Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication
Abstract
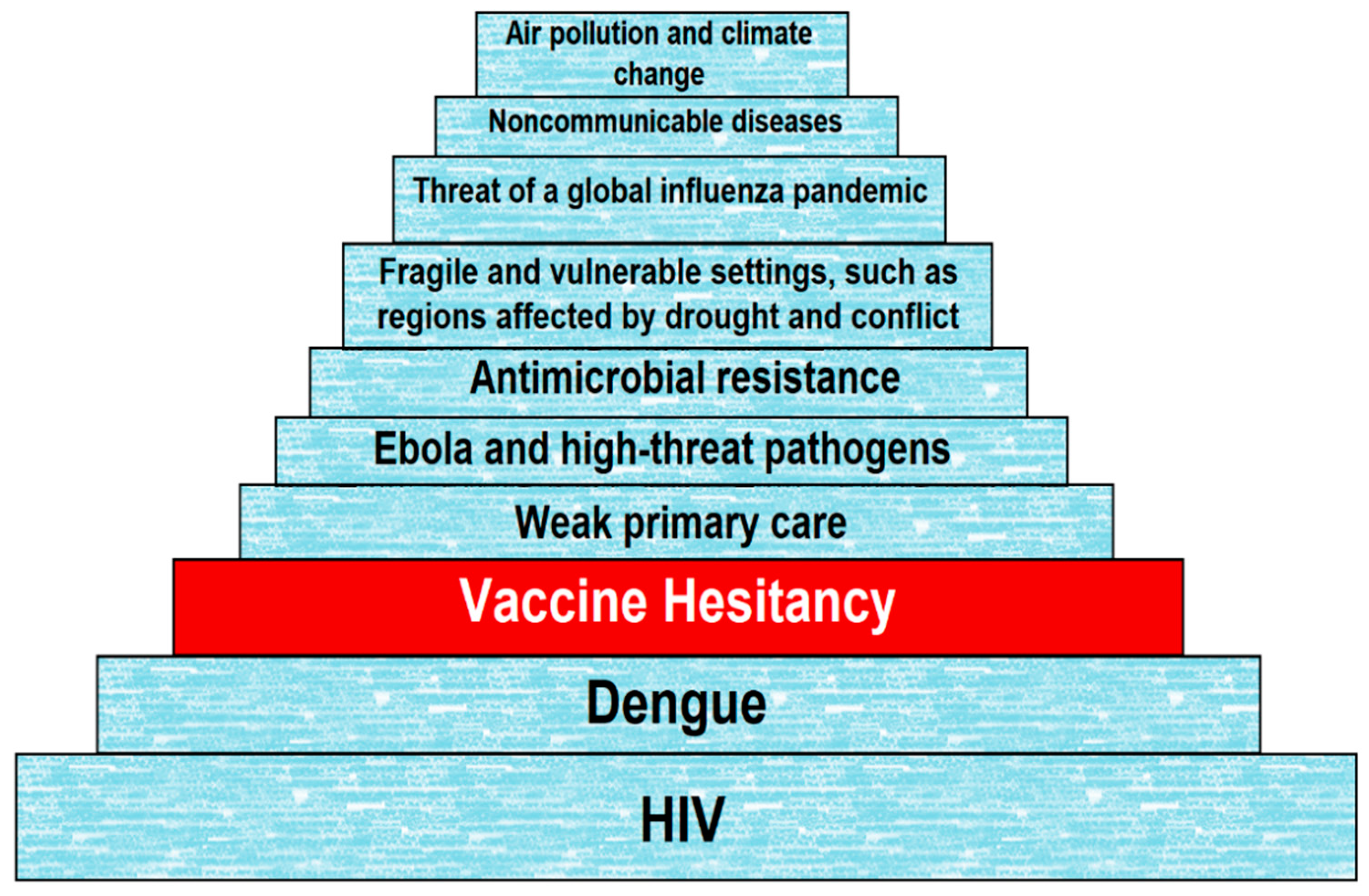
1. Introduction
2. Materials and Methods
2.1. Cameroon Demographics and Health System
2.2. Study Design
2.3. Sample Size
2.4. Data Collection
- from 0.0 to 0.2 = slight agreement
- 0.21 to 0.40 = fair agreement
- 0.41 to 0.60 = moderate agreement
- 0.61 to 0.80 = substantial agreement
- 0.81 to 1.00 = near perfect or perfect agreement.
2.5. Ethical Statement
2.6. Statistical Analysis
3. Results
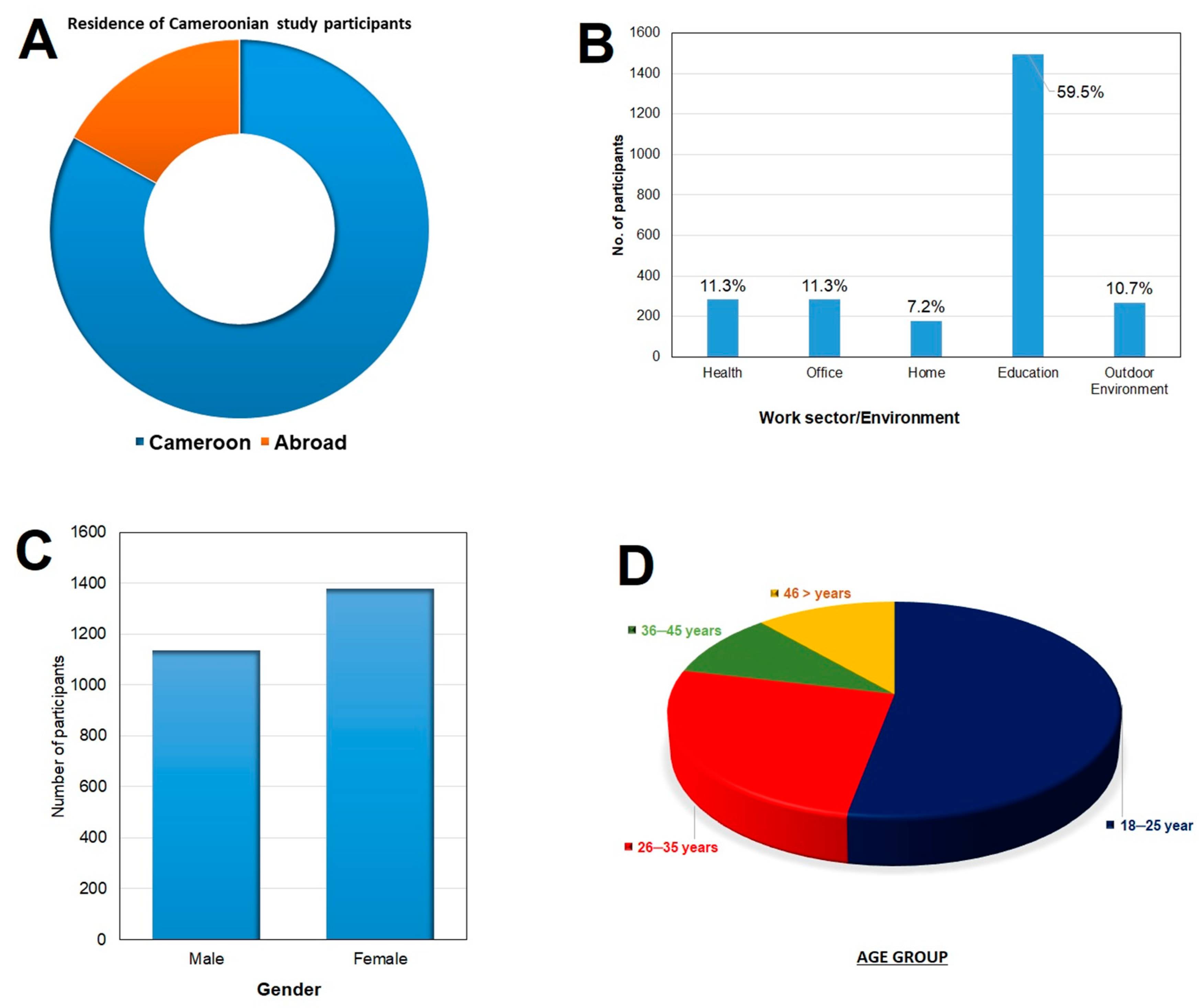
3.1. Demographic Information
3.2. Vaccine Hesitancy to a COVID-19 Vaccine
3.3. Qualitative Thematic Analysis (QTA)
3.4. Contextual Influences
3.4.1. Item 1 “Communication and Media Environment”
3.4.2. Item 7 “Perception of the Pharmaceutical Industry”
- Participant 2285 stated, “I don’t think these companies really care about our health”.
- Participant 438 opined “Vaccine companies will send suboptimal vaccines to Africa”,
- Participant 2421 affirmed, “They take advantage of the political system to come and test vaccines and other products in Africa that they would not otherwise test in their own country and hence they will not respect standard ethical procedures”.
3.4.3. Item 18 “Reliability and/or Source of Vaccine”
- Participant 942 replied “why would they label drugs and vaccines for human use as “Not for use in USA and EU?”
- Participant 1985 wondered, “the vaccine sent to Africa will be of poor standards”,
- Participant 1469 declared, “I will only accept a COVID-19 vaccine from a reliable organization that has been tested and proven effective”.
3.4.4. Item 20 “Cost”
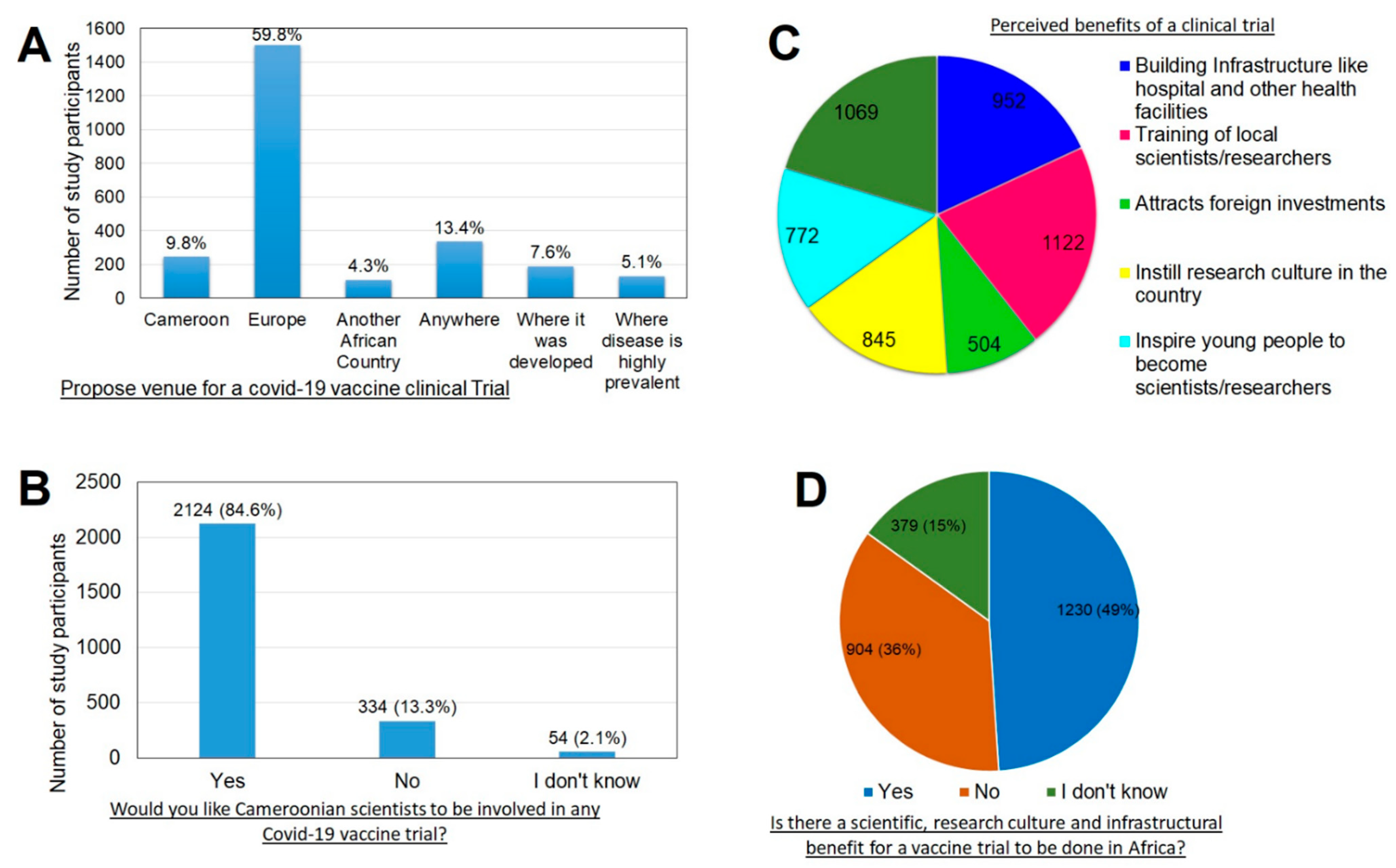
3.5. Perception of a COVID-19 Vaccine Clinical Trial
3.5.1. Proposed Venue of a Clinical Trial
3.5.2. Involving Cameroonian Scientists
3.5.3. Knowledge of the Benefits of a Clinical Trial
4. Discussion
4.1. Strengths of The Study
4.2. Limitations of The Study
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Questionnaire
- Where do you live?Cameroon Rest of the World
- Town: ………………………………
- Gender:Female Male
- Age: 18–25 years 26–35 years 36–45 years above 46 years
- Profession: ……………………………………
- Which of the following best describes your working environment?Hospital Office Home School Outdoor environment
- Is there a vaccine against COVID-19?Yes No I don’t know? Others: ……………………………………………….
- Have you heard information about the COVID-19 vaccines in development?Yes No Others: ….
- Where did you hear about this information?Social Media Government radio TV Newspapers InternetMy surroundings Others: ….
- What type of information from RELIABLE sources would you like to have on COVID-19 vaccines?Administration route Dosage Producer Country of originOthers: ……………………………………………….
- Should the COVID-19 vaccine be paid or given free of charge?Only free for children and elders Free for everybodyOnly free for health personnel Paid for everybody I don’t knowOthers: …………………………………………………………
- Would you agree to receive a COVID-19 vaccine?Yes No I will need more informationI don’t know
- Through which channel would you like to receive all valid information on a COVID-19 vaccine?In a book In a newspaper On Radio/TVInternet/Social media Others: …………………………..
- Where would you like that a covid19 vaccine trial be carried out?In Cameroon In another African countryIn EuropeOthers: …………………………..
- Would you like Cameroonian scientists to be involved in any COVID-19 vaccine trial?Yes No I don’t know
- What are the benefits of well-done clinical trial?Building Infrastructure like hospital and other health facilitiesTraining of local scientists/researchersAttracts foreign investments by international companiesInstill research culture in the countryInspire young people to become scientists/researchersbrings about new drugs, vaccines and different ways of treatmentOthers: ………………………………………..
- Is there a scientific, research culture and infrastructure benefit for a vaccine trial to be done in Africa?Yes No I don’t know
Appendix B
| Words/Ideas/Phrase/Pattern Found in the Answer of the Study Participants to the Selected Questions | Item of MxDt Attributed to |
|---|---|
| Fake news, specific/unspecifc statement to serious side reaction of absurd or serious nature | 1 |
| Information from the media about the effects of vaccines | |
| Misinformation or conspiracy-like tone information about the health system | |
| Concerns about bad or misinformation | |
| Misinformation or concerns about bad information | 2 |
| Concerns about the interest and intentions of the health system | |
| Information on past vaccination campaigns and their outcome | 3 |
| Answers related to religion, culture and gender | 4 |
| Government policies, political in nature, community perception of vaccination | 5 |
| Related to geographical barriers | 6 |
| Distance from vaccination site | |
| Trust in the health care personnel | 7 |
| Fake news, specific/unspecifc statement to serious side reaction of absurd or serious nature | |
| Giving consent | |
| Little or no information about adverse effects | |
| Little or no information about manufacturer | |
| No precise additional information | |
| Personal experience or any community member of vaccination | 8 |
| Misinformation or concerns about bad information | 9 |
| Serious side effects/reactions | |
| “afraid of” or “fear” | |
| Correct statements about vaccination | 10 |
| Failure to be informed or lack of information | |
| Serious side effects/reactions | |
| Concerns about misinformation or failure to inform oneself | |
| No precise additional information | 11 |
| Misinformation or conspiracy-like tone information about the health system | |
| Concerns about the interest and intentions of the health system | |
| Issue of trust when it comes to vaccines | |
| Giving consent | |
| “afraid of” or “fear” | 12 |
| Correct statements about vaccination | |
| Safety concerns | |
| Little or no information about adverse effects | |
| Risks and benefits | |
| Social norm | 13 |
| Community participation | |
| Necessity of vaccine | |
| Concerns about misinformation or failure to inform oneself | |
| Concerns about misinformation or failure to inform oneself | 14 |
| “afraid of” or “fear” | |
| Safety concerns and efficiency | |
| True statement or trust associated with vaccination | |
| Lack of information | |
| Little or no information about adverse effects | |
| inform about about content | |
| failure to inform oneself | |
| Lack of information of health systems or vaccine manufacturers | |
| Necessity of vaccines | |
| Little or no information about adverse effects | |
| Route of administration | |
| Old vs new vaccines | 15 |
| Route of administration | 16 |
| Misinformation or conspiracy-like tone information about the health system | 17 |
| Lack of information of health systems | |
| Reputation/misinformation about vaccination programs | |
| Lack of information of health systems | 18 |
| Availability of vaccines | |
| Lack of information on vaccine manufacturers | |
| Health issues that can lead to delay in vaccination | 19 |
| timing | |
| Distance from vaccination site | 20 |
| Availability of vaccines | |
| Low income | |
| Little or no information about adverse effects | 21 |
| Lack of information of health systems | |
| Lack of information on vaccine manufacturers | |
| Lack of information | |
| Giving consent | |
| Confidence in health care personnel | |
| Misinformation or conspiracy-like tone information about the health system |
References
- University John Hopkins. COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University. 2020. Available online: https://coronavirus.jhu.edu/map.html (accessed on 17 August 2020).
- World Health Organization. Available online: https://www.who.int/publications/m/item/draft-landscape-of-covid-19-candidate-vaccines (accessed on 8 February 2021).
- WHO. 2020. Available online: https://www.who.int/news/item/31-12-2020-who-issues-its-first-emergency-use-validation-for-a-covid-19-vaccine-and-emphasizes-need-for-equitable-global-access (accessed on 2 February 2021).
- Macdonald, N.E. SAGE Working Group on Vaccine Hesitancy. Vaccine Hesitancy 2015, 33, 4161–4164. [Google Scholar] [CrossRef] [PubMed]
- Marti, M.; De Cola, M.; Macdonald, N.E.; Dumolard, L.; Duclos, P. Assessments of global drivers of vaccine hesitancy in 2014—Looking beyond safety concerns. PLoS ONE 2017, 12, e0172310. [Google Scholar] [CrossRef] [PubMed]
- Lane, S.; Macdonald, N.E.; Marti, M.; Dumolard, L. Vaccine hesitancy around the globe: Analysis of three years of WHO/UNICEF Joint Reporting Form data-2015–2017. Vaccine 2018, 36, 3861–3867. [Google Scholar] [CrossRef]
- World Health Organization. 2018 Assessment Report of the Global Vaccine Action Plan. 2018. Available online: https://apps.who.int/iris/bitstream/handle/10665/276967/WHO-IVB-18.11-eng.pdf?ua=1 (accessed on 21 August 2020).
- World Health Organization. Ten threats to global health in 2019. 2019. Available online: https://www.who.int/news-room/feature-stories/ten-threats-to-global-health-in-2019 (accessed on 20 August 2020).
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J.A. Vaccine hesitancy: An overview. Hum. Vaccine Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef] [PubMed]
- Larson, H.J.; Jarrett, C.; Eckersberger, E.; Smith, D.M.D.; Paterson, P. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: A systematic review of published literature, 2007–2012. Vaccine 2014, 32, 2150–2159. [Google Scholar] [CrossRef] [PubMed]
- Taddio, A. Setting the stage for improved practices during vaccine injections: A knowledge synthesis of interventions for the management of pain and fear. Clin. J. Pain. 2015, 31, S1–S2. [Google Scholar] [CrossRef] [PubMed]
- Kata, A. Anti-vaccine activists, Web 2.0, and the postmodern paradigm—An overview of tactics and tropes used online by the anti-vaccination movement. Vaccine 2012, 30, 3778–3789. [Google Scholar] [CrossRef] [PubMed]
- Betsch, C.; Brewer, N.T.; Brocard, P.; Davies, P.; Gaissmaier, W.; Haase, N.; Leask, J.; Renkewitz, F.; Renner, B.; Reyna, V.F.; et al. Opportunities and challenges of Web 2.0 for vaccination decisions. Vaccine 2012, 30, 3727–3733. [Google Scholar] [CrossRef]
- Kennedy, A.; Lavail, K.; Nowak, G.; Basket, M.; Landry, S. Confidence about vaccines in the United States: Understanding parents’ perceptions. Health Aff. 2011, 30, 1151–1159. [Google Scholar] [CrossRef]
- Cooper, L.; Larson, H.; Katz, S. Protecting public trust in immunization. Pediatrics 2008, 122, 149–153. [Google Scholar] [CrossRef]
- Dubé, E.; A Bettinger, J.; A Fisher, W.; Naus, M.; Mahmud, S.M.; Hilderman, T. Vaccine acceptance, hesitancy and refusal in Canada: Challenges and potential approaches. Can. Commun. Dis. Rep. 2016, 42, 246–251. [Google Scholar] [CrossRef]
- Kahan, D.M. A Risky Science Communication Environment for Vaccines. Science 2013, 342, 53–54. [Google Scholar] [CrossRef] [PubMed]
- Hobson-West, P. Understanding vaccination resistance: Moving beyond risk. Health Risk Soc. 2003, 5, 273–283. [Google Scholar] [CrossRef]
- Streefland, P.; Chowdhury, A.; Ramos-Jimenez, P. Patterns of vaccination acceptance. Soc. Sci. Med. 1999, 49, 1705–1716. [Google Scholar] [CrossRef]
- Worldometer. Cameroon Demographics. Worldometer. 2020. Available online: https://www.worldometers.info/demographics/cameroon-demographics/ (accessed on 16 September 2020).
- MINSANTE. Health Sector Strategy 2016–2027. Available online: https://www.minsante.cm/site/?q=en/content/health-sector-strategy-2016-2027-0 (accessed on 1 September 2020).
- World Health Organization. Report of the SAGE Working Group on Vaccine hesitancy. Available online: https://www.who.int/immunization/sage/meetings/2014/october/1_Report_WORKING_GROUP_vaccine_hesitancy_final.pdf (accessed on 16 September 2020).
- Raosoft Inc. Available online: http://www.raosoft.com/samplesize.html (accessed on 1 May 2020).
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Miko, D.; Costache, C.; Colosi, H.A.; Neculicioiu, V.; Colosi, I.A. Qualitative Assessment of Vaccine Hesitancy in Romania. Medicina 2019, 55, 282. [Google Scholar] [CrossRef]
- Freelon, D.G. ReCal: Intercoder Reliability Calculation as a Web Service. Int. J. Internet Sci. 2010, 8, 10–16. [Google Scholar]
- Hallgren, K.A. NIH Public Access. Tutor Quant Methods Psychol. 2012, 8, 23–24. [Google Scholar] [CrossRef]
- Murrero, M.; Rice, R.E. The Internet and Health Care: Theory, Research and Practice; Routledge: Abingdon, UK, 2013. [Google Scholar]
- Betsch, C.; Sachse, K. Dr. Jekyll or Mr. Hyde? (How) the Internet influences vaccination decisions: Recent evidence and tentative guidelines for online vaccine communication. Vaccine 2012, 28, 3723–3726. [Google Scholar] [CrossRef] [PubMed]
- Kang, G.J.; Ewing-Nelson, S.R.; Mackey, L.; Schlitt, J.T.; Marathe, A.; Abbas, K.M.; Swarup, S. Semantic network analysis of vaccine sentiment in online social media. Vaccine 2017, 35, 3621–3638. [Google Scholar] [CrossRef] [PubMed]
- Ropeik, D. How society should respond to the risk of vaccine rejection. Hum. Vaccine Immunother. 2013, 9, 1815–1818. [Google Scholar] [CrossRef] [PubMed]
- Bennett, S. New Places; New Cultures; New Experiences: Why Travel Broadens the Mind. 2019. Available online: https://lesroches.edu/blog/how-travel-broadens-mind/ (accessed on 9 September 2020).
- Dubé, E.; Gagnon, D.; Nickels, E.; Jeram, S.; Schuster, M. Mapping vaccine hesitancy-Country-specific characteristics of a global phenomenon. Vaccine 2014, 32, 6649–6654. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, G.K.; Tatar, O.; Dube, E.; Amsel, R.; Knauper, B.; Naz, A.; Perez, S.; Rosberger, Z. The vaccine hesitancy scale: Psychometric properties and validation. Vaccine 2018, 36, 660–667. [Google Scholar] [CrossRef] [PubMed]
| Contextual influences | 1 | Communication & media environment |
| 2 | Influential leaders, immune | |
| 3 | Historical influences | |
| 4 | Religion/culture/gender/socio-economic | |
| 5 | Politics/policies | |
| 6 | Geographical barriers | |
| 7 | Perception of pharmaceutical industry | |
| Individual and group influences | 8 | Personal, family, and/or community member experience with vaccination, including pain |
| 9 | Beliefs, attitudes | |
| 10 | Knowledge/awareness | |
| 11 | Health system and providers-trust and personal experience | |
| 12 | Risk/benefits (perceived, heuristics) | |
| 13 | Immunization as a social norm | |
| Vaccine/vaccination specific issues | 14 | Risk/benefits (epidemiological and scientific evidence) |
| 15 | Introduction of a new vaccine | |
| 16 | Mode of administration | |
| 17 | Design of vaccination program | |
| 18 | Reliability and/or source of vaccine | |
| 19 | Vaccination schedule | |
| 20 | Costs | |
| 21 | Strength of recommendation |
| Item | Percent Agreement | Scott’s Pi | Cohen’s Kappa | Krippendorff’s Alpha | No. of Agreements | No. of Disagreements | No. Cases | No. of Decisions |
|---|---|---|---|---|---|---|---|---|
| Item 1 | 99.84 | 0.996 | 0.996 | 0.996 | 3691 | 6 | 3697 | 7394 |
| Item 2 | 99.78 | 0.966 | 0.967 | 0.967 | 3689 | 8 | 3697 | 7394 |
| Item 3 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 4 | 99.92 | 0.998 | 0.998 | 0.998 | 3694 | 3 | 3697 | 7394 |
| Item 5 | 99.84 | 0.978 | 0.978 | 0.978 | 3691 | 6 | 3697 | 7394 |
| Item 6 | 99.97 | −0.001 | 0 | 0.000 | 3696 | 1 | 3697 | 7394 |
| Item 7 | 99.59 | 0.988 | 0.988 | 0.988 | 3682 | 15 | 3697 | 7394 |
| Item 8 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 9 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 10 | 99.89 | 0.997 | 0.998 | 0.998 | 3693 | 4 | 3697 | 7394 |
| Item 11 | 99.95 | 0.994 | 0.994 | 0.994 | 3695 | 2 | 3697 | 7394 |
| Item 12 | 99.92 | 0.996 | 0.996 | 0.996 | 3694 | 3 | 3697 | 7394 |
| Item 13 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 14 | 99.76 | 0.995 | 0.995 | 0.995 | 3688 | 9 | 3697 | 7394 |
| Item 15 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 16 | 99.65 | 0.992 | 0.992 | 0.992 | 3684 | 13 | 3697 | 7394 |
| Item 17 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 18 | 99.24 | 0.969 | 0.969 | 0.969 | 3669 | 28 | 3697 | 7394 |
| Item 19 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| Item 20 | 99.62 | 0.992 | 0.992 | 0.992 | 3683 | 14 | 3697 | 7394 |
| Item 21 | 100 | 1 | 1 | 1 | 3697 | 0 | 3697 | 7394 |
| SAGE WG Vaccine Hesitancy Model a | |||||
|---|---|---|---|---|---|
| Contextual Influences | Individual and Group Influences | Vaccine and Vaccination-Specific Issues | |||
| Item | Iterations | Item | Iterations | Item | Iterations |
| 1 | 2356 | 8 | 80 | 14 | 1314 |
| 2 | 120 | 9 | 214 | 15 | 208 |
| 3 | 30 | 10 | 1362 | 16 | 1338 |
| 4 | 974 | 11 | 170 | 17 | 22 |
| 5 | 138 | 12 | 380 | 18 | 3184 |
| 6 | 0 | 13 | 30 | 19 | 2 b |
| 7 | 2878 | 20 | 2072 | ||
| 21 | 120 | ||||
| TOTAL | 6494 (38.2%) | TOTAL | 2236 (13.2%) | TOTAL | 8260 (48.6%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dinga, J.N.; Sinda, L.K.; Titanji, V.P.K. Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication. Vaccines 2021, 9, 175. https://doi.org/10.3390/vaccines9020175
Dinga JN, Sinda LK, Titanji VPK. Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication. Vaccines. 2021; 9(2):175. https://doi.org/10.3390/vaccines9020175
Chicago/Turabian StyleDinga, Jerome Nyhalah, Leontine Kouemou Sinda, and Vincent P. K. Titanji. 2021. "Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication" Vaccines 9, no. 2: 175. https://doi.org/10.3390/vaccines9020175
APA StyleDinga, J. N., Sinda, L. K., & Titanji, V. P. K. (2021). Assessment of Vaccine Hesitancy to a COVID-19 Vaccine in Cameroonian Adults and Its Global Implication. Vaccines, 9(2), 175. https://doi.org/10.3390/vaccines9020175






