Beetroot, A Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies
Abstract
1. Introduction
2. Beetroot (Beta vulgaris L.) Formulations
3. Nutritional Composition of Beetroot Formulations
4. Bioactive Compounds in Beetroot Product Interventions
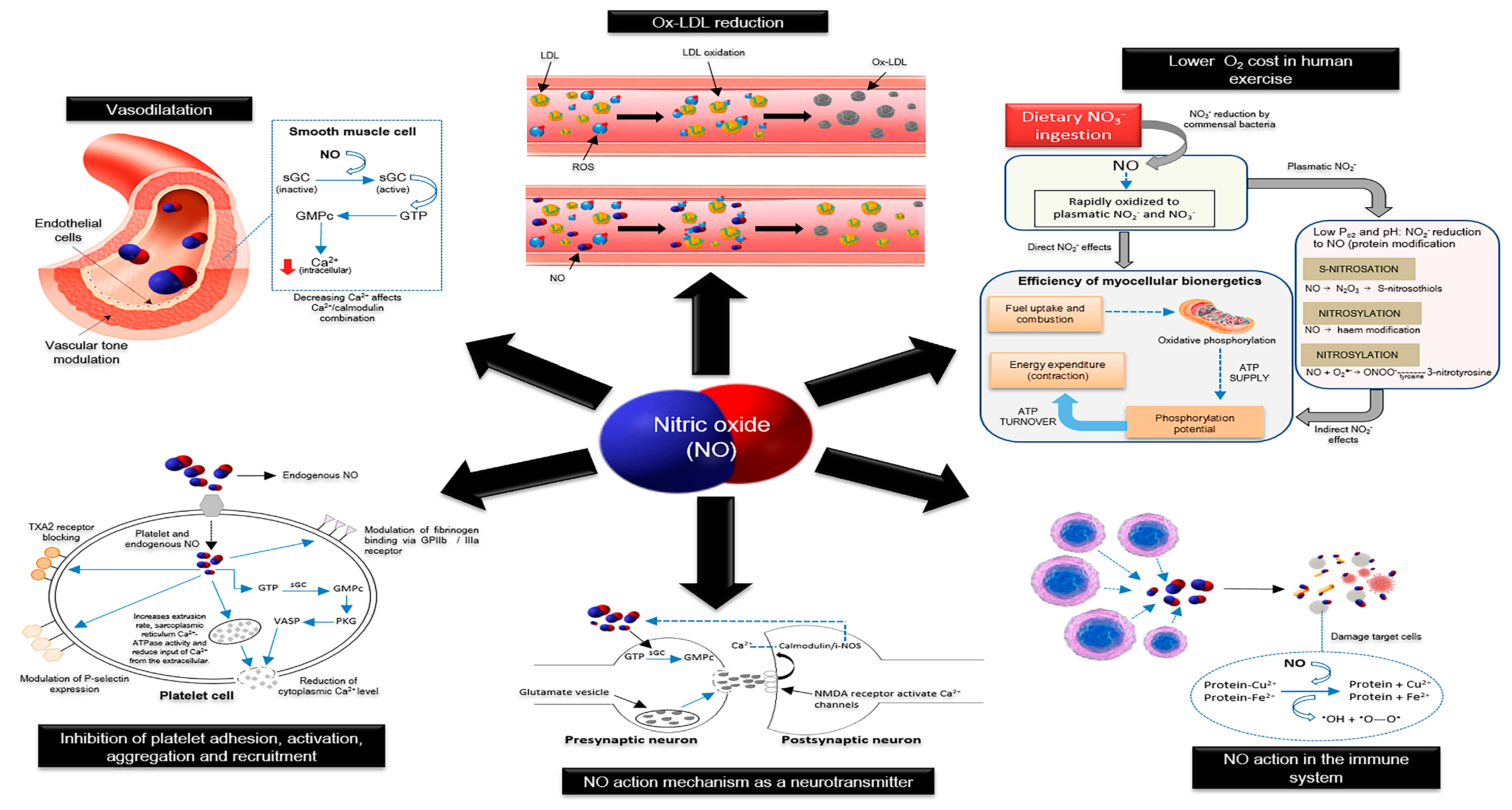
4.1. NO3− and NO2−
4.2. Saponins
4.3. Organic Acids (OAs)
4.4. Phenolic Compounds (PCs)
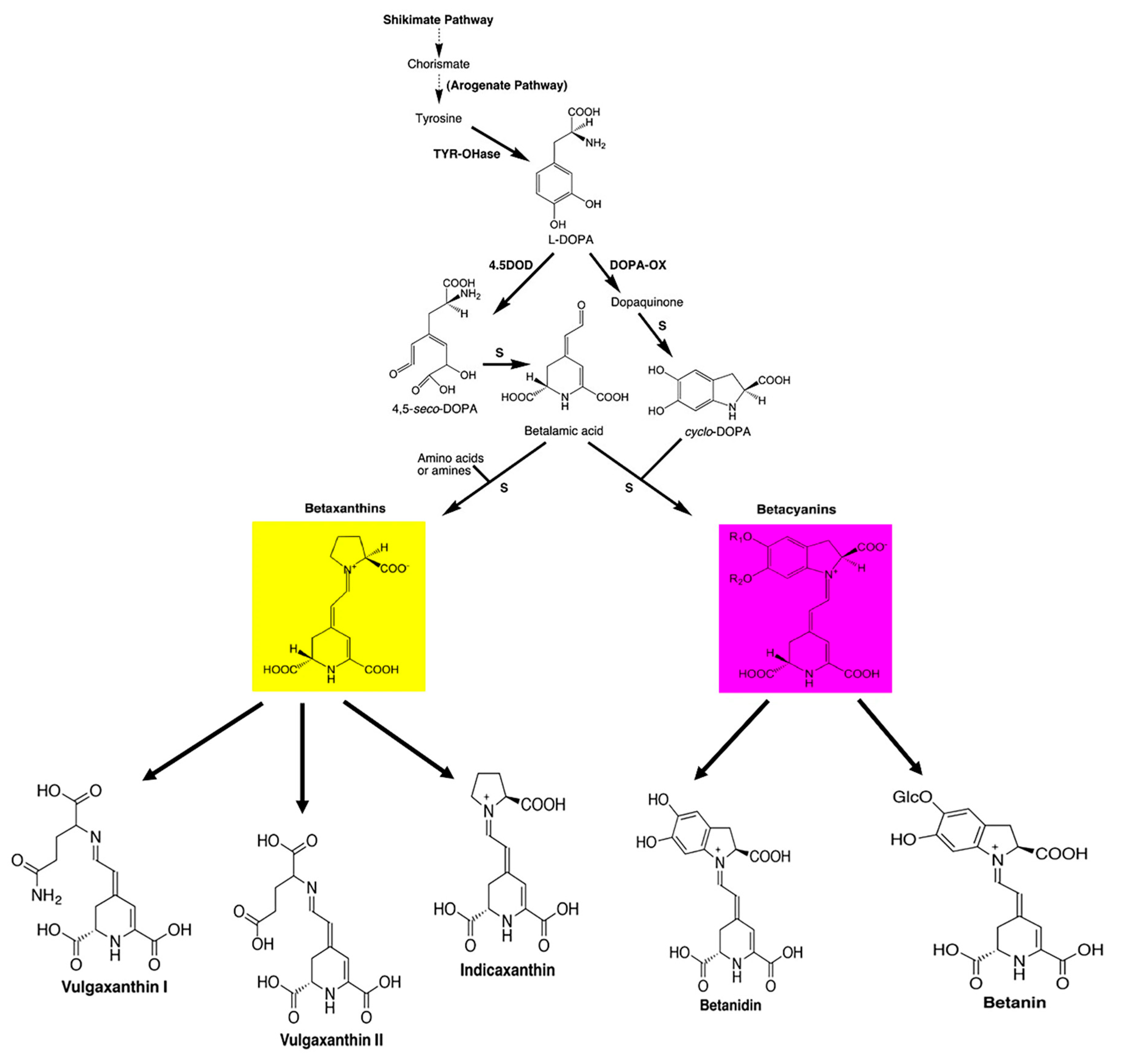
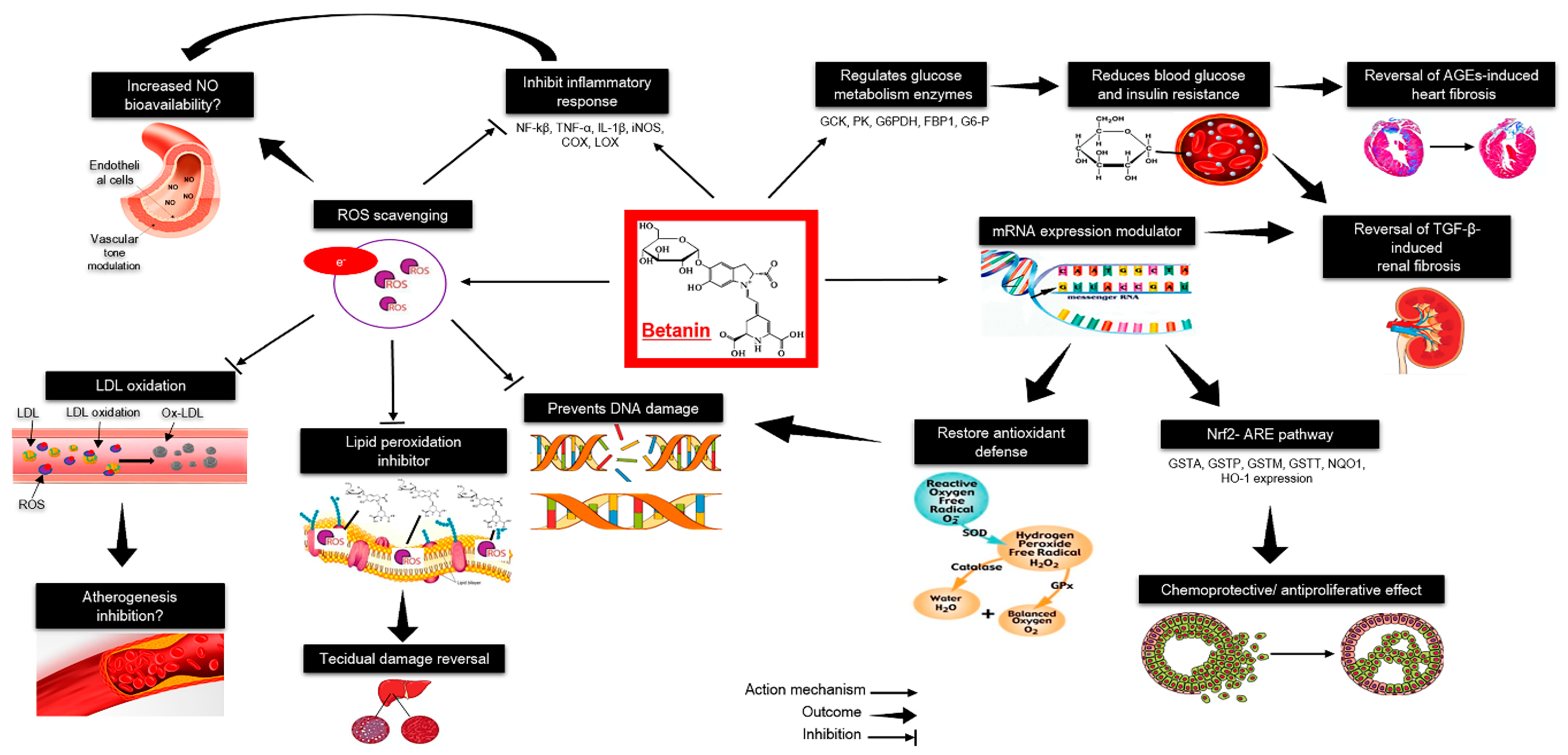
4.5. Betalains
5. Beetroot Product Interventions Increase Nitric Oxide Production and Promote Health Benefits
6. Bioactive Beetroot Compounds—NO3− and Betanin—Modulate the Transcription of Genes Responsible for Regulating Redox Imbalance in a Rodent Model
7. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Baião, D.S.; Silva, F.O.; d’El-Rei, J.; Neves, M.F.; Perrone, D.; Del Aguila, E.M.; Paschoalin, V.M.F. A new functional beetroot formulation enhances adherence to nitrate supplementation and health outcomes in clinical practice. SDRP J. Food Sci. Technol. 2018, 3, 484–498. [Google Scholar] [CrossRef]
- World Health Organization/Food and Agriculture Organization. Diet, Nutrition and the Prevalence of Chronic Diseases; Technical Report Series 916; WHO/FAO Expert Consultation: Geneva, Switzerland, 2003; Available online: https://apps.who.int/iris/bitstream/handle/10665/42665/WHO_TRS_916.pdf;jsessionid=BEF89E3C1909472E84B2426ED26F0694?sequence=1 (accessed on 20 March 2020).
- Baião, D.S.; da Silva, D.V.T.; Del Aguila, E.M.; Paschoalin, V.M.F. Nutritional, bioactive and physicochemical characteristics of different beetroot formulations. In Food Additives; Karunaratne, D.N., Pamunuwa, G., Eds.; Intech Open: London, UK, 2017; Chapter 2; pp. 21–44. [Google Scholar] [CrossRef]
- Babateen, A.M.; Fornelli, G.; Donini, L.M.; Mathers, J.C.; Siervo, M. Assessment of dietary nitrate intake in humans: A systematic review. Am. J. Clin. Nutr. 2018, 108, 878–888. [Google Scholar] [CrossRef] [PubMed]
- Lidder, S.; Webb, A.J. Vascular effects of dietary nitrate (as found in green leafy vegetables and beetroot) via the nitrate-nitrite-nitric oxide pathway. Br. J. Clin. Pharm. 2013, 75, 677–696. [Google Scholar] [CrossRef] [PubMed]
- Blekkenhorst, L.C.; Bondonno, N.P.; Liu, A.H.; Ward, N.C.; Prince, R.L.; Lewis, J.R.; Devine, A.; Croft, K.D.; Hodgson, J.M.; Bondonno, C.P. Nitrate, the oral microbiome, and cardiovascular health: A systematic literature review of human and animal studies. Am. J. Clin. Nutr. 2018, 107, 504–522. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Moustaid-Moussa, N.; Chen, L.; Mo, H.; Shastri, A.; Su, R. Novel insights of dietary polyphenols and obesity. J. Nutr. Biochem. 2014, 25, 1–18. [Google Scholar] [CrossRef]
- Grosso, G.; Micek, A.; Godos, J.; Pajak, A.; Sciacca, S.; Galvano, F.; Giovannucci, E.L. Dietary flavonoid and lignan intake and mortality in prospective cohort studies: Systematic deview and dose-response meta-analysis. Am. J. Epidemiol. 2017, 185, 1304–1316. [Google Scholar] [CrossRef]
- Menezes, R.; Rodriguez-Mateos, A.; Kaltsatou, A.; González-Sarrías, A.; Greyling, A.; Giannaki, C.; Andres-Lacueva, C.; Milenkovic, D.; Gibney, E.R.; Dumont, J.; et al. Impact of flavonols on cardiometabolic biomarkers: A meta-analysis of randomized controlled human trials to explore the role of inter-individual variability. Nutrients 2017, 9, 117. [Google Scholar] [CrossRef]
- Nowacka, M.; Tappi, S.; Wiktor, A.; Rybak, K.; Miszczykowska, A.; Czyzewski, J.; Drozdzal, K.; Witrowa-Rajchert, D.; Tylewicz, U. The Impact of pulsed electric field on the extraction of bioactive compounds from beetroot. Foods 2019, 8, 244. [Google Scholar] [CrossRef]
- Baião, D.S.; Conte-Junior, C.A.; Paschoalin, V.M.F.; Alvares, T.S. Beetroot juice increase nitric oxide metabolites in both men and women regardless of body mass. Int. J. Food Sci. Nutr. 2016, 67, 40–46. [Google Scholar] [CrossRef]
- Da Silva, D.V.; Silva, F.O.; Perrone, D.; Pierucci, A.P.T.R.; Conte-Junior, C.A.; Alvares, T.S.; Del Aguila, E.M.; Paschoalin, V.M.F. Physicochemical, nutritional, and sensory analyses of a nitrate-enriched beetroot gel and its effects on plasmatic nitric oxide and blood pressure. Food Nutr. Res. 2016, 60, 1–9. [Google Scholar] [CrossRef]
- Tullio, J.A.; Otto, R.F.; Boer, A.; Ohse, S. Cultivo de beterraba em ambientes protegidos e natura na época de verão. Rev. Bras. Eng. Agríc. Ambient. 2013, 17, 1074–1079. [Google Scholar] [CrossRef]
- Sediyama, M.A.N.; Santos, M.R.; Vidigal, S.M.; Salgado, L.T. Produtividade e exportação de nutritentes em beterraba cultivada com cobertura morta e adubação orgânica. Rev. Bras. Eng. Agríc. Ambient. 2011, 15, 883–889. [Google Scholar] [CrossRef]
- Ravichandran, K.; Saw, N.M.M.T.; Mohdaly, A.A.A.; Gabr, A.M.M.; Kastell, A.; Riedel, H.; Cai, Z.; Knorr, D.; Smetanska, I. Impact of processing of red beet on betalain content and antioxidant activity. Food Res. Int. 2013, 50, 670–675. [Google Scholar] [CrossRef]
- Bian, Z.; Wang, Y.; Zhang, X.; Li, T.; Grundy, S.; Yang, Q.; Cheng, R. A review of environment effects on nitrate accumulation in leafy vegetables grown in controlled environments. Foods 2020, 9, 732. [Google Scholar] [CrossRef] [PubMed]
- Ciurzyńska, A.; Lenart, A. Freeze-drying—Application in food processing and biotechnology—A review. Pol. J. Food. Nutr. Sci. 2011, 61, 165–171. [Google Scholar] [CrossRef]
- Vasconcellos, J.; Conte-Junior, C.; Silva, D.; Pierucci, A.P.; Paschoalin, V.M.F.; Alvares, T.S. Comparison of total antioxidant potential, and total phenolic, nitrate, sugar, and organic acid contents in beetroot juice, chips, powder, and cooked beetroot. Food Sci. Biotechnol. 2016, 25, 79–84. [Google Scholar] [CrossRef] [PubMed]
- Vasconcellos, J.; Silvestre, D.H.; Baião, D.S.; Werneck-de-Castro, J.P.; Alvares, T.S.; Paschoalin, V.M.F. A single dose of beetroot gel rich in nitrate does not improve performance but lowers blood glucose in physically active individuals. J. Nutr. Metab. 2017, 2017, 7853034. [Google Scholar] [CrossRef] [PubMed]
- Czyżewska, A.; Klewicka, E.; Libudzisz, Z. The influence of lactic acid fermentation process of red beet juice on the stability of biologically colorants. Eur. Food Res. Technol. 2006, 223, 110–116. [Google Scholar] [CrossRef]
- Hobbs, D.A.; Kaffa, N.; George, T.W.; Methven, L.; Lovegrove, J.A. Blood pressure-lowering effects of beetroot juice and novel beetroot-enriched bread products in normotensive male subjects. Br. J. Nutr. 2012, 108, 2066–2074. [Google Scholar] [CrossRef] [PubMed]
- Klewicka, E.; Motyl, I.; Libudzisz, Z. Fermentation of beet juice by bacteria of genus Lactobacillus sp. Eur. Food Res. Technol. 2004, 218, 178–183. [Google Scholar] [CrossRef]
- Sawicki, T.; Wiczkowski, W. The effects of boiling and fermentation on betalain profiles and antioxidant capacities of red beetroot products. Food Chem. 2018, 259, 292–303. [Google Scholar] [CrossRef] [PubMed]
- Sawicki, T.; Topolska, J.; Romaszko, E.; Wiczkowski, W. Profile and content of betalains in plasma and urine of volunteers after long-term exposure to fermented red beet juice. J. Agric. Food Chem. 2018, 66, 4155–4163. [Google Scholar] [CrossRef] [PubMed]
- Hobbs, D.A.; Goulding, M.G.; Nguyen, A.; Malaver, T.; Walker, C.F.; George, T.W.; Methven, L.; Lovegrove, J.A. Acute ingestion of beetroot bread increases endothelium-independent vasodilation and lowers diastolic blood pressure in healthy men: A randomized controlled trial. J. Nutr. 2013, 143, 1399–1405. [Google Scholar] [CrossRef] [PubMed]
- Hobbs, D.A.; George, T.W.; Lovegrove, J.A. Differential effect of beetroot bread on postprandial DBP according to Glu298Asp polymorphism in the eNOS gene: A pilot study. J. Hum. Hypertens. 2014, 28, 726–730. [Google Scholar] [CrossRef] [PubMed]
- Wiczkowski, W.; Romaszko, E.; Szawara-Nowak, D.; Piskula, M.K. The impact of the matrix of red beet products and interindividual variability on betacyanins bioavailability in humans. Food Res. Int. 2018, 108, 530–538. [Google Scholar] [CrossRef]
- Sun-Waterhouse, D.; Teoh, A.; Massarotto, C.; Wibisono, R.; Wadhwa, S. Comparative analysis of fruit-based functional snack bars. Food Chem. 2010, 119, 1369–1379. [Google Scholar] [CrossRef]
- Brazillian National Health Surveillance Agency. Technical Regulation on Complementary Nutrition Information; Resolution RDC n. 54; Ministry of Health: Brasília, Brazil, 2012. Available online: http://bvsms.saude.gov.br/bvs/saudelegis/anvisa/2012/rdc0054_12_11_2012.html (accessed on 13 May 2020).
- Miller, M.G.; Thangthaeng, N.; Poulose, S.M.; Shukitt-Hale, B. Role of fruits, nuts, and vegetables in maintaining cognitive health. Exp. Gerontol. 2017, 94, 24–28. [Google Scholar] [CrossRef]
- Baião, D.S.; Freitas, C.S.; Gomes, L.P.; da Silva, D.; Correa, A.C.N.T.F.; Pereira, P.R.; Del Aguila, E.M.; Paschoalin, V.M.F. Polyphenols from root, tubercles and grains cropped in Brazil: Chemical and nutritional characterization and their effects on human health and diseases. Nutrients 2017, 9, 1044. [Google Scholar] [CrossRef]
- Pawlak-Chaouch, M.; Boissière, J.; Gamelin, F.X.; Cuvelier, G.; Berthoin, S.; Aucouturier, J. Effect of dietary nitrate supplementation on metabolic rate during rest and exercise in human: A systematic review and a meta-analysis. Nitric Oxide 2016, 53, 65–76. [Google Scholar] [CrossRef]
- Kapil, V.; Khambata, R.S.; Robertson, A.; Caulfield, M.J.; Ahluwalia, A. Dietary nitrate provides sustained blood pressure lowering in hypertensive patients: A randomized, phase 2, double-blind, placebo-controlled study. Hypertension 2015, 65, 320–327. [Google Scholar] [CrossRef]
- Gu, L.; Tao, G.; Gu, W.; Prior, R.L. Determination of soyasaponins in soy with LC-MS following structural unification by partial alkaline degradation. J. Agric. Food Chem. 2002, 50, 6951–6959. [Google Scholar] [CrossRef] [PubMed]
- Yoshikawa, M.; Murakami, T.; Kadoya, M.; Matsuda, H.; Muraoka, O.; Yamahara, J.; Murakami, N. Medicinal foodstuff. III. Sugar beet. (1): Hypoglycemic oleanolic acid oligoglycosides, betavulgarosides I, II, III, and IV, from the root of Beta vulgaris L. (Chenopodiaceae). Chem. Pharm. Bull. 1996, 44, 1212–1217. [Google Scholar] [CrossRef] [PubMed]
- López-Bucio, J.; Nieto-Jacobo, M.F.; Ramírez-Rodríguez, V.; Herrera-Estrella, L. Organic acid metabolism in plants: From adaptive physiology to transgenic varieties for cultivation in extreme soils. Plant. Sci. 2000, 160, 1–13. [Google Scholar] [CrossRef]
- Leite, A.M.O.; Leite, D.C.A.; Del Aguila, E.M.; Alvares, T.S.; Peixoto, R.S.; Miguel, M.A.L.; Silva, J.T.; Paschoalin, V.M.F. Microbiological and chemical characteristics of Brazilian kefir during fermentation and storage processes. J. Dairy Sci. 2013, 96, 4149–4159. [Google Scholar] [CrossRef] [PubMed]
- Demigné, C.; Sabboh, H.; Puel, C.; Rémésy, C.; Coxam, V. Organic anions and potassium salts in nutrition and metabolism. Nutr. Res. Ver. 2004, 17, 249–258. [Google Scholar] [CrossRef] [PubMed]
- Kazimierczak, R.; Hallmann, E.; Lipowski, J.; Drela, N.; Kowalik, A.; Püssa, T.; Matt, D.; Luik, A.; Gozdowski, D.; Rembiałkowska, E. Beetroot (Beta vulgaris L.) and naturally fermented beetroot juices from organic and conventional production: Metabolomics, antioxidant levels and anticancer activity. J. Sci. Food Agric. 2014, 94, 2618–2629. [Google Scholar] [CrossRef]
- Petsiou, E.I.; Mitrou, P.I.; Raptis, S.A.; Dimitriadis, G.D. Effect and mechanisms of action of vinegar on glucose metabolism, lipid profile, and body weight. Nutr. Rev. 2014, 72, 651–661. [Google Scholar] [CrossRef] [PubMed]
- Moe, O. Kidney stones: Pathophysiology and medical management. Lancet 2006, 367, 333–344. [Google Scholar] [CrossRef]
- Penniston, K.L.; Nakada, S.Y.; Holmes, R.P.; Assimos, D.G. Quantitative assessment of citric acid in lemon juice, lime juice, and commercially-available fruit juice products. J. Endourol. 2008, 22, 567–570. [Google Scholar] [CrossRef]
- Eisner, B.H.; Asplin, J.R.; Goldfarb, D.S.; Ahmad, A.; Stoller, M.L. Citrate, malate and alkali content in commonly consumed diet sodas: Implications for nephrolithiasis treatment. J. Urol. 2010, 183, 2419–2423. [Google Scholar] [CrossRef]
- Kang, D.; Haleblian, G.E.; Sur, R.L. Long-term lemonade based dietary manipulation in patients with hypocitraturic nephrolithiasis. J. Urol. 2007, 177, 1358–1362. [Google Scholar] [CrossRef] [PubMed]
- Silva, B.M.; Andrade, P.B.; Valentão, P.; Ferreres, F.; Seabra, R.M.; Ferreira, M.A. Quince (Cydonia oblonga Miller) fruit (pulp, peel, and seed) and Jam: Antioxidant activity. J. Agric. Food Chem. 2004, 52, 4705–4712. [Google Scholar] [CrossRef] [PubMed]
- Madhavi, D.L.; Singhal, R.S.; Kulkarni, P.R. Technological aspects of food antioxidants. In Food Antioxidantss Technological, Toxicological and Health Perspectives; Madhavi, D.L., Desphpande, S.S., Salunku, D.K., Eds.; Marcel Dekker: New York, NY, USA, 1996; pp. 19–224. [Google Scholar]
- Zuckerman, J.M.; Assimos, D.G. Hypocitraturia: Pathophysiology and medical management. Rev. Urol. 2009, 11, 134–144. [Google Scholar] [CrossRef] [PubMed]
- United States Department of Agriculture. Nutrient data laboratory (NDL); USDA National Food and Nutrient Analysis Program Wave 6b; Agricultural Research Service (ARS): Beltsville, MD, USA, 2002. Available online: https://www.nal.usda.gov/fnic/usda-nutrient-data-laboratory (accessed on 12 April 2020).
- Carr, A.C.; Maggini, S. Vitamin C and immune function. Nutrients 2017, 9, 1211. [Google Scholar] [CrossRef] [PubMed]
- Young, J.I.; Zuchner, S.; Wang, G. Regulation of the epigenome by vitamin C. Annu. Rev. Nutr. 2015, 35, 545–564. [Google Scholar] [CrossRef] [PubMed]
- Lodish, H.; Berk, A.; Zipursky, S.L.; Matsudaira, P.; Baltimore, D.; Darnell, J. (Eds.) Section 22.3 Collagen: The fibrous proteins of the matrix. In Molecular Cell Biology, 4th ed.; W. H. Freeman: New York, NY, USA, 2000. Available online: https://www.ncbi.nlm.nih.gov/books/NBK21582/ (accessed on 8 October 2020).
- Shoulders, M.D.; Raines, R.T. Collagen structure and stability. Annu. Rev. Biochem. 2009, 78, 929–958. [Google Scholar] [CrossRef]
- Ivanov, V.; Ivanova, S.; Kalinovsky, T.; Niedzwiecki, A.; Rath, M. Inhibition of collagen synthesis by select calcium and sodium channel blockers can be mitigated by ascorbic acid and ascorbyl palmitate. Am. J. Cardiovasc. Dis. 2016, 6, 26–35. [Google Scholar]
- Pullar, J.M.; Carr, A.C.; Vissers, M.C.M. The roles of vitamin C in skin health. Nutrients 2017, 9, 866. [Google Scholar] [CrossRef]
- Murad, S.; Grove, D.; Lindberg, K.A.; Reynolds, G.; Sivarajah, A.; Pinnell, S.R. Regulation of collagen synthesis by ascorbic acid. Proc. Natl. Acad. Sci. USA 1981, 78, 2879–2882. [Google Scholar] [CrossRef]
- Takahashi, Y.; Takahashi, S.; Shiga, Y.; Yoshimi, T.; Miura, T. Hypoxic induction of prolyl 4-hydroxylase alpha (I) in cultured cells. J. Biol. Chem. 2000, 275, 14139–14146. [Google Scholar] [CrossRef]
- Michels, A.J.; Frei, B. Myths, artifacts, and fatal flaws: Identifying limitations and opportunities in vitamin C research. Nutrients 2013, 5, 5161–5192. [Google Scholar] [CrossRef] [PubMed]
- Duarte, T.L.; Cooke, M.S.; Jones, G.D. Gene expression profiling reveals new protective roles for vitamin C in human skin cells. Free Radic. Biol. Med. 2009, 46, 78–87. [Google Scholar] [CrossRef] [PubMed]
- Nusgens, B.V.; Humbert, P.; Rougier, A.; Colige, A.C.; Haftek, M.; Lambert, C.A.; Richard, A.; Creidi, P.; Lapiere, C.M. Topically applied vitamin C enhances the mRNA level of collagens I and III, their processing enzymes and tissue inhibitor of matrix metalloproteinase 1 in the human dermis. J. Investig. Derm. 2001, 116, 853–859. [Google Scholar] [CrossRef] [PubMed]
- Pooyandjoo, M.; Nouhi, M.; Shab-Bidar, S.; Djafarian, K.; Olyaeemanesh, A. The effect of (L-) carnitine on weight loss in adults: A systematic review and meta-analysis of randomized controlled trials. Obes. Rev. 2016, 17, 970–976. [Google Scholar] [CrossRef] [PubMed]
- Montes Diaz, G.; Hupperts, R.; Fraussen, J.; Somers, V. Dimethyl fumarate treatment in multiple sclerosis: Recent advances in clinical and immunological studies. Autoimmun. Rev. 2018, 7, 1240–1250. [Google Scholar] [CrossRef] [PubMed]
- Linker, R.A.; Lee, D.H.; Ryan, S.; van Dam, A.M.; Conrad, R.; Bista, P.; Zeng, W.; Hronowsky, X.; Buko, A.; Chollate, S.; et al. Fumaric acid esters exert neuroprotective effects in neuroinflammation via activation of the Nrf2 antioxidant pathway. Brain 2011, 134, 678–692. [Google Scholar] [CrossRef] [PubMed]
- Scannevin, R.H.; Chollate, S.; Jung, M.Y.; Shackett, M.; Patel, H.; Bista, P.; Zeng, W.; Ryan, S.; Yamamoto, M.; Lukashev, M.; et al. Fumarates promote cytoprotection of central nervous system cells against oxidative stress via the nuclear factor (erythroid-derived 2)-like 2 pathway. J. Pharm. Exp. 2012, 341, 274–284. [Google Scholar] [CrossRef] [PubMed]
- Campolo, M.; Casili, G.; Biundo, F.; Crupi, R.; Cordaro, M.; Cuzzocrea, S.; Esposito, E. The neuroprotective effect of dimethyl fumarate in an MPTP-mouse model of Parkinson’s disease: Involvement of reactive oxygen species/nuclear factor-κB/nuclear transcription factor related to NF-E2. Antioxid. Redox Signal. 2017, 27, 453–471. [Google Scholar] [CrossRef]
- Tavallai, M.; Booth, L.; Roberts, J.L.; McGuire, W.P.; Poklepovic, A.; Dent, P. Ruxolitinib synergizes with DMF to kill viaBIM + BAD-induced mitochondrial dysfunction and via reduced SOD2/TRX expression and ROS. Oncotarget 2016, 7, 17290–17300. [Google Scholar] [CrossRef]
- Saidu, N.E.B.; Kavian, N.; Leroy, K.; Jacob, C.; Nicco, C.; Batteux, F.; Alexandre, J. Dimethyl fumarate, a two-edged drug: Current status and future directions. Med. Res. Rev. 2019, 39, 1923–1952. [Google Scholar] [CrossRef]
- Tretter, L.; Patocs, A.; Chinopoulos, C. Succinate, an intermediate in metabolism, signal transduction, ROS, hypoxia, and tumorigenesis. Biochim. Biophys. Acta. 2016, 1857, 1086–1101. [Google Scholar] [CrossRef] [PubMed]
- Fujiwara, T.; Harigae, H. Biology of heme in mammalian erythroid cells and related disorders. Biomed. Res. Int. 2015, 2015, 278536. [Google Scholar] [CrossRef] [PubMed]
- Mills, E.; O’Neill, L.A.J. Succinate: A metabolic signal in inflammation. Trends Cell Biol. 2014, 24, 313–320. [Google Scholar] [CrossRef] [PubMed]
- Lukyanova, L.D.; Kirova, Y.I.; Germanova, E.L. The Role of succinate in regulation of immediate HIF-1α expression in hypoxia. Bull. Exp. Biol. Med. 2018, 164, 298–303. [Google Scholar] [CrossRef]
- He, W.; Miao, F.J.; Lin, D.C.; Schwandner, R.T.; Wang, Z.; Gao, J.; Chen, J.L.; Tian, H.; Ling, L. Citric acid cycle intermediates as ligands for orphan G-protein-coupled receptors. Nature 2004, 429, 188–193. [Google Scholar] [CrossRef]
- Toma, I.; Kang, J.J.; Sipos, A.; Vargas, S.; Bansal, E.; Hanner, F.; Meer, E.; Peti-Peterdi, J. Succinate receptor GPR91 provides a direct link between high glucose levels and renin release in murine and rabbit kidney. J. Clin. Investig. 2008, 118, 2526–2534. [Google Scholar] [CrossRef]
- Guarás, A.; Perales-Clemente, E.; Calvo, E.; Acín-Pérez, R.; Loureiro-Lopez, M.; Pujol, C.; Martínez-Carrascoso, I.; Nuñez, E.; García-Marqués, F.; Rodríguez-Hernández, M.A.; et al. The CoQH2/CoQ ratio serves as a sensor of respiratory chain efficiency. Cell Rep. 2016, 15, 197–209. [Google Scholar] [CrossRef]
- Tretter, L.; Szabados, G.; Ando, A.; Horvath, I. Effect of succinate on mitochondrial lipid peroxidation. The protective effect of succinate against functional and structural changes induced by lipid peroxidation. J. Bioenerg. Biomembr. 1987, 19, 31–44. [Google Scholar] [CrossRef]
- Bindoli, A.; Cavallini, L.; Jocelyn, P. Mitochondrial lipid peroxidation by cumene hydroperoxide and its prevention by succinate. Biochim. Biophys. Acta 1982, 681, 496–503. [Google Scholar] [CrossRef]
- Ganesan, K.; Xu, B. A critical review on polyphenols and health benefits of black soybeans. Nutrients 2017, 9, 455. [Google Scholar] [CrossRef]
- Jelena, C.H.; Giorgio, R.; Justyna, G.; Neda, M.D.; Natasa, S.; Artur, B.; Giuseppe, G. Beneficial effects of polyphenols on chronic diseases and ageing. Polyphen. Prop. Recovery Appl. 2018, 69–102. [Google Scholar] [CrossRef]
- Rossi, L.; Mazzitelli, S.; Arciello, M.; Capo, C.R.; Rotilio, G. Benefits from dietary polyphenols for brain aging and Alzheimer’s disease. Neurochem. Res. 2008, 33, 2390–2400. [Google Scholar] [CrossRef]
- Noguchi-Shinohara, M.; Yuki, S.; Dohmoto, C.; Ikeda, Y.; Samuraki, M.; Iwasa, K.; Yokogawa, M.; Asai, K.; Komai, K.; Nakamura, H.; et al. Consumption of green tea, but not black tea or coffee, is associated with reduced risk of cognitive decline. PLoS ONE 2014, 9, e96013. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Zheng, J.; Li, Y.; Xu, D.P.; Li, S.; Chen, Y.M.; Li, H.B. Natural polyphenols for prevention and treatment of cancer. Nutrients 2016, 8, 515. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.S.; Landau, J.M.; Huang, M.T.; Newmark, H.L. Inhibition of carcinogenesis by dietary polyphenolic compounds. Annu. Rev. Nutr. 2001, 21, 381–406. [Google Scholar] [CrossRef] [PubMed]
- Xiao, J.B.; Hogger, P. Dietary polyphenols and type 2 diabetes: Current insights and future perspectives. Curr. Med. Chem. 2015, 22, 23–38. [Google Scholar] [CrossRef]
- Jakobek, L. Interactions of polyphenols with carbohydrates, lipids and proteins. Food Chem. 2015, 175, 556–567. [Google Scholar] [CrossRef]
- Wang, X.; Ouyang, Y.Y.; Liu, J.; Zhao, G. Flavonoid intake and risk of CVD: A systematic review and meta-analysis of prospective cohort studies. Br. J. Nutr. 2014, 111, 1–11. [Google Scholar] [CrossRef]
- Proserpio, C.; Fia, G.; Bucalossi, G.; Zanoni, B.; Spinelli, S.; Dinnella, C.; Monteleone, E.; Pagliarini, E. Winemaking byproducts as source of antioxidant components: Consumers’ acceptance and expectations of phenol-enriched plant-based food. Antioxidants 2020, 9, 661. [Google Scholar] [CrossRef]
- Brimson, J.M.; Onlamoon, N.; Tencomnao, T.; Thitilertdecha, P. Clerodendrum petasites S. Moore: The therapeutic potential of phytochemicals, hispidulin, vanillic acid, verbascoside, and apigenin. Biomed. Pharm. 2019, 118, 109319. [Google Scholar] [CrossRef]
- Pei, K.; Ou, J.; Huang, J.; Ou, S. p-Coumaric acid and its conjugates: Dietary sources, pharmacokinetic properties and biological activities. J. Sci. Food. Agric. 2016, 96, 2952–2962. [Google Scholar] [CrossRef] [PubMed]
- Srinivasulu, C.; Ramgopal, M.; Ramanjaneyulu, G.; Anuradha, C.M.; Kumar, S.C. Syringic acid (SA)—A review of its occurrence, biosynthesis, pharmacological and industrial importance. Biomed. Pharm. 2018, 108, 547–557. [Google Scholar] [CrossRef] [PubMed]
- Kujala, T.S.; Loponen, J.M.; Klika, K.D.; Pihlaja, K. Phenolics and betacyanins in red beetroot (Beta vulgaris) root: Distribution and effect of cold storage on the content of total phenolics and three individual compounds. J. Agric. Food Chem. 2000, 48, 5338–5342. [Google Scholar] [CrossRef]
- Kujala, T.S.; Vienola, M.S.; Klika, K.D.; Jyrki, M.; Loponen, J.M.; Pihlaja, K. Betalain and phenolic compositions of four beetroot (Beta vulgaris) cultivars. Eur. Food Res. Technol. 2002, 214, 505–510. [Google Scholar] [CrossRef]
- Wruss, J.; Waldenberger, G.; Huemer, S.; Uygun, P.; Lanzerstorfer, P.; Müller, U.; Höglinger, O.; Weghuber, J. Compositional characteristics of commercial beetroot products and beetroot juice prepared from seven beetroot varieties grown in Upper Austria. J. Food Compos. Anal. 2015, 42, 46–55. [Google Scholar] [CrossRef]
- Fernandes, F.H.; Salgado, H.R. Gallic acid: Review of the methods of determination and quantification. Crit. Rev. Anal. Chem. 2016, 46, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Dludla, P.V.; Nkambule, B.B.; Jack, B.; Mkandla, Z.; Mutize, T.; Silvestri, S.; Orlando, P.; Tiano, L.; Louw, J.; Mazibuko-Mbeje, S.E. Inflammation and oxidative stress in an obese state and the protective effects of gallic acid. Nutrients 2018, 11, 23. [Google Scholar] [CrossRef]
- Ferk, F.; Kundi, M.; Brath, H.; Szekeres, T.; Al-Serori, H.; Mišík, M.; Saiko, P.; Marculescu, R.; Wagner, K.H.; Knasmueller, S. Gallic acid improves health-associated biochemical parameters and prevents oxidative damage of DNA in type 2 diabetes patients: Results of a placebo-controlled pilot study. Mol. Nutr. Food Res. 2018, 62, 1–30. [Google Scholar] [CrossRef]
- Doan, K.V.; Ko, C.M.; Kinyua, A.W.; Yang, D.J.; Choi, Y.W.; Oh, I.Y.; Nguyen, N.M.; Ko, A.; Choi, J.W.; Jeong, Y.; et al. Gallic acid regulates body weight and glucose homeostasis through AMPK activation. Endocrinology 2015, 156, 157–168. [Google Scholar] [CrossRef]
- Prasad, C.N.; Anjana, T.; Banerji, A.; Gopalakrishnapillai, A. Gallic acid induces GLUT4 translocation and glucose uptake activity in 3T3-L1 cells. FEBS Lett. 2010, 584, 531–536. [Google Scholar] [CrossRef]
- Gandhi, G.R.; Jothi, G.; Antony, P.J.; Balakrishna, K.; Paulraj, M.G.; Ignacimuthu, S.; Stalin, A.; Al-Dhabi, N.A. Gallic acid attenuates high-fat diet fed-streptozotocin-induced insulin resistance via partial agonism of PPARgamma in experimental type 2 diabetic rats and enhances glucose uptake through translocation and activation of GLUT4 in PI3K/p-Akt signaling pathway. Eur. J. Pharm. 2014, 745, 201–216. [Google Scholar] [CrossRef]
- Abdel-Moneim, A.; El-Twab, S.M.A.; Yousef, A.I.; Reheim, E.S.A.; Ashour, M.B. Modulation of hyperglycemia and dyslipidemia in experimental type 2 diabetes by gallic acid and p-coumaric acid: The role of adipocytokines and PPARγ. Biom. Pharm. 2018, 105, 1091–1097. [Google Scholar] [CrossRef] [PubMed]
- Ellulu, M.S.; Patimah, I.; Khaza’ai, H.; Rahmat, A.; Abed, Y. Obesity and inflammation: The linking mechanism and the complications. Arch. Med. Sci. 2017, 13, 851–863. [Google Scholar] [CrossRef] [PubMed]
- Oi, Y.; Hou, I.C.; Fujita, H.; Yazawa, K. Antiobesity effects of Chinese black tea (Pu-erh tea) extract and gallic acid. Phytother. Res. 2012, 26, 475–481. [Google Scholar] [CrossRef]
- Makihara, H.; Shimada, T.; Machida, E.; Oota, M.; Nagamine, R.; Tsubata, M.; Kinoshita, K.; Takahashi, K.; Aburada, M. Preventive effect of Terminalia bellirica on obesity and metabolic disorders in spontaneously obese type 2 diabetic model mice. J. Nat. Med. 2012, 66, 459–467. [Google Scholar] [CrossRef]
- Yuda, N.; Tanaka, M.; Suzuki, M.; Asano, Y.; Ochi, H.; Iwatsuki, K. Polyphenols extracted from black tea (Camellia sinensis) residue by hot-compressed water and their inhibitory effect on pancreatic lipase in vitro. J. Food Sci. 2012, 77, H254–H261. [Google Scholar] [CrossRef]
- Huang, D.W.; Chang, W.C.; Yang, H.J.; Wu, J.S.; Shen, S.C. Gallic acid alleviates hypertriglyceridemia and fat accumulation via modulating glycolysis and lipolysis pathways in perirenal adipose tissues of rats fed a high-fructose diet. Int. J. Mol. Sci. 2018, 19, 254. [Google Scholar] [CrossRef]
- Park, Y.K.; Lee, J.; Hong, V.S.; Choi, J.S.; Lee, T.Y.; Jang, B.C. Identification of KMU-3, a novel derivative of gallic acid, as an inhibitor of adipogenesis. PLoS ONE 2014, 9, e109344. [Google Scholar] [CrossRef]
- Graf, E. Antioxidant potential of ferulic acid. Free Radic. Biol. Med. 1992, 13, 435–448. [Google Scholar] [CrossRef]
- Srinivasan, M.; Sudheer, A.R.; Menon, V.P. Ferulic acid: Therapeutic potential through its antioxidant property. J. Clin. Biochem. Nutr. 2007, 40, 92–100. [Google Scholar] [CrossRef]
- Alam, M.A. Anti-hypertensive effect of cereal antioxidant ferulic acid and its mechanism of action. Front. Nutr. 2019, 6, 121. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.W.; Wang, S.L.; Chen, X.Y. Preliminary study on effects of sodium ferulate in treating diabetic nephropathy. Zhongguo Zhong Xi Yi Jie He Za Zhi 2006, 26, 803–806. [Google Scholar] [PubMed]
- Bumrungpert, A.; Lilitchan, S.; Tuntipopipat, S.; Tirawanchai, N.; Komindr, S. Ferulic acid supplementation improves lipid profiles, oxidative stress, and inflammatory status in hyperlipidemic subjects: A randomized, double-blind, placebo-controlled clinical trial. Nutrients 2018, 10, 713. [Google Scholar] [CrossRef] [PubMed]
- Saija, A.; Tomaino, A.; Trombetta, D.; De Pasquale, A.; Uccella, N.; Barbuzzi, T.; Paolino, D.; Bonina, F. In vitro and in vivo evaluation of caffeic and ferulic acids as topical photoprotective agents. Int. J. Pharm. 2000, 199, 39–47. [Google Scholar] [CrossRef]
- Murray, J.C.; Burch, J.A.; Streilein, R.D.; Iannacchione, M.A.; Hall, R.P.; Pinnell, S.R. A topical antioxidant solution containing vitamins C and E stabilized by ferulic acid provides protection for human skin against damage caused by ultraviolet irradiation. J. Am. Acad. Derm. 2008, 59, 418–425. [Google Scholar] [CrossRef]
- Oresajo, C.; Stephens, T.; Hino, P.D.; Law, R.M.; Yatskayer, M.; Foltis, P.; Pillai, S.; Pinnell, S.R. Protective effects of a topical antioxidant mixture containing vitamin C, ferulic acid, and phloretin against ultraviolet-induced photodamage in human skin. J. Cosmet. Derm. 2008, 7, 290–297. [Google Scholar] [CrossRef]
- Wu, Y.; Zheng, X.; Xu, X.G.; Li, Y.H.; Wang, B.; Gao, X.H.; Chen, H.D.; Yatskayer, M.; Oresajo, C. Protective effects of a topical antioxidant complex containing vitamins C and E and ferulic acid against ultraviolet irradiation-induced photodamage in Chinese women. J. Drugs Derm. 2013, 12, 464–468. [Google Scholar] [CrossRef]
- Balasubashini, M.S.; Rukkumani, R.; Viswanathan, P.; Menon, V.P. Ferulic acid alleviates lipid peroxidation in diabetic rats. Phytother. Res. 2004, 18, 310–314. [Google Scholar] [CrossRef]
- Yeh, C.T.; Ching, L.C.; Yen, G.C. Inducing gene expression of cardiac antioxidant enzymes by dietary phenolic acids in rats. J. Nutr. Biochem. 2009, 20, 163–171. [Google Scholar] [CrossRef]
- Son, M.J.; Rico, C.W.; Nam, S.H.; Kang, M.Y. Influence of oryzanol and ferulic acid on the lipid metabolism and antioxidative status in high fat-fed mice. J. Clin. Biochem. Nutr. 2010, 46, 150–156. [Google Scholar] [CrossRef]
- Maurya, D.K.; Devasagayam, T.P.A. Antioxidant and prooxidant nature of hydroxycinnamic acid derivatives ferulic and caffeic acids. Food Chem. Toxicol. 2010, 48, 3369–3373. [Google Scholar] [CrossRef] [PubMed]
- Ou, L.; Kong, L.Y.; Zhang, X.M.; Niwa, M. Oxidation of ferulic acid by Momordica charantia peroxidase and related anti-inflammation activity changes. Biol. Pharm. Bull. 2003, 26, 1511–1516. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.O.; Min, K.J.; Kwon, T.K.; Um, B.H.; Moreau, R.A.; Choi, S.W. Anti-inflammatory activity of hydroxycinnamic acid derivatives isolated from corn bran in lipopolysaccharide-stimulated Raw 264.7 macrophages. Food Chem. Toxicol. 2012, 50, 1309–1316. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, A.; Kagawa, D.; Fujii, A.; Ochiai, R.; Tokimitsu, I.; Saito, I. Short- and long-term effects of ferulic acid on blood pressure in spontaneously hypertensive rats. Am. J. Hypertens. 2002, 15, 351–357. [Google Scholar] [CrossRef]
- Ardiansyah, O.Y.; Shirakawa, H.; Koseki, T.; Komai, M. Novel effects of a single administration of ferulic acid on the regulation of blood pressure and the hepatic lipid metabolic profile in stroke-prone spontaneously hypertensive rats. J. Agric. Food Chem. 2008, 56, 2825–2830. [Google Scholar] [CrossRef]
- Kwon, E.Y.; Do, G.M.; Cho, Y.Y.; Park, Y.B.; Jeon, S.M.; Choi, M.S. Anti-atherogenic property of ferulic acid in apolipoprotein E-deficient mice fed western diet: Comparison with clofibrate. Food Chem. Toxicol. 2010, 48, 2298–2303. [Google Scholar] [CrossRef]
- Genaro-Mattos, T.C.; Maurício, Â.Q.; Rettori, D.; Alonso, A.; Hermes-Lima, M. Antioxidant activity of caffeic acid against iron-induced free radical generation—A chemical approach. PLoS ONE 2015, 10, e0129963. [Google Scholar] [CrossRef]
- Liang, N.; Kitts, D.D. Role of chlorogenic acids in controlling oxidative and inflammatory stress conditions. Nutrients 2015, 8, 16. [Google Scholar] [CrossRef]
- Hardie, D. AMPK: A target for drugs and natural products with effects on both diabetes and cancer. Diabetes 2013, 62, 2164–2172. [Google Scholar] [CrossRef]
- Tyszka-Czochara, M.; Konieczny, P.; Majka, M. Caffeic acid expands anti-tumor effect of metformin in human metastatic cervical carcinoma HTB-34 cells: Implications of AMPK activation and impairment of fatty acids de novo biosynthesis. Int. J. Mol. Sci. 2017, 18, 462. [Google Scholar] [CrossRef]
- Min, J.; Shen, H.; Xi, W.; Wang, Q.; Yin, L.; Zhang, Y.; Yu, Y.; Yang, Q.; Wang, Z.N. Synergistic anticancer activity of combined use of caffeic acid with paclitaxel enhances apoptosis of non-small-cell lung cancer h1299 cells in vivo and in vitro. Cell Physiol. Biochem. 2018, 48, 1433–1442. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.X.; Yu, P.F.; Gao, Z.M.; Yuan, J.; Zhang, Z. Caffeic acid n-butyl ester-triggered necrosis-like cell death in lung cancer cell line A549 is prompted by ROS mediated alterations in mitochondrial membrane potential. Eur. Rev. Med. Pharm. Sci. 2017, 21, 1665–1671. [Google Scholar]
- Dziedzic, A.; Kubina, R.; Kabała-Dzik, A.; Wojtyczka, R.D.; Morawiec, T.; Bułdak, R.J. Caffeic acid reduces the viability and migration rate of oral carcinoma cells (SCC-25) exposed to low concentrations of ethanol. Int. J. Mol. Sci. 2014, 15, 18725–18741. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.J.; Shin, J.A.; Yang, I.H.; Won, D.H.; Ahn, C.H.; Kwon, H.J.; Lee, J.S.; Cho, N.P.; Kim, E.C.; Yoon, H.J.; et al. Apoptosis induced by caffeic acid phenethyl ester in human oral cancer cell lines: Involvement of puma and bax activation. Arch. Oral. Biol. 2017, 84, 94–99. [Google Scholar] [CrossRef]
- Guerriero, E.; Sorice, A.; Capone, F.; Costantini, S.; Palladino, P.; D’ischia, M.; Castello, G. Effects of lipoic acid, caffeic acid and a synthesized lipoyl-caffeic conjugate on human hepatoma cell lines. Molecules 2011, 16, 6365–6377. [Google Scholar] [CrossRef]
- Brautigan, D.L.; Gielata, M.; Heo, J.; Kubicka, E.; Wilkins, L.R. Selective toxicity of caffeic acid in hepatocellular carcinoma cells. Biochem. Biophys. Res. Commun. 2018, 505, 612–617. [Google Scholar] [CrossRef]
- Jaganathan, S.K. Growth inhibition by caffeic acid, one of the phenolic constituents of honey, in HCT 15 colon cancer cells. TSWJ 2012, 2012, 372345. [Google Scholar] [CrossRef]
- Tang, H.; Yao, X.; Yao, C.; Zhao, X.; Zuo, H.; Li, Z. Anti-colon cancer effect of caffeic acid p-nitro-phenethyl ester in vitro and in vivo and detection of its metabolites. Sci. Rep. 2017, 7, 7599. [Google Scholar] [CrossRef]
- Mc Cubrey, J.A.; Steelman, L.S.; Chappel, I.W.H.; Abrams, S.L.; Wong, E.W.; Chang, F.; Lehmann, B.; Terrian, D.M.; Milella, M.; Tafuri, A.; et al. Roles of the Raf/MEK/ERK pathway in cell growth, malignant transformation and drug resistance. Biochim. Biophys. Acta 2007, 1773, 1263–1284. [Google Scholar] [CrossRef]
- Khan, F.A.; Maalik, A.; Murtaza, G. Inhibitory mechanism against oxidative stress of caffeic acid. J. Food Drug Anal. 2016, 24, 695–702. [Google Scholar] [CrossRef]
- Nardini, M.; D’Aquino, M.; Tomassi, G.; Gentili, V.; Di Felice, M.; Scaccini, C. Inhibition of human low-density lipoprotein oxidation by caffeic acid and other hydroxycinnamic acid derivatives. Free Radic. Biol. Med. 1995, 19, 541–552. [Google Scholar] [CrossRef]
- Son, S.; Lewis, B.A. Free radical scavenging and antioxidative activity of caffeic acid amide and ester analogues: Structure-activity relationship. J. Agric. Food Chem. 2002, 50, 468–472. [Google Scholar] [CrossRef] [PubMed]
- Cheng, J.C.; Dai, F.; Zhou, B.; Yang, L.; Liu, Z.L. Antioxidant activity of hydroxycinnamic acid derivatives in human low-density lipoprotein: Mechanism and structure-activity relationship. Food Chem. 2007, 104, 132–139. [Google Scholar] [CrossRef]
- Clifford, M.N. Chlorogenic acids and other cinnamates—Nature, occurrence, dietary burden, absorption and metabolism. J. Sci. Food. Agric. 2000, 80, 1033–1043. [Google Scholar] [CrossRef]
- Santana-Gálvez, J.; Cisneros-Zevallos, L.; Jacobo-Velázquez, D.A. Chlorogenic acid: Recent advances on its dual role as a food additive and a nutraceutical against metabolic syndrome. Molecules 2017, 22, 358. [Google Scholar] [CrossRef] [PubMed]
- Naveed, M.; Hejazi, V.; Abbas, M.; Kamboh, A.A.; Khan, G.J.; Shumzaid, M.; Ahmad, F.; Babazadeh, D.; Fang, F.X.; Modarresi-Ghazani, F.; et al. Chlorogenic acid (CGA): A pharmacological review and call for further research. Biomed. Pharm. 2018, 97, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Clifford, M.N.; Jaganath, I.B.; Ludwig, I.A.; Crozier, A. Chlorogenic acids and the acyl-quinic acids: Discovery, biosynthesis, bioavailability and bioactivity. Nat. Prod. Rep. 2017, 34, 1391–1421. [Google Scholar] [CrossRef]
- Nabavi, S.F.; Tejada, S.; Setzer, W.N.; Gortzi, O.; Sureda, A.; Braidy, N.; Daglia, M.; Manayi, A.; Nabavi, S.M. Chlorogenic acid and mental diseases: From chemistry to medicine. Curr. Neuropharmacol. 2017, 15, 471–479. [Google Scholar] [CrossRef] [PubMed]
- Shi, H.; Shi, A.; Dong, L.; Lu, X.; Wang, Y.; Zhao, J.; Dai, F.; Guo, X. Chlorogenic acid protects against liver fibrosis in vivo and in vitro through inhibition of oxidative stress. Clin. Nutr. 2016, 35, 1366–1373. [Google Scholar] [CrossRef]
- Han, D.; Gu, X.; Gao, J.; Wang, Z.; Liu, G.; Barkema, H.W.; Han, B. Chlorogenic acid promotes the Nrf2/HO-1 anti-oxidative pathway by activating p21Waf1/Cip1 to resist dexamethasone-induced apoptosis in osteoblastic cells. Free Radic. Biol. Med. 2019, 137, 1–12. [Google Scholar] [CrossRef]
- Bao, L.; Li, J.; Zha, D.; Zhang, L.; Gao, P.; Yao, T.; Wu, X. Chlorogenic acid prevents diabetic nephropathy by inhibiting oxidative stress and inflammation through modulation of the Nrf2/HO-1 and NF-ĸB pathways. Int. Immunopharmacol. 2018, 54, 245–253. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.M.; Chen, R.X.; Zhang, L.L.; Ding, N.N.; Liu, C.; Cui, Y.; Cheng, Y.X. In vivo protective effects of chlorogenic acid against triptolide-induced hepatotoxicity and its mechanism. Pharm. Biol. 2018, 56, 626–631. [Google Scholar] [CrossRef] [PubMed]
- Ward, N.C.; Hodgson, J.M.; Woodman, R.J.; Zimmermann, D.; Poquet, L.; Leveques, A.; Actis-Goretta, L.; Puddey, I.B.; Croft, K.D. Acute effects of chlorogenic acids on endothelial function and blood pressure in healthy men and women. Food Funct. 2016, 7, 2197–2203. [Google Scholar] [CrossRef] [PubMed]
- Saitou, K.; Ochiai, R.; Kozuma, K.; Sato, H.; Koikeda, T.; Osaki, N.; Katsuragi, Y. Effect of chlorogenic acids on cognitive function: A randomized, double-blind, placebo-controlled trial. Nutrients 2018, 10, 1337. [Google Scholar] [CrossRef] [PubMed]
- Harris, N.N.; Javellana, J.; Davies, K.M.; Lewis, D.H.; Jameson, P.E.; Deroles, S.C.; Calcott, K.E.; Gould, K.S.; Schwinn, K.E. Betalain production is possible in anthocyanin-producing plant species given the presence of DOPA-dioxygenase and L-DOPA. BMC Plant. Biol. 2012, 12, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Barbu, V.; Cotârleț, M.; Bolea, C.A.; Cantaragiu, A.; Andronoiu, D.G.; Bahrim, G.E.; Enachi, E. three types of beetroot products enriched with lactic acid bacteria. Foods 2020, 9, 786. [Google Scholar] [CrossRef]
- Tzin, V.; Galili, G. New insights into the shikimate and aromatic amino acids biosynthesis pathways in plants. Mol. Plants 2010, 3, 956–972. [Google Scholar] [CrossRef]
- Steglich, W.; Strack, D. Chapter 1 Betalains. In The Alkaloids: Chemistry and Pharmacology; Elsevier: Amsterdam, The Netherlands, 1990; Volume 39, pp. 1–62. [Google Scholar] [CrossRef]
- Girod, P.A.; Zryd, J.P. Biogenesis of betalains: Purification and partial characterization of dopa 4,5-dioxygenase from Amanita muscaria. Phytochemistry 1991, 30, 169–174. [Google Scholar] [CrossRef]
- Christinet, L.; Burdet, F.R.X.; Zaiko, M.; Hinz, U.; Zryd, J.P. Characterization and functional identification of a novel plant 4,5-extradiol dioxygenase involved in betalain pigment biosynthesis in Portulaca grandiflora. Plant Physiol. 2004, 134, 265–274. [Google Scholar] [CrossRef]
- Schliemann, W.; Kobayashi, N.; Strack, D. The decisive step in betaxanthin biosynthesis is a spontaneous reaction. Plant. Physiol. 1999, 119, 1217–1232. [Google Scholar] [CrossRef]
- Gandía-Herrero, F.; García-Carmona, F. Biosynthesis of betalains: Yellow and violet plant pigments. Trends Plant Sci. 2013, 18, 334–343. [Google Scholar] [CrossRef] [PubMed]
- Stintzing, F.C.; Carle, R. Functional properties of anthocyanins and betalains in plants, food, and in human nutrition. Trends Food Sci. Technol. 2004, 15, 19–38. [Google Scholar] [CrossRef]
- Belhadj Slimen, I.; Najar, T.; Abderrabba, M. Chemical and antioxidant properties of betalains. J. Agric. Food Chem. 2017, 65, 675–689. [Google Scholar] [CrossRef] [PubMed]
- Cai, Y.; Sun, M.; Corke, H. Identification and distribution of simple and acylated betacyanins in the Amaranthaceae. J. Agric. Food Chem. 2001, 49, 1971–1978. [Google Scholar] [CrossRef] [PubMed]
- Vulić, J.; Čanadanović-Brunet, J.; Ćetković, G.; Tumbas, V.; Djilas, S.; Četojević-Simin, D.; Čanadanović, V. Antioxidant and cell growth activities of beetroot pomace extracts. J. Funct. Food 2012, 4, 670–688. [Google Scholar] [CrossRef]
- Vulić, J.J.; Ćebović, T.N.; Čanadanović-Brunet, J.M.; Ćetković, G.S.; Čanadanović, V.M.; Djilas, S.M.; Šaponjac, V.T.T. In vivo and in vitro antioxidant effects of beetroot pomace extracts. J. Funct. Food 2014, 6, 168–175. [Google Scholar] [CrossRef]
- De Mejia, E.G.; Zhang, Q.; Penta, K.; Eroğlu, A.; Lila, M.A. The colors of health: Chemistry, bioactivity, and market demand for colorful foods and natural food sources of colorants. Annu. Rev. Nutr. 2020, 11, 145–182. [Google Scholar] [CrossRef]
- Silva, V.T.; Baião, D.S.; Silva, O.; Alves, G.; Perrone, D.; Del Aguila, E.M.; Paschoalin, V.M.F. Betanin, a natural food additive: Stability, bioavailability, antioxidant and preservative ability assessments. Molecules 2019, 24, 458. [Google Scholar] [CrossRef]
- European Food Safety Authority. Scientific opinion on the re-evaluation of beetroot red (E 162) as a food additive. EFSA J. 2015, 13, 4318. [Google Scholar] [CrossRef]
- US Food and Drug Administration (FDA). Code of Federal Regulations. 2009. Available online: https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfcfr/CFRSearch.cfm?fr=73.260 (accessed on 28 January 2020).
- Sucu, C.; Yildiz, G.T. The investigation of the use of beetroot powder in Turkish fermented beef sausage (sucuk) as nitrite alternative. Meat. Sci. 2018, 140, 158–166. [Google Scholar] [CrossRef]
- Tesoriere, L.; Allegra, M.; Butera, D.; Livrea, M.A. Absorption, excretion, and distribution of dietary antioxidant betalains in LDLs: Potential health effects of betalains in humans. Am. J. Clin. Nutr. 2004, 80, 941–945. [Google Scholar] [CrossRef] [PubMed]
- Sawicki, T.; Juśkiewicz, J.; Wiczkowski, W. Using the SPE and Micro-HPLC-MS/MS method for the analysis of betalains in rat plasma after red beet administration. Molecules 2017, 22, 2137. [Google Scholar] [CrossRef] [PubMed]
- Tesoriere, L.; Gentile, C.; Angileri, F.; Attanzio, A.; Tutone, M.; Allegra, M.; Livrea, M.A. Trans-epithelial transport of the betalain pigments indicaxanthin and betanin across Caco-2 cell monolayers and influence of food matrix. Eur. J. Nutr. 2013, 52, 1077–1087. [Google Scholar] [CrossRef] [PubMed]
- Moreno, D.A.; García-Viguera, C.; Gil, J.I.; Gil-Izquierdo, A. Betalains in the era of global agri-food science, technology and nutritional health. Phytochem. Rev. 2008, 7, 261–280. [Google Scholar] [CrossRef]
- Frank, T.; Stintzing, F.C.; Carle, R.; Bitsch, I.; Quaas, D.; Strass, G.; Bitsch, R.; Netzel, M. Urinary pharmacokinetics of betalains following consumption of red beet juice in healthy humans. Pharm. Res. 2005, 52, 290–297. [Google Scholar] [CrossRef] [PubMed]
- Tesoriere, L.; Fazzari, M.; Angileri, F.; Gentile, C.; Livrea, M.A. In vitro digestion of betalainic foods. Stability and bioaccessibility of betaxanthins and betacyanins and antioxidative potential of food digesta. J. Agric. Food Chem. 2008, 56, 10487–11092. [Google Scholar] [CrossRef] [PubMed]
- Netzel, M.; Stintzing, F.C.; Quaas, D.; Strab, G.; Carle, R.; Bitsch, R.; Bitsch, I.; Frank, T. Renal excretion of antioxidative constituents from red beet in humans. Food Res. Int. 2005, 38, 1051–1058. [Google Scholar] [CrossRef]
- Kanner, J.; Harel, S.; Granit, R. Betalains—A new class of dietary cationized antioxidants. J. Agric. Food Chem. 2001, 49, 5178–5185. [Google Scholar] [CrossRef]
- Clifford, T.; Constantinou, C.M.; Keane, K.M.; West, D.J.; Howatson, G.; Stevenson, E.J. The plasma bioavailability of nitrate and betanin from Beta vulgaris rubra in humans. Eur. J. Nutr. 2017, 56, 1245–1254. [Google Scholar] [CrossRef]
- Rahimi, P.; Mesbah-Namin, S.A.; Ostadrahimi, A.; Abedimanesh, S.; Separham, A.; Asghary, J.M. Effects of betalains on atherogenic risk factors in patients with atherosclerotic cardiovascular disease. Food Funct. 2019, 10, 8286–8297. [Google Scholar] [CrossRef]
- Zielińska-Przyjemska, M.; Olejnik, A.; Kostrzewa, A.; Łuczak, M.; Jagodziński, P.P.; Baer-Dubowska, W. The beetroot component betanin modulates ROS production, DNA damage and apoptosis in human polymorphonuclear neutrophils. Phytother. Res. 2012, 26, 845–852. [Google Scholar] [CrossRef] [PubMed]
- Sakihama, Y.; Maeda, M.; Hashimoto, M.; Tahara, S.; Hashidoko, Y. Beetroot betalain inhibits peroxynitrite-mediated tyrosine nitration and DNA strand cleavage. Free Radic. Res. 2012, 46, 93–99. [Google Scholar] [CrossRef] [PubMed]
- Vidal, P.J.; López-Nicolás, J.M.; Gandía-Herrero, F.; García-Carmona, F. Inactivation of lipoxygenase and cyclooxygenase by natural betalains and semi-synthetic analogues. Food Chem. 2014, 154, 246–254. [Google Scholar] [CrossRef] [PubMed]
- Gentile, C.; Tesoriere, L.; Allegra, M.; Livrea, M.A.; D’Alessio, P. Antioxidant betalains from cactus pear (Opuntiaficus-indica) inhibit endothelial ICAM-1 expression. Ann. N. Y. Acad. Sci. 2004, 1028, 481–486. [Google Scholar] [CrossRef]
- Kapadia, G.J.; Azuine, M.A.; Rao, G.S.; Arai, T.; Lida, A.; Tokuda, H. Cytotoxic effect of the red beetroot (Beta vulgaris L.) extract compared to doxorubicin (Adriamycin) in the human prostate (PC-3) and breast (MCF-7) cancer cell lines. Anticancer Agents Med. Chem. 2011, 11, 280–284. [Google Scholar] [CrossRef] [PubMed]
- Tan, D.; Wang, Y.; Bai, B.; Yang, X.; Han, J. Betanin attenuates oxidative stress and inflammatory reaction in kidney of paraquat-treated rat. Food Chem. Toxicol. 2015, 78, 141–146. [Google Scholar] [CrossRef]
- Dhananjayan, I.; Kathiroli, S.; Subramani, S.; Veerasamy, V. Ameliorating effect of betanin, a natural chromoalkaloid by modulating hepatic carbohydrate metabolic enzyme activities and glycogen content in streptozotocin - nicotinamide induced experimental rats. Biomed. Pharm. 2017, 88, 1069–1079. [Google Scholar] [CrossRef]
- Han, J.; Tan, C.; Wang, Y.; Yang, S.; Tan, D. Betanin reduces the accumulation and cross-links of collagen in high-fructose-fed rat heart through inhibiting non-enzymatic glycation. Chem. Biol. Interact. 2015, 227, 37–44. [Google Scholar] [CrossRef]
- Sutariya, B.; Saraf, M. Betanin, isolated from fruits of Opuntia elatior Mill attenuates renal fibrosis in diabetic rats through regulating oxidative stress and TGF-β pathway. J. Ethnopharmacol. 2017, 198, 432–443. [Google Scholar] [CrossRef]
- Silva, D.V.T.; Pereira, A.D.; Boaventura, G.T.; Ribeiro, R.S.A.; Verícimo, M.A.; Carvalho-Pinto, C.E.; Baião, D.S.; Del Aguila, E.M.; Paschoalin, V.M.F. Short-term betanin intake reduces oxidative stress in wistar rats. Nutrients 2019, 11, 1978. [Google Scholar] [CrossRef]
- Hasler, C.M. The changing face of functional foods. J. Am. Coll. Nutr. 2000, 19, 499S–506S. [Google Scholar] [CrossRef] [PubMed]
- Joshipura, K.J.; Hu, F.B.; Manson, J.E.; Stampfer, M.J.; Rimm, E.B.; Speizer, F.E.; Colditz, G.; Ascherio, A.; Rosner, B.; Spiegelman, D.; et al. The effect of fruit and vegetable intake on risk for coronary heart disease. Ann. Intern. Med. 2001, 134, 1106–1114. [Google Scholar] [CrossRef] [PubMed]
- Lundberg, J.O.; Gladwin, M.T.; Ahluwalia, A.; Benjamin, N.; Bryan, N.S.; Butler, A.; Cabrales, P.; Fago, A.; Feelisch, M.; Ford, P.C.; et al. Nitrate and nitrite in biology, nutrition and therapeutics. Nat. Chem. Biol. 2009, 5, 865–869. [Google Scholar] [CrossRef] [PubMed]
- Burleigh, M.; Liddle, L.; Muggeridge, D.J.; Monaghan, C.; Sculthorpe, N.; Butcher, J.; Henriquez, F.; Easton, C. Dietary nitrate supplementation alters the oral microbiome but does not improve the vascular responses to an acute nitrate dose. Nitric Oxide 2019, 89, 54–63. [Google Scholar] [CrossRef] [PubMed]
- Karwowska, M.; Kononiuk, A. Nitrates/nitrites in food—Risk for nitrosative stress and benefits. Antioxidants 2020, 9, 241. [Google Scholar] [CrossRef] [PubMed]
- Vong, L.B.; Nagasaki, Y. Nitric oxide nano-delivery systems for cancer therapeutics: Advances and challenges. Antioxidants 2020, 9, 791. [Google Scholar] [CrossRef] [PubMed]
- Richardson, G.; Hicks, S.L.; O’Byrne, S.; Frost, M.T.; Moore, K.; Benjamin, N.; McKnight, G.M. The ingestion of inorganic nitrate increases gastric S-nitrosothiol levels and inhibits platelet function in humans. Nitric Oxide 2002, 7, 24–29. [Google Scholar] [CrossRef]
- Hobbs, A.J.; Moncada, S. Antiplatelet properties of a novel, non-NO-based soluble guanylate cyclase activator. Vasc. Pharm. 2003, 40, 149–154. [Google Scholar] [CrossRef]
- Bradley, S.A.; Steinert, J.R. Nitric oxide-mediated posttranslational modifications: Impacts at the synapse. Ox. Med. Cell. Long. 2016, 2016, 5681036. [Google Scholar] [CrossRef]
- Hartwig, J.; Italiano, J., Jr. The birth of the platelet. J. Thromb. Haemost. 2003, 1, 1580–1586. [Google Scholar] [CrossRef]
- Stankevičius, E.; Kevelaitis, E.; Vainorius, E.; Simonsen, U. Role of nitric oxide and other endothelium-derived factors. Medicina (Kaunas) 2003, 39, 333–341. [Google Scholar]
- Zago, A.S.; Zanesco, A. Nitric oxide, cardiovascular disease and physical exercise. Arq. Bras. Cardiol. 2006, 87, 264–270. [Google Scholar] [CrossRef] [PubMed]
- Chamchoi, A.; Srihirun, S.; Paiboonsukwong, K.; Sriwantana, T.; Sathavorasmith, P.; Pattanapanyasat, K.; Hirsch, R.E.; Schechter, A.N.; Sibmooh, N. Decreased nitrite reductase activity of deoxyhemoglobin correlates with platelet activation in hemoglobin E/ß-thalassemia subjects. PLoS ONE 2018, 13, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Jajja, A.; Sutyarjoko, A.; Lara, J.; Rennie, K.; Brandt, K.; Qadir, O.; Siervo, M. Beetroot supplementation lowers daily systolic blood pressure in older, overweight subjects. Nutr. Res. 2014, 34, 868–875. [Google Scholar] [CrossRef]
- Bondonno, C.P.; Liu, A.H.; Croft, K.D.; Ward, N.C.; Shinde, S.; Moodley, Y.; Lundberg, J.O.; Puddey, I.B.; Woodman, R.J.; Hodgson, J.M. Absence of an effect of high nitrate intake from beetroot juice on blood pressure in treated hypertensive individuals: A randomized controlled trial. Am. J. Clin. Nutr. 2015, 102, 368–375. [Google Scholar] [CrossRef] [PubMed]
- Velmurugan, S.; Gan, J.M.; Rathod, K.S.; Khambata, R.S.; Ghosh, S.M.; Hartley, A.; Eijl, S.V.; Sagi-Kiss, V.; Chowdhury, T.A.; Curtis, M.; et al. Dietary nitrate improves vascular function in patients with hypercholesterolemia: A randomized, double-blind, placebo-controlled study. Am. J. Clin. Nutr. 2016, 103, 25–38. [Google Scholar] [CrossRef] [PubMed]
- Bock, J.M.; Ueda, K.; Schneider, A.C.; Hughes, W.E.; Limberg, J.K.; Bryan, N.S.; Casey, D.P. Inorganic nitrate supplementation attenuates peripheral chemoreflex sensitivity but does not improve cardiovagal baroreflex sensitivity in older adults. Am. J. Physiol. Hear. Circ. Physiol. 2018, 314, H45–H51. [Google Scholar] [CrossRef]
- Cuenca, E.; Jodra, P.; Pérez-López, A.; González-Rodríguez, L.G.; Silva, S.F.; Veiga-Herreros, P.; Domíngue, R. Effects of beetroot juice supplementation on performance and fatigue in a 30-s all-out sprint exercise: A randomized, double-blind cross-over study. Nutrients 2018, 10, 1222. [Google Scholar] [CrossRef]
- De Castro, T.F.; Manoel, F.A.; Figueiredo, D.H.; Figueiredo, D.H.; Machado, F.A. Effect of beetroot juice supplementation on 10-km performance in recreational runners. Appl. Physiol. Nutr. Metab. 2019, 44, 90–94. [Google Scholar] [CrossRef]
- Baião, D.S.; D’El Rei, J.; Alves, G.; Neves, M.F.; Perrone, D.; Del Aguila, E.M.; Paschoalin, V.M.F. Chronic effects of nitrate supplementation with a newly designed beetroot formulation on biochemical and hemodynamic parameters of individuals presenting risk factors for cardiovascular diseases: A pilot study. J. Funct. Foods 2019, 58, 85–94. [Google Scholar] [CrossRef]
- Bezerra, Á.D.L.; Costa, E.C.; Pacheco, D.A.; Souza, D.C.; Farias-Junior, L.F.; Ritti-Dia, R.M.; Grigolo, G.B.; de Bittencourt Júnior, P.I.H.; Krause, M.; Fayh, A.P.T. Effect of acute dietary nitrate supplementation on the post-exercise ambulatory blood pressure in obese males: A randomized, controlled, crossover trial. J. Sports Sci. Med. 2019, 18, 118–127. [Google Scholar]
- Berends, J.E.; van den Berg, L.M.M.; Guggeis, M.A.; Henckens, N.F.T.; Hossein, I.J.; de Joode, M.E.J.R.; Zamani, H.; van Pelt, K.A.A.J.; Beelen, N.A.; Kuhnle, G.G.; et al. Consumption of nitrate-rich beetroot juice with or without vitamin C supplementation increases the excretion of urinary nitrate, nitrite, and N-nitroso compounds in humans. Int. J. Mol. Sci. 2019, 20, 2277. [Google Scholar] [CrossRef] [PubMed]
- Husmann, F.; Bruhn, S.; Mittlmeier, T.; Zschorlich, V.; Behrens, M. Dietary nitrate supplementation improves exercise tolerance by reducing muscle fatigue and perceptual responses. Front. Physiol. 2019, 10, 404. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.J.K.; Roe, C.A.; Somani, Y.B.; Moore, D.J.; Barrett, M.A.; Flanagan, M.; Kim-Shapiro, D.B.; Basu, S.; Muller, M.D.; Proctor, D.N. Effects of acute dietary nitrate supplementation on aortic blood pressures and pulse wave characteristics in post-menopausal women. Nitric Oxide 2019, 85, 10–16. [Google Scholar] [CrossRef]
- Kukadia, S.; Dehbi, H.M.; Tillin, T.; Coady, E.; Chaturvedi, N.; Hughes, A.D. A Double-blind placebo-controlled crossover study of the effect of beetroot juice containing dietary nitrate on aortic and brachial blood pressure over 24 h. Front. Physiol. 2019, 10, 47. [Google Scholar] [CrossRef]
- Ritz, T.; Werchan, C.A.; Kroll, J.L.; Rosenfield, D. Beetroot juice supplementation for the prevention of cold symptoms associated with stress: A proof-of-concept study. Physiol. Behav. 2019, 202, 45–51. [Google Scholar] [CrossRef]
- Rokkedal-Lausch, T.; Franch, J.; Poulsen, M.K.; Thomsen, L.P.; Weitzberg, E.; Kamavuako, E.N.; Karbing, D.S.; Larsen, R.G. Chronic high-dose beetroot juice supplementation improves time trial performance of well-trained cyclists in normoxia and hypoxia. Nitric Oxide 2019, 85, 44–52. [Google Scholar] [CrossRef]
- Jones, T.; Dunn, E.L.; Macdonald, J.H.; Kubis, H.P.; McMahon, N.; Sandoo, A. The effects of beetroot juice on blood pressure, microvascular function and large-vessel endothelial function: A Randomized, double-blind, placebo-controlled pilot study in healthy older adults. Nutrients 2019, 11, 1792. [Google Scholar] [CrossRef]
- Smith, K.; Muggeridge, D.J.; Easton, C.; Ross, M.D. An acute dose of inorganic dietary nitrate does not improve high-intensity, intermittent exercise performance in temperate or hot and humid conditions. Eur. J. Appl. Physiol. 2019, 119, 723–733. [Google Scholar] [CrossRef]
- Lara, J.; Ashor, A.W.; Oggioni, C.; Ahluwalia, A.; Mathers, J.C.; Siervo, M. Effects of inorganic nitrate and beetroot supplementation on endothelial function: A systematic review and meta-analysis. Eur. J. Nutr. 2016, 55, 451–459. [Google Scholar] [CrossRef]
- Barouch, L.A.; Harrison, R.W.; Skaf, M.W.; Rosas, G.O.; Cappola, T.P.; Kobeissi, Z.A.; Hobai, I.A.; Lemmon, C.A.; Burnett, A.L.; O’Rourke, B.; et al. Nitric oxide regulates the heart by spatial confinement of nitric oxide synthase isoforms. Nature 2002, 416, 337–339. [Google Scholar] [CrossRef] [PubMed]
- Adachi, T.; Weisbrod, R.M.; Pimentel, D.R.; Ying, J.; Sharov, V.S.; Schöneich, C.; Cohen, R.A. S-glutathiolation by peroxynitrite activates SERCA during arterial relaxation by nitric oxide. Nat. Med. 2004, 10, 1200–1207. [Google Scholar] [CrossRef] [PubMed]
- Lima, B.; Forrester, M.T.; Hess, D.T.; Stamler, J.S. S-nitrosylation in cardiovascular signaling. Circ. Res. 2010, 106, 633–646. [Google Scholar] [CrossRef] [PubMed]
- Hernández, A.; Schiffer, T.A.; Ivarsson, N.; Cheng, A.J.; Bruton, J.D.; Lundberg, J.O.; Weitzberg, E.; Westerblad, H. Dietary nitrate increases tetanic [Ca2+]i and contractile force in mouse fast-twitch muscle. J. Physiol. 2012, 590, 3575–3583. [Google Scholar] [CrossRef] [PubMed]
- Rammos, C.; Totzeck, M.; Deenen, R.; Köhrer, K.; Kelm, M.; Rassaf, T.; Hendgen-Cotta, H.B. Dietary nitrate is a modifier of vascular gene expression in old male mice. Oxid. Med. Cell Longev. 2015, 2015, 1–12. [Google Scholar] [CrossRef]
- Raat, N.J.; Noguchi, A.C.; Liu, V.B.; Raghavachari, N.; Liu, D.; Xu, X.; Shiva, S.; Munson, P.J.; Gladwin, M.T. Dietary nitrate and nitrite modulate blood and organ nitrite and the cellular ischemic stress response. Free Radic. Biol. Med. 2009, 47, 510–517. [Google Scholar] [CrossRef]
- Krajka-Kuźniak, V.; Paluszczak, J.; Szaefer, H.; Baer-Dubowska, W. Betanin, a beetroot component, induces nuclear factor erythroid-2-related factor 2-mediated expression of detoxifying/antioxidant enzymes in human liver cell lines. Br. J. Nutr. 2013, 110, 2138–2149. [Google Scholar] [CrossRef]
- Stefanson, A.L.; Bakovic, M. Dietary regulation of Keap1/Nrf2/ARE pathway: Focus on plant-derived compounds and trace minerals. Nutrients 2014, 6, 3777–3801. [Google Scholar] [CrossRef]
| Compound | Beetroot Formulations | |||
|---|---|---|---|---|
| Cereal Bar | Gel | Chips | Juice | |
| Ashes (%) | 1.30 ± 0.06 b | 2.01 ± 0.13 a | 1.00 ± 0.05 c | 0.80 ± 0.06 d |
| Moisture (%) | 12.90 ± 0.50 b | 76.14 ± 0.48 a | 4.66 ± 0.57 c | 85.50 ± 0.50 a |
| Energy (kilocalorie) | 325.58 ± 2.5 b | 148.50 ± 0.01 c | 365.05 ± 2.10 a | 94.90 ± 1.70 d |
| Carbohydrate (g) | 62.97 ± 0.97 b | 42.62 ± 0.31 c | 89.96 ± 0.52 a | 22.67 ± 0.40 d |
| Protein (g) | 16.20 ± 0.39 a | 3.02 ± 0.09 b | 0.97 ± 0.01 c | 0.70 ± 0.07 c |
| Lipids (g) | 0.97 ± 1.00 a | 0.66 ± 0.01 b | 0.14 ± 0.01 c | 0.16 ± 0.01 c |
| Total dietary fibers (g) | 4.07 ± 0.14 a | 3.71 ± 0.10 c | 3.22 ± 0.63 b | 0.91 ± 0.31 d |
| Total sugars (g) | 37.72 ± 0.70 a | 14.90 ± 0.23 c | 18.79 ± 0.13 b | 12.11 ± 0.35 d |
| Fructose (g) | 2.79 ± 0.15 a | 1.21 ± 0.15 b | 1.47 ± 0.11 b | 0.86 ± 0.19 c |
| Glucose (g) | 4.71 ± 0.16 a | 2.61 ± 0.12 b | 2.70 ± 0.11 b | 2.45 ± 0.21 b |
| Sucrose (g) | 26.59 ± 0.80 a | 11.60 ± 0.13 c | 14.62 ± 0.17 b | 8.80 ± 0.65 d |
| Maltose (g) | 3.63 ± 0.19 a | 0.00 b | 0.00 b | 0.00 b |
| NO3− (mmol) | 14.00 ± 0.05 a | 6.30 ± 0.01 b | 6.90 ± 0.02 b | 4.10 ± 0.01 c |
| NO2− (mmol) | 0.20 ± 0.01 a | 0.11 ± 0.02 b | 0.13 ± 0.02 b | 0.10 ± 0.02 b |
| Betanin (mg·g−1) | 173 ± 0.12 c | 246 ± 0.07 b | 1274 ± 0.01 d | 298.5 ± 0.03 a |
| Compounds | Beetroot Product Interventions | |||
|---|---|---|---|---|
| Cereal Bar | Chips | Gel | Juice | |
| OAs (mg/g) | ||||
| Citric acid | 2.31 ± 0.14 a | 1.52 ± 0.06 b | 1.04 ± 0.10 c | 0.89 ± 0.10 d |
| Ascorbic acid | 1.55 ± 0.21 a | 0.93 ± 0.09 b | 0.53 ± 0.04 c | 0.41 ± 0.03 d |
| Malic acid | 3.00 ± 0.10 a | 2.26 ± 0.10 b | 1.59 ± 0.01 c | 1.34 ± 0.20 d |
| Fumaric acid | 0.81 ± 0.10 a | 0.63 ± 0.10 a,b | 0.41 ± 0.20 b | 0.18 ± 0.10 c |
| Succinic acid | 0.51 ± 0.01 | - | - | - |
| Oxalic acid | 0.50 ± 0.15 | - | - | - |
| Total | 9.19 ± 0.71 a | 5.34 ± 0.35 b | 3.57 ± 0.35 c | 2.84 ± 0.70 d |
| PCs (mg/100 g) | ||||
| Vanillic acid | 13.14 ± 0.11 | - | - | - |
| p-Coumaric acid | 39.68 ± 1.21 | - | - | - |
| Rosmarinic acid | 4.25 ± 0.04 | - | - | - |
| 3,4-Dihydroxybenzoic acid | 9.97 ± 0.12 a | 7.85 ± 0.10 b | 5.43 ± 0.81 c | 3.79 ± 0.03 d |
| Gallic acid | 60.50 ± 1.76 a | 22.49 ± 1.18 b | 8.81 ± 0.15 c | 4.10 ± 0.06 d |
| Syringic acid | 4.48 ± 0.00 a | 4.47 ± 0.01 a | 3.78 ± 0.02 b | 3.27 ± 0.05 b |
| Caffeic acid | 5.94 ± 0.03 a | 3.57 ± 0.06 b | 3.34 ± 0.21 b | 2.90 ± 0.00 c |
| Ferulic acid | 3.23 ± 0.01 a | 0.88 ± 0.04 b | 0.82 ± 0.11 b | 0.77 ± 0.01 b |
| Chlorogenic acid | 5.69 ± 0.01 a | 3.36 ± 0.02 b | 3.27 ± 0.12 b | 3.17 ± 0.45 b |
| Total | 147.73 ± 3.30 a | 42.62 ± 1.39 b | 25.45 ± 1.42 c | 18.00 ± 0.61 d |
| Saponins (mg/100 g) | 8648.00 ± 1.85 a | 6371.00 ± 1.26 b | 2200.00 ± 0.17 d | 2599.00 ± 1.27 c |
| Study | Beetroot Product Intervention | Bioactive Compounds | Experimental Population | Trial Features | Biochemical and Metabolic Effects | Hemodynamic Effects |
|---|---|---|---|---|---|---|
| Hobbs et al. [26] | Beetroot bread | NO3− (1.1 mmol) NO2− (<0.03) Betacyanins (12.1 mg) | Fourteen men genotyped for the Glu298Asp polymorphism in the eNOS gene | Randomized Single-blind Crossover Placebo-controlled Acute ingestion (10 days washout) | ↑ plasmatic NO3− and NO2− | ↓ clinic DBP iAUC 0–6 h (–36 ± 12 mm Hg) ↓ clinic SBP iAUC 0–6 h (−29 ± 17 mm Hg) |
| Jajja et al. [202] | Beetroot juice (70 mL) Blackcurrant juice (70 mL) | NO3−(≈6.45 mmol) NO2− (ND) NO3− (≈0.04 mmol) NO2− (ND) | Twenty-four older and overweight subjects | Randomized Double-blind Placebo-controlled Chronic ingestion (3 weeks and 1 week washout) | ↑urinary NO3− and NO2− concentration ↑salivary NO3− and NO2− concentration No changes in NO synthesis after blackcurrant juice ingestion | No changes in resting clinic BP or 24-h ABPM ↓ daily SBP (−7.3 ± 5.9 mm Hg) ↓ BP was not maintained after the interruption of beetroot juice supplementation |
| Baião et al. [11] | Beetroot juice (100 mL) Nitrate-depleted beetroot juice (100 mL) | NO3− (1.60 mmol) NO2− (< 0.01 mmol) PCs (17.99 mg) OAs (284 mg) NO3− (0.005 mmol) NO2− (< 0.01 mmol) PCs (14.22 mg) OAs (241 mg) | Forty healthy subjects with no cardiovascular, pulmonary, and/or metabolic Diseases | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1 week washout) | ↑ urinary NO3− and NO2− concentrations No changes in NO synthesis between men and women No changes in NO synthesis after placebo juice ingestion | - |
| Bondonno et al. [203] | Beetroot juice (140 mL) Nitrate-depleted beetroot juice (140 mL) | NO3− (7 mmol) NO2− (<0.001 mmol) NO3− (0.001 mmol) NO2− (< 50 nmol) | Twenty-seven treated hypertensive individuals | Randomized Double-blind Crossover Placebo-controlled (1 week ingestion and 1 week washout) | ↑plasmatic NO3− and NO2− concentrations ↑salivary NO3− and NO2− concentrations ↑ urinary NO3− and NO2− concentrations | No differences in home BP and 24-h ambulatory BP |
| Kapil et al. [29] | Beetroot juice (250 mL) Placebo beetroot juice (250 mL) | NO3− (≈ 6.4 mmol) NO2− (< 50 nmol/L) NO3− (≈ 0.007 mmol) NO2− (< 50 nmol/L) | Thirty-four drug-naive and 34 treated patients with hypertension | Randomized Double-blind Placebo-controlled Chronic ingestion (4 week and 1 week washout) | ↑plasmatic NO3− and NO2− concentrations ↑plasmatic cGMP concentrations | ↓ clinic BP, 24-h ambulatory BP and home BP. No evidence of tachyphylaxis over the 4-weeks intervention period. ↑ endothelial function by ≈20% ↓ arterial stiffness by 0.59 m/s |
| Velmurugan et al. [204] | Beetroot juice (250 mL) Placebo beetroot juice (250 mL) | NO3− (6.0 mmol) NO2− (< 50.0 nmol) NO3− (0.001 mmol) NO2− (< 50.0 nmol) | Sixty-five hypercholesterolemic subjects (32 received placebo and 33 received dietary NO3−) | Randomized Double-blind Placebo-controlled Chronic ingestion (6 weeks and 1 week washout) | ↑ urinary, salivary and plasmatic NO3− and NO2− concentration No changes in electrolytes (Na+, K+ and Cl−) ↓ platelet-monocyte aggregates ↓ stimulated P-selectin expression | ↑ FMD ↓ AIx ↓ aPWV ↓ SBP but not DBP and heart rate |
| da Silva et al. [12] | Beetroot Gel (100 g) | NO3- (6.30 mmol) NO2− (0.003 mmol) PCs (24.20 mg) OAs (357 mg) Saponins (3200 mg) Betanin (87 mg) | Five healthy volunteers with no cardiovascular, pulmonary, and/or metabolic diseases | Double-blind Acute ingestion (3 h of data collection) | ↑ plasmatic NO2− concentration | Minimal effects on brachial SBP and DBP |
| Vasconcellos et al. [19] | Beetroot gel (100 g) Placebo beetroot gel (100 g) | NO3− (9.92 mmol) NO2− (< 10 μmol) PCs (27.13 mg) OAs (366 mg) Saponins (3659 mg) Betanin (82 mg) NO3− (0.33 mmol) NO2− (< 10 μmol) PCs (21.13 mg) OAs (313 mg) Saponins (3059 mg) Betanin (63 mg) | Twenty-five physically active, runners, with no cardiovascular, pulmonary, and/or metabolic diseases | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | ↑ urinary NO3− and NO2− after 60, BE(T90) and AE concentration ↑ Blood glucose concentrations after AE and +20 (93.95±19.32 mg⋅dL−1) No changes in blood lactate, serum cortisol, and urinary urea concentration | No changes in VO2peak, time to fatigue, respiratory quotient, SBP, and DBP |
| Bock et al. [205] | Beetroot powder (10 g) Placebo beetroot powder (10 g) | NO3− (≈ 4.03 mmol) NO2− (≈ 0.29 mmol) | Thirteen healthy older adults with no cardiovascular, respiratory, or metabolic diseases, non-obese, and non-smokers | Randomized Double-blind Crossover Placebo-controlled 4 weeks ingestion and 1 week washout) | - | ↓ ventilatory responsiveness to hypoxia ↓ SBP and mean BP No changes in heart rate responsiveness No changes in spontaneous cardiovagal BRS |
| Cuenca et al. [206] | Beetroot juice (70 mL) Nitrate-free juice (70 mL) | NO3− (6.4 mmol) NO2− (≈ 0.04 mmol) | Fifteen healthy resistance-trained men | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | No changes in blood lactate concentration | ↑ peak and mean power output and ↓ time taken to reach Wpeak in the Wingate test No changes in fatigue index, over time and power CMJ height |
| de Castro et al. [207] | Beetroot juice (420 mL) Placebo NO3−-depleted (420 mL) | NO3− (8.4 mmol) NO2− (ND) NO3− (0.01 mmol) NO2− (ND) | Fourteen male recreational runners | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | No changes in Lapeak, Lapost, Glypre, and Glypost. | No changes in 10-km running time performance and total MV |
| Baião et al. [208] | Beet-cereal bar (60 g) Placebo beet-cereal bar (60 g) | NO3− (9.57 mmol) NO2− (0.12 mmol) PCs (88.60 mg) OAs (551.4 mg) Saponins (8648 mg) Betanin (66 mg) NO3− (0.02 mmol) NO2− (0.07 mmol) PCs (83.36 mg) OAs (431.2 mg) Saponins (7566 mg) Betanin (48 mg) | Five patients displaying three risk factors for cardiovascular diseases development | Randomized Double-blind Crossover Placebo-controlled 3 weeks ingestion trial and 1-week washout | ↑ plasmatic NO3− and NO2− concentration. | ↓ arterial stiffness through AIx, aoPP, and PWV ↓ arterial blood pressures ↓ endothelial dysfunction by improvements in cutaneous microvascular conductance peak No changes in endothelial dysfunction, arterial stiffness, and arterial blood pressure after placebo cereal bar ingestion |
| Bezerra et al. [209] | Beetroot juice (200 mL) Fruit soda (200 mL) Water (200 mL) | NO3− (≈ 13.0 mmol) NO2− (ND) NO3− (≈ 0.08 mmol) NO2− (ND) NO3− (ND) NO2− (ND) | Fourteen non-hypertensive obese males | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | ↑ NOx plasmatic concentration sustained for 1 h post-intervention | No changes in ambulatory SBP and DBP. |
| Berends et al. [210] | Beetroot juice (70 mL) Beetroot juice + vitamin C (70 mL) | NO3− (6.45 mmol) NO2− (ND) NO3− (6.45 mmol) NO2− (ND) Vitamin C (1000 mg) | Twenty-nine recreational sports subjects | Randomized Double-blinded 1 week ingestion and 1 week washout) | ↑ urinary NO3− and NO2− after beetroot juice ↑ urinary NO3− and NO2− after beetroot juice + vitamin C No changes in urinary vitamin C excretion in both interventions Beetroot juice + vitamin C ingestion inhibited N-nitroso compounds increases | - |
| Husmann et al. [211] | Beetroot juice (70 mL) Placebo NO3−depleted | NO3− (6.5 mmol) NO2− (ND) NO3− (0.04 mmol) NO2− (ND) | Twelve recreational active males | Randomized Double-blind Crossover Placebo-controlled Ingestion for 5 days (1-week washout) | - | ↑ time-to-exhaustion ↓ both lower ΔMVT and ΔPS100 ↓ perception of effort and leg muscle pain |
| Kim et al. [212] | Beetroot juice (140 mL) NO3−-depleted beetroot juice (140 mL) | NO3− (9.7 mmol) NO2− (< 50.0 nmol) - | Thirteen healthy post-menopausal and 10 pre-menopausal women | Randomized Double-blind Placebo-controlled Acute ingestion (1-week washout) | ↑ plasmatic NO3− and NO2− concentrations after 100 min and at the end of the study | Brachial and derived-aortic variables showed the expected age-associated differences in these women ↓ brachial SBP, brachial mean BP, aSBP, and mean aBP and ↑ PP amplification |
| Kukadia et al. [213] | Beetroot juice (70 mL) Nitrate-free juice (70 mL) | NO3− (7.3 mmol) NO3− (< 0.06 mmol) | Fifteen healthy subjects with no hypertension or any medication (other than an oral contraceptive pill) | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | - | Minimal effects on brachial BP and cfPWV. No sustained changes in aortic SBP over subsequent 24 h No sustained changes in hemodynamic parameters during ambulatory monitoring. |
| Ritz et al. [214] | Beetroot juice (70 mL) No-beetroot control (70 mL) | NO3− (6.5 mmol) - | Sixty healthy subjects (16 volunteers with asthma) | Single-blind Randomized Placebo-controlled 1-week ingestion and 1-week washout | - | ↓ cold symptom severity and global sickness during and after final exams Healthy vs asthma group interaction was significant for cold symptom severity and global sickness, indicating that the advantage of the beetroot juice group was greater for participants with asthma than for healthy volunteers. |
| Rokkedal-Lausch et al. [215] | Beetroot juice (140 mL) NO3--depleted beetroot juice (140 mL) | NO3− (12.4 mmol) NO3− (≈ 0.001 mmol) | Twenty healthy male cyclists | Randomized Double-blinded Counter balanced-crossover Placebo-controlled 1-week ingestion and 1 week washout | ↑ plasmatic NO3− and NO2− concentrations prior to time trial tests in normoxia and hypoxia conditions. ↑ TT performance with no difference between normoxia and hypoxia. | ↑ VO2 and VE during TT, with no difference between normoxia and hypoxia. No changes in heart rate, oxygen saturation, or muscle oxygenation during TT. |
| Jones et al. [216] | Beetroot juice (70 mL) Prune juice (70 mL) | NO3− (6.45 mmol) NO2− (ND) NO3− (< 0.01 mmol) NO2− (ND) | Twenty older subjects | Randomized Double-blinded Placebo-controlled Chronic intervention (2 weeks ingestion and 1-week washout | ↑ plasmatic NO3− concentrations No changes in endothelium-dependent (by Ach administration) or endothelium-independent (by SNP administration) microvascular responses between groups | ↓ SBP by −6±7 mm Hg and DBP by −4±3 mm Hg ↓ SBP by −4±10 mm Hg and DBP by −2±6 mm Hg after the 4 weeks treatment ↑ FMD values by 1.5%±1.8% after 4 weeks |
| Smith et al. [217] | Beetroot juice (70 mL) Nitrate-depleted placebo (70 mL) | NO3− (≈6.2 mmol) NO2− (ND) NO3− (< 0.004 mmol) NO2− (ND) | Twelve recreational trained male university students | Randomized Double-blind Crossover Placebo-controlled Acute ingestion (1-week washout) | - | No changes on sprint performance and total work done in either temperate or hot, humid conditions. No changes between trials for tympanic temperature measured at the conclusion of the exercise trial ↓ peak and mean power output in the hot and humid conditions |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
dos S. Baião, D.; da Silva, D.V.T.; Paschoalin, V.M.F. Beetroot, A Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies. Antioxidants 2020, 9, 960. https://doi.org/10.3390/antiox9100960
dos S. Baião D, da Silva DVT, Paschoalin VMF. Beetroot, A Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies. Antioxidants. 2020; 9(10):960. https://doi.org/10.3390/antiox9100960
Chicago/Turabian Styledos S. Baião, Diego, Davi V. T. da Silva, and Vania M. F. Paschoalin. 2020. "Beetroot, A Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies" Antioxidants 9, no. 10: 960. https://doi.org/10.3390/antiox9100960
APA Styledos S. Baião, D., da Silva, D. V. T., & Paschoalin, V. M. F. (2020). Beetroot, A Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies. Antioxidants, 9(10), 960. https://doi.org/10.3390/antiox9100960







