Oxygen-Sensitivity and Pulmonary Selectivity of Vasodilators as Potential Drugs for Pulmonary Hypertension
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Efficacy and Potency as Vasodilators
3.2. Pulmonary and Oxygen Selectivity
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Simonneau, G.; Montani, D.; Celermajer, D.S.; Denton, C.P.; Gatzoulis, M.A.; Krowka, M.; Williams, P.G.; Souza, R. Haemodynamic definitions and updated clinical classification of pulmonary hypertension. Eur. Respir. J. 2019, 53. [Google Scholar] [CrossRef] [PubMed]
- Humbert, M.; Guignabert, C.; Bonnet, S.; Dorfmüller, P.; Klinger, J.R.; Nicolls, M.R.; Olschewski, A.J.; Pullamsetti, S.S.; Schermuly, R.T.; Stenmark, K.R.; et al. Pathology and pathobiology of pulmonary hypertension: State of the art and research perspectives. Eur. Respir. J. 2019, 53, 1801887. [Google Scholar] [CrossRef] [PubMed]
- Southgate, L.; Machado, R.D.; Gräf, S.; Morrell, N.W. Molecular genetic framework underlying pulmonary arterial hypertension. Nat. Rev. Cardiol. 2020, 1, 85–95. [Google Scholar] [CrossRef] [PubMed]
- Lau, E.M.T.; Giannoulatou, E.; Celermajer, D.S.; Humbert, M. Epidemiology and treatment of pulmonary arterial hypertension. Nat. Rev. Cardiol. 2017, 14, 603–614. [Google Scholar] [CrossRef] [PubMed]
- Stewart, D.J.; Levy, R.D.; Cernacek, P.; Langleben, D. Increased plasma endothelin-1 in pulmonary hypertension: Marker or mediator of disease? Ann. Intern. Med. 1991, 114, 464–469. [Google Scholar] [CrossRef] [PubMed]
- Herve, P.; Launay, J.M.; Scrobohaci, M.L.; Brenot, F.; Simonneau, G.; Petitpretz, P.; Poubeau, P.; Cerrina, J.; Duroux, P.; Drouet, L. Increased plasma serotonin in primary pulmonary hypertension. Am. J. Med. 1995, 99, 249–254. [Google Scholar] [CrossRef]
- Christman, B.W.; McPherson, C.D.; Newman, J.H.; King, G.A.; Bernard, G.R.; Groves, B.M.; Loyd, J.E. An imbalance between the excretion of thromboxane and prostacyclin metabolites in pulmonary hypertension. N. Engl. J. Med. 1992, 327, 70–75. [Google Scholar] [CrossRef]
- Sahay, S.; Humbert, M.; Sitbon, O. Medical Treatment of Pulmonary Arterial Hypertension. Semin. Respir. Crit. Care Med. 2017, 38, 686–700. [Google Scholar] [CrossRef]
- MacKenzie, A.M.; Peacock, A.J. Medical Therapies for the Treatment of Pulmonary Arterial Hypertension: How Do We Choose? Curr. Hypertens. Rep. 2015, 17, 56. [Google Scholar] [CrossRef]
- Cogolludo, A.; Moreno, L.; Frazziano, G.; Moral-Sanz, J.; Menendez, C.; Castaneda, J.; Gonzalez, C.; Villamor, E.; Perez-Vizcaino, F. Activation of neutral sphingomyelinase is involved in acute hypoxic pulmonary vasoconstriction. Cardiovasc. Res. 2009, 82, 296–302. [Google Scholar] [CrossRef]
- Tonelli, A.R.; Alnuaimat, H.; Mubarak, K. Pulmonary vasodilator testing and use of calcium channel blockers in pulmonary arterial hypertension. Respir. Med. 2010, 104, 481–496. [Google Scholar] [CrossRef] [PubMed]
- Sakao, S.; Tatsumi, K.; Voelkel, N.F. Reversible or irreversible remodeling in pulmonary arterial hypertension. Am. J. Respir. Cell Mol. Biol. 2010, 43, 629–634. [Google Scholar] [CrossRef] [PubMed]
- Connolly, M.J.; Aaronson, P.I. Key role of the RhoA/Rho kinase system in pulmonary hypertension. Pulm. Pharmacol. Ther. 2011, 24, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Zungu-Edmondson, M.; Shults, N.V.; Melnyk, O.; Suzuki, Y.J. Natural reversal of pulmonary vascular remodeling and right ventricular remodeling in SU5416/hypoxia-treated Sprague-Dawley rats. PLoS ONE 2017, 12, e0182551. [Google Scholar] [CrossRef]
- Cogolludo, A.; Moreno, L.; Lodi, F.; Tamargo, J.; Perez-Vizcaino, F. Postnatal maturational shift from PKCzeta and voltage-gated K+ channels to RhoA/Rho kinase in pulmonary vasoconstriction. Cardiovasc. Res. 2005, 66, 84–93. [Google Scholar] [CrossRef]
- McMurtry, I.F.; Abe, K.; Ota, H.; Fagan, K.A.; Oka, M. Rho kinase-mediated vasoconstriction in pulmonary hypertension. Adv. Exp. Med. Biol. 2010, 661, 299–308. [Google Scholar]
- Cogolludo, A.; Moreno, L.; Villamor, E. Mechanisms controlling vascular tone in pulmonary arterial hypertension: Implications for vasodilator therapy. Pharmacology 2007, 79, 65–75. [Google Scholar] [CrossRef]
- Aaronson, P.I.; Robertson, T.P.; Knock, G.A.; Becker, S.; Lewis, T.H.; Snetkov, V.; Ward, J.P.T. Hypoxic pulmonary vasoconstriction: Mechanisms and controversies. J. Physiol. 2006, 570, 53–58. [Google Scholar] [CrossRef]
- Ried, M.; Potzger, T.; Neu, R.; Sziklavari, Z.; Szoke, T.; Liebold, A.; Hofmann, H.S.; Hoenicka, M. Combination of sildenafil and bosentan for pulmonary hypertension in a human ex vivo model. Cardiovasc. Drugs Ther. 2014, 28, 45–51. [Google Scholar] [CrossRef]
- Moreno, L.; Losada, B.; Cogolludo, A.; Lodi, F.; Lugnier, C.; Villamor, E.; Moro, M.; Tamargo, J.; Perez-Vizcaino, F. Postnatal maturation of phosphodiesterase 5 (PDE5) in piglet pulmonary arteries: Activity, expression, effects of PDE5 inhibitors, and role of the nitric oxide/cyclic GMP pathway. Pediatr. Res. 2004, 56, 563–570. [Google Scholar] [CrossRef][Green Version]
- Bawankule, D.U.; Sathishkumar, K.; Sardar, K.K.; Chanda, D.; Krishna, A.V.; Prakash, V.R.; Mishra, S.K. BAY 41-2272 [5-cyclopropyl-2-[1-(2-fluoro-benzyl)-1H-pyrazolo[3,4-b]pyridine-3-yl]pyrimidin-4 -ylamine]-induced dilation in ovine pulmonary artery: Role of sodium pump. J. Pharmacol. Exp. Ther. 2005, 314, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Moreno, L.; Gonzalez-Luis, G.; Cogolludo, A.; Lodi, F.; Lopez-Farre, A.; Tamargo, J.; Villamor, E.; Perez-Vizcaino, F. Soluble guanylyl cyclase during postnatal porcine pulmonary maturation. Am. J. Physiol. Lung Cell. Mol. Physiol. 2005, 288, L125–L130. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Chamorro, V.; Morales-Cano, D.; Milara, J.; Barreira, B.; Moreno, L.; Callejo, M.; Mondejar-Parreno, G.; Esquivel-Ruiz, S.; Cortijo, J.; Cogolludo, A.; et al. Riociguat versus sildenafil on hypoxic pulmonary vasoconstriction and ventilation/perfusion matching. PLoS ONE 2018, 13, e0191239. [Google Scholar] [CrossRef] [PubMed]
- Ballester, E.; Roca, J.; Rodriguez-Roisin, R.; Agusti-Vidal, A. Effect of nifedipine on arterial hypoxaemia occurring after methacholine challenge in asthma. Thorax 1986, 41, 468–472. [Google Scholar] [CrossRef] [PubMed]
- Ghofrani, H.A.; Voswinckel, R.; Reichenberger, F.; Olschewski, H.; Haredza, P.; Karadas, B.; Schermuly, R.T.; Weissmann, N.; Seeger, W.; Grimminger, F. Differences in hemodynamic and oxygenation responses to three different phosphodiesterase-5 inhibitors in patients with pulmonary arterial hypertension—A randomized prospective study. J. Am. Coll. Cardiol. 2004, 44, 1488–1496. [Google Scholar]
- Rothermund, L.; Friebe, A.; Paul, M.; Koesling, D.; Kreutz, R. Acute blood pressure effects of YC-1-induced activation of soluble guanylyl cyclase in normotensive and hypertensive rats. Br. J. Pharmacol. 2000, 130, 205–208. [Google Scholar] [CrossRef]
- Evgenov, O.V.; Ichinose, F.; Evgenov, N.V.; Gnoth, M.J.; Falkowski, G.E.; Chang, Y.C.; Bloch, K.D.; Zapol, W.M. Soluble guanylate cyclase activator reverses acute pulmonary hypertension and augments the pulmonary vasodilator response to inhaled nitric oxide in awake lambs. Circulation 2004, 110, 2253–2259. [Google Scholar] [CrossRef]
- Grimminger, F.; Weimann, G.; Frey, R.; Voswinckel, R.; Thamm, M.; Bolkow, D.; Weissmann, N.; Muck, W.; Unger, S.; Wensing, G.; et al. First acute haemodynamic study of soluble guanylate cyclase stimulator riociguat in pulmonary hypertension. Eur. Respir. J. 2009, 33, 785–792. [Google Scholar] [CrossRef]
- Ghofrani, H.A.; Staehler, G.; Grunig, E.; Halank, M.; Mitrovic, V.; Unger, S.; Mueck, W.; Frey, R.; Grimminger, F.; Schermuly, R.T.; et al. Acute effects of riociguat in borderline or manifest pulmonary hypertension associated with chronic obstructive pulmonary disease. Pulm. Circ. 2015, 5, 296–304. [Google Scholar] [CrossRef]
- PerezVizcaino, F.; Villamor, E.; Moro, M.; Tamargo, J. Pulmonary versus systemic effects of vasodilator drugs: An in vitro study in isolated intrapulmonary and mesenteric arteries of neonatal piglets. Eur. J. Pharmacol. 1996, 314, 91–98. [Google Scholar] [CrossRef]
- Melot, C.; Hallemans, R.; Naeije, R.; Mols, P.; Lejeune, P. Deleterious Effect of Nifedipine on Pulmonary Gas-Exchange in Chronic Obstructive Pulmonary-Disease. Am. Rev. Respir. Dis. 1984, 130, 612–616. [Google Scholar] [PubMed]
- Wanstall, J.C. Vasorelaxation by pinacidil in isolated perfused lungs is enhanced in rats with hypoxic pulmonary hypertension but is dependent on the constrictor. Physiol. Res. 1995, 44, 1–6. [Google Scholar] [PubMed]
- Mondejar-Parreno, G.; Barreira, B.; Callejo, M.; Morales-Cano, D.; Barrese, V.; Esquivel-Ruiz, S.; Olivencia, M.A.; Macias, M.; Moreno, L.; Greenwood, I.A.; et al. Uncovered Contribution of Kv7 Channels to Pulmonary Vascular Tone in Pulmonary Arterial Hypertension. Hypertension 2020, 76, 1134–1146. [Google Scholar] [CrossRef] [PubMed]
- Barbera, J.A.; Blanco, I. Pulmonary Hypertension in Patients with Chronic Obstructive Pulmonary Disease Advances in Pathophysiology and Management. Drugs 2009, 69, 1153–1171. [Google Scholar] [CrossRef] [PubMed]
- Blanco, I.; Gimeno, E.; Munoz, P.A.; Pizarro, S.; Gistau, C.; Rodriguez-Roisin, R.; Roca, J.; Barbera, J.A. Hemodynamic and Gas Exchange Effects of Sildenafil in Patients with Chronic Obstructive Pulmonary Disease and Pulmonary Hypertension. Am. J. Resp. Crit. Care 2010, 181, 270–278. [Google Scholar] [CrossRef] [PubMed]
- Harrington, L.S.; Moreno, L.; Reed, A.; Wort, S.J.; Desvergne, B.; Garland, C.; Zhao, L.; Mitchell, J.A. The PPAR beta/delta Agonist GW0742 Relaxes Pulmonary Vessels and Limits Right Heart Hypertrophy in Rats with Hypoxia-Induced Pulmonary Hypertension. PLoS ONE 2010, 5, e9526. [Google Scholar] [CrossRef] [PubMed]
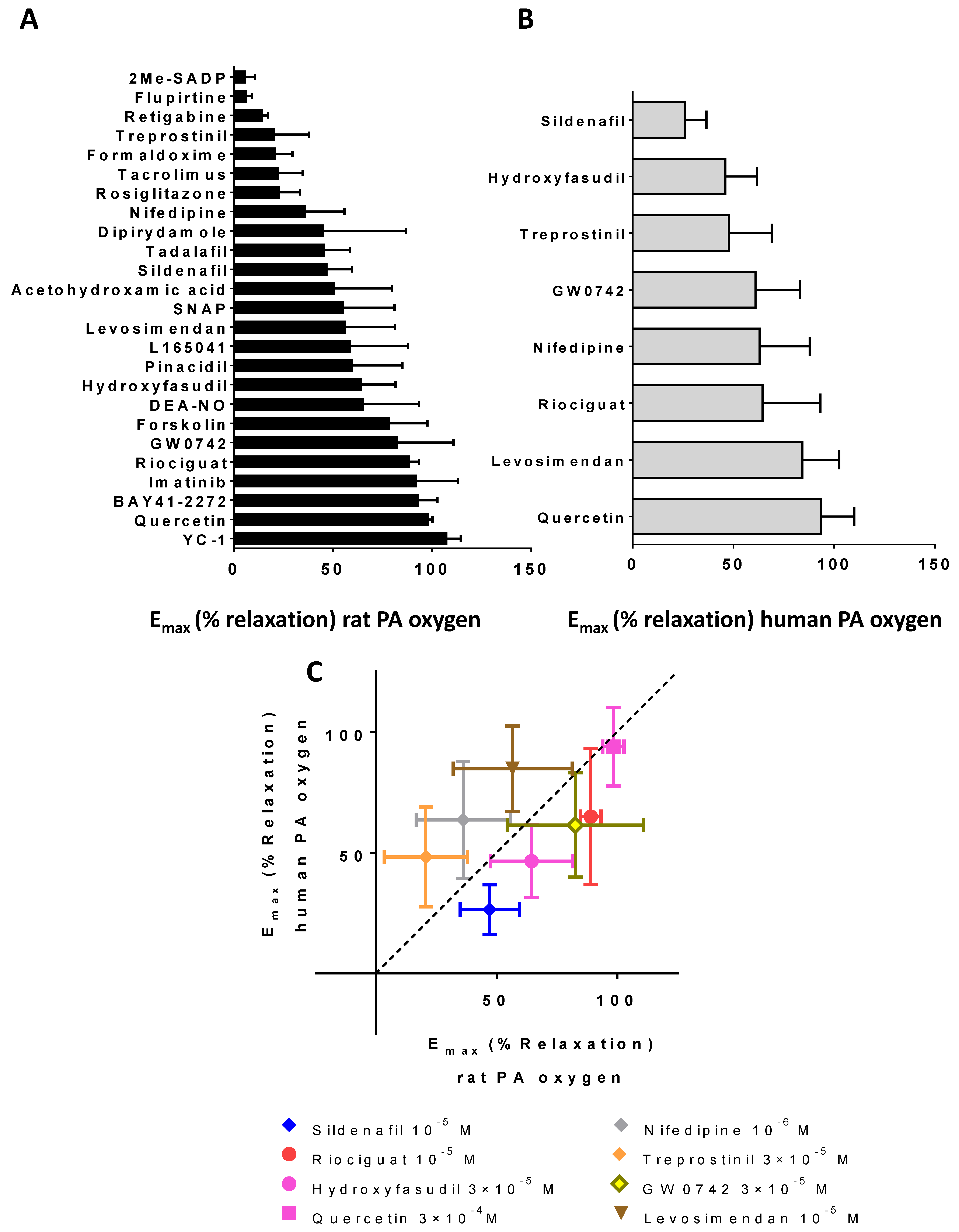
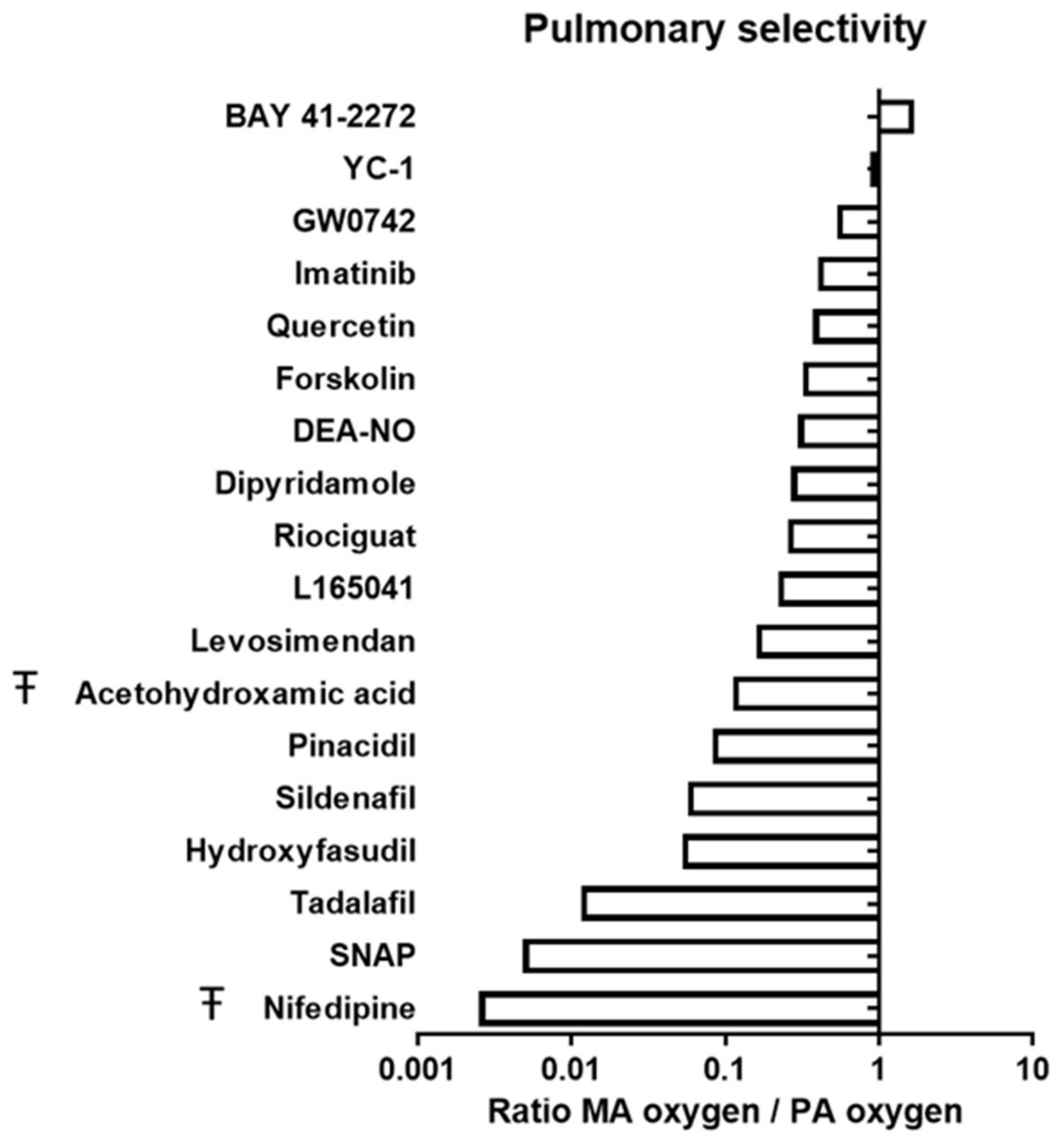
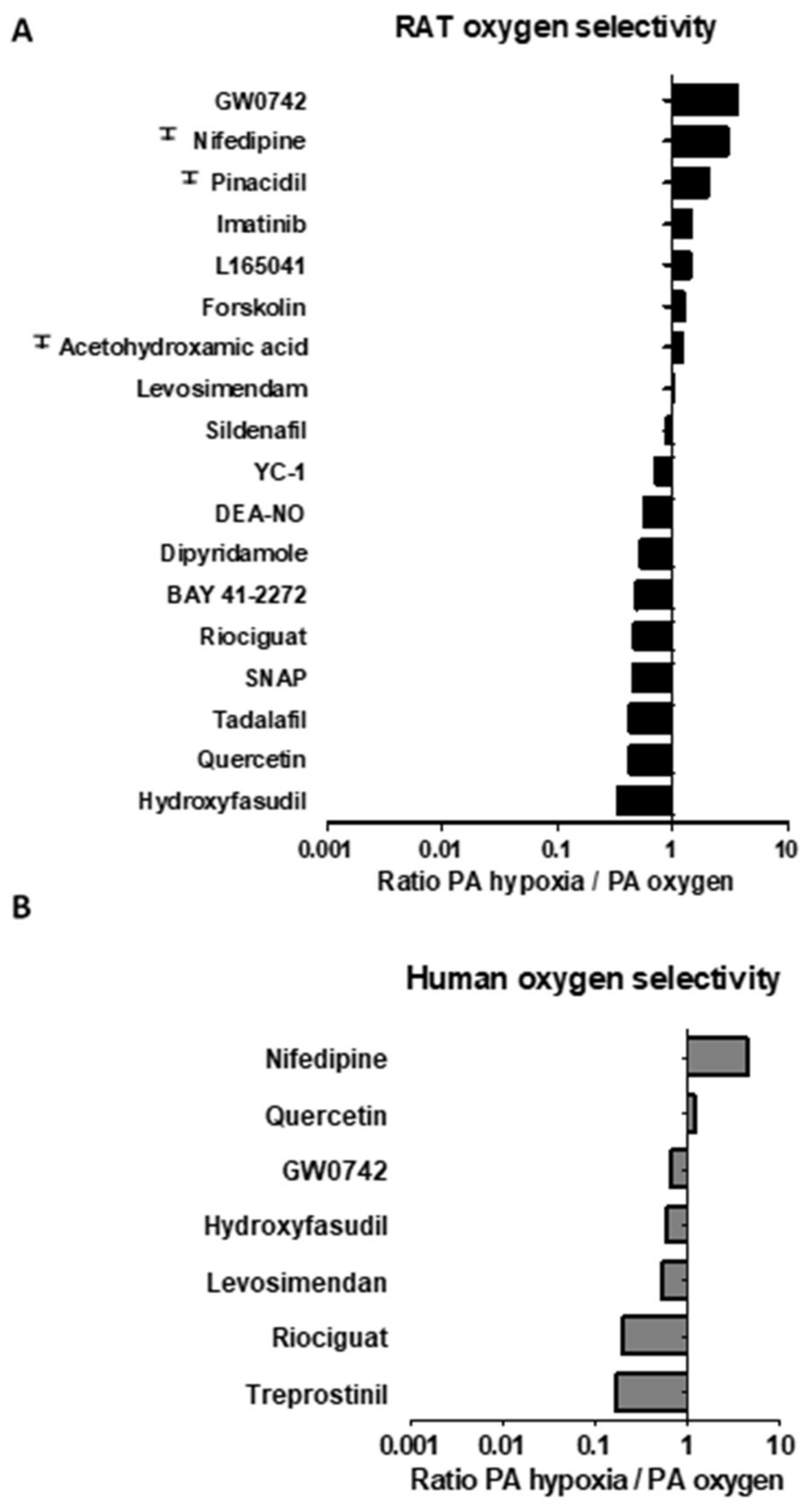
| Drug | Rat Mesenteric Artery | Rat Pulmonary Artery | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Hypoxia | Oxygen | ||||||||
| pIC50 | Emax * | n | pIC50 | Emax | n | pIC50 | Emax * | N | |
| Sildenafil | 6.18 ± 0.59 | ≥74.6 ± 22.7 a | 5 | 4.98 ± 1.08 | ≥49.9 ± 20.7 | 5 | 4.94 ± 1.44 | ≥47.1 ± 12.3 | 7 |
| Tadalafil | 7.01 ± 0.59 a | ≥84.9 ± 17.6 a | 4 | 5.44 ± 0.92 | ≥51.8 ± 21.0 | 3 | 5.08 ± 0.80 | ≥45.7 ± 12.8 | 4 |
| Dipyridamole | 5.37 ± 0.27 | ≥62.6 ± 19.1 | 3 | 5.07 ± 0.37 | ≥51.5 ± 13.5 | 3 | 4.80 ± 0.71 | ≥45.4 ± 41.3 | 3 |
| YC-1 | 6.38 ± 0.19 | 110.5 ± 11.3 | 5 | 6.46 ± 0.17 | 107.4 ± 4.9 | 6 | 6.32 ± 0.15 | 107.7 ± 16.5 | 6 |
| BAY 41-2272 | 7.42 ± 0.26 | 91.9 ± 17.1 | 6 | 7.96 ± 0.17 c | 111.4 ± 10.0 | 6 | 7.65 ± 0.20 | 93.1 ± 23.4 | 6 |
| Riociguat | 7.45 ± 0.19 b | 107.8 ± 12.8 a | 6 | 7.19 ± 0.21 c | 89.9 ± 14.5 | 6 | 6.86 ± 0.09 | 89.0 ± 4.3 | 6 |
| Hydroxyfasudil | 6.03 ± 0.13 b | 95.1 ± 3.7 b | 7 | 5.23 ± 0.27 d | ≥70.2 ± 26.0 | 7 | 4.75 ± 0.19 | ≥64.5 ± 17.0 | 8 |
| Imatinib | 5.70 ± 0.22 b | 101.9 ± 20.5 | 5 | 5.13 ± 0.18 | ≥88.3 ± 18.2 | 5 | 5.30 ± 0.17 | ≥92.3 ± 20.8 | 6 |
| Quercetin | 5.71 ± 0.09 b | 102.3 ± 6.7 | 6 | 5.65 ± 0.16 d | 111.9 ± 12.7 c | 6 | 5.28 ± 0.10 | 98.3 ± 4.4 | 6 |
| GW0742 | 5.44 ± 0.20 | 94.3 ± 20.3 | 7 | 4.60 ± 0.22 d | ≥57.9 ± 32.8 | 9 | 5.17 ± 0.29 | ≥82.6 ± 28.3 | 10 |
| L165041 | 5.27 ± 0.26 b | 94.1 ± 34.0 | 8 | 4.47 ± 0.29 | ≥50.0 ± 21.1 | 7 | 4.62 ± 0.22 | ≥59.0 ± 28.9 | 7 |
| Rosiglitazone | 4.78 ± 0.19 | ≥72.6 ± 2 | 4 | N/A | ≥39.2 ± 2.9 | 4 | N/A | ≥23.3 ± 10.1 | 4 |
| SNAP | 6.57 ± 0.71 b | 81.9 ± 29.3 | 4 | 4.60 ± 0.29 | ≥61.9 ± 13.0 | 4 | 4.25 ± 0.58 | ≥55.6 ± 25.5 | 4 |
| DEA-NO | 6.24 ± 0.17 b | 94.7 ± 18.7 | 5 | 5.96 ± 0.16 | 83.9 ± 19.6 | 5 | 5.71 ± 0.16 | ≥65.4 ± 28.0 | 3 |
| Acetohydroxamic acid | 3.70 ± 0.28 | ≥68.2 ± 12.9 | 3 | N/A | ≥44.8 ± 10.8 | 3 | N/A | ≥51.0 ± 28.9 | 3 |
| Formaldoxime | N/A | ≥43.1 ± 20.1 | 5 | N/A | ≥47.1 ± 22.9 | 5 | N/A | ≥21.2 ± 8.4 | 3 |
| Treprostinil | 6.05 ± 0.41 | ≥61.9 ± 28.2 b | 7 | N/A | ≥24.5 ± 23.0 | 6 | N/A | ≥20.6 ± 17.3 | 8 |
| Forskolin | 7.25 ± 0.07 b | 96.6 ± 5.5 | 3 | 6.65 ± 0.05 | ≥83.2 ± 3.1 | 3 | 6.76 ± 0.08 | ≥78.9 ± 18.7 | 3 |
| Nifedipine | 8.78 ± 0.27 | 97.3 ± 13.8 b | 8 | N/A | ≥28.3 ± 20.2 | 8 | N/A | ≥36.2 ± 19.6 | 9 |
| Retigabine | 5.14 ± 0.18 | 93.0 ± 10.0 b | 3 | N/A | ≥8.1 ± 6.4 | 3 | N/A | ≥14.4 ± 2.7 | 3 |
| Flupirtine | 4.92 ± 0.48 | ≥70.1 ± 18.7 b | 3 | N/A | ≥5.6 ± 12.3 | 3 | N/A | ≥6.4 ± 2.7 | 3 |
| Pinacidil | 6.49 ± 0.24 b | 102.3 ± 3.0 b | 5 | N/A | ≥46.4 ± 23.5 | 5 | 5.40 ± 0.15 | ≥60.0 ± 25.0 | 5 |
| 2Me-SADP | N/A | ≥15.5 ± 11.8 | 4 | N/A | ≥25.4 ± 21.2 | 4 | N/A | ≥6.1 ± 4.6 | 4 |
| Tacrolimus | 5.01 ± 1.04 | ≥50.39 ± 16.7 a | 3 | N/A | ≥37.2 ± 5.4 | 3 | N/A | ≥22.8 ± 11.9 | 3 |
| Levosimendan | 6.28 ± 0.28 | 91.3 ± 16.2 a | 4 | 5.47 ± 0.62 | ≥67.1 ± 24.4 | 7 | 5.48 ± 0.18 | ≥56.6 ± 24.6 | 15 |
| Drug | Human Pulmonary Artery Hipoxia | Human Pulmonary Artery Oxygen | ||||
|---|---|---|---|---|---|---|
| pIC50 | Emax * | n | pIC50 | Emax * | n | |
| Hydroxyfasudil | 4.80 ± 0.59 | ≥55.2 ± 28.0 | 6 | 4.58 ± 0.53 | ≥46.5 ± 15.2 | 5 |
| Nifedipine | 5.16 ± 0.57 | ≥53.9 ± 21.9 | 6 | 5.82 ± 0.62 | ≥63.5 ± 24.3 | 6 |
| Sildenafil | 5.09 ± 1.05 | ≥48.0 ± 9.9 a | 4 | N/A | ≥26.4 ± 10.3 | 5 |
| Quercetin | 4.47 ± 0.27 | 88.8 ± 33.5 | 6 | 4.56 ± 0.14 | 93.8 ± 16.2 | 8 |
| GW0742 | 4.79 ± 0.38 | ≥69.0 ± 31.4 | 3 | 4.63 ± 0.15 | ≥61.5 ± 21.6 | 5 |
| Levosimendan | 6.54 ± 0.49 | 74.8 ± 35.3 | 5 | 6.27 ± 0.24 | 84.7 ± 17.7 | 5 |
| Riociguat | 6.62 ± 0.23 b | ≥79.3 ± 17.4 | 11 | 5.93 ± 0.39 | ≥65.9 ± 28.2 | 10 |
| Treprostinil | 5.55 ± 0.37 | ≥58.0 ± 26.9 | 3 | 4.79 ± 0.52 | ≥48.2 ± 20.8 | 5 |
| Drug | Rat Mesenteric Artery | Rat Pulmonary Artery | ||||
|---|---|---|---|---|---|---|
| Hypoxia | Oxygen | |||||
| pIC30 | n | pIC30 | N | pIC30 | n | |
| Rosiglitazone | 5.18 ± 0.20 b | 4 | 4.65 ± 0.10 | 4 | N/A | 4 |
| Acetohydroxamic acid | 4.60 ± 0.29 a | 3 | 3.56 ± 0.28 | 3 | 3.65 ± 0.36 | 3 |
| Formaldoxime | 4.85 ± 0.68 | 5 | 4.63 ± 0.36 | 5 | N/A | 3 |
| Treprostinil | 6.97 ± 0.47 | 7 | 5.39 ± 0.81 | 6 | N/A | 8 |
| Nifedipine | 9.03 ± 0.37 b | 8 | 5.96 ± 1.16 | 8 | 6.43 ± 0.54 | 9 |
| Pinacidil | 6.90 ± 0.30 b | 5 | 5.78 ± 0.39 | 5 | 6.10 ± 0.33 | 5 |
| Tacrolimus | 6.78 ± 0.68 | 3 | 5.61 ± 0.33 | 3 | N/A | 3 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Morales-Cano, D.; Barreira, B.; De Olaiz Navarro, B.; Callejo, M.; Mondejar-Parreño, G.; Esquivel-Ruiz, S.; Lorente, J.A.; Moreno, L.; Barberá, J.A.; Cogolludo, Á.; et al. Oxygen-Sensitivity and Pulmonary Selectivity of Vasodilators as Potential Drugs for Pulmonary Hypertension. Antioxidants 2021, 10, 155. https://doi.org/10.3390/antiox10020155
Morales-Cano D, Barreira B, De Olaiz Navarro B, Callejo M, Mondejar-Parreño G, Esquivel-Ruiz S, Lorente JA, Moreno L, Barberá JA, Cogolludo Á, et al. Oxygen-Sensitivity and Pulmonary Selectivity of Vasodilators as Potential Drugs for Pulmonary Hypertension. Antioxidants. 2021; 10(2):155. https://doi.org/10.3390/antiox10020155
Chicago/Turabian StyleMorales-Cano, Daniel, Bianca Barreira, Beatriz De Olaiz Navarro, María Callejo, Gema Mondejar-Parreño, Sergio Esquivel-Ruiz, Jose A. Lorente, Laura Moreno, Joan A. Barberá, Ángel Cogolludo, and et al. 2021. "Oxygen-Sensitivity and Pulmonary Selectivity of Vasodilators as Potential Drugs for Pulmonary Hypertension" Antioxidants 10, no. 2: 155. https://doi.org/10.3390/antiox10020155
APA StyleMorales-Cano, D., Barreira, B., De Olaiz Navarro, B., Callejo, M., Mondejar-Parreño, G., Esquivel-Ruiz, S., Lorente, J. A., Moreno, L., Barberá, J. A., Cogolludo, Á., & Perez-Vizcaino, F. (2021). Oxygen-Sensitivity and Pulmonary Selectivity of Vasodilators as Potential Drugs for Pulmonary Hypertension. Antioxidants, 10(2), 155. https://doi.org/10.3390/antiox10020155






