Vaccine Hesitancy in the Time of COVID-19: Attitudes and Intentions of Teens and Parents Regarding the COVID-19 Vaccine
Abstract
:1. Introduction
2. Methods
3. Results
3.1. COVID-19 Experiences
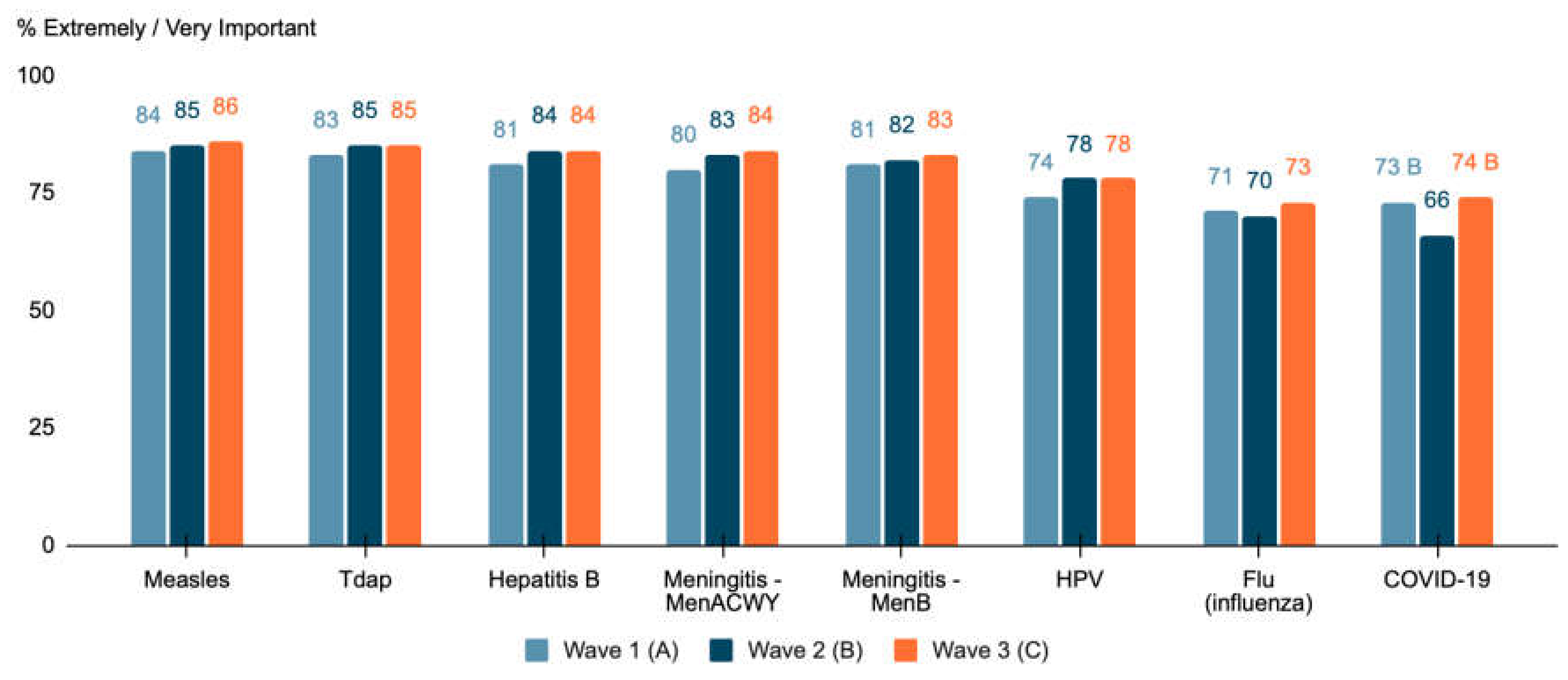
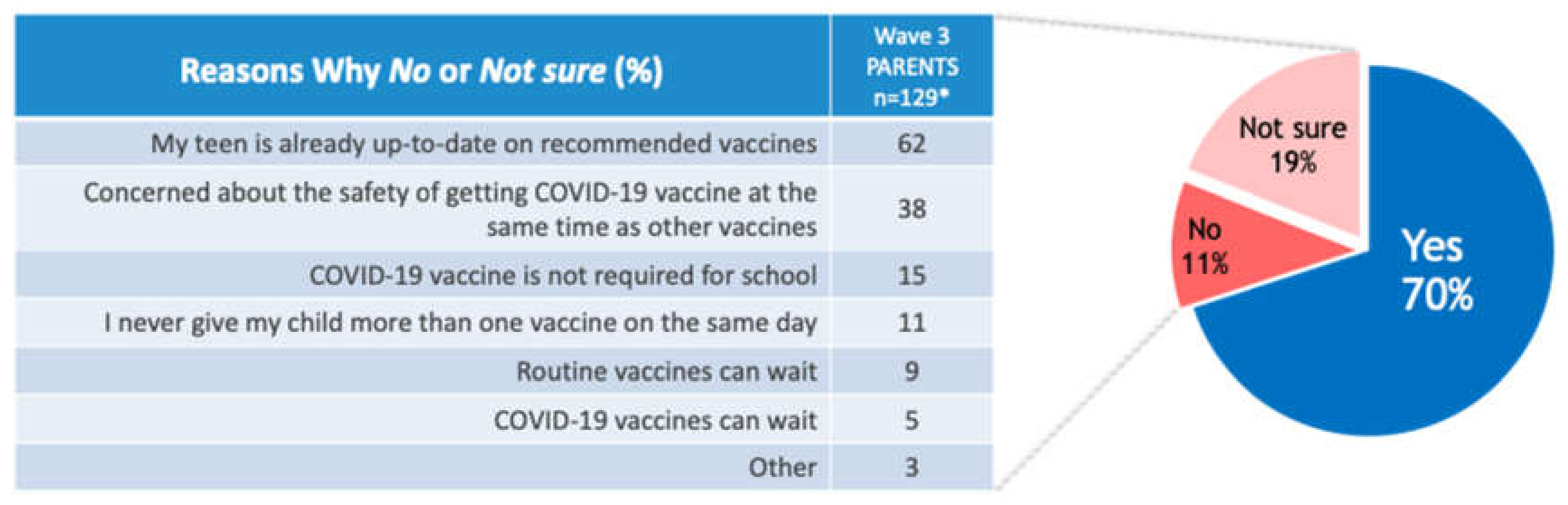
3.2. Routine Immunizations
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hopkins, J.S. How Pfizer Delivered a COVID Vaccine in Record Time: Crazy Deadlines, a Pushy CEO. Available online: https://www.wsj.com/articles/how-pfizer-delivered-a-covid-vaccine-in-record-time-crazy-deadlines-a-pushy-ceo-11607740483 (accessed on 12 December 2020).
- National Institutes of Health (NIH). Experimental Coronavirus Vaccine is Safe and Produces Immune Response. Available online: https://www.nih.gov/news-events/nih-research-matters/experimental-coronavirus-vaccine-safe-produces-immune-response (accessed on 20 July 2020).
- Ten Health Issues WHO Will Tackle This Year. Available online: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019 (accessed on 22 August 2021).
- Larson, H.J.; Jarrett, C.; Eckersberger, E.; Smith, D.M.D.; Paterson, P. Understanding Vaccine Hesitancy around Vaccines and Vaccination from a Global Perspective: A Systematic Review of Published Literature, 2007–2012. Vaccine 2014, 32, 2150–2159. [Google Scholar] [CrossRef]
- Harrison, E.A.; Wu, J.W. Vaccine confidence in the time of COVID-19. Eur. J. Epidemiol. 2020, 35, 325–330. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fisher, K.A.; Bloomstone, S.J.; Walder, J.; Crawford, S.; Fouayzi, H.; Mazor, K.M. Attitudes toward a potential SARS-CoV-2 vaccine: A survey of U.S. adults: A survey of U.S. adults. Ann. Intern. Med. 2020, 173, 964–973. [Google Scholar] [CrossRef] [PubMed]
- Hammer, C.C.; Cristea, V.; Dub, T.; Sivelä, J. High but slightly declining COVID-19 vaccine acceptance and reasons for vaccine acceptance, Finland April to December 2020. Epidemiol. Infect. 2021, 149, 1–19. [Google Scholar] [CrossRef]
- Lang, R.; Benham, J.L.; Atabati, O.; Hollis, A.; Tombe, T.; Shaffer, B.; Burns, K.K.; MacKean, G.; Léveillé, T.; McCormack, B.; et al. Attitudes, behaviours and barriers to public health measures for COVID-19: A survey to inform public health messaging. BMC Public Health 2021, 21, 765. [Google Scholar] [CrossRef] [PubMed]
- Ruiz, J.B.; Bell, R.A. Predictors of intention to vaccinate against COVID-19: Results of a nationwide survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef]
- Cai, H.; Bai, W.; Liu, S.; Liu, H.; Chen, X.; Qi, H.; Liu, R.; Cheung, T.; Su, Z.; Ng, C.H.; et al. Attitudes Toward COVID-19 Vaccines in Chinese Adolescents. Front. Med. 2021, 8, 691079. [Google Scholar] [CrossRef]
- Mant, M.; Aslemand, A.; Prine, A.; Holland, A.J. University students’ perspectives, planned uptake, and hesitancy regarding the COVID-19 vaccine: A multi-methods study. PLoS ONE 2021, 16, e0255447. [Google Scholar] [CrossRef]
- Brandt, E.J.; Rosenberg, J.; Waselewski, M.E.; Amaro, X.; Wasag, J.; Chang, T. National Study of Youth Opinions on Vaccination for COVID-19 in the U.S. J. Adolesc. Health 2021, 68, 869–872. [Google Scholar] [CrossRef] [PubMed]
- Adams, S.H.; Schaub, J.P.; Nagata, J.M.; Park, M.J.; Brindis, C.D.; Irwin, C.E. Young Adult Perspectives on COVID-19 Vaccinations. J. Adolesc. Health 2021, 69, 511–514. [Google Scholar] [CrossRef]
- Montalti, M.; Rallo, F.; Guaraldi, F.; Bartoli, L.; Po, G.; Stillo, M.; Perrone, P.; Squillace, L.; Dallolio, L.; Pandolfi, P.; et al. Would Parents Get Their Children Vaccinated Against SARS-CoV-2? Rate and Predictors of Vaccine Hesitancy According to a Survey over 5000 Families from Bologna, Italy. Vaccines 2021, 9, 366. [Google Scholar] [CrossRef] [PubMed]
- Kelly, B.J.; Southwell, B.G.; McCormack, L.A.; Bann, C.M.; MacDonald, P.D.M.; Frasier, A.M.; Bevc, C.A.; Brewer, N.T.; Squiers, L.B. Predictors of willingness to get a COVID-19 vaccine in the U.S. BMC Infect. Dis. 2021, 21, 338. [Google Scholar] [CrossRef] [PubMed]
- Oliver, S.E. EtR Framework: Pfizer-BioNTech COVID-19 Vaccine in Adolescents Aged 12–15 years. [Meeting Session] Advisory Committee on Immunization Practices Meeting, Centers for Disease Control and Prevention, Atlanta, GA. Available online: https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2021-05-12/04-COVID-Oliver-508.pdf (accessed on 20 December 2021).
- Dooling, K.; McClung, N.; Chamberland, M.; Marin, M.; Wallace, M.; Bell, B.P.; Lee, G.M.; Talbot, H.K.; Romero, J.R.; Oliver, S.E. The Advisory Committee on Immunization Practices’ Interim Recommendation for Allocating Initial Supplies of COVID-19 Vaccine—United States, 2020. MMWR. Morb. Mortal. Wkly. Rep. 2020, 69, 1857–1859. [Google Scholar] [CrossRef] [PubMed]
- Oliver, S.E.; Gargano, J.W.; Marin, M.; Wallace, M.; Curran, K.G.; Chamberland, M.; McClung, N.; Campos-Outcalt, D.; Morgan, R.L.; Mbaeyi, S.; et al. The Advisory Committee on Immunization Practices’ Interim Recommendation for Use of Pfizer-BioNTech COVID-19 Vaccine—United States, December 2020. MMWR. Morb. Mortal. Wkly. Rep. 2020, 69, 1922–1924. [Google Scholar] [CrossRef]
- Wallace, M.; Woodworth, K.R.; Gargano, J.W.; Scobie, H.M.; Blain, A.E.; Moulia, D.; Chamberland, M.; Reisman, N.; Hadler, S.C.; MacNeil, J.R.; et al. The Advisory Committee on Immunization Practices’ Interim Recommendation for Use of Pfizer-BioNTech COVID-19 Vaccine in Adolescents Aged 12–15 Years—United States, May 2021. MMWR. Morb. Mortal. Wkly. Rep. 2021, 70, 749–752. [Google Scholar] [CrossRef]
- Delahoy, M.J.; Ujamaa, D.; Whitaker, M.; O’Halloran, A.; Anglin, O.; Burns, E.; Cummings, C.; Holstein, R.; Kambhampati, A.K.; Milucky, J.; et al. Hospitalizations Associated with COVID-19 Among Children and Adolescents—COVID-NET, 14 States, March 1, 2020–August 14, 2020. MMWR. Morb. Mortal. Wkly. Rep. 2021, 70, 1255–1260. [Google Scholar] [CrossRef]
- Bell, S.; Clarke, R.; Mounier-Jack, S.; Walker, J.L.; Paterson, P. Parents’ and guardians’ views on the acceptability of a future COVID-19 vaccine: A multi-methods study in England. Vaccine 2020, 38, 7789–7798. [Google Scholar] [CrossRef]
- Weitzman, E.R.; Sherman, A.C.; Levy, O. SARS-CoV-2 mRNA Vaccine Attitudes as Expressed in U.S. FDA Public Commentary: Need for a Public-Private Partnership in a Learning Immunization System. Front. Public Health 2021, 9, 695807. [Google Scholar] [CrossRef]
- Kaplan, R.M.; Spittel, M.L.; Zeno, T.L. Educational Attainment and Life Expectancy. Policy Insights Behav. Brain Sci. 2014, 1, 189–194. [Google Scholar] [CrossRef]
- Romer, D.; Jamieson, K.H. Conspiracy theories as barriers to controlling the spread of COVID-19 in the U.S. Soc. Sci. Med. 2020, 263, 113356. [Google Scholar] [CrossRef] [PubMed]
- Stein, R.A.; Ometa, O.; Shetty, S.P.; Katz, A.; Popitiu, M.I.; Brotherton, R. Conspiracy theories in the era of COVID-19: A tale of two pandemics. Int. J. Clin. Pract. 2021, 75, e13778. [Google Scholar] [CrossRef] [PubMed]
- Wilson, S.L.; Wiysonge, C. Social media and vaccine hesitancy. BMJ Glob. Health 2020, 5, e004206. [Google Scholar] [CrossRef] [PubMed]
- Loomba, S.; de Figueiredo, A.; Piatek, S.J.; de Graaf, K.; Larson, H.J. Measuring the impact of COVID-19 vaccine misinformation on vaccination intent in the UK and USA. Nat. Hum. Behav. 2021, 5, 337–348. [Google Scholar] [CrossRef] [PubMed]
- Shih, S.-F.; Wagner, A.L.; Masters, N.B.; Prosser, L.A.; Lu, Y.; Zikmund-Fisher, B.J. Vaccine Hesitancy and Rejection of a Vaccine for the Novel Coronavirus in the United States. Front. Immunol. 2021, 12, 558270. [Google Scholar] [CrossRef]
- Thompson, H.S.; Manning, M.; Mitchell, J.; Kim, S.; Harper, F.W.K.; Cresswell, S.; Johns, K.; Pal, S.; Dowe, B.; Tariq, M.; et al. Factors Associated with Racial/Ethnic Group–Based Medical Mistrust and Perspectives on COVID-19 Vaccine Trial Participation and Vaccine Uptake in the US. JAMA Netw. Open 2021, 4, e2111629. [Google Scholar] [CrossRef] [PubMed]
- Coyne-Beasley, T.; Hill, S.V.; Zimet, G.; Kanbur, N.; Kimberlin, D.; Raymond-Flesch, M.; Simpson, T.; Svetaz, M.V.; Trent, M.; Walker-Harding, L. COVID-19 Vaccination of Adolescents and Young Adults of Color: Viewing Acceptance and Uptake with a Health Equity Lens. J. Adolesc. Health 2021, 68, 844–846. [Google Scholar] [CrossRef] [PubMed]
- Biasio, L.R.; Bonaccorsi, G.; Lorini, C.; Pecorelli, S. Assessing COVID-19 vaccine literacy: A preliminary online survey. Hum. Vaccines Immunother. 2021, 17, 1304–1312. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Coadministration of COVID-19 Vaccines with Other Vaccines. Available online: https://www.cdc.gov/vaccines/covid-19/clinical-considerations/covid-19-vaccines-us.html#Coadministration (accessed on 8 September 2021).
- Rutten, L.J.F.; Zhu, X.; Leppin, A.L.; Ridgeway, J.L.; Swift, M.D.; Griffin, J.M.; Sauver, J.L.S.; Virk, A.; Jacobson, R.M. Evidence-Based Strategies for Clinical Organizations to Address COVID-19 Vaccine Hesitancy. Mayo Clin. Proc. 2021, 96, 699–707. [Google Scholar] [CrossRef]
- O’Leary, S.T.; Middleman, A.B.; Rockwell, P.G. Improving Vaccination Coverage in Children and Adolescents: The Role of Professional Societies. Acad. Pediatr. 2021, 21, S5–S6. [Google Scholar] [CrossRef]
- Unity Consortium. Available online: https://www.unity4teenvax.org/ (accessed on 7 September 2021).
- Olusanya, O.A.; Bednarczyk, R.A.; Davis, R.L.; Shaban-Nejad, A. Addressing Parental Vaccine Hesitancy and Other Barriers to Childhood/Adolescent Vaccination Uptake During the Coronavirus (COVID-19) Pandemic. Front. Immunol. 2021, 12, 663074. [Google Scholar] [CrossRef]
- Opel, D.J.; Heritage, J.; Taylor, J.; Mangione-Smith, R.; Salas, H.S.; DeVere, V.; Zhou, C.; Robinson, J.D. The Architecture of Provider-Parent Vaccine Discussions at Health Supervision Visits. Pediatrics 2013, 132, 1037–1046. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Freeman, D.; Loe, B.S.; Yu, L.-M.; Freeman, J.; Chadwick, A.; Vaccari, C.; Shanyinde, M.; Harris, V.; Waite, F.; Rosebrock, L.; et al. Effects of different types of written vaccination information on COVID-19 vaccine hesitancy in the UK (OCEANS-III): A single-blind, parallel-group, randomised controlled trial. Lancet Public Health 2021, 6, e416–e427. [Google Scholar] [CrossRef]
- Murthy, B.P.; Zell, E.; Saelee, R.; Murthy, N.; Meng, L.; Meador, S.; Reed, K.; Shaw, L.; Gibbs-Scharf, L.; McNaghten, A.; et al. COVID-19 Vaccination Coverage Among Adolescents Aged 12–17 Years—United States, December 14, 2020–July 31, 2021. MMWR. Morb. Mortal. Wkly. Rep. 2021, 70, 1206–1213. [Google Scholar] [CrossRef] [PubMed]
| Parents/Guardians | Teens | |||||
|---|---|---|---|---|---|---|
| Wave 1 | Wave 2 | Wave 3 | Wave 1 | Wave 2 | Wave 3 | |
| TOTAL Weighted | 593 | - | - | 300 | - | - |
| TOTAL Unweighted | 582 | 531 | 500 | 300 | 300 | 300 |
| US Region (U.S. Department of Commerce, Economics and Statistics Administration U.S. Census Bureau) | ||||||
| Northeast | 109 | 77 | 91 | 79 | 53 | 60 |
| 19% | 15% | 18% | 26% | 18% | 20% | |
| Midwest | 125 | 124 | 103 | 53 | 60 | 65 |
| 22% | 23% | 21% | 18% | 20% | 22% | |
| South | 215 | 202 | 193 | 98 | 121 | 94 |
| 37% | 38% | 39% | 33% | 40% | 31% | |
| West | 133 | 128 | 113 | 71 | 66 | 81 |
| 23% | 24% | 23% | 24% | 22% | 27% | |
| Gender | ||||||
| Male | 264 | 176 | 215 | 133 | 165 | 152 |
| 45% | 33% | 43% | 44% | 55% | 51% | |
| Female | 314 | 354 | 285 | 164 | 131 | 144 |
| 54% | 67% | 57% | 55% | 44% | 48% | |
| Non-binary/Other | 0 | 0 | 0 | 2 | 3 | 2 |
| - | - | - | 1% | 1% | 1% | |
| Prefer not to say | 4 | 1 | 0 | 1 | 1 | 2 |
| 1% | * | - | * | * | 1% | |
| Age of Parent/Guardian Participants | ||||||
| Age 25–34 | 34 | 34 | 33 | - | - | - |
| 6% | 6% | 7% | - | - | - | |
| Age 35–44 | 251 | 282 | 223 | - | - | - |
| 43% | 53% | 45% | - | - | - | |
| Age 45–54 | 203 | 160 | 159 | - | - | - |
| 35% | 30% | 32% | - | - | - | |
| Age 55–64 | 88 | 42 | 72 | - | - | - |
| 15% | 8% | 14% | - | - | - | |
| Age 65 or older | 6 | 13 | 13 | - | - | - |
| 1% | 2% | 2% | - | - | - | |
| Mean | 45.8 | 44.1 | 45.5 | - | - | - |
| Age of Teens | Age of the Parent/Guardian Participant’s Teen Child | Age of Teen Participant | ||||
| Age 13 | 114 | 71 | 102 | 74 | 50 | 76 |
| 19% | 13% | 20% | 25% | 17% | 25% | |
| Age 14 | 114 | 113 | 98 | 36 | 64 | 52 |
| 20% | 21% | 20% | 12% | 21% | 17% | |
| Age 15 | 102 | 112 | 92 | 38 | 61 | 60 |
| 17% | 21% | 18% | 13% | 20% | 20% | |
| Age 16 | 113 | 97 | 80 | 59 | 55 | 45 |
| 19% | 18% | 16% | 20% | 18% | 15% | |
| Age 17 | 110 | 113 | 100 | 59 | 62 | 55 |
| 19% | 21% | 20% | 20% | 21% | 18% | |
| Age 18 | 30 | 25 | 28 | 33 | 8 | 12 |
| 5% | 5% | 6% | 11% | 3% | 4% | |
| Mean | 15.1 | 15.3 | 15.0 | 15.3 | 15.1 | 15.0 |
| Median | 15.0 | 15.0 | 15.0 | 16.0 | 15.0 | 15.0 |
| Std Deviation | 1.5 | 1.5 | 1.6 | 1.7 | 1.5 | 1.6 |
| Std Error | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 | 0.1 |
| Race | ||||||
| Black or African American | 77 | 67 | 70 | 39 | 45 | 45 |
| 13% | 13% | 14% | 13% | 15% | 15% | |
| American Indian or Alaska Native | 15 | 2 | 5 | 8 | 2 | 2 |
| 3% | * | 1% | 3% | 1% | 1% | |
| Asian | 15 | 20 | 25 | 8 | 11 | 6 |
| 3% | 4% | 5% | 3% | 4% | 2% | |
| White | 427 | 396 | 359 | 216 | 225 | 232 |
| 73% | 75% | 72% | 72% | 75% | 77% | |
| Native Hawaiian or other Pacific Islander | 4 | 4 | 1 | 8 | 0 | 1 |
| 1% | 1% | * | 3% | - | * | |
| Mixed race | 15 | 19 | 20 | 8 | 8 | 9 |
| 3% | 4% | 3% | 3% | 3% | 3% | |
| Some other race | 15 | 19 | 17 | 8 | 6 | 5 |
| 3% | 4% | 3% | 3% | 2% | 2% | |
| Prefer not to answer | 15 | 4 | 3 | 8 | 3 | 0 |
| 3% | 1% | 1% | 3% | 1% | - | |
| Hispanic Ethnicity | ||||||
| Hispanic | 33 | 90 | 90 | 31 | 54 | 55 |
| 6% | 17% | 18% | 10% | 18% | 18% | |
| Non-Hispanic | 536 | 434 | 407 | 268 | 243 | 245 |
| 92% | 82% | 81% | 90% | 81% | 82% | |
| Prefer not to answer | 13 | 7 | 3 | 1 | 3 | 0 |
| 2% | 1% | 1% | * | 1% | - | |
| Community Type | ||||||
| Urban | 199 | 167 | 207 | 109 | 128 | 145 |
| 34% | 31% | 41% | 36% | 43% | 48% | |
| Suburban | 284 | 242 | 199 | 134 | 120 | 110 |
| 49% | 46% | 40% | 45% | 40% | 37% | |
| Rural | 99 | 122 | 94 | 57 | 52 | 45 |
| 17% | 23% | 19% | 19% | 17% | 15% | |
| Household Income | ||||||
| Less than $50,000 | 138 | 228 | 134 | 95 | 113 | 72 |
| 24% | 43% | 27% | 32% | 38% | 24% | |
| $50,000 to $99,999 | 173 | 155 | 141 | 76 | 85 | 93 |
| 30% | 29% | 28% | 25% | 28% | 31% | |
| $100,000 or more | 247 | 134 | 211 | 107 | 93 | 128 |
| 42% | 25% | 42% | 36% | 31% | 43% | |
| Prefer not to answer | 25 | 14 | 14 | 22 | 9 | 7 |
| 4% | 3% | 3% | 7% | 3% | 2% | |
| Topic | Parents/Guardians | Teens | ||||
|---|---|---|---|---|---|---|
| Wave 1 | Wave 2 | Wave 3 | Wave 1 | Wave 2 | Wave 3 | |
| Column A | Column B | Column C | Column D | Column E | Column F | |
| Percentage choosing strongly agree/somewhat agree | ||||||
| COVID-19 Experience | ||||||
| COVID-19 is a serious disease. | 82 | 83 | 86 | 83 | 82 | 85 |
| It’s possible I will get infected with COVID-19. | 62 | 63 | 60 | 60 | 59 | 57 |
| Routine Vaccines | ||||||
| It is important for all teens to get the vaccines recommended for them. | 80 D | 78 | 77 | 72 | 73 | 74 |
| I have some concerns about the safety of vaccines. | 52 | 61 A | 63 A | 56 | 64 | 62 |
| I have some concerns about the effectiveness of some vaccines. | 54 | 60 A | 67 AB | 55 | 64 | 63 |
| What I have read on social media has concerned me about the safety of some vaccines. | 41 | 49 A | 51A | 50 A | 56 B | 57 |
| If my friends get vaccinated, I think I would need to get vaccinated, too. | - | - | - | 58 | 54 | 63 E |
| Percentage choosing the option from “select all that apply” | ||||||
| COVID-19 Vaccines | ||||||
| Reasons to NOT get the vaccine: | ||||||
| I am concerned about possible side effects. | 41 | 54 A | 62 AB | 40 | 47 | 58 DE |
| I am concerned my teen/I could get COVID-19 from the vaccine. | 20 | 22 | 22 | 23 | 20 | 15 |
| I do not think the COVID-19 vaccine will work well. | 21 | 20 | 18 | 17 | 20 | 22 |
| My teen does not/I do not like getting shots/needles. | 12 B | 8 | 13 B | 20 A | 20B | 21 |
| I think the COVID-19 outbreak is not as serious as some say. | 16 B | 11 | 14 | 12 | 14 | 14 |
| I’m worried I/my parent might have to pay for it. | 11 BC | 7 | 4 | 18 AF | 15 BF | 6 |
| I think teens do not get seriously ill from COVID-19. | 10 | 10 | 17 AB | 11 | 16 B | 19 |
| Reasons TO get the vaccine: | ||||||
| I want to protect my teen/myself. | 51 | 55 | 54 | 53 | 49 | 51 |
| I want to protect everyone in my family. | 51 | 50 | 47 | 47 | 52 | 44 |
| Vaccination is the best way for my teen/me to avoid a potentially serious disease. | 39 | 40 | 43 | 37 | 38 | 38 |
| I want to help protect my community. | 39 | 39 | 36 | 35 | 36 | 34 |
| Life will not go back to normal until most people are vaccinated, including teens. | 38 | 39 | 35 | 37 | 35 | 34 |
| My teen/I would be safe around other people. | 34 | 36 | 41 A | 38 | 39 | 37 |
| A family member is at high risk for COVID-19. | 34 | 36C | 29 | 31 | 35 | 30 |
| Percentage choosing one of the following options | ||||||
| When COVID-19 is approved and available, which statement most closely represents what you will do for you? * | ||||||
| Get vaccinated as soon as possible | 30 | 28 | 8 | - | - | - |
| Get vaccinated when I have time/make it a priority/others have safely been vaccinated | 46 | 29 | 19 | - | - | - |
| Only if required for my job/school | 8 | 4 | 3 | - | - | - |
| I have received at least one dose of vaccine | - | 14 | 56 | |||
| I do NOT plan to get a COVID-19 vaccine | 16 | 24 | 14 | - | - | - |
| When COVID-19 is approved and available, which statement most closely represents what you will do for your teen? * | ||||||
| Get vaccinated as soon as possible | 28 | 29 | 12 ^ | - | - | - |
| Get vaccinated when I have time/make it a priority/others have safely been vaccinated | 50 | 58 | 42 ^ | - | - | - |
| Only if required for my teen’s school | 8 | 10 | 13 ^ | - | - | - |
| I do NOT plan to get a COVID-19 vaccine | 14 | 19 | 33 ^ | - | - | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Middleman, A.B.; Klein, J.; Quinn, J. Vaccine Hesitancy in the Time of COVID-19: Attitudes and Intentions of Teens and Parents Regarding the COVID-19 Vaccine. Vaccines 2022, 10, 4. https://doi.org/10.3390/vaccines10010004
Middleman AB, Klein J, Quinn J. Vaccine Hesitancy in the Time of COVID-19: Attitudes and Intentions of Teens and Parents Regarding the COVID-19 Vaccine. Vaccines. 2022; 10(1):4. https://doi.org/10.3390/vaccines10010004
Chicago/Turabian StyleMiddleman, Amy B., Judy Klein, and Jane Quinn. 2022. "Vaccine Hesitancy in the Time of COVID-19: Attitudes and Intentions of Teens and Parents Regarding the COVID-19 Vaccine" Vaccines 10, no. 1: 4. https://doi.org/10.3390/vaccines10010004
APA StyleMiddleman, A. B., Klein, J., & Quinn, J. (2022). Vaccine Hesitancy in the Time of COVID-19: Attitudes and Intentions of Teens and Parents Regarding the COVID-19 Vaccine. Vaccines, 10(1), 4. https://doi.org/10.3390/vaccines10010004






