Serum Antibody Response Comparison and Adverse Reaction Analysis in Healthcare Workers Vaccinated with the BNT162b2 or ChAdOx1 COVID-19 Vaccine
Abstract
:1. Introduction
2. Methods
2.1. Study Design and Participants
2.2. Serological Assays
2.3. Outcomes
2.4. Statistical Analysis
3. Results
3.1. Demographics of Participants
3.2. Serology Results
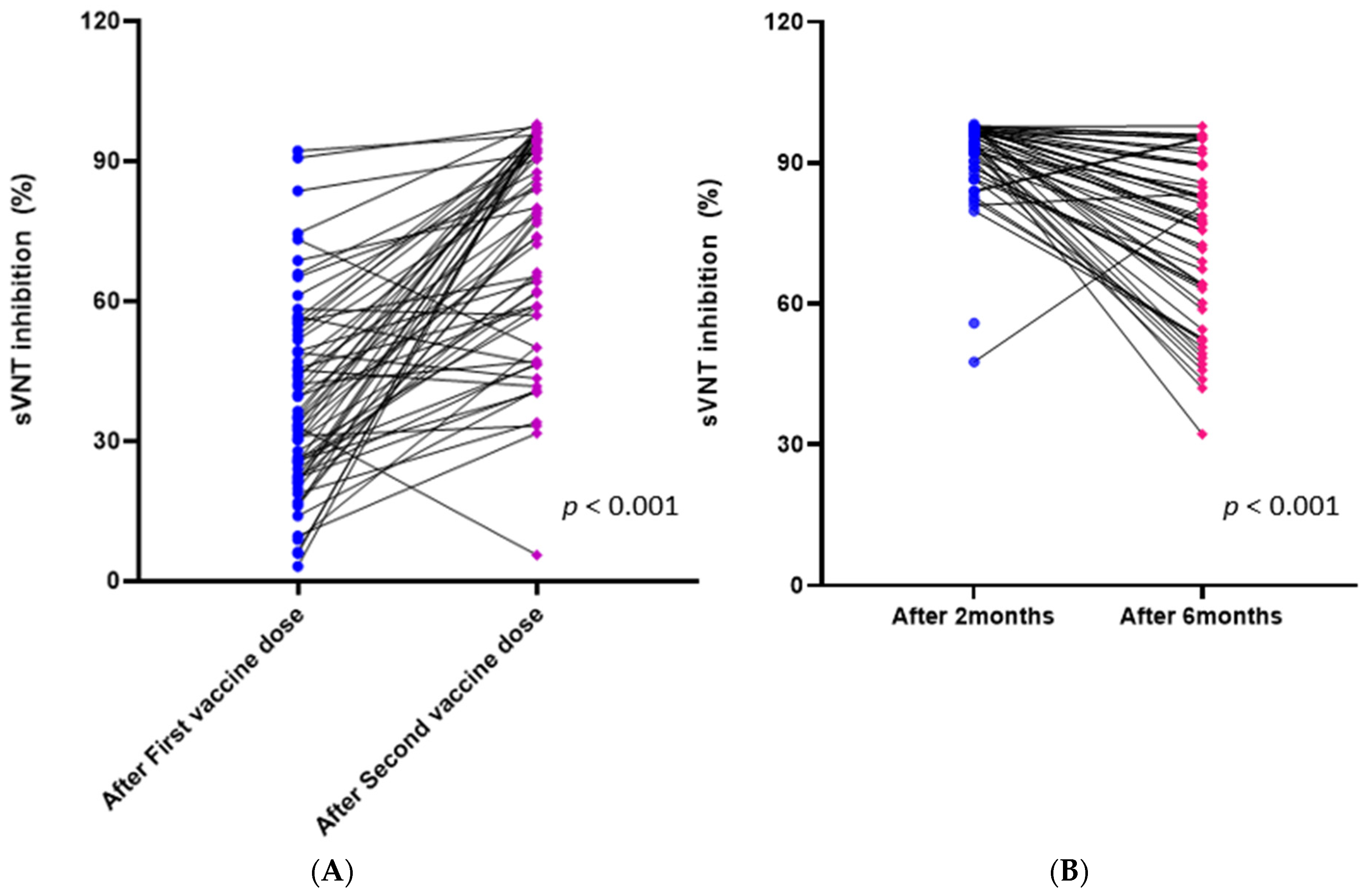
3.3. Changes in Immune Response in the BNT162b2 Group
3.4. Adverse Events
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef] [Green Version]
- WHO. Coronavirus Disease (COVID-19) Dashboard. 2021. Available online: https://covid19.who.int (accessed on 1 July 2021).
- CDC (Central Disease Control). Coronavirus (COVID-19) Dashboard, Republic of Korea. 2021. Available online: http://ncov.mohw.go.kr/en/ (accessed on 15 July 2021).
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Pérez Marc, G.; Moreira, E.D.; Zerbini, C.; et al. Safety and Efficacy of the BNT162b2 mRNA COVID-19 Vaccine. N. Engl. J. Med. 2020, 383, 2603–2615. [Google Scholar] [CrossRef] [PubMed]
- Voysey, M.; Clemens, S.A.C.; Madhi, S.A.; Weckx, L.Y.; Folegatti, P.M.; Aley, P.K.; Angus, B.; Baillie, V.L.; Barnabas, S.L.; Bhorat, Q.E.; et al. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: An interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. Lancet 2021, 397, 99–111. [Google Scholar] [CrossRef]
- Baden, L.R.; El Sahly, H.M. Efficacy and Safety of the mRNA-1273 SARS-CoV-2 Vaccine. N. Engl. J. Med. 2021, 384, 403–416. [Google Scholar] [CrossRef] [PubMed]
- Tan, C.W.; Chia, W.N.; Qin, X.; Liu, P.; Chen, M.I.; Tiu, C.; Hu, Z.; Chen, V.C. A SARS-CoV-2 surrogate virus neutralization test based on antibody-mediated blockage of ACE2-spike protein-protein interaction. Nat. Biotechnol. 2020, 38, 1073–1078. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S.C.; Hurst, B.; Charlton, C.L. A New SARS-CoV-2 Dual-Purpose Serology Test: Highly Accurate Infection Tracing and Neutralizing Antibody Response Detection. J. Clin. Microbiol. 2021, 59, e02438-20. [Google Scholar] [CrossRef] [PubMed]
- Hinton, R.D.M. Table of Tests Acceptable for Use in the Manufacture of High Titer COVID-19. Convalescent Plasma. 2021. Available online: https://www.covid19treatmentguidelines.nih.gov/therapies/anti-sars-cov-2-antibody-products/convalescent-plasma/ (accessed on 20 November 2021).
- Padoan, A.; Bonfante, F.; Pagliari, M.; Bortolami, A.; Negrini, D.; Zuin, S.; Bozzato, D.; Cosma, C.; Sciacovelli, L.; Plebani, M. Analytical and clinical performances of five immunoassays for the detection of SARS-CoV-2 antibodies in comparison with neutralization activity. EBioMedicine 2020, 62, 103101. [Google Scholar] [CrossRef] [PubMed]
- Addetia, A.; Crawford, K.H.D.; Dingens, A.; Zhu, H.; Roychoudhury, P.; Huang, M.L.; Jerome, K.R.; Bloom, J.D. Neutralizing Antibodies Correlate with Protection from SARS-CoV-2 in Humans during a Fishery Vessel Outbreak with a High Attack Rate. Clin. Microbiol. 2020, 58, e02107-20. [Google Scholar] [CrossRef] [PubMed]
- Khoury, D.S.; Cromer, D. Neutralizing antibody levels are highly predictive of immune protection from symptomatic SARS-CoV-2 infection. Nat. Med. 2021, 27, 1205–1211. [Google Scholar] [CrossRef] [PubMed]
- Bošnjak, B.; Stein, S.C.; Willenzon, S.; Cordes, A.K.; Puppe, W.; Bernhardt, G.; Ravens, I.; Ritter, C.; Schultze-Florey, C.R.; Gödecke, N.; et al. Low serum neutralizing anti-SARS-CoV-2 S antibody levels in mildly affected COVID-19 convalescent patients revealed by two different detection methods. Cell. Mol. Immunol. 2021, 18, 936–944. [Google Scholar] [CrossRef] [PubMed]
- Park, J.Y.; Choi, S.H. Systemic Adverse Events and Use of Antipyretics Predict the Neutralizing Antibody Positivity Early after the First Dose of ChAdOx1 Coronavirus Disease Vaccine. J. Clin. Med. 2021, 10, 2844. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.; Park, S.Y.; Yu, S.; Park, J.W.; Lee, E.; Jeon, M.H.; Kim, T.H.; Choo, E.J. Impacts of Side Effects to BNT162b2 and the First Dose of ChAdOx1 Anti-SARS-CoV-2 Vaccination on Work Productivity, the Need for Medical Attention, and Vaccine Acceptance: A Multicenter Survey on Healthcare Workers in Referral Teaching Hospitals in the Republic of Korea. Vaccines 2021, 9, 648. [Google Scholar] [CrossRef] [PubMed]
- Cox, R.J.; Brokstad, K.A. Not just antibodies: B cells and T cells mediate immunity to COVID-19. Nat. Rev. Immunol. 2020, 20, 581–582. [Google Scholar] [CrossRef] [PubMed]
- Naaber, P.; Tserel, L.; Kangro, K.; Sepp, E.; Jürjenson, V.; Adamson, A.; Haljasmägi, L.; Rumm, A.P.; Maruste, R.; Kärner, J.; et al. Dynamics of antibody response to BNT162b2 vaccine after six months: A longitudinal prospective study. Lancet Reg. Health Eur. 2021, 10, 100208. [Google Scholar] [CrossRef] [PubMed]
- Chia, W.N.; Zhu, F.; Ong, S.W.X.; Young, B.E.; Fong, S.W.; Le Bert, N.; Tan, C.W.; Tiu, C.; Zhang, J.; Tan, S.Y.; et al. Dynamics of SARS-CoV-2 neutralising antibody responses and duration of immunity: A longitudinal study. Lancet Microbe 2021, 2, e240–e249. [Google Scholar] [CrossRef]
- Tartof, S.Y.; Slezak, J.M.; Fischer, H.; Hong, V.; Ackerson, B.K.; Ranasinghe, O.N.; Frankland, T.B.; Ogun, O.A.; Zamparo, J.M.; Gray, S.; et al. Effectiveness of mRNA BNT162b2 COVID-19 vaccine up to 6 months in a large integrated health system in the USA: A retrospective cohort study. Lancet 2021, 398, 1407–1416. [Google Scholar] [CrossRef]


| Variables | ChAdOx1 (AstraZeneca/Oxford) Group (n = 65) | BNT162b2 (Pfizer) Group (n = 50) | p Value |
|---|---|---|---|
| Age, years | |||
| Mean ± SD (range) | 41.7 ± 13.6 (23–72) | 43.5 ± 9.35 (24–60) | 0.411 |
| Sex | 0.826 | ||
| Male | 16 (24.6) | 11 (22.0) | |
| Female | 49 (75.4) | 39 (78.0) | |
| Previous allergy/anaphylaxis history | 0.079 | ||
| None | 62 (95.4%) | 41 (82.0%) | |
| Drug/Food | 2 (3.1%) | 5 (10.0%) | |
| Anaphylaxis to drug/food | 0 | 2 (4.0%) | |
| Vaccine allergy | 0 | 2 (4.0%) | |
| Vaccine anaphylaxis | 1 (1.5%) | 0 | |
| Days post 2nd vaccination, mean/median (range) | 56.1/56.0 (41–57) | 56.9/56.0 (54–63) | 0.999 |
| ChAdOx1 (AstraZeneca/Oxford) Group (n = 65) | BNT162b2 (Pfizer) Group (n = 50) | ||
|---|---|---|---|
| Seropositive, No (%) | 64 (98.5) | 50 (100) | 0.999 |
| sVNT inhibition (%) | |||
| Mean ± Std | 73.25 ± 22.57 | 91.44 ± 9.68 | <0.01 |
| Median | 79.05 | 94.48 | |
| Q1, Q3 | 57.01, 93.76 | 89.37, 97.08 | |
| Range | 5.64~97.94 | 47.67~98.25 | |
| Presumed Protection Rates of COVID-19 * | |||
| ≥68% *, No (%) | 39 (60.0) | 48 (96.0) | <0.01 |
| <68%, No (%) | 26 (40.0) | 2 (4.0) | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lim, S.-H.; Choi, S.-H.; Kim, B.; Kim, J.-Y.; Ji, Y.-S.; Kim, S.-H.; Kim, C.-K.; Kim, T.; Choo, E.-J.; Moon, J.-E.; et al. Serum Antibody Response Comparison and Adverse Reaction Analysis in Healthcare Workers Vaccinated with the BNT162b2 or ChAdOx1 COVID-19 Vaccine. Vaccines 2021, 9, 1379. https://doi.org/10.3390/vaccines9121379
Lim S-H, Choi S-H, Kim B, Kim J-Y, Ji Y-S, Kim S-H, Kim C-K, Kim T, Choo E-J, Moon J-E, et al. Serum Antibody Response Comparison and Adverse Reaction Analysis in Healthcare Workers Vaccinated with the BNT162b2 or ChAdOx1 COVID-19 Vaccine. Vaccines. 2021; 9(12):1379. https://doi.org/10.3390/vaccines9121379
Chicago/Turabian StyleLim, Sung-Hee, Seong-Hyeok Choi, Bora Kim, Ji-Youn Kim, Young-Sok Ji, Se-Hyung Kim, Chan-Kyu Kim, Tark Kim, Eun-Ju Choo, Ji-Eun Moon, and et al. 2021. "Serum Antibody Response Comparison and Adverse Reaction Analysis in Healthcare Workers Vaccinated with the BNT162b2 or ChAdOx1 COVID-19 Vaccine" Vaccines 9, no. 12: 1379. https://doi.org/10.3390/vaccines9121379
APA StyleLim, S.-H., Choi, S.-H., Kim, B., Kim, J.-Y., Ji, Y.-S., Kim, S.-H., Kim, C.-K., Kim, T., Choo, E.-J., Moon, J.-E., Yun, J., & Park, S.-K. (2021). Serum Antibody Response Comparison and Adverse Reaction Analysis in Healthcare Workers Vaccinated with the BNT162b2 or ChAdOx1 COVID-19 Vaccine. Vaccines, 9(12), 1379. https://doi.org/10.3390/vaccines9121379






