Analysis of the Effectiveness of Measures on the COVID-19 Vaccination Rate in Hong Kong
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Data Collection
2.2. Data Analysis
3. Results
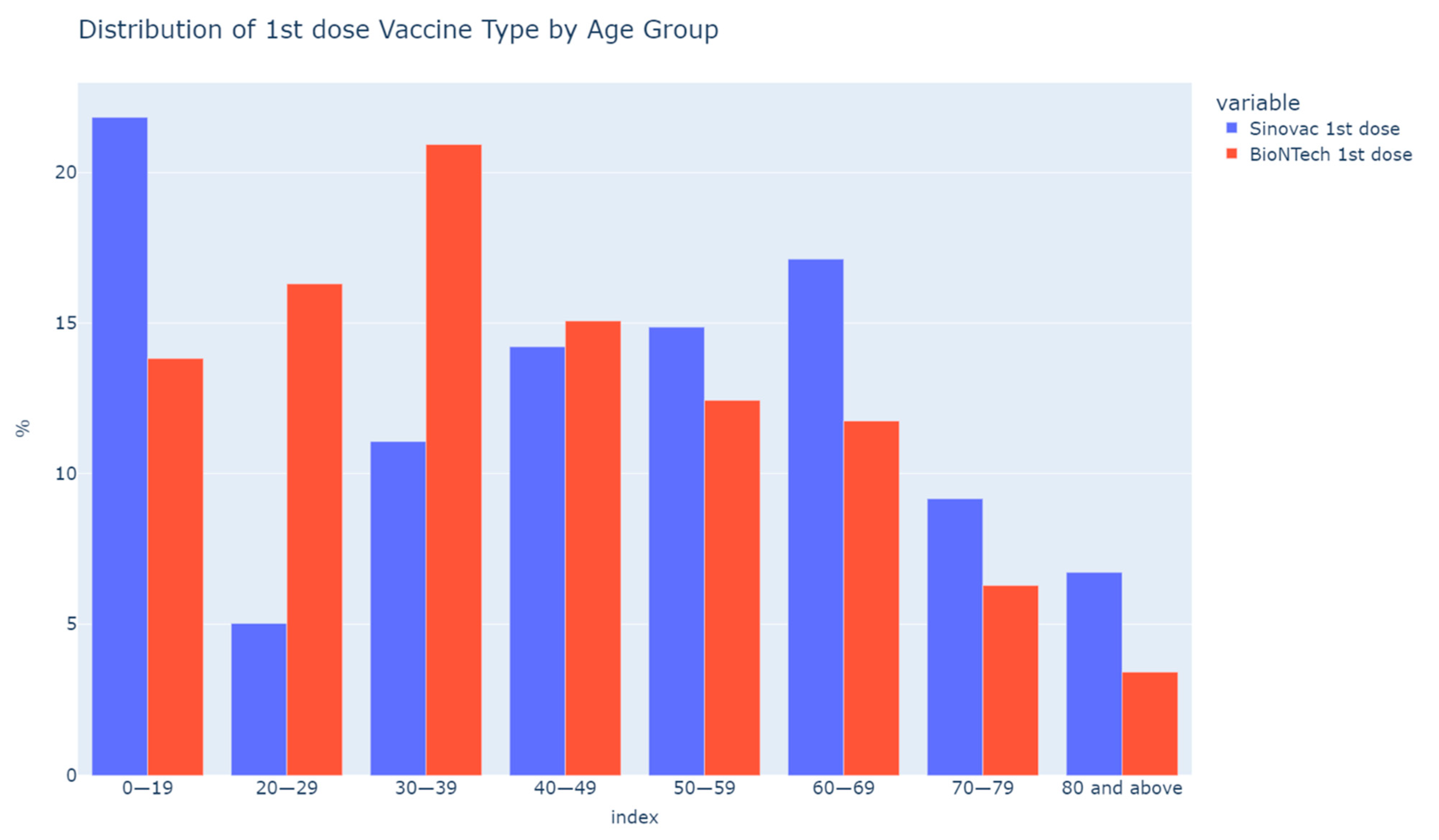
3.1. Study Participants and Characteristics
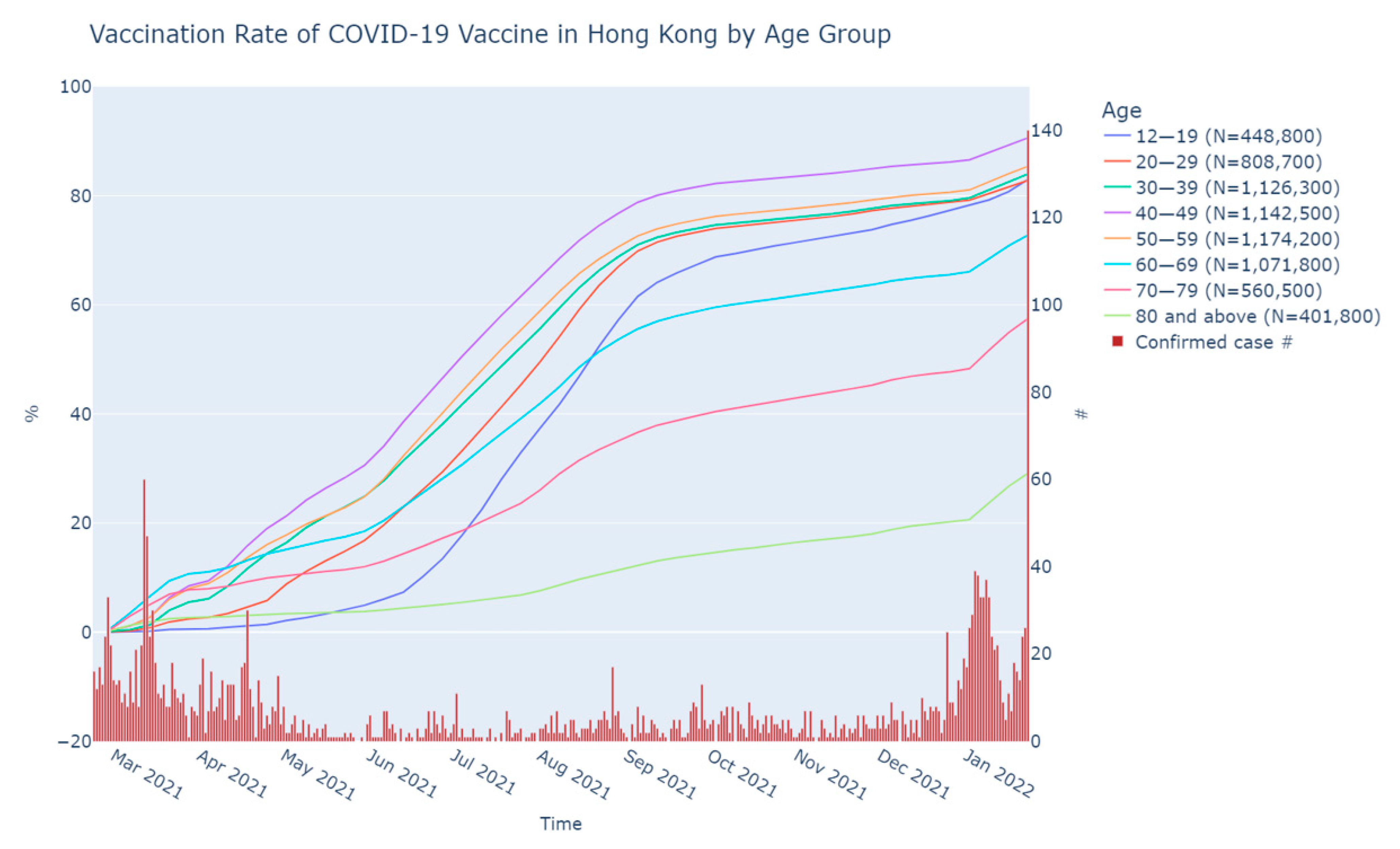
3.2. Vaccination Rate by Age
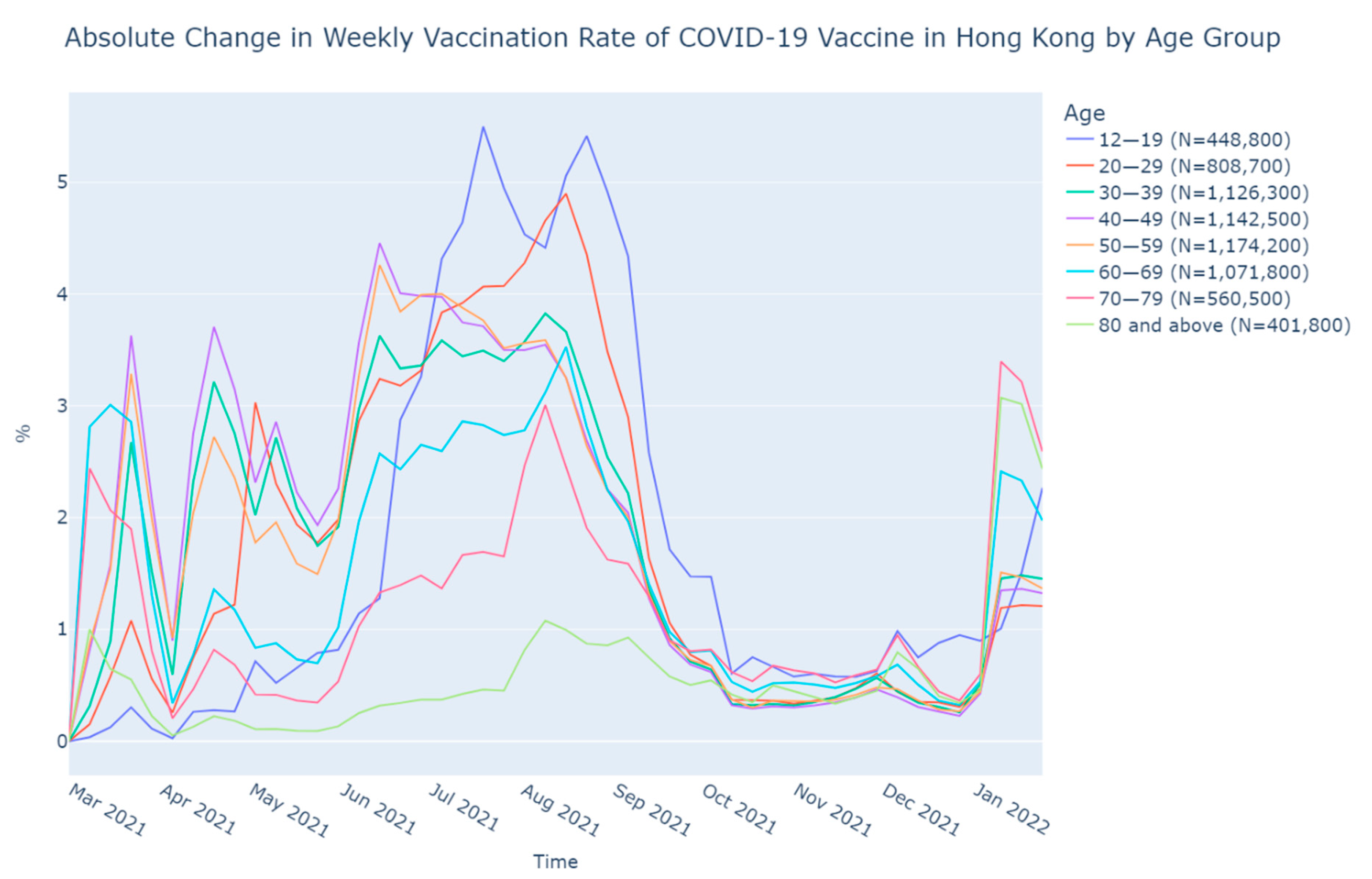
3.3. Absolute Change in Weekly Vaccination Rate by Age
3.4. Effectiveness of Measures
3.4.1. Eligibility
3.4.2. Accessibility
3.4.3. Incentive
3.4.4. Restriction
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AVR | Acceleration of Vaccination Rate |
| AWAVR | Age-Weighted Acceleration of Vaccination Rate |
| BioNTech | Fosun Pharma/BioNTech (BioNTech) Vaccine |
| COVID-19 | Coronavirus disease 2019 |
| CVC | Community Vaccination Centres |
| HK | Hong Kong |
| Sinovac | Sinovac Biotech (Hong Kong) Limited |
| VR | Vaccination Rate |
| WHO | World Health Organization |
References
- World Health Organization. WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 28 January 2022).
- U.S. Food & Drug Administration. Emergency Use Authorization. 2022. Available online: https://www.fda.gov/emergency-preparedness-and-response/mcm-legal-regulatory-and-policy-framework/emergency-use-authorization (accessed on 28 January 2022).
- Glatman-Freedman, A.; Bromberg, M.; Dichtiar, R.; Hershkovitz, Y.; Keinan-Boker, L. The BNT162b2 vaccine effectiveness against new COVID-19 cases and complications of breakthrough cases: A nation-wide retrospective longitudinal multiple cohort analysis using individualised data. EBioMedicine 2021, 72, 103574. [Google Scholar] [CrossRef] [PubMed]
- Mathieu, E.; Ritchie, H.; Ortiz-Ospina, E.; Roser, M.; Hasell, J.; Appel, C.; Rodés-Guirao, L. A global database of COVID-19 vaccinations. Nat. Hum. Behav. 2021, 5, 947–953. [Google Scholar] [CrossRef] [PubMed]
- The Government of the Hong Kong Special Administrative Region. SFH Authorises COVID-19 Vaccine by Fosun Pharma/BioNTech for Emergency Use in Hong Kong. Available online: https://www.info.gov.hk/gia/general/202101/25/P2021012500829.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. SFH Authorises COVID-19 Vaccine by Sinovac for Emergency use in Hong Kong. Available online: https://www.info.gov.hk/gia/general/202102/18/P2021021800495.htm (accessed on 28 January 2022).
- Cheng, S.M.S.; Mok, C.K.P.; Leung, Y.W.Y.; Ng, S.S.; Chan, K.C.K.; Ko, F.W.; Chen, C.; Yiu, K.; Lam, B.H.S.; Lau, E.H.Y.; et al. Neutralizing antibodies against the SARS-CoV-2 Omicron variant BA.1 following homologous and heterologous CoronaVac or BNT162b2 vaccination. Nat. Med. 2022, 28, 486–489. [Google Scholar] [CrossRef]
- Self, W.H.; Tenforde, M.W.; Rhoads, J.P.; Gaglani, M.; Ginde, A.A.; Douin, D.J.; Olson, S.M.; Talbot, H.K.; Casey, J.D.; Mohr, N.M.; et al. Comparative effectiveness of Moderna, Pfizer-BioNTech, and Janssen (Johnson & Johnson) vaccines in preventing COVID-19 hospitalizations among adults without immunocompromising conditions—United States, March–August 2021. Morb. Mortal. Wkly. Rep. 2021, 70, 1337. [Google Scholar]
- LKS Faculty of Medicine The University of Hong Kong. Real-Time Population Data on Vaccine Confidence. Available online: http://www.med.hku.hk/en/news/press/-/media/DBC3EE616CDF475C9C402F72A844D5C1.ashx (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Hong Kong Vaccination Dashboard. 2022. Available online: https://www.covidvaccine.gov.hk/en/dashboard (accessed on 28 January 2022).
- Global Change Data Lab. Coronavirus (COVID-19) Vaccinations. Available online: https://ourworldindata.org/covid-vaccinations (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. COVID-19 Vaccination Programme Opens to Persons Aged 16 or Above. Available online: https://www.info.gov.hk/gia/general/202104/15/P2021041500565.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Scientific Committees under CHP Issue Consensus Interim Recommendations on COVID-19 Vaccination. Available online: https://www.info.gov.hk/gia/general/202109/15/P2021091501003.htm?fontSize=1. (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. First School has Students Get Vaccinated at Community Vaccination Centre Via Group Booking (with Photos/Video). Available online: https://www.info.gov.hk/gia/general/202106/21/P2021062100431.htm. (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Outreach Vaccination Arrangement for RCHs under COVID-19 Vaccination Programme Starts. Available online: https://www.info.gov.hk/gia/general/202104/13/P2021041300415.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Vaccination Leave for Government Employees after COVID-19 Vaccination. Available online: https://www.info.gov.hk/gia/general/202105/31/P2021053100575.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Same-Day Tickets for elderly to Receive COVID-19 Vaccination to be Distributed from Thursday. Available online: https://www.info.gov.hk/gia/general/202107/27/P2021072700240.htm (accessed on 28 January 2022).
- Group, S. Registration for Lucky Draw Opens on 15 June 2021. Available online: https://www.sino.com/en/media-centre/press-release/2021/registration-for-lucky-draw-opens-on-15-june-2021/ (accessed on 28 January 2022).
- Education Bureau Government Secretariat; The Government of the Hong Kong Special Administrative Region. Face-to-Face Class Arrangements for Schools in Hong Kong in the 2021/22 School Year-Recommendation on Students Aged 12 to 17 Years to Receive One Dose of the Comirnaty Vaccine. Available online: https://www.edb.gov.hk/attachment/en/sch-admin/admin/about-sch/diseases-prevention/edb_20210916_eng.pdf (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Further Measures to Push forward COVID-19 Vaccination of Government Employees. Available online: https://www.info.gov.hk/gia/general/202111/09/P2021110900700.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. COVID-19 Vaccination in Lieu of Regular Testing Arrangement for Government Employees to be Further Tightened. Available online: https://www.info.gov.hk/gia/general/202112/21/P2021122100384.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Vaccination in Lieu of Regular Testing Arrangement Covers all Government Employees. Available online: https://www.info.gov.hk/gia/general/202108/02/P2021080200742.htm (accessed on 28 January 2022).
- The Government of the Hong Kong Special Administrative Region. Vaccine Bubble Expansion on 24 February 2022. Available online: https://www.news.gov.hk/eng/2022/01/20220104/20220104_104319_940.html (accessed on 28 January 2022).
- National Health Service. COVID-19 Vaccination Statistics. Available online: https://www.england.nhs.uk/statistics/wp-content/uploads/sites/2/2021/12/COVID-19-weekly-announced-vaccinations-23-December-2021.pdf (accessed on 28 January 2022).
- Centers for Disease Control and Prevention. COVID-19 Vaccination and Case Trends by Age Group, United States Vaccinations. 2022. Available online: https://data.cdc.gov/Vaccinations/COVID-19-Vaccination-and-Case-Trends-by-Age-Group-/gxj9-t96f (accessed on 28 January 2022).
- Staddon, J.E.; Cerutti, D.T. Operant conditioning. Annu. Rev. Psychol. 2003, 54, 115–144. [Google Scholar] [CrossRef] [Green Version]
- Campos-Mercade, P.; Meier, A.N.; Schneider, F.H.; Meier, S.; Pope, D.; Wengström, E. Monetary incentives increase COVID-19 vaccinations. Science 2021, 374, 879–882. [Google Scholar] [CrossRef] [PubMed]
- Sehgal, N.K. Impact of Vax-a-Million lottery on COVID-19 vaccination rates in Ohio. Am. J. Med. 2021, 134, 1424–1426. [Google Scholar] [CrossRef] [PubMed]
- Zhai, Y.; Santibanez, T.A.; Kahn, K.E.; Black, C.L.; de Perio, M.A. Paid sick leave benefits, influenza vaccination, and taking sick days due to influenza-like illness among US workers. Vaccine 2018, 36, 7316–7323. [Google Scholar] [CrossRef] [PubMed]
- Wong, M.; Wong, E.L.; Cheung, A.W.; Huang, J.; Lai, C.K.C.; Yeoh, E.K.; Chan, P.K.S. COVID-19 vaccine hesitancy in a city with free choice and sufficient doses. Vaccines 2021, 9, 1250. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Wong, E.L.-Y.; Ho, K.-F.; Cheung, A.W.-L.; Yau, P.S.-Y.; Dong, D.; Yeoh, E.K.; Wong, S.Y. Change of willingness to accept COVID-19 vaccine and reasons of vaccine hesitancy of working people at different waves of local epidemic in Hong Kong, China: Repeated cross-sectional surveys. Vaccines 2021, 9, 62. [Google Scholar] [CrossRef] [PubMed]
- Wan, E.Y.F.; Chui, C.S.L.; Lai, F.T.T.; Chan, E.W.Y.; Li, X.; Yan, V.K.C.; Wong, I.C.K.; Gao, L.; Yu, Q.; Lam, I.C.H.; et al. Bell′s palsy following vaccination with mRNA (BNT162b2) and inactivated (CoronaVac) SARS-CoV-2 vaccines: A case series and nested case-control study. Lancet Infect. Dis. 2022, 22, 64–72. [Google Scholar] [CrossRef]
- Siu, J.Y.-M.; Cao, Y.; Shum, D.H. Perceptions of and hesitancy toward COVID-19 vaccination in older Chinese adults in Hong Kong: A qualitative study. BMC Geriatr. 2022, 22, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Wong, C.L.; Leung, A.W.; Chung, O.M.H.; Chien, W.T. Factors influencing COVID-19 vaccination uptake among community members in Hong Kong: A cross-sectional online survey. BMJ Open 2022, 12, e058416. [Google Scholar] [CrossRef] [PubMed]
- Cuadros, D.F.; Miller, F.D.; Awad, S.; Coule, P.; MacKinnon, N.J. Analysis of Vaccination Rates and New COVID-19 Infections by US County, July–August 2021. JAMA Netw. Open 2022, 5, e2147915. [Google Scholar] [CrossRef] [PubMed]
| Category of Measure | p-Value 1 | List of Measures | Date of Announcement | Target Age Group | AWAVR Mean (SD) 2 |
|---|---|---|---|---|---|
| Eligibility | 0.12 | Extended eligibility of BioNTech and Sinovac to those aged 16 or above and 18, respectively [12] | 15 April 2021 | 12–19 | +0.23% (0.35%) |
| Extended eligibility of Sinovac to 12–17 [13] | 15 September 2021 | 12–19 | −1.46% (1.29%) | ||
| Accessibility | <0.0001 | Launched group booking vaccination services [14] | 21 June 2021 | 12–19 | +1.51% (0.99%) |
| Provided outreach vaccination arrangements for Residential care homes [15] | 13 April 2021 | 60 or above | +0.18% (0.63%) | ||
| Launched government’s school outreach service for COVID-19 vaccination [16] | 2 July 2021 | 12–19 | +1.16% (0.59%) | ||
| Distributed in-person same day quota that no need booking for elderly who aged 70 or above [17] | 29 July 2021 | 70 or above | +0.37% (0.39%) | ||
| Incentives | <0.0001 | Provided vaccination leave for government employees who injected first dose on or before 31 August, 2021. Other companies followed suit [16] | 31 May 2021 | 20–69 | +0.68% (0.56%) |
| Launched lucky draw by Sino Group. Over 30 enterprises followed suits [18] | 2 June 2021 | 18 or above | +0.68% (0.56%) | ||
| Announced resume face-to-face whole day classes and school activities when 70% of students are vaccinated [19] | 2 August 2021 | 12–19 | +0.11% (0.79%) | ||
| Restrictions | <0.0001 | Demanded all government and hospital authority staff without vaccination to undergo USD 30 self-paid combined nasal and throat swabs once every two weeks outside their working time [20] | 2 August 2021 | 20–69 | +0.11% (0.79%) |
| Further tightened the testing scheme for those who had not been vaccinated from once in two weeks to once a week [21] | 9 November 2021 | 20–69 | +0.02% (0.10%) | ||
| Further tightened testing schedule from once a week to every three days [22] | 21 December 2021 | 20–69 | +1.21% (2.15%) | ||
| Forbidden entering all venues without the proof of vaccination certificate [23] | 4 January 2022 | All | +1.25% (2.12%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chu, Y.-K.; Chung, P.-H.; Pang, F.-C. Analysis of the Effectiveness of Measures on the COVID-19 Vaccination Rate in Hong Kong. Vaccines 2022, 10, 747. https://doi.org/10.3390/vaccines10050747
Chu Y-K, Chung P-H, Pang F-C. Analysis of the Effectiveness of Measures on the COVID-19 Vaccination Rate in Hong Kong. Vaccines. 2022; 10(5):747. https://doi.org/10.3390/vaccines10050747
Chicago/Turabian StyleChu, Yui-Ki, Pui-Hong Chung, and Fei-Chau Pang. 2022. "Analysis of the Effectiveness of Measures on the COVID-19 Vaccination Rate in Hong Kong" Vaccines 10, no. 5: 747. https://doi.org/10.3390/vaccines10050747
APA StyleChu, Y.-K., Chung, P.-H., & Pang, F.-C. (2022). Analysis of the Effectiveness of Measures on the COVID-19 Vaccination Rate in Hong Kong. Vaccines, 10(5), 747. https://doi.org/10.3390/vaccines10050747






