Hesitancy Rates across Studies
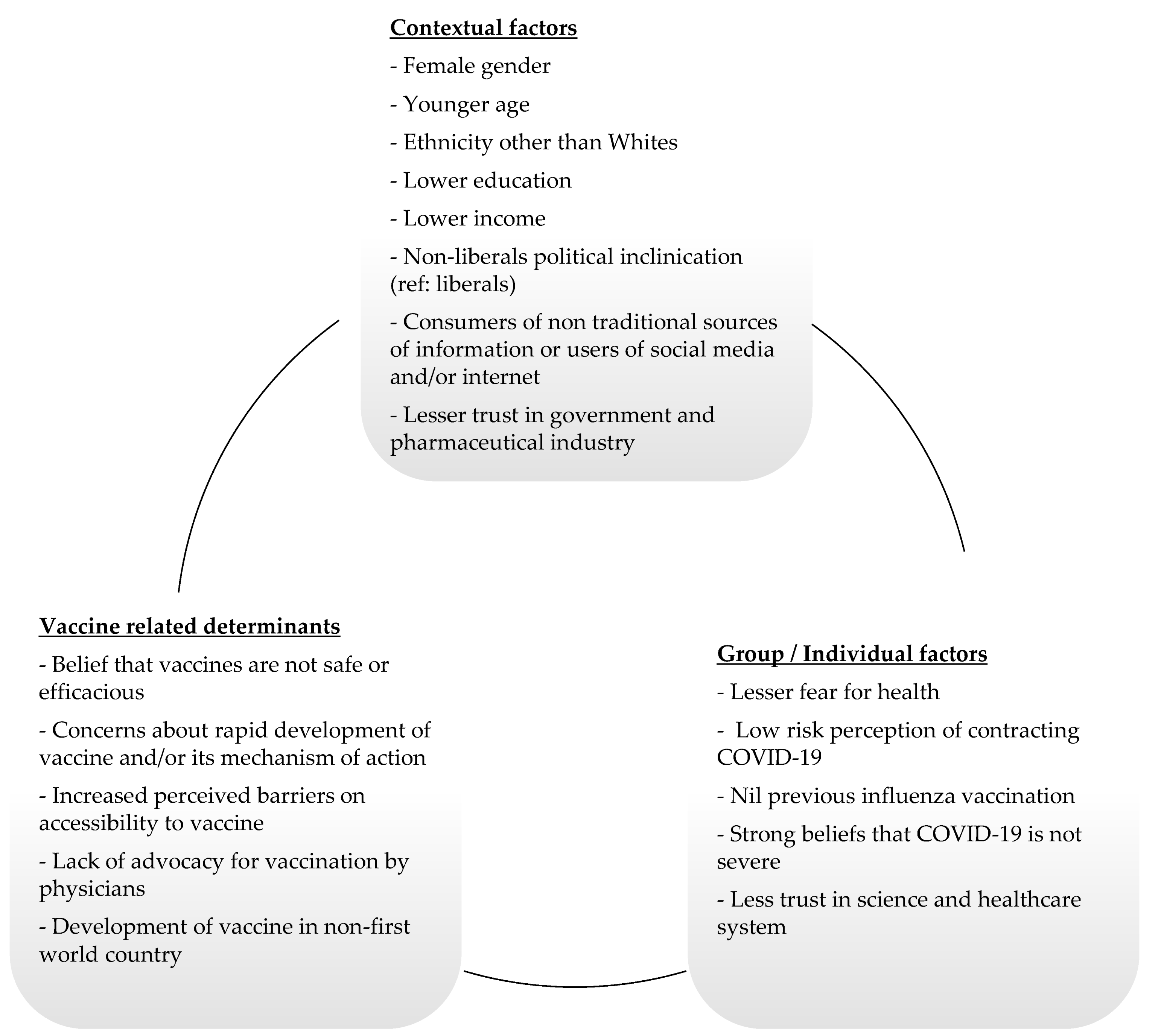
3.4. Determinants of Vaccine Hesitancy
3.4.1. Contextual Related Factors
3.4.2. Group/Individual Related Factors
3.4.3. Vaccine Related Factors
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- World Health Organization. WHO Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 24 June 2021).
- Hiscott, J.; Alexandridi, M.; Muscolini, M.; Tassone, E.; Palermo, E.; Soultsioti, M.; Zevini, A. The global impact of the coronavirus pandemic. Cytokine Growth Factor Rev. 2020, 53, 1–9. [Google Scholar] [CrossRef] [PubMed]
- World Tourism Organization. UNWTO World Tourism Barometer, May 2020—Special Focus on the Impact of COVID-19 (Summary). 2020. Available online: https://www.e-unwto.org/doi/book/10.18111/9789284421817 (accessed on 21 March 2021).
- International Labor Organization. Almost 25 Million Jobs Could Be Lost Worldwide as a Result of COVID-19, Says ILO. Available online: https://www.ilo.org/global/about-the-ilo/newsroom/news/WCMS_738742/lang--en/index.htm (accessed on 21 March 2021).
- Schoch-Spana, M.; Brunson, E.K.; Long, R.; Ruth, A.; Ravi, S.J.; Trotochaud, M.; Borio, L.; Brewer, J.; Buccina, J.; Connell, N.; et al. The public’s role in COVID-19 vaccination: Human-centered recommendations to enhance pan-demic vaccine awareness, access, and acceptance in the United States. Vaccine 2020. [Google Scholar] [CrossRef] [PubMed]
- World Health Organisation. Report of the SAGE Working Group on Vaccine Hesitancy. 2014. Available online: https://www.who.int/immunization/sage/meetings/2014/october/1_Report_WORKING_GROUP_vaccine_hesitancy_final.pdf (accessed on 27 March 2021).
- Wellcome. Wellcome Global Monitor 2018. Available online: https://wellcome.ac.uk/reports/wellcome-global-monitor/2018 (accessed on 27 March 2021).
- Bhopal, S.; Nielsen, M. Vaccine hesitancy in low- and middle-income countries: Potential implications for the COVID-19 response. Arch. Dis. Child. 2021, 106, 113–114. [Google Scholar] [CrossRef]
- World Bank Blogs. New Country Classifications by Income Level: 2019–2020. 1 July 2019. Available online: https://blogs.worldbank.org/opendata/new-country-classifications-income-level-2019-2020 (accessed on 24 March 2021).
- Arce, J.S.S.; Warren, S.S.; Meriggi, N.F.; Scacco, A.; McMurry, N.; Voors, M.; Syunyaev, G.; Malik, A.A.; Aboutajdine, S.; Adeojo, O.; et al. COVID-19 vaccine acceptance and hesitancy in low- and middle-income countries. Nat. Med. 2021, 1–10. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 Vaccine Hesitancy Worldwide: A Concise Systematic Review of Vaccine Acceptance Rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2020, 9, 16. [Google Scholar] [CrossRef]
- Smith, L.E.; Amlôt, R.; Weinman, J.A.; Yiend, J.; Rubin, G.J. A systematic review of factors affecting vaccine uptake in young children. Vaccine 2017, 35, 6059–6069. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dror, A.A.; Eisenbach, N.; Taiber, S.; Morozov, N.G.; Mizrachi, M.; Zigron, A.; Srouji, S.; Sela, E. Vaccine hesitancy: The next challenge in the fight against COVID-19. Eur. J. Epidemiol. 2020, 35, 775–779. [Google Scholar] [CrossRef]
- Anderson, R.M.; Vegvari, C.; Truscott, J.; Collyer, B.S. Challenges in creating herd immunity to SARS-CoV-2 infection by mass vaccination. Lancet 2020, 396, 1614–1616. [Google Scholar] [CrossRef]
- Larson, H.J.; Jarrett, C.; Eckersberger, E.; Smith, D.M.D.; Paterson, P. Understanding Vaccine Hesitancy around Vaccines and Vaccination from a Global Perspective: A Systematic Review of Published Literature, 2007–2012. Vaccine 2014, 32, 2150–2159. [Google Scholar] [CrossRef] [PubMed]
- Klein, J.K.; Middleman, A.B.; Quinn, J.R. 10. COVID-19 Impact on Parent/Young Adult Attitudes and Beliefs Toward Vaccines for Adolescents and Young Adults. J. Adolesc. Health 2021, 68, S6. [Google Scholar] [CrossRef]
- AlHajri, B.; Alenezi, D.; Alfouzan, H.; Altamimi, S.; Alzalzalah, S.; Almansouri, W.; Alqudeimat, Y.; Almokhaizeem, Z.; Ziyab, A.H. Willingness of parents to vaccinate their children against influenza and the novel coronavirus disease-2019. J. Pediatr. 2021, 231, 298–299. [Google Scholar] [CrossRef]
- Alabdulla, M.; Reagu, S.M.; Al-Khal, A.; Elzain, M.; Jones, R.M. COVID-19 vaccine hesitancy and attitudes in Qatar: A national cross-sectional survey of a migrant-majority population. Influenza Other Respir. Viruses 2021, 15, 361–370. [Google Scholar] [CrossRef] [PubMed]
- Beesley, R.P.; Costello, W.; Angevare, S.P.; Wouters, C.; Wulffraat, N.; Uziel, Y. Survey of adult and paediatric rheumatology patients suggests information about COVID-19 vaccination will aid uptake. Rheumatology 2021, 60, 3474–3475. [Google Scholar] [CrossRef] [PubMed]
- Pogue, K.; Jensen, J.L.; Stancil, C.K.; Ferguson, D.G.; Hughes, S.J.; Mello, E.J.; Burgess, R.; Berges, B.K.; Quaye, A.; Poole, B.D. Influences on Attitudes Regarding Potential COVID-19 Vaccination in the United States. Vaccines 2020, 8, 582. [Google Scholar] [CrossRef] [PubMed]
- Bell, S.; Clarke, R.; Mounier-Jack, S.; Walker, J.L.; Paterson, P. Parents’ and guardians’ views on the acceptability of a future COVID-19 vaccine: A multi-methods study in England. Vaccine 2020, 38, 7789–7798. [Google Scholar] [CrossRef]
- Goldman, R.D.; Marneni, S.R.; Seiler, M.; Brown, J.C.; Klein, E.J.; Cotanda, C.P.; Gelernter, R.; Yan, T.D.; Hoeffe, J.; Davis, A.L.; et al. Caregivers’ Willingness to Accept Expedited Vaccine Research During the COVID-19 Pandemic: A Cross-sectional Survey. Clin. Ther. 2020, 42, 2124–2133. [Google Scholar] [CrossRef]
- Goldman, R.D.; Yan, T.D.; Seiler, M.; Cotanda, C.P.; Brown, J.C.; Klein, E.J.; Hoeffe, J.; Gelernter, R.; Hall, J.E.; Davis, A.L.; et al. Caregiver willingness to vaccinate their children against COVID-19: Cross sectional survey. Vaccine 2020, 38, 7668–7673. [Google Scholar] [CrossRef]
- Benham, J.L.; Lang, R.; Burns, K.K.; MacKean, G.; Léveillé, T.; McCormack, B.; Sheikh, H.; Fullerton, M.M.; Tang, T.; Boucher, J.-C.; et al. Attitudes, current behaviours and barriers to public health measures that reduce COVID-19 transmission: A qualitative study to inform public health messaging. PLoS ONE 2021, 16, e0246941. [Google Scholar] [CrossRef]
- Momplaisir, F.; Haynes, N.; Nkwihoreze, H.; Nelson, M.; Werner, R.M.; Jemmott, J. Understanding Drivers of COVID-19 Vaccine Hesitancy Among Blacks. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2021. [Google Scholar] [CrossRef]
- Peretti-Watel, P.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Fressard, L.; Beck, F.; Legleye, S.; L’Haridon, O.; et al. A future vaccination campaign against COVID-19 at risk of vaccine hesitancy and politicisation. Lancet Infect. Dis. 2020, 20, 769–770. [Google Scholar] [CrossRef]
- Attwell, K.; Lake, J.; Sneddon, J.; Gerrans, P.; Blyth, C.; Lee, J. Converting the maybes: Crucial for a successful COVID-19 vaccination strategy. PLoS ONE 2021, 16, e0245907. [Google Scholar] [CrossRef]
- Barrière, J.; Gal, J.; Hoch, B.; Cassuto, O.; Leysalle, A.; Chamorey, E.; Borchiellini, D. Acceptance of SARS-CoV-2 vaccination among French patients with cancer: A cross-sectional survey. Ann. Oncol. 2021, 32, 673–674. [Google Scholar] [CrossRef]
- Callaghan, T.; Moghtaderi, A.; Lueck, J.A.; Hotez, P.; Strych, U.; Dor, A.; Fowler, E.F.; Motta, M. Correlates and disparities of intention to vaccinate against COVID-19. Soc. Sci. Med. 2021, 272, 113638. [Google Scholar] [CrossRef]
- Detoc, M.; Bruel, S.; Frappe, P.; Tardy, B.; Botelho-Nevers, E.; Gagneux-Brunon, A. Intention to participate in a COVID-19 vaccine clinical trial and to get vaccinated against COVID-19 in France during the pandemic. Vaccine 2020, 38, 7002–7006. [Google Scholar] [CrossRef]
- Feleszko, W.; Lewulis, P.; Czarnecki, A.; Waszkiewicz, P. Flattening the Curve of COVID-19 Vaccine Rejection—An International Overview. Vaccines 2021, 9, 44. [Google Scholar] [CrossRef]
- Freeman, D.; Loe, B.S.; Chadwick, A.; Vaccari, C.; Waite, F.; Rosebrock, L.; Jenner, L.; Petit, A.; Lewandowsky, S.; Vanderslott, S.; et al. COVID-19 vaccine hesitancy in the UK: The Oxford coronavirus explanations, attitudes, and narratives survey (Oceans) II. Psychol. Med. 2020, 1–15. [Google Scholar] [CrossRef]
- Gagneux-Brunon, A.; Detoc, M.; Bruel, S.; Tardy, B.; Rozaire, O.; Frappe, P.; Botelho-Nevers, E. Intention to get vaccinations against COVID-19 in French healthcare workers during the first pandemic wave: A cross-sectional survey. J. Hosp. Infect. 2021, 108, 168–173. [Google Scholar] [CrossRef] [PubMed]
- Grüner, S.; Krüger, F. The intention to be vaccinated against COVID-19: Stated preferences before vaccines were available. Appl. Econ. Lett. 2020, 1–5. [Google Scholar] [CrossRef]
- Hursh, S.R.; Strickland, J.C.; Schwartz, L.P.; Reed, D.D. Quantifying the Impact of Public Perceptions on Vaccine Acceptance Using Behavioral Economics. Front. Public Health 2020, 8, 608852. [Google Scholar] [CrossRef]
- Karlsson, L.C.; Soveri, A.; Lewandowsky, S.; Karlsson, L.; Karlsson, H.; Nolvi, S.; Karukivi, M.; Lindfelt, M.; Antfolk, J. Fearing the disease or the vaccine: The case of COVID-19. Personal. Individ. Differ. 2021, 172, 110590. [Google Scholar] [CrossRef]
- Khubchandani, J.; Sharma, S.; Price, J.H.; Wiblishauser, M.J.; Sharma, M.; Webb, F.J. COVID-19 Vaccination Hesitancy in the United States: A Rapid National Assessment. J. Community Health 2021, 46, 270–277. [Google Scholar] [CrossRef]
- Kociolek, L.K.; Elhadary, J.; Jhaveri, R.; Patel, A.B.; Stahulak, B.; Cartland, J. Coronavirus disease 2019 vaccine hesitancy among children’s hospital staff: A single-center survey. Infect. Control Hosp. Epidemiol. 2021, 2021, 1–3. [Google Scholar] [CrossRef]
- Kreps, S.; Prasad, S.; Brownstein, J.S.; Hswen, Y.; Garibaldi, B.T.; Zhang, B.; Kriner, D.L. Factors Associated With US Adults’ Likelihood of Accepting COVID-19 Vaccination. JAMA Netw. Open 2020, 3, e2025594. [Google Scholar] [CrossRef] [PubMed]
- Kuter, B.J.; Browne, S.; Momplaisir, F.M.; Feemster, K.A.; Shen, A.K.; Green-McKenzie, J.; Faig, W.; Offit, P.A. Perspectives on the receipt of a COVID-19 vaccine: A survey of employees in two large hospitals in Philadelphia. Vaccine 2021, 39, 1693–1700. [Google Scholar] [CrossRef] [PubMed]
- Latkin, C.A.; Dayton, L.; Yi, G.; Colon, B.; Kong, X. Mask usage, social distancing, racial, and gender correlates of COVID-19 vaccine intentions among adults in the US. PLoS ONE 2021, 16, e0246970. [Google Scholar] [CrossRef] [PubMed]
- Malik, A.A.; McFadden, S.M.; Elharake, J.; Omer, S.B. Determinants of COVID-19 vaccine acceptance in the US. EClinicalMedicine 2020, 26, 100495. [Google Scholar] [CrossRef]
- Manning, M.L.; Gerolamo, A.M.; Marino, M.A.; Hanson-Zalot, M.E.; Pogorzelska-Maziarz, M. COVID-19 vaccination readiness among nurse faculty and student nurses. Nurs. Outlook 2021. [Google Scholar] [CrossRef]
- Nguyen, K.H.; Srivastav, A.; Razzaghi, H.; Williams, W.; Lindley, M.C.; Jorgensen, C.; Abad, N.; Singleton, J.A. COVID-19 Vaccination Intent, Perceptions, and Reasons for not Vaccinating among Groups Prioritized for Early Vaccination—United States, September And December 2020. 2021. Available online: https://www.cdc.gov/vaccines/imz-managers/coverage/adultvaxview/pubs-resources/COVID-online-report2020.html (accessed on 26 January 2021).
- Priori, R.; Pellegrino, G.; Colafrancesco, S.; Alessandri, C.; Ceccarelli, F.; Di Franco, M.; Riccieri, V.; Scrivo, R.; Scavalli, A.S.; Spinelli, F.R.; et al. SARS-CoV-2 vaccine hesitancy among patients with rheumatic and musculoskeletal diseases: A message for rheumatologists. Ann. Rheum. Dis. 2021, 80, 953–954. [Google Scholar] [CrossRef]
- Reiter, P.L.; Pennell, M.L.; Katz, M.L. Acceptability of a COVID-19 vaccine among adults in the United States: How many people would get vaccinated? Vaccine 2020, 38, 6500–6507. [Google Scholar] [CrossRef]
- Ruiz, J.B.; Bell, R.A. Predictors of intention to vaccinate against COVID-19: Results of a nationwide survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef]
- Schmelz, K. Enforcement may crowd out voluntary support for COVID-19 policies, especially where trust in government is weak and in a liberal society. Proc. Natl. Acad. Sci. USA 2021, 118, e2016385118. [Google Scholar] [CrossRef] [PubMed]
- Schwarzinger, M.; Watson, V.; Arwidson, P.; Alla, F.; Luchini, S. COVID-19 vaccine hesitancy in a representative working-age population in France: A survey experiment based on vaccine characteristics. Lancet Public Health 2021, 6, e210–e221. [Google Scholar] [CrossRef]
- Shaw, J.; Stewart, T.; Anderson, K.B.; Hanley, S.; Thomas, S.J.; Salmon, D.A.; Morley, C. Assessment of U.S. Health Care Personnel (HCP) Attitudes towards COVID-19 Vaccination in a large University Health Care System. Clinical Infectious Diseases: An Official Publication of the Infectious Diseases Society of America. 2021. Available online: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciab054/6118651 (accessed on 21 March 2021).
- Shekhar, R.; Sheikh, A.; Upadhyay, S.; Singh, M.; Kottewar, S.; Mir, H.; Barrett, E.; Pal, S. COVID-19 Vaccine Acceptance among Health Care Workers in the United States. Vaccines 2021, 9, 119. [Google Scholar] [CrossRef] [PubMed]
- Sherman, S.M.; Smith, L.E.; Sim, J.; Amlôt, R.; Cutts, M.; Dasch, H.; Rubin, G.J.; Sevdalis, N. COVID-19 vaccination intention in the UK: Results from the COVID-19 vaccination acceptability study (CoVAccS), a nationally representative cross-sectional survey. Hum. Vaccines Immunother. 2021, 17, 1612–1621. [Google Scholar] [CrossRef]
- Szilagyi, P.G.; Thomas, K.; Shah, M.D.; Vizueta, N.; Cui, Y.; Vangala, S.; Kapteyn, A. National Trends in the US Public’s Likelihood of Getting a COVID-19 Vaccine—1 April to 8 December 2020. JAMA 2021, 325, 396. [Google Scholar] [CrossRef]
- Unroe, K.T.; Evans, R.; Weaver, L.; Rusyniak, D.; Blackburn, J. Willingness of Long-Term Care Staff to Receive a COVID-19 Vaccine: A Single State Survey. J. Am. Geriatr. Soc. 2021, 69, 593–599. [Google Scholar] [CrossRef]
- Verger, P.; Scronias, D.; Dauby, N.; Adedzi, K.A.; Gobert, C.; Bergeat, M.; Gagneur, A.; Dubé, E. Attitudes of healthcare workers towards COVID-19 vaccination: A survey in France and French-speaking parts of Belgium and Canada, 2020. Eurosurveillance 2021, 26, 2002047. [Google Scholar] [CrossRef]
- Wang, K.; Wong, E.L.Y.; Ho, K.F.; Cheung, A.W.L.; Chan, E.Y.Y.; Yeoh, E.K.; Wong, S.Y.S. Intention of nurses to accept coronavirus disease 2019 vaccination and change of intention to accept seasonal influenza vaccination during the coronavirus disease 2019 pandemic: A cross-sectional survey. Vaccine 2020, 38, 7049–7056. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Wong, E.L.Y.; Ho, K.-F.; Cheung, A.W.L.; Yau, P.S.Y.; Dong, D.; Wong, S.Y.S.; Yeoh, E.-K. Change of willingness to accept COVID-19 vaccine and reasons of vaccine hesitancy of working people at different waves of local epidemic in Hong Kong, China: Repeated cross-sectional surveys. Vaccines 2021, 9, 62. [Google Scholar] [CrossRef]
- Ward, J.K.; Alleaume, C.; Peretti-Watel, P.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Beck, F.; Legleye, S.; et al. The French public’s attitudes to a future COVID-19 vaccine: The politicization of a public health issue. Soc. Sci. Med. 2020, 265, 113414. [Google Scholar] [CrossRef] [PubMed]
- Yoda, T.; Katsuyama, H. Willingness to Receive COVID-19 Vaccination in Japan. Vaccines 2021, 9, 48. [Google Scholar] [CrossRef]
- Al-Mohaithef, M.; Padhi, B.K. Determinants of COVID-19 Vaccine Acceptance in Saudi Arabia: A Web-Based National Survey. J. Multidiscip. Health 2020, 13, 1657–1663. [Google Scholar] [CrossRef] [PubMed]
- Caban-Martinez, A.J.; Silvera, C.A.; Santiago, K.M.; Louzado-Feliciano, P.; Burgess, J.L.; Smith, D.L.; Jahnke, S.; Horn, G.P.; Graber, J.M. COVID-19 Vaccine Acceptability among U.S. Firefighters and Emergency Medical Services Workers: A Cross-Sectional Study. J. Occup. Environ. Med. 2021, 63, 369. [Google Scholar] [CrossRef] [PubMed]
- Dodd, R.H.; Cvejic, E.; Bonner, C.; Pickles, K.; McCaffery, K.J.; Ayre, J.; Batcup, C.; Copp, T.; Cornell, S.; Dakin, T.; et al. Willingness to vaccinate against COVID-19 in Australia. Lancet Infect. Dis. 2021, 21, 318–319. [Google Scholar] [CrossRef]
- Faasse, K.; Newby, J. Public Perceptions of COVID-19 in Australia: Perceived Risk, Knowledge, Health-Protective Behaviors, and Vaccine Intentions. Front. Psychol. 2020, 11, 551004. [Google Scholar] [CrossRef]
- Fisher, K.A.; Bloomstone, S.J.; Walder, J.; Crawford, S.; Fouayzi, H.; Mazor, K.M. Attitudes toward a potential SARS-CoV-2 vaccine: A survey of US adults. Ann. Intern. Med. 2020, 173, 964–973. [Google Scholar] [CrossRef]
- Gadoth, A.; Halbrook, M.; Martin-Blais, R.; Gray, A.; Tobin, N.H.; Ferbas, K.G.; Aldrovandi, G.M.; Rimoin, A.W. Cross-sectional assessment of COVID-19 vaccine acceptance among health care workers in Los Angeles. Ann. Intern. Med. 2021. [Google Scholar] [CrossRef]
- Head, K.J.; Kasting, M.L.; Sturm, L.A.; Hartsock, J.A.; Zimet, G.D. A National Survey Assessing SARS-CoV-2 Vaccination Intentions: Implications for Future Public Health Commu-nication Efforts. Sci. Commun. 2020, 42, 698–723. [Google Scholar] [CrossRef]
- La Vecchia, C.; Negri, E.; Alicandro, G.; Scarpino, V. Attitudes towards influenza vaccine and a potential COVID-19 vaccine in Italy and differences across occupational groups, September 2020. Med. Lav. 2020, 111, 445–448. [Google Scholar]
- McPhedran, R.; Toombs, B. Efficacy or delivery? An online Discrete Choice Experiment to explore preferences for COVID-19 vaccines in the UK. Econ. Lett. 2021, 200, 109747. [Google Scholar] [CrossRef]
- Mercadante, A.R.; Law, A.V. Will they, or Won’t they? Examining patients’ vaccine intention for flu and COVID-19 using the Health Belief Model. Res. Soc. Adm. Pharm. 2021, 17, 1596–1605. [Google Scholar] [CrossRef]
- Romer, D.; Jamieson, K.H. Conspiracy theories as barriers to controlling the spread of COVID-19 in the U.S. Soc. Sci. Med. 2020, 263, 113356. [Google Scholar] [CrossRef] [PubMed]
- Seale, H.; Heywood, A.E.; Leask, J.; Sheel, M.; Durrheim, D.N.; Bolsewicz, K.; Kaur, R. Examining Australian public perceptions and behaviors towards a future COVID-19 vaccine. BMC Infect. Dis. 2021, 21, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Amin, D.P.; Palter, J.S. COVID-19 vaccination hesitancy among healthcare personnel in the emergency department de-serves con-tinued attention. Am. J. Emerg. Med. 2021. [Google Scholar] [CrossRef] [PubMed]
- Largent, E.A.; Persad, G.; Sangenito, S.; Glickman, A.; Boyle, C.; Emanuel, E.J. US Public Attitudes Toward COVID-19 Vaccine Mandates. JAMA Netw. Open 2020, 3, e2033324. [Google Scholar] [CrossRef] [PubMed]
- Olagoke, A.A.; Olagoke, O.; Hughes, A.M. Intention to Vaccinate Against the Novel 2019 Coronavirus Disease: The Role of Health Locus of Control and Religiosity. J. Relig. Health 2021, 60, 65–80. [Google Scholar] [CrossRef]
- KFF/The Undefeated Survey on Race and Health. 2020. Available online: https://www.kff.org/racial-equity-and-health-policy/report/kff-the-undefeated-survey-on-race-and-health/ (accessed on 1 May 2021).
- Alley, S.J.; Stanton, R.; Browne, M.; To, Q.G.; Khalesi, S.; Williams, S.L.; Thwaite, T.L.; Fenning, A.S.; Vandelanotte, C. As the Pandemic Progresses, How Does Willingness to Vaccinate against COVID-19 Evolve? Int. J. Environ. Res. Public Health 2021, 18, 797. [Google Scholar] [CrossRef]
- Bogart, L.M.; Ojikutu, B.O.; Tyagi, K.; Klein, D.J.; Mutchler, M.G.; Dong, L.; Lawrence, S.J.; Thomas, D.R.; Kellman, S. COVID-19 Related Medical Mistrust, Health Impacts, and Potential Vaccine Hesitancy Among Black Americans Living With HIV. JAIDS J. Acquir. Immune Defic. Syndr. 2021, 86, 200–207. [Google Scholar] [CrossRef]
- Campochiaro, C.; Trignani, G.; Tomelleri, A.; Cascinu, S.; Dagna, L. Potential acceptance of COVID-19 vaccine in rheumatological patients: A monocentric comparative survey. Ann. Rheum. Dis. 2021, 80, 816–817. [Google Scholar] [CrossRef]
- Ehde, D.M.; Roberts, M.K.; Herring, T.E.; Alschuler, K.N. Willingness to obtain COVID-19 vaccination in adults with multiple sclerosis in the United States. Mult. Scler. Relat. Disord. 2021, 49, 102788. [Google Scholar] [CrossRef]
- Niankara, I.; Muqattash, R.; Niankara, A.; Traoret, R.I. COVID-19 Vaccine Development in a Quadruple Helix Innovation System: Uncovering the Preferences of the Fourth Helix in the UAE. J. Open Innov. Technol. Mark. Complex. 2020, 6, 132. [Google Scholar] [CrossRef]
- Williams, L.; Flowers, P.; McLeod, J.; Young, D.; Rollins, L.; The Catalyst Project Team. Social Patterning and Stability of Intention to Accept a COVID-19 Vaccine in Scotland: Will Those Most at Risk Accept a Vaccine? Vaccines 2021, 9, 17. [Google Scholar] [CrossRef]
- Murphy, J.; Vallières, F.; Bentall, R.P.; Shevlin, M.; McBride, O.; Hartman, T.K.; McKay, R.; Bennett, K.; Mason, L.; Gibson-Miller, J.; et al. Psychological characteristics associated with COVID-19 vaccine hesitancy and resistance in Ireland and the United Kingdom. Nat. Commun. 2021, 12, 1–15. [Google Scholar] [CrossRef]
- Guidry, J.P.; Laestadius, L.I.; Vraga, E.K.; Miller, C.A.; Perrin, P.B.; Burton, C.W.; Ryan, M.; Fuemmeler, B.F.; Carlyle, K.E. Willingness to get the COVID-19 vaccine with and without emergency use authorization. Am. J. Infect. Control 2021, 49, 137–142. [Google Scholar] [CrossRef]
- Jeffs, E.; Lucas, N.; Walls, T. CoVID-19: Parent and caregiver concerns about reopening New Zealand schools. J. Paediatr. Child Health 2021, 57, 403–408. [Google Scholar] [CrossRef] [PubMed]
- Muqattash, R.; Niankara, I.; Traoret, R.I. Survey data for COVID-19 vaccine preference analysis in the United Arab Emirates. Data Brief 2020, 33, 106446. [Google Scholar] [CrossRef] [PubMed]
- Underschultz, J.G.; Barber, P.; Richard, D.; Hillier, T. What drives resistance to public health measures in Canada’s COVID-19 pandemic? An online survey of Canadians’ knowledge, attitudes, and practices. Univ. Tor. Med. J. 2021, 98, 35–40. [Google Scholar]
- Hoke, A.M.; Keller, C.M.; Calo, W.A.; Sekhar, D.L.; Lehman, E.B.; Kraschnewski, J.L. School Nurse Perspectives on COVID-19. J. Sch. Nurs. 2021, 37, 292–297. [Google Scholar] [CrossRef]
- Taylor, S.; Landry, C.A.; Paluszek, M.M.; Groenewoud, R.; Rachor, G.S.; Asmundson, G.J. A proactive approach for managing COVID-19: The importance of understanding the motivational roots of vaccination hesitancy for SARS-CoV2. Front. Psychol. 2020, 11, 2890. [Google Scholar] [CrossRef]
- Wong, M.C.; Wong, E.L.; Huang, J.; Cheung, A.W.; Law, K.; Chong, M.K.; Ng, R.W.; Lai, C.K.; Boon, S.S.; Lau, J.T.; et al. Acceptance of the COVID-19 vaccine based on the health belief model: A population-based survey in Hong Kong. Vaccine 2021, 39, 1148–1156. [Google Scholar] [CrossRef]
- Kwok, K.O.; Li, K.-K.; Wei, W.I.; Tang, A.; Wong, S.Y.S.; Lee, S.S. Influenza vaccine uptake, COVID-19 vaccination intention and vaccine hesitancy among nurses: A survey. Int. J. Nurs. Stud. 2021, 114, 103854. [Google Scholar] [CrossRef] [PubMed]
- Sprengholz, P.; Eitze, S.; Felgendreff, L.; Korn, L.; Betsch, C. Money is not everything: Experimental evidence that payments do not increase willingness to be vaccinated against COVID-19. J. Med. Ethics 2021, 47, 547–548. [Google Scholar] [CrossRef] [PubMed]
- Bokemper, S.E.; Huber, G.A.; Gerber, A.S.; James, E.K.; Omer, S.B. Timing of COVID-19 vaccine approval and endorsement by public figures. Vaccine 2021, 39, 825–829. [Google Scholar] [CrossRef] [PubMed]
- Lucia, V.C.; Kelekar, A.; Afonso, N.M. COVID-19 vaccine hesitancy among medical students. J. Public Health 2020, fdaa230. [Google Scholar] [CrossRef] [PubMed]
- Prati, G. Intention to receive a vaccine against SARS-CoV-2 in Italy and its association with trust, worry and beliefs about the origin of the virus. Health Educ. Res. 2020, 35, 505–511. [Google Scholar] [CrossRef] [PubMed]
- Williams, L.; Gallant, A.J.; Rasmussen, S.; Nicholls, L.A.B.; Cogan, N.; Deakin, K.; Young, D.; Flowers, P. Towards intervention development to increase the uptake of COVID-19 vaccination among those at high risk: Outlining evidence-based and theoretically informed future intervention content. Br. J. Health Psychol. 2020, 25, 1039–1054. [Google Scholar] [CrossRef] [PubMed]
- Chu, H.; Liu, S. Integrating health behavior theories to predict American’s intention to receive a COVID-19 vaccine. Patient Educ. Couns. 2021, 104, 1878–1886. [Google Scholar] [CrossRef]
- Palamenghi, L.; Barello, S.; Boccia, S.; Graffigna, G. Mistrust in biomedical research and vaccine hesitancy: The forefront challenge in the battle against COVID-19 in Italy. Eur. J. Epidemiol. 2020, 35, 785–788. [Google Scholar] [CrossRef]
- Kourlaba, G.; Kourkouni, E.; Maistreli, S.; Tsopela, C.-G.; Molocha, N.-M.; Triantafyllou, C.; Koniordou, M.; Kopsidas, I.; Chorianopoulou, E.; Maroudi-Manta, S.; et al. Willingness of Greek general population to get a COVID-19 vaccine. Glob. Health Res. Policy 2021, 6, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Barello, S.; Nania, T.; Dellafiore, F.; Graffigna, G.; Caruso, R. ‘Vaccine hesitancy’ among university students in Italy during the COVID-19 pandemic. Eur. J. Epidemiol. 2020, 35, 781–783. [Google Scholar] [CrossRef] [PubMed]
- Jung, H.; Albarracín, D. Concerns for others increases the likelihood of vaccination against influenza and COVID-19 more in sparsely rather than densely populated areas. Proc. Natl. Acad. Sci. USA 2021, 118, 118. [Google Scholar] [CrossRef] [PubMed]
- Caserotti, M.; Girardi, P.; Rubaltelli, E.; Tasso, A.; Lotto, L.; Gavaruzzi, T. Associations of COVID-19 risk perception with vaccine hesitancy over time for Italian residents. Soc. Sci. Med. 2021, 272, 113688. [Google Scholar] [CrossRef] [PubMed]
- Graffigna, G.; Palamenghi, L.; Boccia, S.; Barello, S. Relationship between Citizens’ Health Engagement and Intention to Take the COVID-19 Vaccine in Italy: A Me-diation Analysis. Vaccines 2020, 8, 576. [Google Scholar] [CrossRef] [PubMed]
- Freeman, D.; Waite, F.; Rosebrock, L.; Petit, A.; Causier, C.; East, A.; Jenner, L.; Teale, A.-L.; Carr, L.; Mulhall, S.; et al. Coronavirus conspiracy beliefs, mistrust, and compliance with government guidelines in England. Psychol. Med. 2020, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Hughes, S.; Machan, L. It’s a conspiracy: Covid-19 conspiracies link to psychopathy, Machiavellianism and collective narcissism. Pers. Individ. Differ. 2021, 171, 110559. [Google Scholar] [CrossRef]
- Neumann-Böhme, S.; Varghese, N.E.; Sabat, I.; Barros, P.P.; Brouwer, W.; Van Exel, J.; Schreyögg, J.; Stargardt, T. Once we have it, will we use it? A European survey on willingness to be vaccinated against COVID-19. Eur. J. Health Econ. 2020, 21, 977–982. [Google Scholar] [CrossRef]
- Szmyd, B.; Bartoszek, A.; Karuga, F.F.; Staniecka, K.; Błaszczyk, M.; Radek, M. Medical students and SARS-CoV-2 vaccination: Attitude and behaviors. Vaccines 2021, 9, 128. [Google Scholar] [CrossRef] [PubMed]
- Loomba, S.; de Figueiredo, A.; Piatek, S.J.; de Graaf, K.; Larson, H.J. Measuring the impact of COVID-19 vaccine misinformation on vaccination intent in the UK and USA. Nat. Hum. Behav. 2021, 5, 337–348. [Google Scholar] [CrossRef]
- Borriello, A.; Master, D.; Pellegrini, A.; Rose, J.M. Preferences for a COVID-19 vaccine in Australia. Vaccine 2021, 39, 473–479. [Google Scholar] [CrossRef]
- Motta, M. Can a COVID-19 vaccine live up to Americans’ expectations? A conjoint analysis of how vaccine characteristics influence vaccination intentions. Soc. Sci. Med. 2021, 272, 113642. [Google Scholar] [CrossRef] [PubMed]
- Boulton, M.L.; Carlson, B.F.; Power, L.E.; Wagner, A.L. Socioeconomic factors associated with full childhood vaccination in Bangladesh, 2014. Int. J. Infect. Dis. 2018, 69, 35–40. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wiysonge, C.S.; Uthman, O.A.; Ndumbe, P.M.; Hussey, G.D. Individual and Contextual Factors Associated with Low Childhood Immunisation Coverage in Sub-Saharan Africa: A Multilevel Analysis. PLoS ONE 2012, 7, e37905. [Google Scholar] [CrossRef] [Green Version]
- Crocker-Buque, T.; Mindra, G.; Duncan, R.; Mounier-Jack, S. Immunization, urbanization and slums—A systematic review of factors and interventions. BMC Public Health 2017, 17, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Dror, A.A.; Daoud, A.; Morozov, N.G.; Layous, E.; Eisenbach, N.; Mizrachi, M.; Rayan, D.; Bader, A.; Francis, S.; Kaykov, E.; et al. Vaccine hesitancy due to vaccine country of origin, vaccine technology, and certification. Eur. J. Epidemiol. 2021, 2021, 1–6. [Google Scholar] [CrossRef]
- Richie, H.; Ortiz-Ospina, E.; Beltekian, D.; Methieu, E.; Hasell, J.; Macdonald, B.; Giattino, C.; Appel, C.; Rodes-Guirao, L.; Roser, M. Coronavirus (COVID-19) Vaccinations Statistics and Research. 2021. Available online: https://ourworldindata.org/covid-vaccinations (accessed on 16 May 2021).
- Sallam, M.; Dababseh, D.; Yaseen, A.; Al-Haidar, A.; Taim, D.; Eid, H.; Ababneh, N.A.; Bakri, F.G.; Mahafzah, A. COVID-19 misinformation: Mere harmless delusions or much more? A knowledge and attitude cross-sectional study among the general public residing in Jordan. PLoS ONE 2020, 15, e0243264. [Google Scholar] [CrossRef]
- Mohan, S.; Reagu, S.; Lindow, S.; Alabdulla, M. COVID-19 vaccine hesitancy in perinatal women: A cross sectional survey. J. Périnat. Med. 2021, 49, 678–685. [Google Scholar] [CrossRef]
- Editorial, A.B. Why Millennials and Gen. Z Aren’t Getting Vaccinated—and What to Do about It. Available online: https://www.advisory.com/en/daily-briefing/2021/04/26/vaccine-hesitancy (accessed on 16 May 2021).
- Bogart, L.M.; Dong, L.; Gandhi, P.; Ryan, S.; Smith, T.L.; Klein, D.J.; Fuller, L.-A.; Ojikutu, B.O. What Contributes to COVID-19 Vaccine Hesitancy in Black Communities, and How Can It Be Addressed? RAND Corporation: Santa Monica, CA, USA, 2021. [Google Scholar]
- Edwards, B.; Biddle, N.; Gray, M.; Sollis, K. COVID-19 vaccine hesitancy and resistance: Correlates in a nationally representative longitudinal survey of the Australian population. PLoS ONE 2021, 16, e0248892. [Google Scholar] [CrossRef]
- Shore, D.A. Communicating in times of uncertainty: The need for trust. J. Health Commun. 2003, 8, 13–14. [Google Scholar] [CrossRef] [PubMed]
- Wouters, O.J.; Shadlen, K.C.; Salcher-Konrad, M.; Pollard, A.J.; Larson, H.J.; Teerawattananon, Y.; Jit, M. Challenges in ensuring global access to COVID-19 vaccines: Production, affordability, allocation, and deployment. Lancet 2021, 397, 1023–1034. [Google Scholar] [CrossRef]
- Mathieu, E.; Ritchie, H.; Ortiz-Ospina, E.; Roser, M.; Hasell, J.; Appel, C.; Giattino, C. A global database of COVID-19 vaccinations. Nat. Hum. Behav. 2021, 1–7. [Google Scholar] [CrossRef]
- Bartsch, S.M.; O’Shea, K.J.; Ferguson, M.C.; Bottazzi, M.E.; Wedlock, P.T.; Strych, U.; McKinnell, J.A.; Siegmund, S.S.; Cox, S.N.; Hotez, P.J.; et al. Vaccine efficacy needed for a COVID-19 coronavirus vaccine to prevent or stop an epidemic as the sole intervention. Am. J. Prev. Med. 2020, 59, 493–503. [Google Scholar] [CrossRef]
- Morgul, E.; Bener, A.; Atak, M.; Akyel, S.; Aktaş, S.; Bhugra, D.; Ventriglio, A.; Jordan, T.R. COVID-19 pandemic and psychological fatigue in Turkey. Int. J. Soc. Psychiatry 2021, 67, 128–135. [Google Scholar] [CrossRef]
- Webber-Ritchey, K.J.; Simonovich, S.D.; Spurlark, R.S. COVID-19: Qualitative Research With Vulnerable Populations. Nurs. Sci. Q. 2021, 34, 13–19. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, S.; Castiglione, S.; Audet, L.-A.; Desmarais, M.; Horace, M.; Peláez, S. Conducting Qualitative Research to Respond to COVID-19 Challenges: Reflections for the Present and Beyond. Int. J. Qual. Methods 2021, 20. [Google Scholar] [CrossRef]
- Wright, K.B. Researching Internet-Based Populations: Advantages and Disadvantages of Online Survey Research, Online Question-naire Authoring Software Packages, and Web Survey Services. J. Comput. Mediat. Commun. 2017, 10, JCMC1034. [Google Scholar] [CrossRef]
- Eysenbach, G. Improving the quality of Web surveys: The Checklist for Reporting Results of Internet E-Surveys (CHER-RIES). J. Med. Internet Res. 2004, 6, e34. [Google Scholar] [CrossRef]
- McCaffery, K.J.; Dodd, R.H.; Cvejic, E.; Ayrek, J.; Isautier, J.M.; Copp, T.; Bonner, C.; Pickles, K.; Nickel, B.; Dakin, T.; et al. Health literacy and disparities in COVID-19–related knowledge, attitudes, beliefs and behaviours in Australia. Public Health Res. Pract. 2020, 30, 30342012. [Google Scholar] [CrossRef]
| Variables | n (%) |
|---|---|
| Year of study | |
| 2019 | 0 (0) |
| 2020 | 48 (49.5) |
| 2021 | 49 (50.5) |
| Continent of study | |
| North America | 42 (43.3) |
| Europe | 33 (34) |
| Asia | 11 (11.3) |
| Oceania | 7 (7.2) |
| Cross-continents | 4 (4.1) |
| Country of study | |
| USA | 39 (40.2) |
| Italy | 9 (9.3) |
| Multiple countries | 9 (9.3) |
| Australia | 6 (6.2) |
| France | 6 (6.2) |
| Hong Kong | 4 (4.1) |
| U.K. | 8 (8.2) |
| Germany | 2 (2.1) |
| Poland | 2 (2.1) |
| UAE | 2 (2.1) |
| Canada | 2 (2.1) |
| Other countries a | 8 (8.2) |
| Patient populations | |
| General public | 71 (73.2) |
| Healthcare workers | 13 (13.4) |
| University students and/or university staff | 5 (5.2) |
| Patients with autoimmune conditions | 3 (3.1) |
| Patients with malignancy | 1 (1) |
| Adolescents and/or children | 1 (1) |
| Others b | 3 (3.1) |
| Number of study participants | |
| 0–1000 | 28 (28.9) |
| 1001–2000 | 32 (33) |
| 2001–5000 | 25 (25.8) |
| 5001–10,000 | 11 (11.3) |
| >10,000 | 1 (1) |
| Study design | |
| Cross-sectional study | 75 (77.3) |
| Mixed methods | 14 (14.4) |
| Randomized controlled trials | 2 (2.1) |
| Pure qualitative study | 1 (1) |
| Case control study | 2 (2.1) |
| Longitudinal study | 3 (3.1) |
| Methodology of data collection # | |
| Online survey | 87 (89.7) |
| Telephone interview | 7 (7.2) |
| Paper questionnaire | 3 (3.1) |
| Face-to-face survey | 2 (2.1) |
| Focus group discussion | 2 (2.1) |
| Combinations of methods c | 5 (5.2) |
| Response rates | |
| 0–<25% | 5 (5.2) |
| 25–<50% | 7 (7.2) |
| 50–<75% | 15 (15.5) |
| 75–100% | 17 (17.5) |
| Not specified | 53 (54.6) |
| Use of validated questionnaire | |
| Yes | 26 (26.8) |
| No | 71 (73.2) |
| COVID-19 vaccine hesitancy 30% or more across continents d,e | |
| North America | 25/42 (59.5) |
| Europe | 11/33 (33.3) |
| Asia | 8/11 (72.7) |
| Oceania | 2/7 (28.6) |
| Factor | Number of Supporting Studies | References | Number of Studies Which Found no Significance | References | Number of Disagreeing Studies | References |
|---|---|---|---|---|---|---|
| Communication and media environment | ||||||
| Participants whose sources of information are mainly via social media/internet | 6 | [28,29,30,31,32,33] | 1 | [34] | 0 | |
| Lack of widely accessible information on vaccine related information | 5 | [29,35,36,37,38] | 1 | [39] | 0 | |
| Participants who are mainly users of non-traditional media (not radio, not newspapers, not television) | 3 | [30,32,34] | 1 | [33] | 0 | |
| Influential leaders, gatekeepers and anti or pro-vaccination lobbies | ||||||
| Preferences for Donald Trump endorsements of vaccination | 2 | [40,41] | 1 | [42] | 0 | |
| Preferences for Dr. Anthony Fauci pro-vaccination endorsements | 0 | 0 | 2 | [41,42] | ||
| Policies/politics | ||||||
| Political inclination: U.S. Democrats supporters | 0 | 0 | 8 | [33,40,41,43,44,45,46,47] | ||
| Political inclination: Non liberals (Far right, far left, conservative) | 8 | [40,46,48,49,50,51,52,53] | 2 | [22,54] | 0 | |
| Mandatory vaccination | 2 | [55,56] | 0 | 0 | ||
| Political inclination: Vote abstinence | 1 | [48] | 0 | 0 | ||
| Religion | ||||||
| Increased religiosity | 5 | [31,37,40,56,57] | 2 | [41,43] | 1 | [30] |
| Sociodemographic related | ||||||
| Females | 37 | [15,20,24,33,35,36,37,40,41,44,46,48,50,51,52,53,54,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75] | 12 | [22,34,38,43,76,77,78,79,80,81,82,83] | 1 | [84] |
| Younger participants | 31 | [32,35,36,37,41,46,49,53,54,56,60,63,65,66,67,68,70,71,72,73,76,78,79,83,84,85,86,87,88,89] | 12 | [15,34,50,52,58,61,74,77,81,90,91,92] | 10 | [20,30,31,43,48,57,59,75,93,94] |
| Non-whites | 24 | [23,31,32,37,40,41,45,47,49,51,52,54,64,65,68,70,71,72,78,86,87,89,93] | 6 | [22,33,50,79,84,90] | 1 | [43] |
| Lower education (below college) | 19 | [32,34,36,41,49,54,65,66,68,69,71,77,82,85,86,89,95,96,97] | 14 | [20,30,33,38,43,53,56,58,76,78,79,90,92,98] | 0 | |
| Lower income | 13 | [23,30,40,44,48,49,51,52,53,54,82,89,97] | 12 | [22,33,50,56,58,68,77,80,81,86,90,92] | 0 | |
| HCW without clinical roles (ref: HCW with clinical roles) | 7 | [15,61,64,65,70,73,87] | 0 | 2 | [67,72] | |
| Students in HC discipline (ref: students in non-HC disciplines) | 0 | 1 | [99] | 0 | ||
| Non-Asians | 4 | [66,70,71,89] | 3 | [65,79,90] | 1 | [87] |
| Presence of child at home | 3 | [15,44,54] | 4 | [30,58,84,98] | 0 | |
| Married | 2 | [54,78] | 5 | [33,38,51,92,98] | 3 | [20,75,76] |
| Geographical barriers (i.e., accessibility) | ||||||
| Rural regions (residence, place of practice) | 5 | [46,65,68,86,100] | 3 | [38,51,101] | 1 | [57] |
| Pharmaceutical/governmental motives | ||||||
| Lower trust in pharmaceutical industry | 4 | [37,41,92,102] | 0 | 0 | ||
| Lower trust in government | 3 | [20,56,79] | 0 | 0 | ||
| Others | ||||||
| Increased passage of time longitudinally in pandemic | 5 | [34,68,71,75,94] | 2 | [56,82] | 0 | |
| Participants without healthcare insurance | 3 | [52,68,84] | 0 | 0 |
| Factor | Number of Supporting Studies | References | Number of Studies Which Found no Significance | References | Number of Disagreeing Studies | References |
|---|---|---|---|---|---|---|
| Experience with past vaccination | ||||||
| History of influenza vaccination | 0 | 1 | [103] | 28 | [15,19,20,22,25,33,35,36,37,41,46,47,49,50,58,61,65,66,68,73,74,75,78,79,86,89,90,95,104] | |
| Having children with up-to-date vaccinations | 0 | 0 | 1 | [25] | ||
| Beliefs, attitudes about health and prevention | ||||||
| Lesser fear for health or worry about COVID-19 | 16 | [32,33,35,37,38,40,49,53,54,59,61,67,68,79,81,90] | 2 | [80,103] | 2 | [28,37] |
| Perception of lower risk of contracting COVID-19 | 15 | [28,43,44,49,52,54,59,61,63,81,94,96,98,104,105] | 4 | [51,55,74,92] | 1 | [69] |
| Belief that COVID-19 is not severe | 12 | [22,36,41,49,52,58,63,64,81,92,98,105] | 1 | [43] | 1 | [69] |
| Greater conspiracy beliefs | 8 | [30,32,50,54,98,106,107,108] | 1 | [80] | 0 | |
| Belief in greater efficacy of complementary alternative medicine or one’s natural immune system | 5 | [20,29,62,73,102] | 0 | 0 | ||
| Belief that COVID-19 is not a disease | 4 | [20,58,85,109] | 0 | 0 | ||
| Belief that threat of COVID-19 is exaggerated | 2 | [85,109] | 0 | 0 | ||
| Lesser compliance with COVID-19 prevention behaviors | 2 | [22,51] | 0 | 0 | ||
| Knowledge and awareness | ||||||
| Lower knowledge about COVID-19 | 4 | [38,79,85,98] | 3 | [22,37,52] | 0 | |
| Lower knowledge about vaccination | 1 | [33] | 2 | [22,37] | 0 | |
| Health-system and providers—trust and personal experience | ||||||
| Lesser trust in healthcare system | 11 | [22,30,32,50,62,68,73,92,106,107,108] | 2 | [80,81] | 0 | |
| Lesser trust in science or in scientist | 9 | [30,33,35,40,54,55,58,73,91] | 0 | 0 | ||
| Immunization as a social norm vs. not needed/harmful | ||||||
| Belief that vaccination is non-beneficial and/or unimportant | 12 | [20,31,37,43,54,68,78,90,91,92,102,105] | 0 | 0 | ||
| Belief that vaccination is a hoax/harmful | 1 | (32, 92) | 1 | [20] | 0 | |
| Humanistic traits | ||||||
| Lesser sense of collective responsibility e.g., protect loved ones, neighbors | 10 | [30,35,37,49,54,89,90,94,101,109] | 2 | [55,103] | 0 | |
| Lower self-efficacy | 4 | [31,43,54,105] | 0 | 0 | ||
| Other factors | ||||||
| No concomitant chronic diseases or not taking regular medications | 11 | [20,30,33,36,57,62,74,78,82,89,98] | 8 | [25,33,46,61,75,84,90,92] | 2 | [64,69] |
| Peers or family with previous COVID-19 infection | 0 | 4 | [22,30,46,103] | 3 | [33,67,89] | |
| Greater desire to return to normalcy | 0 | 0 | 2 | [35,37] | ||
| Previously tested for COVID-19 antibodies or do not mind testing for COVID-19 antibodies | 0 | 0 | 3 | [40,54,65] |
| Factor | Number of Supporting Studies | References | Number of Studies Which Found no Significance | References | Number of Disagreeing Studies | References |
|---|---|---|---|---|---|---|
| Risk/benefit (scientific evidence) | ||||||
| Belief that the COVID-19 vaccines are unsafe or ineffective | 24 | [20,22,29,35,36,37,40,41,43,50,52,54,55,63,68,73,88,90,94,102,103,108,110,111] | 1 | [69] | 0 | |
| Perceived duration of protection from COVID-19 vaccines to be short (one year or less) | 1 | [73] | 0 | 0 | ||
| Introduction of new vaccine/formulation | ||||||
| Concerns about rapid development, novelty, and/or mechanism of action of vaccine | 9 | [20,22,24,41,43,50,54,108,110] | 1 | [22] | 0 | |
| Mode of administration | ||||||
| Fear of needles as a route of vaccine administration | 2 | [37,111] | 0 | 0 | ||
| Reliability or source of vaccine supply | ||||||
| Vaccines developed by first world regions (US and European Union) | 0 | 0 | 3 | [22,36,110] | ||
| Vaccination schedule | ||||||
| Concerns about vaccine requiring more than one dose | 2 | [88,110] | 0 | 0 | ||
| Design of vaccination program/mode of delivery | ||||||
| Presence of perceived barriers to accessibility of vaccine (i.e., location for vaccination, time spent on transport) | 4 | [36,92,97,111] | 0 | 0 | ||
| Role of Healthcare professional | ||||||
| Lack of advocacy for COVID-19 vaccination from attending physician | 3 | [49,52,88] | 1 | [34] | 0 | |
| Costs | ||||||
| Concerns for costs of COVID-19 vaccination | 2 | [97,104] | 2 | [43,90] | 0 | |
| Availability of monetary incentives to get vaccinated | 0 | 1 | [39] | 0 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aw, J.; Seng, J.J.B.; Seah, S.S.Y.; Low, L.L. COVID-19 Vaccine Hesitancy—A Scoping Review of Literature in High-Income Countries. Vaccines 2021, 9, 900. https://doi.org/10.3390/vaccines9080900
Aw J, Seng JJB, Seah SSY, Low LL. COVID-19 Vaccine Hesitancy—A Scoping Review of Literature in High-Income Countries. Vaccines. 2021; 9(8):900. https://doi.org/10.3390/vaccines9080900
Chicago/Turabian StyleAw, Junjie, Jun Jie Benjamin Seng, Sharna Si Ying Seah, and Lian Leng Low. 2021. "COVID-19 Vaccine Hesitancy—A Scoping Review of Literature in High-Income Countries" Vaccines 9, no. 8: 900. https://doi.org/10.3390/vaccines9080900
APA StyleAw, J., Seng, J. J. B., Seah, S. S. Y., & Low, L. L. (2021). COVID-19 Vaccine Hesitancy—A Scoping Review of Literature in High-Income Countries. Vaccines, 9(8), 900. https://doi.org/10.3390/vaccines9080900






