Nitric Oxide-Releasing Polymeric Materials for Antimicrobial Applications: A Review
Abstract
1. Introduction
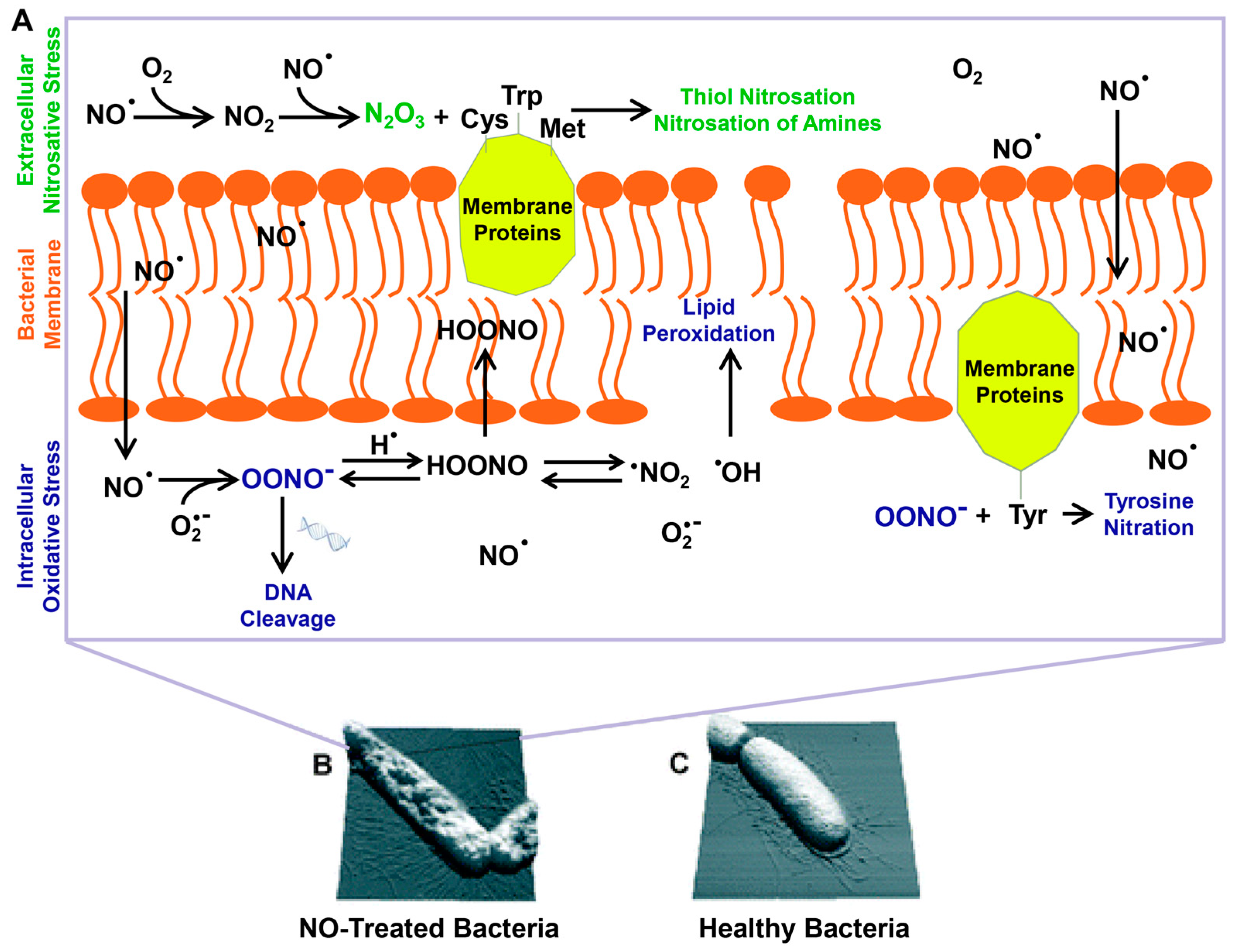
2. Antibacterial Mechanism of NO
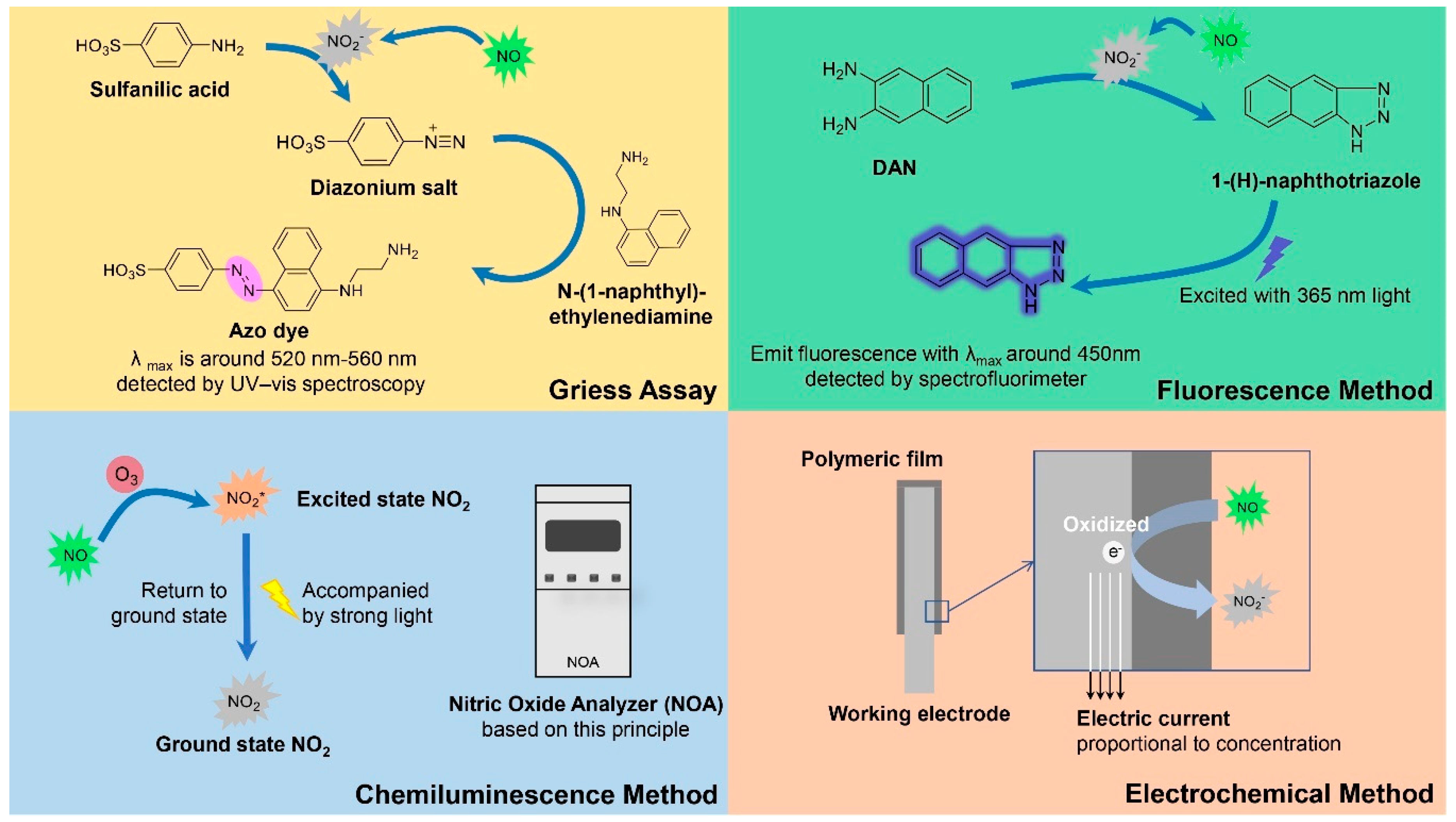
3. Methods for Detecting NO Release
3.1. Griess Assay
3.2. Fluorescence Method
3.3. Chemiluminescence Method
3.4. Electrochemical Method
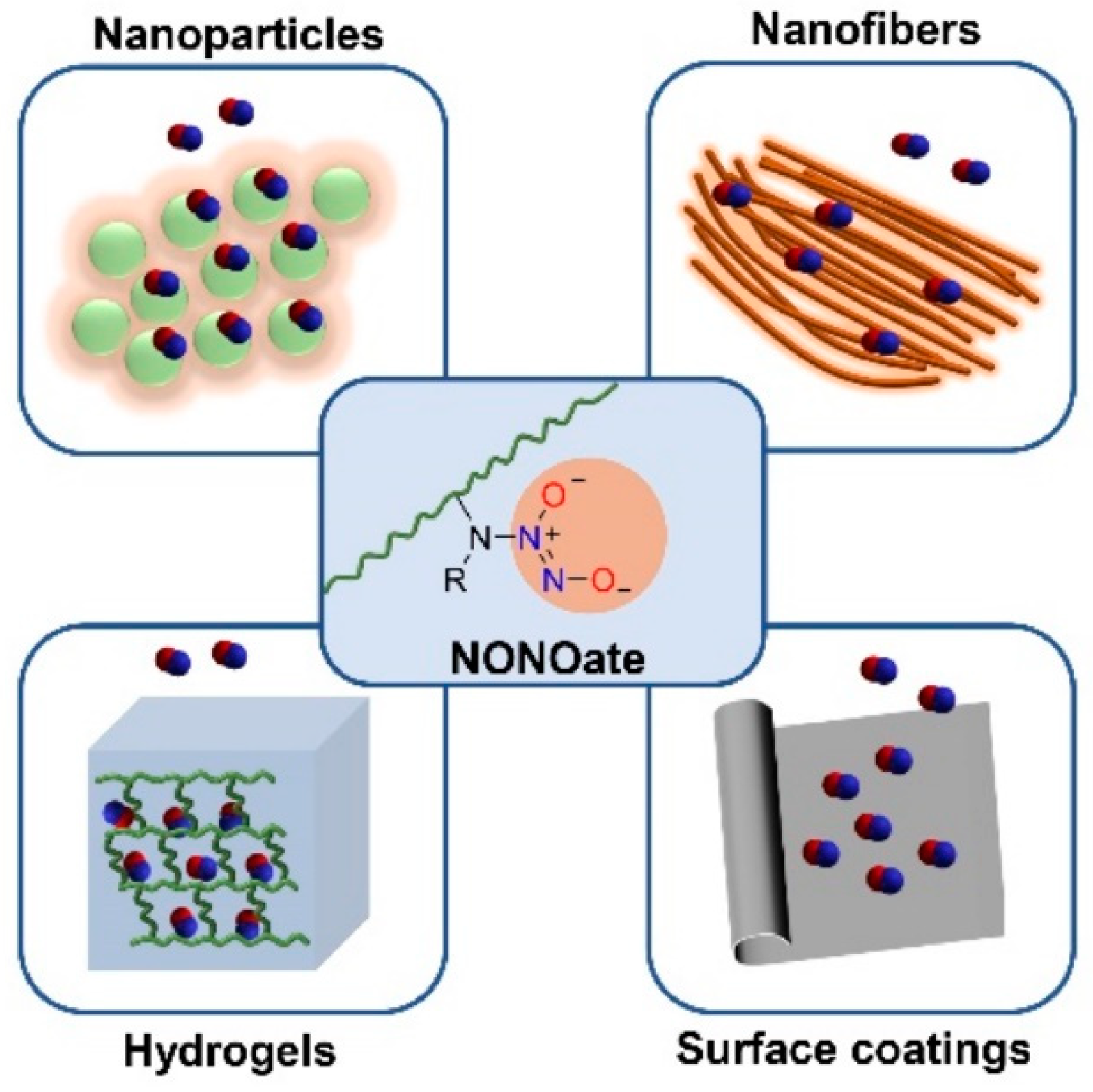
4. NO Donors for Antibacterial Application
5. NO Releasing Polymeric Materials for Antibacterial Applications
5.1. NONOate Conjugated NO Releasing Polymeric Materials
5.2. RSNO Conjugated NO Releasing Polymeric Materials
5.3. Visible Light Responsive NO Releasing Polymeric Materials
6. Anti-Biofilm Properties of NO
7. NO Releasing Polymers Applied in Indwelling Medical Devices
8. Conclusions and Prospects
Author Contributions
Funding
Conflicts of Interest
References
- Laxminarayan, R.; Duse, A.; Wattal, C.; Zaidi, A.K.M.; Wertheim, H.F.L.; Sumpradit, N.; Vlieghe, E.; Hara, G.L.; Gould, I.M.; Goossens, H.; et al. Antibiotic resistance—The need for global solutions. Lancet Infect. Dis. 2013, 13, 1057–1098. [Google Scholar] [CrossRef]
- Stanley, R.E.; Blaha, G.; Grodzicki, R.L.; Strickler, M.D.; Steitz, T.A. The structures of the anti-tuberculosis antibiotics viomycin and capreomycin bound to the 70S ribosome. Nat. Struct. Mol. Biol. 2010, 17, 289–293. [Google Scholar] [CrossRef]
- Costerton, J.W.; Stewart, P.S.; Greenberg, E.P. Bacterial biofilms: A common cause of persistent infections. Science 1999, 284, 1318–1322. [Google Scholar] [CrossRef]
- Flemming, H.-C.; Wingender, J. The biofilm matrix. Nat. Rev. Microbiol. 2010, 8, 623–633. [Google Scholar] [CrossRef]
- Stewart, P.S.; Costerton, J.W. Antibiotic resistance of bacteria in biofilms. Lancet 2001, 358, 135–138. [Google Scholar] [CrossRef]
- Alanis, A.J. Resistance to antibiotics: Are we in the post-antibiotic era? Arch. Med. Res. 2005, 36, 697–705. [Google Scholar] [CrossRef]
- Wang, Z.; Zhang, H.; Han, J.; Xing, H.; Wu, M.C.; Yang, T. Deadly Sins of Antibiotic Abuse in China. Infect. Control Hosp. Epidemiol. 2017, 38, 758–759. [Google Scholar] [CrossRef][Green Version]
- Rai, M.; Yadav, A.; Gade, A. Silver nanoparticles as a new generation of antimicrobials. Biotechnol. Adv. 2009, 27, 76–83. [Google Scholar] [CrossRef]
- Cheng, D.S.; He, M.T.; Li, W.B.; Wu, J.H.; Ran, J.H.; Cai, G.M.; Wang, X. Hydrothermal growing of cluster-like ZnO nanoparticles without crystal seeding on PET films via dopamine anchor. Appl. Surf. Sci. 2019, 467, 534–542. [Google Scholar] [CrossRef]
- Jennings, M.C.; Minbiole, K.P.C.; Wuest, W.M. Quaternary Ammonium Compounds: An Antimicrobial Mainstay and Platform for Innovation to Address Bacterial Resistance. ACS Infect. Dis. 2015, 1, 288–303. [Google Scholar] [CrossRef]
- Rabea, E.I.; Badawy, M.E.T.; Stevens, C.V.; Smagghe, G.; Steurbaut, W. Chitosan as antimicrobial agent: Applications and mode of action. Biomacromolecules 2003, 4, 1457–1465. [Google Scholar] [CrossRef]
- Yeaman, M.R.; Yount, N.Y. Mechanisms of antimicrobial peptide action and resistance. Pharmacol. Rev. 2003, 55, 27–55. [Google Scholar] [CrossRef]
- Jia, Q.; Song, Q.; Li, P.; Huang, W. Rejuvenated Photodynamic Therapy for Bacterial Infections. Adv. Healthc. Mater. 2019, 8, 1900608. [Google Scholar] [CrossRef]
- Soto, R.J.; Merricks, E.P.; Bellinger, D.A.; Nichols, T.C.; Schoenfisch, M.H. Influence of diabetes on the foreign body response to nitric oxide-releasing implants. Biomaterials 2018, 157, 76–85. [Google Scholar] [CrossRef]
- Ma, Y.Y.; Fu, L.; Hussain, Z.; Huang, D.D.; Zhu, S.H. Enhancement of storability and antioxidant systems of sweet cherry fruit by nitric oxide-releasing chitosan nanoparticles (GSNO-CS NPs). Food Chem. 2019, 285, 10–21. [Google Scholar] [CrossRef]
- Wareham, L.K.; Southam, H.M.; Poole, R.K. Do nitric oxide, carbon monoxide and hydrogen sulfide really qualify as ‘gasotransmitters’ in bacteria? Biochem. Soc. Trans. 2018, 46, 1107–1118. [Google Scholar] [CrossRef]
- Bolanos, J.P.; Almeida, A.; Stewart, V.; Peuchen, S.; Land, J.M.; Clark, J.B.; Heales, S.J.R. Nitric oxide-mediated mitochondrial damage in the brain: Mechanisms and implications for neurodegenerative diseases. J. Neurochem. 1997, 68, 2227–2240. [Google Scholar] [CrossRef]
- Furchgott, R.F.; Zawadzki, J.V. The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature 1980, 288, 373–376. [Google Scholar] [CrossRef]
- Rapoport, R.M.; Draznin, M.B.; Murad, F. Endothelium-dependent relaxation in rat aorta may be mediated through cyclic GMP-dependent protein phosphorylation. Nature 1983, 306, 174–176. [Google Scholar] [CrossRef]
- Ignarro, L.J.; Buga, G.M.; Wood, K.S.; Byrns, R.E.; Chaudhuri, G. Endothelium-derived relaxing factor produced and released from artery and vein is nitric oxide. Proc. Natl. Acad. Sci. USA 1987, 84, 9265–9269. [Google Scholar] [CrossRef]
- Culotta, E.; Koshland, D. NO news is good news. Science 1992, 258, 1862–1865. [Google Scholar] [CrossRef] [PubMed]
- Palmer, R.M.J.; Ferrige, A.G.; Moncada, S. Nitric oxide release accounts for the biological activity of endothelium-derived relaxing factor. Nature 1987, 327, 524–526. [Google Scholar] [CrossRef] [PubMed]
- Alimoradi, H.; Barzegar-Fallah, A.; Sammut, I.A.; Greish, K.; Giles, G.I. Encapsulation of tDodSNO generates a photoactivated nitric oxide releasing nanoparticle for localized control of vasodilation and vascular hyperpermeability. Free Radic. Biol. Med. 2019, 130, 297–305. [Google Scholar] [CrossRef] [PubMed]
- Prast, H.; Philippu, A. Nitric oxide as modulator of neuronal function. Prog. Neurobiol. 2001, 64, 51–68. [Google Scholar] [CrossRef]
- Džoljić, E.; Grbatinić, I.; Kostić, V. Why is nitric oxide important for our brain? Funct. Neurol. 2015, 30, 159–163. [Google Scholar] [CrossRef]
- Moncada, S.; Palmer, R.M.J.; Higgs, E.A. Nitric Oxide: Physiology, Pathophysiology, and Pharmacology. Pharmacol. Rev. 1991, 43, 109–142. [Google Scholar]
- Elewski, B.E.; Kircik, L.H.; Stasko, N.; De Leon, E.; Enloe, C.; Durham, T.; Maeda-Chubachi, T. A Phase 2, Controlled, Dose-Ranging Study of SB208, an Investigational Topical Nitric Oxide-Releasing Drug, for the Treatment of Tinea Pedis. J. Drugs Dermatol. 2018, 17, 888–893. [Google Scholar]
- Lancheros, C.A.C.; Pelegrino, M.T.; Kian, D.; Tavares, E.R.; Hiraiwa, P.M.; Goldenberg, S.; Nakamura, C.V.; Yamauchi, L.M.; Pinge, P.; Seabra, A.B.; et al. Selective Antiprotozoal Activity of Nitric Oxide-releasing Chitosan Nanoparticles Against Trypanosoma cruzi: Toxicity and Mechanisms of Action. Curr. Pharm. Des. 2018, 24, 830–839. [Google Scholar] [CrossRef]
- Weiss, J.M.; Ridnour, L.A.; Back, T.; Hussain, S.P.; He, P.; Maciag, A.E.; Keefer, L.K.; Murphy, W.J.; Harris, C.C.; Wink, D.A.; et al. Macrophage-dependent nitric oxide expression regulates tumor cell detachment and metastasis after IL-2/anti-CD40 immunotherapy. J. Exp. Med. 2010, 207, 2455–2467. [Google Scholar] [CrossRef]
- Pacher, P.; Beckman, J.S.; Liaudet, L. Nitric oxide and peroxynitrite in health and disease. Physiol. Rev. 2007, 87, 315–424. [Google Scholar] [CrossRef]
- Lee, Y.J.; Kim, Y.R.; Jeong, W.Y.; Lee, S.; Shin, J.H.; Lee, G.J. Potential Protective Effect of Nitric Oxide-Releasing Nanofibers in Hypoxia/Reoxygenation-Induced Cardiomyocyte Injury. J. Nanosci. Nanotechnol. 2019, 19, 6539–6545. [Google Scholar] [CrossRef]
- Ramadass, S.K.; Nazir, L.S.; Thangam, R.; Perumal, R.K.; Manjubala, I.; Madhan, B.; Seetharaman, S. Type I collagen peptides and nitric oxide releasing electrospun silk fibroin scaffold: A multifunctional approach for the treatment of ischemic chronic wounds. Colloids Surf. B 2019, 175, 636–643. [Google Scholar] [CrossRef]
- Zhang, Y.; Tang, K.Y.; Chen, B.; Zhou, S.; Li, N.; Liu, C.W.; Yang, J.Y.; Lin, R.; Zhang, T.; He, W.L. A polyethylenimine-based diazeniumdiolate nitric oxide donor accelerates wound healing. Biomater. Sci. 2019, 7, 1607–1616. [Google Scholar] [CrossRef]
- Efron, D.T.; Most, D.; Barbul, A. Role of nitric oxide in wound healing. Curr. Opin. Clin. Nutr. Metab. Care 2000, 3, 197–204. [Google Scholar] [CrossRef]
- Tessaro, A.L.; Fraix, A.; da Silva, A.C.P.; Gazzano, E.; Riganti, C.; Sortino, S. “Three-Bullets” Loaded Mesoporous Silica Nanoparticles for Combined Photo/Chemotherapy. Nanomaterials 2019, 9, 823. [Google Scholar] [CrossRef] [PubMed]
- Alimoradi, H.; Greish, K.; Barzegar-Fallah, A.; Alshaibani, L.; Pittala, V. Nitric oxide-releasing nanoparticles improve doxorubicin anticancer activity. Int. J. Nanomed. 2018, 13, 7771–7787. [Google Scholar] [CrossRef] [PubMed]
- Pramanick, S.; Kim, J.; Kim, J.; Saravanakumar, G.; Park, D.; Kim, W.J. Synthesis and Characterization of Nitric Oxide-Releasing Platinum(IV) Prodrug and Polymeric Micelle Triggered by Light. Bioconj. Chem. 2018, 29, 885–897. [Google Scholar] [CrossRef]
- Cheng, J.; He, K.W.; Shen, Z.Q.; Zhang, G.Y.; Yu, Y.Q.; Hu, J.M. Nitric Oxide (NO)-Releasing Macromolecules: Rational Design and Biomedical Applications. Front. Chem. 2019, 7, 00530. [Google Scholar] [CrossRef]
- Yang, L.; Feura, E.S.; Ahonen, M.J.R.; Schoenfisch, M.H. Nitric Oxide-Releasing Macromolecular Scaffolds for Antibacterial Applications. Adv. Healthc. Mater. 2018, 7, 18. [Google Scholar] [CrossRef]
- Bryan, N.S.; Lancaster, J.R. Nitric Oxide Signaling in Health and Disease. In Nitrite and Nitrate in Human Health and Disease; Bryan, N.S., Loscalzo, J., Eds.; Humana Press: Totowa, NJ, USA, 2011; pp. 169–186. [Google Scholar]
- Bowman, L.A.H.; Mclean, S.; Poole, R.K.; Fukuto, J.M. The Diversity of Microbial Responses to Nitric Oxide and Agents of Nitrosative Stress: Close Cousins but Not Identical Twins. Adv. Microb. Physiol. 2011, 59, 135–219. [Google Scholar]
- Poole, R.K.; Hughes, M.N. New functions for the ancient globin family: Bacterial responses to nitric oxide and nitrosative stress. Mol. Microbiol. 2010, 36, 775–783. [Google Scholar] [CrossRef] [PubMed]
- Stuehr, D.J.; Vasquez-Vivar, J. Nitric oxide synthases from genes to function. Nitric Oxide Biol. Chem. 2011, 63, 29. [Google Scholar] [CrossRef] [PubMed]
- Gusarov, I.; Shatalin, K.; Starodubtseva, M.; Nudler, E. Endogenous Nitric Oxide Protects Bacteria Against a Wide Spectrum of Antibiotics. Science 2009, 325, 1380–1384. [Google Scholar] [CrossRef]
- Gusarov, I.; Nudler, E. NO-mediated cytoprotection: Instant adaptation to oxidative stress in bacteria. Proc. Natl. Acad. Sci. USA 2005, 102, 13855–13860. [Google Scholar] [CrossRef]
- Ischiropoulos, H.; Al-Mehdi, A.B. Peroxynitrite-mediated oxidative protein modifications. FEBS Lett. 1995, 364, 279–282. [Google Scholar] [CrossRef]
- Carpenter, A.W.; Schoenfisch, M.H. Nitric oxide release: Part II. Therapeutic applications. Chem. Inform. 2012, 43, 3742–3752. [Google Scholar] [CrossRef] [PubMed]
- Fang, F.C. Perspectives series: Host/pathogen interactions. Mechanisms of nitric oxide-related antimicrobial activity. J. Clin. Investig. 1997, 99, 2818–2825. [Google Scholar] [CrossRef]
- Juedes, M.J.; Wogan, G.N. Peroxynitrite-induced mutation spectra of pSP189 following replication in bacteria and in human cells. Mutat. Res. Fundam. Mol. Mech. Mutagen. 1996, 349, 51–61. [Google Scholar] [CrossRef]
- Freeman, B.A.; White, C.R.; Gutierrez, H.; Paler-Martínez, A.; Tarpey, M.M.; Rubbo, H. Oxygen Radical-Nitric Oxide Reactions in Vascular Diseases. In Advances in Pharmacology; Ignarro, L., Murad, F., Eds.; Academic Press: Amsterdam, The Netherlands, 1995; Volume 34, pp. 45–69. [Google Scholar]
- Jones, M.L.; Ganopolsky, J.G.; Labbé, A.; Wahl, C.; Prakash, S. Antimicrobial properties of nitric oxide and its application in antimicrobial formulations and medical devices. Appl. Microbiol. Biotechnol. 2010, 88, 401–407. [Google Scholar] [CrossRef]
- Griess, P. Bemerkungen zu der Abhandlung der HH. Weselsky und Benedikt “Ueber einige Azoverbindungen”. Ber. Dtsch. Chem. Ges. 1879, 12, 426–428. [Google Scholar] [CrossRef]
- Fox, J.B. Kinetics and mechanisms of the Griess reaction. Anal. Chem. 1979, 51, 1493–1502. [Google Scholar] [CrossRef]
- Xu, J.; Xu, X.; Verstraete, W. Adaptation of E. coli cell method for micro-scale nitrate measurement with the Griess reaction in culture media. J. Microbiol. Methods 2000, 41, 23–33. [Google Scholar] [CrossRef]
- Sun, J.; Zhang, X.J.; Broderick, M.; Fein, H. Measurement of nitric oxide production in biological systems by using Griess Reaction assay. Sensors 2003, 3, 276–284. [Google Scholar] [CrossRef]
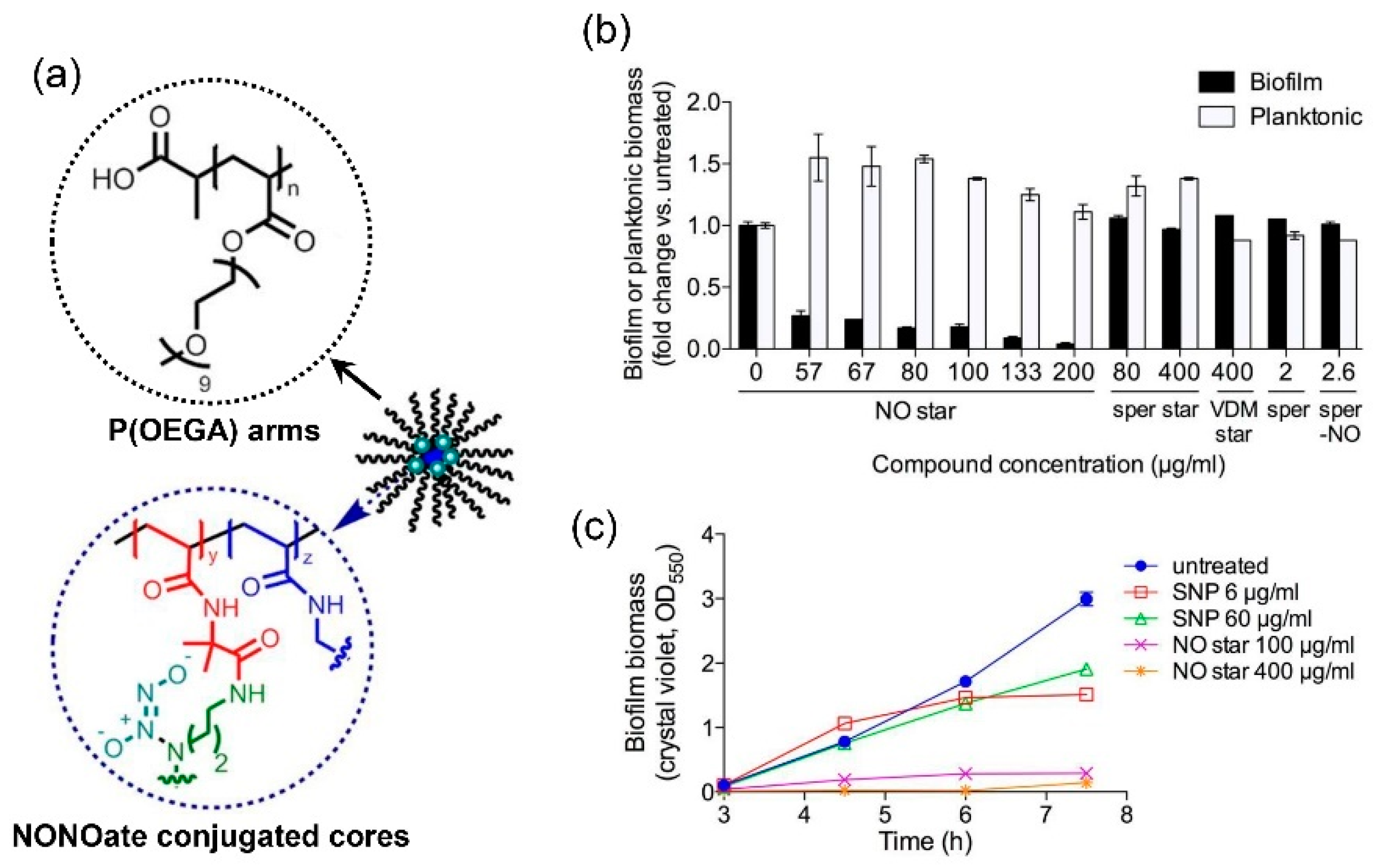
- Duong, H.T.T.; Jung, K.; Kutty, S.K.; Agustina, S.; Adnan, N.N.; Basuki, J.S.; Kumar, N.; Davis, T.P.; Barraud, N.; Boyer, C. Nanoparticle (star polymer) delivery of nitric oxide effectively negates Pseudomonas aeruginosa biofilm formation. Biomacromolecules 2014, 15, 2583–2589. [Google Scholar] [CrossRef] [PubMed]
- Damiani, P.; Burini, G. Fluorometric determination of nitrite. Talanta 1986, 33, 649–652. [Google Scholar] [CrossRef]
- Misko, T.P.; Schilling, R.J.; Salvemini, D.; Moore, W.M.; Currie, M.G. A Fluorometric Assay for the Measurement of Nitrite in Biological Samples. Anal. Biochem. 1993, 214, 11–16. [Google Scholar] [CrossRef] [PubMed]
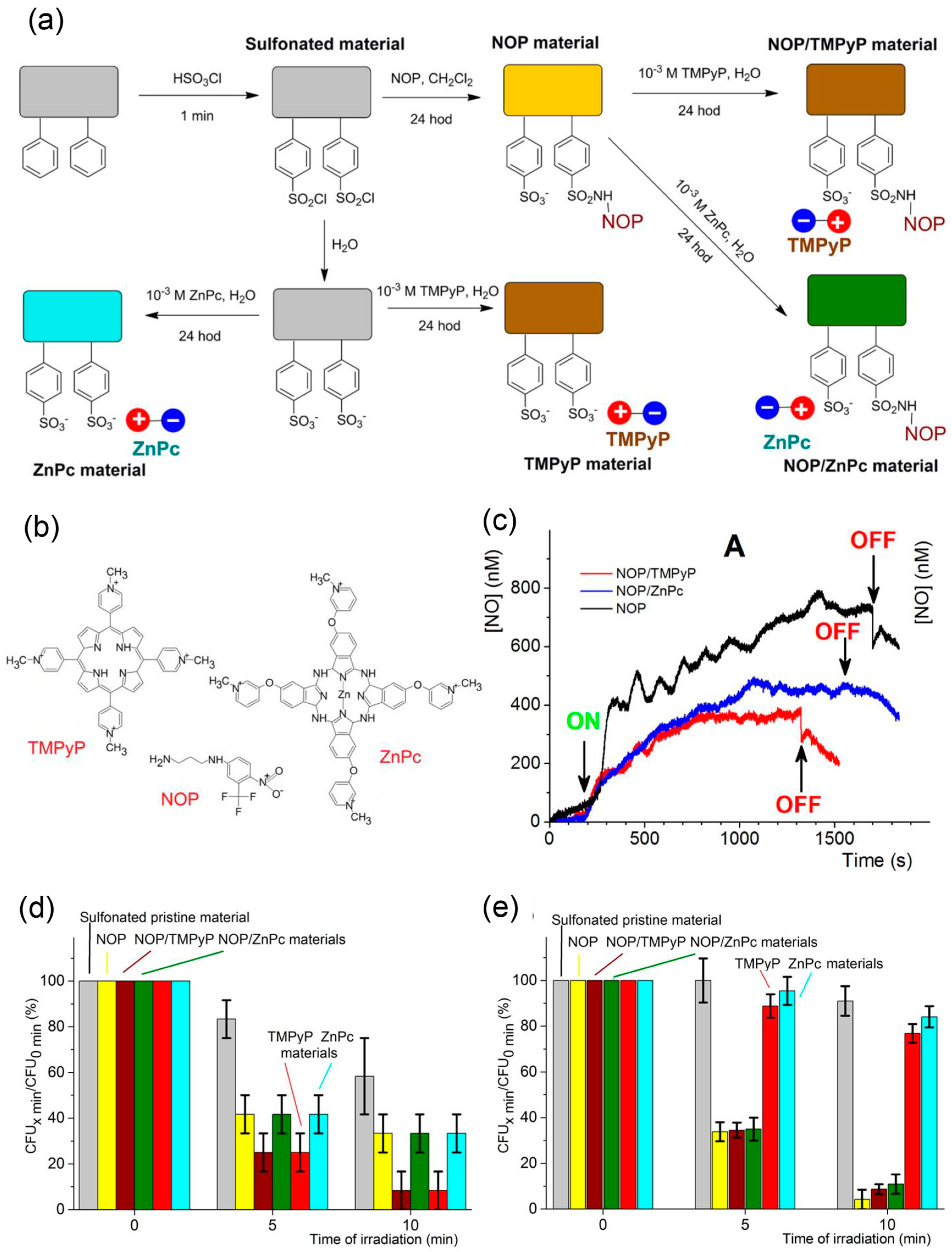
- Dolanský, J.; Henke, P.; Kubát, P.; Fraix, A.; Sortino, S.; Mosinger, J. Polystyrene Nanofiber Materials for Visible-Light-Driven Dual Antibacterial Action via Simultaneous Photogeneration of NO and O2(1Δg). ACS Appl. Mater. Interfaces 2015, 7, 22980–22989. [Google Scholar] [CrossRef]
- Kojima, H.; Urano, Y.; Kikuchi, K.; Higuchi, T.; Hirata, Y.; Nagano, T. Fluorescent Indicators for Imaging Nitric Oxide Production. Angew. Chem. Int. Ed. 1999, 38, 3209–3212. [Google Scholar] [CrossRef]
- Baudouin, E.; Pieuchot, L.; Engler, G.; Pauly, N.; Puppo, A. Nitric Oxide Is Formed in Medicago truncatula-Sinorhizobium meliloti Functional Nodules. Mol. Plant-Microbe Interact. 2006, 19, 970–975. [Google Scholar] [CrossRef]
- Molina-Favero, C.; Creus, C.M.; Simontacchi, M.; Puntarulo, S.; Lamattina, L. Aerobic Nitric Oxide Production by Azospirillum brasilense Sp245 and Its Influence on Root Architecture in Tomato. Mol. Plant-Microbe Interact. 2008, 21, 1001–1009. [Google Scholar] [CrossRef]
- Shatalin, K.; Gusarov, I.; Avetissova, E.; Shatalina, Y.; McQuade, L.E.; Lippard, S.J.; Nudler, E. Bacillus anthracis-derived nitric oxide is essential for pathogen virulence and survival in macrophages. Proc. Natl. Acad. Sci. USA 2008, 105, 1009–1013. [Google Scholar] [CrossRef]
- Patel, B.A.; Moreau, M.; Widom, J.; Chen, H.; Yin, L.; Hua, Y.; Crane, B.R. Endogenous nitric oxide regulates the recovery of the radiation-resistant bacterium Deinococcus radiodurans from exposure to UV light. Proc. Natl. Acad. Sci. USA 2009, 106, 18183–18188. [Google Scholar] [CrossRef] [PubMed]
- Stedman, D.H.; Daby, E.E.; Stuhl, F.; Niki, H. Analysis of Ozone and Nitric Oxide by a Chemiluminescent Method in Laboratory and Atmospheric Studies of Photochemical Smog. J. Air Pollut. Control Assoc. 1972, 22, 260–263. [Google Scholar] [CrossRef]
- Park, J.; Kim, J.; Singha, K.; Han, D.-K.; Park, H.; Kim, W.J. Nitric oxide integrated polyethylenimine-based tri-block copolymer for efficient antibacterial activity. Biomaterials 2013, 34, 8766–8775. [Google Scholar] [CrossRef]
- Brisbois, E.J.; Davis, R.P.; Jones, A.M.; Major, T.C.; Bartlett, R.H.; Meyerhoff, M.E.; Handa, H. Reduction in thrombosis and bacterial adhesion with 7 day implantation of S-nitroso-N-acetylpenicillamine (SNAP)-doped Elast-eon E2As catheters in sheep. J. Mater. Chem. B 2015, 3, 1639–1645. [Google Scholar] [CrossRef] [PubMed]
- Brisbois, E.J.; Major, T.C.; Goudie, M.J.; Meyerhoff, M.E.; Bartlett, R.H.; Handa, H. Attenuation of thrombosis and bacterial infection using dual function nitric oxide releasing central venous catheters in a 9 day rabbit model. Acta Biomater. 2016, 44, 304–312. [Google Scholar] [CrossRef]
- Pant, J.; Gao, J.; Goudie, M.J.; Hopkins, S.P.; Locklin, J.; Handa, H. A multi-defense strategy: Enhancing bactericidal activity of a medical grade polymer with a nitric oxide donor and surface-immobilized quaternary ammonium compound. Acta Biomater. 2017, 58, 421–431. [Google Scholar] [CrossRef]
- Hopkins, S.P.; Pant, J.; Goudie, M.J.; Schmiedt, C.; Handa, H. Achieving Long-Term Biocompatible Silicone via Covalently Immobilized S-Nitroso-N-acetylpenicillamine (SNAP) That Exhibits 4 Months of Sustained Nitric Oxide Release. ACS Appl. Mater. Interfaces 2018, 10, 27316–27325. [Google Scholar] [CrossRef]
- Xiaorong, T.; Cheng, F.; Bing, Y.; Wuming, Z. Determination of Nitric Oxide by Glassy Carbon Electrodes Modified with Poly (Neutral Red). Microchem. J. 1999, 62, 377–385. [Google Scholar] [CrossRef]
- World Precision Instruments│Biosensing│Nitric Oxide Detection│ISO-NOPF200. 2019. Available online: https://www.wpi-europe.com/products/biosensing/nitric-oxide-detection/iso-nopf200.aspx (accessed on 14 November 2019).
- Marino, N.; Perez-Lloret, M.; Blanco, A.R.; Venuta, A.; Quaglia, F.; Sortino, S. Photo-antimicrobial polymeric films releasing nitric oxide with fluorescence reporting under visible light. J. Mater. Chem. B 2016, 4, 5138–5143. [Google Scholar] [CrossRef]
- Bang, I.-S.; Liu, L.; Vazquez-Torres, A.; Crouch, M.-L.; Stamler, J.S.; Fang, F.C. Maintenance of nitric oxide and redox homeostasis by the Salmonella flavohemoglobin Hmp. J. Biol. Chem. 2006, 281, 28039–28047. [Google Scholar] [CrossRef] [PubMed]
- Ouellet, H.; Ouellet, Y.; Richard, C.; Labarre, M.; Wittenberg, B.; Wittenberg, J.; Guertin, M. Truncated hemoglobin HbN protects Mycobacterium bovis from nitric oxide. Proc. Natl. Acad. Sci. USA 2002, 99, 5902–5907. [Google Scholar] [CrossRef] [PubMed]
- Arai, H.; Hayashi, M.; Kuroi, A.; Ishii, M.; Igarashi, Y. Transcriptional regulation of the flavohemoglobin gene for aerobic nitric oxide detoxification by the second nitric oxide-responsive regulator of Pseudomonas aeruginosa. J. Bacteriol. 2005, 187, 3960–3968. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D.D. Breathing new life into nitric oxide signaling: A brief overview of the interplay between oxygen and nitric oxide. Redox Biol. 2015, 5, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Hetrick, E.M.; Shin, J.H.; Stasko, N.A.; Johnson, C.B.; Wespe, D.A.; Holmuhamedov, E.; Schoenfisch, M.H. Bactericidal efficacy of nitric oxide-releasing silica nanoparticles. ACS Nano 2008, 2, 235–246. [Google Scholar] [CrossRef]
- Stasko, N.A.; Schoenfisch, M.H. Dendrimers as a scaffold for nitric oxide release. J. Am. Med. Assoc. 2006, 128, 8265–8271. [Google Scholar] [CrossRef]
- Riccio, D.A.; Dobmeier, K.P.; Hetrick, E.M.; Privett, B.J.; Paul, H.S.; Schoenfisch, M.H. Nitric oxide-releasing S-nitrosothiol-modified xerogels. Biomaterials 2009, 30, 4494–4502. [Google Scholar] [CrossRef]
- Grommersch, B.M.; Pant, J.; Hopkins, S.P.; Goudie, M.J.; Handa, H. Biotemplated Synthesis and Characterization of Mesoporous Nitric Oxide-Releasing Diatomaceous Earth Silica Particles. ACS Appl. Mater. Interfaces 2018, 10, 2291–2301. [Google Scholar] [CrossRef]
- Veleeparampil, M.M.; Aravind, U.K.; Aravindakumar, C.T. Decomposition of S-Nitrosothiols Induced by UV and Sunlight. Adv. Phys. Chem. 2009, 2009, 890346. [Google Scholar] [CrossRef]
- Stotz, W.; Brown, L.A.S.; Jain, L. Elevated Temperature Enhances Release of Nitric Oxide from S-Nitroso-glutathione (GSNO) 351. Pediatr. Res. 1998, 43, 62. [Google Scholar] [CrossRef][Green Version]
- Swift, H.R.; Lyn, H.; Williams, D. Decomposition of S-nitrosothiols by mercury(II) and silver salts. J. Chem. Soc. Perkin Trans. 2 1997, 10, 1933–1935. [Google Scholar] [CrossRef]
- Moran, E.E.; Timerghazin, Q.K.; Kwong, E.; English, A.M. Kinetics and Mechanism of S-Nitrosothiol Acid-Catalyzed Hydrolysis: Sulfur Activation Promotes Facile NO+ Release. J. Phys. Chem. B 2011, 115, 3112–3126. [Google Scholar] [CrossRef] [PubMed]
- Smith, B.C.; Marletta, M.A. Mechanisms of S-nitrosothiol formation and selectivity in nitric oxide signaling. Curr. Opin. Chem. Biol. 2012, 16, 498–506. [Google Scholar] [CrossRef] [PubMed]
- Sortino, S. Light-controlled nitric oxide delivering molecular assemblies. Chem. Soc. Rev. 2010, 39, 2903–2913. [Google Scholar] [CrossRef] [PubMed]
- de Carvalho, C.C.C.R. Biofilms: Microbial Strategies for Surviving UV Exposure. In Ultraviolet Light in Human Health, Diseases and Environment; Ahmad, S.I., Ed.; Springer International Publishing: Cham, Switzerland, 2017; pp. 233–239. [Google Scholar]
- Elasri, M.O.; Miller, R.V. Study of the Response of a Biofilm Bacterial Community to UV Radiation. Appl. Environ. Microbiol. 1999, 65, 2025–2031. [Google Scholar] [PubMed]
- Fraix, A.; Blangetti, M.; Guglielmo, S.; Lazzarato, L.; Marino, N.; Cardile, V.; Graziano, A.C.; Manet, I.; Fruttero, R.; Gasco, A.; et al. Light-Tunable Generation of Singlet Oxygen and Nitric Oxide with a Bichromophoric Molecular Hybrid: A Bimodal Approach to Killing Cancer Cells. Chem. Med. Chem. 2016, 11, 1371–1379. [Google Scholar] [CrossRef] [PubMed]
- Drago, R.S.; Paulik, F.E. The Reaction of Nitrogen(II) Oxide with Diethylamine. J. Am. Chem. Soc. 1960, 82, 96–98. [Google Scholar] [CrossRef]
- Drago, R.S.; Karstetter, B.R. The Reaction of Nitrogen (II) Oxide with Various Primary and Secondary Amines. J. Am. Chem. Soc. 1961, 83, 1819–1822. [Google Scholar] [CrossRef]
- Lowe, A.; Deng, W.; Smith, D.W., Jr.; Balkus, K.J., Jr. Acrylonitrile-Based Nitric Oxide Releasing Melt-Spun Fibers for Enhanced Wound Healing. Macromolecules 2012, 45, 5894–5900. [Google Scholar] [CrossRef]
- Ragsdale, R.O.; Karstetter, B.R.; Drago, R.S. Decomposition of the Adducts of Diethylamine and Isopropylamine with Nitrogen (II) Oxide. Inorg. Chem. 1965, 4, 420–422. [Google Scholar] [CrossRef]
- Kim, J.; Lee, Y.; Singha, K.; Kim, H.W.; Shin, J.H.; Jo, S.; Han, D.-K.; Kim, W.J. NONOates–Polyethylenimine Hydrogel for Controlled Nitric Oxide Release and Cell Proliferation Modulation. Bioconj. Chem. 2011, 22, 1031–1038. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, T.K.; Selvanayagam, R.; Ho, K.K.K.; Chen, R.; Kutty, S.K.; Rice, S.A.; Kumar, N.; Barraud, N.; Duong, H.T.T.; Boyer, C. Co-delivery of nitric oxide and antibiotic using polymeric nanoparticles. Chem. Sci. 2016, 7, 1016–1027. [Google Scholar] [CrossRef] [PubMed]
- Sadrearhami, Z.; Yeow, J.; Nguyen, T.K.; Ho, K.K.K.; Kumar, N.; Boyer, C. Biofilm dispersal using nitric oxide loaded nanoparticles fabricated by photo-PISA: Influence of morphology. Chem. Commun. 2017, 53, 12894–12897. [Google Scholar] [CrossRef] [PubMed]
- Lowe, A.; Bills, J.; Verma, R.; Lavery, L.; Davis, K.; Balkus, K.J. Electrospun nitric oxide releasing bandage with enhanced wound healing. Acta Biomater. 2015, 13, 121–130. [Google Scholar] [CrossRef] [PubMed]
- Sadrearhami, Z.; Shafiee, F.N.; Ho, K.K.K.; Kumar, N.; Krasowska, M.; Blencowe, A.; Wong, E.H.H.; Boyer, C. Antibiofilm Nitric Oxide-Releasing Polydopamine Coatings. ACS Appl. Mater. Interfaces 2019, 11, 7320–7329. [Google Scholar] [CrossRef] [PubMed]
- Storm, W.L.; Youn, J.; Reighard, K.P.; Worley, B.V.; Lodaya, H.M.; Shin, J.H.; Schoenfisch, M.H. Superhydrophobic nitric oxide-releasing xerogels. Acta Biomater. 2014, 10, 3442–3448. [Google Scholar] [CrossRef]
- Storm, W.L.; Johnson, J.A.; Worley, B.V.; Slomberg, D.L.; Schoenfisch, M.H. Dual action antimicrobial surfaces via combined nitric oxide and silver release. J. Biomed. Mater. Res. Part A 2015, 103, 1974–1984. [Google Scholar] [CrossRef]
- Fleming, G.; Aveyard, J.; Fothergill, J.L.; McBride, F.; Raval, R.; D’Sa, R.A. Nitric Oxide Releasing Polymeric Coatings for the Prevention of Biofilm Formation. Polymers 2017, 9, 601. [Google Scholar] [CrossRef]
- Duong, H.T.T.; Adnan, N.N.M.; Barraud, N.; Basuki, J.S.; Kutty, S.K.; Jung, K.; Kumar, N.; Davis, T.P.; Boyer, C. Functional gold nanoparticles for the storage and controlled release of nitric oxide: Applications in biofilm dispersal and intracellular delivery. J. Mater. Chem. B 2014, 2, 5003–5011. [Google Scholar] [CrossRef]
- Adnan, N.N.M.; Sadrearhami, Z.; Bagheri, A.; Thuy-Khanh, N.; Wong, E.H.H.; Ho, K.K.K.; Lim, M.; Kumar, N.; Boyer, C. Exploiting the Versatility of Polydopamine-Coated Nanoparticles to Deliver Nitric Oxide and Combat Bacterial Biofilm. Macromol. Rapid Commun. 2018, 39, 1800159. [Google Scholar] [CrossRef]
- Yang, L.; Wang, X.Z.; Suchyta, D.J.; Schoenfisch, M.H. Antibacterial Activity of Nitric Oxide-Releasing Hyperbranched Polyamidoamines. Bioconj. Chem. 2018, 29, 35–43. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Jing, L.; Jiao, Y.Z.; Wang, L.F.; Marchesan, J.T.; Offenbacher, S.; Schoenfisch, M.H. In Vivo Antibacterial Efficacy of Nitric Oxide-Releasing Hyperbranched Polymers against Porphyromonas gingivalis. Mol. Pharm. 2019, 16, 4017–4023. [Google Scholar] [CrossRef] [PubMed]
- Ji, Y.; Li, G.; Zhang, W.; Ma, D.; Xue, W. Cross-linked branched polyethylenimine used as a nitric oxide donor for prolonged nitric oxide release. Mater. Sci. Eng. C 2017, 81, 492–499. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Yu, S.; Xue, W.; Ma, D.; Zhang, W. Chitosan-graft-PAMAM loading nitric oxide for efficient antibacterial application. Chem. Eng. J. 2018, 347, 923–931. [Google Scholar] [CrossRef]
- Wo, Y.; Brisbois, E.J.; Bartlett, R.H.; Meyerhoff, M.E. Recent advances in thromboresistant and antimicrobial polymers for biomedical applications: Just say yes to nitric oxide (NO). Biomater. Sci. 2016, 4, 1161–1183. [Google Scholar] [CrossRef]
- Konorev, E.A.; Tarpey, M.M.; Joseph, J.; Baker, J.E.; Kalyanaraman, B. S-nitrosoglutathione improves functional recovery in the isolated rat heart after cardioplegic ischemic arrest-evidence for a cardioprotective effect of nitric oxide. J. Pharmacol. Exp. Ther. 1995, 274, 200–206. [Google Scholar]
- Ignarro, L.J.; Lippton, H.; Edwards, J.C.; Baricos, W.H.; Hyman, A.L.; Kadowitz, P.J.; Gruetter, C.A. Mechanism of vascular smooth muscle relaxation by organic nitrates, nitrites, nitroprusside and nitric oxide: Evidence for the involvement of S-nitrosothiols as active intermediates. J. Pharmacol. Exp. Ther. 1981, 218, 739–749. [Google Scholar]
- Williams, D.L.H. The Chemistry of S-Nitrosothiols. Cheminform 1999, 30, 869–876. [Google Scholar] [CrossRef]
- Mcaninly, J.; Williams, D.L.H.; Askew, S.C.; Butler, A.R.; Russell, C. Metal ion catalysis in nitrosothiol (RSNO) decomposition. J. Chem. Soc. Chem. Commun. 1993, 23, 1758–1759. [Google Scholar] [CrossRef]
- McDougald, D.; Rice, S.A.; Barraud, N.; Steinberg, P.D.; Kjelleberg, S. Should we stay or should we go: Mechanisms and ecological consequences for biofilm dispersal. Nat. Rev. Microbiol. 2012, 10, 39–50. [Google Scholar] [CrossRef]
- Cao, G.J.; Fisher, C.M.; Jiang, X.M.; Chong, Y.; Zhang, H.; Guo, H.Y.; Zhang, Q.; Zheng, J.W.; Knolhoff, A.M.; Croley, T.R.; et al. Platinum nanoparticles: An avenue for enhancing the release of nitric oxide from S-nitroso-N-acetylpenicillamine and S-nitrosoglutathione. Nanoscale 2018, 10, 11176–11185. [Google Scholar] [CrossRef] [PubMed]
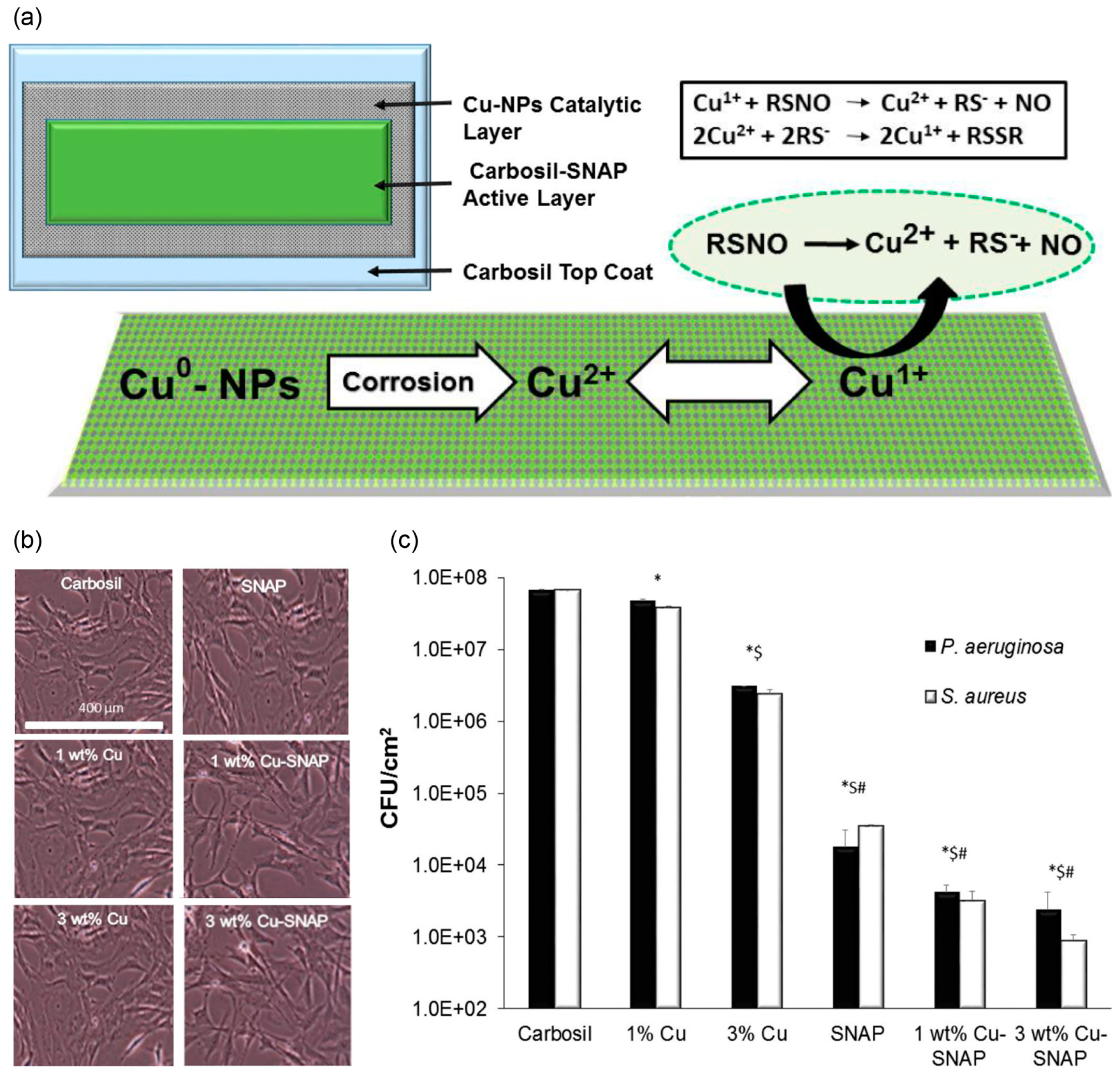
- Pant, J.; Goudie, M.J.; Hopkins, S.P.; Brisbois, E.J.; Handa, H. Tunable Nitric Oxide Release from S-Nitroso-N-acetylpenicillamine via Catalytic Copper Nanoparticles for Biomedical Applications. ACS Appl. Mater. Interfaces 2017, 9, 15254–15264. [Google Scholar] [CrossRef] [PubMed]
- Kao, P.T.; Lee, I.J.; Liau, I.; Yeh, C.S. Controllable NO release from Cu1.6S nanoparticle decomposition of S-nitrosoglutathiones following photothermal disintegration of polymersomes to elicit cerebral vasodilatory activity. Chem. Sci. 2017, 8, 291–297. [Google Scholar] [CrossRef] [PubMed]
- Singha, P.; Workman, C.D.; Pant, J.; Hopkins, S.P.; Handa, H. Zinc-oxide nanoparticles act catalytically and synergistically with nitric oxide donors to enhance antimicrobial efficacy. J. Biomed. Mater. Res. Part A 2019, 107, 1425–1433. [Google Scholar] [CrossRef] [PubMed]
- Cai, W.; Wu, J.; Xi, C.; Ashe, A.J., III; Meyerhoff, M.E. Carboxyl-ebselen-based layer-by-layer films as potential antithrombotic and antimicrobial coatings. Biomaterials 2011, 32, 7774–7784. [Google Scholar] [CrossRef]
- Mondal, A.; Douglass, M.; Hopkins, S.P.; Singha, P.; Tran, M.; Handa, H.; Brisbois, E.J. Multifunctional S-nitroso-N-acetylpenicillamine Incorporated Medical Grade Polymer with Selenium Interface for Biomedical Applications. ACS Appl. Mater. Interfaces 2019, 11, 34652–34662. [Google Scholar] [CrossRef]
- Wo, Y.; Li, Z.; Brisbois, E.J.; Colletta, A.; Wu, J.; Major, T.C.; Xi, C.; Bartlett, R.H.; Matzger, A.J.; Meyerhoff, M.E. Origin of Long-Term Storage Stability and Nitric Oxide Release Behavior of CarboSil Polymer Doped with S-Nitroso-N-acetyl-d-penicillamine. ACS Appl. Mater. Interfaces 2015, 7, 22218–22227. [Google Scholar] [CrossRef]
- Lautner, G.; Meyerhoff, M.E.; Schwendeman, S.P. Biodegradable poly(lactic-co-glycolic acid) microspheres loaded with S-nitroso-N-acetyl-d-penicillamine for controlled nitric oxide delivery. J. Controll. Release 2016, 225, 133–139. [Google Scholar] [CrossRef]
- Seabra, A.B.; Manosalva, N.; Lima, B.D.A.; Pelegrino, M.T.; Brocchi, M.; Rubilar, O.; Duran, N. Antibacterial activity of nitric oxide releasing silver nanoparticles. In Proceedings of the 5th Nanosafe International Conference on Health and Safety Issues Related to Nanomaterials for a Socially Responsible Approach, Grenoble, France, 7–10 November 2017; Volume 838. [Google Scholar]
- Pelegrino, M.T.; Lima, B.D.A.; do Nascimento, M.H.M.; Lombello, C.B.; Brocchi, M.; Seabra, A.B. Biocompatible and Antibacterial Nitric Oxide-Releasing Pluronic F-127/Chitosan Hydrogel for Topical Applications. Polymers 2018, 10, 452. [Google Scholar] [CrossRef]
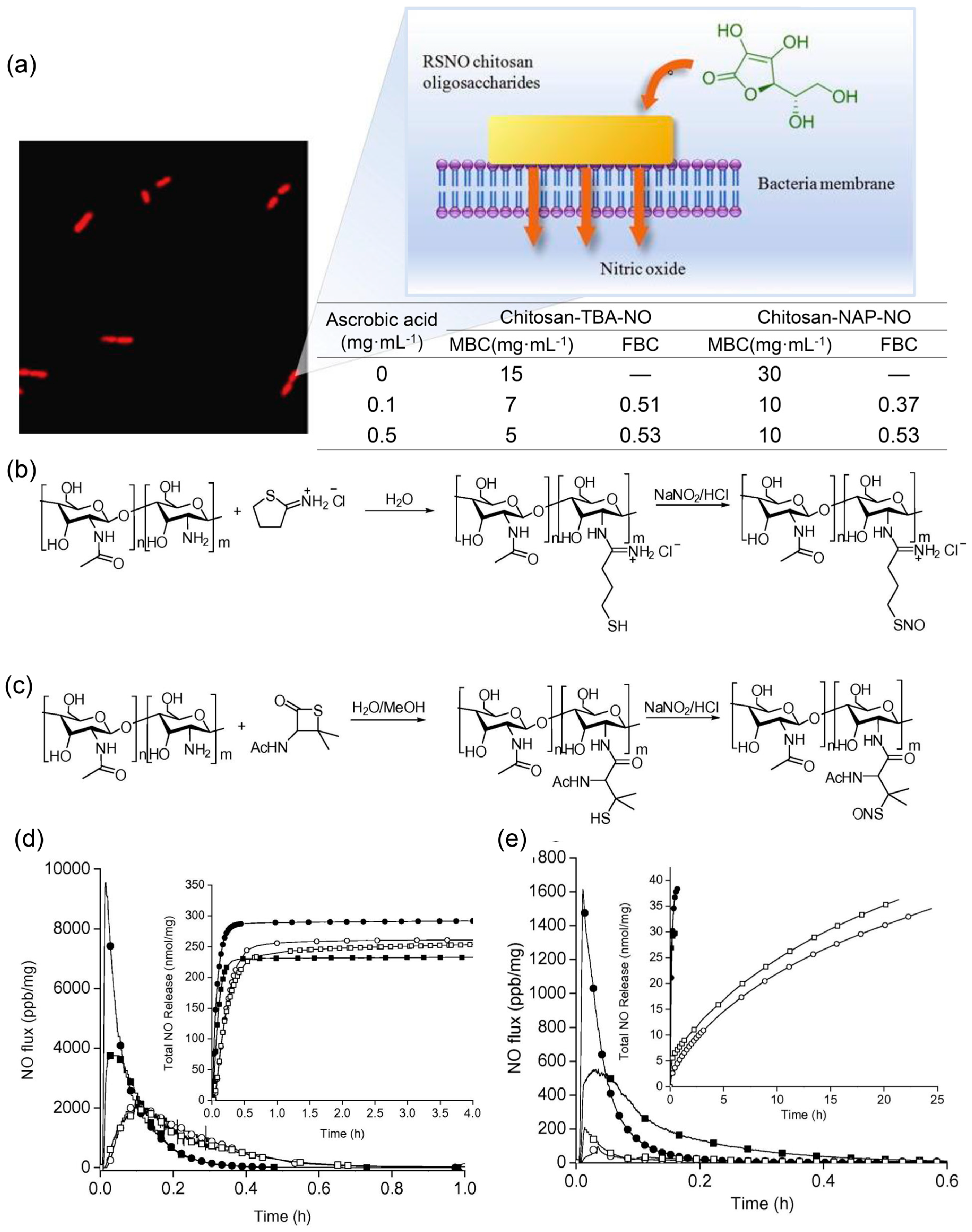
- Lu, Y.; Shah, A.; Hunter, R.A.; Soto, R.J.; Schoenfisch, M.H. S-Nitrosothiol-modified nitric oxide-releasing chitosan oligosaccharides as antibacterial agents. Acta Biomater. 2015, 12, 62–69. [Google Scholar] [CrossRef]
- Nakagawa, H. Photo-Controlled Release of Small Signaling Molecules to Induce Biological Responses. Chem. Rec. 2018, 18, 1708–1716. [Google Scholar] [CrossRef] [PubMed]
- Vittorino, E.; Cicciarella, E.; Sortino, S. A “Dual-Function” Photocage Releasing Nitric Oxide and an Anthrylmethyl Cation with a Single Wavelength Light. Chem. Eur. J. 2009, 15, 6802–6806. [Google Scholar] [CrossRef] [PubMed]
- Thomsen, H.; Marino, N.; Conoci, S.; Sortino, S.; Ericson, M.B. Confined photo-release of nitric oxide with simultaneous two-photon fluorescence tracking in a cellular system. Sci. Rep. 2018, 8, 8. [Google Scholar] [CrossRef] [PubMed]
- Rose, M.J.; Olmstead, M.M.; Mascharak, P.K. Photosensitization via Dye Coordination: A New Strategy to Synthesize Metal Nitrosyls That Release NO under Visible Light. J. Am. Chem. Soc. 2007, 129, 5342–5343. [Google Scholar] [CrossRef]
- Blangetti, M.; Fraix, A.; Lazzarato, L.; Marini, E.; Rolando, B.; Sodano, F.; Fruttero, R.; Gasco, A.; Sortino, S. A Nonmetal-Containing Nitric Oxide Donor Activated with Single-Photon Green Light. Chemistry 2017, 23, 9026–9029. [Google Scholar] [CrossRef]
- Huang, P.J.; Garcia, J.V.; Fenwick, A.; Wu, G.; Ford, P.C. Nitric Oxide Uncaging from a Hydrophobic Chromium(III) PhotoNORM: Visible and Near-Infrared Photochemistry in Biocompatible Polymer Disks. ACS Omega 2019, 4, 9181–9187. [Google Scholar] [CrossRef]
- Garcia, J.V.; Yang, J.; Shen, D.; Yao, C.; Li, X.; Wang, R.; Stucky, G.D.; Zhao, D.; Ford, P.C.; Zhang, F. NIR-Triggered Release of Caged Nitric Oxide using Upconverting Nanostructured Materials. Small 2012, 8, 3800–3805. [Google Scholar] [CrossRef]
- Deng, Q.; Xiang, H.J.; Tang, W.W.; An, L.; Yang, S.P.; Zhang, Q.L.; Liu, J.G. Ruthenium nitrosyl grafted carbon dots as a fluorescence-trackable nanoplatform for visible light-controlled nitric oxide release and targeted intracellular delivery. J. Inorg. Biochem. 2016, 165, 152–158. [Google Scholar] [CrossRef]
- Evans, M.A.; Huang, P.J.; Iwamoto, Y.; Ibsen, K.N.; Chan, E.M.; Hitomi, Y.; Ford, P.C.; Mitragotri, S. Macrophage-mediated delivery of light activated nitric oxide prodrugs with spatial, temporal and concentration control. Chem. Sci. 2018, 9, 3729–3741. [Google Scholar] [CrossRef]
- Heilman, B.; Mascharak, P.K. Light-triggered nitric oxide delivery to malignant sites and infection. Philos. Trans. R. Soc. A-Math. Phys. Eng. Sci. 2013, 371, 1–12. [Google Scholar] [CrossRef]
- Nagashima, S.; Nakasako, M.; Dohmae, N.; Tsujimura, M.; Takio, K.; Odaka, M.; Yohda, M.; Kamiya, N.; Endo, I. Novel non-heme iron center of nitrile hydratase with a claw setting of oxygen atoms. Nat. Struct. Biol. 1998, 5, 347–351. [Google Scholar] [CrossRef] [PubMed]
- Sortino, S.; Petralia, S.; Compagnini, G.; Conoci, S.; Condorelli, G. Light-Controlled Nitric Oxide Generation from a Novel Self-Assembled Monolayer on a Gold Surface. Angew. Chem. Int. Ed. 2002, 41, 1914–1917. [Google Scholar] [CrossRef]
- Sortino, S.; Giuffrida, S.; De Guidi, G.; Chillemi, R.; Petralia, S.; Marconi, G.; Condorelli, G.; Sciuto, S. The Photochemistry of Flutamide and its Inclusion Complex with β-Cyclodextrin. Dramatic Effect of the Microenvironment on the Nature and on the Efficiency of the Photodegradation Pathways. Photochem. Photobiol. 2001, 73, 6–13. [Google Scholar] [CrossRef]
- Fraix, A.; Guglielmo, S.; Cardile, V.; Graziano, A.C.E.; Gref, R.; Rolando, B.; Fruttero, R.; Gasco, A.; Sortino, S. A multi-photoresponsive molecular-hybrid for dual-modal photoinactivation of cancer cells. RSC Adv. 2014, 4, 44827–44836. [Google Scholar] [CrossRef]
- Sodano, F.; Gazzano, E.; Fraix, A.; Rolando, B.; Lazzarato, L.; Russo, M.; Blangetti, M.; Riganti, C.; Fruttero, R.; Gasco, A.; et al. A Molecular Hybrid for Mitochondria-Targeted NO Photodelivery. ChemMedChem 2018, 13, 87–96. [Google Scholar] [CrossRef]
- He, H.H.; Liu, Y.X.; Zhou, Z.N.; Guo, C.L.; Wang, H.Y.; Wang, Z.; Wang, X.L.; Zhang, Z.Q.; Wu, F.G.; Wang, H.L.; et al. A Photo-triggered and photo-calibrated nitric oxide donor: Rational design, spectral characterizations, and biological applications. Free Radic. Biol. Med. 2018, 123, 1–7. [Google Scholar] [CrossRef]
- He, H.H.; Xia, Y.; Qi, Y.X.; Wang, H.Y.; Wang, Z.; Bao, J.M.; Zhang, Z.Q.; Wu, F.G.; Wang, H.L.; Chen, D.J.; et al. A Water-Soluble, Green-Light Triggered, and Photo-Calibrated Nitric Oxide Donor for Biological Applications. Bioconj. Chem. 2018, 29, 1194–1198. [Google Scholar] [CrossRef]
- He, H.H.; Ye, Z.W.; Xiao, Y.; Yang, W.; Qian, X.H.; Yang, Y.J. Super-Resolution Monitoring of Mitochondrial Dynamics upon Time-Gated Photo-Triggered Release of Nitric Oxide. Anal. Chem. 2018, 90, 2164–2169. [Google Scholar] [CrossRef]
- Ieda, N.; Oka, Y.; Yoshihara, T.; Tobita, S.; Sasamori, T.; Kawaguchi, M.; Nakagawa, H. Structure-efficiency relationship of photoinduced electron transfer-triggered nitric oxide releasers. Sci. Rep. 2019, 9, 1430. [Google Scholar] [CrossRef]
- Parisi, C.; Failla, M.; Fraix, A.; Rolando, B.; Gianquinto, E.; Spyrakis, F.; Gazzano, E.; Riganti, C.; Lazzarato, L.; Fruttero, R.; et al. Fluorescent Nitric Oxide Photodonors Based on BODIPY and Rhodamine Antennae. Chem. Eur. J. 2019, 25, 11080–11084. [Google Scholar] [CrossRef]
- Shen, Z.; He, K.; Ding, Z.; Zhang, M.; Yu, Y.; Hu, J. Visible-Light-Triggered Self-Reporting Release of Nitric Oxide (NO) for Bacterial Biofilm Dispersal. Macromolecules 2019. [Google Scholar] [CrossRef]
- Arora, D.P.; Hossain, S.; Xu, Y.; Boon, E.M. Nitric Oxide Regulation of Bacterial Biofilms. Biochemistry 2015, 54, 3717–3728. [Google Scholar] [CrossRef]
- del Pozo, J.; Patel, R. The Challenge of Treating Biofilm-associated Bacterial Infections. Clin. Pharmacol. Ther. 2007, 82, 204–209. [Google Scholar] [CrossRef]
- Lebeaux, D.; Ghigo, J.-M.; Beloin, C. Biofilm-Related Infections: Bridging the Gap between Clinical Management and Fundamental Aspects of Recalcitrance toward Antibiotics. Microbiol. Mol. Biol. Rev. 2014, 78, 510–543. [Google Scholar] [CrossRef] [PubMed]
- Hall-Stoodley, L.; Costerton, J.W.; Stoodley, P. Bacterial biofilms: From the Natural environment to infectious diseases. Nat. Rev. Microbiol. 2004, 2, 95–108. [Google Scholar] [CrossRef] [PubMed]
- Howlin, R.P.; Cathie, K.; Hall-Stoodley, L.; Cornelius, V.; Duignan, C.; Allan, R.N.; Fernandez, B.O.; Barraud, N.; Bruce, K.D.; Jefferies, J.; et al. Low-Dose Nitric Oxide as Targeted Anti-biofilm Adjunctive Therapy to Treat Chronic Pseudomonas aeruginosa Infection in Cystic Fibrosis. Mol. Ther. 2017, 25, 2104–2116. [Google Scholar] [CrossRef] [PubMed]
- Sadrearhami, Z.; Thuy-Khanh, N.; Namivandi-Zangeneh, R.; Jung, K.; Wong, E.H.H.; Boyer, C. Recent advances in nitric oxide delivery for antimicrobial applications using polymer-based systems. J. Mater. Chem. B 2018, 6, 2945–2959. [Google Scholar] [CrossRef]
- Barraud, N.; Hassett, D.J.; Hwang, S.H.; Rice, S.A.; Kjelleberg, S.; Webb, J.S. Involvement of nitric oxide in biofilm dispersal of Pseudomonas aeruginosa. J. Bacteriol. 2006, 188, 7344–7353. [Google Scholar] [CrossRef]
- Nicolas, B.; Kelso, M.J.; Rice, S.A.; Kjelleberg, S. Nitric oxide: A key mediator of biofilm dispersal with applications in infectious diseases. Curr. Pharm. Des. 2015, 21, 31–42. [Google Scholar]
- Namivandi-Zangeneh, R.; Sadrearhami, Z.; Bagheri, A.; Maeva, S.-N.; Ho, K.K.K.; Kumar, N.; Wong, E.H.H.; Boyer, C. Nitric Oxide-Loaded Antimicrobial Polymer for the Synergistic Eradication of Bacterial Biofilm. ACS Macro Lett. 2018, 7, 592–597. [Google Scholar] [CrossRef]
- Ahonen, M.J.R.; Suchyta, D.J.; Zhu, H.Y.; Schoenfisch, M.H. Nitric Oxide-Releasing Alginates. Biomacromolecules 2018, 19, 1189–1197. [Google Scholar] [CrossRef]
- Xu, L.-C.; Wo, Y.; Meyerhoff, M.E.; Siedlecki, C.A. Inhibition of bacterial adhesion and biofilm formation by dual functional textured and nitric oxide releasing surfaces. Acta Biomater. 2017, 51, 53–65. [Google Scholar] [CrossRef]
- Singha, P.; Locklin, J.; Handa, H. A review of the recent advances in antimicrobial coatings for urinary catheters. Acta Biomater. 2017, 50, 20–40. [Google Scholar] [CrossRef]
- Jones, A.; Pant, J.; Lee, E.; Goudie, M.J.; Gruzd, A.; Mansfield, J.; Mandal, A.; Sharma, S.; Handa, H. Nitric oxide-releasing antibacterial albumin plastic for biomedical applications. J. Biomed. Mater. Res. Part A 2018, 106, 1535–1542. [Google Scholar] [CrossRef]
- Wang, X.W.; Jolliffe, A.; Carr, B.; Zhang, Q.; Bilger, M.; Cui, Y.; Wu, J.F.; Wang, X.L.; Mahoney, M.; Rojas-Pena, A.; et al. Nitric oxide-releasing semi-crystalline thermoplastic polymers: Preparation, characterization and application to devise anti-inflammatory and bactericidal implants. Biomater. Sci. 2018, 6, 3189–3201. [Google Scholar] [CrossRef]
- Lautner, G.; Stringer, B.; Brisbois, E.J.; Meyerhoff, M.E.; Schwendeman, S.P. Controlled light-induced gas phase nitric oxide release from S-nitrosothiol-doped silicone rubber films. Nitric Oxide-Biol. Chem. 2019, 86, 31–37. [Google Scholar] [CrossRef]
- Malone-Povolny, M.J.; Schoenfisch, M.H. Extended Nitric Oxide-Releasing Polyurethanes via S-Nitrosothiol-Modified Mesoporous Silica Nanoparticles. ACS Appl. Mater. Interface 2019, 11, 12216–12223. [Google Scholar] [CrossRef]
- Hopkins, S.P.; Frost, M.C. Synthesis and Characterization of Controlled Nitric Oxide Release from S-Nitroso-N-Acetyl-d-Penicillamine Covalently Linked to Polyvinyl Chloride (SNAP-PVC). Bioengineering 2018, 5, 72. [Google Scholar] [CrossRef]
- Wo, Y.; Xu, C.; Li, Z.; Matzger, A.J.; Meyerhoffa, M.E.; Siedlecki, C.A. Antimicrobial nitric oxide releasing surfaces based on S-nitroso-N-acetylpenicillamine impregnated polymers combined with submicron-textured surface topography. Biomater. Sci. 2017, 5, 1265–1278. [Google Scholar] [CrossRef]
- Maitz, M.F. Applications of synthetic polymers in clinical medicine. Biosurf. Biotribol. 2015, 1, 161–176. [Google Scholar] [CrossRef]
- Teo, A.J.T.; Mishra, A.; Park, I.; Kim, Y.-J.; Park, W.-T.; Yoon, Y.-J. Polymeric Biomaterials for Medical Implants and Devices. ACS Biomater. Sci. Eng. 2016, 2, 454–472. [Google Scholar] [CrossRef]
- Zhou, Y.; Tan, J.; Wu, J.; Zhang, Q.; Andre, J.; Xi, C.; Chen, Z.; Meyerhoff, M.E. Nitric oxide releasing poly(vinylidene fluoride-co-hexafluoropropylene) films using a fluorinated nitric oxide donor to greatly decrease chemical leaching. Acta Biomater. 2019, 90, 112–121. [Google Scholar] [CrossRef]
- Zhou, Y.; Zhang, Q.; Wu, J.; Xi, C.; Meyerhoff, M.E. Synthesis and characterization of a fluorinated S-nitrosothiol as the nitric oxide donor for fluoropolymer-based biomedical device applications. J. Mater. Chem. B 2018, 6, 6142–6152. [Google Scholar] [CrossRef]
- Cho, W.K.; Kong, B.; Choi, I.S. Highly Efficient Non-Biofouling Coating of Zwitterionic Polymers: Poly((3-(methacryloylamino)propyl)-dimethyl(3-sulfopropyl)ammonium hydroxide). Langmuir 2007, 23, 5678–5682. [Google Scholar] [CrossRef]
- Chen, S.; Li, L.; Zhao, C.; Zheng, J. Surface hydration: Principles and applications toward low-fouling/nonfouling biomaterials. Polymer 2010, 51, 5283–5293. [Google Scholar] [CrossRef]
- Ladd, J.; Zhang, Z.; Chen, S.; Hower, J.C.; Jiang, S. Zwitterionic Polymers Exhibiting High Resistance to Nonspecific Protein Adsorption from Human Serum and Plasma. Biomacromolecules 2008, 9, 1357–1361. [Google Scholar] [CrossRef]
- Liu, Q.; Singha, P.; Handa, H.; Locklin, J. Covalent Grafting of Antifouling Phosphorylcholine-Based Copolymers with Antimicrobial Nitric Oxide Releasing Polymers to Enhance Infection-Resistant Properties of Medical Device Coatings. Langmuir 2017, 33, 13105–13113. [Google Scholar] [CrossRef]
- Devine, R.; Singha, P.; Handa, H. Versatile biomimetic medical device surface: Hydrophobin coated, nitric oxide-releasing polymer for antimicrobial and hemocompatible applications. Biomater. Sci. 2019, 7, 3438–3449. [Google Scholar] [CrossRef]
- Bechert, D.W.; Bruse, M.; Hage, W. Experiments with three-dimensional riblets as an idealized model of shark skin. Exp. Fluids 2000, 28, 403–412. [Google Scholar] [CrossRef]
- Scardino, A.J.; Hudleston, D.; Peng, Z.; Paul, N.A.; de Nys, R. Biomimetic characterisation of key surface parameters for the development of fouling resistant materials. Biofouling 2009, 25, 83–93. [Google Scholar] [CrossRef]
- Barthlott, W.; Neinhuis, C. Purity of the sacred lotus, or escape from contamination in biological surfaces. Planta 1997, 202, 1–8. [Google Scholar] [CrossRef]
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rong, F.; Tang, Y.; Wang, T.; Feng, T.; Song, J.; Li, P.; Huang, W. Nitric Oxide-Releasing Polymeric Materials for Antimicrobial Applications: A Review. Antioxidants 2019, 8, 556. https://doi.org/10.3390/antiox8110556
Rong F, Tang Y, Wang T, Feng T, Song J, Li P, Huang W. Nitric Oxide-Releasing Polymeric Materials for Antimicrobial Applications: A Review. Antioxidants. 2019; 8(11):556. https://doi.org/10.3390/antiox8110556
Chicago/Turabian StyleRong, Fan, Yizhang Tang, Tengjiao Wang, Tao Feng, Jiang Song, Peng Li, and Wei Huang. 2019. "Nitric Oxide-Releasing Polymeric Materials for Antimicrobial Applications: A Review" Antioxidants 8, no. 11: 556. https://doi.org/10.3390/antiox8110556
APA StyleRong, F., Tang, Y., Wang, T., Feng, T., Song, J., Li, P., & Huang, W. (2019). Nitric Oxide-Releasing Polymeric Materials for Antimicrobial Applications: A Review. Antioxidants, 8(11), 556. https://doi.org/10.3390/antiox8110556






