A Unique SARS-CoV-2 Spike Protein P681H Variant Detected in Israel
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample Collection for Sequencing
2.2. Library Preparation and Sequencing
2.3. Bioinformatics Analysis
2.4. Neutralization Assays
3. Results
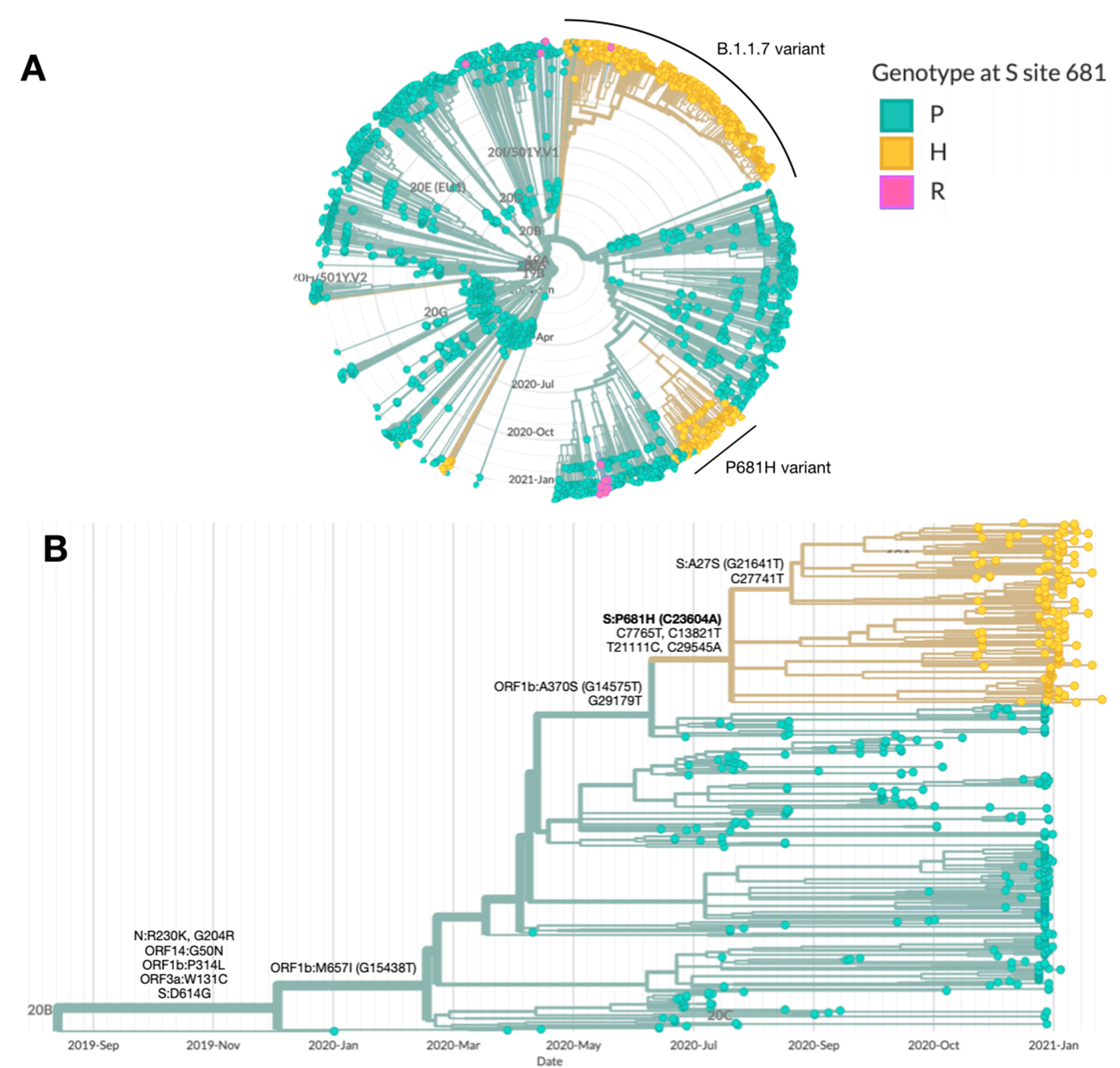
3.1. Characterization of the B.1.1.50 + P681H Variant
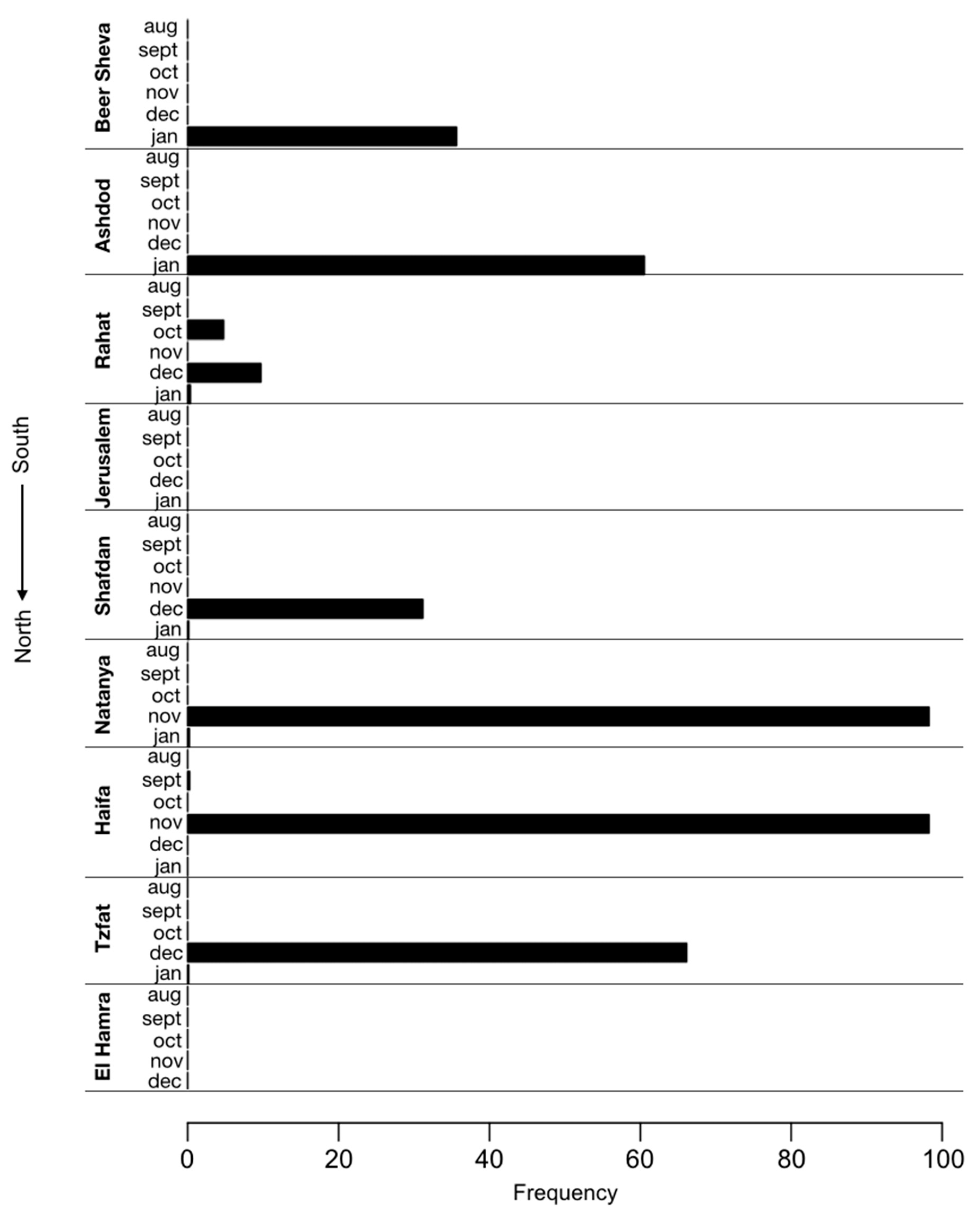
3.2. Identification of the P681H Mutation in Sewage
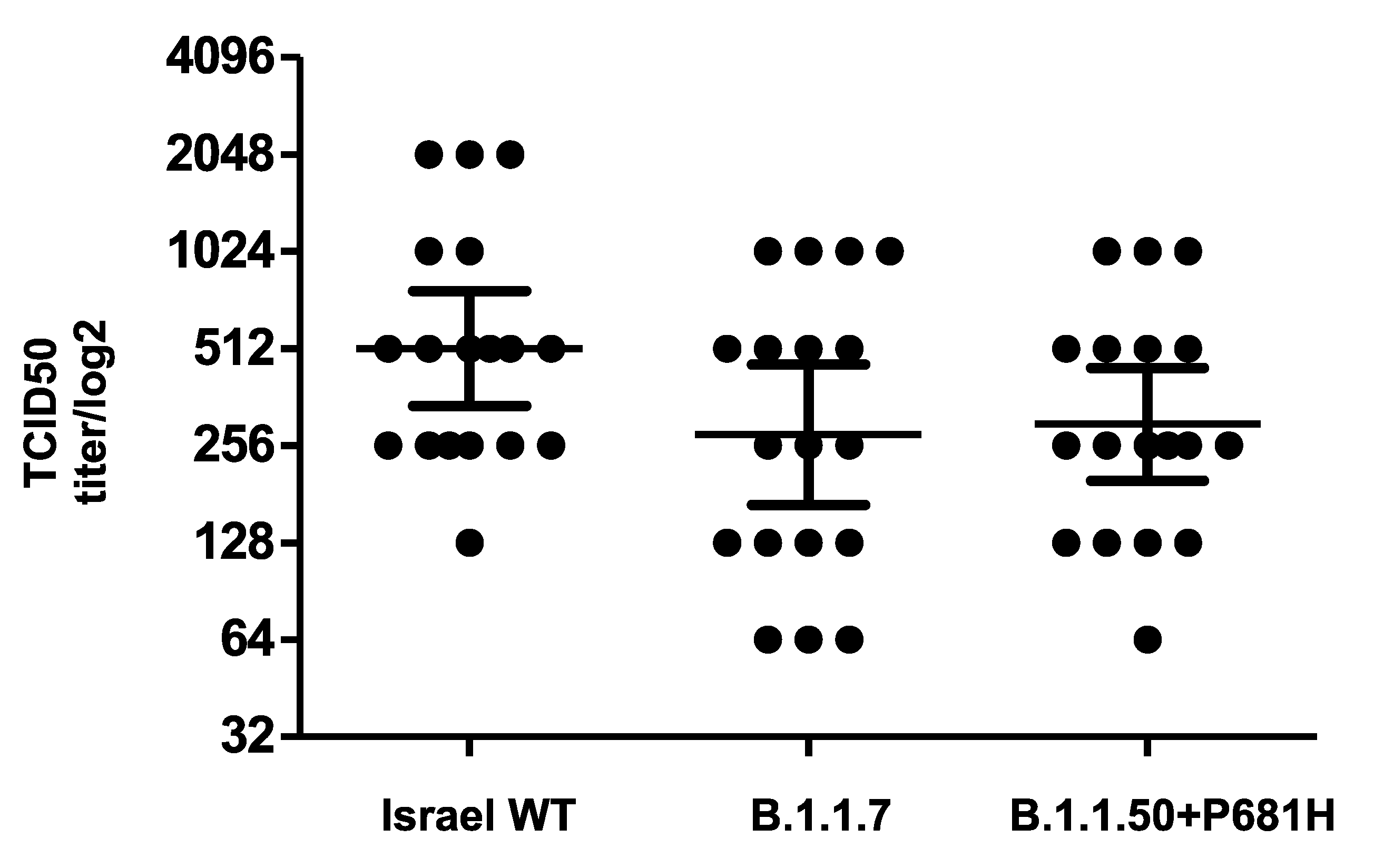
3.3. Effective Neutralization of the B.1.1.50 + P681H Variant
4. Discussion and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lu, H.; Stratton, C.W.; Tang, Y. Outbreak of pneumonia of unknown etiology in Wuhan, China: The mystery and the miracle. J. Med. Virol. 2020, 92, 401–402. [Google Scholar] [CrossRef] [PubMed]
- Shu, Y.; McCauley, J. GISAID: Global initiative on sharing all influenza data—From vision to reality. Eurosurveillance 2017, 22. [Google Scholar] [CrossRef] [PubMed]
- Hadfield, J.; Megill, C.; Bell, S.M.; Huddleston, J.; Potter, B.; Callender, C.; Sagulenko, P.; Bedford, T.; A Neher, R. Nextstrain: Real-time tracking of pathogen evolution. Bioinformatics 2018, 34, 4121–4123. [Google Scholar] [CrossRef]
- Rambaut, A.; Holmes, E.C.; O’Toole, Á.; Hill, V.; McCrone, J.T.; Ruis, C.; Du Plessis, L.; Pybus, O.G. A dynamic nomenclature proposal for SARS-CoV-2 lineages to assist genomic epidemiology. Nat. Microbiol. 2020, 5, 1403–1407. [Google Scholar] [CrossRef]
- O’Toole, Á.; Scher, E.; Anthony Underwood, B.J.; Verity Hill, J.T.; McCrone, C.R.; Khali, A.D.; Ben Taylor, C.Y. Louis du Plessis, David Aanensen, Eddie Holmes, Oliver Pybus. Pangolin: Lineage Assignment in an Emerging Pandemic as an Epidemiological Tool. Available online: github.com/cov-lineages/pangolin (accessed on 1 June 2021).
- Tang, J.W.; A Tambyah, P.; Hui, D.S. Emergence of a new SARS-CoV-2 variant in the UK. J. Infect. 2021, 82, e27–e28. [Google Scholar] [CrossRef]
- Tegally, H.; Wilkinson, E.; Giovanetti, M.; Iranzadeh, A.; Fonseca, V.; Giandhari, J.; Doolabh, D.; Pillay, S.; San, E.J.; Msomi, N.; et al. Emergence and rapid spread of a new severe acute respiratory syndrome-related coronavirus 2 (SARS-CoV-2) line-age with multiple spike mutations in South Africa. medRxiv 2020. [Google Scholar] [CrossRef]
- Sabino, E.C.; Buss, L.F.; Carvalho, M.P.; Prete, C.A.; Crispim, M.A.; Fraiji, N.A.; Pereira, R.H.; Parag, K.V.; da Silva Peixoto, P.; Kraemer, M.U.; et al. Resurgence of COVID-19 in Manaus, Brazil, despite high seroprevalence. Lancet 2021, 397, 452–455. [Google Scholar] [CrossRef]
- Hoffmann, M.; Arora, P.; Groß, R.; Seidel, A.; Hörnich, B.F.; Hahn, A.S.; Krüger, N.; Graichen, L.; Hofmann-Winkler, H.; Kempf, A.; et al. SARS-CoV-2 variants B.1.351 and P.1 escape from neutralizing antibodies. Cell 2021. [Google Scholar] [CrossRef]
- Davies, N.G.; Abbott, S.; Barnard, R.C.; Jarvis, C.I.; Kucharski, A.J.; Munday, J.D.; Pearson, C.A.B.; Russell, T.W.; Tully, D.C.; Washburne, A.D.; et al. Estimated transmissibility and impact of SARS-CoV-2 lineage B.1.1.7 in England. Science 2021, 372, eabg3055. [Google Scholar] [CrossRef]
- Brielle, E.S.; Schneidman-Duhovny, D.; Linial, M. The SARS-CoV-2 Exerts a Distinctive Strategy for Interacting with the ACE2 Human Receptor. Viruses 2020, 12, 497. [Google Scholar] [CrossRef] [PubMed]
- Tian, F.; Tong, B.; Sun, L.; Shi, S.; Zheng, B.; Wang, Z.; Dong, X.; Zheng, P. Mutation N501Y in RBD of Spike Protein Strengthens the Interaction between COVID-19 and its Receptor ACE2. bioRxiv 2021. [Google Scholar] [CrossRef]
- Shang, J.; Wan, Y.; Luo, C.; Ye, G.; Geng, Q.; Auerbach, A.; Li, F. Cell entry mechanisms of SARS-CoV-2. Proc. Natl. Acad. Sci. USA 2020, 117, 11727–11734. [Google Scholar] [CrossRef]
- Lasek-Nesselquist, E.; Pata, J.; Schneider, E.; George, K.S. A tale of three SARS-CoV-2 variants with independently acquired P681H mutations in New York State. medRxiv 2021. [Google Scholar] [CrossRef]
- Coutard, B.; Valle, C.; De Lamballerie, X.; Canard, B.; Seidah, N.; Decroly, E. The spike glycoprotein of the new coronavirus 2019-nCoV contains a furin-like cleavage site absent in CoV of the same clade. Antivir. Res. 2020, 176, 104742. [Google Scholar] [CrossRef] [PubMed]
- Bugembe, D.L.; Phan, M.V.; Ssewanyana, I.; Semanda, P.; Nansumba, H.; Dhaala, B.; Nabadda, S.; O’Toole, A.; Rambaut, A.; Kaleebu, P.; et al. A SARS-CoV-2 lineage A variant (A.23.1) with altered spike has emerged and is dominating the current Uganda epidemic. medRxiv 2021. [Google Scholar] [CrossRef]
- Shulman, L.M.; Manor, Y.; Hindiyeh, M.; Sofer, D.; Mendelson, E. Molecular Characterization of Polio from Environmental Samples: ISSP, The Israeli Sewage Surveillance Protocol. In Poliovirus; Humana Press: New York, NY, USA, 2016; pp. 55–107. [Google Scholar]
- Ewels, P.; Magnusson, M.; Lundin, S.; Käller, M. MultiQC: Summarize analysis results for multiple tools and samples in a single report. Bioinformatics 2016, 32, 3047–3048. [Google Scholar] [CrossRef]
- Bolger, A.M.; Lohse, M.; Usadel, B. Trimmomatic: A flexible trimmer for Illumina sequence data. Bioinformatics 2014, 30, 2114–2120. [Google Scholar] [CrossRef]
- Li, H.; Durbin, R. Fast and accurate long-read alignment with Burrows–Wheeler transform. Bioinformatics 2010, 26, 589–595. [Google Scholar] [CrossRef]
- Li, H. A statistical framework for SNP calling, mutation discovery, association mapping and population genetical parameter estimation from sequencing data. Bioinformatics 2011, 27, 2987–2993. [Google Scholar] [CrossRef]
- Katoh, K.; Misawa, K.I.; Kuma, K.; Miyata, T. MAFFT: A novel method for rapid multiple sequence alignment based on fast Fourier transform. Nucleic Acids Res. 2002, 30, 3059–3066. [Google Scholar] [CrossRef] [PubMed]
- Charif, D.; Lobry, J.R. SeqinR 1.0-2: A Contributed Package to the R Project for Statistical Computing Devoted to Biological Sequences Retrieval and Analysis. In Structural Approaches to Sequence Evolution; Springer: Berlin/Heidelberg, Germany, 2007; pp. 207–232. [Google Scholar]
- Nguyen, L.-T.; Schmidt, H.A.; Von Haeseler, A.; Minh, B.Q. IQ-TREE: A Fast and Effective Stochastic Algorithm for Estimating Maximum-Likelihood Phylogenies. Mol. Biol. Evol. 2015, 32, 268–274. [Google Scholar] [CrossRef] [PubMed]
- Sagulenko, P.; Puller, V.; Neher, R.A. TreeTime: Maximum-likelihood phylodynamic analysis. Virus Evol. 2018, 4, vex042. [Google Scholar] [CrossRef] [PubMed]
- Morgan, M.; Pagès, H.; Obenchain, V.; Hayden, N. Rsamtools: Binary Alignment (BAM), FASTA, Variant Call (BCF), and Tabix File Import. 2020. R package version 2.8.0. Available online: https://bioconductor.org/packages/Rsamtools (accessed on 1 June 2021).
- Wang, P.; Nair, M.S.; Liu, L.; Iketani, S.; Luo, Y.; Guo, Y.; Wang, M.; Yu, J.; Zhang, B.; Kwong, P.D.; et al. Increased Resistance of SARS-CoV-2 Variants B.1.351 and B.1.1.7 to Antibody Neutralization. bioRxiv 2021. [Google Scholar] [CrossRef]
- Edara, V.V.; Floyd, K.; Lai, L.; Gardner, M.; Hudson, W.; Piantadosi, A.; Waggoner, J.; Babiker, A.; Ahmed, R.; Xie, X.; et al. Infection and mRNA-1273 vaccine antibodies neutralize SARS-CoV-2 UK variant. medRxiv 2021. [Google Scholar] [CrossRef]
| November | December | January | ||
|---|---|---|---|---|
| gender | Male | 10 | 30 | 25 |
| Female | 8 | 24 | 23 | |
| Unknown | 9 | 17 | 35 | |
| age | 39.3 ± 21.3 | 33.8 ± 25.3 | 35.8 ± 22 | |
| reason | random | 27 | 55 | 80 |
| outbreaks | 10 | |||
| ret. abroad | 6 | 3 | ||
| district | Northern | 3 | 7 | 14 |
| Haifa | 4 | 2 | 5 | |
| Central | 4 | 19 | 32 | |
| Tel Aviv | 1 | 11 | 10 | |
| Jerusalem | 1 | 9 | 9 | |
| Jud & Sam | 1 | 5 | ||
| Southern | 1 | 4 | 3 | |
| Unknown | 12 | 19 | 5 | |
| total B.1.1.50 + P681H |  | 27 | 71 | 83 |
| % of random | 12.74 | 8.31 | 3.29 | |
| total B.1.1.7 |  | 0 | 64 | 1008 |
| % of random | 0.00 | 7.49 | 39.97 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zuckerman, N.S.; Fleishon, S.; Bucris, E.; Bar-Ilan, D.; Linial, M.; Bar-Or, I.; Indenbaum, V.; Weil, M.; Lustig, Y.; Mendelson, E.; et al. A Unique SARS-CoV-2 Spike Protein P681H Variant Detected in Israel. Vaccines 2021, 9, 616. https://doi.org/10.3390/vaccines9060616
Zuckerman NS, Fleishon S, Bucris E, Bar-Ilan D, Linial M, Bar-Or I, Indenbaum V, Weil M, Lustig Y, Mendelson E, et al. A Unique SARS-CoV-2 Spike Protein P681H Variant Detected in Israel. Vaccines. 2021; 9(6):616. https://doi.org/10.3390/vaccines9060616
Chicago/Turabian StyleZuckerman, Neta S., Shay Fleishon, Efrat Bucris, Dana Bar-Ilan, Michal Linial, Itay Bar-Or, Victoria Indenbaum, Merav Weil, Yaniv Lustig, Ella Mendelson, and et al. 2021. "A Unique SARS-CoV-2 Spike Protein P681H Variant Detected in Israel" Vaccines 9, no. 6: 616. https://doi.org/10.3390/vaccines9060616
APA StyleZuckerman, N. S., Fleishon, S., Bucris, E., Bar-Ilan, D., Linial, M., Bar-Or, I., Indenbaum, V., Weil, M., Lustig, Y., Mendelson, E., Mandelboim, M., Mor, O., Zuckerman, N., & on behalf of the Israel National Consortium for SARS-CoV-2 Sequencing. (2021). A Unique SARS-CoV-2 Spike Protein P681H Variant Detected in Israel. Vaccines, 9(6), 616. https://doi.org/10.3390/vaccines9060616







