Fear of COVID-19 and Perceived COVID-19 Infectability Supplement Theory of Planned Behavior to Explain Iranians’ Intention to Get COVID-19 Vaccinated
Abstract
:1. Introduction
2. Materials and Methods
2.1. Participants and Recruitment Procedure
2.2. Measures
2.2.1. Fear of COVID-19
2.2.2. Perceived COVID-19 Infectability
2.2.3. Perceived Behavioral Control over COVID-19 Vaccination
2.2.4. Subjective Norm of COVID-19 Vaccination
2.2.5. Attitude toward COVID-19 Vaccination
2.2.6. Intention to Get COVID-19 Vaccinated
2.3. Data Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Crayne, M.P. The traumatic impact of job loss and job search in the aftermath of COVID-19. Psychol. Trauma 2020, 12, S180–S182. [Google Scholar] [CrossRef] [PubMed]
- McIntyre, R.S.; Lee, Y. Preventing suicide in the context of the COVID-19 pandemic. World J. Psychiatry 2020, 19, 250–251. [Google Scholar] [CrossRef] [PubMed]
- Oksanen, A.; Kaakinen, M.; Latikka, R.; Savolainen, I.; Savela, N.; Koivula, A. Regulation and trust: 3-month follow-up study on COVID-19 mortality in 25 European countries. JMIR Public Health Surveill. 2020, 6, e19218. [Google Scholar] [CrossRef] [PubMed]
- Torales, J.; O’Higgins, M.; Castaldelli-Maia, J.M.; Ventriglio, A. The outbreak of COVID-19 coronavirus and its impact on global mental health. Int. J. Soc. Psychiatry 2020, 66, 317–320. [Google Scholar] [CrossRef] [Green Version]
- WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed on 4 May 2021).
- Rundle, A.G.; Park, Y.; Herbstman, J.B.; Kinsey, E.W.; Wang, Y.C. COVID-19 related school closings and risk of weight gain among children. Obesity 2020, 28, 1008–1009. [Google Scholar] [CrossRef] [Green Version]
- DRAFT Landscape of COVID-19 Candidate Vaccines. 2021. Available online: https://www.who.int/publications/m/item/draft-landscape-of-covid-19-candidate-vaccines (accessed on 23 February 2021).
- Hotez, P. America and Europe’s new normal: The return of vaccine-preventable diseases. Pediatr. Res. 2019, 85, 912–914. [Google Scholar] [CrossRef]
- Dubé, E.; Vivion, M.; MacDonald, N.E. Vaccine hesitancy, vaccine refusal and the anti-vaccine movement: Influence, impact and implications. Expert. Rev. Vaccines 2015, 14, 99–117. [Google Scholar] [CrossRef]
- Trogen, B.; Oshinsky, D.; Caplan, A. Adverse consequences of rushing a SARS-CoV-2 vaccine: Implications for public trust. JAMA 2020, 323, 2460–2461. [Google Scholar] [CrossRef]
- Prestwich, A.; Webb, T.L.; Conner, M. Using theory to develop and test interventions to promote changes in health behaviour: Evidence, issues, and recommendations. Curr. Opin. Psychol. 2015, 5, 1–5. [Google Scholar] [CrossRef]
- Rogers, R.W. Cognitive and physiological processes in fear appeals and attitude change: A revised theory of protection motivation. In Social Psychophysiology; Cacioppo, J., Petty, R., Eds.; Guilford Press: New York, NY, USA, 1983. [Google Scholar]
- Rosenstock, I.M. Why people use health services. Milbank Mem. Fund Q. 1966, 44, 94–127. [Google Scholar] [CrossRef] [Green Version]
- Ajzen, I. The theory of planned behavior. Organ Behav. Hum. Decis. Process 1991, 50, 179–211. [Google Scholar] [CrossRef]
- Schmid, P.; Rauber, D.; Betsch, C.; Lidolt, G.; Denker, M.L. Barriers of influenza vaccination intention and behavior—A systematic review of influenza vaccine hesitancy, 2005–2016. PLoS ONE 2017, 12, e0170550. [Google Scholar] [CrossRef]
- Wu, A.M.S.; Lau, J.T.F.; Ma, Y.L.; Cheng, K.M.; Lau, M.M.C. A longitudinal study using parental cognitions based on the theory of planned behavior to predict childhood influenza vaccination. J. Infect. Public Health 2020, 13, 970–979. [Google Scholar] [CrossRef]
- Catalano, H.P.; Knowlden, A.P.; Birch, D.A.; Leeper, J.D.; Paschal, A.M.; Usdan, S.L. Using the theory of planned behavior to predict HPV vaccination intentions of college men. J. Am. Coll. Health 2017, 65, 197–207. [Google Scholar] [CrossRef]
- Shmueli, L. Predicting intention to receive COVID-19 vaccine among the general population using the health belief model and the theory of planned behavior model. BMC Public Health 2021, 21, 804. [Google Scholar] [CrossRef]
- Xiao, X.; Wong, R.M. Vaccine hesitancy and perceived behavioral control: A meta-analysis. Vaccine 2020, 38, 5131–5138. [Google Scholar] [CrossRef]
- Sniehotta, F.F.; Presseau, J.; Araújo-Soares, V. Time to retire the theory of planned behaviour. Health Psychol. Rev. 2014, 8, 1–7. [Google Scholar] [CrossRef]
- Ajzen, I. The theory of planned behaviour is alive and well, and not ready to retire: A commentary on Sniehotta, Presseau, and Araújo-Soares. Health Psychol. Rev. 2015, 9, 131–137. [Google Scholar] [CrossRef]
- Armitage, C.J. Time to retire the theory of planned behaviour? A commentary on Sniehotta, Presseau and Araújo-Soares. Health Psychol. Rev. 2015, 9, 151–155. [Google Scholar] [CrossRef]
- Conner, M. Extending not retiring the theory of planned behaviour: A commentary on Sniehotta, Presseau and Araújo-Soares. Health Psychol. Rev. 2015, 9, 141–145. [Google Scholar] [CrossRef] [Green Version]
- Ogden, J. Time to retire the theory of planned behaviour? One of us will have to go! A commentary on Sniehotta, Presseau and Araújo-Soares. Health Psychol. Rev. 2015, 9, 165–167. [Google Scholar] [CrossRef]
- Roger, R.W. A protection motivation theory of fear appeals and attitude change. J. Psychol. 1975, 91, 93–114. [Google Scholar] [CrossRef]
- Ling, M.; Kothe, E.J.; Mullan, B.A. Predicting intention to receive a seasonal influenza vaccination using Protection Motivation Theory. Soc. Sci. Med. 2019, 233, 87–92. [Google Scholar] [CrossRef] [Green Version]
- Wang, P.-W.; Ahorsu, D.K.; Lin, C.-Y.; Chen, I.-H.; Yen, C.-F.; Kuo, Y.-J.; Griffiths, M.D.; Pakpour, A.H. Motivation to have COVID-19 vaccination explained Using an extended protection motivation theory among university students in China: The role of information sources. Vaccines 2021, 9, 380. [Google Scholar] [CrossRef]
- Zhang, K.C.; Fang, Y.; Cao, H.; Chen, H.; Hu, T.; Chen, Y.; Zhou, X.; Wang, Z. Behavioral intention to receive a COVID-19 vaccination among Chinese factory workers: Cross-sectional online survey. J. Med. Internet Res. 2021, 23, e24673. [Google Scholar] [CrossRef]
- Sturman, D.; Auton, J.C.; Thacker, J. Knowledge of social distancing measures and adherence to restrictions during the COVID-19 pandemic. Health Promot. J. Aust. 2021, 32, 344–351. [Google Scholar] [CrossRef]
- Cordina, M.; Lauri, M.A.; Lauri, J. Attitudes towards COVID-19 vaccination, vaccine hesitancy and intention to take the vaccine. Pharm. Pract. 2021, 19, 2317. [Google Scholar] [CrossRef]
- Guidry, J.P.D.; Laestadius, L.I.; Vraga, E.K.; Miller, C.A.; Perrin, P.B.; Burton, C.W.; Ryan, M.; Fuemmeler, B.F.; Carlyle, K.E. Willingness to get the COVID-19 vaccine with and without emergency use authorization. Am. J. Infect. Control 2021, 49, 137–142. [Google Scholar] [CrossRef]
- Ahorsu, D.K.; Lin, C.-Y.; Imani, V.; Saffari, M.; Griffiths, M.D.; Pakpour, A.H. Fear of COVID-19 Scale: Development and initial validation. Int. J. Ment. Health Addict. 2020. [Google Scholar] [CrossRef] [Green Version]
- Chang, K.-C.; Hou, W.-L.; Pakpour, A.H.; Lin, C.-Y.; Griffiths, M.D. Psychometric testing of three COVID-19-related scales among people with mental illness. Int. J. Ment. Health Addict. 2020. [Google Scholar] [CrossRef]
- Lin, C.-Y.; Hou, W.-L.; Mamun, M.A.; da Silva, J.A.; Broche-Pérez, Y.; Ullah, I.; Masuyama, A.; Wakashima, K.; Mailliez, M.; Carre, A.; et al. Fear of COVID-19 Scale (FCV-19S) across countries: Measurement invariance issues. Nurs. Open 2021. [Google Scholar] [CrossRef]
- Hu, L.-T.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Modeling 1999, 6, 1–55. [Google Scholar] [CrossRef]
- COVID-19 Data. Available online: https://github.com/owid/covid-19-data/blob/master/public/data/vaccinations/country_data/Iran.csv (accessed on 27 April 2021).
- Adeli, O.A.; Kah Kashi, S.R. Estimating willingness to pay for the Covid-19 vaccine using the conditional valuation method. J. Iran Inst. Health Sci. Res. 2021, 20, 1–14. [Google Scholar]
- Armitage, C.J.; Conner, M. Efficacy of the Theory of Planned Behaviour: A meta-analytic review. Br. J. Soc. Psychol. 2001, 40, 471–499. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hagger, M.S.; Hamilton, K. Effects of socio-structural variables in the theory of planned behavior: A mediation model in multiple samples and behaviors. Psychol. Health 2021, 36, 307–333. [Google Scholar] [CrossRef] [PubMed]
- Rich, A.; Brandes, K.; Mullan, B.; Hagger, M.S. Theory of planned behavior and adherence in chronic illness: A meta-analysis. J. Behav. Med. 2015, 38, 673–688. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Detoc, M.; Bruel, S.; Frappe, P.; Tardy, B.; Botelho-Nevers, E.; Gagneux-Brunon, A. Intention to participate in a COVID-19 vaccine clinical trial and to get vaccinated against COVID-19 in France during the pandemic. Vaccine 2020, 38, 7002–7006. [Google Scholar] [CrossRef]
- Gagneux-Brunon, A.; Detoc, M.; Bruel, S.; Tardy, B.; Rozaire, O.; Frappe, P.; Botelho-Nevers, E. Intention to get vaccinations against COVID-19 in French healthcare workers during the first pandemic wave: A cross-sectional survey. J. Hosp. Infect. 2021, 108, 168–173. [Google Scholar] [CrossRef]
- Qiao, S.; Tam, C.C.; Li, X. Risk exposures, risk perceptions, negative attitudes toward general vaccination, and COVID-19 vaccine acceptance among college students in South Carolina. medRxiv 2020. preprint. [Google Scholar] [CrossRef]

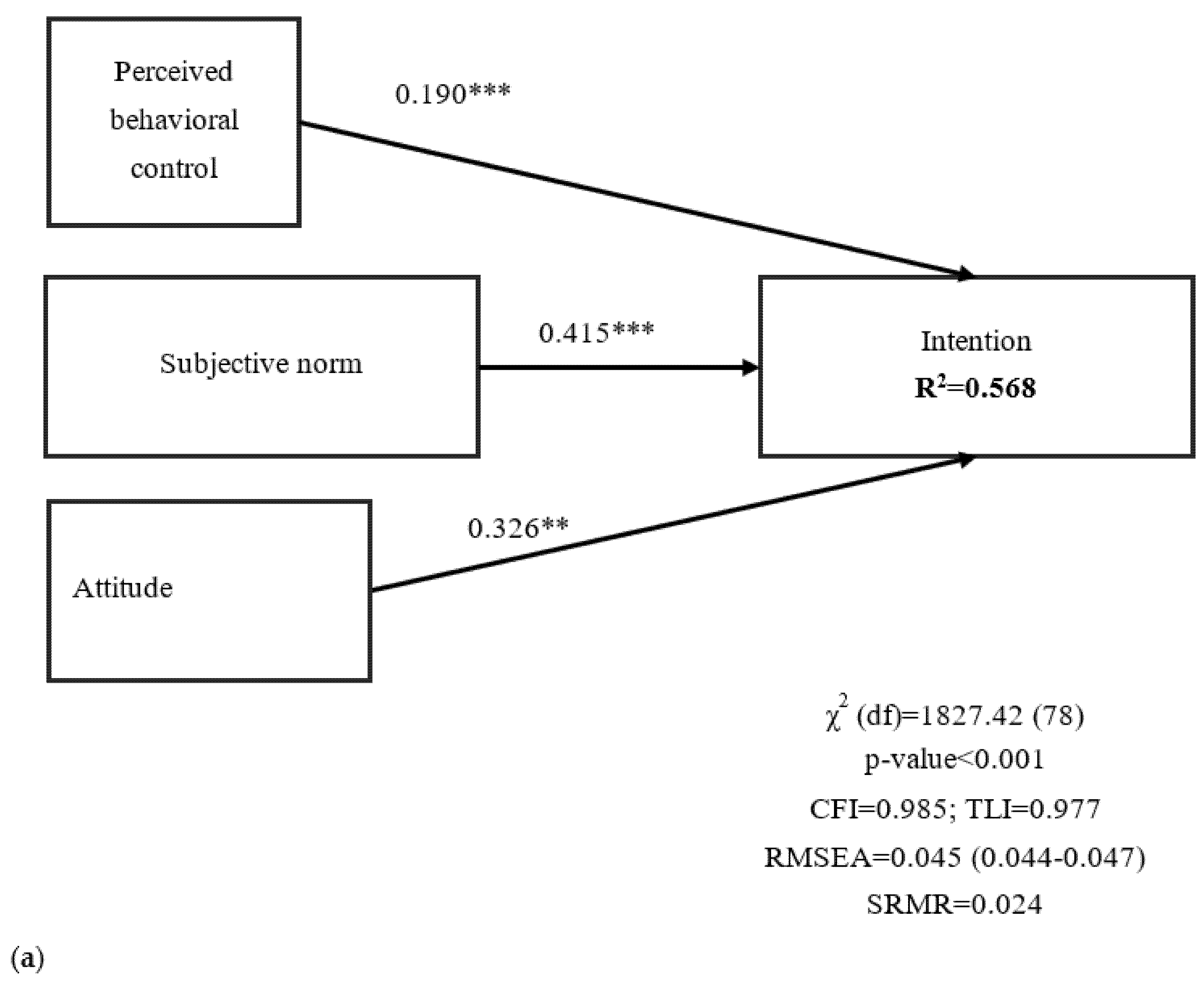
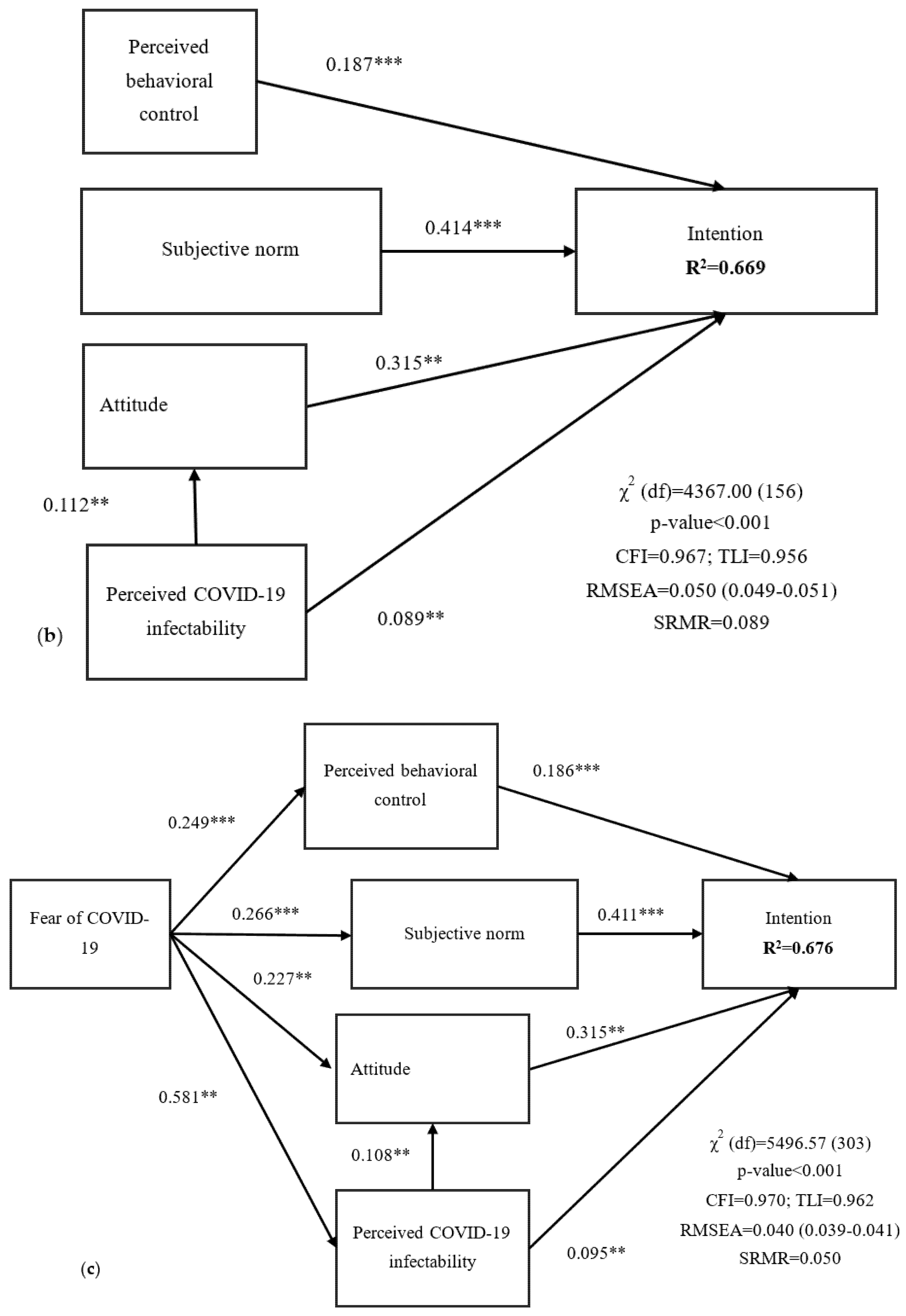
| Demographic Variable | Mean ± SD or n (%) |
|---|---|
| Age | 35.54 ± 12.00 |
| Gender | |
| Male | 4092 (37.7%) |
| Educational levels | |
| University | 4230 (39.0%) |
| Diploma | 2761 (25.5%) |
| High school | 974 (9.0%) |
| Secondary school | 1540 (14.2%) |
| Primary school | 986 (9.1%) |
| Illiterate | 352 (3.2%) |
| Marital status | |
| Married | 8092 (74.6%) |
| Single | 2751 (25.4%) |
| Accommodation | |
| City | 8186 (75.5%) |
| Rural | 2656 (24.5%) |
| Variable | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|
| 1. Fear of COVID-19 | 1 | |||||
| 2. Perceived infectability | 0.419 ** | 1 | ||||
| 3. Perceived behavioral control | 0.172 ** | 0.241 ** | 1 | |||
| 4. Subjective norms | 0.213 ** | 0.318 ** | 0.487 ** | 1 | ||
| 5. Attitude | 0.232 ** | 0.345 ** | 0.492 ** | 0.765 ** | 1 | |
| 6. Intention | 0.219 ** | 0.325 ** | 0.523 ** | 0.686 ** | 0.740 ** | 1 |
| Construct; Mean (SD) | Measurement Item | λ | α | CR | AVE |
|---|---|---|---|---|---|
| Fear of COVID-19; 21.12 (6.94) | 0.88 | 0.87 | 0.48 | ||
| I am most afraid of coronavirus-19 | 0.648 | ||||
| It makes me uncomfortable to think about coronavirus-19 | 0.742 | ||||
| My hands become clammy when I think about coronavirus-19 | 0.631 | ||||
| I am afraid of losing my life because of coronavirus-19 | 0.735 | ||||
| When watching news and stories about coronavirus-19 on social media, I become nervous or anxious | 0.765 | ||||
| I cannot sleep because I’m worrying about getting coronavirus-19 | 0.650 | ||||
| My heart races or palpitates when I think about getting coronavirus-19 | 0.670 | ||||
| Perceived COVID-19 infectability; 3.12 (1.10) | 0.70 | 0.67 | 0.30 | ||
| If a COVID-19 patient is “going around in his/her immediate locality”, I will get it | 0.703 | ||||
| My past experiences make me believe I am not likely to get COVID-19 even when my friends are sick | 0.384 | ||||
| In general, I am very susceptible to colds, flu, COVID-19 and other infectious diseases | 0.529 | ||||
| I am unlikely to catch a cold, flu, COVID-19 or other illness, even if it is “going around in the immediate locality” | 0.457 | ||||
| My immune system protects me from COVID-19 that other people get | 0.615 | ||||
| Perceived Behavioral Control; 3.84 (1.05) | 0.75 | 0.76 | 0.61 | ||
| Whether or not I get COVID-19 vaccination is completely up to me. | 0.720 | ||||
| I have resources, time and opportunities to get COVID-19 vaccination | 0.837 | ||||
| Subjective norms; 3.83 (1.10) | Most people who are important to me would… | 0.89 | 0.88 | 0.79 | |
| want me to get COVID-19 vaccination | 0.881 | ||||
| think I should get COVID-19 vaccination | 0.898 | ||||
| Attitude; 3.86 (0.96) | For me, getting the COVID-19 vaccination would be … | 0.94 | 0.94 | 0.72 | |
| extremely bad (1)/extremely good (5) | 0.816 | ||||
| extremely undesirable (1)/extremely desirable (5) | 0.879 | ||||
| extremely unimportant (1)/extremely important (5) | 0.909 | ||||
| extremely useless (1)/extremely useful (5) | 0.808 | ||||
| extremely unfavorable (1)/extremely favorable (5) | 0.809 | ||||
| extremely harmful (1)/extremely beneficial (5) | 0.794 | ||||
| Intentions; 3.84 (1.10) | 0.92 | 0.91 | 0.84 | ||
| I am willing to get COVID-19 vaccination | 0.927 | ||||
| I want to get COVID-19 vaccination | 0.907 |
| Model and Comparisons | Fit Statistics | ||||||
|---|---|---|---|---|---|---|---|
| χ2 (df) | ∆χ2 (∆df) | CFI | ∆CFI | TLI | ∆TLI | RMSEA | |
| Gender (male vs. female) | |||||||
| M1: Unconstrained | 5257.24 (460) * | - | 0.971 | - | 0.965 | - | 0.031 |
| M2: Measurement weights | 5305.79 (478) * | 45.552(18) * | 0.971 | 0 | 0.967 | 0.002 | 0.031 |
| M3: Measurement intercepts | 5889.68 (502) * | 632.44(42) * | 0.968 | −0.002 | 0.964 | −0.001 | 0.031 |
| M4: Structural weights | 5909.02 (512) * | 651.78(52) * | 0.968 | −0.002 | 0.965 | 0.00 | 0.031 |
| M5: Structural Covariances | 5914.90 (513) * | 657.66(53) * | 0.968 | −0.002 | 0.965 | 0.00 | 0.031 |
| M6: Structural Residuals | 6009.70 (521) * | 752.46(61) * | 0.967 | −0.003 | 0.965 | 0.00 | 0.031 |
| M7: Measurement Residuals | 6726.63 (554) * | 1469.39(94) * | 0.963 | −0.008 | 0.963 | 0.002 | 0.032 |
| Age (above 35 years vs. below 35 years) | |||||||
| M1: Unconstrained | 5307.66 (460) * | - | 0.971 | - | 0.965 | - | 0.031 |
| M2: Measurement weights | 5365.10 (478) * | 57.44(18) * | 0.971 | 0 | 0.966 | 0.001 | 0.031 |
| M3: Measurement intercepts | 5606.77 (502) * | 299.11(42) * | 0.969 | −0.002 | 0.966 | 0.001 | 0.031 |
| M4: Structural weight | 5610.44 (512) * | 302.78(52) | 0.970 | −0.001 | 0.967 | 0.002 | 0.030 |
| M5: Structural Covariances | 5610.57 (513) * | 302.91(53) * | 0.970 | −0.001 | 0.967 | 0.002 | 0.030 |
| M6: Structural Residuals | 5706.17 (521) * | 398.51(61) * | 0.969 | −0.001 | 0.967 | 0.002 | 0.030 |
| M7: Measurement Residuals | 6263.78 (554) * | 956.12(94) * | 0.966 | −0.005 | 0.966 | 0.001 | 0.031 |
| Living (city vs. rural) | |||||||
| M1: Unconstrained | 5214.69 (460) * | - | 0.972 | - | 0.966 | - | 0.031 |
| M2: Measurement weights | 5259.74 (478) * | 45.05 (18) * | 0.971 | −0.001 | 0.967 | 0.001 | 0.030 |
| M3: Measurement intercepts | 5419.85 (502) * | 205.16(42) * | 0.971 | −0.001 | 0.968 | 0.002 | 0.030 |
| M4: Structural weights | 5450.73 (512) * | 236.03(52) * | 0.970 | −0.002 | 0.968 | 0.002 | 0.030 |
| M5: Structural Covariances | 5450.74 (513) * | 236.05(53) * | 0.970 | −0.002 | 0.968 | 0.002 | 0.030 |
| M6: Structural Residuals | 5508.89 (521) * | 294.20(61) * | 0.970 | −0.002 | 0.968 | 0.002 | 0.030 |
| M7: Measurement Residuals | 5692.11 (554) * | 477.42(94) * | 0.969 | −0.003 | 0.969 | 0.003 | 0.029 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yahaghi, R.; Ahmadizade, S.; Fotuhi, R.; Taherkhani, E.; Ranjbaran, M.; Buchali, Z.; Jafari, R.; Zamani, N.; Shahbazkhania, A.; Simiari, H.; et al. Fear of COVID-19 and Perceived COVID-19 Infectability Supplement Theory of Planned Behavior to Explain Iranians’ Intention to Get COVID-19 Vaccinated. Vaccines 2021, 9, 684. https://doi.org/10.3390/vaccines9070684
Yahaghi R, Ahmadizade S, Fotuhi R, Taherkhani E, Ranjbaran M, Buchali Z, Jafari R, Zamani N, Shahbazkhania A, Simiari H, et al. Fear of COVID-19 and Perceived COVID-19 Infectability Supplement Theory of Planned Behavior to Explain Iranians’ Intention to Get COVID-19 Vaccinated. Vaccines. 2021; 9(7):684. https://doi.org/10.3390/vaccines9070684
Chicago/Turabian StyleYahaghi, Rafat, Safie Ahmadizade, Razie Fotuhi, Elham Taherkhani, Mehdi Ranjbaran, Zeinab Buchali, Robabe Jafari, Narges Zamani, Azam Shahbazkhania, Hengame Simiari, and et al. 2021. "Fear of COVID-19 and Perceived COVID-19 Infectability Supplement Theory of Planned Behavior to Explain Iranians’ Intention to Get COVID-19 Vaccinated" Vaccines 9, no. 7: 684. https://doi.org/10.3390/vaccines9070684
APA StyleYahaghi, R., Ahmadizade, S., Fotuhi, R., Taherkhani, E., Ranjbaran, M., Buchali, Z., Jafari, R., Zamani, N., Shahbazkhania, A., Simiari, H., Rahmani, J., Yazdi, N., Alijani, H., Poorzolfaghar, L., Rajabi, F., Lin, C.-Y., Broström, A., Griffiths, M. D., & Pakpour, A. H. (2021). Fear of COVID-19 and Perceived COVID-19 Infectability Supplement Theory of Planned Behavior to Explain Iranians’ Intention to Get COVID-19 Vaccinated. Vaccines, 9(7), 684. https://doi.org/10.3390/vaccines9070684







