Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy
Abstract
1. Introduction
2. Materials and Methods
2.1. Questionnaire
2.2. Statistical Analysis
3. Results
3.1. Sample Features
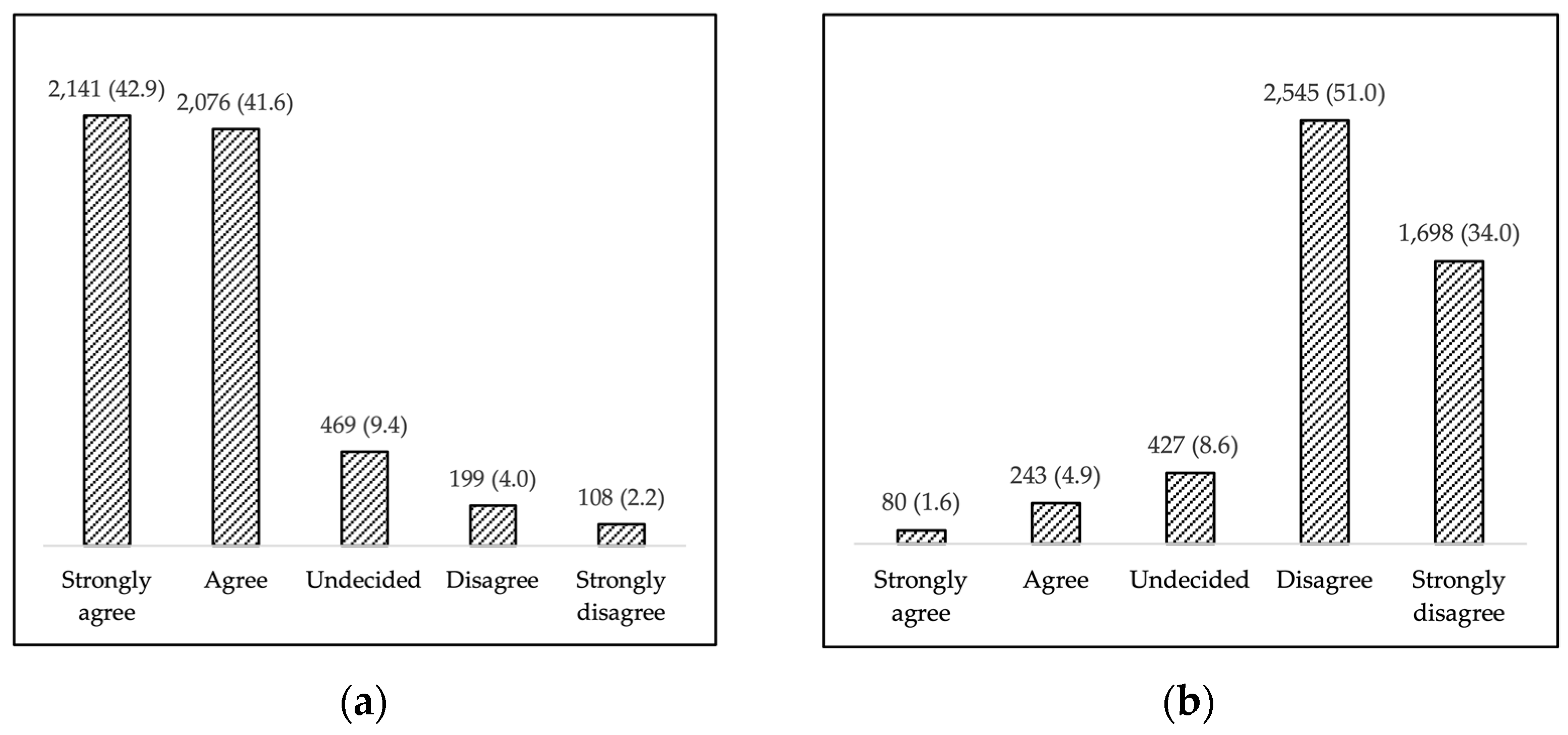
3.2. Attitude toward COVID-19 Vaccination and Main Determinants
3.3. Adherence and Perception of the Policy on Obligatory Vaccination (Law n. 119/2017)
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- COVID-19 in Children and the Role of School Settings in COVID-19 Transmission. Available online: https://www.ecdc.europa.eu/sites/default/files/documents/COVID-19-schools-transmission-August%202020.pdf (accessed on 24 March 2021).
- UNESCO Half of World’s Student Population Not Attending School: UNESCO Launches Global Coalition to Accelerate Deployment of Remote Learning Solutions. Available online: https://en.unesco.org/news/half-worlds-student-population-not-attending-school-unesco-launches-global-coalition-accelerate (accessed on 24 March 2021).
- Fantini, M.P.; Reno, C.; Biserni, G.B.; Savoia, E.; Lanari, M. COVID-19 and the Re-Opening of Schools: A Policy Maker’s Dilemma. Ital. J. Pediatr. 2020, 46, 79. [Google Scholar] [CrossRef]
- UNESCO. Adverse Consequences of School Closures. Available online: https://en.unesco.org/covid19/educationresponse/consequences (accessed on 24 March 2021).
- COVID-19 in Children and the Role of School Settings in Transmission—First Update. Available online: https://www.ecdc.europa.eu/sites/default/files/documents/COVID-19-in-children-and-the-role-of-school-settings-in-transmission-first-update_1.pdf (accessed on 24 March 2021).
- Bhopal, S.S.; Bagaria, J.; Olabi, B.; Bhopal, R. Children and Young People Remain at Low Risk of COVID-19 Mortality. Lancet Child Adolesc. Health 2021. [Google Scholar] [CrossRef]
- Brookman, S.; Cook, J.; Zucherman, M.; Broughton, S.; Harman, K.; Gupta, A. Effect of the New SARS-CoV-2 Variant B.1.1.7 on Children and Young People. Lancet Child Adolesc. Health 2021, 5, e9–e10. [Google Scholar] [CrossRef]
- Further Implementing Provisions of Decree-Law No. 6 of February 23, 2020, on Urgent Measures for the Containment and Management of the Epidemiological Emergency from COVID-19. Available online: https://www.gazzettaufficiale.it/eli/id/2020/03/01/20A01381/sg (accessed on 24 March 2021).
- COVID-19 Epidemic, National Update, 5 January 2021. Available online: https://www.epicentro.iss.it/coronavirus/bollettino/Bollettino-sorveglianza-integrata-COVID-19_5-gennaio-2021.pdf (accessed on 24 March 2021).
- Colao, A.; Piscitelli, P.; Pulimeno, M.; Colazzo, S.; Miani, A.; Giannini, S. Rethinking the Role of the School after COVID-19. Lancet Public Health 2020, 5, e370. [Google Scholar] [CrossRef]
- Regional School Office for Emilia-Romagna. Update Protocol Management Case Covid-19 Confirmed in School Setting. 2020. Available online: https://www.istruzioneer.gov.it/2020/11/27/aggiornamento-protocollo-gestione-caso-covid-19-confermato-in-ambito-scolastico/ (accessed on 24 March 2021).
- Urgent Measures on the Containment and Management of the Epidemiological Emergency from COVID-2019. Ministry of Health in Agreement with the President of the Emilia-Romagna Region. Available online: https://www.regione.emilia-romagna.it/notizie/2020/febbraio/sospesa-attivita-scuole-nidi-e-manifestazioni-tutte-le-misure-adottate-contro-il-coronavirus/ordinanza-n-1-2020-covid-19.pdf (accessed on 24 March 2021).
- Italian Ministry of Health. Anti-Covid-19 National Vaccination Plan. Available online: http://www.salute.gov.it/portale/nuovocoronavirus/dettaglioContenutiNuovoCoronavirus.jsp?lingua=italiano&id=5452&area=nuovoCoronavirus&menu=vuoto (accessed on 24 March 2021).
- World Health Organization. Global Vaccine Action Plan 2011–2018. Available online: https://www.afro.who.int/sites/default/files/2017-06/9789241504980_eng.pdf (accessed on 24 March 2021).
- Mahase, E. Covid Vaccine Could Be Rolled out to Children by Autumn. BMJ 2021, 372, n723. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, N.E. SAGE Working Group on Vaccine Hesitancy Vaccine Hesitancy: Definition, Scope and Determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- Conversion into Law, with Amendments, of Decree-Law No. 73 of June 7, 2017, Containing Urgent Provisions on Vaccine Prevention. Available online: https://www.trovanorme.salute.gov.it/norme/dettaglioAtto?id=60201 (accessed on 24 March 2021).
- Larson, H.J.; Jarrett, C.; Schulz, W.S.; Chaudhuri, M.; Zhou, Y.; Dube, E.; Schuster, M.; MacDonald, N.E.; Wilson, R. SAGE Working Group on Vaccine Hesitancy Measuring Vaccine Hesitancy: The Development of a Survey Tool. Vaccine 2015, 33, 4165–4175. [Google Scholar] [CrossRef]
- Sallam, M. COVID-19 Vaccine Hesitancy Worldwide: A Concise Systematic Review of Vaccine Acceptance Rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef]
- Neumann-Böhme, S.; Varghese, N.E.; Sabat, I.; Barros, P.P.; Brouwer, W.; van Exel, J.; Schreyögg, J.; Stargardt, T. Once We Have It, Will We Use It? A European Survey on Willingness to Be Vaccinated against COVID-19. Eur. J. Health Econ. 2020, 21, 977–982. [Google Scholar] [CrossRef]
- Lazarus, J.V.; Ratzan, S.C.; Palayew, A.; Gostin, L.O.; Larson, H.J.; Rabin, K.; Kimball, S.; El-Mohandes, A. A Global Survey of Potential Acceptance of a COVID-19 Vaccine. Nat. Med. 2021, 27, 225–228. [Google Scholar] [CrossRef]
- Barello, S.; Nania, T.; Dellafiore, F.; Graffigna, G.; Caruso, R. ‘Vaccine Hesitancy’ among University Students in Italy during the COVID-19 Pandemic. Eur. J. Epidemiol. 2020, 35, 781–783. [Google Scholar] [CrossRef] [PubMed]
- COVID-19 Vaccination and Prioritisation Strategies in the EU/EEA. Available online: https://www.ecdc.europa.eu/en/publications-data/covid-19-vaccination-and-prioritisation-strategies-eueea (accessed on 24 March 2021).
- Mintz, K.; Jardas, E.; Shah, S.; Grady, C.; Danis, M.; Wendler, D. Enrolling Minors in COVID-19 Vaccine Trials. Pediatrics 2021, 147. [Google Scholar] [CrossRef]
- Klass, P.; Ratner, A.J. Vaccinating Children against Covid-19—The Lessons of Measles. N. Engl. J. Med. 2021, 384, 589–591. [Google Scholar] [CrossRef]
- Loades, M.E.; Chatburn, E.; Higson-Sweeney, N.; Reynolds, S.; Shafran, R.; Brigden, A.; Linney, C.; McManus, M.N.; Borwick, C.; Crawley, E. Rapid Systematic Review: The Impact of Social Isolation and Loneliness on the Mental Health of Children and Adolescents in the Context of COVID-19. J. Am. Acad. Child Adolesc. Psychiatry 2020, 59, 1218–1239.e3. [Google Scholar] [CrossRef]
- Haleemunnissa, S.; Didel, S.; Swami, M.K.; Singh, K.; Vyas, V. Children and COVID19: Understanding Impact on the Growth Trajectory of an Evolving Generation. Child. Youth Serv. Rev. 2021, 120, 105754. [Google Scholar] [CrossRef] [PubMed]
- How Can We Address Covid-19 Vaccine Hesitancy and Improve Vaccine Acceptance?—The BMJ. Available online: https://blogs.bmj.com/bmj/2021/02/19/how-can-we-address-covid-19-vaccine-hesitancy-and-improve-vaccine-acceptance/ (accessed on 24 March 2021).
- Zhang, K.C.; Fang, Y.; Cao, H.; Chen, H.; Hu, T.; Chen, Y.Q.; Zhou, X.; Wang, Z. Parental Acceptability of COVID-19 Vaccination for Children Under the Age of 18 Years: Cross-Sectional Online Survey. JMIR Pediatr. Parent. 2020, 3, e24827. [Google Scholar] [CrossRef] [PubMed]
- Rhodes, A.; Hoq, M.; Measey, M.-A.; Danchin, M. Intention to Vaccinate against COVID-19 in Australia. Lancet Infect. Dis. 2020. [Google Scholar] [CrossRef]
- Bell, S.; Clarke, R.; Mounier-Jack, S.; Walker, J.L.; Paterson, P. Parents’ and Guardians’ Views on the Acceptability of a Future COVID-19 Vaccine: A Multi-Methods Study in England. Vaccine 2020, 38, 7789–7798. [Google Scholar] [CrossRef]
- Ward, J.K.; Alleaume, C.; Peretti-Watel, P. The French Public’s Attitudes to a Future COVID-19 Vaccine: The Politicization of a Public Health Issue. Soc. Sci. Med. 2020, 265, 113414. [Google Scholar] [CrossRef]
- Lin, C.; Tu, P.; Beitsch, L.M. Confidence and Receptivity for COVID-19 Vaccines: A Rapid Systematic Review. Vaccines 2020, 9, 16. [Google Scholar] [CrossRef] [PubMed]
- Schwarzinger, M.; Watson, V.; Arwidson, P.; Alla, F.; Luchini, S. COVID-19 Vaccine Hesitancy in a Representative Working-Age Population in France: A Survey Experiment Based on Vaccine Characteristics. Lancet Public Health 2021. [Google Scholar] [CrossRef]
- Flanagan, K.L.; Fink, A.L.; Plebanski, M.; Klein, S.L. Sex and Gender Differences in the Outcomes of Vaccination over the Life Course. Annu. Rev. Cell Dev. Biol. 2017, 33, 577–599. [Google Scholar] [CrossRef] [PubMed]
- Klein, S.L.; Marriott, I.; Fish, E.N. Sex-Based Differences in Immune Function and Responses to Vaccination. Trans. R. Soc. Trop. Med. Hyg. 2015, 109, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Bocquier, A.; Fressard, L.; Cortaredona, S.; Zaytseva, A.; Ward, J.; Gautier, A.; Peretti-Watel, P.; Verger, P.; Baromètre Santé 2016 Group. Social Differentiation of Vaccine Hesitancy among French Parents and the Mediating Role of Trust and Commitment to Health: A Nationwide Cross-Sectional Study. Vaccine 2018, 36, 7666–7673. [Google Scholar] [CrossRef] [PubMed]
- Kempe, A.; Saville, A.W.; Albertin, C.; Zimet, G.; Breck, A.; Helmkamp, L.; Vangala, S.; Dickinson, L.M.; Rand, C.; Humiston, S.; et al. Parental Hesitancy About Routine Childhood and Influenza Vaccinations: A National Survey. Pediatrics 2020, 146, e20193852. [Google Scholar] [CrossRef] [PubMed]
- Gualano, M.R.; Bert, F.; Voglino, G.; Buttinelli, E.; D’Errico, M.M.; De Waure, C.; Di Giovanni, P.; Fantini, M.P.; Giuliani, A.R.; Marranzano, M.; et al. Attitudes towards Compulsory Vaccination in Italy: Results from the NAVIDAD Multicentre Study. Vaccine 2018, 36, 3368–3374. [Google Scholar] [CrossRef]
- Deiner, M.S.; Fathy, C.; Kim, J.; Niemeyer, K.; Ramirez, D.; Ackley, S.F.; Liu, F.; Lietman, T.M.; Porco, T.C. Facebook and Twitter Vaccine Sentiment in Response to Measles Outbreaks. Health Inform. J. 2019, 25, 1116–1132. [Google Scholar] [CrossRef]
- Kang, G.J.; Ewing-Nelson, S.R.; Mackey, L.; Schlitt, J.T.; Marathe, A.; Abbas, K.M.; Swarup, S. Semantic Network Analysis of Vaccine Sentiment in Online Social Media. Vaccine 2017, 35, 3621–3638. [Google Scholar] [CrossRef]
- Puri, N.; Coomes, E.A.; Haghbayan, H.; Gunaratne, K. Social Media and Vaccine Hesitancy: New Updates for the Era of COVID-19 and Globalized Infectious Diseases. Hum. Vaccin. Immunother. 2020, 16, 2586–2593. [Google Scholar] [CrossRef]
- Guess, A.M.; Nyhan, B.; O’Keeffe, Z.; Reifler, J. The Sources and Correlates of Exposure to Vaccine-Related (Mis)Information Online. Vaccine 2020, 38, 7799–7805. [Google Scholar] [CrossRef] [PubMed]
- Johnson, N.F.; Velásquez, N.; Restrepo, N.J.; Leahy, R.; Gabriel, N.; El Oud, S.; Zheng, M.; Manrique, P.; Wuchty, S.; Lupu, Y. The Online Competition between Pro- and Anti-Vaccination Views. Nature 2020, 582, 230–233. [Google Scholar] [CrossRef] [PubMed]
- Ruiz, J.B.; Bell, R.A. Predictors of Intention to Vaccinate against COVID-19: Results of a Nationwide Survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef] [PubMed]
- Average Age of Mothers. Emilia-Romagna Region Report. Available online: https://applicazioni.regione.emilia-romagna.it/ReportERHome/stats/report/eJxVyTsKAjEQANA-p5gjTOIaMd0mG2TB0l6GzICB_cAYUnga7-LFtLV5zUM84QEdOjPN8z16P3jrbZ5ySulsnY3DGBzao9EeLqKk5VEJnsICXEG6bG03pYdUWyOuG20vApZlIViJVQz1kNvnDatw_R9lDNaUn2i0hdsYr_kLsvgsOA$2E$$2E$ (accessed on 24 March 2021).
| (a) | |||||||||
| Age (Years) | Primary School Degree | High School Degree | University Degree | Post-University Master Degree | Total | ||||
| (Grades 1–8) | (Grades 9–13) | N (%) | |||||||
| M | F | M | F | M | F | M | F | ||
| ≤29 | 3 | 21 | 4 | 41 | 3 | 15 | 2 | 0 | 89 (1.8) |
| 30–39 | 22 | 82 | 48 | 369 | 53 | 264 | 22 | 82 | 942 (18.9) |
| 40–49 | 80 | 175 | 252 | 973 | 171 | 765 | 62 | 286 | 2764 (55.4) |
| ≥50 | 50 | 60 | 216 | 372 | 147 | 236 | 34 | 83 | 1198 (24.0) |
| Total N (%) | 155 (3.1) | 338 (6.8) | 520 (10.4) | 1755 (35.1) | 374 (7.5) | 1280 (25.6) | 120 (2.4) | 451 (9.0) | 4993 |
| (b) | |||||||||
| Age | N (%) | ||||||||
| 0–5 | 633 (12.7) | ||||||||
| 06-ott | 1807 (36.2) | ||||||||
| nov-13 | 1312 (26.3) | ||||||||
| ≥14 | 1241 (24.9) | ||||||||
| Total | 4993 | ||||||||
| Information Source | Propensity toward Vaccination | |
|---|---|---|
| Yes | No | |
| Medical advice | 4214 (84.4) | 779 (15.6) |
| Personal beliefs | 1432 (28.7) | 3557 (71.2) |
| Web/Social Media | 362 (7.3) | 4631 (92.7) |
| Television | 295 (5.9) | 4698 (94.1) |
| Opinion of politics/religious authorities/celebrities | 64 (1.3) | 4929 (98.7) |
| Vaccine Hesitancy | OR | SE | p-Value | 95% C.I. | |
|---|---|---|---|---|---|
| Parental Age | ≤29 | 1.89 | 0.51 | 0.019 | 1.11–3.23 |
| 30–39 | 1.51 | 0.18 | 0.001 | 1.19–1.93 | |
| 40–49 | 1.34 | 0.12 | 0.001 | 1.12–1.61 | |
| ≥50 | 1 | ||||
| Parental Gender | 1.62 | 0.13 | <0.001 | 1.37–1.91 | |
| Parental Educational Level | Primary school qualification | 1.47 | 0.22 | 0.011 | 1.09–1.96 |
| High school qualification | 1.31 | 0.15 | 0.020 | 1.04–1.64 | |
| University degree | 1.24 | 0.15 | 0.071 | 0.98–1.56 | |
| Post-university Master’s degree | 1 | ||||
| Children Age | 0–5 | 1.57 | 0.21 | 0.001 | 1.21–2.04 |
| 6–10 | 1.71 | 0.17 | <0.001 | 1.40–2.07 | |
| 11–13 | 1.53 | 0.15 | <0.001 | 1.26–1.85 | |
| ≥14 | 1 | ||||
| Determinants (SAGE) | Medical advice | 0.63 | 0.07 | <0.001 | 0.51–0.78 |
| Personal beliefs | 0.74 | 0.07 | 0.001 | 0.62–0.88 | |
| Web/Social Media | 1.86 | 0.27 | <0.001 | 1.41–2.47 | |
| Television | 0.71 | 0.11 | 0.031 | 0.52–0.97 | |
| Dislike of Mandatory Vaccination Policies | 2.62 | 0.12 | <0.001 | 2.41–2.86 | |
| Change in Policies Perception | 1.5 | 0.05 | <0.001 | 1.40–1.61 | |
| Primary School Degree | High School Degree | University Degree | Post-University Master Degree | Total | ||
|---|---|---|---|---|---|---|
| Medical Advice | No | 135 (27.4) | 375 (16.5) | 211 (12.8) | 57 (10.0) | 778 (15.6) |
| Yes | 358 (72.6) | 1900 (83.5) | 1443 (87.2) | 514 (90.0) | 4215 (84.4) | |
| Web/Social Media | No | 448 (90.9) | 2107 (92.7) | 1538 (93.0) | 537 (94.0) | 4631 (92.7) |
| Yes | 45 (9.1) | 167 (7.3) | 116 (7.0) | 34 (6.0) | 362 (7.3) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Montalti, M.; Rallo, F.; Guaraldi, F.; Bartoli, L.; Po, G.; Stillo, M.; Perrone, P.; Squillace, L.; Dallolio, L.; Pandolfi, P.; et al. Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy. Vaccines 2021, 9, 366. https://doi.org/10.3390/vaccines9040366
Montalti M, Rallo F, Guaraldi F, Bartoli L, Po G, Stillo M, Perrone P, Squillace L, Dallolio L, Pandolfi P, et al. Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy. Vaccines. 2021; 9(4):366. https://doi.org/10.3390/vaccines9040366
Chicago/Turabian StyleMontalti, Marco, Flavia Rallo, Federica Guaraldi, Lapo Bartoli, Giulia Po, Michela Stillo, Paola Perrone, Lorena Squillace, Laura Dallolio, Paolo Pandolfi, and et al. 2021. "Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy" Vaccines 9, no. 4: 366. https://doi.org/10.3390/vaccines9040366
APA StyleMontalti, M., Rallo, F., Guaraldi, F., Bartoli, L., Po, G., Stillo, M., Perrone, P., Squillace, L., Dallolio, L., Pandolfi, P., Resi, D., Fantini, M. P., Reno, C., & Gori, D. (2021). Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy. Vaccines, 9(4), 366. https://doi.org/10.3390/vaccines9040366











